Pulpotomy: Complete Guide
Key Takeaways
- Experiencing a toothache can be a daunting experience, especially when it affects a child. You might wonder if it’s a simple cavity or something more serious, potentially leading to questions like "does a root canal hurt?" or "what are my options?" When decay or trauma reaches the inner, vital tissu
Pulpotomy: Complete Guide
Experiencing a toothache can be a daunting experience, especially when it affects a child. You might wonder if it’s a simple cavity or something more serious, potentially leading to questions like "does a root canal hurt?" or "what are my options?" When decay or trauma reaches the inner, vital tissue of a tooth – known as the dental pulp – timely intervention is critical to save the tooth. One such intervention, particularly common in pediatric dentistry but also applicable in specific adult cases, is a pulpotomy. This procedure aims to preserve the healthy portion of the tooth's pulp, preventing the need for more extensive treatments and helping to maintain the natural integrity of your smile.

A pulpotomy is a specialized dental procedure within the field of endodoncia (the study and treatment of the dental pulp), designed to remove only the infected or inflamed part of the pulp, primarily located in the crown of the tooth. By addressing this issue early, dentists can often prevent the infection from spreading to the root canals, thereby avoiding a full root canal treatment or even tooth extraction. This article will serve as your comprehensive guide to understanding pulpotomy, covering everything from what it is and why it's performed to costs, recovery, and prevention, ensuring you have all the information needed to make informed decisions about your dental health.
Key Takeaways:
- A pulpotomy is a procedure to remove the inflamed or infected coronal (crown) portion of the dental pulp, aiming to preserve the vital root pulp.
- It is most commonly performed on primary (baby) teeth, but can also be used on young permanent teeth with immature roots.
- The procedure typically takes 30-60 minutes per tooth and is done under local anesthesia.
- Costs in the US range from $200 to $600 for primary teeth and $400 to $800+ for permanent teeth, often covered partially by dental insurance.
- Recovery is usually quick, with mild discomfort manageable with over-the-counter pain relievers, and the tooth is often restored with a stainless steel crown (for children) or permanent crown/filling.
- Success rates are high, especially for primary teeth, enabling the tooth to be retained until its natural exfoliation or continued development.
- Prevention hinges on excellent oral hygiene, regular dental check-ups, and prompt treatment of cavities or trauma.
What It Is / Overview
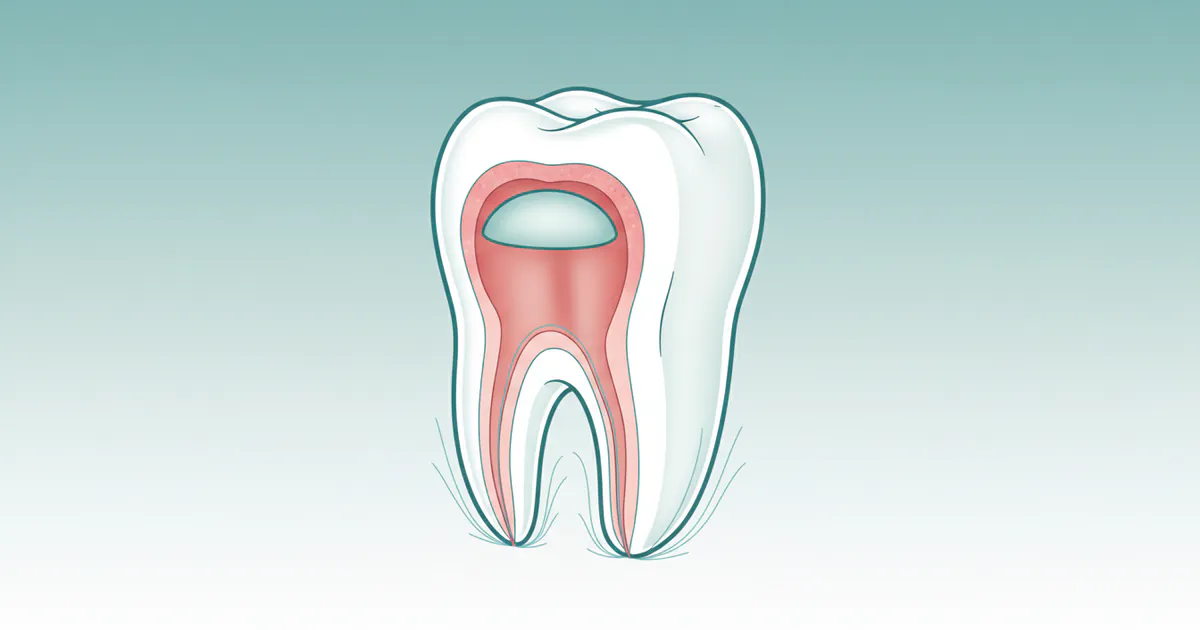
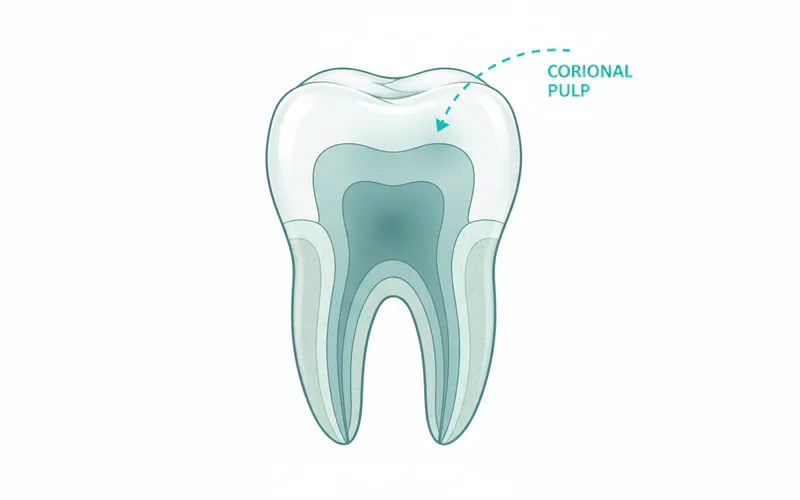
At its core, a pulpotomy is a conservative dental procedure focused on preserving the vitality of a tooth that has experienced pulp inflammation or infection. To truly understand a pulpotomy, it's essential to first grasp the anatomy of a tooth. Inside every tooth lies the dental pulp – a soft tissue containing nerves, blood vessels, and connective tissue. This pulp extends from the crown of the tooth (the visible part above the gum line) down into the roots, through narrow channels called root canals. The part of the pulp within the crown is called the coronal pulp, and the part within the roots is the radicular pulp.
