Can You Drive After a Root Canal

Key Takeaways
- Undergoing a root canal procedure can understandably bring up a host of questions and concerns, from understanding the process itself to managing recovery. One of the most common and practical inquiries people have is: can you drive after a root canal? The answer isn't always a simple yes or no,
Introduction
Undergoing a root canal procedure can understandably bring up a host of questions and concerns, from understanding the process itself to managing recovery. One of the most common and practical inquiries people have is: can you drive after a root canal? The answer isn't always a simple yes or no, as it heavily depends on factors such as the type of anesthesia or sedation used during your treatment. An estimated 15 million root canal treatments are performed annually in the United States, making this a highly relevant topic for many patients seeking to restore their dental health.
This procedure, formally known as endodontic treatment, is designed to save a tooth that has become infected or severely decayed, preventing extraction and preserving your natural smile. While modern root canals are significantly less painful than their historical reputation suggests, the immediate aftermath involves managing anesthetic effects and mild discomfort. Understanding what to expect regarding recovery, pain management, and the financial investment (including the cost of a root canal and insurance considerations) is crucial for a smooth experience. This comprehensive guide will delve into these aspects, ensuring you are well-prepared for your root canal procedure and confident in navigating your post-treatment care, including when it’s safe to get back behind the wheel. We'll cover everything from the intricate steps of the procedure and typical recovery timelines to prevention strategies and common questions like how painful is a root canal, providing you with authoritative, accessible information.
Key Takeaways:
- Driving Safety: You generally cannot drive after a root canal if you've received oral sedation, IV sedation, or general anesthesia. Local anesthesia alone typically allows for driving, but always confirm with your dentist.
- Pain Management: Root canals are not inherently painful; discomfort is managed with local anesthesia during the procedure and over-the-counter pain relievers afterward. Expect mild soreness, not severe pain.
- Cost Variation: The cost of a root canal ranges widely from $700 to $2,500 or more, depending on the tooth treated (front, premolar, molar) and geographic location in the US.
- Insurance Coverage: Most dental insurance plans cover a significant portion of root canal costs (typically 50-80% after deductible), but coverage varies.
- Recovery Timeline: Initial soreness usually subsides within a few days. The tooth may be sensitive for a week or two, but full functionality returns quickly.
- Crown Placement: A permanent crown or filling is usually placed a few weeks after the root canal to protect the treated tooth from fracture and ensure long-term success.
- Prevention: Good oral hygiene, regular dental check-ups, and a balanced diet are key to preventing the need for root canal treatment.
What Is a Root Canal? An Overview
A root canal, or endodontic treatment, is a common dental procedure designed to save a tooth that has been severely damaged due to deep decay, cracks, chips, or trauma. At the heart of every tooth lies the pulp, a soft tissue containing nerves, blood vessels, and connective tissue. This pulp extends from the crown of the tooth down into the root canals (hence the name "root canal"). When the pulp becomes infected or inflamed due to bacterial invasion (often from untreated cavities) or injury, it can cause significant pain and lead to serious dental abscesses if left untreated.
The purpose of a root canal is to remove the infected or inflamed pulp, clean and disinfect the inside of the tooth, and then fill and seal the space. This process eliminates the infection, relieves pain, and protects the tooth from future microbial invasion. By performing a root canal, dentists can save your natural tooth, preventing the need for extraction and maintaining the alignment of your other teeth, proper chewing function, and the aesthetics of your smile.
Types of Root Canal Procedures
While the general principle of a root canal remains the same, variations exist depending on the tooth affected and the complexity of the case.
- Standard Root Canal Treatment (RCT): This is the most common procedure performed on a tooth with an infected or inflamed pulp. It involves accessing the pulp chamber, removing the diseased tissue, cleaning and shaping the root canals, and then filling them with a biocompatible material called gutta-percha. A temporary filling is placed, and a permanent restoration (usually a crown) follows.
- Apicoectomy (Root-End Resection): This is a surgical procedure performed when a standard root canal treatment isn't sufficient to resolve an infection, or if re-infection occurs after a previous root canal. During an apicoectomy, the endodontist (a dental specialist in root canals) removes the tip of the tooth's root along with any infected tissue, then seals the root canal with a small filling. This is typically done through the gum and bone, bypassing the crown of the tooth.
