Extraction
4,823 words · 16 min read
Quick Definition
The removal of a tooth from its socket in the jawbone, performed when a tooth is too damaged to repair or for orthodontic or other clinical reasons.
An extraction, in the realm of dental health, refers to the removal of a tooth from its socket in the jawbone. This procedure is performed when a tooth is irreparably damaged by decay or trauma, or for various other clinical reasons such as orthodontic treatment, impaction, or severe periodontal disease. While often considered a last resort, a tooth extraction can be a crucial step in preserving overall oral health, preventing the spread of infection, alleviating chronic pain, and preparing the mouth for restorative treatments.
Dental extractions are a common procedure globally, with millions performed in the United States each year. For instance, approximately 5 million wisdom teeth extractions are conducted annually, representing a significant portion of all dental extractions. Beyond wisdom teeth, many other extractions are necessary due to severe tooth decay, advanced gum disease, or traumatic injuries. Understanding the process, recovery, and preventative measures associated with extractions is vital for anyone seeking to maintain optimal dental wellness. This comprehensive guide aims to be your definitive resource for all things related to tooth extraction.
Key Takeaways:
- An extraction is the surgical removal of a tooth from its socket in the jawbone.
- Reasons for extraction include severe decay, gum disease, trauma, impaction (like wisdom teeth), or orthodontic needs.
- Extractions can be simple (for visible teeth) or surgical (for impacted or broken teeth).
- Proper aftercare is critical to prevent complications such as dry socket or infection.
- Tooth replacement options, like a dental implant or bridge, are often recommended after extraction to maintain oral health and function.
- Pain is managed effectively with local anesthesia during the procedure and prescribed medication during recovery.
Detailed Explanation of Tooth Extraction
Types and Classifications of Extractions
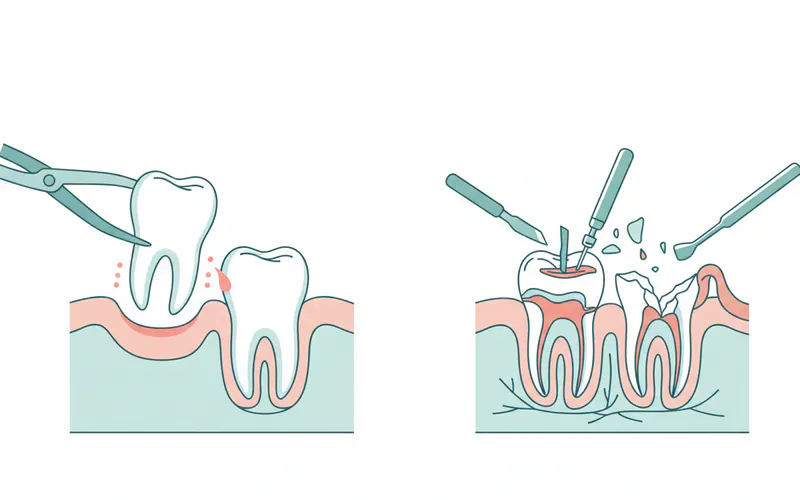
Tooth extractions are broadly categorized into two main types based on the complexity of the procedure:
-
Simple Extraction: This type of extraction is performed on teeth that are fully visible in the mouth and have a relatively intact crown. The tooth is typically loosened using an instrument called an elevator, which gently wiggles the tooth in its socket. Once sufficiently loose, the tooth is removed with forceps. Simple extractions are usually performed under local anesthesia and are generally less invasive, requiring less recovery time. This category includes extractions for severe decay, advanced gum disease, or orthodontic spacing.
-
Surgical Extraction: Surgical extractions are more complex and are necessary for teeth that are not easily accessible. This includes teeth that are impacted (unable to erupt properly, such as many wisdom teeth), broken off at or below the gum line, or have unusually curved roots. During a surgical extraction, the dentist or oral surgeon will make an incision in the gum tissue to gain access to the tooth and surrounding bone. Sometimes, a small amount of bone may need to be removed to free the tooth, or the tooth itself may be sectioned into smaller pieces for easier removal. Surgical extractions often require stitches and may involve sedation in addition to local anesthesia.
