How to Stop Throbbing Pain After Root Canal
Key Takeaways
- Undergoing a root canal procedure is often a necessary step to save a tooth severely damaged by decay or infection, preventing further complications and excruciating pain. While the procedure itself is performed under local anesthesia to ensure comfort, it's common for patients to experience some le
How to Stop Throbbing Pain After Root Canal: A Comprehensive Guide to Relief
Undergoing a root canal procedure is often a necessary step to save a tooth severely damaged by decay or infection, preventing further complications and excruciating pain. While the procedure itself is performed under local anesthesia to ensure comfort, it's common for patients to experience some level of discomfort during the recovery phase. In fact, up to 70% of patients report some post-treatment pain, with a significant portion describing it as a throbbing sensation. If you've recently had a root canal and are wondering how to stop throbbing pain after root canal, you're not alone. This article from SmilePedia.net will provide an in-depth, medically accurate guide to understanding, managing, and preventing post-root canal throbbing pain, ensuring your recovery is as smooth and comfortable as possible. We’ll explore why this pain occurs, effective immediate and long-term relief strategies, what to expect during recovery, and when to seek urgent dental attention.
Key Takeaways:
- Normal vs. Concerning Pain: Mild to moderate throbbing pain for 1-3 days post-procedure is common and manageable with OTC pain relievers. Severe, worsening, or prolonged pain (beyond a week) requires immediate dental evaluation.
- Immediate Relief: Combine over-the-counter NSAIDs (like ibuprofen) and acetaminophen. Apply cold compresses for the first 24-48 hours, then switch to warm. Saltwater rinses can also soothe. Professional Intervention: If pain is severe or accompanied by swelling, fever, or pus, contact your dentist or endodontist immediately. They may prescribe stronger medication, perform an adjustment, or recommend further treatment.
- Cost of Root Canal: A single root canal typically ranges from $700 to $2,000 for front teeth, $800 to $2,200 for premolars, and $1,000 to $2,500+ for molars, varying by region and endodontist.
- Recovery Timeline: Most patients experience significant pain reduction within 2-3 days, with full healing taking several weeks. Final restoration (crown) is crucial within weeks to months.
- Prevention: Following post-operative instructions diligently, maintaining excellent oral hygiene, and attending follow-up appointments are vital to prevent complications and recurrence of pain.
- When to See a Dentist: If throbbing pain escalates, isn't relieved by medication, or you develop new symptoms like swelling, fever, or a bad taste, contact your dental professional immediately.
Understanding Root Canal Treatment: A Foundation
Before diving into pain management, it's crucial to understand what a root canal is and why it's performed. This context will help clarify why some post-procedure discomfort is expected.
What is a Root Canal?
A root canal, or endodontic treatment, is a dental procedure designed to save a tooth that has become severely infected or decayed. Inside each tooth, beneath the hard enamel and dentin layers, is a soft tissue called the pulp. This pulp contains nerves, blood vessels, and connective tissue, extending from the crown of the tooth down to the tip of its roots. When the pulp becomes inflamed or infected – often due to deep decay, repeated dental procedures on the tooth, cracks, chips, or trauma – it can cause significant pain and lead to an abscess if left untreated.
The root canal procedure involves removing the infected or inflamed pulp, carefully cleaning and shaping the inside of the root canal system, and then filling and sealing the space. After the root canal, a crown or other restoration is placed to protect the tooth and restore its full function.
Pro Tip: Thinking about the internal structure of your tooth as a "canal" helps visualize why the cleaning and sealing process is so critical and delicate.
When Do You Need a Root Canal?
Understanding the signs that necessitate a root canal can help you recognize the severity of the initial problem, which can sometimes influence post-treatment pain levels. You typically need a root canal if you experience:
- Severe toothache pain upon chewing or application of pressure.
- Prolonged sensitivity to hot or cold temperatures, even after the source of the temperature has been removed.
- Discoloration (darkening) of the tooth.
- Swelling and tenderness in the gums near the infected tooth.
- A persistent or recurring pimple-like lesion on the gums (a fistula), indicating an infection draining.
- Sometimes, there are no symptoms, and an infection is only discovered during a routine dental check-up with X-rays.
Ignoring these symptoms can lead to worsening infection, bone loss around the tooth, and eventually, tooth loss.
Does Root Canal Hurt? Addressing a Common Fear
One of the most common questions and fears surrounding root canal treatment is, "does root canal hurt?" The good news is that thanks to modern anesthesia and advanced techniques, the actual root canal procedure itself is typically no more uncomfortable than getting a filling. During the treatment, the area is completely numbed, so you should not feel pain.
