Graft
4,770 words · 16 min read
Quick Definition
A surgical procedure that transplants tissue from one area to another. In dentistry, bone grafts rebuild jawbone for implants, and gum grafts cover exposed tooth roots.
Graft: Rebuilding the Foundations of a Healthy Smile
Graft. In the realm of dental health, this seemingly simple word unlocks a world of sophisticated surgical procedures designed to rebuild, restore, and rejuvenate the crucial tissues supporting your teeth and smile. A graft is, at its core, a surgical procedure that transplants tissue from one area of the body (or an external source) to another to repair a defect or enhance volume. In dentistry, this most often refers to bone grafts, which restore lost jawbone structure, and gum grafts, which mend receding gumlines.
These procedures are not merely cosmetic; they are fundamental to maintaining oral health, enabling advanced treatments like dental implants, preserving natural teeth, and preventing further deterioration. Without adequate bone support, teeth can loosen and be lost; without healthy gums, roots become exposed, leading to sensitivity, decay, and ultimately, tooth loss. Dental grafts provide the essential scaffolding needed to maintain the integrity and longevity of your oral structures.
Who needs a dental graft? Millions of Americans annually confront issues that necessitate grafting. Bone loss in the jaw, for instance, affects a significant portion of the adult population, often as a consequence of tooth extractions, advanced periodontal disease, or trauma. Statistics from the Centers for Disease Control and Prevention (CDC) indicate that 47.2% of adults aged 30 years and older have some form of periodontal disease, with 70.1% of adults 65 years and older experiencing it. This chronic inflammatory condition is a leading cause of bone loss and gum recession, frequently paving the way for the need for grafts. Gum recession, another common issue, impacts a vast number of individuals, with some estimates suggesting it affects between 4% and 90% of the population, depending on age and diagnostic criteria. The ability to effectively replace lost bone and gingival tissue through grafting is a cornerstone of modern restorative and preventive dentistry, helping countless individuals regain their oral health and confidence.
Key Takeaways:
- A dental graft is a surgical procedure that transplants tissue to repair or augment bone or gum deficiencies.
- The two primary types in dentistry are bone grafts (to rebuild jawbone) and gum grafts (to cover exposed tooth roots).
- Bone grafts are often critical prerequisites for successful dental implant placement.
- Gum grafts protect teeth from sensitivity, decay, and further recession caused by issues like periodontal disease.
- These procedures are essential for long-term oral health, preserving teeth, and restoring both function and aesthetics.
- Grafts are generally safe, effective procedures performed by specialists like periodontists and oral surgeons.
Detailed Explanation of Dental Grafts
Dental grafts represent a sophisticated blend of biology and surgical expertise, addressing critical deficiencies in both hard (bone) and soft (gum) tissues within the oral cavity. Understanding the various types, causes, and treatments is key to appreciating their vital role in modern dentistry.
Types and Classifications of Dental Grafts
Dental grafts are broadly categorized into two main types: bone grafts and gum grafts. Each serves a distinct purpose and utilizes different tissue sources and techniques.
Bone Grafts
Bone grafts are surgical procedures that augment or rebuild areas of the jawbone where insufficient bone volume or density exists. This is crucial for providing a stable foundation for dental implants, improving denture retention, or correcting jawbone deformities.
There are four primary sources for bone graft material:
-
Autograft:
- Source: The patient's own bone, typically harvested from another site in the mouth (e.g., chin, ramus of the jaw), hip, or tibia.
- Pros: Considered the "gold standard" due to superior biological compatibility; no risk of disease transmission or immunological rejection. It contains living bone cells (osteocytes) and growth factors (osteogenic cells) that actively promote new bone formation.
- Cons: Requires a second surgical site for harvesting, which can increase discomfort, procedure time, and potential complications at the donor site. Limited availability of donor bone.
-
Allograft:
- Source: Bone from a deceased human donor, processed to ensure safety and sterility.
- Pros: Readily available in various forms and sizes; avoids the need for a second surgical site for harvesting.
