Plaque
4,040 words · 13 min read
Quick Definition
A soft, sticky, colorless film of bacteria that continuously forms on teeth and along the gumline. Plaque is the primary cause of tooth decay and gum disease.
Plaque: The Definitive Guide to Your Mouth's Most Persistent Problem
Introduction
Plaque is a term you’ve likely heard countless times in the context of dental health, often with a hint of concern. But what exactly is this invisible adversary, and why does it command so much attention from dental professionals? Simply put, plaque is a soft, sticky, colorless film of bacteria that continuously forms on your teeth, restorations, and along your gumline. It’s not just a surface film; it's a complex, living biofilm teeming with millions of bacteria, their byproducts, and food debris. Think of it as a microscopic, self-assembling city of microbes constantly at work in your mouth.
While it might sound innocuous, plaque is, in fact, the primary cause of tooth decay (dental caries) and gum disease (gingivitis and periodontal disease). Its constant presence and activity are responsible for the vast majority of oral health issues faced by individuals worldwide. The statistics are stark: according to the Centers for Disease Control and Prevention (CDC), over 90% of adults in the United States have had a cavity, and nearly half of all adults aged 30 and older show signs of gum disease, both conditions largely initiated and exacerbated by plaque accumulation. Understanding plaque is not just about avoiding a dental lecture; it's about safeguarding your overall health, as poor oral hygiene linked to plaque has been associated with systemic conditions like heart disease, diabetes, and even certain types of dementia. This comprehensive guide will arm you with everything you need to know about plaque – from its formation to prevention and professional management – ensuring you have the tools to keep your smile healthy and vibrant.
Key Takeaways:
- Plaque is a continuous bacterial biofilm that forms on teeth and gumlines.
- It is colorless, soft, and sticky in its early stages, making it hard to see without disclosing agents.
- Plaque is the root cause of dental caries (cavities) and gum disease (gingivitis, periodontitis).
- If left undisturbed, plaque hardens into calculus (tartar), which cannot be removed by brushing or flossing alone.
- Regular brushing, flossing, and professional dental cleanings are essential for managing plaque.
- Dietary choices, especially sugary and starchy foods, significantly impact plaque formation and activity.
Detailed Explanation
Types and Classifications
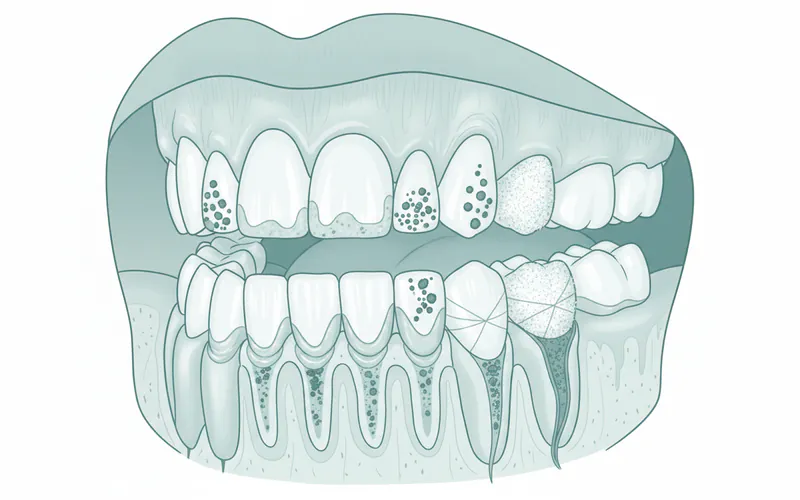
Plaque isn't a monolithic entity; it exists in different forms and locations within the mouth, each with specific implications for oral health. Understanding these classifications helps in comprehending its impact:
-
Supragingival Plaque: This type of plaque forms on the tooth surfaces above the gumline. It's the most common and visible form (when stained with a disclosing tablet). Supragingival plaque is primarily involved in initiating dental caries (cavities), as the acids it produces directly attack tooth enamel. Its composition is often dominated by aerobic (oxygen-loving) bacteria.