The misconception that root canals are painful often stems from the severe pain patients experience before the procedure, when the pulp is infected. The root canal treatment is designed to relieve that pain, not cause it. However, it's the post-procedure period where some discomfort, including throbbing pain, can arise.
Types of Root Canal Procedures
While the general concept remains the same, there are variations depending on the tooth's condition and previous treatments:
- Initial Root Canal Treatment: This is the most common procedure performed on a tooth for the first time.
- Root Canal Retreatment: If a tooth that has already had a root canal becomes reinfected or fails to heal, the previous root canal filling material is removed, the canal is re-cleaned and re-shaped, and new filling material is placed. This is often more complex.
- Apicoectomy: A surgical procedure performed when an infection or inflammation persists after a root canal (or retreatment). It involves removing the tip of the tooth's root and sealing the end of the root canal.
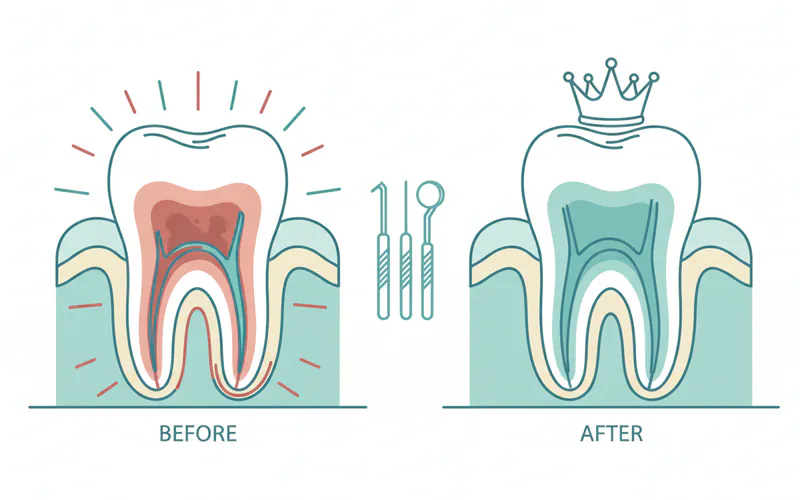
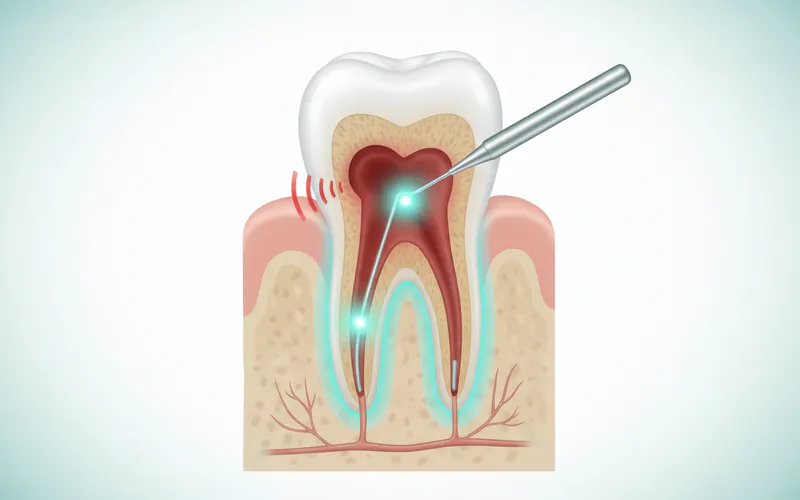
Why You Might Experience Throbbing Pain After a Root Canal
Experiencing some level of throbbing pain after a root canal is not uncommon and is often a normal part of the healing process. However, understanding the difference between normal post-operative discomfort and signs of a complication is key to effective management.
Normal Post-Procedure Sensitivity
Even after the infected pulp is removed, the tissues surrounding the tooth and root can remain inflamed. This inflammation is a natural response to the procedure itself, as well as the healing process.
- Tissue Healing: Your body is repairing the area where the infection was and where instruments worked. This inflammatory response can cause tenderness and a throbbing sensation.
- Ligament and Bone Sensitivity: The tooth sits in a socket, connected by a periodontal ligament. During the procedure, the tooth is isolated and manipulated, which can put stress on these surrounding structures, leading to temporary soreness.
- Pre-existing Inflammation: If the infection was severe before the root canal, the surrounding bone and gum tissue might have been significantly inflamed, contributing to more pronounced post-operative pain as they recover.
