Caries
3,391 words · 11 min read
Quick Definition
The scientific term for tooth decay, a disease process caused by bacteria that produce acids which dissolve tooth enamel and dentin, creating cavities.
Caries: An In-Depth Guide to Tooth Decay
Welcome to SmilePedia.net, your definitive resource for understanding dental health. In this comprehensive article, we delve deep into "caries," the scientific term for what most people know as tooth decay. More than just a simple "cavity," caries is a complex disease process that affects billions worldwide, making it one of the most prevalent chronic conditions across all age groups. Understanding caries is fundamental to maintaining lifelong oral health, as it's a primary reason for dental pain, tooth loss, and expensive treatments.
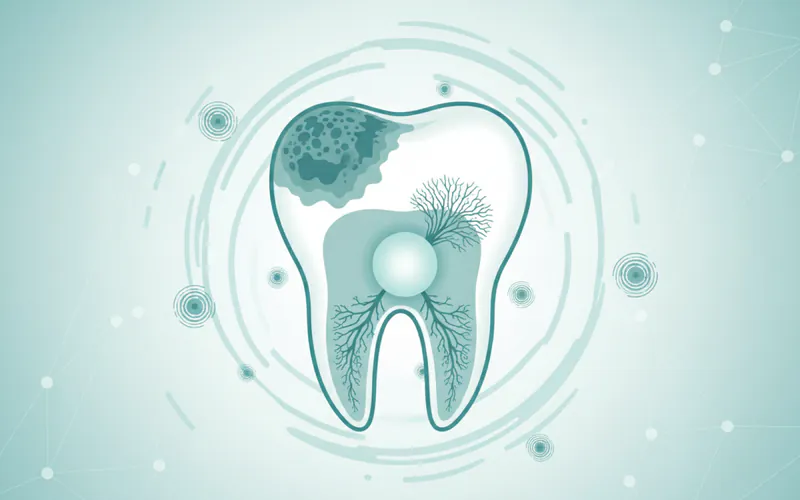
Caries is a progressive destruction of the tooth structure, initiated by specific types of bacteria found in the mouth. These bacteria produce acids that attack and dissolve the tooth's hard outer layer, the enamel, and the softer layer beneath it, the dentin, eventually creating a hole or cavity. While entirely preventable, if left untreated, caries can lead to severe infection, chronic pain, and ultimately, the loss of the affected tooth. Globally, the World Health Organization estimates that 3.5 billion people are affected by oral diseases, with dental caries being the most common condition. In the United States, statistics from the Centers for Disease Control and Prevention (CDC) reveal that over 1 in 4 adults aged 20-64 currently have dental caries, and a staggering 9 out of 10 adults in this age group have had caries in their permanent teeth. For children, approximately 1 in 5 (20%) aged 2-11 have untreated caries, highlighting the widespread impact of this disease.
Key Takeaways:
- Caries is the scientific term for tooth decay, a bacterial disease that creates cavities.
- It's caused by acids produced by bacteria that erode tooth enamel and dentin.
- Caries is one of the most common chronic diseases globally, affecting both children and adults.
- Early detection and treatment are crucial to prevent pain, infection, and tooth loss.
- Excellent oral hygiene, a healthy diet, fluoride, and sealants are key prevention strategies.
- Treatment often involves fillings, but can extend to root canals or extractions for severe cases.
Detailed Explanation
Types and Classifications of Caries
Caries can manifest in different ways, depending on its location and progression:
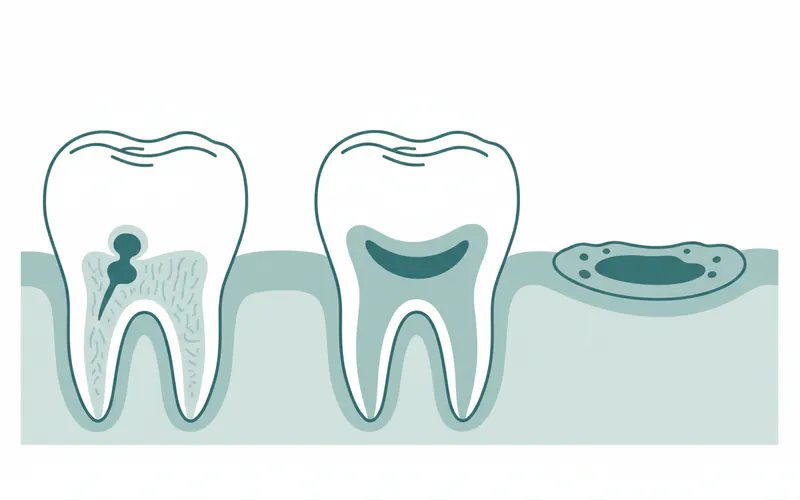
- Coronal Caries: This is the most common type, occurring on the chewing surfaces (occlusal surfaces) or between the teeth (interproximal surfaces) of permanent teeth. It often affects the pits and fissures of molars and premolars, which are natural grooves where food particles and bacteria can easily accumulate.
