Pain After Root Canal: Complete Guide
Key Takeaways
- Experiencing pain after a root canal can be a confusing and sometimes alarming experience. While many people anticipate immediate relief from the often excruciating pain that necessitates a root canal, some degree of discomfort post-procedure is quite common and entirely normal. In fact, researc
Pain After Root Canal: Complete Guide
Experiencing pain after a root canal can be a confusing and sometimes alarming experience. While many people anticipate immediate relief from the often excruciating pain that necessitates a root canal, some degree of discomfort post-procedure is quite common and entirely normal. In fact, research indicates that up to 90% of patients report some level of mild to moderate pain for a few days after a root canal. This article, brought to you by SmilePedia.net, aims to demystify post-root canal pain, offering a comprehensive guide to understanding why it happens, what’s normal, when to be concerned, and how to manage it effectively. We'll explore the intricate details of what a root canal entails, delve into the various causes of post-procedure discomfort, outline effective treatment strategies, provide insights into costs, and ultimately empower you with the knowledge to navigate your recovery confidently and protect your dental health, potentially helping you understand how to avoid a root canal in the future.
Key Takeaways:
- Initial Discomfort is Normal: Expect mild to moderate pain for 3-5 days after a root canal, often managed with over-the-counter pain relievers.
- Common Causes of Pain: Inflammation, temporary filling issues, jaw soreness, and nerve sensitivity are typical. Persistent or severe pain may indicate complications like infection or incomplete treatment.
- Average Cost: A root canal in the US can range from $700 to $2,000 for front teeth, and $1,000 to $3,000+ for molars, often covered significantly by dental insurance.
- Recovery Timeline: Most patients feel significantly better within a week. Full healing, including crown placement, can take several weeks or months.
- Red Flags: Severe, throbbing, or worsening pain, swelling, fever, or a bad taste in your mouth are signs to contact your dentist immediately.
- Prevention is Key: Regular dental check-ups, good oral hygiene, and prompt treatment of cavities can how to avoid a root canal altogether.
- Treatment for Persistent Pain: Options include medication, re-treatment (costing $800-$2,500), apicoectomy (costing $900-$2,000), or in rare cases, extraction.
What a Root Canal Is: An Overview
Before diving into post-procedure pain, it's crucial to understand what a root canal actually is. A root canal, technically known as endodontic therapy, is a dental procedure designed to save a tooth that has become severely infected or damaged in its pulp—the soft tissue inside your tooth that contains nerves, blood vessels, and connective tissue. The pulp extends from the crown of the tooth down to the tip of the root.
When the pulp becomes inflamed or infected, usually due to deep decay, repeated dental procedures on the tooth, a crack or chip in the tooth, or trauma, it can cause significant pain and lead to an abscess if left untreated. An abscess is a pus-filled pocket that forms at the tip of the root in the jawbone.
During a root canal, an endodontist (a dentist specializing in root canals) or a general dentist removes the inflamed or infected pulp, carefully cleans and disinfects the inside of the tooth, and then fills and seals the space. Finally, the tooth is usually restored with a filling or a crown to protect it and restore its full function. The goal is to eliminate the infection and pain, and to save the natural tooth, preventing the need for extraction.
The Purpose of a Root Canal
The primary purpose of a root canal is to:
- Relieve pain caused by pulp inflammation or infection.
- Prevent the spread of infection to other teeth or into the jawbone.
- Save the natural tooth, maintaining your bite and natural appearance.
- Avoid the need for bridges or dental implants, which can be more costly and invasive.
It's a highly effective procedure with a success rate often exceeding 95% when performed correctly and followed by appropriate restoration.
![A cross-section of a tooth showing an infected pulp, with an arrow pointing to the area where the root canal procedure(/root-canal/complete-guide-to-endodontics-root-canal-everything-you-need-to-know) cleans out the infected tissue.]
Understanding Pain After Root Canal: Normal vs. Abnormal
Experiencing some level of pain after a root canal is very common. The intensity and duration of this pain are key indicators of whether it's part of the normal healing process or a sign of a complication.
