Complete Guide to Endodontics (Root Canal): Everything You Need to Know
Key Takeaways
- Imagine experiencing a toothache so severe it disrupts your sleep, makes eating a chore, and casts a shadow over your entire day. This agonizing pain is a common indicator of an infected or inflamed dental pulp – the soft tissue inside your tooth containing nerves, blood vessels, and connective tiss
Complete Guide to Endodontics (Root Canal): Everything You Need to Know
Imagine experiencing a toothache-conditions-diseases-everything-you-need-to-know "Complete Guide to Dental Conditions & Diseases: Everything You Need to Know") so severe it disrupts your sleep, makes eating a chore, and casts a shadow over your entire day. This agonizing pain is a common indicator of an infected or inflamed dental pulp – the soft tissue inside your tooth containing nerves, blood vessels, and connective tissue. When this vital pulp becomes compromised, a root canal is often the most effective solution to save your natural tooth, alleviate pain, and prevent further infection. In the United States, millions of root canal procedures are performed successfully each year, demonstrating its crucial role in maintaining oral health.
This comprehensive guide from SmilePedia.net will demystify endodontics and the root canal procedure, providing you with everything you need to know. We’ll delve into what causes the need for this treatment, the step-by-step process, what to expect regarding recovery, potential costs, and crucial prevention strategies. Our goal is to empower you with knowledge, reduce anxiety, and help you understand why a root canal is a tooth-saving procedure, not a tooth-losing one.
Key Takeaways:
- What it is: A root canal (endodontic treatment) is a procedure to remove infected or inflamed pulp from inside a tooth, clean and disinfect the internal canals, and then fill and seal them.
- Primary Goal: To save a damaged tooth from extraction, preserve its function, and eliminate pain.
- Procedure Duration: Typically 1-2 hours per tooth for a conventional root canal, often completed in one or two appointments.
- Pain Level: Modern root canal treatments are generally no more uncomfortable than a routine filling, thanks to advanced anesthetics and techniques. The pain relief after treatment is usually significant.
- Cost (US Averages): Ranges from $700 to $1,500 for a front tooth, $800 to $1,800 for a premolar, and $1,000 to $2,000+ for a molar, depending on complexity, location, and the dental professional (general dentist vs. endodontist). These figures are before insurance.
- Success Rate: Over 95% for initial root canal treatments when properly restored with a crown or filling afterward.
- Recovery: Most patients resume normal activities within 24-48 hours, with mild soreness managed by over-the-counter pain relievers. A permanent restoration (e.g., a dental crown) is crucial for long-term success.
What is Endodontics and a Root Canal? An Overview
Endodontics is a specialized branch of dentistry focused on the study and treatment of the dental pulp and the tissues surrounding the roots of a tooth. The term "endodontics" literally means "inside the tooth" (from Greek "endo" meaning inside and "odont" meaning tooth). An endodontist is a dental specialist who has completed at least two to three additional years of post-doctoral training in this field beyond dental school, focusing on diagnosing tooth pain and performing root canal treatment and other procedures related to the internal structures of the tooth.
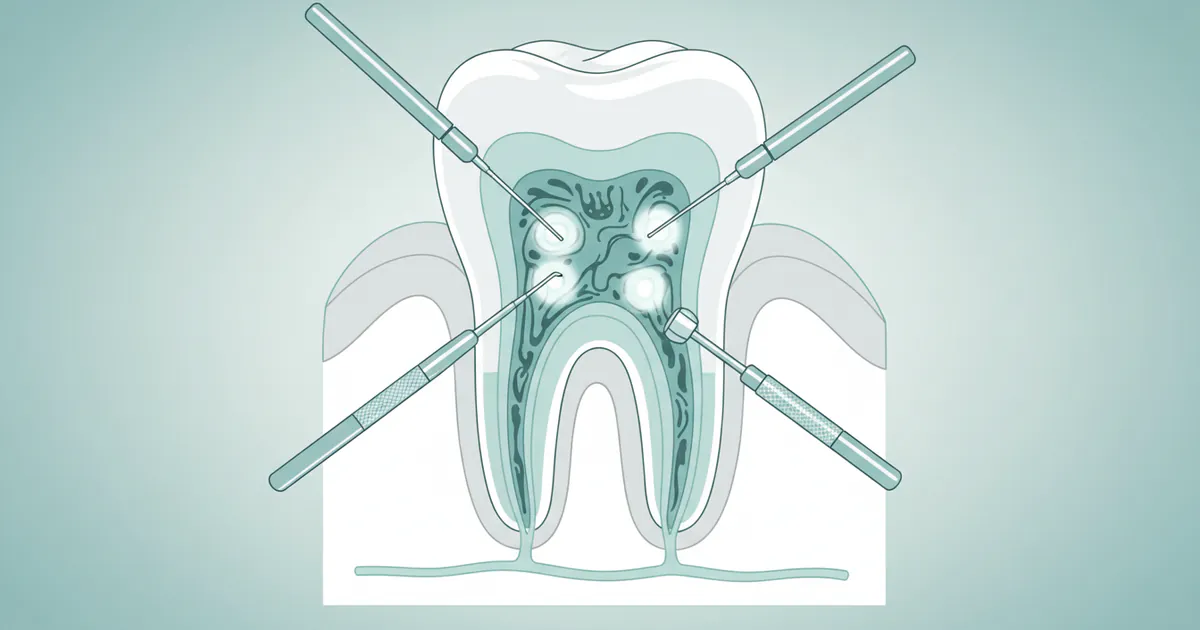
A root canal treatment, also formally known as endodontic treatment, is a common procedure performed by both general dentists and endodontists to remove infected or inflamed tissue from inside a tooth. This "pulp" tissue, located in the center of the tooth, contains nerves, blood vessels, and connective tissue. When the pulp becomes diseased or injured, it can cause severe pain and lead to abscesses if left untreated. The root canal procedure cleans out this diseased pulp, disinfects the internal chamber and canals, and then fills and seals them to prevent further infection. This process effectively saves the tooth, allowing it to remain in your mouth and function normally.