- Root Caries: As people age, gums can recede, exposing the tooth roots. Unlike enamel, which covers the crown, the root surface is covered by cementum, a softer tissue that is more vulnerable to acid attack. Root caries is particularly common in older adults and those with gum disease.
- Recurrent (Secondary) Caries: This type forms around the edges or beneath existing dental restorations, such as fillings or crowns. Bacteria can penetrate tiny gaps that form over time, leading to new decay in an area that was previously treated.
- Early Childhood Caries (ECC): Formerly known as "baby bottle tooth decay," ECC is a severe form of caries affecting infants and young children, often involving the upper front teeth. It can result from prolonged exposure to sugary liquids, such as milk, juice, or sweetened formula, especially during sleep. This is covered in more detail in the "For Parents" section.
Causes and Risk Factors
Caries develops when a complex interplay of factors creates an environment conducive to tooth destruction:
- Bacteria and Plaque: Your mouth is home to hundreds of types of bacteria. Certain strains, particularly Streptococcus mutans and Lactobacillus, thrive on sugars from food and drinks. They convert these sugars into acids. These bacteria, along with food debris, saliva, and other substances, form a sticky, colorless film called plaque that constantly adheres to your teeth.
- Sugary and Starchy Foods: Frequent consumption of sugary drinks, candies, pastries, and even starchy foods like bread and chips provides fuel for acid-producing bacteria. The longer these foods linger on your teeth, the more time bacteria have to produce harmful acids.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque to accumulate and acids to continually attack tooth enamel. Regular brushing (at least twice a day) and flossing (at least once a day) are essential to remove plaque and food particles.
- Insufficient Fluoride: Fluoride is a natural mineral that helps strengthen tooth enamel and makes it more resistant to acid attacks. It can even reverse very early stages of decay (demineralization). Lack of fluoride exposure (from fluoridated water, toothpaste, or professional treatments) is a significant risk factor.
- Dry Mouth (Xerostomia): Saliva plays a crucial role in oral health by washing away food particles, neutralizing acids, and providing minerals that help repair enamel. Conditions that reduce saliva flow, such as certain medications (antihistamines, decongestants, antidepressants), medical treatments (radiation therapy), or diseases (Sjögren's syndrome), significantly increase caries risk.
- Medical Conditions and Treatments: Gastric reflux disease (GERD) can bring stomach acid into the mouth, eroding enamel. Eating disorders like bulimia also expose teeth to stomach acid. Certain medical treatments that impair saliva flow or manual dexterity can also contribute.
- Worn or Broken Fillings/Restorations: Old fillings can crack, chip, or pull away from the tooth, creating crevices where bacteria can collect and initiate recurrent caries.
- Genetics: While not the primary cause, genetic factors can influence tooth structure, enamel hardness, saliva composition, and even dietary preferences, indirectly affecting caries susceptibility.
Signs and Symptoms to Watch For
In its earliest stages, caries often presents no noticeable symptoms. This is why regular dental check-ups are so important. As decay progresses, you might experience:
- White Spots: The very first visible sign of demineralization on enamel is a chalky white spot, indicating loss of minerals. At this stage, it's often reversible with fluoride treatments.
- Tooth Sensitivity: A common symptom, particularly when consuming hot, cold, sweet, or acidic foods and drinks. This indicates that the decay has reached the dentin, which contains microscopic tubules leading to the tooth's nerve.
- Mild to Sharp Pain: Pain that occurs spontaneously or when biting down, typically indicating more significant decay that has approached or reached the pulp (the innermost part of the tooth containing nerves and blood vessels).
- Visible Pits or Holes (Cavities): As decay progresses, a visible opening or cavity forms in the tooth. These can be small and hard to see or large and obvious.
- Staining: Brown, black, or grey staining on the surface of a tooth.
- Bad Breath (Halitosis): Accumulated bacteria and decaying tooth structure can produce unpleasant odors.
- Swelling Around the Gums: If the infection from deep decay spreads, it can cause an abscess (a pocket of pus) at the tooth's root, leading to swelling and severe pain.
