Abutment
4,921 words · 16 min read
Quick Definition
A tooth, root, or implant that serves as the support or anchor for a dental prosthesis such as a bridge, partial denture, or implant crown. The abutment connects the replacement tooth to the underlying structure.
Understanding the Abutment: Your Foundation for a Restored Smile
In the intricate world of dentistry, where precision meets artistry, the term abutment holds a foundational significance. Far from being a mere piece of dental jargon, an abutment is the unsung hero that supports and anchors a wide array of dental prostheses, connecting a replacement tooth or teeth to the underlying structure. Whether you're considering a dental implant, a bridge, or a partial denture, understanding what an abutment is and its crucial role is key to appreciating your restorative treatment.
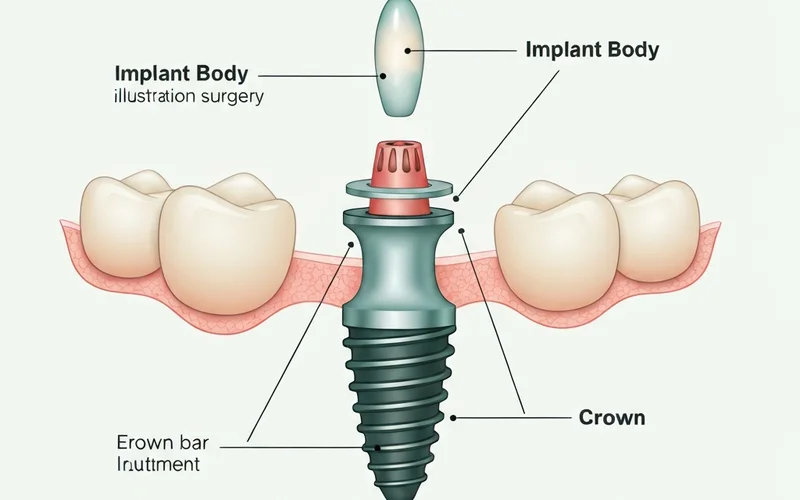
Essentially, an abutment is the natural tooth, root, or implant that acts as the sturdy base for a new dental device. It serves as the critical intermediary, transferring chewing forces and ensuring the stability of your new smile. This foundational component is vital for millions of Americans who have experienced tooth loss. In fact, over 178 million Americans are missing at least one tooth, and a staggering 35 million are missing all their teeth in one or both arches. These statistics underscore the widespread need for dental prostheses, and consequently, the critical function of abutments in restoring oral health, function, and aesthetics across the US. Without a robust abutment, the success and longevity of these restorative solutions would be significantly compromised.
Key Takeaways:
- An abutment is the essential supporting structure—a natural tooth, root, or dental implant—for a dental prosthesis like a bridge, crown, or implant-supported restoration.
- It acts as the crucial connection between the replacement tooth and your jawbone or existing teeth.
- Abutments ensure the stability, function, and longevity of dental prostheses.
- They are vital for anyone receiving a dental bridge, an implant-supported crown, or certain types of partial dentures.
- Proper care and maintenance of abutments are critical for the long-term success of your dental restorations.
- Abutments come in various types and materials, chosen specifically for your individual needs and the type of prosthesis.
Detailed Explanation of Abutments
The term "abutment" might sound technical, but its role in restoring your smile is quite straightforward: it's the anchor. Let's delve deeper into every aspect of this vital dental component.
Types and Classifications of Abutments
Abutments can be broadly categorized based on what they support, and their characteristics vary significantly depending on whether they are natural teeth or dental implants.
1. Natural Tooth Abutments
When a dental bridge or a removable partial denture is used to replace missing teeth, the healthy teeth adjacent to the gap often serve as natural tooth abutments. These teeth are prepared (usually by removing a small amount of enamel) to create space for the crowns that will anchor the prosthesis.
- For Dental Bridges: In a traditional bridge, the teeth on either side of the missing tooth (or teeth) are crowned. These abutment crowns are cemented onto the prepared natural teeth, and they hold the false tooth (pontic) in place.
- For Removable Partial Dentures-dentures-everything-you-need-to-know "Complete Guide to Prosthodontics & Dentures: Everything You Need to Know"): Clasps or precision attachments on the partial denture hook onto or fit into specific features on the natural teeth, which then act as abutments.