The Pulp and Its Importance
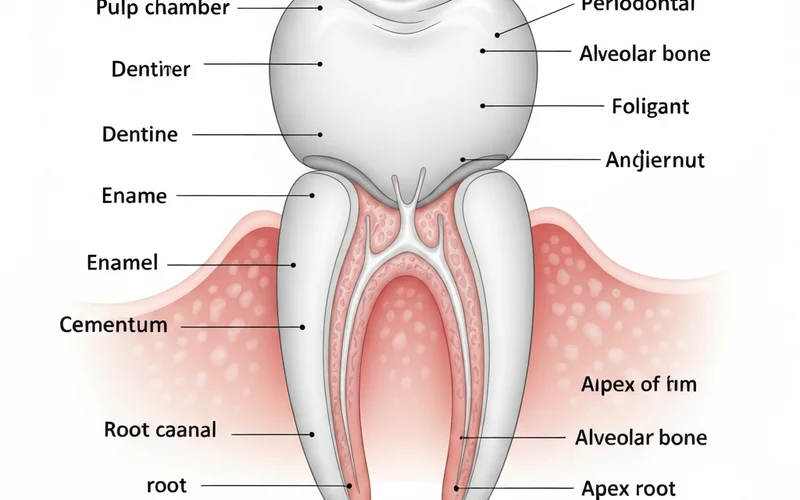
To understand a root canal, it's essential to understand the tooth's anatomy. Each tooth consists of three main layers:
- Enamel: The hard, outer protective layer.
- Dentin: The layer beneath the enamel, softer than enamel but harder than bone.
- Pulp: The innermost chamber and root canals, housing the nerves, blood vessels, and connective tissue.
The pulp plays a crucial role during tooth development, providing nourishment and sensation. Once a tooth is fully developed, it can survive without the pulp, as it continues to be nourished by the surrounding tissues. Therefore, removing the infected pulp during a root canal treatment does not compromise the tooth's structural integrity or its ability to function. It simply removes the source of infection and pain.
Why Might You Need a Root Canal? Common Causes
The need for a root canal arises when the dental pulp becomes inflamed, irritated, or infected. This pulp damage can stem from various sources, primarily:
Deep Decay Reaching the Pulp
This is the most frequent reason. When tooth decay (cavities) progresses untreated, bacteria penetrate the enamel and dentin, eventually reaching the pulp chamber. Once bacteria invade the pulp, they cause inflammation (pulpitis) and infection, leading to severe pain and potentially an abscess.
Dental Trauma
A sudden impact or injury to a tooth can damage the pulp, even if there's no visible crack or chip. The trauma can sever the blood supply to the pulp, causing it to die and become necrotic (dead tissue). This necrotic pulp is highly susceptible to bacterial infection. Common causes include sports injuries, falls, or car accidents.
Cracked or Chipped Teeth
Fractures in a tooth, especially those that extend deep into the dentin or reach the pulp, create pathways for bacteria to enter and infect the pulp. Even hairline cracks that are difficult to see can cause significant problems. Chewing on hard foods, teeth grinding-teeth-grinding-everything-you-need-to-know "Complete Guide to Bruxism & Teeth Grinding: Everything You Need to Know") (bruxism), or large old fillings can all lead to cracks.
Repeated Dental Procedures on the Same Tooth
While dental restorations are designed to protect teeth, repeated procedures on the same tooth (e.g., multiple fillings, crown placements) can sometimes irritate the pulp over time. Each procedure, though carefully performed, can cause minor trauma to the delicate pulp tissue, eventually leading to inflammation or necrosis, necessitating a root canal.
Other Less Common Causes
- Severe Gum Disease: In advanced stages, gum disease can affect the bone supporting the tooth, potentially leading to infection that spreads to the root tip and pulp.
- Resorption: A rare condition where the body's own cells begin to "eat away" at the tooth structure, internally or externally, sometimes affecting the pulp.
Understanding these causes highlights the importance of regular dental check-ups and prompt treatment of dental issues to prevent the need for a root canal.
Recognizing the Signs: Symptoms of Needing a Root Canal
Knowing the symptoms that indicate a compromised dental pulp is crucial for seeking timely treatment. While sometimes the infection can be asymptomatic, the following are the most common warning signs:
Persistent Pain
This is the hallmark symptom. The pain can vary in intensity from mild to excruciating and might be constant or intermittent. It often worsens when chewing or applying pressure to the tooth, indicating inflammation of the ligament surrounding the root. The pain may even radiate to other parts of the face, jaw, or head.
