Molar
4,806 words · 16 min read
Quick Definition
The large, flat teeth at the back of the mouth designed for grinding and chewing food. Adults have 12 molars, including the third molars (wisdom teeth).
Introduction: What is a Molar?
Molars are the unsung workhorses of our mouths, the large, flat teeth positioned at the very back that are expertly designed for the crucial task of grinding and pulverizing food. Unlike the sharp incisors for biting or the pointed canines for tearing, molars feature broad, uneven chewing surfaces perfectly adapted to break down food into smaller, more digestible pieces. This essential function not only aids digestion but also plays a vital role in nutrient absorption. In a healthy adult dentition, there are typically 12 molars – three on each side of both the upper and lower jaws. These include the often-discussed third molars, commonly known as wisdom teeth.
Understanding molars is paramount for maintaining optimal dental health. Due to their location at the back of the mouth and their complex anatomy, molars are particularly susceptible to issues like tooth decay and gum disease. Their deeply grooved surfaces, known as fissures, can easily trap food particles and bacteria, making them prime targets for cavities. Moreover, wisdom teeth, as the last teeth to erupt, frequently cause complications such as impaction, pain, and infection. Globally, dental caries (cavities), which disproportionately affect molars, are among the most common chronic diseases, impacting millions of Americans annually. A significant percentage of adults experience at least one molar-related issue throughout their lives, highlighting the need for vigilance and proper care. This comprehensive guide will delve into every aspect of molars, from their anatomy and function to common problems, treatments, and essential prevention strategies, ensuring you have the definitive resource for protecting these vital teeth.
Key Takeaways:
- Primary Function: Molars are the large, flat back teeth crucial for grinding and chewing food, aiding digestion.
- Adult Count: Adults typically have 12 molars, including the third molars (wisdom teeth).
- Vulnerability: Their deep grooves (fissures) make molars highly susceptible to cavities and food impaction.
- Wisdom Teeth: Third molars often cause complications like impaction, pain, and infection.
- Prevention is Key: Regular hygiene, dental check-ups, and preventative measures like sealants are essential for molar health.
- Costly Issues: Treating molar problems like deep cavities or impacted wisdom teeth can be expensive, ranging from $150 to $4,000+ depending on the complexity.
Detailed Explanation
Types and Classifications of Molars
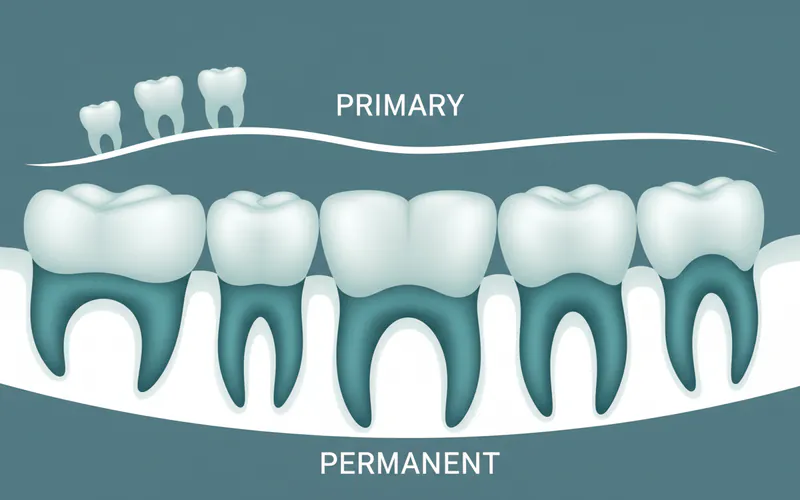
Molars are categorized in several ways, primarily by their position in the arch and whether they are primary (baby) or permanent teeth.
-
Permanent Molars:
- First Molars (Six-Year Molars): These are usually the first permanent teeth to erupt, typically around age 6. They emerge behind the last baby teeth, often without any baby tooth falling out first, which can sometimes lead parents to mistake them for baby teeth. These molars are crucial for establishing the bite and are often the largest teeth in the mouth.