A pulpotomy specifically targets the coronal pulp. When deep decay or trauma causes inflammation or infection in this coronal portion, a pulpotomy is performed to remove only the affected tissue while leaving the healthy, vital radicular pulp intact. This approach is distinct from a pulpectomy, where the entire pulp (both coronal and radicular) is removed, and from a full root canal treatment (RCT), which typically involves cleaning and filling the entire root canal system in permanent teeth.
The primary goal of a pulpotomy is to:
- Eliminate infection and inflammation: By removing the diseased coronal pulp.
- Preserve vitality: To keep the radicular pulp healthy and functional.
- Maintain tooth function: Allow the tooth to remain in the arch until its natural exfoliation (for primary teeth) or complete root development (for young permanent teeth).
- Prevent further spread of infection: Stopping bacteria from reaching the periapical (around the root tip) tissues, which could lead to abscesses or systemic infection.
This procedure is a vital part of endodoncia, the branch of dentistry dealing with the prevention, diagnosis, and treatment of diseases and injuries of the dental pulp. Often referred to simply as "pulp therapy," it is a common procedure, especially in pediatric dentistry, where preserving primary teeth is crucial for guiding the eruption of permanent teeth, maintaining space, and ensuring proper chewing and speech development.
Types / Variations
While the core principle of a pulpotomy remains consistent – removing diseased coronal pulp – there are different approaches and variations, primarily influenced by the extent of pulp involvement and the tooth type (primary vs. permanent).
1. Coronal Pulpotomy (Traditional Pulpotomy)
This is the most common type and what is generally referred to when discussing a pulpotomy. It involves:
- Accessing the pulp chamber.
- Removing all the coronal pulp tissue.
- Achieving hemostasis (stopping bleeding).
- Placing a medicament over the remaining radicular pulp stumps to promote healing and maintain vitality.
- Sealing the tooth with a restorative material.
Materials Used in Coronal Pulpotomies:
- Formocresol: Historically a widely used medicament, especially in pediatric dentistry. It acts as a fixative and antibacterial agent. However, due to concerns about its potential toxicity and carcinogenicity, its use has significantly declined, and it's being replaced by safer alternatives.
- Mineral Trioxide Aggregate (MTA): Considered the gold standard by many practitioners today. MTA is a biocompatible cement that promotes healing and hard tissue formation (dentin bridge) over the vital pulp. It has excellent sealing properties and a high success rate.
- Calcium Hydroxide: Another common material that stimulates dentin bridge formation. While effective, it generally has a lower success rate than MTA, especially in cases of significant inflammation.
- Biodentine: A newer calcium silicate-based cement similar to MTA, offering excellent biocompatibility, sealing ability, and dentinogenic properties. It's often used as a dentin substitute and for pulp capping.
- Ferric Sulfate: Used for its hemostatic properties, it helps control bleeding from the radicular pulp stumps before a restorative material is placed. Its long-term pulpal effects are debated compared to materials that promote healing.
2. Partial Pulpotomy (Cvek Pulpotomy)
Also known as a Cvek pulpotomy, this procedure is even more conservative than a traditional coronal pulpotomy. It is specifically indicated when:
- Only a small, localized portion of the coronal pulp is exposed due to trauma or a very small carious exposure.
- The exposed pulp tissue is only superficially inflamed, and the deeper pulp is deemed healthy and vital.
- The goal is to remove only the superficial, necrotic, or irreversibly inflamed pulp tissue (usually 1-3mm deep) directly at the exposure site.
- A biocompatible material (like MTA or Calcium Hydroxide) is placed directly over the remaining healthy pulp.
Partial pulpotomies are often performed on young permanent teeth where it's critical to preserve as much vital pulp as possible to allow for continued root development (apexogenesis). This procedure has a very high success rate when properly indicated.
3. Deep Caries Management / Indirect Pulp Cap
While not strictly a pulpotomy, deep caries management (indirect pulp cap) is a related, even more conservative approach to pulp preservation. In this technique, decay is removed, but a thin layer of demineralized dentin directly overlying the pulp is intentionally left behind to avoid pulp exposure. A medicament (often calcium hydroxide or MTA) is then placed over this thin dentin layer, followed by a permanent restoration. The goal is to remineralize the affected dentin and stimulate secondary dentin formation, thereby protecting the pulp without direct pulp exposure. This is typically done when there is no irreversible pulpitis.
Comparison of Pulp Preservation Techniques
| Feature | Indirect Pulp Cap | Partial Pulpotomy (Cvek) | Coronal Pulpotomy | Pulpectomy | Root Canal Treatment (RCT) |
|---|---|---|---|---|---|
| Pulp Condition | Reversible pulpitis, no pulp exposure | Reversible pulpitis, small mechanical/traumatic exposure | Reversible/Irreversible pulpitis, carious/traumatic exposure (coronal) | Irreversible pulpitis, necrosis (total pulp) | Irreversible pulpitis, necrosis (total pulp) |
| Pulp Removal | None (decay near pulp left) | Superficial (1-3mm) inflamed/exposed pulp | Entire coronal pulp | Entire coronal & radicular pulp (primary teeth) | Entire coronal & radicular pulp (permanent teeth) |
| Pulp Preservation | Maximize, no direct exposure | Maximize, healthy deep pulp retained | Radicular pulp retained | None (entire pulp removed) | None (entire pulp removed) |
| Tooth Type | Primary & Permanent | Young Permanent, sometimes Primary | Primary (common), Young Permanent (select cases) | Primary (common) | Permanent (common), Young Permanent |
| Goal | Prevent exposure, stimulate repair | Maintain vitality, allow root development | Maintain vitality, allow natural exfoliation/root development | Retain tooth, prevent infection (primary teeth) | Retain tooth, prevent infection (permanent teeth) |
| Restoration | Filling/Crown | Filling/Crown | Crown (primary), Filling/Crown (permanent) | Crown (primary) | Crown (permanent) |
Causes / Why It Happens
Understanding why a pulpotomy becomes necessary often boils down to two primary culprits: deep dental decay and trauma. Both can compromise the protective layers of a tooth and expose the delicate dental pulp to bacteria and irritants, leading to inflammation or infection.
1. Deep Dental Caries (Cavities)
This is by far the most common reason for a pulpotomy, particularly in primary teeth.
- Progressive Decay: Untreated cavities start on the enamel, then penetrate the dentin. If allowed to progress further, the bacteria and their byproducts eventually reach the pulp chamber.
- Pulp Exposure: As the decay gets closer to the pulp, it causes inflammation (pulpitis). If the decay directly penetrates the pulp chamber, it creates a pathway for bacteria to enter, leading to infection.
