Impaction
4,235 words · 14 min read
Quick Definition
A condition where a tooth fails to fully emerge through the gums into its normal position, often because it is blocked by bone, other teeth, or dense soft tissue.
Impaction: A Comprehensive Guide to Understanding Blocked Teeth
Welcome to SmilePedia.net, your definitive resource for dental health information. This in-depth guide will demystify impaction, a common dental condition that affects millions of Americans. Whether you’re experiencing discomfort, researching a diagnosis, or simply seeking to understand more about your oral health, you’ve come to the right place.
Impaction is a condition where a tooth fails to fully emerge through the gums into its normal position, often because it is blocked by bone, other teeth, or dense soft tissue. This means the tooth remains partially or completely embedded within the jawbone or under the gum line, unable to erupt into its proper alignment and function.
Understanding impaction is crucial for maintaining good dental health. An impacted tooth, if left untreated, can lead to a host of problems including pain, infection, damage to adjacent teeth, and even more serious oral health complications. While any tooth can become impacted, the wisdom teeth (or third molars) are by far the most commonly affected. In fact, studies suggest that up to 80% of adults will experience at least one impacted wisdom tooth during their lifetime, making it one of the most frequent reasons for dental extraction. Other teeth, such as canines (cuspids) and premolars, can also become impacted, though less frequently.
Key Takeaways:
- An impacted tooth fails to fully erupt into its normal position in the mouth.
- Wisdom teeth are the most commonly impacted teeth, affecting up to 80% of adults.
- Impaction can cause pain, infection, gum disease, cysts, and damage to adjacent teeth.
- Diagnosis typically involves a clinical exam and dental X-rays.
- Treatment often involves surgical extraction, but monitoring or orthodontics can also be options for certain types of impaction.
- Early detection is key to preventing complications.
Detailed Explanation
Understanding the nuances of impaction is essential for proper diagnosis and treatment. This section will delve into the various aspects of this condition, from its classifications to its management.
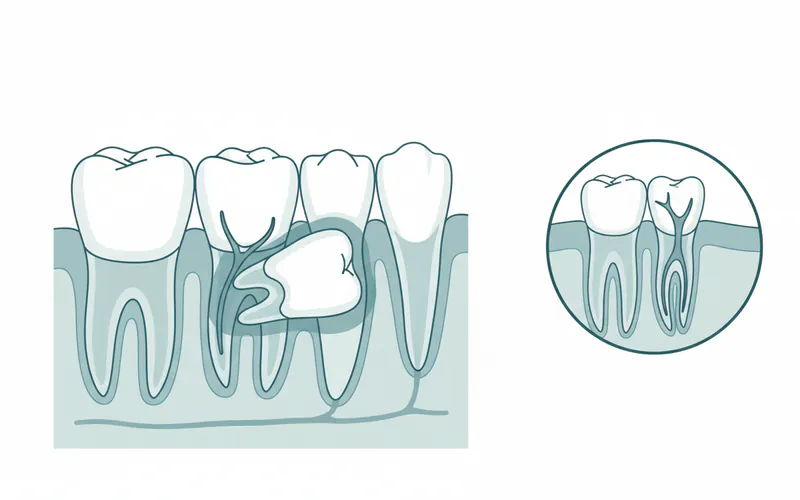
Types and Classifications of Impaction
Impaction can be classified in several ways, primarily by the type of tooth involved, its angulation, and the amount of surrounding tissue that covers it.
1. By Tooth Type:
- Wisdom Teeth (Third Molars): These are the most frequently impacted teeth. Located at the very back of the mouth, they are the last teeth to erupt, typically between the ages of 17 and 25. Often, there isn't enough room in the jaw for them to emerge properly.
- Canines (Cuspids): Upper canines are the second most common teeth to be impacted. These "eyeteeth" are critical for biting and tearing food and play a significant role in facial aesthetics. If they don't erupt by age 13-14, impaction is a concern.
- Premolars: Less commonly, the first or second premolars can also become impacted.
- Supernumerary Teeth: These are extra teeth that can develop in the mouth and block the eruption path of normal teeth, leading to impaction.
2. By Angulation (primarily for Wisdom Teeth): The way an impacted wisdom tooth is angled within the jaw can significantly influence the difficulty of its extraction and the potential for complications.