- Second Molars (Twelve-Year Molars): These erupt around age 12, positioned behind the first molars. Like the first molars, they play a significant role in chewing efficiency and maintaining the proper alignment of the dental arch.
- Third Molars (Wisdom Teeth): These are the last teeth to erupt, usually between ages 17 and 25. Not everyone develops all four wisdom teeth, and many people have them removed due to impaction, crowding, or other complications. They are named "wisdom teeth" because they appear at a more mature age.
-
Primary (Deciduous) Molars:
- Children have 8 primary molars – two on each side of the upper and lower jaws. These are crucial for chewing during childhood, holding space for the permanent teeth to erupt correctly, and guiding their development. They are gradually replaced by premolars and permanent molars between the ages of 6 and 12.
- First Primary Molars typically erupt around 13-19 months.
- Second Primary Molars typically erupt around 25-33 months.
Anatomy and Function: Molars are characterized by their multi-cusped chewing surface and multiple roots, which firmly anchor them in the jawbone.
- Cusps: These are the raised points on the chewing surface, vital for grinding food. Upper molars typically have three or four cusps, while lower molars usually have four or five.
- Fissures and Grooves: The valleys and depressions between the cusps are called fissures and grooves. While essential for efficient chewing, these deep, narrow areas are highly prone to trapping food particles and bacteria, making them primary sites for cavity formation. This is why dental sealants are so effective on molars.
- Roots: Molars have a robust root system for stability. Upper molars typically have three roots, while lower molars usually have two roots. These roots contain the pulp chamber and root canals, housing the nerves and blood vessels of the tooth.
Common Issues Affecting Molars
Molars are susceptible to various dental problems due to their anatomy, location, and role in chewing.
- Dental Caries (Cavities): The most prevalent issue. Deep fissures on the chewing surfaces easily trap plaque and food, leading to decay. Cavities in molars can progress rapidly if not addressed, potentially leading to pulp infection. According to the CDC, 91% of adults aged 20-64 have had dental caries in their permanent teeth, with molars being significantly affected.
- Impacted Wisdom Teeth: When third molars don't have enough space to erupt properly, they can become impacted, growing in at an angle or remaining fully or partially submerged beneath the gum line. This can lead to pain, infection, cysts, damage to adjacent teeth, and orthodontic problems.
- Cracked or Fractured Molars: Due to the intense chewing forces they endure, molars are prone to cracks, especially in individuals who grind their teeth (bruxism) or have large fillings that weaken the tooth structure. Cracks can range from minor chips to severe fractures extending into the root.
- Periodontal Disease (Gum Disease): Molars, especially those in hard-to-reach areas, can accumulate plaque and tartar, leading to gingivitis and eventually periodontitis. This infection of the gums and supporting bone can cause tooth loosening and even loss if untreated.
- Bruxism (Teeth Grinding): Chronic grinding or clenching puts immense pressure on molars, leading to excessive wear, sensitivity, fractures, and damage to existing restorations.
- Abfraction: A type of non-carious tooth tissue loss that occurs at the gum line due to biomechanical loading forces on the teeth (often from clenching/grinding).
Causes and Risk Factors
Several factors contribute to molar-related dental problems:
- Poor Oral Hygiene: Inadequate brushing and flossing, especially in the posterior regions, allow plaque to accumulate in molar fissures and along the gum line, fostering decay and gum disease.
- High-Sugar and Acidic Diet: Frequent consumption of sugary foods and drinks feeds cavity-causing bacteria. Acidic foods and beverages contribute to enamel erosion.
- Genetics: Predisposition to certain dental conditions, such as enamel weakness, specific jaw structures (leading to wisdom tooth impaction), or susceptibility to gum disease, can be inherited.
- Lack of Fluoride: Fluoride strengthens enamel, making teeth more resistant to acid attacks. Insufficient fluoride exposure is a risk factor for cavities.
- Dry Mouth (Xerostomia): Saliva helps wash away food particles and neutralize acids. Reduced saliva flow (due to medications, medical conditions, or aging) increases cavity risk.
- Bruxism/Clenching: Unconscious grinding or clenching of teeth places excessive stress on molars, leading to wear, cracks, and fractures.