- Irreversible Pulpitis: At this stage, the inflammation is severe and the pulp cannot heal on its own. While the radicular pulp might still be healthy and vital, the coronal pulp is compromised. This is a key indication for a pulpotomy – to remove the irreversibly inflamed coronal pulp and save the remaining vital root pulp.
2. Dental Trauma
Injuries to the mouth and teeth, common in children and athletes, can also necessitate a pulpotomy.
- Fractured Teeth: A blow to the mouth can cause a tooth to fracture. If the fracture extends deep enough to expose the pulp chamber, bacteria can enter, leading to inflammation or infection.
- Concussive Injuries: Even without a visible fracture, a severe impact can damage the blood supply to the pulp or cause internal inflammation that progresses to necrosis (pulp death). While less directly linked to pulpotomy indications, trauma can lead to pulp complications that may require pulp therapy.
- Attrition/Abrasion: While less common for acute pulpal exposure, severe wear from grinding (bruxism) or aggressive brushing can, over a long period, wear down enamel and dentin, eventually exposing the pulp.
3. Iatrogenic Exposure
This refers to an accidental pulp exposure during a dental procedure, most commonly during cavity preparation. If a dentist is removing a deep cavity and accidentally exposes the pulp, a pulpotomy (or partial pulpotomy, depending on the exposure size and pulp health) might be performed immediately to prevent future infection.
Reversible vs. Irreversible Pulpitis: The Diagnostic Key
The decision to perform a pulpotomy hinges on the dentist's assessment of the pulp's health, specifically differentiating between reversible and irreversible pulpitis:
- Reversible Pulpitis: Mild inflammation where the pulp can recover if the irritant (e.g., shallow decay, temporary cold sensitivity) is removed. Symptoms are usually mild and short-lived. A simple filling or indirect pulp cap might suffice.
- Irreversible Pulpitis: Severe inflammation where the pulp cannot heal and will eventually die if untreated. Symptoms are often characterized by spontaneous pain, prolonged sensitivity to hot/cold, and pain that lingers even after the stimulus is removed. In these cases, especially when affecting the coronal pulp primarily, a pulpotomy is indicated to save the rest of the tooth. If the entire pulp (including radicular) is irreversibly inflamed or necrotic, then a pulpectomy or root canal treatment would be necessary.
Pro Tip: Early detection of cavities and addressing dental trauma promptly are your best defenses against needing a pulpotomy. Regular dental check-ups allow your dentist to catch decay before it becomes a significant problem.
Signs and Symptoms
Recognizing the signs and symptoms that might indicate a need for a pulpotomy is crucial for timely intervention. While children may not always articulate their discomfort clearly, attentive parents and individuals can look for these common indicators:
1. Pain
- Spontaneous Pain: Pain that occurs without any apparent stimulus, often waking a child up at night. This is a strong indicator of irreversible pulpitis.
- Prolonged Sensitivity: Lingering pain after exposure to hot or cold temperatures, lasting for more than a few seconds. This suggests significant inflammation.
- Pain with Chewing or Biting: Pressure on the tooth can exacerbate discomfort, indicating inflammation reaching the ligament supporting the tooth.
- Referred Pain: Pain that radiates to other teeth, the jaw, or even the ear, making it difficult to pinpoint the exact source.
2. Swelling
- Localized Swelling: Swelling around the affected tooth, on the gum line, or even in the facial region, indicates an infection that may have spread beyond the tooth.
- Pimple-like Bump (Fistula/Abscess): A small, pus-filled bump on the gums near the tooth, which may intermittently drain. This is a sign of an active infection (dental abscess) trying to find an exit point.
3. Tenderness
- Tenderness to Touch: The tooth or surrounding gum tissue may be sensitive when touched or pressed.
- Sensitivity to Percussion: Tapping on the tooth can elicit pain.
4. Discoloration
- Tooth Discoloration: The affected tooth may appear darker or grayish, especially after trauma. This can signify internal bleeding within the pulp or necrosis (pulp death).
5. Other Symptoms
- Fever: In cases of severe infection or abscess, a fever may be present.
- Bad Taste/Odor: Persistent bad breath or a foul taste in the mouth can be indicative of infection or draining pus.
- Difficulty Eating: Due to pain or swelling, a child might avoid chewing on the affected side.
It's important to note that sometimes, particularly in children, symptoms can be subtle or intermittent. A child might simply refuse to eat certain foods, be irritable, or have difficulty sleeping. For adults, deep decay might initially only cause minor sensitivity before progressing to more severe, spontaneous pain.
When to See a Dentist: Any persistent tooth pain, sensitivity, swelling, or changes in tooth color warrants a prompt visit to the dentist. Early diagnosis is key to successful treatment and preventing more severe complications.
Treatment Options
When the dental pulp is compromised, a pulpotomy is one of several treatment options available, each suited for different degrees of pulp involvement and tooth types. The decision hinges on a thorough diagnosis, including clinical examination, X-rays, and pulp vitality tests.
1. Pulpotomy
- Indication: Irreversible inflammation or infection of the coronal pulp, but with a healthy, vital radicular pulp. Often performed on primary teeth, and sometimes on young permanent teeth with immature roots where full root development is still possible.
- Pros:
- Tooth Preservation: Saves the tooth from extraction.
- Space Maintenance (Primary Teeth): Keeps the baby tooth until the permanent tooth is ready to erupt, preventing adjacent teeth from drifting and maintaining proper alignment.
- Less Invasive: More conservative than a pulpectomy or root canal.
- Allows Root Development (Young Permanent Teeth): Preserves the vital root pulp, allowing the root to fully form and strengthen.
- Cons:
- Risk of Failure: Though generally high, there's a chance the radicular pulp may still become necrotic, requiring further treatment.
- Requires Definitive Restoration: The tooth must be sealed with a strong restoration (often a stainless steel crown in children, or a permanent crown/filling in adults) immediately after to protect the treated pulp.
2. Pulpectomy
- Indication: When the entire pulp (both coronal and radicular) is irreversibly inflamed or necrotic. This procedure is primarily performed on primary teeth.
- Pros:
- Saves Primary Tooth: Allows the primary tooth to be retained until natural exfoliation, preventing premature space loss.
- Eliminates Infection: Removes all infected pulp tissue.
- Cons:
- More Invasive: Involves cleaning out the entire root canal system of a primary tooth.
- Technical Challenges: Primary teeth have complex root canal anatomy.
- Not for Permanent Teeth: For permanent teeth, this is essentially a root canal treatment.
3. Root Canal Treatment (RCT) / Endodontic Therapy
- Indication: Irreversible pulpitis or pulp necrosis in permanent teeth, where the entire pulp (coronal and radicular) is diseased.
