Cavity
4,200 words · 14 min read
Quick Definition
A hole in a tooth caused by decay (caries), resulting from acid-producing bacteria that dissolve tooth structure over time.
Cavity: Understanding the Silent Threat to Your Smile
A cavity-conditions-diseases-everything-you-need-to-know "Complete Guide to Dental Conditions & Diseases: Everything You Need to Know"), clinically known as dental caries, is a permanent hole or structural damage to a tooth. It's the unfortunate result of a complex process where acid-producing bacteria in your mouth dissolve the hard outer layers of your teeth. Imagine your tooth enamel, the hardest substance in your body, being slowly eroded – that's the insidious work of a cavity. This damage, if left untreated, can progress through the tooth, causing pain, infection, and eventually, tooth loss.
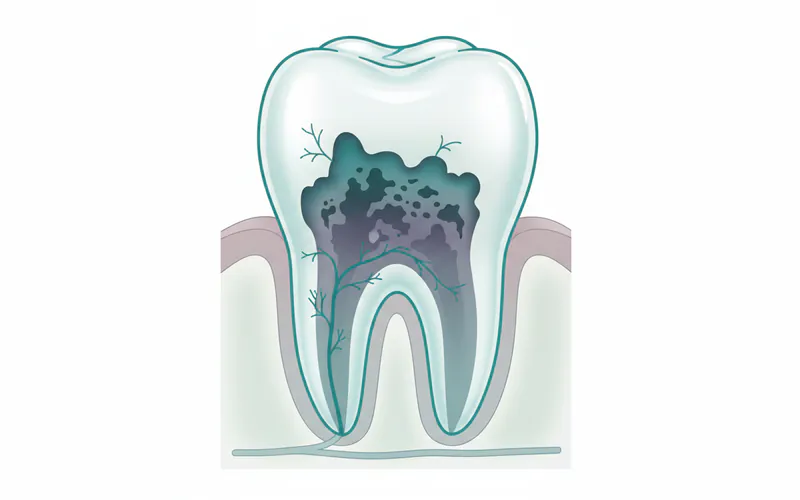
Cavities are a significant public health concern and one of the most common chronic diseases globally, affecting people of all ages. In the United States, data from the Centers for Disease Control and Prevention (CDC) indicates that 26% of adults aged 20-64 currently have untreated dental caries. Among children, one in five aged 5-11 years has at least one untreated decayed tooth, and this number rises to one in four among adolescents aged 12-19 years. These statistics underscore why understanding cavities – their causes, symptoms, and prevention – is crucial for maintaining overall dental and systemic health. Early detection and treatment are paramount to preventing further damage and preserving your natural teeth for a lifetime.
Key Takeaways:
- A cavity is a permanent hole in a tooth caused by acid from bacteria.
- Also known as dental caries, it's one of the most common chronic diseases.
- Cavities are largely preventable with good oral hygiene and diet.
- Untreated cavities can lead to pain, infection, and tooth loss.
- Early detection and treatment are vital to save the tooth and prevent complications.
- Regular dental check-ups and cleanings are your best defense.
Detailed Explanation
Types and Classifications of Cavities
Cavities don't all look or behave the same. Dentists classify them based on their location and severity. Understanding these types can help you recognize potential issues and appreciate the varied treatment approaches.
- Pit and Fissure Cavities: These are the most common type, forming on the chewing surfaces of your back teeth (molars and premolars). These surfaces have natural grooves and pits that can easily trap food particles and bacteria, making them difficult to clean effectively with a toothbrush.
- Smooth Surface Cavities: These form on the smooth, flat outer surfaces of teeth, often between teeth where floss doesn't reach effectively, or near the gum line. They are less common than pit and fissure cavities but can be challenging to detect without X-rays.
- Root Caries: As we age, gums can recede, exposing the tooth roots. Unlike enamel, the root surface is covered by cementum, a softer tissue that is more vulnerable to acid attack. Root caries are common in older adults, particularly those with gum disease or dry mouth.
- Recurrent (Secondary) Caries: These cavities form around existing fillings or dental restorations. They occur when bacteria leak beneath a filling that has fractured, worn down, or developed a poor seal with the tooth, creating a new area for decay.
