Implant
4,651 words · 16 min read
Quick Definition
A titanium or zirconia post surgically placed into the jawbone to serve as an artificial tooth root, supporting a crown, bridge, or denture.
Implant: The Definitive Guide to Restoring Your Smile and Oral Health
Imagine a solution to missing teeth that feels, functions, and looks just like your natural teeth. This isn't a futuristic dream; it's the reality of a dental implant. For millions across the US, dental implants have transformed smiles, restored confidence, and improved overall quality of life. At SmilePedia.net, we understand that when you search "what is implant" or "implant dental," you're looking for clear, comprehensive answers. This article aims to be your definitive guide.
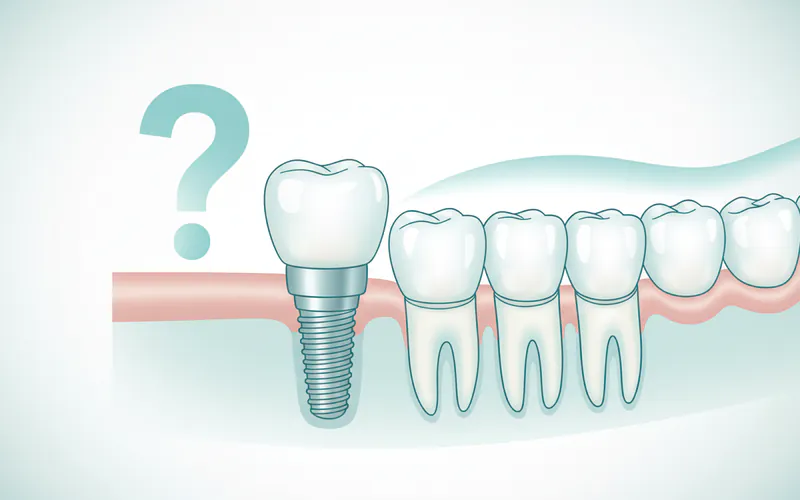
A dental implant is a titanium or zirconia post surgically placed into the jawbone to serve as an artificial tooth root. This robust foundation then supports a custom-made crown, bridge, or even a full denture, seamlessly filling the gaps left by missing teeth. More than just a cosmetic fix, implants are crucial for maintaining jawbone health, preserving the alignment of surrounding teeth, and enabling proper chewing and speech.
Tooth loss is a widespread concern in the United States. According to the Centers for Disease Control and Prevention (CDC), 1 in 4 adults aged 65 or older have lost all of their teeth, and 1 in 6 adults aged 45-64 has lost at least one permanent tooth due to decay or gum disease. While traditional solutions like dentures and bridges have served well, dental implants represent a significant leap forward, offering a durable, long-term, and natural-feeling alternative that addresses not just the visible gap, but also the underlying structural and health implications of tooth loss.
Key Takeaways:
- Dental implants are artificial tooth roots, typically made of titanium or zirconia, surgically placed into the jawbone.
- They are the most durable and natural-feeling solution for replacing missing teeth, supporting crowns, bridges, or dentures.
- Implants help preserve jawbone structure, preventing the bone loss that often occurs with missing teeth.
- The process involves a surgical placement, followed by a healing period called osseointegration, and then the attachment of a restoration.
- With proper care, dental implants can last for decades, often a lifetime.
- While a significant investment, implants offer long-term benefits for oral health, function, and aesthetics that often outweigh traditional alternatives.
Detailed Explanation
Types and Classifications of Dental Implants
Dental implants are not a one-size-fits-all solution. They come in various forms and are used to support different types of dental prosthetics. Understanding the classifications helps in appreciating the versatility of implant dental procedures.
-
Based on Placement Method:
- Endosteal Implants: These are the most common type of implant. "Endosteal" means "in the bone." They are typically screw-shaped (like a small screw or cylinder) and are surgically placed directly into the jawbone. They are suitable for most patients with sufficient bone density.
- Subperiosteal Implants: Historically, these were placed on top of the jawbone but under the gum tissue. They are rarely used today due to lower success rates compared to endosteal implants, primarily reserved for patients who cannot wear conventional dentures and have minimal bone height.
- Zygomatic Implants: A specialized type of implant used when there is severe bone loss in the upper jaw, making conventional implants impossible without extensive bone grafting. These longer implants anchor into the dense zygomatic bone (cheekbone).
