Sealant
4,759 words · 16 min read
Quick Definition
A thin, protective coating applied to the chewing surfaces of back teeth (molars and premolars) to prevent decay by sealing the deep grooves and fissures where bacteria accumulate.
What Exactly is a Dental Sealant? An In-Depth Guide to Protecting Your Smile
Short Definition: A thin, protective coating applied to the chewing surfaces of back teeth (molars and premolars) to prevent decay by sealing the deep grooves and fissures where bacteria accumulate.
Introduction
Welcome to SmilePedia.net, your definitive resource for understanding crucial dental health topics. Today, we're diving deep into the world of dental sealants – a powerful, yet often underestimated, tool in the fight against cavities. If you've ever searched "what is sealant" or "sealant dental," you've come to the right place.
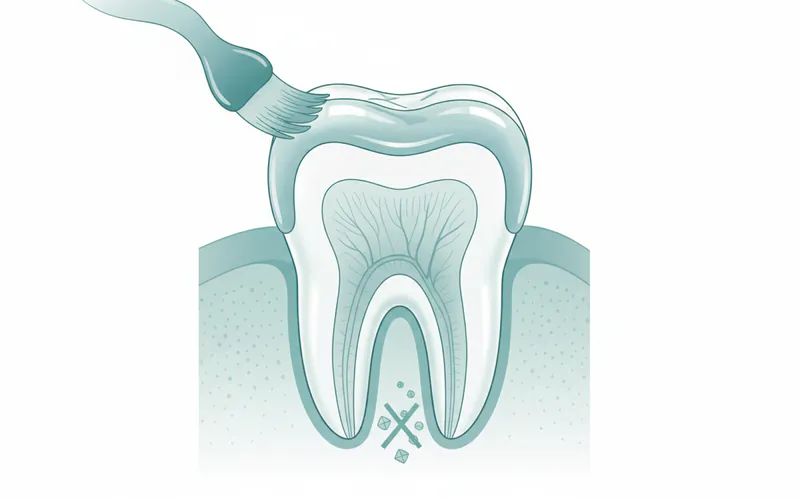
A dental sealant is precisely what its name suggests: a durable, protective barrier that seals off the vulnerable chewing surfaces of your teeth. These surfaces, particularly on your back teeth (known as molars and premolars), are naturally etched with tiny depressions, pits, and grooves called fissures. While these fissures are a normal part of tooth anatomy, they act as ideal hiding spots for food particles and plaque bacteria. Unfortunately, the bristles of a toothbrush often can't reach deep enough into these narrow crevices, leaving them susceptible to decay. This is where dental sealants step in, creating a smooth, impervious surface that starves bacteria and prevents the formation of caries, the technical term for cavities.
The importance of dental sealants for maintaining optimal oral health cannot be overstated. They are a cornerstone of preventative dentistry, especially for children and teenagers whose permanent teeth are newly erupted and most vulnerable. Studies show that sealants can reduce the risk of decay in molars by 80% for two years and continue to protect against 50% of cavities for up to four years. With dental decay affecting one in five (20%) children aged 5-11 and one in seven (13%) adolescents aged 12-19 in the US, sealants represent a simple, effective, and non-invasive solution to a widespread problem. This article will serve as your ultimate guide, exploring every facet of dental sealants to empower you with knowledge and help you make informed decisions about your family's oral health.
Key Takeaways:
- Dental sealants are thin, plastic coatings applied to chewing surfaces of back teeth.
- They primarily protect molars and premolars from caries (cavities).
- Sealants work by filling in deep fissures that toothbrushes cannot reach.
- They are highly effective, reducing decay risk by up to 80% in the first two years.
- The application process is quick, painless, and non-invasive.
- While ideal for children, adults can also benefit from sealants on vulnerable teeth.
What Exactly Is a Dental Sealant?