- Pros:
- High Success Rate: Extremely effective at saving permanent teeth.
- Long-term Solution: With proper restoration, a root canal-treated tooth can last a lifetime.
- Eliminates Pain & Infection: Resolves the source of pain and prevents further infection.
- Cons:
- More Invasive and Complex: Involves cleaning, shaping, and filling the entire root canal system.
- Time-Consuming: May require multiple appointments.
- Higher Cost: Generally more expensive than a pulpotomy.
- Requires Crown: Most root canal treated posterior teeth require a crown for protection against fracture.
- Self-correction: Addressing "does a root canal hurt" directly: While the procedure itself is done under local anesthesia and should be painless, some mild discomfort post-procedure is common. The pain associated with the infection before a root canal is typically far worse than any post-treatment soreness.
4. Tooth Extraction
- Indication: When a tooth is so severely damaged or infected that it cannot be saved by any other means, or if other treatments are not feasible/desired.
- Pros:
- Immediate Pain Relief: Removes the source of infection.
- Less Costly (Initially): Cheapest option upfront compared to restorative treatments.
- Cons:
- Loss of Natural Tooth: Can lead to chewing difficulties, speech problems, and aesthetic concerns.
- Space Loss: Adjacent teeth may shift, affecting bite alignment.
- Future Costs: Often requires subsequent replacement (bridge, implant) which is far more expensive than preserving the natural tooth.
Treatment Option Comparison Table
| Treatment | Tooth Type | Pulp Condition | Key Feature | Cost Range (US) | Recovery Time | Success Rate |
|---|---|---|---|---|---|---|
| Pulpotomy | Primary, Young Permanent | Coronal pulp inflamed/infected, radicular healthy | Removes coronal pulp, preserves root pulp | $200 - $800 | Days | High (85-95%) |
| Pulpectomy | Primary | Entire pulp inflamed/necrotic | Removes all pulp in primary tooth | $300 - $700 | Days | Moderate-High |
| Root Canal (RCT) | Permanent | Entire pulp inflamed/necrotic | Removes all pulp, cleans/fills root canals | $700 - $2,000+ | Days to Weeks | High (90-95%) |
| Extraction | Any | Unrestorable, severe infection | Complete removal of tooth | $75 - $400 | Days to Weeks | N/A (tooth removed) |
Step-by-Step Process
Undergoing a pulpotomy can feel less intimidating when you understand each step involved. The procedure is typically straightforward and performed in a single visit.
1. Diagnosis and Treatment Planning
- Clinical Examination: The dentist will examine the affected tooth, surrounding gums, and ask about symptoms (pain, sensitivity).
- Radiographs (X-rays): X-rays are essential to assess the depth of decay, the extent of pulp involvement, the condition of the root tips, and to rule out any abscesses.
- Pulp Vitality Tests: In some cases, tests like cold or electric pulp tests might be performed (more common for permanent teeth) to gauge the pulp's health and responsiveness.
- Informed Consent: The dentist will explain the procedure, its benefits, risks, and alternatives, obtaining your (or your child's parent/guardian's) informed consent.
2. Anesthesia
- Local Anesthesia: The area around the tooth will be numbed using a local anesthetic. This ensures you or your child will not feel any pain during the procedure. The numbing sensation usually lasts for a few hours after the procedure.
3. Isolation
- Rubber Dam Placement: A rubber dam (a thin sheet of latex or non-latex material) is typically placed around the tooth. This isolates the tooth from the rest of the mouth, keeping it dry and free from saliva and bacteria, which is critical for preventing further contamination and ensuring the success of the procedure.
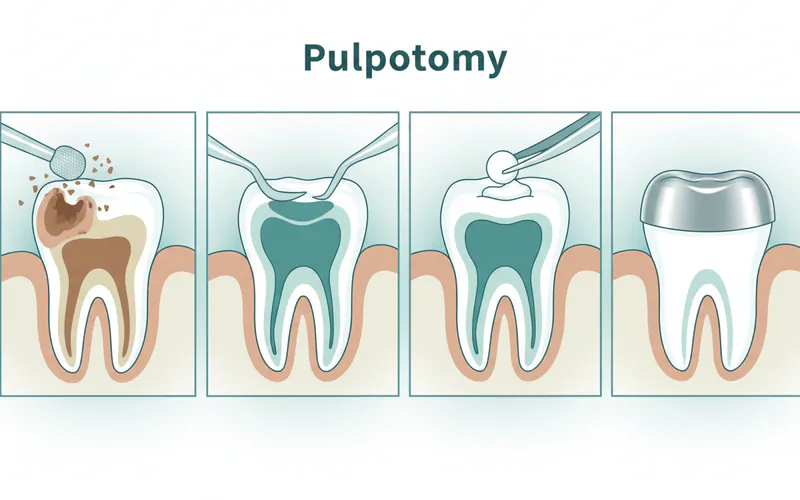
4. Decay Removal and Pulp Chamber Access
- Caries Removal: The dentist will use a dental drill to carefully remove all decayed tooth structure.
- Pulp Chamber Access: Once the decay is removed, an opening is created to access the pulp chamber located in the center of the tooth's crown.
5. Coronal Pulp Removal and Hemostasis
- Coronal Pulp Removal: Specialized instruments (usually a small, sterile dental spoon excavator or high-speed handpiece) are used to carefully remove the entire coronal portion of the pulp tissue from the pulp chamber.
- Hemostasis: After removing the coronal pulp, the dentist will control any bleeding from the remaining radicular pulp stumps. This is often achieved by applying gentle pressure with a sterile cotton pellet or by using a hemostatic agent like ferric sulfate. It's crucial for the bleeding to stop to ensure proper healing.
6. Placement of Medicament
- Pulp Dressing: Once hemostasis is achieved, a biocompatible medicament (such as MTA, Biodentine, or Calcium Hydroxide) is placed directly over the vital radicular pulp stumps. This material promotes healing, stimulates the formation of a dentin bridge, and helps maintain the vitality of the remaining pulp.
7. Final Restoration
- Base Material: A suitable base material is placed over the medicament to seal the pulp chamber.
- Definitive Restoration: The tooth is then permanently restored.