-
Based on Material:
- Titanium Implants: By far the most common material. Titanium is highly biocompatible, meaning the body accepts it well, and it has an excellent track record for integrating with bone (a process called osseointegration).
- Zirconia Implants: A newer alternative, zirconia implants are metal-free and tooth-colored, offering an aesthetic advantage for some patients, particularly those with thin gum tissue. They also promote good gum health due to their smooth surface.
-
Based on the Number of Teeth Replaced:
- Single Tooth Implant: Replaces one missing tooth. A single implant post supports one crown.
- Implant-Supported Bridge: Replaces several missing teeth in a row. Two or more implants can support a bridge that spans the gap, eliminating the need to modify adjacent natural teeth (unlike a traditional bridge).
- Implant-Supported Denture (Full Arch): Replaces an entire arch of missing teeth (upper or lower).
- Removable Overdenture: Attaches to implants using clips or bars, providing significantly more stability than conventional dentures but can still be removed by the patient for cleaning.
- Fixed Hybrid Denture (e.g., All-on-4® or All-on-6®): A full arch of teeth is permanently attached to typically 4 to 6 implants. This type is not removable by the patient, offering maximum stability, chewing efficiency, and a feeling very similar to natural teeth.
Causes and Risk Factors for Tooth Loss
Understanding why teeth are lost is crucial for appreciating the preventative and restorative role of dental implants.
- Severe Tooth Decay: Uncontrolled cavities can destroy tooth structure to the point where the tooth cannot be saved.
- Periodontal Disease (Gum Disease): Advanced gum disease, or periodontitis, is the leading cause of tooth loss in adults. It destroys the bone and tissues supporting the teeth.
- Trauma or Injury: Accidents, sports injuries, or falls can cause teeth to be knocked out or severely fractured.
- Congenital Absence: Some individuals are born without certain permanent teeth.
- Failed Root Canal Treatment: Sometimes, a tooth that has undergone root canal therapy may still fail due to re-infection or fracture.
- Excessive Wear and Tear: Severe grinding (bruxism) or acidic erosion can compromise tooth structure over time.
While implants are a solution for tooth loss, certain risk factors can also affect the success of the implant procedure itself or the longevity of the implant:
- Smoking: Significantly reduces blood flow, impairs healing, and increases the risk of implant failure. Smokers have a much higher rate of peri-implantitis (gum disease around implants).
- Uncontrolled Diabetes: Can compromise the body's healing ability and increase susceptibility to infection.
- Poor Oral Hygiene: Inadequate brushing and flossing can lead to bacterial infection around the implant, a condition called peri-implantitis.
- Certain Medications: Some medications, such as certain bisphosphonates (used for osteoporosis), can affect bone metabolism and healing, potentially complicating implant placement.
- Radiation Therapy to the Head/Neck: Can impair bone healing and increase risk of complications.
- Compromised Immune System: Conditions like HIV/AIDS or immunosuppressive drugs can increase infection risk.
- Insufficient Jawbone: Without adequate bone volume and density, an implant cannot be stably placed, often requiring a bone graft first.
Signs and Symptoms to Watch For (Indicating Potential Need for Implants)
The primary "symptom" indicating a need for implants is a missing tooth or teeth. However, there are often secondary signs that highlight the implications of these gaps:
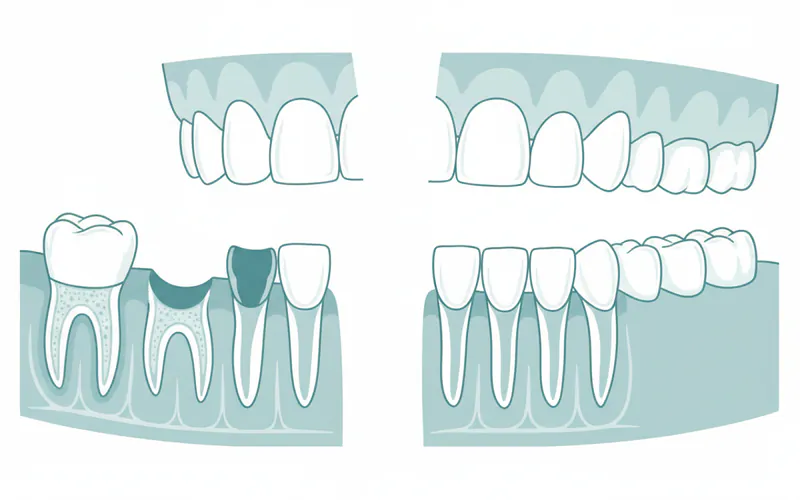
- Visible Gaps in Your Smile: The most obvious sign, affecting aesthetics and self-confidence.