- Smoking/Tobacco Use: Significantly increases the risk of gum disease, slows healing, and can mask symptoms of oral issues.
- Age: The longer teeth are in the mouth, the more exposure they have to wear, tear, and potential decay. Wisdom teeth complications are also age-related.
Signs and Symptoms to Watch For
Recognizing early signs can prevent minor issues from becoming major problems.
- Pain:
- Sharp pain when biting down suggests a crack, deep cavity, or loose filling.
- Lingering pain after consuming hot or cold foods/drinks indicates potential pulp damage.
- Dull ache in the back of the jaw could signal a growing cavity, gum infection, or wisdom tooth impaction.
- Sensitivity: Especially to hot, cold, or sweet foods/drinks, which can indicate enamel erosion, receding gums, or a cavity.
- Swelling: Swelling around a molar or in the jaw can point to an abscess, severe infection, or an erupting/impacted wisdom tooth.
- Difficulty Chewing: Pain or discomfort while chewing, especially on one side, suggests a problem with the affected molar.
- Persistent Bad Breath or Unpleasant Taste: Can be a sign of infection, deep decay, or periodontal disease.
- Visible Holes or Pits: A clear indication of a cavity.
- Red, Swollen, or Bleeding Gums: Symptoms of gingivitis or periodontitis around the molar.
- Clicking or Popping Jaw: In some cases, impacted wisdom teeth can affect jaw joint function.
Diagnosis Process — What Your Dentist Does
A thorough dental examination is crucial for diagnosing molar problems.
- Clinical Examination: Your dentist will visually inspect your molars for visible signs of decay, cracks, gum inflammation, and any abnormalities. They will use a dental explorer to gently probe the surfaces for soft spots indicating decay.
- Dental X-rays:
- Bitewing X-rays: These show the crowns of the upper and lower posterior teeth, revealing decay between teeth (interproximal decay) and beneath existing fillings, which are common in molars.
- Periapical X-rays: These capture the entire tooth, from crown to root tip, and the surrounding bone, useful for detecting root infections, abscesses, and bone loss due to periodontal disease.
- Panoramic X-rays: A single image of the entire mouth, showing all teeth, jawbones, and sinuses. This is invaluable for assessing wisdom tooth position, impaction, and potential issues before they erupt.
- CBCT (Cone Beam Computed Tomography): For complex cases, such as deeply impacted wisdom teeth or intricate root canal anatomy, a 3D scan provides detailed imaging.
- Pulp Vitality Testing: If an infection is suspected within the tooth, tests using cold (e.g., endo-ice) or an electric pulp tester can determine if the nerve is still alive and responsive.
- Periodontal Probing: A small ruler-like probe measures the depth of gum pockets around molars to detect gum disease.
- Bite Test: If a cracked tooth is suspected, the dentist may have you bite on a tooth slooth or similar instrument to localize the pain.
Treatment Options with Pros, Cons, and Costs
Treatment for molar problems varies widely depending on the diagnosis.
1. Dental Fillings (for cavities)
- Description: Removal of decayed tooth material and filling the space with a restorative material.
- Types:
- Amalgam (Silver) Fillings: Durable, cost-effective.
- Pros: Very strong, lasts a long time, relatively inexpensive.
- Cons: Silver appearance, mercury content (though considered safe by ADA), can expand/contract, potentially causing cracks over time.
- Cost: $50 - $200 per tooth (without insurance).
- Composite (Tooth-Colored) Fillings: Esthetically pleasing.
- Pros: Matches natural tooth color, chemically bonds to tooth structure, mercury-free.
- Cons: Less durable than amalgam for very large restorations, can stain over time, typically more expensive.
- Cost: $100 - $350 per tooth (without insurance).
- Amalgam (Silver) Fillings: Durable, cost-effective.
- Comparison:
Feature Amalgam Filling Composite Filling Appearance Silver/Metallic Tooth-colored, blends naturally Durability Very high, good for back teeth Good, but slightly less for large fills Cost (USA) $50 - $200 $100 - $350 Material Metal alloy (mercury, silver, tin) Resin and glass particles Bonding Mechanical retention Chemical bond to tooth Time to Place Shorter Longer (layering, curing)
2. Dental Crowns (Caps)
- Description: A custom-made cap placed over a damaged tooth to restore its shape, size, strength, and appearance. Used for large cavities, fractured molars, or after a root canal.