Beyond these two main types, extractions can also be classified by their reason:
- Restorative Extractions: Performed when a tooth is too damaged by decay or trauma to be saved by a filling, crown, or root canal.
- Periodontal Extractions: Necessary for teeth with severe bone loss and mobility due to advanced periodontal (gum) disease.
- Orthodontic Extractions: Done to create space in the arch for orthodontic treatment, allowing other teeth to move into proper alignment.
- Prophylactic Extractions: Primarily seen with impacted wisdom teeth or supernumerary (extra) teeth, removed to prevent future problems like infection, crowding, or damage to adjacent teeth.
Causes and Risk Factors for Extraction
Several factors can necessitate a tooth extraction. Understanding these can help in prevention:
- Severe Tooth Decay: When a cavity progresses deep into the tooth, damaging the pulp (nerve and blood vessels) and the surrounding tooth structure beyond repair with a filling or root canal, extraction becomes necessary to prevent infection from spreading.
- Advanced Periodontal (Gum) Disease: Chronic gum disease leads to the destruction of the bone and tissues supporting the teeth. As the bone loss progresses, teeth become loose and eventually fall out or require extraction due to their instability and the risk of infection.
- Trauma or Injury: Teeth that are severely fractured, cracked, or dislodged due to an accident, sports injury, or fall may be irreparable and require removal.
- Impacted Teeth: This occurs when a tooth, most commonly a wisdom tooth (third molar), is blocked from erupting fully into the mouth by gum tissue, bone, or another tooth. Impacted teeth can cause pain, infection, cysts, or damage to neighboring teeth.
- Orthodontic Treatment: In some cases, to correct overcrowding or create space for teeth to move into proper alignment during braces or clear aligner treatment, the removal of one or more permanent teeth may be recommended.
- Overcrowding: Even without orthodontic treatment, if teeth are severely overcrowded, extraction may be necessary to alleviate pressure and improve oral hygiene.
- Infection: If an infection (dental abscess) originating from a tooth cannot be resolved with root canal treatment or antibiotics, the tooth may need to be extracted to eliminate the source of infection.
- Compromised Immune System: Patients with weakened immune systems (e.g., those undergoing chemotherapy, organ transplant recipients) may have teeth extracted that pose a high risk of future infection, even if they could otherwise be saved.
- Cysts or Tumors: The presence of benign or malignant growths in the jawbone near a tooth can sometimes necessitate its removal.
Signs and Symptoms to Watch For
Recognizing the signs and symptoms that might indicate the need for an extraction is crucial for timely dental intervention:
- Severe, Persistent Toothache: A deep, throbbing pain that doesn't subside, especially if it worsens with biting or temperature changes, could indicate severe decay or infection.
- Swelling in the Gum or Jaw: Localized swelling around a tooth, or general facial swelling, often points to an infection or abscess.
- Redness or Tenderness Around a Tooth: Inflamed gums that are painful to touch can be a sign of infection or periodontal disease.
- Pus Discharge: Visible pus draining from the gum line near a tooth is a definitive sign of infection.
- Difficulty Opening Mouth or Chewing: This can be a symptom of a severe infection, an impacted tooth (wisdom tooth), or temporomandibular joint (TMJ) issues exacerbated by a problematic tooth.
- Loose Tooth: A tooth that feels significantly loose, particularly in an adult, may indicate severe bone loss from gum disease or trauma.
- Bad Breath or Unpleasant Taste: Persistent bad breath or a foul taste in the mouth, despite good oral hygiene, can be a symptom of an infected tooth or advanced gum disease.
- Headaches or Jaw Pain: Particularly common with impacted wisdom teeth, which can exert pressure on surrounding structures.
Diagnosis Process – What Your Dentist Does
When you present with symptoms that might require an extraction, your dentist will follow a systematic diagnostic process:
- Comprehensive Dental Examination: The dentist will visually inspect your mouth, teeth, and gums, looking for signs of decay, inflammation, swelling, and tooth mobility. They will use instruments to probe for cavities and assess gum health.