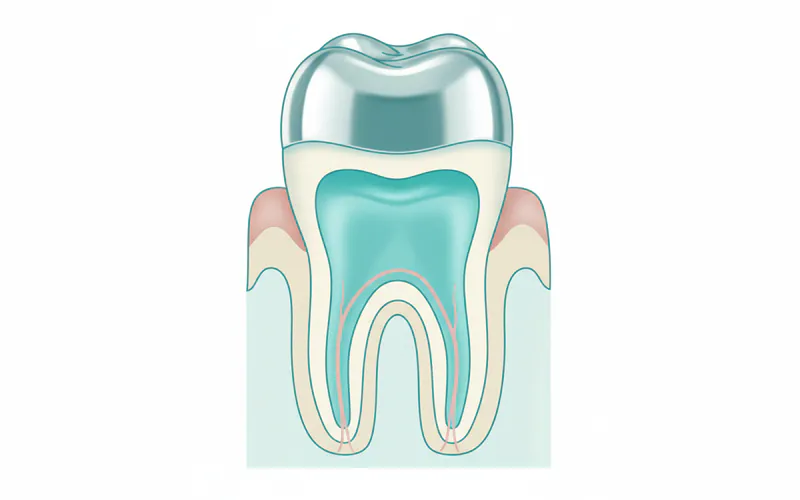
- For Primary Teeth: A stainless steel crown is the preferred restoration after a pulpotomy due to its durability and ability to protect the compromised tooth until it naturally exfoliates.
- For Permanent Teeth: A composite resin filling or a dental crown (porcelain, zirconia, etc.) will be placed, depending on the extent of tooth structure lost and the bite forces.
The entire procedure typically takes 30 to 60 minutes, depending on the tooth's complexity and the patient's cooperation.
Cost and Insurance
The cost of a pulpotomy in the US can vary significantly based on several factors, including the type of tooth (primary vs. permanent), the specific materials used, the complexity of the case, the dentist's fees, and geographic location.
Average US Pulpotomy Costs (Without Insurance)
| Category | Low Range | Mid Range | High Range |
|---|---|---|---|
| Primary (Baby) Tooth | $200 - $350 | $350 - $500 | $500 - $600 |
| Permanent Tooth | $400 - $600 | $600 - $750 | $750 - $900+ |
| Add-on: Stainless Steel Crown (Primary) | $150 - $250 | $250 - $400 | $400 - $500+ |
| Add-on: Permanent Crown (Composite/Porcelain) | $800 - $1,500 | $1,500 - $2,500 | $2,500 - $3,500+ |
Key Cost Considerations:
- Geographic Location: Costs are generally higher in metropolitan areas and on the coasts (e.g., New York, California) compared to rural areas or the Midwest.
- Dentist's Fees: Specialist pediatric dentists or endodontists may charge slightly more than a general dentist.
- Materials Used: Advanced biocompatible materials like MTA or Biodentine may incur higher costs than older materials like Formocresol.
- Associated Procedures: The cost of the final restoration (crown or large filling) is a separate charge and typically adds significantly to the total treatment expense, especially for permanent teeth. Diagnostic X-rays and exams are also separate fees.
Insurance Coverage
Most dental insurance plans in the US offer some level of coverage for pulpotomies, as it's considered a restorative or basic procedure aimed at preserving the natural tooth.
- Typical Coverage: Insurance plans often cover 50% to 80% of the procedure cost, after you've met your deductible.
- CDT Codes: Dental procedures are identified by Current Dental Terminology (CDT) codes.
- D3220: Pulpotomy - therapeutic, for maintaining vitality of pulp of primary tooth (excluding final restoration).
- D3221: Pulpal debridement, primary and permanent teeth. (This may be used for initial pulp treatment but D3220 is more specific for pulpotomy).
- D3310: Endodontic therapy, anterior tooth (for permanent tooth root canal).
- D2930/D2931: Prefabricated Stainless Steel Crown - primary/permanent (for the crown restoration).
- Deductibles and Annual Maximums: Be aware of your plan's deductible (the amount you pay out-of-pocket before insurance kicks in) and annual maximum (the total amount your insurance will pay in a year). A pulpotomy and crown might push you close to or over your annual maximum, especially if other dental work is needed.
- Pre-authorization: For more expensive procedures or combined treatments (pulpotomy + crown), your dentist may submit a pre-treatment estimate to your insurance company to determine your exact out-of-pocket expenses beforehand. This is highly recommended.
Payment Plans and Financing Options
For those without insurance or with high out-of-pocket costs, several options can help manage expenses:
- Dental Savings Plans: These are not insurance but membership programs that offer discounted rates on dental services from participating providers.
- Payment Plans: Many dental offices offer in-house payment plans, allowing you to pay for treatment in installments.
- Third-Party Financing: Services like CareCredit or LendingClub offer specialized healthcare credit cards with low or no-interest promotional periods, making extensive dental work more manageable.
- Health Savings Accounts (HSAs) or Flexible Spending Accounts (FSAs): If you have an HSA or FSA, you can use these tax-advantaged accounts to pay for dental expenses.
Pro Tip: Always discuss costs and insurance coverage with your dental office's administrative staff before treatment. They can provide a detailed estimate and help you understand your insurance benefits.
Recovery and Aftercare
After a pulpotomy, most patients experience a relatively smooth recovery. Understanding what to expect and following aftercare instructions are crucial for the success of the procedure and your comfort.
Immediate Post-Procedure
- Numbness: The local anesthetic will wear off within a few hours. Until then, it's important to be careful not to bite your tongue, cheek, or lip, especially for children.
- Mild Discomfort: It's common to experience some mild discomfort or sensitivity around the treated tooth and gums once the numbness fades. This is usually manageable with over-the-counter pain relievers.
Pain Management
- Over-the-Counter Pain Relievers: Ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are usually sufficient to manage any post-operative pain. Follow dosage instructions based on age and weight, especially for children.
- Prescription Pain Relievers: Rarely needed for a pulpotomy. If pain is severe or persistent, contact your dentist.
Diet and Eating
- Soft Foods: Stick to soft foods for the first 24-48 hours. Avoid hard, crunchy, or sticky foods that could dislodge the temporary filling (if applicable) or put excessive pressure on the newly restored tooth.
- Avoid Chewing on the Treated Side: Until the final restoration is firmly in place and symptoms subside, try to chew on the opposite side of your mouth.
- Temperature Sensitivity: You might experience temporary sensitivity to hot or cold foods/drinks. This should diminish over time.
Oral Hygiene
- Gentle Brushing: Continue to brush and floss gently around the treated tooth. Good oral hygiene is vital to prevent new decay or gum irritation.
- Saltwater Rinses: Rinsing with warm salt water (1/2 teaspoon salt in 8 ounces of warm water) several times a day can help reduce swelling and promote healing of the gum tissue around the tooth.
What to Watch For (When to Call Your Dentist)
While pulpotomies have a high success rate, complications can occur. Contact your dentist immediately if you experience any of the following:
- Severe or Worsening Pain: Pain that is not controlled by over-the-counter medication or that increases in intensity.
- Persistent Swelling: Swelling in the face, gums, or lymph nodes that doesn't subside or worsens.