- Pulpotomy: Often considered a "partial root canal," a pulpotomy is more common in primary (baby) teeth. It involves removing only the infected part of the pulp in the crown, leaving the healthy pulp in the root canals intact. This aims to keep the primary tooth vital until it naturally exfoliates.
- Pulpectomy: Also more common in primary teeth or in some emergency situations for permanent teeth, a pulpectomy involves removing all the pulp tissue from both the crown and root canals. The canals are then filled, usually with a material that can be absorbed if it's a primary tooth.
- Root Canal Retreatment: If a tooth that has already undergone a root canal becomes re-infected or fails to heal properly, a root canal retreatment may be necessary. This involves reopening the tooth, removing the previous filling material, cleaning and reshaping the canals again, and then refilling and sealing them.
Causes: Why Do You Need a Root Canal?
The primary reason for needing a root canal is an infection or inflammation of the dental pulp. This typically occurs due to several factors:
- Deep Decay: Untreated cavities can progress, eventually reaching the pulp chamber. Once bacteria penetrate the pulp, they cause inflammation (pulpitis) and infection.
- Repeated Dental Procedures: Multiple fillings or other extensive dental work on the same tooth can stress the pulp, leading to inflammation over time.
- Cracked or Chipped Tooth: A crack or chip in the tooth, especially if it extends below the gum line or into the pulp, can create an entry point for bacteria, leading to infection.
- Trauma to the Tooth: A severe blow or injury to a tooth, even if there's no visible crack, can damage the blood supply to the pulp, causing it to die and become infected.
- Gum Disease: In advanced stages, gum disease can affect the bone supporting the teeth, potentially leading to pulp exposure and infection, although this is less common.
Signs and Symptoms You Might Need a Root Canal
Recognizing the signs and symptoms early can help you seek timely treatment and prevent further complications. While some people experience no symptoms, common indicators include:
- Persistent Tooth Pain: This is the most common symptom. The pain can range from mild to severe and may be constant or intermittent. It might worsen when chewing or applying pressure.
- Sensitivity to Hot and Cold: Lingering sensitivity to hot or cold temperatures, even after the stimulus is removed, is a strong indicator of pulp inflammation.
- Swelling and Tenderness in the Gums: The area around the affected tooth may become swollen, red, and tender to the touch. This can indicate an abscess.
- Pimple-Like Bump on the Gums (Fistula): A small bump, often called a "pimple" or "gum boil," may appear on the gums near the infected tooth. This is a sign of an abscess draining pus.
- Discoloration of the Tooth: The affected tooth may darken or become discolored, often a grayish or yellowish hue, indicating that the pulp tissue is dying.
- Pain When Chewing or Touching the Tooth: Sensitivity or pain when biting down or touching the tooth is another common symptom.
- Pus Drainage: In some cases, pus may drain from the affected tooth or gums.
If you experience any of these symptoms, it's crucial to schedule an appointment with your dentist promptly for an accurate diagnosis and appropriate treatment.
Treatment Options for an Infected Tooth
When faced with an infected or severely damaged tooth, your dentist will present primary treatment options. The goal is always to preserve your natural tooth if possible.
- Root Canal Treatment (Endodontic Therapy):
- Pros: Saves your natural tooth, preserves your bite and smile, highly successful (over 95% success rate), prevents the need for extraction and subsequent prosthetic solutions.
- Cons: Requires multiple appointments (diagnosis, root canal, permanent restoration), can be more costly than an extraction initially (but often less costly long-term than replacing a missing tooth).
- Recommendation: The preferred treatment for saving a tooth with infected pulp.
- Tooth Extraction:
- Pros: Immediate relief from the infected tooth, often a simpler procedure than a root canal, potentially lower upfront cost.
- Cons: Permanent tooth loss, can lead to shifting of adjacent teeth, bone loss in the jaw, altered bite, potential speech difficulties, requires subsequent procedures (bridge, implant, partial denture) to replace the missing tooth, which are typically more expensive than a root canal in the long run.
- Recommendation: Considered when a tooth is too damaged to be saved by a root canal, or if a root canal has failed and retreatment is not viable.