- Pros: Non-invasive to the abutment teeth compared to bridges (no grinding down required for clasps), more affordable.
- Cons: Less stable than fixed prostheses, can place uneven forces on abutment teeth over time, may accumulate plaque more easily.
2. Dental Implant Abutments
Perhaps the most recognized use of the term today, an implant abutment is the connector piece that screws into a dental implant (which is surgically placed into the jawbone) and extends above the gum line. This visible part then supports the final crown, bridge, or denture.
- Materials: Implant abutments are made from various biocompatible materials, each with specific advantages:
- Titanium: The most common material due to its strength, biocompatibility, and cost-effectiveness. Ideal for posterior teeth where aesthetics are less critical.
- Zirconia: A white ceramic material that offers superior aesthetics, making it ideal for anterior teeth (front teeth) where translucency and color matching are crucial. It's also very strong.
- Gold Alloy: Less common now, but historically used for its strength and ability to be custom cast. Can be visible through thinner gum tissue.
- PEEK (Polyetheretherketone): A high-performance polymer offering excellent shock absorption and lighter weight, sometimes used for temporary or specific clinical situations.
- Types of Implant Abutments:
- Standard (Stock) Abutments: These are pre-manufactured abutments available in various sizes, shapes, and angulations. They are cost-effective and suitable for many straightforward cases where there's enough gum tissue height and ideal implant positioning.
- Custom Abutments: These are custom-milled specifically for each patient's unique anatomy and restorative needs. They offer the best fit, emergence profile (how the crown emerges from the gum), and aesthetic outcome, especially for anterior teeth. They are typically made from zirconia or titanium.
- Angled Abutments: Used when the dental implant is placed at an angle due to bone availability, but the final restoration needs to be straight. The angled abutment corrects the trajectory, allowing for a properly aligned crown.
- Healing Abutments: These are temporary abutments placed on the dental implant after surgery. They shape the gum tissue as it heals, creating a natural emergence profile for the final crown. They are usually smooth, round, and slightly wider than the implant itself.
- Multi-Unit Abutments: Designed to support multiple teeth, often used for implant-supported bridges or full arch restorations (like "All-on-4"). They allow for the placement of implants at various angles while providing a common platform for the prosthesis.
- Ball/Locator Abutments: These are specialized abutments used to secure removable overdentures to dental implants, providing retention while still allowing the denture to be removed by the patient for cleaning.
Causes and Risk Factors Affecting Abutments
While an abutment is a critical component, its integrity can be compromised. The "causes" here refer to factors that lead to the need for an abutment, as well as risks to its health once in place.
Factors Leading to the Need for Abutments:
- Tooth Loss: The primary reason for needing abutments. This can be due to:
- Severe Decay: Extensive cavities that compromise tooth structure beyond repair.
- Periodontal Disease: Advanced gum disease leading to bone loss and tooth mobility.
- Trauma: Accidents or injuries that cause tooth fracture or avulsion (tooth knocked out).
- Congenital Anomalies: Missing teeth from birth.
- Failed Restorations: Previously failed crowns, bridges, or fillings that necessitate replacement with a more comprehensive solution.
Risk Factors for Abutment Complications:
- Poor Oral Hygiene: Plaque buildup around natural tooth abutments can lead to decay and gum disease, while around implant abutments it can cause peri-implantitis (gum disease around implants).
- Bruxism/Clenching: Excessive grinding or clenching of teeth can put immense stress on both natural and implant abutments, potentially leading to fractures, loosening of screws, or bone loss around implants.
- Smoking: Significantly increases the risk of peri-implantitis and reduces the healing capacity of tissues around implants, potentially leading to abutment failure.
- Systemic Diseases: Uncontrolled diabetes, autoimmune diseases, or conditions requiring medications that affect bone metabolism can compromise the success of implants and the health of natural tooth abutments.
- Insufficient Bone Density: For dental implants, inadequate bone quality or quantity at the implant site can affect initial stability and long-term success.
- Poorly Designed Prosthesis: An ill-fitting crown, bridge, or denture can place undue stress on the abutments, leading to complications.