- Mesial Impaction: The most common type, where the tooth is angled forward, towards the front of the mouth, pressing against the second molar.
- Vertical Impaction: The tooth is oriented correctly (upright) but is still unable to erupt due to lack of space or obstruction.
- Horizontal Impaction: The tooth lies completely sideways, usually pressing against the root of the adjacent second molar. This is often the most problematic type.
- Distal Impaction: The least common type, where the tooth is angled backward, towards the rear of the jaw.
3. By Depth and Tissue Coverage: This classification describes how much of the impacted tooth is covered by gum tissue or bone.
- Soft Tissue Impaction: The tooth is covered only by gum tissue. This is often the easiest type to extract, but still prone to infection (pericoronitis).
- Partial Bony Impaction: The tooth is partially covered by both gum tissue and jawbone. This typically requires minor bone removal during extraction.
- Full Bony Impaction: The tooth is completely encased within the jawbone, fully covered by both bone and gum tissue. This is generally the most complex type to remove, requiring significant bone removal.
Causes and Risk Factors
The primary reason for impaction is a mismatch between the size of the teeth and the size of the jawbone. When there isn't enough room for a tooth to erupt into its proper position, it becomes blocked.
Key causes and risk factors include:
- Lack of Jaw Space: Modern diets and genetics may contribute to smaller jaw sizes compared to our ancestors, making proper eruption of all 32 adult teeth (including four wisdom teeth) challenging.
- Genetic Predisposition: Jaw size, tooth size, and eruption patterns can be inherited, making some individuals more prone to impaction.
- Obstruction by Other Teeth: The presence of adjacent teeth can physically block the eruption path of another tooth.
- Abnormal Tooth Development or Angulation: Sometimes, a tooth forms at an unusual angle, making normal eruption impossible.
- Dense Bone Tissue: Overly dense jawbone can present a formidable barrier to tooth eruption.
- Early Loss or Retention of Primary Teeth: In children, the premature loss of a baby tooth or, conversely, its over-retention can affect the eruption path of the underlying permanent tooth.
- Cysts or Tumors: Rarely, a cyst or tumor can form around an unerupted tooth, blocking its path.
Signs and Symptoms to Watch For
A significant challenge with impacted teeth is that they are often asymptomatic, meaning they cause no noticeable symptoms for extended periods. This is why regular dental check-ups and X-rays are crucial for early detection. However, when symptoms do arise, they can range from mild discomfort to severe pain and infection.
Common signs and symptoms include:
- Pain or Tenderness: Localized pain in the jaw or gums, especially at the back of the mouth, or a dull, throbbing ache that can radiate to the ear or temple.
- Red, Swollen, or Bleeding Gums: Inflammation and irritation of the gum tissue around the impacted or partially erupted tooth.
- Bad Breath (Halitosis) or Unpleasant Taste: Food particles and bacteria can easily get trapped under the gum flap covering a partially erupted tooth, leading to infection and foul odor. This condition is known as pericoronitis.
- Difficulty Opening Mouth (Trismus): Inflammation or infection can lead to muscle spasms, making it painful or difficult to fully open the jaw.
- Swelling Around the Jaw: Visible swelling on the outside of the jaw or cheek.
- Headaches, Earaches, or Facial Pain: Pain can be referred from the impacted tooth to other areas of the head and face.
- Crowding of Adjacent Teeth: An impacted tooth pushing against neighboring teeth can cause them to shift, leading to misalignment or crowding.
- Cyst Formation: In rare cases, a fluid-filled sac (dentigerous cyst) can develop around the crown of an impacted tooth, potentially damaging bone, teeth, and nerves.
Diagnosis Process — What Your Dentist Does
Diagnosing an impacted tooth is typically straightforward and involves a combination of a clinical examination and diagnostic imaging.
- Clinical Oral Examination: Your dentist will visually inspect your mouth, checking for signs of inflammation, swelling, or any visible portion of an erupting tooth. They will ask about any symptoms you're experiencing, your medical history, and your oral hygiene habits.
- Dental X-rays: This is the most crucial diagnostic tool.
- Panoramic X-ray: This type of X-ray provides a comprehensive view of your entire mouth, including all teeth (erupted and unerupted), jawbones, and temporomandibular joints. It's excellent for identifying the presence, position, and angulation of impacted teeth, especially wisdom teeth.