Comparison of Root Canal vs. Extraction
| Feature | Root Canal Treatment | Tooth Extraction |
|---|---|---|
| Purpose | Save natural tooth | Remove natural tooth |
| Longevity | Can last a lifetime with proper care | Permanent tooth loss, requires replacement |
| Impact on Bite | Preserves natural bite and alignment | Can lead to shifting teeth, bite changes, bone loss |
| Procedure Steps | Pulp removal, cleaning, filling, sealing, crown | Tooth removal |
| Cost (Initial) | Higher than simple extraction | Lower than root canal initially |
| Cost (Long-term) | Generally lower than extraction + replacement | Higher due to cost of bridge, implant, or denture |
| Recovery | Mild soreness for a few days | Mild soreness, potential swelling, sometimes dry socket |
| Ideal For | Salvageable teeth with infected pulp | Severely damaged or untreatable teeth |
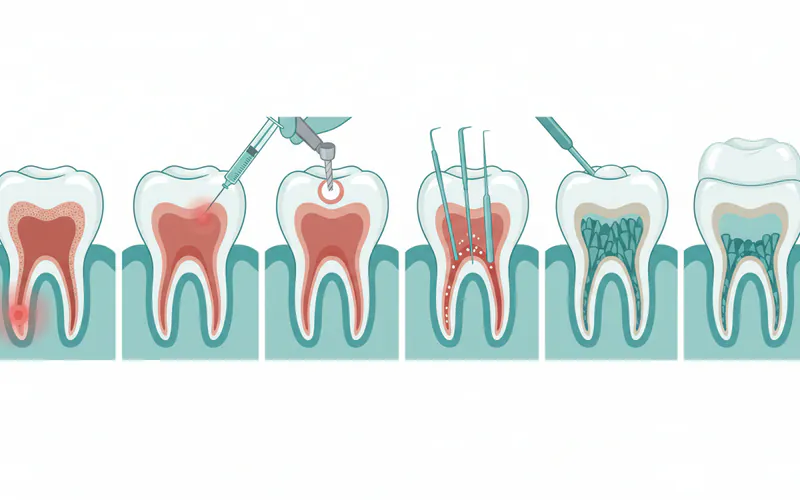
Step-by-Step Root Canal Process
Understanding the procedure can help alleviate anxiety. A root canal is typically performed over one or two appointments.
-
Diagnosis and Anesthesia:
- Your dentist will examine your tooth, take X-rays, and conduct tests to confirm the pulp infection.
- Local anesthesia is administered to numb the tooth and surrounding area, ensuring you feel no pain during the procedure. This is the critical factor for whether you can you drive after a root canal.
- If you're particularly anxious, your dentist may offer sedation dentistry options, which will impact your ability to drive.
-
Isolation:
- A small sheet of latex or non-latex material called a dental dam is placed around the affected tooth. This isolates the tooth, keeps it clean and dry, and prevents bacteria from the saliva from entering during the procedure.
-
Access Hole Creation:
- The dentist or endodontist drills a small access hole through the crown of the tooth, usually on the biting surface for molars or the back surface for front teeth, to reach the pulp chamber and root canals.
-
Pulp Removal and Cleaning:
- Tiny instruments, called files, are used to remove the infected or inflamed pulp tissue from the pulp chamber and the intricate root canals.
- The canals are then thoroughly cleaned, shaped, and disinfected using antibacterial solutions. This step is crucial for eliminating bacteria and preventing re-infection.
-
Filling and Sealing:
- Once the canals are meticulously cleaned and shaped, they are filled with a rubber-like, biocompatible material called gutta-percha. This material is inserted along with an adhesive sealer to completely fill and seal the root canals, preventing future bacterial invasion.
-
Temporary Restoration:
- After the root canals are sealed, a temporary filling is placed over the access hole to protect the tooth until a permanent restoration can be placed.
-
Permanent Restoration (Crown):
- In most cases, especially for back teeth that endure significant chewing forces, a permanent dental crown is necessary to fully protect the treated tooth from fracture and restore its full function. This is typically done in a separate appointment, a few weeks after the root canal. For front teeth, a permanent filling may suffice.