Diagnosis Process — What Your Dentist Does
Diagnosing caries involves a combination of methods:
- Visual Examination: Your dentist will carefully examine your teeth for any visible signs of decay, such as white spots, dark spots, or obvious cavities. They'll also check for any compromised fillings or crowns.
- Dental Explorer: A small, sharp instrument called a dental explorer is gently used to probe for soft spots on the tooth surface. Healthy enamel is hard, while decayed areas will feel soft or sticky.
- X-rays (Radiographs): Bitewing X-rays are crucial for detecting caries between teeth (interproximal caries) or under existing fillings that are not visible during a clinical exam. Decay appears as darker areas on the X-ray images.
- ``
- Transillumination: A bright light shone through the tooth can sometimes reveal shadows indicative of decay, especially in the front teeth.
- Caries Detection Dyes: In some cases, a special dye might be applied to highlight decayed areas, particularly during cavity preparation.
- Laser Fluorescence: Some advanced tools use laser fluorescence to detect early enamel changes and provide a numerical reading of potential decay, though this is less common for routine diagnosis.
Treatment Options with Pros, Cons, and Costs
Treatment for caries depends on the extent and severity of the decay. The goal is always to remove the decayed portion, clean the area, and restore the tooth's structure and function.
| Treatment Option | Description | Pros | Cons | Average Cost Range (US, without insurance) |
|---|---|---|---|---|
| Fluoride Treatment | High-concentration fluoride varnish, gel, or foam applied to teeth to remineralize early enamel lesions (white spots) before a cavity forms. | Non-invasive, can reverse early decay, strengthens enamel. | Only effective for very early, surface demineralization; not for established cavities. | $25 - $75 |
| Dental Filling | The most common treatment. The decayed part of the tooth is removed, and the remaining space is filled with a restorative material. Materials include: Amalgam (Silver): A mixture of mercury, silver, tin, and copper. Composite (Tooth-Colored): Resin-based material matched to tooth color. Glass Ionomer: Similar to composite, often used for smaller cavities or near the gum line. |
Amalgam: Durable, less expensive, moisture-resistant. Composite: Aesthetically pleasing, bonds to tooth structure, mercury-free. Glass Ionomer: Releases fluoride, good for pediatric/root fillings. |
Amalgam: Not aesthetic, contains mercury (though deemed safe by ADA), requires more tooth removal, can expand/contract. Composite: More expensive, less durable than amalgam for very large fillings, prone to staining, longer placement time. Glass Ionomer: Less strong/durable than other options. |
Amalgam: $50 - $300 Composite: $90 - $450 Glass Ionomer: $70 - $200 |
| Dental Crown | A custom-made cap that covers the entire visible portion of a severely damaged or weakened tooth, often after a large filling or root canal. Made from porcelain, metal, or a combination. | Restores strength, protects the remaining tooth structure, improves aesthetics and function. | More invasive (requires significant tooth reduction), more expensive, requires multiple visits. | $800 - $3,000+ |
| Root Canal Therapy | When decay reaches the pulp, causing infection or inflammation, the infected pulp is removed, the root canals are cleaned and disinfected, and then filled and sealed. The tooth is typically then restored with a filling and a crown. | Saves the natural tooth from extraction, relieves pain, preserves chewing function. | Invasive, more expensive, requires multiple visits, tooth can become brittle without a crown. | $700 - $2,500+ (varies by tooth) |
| Tooth Extraction | If the tooth is too severely damaged by decay to be saved, or if infection is uncontrollable, the tooth is removed. | Removes source of infection/pain, prevents spread of disease. | Loss of natural tooth, can lead to shifting of adjacent teeth, requires replacement (implant, bridge) to maintain bite and aesthetics, which adds further cost. | $75 - $650+ (simple vs. surgical) |
Cost Ranges in the US (with/without insurance): The costs listed above are general averages without dental insurance. With insurance, coverage typically ranges from 50% to 80% for basic restorative procedures like fillings after you meet your deductible. Major procedures like crowns and root canals might be covered at 50%. Preventative care (cleanings, X-rays, fluoride treatments) is often covered at 100% or a very high percentage. Always check with your specific insurance provider for exact coverage details.
Step-by-Step: What to Expect During Treatment (for a standard filling)
- Numbing: The dentist will numb the area around the affected tooth using a local anesthetic. This ensures you won't feel pain during the procedure.
- Decay Removal: Using a dental drill, laser, or air abrasion instrument, the dentist will carefully remove all decayed tooth material.