- Fever: A sign of spreading infection.
- Allergic Reaction: To medication (rash, itching, difficulty breathing).
- Loss of Restoration: If the filling or crown comes off, the tooth is no longer protected, and the pulp could become re-infected.

Long-Term Outlook
For primary teeth treated with a pulpotomy and stainless steel crown, the goal is to retain the tooth until it naturally exfoliates (falls out) to make way for the permanent tooth. Regular dental check-ups will monitor the tooth's condition and the eruption of the permanent successor.
For permanent teeth, a pulpotomy aims to preserve vitality and allow for complete root formation. These teeth will require diligent long-term care, including regular dental visits and excellent home hygiene, similar to any other tooth. The treated tooth should then function normally for many years.
Prevention
Preventing the conditions that necessitate a pulpotomy primarily involves maintaining excellent oral hygiene and adopting healthy lifestyle habits. Many of these recommendations align with general dental health guidelines from organizations like the American Dental Association (ADA).
1. Excellent Oral Hygiene
- Brush Twice Daily: Brush your teeth for at least two minutes, twice a day, using a fluoride toothpaste. Ensure all tooth surfaces are cleaned, especially around the gum line and chewing surfaces.
- Floss Daily: Floss once a day to remove plaque and food particles from between teeth and under the gum line, where toothbrushes can't reach. This prevents interproximal (between teeth) cavities that can silently progress.
- Antiseptic Mouthwash: Consider using an ADA-accepted antiseptic mouthwash to reduce bacteria in the mouth, especially if you're prone to gingivitis or high caries risk.
2. Regular Dental Check-ups and Cleanings
- Bi-annual Visits: Visit your dentist every six months for a professional cleaning and check-up. This allows the dentist to:
- Identify and treat cavities when they are small, before they reach the pulp.
- Monitor the health of your teeth and gums.
- Take X-rays to detect hidden decay between teeth or under existing restorations.
- Early Intervention: Catching decay early is the most effective way to prevent the need for a pulpotomy or more extensive procedures like root canals.
3. Balanced Diet
- Limit Sugary Foods and Drinks: Frequent consumption of sugary snacks, sodas, and juices feeds the bacteria that cause cavities. Reduce your intake and rinse your mouth with water after consuming them.
- Eat Nutrient-Rich Foods: A diet rich in fruits, vegetables, lean proteins, and dairy products (for calcium) supports overall oral health.
4. Protect Your Teeth
- Mouthguards for Sports: If you or your child participate in contact sports, a custom-fitted mouthguard is essential to protect teeth from trauma and fractures that could expose the pulp.
- Address Bruxism (Teeth Grinding): If you grind your teeth, especially at night, a nightguard can protect them from excessive wear and potential fractures.
- Avoid Using Teeth as Tools: Do not use your teeth to open packages, cut strings, or bite on hard objects (ice, unpopped popcorn kernels), as this can cause fractures.
5. Fluoride Protection
- Fluoridated Water: If your community water is fluoridated, drink it regularly. Fluoride strengthens tooth enamel, making it more resistant to decay.
- Topical Fluoride: Your dentist may recommend professional fluoride treatments, especially for children or adults at high risk of cavities.
Pro Tip: Teach children good oral hygiene habits from a very young age. Supervise their brushing until they are about 7-8 years old to ensure thorough cleaning. Dental sealants on permanent molars are also highly effective at preventing decay in susceptible grooves.
Risks and Complications
While a pulpotomy is generally a safe and effective procedure, like any medical intervention, it carries potential risks and complications. It's important to be aware of these, though they are relatively uncommon when performed correctly.
1. Treatment Failure
- Pulp Necrosis: Despite the removal of the coronal pulp, the remaining radicular pulp may still become irreversibly inflamed or die (necrose). This can happen if the initial infection was more extensive than diagnosed, if bacteria leaked in due to a compromised seal, or if the pulp tissue simply didn't heal properly.
- Persistent Infection: The infection may persist or recur, leading to symptoms such as pain, swelling, or the formation of an abscess (a pus-filled pocket).
- Signs of Failure: Increased pain, swelling, a "pimple" on the gum, or an X-ray showing signs of infection around the root tips are indicators of failure.
2. Need for Further Treatment
- If a pulpotomy fails, the tooth will likely require a more extensive procedure:
- Pulpectomy: For primary teeth, if the entire pulp becomes infected.
- Root Canal Treatment (RCT): For permanent teeth, if the entire pulp becomes infected.
- Extraction: If the tooth cannot be saved by further pulp therapy.
3. Discoloration of the Tooth
- The treated tooth, especially a permanent tooth, may sometimes darken slightly over time. This can be due to residual blood products within the dentin tubules or the medicament used. While not a health risk, it can be an aesthetic concern.
4. Resorption of the Root
- In some primary teeth, particularly if there's chronic inflammation or persistent infection, internal or external root resorption can occur. This is where the root structure starts to dissolve. While primary roots naturally resorb before exfoliation, premature or pathological resorption can compromise the tooth's stability.
5. Damage to the Developing Permanent Tooth (for Primary Teeth)
- Although rare with modern techniques, severe infection in a primary tooth, especially if left untreated or if the pulpotomy fails, could potentially affect the enamel formation of the underlying permanent tooth bud.
6. Allergic Reaction
- While rare, an individual may have an allergic reaction to the local anesthetic, the medicaments used (e.g., Formocresol, though less common now), or the restorative materials.
7. Post-operative Sensitivity
- Some temporary sensitivity to hot, cold, or biting pressure is normal for a few days after the procedure. However, prolonged or severe sensitivity could indicate an issue.
To minimize these risks, it's crucial to:
- Choose an Experienced Dentist: Especially for children, a pediatric dentist has specialized training in pulp therapy.
- Follow Post-Operative Instructions: Adhere to dietary restrictions and oral hygiene advice.
- Attend Follow-up Appointments: These allow your dentist to monitor the healing process and the long-term success of the pulpotomy.
- Ensure a Good Final Restoration: A properly sealed final restoration (filling or crown) is paramount to preventing bacterial re-entry and protecting the treated pulp.
Children / Pediatric Considerations
Pulpotomies are exceptionally common in pediatric dentistry, making them a cornerstone of preserving primary (baby) teeth. The rationale and specific considerations for children are distinct and crucial for their developing oral health.
Why Pulpotomies are Crucial for Primary Teeth
Many parents might question why save a "baby tooth" that will eventually fall out. The reasons are significant:
- Space Maintainers: Primary teeth act as natural space maintainers, guiding the permanent teeth into their correct positions. Premature loss of a primary tooth due to untreated infection can lead to adjacent teeth drifting, causing crowding and orthodontic problems for the permanent dentition.