- Cons: No living bone cells, so it primarily acts as a scaffold for the patient's own bone to grow into (osteoinductive and osteoconductive). Minimal, but not zero, risk of disease transmission (though extremely rare with modern processing).
-
Xenograft:
- Source: Bone derived from an animal species, most commonly bovine (cow) or porcine (pig). These materials are highly purified and sterilized.
- Pros: Abundant supply; avoids a second surgical site; excellent scaffold (osteoconductive) for new bone growth.
- Cons: Slower integration compared to autografts; no living cells or growth factors. Minimal theoretical risk of immune reaction, though modern processing makes this rare.
-
Alloplast:
- Source: Synthetic, biocompatible materials such as hydroxyapatite, tricalcium phosphate, or bioactive glass.
- Pros: Unlimited supply; no donor site needed; eliminates concerns about disease transmission or immune rejection.
- Cons: Purely osteoconductive (provides a scaffold but doesn't actively stimulate bone growth); integration can be slower and less predictable than biological grafts.
Common Bone Graft Procedures:
- Socket Preservation (Ridge Preservation): Performed immediately after tooth extraction to prevent the collapse of the alveolar ridge (the bone that holds the tooth). This is crucial for future implant placement.
- Sinus Lift (Sinus Augmentation): When upper back teeth are removed, the maxillary sinus can expand downwards, reducing bone height for implants. A sinus lift elevates the sinus membrane and places graft material into the space to create new bone.
- Ridge Augmentation: Used to restore the natural contour of the jawbone when it has atrophied due to tooth loss, trauma, or periodontal disease, often making it too narrow or short for implants.
- Major Bone Grafting: For extensive bone loss, often due to trauma, tumor removal, or congenital defects, which may require larger blocks of bone or more complex surgical approaches.
Gum Grafts (Soft Tissue Grafts)
Gum grafts, also known as soft tissue grafts, are surgical procedures used to treat gingival recession, where the gum tissue pulls away from the tooth, exposing the root surface. This can lead to sensitivity, root decay, and an unappealing aesthetic.
There are three primary types of gum grafts:
-
Connective Tissue Graft:
- Source: Tissue harvested from beneath the surface layer of the patient's palate (roof of the mouth).
- Pros: The most common and highly successful type for covering exposed roots and thickening existing gum tissue; offers excellent aesthetic results.
- Cons: Requires a second surgical site on the palate, which can cause temporary discomfort.
-
Free Gingival Graft:
- Source: A small piece of tissue harvested directly from the surface of the patient's palate.
- Pros: Good for thickening thin gum tissue or increasing the amount of attached gingiva (gum tissue firmly bound to the bone).
- Cons: The color match with surrounding gums may not be as precise as with connective tissue grafts; the palate donor site can be more uncomfortable during healing.
-
Pedicle Graft (Lateral Sliding or Rotational Flap):
- Source: Tissue is taken from the gum adjacent to the receded area and rotated or pulled over to cover the exposed root.
- Pros: No second surgical site for harvesting; excellent blood supply to the graft, leading to predictable healing.
- Cons: Only feasible if there is sufficient healthy gum tissue immediately next to the receded tooth; less predictable if the adjacent tissue is thin.
-
Acellular Dermal Matrix (ADM) Graft:
- Source: Processed human donor tissue (allograft), similar to allografts for bone but for soft tissue. It's decellularized to remove genetic material and prevent immune rejection.
- Pros: Avoids a second surgical site; readily available; can treat multiple teeth at once.
- Cons: While safe, it does not contain living cells, so it acts as a scaffold for the body's own cells to grow into.
Causes and Risk Factors for Needing Dental Grafts
The need for dental grafts is usually a result of tissue loss, which can stem from various factors:
Causes and Risk Factors for Bone Grafts:
- Tooth Extractions: When a tooth is removed, the bone that once supported it begins to resorb or shrink almost immediately if not preserved. Within the first year, a significant percentage of bone width can be lost.
- Periodontal Disease (Gum Disease): This chronic bacterial infection destroys the supporting bone and soft tissues around the teeth. Untreated periodontal disease is the most common cause of significant bone loss in adults.