- Periapical X-rays: These provide detailed images of individual teeth and their surrounding bone, which can be useful for assessing specific impacted teeth.
- Cone Beam Computed Tomography (CBCT): For complex cases, especially those involving close proximity to nerves or other critical structures, a 3D CBCT scan may be recommended. This provides a highly detailed, three-dimensional view of the impacted tooth and its surrounding anatomy, aiding in precise surgical planning.
Based on these findings, your dentist will determine the type of impaction, assess potential risks, and discuss appropriate treatment options.
Treatment Options with Pros, Cons, and Costs
The treatment for an impacted tooth depends on several factors, including the type of impaction, the tooth involved, the presence and severity of symptoms, and the patient's overall health and age.
1. Monitoring/Observation (Watchful Waiting)
- Description: For asymptomatic impacted teeth that pose a low risk of future problems, your dentist may recommend regular check-ups and X-rays to monitor the tooth's status.
- Pros: Avoids surgical intervention and its associated risks and recovery time.
- Cons: The tooth could still develop problems later, necessitating future extraction or treatment. Potential for silent damage to adjacent teeth or bone.
- Typical Cost (US$): Cost of regular dental check-ups, typically $50 - $200 per visit, plus X-ray fees.
2. Surgical Extraction
- Description: This is the most common treatment for problematic impacted teeth, especially wisdom teeth. It involves a surgical procedure to remove the tooth from the jawbone.
- Pros: Resolves pain and infection, prevents future complications, eliminates the source of potential damage to adjacent teeth or bone.
- Cons: It's an invasive surgical procedure with a recovery period and potential risks (e.g., nerve damage, dry socket, infection, swelling, bleeding).
- Typical Cost (US$): Highly variable depending on the complexity of the impaction, the number of teeth, type of anesthesia, and geographical location.
- Soft Tissue Impaction: $200 - $750 per tooth.
- Partial Bony Impaction: $300 - $850 per tooth.
- Full Bony Impaction: $400 - $1,100+ per tooth.
- Anesthesia (sedation/general): An additional $100 - $500 per hour.
- Total for all four wisdom teeth (surgical): $1,000 - $4,000+ without insurance.
3. Orthodontic Treatment (Exposure and Bonding)
- Description: Primarily used for impacted canines, this treatment involves a minor surgical procedure to expose the impacted tooth, followed by orthodontic braces to gently guide it into its proper position in the dental arch.
- Pros: Saves the natural tooth, improves aesthetics and chewing function, maintains proper occlusion (bite).
- Cons: A lengthy treatment process involving multiple stages and appointments. Can be more expensive than extraction due to the combined surgical and orthodontic costs. Not suitable for all impacted teeth.
- Typical Cost (US$):
- Surgical Exposure: $200 - $600 per tooth.
- Full Orthodontic Treatment: $3,000 - $8,000 (this cost covers the entire braces treatment, including the impacted tooth's guidance).
Comparison of Treatment Options
| Treatment Option | Description | Pros | Cons | Typical Cost (per tooth, US$) |
|---|---|---|---|---|
| Monitoring | Regular check-ups for asymptomatic, low-risk impactions | Avoids surgery, no recovery time | Potential for future problems, silent damage | ~$50 - $200 (per visit) |
| Surgical Extraction | Surgical removal of the impacted tooth, often involving bone and tissue removal | Resolves pain, prevents infection/damage, definitive | Invasive, recovery period, potential risks (e.g., dry socket, nerve damage) | ~$200 - $1,100+ (plus anesthesia) |
| Orthodontic Exposure & Bonding | Surgical exposure followed by braces to guide the tooth into alignment | Saves natural tooth, improves aesthetics and function | Lengthy process, multiple procedures, higher overall cost, not for all teeth | ~$200 - $600 (exposure) + ~$3,000 - $8,000 (full ortho) |
| `` |
Step-by-Step: What to Expect During Treatment (Focus on Surgical Extraction)
For most impacted teeth, particularly wisdom teeth, surgical extraction is the recommended course of action. Here’s a general overview of what to expect:
1. Pre-Procedure Consultation:
- Your dentist or oral surgeon will review your X-rays and CBCT scans (if taken) to plan the procedure.