- Improper Occlusion (Bite): An unbalanced bite can lead to excessive forces on specific abutments, causing wear, fracture, or loosening.
- Implant Overloading: Applying excessive chewing forces too soon after implant placement, or having too few implants supporting too many teeth.
Signs and Symptoms to Watch For
Recognizing issues with an abutment early can prevent more serious complications. Signs can vary depending on whether it's a natural tooth or an implant abutment.
For Natural Tooth Abutments (under a bridge or partial denture):
- Pain or Sensitivity: Persistent pain when biting, sensitivity to hot/cold, or a dull ache. This could indicate decay under the crown, nerve issues, or fracture of the abutment tooth.
- Gum Inflammation/Bleeding: Red, swollen, or bleeding gums around the abutment teeth. This often signals gum disease or an ill-fitting crown.
- Mobility of the Bridge/Denture: If the bridge feels loose, or the partial denture doesn't fit securely.
- Bad Breath or Taste: Persistent foul odor or metallic taste could indicate decay or infection.
- Visible Decay: Dark spots or holes visible around the margin of the crown where it meets the tooth.
- Loss of Cement: The bridge feels loose or comes off entirely due to cement washing out.
For Dental Implant Abutments:
- Pain or Discomfort: While some initial tenderness is normal after surgery, persistent or increasing pain around the implant site is a red flag.
- Swelling or Redness: Inflammation of the gum tissue around the implant abutment could indicate infection (peri-implantitis).
- Bleeding Gums: Gums bleeding easily when brushing or flossing around the abutment.
- Pus Discharge: A sign of active infection.
- Mobility of the Crown/Bridge/Denture: If the crown feels loose or wobbly, it could indicate a loose abutment screw, a fractured abutment, or even implant failure.
- Exposed Abutment/Implant Threads: If the gum tissue recedes, revealing parts of the abutment or even the implant threads, it's a sign of bone loss.
- Difficulty Chewing: Discomfort or inability to chew normally on the restored side.
Diagnosis Process — What Your Dentist Does
When you present with concerns about an abutment, your dentist will conduct a thorough examination to pinpoint the problem.
-
Clinical Examination:
- Visual Inspection: Your dentist will look for signs of inflammation, redness, swelling, pus, or recession around the abutment. They will also check the integrity of the prosthesis (e.g., condition of the crown on an abutment tooth, fit of a partial denture).
- Probing: A periodontal probe is used to measure pocket depths around natural tooth abutments or implant abutments. Increased depths can indicate gum disease or peri-implantitis.
- Palpation: Gently feeling the area for tenderness or swelling.
- Occlusal Assessment: Checking your bite (occlusion) to identify any areas of excessive force on the abutment or prosthesis.
- Mobility Test: Gently wiggling the crown or prosthesis to check for looseness.
-
Radiographic Evaluation (X-rays):
- Periapical X-rays: Provide detailed views of the tooth roots, surrounding bone, and the apex of the implant. They can reveal decay under crowns, bone loss around implants or natural teeth, and periapical lesions.
- Bitewing X-rays: Excellent for detecting interproximal (between teeth) decay on natural tooth abutments.
- Panoramic X-rays: Offer a broader view of the entire jaw, useful for assessing overall bone levels and identifying wider issues.
- CBCT (Cone Beam Computed Tomography) Scans: For dental implants, a 3D CBCT scan provides invaluable detailed information about bone density, bone volume, the position of the implant, and surrounding anatomical structures. This is particularly useful for diagnosing subtle issues like implant fracture or peri-implantitis.
-
Specialized Tests:
- Vitality Testing: For natural tooth abutments, an electric pulp tester or cold test can assess the vitality (health) of the tooth's nerve.
- Percussion/Palpation Tests: Tapping on the tooth/implant and feeling the surrounding tissues can help identify localized inflammation or infection.
- Photography: Documenting the condition for comparison and tracking progress.
Treatment Options with Pros, Cons, and Costs
Treatment for abutment issues depends entirely on the underlying problem and whether the abutment is natural or an implant.
A. Treatment for Natural Tooth Abutment Issues:
- Decay Under an Abutment Crown:
- Treatment: Remove the crown, treat the decay (filling or root canal if necessary), then fabricate and place a new crown.