-
Subgingival Plaque: This is the more insidious form, developing below the gumline, within the gingival sulcus (the shallow space between the tooth and gum) and periodontal pockets (deeper spaces that form as gum disease progresses). Subgingival plaque is harder to detect and remove and is the main culprit behind gingivitis and periodontal disease. It contains a higher proportion of anaerobic (oxygen-avoiding) bacteria, which are particularly destructive to gum tissues and bone. Subgingival plaque can also be further classified into:
- Tooth-associated plaque: Firmly attached to the tooth surface, often calcifying into subgingival calculus.
- Tissue-associated plaque: Loosely attached to the soft tissues lining the periodontal pocket, highly virulent and associated with tissue destruction.
- Unattached plaque: Free-floating bacteria within the pocket.
Causes and Risk Factors
Plaque formation is a natural and continuous biological process. However, several factors can accelerate its growth and increase its harmful potential:
- Poor Oral Hygiene: This is the number one cause. Infrequent or ineffective brushing and flossing allow plaque to accumulate undisturbed, giving bacteria ample time to multiply and produce harmful acids and toxins.
- Dietary Habits: Consuming a diet rich in sugary and starchy foods and drinks (e.g., candy, soda, pastries, white bread, chips) provides the plaque bacteria with their preferred fuel source. When these bacteria metabolize sugars, they produce acids that demineralize tooth enamel, leading to caries.
- Dry Mouth (Xerostomia): Saliva plays a crucial role in oral health by neutralizing acids, washing away food particles, and providing minerals for enamel remineralization. Reduced saliva flow, often due to medications, certain medical conditions (like Sjögren's syndrome), or aging, significantly increases plaque accumulation and the risk of both caries and gum disease.
- Orthodontic Appliances: Braces, retainers, and other orthodontic devices create additional surfaces and traps for food particles and bacteria, making effective plaque removal more challenging.
- Rough Tooth Surfaces or Restorations: Chips, cracks, ill-fitting fillings or crowns, or rough enamel surfaces provide ideal attachment sites for plaque bacteria, making it harder to clean these areas effectively.
- Smoking and Tobacco Use: Tobacco products compromise the immune system, reduce blood flow to the gums, and hinder the body's ability to fight off bacterial infections. Smokers are at a significantly higher risk for severe periodontal disease and faster plaque accumulation.
- Systemic Diseases: Conditions like diabetes can impair the body's immune response, making individuals more susceptible to plaque-related infections and inflammation.
- Genetic Predisposition: While hygiene is paramount, some individuals may have a genetic predisposition that makes them more susceptible to developing gingivitis or periodontal disease in response to plaque.
Signs and Symptoms to Watch For
Since plaque is often colorless, especially in its early stages, it can be difficult to spot without specialized tools. However, its effects become noticeable as it accumulates and matures:
- A "Fuzzy" Feeling on Teeth: This is one of the earliest signs. If you run your tongue over your teeth and they don't feel smooth and clean, you're likely feeling a layer of plaque. This sensation is most pronounced in the morning or after skipping brushing.
- Bad Breath (Halitosis): The metabolic byproducts and gases produced by plaque bacteria are a common cause of persistent bad breath.
- Red, Swollen, or Tender Gums: Plaque near the gumline irritates the gingival tissues, leading to inflammation – the hallmark of gingivitis, the earliest stage of gum disease.
- Bleeding Gums: Gums that bleed easily during brushing, flossing, or even when eating certain foods are a strong indicator of gingivitis caused by plaque. This should never be considered normal.
- Increased Tooth Sensitivity: As plaque acids erode enamel, teeth can become more sensitive to hot, cold, or sweet stimuli.
- Visible Tartar/Calculus: If plaque is left undisturbed, it absorbs minerals from saliva and hardens into calculus (tartar). This yellow or brownish deposit, often seen at the gumline or between teeth, is porous and provides an even rougher surface for more plaque to accumulate. Once calculus forms, it cannot be removed by at-home methods.
Diagnosis Process — What Your Dentist Does
Dentists and dental hygienists are experts in identifying plaque and its consequences. A typical diagnostic process involves:
- Visual Inspection: During a routine check-up, your dental professional will visually inspect your teeth and gums for signs of plaque, calculus, inflammation, and caries.