- ``
- Preparation: Once the decay is removed, the remaining tooth structure is shaped to ensure the filling material can bond properly and effectively.
- Filling Application:
- Composite Fillings: The tooth is etched with an acid gel, rinsed, and a bonding agent is applied. The tooth-colored resin material is then applied in layers, each hardened with a special curing light. Finally, the filling is shaped and polished.
- Amalgam Fillings: The amalgam material is prepared and then packed into the prepared cavity. The dentist shapes it before it hardens, then polishes it.
- Bite Check: After the filling is placed, your dentist will check your bite to ensure the filling doesn't interfere with your occlusion. Any high spots will be adjusted.
Recovery Timeline and Aftercare
For a simple filling, recovery is usually straightforward:
- Numbness: The numbness from the local anesthetic will typically wear off within 1-3 hours. Be careful not to bite your tongue or cheek during this time.
- Sensitivity: It's common to experience some sensitivity to hot, cold, or pressure for a few days to a few weeks after a filling, especially with deeper cavities. This should gradually subside.
- Eating: You can usually eat once the numbness wears off, but try to avoid hard or sticky foods on the filled tooth for the first 24 hours. If you received an amalgam filling, your dentist might advise waiting longer to allow it to fully harden.
- Pain Relief: Over-the-counter pain relievers like ibuprofen can help manage any discomfort.
- Oral Hygiene: Continue your regular brushing and flossing routine.
- When to Call Your Dentist: If you experience persistent or severe pain, swelling, a feeling that your bite is uneven, or if the filling feels loose or falls out, contact your dentist immediately.
Prevention Strategies
Preventing caries is far easier, less painful, and less expensive than treating it. Here are key strategies:
- Brush Twice Daily with Fluoride Toothpaste: Use a soft-bristled brush and brush for two minutes, morning and night. Fluoride toothpaste is essential for strengthening enamel and fighting decay.
- Floss Daily: Flossing removes plaque and food particles from between your teeth and under the gum line, where your toothbrush can't reach. This is critical for preventing interproximal caries.
- Limit Sugary and Starchy Foods and Drinks: Reduce frequency of consumption. If you do indulge, try to do so with meals rather than throughout the day, as saliva production increases during meals, helping to wash away food and neutralize acids.
- Drink Fluoridated Water: Many community water systems are fluoridated, providing a constant, low-level exposure to fluoride that helps prevent decay. If your water isn't fluoridated, ask your dentist about fluoride supplements.
- Dental Sealants: For children and sometimes adults, dental sealants are thin, protective coatings applied to the chewing surfaces of back teeth (molars and premolars). They effectively seal off the deep pits and fissures, preventing food and bacteria from getting trapped and causing decay.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and examinations. Your dentist can detect early signs of caries, even before you feel symptoms, and apply professional fluoride treatments if needed.
- Consider Fluoride Treatments: Your dentist may recommend in-office fluoride varnishes or gels, or prescription fluoride rinses or toothpastes, especially if you are at high risk for caries.
- Chew Sugar-Free Gum: Chewing sugar-free gum after meals can stimulate saliva flow, which helps neutralize acids and wash away food particles.
- Avoid Tobacco Products: Smoking and chewing tobacco increase the risk of dry mouth and gum disease, both of which contribute to caries.
For Parents / Pediatric Considerations
Caries is a significant concern for children, and parents play a vital role in prevention.
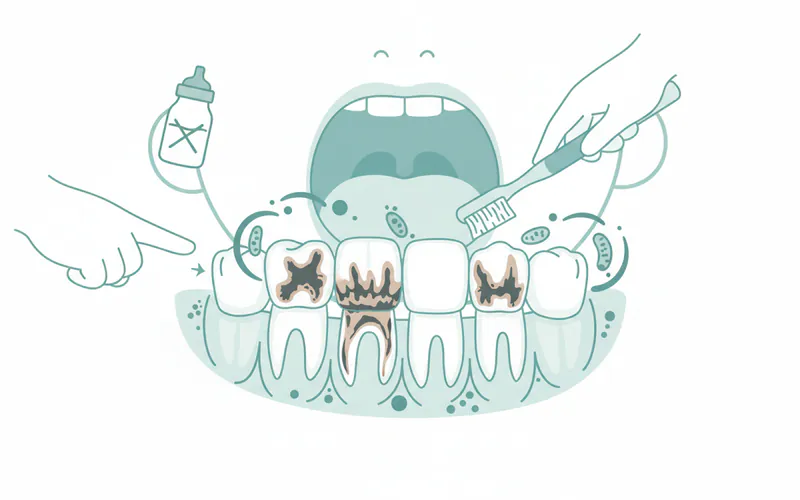
- Early Childhood Caries (ECC): This aggressive form of decay affects young children, sometimes as early as infancy. It's often linked to prolonged use of baby bottles containing sugary liquids (milk, formula, juice) especially at bedtime or as a pacifier substitute. The sugars pool around the teeth, providing a constant food source for decay-causing bacteria.