Cost and Insurance: How Much Does a Root Canal Cost?
Understanding the cost of a root canal is a significant concern for many patients. Prices can vary widely based on several factors: the tooth's location, the complexity of the case, the experience of the dental professional, and geographic location within the US.

Average US Cost Ranges for Root Canals
The general range for a root canal in the United States is typically between $700 and $2,500, sometimes extending higher for complex cases or specialist care.
- Front Tooth (Incisor or Canine): These teeth usually have only one root canal, making the procedure less complex and therefore generally less expensive.
- Average Cost: $700 - $1,200
- Premolar (Bicuspid): These teeth typically have one or two root canals.
- Average Cost: $800 - $1,500
- Molar: Molars have multiple roots (two to four or more) and are often the most complex to treat, requiring more time and specialized instruments.
- Average Cost: $1,200 - $2,500+
- Endodontist vs. General Dentist: An endodontist (a root canal specialist) typically charges slightly more than a general dentist due to their specialized training, equipment, and expertise.
- Specialist Surcharge: $100 - $500+
Additional Costs to Consider
The cost of the root canal procedure itself doesn't always include the final restoration:
- Dental Crown: After a root canal, a permanent crown is usually required to protect the weakened tooth.
- Average Cost: $800 - $2,500 per crown, depending on the material (porcelain, ceramic, metal alloy) and lab fees. This is a significant additional expense.
- Post and Core: If there isn't enough natural tooth structure left to support a crown, a "post and core" buildup may be needed.
- Average Cost: $200 - $500
- Consultation/X-rays: Initial diagnostic costs can add $50 - $200.
Impact of Dental Insurance on Root Canal Costs
Most dental insurance plans do offer coverage for root canal treatment. However, the extent of coverage varies greatly.
- Coverage Percentage: Many plans categorize root canals as a "major procedure" and typically cover 50% to 80% of the cost after your deductible has been met.
- Deductibles: You will likely need to pay an annual deductible (e.g., $50 - $100) before your insurance starts paying.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit (e.g., $1,000 - $2,000). If your root canal and crown exceed this, you'll pay the remainder out-of-pocket.
- Waiting Periods: Some plans have waiting periods for major procedures, meaning you might have to wait 6-12 months after enrollment before a root canal is covered.
- In-Network vs. Out-of-Network: Choosing an in-network provider will typically result in lower out-of-pocket costs.
Example Scenario (Molar Root Canal with Crown):
- Total Estimated Cost (Root Canal + Crown): $1,800 (root canal) + $1,500 (crown) = $3,300
- Your Deductible: $50
- Insurance Pays 70% of remaining ($3,300 - $50 = $3,250 * 0.70 = $2,275)
- Your Out-of-Pocket: $50 (deductible) + $975 (30% co-insurance) = $1,025 (assuming no annual maximum reached).
- If your annual maximum is $1,500, and you've already used $500 for other treatments, your insurance will only pay $1,000, leaving you with a higher out-of-pocket cost.
Cost Comparison Table (Without Insurance)
| Tooth Type | General Dentist (Avg. Range) | Endodontist (Avg. Range) |
|---|---|---|
| Front Tooth | $700 - $1,000 | $800 - $1,200 |
| Premolar | $800 - $1,300 | $950 - $1,500 |
| Molar | $1,200 - $1,800 | $1,500 - $2,500+ |
Pro Tip: Always get a detailed treatment plan and estimate from your dentist before beginning treatment. Contact your insurance provider directly to understand your specific coverage, deductibles, and annual maximums.
Payment Plans and Financing Options
If you don't have insurance or face high out-of-pocket costs, several options can help:
- In-Office Payment Plans: Many dental offices offer flexible payment schedules directly, allowing you to pay in installments.
- Dental Savings Plans: These are not insurance but offer discounted rates (10-60%) on dental procedures for an annual membership fee.
- Healthcare Credit Cards (e.g., CareCredit): These specialized credit cards offer low or no-interest financing options for healthcare expenses over a set period.
- Personal Loans: Banks or credit unions offer personal loans for larger medical expenses.
- Community Dental Clinics/Dental Schools: These often provide services at a reduced cost.