- Chewing and Nutrition: Healthy primary teeth are essential for proper chewing, allowing children to eat a varied and nutritious diet.
- Speech Development: The presence of all teeth plays a role in clear speech.
- Self-Esteem: A healthy, pain-free smile contributes to a child's confidence and overall well-being.
- Preventing Infection Spread: Untreated infections in primary teeth can spread, causing pain, swelling, and potentially affecting the developing permanent tooth bud or even leading to more serious systemic infections.
Unique Aspects of Pulpotomies in Children
- Pulp Anatomy: The pulp horns of primary teeth are generally closer to the tooth surface, making them more susceptible to exposure from decay. The root canals are also wider and more variable in shape.
- Diagnosis Challenges: Children may have difficulty articulating their symptoms. Dentists rely heavily on clinical examination, X-rays, and parental observations.
- Behavioral Management: Pediatric dentists are trained to manage anxious children, using techniques like "tell-show-do," distraction, and sometimes sedation to ensure a calm and cooperative experience.
- Restoration Choice: After a pulpotomy on a primary molar, a stainless steel crown (SSC) is the restoration of choice. SSCs are highly durable, provide excellent protection against fracture, and create a tight seal, significantly increasing the success rate of the pulpotomy. While composite fillings can be used on anterior primary teeth for aesthetic reasons, they are generally not recommended for molars after a pulpotomy due to lower durability.
- Medicaments: While Formocresol was historically common, many pediatric dentists now favor MTA, Biodentine, or Ferric Sulfate due to concerns about Formocresol's potential toxicity. The ADA regularly reviews guidelines on preferred materials.
Parental Guidance
- Early Dental Visits: The ADA recommends a child's first dental visit by age one or after the first tooth erupts. Early visits help establish good habits and identify problems promptly.
- Oral Hygiene at Home: Parents must be diligent about brushing and flossing their child's teeth, especially if the child is too young or lacks the dexterity to do so effectively.
- Dietary Habits: Limit sugary snacks and drinks, and encourage water consumption.
- Monitor for Symptoms: Be vigilant for any signs of tooth pain, sensitivity, swelling, or changes in behavior that might indicate a dental issue.
- Post-Treatment Care: Follow all post-operative instructions carefully, especially regarding diet and pain management. Ensure the child wears their mouthguard if they participate in sports.
A pulpotomy in a child is an investment in their overall oral health and contributes significantly to the proper development of their permanent dentition.
Cost Breakdown
While the "Cost and Insurance" section provided an overview, let's dive into a more specific breakdown of costs, with and without insurance, and discuss financing options. Understanding the nuances of dental costs can help you budget and plan for treatment.
Average US Costs (Low, Mid, High) by Tooth Type
| Procedure | Average Low (No Insurance) | Average Mid (No Insurance) | Average High (No Insurance) |
|---|---|---|---|
| Pulpotomy (Primary Tooth) | $200 | $350 | $600 |
| Pulpotomy (Permanent Tooth) | $400 | $650 | $900 |
| Stainless Steel Crown (Primary) | $150 | $275 | $500 |
| Composite Filling (Permanent) | $150 | $250 | $400+ |
| Porcelain/Zirconia Crown (Permanent) | $800 | $1,500 | $3,000+ |
| Initial Exam & X-rays (Diagnostic) | $50 - $150 | $150 - $250 | $250 - $400 |
Important Note: These are national averages. Your actual cost will depend on your specific location (e.g., urban vs. rural, cost of living), the dental practice, and the materials used. The total cost of a pulpotomy treatment often includes the pulpotomy procedure itself PLUS the final restorative material.
With vs. Without Insurance
Without Dental Insurance: You are responsible for the full cost of the procedure. This is where the "Average Low, Mid, High" ranges above are most relevant. If you don't have insurance, inquire about potential cash discounts or payment plans directly with the dental office.
With Dental Insurance:
- PPO/HMO Plans: Most dental insurance plans categorize a pulpotomy as a "basic" or "restorative" procedure.
- Coverage Percentage: Typically, insurance will cover 50% to 80% of the Usual, Customary, and Reasonable (UCR) fee for a pulpotomy. For example, if the dentist's fee is $400 and your plan covers 80%, you'd pay $80 (assuming deductible met).
- Deductible: Most plans have an annual deductible (e.g., $50-$100) that you must pay out-of-pocket before your insurance benefits begin.
- Annual Maximum: Insurance plans also have an annual maximum benefit (e.g., $1,000-$2,000) that they will pay out in a year. A pulpotomy plus a crown could quickly approach this limit, especially if other dental work is needed.
- Pre-authorization/Pre-determination: For combined treatments (pulpotomy + crown), it's highly advisable for your dentist to submit a pre-treatment estimate to your insurance company. This will give you a precise breakdown of what your insurance will cover and your estimated out-of-pocket expense.
Example Scenario (Child's Primary Molar):
- Procedure Cost (without insurance): Pulpotomy ($350) + Stainless Steel Crown ($275) = $625
- With Insurance (80% coverage, $50 deductible):
- You pay $50 (deductible).
- Insurance covers 80% of remaining $575 = $460.
- You pay $575 - $460 = $115.
- Total out-of-pocket: $50 (deductible) + $115 = $165
Payment Plans and Financing Options
If the out-of-pocket costs are substantial, consider:
- In-Office Payment Plans: Many dental practices offer flexible payment schedules directly with their patients.
- Third-Party Medical Financing: Companies like CareCredit or LendingClub provide specialized credit cards for healthcare expenses. They often offer interest-free promotional periods if paid in full within a certain timeframe (e.g., 6, 12, or 18 months).
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to save and spend pre-tax money on qualified medical and dental expenses.
- Dental Schools: University dental schools often provide services at a reduced cost, as treatment is performed by students under the supervision of experienced faculty.
Cost-Saving Tips
- Preventative Care: The absolute best way to save money on dental care is consistent preventative care (brushing, flossing, regular check-ups) to avoid severe issues in the first place.
- Shop Around (Carefully): While expertise is paramount, some practices may have different pricing structures. Get a few quotes for non-emergency procedures.
- Discuss Options: Always discuss the full cost and your payment options with your dental office's financial coordinator before treatment begins.
Frequently Asked Questions
Is a pulpotomy painful?
No, a pulpotomy itself is not painful. The procedure is performed under local anesthesia, completely numbing the tooth and surrounding area, so you or your child will not feel anything during the treatment. Afterward, it's normal to experience some mild discomfort or soreness once the anesthesia wears off, which can typically be managed with over-the-counter pain relievers.
How long does a pulpotomy last?