- Temporary Filling: If a temporary filling was placed, it might not perfectly match your bite, causing slight pressure on the tooth when chewing.
This "normal" throbbing pain typically peaks within the first 24-48 hours and gradually subsides over the next few days. It should be manageable with over-the-counter pain relievers.
Identifying Potential Complications
While some throbbing is normal, persistent or worsening pain, especially beyond a few days, could indicate a complication. It's crucial to be aware of these possibilities:
- Incomplete Cleaning/Persistent Infection: Although rare with modern techniques, if all infected tissue or bacteria were not completely removed, or if there were accessory canals not adequately treated, the infection might persist or recur. This can lead to ongoing pain.
- High Bite: After the procedure, if the temporary or permanent filling/crown is slightly too high, it can cause the treated tooth to bear excessive force when you bite down. This constant pressure irritates the periodontal ligament, leading to significant throbbing pain, especially when chewing.
- Cracked Tooth or Root Fracture: Sometimes, a crack in the tooth or root might not be visible during the initial diagnosis but can develop or worsen during or after the procedure. This can be a source of sharp, intermittent, or throbbing pain.
- Missed Canal: Teeth, especially molars, can have complex root canal anatomy with multiple, sometimes tiny, canals. If a canal is missed during treatment, it can harbor infection, leading to continued pain.
- Nerve Damage: While extremely rare, accidental damage to adjacent nerves (e.g., during injection of anesthesia or instrumentation) can cause persistent pain, numbness, or altered sensation.
- Allergic Reaction: Though uncommon, an allergic reaction to materials used during the procedure (e.g., the filling material or irrigants) could cause inflammation and pain.
- Abscess Formation: If the infection was particularly aggressive or if bacteria re-enter the tooth, an abscess (a pocket of pus) can form at the root tip, causing severe throbbing pain, swelling, and fever.
Contributing Factors to Increased Pain
Several factors can influence the intensity and duration of post-root canal pain:
- Severity of Pre-existing Infection: The more extensive and chronic the infection was prior to treatment, the more inflammation and tissue damage there might be, leading to a longer and more painful recovery.
- Individual Pain Threshold: People have different tolerances for pain. What one person considers mild discomfort, another might perceive as significant throbbing pain.
- Patient Compliance: Not following post-operative instructions, such as avoiding chewing on the treated tooth or missing prescribed medications, can exacerbate pain.
- Bruxism (Teeth Grinding): Patients who grind or clench their teeth, especially unconsciously at night, can put immense pressure on a healing tooth, leading to increased throbbing pain and tenderness.
Immediate Strategies: How to Stop Throbbing Pain After Root Canal
When throbbing pain strikes after a root canal, your immediate priority is relief. Here are medically sound strategies you can implement at home, often recommended by your dental professional.
Over-the-Counter (OTC) Pain Relief
For most mild to moderate post-root canal pain, OTC pain relievers are highly effective.
- Nonsteroidal Anti-inflammatory Drugs (NSAIDs): Medications like ibuprofen (Advil, Motrin) or naproxen (Aleve) are often the first line of defense. They work by reducing inflammation, which is a primary cause of throbbing pain.
- Dosage: For adults, ibuprofen is typically taken at a dose of 400-600 mg every 4-6 hours, not exceeding 2400 mg in 24 hours. Naproxen can be taken at 220-440 mg every 8-12 hours. Always follow package directions or your dentist's specific recommendations.
- Pros: Highly effective for inflammatory pain, readily available.
- Cons: Can cause stomach upset, not suitable for individuals with certain medical conditions (e.g., kidney disease, heart conditions, asthma, or those on blood thinners).
- Acetaminophen (Tylenol): This pain reliever works differently than NSAIDs by affecting pain pathways in the brain.
- Dosage: Typically 500-1000 mg every 4-6 hours, not exceeding 3000 mg (or 4000 mg depending on formulation) in 24 hours.
- Pros: Generally well-tolerated, suitable for those who cannot take NSAIDs.
- Cons: No anti-inflammatory properties, can be toxic to the liver in high doses.
Pro Tip: For enhanced pain relief, many dentists recommend alternating doses of ibuprofen and acetaminophen. For example, take ibuprofen, and three hours later, take acetaminophen. This provides continuous pain control and targets pain through different mechanisms. Always consult your dentist or pharmacist before combining medications.
Prescription Pain Medications
If OTC options aren't sufficient, your dentist may prescribe stronger medications.
