Wisdom Tooth
3,881 words · 13 min read
Quick Definition
The third and final set of molars that typically emerge between ages 17 and 25. Wisdom teeth often become impacted due to insufficient space in the jaw and frequently require extraction.
Welcome to SmilePedia.net, your definitive resource for understanding all aspects of dental health. In this comprehensive article, we delve deep into the topic of wisdom teeth, often a source of curiosity, concern, and sometimes, discomfort for many adults.
Introduction
A wisdom tooth, medically known as a third molar, is the final set of molars to emerge in the mouth. These teeth typically make their appearance much later than other permanent teeth, usually erupting between the ages of 17 and 25. This period, often associated with the transition from adolescence to adulthood, is where the term "wisdom tooth" originated, as it's when individuals are supposedly "wiser."
However, wisdom teeth are not always a welcome addition to the dental arcade. For a significant portion of the population, their eruption can lead to a host of problems due to a lack of sufficient space in the jaw. This common issue often results in impaction, where the tooth is unable to fully emerge or grows at an abnormal angle, leading to pain, infection, or damage to adjacent teeth. Consequently, the extraction of wisdom teeth has become one of the most common oral surgical procedures performed worldwide.
Understanding what wisdom teeth are, why they cause problems, and the available treatment options is crucial for maintaining optimal oral health. Approximately 85% of wisdom teeth will eventually need to be removed, affecting millions of individuals in the United States alone each year. This article aims to equip you with all the knowledge you need to navigate the complexities surrounding your wisdom teeth.
Key Takeaways:
- Wisdom teeth are the third and final set of molars, emerging between 17 and 25 years old.
- Many people lack sufficient jaw space for wisdom teeth, leading to impaction.
- Impaction can cause pain, infection, and damage to surrounding teeth.
- Extraction is a common solution for problematic wisdom teeth.
- Regular dental check-ups with X-rays are vital for monitoring wisdom teeth.
- Ignoring wisdom tooth problems can lead to more severe dental health issues.
Detailed Explanation
Types and Classifications of Wisdom Teeth
Wisdom teeth can present in various ways, largely categorized by their state of eruption and position. Understanding these classifications helps determine the potential risks and necessary treatment.
-
Erupted Wisdom Teeth: These are wisdom teeth that have fully emerged through the gum line and are properly aligned with the rest of your teeth. If they are functional, cleanable, and not causing issues, they may not require removal.
-
Impacted Wisdom Teeth: This is the most common and problematic scenario. An impacted wisdom tooth is one that is blocked from fully erupting into its proper position. Impaction can be caused by various factors, including insufficient jaw space or obstruction by another tooth. Impacted teeth are further classified by their angle and the amount of gum and bone covering them:
- Angular (Mesial or Distal Impaction):
- Vertical Impaction: The tooth is oriented correctly (straight up and down) but is stuck below the gum line or against the second molar.
- Horizontal Impaction: The tooth is lying completely on its side, usually pressing directly into the adjacent second molar, often causing significant damage.
- Soft Tissue Impaction: The tooth has partially erupted but is still covered by gum tissue. This can create a flap of gum (operculum) that traps food and bacteria, leading to infection (pericoronitis).
- Partial Bony Impaction: A portion of the tooth has erupted, but part of it remains embedded in the jawbone and covered by gum tissue. Like soft tissue impaction, this can also lead to pericoronitis.
- Full Bony Impaction: The tooth is completely encased within the jawbone and has not broken through the gum line at all. These are often the most complex to remove.
Causes and Risk Factors
The primary reason wisdom teeth often become problematic lies in human evolution. Over millennia, human jaws have progressively become smaller, likely due to changes in diet and food preparation (less chewing of tough, raw foods). While our jaws have shrunk, the number of teeth has largely remained the same, leading to a common mismatch between jaw size and tooth size.
Key causes and risk factors include:
- Insufficient Jaw Space: This is the overwhelming factor. Modern human jaws often simply do not have enough room to accommodate these extra molars without crowding existing teeth.
- Genetics: Jaw size and tooth size are largely inherited. If your parents or close relatives had impacted wisdom teeth, you might be more prone to them.