Sensitivity to Hot and Cold
While temporary sensitivity to temperature changes can indicate minor issues, sensitivity that lingers for an extended period (several seconds or minutes) after the stimulus is removed is a strong sign of irreversible pulp inflammation or infection.
Swelling or Tenderness
Inflammation in the pulp can lead to swelling in the surrounding gum tissue, which may manifest as a tender, swollen area near the affected tooth. This swelling can sometimes spread to the face, neck, or lymph nodes, indicating a more severe infection or abscess.
Discoloration of the Tooth
An infected or dying pulp can cause the tooth to darken or take on a grayish-black hue. This discoloration occurs as the internal blood vessels break down and blood products seep into the dentin.
A Pimple-like Bump on the Gums (Fistula)
This small bump, often called a sinus tract or fistula, appears on the gum near the affected tooth. It's a sign that the infection has created a pathway for pus to drain from the abscess to the surface. While this might temporarily relieve pressure and pain, it signifies a serious ongoing infection that requires immediate attention.
Pain When Touching the Tooth or Chewing
If you experience sharp pain when you bite down or touch the tooth, it suggests inflammation in the periodontal ligament surrounding the tooth's root, often due to an infection that has spread from the pulp.
If you experience any of these symptoms, it's vital to see a dentist immediately. Delaying treatment can lead to more severe infections, bone loss, and eventually, the loss of the tooth itself.
Understanding Endodontic Specialists: The Endodontist
While many general dentists are proficient in performing routine root canal treatments, an endodontist specializes exclusively in diagnosing and treating problems related to the dental pulp and roots. They complete an additional two to three years of advanced education beyond dental school, focusing on complex cases, advanced techniques, and pain management specific to endodontics.
When might an endodontist be recommended?
- Complex Anatomy: Teeth with multiple or unusually curved roots, narrow canals, or calcified canals are more challenging and benefit from an endodontist's expertise and specialized equipment (e.g., operating microscopes).
- Retreatment: If a tooth has already had a root canal that failed, an endodontist is better equipped to perform an endodontic retreatment, which involves removing old filling material and re-cleaning the canals.
- Traumatic Injuries: Endodontists are experts in managing dental injuries, including fractured roots or displaced teeth.
- Persistent Pain: If a patient experiences ongoing pain that is difficult to diagnose, an endodontist's specialized diagnostic skills can be invaluable.
- Surgical Endodontics: Procedures like apicoectomies, which involve surgical removal of the root tip, are typically performed by endodontists.
An endodontist's office is often equipped with state-of-the-art technology, such as dental operating microscopes for enhanced visualization, digital radiography for precise imaging, and specialized instruments for cleaning and shaping canals. This advanced toolkit allows for higher precision and increased success rates, especially in challenging situations.
!Diagram illustrating the internal structure of a tooth, showing pulp, dentin, enamel, cementum, periodontal ligament, alveolar bone, and root canals, clearly labeling each part.
Types of Root Canal Procedures
While the conventional root canal treatment is the most common, there are several variations depending on the tooth's condition and history.
Conventional Root Canal Treatment (RCT)
This is the standard procedure performed when the pulp is irreversibly inflamed or infected. As described earlier, it involves accessing the pulp chamber, removing the diseased pulp, cleaning and shaping the root canals, and then filling and sealing them. This is typically what people refer to when they say "getting a root canal."
Endodontic Retreatment
Sometimes, a tooth that has undergone a root canal can become reinfected or fail to heal. This can happen due to new decay, an inadequate initial seal, a missed canal, or a crack in the tooth or restoration. Endodontic retreatment involves reopening the tooth, removing the previous filling material, thoroughly cleaning and reshaping the canals again, and then refilling and sealing them. This procedure is often more complex than the initial root canal and usually performed by an endodontist.
Apicoectomy (Endodontic Surgery)
If an infection or inflammation persists at the tip of the tooth's root after a conventional root canal or retreatment, an apicoectomy may be necessary. This surgical procedure involves making an incision in the gum tissue to expose the bone and the infected root tip. The endodontist then removes the infected tissue and the very tip of the root, and a small filling is placed to seal the end of the root canal. This is typically a last resort to save a tooth that has not responded to non-surgical treatment.
Pulpotomy and Pulpectomy (Pediatric Considerations)
These procedures are primarily performed on children's primary (baby) teeth, but sometimes on immature permanent teeth.
- Pulpotomy: Only the infected or inflamed pulp in the crown (the visible part of the tooth) is removed, while the healthy pulp in the root canals is left intact. This is often done when decay has reached the pulp but the infection is confined to the coronal pulp.
- Pulpectomy: All of the pulp, both in the crown and the root canals, is removed. This is similar to a full root canal but performed on primary teeth to remove a severely infected pulp, preparing the tooth for an internal filling.