Expanding on our initial definition, a dental sealant is a liquid plastic material that, once applied to the tooth, hardens to form a durable, clear or tooth-colored shield. The primary targets for sealants are the occlusal (chewing) surfaces of your back teeth – specifically the molars and premolars. These teeth are designed to grind food, and their complex topography includes a network of pits and fissures that are incredibly difficult to clean. These areas are known as "retentive" sites, meaning they readily retain food debris and plaque, fostering an environment where cavity-causing bacteria thrive.
The sealant material itself is typically made from a resin-based composite, similar to the material used for white dental fillings. Some sealants also contain fluoride, which can slowly release into the tooth structure, further enhancing its decay-preventing capabilities. When applied, the liquid sealant flows into these microscopic grooves and pits, creating a smooth surface that effectively "seals" them off. This smooth surface makes it much easier for a toothbrush to clean, drastically reducing the chances of plaque accumulation and subsequent caries formation. Think of it as putting a protective, non-stick coating on your teeth that actively repels harmful bacteria and food particles.
Why Are Dental Sealants So Important?
The significance of dental sealants lies in their preventative power. Dental decay, or caries, is one of the most common chronic diseases globally, and it's almost entirely preventable. The pits and fissures of molars and premolars are responsible for a large percentage of all posterior tooth decay, precisely because they are so hard to clean. Even with diligent brushing and flossing, these deep, narrow grooves can harbor bacteria that produce acids, slowly eroding the tooth enamel and leading to cavities.
Sealants provide a crucial physical barrier against these threats. By denying bacteria and food particles access to the vulnerable enamel, they essentially "starve" the decay process. This preventative approach is far superior to treating decay once it has occurred, as fillings always involve removing some healthy tooth structure. Sealants preserve the natural tooth, making them a conservative and highly effective intervention.
Furthermore, sealants complement other preventative measures like regular brushing, flossing, and fluoride treatments. While fluoride strengthens tooth enamel, making it more resistant to acid attacks, it is less effective at preventing decay in the deep pits and fissures compared to smooth surfaces. Sealants work synergistically with fluoride, offering comprehensive protection, particularly in the most susceptible areas of the mouth. For instance, children who receive sealants are less likely to experience tooth pain, infection, or the need for more invasive and costly dental procedures like fillings or extractions later in life. This proactive measure not only safeguards oral health but also contributes to overall well-being and reduces long-term dental expenses.
Who Benefits Most from Dental Sealants?
While anyone with deep fissures in their molars or premolars can benefit from sealants, certain groups are particularly strong candidates due to their increased risk of decay or the specific stage of their dental development.
-
Children and Adolescents: This is the primary target group for dental sealants. The permanent molars, especially the first molars (erupting around age 6) and second molars (erupting around age 12), are most susceptible to decay soon after they emerge. Applying sealants shortly after these teeth fully erupt, before decay has a chance to set in, is the most effective strategy. Their newly erupted enamel is still maturing and is more porous and vulnerable than adult enamel. In the US, it's estimated that only about 42% of children aged 6-11 and 50% of adolescents aged 12-19 have had sealants applied. This represents a significant gap in preventative care, as the Centers for Disease Control and Prevention (CDC) highlights sealants as a key intervention to improve children's oral health.
-
Adults: While commonly associated with children, adults can absolutely benefit from dental sealants. If an adult has deep grooves in their molars or premolars that have never had caries and are free of existing fillings, sealants can be a wise preventative measure. This is especially true for individuals who might be at higher risk for decay due to genetics, certain medical conditions, medications causing dry mouth, or a history of frequent cavities. A thorough dental examination will determine if an adult's teeth would benefit from sealant application.
-
Individuals with High Caries Risk: Patients with poor oral hygiene habits, a diet high in sugary foods, or a history of multiple cavities are excellent candidates for sealants, regardless of age. Their teeth are under constant threat from acid attacks, and sealants provide an essential layer of defense.
-
Special Needs Patients: Individuals who may have difficulty with routine oral hygiene due to physical or cognitive limitations can particularly benefit from the added protection that sealants offer.