- Early Childhood Caries (ECC): Formerly known as "baby bottle tooth decay," ECC affects infants and young children, often due to prolonged exposure to sugary liquids (like milk, juice, or sweetened formula) in bottles or sippy cups, especially at bedtime. It often affects the upper front teeth first.
- Interproximal Caries: This refers specifically to cavities that form between teeth, often only detectable via dental X-rays. They are a subset of smooth surface caries.
Causes and Risk Factors
The formation of a cavity is a multi-factorial process involving bacteria, diet, and time. Here’s how it typically unfolds:
- Bacteria and Plaque: Your mouth is home to hundreds of types of bacteria. Certain types, particularly Streptococcus mutans, feed on the sugars you consume. When these bacteria combine with food particles, saliva, and other substances, they form a sticky, colorless film called plaque that adheres to your teeth.
- Acid Production: When the bacteria in plaque metabolize sugars and carbohydrates (like those found in candies, soda, bread, and fruits), they produce acids as a byproduct.
- Demineralization: These acids attack the tooth enamel, dissolving its mineral content (calcium and phosphate). This process is called demineralization. Initially, enamel can repair itself through remineralization, using minerals from saliva and fluoride. However, if acid attacks are frequent and prolonged, the tooth loses more minerals than it can regain.
- Cavity Formation: Over time, as demineralization continues, the enamel weakens and eventually breaks down, forming a small hole – a cavity. If not treated, this hole can grow larger and penetrate deeper into the dentin (the softer layer beneath enamel) and then into the pulp (the innermost part of the tooth containing nerves and blood vessels).
Key Risk Factors:
- Frequent Snacking/Sugary Drinks: Constant exposure to sugars fuels acid production.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque to accumulate and acids to persist.
- Dry Mouth (Xerostomia): Saliva helps wash away food particles, neutralize acids, and provides minerals for remineralization. Conditions like certain medications, medical treatments (e.g., radiation), and systemic diseases (e.g., Sjögren's syndrome) can reduce saliva flow, increasing cavity risk.
- Lack of Fluoride: Fluoride strengthens enamel and helps resist acid attacks. Many public water supplies are fluoridated, and fluoride is found in most toothpastes and some mouthwashes.
- Infant Feeding Practices: As mentioned with ECC, prolonged bottle use with sugary liquids can be detrimental.
- Worn Dental Restorations: Old, chipped, or cracked fillings can create crevices where bacteria can hide and lead to recurrent caries.
- Gum Recession: Exposes the softer root surface to decay.
- Poor Diet: A diet high in processed carbohydrates and sugars.
- Genetics: While not a direct cause, some people may have genetically thinner or weaker enamel, or a natural oral microbiome that makes them more susceptible.
- Certain Medical Conditions: Conditions like acid reflux or bulimia can expose teeth to stomach acids, eroding enamel.
Signs and Symptoms to Watch For
In its earliest stages, a cavity often presents no noticeable symptoms, which is why regular dental check-ups are so important. As decay progresses, however, you may begin to experience:
- Tooth Sensitivity: A mild, fleeting sensitivity to hot, cold, or sweet foods and drinks. This is often an early sign as the decay reaches the dentin.
- Mild to Sharp Pain: Pain when eating or drinking something sweet, hot, or cold. The pain may linger after the stimulus is removed.
- Pain When Biting Down: Pressure from chewing can cause discomfort if the cavity is significant or has reached the inner layers of the tooth.
- Visible Holes or Pits in Your Teeth: As the cavity grows, you might be able to see a visible hole or pit on the tooth surface.
- Brown, Black, or White Staining on a Tooth Surface: These discolorations can indicate areas of decay.
- Pus Around a Tooth or Swelling of the Gums: This is a sign of a severe infection (abscess) that has likely reached the tooth's pulp.
- Bad Breath or Unpleasant Taste in the Mouth: Can be associated with deep decay and infection.
If you experience any of these symptoms, especially persistent pain or sensitivity, it's crucial to schedule an appointment with your dentist immediately.
Diagnosis Process — What Your Dentist Does
Diagnosing a cavity is a routine part of a comprehensive dental exam. Your dentist uses a combination of visual inspection, tactile examination, and imaging to detect decay.