The Root Canal Procedure: A Step-by-Step Guide
The thought of a root canal can be intimidating, but understanding the process can alleviate anxiety. Modern root canal treatment is a highly effective and generally comfortable procedure designed to save your tooth. Here's what to expect:
Step 1: Diagnosis and Treatment Planning
Your dentist or endodontist will thoroughly examine your tooth, take X-rays to assess the extent of the infection and the root canal anatomy, and perform vitality tests to determine the health of the pulp. This step is crucial for accurate diagnosis and planning the most appropriate treatment.
Step 2: Anesthesia
Before starting the procedure, the area around the affected tooth will be numbed using a local anesthetic. This ensures you feel no pain during the treatment, only pressure. Many patients report that getting the anesthetic injection is the most uncomfortable part of the entire procedure.
Step 3: Isolation of the Tooth
Once the tooth is numb, your dentist will place a small sheet of latex or non-latex material called a "dental dam" around the tooth. This dam isolates the tooth, keeps it clean and dry from saliva, and prevents bacteria from re-entering the tooth during treatment. It also protects you from swallowing any debris.
Step 4: Access Opening
A small opening is created through the crown of the tooth, either on the chewing surface (for back teeth) or the back (for front teeth), to gain access to the pulp chamber and root canals. This opening allows the dentist to reach the infected pulp.
Step 5: Cleaning and Shaping the Root Canals
Using very small, flexible instruments called files, the infected and inflamed pulp tissue is carefully removed from the pulp chamber and the intricate root canals. These instruments are used to clean, enlarge, and shape the canals, removing bacteria and debris. The dentist will frequently irrigate the canals with an antibacterial solution (like sodium hypochlorite) to disinfect them thoroughly. This step is meticulous and requires precision.
!Step-by-step illustration of the root canal procedure, showing: 1. Infected tooth, 2. Access opening and pulp removal, 3. Cleaning and shaping the canals, 4. Filling the canals with gutta-percha, 5. Final restoration with a crown.
Step 6: Filling the Root Canals (Obturation)
Once the canals are thoroughly cleaned, shaped, and disinfected, they are filled with a biocompatible, rubber-like material called gutta-percha. Gutta-percha, combined with a specialized adhesive sealer, is packed into the canals to completely fill and seal them, preventing reinfection.
Step 7: Temporary Filling and Restoration
After the root canals are filled, a temporary filling is placed in the access opening to seal the tooth until a permanent restoration can be applied. In some cases, if there's significant infection or inflammation, the dentist might place a medicament inside the tooth and seal it with a temporary filling, requiring a second appointment to complete the filling and sealing of the canals.
Pro Tip: Do not delay getting your final restoration (crown or permanent filling) after a root canal. The treated tooth, while no longer housing a nerve, can become brittle and prone to fracture without proper protection. A permanent restoration provides the necessary strength and seal to ensure the long-term success of the root canal.
How Long Does a Root Canal Take?
The duration of a root canal procedure varies depending on several factors, including the tooth's location, the complexity of its root canal system, and the extent of the infection.
- Front Teeth (Incisors and Canines): These teeth typically have a single root and one canal. A root canal for a front tooth often takes 60-90 minutes for a general dentist or 45-75 minutes for an endodontist due to their specialized efficiency.
- Premolars (Bicuspids): Located between the front teeth and molars, premolars usually have one or two roots and one or two canals. The procedure typically lasts 90-120 minutes.
- Molars (Back Teeth): Molars are the most complex, often having three or more roots and multiple canals (sometimes 3-4 or more). A root canal on a molar can take 90 minutes to 2 hours or even longer for very complex cases.
Most conventional root canal treatments can be completed in one appointment. However, if there's a severe infection, significant inflammation, or complex anatomy, your dentist may opt for two appointments. In such cases, the tooth is cleaned and a medicament is placed inside during the first visit, and the canals are filled and sealed during the second visit, usually a week or two later.
Table 1: Estimated Root Canal Procedure Duration
| Tooth Type | Number of Roots/Canals (Typical) | Estimated Time (General Dentist) | Estimated Time (Endodontist) |
|---|---|---|---|
| Front Tooth (Incisor/Canine) | 1 root, 1 canal | 60-90 minutes | 45-75 minutes |
| Premolar (Bicuspid) | 1-2 roots, 1-2 canals | 90-120 minutes | 75-100 minutes |
| Molar (Back Tooth) | 2-4 roots, 3-4+ canals | 90 minutes - 2+ hours | 75 minutes - 1.5+ hours |
Note: These are estimates. Individual cases may vary based on complexity.
Root Canal Treatment vs. Tooth Extraction: Making an Informed Choice
When faced with an infected or severely damaged tooth, the primary treatment options are often a root canal or tooth extraction. The decision should be made in consultation with your dentist or endodontist, weighing the pros and cons of each. The American Dental Association (ADA) generally recommends saving your natural teeth whenever possible.
Root Canal Treatment: Preserving Your Natural Tooth
Pros:
- Preserves Natural Tooth: Keeps your original tooth, which maintains your natural bite, chewing efficiency, and aesthetic appearance.
- Prevents Shifting: Prevents adjacent teeth from shifting into the empty space, which can lead to bite problems and jaw issues.
- Cost-Effective Long-Term: While the initial cost of a root canal plus a crown might seem higher than an extraction, replacing an extracted tooth with an implant or bridge can be significantly more expensive in the long run.