Types of Dental Sealants
Dental sealants generally fall into a few categories based on their material composition and appearance:
-
Resin-Based Sealants: These are the most common type and are made from a plastic material called Bis-GMA (bisphenol A-glycidyl methacrylate) or similar acrylic resins. They are highly durable and offer excellent adhesion to the tooth surface.
- Clear or Tooth-Colored: Many resin sealants are clear or slightly tinted (often white or light yellow) to blend in with the natural tooth color, making them aesthetically pleasing.
- Opaque/Tinted: Some sealants are opaque white or have a distinct color (like light blue) when first applied. This tint helps the dentist easily see the sealant during application and subsequent check-ups to monitor its integrity. Over time, these tints can fade, becoming less noticeable.
-
Glass Ionomer Sealants: These sealants are made from a combination of glass particles and polyacrylic acid. A key advantage of glass ionomer sealants is their ability to release fluoride over time, providing additional protection against caries. They are also less sensitive to moisture during application, making them a good choice in situations where maintaining a completely dry field (which is critical for resin sealants) is challenging, such as with very young children or patients with salivary control issues. However, they may not be as durable or long-lasting as resin-based sealants.
-
Flowable Composite Resins: Sometimes, a dentist might use a flowable composite resin, which is a type of filling material, as a sealant. These are similar to traditional resin sealants but are designed to flow even more easily into very fine fissures.
The choice of sealant material often depends on the individual patient's needs, the specific tooth being sealed, and the dentist's preference. Your dentist will discuss the best option for you or your child.
The Science Behind Sealants: How Do They Work?
The effectiveness of dental sealants stems from a simple yet powerful scientific principle: creating a physical barrier. Here's a breakdown of how they operate to protect your teeth from caries:
-
Physical Barrier: The primary mechanism is the formation of a smooth, protective shield over the intricate fissures and pits on the chewing surfaces of molars and premolars. These grooves, often no wider than a single hair, are too narrow for toothbrush bristles to effectively clean. Sealants fill these spaces entirely, creating an impenetrable physical barrier that prevents food particles, sugars, and plaque bacteria from lodging in these vulnerable areas.
-
Starving Bacteria: Caries develops when specific bacteria in plaque consume sugars from our diet and produce acids. These acids then dissolve the enamel, leading to a cavity. By sealing off the fissures, sealants deny these bacteria access to their food source (sugars) and a protected environment to grow. Without sugars, the bacteria cannot produce the harmful acids necessary to initiate decay.
-
Reduced Plaque Accumulation: The smooth surface created by the sealant makes it much easier for regular brushing to remove any plaque and food debris that does accumulate. This dramatically reduces the overall bacterial load on the tooth surface.
-
Fluoride Release (for some sealants): As mentioned, some sealants (particularly glass ionomers) contain and slowly release fluoride. This released fluoride is then incorporated into the tooth enamel, making it stronger and more resistant to acid attacks. This provides an additional layer of chemical protection, complementing the physical barrier.
In essence, sealants disrupt the entire decay process at its earliest stage. They are a passive, continuous defense mechanism that works 24/7, safeguarding the teeth in their most vulnerable areas against the constant onslaught of diet and bacteria.