- Difficulty Chewing: Missing teeth can make it challenging to bite and chew food properly, leading to dietary limitations.
- Speech Changes: Gaps, particularly in the front teeth, can affect articulation and cause a lisp.
- Shifting or Tilting Adjacent Teeth: When a tooth is lost, the neighboring teeth may drift into the empty space, leading to misalignment and bite problems.
- Super Eruption of Opposing Teeth: The tooth in the opposing arch (upper or lower) may move out of its socket in an attempt to find a biting partner.
- Jaw Pain or Discomfort: Missing teeth can lead to an imbalanced bite, putting stress on other teeth and the temporomandibular joint (TMJ).
- Changes in Facial Structure: Over time, the jawbone beneath a missing tooth will resorb (shrink) due to lack of stimulation. This can lead to a "caved-in" appearance around the mouth, making a person look older.
- Denture Instability: If you wear traditional dentures that slip, click, or cause sores, this is a clear sign that implant-supported options could dramatically improve your quality of life.
Diagnosis Process — What Your Dentist Does
A thorough diagnostic process is essential to determine if dental implants are the right solution for you and to plan the procedure meticulously.
- Initial Consultation: Your dentist or oral surgeon will discuss your medical and dental history, your goals for tooth replacement, and answer your initial questions about "what is implant" and the process.
- Comprehensive Oral Examination: This includes evaluating the remaining teeth, gums, and general oral health.
- Dental X-rays:
- Periapical X-rays: Provide detailed images of individual teeth and their roots.
- Panoramic X-rays: Offer a broad view of the entire jaw, showing all teeth, sinuses, and nerve pathways.
- 3D Imaging (CBCT Scan): This is a critical step for implant planning. A Cone Beam Computed Tomography (CBCT) scan provides highly detailed, three-dimensional images of your jawbone, soft tissues, nerve pathways, and bone density. This allows the dental professional to:
- Accurately measure the available bone height and width.
- Identify the exact location of critical structures like nerves (e.g., inferior alveolar nerve) and sinuses, ensuring they are avoided during surgery.
- Plan the optimal implant size, type, and precise placement angle.
- Dental Models/Impressions: Impressions of your mouth are taken to create plaster models. These models help in planning the final restoration and assessing your bite.
- Review of Medical History: Your general health is paramount. Conditions like diabetes, heart disease, or medications (e.g., blood thinners, bisphosphonates) need to be carefully reviewed to ensure you are a suitable candidate for surgery.
- Discussion of Treatment Plan: Based on all diagnostic information, your dental professional will present a detailed treatment plan, explaining the proposed procedure, timeline, estimated costs, and any necessary pre-procedures like a bone graft.
Treatment Options for Missing Teeth
While dental implants are often considered the gold standard, it's important to understand them in the context of other tooth replacement options.