- High Success Rate: Modern root canal treatments have a high success rate, often lasting a lifetime with proper care.
- Less Invasive: Generally less invasive than extraction followed by implant placement.
Cons:
- Requires Restoration: The tooth will almost always need a permanent crown after the root canal to protect it from fracture.
- Potential for Retreatment: In a small percentage of cases, the tooth may require retreatment if the initial procedure fails.
Tooth Extraction: Removing the Damaged Tooth
Pros:
- Immediate Pain Relief: Once the tooth is removed, the source of infection and pain is gone.
- Less Complex Initial Procedure: Extraction itself is often a quicker and simpler procedure than a root canal.
Cons:
- Loss of Natural Tooth: Permanent loss of your natural tooth.
- Gap in Smile: Creates a visible gap, especially for front teeth.
- Shifting Teeth: Adjacent teeth can shift into the empty space, leading to bite problems, crooked teeth, and difficulty cleaning.
- Bone Loss: The jawbone in the area of the missing tooth will begin to resorb (shrink) over time due to lack of stimulation.
- Chewing Difficulties: Can affect chewing ability and speech.
- Higher Long-Term Costs: Requires replacement options like a dental implant, bridge, or partial denture, which are generally more expensive and involve additional procedures. A dental implant and crown can cost $3,000 - $6,000+.
Table 2: Root Canal vs. Extraction Comparison
| Feature | Root Canal Treatment (RCT) | Tooth Extraction (and Replacement) |
|---|---|---|
| Primary Goal | Save natural tooth, eliminate infection | Remove infected/damaged tooth |
| Tooth Preservation | Yes | No |
| Procedure Steps | Clean, shape, fill canals; usually followed by crown | Remove tooth; may involve bone grafting |
| Cost (Initial) | $700 - $2,000+ (RCT only) | $200 - $500 (Simple extraction) |
| Cost (Long-Term) | $1,500 - $3,500+ (RCT + Crown) | $2,000 - $7,000+ (Extraction + Bridge/Implant) |
| Recovery Time | Days to mild soreness | Days, potentially longer for complex extractions |
| Impact on Adjacent Teeth | None | Potential shifting, increased wear |
| Impact on Jawbone | Preserves bone | Leads to bone loss over time |
| Function/Aesthetics | Preserves natural function and appearance | Requires replacement for optimal function and aesthetics |
| Typical Success Rate | 95%+ with proper restoration | 100% (tooth removed), but potential complications with replacement |
Recovery and Aftercare Following a Root Canal
Proper aftercare is crucial for the long-term success of your root canal treatment. While you can typically return to normal activities fairly quickly, following your dentist's instructions will minimize discomfort and prevent complications.
Immediate Post-Procedure Care
- Numbness: The local anesthetic will wear off within a few hours. Avoid chewing on the treated side until the numbness subsides to prevent accidentally biting your tongue or cheek.
- Mild Soreness: It's common to experience some mild discomfort or soreness in the area for a few days, especially when chewing. This is due to inflammation from the procedure and should gradually subside. Over-the-counter pain relievers like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are usually sufficient to manage this.
- Sensitivity: You might notice some sensitivity to hot or cold for a short period, especially if the area was severely inflamed prior to treatment. This is normal and typically resolves.
Pain Management
- Over-the-Counter (OTC) Pain Relievers: For most patients, ibuprofen (400-600mg every 6 hours) or acetaminophen (500-1000mg every 4-6 hours) are effective. You can often alternate between these two for better pain control, as advised by your dentist.
- Prescription Pain Relievers: In rare cases of severe pre-existing infection or complex procedures, your dentist might prescribe a stronger pain medication or antibiotics. Always follow the prescribed dosage.
Oral Hygiene
- Brush and Floss Normally: Continue your regular oral hygiene routine, brushing and flossing around the treated tooth carefully. Maintaining good oral hygiene is essential to prevent new decay or gum disease.
- Avoid the Treated Tooth (Temporarily): If you have a temporary filling, try to avoid chewing hard or sticky foods on that side of your mouth until your permanent restoration is placed, as the temporary filling can dislodge or fracture.
Diet and Chewing
- Soft Foods: Stick to soft foods for the first few days after the procedure.
- Avoid Hard/Sticky Foods: Refrain from chewing on hard, crunchy, or sticky foods, especially on the treated tooth, until your permanent crown or filling is placed. The treated tooth is more fragile until it's properly restored and can be prone to fracture.
Follow-Up Appointments
- Permanent Restoration: This is critical. After the root canal is complete, you will need to return to your general dentist (or endodontist, if they also do restorative work) to have a permanent crown or filling placed. This usually happens within a few weeks to a month. A crown is typically recommended for back teeth (molars and premolars) to provide maximum protection, as they bear significant chewing forces. Front teeth may only require a durable filling if there is enough natural tooth structure remaining.
- Check-up: Your endodontist or general dentist may schedule a follow-up appointment several months later to check on the healing process with an X-ray.
Pro Tip: Protecting your treated tooth with a permanent restoration is paramount. The long-term success of your root canal depends heavily on this step. Without it, the tooth is susceptible to fracture, and the root canal can become compromised, leading to reinfection or failure.