The Dental Sealant Application Process: What to Expect
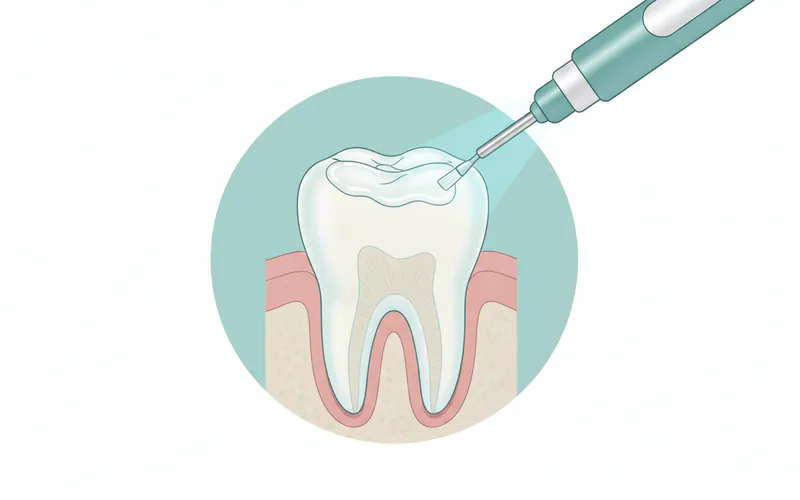
The application of dental sealants is a quick, painless, and non-invasive procedure that typically takes only a few minutes per tooth. No drilling or anesthesia is usually required, making it a very patient-friendly experience, especially for children. Here's a step-by-step guide to what you can expect:
-
Tooth Cleaning: The first step involves thoroughly cleaning the tooth surface to be sealed. The dentist or dental hygienist will use a special brush and abrasive paste (prophy paste) to remove any plaque, food debris, and surface stains from the chewing surface of the molar or premolar. This ensures optimal bonding of the sealant.
-
Isolation and Drying: Once cleaned, the tooth must be kept completely dry. Cotton rolls or a rubber dam (a thin sheet of latex or non-latex material) will be placed around the tooth to isolate it from saliva and moisture. Drying the tooth surface thoroughly with an air syringe is crucial for the sealant to adhere properly.
-
Etching (Conditioning): A mild acidic solution, often phosphoric acid, is applied to the chewing surface of the tooth for a short period (usually 15-30 seconds). This etching gel creates microscopic porosities or roughens the enamel surface, much like sanding wood before painting. This step is vital as it enhances the mechanical bond between the sealant and the tooth enamel. It might feel slightly tingly but is not painful.
-
Rinsing and Drying (Again): After the etching gel has done its job, it is thoroughly rinsed off with water. The tooth is then meticulously dried again. If the tooth becomes contaminated with saliva at this stage, the process may need to be repeated to ensure proper adhesion. The etched enamel will appear dull and frosty white.
-
Sealant Application: The liquid sealant material is carefully painted directly onto the etched and dried chewing surface of the tooth, flowing into all the pits and fissures. The dentist or hygienist will ensure complete coverage without overfilling.
-
Curing (Hardening): Most modern dental sealants are light-cured. A special blue curing light is shined directly onto the sealant for 20-30 seconds per tooth. This light activates a chemical reaction that causes the liquid sealant to harden rapidly into a tough, plastic coating.
-
Checking the Bite: Finally, the dentist will check your bite to ensure the sealant isn't too high and interfering with your occlusion. If necessary, minor adjustments can be made with a dental bur.
The entire process for a single tooth typically takes less than 5 minutes. For multiple teeth, it might take a bit longer but is still a very efficient procedure.
Recovery and Aftercare
Once the dental sealant is applied and hardened, there is virtually no recovery period. You can eat and drink immediately after leaving the dental office.
Immediate Aftercare:
- Avoid chewing on hard candies or extremely sticky foods immediately after the application, though the sealant is fully cured and should be durable.
- The sealant might feel slightly different to your tongue for a few hours, but you should not experience any discomfort or pain.
Long-Term Maintenance:
- Maintain Excellent Oral Hygiene: Sealants are a preventative measure, not a substitute for good oral hygiene. Continue to brush your teeth twice a day with fluoride toothpaste and floss daily.
- Regular Dental Check-ups: Visit your dentist for routine check-ups and cleanings as recommended (typically every six months). During these appointments, your dentist will examine the integrity of your sealants.
- Avoid Excessive Force: While durable, sealants can wear down or chip over time. Avoid chewing on ice, hard nuts, or non-food items (like pen caps) that could damage them.
- Monitor for Wear: If you notice a rough spot, a chip, or a piece of sealant missing, contact your dentist. Small repairs are usually quick and easy to perform.