- Prevention of ECC:
- Never put your baby to bed with a bottle containing anything other than water.
- Limit sugary drinks and snacks.
- Wipe your baby's gums with a clean, damp cloth after feedings, even before teeth erupt.
- Once teeth appear, brush twice daily with a tiny smear of fluoride toothpaste (rice-grain size) for children under 3, and a pea-sized amount for children 3-6 years old.
- Prevention of ECC:
- First Dental Visit: Schedule your child's first dental visit by their first birthday or when their first tooth erupts. Early visits help establish a "dental home" and allow the dentist to assess risk and provide preventive advice.
- Dental Sealants for Children: Sealants are highly effective in preventing pit and fissure caries in children's permanent molars, which typically erupt around ages 6 and 12. They can reduce the risk of decay in these teeth by 80%.
- Fluoride Varnish: Pediatric dentists often apply fluoride varnish to children's teeth during routine check-ups to strengthen enamel and prevent decay.
Frequently Asked Questions
How much does it cost to treat caries in the US?
The cost of treating caries varies significantly depending on the severity of the decay, the type of treatment needed, and whether you have dental insurance. A simple filling can range from $50 to $450 without insurance, while a root canal can be $700 to $2,500+, and a crown $800 to $3,000+. With dental insurance, a portion of these costs is usually covered, often 50-80% for fillings and 50% for major procedures after deductibles are met. Preventative care like cleanings and X-rays are frequently covered at 100%.
Is treating caries painful?
During treatment, your dentist will use a local anesthetic to numb the area, so you should not feel pain. You might feel pressure or vibrations, but not sharp pain. After the numbing wears off, some sensitivity or mild discomfort is common for a few days, especially with deeper cavities, but this can usually be managed with over-the-counter pain relievers.
How long does treatment for caries take?
A standard filling procedure usually takes between 20 minutes to an hour, depending on the size and location of the cavity and the material used. More complex treatments like root canals or crowns often require one to two visits, each lasting 1-2 hours.
Can caries heal itself or go away without treatment?
Once a true cavity (a hole in the enamel or dentin) has formed, it cannot heal itself. The tooth structure that has been destroyed cannot naturally regenerate. While very early stages of enamel demineralization (white spots) can sometimes be reversed with intensive fluoride exposure, an established cavity requires professional intervention to prevent further progression and complications.
What happens if caries is left untreated?
If left untreated, caries will continue to progress, leading to larger cavities, more severe pain, and potential complications. The decay can reach the pulp of the tooth, causing infection and inflammation (pulpitis), which often necessitates a root canal. If the infection spreads further, it can lead to an abscess, bone loss, and eventually, the need for tooth extraction. Untreated infections can even spread to other parts of the body, causing serious health issues.
Does dental insurance cover caries treatment?
Most dental insurance plans in the US do cover a portion of caries treatment. Preventative services (cleanings, exams, X-rays, fluoride) are often covered at 100%. Basic restorative services, like fillings, are typically covered at 70-80%. Major restorative services, such as crowns and root canals, are usually covered at 50%. However, coverage varies widely between plans, so it's always best to check your specific policy details.
When to See a Dentist
Regular dental check-ups, ideally every six months, are crucial for preventing caries and detecting it in its earliest, most treatable stages.
You should schedule an appointment with your dentist immediately if you experience any of the following:
- Persistent Toothache: Especially if it's severe, spontaneous, or worsens with hot or cold temperatures, or when biting.
- Visible Holes or Pits in Your Teeth: Even if you don't feel pain.
- Sensitivity: New or worsening sensitivity to hot, cold, or sweet foods/drinks.
- Pus or Swelling: Around a tooth or in your gums, indicating a possible infection or abscess.
- Bad Taste in Your Mouth or Persistent Bad Breath: Which could signal an underlying infection.
- A Broken or Lost Filling: Which can leave the tooth vulnerable to further decay.
Don't wait for pain to seek dental care. Early detection and intervention are key to preserving your oral health and preventing more extensive and costly treatments.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.