Risks and Potential Complications of Root Canal Treatment
While root canal treatment has a high success rate (over 95% for initial treatments), like any medical procedure, there are potential risks and complications, though they are generally rare.
Persistent Infection
Despite thorough cleaning and disinfection, sometimes an infection can persist or recur. This can happen due to:
- Missed Canals: Some teeth have very narrow or extra canals that are difficult to locate, especially without specialized equipment like an operating microscope.
- Incomplete Cleaning: If all bacteria are not eliminated, the infection can linger.
- Cracked Root: An undetected crack in the tooth's root can allow bacteria to re-enter.
- Compromised Seal: If the final restoration (filling or crown) is not placed properly or cracks, bacteria can re-enter.
- New Decay: New decay around the crown or filling can expose the treated area to bacteria.
In these cases, retreatment or an apicoectomy may be necessary.
Structural Damage to the Tooth
- Fracture of the Tooth: A treated tooth, especially a molar, can become more brittle over time because it no longer has vital pulp supplying moisture. This makes it more susceptible to fracture, particularly if a crown is not placed promptly after the root canal.
- Instrument Separation: Very rarely, a tiny file used during the cleaning process can break inside a canal. While this can complicate the procedure, skilled endodontists can often bypass or remove the fragment, or seal it within the tooth, without affecting the outcome. If it cannot be removed, it may still be possible to save the tooth.
- Perforation: Accidental creation of an extra opening through the side of the tooth's root during the procedure. While rare with modern techniques, if it occurs, it can often be repaired.
Missed Canals
As mentioned, some teeth, particularly molars, can have complex root canal anatomy with extra or very fine canals that are challenging to identify and clean. If a canal is missed, the bacteria within it can continue to cause infection, leading to a failed root canal. This is one reason why an endodontist, with their specialized training and equipment, is often recommended for complex cases.
Allergic Reaction to Materials
Though very uncommon, a patient could have an allergic reaction to the materials used during the root canal, such as the latex in the dental dam, the gutta-percha, or the sealer.
Post-Procedure Pain or Flare-ups
While most patients experience minimal discomfort, some may have a "flare-up" of pain or swelling after the procedure. This is more common in teeth that were highly infected before treatment. This usually resolves with medication but can be distressing.
Despite these potential risks, the overall success rate of root canal treatment is very high. With proper diagnosis, skilled execution, and timely final restoration, the vast majority of treated teeth remain healthy and functional for many years, often a lifetime.
Children and Pediatric Endodontics
Children can also experience dental issues that affect the pulp, sometimes necessitating endodontic procedures, particularly in cases of deep decay or dental trauma. The goal in pediatric endodontics is often to preserve the primary (baby) tooth until it's naturally ready to fall out, or to help an immature permanent tooth continue its development.
Pulpotomy and Pulpectomy for Primary Teeth
- Pulpotomy (Pulp Capping): Often called a "baby root canal," this procedure is performed when decay has reached the pulp chamber of a primary tooth, but the infection or inflammation is limited to the crown portion of the pulp. The dentist removes only the infected pulp from the crown, disinfects the area, and places a medicated filling (like MTA or formocresol) to keep the remaining root pulp healthy. The tooth is then typically restored with a stainless steel crown. The goal is to keep the primary tooth in place until it naturally exfoliates, reserving space for the permanent tooth.
- Pulpectomy: If the infection has spread throughout the entire pulp system (crown and roots) of a primary tooth, a pulpectomy is performed. This involves removing all the pulp tissue from both the crown and the root canals, much like a conventional root canal on a permanent tooth. The canals are then disinfected and filled with a resorbable material (unlike gutta-percha, which is permanent) that allows the tooth to eventually be reabsorbed by the body and make way for the permanent tooth. The tooth is then usually restored with a stainless steel crown.
Apexification and Apexogenesis for Immature Permanent Teeth
When a permanent tooth erupts, its root ends (apices) are not fully formed. If such a tooth sustains trauma or severe decay and its pulp becomes infected, specialized procedures are required to encourage root development.
- Apexogenesis: This procedure is performed when the pulp is still vital but exposed or inflamed. The goal is to preserve the healthy pulp tissue to allow the root to continue forming naturally. The dentist removes the inflamed pulp and places a biocompatible material (like MTA) over the remaining healthy pulp to encourage the root end to close.
- Apexification: If the pulp of an immature permanent tooth is necrotic (dead) and the root apex is open, apexification is used. The dentist cleans and disinfects the canal, then places a material (often MTA or calcium hydroxide) at the root tip to induce the formation of a hard tissue barrier, which allows the root end to close. Once the apex is closed, the tooth can then undergo a conventional root canal filling.
These procedures highlight the specialized approaches needed for children to preserve their dental health and guide the development of their permanent dentition.
Root Canal Cost and Insurance Coverage
Understanding the cost of a root canal is a major concern for many patients. The price can vary significantly based on several factors, but typically ranges from a few hundred to over two thousand dollars in the US.
Factors Influencing Cost
- Tooth Location:
- Front Teeth (Incisors/Canines): Generally the least expensive as they have one root and one canal.
- Premolars (Bicuspids): Mid-range, usually 1-2 roots/canals.