- Pros: Preserves the natural tooth.
- Cons: Requires removal and replacement of the crown (and potentially the entire bridge), can be complex if decay is extensive.
- Cost: $800 - $3,000+ per tooth for root canal and new crown, plus removal of old bridge.
- Periodontal Disease (Gum Disease) Affecting Abutment Teeth:
- Treatment: Scaling and root planing (deep cleaning), antibiotic therapy, potentially periodontal surgery to reduce pocket depths or regenerate lost tissue.
- Pros: Can halt disease progression and save the abutment teeth.
- Cons: May require ongoing maintenance, significant tissue loss might persist.
- Cost: $200 - $1,500+ depending on severity and procedures (e.g., deep cleaning vs. surgery).
- Abutment Tooth Fracture:
- Treatment: Depending on the severity, may require a new crown, root canal, or extraction and replacement with a dental implant or a new bridge spanning an extra tooth.
- Pros: Can potentially save the tooth if fracture is minor.
- Cons: Major fractures often lead to tooth loss.
- Cost: Highly variable, $500 - $5,000+ depending on whether the tooth can be saved or needs replacement.
- Loose Bridge (Cement Washout):
- Treatment: If no decay, clean the crowns and abutment teeth, then re-cement the bridge. If decay is present, treat decay and potentially replace the bridge.
- Pros: Quick and relatively inexpensive if no underlying issues.
- Cons: Can be a recurring problem if bite issues or poor fit are not addressed.
- Cost: $100 - $400 for re-cementation, significantly more if a new bridge is needed.
B. Treatment for Dental Implant Abutment Issues:
- Loose Abutment Screw:
- Treatment: The dentist will access the screw through the crown (if it's an access hole crown) or remove the crown, then retighten or replace the abutment screw.
- Pros: Often a simple, quick fix.
- Cons: Can recur if bite issues are not corrected; may require a new crown if the access hole cannot be properly restored.
- Cost: $100 - $500 for screw tightening; up to $1,000 - $2,000+ if crown needs replacement.
- Peri-implantitis (Infection Around Implant):
- Treatment: Non-surgical (scaling, irrigation with antimicrobials) or surgical (debridement, bone graft, guided tissue regeneration) approaches.
- Pros: Can save the implant if caught early.
- Cons: Can be challenging to treat, may lead to implant failure if advanced.
- Cost: $300 - $3,000+ depending on severity and chosen treatment.
- Abutment Fracture:
- Treatment: Removal of the fractured abutment and replacement with a new one. This often requires fabricating a new crown as well.
- Pros: Implant itself may still be salvageable.
- Cons: Requires new prosthetic components, can be costly.
- Cost: $800 - $2,500+ for a new abutment and crown.
- Implant Failure (Mobility, Severe Bone Loss):
- Treatment: Removal of the failing implant, potentially bone grafting, and then replacement with a new implant after a healing period.
- Pros: Allows for a fresh start with a new, healthy implant.
- Cons: Invasive, time-consuming, costly.
- Cost: $1,500 - $6,000+ for removal, bone graft, and new implant placement.
Comparison Table: Natural Tooth vs. Dental Implant Abutments
| Feature | Natural Tooth Abutment | Dental Implant Abutment |
|---|---|---|
| Supporting Structure | Healthy adjacent tooth/root | Surgically placed titanium (or zirconia) implant |
| Primary Prosthesis | Dental Bridge, Removable Partial Denture | Implant Crown, Implant Bridge, Overdenture |
| Tooth Preparation | Often requires irreversible enamel reduction | No preparation of adjacent natural teeth |
| Bone Health Impact | Does not directly stimulate bone, may be stressed | Preserves jawbone by mimicking a natural root, stimulates bone |
| Long-term Health | Susceptible to decay, nerve issues, periodontal disease | Susceptible to peri-implantitis, screw loosening |
| Esthetics | Good, but requires intact natural teeth | Excellent, especially with custom zirconia abutments |
| Cost (Abutment only) | Cost is integrated into crown or bridge price | $300 - $1,500+ (excluding implant & crown) |
| Longevity | 5-15 years for bridges | 15-25+ years for implants (with proper care) |
| Removability | Fixed (bridge), or removable (partial denture) | Fixed (crown/bridge), or removable (overdenture) |
Step-by-Step: What to Expect During Treatment
The treatment process for an abutment issue will vary widely based on the specific problem and the type of abutment. However, here's a general overview:
For Natural Tooth Abutment Restoration (e.g., new bridge):
- Preparation: The abutment teeth are carefully reshaped, usually by removing a small amount of enamel, to create space for the crowns.