- Early Loss of Permanent Teeth: While less common, the early loss of other permanent teeth can sometimes lead to slight shifts in tooth positioning, potentially impacting wisdom tooth eruption.
- Developmental Anomalies: Rarely, abnormal development of the tooth bud can lead to unusual shapes or positions that contribute to impaction.
Signs and Symptoms to Watch For
Not all problematic wisdom teeth will immediately cause symptoms, but when they do, it's a clear signal to see your dentist.
- Pain: Often dull and throbbing, located at the back of the jaw, or sharp when biting. It can radiate to the ear, head, or neck.
- Swelling: Swelling of the gums, jaw, or even the face around the affected area.
- Infection (Pericoronitis): This is an inflammation of the gum tissue surrounding a partially erupted wisdom tooth, caused by trapped food and bacteria. Symptoms include intense pain, redness, swelling, pus discharge, bad taste in the mouth, and sometimes fever.
- Bad Breath (Halitosis): Due to bacterial accumulation around an impacted or partially erupted tooth.
- Difficulty Opening Mouth (Trismus): Muscle spasms or inflammation can make it painful or difficult to open your jaw fully.
- Jaw Stiffness or Tenderness: Localized discomfort in the jaw muscles.
- Damage to Adjacent Teeth: Pressure from an impacted wisdom tooth can cause resorption (erosion) or cavities in the neighboring second molar.
- Cyst Formation: In rare cases, a fluid-filled sac (cyst) can develop around the crown of an impacted tooth, potentially damaging bone and surrounding tissues.
Diagnosis Process — What Your Dentist Does
Diagnosing wisdom tooth issues is a straightforward process typically involving a combination of clinical examination and imaging.
- Visual Examination: Your dentist will examine your mouth, checking for signs of swelling, redness, tenderness, or any visible wisdom teeth. They will look for indications of pericoronitis or other soft tissue inflammation.
- Dental X-rays: This is the most critical diagnostic tool.
- Panoramic X-ray: This single X-ray image captures a comprehensive view of your entire mouth, including all teeth, both jaws, and surrounding structures. It's invaluable for visualizing the position, angle, and stage of development of all four wisdom teeth, as well as their relationship to adjacent teeth and important anatomical structures like nerves and sinuses.
- Periapical X-rays: Sometimes, smaller, more detailed X-rays of a specific area might be taken to get a closer look at a single wisdom tooth.
- Discussion of Symptoms: Your dentist will ask about any pain, swelling, or other symptoms you've been experiencing. They will also inquire about your medical history and any medications you are taking.
Based on this information, your dentist can accurately diagnose any issues and recommend the appropriate course of action.
Treatment Options
For problematic wisdom teeth, extraction is the most common and often the only effective treatment. However, in some limited cases, monitoring may be an option.
1. Monitoring (Observation)
- Description: For wisdom teeth that are fully erupted, aligned, functional, and easily cleanable, or for those that are deeply impacted and asymptomatic, your dentist might recommend a "wait and see" approach. This involves regular dental check-ups and X-rays to monitor for any changes.
- Pros: Avoids surgery and associated risks. No recovery time.
- Cons: Potential for future problems (pain, infection, damage) to arise unexpectedly. Requires diligent oral hygiene and regular professional monitoring.
- Cost: Minimal, limited to routine check-up and X-ray fees (typically $50 - $200 per visit without insurance).
2. Wisdom Tooth Extraction
This is the removal of one or more wisdom teeth. The complexity of the extraction depends on whether the tooth is erupted or impacted.
- Simple Extraction:
- Description: Performed on fully erupted wisdom teeth that are visible in the mouth, similar to the removal of any other visible tooth. The tooth is loosened with instruments and then gently removed.
- Pros: Less invasive than surgical extraction. Shorter procedure time. Generally faster recovery.
- Cons: Not suitable for impacted teeth.
- Cost: Typically $75 - $250 per tooth without insurance.