- Stronger NSAIDs: Prescription-strength NSAIDs can provide more potent anti-inflammatory and pain-relieving effects.
- Opioid Analgesics (e.g., Codeine, Hydrocodone): These are sometimes prescribed for severe pain, but their use is increasingly limited due to concerns about addiction and side effects. They are generally reserved for very short-term use and severe cases.
- Pros: Highly effective for severe pain.
- Cons: Risk of addiction, drowsiness, constipation, nausea, should be used with extreme caution and only as directed.
- Muscle Relaxants: If clenching or grinding (bruxism) is contributing to the pain, a muscle relaxant might be prescribed to help jaw muscles relax.
- Pros: Can alleviate pain caused by muscle tension.
- Cons: Can cause drowsiness.
Cold and Warm Compress Therapy
This simple technique can provide significant relief for inflammation and soreness.
- Cold Compress (First 24-48 hours): Apply an ice pack or a bag of frozen peas wrapped in a thin cloth to the outside of your cheek, near the treated tooth, for 15-20 minutes at a time, every few hours.
- Benefits: Reduces swelling, constricts blood vessels, and numbs the area, helping to alleviate throbbing pain.
- Warm Compress (After 48 hours, if swelling has subsided): A warm, moist cloth applied to the same area can promote blood flow and muscle relaxation.
- Benefits: Can be soothing and help with residual soreness or muscle stiffness.
Oral Hygiene Practices
Maintaining cleanliness in your mouth is crucial for healing.
- Gentle Brushing: Continue brushing and flossing regularly, but be extra gentle around the treated tooth.
- Saltwater Rinses: Rinse your mouth several times a day with a warm saltwater solution (1/2 teaspoon of salt in 8 ounces of warm water).
- Benefits: Helps to reduce inflammation, clean the area, and promote healing. It's a natural antiseptic.
- Antiseptic Mouthwash: Your dentist might recommend a chlorhexidine gluconate rinse for a few days if there was significant infection or inflammation.
- Benefits: Kills bacteria and reduces the risk of secondary infection.
Dietary Modifications
What you eat (and how you eat it) directly impacts the treated tooth.
- Soft Foods: Stick to a soft food diet for the first few days. Examples include mashed potatoes, yogurt, smoothies, soups, scrambled eggs, and cooked vegetables.
- Avoid Chewing on the Treated Side: Until the tooth is fully restored with a permanent crown, it remains vulnerable to fracture. Avoid biting or chewing directly on the treated tooth.
- Avoid Hard, Crunchy, or Sticky Foods: These can damage the temporary filling or even fracture the tooth.
- Avoid Hot or Cold Extremes: While the nerve has been removed, the surrounding tissues can still be sensitive to temperature changes.
Avoiding Triggers
Identifying and avoiding activities that aggravate your pain can hasten recovery.
- Clenching or Grinding: If you clench or grind your teeth, especially at night, this can put undue stress on the healing tooth. Your dentist might suggest a nightguard.
- Smoking/Alcohol: Both can impede healing and increase the risk of complications. It's best to avoid them during recovery.
When to Seek Professional Help: Persistent or Worsening Pain
While mild throbbing pain is normal, certain signs indicate that you need to contact your dentist or endodontist immediately. Do not ignore these red flags.
Signs of Complications
- Severe Pain That Worsens: If the throbbing pain becomes intense, is not relieved by prescribed or OTC medications, or gets worse over time instead of improving after 2-3 days.
- Visible Swelling: Swelling inside your mouth (gums, palate) or outside your face (cheek, jawline) can indicate a spreading infection or abscess.
- Fever: A fever, especially accompanied by facial swelling, is a strong indicator of an active infection that needs urgent medical attention.
- Pus Drainage: If you notice pus draining from the treated tooth or surrounding gum tissue, or experience a foul taste, it signifies an active infection.
- Allergic Reaction Symptoms: Rash, hives, difficulty breathing, or significant swelling after taking medication should prompt immediate emergency medical care.
- Dislodged Temporary Filling: If your temporary filling comes out completely, the tooth is exposed to bacteria and vulnerable to fracture. Contact your dentist to have it replaced.
- Persistent Pressure or Sensitivity: If you feel an uncomfortable "high spot" when biting that doesn't resolve after a day or two, it might need adjustment.
What Your Dentist Can Do
If you experience these symptoms, your dentist or endodontist will perform a thorough examination, which may include:
- Re-evaluation and X-rays: To check for persistent infection, missed canals, or other issues.