- Trauma: Injuries to the face or mouth can fracture or displace jawbone segments, leading to bone loss.
- Developmental Defects: Some individuals are born with insufficient jawbone volume or structural abnormalities.
- Tumors or Cysts: Surgical removal of benign or malignant growths in the jaw can result in bone deficits.
- Long-term Denture Use: Dentures that don't fit properly can rub against the gums and underlying bone, accelerating bone resorption over time.
- Missing Teeth (Long-Term): Even without periodontal disease, if a missing tooth is not replaced, the body naturally resorbs the bone in that area, as it's no longer stimulated.
Causes and Risk Factors for Gum Grafts:
- Periodontal Disease: As mentioned, advanced gum disease not only causes bone loss but also leads to severe gum recession as the infection destroys the supporting tissues.
- Aggressive Tooth Brushing: Brushing too hard with a stiff-bristled toothbrush can physically abrade and wear away the delicate gum tissue over time.
- Genetics: Some individuals are genetically predisposed to having thin gum tissue or a higher susceptibility to recession.
- Tobacco Use: Smoking and chewing tobacco are significant risk factors for periodontal disease and can directly contribute to gum recession by constricting blood flow and impairing tissue healing.
- Misaligned Teeth or Malocclusion: Crooked teeth or an improper bite can place excessive stress on certain gum areas, leading to recession.
- Lip or Tongue Piercings: Jewelry can continuously rub against the gum tissue, causing chronic irritation and recession.
- Bruxism (Teeth Grinding/Clenching): Chronic grinding can put undue stress on the supporting structures of the teeth, contributing to gum recession.
Signs and Symptoms to Watch For
Recognizing the signs that you might need a dental graft is crucial for early intervention and better outcomes.
Signs of Bone Loss (Potentially Requiring Bone Graft):
- Loose or Shifting Teeth: A primary indicator of insufficient bone support.
- Changes in Bite: Your teeth no longer fit together as they once did.
- Difficulty with Dentures: If existing dentures suddenly feel loose or uncomfortable.
- Visible Jawbone Resorption: A "caved-in" or sunken appearance in the area of a missing tooth, or a change in facial profile.
- Pain or Tenderness: Especially around areas of missing teeth or advanced periodontal disease.
Signs of Gum Recession (Potentially Requiring Gum Graft):
- Tooth Sensitivity: Exposed tooth roots are highly sensitive to hot, cold, or sweet stimuli because they lack the protective enamel.
- Teeth Appear "Longer": As gums recede, more of the tooth structure (the root) becomes visible, making teeth look elongated.
- Visible Root Surfaces: The yellowish or darker dentin of the root becomes apparent above the gumline.
- Bleeding Gums: While a sign of periodontal disease generally, receding gums can be more prone to bleeding during brushing.
- Notches Near the Gumline: These can be caused by aggressive brushing on exposed root surfaces.
- Discomfort or Pain: In severe cases, inflammation or infection can cause localized pain.
Diagnosis Process — What Your Dentist Does
A thorough diagnostic process is essential to determine the type, extent, and appropriate treatment for bone or gum deficiencies.
- Comprehensive Clinical Examination: Your dentist will visually inspect your gums, teeth, and overall oral cavity. They will use a periodontal probe to measure the depth of gum pockets and assess the extent of gum recession around each tooth.
- Dental X-rays: Traditional X-rays (periapical and panoramic) provide a two-dimensional view of the bone levels around the teeth, helping to identify areas of bone loss.
- 3D Imaging (Cone Beam Computed Tomography - CBCT Scan): For bone graft planning, especially for dental implants or complex cases, a CBCT scan is indispensable. This advanced imaging provides highly detailed three-dimensional images of the jawbone, revealing precise bone height, width, and density, as well as the proximity of vital structures like nerves and sinuses.
- Photography: Clinical photos are often taken to document the initial condition and track progress.