- Surgical Extraction:
- Description: Required for impacted wisdom teeth, especially those partially or fully embedded in bone or under the gum line. This procedure involves making an incision in the gum, sometimes removing a small amount of bone covering the tooth, and often sectioning (cutting) the tooth into smaller pieces for easier removal. The gum is then sutured closed.
- Pros: Effectively removes problematic impacted teeth, preventing future complications.
- Cons: More invasive procedure. Longer recovery time. Higher risk of complications (e.g., dry socket, nerve damage, infection, swelling).
- Cost: Typically $200 - $750+ per tooth, or even more for very complex cases, without insurance.
Comparison Table: Simple vs. Surgical Wisdom Tooth Extraction
| Feature | Simple Extraction | Surgical Extraction |
|---|---|---|
| Tooth Status | Fully erupted, visible | Impacted (partially or fully in bone/gum) |
| Procedure | Loosening and removal with forceps | Incision, bone removal, tooth sectioning, sutures |
| Anesthesia | Local anesthesia (novocaine) | Local anesthesia, often combined with IV sedation/general |
| Duration | 5-15 minutes per tooth | 20-60 minutes per tooth |
| Recovery | 1-3 days | 3-7 days for initial recovery, weeks for full healing |
| Post-Op Pain | Mild to moderate | Moderate to severe |
| Risks | Minor bleeding, swelling | Increased risk of dry socket, nerve damage, infection |
| Cost (per tooth) | $75 - $250 (without insurance) | $200 - $750+ (without insurance) |
Step-by-Step: What to Expect During Treatment
The following outlines what to expect during a typical surgical wisdom tooth extraction. Simple extractions follow a similar but less complex path.
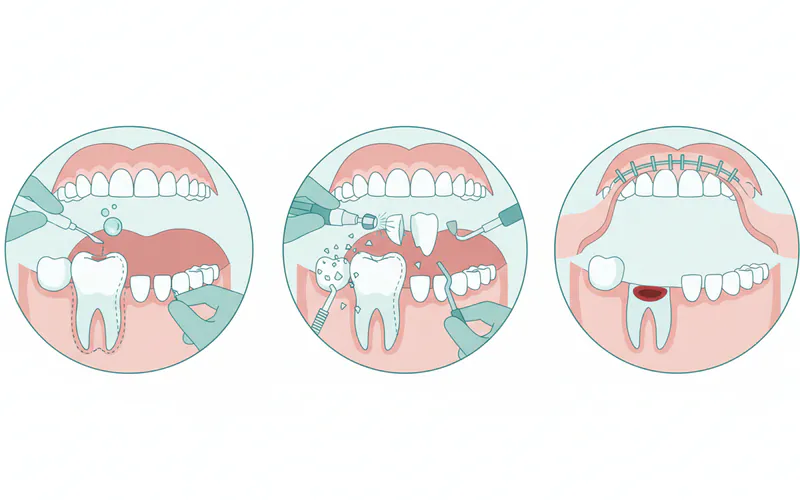
-
Pre-Procedure Consultation:
- You'll discuss the procedure with your oral surgeon or dentist.
- X-rays will be reviewed to plan the extraction carefully, noting the tooth's position and proximity to nerves or sinuses.
- You'll receive instructions on pre-operative care, including fasting guidelines if sedation is used, and what medications to avoid.
- Anesthesia options will be discussed.
-
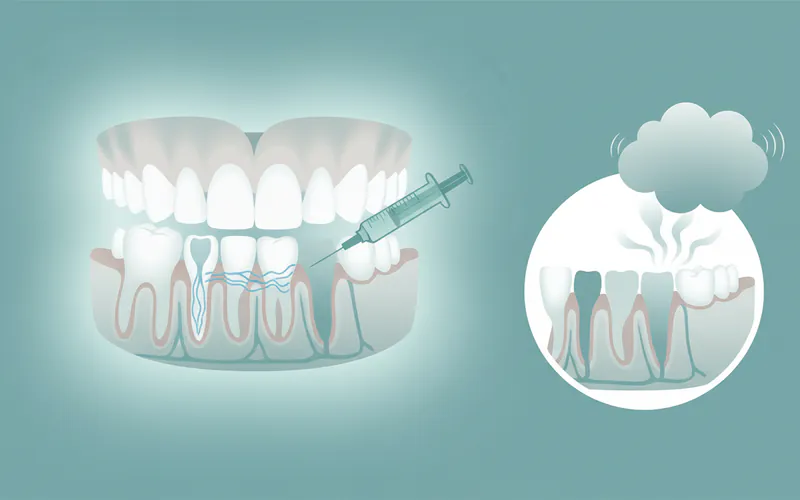
Anesthesia:
- Local Anesthesia: Numbing medication (e.g., lidocaine) is injected around the wisdom tooth to numb the area, so you feel no pain during the procedure, though you may feel pressure.