| Feature | Dental Implant | Fixed Dental Bridge | Removable Partial/Full Denture |
|---|---|---|---|
| Description | An artificial root (titanium/zirconia) surgically placed into the jawbone, topped with a crown, bridge, or denture. | A false tooth (or teeth) held in place by crowns cemented onto natural teeth on either side of the gap. | A removable appliance (plastic/metal) with artificial teeth, resting on the gums and held by clasps (partial) or suction (full). |
| Bone Preservation | YES – Stimulates the jawbone, preventing bone loss (resorption) and maintaining facial structure. | NO – Does not stimulate the bone beneath the missing tooth, leading to eventual bone loss in that area. | NO – Bone loss continues beneath the denture, often accelerating it, leading to changes in facial structure and denture fit. |
| Adjacent Teeth | Unaffected. No need to alter healthy neighboring teeth. | Requires modification. Healthy adjacent teeth must be ground down to accommodate the supporting crowns, potentially weakening them. | Unaffected (if partial, clasps may put pressure on existing teeth); full dentures don't rely on existing teeth. |
| Stability/Function | Excellent. Highly stable, strong, feels like natural teeth, allows normal chewing and speech. | Good. Offers decent stability and function, but not as strong as implants. Can be challenging to clean underneath. | Variable. Can be unstable, especially full dentures. May slip, cause sore spots, and limit food choices. Significantly lower biting force. |
| Durability | Long-term. Can last 20+ years, often a lifetime, with proper care. High success rate (over 95%). | Medium-term. Typically lasts 5-15 years. May require replacement due to wear or issues with supporting teeth. | Short-term. Typically 5-10 years. Requires relining/replacement as jawbone changes. Prone to breakage. |
| Aesthetics | Excellent. Looks and feels most like natural teeth, preserving facial structure. | Good. Can look natural, but bone loss underneath may eventually create a visible gap at the gum line. | Fair to Good. Can look natural, but often bulky, and may affect speech and taste. Bone loss can alter facial aesthetics over time. |
| Cost Range (US) | High. $3,000-$6,000+ per implant (post, abutment, crown); Full arch (e.g., All-on-4) $20,000-$50,000+. | Medium. $2,000-$5,000+ per unit (e.g., a 3-unit bridge replacing one tooth means 3 units). | Low to Medium. Partial: $600-$2,500; Full: $1,500-$5,000+ per arch. |
| Procedure Time | Long. Several months (3-9+) due to surgical stages and healing time (osseointegration). | Medium. Typically 2-4 appointments over a few weeks. | Short. A few weeks for impressions and fabrication. |
| Pros | Most natural feel/look, preserves bone, no harm to adjacent teeth, highly durable. | Faster, less invasive than implants, good for replacing multiple teeth with natural teeth nearby. | Least expensive, non-invasive, quick to fabricate. |
| Cons | High initial cost, surgical procedure, longer treatment time, requires sufficient bone. | Requires grinding down healthy teeth, doesn't prevent bone loss, potentially more difficult to clean, supporting teeth can still decay. | Least stable, continued bone loss, potential for sore spots, dietary restrictions, may affect speech, needs frequent relines. |
Step-by-Step: What to Expect During Treatment
The implant dental process is a journey that typically spans several months, involving multiple stages to ensure proper healing and long-term success.
- Initial Consultation and Treatment Planning: As discussed, this involves a thorough examination, X-rays, CBCT scans, and discussion of your medical history to create a personalized treatment plan.
- Bone Grafting (If Necessary): If your jawbone lacks sufficient density or volume to support an implant, a bone graft procedure will be performed first. This involves placing bone material (from your own body, a donor, or synthetic) to rebuild the jawbone. This typically requires several months (3-9 months) of healing before the implant can be placed.
- Implant Placement Surgery:
- Anesthesia: The procedure is usually performed under local anesthesia, though sedation (oral or IV) or general anesthesia may be an option for patient comfort.
- Incision: The surgeon makes a small incision in the gum tissue to expose the jawbone.
- Drilling: Using specialized drills, a small pilot hole is carefully created in the bone at the planned location. This hole is then gradually widened to the precise size needed for the implant.
- Implant Insertion: The titanium or zirconia implant post is gently screwed or tapped into the prepared bone socket.
- Suturing: The gum tissue is then repositioned and sutured over the implant, completely covering it, or sometimes a healing abutment is attached immediately, leaving a small portion exposed through the gum. ``
- Osseointegration (Healing Phase): This is the most crucial phase. Over the next 3 to 6 months, the jawbone naturally grows around and fuses with the implant surface, creating a strong, stable anchor. This biological process is called osseointegration. During this time, you may wear a temporary denture or bridge.
- Abutment Placement (If Not Placed During Surgery): Once osseointegration is complete, a minor surgical procedure may be needed if the implant was completely covered by gum tissue. A small incision is made to expose the top of the implant, and a small connector post called an abutment is attached. The abutment protrudes through the gum line and will serve as the attachment point for your new tooth. The gum tissue is allowed a few weeks to heal around the abutment.
- Restoration Fabrication and Placement:
- Impressions: Once the gums have healed around the abutment, impressions (or digital scans) of your mouth are taken.
- Custom Fabrication: These impressions are sent to a dental lab where your custom-made crown, bridge, or denture is meticulously fabricated to match the color, shape, and size of your natural teeth.
- Final Attachment: At your final appointment, the custom-made restoration is securely attached to the abutment with cement or a screw. Your new tooth is now ready!
``
Recovery Timeline and Aftercare
Successful dental implant treatment relies heavily on proper recovery and diligent aftercare.