- Bite Adjustment: If the filling or crown is too high, they can carefully adjust it to relieve pressure.
- Prescription for Antibiotics: If an infection is present or suspected.
- Prescription for Stronger Pain Medication: If your pain is severe and unmanageable.
- Root Canal Retreatment: If the initial treatment was unsuccessful due to missed canals or persistent infection.
- Apicoectomy: In rare cases, if retreatment isn't an option or is insufficient.
- Tooth Extraction: As a last resort, if the tooth cannot be saved.
The Root Canal Process: What to Expect
Understanding the steps involved in a root canal can help contextualize why post-procedure pain occurs and what care is needed.
1. Diagnosis
Your dentist will perform a thorough examination, including:
- Dental X-rays: To visualize the extent of decay, infection, and root anatomy.
- Pulp Vitality Tests: To determine if the pulp is alive, inflamed, or necrotic (dead).
- Patient History: Discussing your symptoms and medical history.
2. Anesthesia and Isolation
Local anesthesia is administered to numb the tooth and surrounding area. A dental dam (a small sheet of latex or non-latex material) is placed around the tooth to keep it dry and free from saliva and bacteria during the procedure.
3. Access and Cleaning
- A small opening is made in the crown of the tooth to access the pulp chamber.
- Using tiny dental instruments (files), the infected or inflamed pulp is carefully removed from the pulp chamber and root canals.
- The canals are then cleaned, shaped, and disinfected using irrigating solutions (like sodium hypochlorite) to remove bacteria and debris.
4. Filling and Sealing
- Once the canals are thoroughly cleaned and shaped, they are filled with a biocompatible, rubber-like material called gutta-percha.
- A special adhesive sealer is used with the gutta-percha to ensure a complete seal and prevent re-infection.
5. Temporary or Permanent Restoration
- After the root canal is complete, a temporary filling is usually placed in the access opening to protect the tooth until a permanent restoration can be placed.
- In most cases, a dental crown is recommended to protect the treated tooth from fracture and restore its full function and appearance. The crown appointment typically happens a few weeks or months after the root canal.
Recovery and Aftercare: Ensuring a Smooth Healing Process
Proper aftercare is paramount to minimize pain and ensure the long-term success of your root canal.
Medication Adherence
- Take Prescribed Medications: If your dentist prescribed antibiotics, finish the entire course, even if you feel better. Take prescribed pain relievers as directed.
- Follow OTC Dosing: Do not exceed recommended dosages for OTC pain relievers.
Oral Care
- Gentle Brushing and Flossing: Continue your regular oral hygiene routine, but be gentle around the treated tooth for a few days.
- Saltwater Rinses: Rinse with warm salt water several times a day to aid healing and reduce inflammation.
- Avoid Harsh Mouthwashes: Some alcohol-based mouthwashes can irritate the healing tissues.
Activity Restrictions
- Avoid Chewing on the Treated Tooth: Especially if it only has a temporary filling. This is crucial to prevent fracture.
- Limit Strenuous Activity: For the first 24-48 hours, avoid intense physical activity that might increase blood flow to the head and exacerbate throbbing.
Follow-up Appointments
- Attend All Scheduled Appointments: The follow-up appointment for your permanent crown or restoration is critical. The temporary filling is not designed for long-term use and can leak or break, leading to re-infection if not replaced promptly. Your dentist will also check the healing progress.
Preventing Post-Root Canal Pain and Future Issues
While some pain is normal, proactive steps can minimize discomfort and ensure the longevity of your treated tooth.
Choosing an Experienced Practitioner
- Endodontist vs. General Dentist: While many general dentists perform root canals, an endodontist is a dental specialist who has undergone additional training (2-3 years) specifically in diagnosing and treating diseases of the dental pulp. For complex cases, retreatments, or difficult anatomy, an endodontist's expertise can lead to higher success rates and potentially fewer post-operative complications.
Following Post-Op Instructions Diligently
- Listen Carefully: Pay close attention to your dentist's specific instructions regarding medication, diet, and activity restrictions.
- Ask Questions: If anything is unclear, don't hesitate to ask for clarification.
Maintaining Excellent Oral Hygiene
- Brush and Floss Regularly: This prevents new decay in other teeth and keeps your gums healthy, which is vital for the overall health of your treated tooth.
- Use Fluoride Toothpaste: Strengthens enamel and prevents decay.
Regular Dental Check-ups
- Routine Visits: Continue with your regular dental check-ups and cleanings (every six months) to allow your dentist to monitor the health of your treated tooth and address any emerging issues promptly.