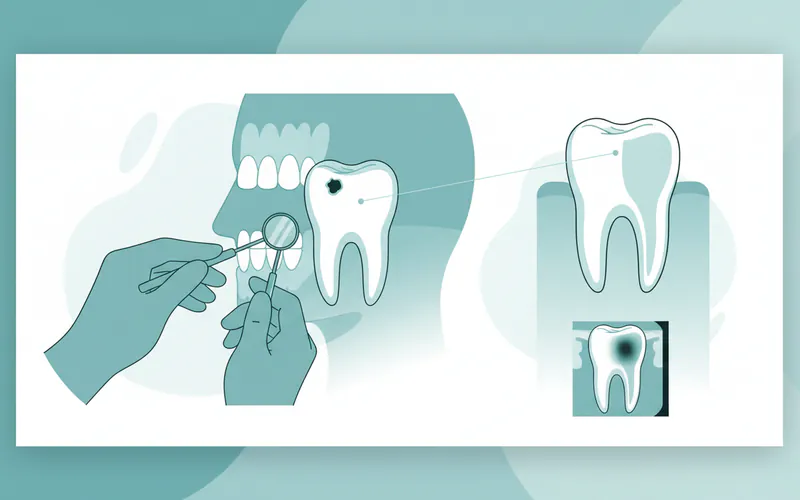
- Visual Examination: Your dentist will carefully examine all surfaces of your teeth, looking for visible holes, pits, discolored spots (white, brown, or black), and signs of enamel breakdown.
- Dental Explorer: A small, sharp metal instrument called a "dental explorer" is used to gently probe the tooth surfaces, particularly the pits and grooves. If the explorer "sticks" in a certain spot, it can indicate a softened area of enamel or a cavity.
- Dental X-rays (Radiographs): These are indispensable for detecting cavities, especially those between teeth (interproximal cavities) or under existing fillings, which are not visible to the naked eye. Bitewing X-rays are most commonly used for cavity detection, showing the crowns of upper and lower back teeth.
- Cavity Detection Dyes: In some cases, a special dye may be applied to the tooth. The dye stains decayed areas, making them easier to identify and differentiate from healthy tooth structure.
- Transillumination: A high-intensity light source is shone through the tooth. Healthy enamel transmits light evenly, while areas of decay appear as shadows. This can be particularly useful for detecting interproximal cavities.
- Laser Fluorescence Devices: Devices like DIAGNOdent use a laser to detect changes in tooth structure indicative of early decay, often before it's visible or detectable by an explorer.
Once a cavity is detected, your dentist will determine its size, depth, and location to recommend the most appropriate treatment.
Treatment Options with Pros, Cons, and Costs
The treatment for a cavity depends entirely on its size and severity. The goal is always to remove the decayed portion of the tooth and restore its structure and function.
| Treatment Option | Description | Pros | Cons | Estimated US Cost (Without Insurance) |
|---|---|---|---|---|
| Fluoride Treatment | Topical application of fluoride varnish, gel, or foam to strengthen enamel and reverse very early demineralization (not a true cavity). | Non-invasive, quick, can prevent cavity progression if caught early. | Only effective for initial enamel demineralization (white spots), not for actual holes. | $25 - $75 |
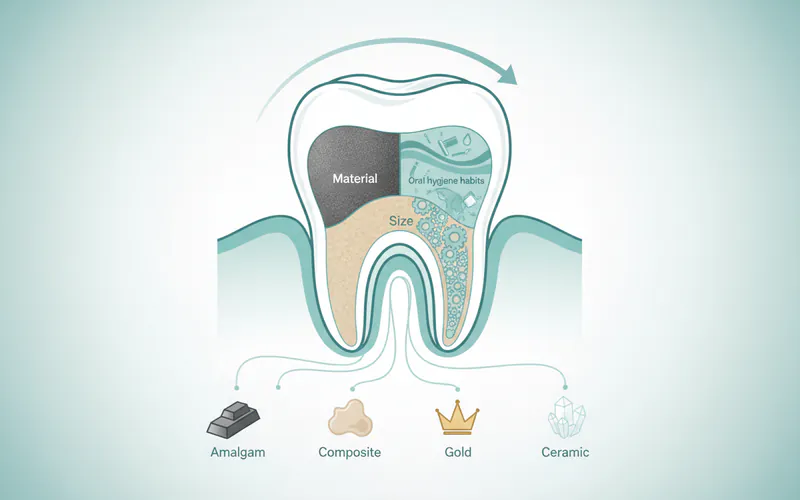
| Dental Fillings | Removal of decayed tooth material and filling the resulting hole with a restorative material. | Most common treatment. Stops decay, restores tooth function. Various materials available (composite, amalgam, glass ionomer, ceramic). | Requires removal of tooth structure. Different materials have varying aesthetics, durability, and cost. Can cause temporary sensitivity. Limited to cavities of moderate size. | |
| Composite (Resin) | Tooth-colored plastic and glass mixture. | Aesthetically pleasing (matches tooth color), bonds directly to tooth structure (can strengthen it), mercury-free. | Less durable than amalgam for large restorations, prone to staining over time, can be more technique-sensitive for placement, typically more expensive than amalgam. | $150 - $450 |
| Amalgam (Silver) | Silver-colored alloy of mercury, silver, tin, and copper. | Very durable, cost-effective, time-tested (long clinical history). | Not aesthetically pleasing (silver color), contains mercury (though deemed safe by ADA), requires removal of more healthy tooth structure for retention, can expand/contract with temperature changes. | $100 - $300 |