- Medical History Review: You will be asked about your general health, medications you are taking (especially blood thinners, bisphosphonates, or immunosuppressants), allergies, and any previous dental treatments. This information is vital for planning the extraction and minimizing risks.
- Symptom Assessment: The dentist will ask about your specific symptoms, including the nature, duration, and intensity of pain, and any other related discomfort.
- X-rays: This is a critical diagnostic tool.
- Periapical X-rays: Provide detailed images of one or two teeth, showing the entire tooth from crown to root tip, and the surrounding bone.
- Panoramic X-rays: Offer a broad view of the entire mouth, including all teeth in both jaws, the jawbones, sinuses, and nerves. This is particularly useful for assessing impacted wisdom teeth and their proximity to vital structures.
- 3D Cone Beam Computed Tomography (CBCT) Scans: In complex cases, a 3D scan may be taken to provide highly detailed images of the tooth, bone, and surrounding anatomical structures, which is invaluable for planning surgical extractions.
- Clinical Tests: The dentist may perform sensitivity tests (to hot/cold) or percussion tests (gently tapping the tooth) to assess the vitality and health of the tooth.
Based on this comprehensive assessment, your dentist will determine if an extraction is necessary and discuss alternative treatment options if available, as well as the risks and benefits of each.
Treatment Options (Alternatives to Extraction)
Before recommending an extraction, your dentist will always consider alternatives to save the tooth, if possible. Extraction is typically a last resort.
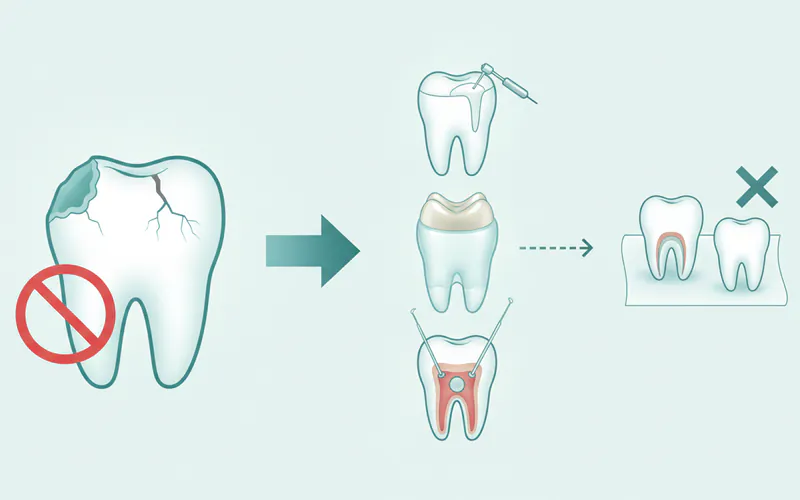
Alternatives to Extraction:
- Fillings: For minor to moderate cavities, a filling can restore the tooth structure and prevent further decay.
- Crowns: If a tooth has significant decay or is fractured but the root structure is sound, a dental crown can cap and protect the remaining tooth, restoring its strength and appearance.
- Root Canal Therapy: For teeth with infected or inflamed pulp due to deep decay or trauma, a root canal can save the tooth by removing the infected pulp, cleaning, and sealing the root canals. After a root canal, a crown is often placed to protect the tooth.
- Periodontal Treatment: For early to moderate gum disease, deep cleaning (scaling and root planing) and other periodontal therapies can help control the infection and save teeth by stabilizing the supporting structures.
- Orthodontic Treatment: For crowded teeth, orthodontics can sometimes create space without extractions, although extractions may still be necessary in severe cases.