Immediate Post-Operative (First Few Days):
- Pain Management: Mild discomfort is normal and can usually be managed with over-the-counter pain relievers (like ibuprofen) or prescription medication if needed.
- Swelling and Bruising: Expect some swelling and possibly bruising around the surgical site, peaking around 24-48 hours. Cold compresses applied externally can help.
- Bleeding: Slight bleeding or oozing is normal. Avoid rinsing vigorously.
- Diet: Stick to soft foods and liquids for the first few days, avoiding very hot or cold items.
- Oral Hygiene: Gently brush remaining teeth, but avoid the surgical site. Your dentist may prescribe an antimicrobial mouthrinse. Do NOT rinse vigorously or spit forcefully.
- Activity: Avoid strenuous activity for 24-48 hours.
- Smoking: Absolutely avoid smoking, as it severely compromises healing.
During Osseointegration (3-6 Months):
- Maintain Excellent Oral Hygiene: This is critical to prevent infection (peri-implantitis). Brush twice daily, floss daily, and use any recommended interdental brushes or water flossers around your existing teeth and temporary prosthetics.
- Soft Diet (if implant covered): If your implant is fully covered, you'll generally return to a normal diet, but avoid chewing directly on the implant site until it has healed.
- Regular Dental Check-ups: Follow your dentist's schedule for follow-up appointments to monitor healing.
Long-Term Aftercare (After Restoration Placement):
- Meticulous Oral Hygiene: Treat your implant-supported teeth just like natural teeth. Brush at least twice a day, floss daily (or use interdental brushes/water flossers around the implant), and use a non-abrasive toothpaste. Specific implant-friendly tools may be recommended.
- Routine Dental Check-ups: Continue with regular check-ups and professional cleanings (typically every 6 months). Your dentist and hygienist are trained to clean around implants effectively and monitor their health.
- Avoid Hard/Sticky Foods: While implants are strong, excessive force on very hard candies, ice, or sticky caramels can potentially damage the crown or abutment.
- Wear a Nightguard: If you grind or clench your teeth (bruxism), a custom nightguard is highly recommended to protect your implants and natural teeth from excessive forces.
- Address Issues Promptly: If you notice any pain, swelling, bleeding, or mobility around an implant, contact your dentist immediately.
Prevention Strategies
Prevention applies in two ways: preventing tooth loss that might necessitate implants, and preventing complications or failure of existing implants.
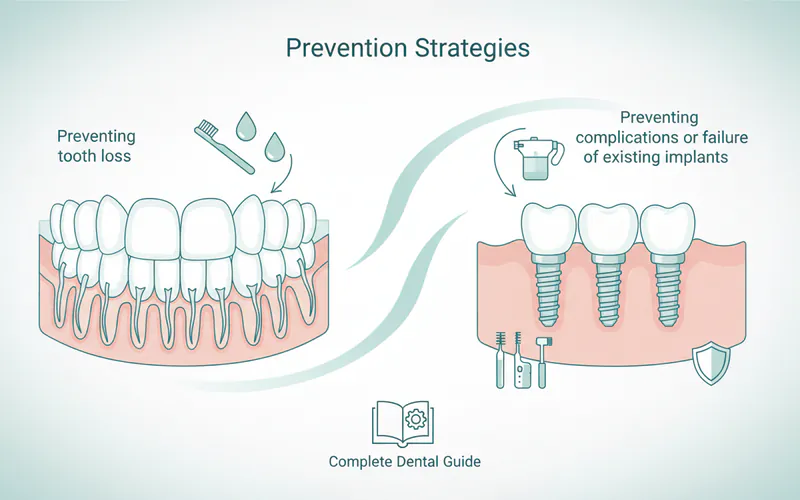
Preventing Tooth Loss:
- Excellent Oral Hygiene: Brush twice daily with fluoride toothpaste and floss daily. This is the cornerstone of preventing cavities and gum disease.
- Regular Dental Check-ups and Cleanings: Professional cleanings remove plaque and tartar that brushing misses, and check-ups catch problems early. Aim for at least every six months.
- Balanced Diet: Limit sugary and acidic foods and drinks that contribute to decay.
- Wear Mouthguards: For contact sports or if you grind your teeth, a protective mouthguard can prevent trauma and wear.