- Dental Probe and Mirror: A small dental mirror helps view hard-to-reach areas, while a dental probe (scaler or explorer) can be used to feel for rough surfaces indicative of calculus or early caries. It can also measure the depth of the gingival sulcus (periodontal probing) to assess gum health and identify periodontal disease.
- Disclosing Tablets or Solutions: These are an invaluable tool. After you chew or rinse with a special dye, plaque (especially new, "immature" plaque) stains brightly (often red or blue), making it clearly visible. This helps both the patient and the clinician identify problem areas.
- X-rays (Radiographs): While X-rays don't show plaque directly, they are crucial for detecting its long-term effects. They can reveal caries (cavities) between teeth or under fillings, as well as bone loss that occurs in advanced periodontal disease due to chronic plaque infection.
- Patient Interview: Your dentist will ask about your oral hygiene habits, dietary choices, and any symptoms you’ve noticed (like bleeding gums or sensitivity) to get a comprehensive picture.
Treatment Options with Pros, Cons, and Costs
The "treatment" for plaque primarily revolves around its removal and preventing its accumulation. Once plaque hardens into calculus, professional intervention is required.
1. At-Home Plaque Removal (Prevention & Management):
- Description: Daily brushing and flossing remove soft plaque before it hardens.
- Pros: Cost-effective, essential for ongoing maintenance, prevents most plaque-related diseases.
- Cons: Requires consistent effort and correct technique; cannot remove hardened calculus.
- Cost: Minimal (cost of toothpaste, toothbrushes, floss). Electric toothbrushes can be $30 - $200+.
2. Professional Dental Cleaning (Prophylaxis):
- Description: A routine cleaning performed by a dental hygienist or dentist to remove supragingival plaque and calculus, as well as polish teeth.
- Pros: Removes deposits missed by at-home care, identifies early problems, freshens breath, brightens smile. Essential every 6-12 months.
- Cons: Cannot address deep subgingival calculus or advanced periodontal disease.
- Cost (US, without insurance): $75 - $200.
3. Scaling and Root Planing (Deep Cleaning):
- Description: A non-surgical procedure to remove subgingival plaque and calculus from below the gumline and smooth the root surfaces. This helps eliminate bacteria and allows gum tissue to reattach to the tooth. Often performed under local anesthetic and typically divided into quadrants.
- Pros: Effective in treating moderate gingivitis and early to moderate periodontal disease, reduces gum inflammation and pocket depths, helps prevent further bone loss.
- Cons: More invasive and time-consuming than a regular cleaning, typically requires multiple appointments, can cause temporary sensitivity.
- Cost (US, without insurance): $200 - $600 per quadrant, or $800 - $2,400 for the full mouth.
4. Adjunctive Therapies (Used with Scaling and Root Planing):
- Description:
- Antibiotics: Oral antibiotics or localized antibiotic placement (e.g., Arestin, Atridox) in deep pockets to target specific bacteria.
- Antimicrobial Rinses: Prescription mouthwashes containing chlorhexidine gluconate to reduce bacterial load.
- Pros: Enhances the effectiveness of scaling and root planing, particularly for aggressive forms of periodontal disease.
- Cons: Potential side effects (e.g., staining with chlorhexidine, antibiotic resistance). Increases overall cost.
- Cost (US, without insurance): Antibiotics $20 - $100 per localized application; Mouthrinses $15 - $30.
Step-by-Step: What to Expect During Treatment
For a Routine Professional Cleaning (Prophylaxis):
- Examination: The hygienist or dentist will first examine your mouth for any obvious issues.
- Plaque and Calculus Removal: Using specialized instruments (hand scalers and/or ultrasonic devices), they will gently scrape or vibrate away plaque and calculus from above and slightly below the gumline. You might hear scraping noises but should feel minimal discomfort.
- Polishing: A rotating brush with a gritty toothpaste-like paste is used to polish your teeth, removing any remaining surface stains and smoothing the enamel.
- Flossing: The hygienist will thoroughly floss your teeth to ensure all interdental spaces are clean.