- Referral to a Specialist: If bone or gum grafting is indicated, your general dentist will typically refer you to a specialist, such as a periodontist (gum specialist) or an oral and maxillofacial surgeon, who has advanced training and experience in performing these complex procedures. The specialist will conduct their own detailed assessment before formulating a treatment plan.
Treatment Options with Pros, Cons, and Costs
As discussed, the "treatment options" for bone and gum deficiencies are grafts, not alternatives to them if the tissue is already lost. Here, we'll summarize the pros and cons of the different types of graft materials and techniques, along with general cost considerations.
Bone Graft Material Comparison:
| Graft Type | Pros | Cons |
|---|---|---|
| Autograft | Gold standard; best integration; contains living cells. | Requires second surgical site (donor); increased discomfort/complexity; limited availability. |
| Allograft | Readily available; no second surgical site. | No living cells (scaffold only); minimal theoretical disease transmission risk. |
| Xenograft | Abundant supply; no second surgical site; good scaffold. | Slower integration; no living cells; minimal theoretical immune reaction risk. |
| Alloplast | Unlimited supply; no second surgical site; no disease risk. | Purely osteoconductive (scaffold only); slower/less predictable integration than biological grafts. |
Gum Graft Technique Comparison:
| Graft Type | Pros | Cons |
|---|---|---|
| Connective Tissue Graft | Highly successful for root coverage; excellent aesthetics. | Requires second surgical site (palate) for harvesting. |
| Free Gingival Graft | Good for thickening thin gums; increases attached gingiva. | Less predictable color match; palate donor site can be more uncomfortable. |
| Pedicle Graft | No second surgical site; good blood supply. | Only feasible with sufficient adjacent healthy gum tissue; limited application. |
| Acellular Dermal Matrix | No second surgical site; treats multiple teeth; readily available. | No living cells (scaffold only); generally more expensive than tissue from palate; variable outcomes. |
Step-by-Step: What to Expect During Treatment
While specifics vary by graft type and individual case, here's a general overview of what to expect:
Bone Graft Procedure:
- Anesthesia: Local anesthesia is administered to numb the surgical area. Sedation options (oral, IV) may also be offered for patient comfort.
- Incision: The surgeon makes an incision in the gum tissue to expose the underlying bone defect.
- Graft Placement: The chosen bone graft material (autograft, allograft, xenograft, or alloplast) is carefully placed into the deficient area.
- Membrane Placement (Optional but Common): Often, a protective membrane (resorbable or non-resorbable) is placed over the graft material. This membrane acts as a barrier, preventing gum tissue from growing into the graft site too quickly and allowing the bone cells to proliferate undisturbed.
- Suturing: The gum tissue is carefully sutured back into place, often using very fine stitches.
Gum Graft Procedure:
- Anesthesia: Local anesthesia is administered to numb both the recipient site (where recession is) and the donor site (if using patient's own tissue).
- Recipient Site Preparation: The surgeon meticulously cleans and prepares the exposed root surface and the surrounding gum tissue to create a healthy bed for the graft.
- Donor Tissue Harvesting (for Connective Tissue or Free Gingival Grafts): For these types, a small piece of tissue is carefully removed from the palate or another area. For pedicle grafts, the tissue is simply moved from an adjacent area. For ADM, the material is prepared from its sterile packaging.
- Graft Placement: The harvested or prepared graft tissue is precisely positioned over the exposed root surface and secured with very fine sutures.
- Suturing: The gum tissue at both the recipient and donor sites (if applicable) is carefully sutured.
Recovery Timeline and Aftercare
Recovery from dental grafts is a gradual process, and adherence to aftercare instructions is vital for success.
Immediate Aftercare (First few days to 1 week):
- Pain Management: Your dentist will prescribe pain medication or recommend over-the-counter options. Swelling and mild discomfort are normal.
- Swelling and Bruising: Apply ice packs to the outside of your face for the first 24-48 hours to minimize swelling. Bruising can occur but is usually mild.
- Bleeding: Slight oozing from the surgical site is normal. Apply gentle pressure with gauze if needed.