Addressing Bruxism (Teeth Grinding)
- Nightguard: If you grind or clench your teeth, especially at night, a custom-fitted nightguard can protect your teeth (including the newly treated one) from excessive forces that could cause pain or even fracture.
Risks and Complications of Root Canal Treatment
While root canals have a high success rate (over 95%), like any medical procedure, there are potential risks and complications. Being aware of these can help you understand certain types of post-procedure pain.
1. Persistent Infection
- Cause: Can occur if the cleaning process didn't remove all bacteria, if there are missed accessory canals, or if the tooth becomes reinfected due to a leaky filling or crown, or a new cavity.
- Symptoms: Continuing pain, swelling, tenderness, or a recurring "pimple" on the gums.
2. Fractured Tooth
- Cause: A tooth that needs a root canal is often significantly weakened by decay or large fillings. The removal of pulp tissue can also make it more brittle. Without a proper permanent restoration (like a crown) in a timely manner, the tooth is highly susceptible to fracture, especially with biting forces.
- Symptoms: Sharp pain when biting, sensitivity to temperature, or visible cracks. A vertical root fracture can be very difficult to treat and often leads to extraction.
3. Procedural Errors
- Missed Canals: As mentioned, complex anatomy can lead to a missed canal, which can harbor infection.
- Perforation: While rare, a small hole can be inadvertently created in the side of the root during cleaning. This can be repaired but may affect the tooth's long-term prognosis.
- Broken Instrument: In rare cases, a small file used during the procedure can break inside the canal. If it can't be removed, it might be sealed within the canal, potentially affecting long-term success if it prevents proper cleaning or sealing.
4. Allergic Reactions
- Allergic reactions to anesthetic, rubber dam material (latex), or filling materials are possible but uncommon.
- Symptoms: Swelling, rash, itching, or, in severe cases, difficulty breathing.
Comparison: Root Canal vs. Tooth Extraction
Deciding between saving a tooth with a root canal or extracting it is a significant decision. Here's a comparison:
| Feature | Root Canal Treatment | Tooth Extraction |
|---|---|---|
| Goal | Save the natural tooth | Remove the diseased tooth |
| Procedure | Remove infected pulp, clean and fill canals, seal, then crown | Pull the tooth from its socket, potentially bone graft |
| Healing Time | 1-3 days initial pain, weeks for full tissue healing | 1-3 days initial pain, weeks for gum/bone healing |
| Long-term | Restored natural tooth, can last a lifetime | Gap in smile, need for replacement (implant, bridge, denture) |
| Cost (Typical) | $700 - $2,500+ (plus crown: $800 - $2,500) | $150 - $400 (simple), $200 - $600 (surgical) |
| Advantages | Retains natural tooth, preserves jawbone, natural bite, aesthetics | Cheaper upfront, immediate removal of infection source |
| Disadvantages | Higher initial cost, potential for retreatment | Leads to bone loss, teeth shifting, impact on chewing/speech, higher long-term costs for replacement |
[TABLE: Root Canal vs. Tooth Extraction Comparison]
Cost of Root Canal Treatment in the US
Understanding the financial aspect is crucial for many patients. The cost of a root canal varies significantly based on several factors, including the location of the tooth, the complexity of the case, the region of the country, and whether a general dentist or an endodontist performs the procedure.
Average Cost Ranges
Costs presented are general ranges and can fluctuate. These figures do not typically include the cost of the final restoration (e.g., a dental crown), which is usually necessary after a root canal and adds another $800 - $2,500+ to the total cost.
| Tooth Type | General Dentist (Average US) | Endodontist (Average US) |
|---|---|---|
| Front Tooth | $700 - $1,200 | $900 - $1,500 |
| Premolar | $800 - $1,500 | $1,000 - $1,800 |
| Molar | $1,000 - $2,000 | $1,200 - $2,500+ |
| Retreatment | $1,000 - $2,500+ | $1,500 - $3,000+ |
[TABLE: Root Canal Cost Comparison by Tooth Type and Practitioner]
Regional Variations: Costs can be higher in metropolitan areas and on the coasts (e.g., New York, Los Angeles) compared to rural areas or the Midwest. For example, a molar root canal in NYC might easily reach $2,500-$3,000 with an endodontist, while the same procedure in a smaller Midwestern town could be $1,500-$2,000.
Insurance Coverage Details
- Dental Insurance: Most dental insurance plans (PPO, HMO, DHMO) provide some coverage for root canals, as it's considered a major restorative procedure.