- Molars (Back Teeth): Most expensive due to their multiple roots (2-4 or more) and complex canal systems, which take more time and skill to treat.
- Complexity of the Case:
- Calcified Canals, Curved Roots, Additional Canals: These factors increase treatment time and require more advanced techniques and equipment, increasing the cost.
- Endodontic Retreatment: Re-doing a failed root canal is typically more expensive than the initial treatment.
- Apicoectomy (Endodontic Surgery): This surgical procedure is more complex and thus more costly.
- Dental Professional:
- General Dentist: May charge less than an endodontist for a root canal.
- Endodontist: Due to their specialized training, advanced equipment (e.g., operating microscopes), and expertise in complex cases, endodontists typically have higher fees.
- Geographic Location:
- Costs can vary significantly by state, city, and even neighborhood. Major metropolitan areas generally have higher dental costs.
- Ancillary Services:
- X-rays and Diagnostic Fees: Included in the overall cost.
- Post and Core: If significant tooth structure is lost, a "post" (a small rod) may be placed in the canal and built up with a "core" filling to support a crown. This is an additional cost (typically $200-$500).
- Permanent Restoration (Crown or Filling): This is a separate and essential cost after the root canal. A dental crown can range from $800 to $2,500+ depending on the material (e.g., porcelain, zirconia, gold) and location.
Average US Root Canal Costs by Tooth Type (Before Insurance)
| Tooth Type | Average Low Range | Average Mid Range | Average High Range |
|---|---|---|---|
| Front Tooth | $700 | $1,000 | $1,500 |
| Premolar | $800 | $1,200 | $1,800 |
| Molar | $1,000 | $1,500 | $2,200+ |
These figures represent the cost of the root canal procedure itself, not including the final crown or restoration.
Impact of Dental Insurance
Most dental insurance plans offer some coverage for root canal treatment, as it's considered a major restorative procedure.
- Coverage Levels: Typically, insurance covers 50-80% of the cost after you meet your deductible, up to your annual maximum.
- Deductibles: You will usually need to pay an annual deductible (e.g., $50-$100) before your insurance begins to pay.
- Annual Maximums: Most plans have an annual maximum benefit (e.g., $1,000-$2,000). If your root canal plus the crown exceeds this, you will pay the difference.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) for major procedures like root canals.
- In-Network vs. Out-of-Network: Your out-of-pocket costs will likely be lower if you choose a dentist or endodontist who is in your insurance network.
It's crucial to contact your insurance provider directly or ask your dental office to provide a pre-treatment estimate to understand your specific out-of-pocket costs.
Payment Plans and Financing Options
For those without insurance or with high out-of-pocket costs, several financing options are available:
- In-Office Payment Plans: Many dental offices offer their own payment plans, allowing you to pay in installments.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest or low-interest payment plans.
- Dental Schools: Dental schools often offer reduced-cost treatment performed by students under the supervision of experienced faculty.
- Community Dental Clinics: Some non-profit or government-funded clinics provide services at a reduced rate based on income.
Pro Tip: Maximizing your dental benefits starts with understanding your plan. Always ask for a detailed cost estimate from your dental office before starting treatment, and confirm your coverage with your insurance company to avoid surprises.
!Infographic showing average root canal costs by tooth type and US region, e.g., "Molar Root Canal: Northeast $1800, Midwest $1500, South $1400, West $1700" with icons for each tooth type.
Preventing the Need for a Root Canal
The best treatment is prevention. While some causes like trauma are hard to avoid, many root canal needs stem from preventable issues.
- Maintain Excellent Oral Hygiene:
- Brush Twice Daily: Brush thoroughly for two minutes twice a day with fluoride toothpaste.
- Floss Daily: Floss once a day to remove plaque and food particles from between teeth and under the gumline, where toothbrushes can't reach.
- Regular Dental Check-ups and Cleanings:
- Visit your dentist every six months for professional cleanings and examinations. This allows your dentist to detect and treat small cavities before they become deep enough to infect the pulp. Regular X-rays help identify problems that aren't visible to the naked eye.
- Prompt Treatment of Cavities:
- If a cavity is detected, get it filled promptly. The longer decay is left untreated, the deeper it progresses, increasing the risk of pulp involvement.
- Protect Your Teeth from Trauma:
- Wear a Mouthguard: If you play contact sports or grind your teeth (bruxism) at night, wear a custom-fitted mouthguard to protect your teeth from impacts and excessive force.
- Avoid Chewing on Hard Objects:
- Refrain from chewing on ice, hard candies, popcorn kernels, or non-food items like pen caps, as these can chip or crack your teeth, creating pathways for infection.
- Healthy Diet:
- Limit sugary and acidic foods and drinks, which contribute to tooth decay.
- Stay hydrated by drinking plenty of water.
By following these preventative measures, you can significantly reduce your risk of developing pulp infections and the need for a root canal.
Frequently Asked Questions
Is a root canal painful?
Modern root canal treatments are generally not painful. Thanks to advanced local anesthetics, the procedure itself is often no more uncomfortable than getting a routine filling. The goal of a root canal is to relieve the severe pain caused by an infected pulp, not to cause more pain. Post-procedure soreness is typically mild and managed with over-the-counter pain relievers.