For primary teeth, a successful pulpotomy, followed by a stainless steel crown, is expected to last until the tooth naturally exfoliates (falls out) to make way for the permanent tooth. For permanent teeth, it aims to preserve the tooth's vitality for many years, allowing the root to fully develop. Its longevity depends on factors like the initial diagnosis, quality of the restoration, and ongoing oral hygiene.
What's the difference between a pulpotomy and a pulpectomy?
A pulpotomy involves removing only the diseased or infected coronal (crown) portion of the pulp, leaving the healthy radicular (root) pulp intact. A pulpectomy, conversely, involves removing all of the pulp tissue – both coronal and radicular – from a primary tooth. Pulpectomies are more extensive and are performed when the entire pulp is irreversibly infected or necrotic.
Is a pulpotomy the same as a root canal?
No, a pulpotomy is not the same as a root canal (full endodontic treatment), though both procedures fall under the field of endodoncia and aim to save a tooth with pulp issues. A pulpotomy is a more conservative treatment that only removes the coronal pulp and leaves the root pulp intact. A root canal treatment involves removing all of the pulp (coronal and radicular) from a permanent tooth, cleaning and shaping the entire root canal system, and then filling it with a sterile material. A pulpotomy is typically less invasive and quicker than a root canal.
Can an adult get a pulpotomy?
While pulpotomies are most commonly performed on primary teeth in children, they can sometimes be performed on young permanent teeth in adults (or adolescents) if the roots are not fully developed (immature apex). This procedure, often a partial pulpotomy (Cvek pulpotomy), aims to preserve the vital pulp to allow for continued root formation and strengthening, known as apexogenesis. It is rarely done on fully mature permanent teeth where a full root canal would be indicated.
What if a pulpotomy fails?
If a pulpotomy fails, it means the remaining radicular pulp has become infected or necrotic. The tooth will typically present with renewed pain, swelling, or signs of infection on an X-ray. In such cases, further treatment will be necessary: usually a pulpectomy or extraction for a primary tooth, or a full root canal treatment or extraction for a permanent tooth.
How long does the procedure take?
A pulpotomy procedure typically takes 30 to 60 minutes per tooth, depending on the complexity of the tooth, the extent of decay, and the patient's cooperation. This time usually includes administering anesthesia, preparing the tooth, performing the pulpotomy, and placing the final restoration (e.g., a stainless steel crown).
What are the alternatives to a pulpotomy?
Alternatives depend on the diagnosis. If the pulpitis is reversible, an indirect pulp cap or a simple filling might be sufficient. If the pulpitis is irreversible and involves the entire pulp, alternatives include a pulpectomy (for primary teeth), a full root canal treatment (for permanent teeth), or ultimately, tooth extraction. The goal is always to choose the most conservative option that preserves the tooth.
When is a pulpotomy not recommended?
A pulpotomy is generally not recommended if there are signs of irreversible pulpitis affecting the entire pulp, if there is evidence of pathology around the root (e.g., a periapical abscess visible on X-ray), if the tooth has mobility due to infection, or if there's extensive root resorption (in primary teeth). In such cases, a more extensive pulp therapy like a pulpectomy/root canal or extraction would be indicated.
When to See a Dentist
Recognizing when to seek professional dental care is crucial for preventing minor issues from escalating into severe problems, especially concerning pulp health.
Clear Warning Signs That Need Immediate Attention:
- Persistent or Spontaneous Tooth Pain: Pain that is constant, throbbing, or occurs without any stimulus (e.g., waking you up at night). This is a strong indicator of irreversible pulp inflammation or infection.
- Swelling in the Gums or Face: Any localized swelling around a tooth, or more widespread facial swelling, is a sign of an active infection that needs immediate attention.
- Pimple-like Bump on the Gums (Fistula): A small bump that may drain pus is a classic sign of a dental abscess and requires urgent treatment.
- Sensitivity to Hot and Cold that Lingers: If sensitivity to temperature changes lasts for more than a few seconds after the stimulus is removed, it suggests significant pulp inflammation.
- Pain Upon Chewing or Biting: Tenderness when biting down can indicate that the infection has spread to the ligament surrounding the tooth root.
- Fever Accompanied by Tooth Pain: A fever, especially in conjunction with dental pain or swelling, suggests a potentially serious infection that may require antibiotics in addition to dental treatment.
- Trauma to a Tooth: If a tooth has been fractured, dislodged, or sustained a significant impact, even without immediate pain, a dental check-up is essential to assess potential pulp damage.
Red Flags vs. Routine Care Guidance:
- Red Flag: Sudden, severe pain; visible swelling; pus; fever – these warrant an emergency dental appointment.
- Routine Care: Mild, transient sensitivity to cold; occasional food impaction; minor chips that don't cause pain – these can typically wait for a scheduled appointment, but should still be addressed.
Emergency vs. Scheduled Appointment Guidance:
- Emergency Appointment: If you or your child are experiencing any of the "Clear Warning Signs" listed above, particularly severe pain, swelling, or fever, contact your dentist immediately. Most dental offices reserve time for emergency visits. If your dentist is unavailable, seek care at an urgent dental clinic or hospital emergency room, especially if swelling compromises breathing or swallowing.
- Scheduled Appointment: For less urgent concerns, such as mild sensitivity, a small cavity, or a loose filling without pain, schedule a regular appointment. However, do not delay if symptoms start to worsen.
Remember, early diagnosis and treatment are critical for preserving teeth and preventing more severe complications. Don't hesitate to contact your dental professional if you have any concerns about your or your child's oral health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Stop Throbbing Pain After Root Canal
Undergoing a root canal procedure is often a necessary step to save a tooth severely damaged by decay or infection, preventing further complications and excruciating pain. While the procedure itself is performed under local anesthesia to ensure comfort, it's common for patients to experience some le
February 22, 2026
Root Canal After Care: Complete Guide
A root canal procedure can be a tooth-saving treatment, offering relief from pain and preventing further infection. However, the success and longevity of this crucial dental intervention heavily rely on diligent root canal after care. Neglecting post-treatment instructions can lead to complicati
February 22, 2026

Can You Drive After a Root Canal
Undergoing a root canal procedure can understandably bring up a host of questions and concerns, from understanding the process itself to managing recovery. One of the most common and practical inquiries people have is: can you drive after a root canal? The answer isn't always a simple yes or no,
February 22, 2026
Is a Root Canal Painful
When facing the prospect of a root canal, one of the most common and immediate questions that comes to mind is: is a root canal painful? It's a valid concern, stemming from outdated perceptions and anecdotal stories. However, modern root canal therapy is a highly effective and generally comforta
February 22, 2026