Pros and Cons of Extraction (when necessary):
| Feature | Pros | Cons |
|---|---|---|
| Pain | Eliminates severe tooth pain and discomfort | Post-operative pain and swelling (manageable) |
| Infection | Removes source of infection, prevents spread | Risk of post-operative infection if aftercare is poor |
| Oral Health | Prevents damage to adjacent teeth, improves overall oral health | Loss of natural tooth, can affect bite and speech |
| Cost | Often less expensive than complex restorative procedures to save a tooth | Requires subsequent tooth replacement (e.g., implant), which adds cost |
| Bone | Can allow for bone grafting if needed for future implant | Can lead to bone loss in the jaw over time if not replaced |
Step-by-Step: What to Expect During Treatment
The extraction procedure, whether simple or surgical, follows a general sequence:
-
Anesthesia and Sedation:
- Local Anesthesia: The most common form, numbing the tooth and surrounding gum tissue so you don't feel pain, only pressure.
- Sedation Options: For anxious patients, complex extractions, or multiple tooth removals, various sedation methods may be offered:
- Nitrous Oxide (Laughing Gas): Inhaled gas that helps you relax.
- Oral Sedation: Pills taken before the appointment to induce drowsiness.
- Intravenous (IV) Sedation: Administered through a vein, leading to a deeper state of relaxation or sleep ("twilight sleep"). Your dentist or oral surgeon will discuss the best option for your comfort and the complexity of the procedure.
-
Loosening the Tooth (Simple Extraction):
- The dentist uses an instrument called an elevator, which is gently placed between the tooth and the gum to loosen the tooth from its socket. This expands the socket and severs the periodontal ligament fibers that hold the tooth in place. You will feel pressure, but no sharp pain.
-
Removing the Tooth (Simple Extraction):
- Once the tooth is sufficiently loose, dental forceps are used to grasp the tooth and gently rock it back and forth until it can be lifted from the socket.
-
Surgical Steps (Surgical Extraction):
- Incision: The surgeon makes a small incision in the gum tissue to expose the tooth and surrounding bone.
- Bone Removal: If bone is covering the tooth or preventing its removal (common with impacted wisdom teeth), a small amount of bone may be carefully removed using a dental drill.
- Tooth Sectioning: In some cases, especially if the tooth has multiple roots or is severely impacted, the tooth may be cut into smaller sections to facilitate easier removal.
- Tooth Removal: Once the tooth or its sections are free, they are carefully removed.
-
Cleaning the Socket:
- After the tooth is removed, the dentist or surgeon will clean the socket thoroughly, removing any infected tissue or bone fragments.
- A bone graft material may be placed in the socket at this stage, especially if you plan to get a dental implant later, to preserve bone volume.
-
Stitches (If Needed):
- If an incision was made or if there's significant bleeding, the gum tissue may be closed with stitches. These can be dissolvable or may need to be removed by the dentist after a few days.
-
Gauze Pack:
- A sterile gauze pad is placed over the extraction site, and you'll be asked to bite down firmly to apply pressure. This helps to form a blood clot, which is essential for proper healing and preventing dry socket.
Recovery Timeline and Aftercare
Proper aftercare is crucial for a smooth recovery and to prevent complications.
Immediate Aftercare (First 24 Hours):
- Bleeding Control: Bite firmly on the gauze pad for 30-60 minutes, changing it if it becomes saturated. Slight oozing for up to 24 hours is normal. If bleeding is heavy or persistent, contact your dentist.
- Pain Management: Take prescribed pain medication or over-the-counter pain relievers (like ibuprofen or acetaminophen) as directed before the anesthesia wears off.
- Swelling Reduction: Apply an ice pack to the outside of your cheek for 20 minutes on, 20 minutes off for the first 24 hours to minimize swelling.
- Rest: Avoid strenuous activity for at least 24-48 hours. Keep your head elevated when lying down.
- Diet: Stick to soft foods (yogurt, mashed potatoes, soup, smoothies) and liquids. Avoid hot, spicy, crunchy, or chewy foods.
- Avoid Rinsing/Spitting: Do NOT rinse your mouth vigorously, spit forcefully, or use a straw for the first 24-48 hours. This can dislodge the blood clot and lead to dry socket.
- Avoid Smoking and Alcohol: Smoking severely impairs healing and dramatically increases the risk of dry socket. Alcohol can interfere with medication and healing. Avoid both for at least 72 hours, preferably longer.