- Address Dental Issues Promptly: Don't ignore toothaches, sensitivity, or bleeding gums. Early intervention can often save a tooth.
Preventing Implant Failure (Peri-Implantitis):
- Strict Oral Hygiene: As detailed above, diligent brushing and flossing are crucial for preventing bacterial buildup around the implant.
- Regular Professional Maintenance: Implants need specialized cleaning and monitoring during routine dental visits.
- Avoid Smoking: This is the single most important lifestyle modification for implant success.
- Manage Systemic Diseases: Keep conditions like diabetes under control, as they can impact healing and immune response.
- Address Bruxism: If you clench or grind, a nightguard can protect your implants from excessive forces.
Cost Ranges in the US (with/without insurance)
The cost of dental implants can be a significant investment, but it's important to view it as a long-term solution that adds immense value to your oral health and quality of life. Prices vary widely based on location, the specific dentist/surgeon, the type of implant and restoration, and whether additional procedures (like bone grafting) are needed.
Average Cost Breakdown for a Single Dental Implant in the US:
- Implant Surgery (Post Placement): $1,500 - $3,000
- Abutment: $500 - $1,500
- Dental Crown (Porcelain Fused to Metal or Zirconia): $1,000 - $3,000
- Total for a single implant with crown: $3,000 - $7,500
Additional Procedures that can increase cost:
- Bone Grafting: $200 - $3,000+ (depending on size and complexity)
- Sinus Lift: $1,500 - $2,500+ per side
- Tooth Extraction (if needed): $75 - $600+
- Temporary Restoration: $300 - $1,500
Cost for Multiple Implants / Full Arch Solutions:
- Implant-Supported Bridge (2 implants, 3-4 unit bridge): $6,000 - $15,000+
- Full Arch Implant-Supported Denture (e.g., All-on-4): $15,000 - $30,000+ per arch (removable overdenture)
- Full Arch Fixed Hybrid Denture (e.g., All-on-4/6): $20,000 - $50,000+ per arch
Insurance Coverage: Dental insurance typically considers implants a major procedure.
- Coverage Varies Greatly: Some plans offer 0% coverage, while others may cover 10-50% of the surgical component, but rarely the entire cost of the abutment and crown. Many plans have an annual maximum (e.g., $1,000 - $2,500), which can quickly be met by implant costs.
- Medical Insurance: In some specific cases, if tooth loss is due to an accident or a medical condition requiring oral surgery, certain aspects of the implant procedure might be partially covered by medical insurance. It's essential to check with both your dental and medical insurance providers.
Financing Options: Many dental practices offer:
- Payment Plans: In-house or third-party financing options (e.g., CareCredit) that allow you to pay in installments.
- Dental Savings Plans: These are not insurance but offer discounts on dental procedures from participating providers.
``
For Parents / Pediatric Considerations
Dental implants are generally not recommended for children or adolescents whose jawbones are still growing and developing. Placing an implant in a growing jaw can lead to it being "submerged" as the surrounding bone continues to grow, resulting in misalignment and complications.
- Timing: Implants are typically only considered once jaw growth is complete, usually in the late teens or early twenties.
- Congenital Absence: For children born without certain permanent teeth (a condition called anodontia or hypodontia), a dental professional will plan for future tooth replacement. This might involve:
- Space Maintainers: To hold the space for a future tooth until the jaw is mature enough for an implant.
- Removable Partial Dentures: A temporary solution for aesthetic and functional needs.
- Orthodontics: To create or maintain space.
- Trauma: If a permanent tooth is lost due to trauma in a child, the focus will be on maintaining the space and assessing the best long-term solution, which may include an implant once growth is complete.
It's crucial for parents to consult with a pediatric dentist or orthodontist to create a long-term treatment plan for missing teeth in children.
Frequently Asked Questions
How much does a dental implant cost?
A single dental implant in the US typically ranges from $3,000 to $7,500, which includes the implant post, abutment, and custom crown. This cost can increase significantly if bone grafting, extractions, or other preparatory procedures are required. Full arch solutions, like All-on-4, can range from $20,000 to $50,000+ per arch. It's an investment, but one that offers long-term benefits and durability unmatched by other options.
Is getting a dental implant painful?