- Rinse: You'll rinse your mouth, often with an antiseptic mouthwash.
- Fluoride Treatment (Optional): A fluoride gel or varnish may be applied to strengthen enamel and prevent caries.
For Scaling and Root Planing (Deep Cleaning):
- Anesthesia: Local anesthetic will be administered to numb the specific area (often one or two quadrants of the mouth at a time) to ensure comfort during the procedure.
- Scaling: The hygienist or dentist uses specialized instruments to meticulously remove all plaque and calculus from both above and below the gumline, extending deep into the periodontal pockets. Ultrasonic devices may be used first to dislodge larger deposits, followed by hand scalers for thorough cleaning.
- Root Planing: The root surfaces of the teeth are then carefully smoothed. This eliminates rough spots where bacteria can easily attach, discourages future plaque accumulation, and allows the gums to reattach more firmly to the clean root surface.
- Irrigation (Optional): An antimicrobial solution might be flushed into the pockets to further reduce bacteria.
- Localized Antibiotics (Optional): In some cases, antibiotic medication might be placed directly into deep pockets.
Recovery Timeline and Aftercare
After a Routine Cleaning:
- Timeline: No downtime. You can immediately resume normal activities.
- Aftercare: Maintain excellent oral hygiene at home (brushing twice daily for two minutes, flossing once daily). Follow your dentist's recommendations for fluoride use or specific mouthwashes.
After Scaling and Root Planing:
- Timeline:
- Immediately after: Numbness will wear off in a few hours.
- First few days: Gums may be sore, tender, and potentially sensitive to hot/cold. Mild bleeding is possible.
- 1-2 weeks: Gums should start to heal, becoming firmer and less red. Sensitivity usually subsides.
- Follow-up: A follow-up appointment (often 4-6 weeks later) is crucial to assess healing and measure pocket depths to ensure the treatment was effective.
- Aftercare:
- Pain Management: Over-the-counter pain relievers (e.g., ibuprofen) can manage discomfort.
- Diet: Stick to soft foods for the first few days to avoid irritating tender gums.
- Oral Hygiene: Continue gentle brushing and flossing. Your dentist might recommend a chlorhexidine mouthwash for a short period to aid healing.
- Avoid Smoking: Smoking significantly impairs healing and can negate the benefits of treatment.
- Maintenance: Regular periodontal maintenance cleanings (often every 3-4 months) are vital after scaling and root planing to prevent recurrence of periodontal disease.
Prevention Strategies
Preventing plaque accumulation is the cornerstone of excellent oral health. It's largely within your control:
- Brush Twice Daily with Fluoride Toothpaste: Use a soft-bristled toothbrush and brush gently but thoroughly for two minutes each time. Focus on all tooth surfaces and the gumline. Fluoride strengthens enamel and helps resist acid attacks from plaque bacteria, preventing caries.
- Floss Daily: Flossing (or using interdental brushes) once a day is critical for removing plaque and food particles from between teeth and under the gumline – areas your toothbrush can't reach. This directly prevents interproximal caries and gingivitis.
- Use an Antimicrobial Mouthwash: While not a substitute for brushing and flossing, a therapeutic (antimicrobial) mouthwash can help reduce bacterial load and further control plaque growth.
- Regular Dental Check-ups and Professional Cleanings: Visit your dentist every six months (or more often if advised) for comprehensive exams and professional cleanings. This allows for early detection and removal of plaque and calculus before significant damage occurs.
- Limit Sugary and Starchy Foods and Drinks: Reduce the frequency of consuming items that feed plaque bacteria. If you do indulge, try to do so with meals and rinse your mouth with water afterward.
- Stay Hydrated: Drinking plenty of water, especially fluoridated water, helps wash away food particles and neutralize acids.
- Avoid Tobacco Products: Quitting smoking or chewing tobacco significantly reduces your risk of periodontal disease and improves overall oral and systemic health.
- Consider Dental Sealants: For children and sometimes adults, dental sealants can be applied to the chewing surfaces of back teeth to fill in grooves and pits, creating a smoother surface that is easier to clean and less prone to plaque accumulation and caries.