- Oral Hygiene: Gently brush your other teeth, but avoid the extraction site. Do not use mouthwash containing alcohol.
Ongoing Aftercare (Days 2-7):
- Rinsing: After 24 hours, you can gently rinse your mouth with warm salt water (1/2 teaspoon salt in 8 ounces warm water) several times a day, especially after meals, to keep the area clean.
- Diet: Gradually reintroduce solid foods as comfort allows.
- Brushing: Carefully brush around the extraction site.
- Physical Activity: Gradually return to normal activities, but avoid heavy lifting or strenuous exercise for about a week.
Potential Complications and What to Do:
- Dry Socket (Alveolar Osteitis): This occurs when the blood clot dislodges or dissolves prematurely, exposing the underlying bone and nerves. It's a painful condition that typically develops 3-5 days after extraction. Symptoms include severe, throbbing pain that radiates to the ear or neck, and a foul odor or taste. If you suspect dry socket, contact your dentist immediately. They will clean the socket and place a medicated dressing to relieve pain and promote healing.
- Infection: While antibiotics may be prescribed pre- or post-extraction, infection can still occur. Signs include increased pain, swelling, fever, pus, or prolonged bleeding. Contact your dentist if you notice these symptoms.
- Prolonged Bleeding: If bleeding is heavy and persistent after 24 hours, bite on a clean, moist tea bag (tannins help with clotting) or a fresh gauze pad and contact your dentist.
- Nerve Damage: A rare complication, particularly with lower wisdom tooth extractions, where the inferior alveolar nerve (supplying sensation to the lip and chin) or the lingual nerve (supplying sensation to the tongue) can be bruised or damaged. This can cause temporary or, in very rare cases, permanent numbness.
- Sinus Perforation: For upper molars, especially if the roots are close to the maxillary sinus, a small opening can occur between the mouth and the sinus. Your dentist will advise you on how to manage this (e.g., avoiding blowing your nose, sneezing with your mouth open) and may perform a small repair.
Prevention Strategies
While not all extractions can be prevented (e.g., some impacted wisdom teeth), many are avoidable through diligent oral hygiene and regular dental care:
- Maintain Excellent Oral Hygiene: Brush your teeth twice a day for two minutes with fluoride toothpaste and floss daily. This removes plaque and food particles, preventing cavities and gum disease.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and examinations. Early detection of cavities, gum disease, or other issues allows for less invasive treatment.
- Prompt Treatment of Dental Issues: Don't delay treatment for cavities, chipped teeth, or gum inflammation. Addressing these issues early can prevent them from escalating to a point where extraction is the only option.
- Protect Your Teeth: Wear a mouthguard during sports activities to prevent traumatic injuries to your teeth. Avoid chewing on hard objects like ice, pens, or popcorn kernels that can crack teeth.
- Healthy Diet: Limit sugary drinks and foods, which contribute to tooth decay. Choose a balanced diet rich in fruits, vegetables, and whole grains.
- Avoid Tobacco Products: Smoking and chewing tobacco are major risk factors for severe gum disease, oral cancer, and impaired healing.
- Address Impacted Wisdom Teeth: If your dentist identifies impacted wisdom teeth that pose a risk of pain, infection, or damage to adjacent teeth, discuss prophylactic extraction before problems arise.
Cost Ranges in the US (with/without insurance)
The cost of a tooth extraction in the United States can vary significantly based on several factors, including the type of extraction (simple vs. surgical), the location of the tooth, the complexity of the case, the dentist's fees, geographical location, and whether sedation is used.
Here are general cost ranges:
-
Simple Extraction (Non-Surgical):
- Without Insurance: $75 - $300 per tooth
- With Insurance: $50 - $200 per tooth (after deductible and co-pay, depending on plan coverage) This typically covers visible teeth that can be removed with local anesthesia and basic instruments.
-
Surgical Extraction (Non-Impacted):
- Without Insurance: $150 - $650 per tooth
- With Insurance: $100 - $400 per tooth This applies to teeth that might be broken below the gum line or require a small incision but are not impacted within the bone.