The implant placement surgery itself is typically performed under local anesthesia, so you shouldn't feel pain during the procedure. Many patients also opt for sedation dentistry (oral, IV, or nitrous oxide) to enhance comfort and reduce anxiety. After the anesthesia wears off, you can expect some discomfort, swelling, and mild pain, which can usually be managed effectively with over-the-counter pain relievers or prescription medication. Most patients report the discomfort is comparable to a tooth extraction.
How long does the dental implant process take?
The entire dental implant process typically spans 3 to 9 months, sometimes longer if extensive bone grafting is needed. This timeline includes:
- Initial Consultation & Planning: 1-2 weeks
- Bone Grafting (if needed): 3-9 months of healing
- Implant Placement Surgery: 1-2 hours
- Osseointegration (Implant-to-bone fusion): 3-6 months
- Abutment Placement (if separate): A quick procedure, followed by 1-2 weeks of gum healing.
- Restoration Fabrication & Placement: 2-4 weeks after impressions. While it's a multi-stage process, each step is crucial for the long-term success of the implant.
What are the alternatives to dental implants?
The main alternatives for replacing missing teeth are:
- Fixed Dental Bridge: Uses adjacent natural teeth as anchors for a false tooth. Pros: Faster, often less expensive initially. Cons: Requires grinding down healthy teeth, doesn't prevent bone loss.
- Removable Partial or Full Denture: A removable appliance that rests on the gums. Pros: Least expensive, non-invasive. Cons: Less stable, continued bone loss, potential for discomfort and dietary limitations. Implants are generally preferred for their superior stability, bone preservation, and natural feel.
Does dental insurance cover implants?
Dental insurance coverage for implants varies widely. Some plans may cover a portion (e.g., 10-50%) of the surgical component, especially if it's coded as a medical necessity or part of oral surgery. However, it's rare for insurance to cover the full cost of the implant, abutment, and crown. Most plans have an annual maximum benefit that implants can quickly exceed. It's crucial to contact your insurance provider directly and get a pre-determination of benefits before starting treatment. Many patients utilize financing plans or health savings accounts (HSAs) to manage costs.
How long do dental implants last?
With proper care and maintenance, dental implants have an excellent success rate and can last for 20 years, 30 years, or even a lifetime. The titanium implant post itself is incredibly durable. While the crown or bridge attached to the implant might need to be replaced after 10-15 years due to normal wear and tear, the implant post typically remains healthy and functional. Factors like oral hygiene, regular dental visits, and avoiding smoking greatly influence longevity.
Am I a candidate for dental implants?
Most healthy individuals are candidates for dental implants. Key requirements include:
- Sufficient Jawbone: Enough bone volume and density to support the implant. If not, a bone graft may be required.
- Good General Health: No uncontrolled systemic diseases (like diabetes or heart disease) that could compromise healing.
- Good Oral Hygiene: A commitment to diligent brushing and flossing to maintain the implant's health.
- Non-Smoker or Willing to Quit: Smoking significantly increases the risk of implant failure. A comprehensive evaluation by a dental professional is necessary to determine your specific candidacy.
Can an implant fail?
While dental implants have a high success rate (over 95%), failure is possible. The most common reason for implant failure is peri-implantitis, an inflammatory condition similar to gum disease that affects the tissues and bone surrounding the implant. Other causes include insufficient osseointegration, infection, excessive force on the implant, or rarely, implant fracture. Signs of potential failure include pain, swelling, tenderness, bleeding around the implant, or mobility of the implant itself. Prompt treatment can often save a failing implant.
When to See a Dentist
Don't wait if you're experiencing dental issues. Early intervention can often lead to simpler, less invasive, and more affordable treatment.
See a Dentist for Routine Care or Evaluation If You:
- Are missing one or more teeth.
- Have a failing crown, bridge, or denture.
- Experience difficulty chewing or speaking due to missing teeth.
- Notice your jawbone shrinking or changes in your facial profile due to tooth loss.
- Want to explore the best long-term solution for tooth replacement.
- Have questions about "what is implant" or implant dental procedures.
See a Dentist Immediately (Emergency Signs) If You:
- Experience severe or persistent pain around an existing implant.
- Notice swelling, redness, or pus around an implant.
- Feel an implant or its attached crown or bridge is loose or mobile.
- Suffer from trauma to the mouth that affects an implant or missing tooth area.
Taking proactive steps for your oral health, especially concerning tooth loss, can lead to a lifetime of confident smiles and optimal function. Dental implants offer a remarkable opportunity to achieve just that.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.