- Types:
- Porcelain-Fused-to-Metal (PFM): Strong with a natural appearance.
- Pros: Durable, good esthetics.
- Cons: Can show a dark line at the gum line, more tooth reduction needed.
- Cost: $800 - $1,500 per crown.
- All-Ceramic (Porcelain or Zirconia): Highly esthetic, metal-free.
- Pros: Excellent esthetics, biocompatible, no dark gum line. Zirconia is exceptionally strong, great for molars.
- Cons: Can be more expensive, porcelain can be abrasive to opposing teeth if not properly polished.
- Cost: $1,000 - $2,500 per crown.
- Gold/Metal Alloys: Extremely durable, rarely chip.
- Pros: Very strong, long-lasting, gentle on opposing teeth, minimal tooth reduction.
- Cons: Esthetics (gold color), higher material cost.
- Cost: $900 - $2,000 per crown.
- Porcelain-Fused-to-Metal (PFM): Strong with a natural appearance.
- Cost Range (General): $800 - $2,500 per molar crown (without insurance).
3. Root Canal Therapy
- Description: Removal of infected or inflamed pulp (nerve tissue) from inside the tooth, cleaning and shaping the root canals, and then filling and sealing the space. A crown is usually placed afterward.
- Pros: Saves the natural tooth, prevents extraction, preserves chewing function.
- Cons: Requires multiple appointments, can be expensive, tooth becomes brittle and often needs a crown.
- Cost: $700 - $1,500 for a molar (root canal only, without a crown) from a general dentist; $900 - $2,000+ from an endodontist. A crown adds another $800 - $2,500.
4. Molar Extraction
- Description: Surgical removal of a tooth that is severely damaged, decayed beyond repair, or causing problems (e.g., impacted wisdom tooth).
- Pros: Eliminates pain/infection, resolves crowding issues.
- Cons: Loss of a natural tooth, can lead to shifting of adjacent teeth, requires replacement (implant, bridge) to maintain bite, potential for dry socket or infection.
- Cost:
- Simple Extraction: $75 - $300 per tooth.
- Surgical Extraction (e.g., impacted wisdom tooth): $200 - $800 per tooth (uncomplicated); $500 - $1,500 per tooth for complex impaction, often performed by an oral surgeon. Anesthesia adds to the cost.
5. Dental Sealants
- Description: A thin, protective coating applied to the chewing surfaces of molars, especially the fissures, to prevent food and bacteria from getting trapped and causing cavities. Primarily used as a preventative measure.
- Pros: Highly effective in preventing molar cavities, non-invasive, quick procedure, pain-free. Reduces cavity risk by 80% in molars.
- Cons: Can wear off over time and need reapplication, not a treatment for existing cavities.
- Cost: $30 - $60 per tooth.
Step-by-Step: What to Expect During Treatment
Let's look at what to expect for a common molar filling and a wisdom tooth extraction.
For a Molar Filling (Composite):
- Anesthesia: The dentist will numb the area around the affected molar using a local anesthetic injection. You might feel a slight pinch, followed by numbness.
- Decay Removal: Using a dental drill, the dentist will carefully remove the decayed tooth structure. The sound and vibration might be noticeable, but you shouldn't feel pain.
- Preparation: The tooth is cleaned, and an etching gel is applied to create microscopic pores for better bonding. A bonding agent is then applied and light-cured.
- Filling Placement: The tooth-colored composite resin is applied in layers, with each layer cured (hardened) using a special blue light.
- Shaping and Polishing: The dentist will shape the filling to match the natural contours of your tooth and ensure it fits your bite. Finally, the filling is polished for a smooth finish.
- Duration: Typically 30-60 minutes for one filling.
For a Wisdom Tooth Extraction:
- Consultation & X-rays: An initial appointment for diagnosis, often including a panoramic X-ray to assess the tooth's position, roots, and proximity to nerves or sinuses.