Normal Post-Procedure Discomfort
It's entirely normal to experience mild to moderate discomfort for a few days after your root canal. This typically manifests as:
- Mild sensitivity: Especially when biting down or chewing, as the ligaments and tissues around the tooth are still healing.
- Dull ache: A general soreness in the area of the treated tooth, similar to muscle soreness after a workout.
- Jaw soreness: From keeping your mouth open during the procedure.
- Temporary filling discomfort: The temporary filling material might feel slightly different or cause minor irritation.
This normal pain usually peaks within the first 24-48 hours and gradually subsides over the next 3-5 days. It should be manageable with over-the-counter (OTC) pain relievers.
When Pain is a Red Flag (Abnormal Pain)
While some discomfort is expected, certain types of pain after root canal indicate a potential problem and warrant immediate attention from your dentist. These "red flags" include:
- Severe or throbbing pain: Pain that is intense, throbbing, or significantly worse than before the root canal, especially if it interferes with sleep or daily activities.
- Pain that worsens over time: If the pain doesn't improve after a few days or gets progressively worse.
- Swelling: Swelling in the gum, cheek, or jaw around the treated tooth.
- Pus or drainage: A foul taste in your mouth or visible pus coming from the tooth or gums.
- Fever: An elevated body temperature, which can indicate an ongoing infection.
- Allergic reaction: Symptoms like rash, itching, or difficulty breathing, which could be a reaction to medication.
- Uneven bite: If the temporary filling or crown feels too high, causing pressure on the tooth when you bite.
If you experience any of these symptoms, contact your dentist or endodontist immediately.
Causes of Pain After Root Canal
Understanding the underlying reasons for pain after root canal can help alleviate anxiety and guide appropriate action.
Common and Expected Causes
- Inflammation of Surrounding Tissues: Even though the infected pulp is removed, the tissues and ligaments supporting the tooth (the periodontal ligament) can become inflamed during the procedure. This is akin to a sprain or bruise and is the most common source of post-op soreness, especially when chewing.
- Jaw Soreness: Keeping your mouth open for an extended period during the procedure can lead to muscle fatigue and soreness in your jaw, known as temporomandibular joint (TMJ) discomfort.
- Temporary Filling/Crown Issues: A temporary filling might be slightly too high, causing uneven pressure when you bite. This can irritate the tooth and cause pain.
- Local Anesthesia Wearing Off: As the numbing agent wears off, you'll naturally start to feel sensations again, which can include the initial throbbing or aching.
- Nerve Sensitivity: Even after the main nerve is removed, microscopic nerves in the surrounding bone and gum tissue can remain sensitive for a period.
Less Common, Complicated Causes
- Incomplete Cleaning/Infection: If any infected tissue or bacteria were not thoroughly removed during the procedure, or if there were undetected accessory canals, the infection could persist or flare up. This is a common reason for persistent or worsening pain.
- Missed Canals: Some teeth, especially molars, have complex root canal systems with multiple canals. If a canal is very narrow, curved, or calcified, it might be missed during the initial treatment, allowing infection to remain.
- Fractured Tooth or Root: A crack or fracture in the tooth (either before the procedure or during it due to forces or instrumentation) can allow bacteria to re-enter, leading to persistent pain and infection.
- Perforation: In rare cases, a small hole (perforation) can be accidentally created in the root during the cleaning process, which can lead to infection or discomfort.
- Allergic Reaction to Filling Material: Although rare, some individuals might have a localized allergic reaction to the materials used to fill the root canal or the temporary restoration.
- Referred Pain: Sometimes, pain felt in the treated tooth might actually be originating from an adjacent tooth, the jaw, or even a sinus infection.
- Overfill or Underfill: The root canal filling material (gutta-percha) should ideally stop precisely at the end of the root. If it's pushed beyond the root tip (overfill) or doesn't extend far enough (underfill), it can cause irritation or allow bacteria to remain.
- Poor Restoration: If the final crown or permanent filling is not placed promptly or correctly, the treated tooth remains vulnerable to fracture or re-infection.
Managing Pain and Recovery After a Root Canal
Proper aftercare is crucial for managing pain after root canal and ensuring a smooth recovery.