Cost Ranges in the US (with/without insurance)
The cost of managing plaque-related issues varies significantly based on the severity of the condition, the type of procedure, and whether you have dental insurance. These are general ranges in the US:
| Service/Procedure | Cost without Insurance (Estimate) | Cost with Insurance (Estimate) | Notes |
|---|---|---|---|
| Routine Dental Cleaning | $75 - $200 | $0 - $50 (often 100% covered) | Typically recommended every 6 months. |
| Dental X-rays (Bitewings) | $30 - $80 | $0 - $30 (often 80-100% covered) | Usually part of routine check-ups. |
| Scaling and Root Planing | $200 - $600 per quadrant | $50 - $200 per quadrant | For deep plaque/calculus below gumline; often 50-80% covered. |
| Periodontal Maintenance | $100 - $250 | $20 - $80 | Special cleanings after scaling/root planing; often 80% covered. |
| Localized Antibiotic | $20 - $100 per site | $10 - $50 per site | Adjunctive therapy for deep pockets; coverage varies. |
| Fluoride Treatment | $20 - $50 | $0 - $20 (often 80-100% covered) | Often included in child cleanings, sometimes for adults. |
| Dental Sealants | $30 - $70 per tooth | $10 - $30 per tooth | Often covered for children up to age 18. |
- Insurance Coverage: Most dental insurance plans prioritize preventive care, meaning routine cleanings and check-ups are often covered at 80-100%. Procedures like scaling and root planing are usually considered basic restorative care and might be covered at 50-80% after a deductible. It's crucial to check your specific policy for details on coverage percentages, annual maximums, and deductibles. Many plans have a waiting period for major procedures.
For Parents / Pediatric Considerations
Plaque is a concern from the moment the first tooth erupts. Parents play a vital role in establishing lifelong habits to prevent plaque-related problems in children.
- Start Early: Begin cleaning your baby's gums even before teeth appear with a soft cloth. Once the first tooth emerges, use a soft baby toothbrush with a tiny smear of fluoride toothpaste (rice-grain size) twice a day.
- Supervise Brushing: Children generally lack the dexterity to brush effectively on their own until around ages 6-8. Parents should supervise and assist with brushing until then, ensuring thorough plaque removal.
- Flossing for Kids: Once two teeth touch, begin flossing. Floss picks can be helpful for small hands.
- Healthy Eating Habits: Limit sugary snacks and drinks, especially between meals. Encourage water consumption.
- First Dental Visit: The American Academy of Pediatric Dentistry (AAPD) recommends a child's first dental visit by their first birthday or within six months of the first tooth erupting. This allows the dentist to assess plaque accumulation, risk for caries, and guide parents on proper oral hygiene.
- Fluoride Varnish: Pediatric dentists often apply fluoride varnish during check-ups to strengthen young enamel and prevent caries where plaque might be an issue.
- Dental Sealants: These protective coatings are highly effective in preventing caries on the chewing surfaces of molars, where plaque can easily collect in pits and grooves. They are typically applied shortly after permanent molars erupt.
- Lead by Example: Children are more likely to adopt good habits if they see their parents prioritizing oral hygiene.
Frequently Asked Questions
How much does plaque removal cost?
The cost of plaque removal depends on its severity and whether it has hardened into calculus. A routine professional cleaning (prophylaxis), which removes soft plaque and light calculus, typically costs $75 - $200 without insurance, but is often fully covered by dental plans. If you have significant subgingival plaque and calculus due to gum disease, you might need scaling and root planing, which costs $200 - $600 per quadrant without insurance. Insurance typically covers a portion of these costs.
Is plaque removal painful?
Routine plaque removal during a professional cleaning is generally not painful, though you might experience some pressure or mild scraping sensations. If you have significant calculus buildup or gingivitis, your gums might be a bit tender during and after the cleaning. For scaling and root planing (deep cleaning), local anesthetic is typically used to ensure you don't feel pain during the procedure. You may experience some soreness and sensitivity for a few days afterward, which can be managed with over-the-counter pain relievers.