Recovery and Aftercare: Post-Procedure Guidelines
After your root canal, proper aftercare is essential for a smooth recovery and the long-term success of your treatment.
Immediate Post-Procedure Care (First 24-48 Hours)
- Manage Discomfort: It's normal to experience some mild discomfort, tenderness, or sensitivity for a few days after the procedure, especially once the local anesthesia wears off. This is a common part of how painful is a root canal recovery, but it's typically manageable.
- Pain Relief: Over-the-counter pain relievers like ibuprofen (Advil, Motrin) or naproxen (Aleve) are usually sufficient. Your dentist may prescribe stronger medication if necessary, but this is rare.
- Cold Compress: Apply a cold compress to the outside of your cheek if there's any swelling.
- Eating and Drinking:
- Avoid Chewing: Do not chew or bite on the treated tooth until the numbness completely wears off to prevent accidental biting of your tongue or cheek.
- Soft Foods: Stick to soft foods for the first few days (yogurt, soup, mashed potatoes, smoothies).
- Avoid Hard/Chewy Foods: Steer clear of hard, crunchy, or sticky foods until the permanent crown is placed, as the temporary filling can be dislodged, or the weakened tooth might fracture.
- Oral Hygiene:
- Continue to brush and floss as usual, but be gentle around the treated tooth.
- Rinsing with warm salt water can help promote healing and reduce inflammation.
- Avoid Alcohol and Smoking: These can hinder the healing process.
Long-Term Aftercare (After Permanent Restoration)
Once your permanent crown or filling is placed:
- Maintain Excellent Oral Hygiene: Brush twice a day, floss daily, and use an antimicrobial mouthwash to keep your teeth and gums healthy.
- Regular Dental Check-ups: Continue with your routine dental check-ups and cleanings as recommended by your dentist.
- Avoid Biting Hard Objects: Be cautious with extremely hard foods or non-food items (like ice or pen caps) to prevent damage to your crown or the treated tooth.
- Nightguard: If you grind or clench your teeth (bruxism), your dentist might recommend a nightguard to protect your new crown and other teeth.
Can You Drive After a Root Canal?
This is a critical question. The ability to drive safely immediately after a root canal depends entirely on the type of anesthesia or sedation you received.
- Local Anesthesia Only: If your root canal was performed using only local anesthesia (an injection to numb the tooth), you should generally be fine to drive yourself home. Local anesthesia numbs only the treatment area and does not impair your cognitive function or motor skills. You might feel a bit numb in your face or jaw, but it won't affect your ability to drive.
- Oral Sedation (e.g., Valium, Halcion): If you were given oral medication to help you relax, even a mild sedative, you cannot drive yourself home. Oral sedatives can cause drowsiness, impaired judgment, and delayed reaction times, making driving unsafe. You will need someone to drive you to and from your appointment.
- IV Sedation (Intravenous Sedation): IV sedation induces a deeper state of relaxation and often partial amnesia of the procedure. Under no circumstances should you drive after IV sedation. You will require a responsible adult to escort you home and remain with you for several hours.
- General Anesthesia: General anesthesia puts you completely to sleep. You will absolutely not be able to drive after general anesthesia. You will need an escort and post-operative monitoring.
Pro Tip: Always discuss the type of anesthesia or sedation planned with your dentist before your appointment. If there's any chance you'll receive more than local anesthesia, arrange for a ride home in advance. Err on the side of caution; if you feel at all groggy, disoriented, or unsure, do not drive.
Prevention: Avoiding the Need for a Root Canal
The best way to avoid a root canal is to prevent the deep decay and infections that necessitate the procedure in the first place.
- Excellent Oral Hygiene:
- Brush Twice Daily: Use a fluoride toothpaste and brush for at least two minutes, covering all surfaces of your teeth.
- Floss Daily: Flossing removes plaque and food particles from between teeth and under the gum line, areas your toothbrush can't reach.
- Regular Dental Check-ups and Cleanings:
- Visit your dentist at least twice a year for professional cleanings and examinations. Early detection of cavities or other issues can prevent them from progressing to a point where a root canal is needed.
- Balanced Diet:
- Limit sugary foods and drinks, which contribute to tooth decay.