- Anesthesia: For simple extractions, local anesthesia is used. For impacted wisdom teeth, oral surgeons often offer options like IV sedation or general anesthesia for a more comfortable, pain-free experience.
- Incision & Bone Removal (if necessary): For impacted teeth, the surgeon may need to make an incision in the gum tissue to access the tooth and remove a small amount of bone covering it.
- Tooth Sectioning: The tooth may be cut into smaller pieces to facilitate easier removal, especially if it's impacted or has complex roots.
- Extraction: The tooth is gently but firmly removed using specialized instruments.
- Sutures & Gauze: The gum flap is typically closed with dissolvable sutures, and gauze is placed over the extraction site to control bleeding and help a blood clot form.
- Duration: A single wisdom tooth extraction can take 20-60 minutes, but multiple extractions or complex cases will take longer.
Recovery Timeline and Aftercare
After a Molar Filling:
- Numbness: Will wear off in 1-3 hours. Avoid eating until then to prevent biting your cheek or tongue.
- Sensitivity: It's common to experience some sensitivity to hot, cold, or pressure for a few days to a few weeks, especially with deeper fillings. This usually subsides.
- Pain: Mild discomfort can be managed with over-the-counter pain relievers (e.g., ibuprofen).
- Eating: You can typically eat immediately after composite fillings, but avoid very hard or sticky foods for the first day.
After Molar/Wisdom Tooth Extraction:
- First 24 Hours:
- Keep gauze in place for 30-45 minutes to encourage blood clot formation. Change as needed.
- Avoid rinsing vigorously, spitting, or using a straw, which can dislodge the blood clot and lead to a painful dry socket.
- Apply ice packs to the outside of your face to reduce swelling.
- Eat soft foods (yogurt, soup, mashed potatoes).
- Take prescribed pain medication as directed.
- Days 2-3:
- Swelling usually peaks and then begins to subside.
- You can gently rinse with warm salt water (1/2 tsp salt in 8 oz water) after 24 hours to help keep the area clean.
- Continue with soft foods.
- Week 1:
- Most pain and swelling should significantly decrease.
- Resume normal oral hygiene gently around the extraction site.
- Sutures, if non-dissolvable, are usually removed by the dentist around this time.
- Weeks 2-6:
- The socket continues to heal and fill in with new bone and tissue.
- Return to a normal diet gradually.
- Full Healing: Can take several months for complete bone regeneration.
Prevention Strategies
Preventing molar issues is far easier and less expensive than treating them.
- Excellent Oral Hygiene:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste for at least two minutes, paying extra attention to the chewing surfaces and back of your molars.
- Floss Daily: Floss between all teeth, especially molars, to remove trapped food and plaque.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleaning and examination. Early detection of cavities or gum disease is crucial.
- Dental Sealants: For children and even adults with deep fissures on their molars, sealants are highly recommended. This protective plastic coating can prevent up to 80% of cavities in molars.
- Balanced Diet: Limit sugary and acidic foods and drinks. Opt for nutrient-rich foods that promote oral health. Drink plenty of water, especially fluoridated water.
- Fluoride Protection: Use fluoride toothpaste and consider fluoride mouthrinses if your dentist recommends them.
- Mouthguards for Bruxism: If you grind or clench your teeth, a custom-fitted nightguard can protect your molars from excessive wear and potential fractures.
- Avoid Harmful Habits: Do not use your teeth as tools (opening bottles, tearing packages). Avoid chewing on ice or hard candies.
- Quit Smoking/Tobacco: Eliminating tobacco products significantly improves oral and overall health.