Immediate Aftercare Instructions
- Avoid chewing on the treated tooth: For at least a few days, and until your permanent crown or filling is placed. This prevents re-contamination and protects the fragile tooth.
- Manage pain with medication:
- Over-the-counter (OTC) pain relievers: Ibuprofen (Advil, Motrin) or naproxen (Aleve) are often recommended as they also have anti-inflammatory properties. Acetaminophen (Tylenol) can also be used. Follow dosage instructions carefully.
- Prescription pain relievers: Your dentist may prescribe a stronger pain medication or a short course of antibiotics if there was a severe infection.
- Maintain good oral hygiene: Brush and floss gently around the treated tooth to keep the area clean and prevent further infection.
- Diet: Stick to soft foods for the first few days (e.g., soup, yogurt, mashed potatoes, scrambled eggs) and avoid extremely hot or cold foods.
- Avoid alcohol and tobacco: These can impede healing.
- Use a cold compress: Applying a cold pack to the outside of your cheek for 15-20 minutes at a time can help reduce swelling and discomfort.
Long-Term Recovery and Restoration
- Return for Permanent Restoration: This is critical. The temporary filling is not designed to withstand biting forces long-term and can break down, allowing bacteria to re-enter. Your permanent crown or filling typically needs to be placed within 2-4 weeks.
- Follow-up appointments: Your dentist or endodontist may want to see you for a follow-up to check on healing.
- Listen to your body: If pain persists or worsens, do not hesitate to contact your dental professional.
Pro Tip: Even if you feel no pain, ensure you return for your permanent restoration. Leaving the temporary filling in place for too long significantly increases the risk of re-infection and potential loss of the tooth.
Step-by-Step Root Canal Process
Understanding the steps involved can demystify the procedure and help explain post-operative sensations.
- Diagnosis and Planning: The dentist examines the tooth, takes X-rays, and performs tests to confirm pulp infection or damage.
- Anesthesia: Local anesthetic is administered to numb the tooth and surrounding area, ensuring you feel no pain during the procedure.
- Isolation: A small rubber sheet called a dental dam is placed around the tooth to isolate it, keeping it clean and dry from saliva and bacteria.
- Access Hole: A small opening is made in the crown of the tooth to access the pulp chamber and root canals.
- Pulp Removal: Using specialized instruments (files), the infected or inflamed pulp is carefully removed from the pulp chamber and the root canals.
- Cleaning and Shaping: The root canals are cleaned, disinfected, and shaped to prepare them for filling. This step is crucial for removing all bacteria.
- Filling the Canals: The cleaned canals are filled with a biocompatible, rubber-like material called gutta-percha, usually sealed with an adhesive cement.
- Temporary Filling: A temporary filling is placed in the access hole to seal the tooth until the permanent restoration (filling or crown) can be placed.
- Permanent Restoration: In a subsequent visit, the temporary filling is removed, and a permanent filling or a dental crown is placed to protect the treated tooth from fracture and restore its function and appearance.
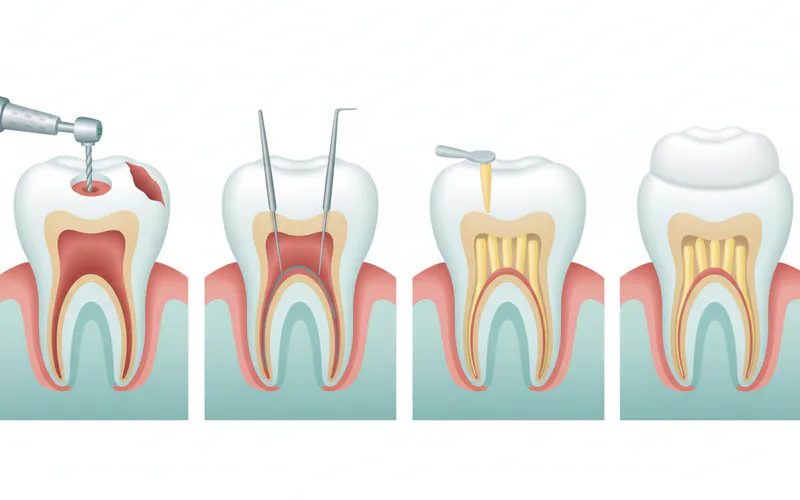
Treatment Options for Persistent Pain After Root Canal
If you experience persistent or severe pain after root canal that doesn't subside with typical recovery, your dentist will investigate the cause and recommend further treatment.