- Eat a diet rich in fruits, vegetables, and dairy products that provide essential nutrients for strong teeth.
- Protect Your Teeth:
- Wear a mouthguard during sports or any activity with a risk of facial impact to prevent traumatic injuries to your teeth.
- If you grind or clench your teeth at night, talk to your dentist about a custom-fitted nightguard.
- Address Dental Issues Promptly:
- Don't ignore tooth pain or sensitivity. Seek dental care immediately if you notice any signs of decay, chips, or cracks.
- Address existing cavities with fillings before they become deep enough to infect the pulp.
Risks and Complications of Root Canal Treatment
While root canal therapy has a high success rate (over 95% according to the American Association of Endodontists), as with any medical procedure, there are potential risks and complications, though they are rare.
- Persistent Infection: Although rare, the infection might not be completely eliminated, or it could return. This can happen if:
- The tooth has additional, undetected canals that were not cleaned.
- The root canal filling material doesn't adequately seal the tooth.
- A crack in the root was not detected.
- The crown placement is delayed, leading to re-contamination.
- In such cases, retreatment or an apicoectomy may be necessary.
- Fracture of the Tooth: A root-canaled tooth, especially one that hasn't received a permanent crown, can become brittle and more susceptible to fracture. This is why a crown is almost always recommended to protect the tooth.
- Procedural Errors:
- Instrument Separation: A tiny dental file can sometimes break off inside the root canal, making it difficult to fully clean and seal the canal. Endodontists often have specialized tools to retrieve these fragments.
- Perforation: During the procedure, the dentist might accidentally create a hole (perforation) in the side of the tooth or root. Small perforations can often be repaired, but larger ones can compromise the tooth's long-term prognosis.
- Nerve Damage: In very rare instances, particularly with lower molars, the instruments used during a root canal could potentially irritate or damage nearby nerves, leading to temporary or (extremely rarely) permanent numbness in the lip, chin, or tongue.
- Allergic Reaction: While uncommon, some individuals may have an allergic reaction to the anesthesia, the materials used (e.g., gutta-percha), or medications prescribed.
- Flare-up: Some patients may experience a temporary increase in pain, swelling, or sensitivity a few days after the procedure. This "flare-up" usually resolves on its own or with medication, but severe cases require further attention.
It is important to discuss any concerns about these risks with your dentist or endodontist. They will take all necessary precautions to minimize these potential complications.
Children / Pediatric Considerations
Root canal therapy is not exclusive to adults. Children can also require endodontic procedures, particularly on their primary (baby) teeth. The goal in pediatric endodontics is to save the primary tooth until it's naturally ready to fall out, preserving space for the permanent tooth and maintaining chewing function.
- Pulpotomy: This is the most common "root canal" procedure performed on baby teeth. It involves removing the infected pulp from the crown of the tooth while leaving the healthy pulp in the roots. The remaining pulp is then medicated, and the tooth is filled, often with a stainless steel crown. A pulpotomy helps prevent premature tooth loss.
- Pulpectomy: If the infection has spread to the root canals of a primary tooth, a pulpectomy may be performed. This involves removing all the pulp from the crown and roots, followed by filling the canals with an absorbable material.
- Indications: Pediatric root canals are needed for deep cavities that reach the pulp, traumatic injuries to the primary teeth, or infections that cause pain and swelling.
- Importance: Saving primary teeth is crucial for several reasons: they help guide the eruption of permanent teeth, maintain proper chewing and speech, and prevent other teeth from shifting. Premature loss of a baby tooth can lead to spacing issues for the permanent successor.
- Driving for Parents: If your child undergoes a root canal procedure with sedation, they will need close supervision and will not be able to participate in activities that require focus. As a parent, you will need to arrange transportation for your child and plan to monitor them for several hours post-procedure.
Cost Breakdown: A Deeper Dive
While we touched on costs earlier, let's consolidate and expand on the various elements that factor into the total expense of a root canal.