How Long Do Dental Sealants Last?
The longevity of dental sealants can vary, but they are generally designed to be quite durable. On average, dental sealants last between 5 to 10 years. However, with proper care and regular dental check-ups, it's not uncommon for them to last even longer.
Several factors can influence how long a sealant remains intact and effective:
- Material Type: Resin-based sealants are generally considered more durable and long-lasting than glass ionomer sealants, although the latter offer the benefit of fluoride release.
- Oral Habits: Clenching or grinding teeth (bruxism), chewing on ice, hard candies, or other non-food items can put excessive stress on sealants, leading to premature wear or chipping.
- Placement Quality: A sealant applied in a completely dry and isolated environment with proper etching and curing will bond more effectively and last longer.
- Diet: A diet high in acidic foods and sugary snacks can contribute to enamel erosion around the sealant, potentially compromising its bond over time.
- Location: Sealants on teeth that experience heavier chewing forces might wear down faster.
During your routine dental check-ups, your dentist will inspect your existing sealants for any signs of wear, chips, or partial loss. If a sealant is compromised, it can usually be repaired by applying a new layer of sealant over the existing one or by completely replacing it. This simple maintenance helps ensure continuous protection against caries.
Potential Side Effects and Risks
Dental sealants are considered an extremely safe and low-risk dental procedure. The potential for side effects or complications is minimal, especially compared to the risks associated with untreated caries.
-
Allergic Reaction: While extremely rare, a patient could potentially have an allergic reaction to the sealant material. This is why it's important to inform your dentist of any known allergies. The primary resin used, Bis-GMA, has raised some concerns due to its theoretical link to BPA (Bisphenol A). However, scientific evidence overwhelmingly indicates that the minute amount of BPA exposure from sealants is negligible and poses no health risk, significantly less than daily exposure from food packaging. Major dental organizations, including the American Dental Association (ADA) and the CDC, affirm the safety of resin-based sealants.
-
Partial Loss/Wear: The most common "issue" is that a sealant might wear down, chip, or partially come off over time. This isn't harmful, but it means the tooth is no longer fully protected. Regular dental check-ups allow your dentist to monitor the integrity of the sealants and reapply or repair them as needed.
-
Bite Discrepancy: Occasionally, a newly applied sealant might feel slightly "high" when you bite down. This is easily corrected by the dentist, who can gently adjust (buff down) the sealant until your bite feels comfortable.
-
Trapped Bacteria (Extremely Rare): If a sealant is applied over an already existing, undetected microscopic cavity or if moisture contamination occurs during application, bacteria could theoretically become trapped underneath. However, modern diagnostic techniques and meticulous application protocols make this exceptionally rare. Even if bacteria are trapped, studies suggest that they are often "starved" and inactive, as the sealant cuts off their nutrient supply, preventing the decay from progressing.
Overall, the benefits of preventing caries with sealants far outweigh these minimal and manageable risks.
Cost of Dental Sealants in the US
The cost of dental sealants in the United States can vary depending on several factors, including the dentist's location, their fees, the type of sealant material used, and whether you have dental insurance.
Without Insurance:
- On average, the cost per tooth for a dental sealant ranges from $30 to $60.
- In some metropolitan areas or for more complex applications, the cost could be slightly higher, potentially reaching $70 to $80 per tooth.
With Insurance:
- Many dental insurance plans, especially those for children, provide significant coverage for dental sealants due to their preventative nature. It is widely recognized as a cost-effective way to prevent more expensive treatments later on.
- Depending on your plan, insurance may cover anywhere from 50% to 100% of the cost, often with no or minimal co-pay.
- Some plans might have age limits for sealant coverage (e.g., only covering children under 18 or 14).
- It's always best to check with your specific insurance provider for detailed information regarding your coverage, deductibles, and co-pays for "sealant dental" procedures.
Considering that the average cost of a single dental filling for a posterior tooth (amalgam or composite) can range from $100 to $250 or more, investing in sealants is a financially prudent preventative measure. Preventing just one cavity with a sealant can save you significantly in the long run.