Diagnostic Steps
- Clinical examination: Your dentist will examine the tooth and surrounding tissues for swelling, tenderness, or signs of infection.
- X-rays: New X-rays will be taken to check for missed canals, incomplete filling, signs of a fracture, or periapical (around the root tip) inflammation.
- CBCT scan: In complex cases, a Cone Beam Computed Tomography (CBCT) scan may be used to get a detailed 3D view of the tooth and bone.
Remedial Treatment Options
| Treatment Option | Description | Pros | Cons | Estimated Cost Range (USD) |
|---|---|---|---|---|
| Root Canal Re-treatment | The existing root canal filling is removed, the canals are re-cleaned, re-shaped, and re-filled. | Can save the natural tooth; addresses underlying issues. | More complex and time-consuming than initial treatment; slightly lower success rate than initial treatment. | $800 - $2,500 |
| Apicoectomy | A surgical procedure where the very tip of the tooth's root is removed, along with any infected tissue. | Addresses issues at the root tip; avoids full re-treatment. | Invasive surgical procedure; not suitable for all cases. | $900 - $2,000 |
| Medication | Antibiotics for infection, stronger anti-inflammatory drugs, or prescription pain relievers. | Non-invasive; can resolve minor inflammation or infection. | Doesn't address structural issues like missed canals or fractures; temporary relief if underlying cause persists. | Varies (Rx cost) |
| Extraction | Removal of the entire tooth. | Eliminates the problem immediately; permanent solution to pain. | Loss of natural tooth; requires replacement (implant, bridge) to maintain bite and aesthetics. | $150 - $600 (simple); $250 - $1,500 (surgical) |
Pro Tip: Always discuss all available options with your dentist, including their success rates, costs, and long-term implications, before deciding on a treatment path for persistent pain after root canal.
Cost and Insurance for Root Canals and Re-treatments
The cost of a root canal can vary significantly based on several factors, including the specific tooth treated, the complexity of the case, the experience of the dental professional (general dentist vs. endodontist), and your geographical location in the US.
Average US Costs
| Procedure | Front Tooth (Incisor/Canine) | Premolar (Bicuspid) | Molar (Back Tooth) |
|---|---|---|---|
| Initial Root Canal (General Dentist) | $700 - $1,200 | $800 - $1,500 | $1,000 - $2,000 |
| Initial Root Canal (Endodontist) | $900 - $1,500 | $1,000 - $1,800 | $1,200 - $3,000+ |
| Root Canal Re-treatment | $800 - $1,500 | $1,000 - $1,800 | $1,200 - $2,500 |
| Apicoectomy | $900 - $1,500 | $1,000 - $1,800 | $1,200 - $2,000 |
| Dental Crown (Additional Cost) | $800 - $2,500 (material dependent) | $800 - $2,500 (material dependent) | $800 - $2,500 (material dependent) |
These are general ranges. Costs can be higher in major metropolitan areas.
Factors Influencing Cost
- Tooth Location: Molars have more roots and canals, making them more complex and expensive.
- Severity of Damage: Severely infected or calcified canals require more time and specialized techniques.
- Specialist vs. General Dentist: Endodontists, who specialize in root canals, often charge more due to their advanced training and equipment, but they may offer higher success rates for complex cases.
- Geographic Location: Costs vary significantly from state to state and even within different cities.
- Type of Restoration: A permanent filling is less expensive than a crown, but a crown is usually recommended for molars and teeth with significant structure loss to protect them from fracture.
Insurance Coverage
Most dental insurance plans provide coverage for root canals, as they are considered a major restorative procedure.
- Coverage Levels: Typically, insurance covers 50% to 80% of the cost of a root canal after your deductible is met.
- Deductibles and Annual Maximums: You will be responsible for your deductible (e.g., $50-$100) before insurance kicks in. Most plans have an annual maximum benefit (e.g., $1,000-$2,000), which can be reached quickly with a root canal and crown.