- Diet: Stick to soft, cool foods. Avoid hot, spicy, crunchy, or chewy foods that could irritate the surgical site or dislodge the graft.
- Oral Hygiene: Gently rinse with an antiseptic mouthwash (e.g., chlorhexidine) as prescribed, but avoid vigorous rinsing or spitting. Avoid brushing directly on the surgical site for a specified period (often 1-2 weeks), but maintain hygiene in other areas.
- Activity Restrictions: Avoid strenuous physical activity for several days to prevent increased bleeding or swelling.
- Avoid Smoking: Tobacco use severely compromises healing and significantly increases the risk of graft failure.
- Follow-up Appointments: Attend all scheduled follow-up visits so your surgeon can monitor healing and remove sutures if necessary.
Longer-Term Recovery (Weeks to Months):
- Bone Grafts:
- Initial healing of the soft tissue takes 1-2 weeks.
- Full integration of the bone graft material with your natural bone (osseointegration) can take anywhere from 3 to 9 months, depending on the graft type and individual healing capacity. During this time, the graft material is gradually replaced by new, healthy bone.
- Only after sufficient bone integration is confirmed (via X-rays or CBCT) can procedures like dental implant placement proceed.
- Gum Grafts:
- Initial healing of the soft tissue takes 2-4 weeks. The graft will gradually blend in with the surrounding gum tissue.
- Complete maturation and full integration of the grafted tissue can take several months. During this period, the blood supply to the graft establishes, and the tissue remodels.
- Protecting the treated area from aggressive brushing is a lifelong commitment.
Prevention Strategies
Preventing the need for dental grafts often boils down to excellent oral hygiene and proactive dental care.
- Maintain Excellent Oral Hygiene: Brush twice daily with a soft-bristled brush, paying attention to proper technique to avoid aggressive scrubbing. Floss daily to remove plaque and food debris between teeth and below the gumline.
- Regular Dental Check-ups and Cleanings: Professional cleanings remove hardened plaque (calculus) that at-home brushing can't. Regular exams allow your dentist to detect early signs of periodontal disease, gum recession, or bone loss.
- Prompt Treatment of Periodontal Disease: If diagnosed with gum disease, follow your dentist's or periodontist's treatment plan diligently to stop its progression and prevent further bone and gum loss.
- Address Tooth Loss Promptly: If a tooth needs extraction, discuss options like socket preservation and dental implants to prevent bone resorption.
- Quit Tobacco Use: Smoking and chewing tobacco are major risk factors for gum disease and impede healing, significantly increasing the likelihood of needing grafts.
- Manage Bruxism: If you grind or clench your teeth, wear a nightguard to protect your teeth and gums from excessive forces.
- Correct Malocclusion: Orthodontic treatment can correct misaligned teeth, reducing stress on gum tissues in certain areas.
- Avoid Lip and Tongue Piercings: These can cause chronic irritation and gum recession.
Cost Ranges in the US (with/without insurance)
Dental graft costs vary significantly based on the type of graft, the extent of the area being treated, the materials used, geographic location, and the specialist's fees. These figures are estimates and can fluctuate.

Bone Grafts:
- Socket Preservation (per tooth): $200 - $600 (often added to the extraction fee).
- Minor Bone Grafting (per site, e.g., ridge augmentation for a single implant): $300 - $1,500.
- Sinus Lift: $1,500 - $3,500 for a single sinus lift; $3,000 - $5,000+ for a bilateral sinus lift.
- Major Bone Grafting (e.g., block graft, extensive ridge augmentation): $1,500 - $3,000+ per site, potentially higher for very complex cases.
Gum Grafts:
- Per tooth/site: $400 - $2,500. The cost varies depending on the technique (connective tissue, free gingival, pedicle, or ADM) and the number of teeth being treated. Treating multiple adjacent teeth in one session can sometimes be more cost-effective per tooth.
Impact of Dental Insurance:
- Dental insurance coverage for grafts is highly variable. Some plans may cover a portion of the cost, especially if the graft is deemed medically necessary (e.g., to prevent further bone loss due to periodontal disease).