- Sedation Options:
- Nitrous Oxide (Laughing Gas): Relaxes you, but you remain awake.
- Oral Sedation: A pill taken before the appointment to make you drowsy.
- IV Sedation: Administered intravenously, making you very relaxed, often with little memory of the procedure.
- General Anesthesia: You are completely unconscious during the procedure (less common for routine wisdom tooth extraction).
- Your dental team will monitor your vital signs throughout the procedure.
-
The Extraction Procedure:
- Incision: The oral surgeon makes a small incision in the gum tissue to expose the tooth and underlying bone.
- Bone Removal (if necessary): If bone is covering the tooth, a small amount may be carefully removed using a dental drill.
- Tooth Sectioning: Often, especially with impacted teeth, the tooth is cut into two or more pieces to make removal easier and minimize trauma to the jawbone.
- Tooth Removal: Each piece of the tooth is gently loosened and extracted using specialized instruments.
- Cleaning: The socket is thoroughly cleaned to remove any debris or infection.
- Sutures: The gum flap is typically repositioned, and sutures (stitches) are used to close the wound. These may be dissolvable or require removal by your dentist in about a week.
- Gauze: A sterile gauze pad is placed over the extraction site to help control bleeding and promote clot formation.
Recovery Timeline and Aftercare
Proper aftercare is crucial for preventing complications like dry socket and ensuring a smooth recovery.
-
Immediately After (First 24 Hours):
- Bleeding: Expect some oozing or light bleeding. Bite firmly on the gauze pads for 30-60 minutes, then replace as needed. If heavy bleeding persists, contact your dentist.
- Swelling: Apply an ice pack to your cheek (20 minutes on, 20 minutes off) for the first 12-24 hours to minimize swelling.
- Pain: Take prescribed pain medication or over-the-counter pain relievers as directed.
- Diet: Stick to soft, cool foods (e.g., yogurt, applesauce, mashed potatoes) and plenty of fluids. Avoid hot liquids, alcohol, and carbonated beverages.
- Avoid Straws, Smoking, Spitting: These actions can dislodge the blood clot and lead to dry socket.
- Rest: Avoid strenuous activity. Elevate your head with pillows while resting.
-
First Few Days (Day 2-3):
- Swelling: Swelling often peaks around 2-3 days post-op and then gradually subsides. Continue ice packs if still beneficial, or switch to warm, moist compresses after 48 hours to aid in healing.
- Oral Hygiene: Gently rinse your mouth with warm salt water (1/2 teaspoon salt in 8 ounces warm water) after meals, starting 24 hours post-surgery. Brush your other teeth carefully, avoiding the surgical site.
- Diet: Gradually introduce semi-soft foods as tolerated. Continue to avoid hard, crunchy, or chewy foods.
- Pain: Pain should gradually decrease. Continue pain medication as needed.
-
First Week (Day 4-7):
- Sutures: If non-dissolvable sutures were used, they will be removed by your dentist.
- Diet: You can slowly return to a more normal diet, being cautious with hard or sharp foods.
- Activity: You can resume light activity, but avoid heavy lifting or strenuous exercise.
- Healing: The gum tissue should be closing, and discomfort should be minimal.
-
Full Recovery:
- Soft tissue healing typically takes about 1-2 weeks.
- Bone healing in the socket can take several weeks to months. It's important to continue good oral hygiene and attend follow-up appointments.