-
Surgical Extraction (Impacted Tooth, e.g., Wisdom Tooth):
- Without Insurance: $250 - $800 per tooth for partially bony impacted teeth.
- Without Insurance: $500 - $1,100 per tooth for fully bony impacted teeth (the most complex).
- With Insurance: $200 - $700 per tooth (for partially bony).
- With Insurance: $400 - $1,000 per tooth (for fully bony). Wisdom tooth extractions often fall into this category due to impaction and the need for surgical techniques. The cost increases significantly if all four wisdom teeth are removed in a single procedure under sedation.
Additional Costs to Consider:
- Sedation:
- Nitrous Oxide: $50 - $150
- Oral Sedation: $100 - $300
- IV Sedation: $250 - $750+ per hour (can add substantial cost, especially for longer procedures)
- X-rays: $25 - $200 (Panoramic or 3D CBCT scans are more expensive)
- Consultation: $50 - $150 (may be included in the extraction fee if done on the same day)
- Post-Operative Medications: Prescriptions for pain or antibiotics typically cost $10 - $50.
- Bone Grafting: If bone preservation is desired for a future implant, a socket preservation graft can add $300 - $800.
It's important to get a detailed cost estimate from your dentist or oral surgeon, including all potential charges, before proceeding with the extraction. Dental insurance plans vary widely, so check your specific coverage for extractions and sedation.
Comparison Table: Simple vs. Surgical Extraction
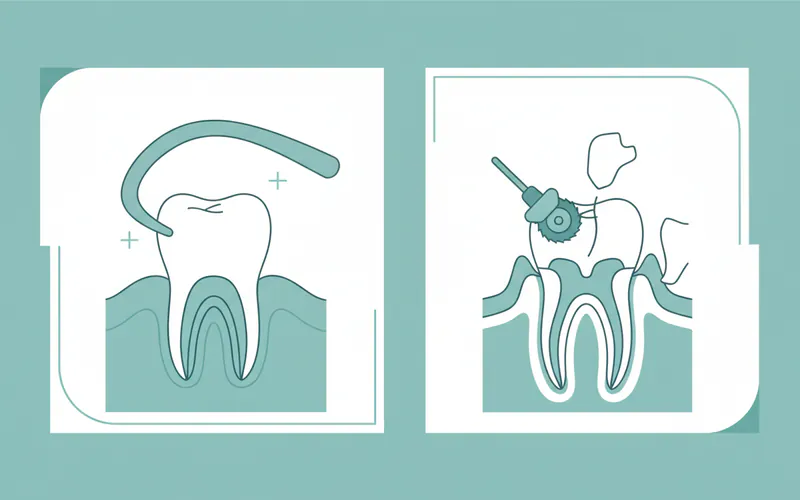
This table highlights the key differences between the two main types of tooth extraction:
| Feature | Simple Extraction | Surgical Extraction |
|---|---|---|
| Tooth Status | Visible, fully erupted, stable | Not visible, impacted, fractured below gum line |
| Procedure | Loosening with elevator, removal with forceps | Incision in gum, bone removal, tooth sectioning (often) |
| Anesthesia | Local anesthesia (e.g., lidocaine) | Local anesthesia, often with sedation (oral, IV, nitrous) |
| Duration | Typically 5-30 minutes per tooth | Typically 20-60 minutes per tooth |
| Recovery | Shorter, less discomfort, usually no stitches | Longer, more swelling/discomfort, stitches often required |
| Cost (US) | $75 - $300 (per tooth, without insurance) | $250 - $1,100+ (per tooth, without insurance) |
| Complexity | Lower | Higher, may require an oral surgeon |
| Risk of Dry Socket | Present, but generally lower | Present, potentially slightly higher due to complexity and trauma to tissue |
| Common Examples | Decayed molars, loose front teeth due to gum disease | Impacted wisdom teeth, fractured teeth below gum line |
For Parents / Pediatric Considerations
Tooth extractions are not just for adults; children may also require them for various reasons, with some specific considerations:
- Primary (Baby) Tooth Extraction:
- Severe Decay: If a baby tooth is too decayed to be filled or repaired, extraction prevents infection from spreading to permanent teeth and the developing jawbone.