How long will a root canal last?
With proper restoration (usually a crown) and good oral hygiene, a treated tooth can last a lifetime. Root canal treatments have a very high success rate, often exceeding 95% for initial procedures. Regular dental check-ups are essential to monitor the tooth's long-term health.
What are the alternatives to a root canal?
The primary alternative to a root canal for an infected tooth is tooth extraction. While extraction removes the source of infection, it also results in the loss of your natural tooth, which can lead to shifting adjacent teeth, bone loss, and the need for costly replacements like a dental implant or bridge to restore function and aesthetics.
Can a root canal fail?
Yes, although rare, a root canal can sometimes fail. This can happen if the tooth becomes reinfected due to missed canals, an incomplete seal, a new crack, or a breakdown of the final restoration. In such cases, endodontic retreatment or an apicoectomy (minor surgery) may be necessary to save the tooth.
How do I find a good endodontist near me?
You can ask your general dentist for a referral, as they often work with trusted specialists. You can also search online directories provided by professional organizations like the American Association of Endodontists (AAE) or the American Dental Association (ADA), which allow you to search for board-certified endodontists in your area. Online reviews and testimonials can also provide insight.
Can I eat normally after a root canal?
Immediately after the procedure, it's best to stick to soft foods and avoid chewing on the treated side until the numbness wears off. If a temporary filling was placed, you should continue to avoid hard or sticky foods on that tooth until your permanent restoration (crown or filling) is placed to prevent dislodging the temporary filling or fracturing the tooth. Once the permanent restoration is in place, you can typically resume normal chewing.
Do I need a crown after a root canal?
In most cases, especially for back teeth (molars and premolars) that endure significant chewing forces, a dental crown is highly recommended after a root canal. A treated tooth can become more brittle without its vital pulp and is prone to fracture. A crown provides crucial protection, reinforces the tooth, and helps ensure the long-term success of the root canal. Front teeth may sometimes only require a strong permanent filling if enough tooth structure remains.
Is it safe to get a root canal while pregnant?
Yes, a root canal is generally considered safe during pregnancy, particularly in the second trimester, if medically necessary to treat an active infection. Untreated dental infections can pose a greater risk to both the mother and the baby. Your dentist or endodontist will take precautions, such as using minimal radiation X-rays with a lead apron, and choosing appropriate local anesthetics.
What is the success rate of a root canal?
Root canal treatment has a very high success rate, with studies showing primary treatments succeeding over 95% of the time when followed by an appropriate permanent restoration. The success rate for retreatment can be slightly lower but is still often very effective in saving the tooth.
Why do I need multiple appointments?
While many root canals are completed in one appointment, some complex cases require two or more. This might be due to a severe infection requiring a medicament to be placed in the tooth for a period, complex canal anatomy that needs more time for thorough cleaning, or if the procedure is particularly lengthy and cannot be completed comfortably in a single session.
When to See a Dentist
Recognizing the signs that warrant a dental visit, especially for potential endodontic issues, is critical for preserving your oral health and preventing more severe problems.
Seek immediate dental attention if you experience any of the following:
- Severe, persistent toothache: Pain that keeps you awake at night, is constant, or worsens with pressure.
- Prolonged sensitivity: Sensitivity to hot or cold that lingers for more than a few seconds after the stimulus is removed.
- Swelling in your gums, face, or neck: This indicates a spreading infection or abscess, which can become serious if left untreated.
- A "pimple" on your gums: A small, persistent bump that may or may not drain pus signifies a draining infection (fistula).
- Tooth discoloration: A tooth that suddenly darkens to gray or black may indicate a dying or necrotic pulp.
- Pain when chewing or touching a specific tooth: This could indicate inflammation around the tooth's root.
These are all red flags that suggest an infected or inflamed pulp that likely requires endodontic treatment. Delaying treatment can lead to the infection spreading, significant bone loss, and ultimately, the loss of the tooth. If you suspect you need a root canal, contact your dentist or an endodontist promptly. Early intervention can save your tooth and significantly alleviate your discomfort.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Stop Throbbing Pain After Root Canal
Undergoing a root canal procedure is often a necessary step to save a tooth severely damaged by decay or infection, preventing further complications and excruciating pain. While the procedure itself is performed under local anesthesia to ensure comfort, it's common for patients to experience some le
February 22, 2026
Root Canal After Care: Complete Guide
A root canal procedure can be a tooth-saving treatment, offering relief from pain and preventing further infection. However, the success and longevity of this crucial dental intervention heavily rely on diligent root canal after care. Neglecting post-treatment instructions can lead to complicati
February 22, 2026

Can You Drive After a Root Canal
Undergoing a root canal procedure can understandably bring up a host of questions and concerns, from understanding the process itself to managing recovery. One of the most common and practical inquiries people have is: can you drive after a root canal? The answer isn't always a simple yes or no,
February 22, 2026
Is a Root Canal Painful
When facing the prospect of a root canal, one of the most common and immediate questions that comes to mind is: is a root canal painful? It's a valid concern, stemming from outdated perceptions and anecdotal stories. However, modern root canal therapy is a highly effective and generally comforta
February 22, 2026