- PPO (Preferred Provider Organization): You can choose any dentist, but going in-network usually means lower out-of-pocket costs. They often cover 50-80% of the cost of a root canal after your deductible is met.
- HMO/DHMO (Health Maintenance Organization/Dental Health Maintenance Organization): You must select a dentist from a specific network, and referrals might be needed. Co-pays are usually fixed, and coverage percentage is often high.
- Waiting Periods: Many plans have waiting periods (e.g., 6-12 months) for major procedures like root canals.
- Annual Maximums: Most plans have an annual maximum benefit (e.g., $1,000 - $2,500). If your root canal and crown exceed this, you'll pay the difference.
- Medicaid: Coverage for root canals under Medicaid varies significantly by state. Some states may cover it fully, while others only cover extractions or very limited restorative care.
- Medicare: Original Medicare does not cover most dental care, including root canals. Some Medicare Advantage (Part C) plans may offer dental benefits.
Payment Plans and Financing Options
If you don't have insurance or face high out-of-pocket costs, several options can help:
- CareCredit and LendingClub: These are healthcare credit cards that offer special financing options, including interest-free periods if paid in full within a certain timeframe.
- In-Office Payment Plans: Many dental offices offer their own payment plans, allowing you to pay in installments.
- Dental Schools: University dental schools often provide services at a reduced cost, as procedures are performed by students under the supervision of experienced faculty.
- Flexible Spending Accounts (FSAs) / Health Savings Accounts (HSAs): If you have one of these through your employer, you can use pre-tax dollars to pay for dental expenses.
Cost-Saving Tips
- Get a Treatment Plan & Estimate: Always ask your dentist for a detailed treatment plan with cost estimates before proceeding.
- Verify Insurance Coverage: Call your insurance provider to understand your specific benefits, deductibles, waiting periods, and annual maximums.
- Compare Costs: For non-emergency situations, you might get a second opinion or compare prices from different dentists or endodontists, especially for complex cases.
- Preventive Care: The best way to save money in the long run is excellent oral hygiene and regular check-ups to prevent the need for root canals in the first place!
Children / Pediatric Considerations
While the focus of this article is on adult root canals and post-operative pain, it's worth noting that children can also experience pulp infections. However, their treatment protocols differ significantly for primary (baby) teeth.
- Pulpotomy (Nerve Treatment): For primary teeth, if the infection is limited to the crown portion of the pulp, a pulpotomy may be performed. This involves removing the infected pulp from the crown, leaving the healthy pulp in the root canals, and placing a medication.
- Pulpectomy (Full Nerve Removal): If the entire pulp, including in the roots, is infected in a primary tooth, a pulpectomy is done, similar to an adult root canal, but using resorbable filling materials designed to dissolve as the permanent tooth erupts.
- Post-Procedure Pain in Children: Similar to adults, children may experience mild soreness after these procedures. Pain management typically involves age-appropriate doses of acetaminophen or ibuprofen. Parents should monitor for persistent pain, swelling, or fever and contact their pediatric dentist if concerns arise.
For permanent teeth in children and adolescents, a full root canal procedure is performed just as it would be for adults.
Frequently Asked Questions
How long does throbbing pain after a root canal usually last?
Mild to moderate throbbing pain is common for the first 1-3 days after a root canal. It should gradually subside each day. If your pain is severe, doesn't improve after a few days, or worsens, you should contact your dentist immediately.
What is the best painkiller for throbbing pain after a root canal?
Over-the-counter NSAIDs like ibuprofen (Advil, Motrin) are highly effective as they reduce inflammation. Acetaminophen (Tylenol) can also be used, and many dentists recommend alternating doses of ibuprofen and acetaminophen for comprehensive pain relief. For severe pain, your dentist may prescribe stronger medication.
Can I chew on the tooth after a root canal?
It's generally advised to avoid chewing on the treated tooth, especially if it only has a temporary filling, until it has been permanently restored with a crown. This prevents potential fracture of the weakened tooth and allows the surrounding tissues to heal properly.
What if the throbbing pain gets worse after a few days?
Worsening or persistent severe throbbing pain after a few days is not normal and is a red flag. It could indicate a persistent infection, a high spot on your filling, or another complication. Contact your dentist or endodontist without delay for an evaluation.
Are there alternatives to a root canal if I'm worried about pain?