| Glass Ionomer | Tooth-colored material that releases fluoride. | Releases fluoride (beneficial for decay prevention), good for small, non-load-bearing areas, particularly useful for children or root cavities. | Weaker than composite or amalgam, less wear-resistant, may not be suitable for chewing surfaces. | $120 - $350 |
| Ceramic (Porcelain) | Tooth-colored, strong material, often created with CAD/CAM technology (e.g., CEREC). | Very aesthetically pleasing, highly durable, resistant to staining, biocompatible. | Most expensive filling option, can be brittle in very thin sections, typically requires two visits if not done with same-day technology. | $300 - $1,000 |
| Dental Crown | A tooth-shaped "cap" placed over a severely damaged or weakened tooth to restore its shape, size, strength, and appearance. | Restores severely decayed or fractured teeth, protects weakened teeth from further damage, can significantly extend tooth life. | More invasive than a filling, requires removal of significant tooth structure, higher cost, typically requires two appointments (unless same-day crown), risk of sensitivity or pulp irritation. | $800 - $2,500+ |
| Root Canal Treatment | Removal of infected or inflamed pulp (nerve tissue) from the inside of the tooth, followed by cleaning, shaping, and sealing the canal. | Saves a severely infected tooth from extraction, eliminates pain and infection, preserves natural tooth structure. | More complex and expensive than a filling, requires a crown afterward for protection, can cause temporary discomfort, rarely fails. | $700 - $2,000 (front) / $1,000 - $3,000 (back) |
| Tooth Extraction | Removal of the entire tooth. | Quick and effective removal of a hopelessly decayed or infected tooth, immediate relief from severe pain/infection. | Permanent tooth loss, can lead to shifting of adjacent teeth, bite problems, bone loss, requires replacement (implant, bridge, partial denture) for long-term health, which adds significant cost. | $75 - $400 (simple) / $200 - $600+ (surgical) |
Step-by-Step: What to Expect During Treatment (for a Filling)
Let's walk through the most common treatment for a cavity: a dental filling.
- Numbing: The dentist will apply a topical anesthetic to your gum, followed by an injection of local anesthetic (e.g., lidocaine) near the affected tooth. This will numb the tooth, gum, and surrounding tissues, ensuring you feel no pain during the procedure.
- Decay Removal: Once the area is numb, the dentist will use a high-speed dental drill to carefully remove all the decayed and softened tooth structure. They will often use a slower-speed drill or hand instruments to remove decay closer to the nerve to minimize trauma.
- Tooth Preparation: After all decay is removed, the remaining tooth structure is prepared to receive the filling. This may involve shaping the cavity walls to ensure the filling material can bond or be retained securely. If a composite filling is used, a mild acid gel may be applied to "etch" the enamel, creating microscopic pores for better adhesion.
- Material Placement:
- Composite Fillings: A bonding agent is applied, followed by layers of tooth-colored composite resin. Each layer is hardened with a special curing light.
- Amalgam Fillings: The amalgam material is packed into the prepared cavity.
- Glass Ionomer Fillings: The material is mixed and placed directly into the cavity.