- Impressions: Digital or traditional impressions are taken of your prepared teeth and bite. These are sent to a dental lab.
- Temporary Bridge: A temporary bridge or crowns are placed to protect the prepared teeth while your custom prosthesis is being fabricated.
- Lab Fabrication: A dental lab creates your permanent bridge (including its abutment crowns) from materials like porcelain, zirconia, or metal alloys. This can take 1-3 weeks.
- Placement: Once ready, the temporary bridge is removed, and the new permanent bridge is carefully fitted and cemented onto your abutment teeth. Adjustments are made to ensure a comfortable bite.
For Dental Implant Abutment and Crown Placement:
- Implant Placement (Prior Step): This precedes abutment placement. A dental implant (titanium screw) is surgically placed into your jawbone. This requires a healing period of 3-6 months for osseointegration (bone fusing with the implant).
- Abutment Connection: Once the implant has fully integrated with the bone, a small incision is made in the gum (if needed) to expose the top of the implant. The implant abutment is then screwed securely into the implant.
- Note: Sometimes, the abutment is placed simultaneously with the implant (one-stage surgery), or a temporary healing abutment is placed initially to shape the gums.
- Healing Period (if healing abutment used): If a healing abutment was placed, the gums will heal around it, forming a natural contour. This typically takes 2-4 weeks.
- Impressions: Once the gum is healed and shaped, impressions (digital or traditional) are taken of the abutment and surrounding teeth. This ensures the final crown or bridge fits perfectly.
- Lab Fabrication: A dental lab meticulously crafts your custom crown or bridge to sit perfectly on the abutment. This also takes 1-3 weeks.
- Final Placement: The temporary restoration (if any) is removed, and your custom crown or bridge is attached to the implant abutment – either cemented or screwed in place. Final bite adjustments are made.
!Diagram showing a dental implant, with the implant body in the bone, the abutment screwed into the implant, and the crown cemented onto the abutment.
Recovery Timeline and Aftercare
Recovery:
- Natural Tooth Abutments: Initial sensitivity to hot/cold or pressure after bridge placement is common and usually subsides within a few days to a couple of weeks. Minor gum irritation can also occur.
- Dental Implant Abutments:
- Abutment Placement: Mild discomfort, swelling, and sensitivity are common for 1-3 days. Pain relievers (over-the-counter or prescription) can manage this.
- Crown Placement: Generally, no significant recovery is needed after the final crown is placed, other than adapting to the new bite.
Aftercare:
Regardless of the type, excellent oral hygiene is paramount for the longevity of your abutments and prostheses.
- Brushing: Brush at least twice a day with a soft-bristled toothbrush. Pay special attention to the areas where the crown or prosthesis meets the gum line.
- Flossing: Floss daily. For bridges, special floss threaders or super floss are necessary to clean underneath the pontic (false tooth) and around the abutment teeth/implants. For implants, non-abrasive floss or implant-specific brushes are recommended.
- Interdental Brushes: Small brushes can effectively clean around implant abutments and under bridges.
- Mouthwash: An antimicrobial mouthwash can help reduce bacteria, especially if recommended by your dentist.
- Regular Dental Check-ups: Visit your dentist every 6 months (or as recommended) for professional cleanings and examinations. Your dentist will monitor the health of your abutments, prosthesis, and surrounding tissues.
- Avoid Hard/Sticky Foods: Especially immediately after placement, and generally for all prostheses, to prevent damage.
- Manage Bruxism: If you grind or clench your teeth, a nightguard can protect your abutments and prostheses from excessive force.
!Side-by-side comparison of proper flossing technique for a natural tooth abutment under a bridge (using a floss threader) and cleaning an implant abutment with an interdental brush.
Prevention Strategies
Preventing abutment issues primarily focuses on preventing the conditions that necessitate them (tooth loss) and maintaining the health of existing abutments.