- Trauma: A severely fractured or dislodged primary tooth that cannot be re-implanted may need removal.
- Over-Retained Teeth: Sometimes a baby tooth doesn't fall out on its own, blocking the eruption path of the underlying permanent tooth. Extraction is then necessary to allow the permanent tooth to come in correctly.
- Orthodontic Needs: In some cases, a pediatric dentist or orthodontist might recommend extracting certain primary teeth as part of "serial extractions" to guide the eruption of permanent teeth and manage crowding.
- Space Maintainers: If a primary tooth is extracted prematurely (before the permanent tooth is ready to erupt), a space maintainer (a small device custom-made for the child's mouth) may be placed. This prevents adjacent teeth from drifting into the empty space, ensuring there's enough room for the permanent tooth to erupt properly.
- Child-Friendly Approach: Pediatric dentists specialize in making dental visits as comfortable as possible for children. They use child-friendly language, distraction techniques, and appropriate local anesthesia and sometimes mild sedation (like nitrous oxide) to manage anxiety and pain.
- Developing Permanent Teeth: Care is taken during primary tooth extractions to avoid damaging the underlying developing permanent tooth. X-rays are crucial for assessing the position of the permanent tooth.
- Oral Hygiene Education: Emphasizing good oral hygiene habits from a young age is the best way to prevent the need for extractions.
Frequently Asked Questions
How much does a tooth extraction cost?
The cost of a tooth extraction in the US varies widely depending on its complexity. A simple extraction can range from $75 to $300 without insurance. A surgical extraction for an impacted tooth, such as a wisdom tooth, can cost significantly more, typically between $250 and $1,100 per tooth without insurance. Additional costs may include X-rays, consultation fees, and sedation. Dental insurance often covers a portion of the cost, but you'll likely have deductibles and co-pays. Always get a detailed estimate from your dentist.
How painful is a tooth extraction?
During the extraction, you should not feel any sharp pain thanks to local anesthesia, which completely numbs the area. You will likely feel pressure and some movement. Post-extraction, it's normal to experience discomfort, swelling, and mild to moderate pain once the anesthesia wears off. This pain is usually manageable with over-the-counter pain relievers or prescribed medication. The peak pain typically occurs within the first 24-48 hours and gradually subsides over the next few days. Following aftercare instructions diligently helps minimize pain and promotes faster healing.
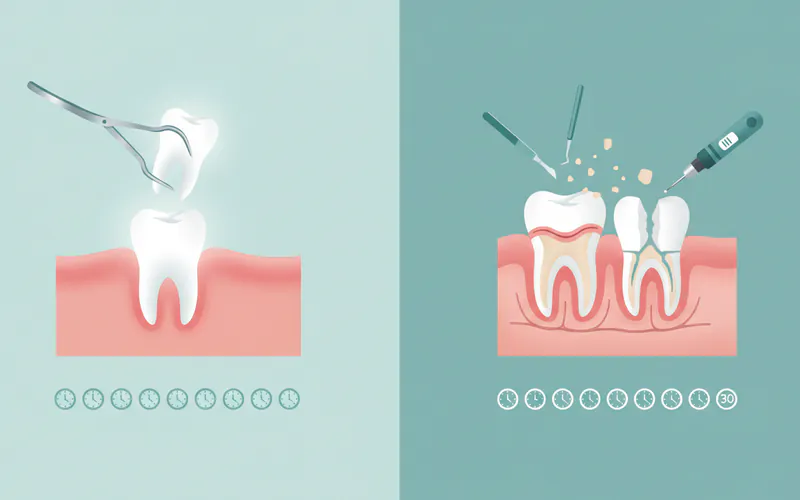
How long does a tooth extraction take?