- Grafts performed as a prerequisite for cosmetic procedures or dental implants (which are often not fully covered by basic insurance) may have limited or no coverage.
- It is crucial to get a detailed treatment plan and pre-authorization from your insurance provider before proceeding to understand your out-of-pocket expenses. Many offices offer payment plans or third-party financing options.
For Parents / Pediatric Considerations
While less common than in adults, children and adolescents can sometimes require dental grafts for specific reasons.
- Bone Grafts in Children:
- Trauma: Accidents that lead to tooth loss or jaw fractures can necessitate bone grafting to restore proper bone volume for future tooth development or replacement.
- Congenital Defects: Children born with cleft lip and palate often require alveolar bone grafts to close the gap in the upper jaw, providing support for permanent teeth to erupt and enabling orthodontic treatment.
- Early Tooth Loss: If a primary (baby) tooth is lost prematurely due to trauma or decay, or if a permanent tooth is congenitally missing, bone preservation techniques may be considered to ensure adequate bone for future tooth eruption or implant placement in adulthood. However, dental implants are generally not placed until jaw growth is complete (late teens/early twenties).
- Gum Grafts in Children:
- Aggressive Brushing: Children can sometimes develop gum recession due to improper or overly aggressive brushing techniques.
- Orthodontic Treatment: In some cases, orthodontic tooth movement can exacerbate thin gum tissue, leading to localized recession.
- High Frenum Attachment: A prominent frenum (the band of tissue connecting the lip or cheek to the gum) can pull on the gum margin, causing recession, which may be corrected with a frenectomy, sometimes combined with a graft.
- Trauma: Injuries can directly damage gum tissue, leading to recession.
Pediatric dentists and orthodontists will carefully assess a child's growth and development before recommending any grafting procedure. The focus is always on long-term oral health and supporting the proper development of the permanent dentition and jaw structures.
Frequently Asked Questions
How much does a dental graft cost?
The cost of a dental graft in the US typically ranges from $200 to $2,500 per site for gum grafts and $200 to $5,000+ for bone grafts, depending on the type, size, complexity, and specific procedure (e.g., socket preservation vs. sinus lift). Prices vary significantly by geographic location and practitioner. Always get a detailed quote from your dental professional.
How painful is a dental graft procedure?
Dental graft procedures are performed under local anesthesia, so you should not feel pain during the surgery. Post-operatively, mild to moderate discomfort, swelling, and bruising are common. Your dentist or surgeon will prescribe pain medication or recommend over-the-counter options to manage any pain. Most patients find the recovery manageable, especially with proper medication and adherence to aftercare instructions.
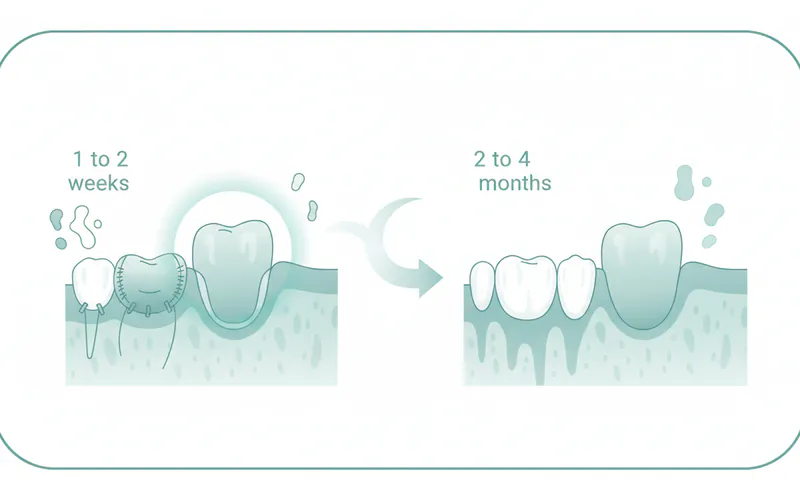
How long does the recovery from a dental graft take?