Cost Ranges in the US (with/without insurance)
Dental costs can vary significantly based on location, the dentist's fees, the complexity of the procedure, and whether it's performed by a general dentist or a specialist (e.g., oral surgeon, endodontist).
| Procedure | Average Cost (Without Insurance) | Average Cost (With Insurance - Patient Out-of-Pocket) |
|---|---|---|
| Composite Filling (Molar) | $100 - $350 | $20 - $100 (after deductible & coinsurance) |
| Amalgam Filling (Molar) | $50 - $200 | $10 - $70 (after deductible & coinsurance) |
| Molar Crown (All-Ceramic) | $1,000 - $2,500 | $250 - $1,200 (often 50% coverage after deductible) |
| Root Canal (Molar) | $700 - $1,500 (general) | $150 - $750 (often 50-80% coverage) |
| Root Canal (Specialist) | $900 - $2,000+ | $200 - $1,000+ |
| Simple Molar Extraction | $75 - $300 | $15 - $100 (often 80% coverage) |
| Surgical Wisdom Tooth Extraction (Impacted) | $500 - $1,500 per tooth | $100 - $750 per tooth (depending on medical/dental plan) |
| Dental Sealant (Per Molar) | $30 - $60 | $0 - $20 (often 80-100% covered for children) |
| Dental Cleaning & Exam | $75 - $200 | $0 - $50 (often 100% covered) |
Most dental insurance plans have annual maximums, typically ranging from $1,000 to $2,000. Once this limit is reached, you are responsible for 100% of costs. Many plans also have waiting periods for major procedures.
``
For Parents / Pediatric Considerations
Molars are particularly important in pediatric dentistry, as both primary and permanent molars play critical roles in a child's oral development.
- Eruption Schedule:
- Primary First Molars: Erupt around 13-19 months.
- Primary Second Molars: Erupt around 25-33 months. These are crucial for proper chewing in toddlers and preschoolers.
- Permanent First Molars (Six-Year Molars): These are often the first permanent teeth to emerge, around age 6, behind the existing baby teeth. It's vital for parents to recognize these are permanent and require diligent care.
- Permanent Second Molars (Twelve-Year Molars): Erupt around age 12.
- Cavity Vulnerability: Children's molars are highly susceptible to cavities for several reasons:
- Deep Fissures: Baby molars and newly erupted permanent molars have deep grooves that are excellent traps for food and bacteria.
- Developing Oral Hygiene: Children may not yet have the dexterity or discipline for thorough brushing, especially in the back of the mouth.
- Diet: Many children consume sugary snacks and drinks, increasing cavity risk.
- Dental Sealants are Key: For newly erupted permanent molars (first and second molars), dental sealants are a highly effective preventative measure. Applying a thin plastic coating to the fissures significantly reduces the risk of decay by sealing out food and plaque. The CDC reports that school-aged children with sealants have nearly 3 times fewer cavities in their first permanent molars than children without.
- Space Maintainers: If a primary molar is lost prematurely due to severe decay or trauma, a space maintainer may be recommended. This device holds the space open for the permanent tooth to erupt correctly, preventing adjacent teeth from shifting and causing orthodontic problems.
- Monitoring Wisdom Teeth: While wisdom teeth don't typically erupt until late teens/early twenties, monitoring their development with X-rays can begin in early adolescence to predict potential impaction or other issues.
- Thumb Sucking/Pacifier Use: Prolonged thumb sucking or pacifier use past early childhood can affect the development of the jaw and the alignment of molars, potentially leading to bite problems.
``
Frequently Asked Questions
Q1: Are molars always painful when they come in, especially wisdom teeth?
A1: Not always, but it's very common. When a permanent molar, particularly a wisdom tooth, erupts, it pushes through the gum tissue, which can cause discomfort, swelling, and tenderness. For wisdom teeth, the pain can be more severe due to insufficient space in the jaw, leading to impaction. This can cause inflammation (pericoronitis), infection, and pressure on adjacent teeth. Over-the-counter pain relievers, warm salt water rinses, and good oral hygiene can help manage symptoms during eruption. If pain is severe or persistent, or if there's swelling, see your dentist.
Q2: How much does a molar filling cost in the US, and is it covered by insurance?
A2: The cost of a molar filling varies based on the material, size, and location. Composite (tooth-colored) fillings typically range from $100 to $350, while amalgam (silver) fillings are generally $50 to $200 without insurance. Most dental insurance plans cover a significant portion of filling costs, usually 70-80% after you've met your deductible. Your out-of-pocket cost with insurance could be anywhere from $10 to $100+, depending on your specific plan's benefits and remaining annual maximum.