The primary alternative to a root canal for a severely infected tooth is extraction. However, extraction leads to a gap in your smile, potential bone loss, and shifting of adjacent teeth, often requiring further costly treatments like dental implants or bridges. A root canal is designed to save your natural tooth, which is usually the best option.
What are the signs of a failed root canal?
Signs of a failed root canal include persistent or recurring pain, swelling, tenderness in the gum, a draining "pimple" on the gum, or sensitivity to hot/cold or biting pressure long after the procedure. These symptoms warrant a dental re-evaluation.
Is it normal for the tooth to be sensitive to hot or cold after a root canal?
Since the nerve has been removed during a root canal, the tooth itself should not be sensitive to hot or cold temperatures. However, the surrounding gums and bone can be temporarily sensitive due to inflammation. If you experience persistent sensitivity to temperature directly in the treated tooth, contact your dentist.
How much does a root canal retreatment cost?
Root canal retreatment is typically more complex and thus more expensive than an initial root canal. In the US, costs can range from $1,000 to $2,500+ if done by a general dentist, and $1,500 to $3,000+ if performed by an endodontist, not including the new crown.
Can I exercise after a root canal?
It's generally recommended to avoid strenuous exercise for at least 24-48 hours after a root canal. Increased blood pressure and flow to the head can exacerbate throbbing pain and potentially dislodge a temporary filling. Stick to light activities or rest during the initial healing period.
What should I do if my temporary filling falls out?
If your temporary filling falls out, contact your dentist's office immediately. The tooth is now exposed to bacteria and vulnerable to fracture or re-infection. They will advise you on whether you need an urgent appointment to have it replaced.
When to See a Dentist
Knowing when to self-manage pain versus when to seek professional help is critical for your dental health and overall well-being.
Clear Warning Signs That Need Immediate Attention:
- Severe, Unmanageable Pain: If your throbbing pain is intense, not controlled by prescribed or over-the-counter medications, or worsens significantly over time.
- Swelling: Any new or worsening swelling inside your mouth (gums, palate) or outside your face (cheek, jaw, under the eye).
- Fever: A fever, especially accompanied by pain and swelling, indicates a serious infection.
- Pus Drainage: A foul taste or visible pus draining from the tooth or gums is a sign of an active infection or abscess.
- Difficulty Swallowing or Breathing: This is an emergency and could indicate a rapidly spreading infection. Seek immediate medical attention at an emergency room or call 911.
- Allergic Reaction Symptoms: Rash, hives, significant swelling, or difficulty breathing after taking medication.
Red Flags vs. Routine Care Guidance:
- Red Flag (Emergency/Urgent Appointment): Any of the symptoms listed above, especially if they appear suddenly or worsen rapidly. This usually means a complication requiring immediate professional intervention.
- Routine Care (Follow-up Appointment): Mild, decreasing soreness; minor sensitivity to pressure that is improving; questions about permanent restoration. These can typically wait for a regular business-hours appointment.
Emergency vs. Scheduled Appointment Guidance:
If you experience any of the severe warning signs, do not wait for a scheduled appointment. Contact your dentist's office immediately. They will advise you on whether you need an emergency visit, a visit to an urgent care clinic with dental capabilities, or referral to an emergency room. Many dental offices have an on-call service for after-hours emergencies.
Remember, your body's pain signals are important. While some discomfort after a root canal is normal, persistent or escalating pain is your body telling you something isn't right. Prompt communication with your dental professional is always the safest course of action.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Root Canal After Care: Complete Guide
A root canal procedure can be a tooth-saving treatment, offering relief from pain and preventing further infection. However, the success and longevity of this crucial dental intervention heavily rely on diligent root canal after care. Neglecting post-treatment instructions can lead to complicati
February 22, 2026

Can You Drive After a Root Canal
Undergoing a root canal procedure can understandably bring up a host of questions and concerns, from understanding the process itself to managing recovery. One of the most common and practical inquiries people have is: can you drive after a root canal? The answer isn't always a simple yes or no,
February 22, 2026
Is a Root Canal Painful
When facing the prospect of a root canal, one of the most common and immediate questions that comes to mind is: is a root canal painful? It's a valid concern, stemming from outdated perceptions and anecdotal stories. However, modern root canal therapy is a highly effective and generally comforta
February 22, 2026
How Much Are Root Canals
Experiencing a persistent toothache can be one of the most unsettling dental issues, often signaling a problem deep within the tooth’s core. For many, this leads to the dreaded question: "Do I need a root canal?" And immediately following that, how much are root canals going to cost me? It's a v
February 22, 2026