Initial healing of the soft tissue usually takes 1 to 2 weeks. For gum grafts, the grafted tissue will gradually mature and blend in over 2 to 4 weeks, with full integration taking several months. For bone grafts, while the initial discomfort subsides in a week or two, the actual bone regeneration and integration (osseointegration) process is much longer, typically 3 to 9 months, before the site is ready for further procedures like dental implant placement.
Are there alternatives to dental grafts?
Direct alternatives to grafting are limited if there is already significant bone or gum tissue loss. For bone loss, if you wish to have a dental implant, a bone graft is often necessary. Without sufficient bone, implant placement may not be possible or successful. For gum recession, a graft is the most effective way to cover exposed roots and prevent further loss. In some very minor cases of recession, careful oral hygiene changes might suffice, but they won't regrow lost tissue. The best "alternative" is prevention: excellent oral hygiene, regular dental check-ups, and prompt treatment of issues like periodontal disease.
Does dental insurance cover grafts?
Dental insurance coverage for grafts is highly variable. Some plans may cover a portion of the cost, especially if the graft is deemed medically necessary (e.g., to treat periodontal disease and prevent further deterioration). However, if the graft is a prerequisite for a dental implant or is primarily cosmetic, coverage may be limited or denied. It's essential to check with your insurance provider and get a pre-treatment estimate from your dental office.
How successful are dental grafts?
Dental grafts have a high success rate when performed by experienced specialists and when patients follow post-operative instructions. Bone grafts typically have a success rate of 90-95% for creating a suitable foundation for implants. Gum grafts also have a high success rate, often exceeding 90%, in achieving root coverage and enhancing gingival health. Factors like smoking, poor oral hygiene, and certain medical conditions can reduce success rates.
Can a dental graft fail?
Yes, while successful in the vast majority of cases, a dental graft can fail. Signs of failure can include infection at the graft site, dislodgment of the graft material, inadequate healing, or the body's rejection of the graft (rare with modern materials). Smoking is a significant risk factor for graft failure. If a graft fails, your dentist or surgeon will discuss further treatment options, which may include another grafting procedure.
What's the difference between a bone graft and a gum graft?
The main difference lies in the type of tissue being repaired and its purpose. A bone graft addresses deficiencies in the hard bone structure of the jaw, often to provide support for teeth or dental implants. A gum graft (or soft tissue graft) addresses deficiencies in the soft gingival tissue, typically to cover exposed tooth roots, reduce sensitivity, and protect against further recession.
When to See a Dentist
Routine Care & Prevention:
- Regular Check-ups: Visit your dentist every six months for comprehensive exams and cleanings. This allows for early detection of any signs of gum recession, bone loss, or developing periodontal disease.
- Persistent Sensitivity: If you notice new or increasing tooth sensitivity, especially to hot, cold, or sweets, it could be a sign of gum recession exposing tooth roots.
- "Longer" Looking Teeth: If your teeth appear elongated or if you can see more of their root surface, consult your dentist.
- Loose or Shifting Teeth: Any mobility in your teeth warrants immediate dental attention, as it can indicate significant bone loss.
- Considering Dental Implants: If you have missing teeth and are considering dental implants, your dentist will assess your bone quality and recommend if a bone graft is necessary.
- Post-Extraction Planning: If you are scheduled for a tooth extraction, discuss socket preservation options with your dentist to prevent future bone loss.
Emergency Signs (Post-Graft Procedure):
Contact your dentist or oral surgeon immediately if you experience any of the following after a graft procedure:
- Severe, uncontrolled pain that doesn't respond to prescribed medication.
- Excessive or persistent bleeding that doesn't stop with pressure.
- Significant swelling that worsens after 48 hours or impedes breathing/swallowing.
- Signs of infection: Pus, fever, severe redness, or foul taste/smell from the surgical site.
- Dislodged graft material or sutures coming out prematurely.
- Numbness or tingling that persists beyond the expected duration of the anesthesia.
Prompt attention to these signs is crucial for proper healing and preventing complications.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.