Q3: What's the main difference between a premolar and a molar?
A3: The primary difference lies in their location, size, and number of cusps. Premolars (also called bicuspids) are located just in front of the molars, behind the canines. Adults have 8 premolars. They are smaller than molars, typically have two cusps, and their function is a hybrid of tearing and grinding food. Molars, on the other hand, are the largest teeth at the very back of the mouth, designed primarily for heavy grinding. They typically have four or five cusps and more complex chewing surfaces.
Q4: Can a molar with a deep cavity always be saved, or does it sometimes need to be extracted?
A4: A molar with a deep cavity can often be saved, especially if the decay hasn't yet reached the pulp (the tooth's nerve). If the decay is extensive and has infected the pulp, a root canal therapy is typically performed to remove the infected tissue and save the tooth. However, if the cavity is so large that it has severely compromised the tooth's structure, or if the tooth is fractured below the gum line or has an untreatable infection, extraction may be the only viable option. Your dentist will assess the extent of the damage with X-rays and a clinical exam to determine the best course of action.
Q5: What are dental sealants and how do they help protect molars?
A5: Dental sealants are thin, plastic coatings painted onto the chewing surfaces of the back teeth (molars and premolars). They flow into the deep fissures and grooves of the tooth, hardening to create a smooth, protective barrier. This barrier effectively seals out food particles and cavity-causing bacteria, preventing them from accumulating in these vulnerable areas. Sealants are particularly effective for children and teenagers whose permanent molars have just erupted, reducing the risk of cavities by up to 80%. They are a safe, painless, and highly recommended preventive measure.
Q6: Does dental insurance cover molar treatments like wisdom tooth removal or root canals?
A6: Yes, most dental insurance plans provide coverage for molar treatments, but the extent of coverage varies significantly.
- Wisdom Tooth Removal: Coverage depends on whether it's classified as a "simple" or "surgical" extraction and if it's considered medically necessary. Many plans cover 50-80% of the cost. Complex impacted wisdom tooth extractions might also have partial coverage under medical insurance if performed by an oral surgeon.
- Root Canals: These are typically categorized as "major procedures" and are usually covered at 50-80% of the cost after your deductible is met. It's crucial to check with your specific insurance provider for details on your plan's benefits, deductibles, co-pays, and annual maximums before undergoing treatment.
``
When to See a Dentist
Knowing when to seek professional dental care is crucial for preserving your molar health.
Routine Care (Schedule an appointment):
- Every 6 months: For a regular dental check-up and professional cleaning. This is essential for early detection and prevention of molar issues.
- When you notice mild, persistent sensitivity: To hot, cold, or sweets, which could be an early sign of a cavity or receding gums.
- If you suspect you're grinding your teeth (bruxism): Especially if you wake up with jaw pain or notice your teeth look flattened.
- For evaluation of newly erupted wisdom teeth: To ensure they are coming in properly and not causing issues.
- If a sealant or filling feels rough or has come loose: It needs to be checked and potentially repaired or replaced.
Emergency Signs (See a dentist immediately or seek urgent care):
- Severe, throbbing, or persistent pain: Especially if it disrupts sleep or is not relieved by over-the-counter medication. This could indicate a deep infection or abscess.
- Swelling in the jaw, face, or around a molar: Swelling can be a sign of a serious infection that requires immediate attention.
- A "pimple" or boil on the gums: Near a molar, which can signify a dental abscess trying to drain.
- Difficulty opening your mouth fully or swallowing: Coupled with molar pain or swelling, this can indicate a spreading infection.
- Trauma to a molar: Such as a completely knocked-out tooth, a severe crack from an injury, or a loose molar after an accident.
- Uncontrolled bleeding: From an extraction site after the initial post-procedure period.
- Signs of a dry socket: Severe pain 3-5 days after an extraction, often radiating to the ear, with a visible empty socket.
Delaying dental care for molar problems can lead to more extensive damage, increased pain, higher treatment costs, and even systemic health issues if infections spread. Prioritize your oral health by staying vigilant and consulting your dental professional regularly.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.