Comparison: Sealants vs. Fluoride vs. Fillings
These three dental interventions all play a role in managing caries, but they serve different purposes. Understanding their distinctions is key to comprehensive oral health.
| Feature | Dental Sealant | Fluoride Treatment | Dental Filling |
|---|---|---|---|
| Primary Goal | Physical barrier to prevent decay in pits/fissures | Strengthen enamel, make it more acid-resistant | Repair existing decay (cavities) |
| Mechanism | Fills and seals deep grooves on chewing surfaces | Incorporates into enamel structure to resist acid | Removes decayed tooth structure, fills void with material |
| Indication | Healthy teeth with deep pits/fissures (preventative) | All tooth surfaces (preventative and remineralizing) | Tooth with existing decay (restorative) |
| Procedure | Quick, painless, no drilling, no anesthesia | Quick, painless, applied as gel, varnish, foam | Requires drilling, local anesthesia often needed |
| Duration | 5-10 years (can be repaired) | Ongoing; applied routinely (e.g., every 6 months) | 5-15+ years (depends on material and care) |
| Cost (US) | Low (approx. $30-$60/tooth) | Low (often covered, part of cleaning cost) | Moderate to High (approx. $100-$250+/tooth) |
| Tooth Structure | Preserves healthy tooth structure completely | Strengthens existing enamel structure | Removes decayed and some healthy tooth structure |
| Safety | Extremely safe, minimal risks | Very safe in appropriate doses | Generally safe; involves invasive procedure |
For Parents / Pediatric Considerations
Dental sealants are a cornerstone of pediatric dentistry and one of the most effective tools parents have to protect their children's teeth from caries. The period when permanent molars erupt is a critical window for sealant application.
- Timing is Key: The first permanent molars typically erupt around age 6, and the second permanent molars around age 12. Applying sealants shortly after these teeth fully emerge and before they have a chance to develop decay is crucial. Dentists often recommend applying sealants as soon as the tooth has completely broken through the gum line, ensuring all the vulnerable fissures are accessible.
- Vulnerability of Young Enamel: Newly erupted permanent teeth have enamel that is not yet fully hardened or mature. This makes them particularly susceptible to acid attacks and caries. Sealants provide immediate and robust protection during this vulnerable phase.
- Ease of Application: The non-invasive nature of sealant application makes it ideal for children. There's no drilling, no shots, and minimal discomfort, which can help foster a positive association with dental visits. This can be a huge benefit for children who may be anxious about dental procedures.
- Cost-Effectiveness: Investing in sealants for children is a highly cost-effective preventative measure. Preventing cavities in childhood reduces the need for more expensive and potentially uncomfortable fillings, crowns, or even extractions later on. It also helps avoid missed school days due to dental pain or appointments.
- Habit Formation: While sealants provide protection, they also complement and reinforce the importance of good oral hygiene. Parents should continue to teach and encourage regular brushing and flossing, as sealants protect specific surfaces but not the entire tooth.
Many pediatric dentists advocate for sealants as a routine part of preventative care for children, often recommending them for all four first permanent molars and all four second permanent molars. Discussing sealants with your child's dentist is an essential conversation for any parent committed to their child's long-term dental health.
Frequently Asked Questions
Are dental sealants painful?
No, dental sealants are not painful to apply. The procedure is entirely non-invasive, meaning there is no drilling, no needles, and no removal of tooth structure. You might feel the tooth being cleaned, rinsed, and dried, and the light used to cure the sealant, but there should be no discomfort. It's often described as one of the easiest and most comfortable dental procedures.
How much do dental sealants cost?
In the US, the average cost for a dental sealant per tooth typically ranges from $30 to $60 without insurance. With dental insurance, especially for children, a significant portion or even the full cost is often covered, as sealants are considered a crucial preventative treatment. It's always best to check with your specific insurance provider for exact coverage details.