- Waiting Periods: Some plans have waiting periods for major procedures, meaning you might have to wait 6-12 months after enrollment before a root canal is covered.
- Pre-authorization: It's often advisable to get a pre-authorization from your insurance company to understand your exact out-of-pocket costs.
Payment Plans and Financing Options
For those without insurance or with high out-of-pocket costs, several options can help manage the expense:
- Dental Payment Plans: Many dental offices offer in-house payment plans, allowing you to pay in installments.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized health care credit cards with low or no-interest financing options for qualified applicants.
- Dental Schools: University dental schools often provide services at a reduced cost, performed by supervised students.
- Community Dental Clinics: Some non-profit clinics offer services on a sliding scale based on income.

Risks and Complications of Root Canals
While root canals are generally safe and effective, like any medical procedure, they carry potential risks and complications beyond normal pain after root canal.
- Persistent Infection or Pain: As discussed, this is the most common complication, often due to missed canals, incomplete cleaning, or re-infection.
- Tooth Fracture: The treated tooth, especially without a timely crown, can become brittle and prone to fracture. A severe fracture might necessitate extraction.
- Perforation: Accidental creation of a hole in the tooth root during treatment.
- Instrument Separation: A dental file can occasionally break off inside the root canal. While often harmless, it can sometimes prevent thorough cleaning or lead to re-infection if it blocks a canal.
- Allergic Reaction: To anesthesia, filling materials, or medications.
- Nerve Damage: Very rare, but adjacent nerves can sometimes be affected, leading to temporary or permanent numbness.
- Discoloration: A treated tooth can sometimes darken over time, though this can usually be addressed with internal bleaching or a crown.
Pro Tip: Choosing an experienced endodontist for complex cases can significantly reduce the risk of many of these complications. The ADA (American Dental Association) emphasizes the importance of selecting a qualified dental professional.
Prevention: How to Avoid a Root Canal
The best way to avoid pain after root canal is to avoid needing a root canal in the first place! Here's how to avoid a root canal:
- Excellent Oral Hygiene:
- Brush twice daily: Use a fluoride toothpaste and brush for at least two minutes, getting all surfaces of your teeth.
- Floss daily: Flossing removes plaque and food particles from between teeth and under the gumline, preventing cavities and gum disease that can lead to pulp infection.
- Use mouthwash: An antimicrobial mouthwash can help reduce bacteria.
- Regular Dental Check-ups and Cleanings:
- Visit your dentist at least twice a year for professional cleanings and examinations. Early detection of cavities or minor cracks can prevent them from becoming deep infections that require a root canal.
- Your dentist can identify potential issues like enamel erosion or grinding before they lead to severe damage.
- Prompt Treatment of Cavities: Don't delay treating small cavities. What starts as a minor cavity can quickly progress to deep decay, reaching the pulp and necessitating a root canal.
- Protect Your Teeth from Trauma:
- Wear a mouthguard: If you play contact sports, a custom-fitted mouthguard can protect your teeth from chips, cracks, and trauma that could damage the pulp.
- Avoid chewing hard objects: Ice, popcorn kernels, and hard candies can crack teeth.
- Address teeth grinding (bruxism): If you grind or clench your teeth, especially at night, your dentist may recommend a nightguard to prevent excessive wear and potential fractures that can expose the pulp.
- Healthy Diet: Limit sugary foods and drinks, which contribute to tooth decay.
- Avoid Tobacco Products: Smoking and chewing tobacco increase your risk of gum disease and other oral health problems that can indirectly lead to root canal issues.
Adhering to these preventive measures is your strongest defense against the need for endodontic treatment.
Children / Pediatric Considerations for Root Canals
While less common, children can also require root canal-like procedures on their primary (baby) teeth. These are typically called pulpotomies or pulpectomies.
- Pulpotomy: If only the crown portion of the pulp is infected, the dentist might perform a pulpotomy, removing only the infected part, disinfecting the remaining pulp, and placing a medicated dressing. This allows the root to remain vital.