Prevention Strategies
While you can't prevent wisdom teeth from forming or impacting, you can prevent the complications associated with them:
- Regular Dental Check-ups: Consistent visits to your dentist allow for early detection of wisdom tooth issues through clinical exams and periodic X-rays. This enables proactive management before severe pain or infection develops.
- Early Assessment: For teenagers and young adults, early assessment (around ages 16-19) with panoramic X-rays is crucial. This allows your dentist or oral surgeon to predict potential problems and recommend extraction before the roots are fully developed, which can make the procedure simpler and recovery faster.
- Good Oral Hygiene: Even with partially erupted wisdom teeth, meticulous brushing and flossing can help reduce the risk of pericoronitis by removing trapped food and bacteria.
Cost Ranges in the US (with/without Insurance)
The cost of wisdom tooth extraction varies significantly based on several factors: the complexity of the impaction, the number of teeth being removed, the type of anesthesia used, the geographic location of the dental practice, and whether you have dental insurance.
- Simple Extraction (Erupted):
- Without Insurance: $75 - $250 per tooth
- With Insurance: Varies widely, but typically 20-80% coverage, leaving an out-of-pocket cost of $20 - $150 per tooth.
- Surgical Extraction (Impacted):
- Without Insurance: $200 - $750+ per tooth (some very complex cases can exceed $1,000 per tooth).
- With Insurance: Coverage typically ranges from 20-70%, with out-of-pocket costs often between $100 - $500+ per tooth.
- Anesthesia Costs: These are usually separate.
- Local Anesthesia: Often included or minimal extra charge.
- Nitrous Oxide: $50 - $150 per visit.
- Oral Sedation: $100 - $300 per visit.
- IV Sedation: $400 - $800+ per hour, can add significantly to the total cost.
- Consultation and X-rays:
- Panoramic X-ray: $80 - $200
- Consultation: $50 - $150
- Total Cost for Four Impacted Wisdom Teeth (Surgical with IV Sedation):
- Without Insurance: Can range from $1,500 to $4,000+.
- With Insurance: Depending on your plan, you might pay $500 to $2,500+ out-of-pocket.
It is always recommended to get a detailed cost estimate from your dentist or oral surgeon, including all associated fees, before proceeding with treatment. Check with your dental insurance provider to understand your specific coverage.
For Parents / Pediatric Considerations
While wisdom teeth typically emerge in late adolescence or early adulthood, parents should be aware of their development. Around ages 10-14, a panoramic X-ray taken as part of routine orthodontic or dental care can often show the presence and position of wisdom tooth buds.
Early monitoring allows dentists and orthodontists to:
- Assess Future Eruption: Predict if there will be enough room in the jaw for the wisdom teeth to erupt properly.
- Plan Ahead: If future impaction is likely, early planning can make the eventual extraction simpler, as the roots are less developed, and the surrounding bone is softer.
- Address Orthodontic Concerns: Sometimes, wisdom teeth can exert pressure that impacts orthodontic treatment outcomes or causes crowding of already straightened teeth.
Decisions about wisdom tooth removal in younger individuals (late teens) are usually made after careful consideration of their jaw growth, the degree of impaction, and potential risks versus benefits. It's a proactive approach to prevent future pain and complications rather than waiting for problems to arise.
Frequently Asked Questions
How much does wisdom tooth extraction cost, and is it covered by insurance?
The cost of wisdom tooth extraction in the US varies widely, ranging from $75 - $250 per tooth for a simple extraction to $200 - $750+ per tooth for surgical removal of impacted teeth. Anesthesia costs (e.g., IV sedation at $400 - $800+ per hour) are often additional. Most dental insurance plans do offer some coverage for wisdom tooth extractions, typically covering 20% to 80% of the cost, depending on your plan and the complexity of the procedure. It's crucial to check with your insurance provider for specific details regarding your benefits and any out-of-pocket expenses.
How painful is wisdom tooth extraction, and how long does the pain last?