- Excellent Oral Hygiene: The foundation of all dental health. Brush and floss diligently to prevent decay and gum disease, which are major threats to natural tooth abutments. For implants, strict hygiene prevents peri-implantitis.
- Regular Dental Check-ups and Cleanings: Professional cleanings remove hardened plaque (calculus) that brushing can miss. Examinations can detect issues early.
- Protective Gear: Wear a mouthguard during contact sports to prevent traumatic tooth loss.
- Address Bruxism: If you clench or grind your teeth, a custom-fitted nightguard can protect your natural teeth and dental implants from excessive forces.
- Healthy Diet: Limit sugary and acidic foods and drinks that contribute to tooth decay.
- Avoid Tobacco Products: Smoking is a significant risk factor for gum disease, decay, and especially peri-implantitis, greatly increasing the chances of implant failure.
- Treat Systemic Conditions: Manage diabetes and other chronic diseases as they can impact oral health and the success of dental treatments.
- Prompt Treatment of Dental Issues: Don't delay treating cavities or gum disease; addressing them early can save natural teeth that might otherwise become abutments.
Cost Ranges in the US (with/without Insurance)
The cost of abutments is usually part of the overall cost of the restorative treatment (bridge, crown, or implant). It's challenging to give an exact figure, as prices vary widely based on location (major cities often cost more), the dentist's experience, the materials used, and the complexity of the case.
For Natural Tooth Abutments:
- The cost of the abutment itself is integrated into the cost of the crowns that go over them.
- Dental Bridge (3-unit, replacing one tooth):
- Without Insurance: $2,000 - $5,000+
- With Insurance: $500 - $2,500+ (insurance typically covers 20-80% of bridge costs after deductible, depending on plan)
For Dental Implant Abutments:
- The implant abutment is a distinct component with its own cost.
- Abutment Only:
- Without Insurance: $300 - $1,500+ (stock abutments are on the lower end, custom zirconia abutments on the higher end).
- Full Dental Implant Procedure (including implant post, abutment, and crown):
- Without Insurance: $3,000 - $6,000+ per tooth.
- Implant post: $1,500 - $3,000
- Abutment: $300 - $1,500
- Crown: $1,000 - $2,500
- With Insurance: $1,500 - $4,000+ per tooth. (Many plans still consider implants cosmetic or only partially cover them; some newer plans are offering better coverage, often 20-50% after deductible up to an annual maximum).
- Without Insurance: $3,000 - $6,000+ per tooth.
- Associated Costs: Bone grafts ($200 - $2,000+), sinus lifts ($1,500 - $3,000+), extractions ($75 - $400+), and temporary restorations can add to the total cost.
It is always advisable to get a detailed treatment plan and cost estimate from your dentist, including a breakdown of what your insurance may cover.
For Parents / Pediatric Considerations
While the term "abutment" primarily applies to adult restorative dentistry, parents should be aware of factors that can lead to the need for abutments in adulthood:
- Early Tooth Loss in Children: Premature loss of primary (baby) teeth due to decay or trauma can affect the eruption of permanent teeth and lead to spacing issues, potentially requiring prostheses later in life.
- Congenitally Missing Teeth: Some children are born without certain permanent teeth (a condition called hypodontia). This often necessitates future prosthetic solutions like bridges or dental implants (once jaw growth is complete, typically late teens/early twenties), where abutments will be crucial.
- Trauma: Injuries to the mouth in childhood can damage permanent teeth, potentially leading to their loss and the need for restorations supported by abutments later.
- Orthodontic Considerations: Early orthodontic intervention can sometimes manage spacing issues related to missing teeth, potentially reducing the complexity of future restorative needs.
Encouraging excellent oral hygiene, regular dental visits, and wearing mouthguards for sports are the best ways to preserve natural teeth and minimize the future need for complex restorative treatments involving abutments.
Frequently Asked Questions
Q1: How much does a dental abutment cost?
A: The cost of a dental abutment itself, particularly for dental implants, typically ranges from $300 to $1,500+ in the US without insurance. This price can vary based on the material (e.g., titanium vs. custom zirconia) and the specific design. For natural tooth abutments, their cost is usually bundled into the overall price of the crown or bridge that is placed on them. The total cost of an implant-supported crown (including the implant, abutment, and crown) can range from $3,000 to $6,000+.