- They will discuss your medical history, medications, and any allergies.
- Anesthesia options will be presented:
- Local Anesthesia: Numbing the area around the tooth. You remain awake.
- Sedation (IV Sedation/Conscious Sedation): You'll be relaxed and drowsy, often with little memory of the procedure.
- General Anesthesia: You'll be completely asleep. Often used for multiple complex extractions or anxious patients.
- You'll receive instructions regarding fasting (if sedation or general anesthesia is used) and pre-operative medications.
2. During the Procedure:
- You'll be made comfortable in the dental chair.
- The chosen anesthesia will be administered.
- Once numb or sedated, the surgeon will make an incision in the gum tissue to access the impacted tooth.
- If the tooth is covered by bone (partial or full bony impaction), a small amount of bone may need to be carefully removed.
- Often, the tooth is sectioned into smaller pieces to facilitate easier and less traumatic removal.
- The tooth fragments are removed, and the socket is thoroughly cleaned to ensure no debris or infection remains.
- The gum tissue is then repositioned and sutured (stitched) back together. Sometimes dissolvable sutures are used; otherwise, they'll need to be removed at a follow-up appointment.
- Gauze is placed over the extraction site to help control bleeding and promote clot formation.
3. Post-Procedure:
- You'll remain under observation until the effects of anesthesia wear off sufficiently.
- You'll receive detailed aftercare instructions and prescriptions for pain medication and possibly antibiotics.
- Someone will need to drive you home if you received sedation or general anesthesia.
``
Recovery Timeline and Aftercare
Proper aftercare is crucial for a smooth and quick recovery, and to prevent complications like dry socket.
Recovery Timeline:
- First 24 Hours: Expect some bleeding, swelling, and mild to moderate pain. The blood clot is forming, which is vital for healing.
- Days 2-3: Swelling usually peaks during this period. Discomfort should start to subside with pain medication.
- Day 7: If non-dissolvable sutures were used, they might be removed. Most acute symptoms like significant pain and swelling should have greatly diminished.
- 2-4 Weeks: The soft tissue around the extraction site should be largely healed. You can typically return to most normal activities.
- Several Months: The jawbone will continue to remodel and fill in the extraction site. Full bone healing takes longer.
Aftercare Instructions:
- Control Bleeding: Bite gently but firmly on the gauze pads for 30-60 minutes, changing them as needed. If bleeding persists, use a clean, moist tea bag (tannic acid helps clotting).
- Manage Pain: Take prescribed pain medication as directed. Over-the-counter pain relievers (e.g., ibuprofen, acetaminophen) can supplement.
- Reduce Swelling: Apply ice packs to the outside of your cheek for 20 minutes on, 20 minutes off for the first 24-48 hours.
- Soft Diet: Stick to soft foods for the first few days (e.g., yogurt, mashed potatoes, soup, smoothies). Gradually introduce firmer foods as comfort allows.
- Avoid Suction: DO NOT use straws, spit forcefully, or smoke for at least 48-72 hours as this can dislodge the blood clot and lead to dry socket.
- Oral Hygiene:
- DO NOT rinse your mouth for the first 24 hours.
- After 24 hours, gently rinse your mouth with warm salt water (1/2 teaspoon salt in 8 ounces warm water) several times a day, especially after meals.
- Brush your other teeth gently, avoiding the extraction site.
- Rest: Get plenty of rest and avoid strenuous activity for several days.
- Follow-Up: Attend all scheduled follow-up appointments with your dentist or oral surgeon.
Prevention Strategies
While it's difficult to completely prevent impaction, especially of wisdom teeth, certain measures can help identify potential issues early or manage other types of impaction.
- Regular Dental Check-ups with X-rays: This is the most effective prevention strategy. Dentists can monitor the development and eruption of teeth over time. Panoramic X-rays taken in the mid-to-late teenage years are crucial for assessing wisdom tooth development and potential impaction.
- Early Orthodontic Evaluation: For children, an orthodontic evaluation around age 7-8 can identify jaw size discrepancies or potential eruption problems (especially with canines or premolars). Early orthodontics (interceptive treatment) might create space for proper tooth eruption, sometimes preventing impaction.