During the extraction, you should feel no pain due to effective anesthesia (local, sedation, or general). After the procedure, it's normal to experience moderate to severe pain as the anesthesia wears off. This pain is usually managed with prescription pain relievers or over-the-counter medications. The most intense pain typically subsides within the first 2-3 days, but mild discomfort can persist for up to a week. Full healing, especially of the bone, can take several weeks or even months.
How long does the actual wisdom tooth extraction procedure take?
A single simple wisdom tooth extraction might take only 5-15 minutes. For a surgical extraction of an impacted tooth, the procedure typically takes 20-60 minutes per tooth, depending on its position and complexity. If all four wisdom teeth are removed in one sitting, the entire surgical procedure, including prep and recovery from sedation, might take 1 to 2 hours.
Are there alternatives to wisdom tooth extraction?
In most cases of problematic or impacted wisdom teeth, extraction is the only definitive treatment. If a wisdom tooth is fully erupted, healthy, functional, and easily cleanable without causing issues, it may be monitored with regular dental check-ups and X-rays. However, for impacted teeth causing pain, infection (pericoronitis), or damage to adjacent teeth, removal is almost always recommended to prevent further complications. There are no non-surgical alternatives for an impacted wisdom tooth that is causing problems.
What is a dry socket, and how can I prevent it?
A dry socket (alveolar osteitis) is a painful condition that can occur after a tooth extraction when the blood clot that forms in the empty socket is dislodged or dissolves prematurely, exposing the underlying bone and nerves. It typically occurs 2-5 days after extraction, causing intense throbbing pain that radiates to the ear, temple, or neck, and often an unpleasant taste or odor. To prevent it, strictly follow aftercare instructions: avoid using straws, smoking, vigorous spitting or rinsing, and consuming alcohol or hot liquids for at least 48 hours (and ideally longer). Maintaining good oral hygiene (gentle salt water rinses after 24 hours) is also important.
How long will my face be swollen after wisdom tooth removal?
Swelling is a normal part of the healing process after wisdom tooth extraction, especially for impacted teeth. It usually peaks around 2-3 days after the procedure. You can help minimize swelling by applying an ice pack to your cheek for the first 12-24 hours. After the first 48 hours, some people find warm, moist compresses helpful. While the most noticeable swelling typically subsides within 3-5 days, minor swelling can linger for up to a week.
When can I eat solid food after wisdom tooth extraction?
You should stick to soft, cool foods for the first 24-48 hours after extraction (e.g., yogurt, mashed potatoes, smoothies without a straw, soup). Gradually introduce semi-soft foods (e.g., scrambled eggs, soft pasta, finely chopped meats) as comfort allows, usually by Day 3-4. It’s crucial to avoid hard, crunchy, or chewy foods for at least a week to prevent dislodging the blood clot or irritating the healing site. Listen to your body and introduce foods slowly.
When to See a Dentist
It's essential to know when to seek professional dental care for your wisdom teeth.
Routine Care & Monitoring:
- Annual Dental Check-ups: Even if you have no symptoms, regular visits allow your dentist to monitor the development and position of your wisdom teeth through clinical examination and periodic X-rays. This is crucial for early detection of potential problems before they become acute.
- Teenage/Young Adult Years (Ages 16-25): If you are in this age range and have not had your wisdom teeth assessed, schedule an appointment for evaluation, even if you feel fine. Proactive assessment can prevent future complications.
Emergency Signs (See a Dentist Immediately):
- Severe, persistent pain at the back of your jaw that interferes with daily activities or sleep.
- Significant swelling in your cheek, jaw, or around the wisdom tooth area.
- Signs of infection, such as redness, warmth, pus discharge, bad taste in your mouth, or fever.
- Difficulty opening your mouth fully or pain when chewing.
- Uncontrolled bleeding from the extraction site (a steady flow, not just light oozing).
- Intense pain several days after extraction that radiates to your ear or neck, along with a foul odor or taste (potential dry socket).
- Numbness or tingling that persists for more than 24 hours after surgery (rare, but warrants immediate attention).
Do not hesitate to contact your dentist or oral surgeon if you experience any of these symptoms. Early intervention can prevent more serious complications and alleviate discomfort.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.