Average US Costs (Low, Mid, High) by Tooth Type (Without Insurance)
| Tooth Type | Low Cost (General Dentist) | Mid Cost (General Dentist/Endodontist) | High Cost (Complex/Specialist) |
|---|---|---|---|
| Front Tooth | $700 | $950 | $1,200 |
| Premolar | $800 | $1,200 | $1,500 |
| Molar | $1,200 | $1,800 | $2,500+ |
These figures are for the root canal procedure only and do not include the cost of a permanent crown or additional services.
With vs. Without Insurance
- Without Insurance (Out-of-Pocket): You will be responsible for 100% of the costs listed above, plus any additional procedures like crowns, posts, or sedation fees. A molar root canal and crown could easily total $2,000 - $5,000+ without any coverage.
- With Insurance: As discussed, insurance typically covers 50-80% of the root canal procedure after your deductible.
- In-Network: Your out-of-pocket expenses will be lower due to negotiated rates.
- Out-of-Network: You may pay more, as the insurance company might cover a smaller percentage, or you may be responsible for the difference between the dentist's fee and what the insurance company considers "usual and customary."
Factors Influencing Cost
- Geographic Location: Dental costs are generally higher in major metropolitan areas and on the coasts compared to rural areas or the Midwest.
- Dentist's Fees: The experience and reputation of the dentist or endodontist can influence their fees.
- Complexity of the Case: Severely curved canals, calcified canals, or unusual anatomy can make a procedure more challenging and thus more expensive.
- Technology Used: Practices utilizing advanced technologies like dental microscopes, CBCT scans, or laser disinfection may charge more.
- Sedation Fees: If you opt for or require sedation, these costs are typically separate from the root canal fee. Oral sedation might add $100-$300, while IV sedation can add $400-$800+.
Cost-Saving Tips
- Comparison Shop: If you have multiple options, get quotes from different dentists, especially for extensive work.
- Dental Schools: Many dental schools offer high-quality treatment at reduced rates, performed by students under the supervision of experienced faculty.
- Community Clinics: Some non-profit or government-subsidized clinics offer dental care on a sliding scale based on income.
- Preventative Care: The most effective cost-saving measure is prevention. Regular check-ups and good oral hygiene can prevent the need for expensive procedures like root canals.
- Maximize Insurance Benefits: Understand your plan's maximums and deductibles. If you're close to your annual maximum at the end of the year, coordinate with your dentist to complete essential treatment before the benefits reset.
Frequently Asked Questions
How painful is a root canal procedure?
Modern root canal procedures are generally not painful during the treatment itself. Dentists use effective local anesthesia to completely numb the tooth and surrounding area, so you should feel no pain, only pressure. The reputation for pain often comes from the severe pain of the infection before treatment, or older techniques.
Will I experience pain after a root canal?
It's common to experience some mild discomfort or tenderness for a few days after a root canal, especially when the local anesthesia wears off. This is typically manageable with over-the-counter pain relievers like ibuprofen or naproxen. If you experience severe pain, swelling, or pressure that worsens, contact your dentist.
How long does a root canal take?
A standard root canal procedure typically takes between 60 to 90 minutes for a front tooth or premolar, and 90 minutes to 2 hours for a molar due to its multiple canals. Complex cases or retreated teeth may take longer. Sometimes, the procedure is split into two appointments.
What are the alternatives to a root canal?
The primary alternative to a root canal for an infected tooth is tooth extraction. While extraction removes the source of the infection, it results in permanent tooth loss, which can lead to further dental issues and often requires replacement with a bridge, dental implant, or partial denture, which are generally more costly long-term.
Why do I need a crown after a root canal?
A crown is almost always recommended after a root canal, especially for back teeth, because the procedure can weaken the tooth structure. The access hole made, along with the removal of internal tooth structure, makes the tooth more susceptible to fracture. A crown provides strength, protection, and restores the tooth's chewing function and appearance.
Can a root canal fail?
While root canals have a very high success rate (over 95%), they can sometimes fail. This can happen if the initial infection wasn't fully cleared, if new bacteria enter the tooth, if the tooth suffers a new fracture, or if the tooth is not properly restored with a crown. In such cases, a retreatment or apicoectomy may be options.
How long does a root canal last?
With proper care and a permanent restoration (usually a crown), a root-canaled tooth can last a lifetime. Its longevity depends on good oral hygiene, regular dental check-ups, and avoiding habits like chewing on hard objects.