- Pulpectomy: If the infection extends into the root canals of a baby tooth, a pulpectomy is performed. The entire pulp (crown and root portions) is removed, and the canals are filled with a resorbable material (unlike the gutta-percha used in adult teeth) to allow for natural tooth exfoliation.
- Purpose: The goal is to save the baby tooth until it's naturally lost, preserving space for the permanent tooth and maintaining chewing function and speech development.
- Pain After Procedure: Similar to adults, children may experience mild sensitivity or discomfort after a pulpotomy or pulpectomy. This is usually managed with children's pain relievers (like ibuprofen or acetaminophen) and typically resolves quickly.
- When to Worry: Parents should look out for persistent or worsening pain, significant swelling, fever, or a bad taste, which could indicate a persistent infection or complication. Contact a pediatric dentist immediately if these symptoms arise.
- Restoration: After these procedures, the baby tooth often requires a stainless steel crown to protect it from fracture until it's time for it to naturally fall out.
Cost Breakdown (for a Root Canal)
To reiterate and provide a more focused look at the financial aspect, here's a general cost breakdown in the US.
Average US Costs by Tooth Type and Provider
- Front Tooth (Incisor/Canine):
- General Dentist: $700 - $1,200
- Endodontist: $900 - $1,500
- Premolar (Bicuspid):
- General Dentist: $800 - $1,500
- Endodontist: $1,000 - $1,800
- Molar (Back Tooth):
- General Dentist: $1,000 - $2,000
- Endodontist: $1,200 - $3,000+
These costs are for the root canal procedure itself and do not include the cost of the final restoration (filling or crown), which is an additional fee.
Cost with vs. Without Insurance
- Without Insurance: You will be responsible for 100% of the costs as listed above.
- With Insurance:
- Deductible: Expect to pay your annual deductible first, typically $50 - $100.
- Co-insurance: After the deductible, your insurance plan might cover 50% - 80% of the remaining cost. For example, if a molar root canal costs $1,500 and your insurance covers 60%, you'd pay $600 plus your deductible.
- Annual Maximum: Be aware of your plan's annual maximum (e.g., $1,500 - $2,000). A root canal and crown can quickly use up this benefit.
Example Scenario:
- Molar Root Canal: $1,500
- Dental Crown: $1,200
- Total without insurance: $2,700
- If insurance covers 60% after a $100 deductible:
- Patient pays deductible: $100
- Remaining balance: $2,600
- Insurance pays 60% of $2,600: $1,560
- Patient pays 40% of $2,600: $1,040
- Total patient out-of-pocket: $100 (deductible) + $1,040 (co-insurance) = $1,140
Payment Plans and Cost-Saving Tips
- Payment Plans: Inquire with your dental office about interest-free payment plans.
- Dental Schools: Consider major university dental schools for potentially lower costs (usually 30-50% less), though treatment may take longer.
- Community Clinics: Look for federally funded health centers or community dental clinics that offer reduced fees based on income.
- Dental Savings Plans: These are not insurance but membership plans where you pay an annual fee for discounted services (typically 10-60% off).
- Compare Quotes: Don't hesitate to get quotes from a few different dentists or endodontists, especially for complex cases.
Frequently Asked Questions
What does "pain after root canal" feel like normally?
Normally, pain after root canal feels like a dull ache or sensitivity, especially when chewing, similar to a bruise. It's usually manageable with over-the-counter pain relievers and should gradually diminish over 3-5 days.
How long does pain last after a root canal?
Mild to moderate pain typically lasts for 3-5 days after the procedure. If the pain persists or worsens beyond a week, or if you experience severe symptoms, it's crucial to contact your dentist, as this could indicate a complication.
Can a root canal fail, and what happens then?
Yes, a root canal can fail, though it's rare. Failure typically occurs due to persistent infection, missed canals, or tooth fracture. If a root canal fails, options include re-treatment, apicoectomy (surgical removal of the root tip), or ultimately, extraction of the tooth.
How much does a root canal cost without insurance?
Without insurance, a root canal can cost anywhere from $700 for a front tooth to $3,000 or more for a molar, depending on complexity and provider. This doesn't include the cost of the necessary crown, which is an additional $800-$2,500.