- Addressing Over-retained Primary Teeth: If a baby tooth doesn't fall out on time and is blocking a permanent tooth's eruption, your dentist may recommend extracting the primary tooth.
Cost Ranges in the US (with/without insurance)
The cost of treating an impacted tooth in the United States can vary significantly based on several factors, including:
- Type and Complexity of Impaction: As discussed, a soft tissue impaction is less expensive than a full bony impaction.
- Number of Teeth Removed: Removing all four wisdom teeth in one sitting is typically more cost-effective than separate procedures.
- Type of Anesthesia: Local anesthesia is less expensive than IV sedation or general anesthesia.
- Geographical Location: Dental costs can vary significantly by state, city, and even neighborhood.
- Provider: Costs can differ between a general dentist and an oral surgeon.
Typical Costs (without insurance):
- Impacted Wisdom Tooth Extraction:
- Soft Tissue Impaction: $200 - $750 per tooth
- Partial Bony Impaction: $300 - $850 per tooth
- Full Bony Impaction: $400 - $1,100+ per tooth
- Anesthesia fees (e.g., IV sedation): Additional $100 - $500 per hour.
- Total for all four wisdom teeth (surgical): $1,000 - $4,000+
- Impacted Canine Exposure and Bonding:
- Surgical Exposure (performed by an oral surgeon or periodontist): $200 - $600 per tooth.
- Orthodontic Treatment (braces): $3,000 - $8,000 for the full course of treatment.
With Dental Insurance: Most dental insurance plans in the US offer coverage for impacted tooth extraction or orthodontic procedures, especially if they are deemed medically necessary (e.g., preventing infection, pain, or damage).
- Coverage Levels: Typically, insurance may cover 50% to 80% of the procedure cost after your deductible is met.
- Deductibles: You will usually need to pay an upfront deductible (e.g., $50 - $200) before insurance begins to cover costs.
- Annual Maximums: Most plans have an annual maximum benefit (e.g., $1,000 - $2,000), which you might exceed if you have multiple complex extractions or extensive orthodontic work.
- Orthodontic Coverage: Orthodontics often has separate, lower coverage limits or may only be covered for children under a certain age. It's crucial to contact your insurance provider beforehand to understand your specific benefits, deductibles, co-pays, and annual maximums. Your dental office can also help you with a pre-treatment estimate.
For Parents / Pediatric Considerations
Impaction isn't just an adult concern. While wisdom teeth are typically an adolescent or adult issue, parents should be aware of impaction possibilities for their children's permanent teeth.
- Early Orthodontic Assessment: The American Association of Orthodontists recommends that children have their first orthodontic evaluation by age 7. At this age, a dentist or orthodontist can assess jaw growth, tooth eruption patterns, and identify potential issues that could lead to impaction, particularly with permanent canines or premolars.
- Monitoring Eruption: Dentists will monitor the eruption of permanent teeth during routine check-ups. If a tooth seems delayed or is not emerging in its proper sequence, an X-ray can confirm if it's impacted or blocked.
- Space Management: In some cases, interceptive orthodontics may involve using appliances to create space in the jaw for teeth to erupt properly, potentially preventing the need for extraction later.
- Supernumerary Teeth: Children can sometimes develop extra teeth (supernumerary teeth) that can block the eruption of normal permanent teeth. These are often identified on X-rays and may need to be removed.
- Impacted Canines: Canines are particularly important for facial aesthetics and chewing. If an upper canine is impacted, early intervention with surgical exposure and orthodontics often yields the best results, guiding the tooth into its correct position and preserving the natural tooth. Delaying treatment can make it more difficult or even impossible to bring the canine into alignment.
Frequently Asked Questions
Q1: How much does it cost to remove an impacted tooth?
A: The cost varies significantly based on the complexity of the impaction, the type of anesthesia used, and your geographical location. Without insurance, a single impacted wisdom tooth extraction can range from $200 for a soft tissue impaction to over $1,100 for a full bony impaction. If all four wisdom teeth are removed surgically with IV sedation, the total cost could be $1,000 to $4,000+. Dental insurance typically covers 50-80% of the cost after your deductible.
Q2: How painful is impacted tooth removal?