Is a root canal covered by dental insurance?
Most dental insurance plans do provide coverage for root canal treatment, typically categorizing it as a major procedure. Coverage usually ranges from 50% to 80% after your deductible is met, up to your annual maximum benefit. It's crucial to check with your specific insurance provider for details.
Can I go to work or school after a root canal?
If you only received local anesthesia and feel well, you can generally return to work or school after a root canal. However, avoid strenuous activity or chewing on the treated side for a few hours. If you received any form of sedation, you should take the rest of the day off and avoid activities requiring focus.
When to See a Dentist
Recognizing when to seek dental care is crucial for preventing severe complications and preserving your oral health.
Clear Warning Signs for Immediate Attention (Emergency)
These symptoms indicate a potentially serious issue requiring prompt evaluation by a dentist, often within 24 hours:
- Severe, persistent toothache: Especially if it's throbbing, keeps you awake at night, or doesn't respond to over-the-counter pain relievers. This often signals a deep infection.
- Swelling in your gums, face, or jaw: This is a strong indicator of an abscess or spreading infection, which can be dangerous if left untreated.
- A "pimple" or boil on your gums (fistula): This indicates an infection draining pus and needs immediate attention.
- Pain when chewing or biting down that worsens: Particularly if accompanied by sensitivity to hot or cold.
- Traumatic injury to a tooth: If a tooth is chipped, cracked, knocked loose, or knocked out due due to an accident, see your dentist as soon as possible.
- Fever accompanied by tooth pain or swelling: This suggests a systemic infection that needs urgent medical and dental intervention.
Red Flags vs. Routine Care Guidance
- Red Flag (Seek prompt care): Lingering sensitivity to hot or cold (lasting more than 30 seconds after the stimulus is removed) suggests pulp damage.
- Routine Care (Schedule an appointment soon): Mild, fleeting sensitivity to hot or cold, or occasional mild tooth pain that comes and goes, might indicate a small cavity or gum recession, which should be addressed before it worsens.
- Red Flag (Seek prompt care): Dark discoloration of a tooth, even without pain, can mean the pulp is dying and requires investigation.
- Routine Care (Regular check-ups): Regular dental cleanings and examinations are essential preventative measures to catch problems like small cavities before they become root canal issues. The ADA recommends at least annual check-ups, and often semi-annual for most adults.
Emergency vs. Scheduled Appointment Guidance
- Emergency: If you have severe pain, significant swelling, signs of an abscess, or a knocked-out tooth, seek emergency dental care immediately. Many dental offices reserve slots for emergencies, or you may need to visit an urgent care dental clinic or emergency room if your dentist is unavailable.
- Scheduled Appointment: For less urgent symptoms like mild sensitivity, a small chip, or a filling that feels rough, schedule a regular appointment at your earliest convenience. Do not wait for these issues to escalate into emergencies.
Pro Tip: Trust your instincts. If something doesn't feel right with your teeth or gums, it's always better to consult your dentist. Early intervention is key to preventing more extensive and costly treatments like root canals.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Stop Throbbing Pain After Root Canal
Undergoing a root canal procedure is often a necessary step to save a tooth severely damaged by decay or infection, preventing further complications and excruciating pain. While the procedure itself is performed under local anesthesia to ensure comfort, it's common for patients to experience some le
February 22, 2026
Root Canal After Care: Complete Guide
A root canal procedure can be a tooth-saving treatment, offering relief from pain and preventing further infection. However, the success and longevity of this crucial dental intervention heavily rely on diligent root canal after care. Neglecting post-treatment instructions can lead to complicati
February 22, 2026
Is a Root Canal Painful
When facing the prospect of a root canal, one of the most common and immediate questions that comes to mind is: is a root canal painful? It's a valid concern, stemming from outdated perceptions and anecdotal stories. However, modern root canal therapy is a highly effective and generally comforta
February 22, 2026
How Much Are Root Canals
Experiencing a persistent toothache can be one of the most unsettling dental issues, often signaling a problem deep within the tooth’s core. For many, this leads to the dreaded question: "Do I need a root canal?" And immediately following that, how much are root canals going to cost me? It's a v
February 22, 2026