What are the alternatives to a root canal if I have severe pulp infection?
If you have a severe pulp infection, the primary alternative to a root canal is tooth extraction. While extraction removes the problem, it leaves a gap that ideally should be replaced with a dental implant or a bridge to maintain your bite and prevent shifting of adjacent teeth, incurring additional costs and procedures.
Why do some dentists recommend an endodontist for a root canal?
Endodontists are dental specialists who have completed additional years of training specifically in diagnosing and treating pulp problems. They have advanced equipment and expertise, making them ideal for complex cases, re-treatments, or situations where a general dentist feels a higher level of specialization is needed.
Is it normal for my jaw to hurt after a root canal?
Yes, it's very common for your jaw to feel sore or stiff after a root canal. This is usually due to keeping your mouth open for an extended period during the procedure and typically resolves within a day or two. Applying a warm compress can help.
How can I make sure my root canal is successful and avoid further pain?
To ensure success and avoid future pain after root canal, follow all post-operative instructions carefully, especially avoiding chewing on the tooth until the permanent restoration is placed. Attend your follow-up appointments, get your permanent crown or filling promptly, and maintain excellent oral hygiene.
What should I do if my temporary filling falls out?
If your temporary filling falls out, contact your dentist immediately. While it's not usually an emergency if you can get in within a day or two, the tooth's canals are now exposed to bacteria, increasing the risk of re-infection and potentially more pain.
Can I eat normally right after a root canal?
You should avoid eating until the numbness wears off completely to prevent accidentally biting your tongue or cheek. For the first few days, stick to soft foods and avoid chewing on the treated tooth side until the permanent crown is placed to prevent dislodging the temporary filling or fracturing the weakened tooth.
When to See a Dentist
While some pain after root canal is normal, it's critical to know when to seek professional dental attention. Don't hesitate to call your dentist or endodontist if you experience any of the following:
- Severe, unrelenting pain: Pain that is intense, throbbing, or worsens significantly after 24-48 hours, especially if it's not relieved by over-the-counter pain medication.
- Pain that persists: If the initial discomfort doesn't improve or gradually fade after 5-7 days.
- Swelling: Any swelling in your gum, cheek, or jaw, which could indicate a developing or persistent infection.
- Visible pus or drainage: A bad taste in your mouth or visible pus coming from around the treated tooth.
- Fever: An elevated body temperature accompanied by tooth pain is a strong indicator of infection.
- Allergic reaction symptoms: Rash, itching, hives, or difficulty breathing, which could be a reaction to medication or materials.
- Uneven bite: If your temporary filling or crown feels too high, causing discomfort or making it hard to close your mouth properly.
- Loss of temporary filling: If the temporary filling falls out completely, exposing the inside of the tooth.
These signs are red flags that could indicate a complication requiring immediate evaluation and potentially further treatment. Delaying care can lead to more severe infection, damage to surrounding teeth, or even loss of the treated tooth. Your dental team is there to help, and they would rather you call with a minor concern than wait until a significant problem develops.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Stop Throbbing Pain After Root Canal
Undergoing a root canal procedure is often a necessary step to save a tooth severely damaged by decay or infection, preventing further complications and excruciating pain. While the procedure itself is performed under local anesthesia to ensure comfort, it's common for patients to experience some le
February 22, 2026
Root Canal After Care: Complete Guide
A root canal procedure can be a tooth-saving treatment, offering relief from pain and preventing further infection. However, the success and longevity of this crucial dental intervention heavily rely on diligent root canal after care. Neglecting post-treatment instructions can lead to complicati
February 22, 2026

Can You Drive After a Root Canal
Undergoing a root canal procedure can understandably bring up a host of questions and concerns, from understanding the process itself to managing recovery. One of the most common and practical inquiries people have is: can you drive after a root canal? The answer isn't always a simple yes or no,
February 22, 2026
Is a Root Canal Painful
When facing the prospect of a root canal, one of the most common and immediate questions that comes to mind is: is a root canal painful? It's a valid concern, stemming from outdated perceptions and anecdotal stories. However, modern root canal therapy is a highly effective and generally comforta
February 22, 2026