A: The procedure itself is usually not painful because you'll receive local anesthesia, sedation, or general anesthesia. You may feel pressure, but no sharp pain. After the anesthesia wears off, you will experience some pain and discomfort for a few days, which can be managed with prescribed pain medication and over-the-counter pain relievers. Swelling and soreness are also common. Following your dentist's aftercare instructions carefully will help minimize discomfort.
Q3: How long does recovery take?
A: Initial recovery from a surgical extraction typically takes 3-7 days for most of the acute symptoms (pain, swelling) to subside. You'll likely need to stick to a soft diet for the first few days. Complete soft tissue healing can take 2-4 weeks, while full bone healing in the socket takes several months. It's important to avoid strenuous activity for the first week to prevent complications like dry socket.
Q4: Are there alternatives to extracting an impacted tooth?
A: For some asymptomatic, low-risk impactions, your dentist may recommend monitoring the tooth with regular check-ups and X-rays rather than immediate extraction. For impacted canines or other non-molar teeth, orthodontic treatment involving surgical exposure and braces can often guide the tooth into its correct position, preserving the natural tooth. However, for most problematic impacted wisdom teeth, extraction is the most common and effective solution.
Q5: Does dental insurance cover impacted tooth removal?
A: Yes, most dental insurance plans typically cover a portion of the cost for impacted tooth removal, especially if it's deemed medically necessary to prevent pain, infection, or damage. Coverage usually ranges from 50% to 80% after your deductible is met. However, it's crucial to check your specific policy details, as there may be annual maximums or different coverage levels for surgical procedures or orthodontics. Always get a pre-treatment estimate from your dental office and verify with your insurance provider.
Q6: Can an impacted tooth cause headaches?
A: Yes, an impacted tooth can indeed cause headaches or referred pain in other areas of the head and face. The pressure from an impacted tooth, particularly a wisdom tooth pushing against other teeth or nerves, can manifest as tension headaches, earaches, or generalized facial pain. Infection (pericoronitis) around a partially erupted impacted tooth can also contribute to these symptoms.
Q7: What is a dry socket?
A: Dry socket (alveolar osteitis) is a common, painful complication that can occur after a tooth extraction. It happens when the blood clot that forms in the empty tooth socket either dislodges or dissolves prematurely, exposing the underlying bone and nerves. This leads to intense pain, often radiating to the ear, and a foul taste or odor. It typically occurs 2-5 days after extraction. Avoiding smoking, using straws, and vigorous rinsing for the first few days significantly reduces the risk. If you suspect dry socket, contact your dentist immediately for treatment.
Q8: Can I prevent impaction?
A: While you cannot completely prevent the genetic factors that lead to impaction, particularly for wisdom teeth, early detection and intervention can help manage some cases. Regular dental check-ups with X-rays, especially during teenage years, allow your dentist to monitor tooth development. For younger patients, early orthodontic evaluation (around age 7-8) can identify jaw size issues or eruption path problems for teeth like canines, and interceptive orthodontics might create space, sometimes preventing impaction.
When to See a Dentist
Given that many impacted teeth are asymptomatic, regular dental check-ups are your first line of defense. A routine panoramic X-ray can reveal impacted teeth long before they cause problems.
Schedule a routine dental appointment if:
- You are between the ages of 17 and 25 and have not had your wisdom teeth checked.
- Your child is 7 years old and has not had an orthodontic evaluation.
- You have a general ache or tenderness in the back of your jaw.
- You notice any persistent bad breath or an unpleasant taste, especially around the back teeth.
- You have difficulty cleaning certain areas of your mouth.
Seek prompt dental attention (within a few days) if you experience:
- Persistent or increasing pain in your jaw or around a tooth.
- Red, swollen, or bleeding gums that don't improve.
- Difficulty or pain when opening your mouth fully.
- Noticeable swelling on the outside of your jaw or cheek.
Seek emergency dental care (immediately) if you experience:
- Severe, unbearable pain that isn't controlled by medication.
- Sudden and rapid swelling that makes it difficult to swallow or breathe.
- A high fever accompanied by swelling and pain, which could indicate a serious infection.
Early detection and appropriate treatment are key to preventing complications and maintaining a healthy, comfortable smile. Don't hesitate to consult your dentist if you have any concerns about impaction or any other aspect of your oral health.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.