A simple extraction can be quite quick, often taking only 5 to 30 minutes. A surgical extraction, which involves incisions, bone removal, or tooth sectioning, will take longer, typically between 20 and 60 minutes per tooth, especially for impacted wisdom teeth. The overall appointment time will also include preparation, anesthesia administration, and post-operative instructions.
What are the alternatives to extraction?
Before recommending extraction, your dentist will always consider options to save the tooth. Alternatives include fillings for cavities, dental crowns for severely damaged but savable teeth, and root canal therapy for infected tooth pulp. For teeth affected by gum disease, periodontal treatment may be an option. Extraction is typically a last resort when a tooth is beyond repair or poses a risk to overall oral health.
Does dental insurance cover extractions?
Yes, most dental insurance plans cover tooth extractions, as they are considered a medically necessary procedure. However, the extent of coverage varies significantly by plan. Many plans cover 50% to 80% of the cost after you meet your deductible, with limitations on annual maximums. Some plans may have waiting periods or specific clauses for complex surgical extractions, especially for wisdom teeth. It's crucial to contact your insurance provider directly to understand your specific benefits and coverage before the procedure.
What is a dry socket, and how can I prevent it?
A dry socket, medically known as alveolar osteitis, is a painful condition that occurs when the blood clot that should form in the extraction site either dislodges or dissolves prematurely, exposing the underlying bone and nerves. It typically develops 3-5 days after the extraction. To prevent dry socket, follow aftercare instructions meticulously: avoid smoking and alcohol, do not use straws, avoid vigorous rinsing or spitting for at least 24-48 hours, and maintain a soft diet. If you suspect dry socket (severe pain, bad taste/odor), contact your dentist immediately.
What can I eat after a tooth extraction?
For the first 24-48 hours, stick to soft, cool, or lukewarm foods and liquids. Examples include yogurt, applesauce, mashed potatoes, soups (not too hot), smoothies (without a straw), scrambled eggs, and pudding. Gradually reintroduce more solid foods as your comfort allows, avoiding anything hard, crunchy, chewy, spicy, or hot that could irritate the extraction site or dislodge the blood clot. Chew on the opposite side of your mouth from the extraction if possible.
When can I exercise after an extraction?
It's generally recommended to avoid strenuous physical activity for at least 24-48 hours after an extraction. Increased blood pressure from exercise can dislodge the blood clot and lead to bleeding or dry socket. After the initial recovery period, you can gradually resume light activities, listening to your body. Avoid heavy lifting or intense workouts for about a week, or until your dentist advises it's safe.
When to See a Dentist
Knowing when to seek dental care is crucial, especially regarding tooth pain or potential extraction needs.
Emergency Situations (Seek immediate dental or medical attention):
- Uncontrolled Bleeding: If bleeding from the extraction site is heavy and persistent (not just light oozing) after several hours of applying pressure with gauze.
- Spreading Swelling: If swelling in your face or jaw rapidly increases, especially if it makes it difficult to breathe or swallow, this could indicate a serious infection or allergic reaction.
- Fever: A high fever accompanying dental pain or post-extraction could signal a significant infection.
- Severe, Unbearable Pain: If pain is extreme and not managed by prescribed medication, or if it suddenly worsens several days after extraction (a sign of dry socket).
Routine Care (Schedule an appointment soon):
- Persistent Toothache: Any toothache that doesn't go away or worsens, even if not excruciating.
- Visible Decay or Cavities: If you notice a hole in your tooth or dark spots.
- Loose Tooth: An adult tooth that feels noticeably loose.
- Swelling or Redness: Any unexplained swelling, tenderness, or redness in your gums.
- Jaw Pain or Difficulty Opening Mouth: Especially if associated with the back of your jaw, which could indicate an impacted wisdom tooth.
- Sensitivity to Hot or Cold: Prolonged sensitivity could be a sign of deep decay or nerve inflammation.
- Broken or Chipped Tooth: Even if not painful, a broken tooth can expose the pulp to bacteria.
Don't wait until pain becomes unbearable. Early diagnosis and treatment can often prevent the need for an extraction and help you maintain your natural teeth for a lifetime. Regular dental check-ups are your best defense against serious dental problems.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.