Q2: Is getting an abutment painful?
A: If a natural tooth is being prepared for an abutment crown for a bridge, local anesthetic will be used, so you should feel no pain during the procedure. There might be some soreness or sensitivity afterward. For dental implants, the abutment is usually placed after the implant has healed and integrated into the bone. This procedure is generally not painful as the area is numbed with local anesthesia. You may experience mild discomfort or soreness for a day or two after, which can be managed with over-the-counter pain relievers.
Q3: How long does an abutment last?
A: An abutment is designed to last as long as the prosthesis it supports. For natural tooth abutments, their longevity depends on the health of the tooth, surrounding gums, and proper oral hygiene – ideally, a bridge can last 5-15 years. For dental implants, the implant abutment itself is extremely durable and, with proper care and maintenance, can last 15-25 years or even a lifetime, just like the implant post. The crown on top of it may need replacement every 10-15 years.
Q4: Are there alternatives to using an abutment?
A: Yes, the need for an abutment arises when you have missing teeth and choose a fixed prosthetic solution. Alternatives for missing teeth include:
- Removable Partial or Full Dentures: These prostheses replace missing teeth but are not fixed to abutments (though partial dentures may use clasps on natural teeth).
- No Treatment: This is generally not recommended as it can lead to shifting teeth, bite problems, and bone loss.
- Orthodontic Treatment: For some minor gaps, orthodontics might close the space, eliminating the need for a prosthetic.
- However, if you want a fixed solution (like a crown or bridge), an abutment is an integral and necessary component.
Q5: Does dental insurance cover abutment costs?
A: Dental insurance coverage for abutment costs varies widely.
- For natural tooth abutments as part of a bridge, many standard dental insurance plans will cover 50-80% of the cost after your deductible, up to your annual maximum.
- For dental implant abutments, coverage is more complex. Historically, implants were often considered cosmetic and not covered. However, more plans are beginning to cover a portion of implant procedures. Coverage typically ranges from 20-50% for the implant components (including the abutment and crown), but it's essential to check with your specific provider regarding their policy on dental implants. Pre-authorization is always recommended.
Q6: Can an abutment get infected?
A: Yes, both natural tooth abutments and implant abutments can be susceptible to infection.
- Natural tooth abutments can develop decay under the crown or suffer from gum disease (periodontitis) if oral hygiene is poor.
- Implant abutments can be affected by peri-implantitis, an inflammatory condition similar to gum disease that affects the tissues around a dental implant, potentially leading to bone loss and implant failure if not treated. Good oral hygiene and regular dental check-ups are crucial for prevention.
Q7: What is the difference between an implant and an abutment?
A: A dental implant is the small, screw-shaped post (usually titanium) that is surgically placed directly into the jawbone, acting as an artificial tooth root. It is the foundation that integrates with your bone. The abutment, on the other hand, is the connector piece that attaches to the top of the dental implant and extends above the gum line. It's what the final crown, bridge, or denture will be secured to. Think of the implant as the "root" and the abutment as the "stump" that the "new tooth" (prosthesis) sits on.
When to See a Dentist
It's always best to be proactive about your dental health. Here's when you should definitely see a dentist regarding abutments:
- Emergency Signs:
- Sudden, severe pain around a natural tooth or dental implant.
- Significant swelling or pus discharge around a prosthesis or implant.
- Mobility or complete dislodgement of a crown, bridge, or dental implant.
- Trauma to the mouth affecting a prosthesis or abutment.
- Persistent bleeding from the gums around an abutment.
- Routine Care & Concerns:
- Any persistent discomfort or sensitivity in an abutment tooth or implant site.
- Red, swollen, or tender gums around a prosthesis.
- Bad breath or a metallic taste that doesn't go away with brushing.
- Difficulty chewing or a change in your bite.
- Visible changes like gum recession around an implant or dark spots/gaps around a crown.
- Regular check-ups and cleanings are crucial for monitoring the health of all your dental work, including abutments. Your dentist can identify potential issues before they become emergencies.
dental abutmentimplant abutmentbridge abutmentabutment toothimplant connector
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.