How long does it take to remove plaque?
Daily removal of soft plaque through brushing and flossing takes about 3-5 minutes each day. A professional dental cleaning to remove accumulated plaque and calculus usually takes 45-60 minutes. If you require scaling and root planing for moderate to severe plaque and calculus below the gumline, this is often done in multiple appointments, with each quadrant taking 60-90 minutes.
Are there natural remedies for plaque?
There are no "natural remedies" that can effectively remove plaque once it's formed or hardened into calculus. While some natural practices (like oil pulling or herbal rinses) are marketed for oral health, they do not replace the mechanical removal of plaque and calculus through brushing, flossing, and professional dental cleanings. These methods are crucial because they physically disrupt and dislodge the bacterial biofilm. Relying solely on natural remedies without proper oral hygiene and professional care can lead to worsening caries and periodontal disease.
Can plaque be removed at home?
Only soft, immature plaque can be effectively removed at home through diligent brushing twice daily with fluoride toothpaste and flossing once daily. Once plaque hardens into calculus (tartar), it becomes strongly adhered to the tooth surface and cannot be removed by brushing or flossing alone. Professional dental instruments are required to scrape off calculus. This is why regular professional cleanings are so important.
Does dental insurance cover plaque removal?
Yes, most dental insurance plans cover plaque removal, especially routine preventive care. Regular dental cleanings (prophylaxis) are often covered at 80-100% because they are considered essential for preventing more serious and costly dental problems like caries and periodontal disease. If more extensive removal like scaling and root planing is needed due to gingivitis or periodontal disease, it is typically covered at a lower percentage, usually 50-80%, after a deductible.
What's the difference between plaque and calculus?
Plaque is a soft, sticky, colorless bacterial film that continuously forms on your teeth. It can be removed with brushing and flossing. Calculus, also known as tartar, is hardened plaque. If plaque is not removed promptly, it absorbs minerals from saliva and calcifies into a rough, porous deposit. Once formed, calculus cannot be removed at home and requires professional dental instruments for removal. Calculus provides an ideal surface for more plaque to accumulate, accelerating both caries and periodontal disease.
Can plaque cause cavities?
Yes, absolutely. Plaque is the primary cause of dental caries, commonly known as cavities. The bacteria within plaque metabolize sugars and starches from your diet, producing acids as a byproduct. These acids attack and demineralize the enamel, which is the hard outer layer of your teeth. Over time, repeated acid attacks weaken the enamel, creating a small hole or cavity. If left untreated, the cavity will deepen and can reach the inner layers of the tooth, causing pain and potentially leading to infection.
Can plaque cause gum disease?
Yes, plaque is the direct cause of gum disease. When plaque accumulates along the gumline, the bacteria and their toxins irritate the gum tissues. This leads to inflammation, which is known as gingivitis – the earliest and mildest form of gum disease. Symptoms include red, swollen, and bleeding gums. If gingivitis is not treated by removing the plaque, it can progress to periodontal disease. In periodontal disease, the inflammation spreads deeper, causing the gums to pull away from the teeth, forming pockets that fill with more plaque and calculus. Eventually, the infection destroys the bone and supporting tissues that hold teeth in place, potentially leading to tooth loss.
When to See a Dentist
Regular dental check-ups are essential for preventing and managing plaque-related issues. You should typically see a dentist at least twice a year, or every six months, for a professional cleaning and examination.
However, certain signs indicate you should schedule an appointment sooner:
- Persistent bad breath that doesn't improve with brushing.
- Gums that are red, swollen, tender, or bleed easily during brushing or flossing (signs of gingivitis).
- A "fuzzy" or rough feeling on your teeth, even after brushing.
- Visible yellow or brown deposits on your teeth, especially near the gumline (calculus).
- Increased tooth sensitivity to hot, cold, or sweet foods.
- Persistent pain in a tooth or your gums.
- Any changes in your bite or the way your teeth fit together.
- If you notice your gums receding or teeth appearing longer, which could indicate advancing periodontal disease.
Don't wait until you're in pain; early detection and intervention are key to successfully managing plaque and preventing serious dental problems.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.