How long does the application take?
The application process for a single dental sealant is very quick, usually taking only about 1 to 3 minutes per tooth. For multiple teeth, the total time will be longer but is still generally completed within a single appointment, often less than 20-30 minutes for all molars.
Are there alternatives to dental sealants?
While there isn't a direct "alternative" that provides the same physical barrier protection for the deep fissures of molars, other preventative measures are crucial. These include:
- Good Oral Hygiene: Consistent brushing with fluoride toothpaste and flossing.
- Fluoride Treatments: Professional fluoride applications, fluoride rinses, and fluoridated water help strengthen enamel against caries.
- Dietary Modifications: Limiting sugary and acidic foods and drinks. However, for the specific vulnerability of pits and fissures, sealants are unparalleled in their effectiveness. Once decay has occurred, the only "alternative" is a dental filling, which is a restorative rather than preventative treatment.
Does dental insurance cover sealants?
Yes, many dental insurance plans, especially those designed for families and children, do cover dental sealants. Because sealants are a highly effective preventative measure, insurance companies often view them as a cost-saving investment, as they reduce the likelihood of more expensive future treatments like fillings or crowns. Coverage levels can vary, but it's common to see 50% to 100% coverage, often with age limits (e.g., up to age 14 or 18). Always confirm with your insurance provider.
Do dental sealants contain BPA?
Modern dental sealants are typically made from resin-based materials like Bis-GMA. While Bis-GMA is related to BPA (Bisphenol A), the amount of BPA that might potentially leach from sealants is extremely minimal – hundreds to thousands of times lower than daily exposure from food and beverage packaging. Leading dental and health organizations, including the American Dental Association (ADA) and the Centers for Disease Control and Prevention (CDC), have affirmed that dental sealants are safe and their health benefits far outweigh any theoretical, negligible risks. For those with significant concerns, glass ionomer sealants are an alternative, though they may be less durable.
Can adults get dental sealants?
Absolutely! While most commonly applied to children's newly erupted permanent teeth, adults can certainly benefit from dental sealants. If an adult has deep fissures in their molars or premolars that are healthy, cavity-free, and not already filled, applying sealants can be an excellent preventative measure against future caries. This is especially true for adults with a high risk of decay due to factors like dry mouth, certain medical conditions, or a history of frequent cavities.
When to See a Dentist
Regular dental check-ups are paramount for maintaining oral health and ensuring the longevity of your dental sealants.
Routine Care:
- Every Six Months: Schedule routine dental examinations and cleanings every six months. During these visits, your dentist or dental hygienist will not only clean your teeth but also inspect all your existing dental sealants for wear, chips, or partial loss.
- Child's First Visit: It's recommended that children have their first dental visit by their first birthday or within six months of the eruption of their first tooth. Early and regular visits help establish good oral hygiene habits and allow the dentist to monitor tooth development, including the readiness for sealant dental application on newly erupted molars.
When to Seek Prompt Dental Attention:
- Damaged Sealant: If you or your child notices that a sealant feels rough, chipped, or a piece seems to be missing, contact your dentist. Even a partially compromised sealant can leave the tooth vulnerable to caries. Often, a simple repair or reapplication can restore protection.
- Sensitivity or Pain: While sealants themselves don't cause pain, if you develop new sensitivity, dull aches, or sharp pain in a sealed tooth, it could indicate an underlying issue such as new decay (if the sealant has failed), a cracked tooth, or other dental problems.
- Persistent Food Trapping: If food consistently gets stuck in a particular tooth even with a sealant, it might indicate an issue with the sealant's integrity or application.
- Visible Hole or Discoloration: Any visible hole or dark discoloration on a tooth, even if it has a sealant, warrants immediate dental evaluation as it could be a sign of caries.
Remember, dental sealants are a highly effective preventative measure, but they are not a "set it and forget it" solution. Consistent monitoring by your dental professional ensures their continued effectiveness in protecting your smile from caries.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.