- Shaping and Polishing: Once the filling material is in place, your dentist will shape it to match the natural contours of your tooth and ensure your bite is comfortable. They will then polish the filling for a smooth finish.
- Final Checks: Your dentist will check your bite and ensure there are no high spots that could cause discomfort or damage.
The entire process for a simple filling typically takes 20 to 60 minutes, depending on the size and location of the cavity.
Recovery Timeline and Aftercare
After a dental filling, recovery is generally straightforward:
- Immediate Aftermath: The numbness from the local anesthetic will wear off within 1-3 hours. It's important to avoid eating or drinking very hot beverages until the numbness subsides to prevent accidentally biting your tongue or cheek, or burning your mouth.
- Sensitivity: It's common to experience some sensitivity to hot, cold, or pressure for a few days to a few weeks after a filling, especially with deeper cavities or composite fillings. This usually subsides on its own. Over-the-counter pain relievers (like ibuprofen or acetaminophen) can help manage discomfort.
- Chewing: You can typically resume normal eating habits once the numbness wears off. If you received an amalgam filling, your dentist might advise waiting 24 hours before chewing heavily on that side to allow the material to fully set.
- Oral Hygiene: Continue your regular brushing and flossing routine. This is crucial for preventing new cavities and maintaining the health of your restored tooth.
- Follow-up: If sensitivity persists, your bite feels uneven, or you experience sharp pain, contact your dentist. A minor adjustment to the filling may be needed, or there could be a deeper issue requiring further evaluation.
Prevention Strategies
The best way to deal with cavities is to prevent them from forming in the first place. This involves a multi-pronged approach:
- Brush Twice Daily with Fluoride Toothpaste: Brush for at least two minutes, using a soft-bristled toothbrush. Fluoride strengthens enamel and helps resist acid attacks.
- Floss Daily: Flossing removes plaque and food particles from between teeth and under the gum line, areas your toothbrush can't reach, preventing interproximal cavities.
- Limit Sugary and Acidic Foods and Drinks: Reduce your intake of soda, fruit juices, candy, pastries, and other sugary snacks. If you do consume them, do so with meals rather than as frequent snacks throughout the day, and rinse your mouth with water afterward.
- Drink Fluoridated Water: Community water fluoridation is one of the most effective and cost-efficient ways to prevent cavities. If your water isn't fluoridated, talk to your dentist about fluoride supplements.
- Regular Dental Check-ups and Cleanings: Visit your dentist at least twice a year for professional cleanings and examinations. This allows your dentist to remove plaque and tartar buildup and detect early signs of decay before they become major problems.
- Dental Sealants: For children and sometimes adults, dental sealants can be applied to the chewing surfaces of molars and premolars. These thin, plastic coatings fill in the pits and grooves, creating a smooth surface that is easier to clean and more resistant to plaque buildup.
- Consider Fluoride Rinses: Your dentist might recommend a daily fluoride mouthwash if you're at high risk for cavities.
- Chew Sugar-Free Gum: Chewing sugar-free gum after meals can stimulate saliva flow, which helps neutralize acids and wash away food particles.
- Maintain Good Overall Health: Address conditions like dry mouth or acid reflux, which can contribute to cavity formation.
Cost Ranges in the US (with/without Insurance)
The cost of cavity treatment in the US varies significantly based on factors such as the type and size of the cavity, the chosen treatment material, the dentist's fees, and your geographic location.

- Dental Fillings:
- Amalgam (1-2 surfaces): $100 - $250 (without insurance)
- Amalgam (3+ surfaces): $150 - $350 (without insurance)
- Composite (1-2 surfaces): $150 - $350 (without insurance)
- Composite (3+ surfaces): $250 - $450 (without insurance)
- With insurance, expect to pay 10-50% of these costs, depending on your plan's coverage for basic restorative procedures.
- Dental Crowns:
- Porcelain Fused to Metal (PFM): $800 - $1,500 (without insurance)
- All-Ceramic/Zirconia: $1,000 - $2,500+ (without insurance)
- Most dental insurance plans cover 50% of the cost for crowns, after your deductible.
- Root Canal Treatment:
- Front Tooth (Incisor/Canine): $700 - $1,500 (without insurance)
- Premolar: $800 - $1,800 (without insurance)
- Molar: $1,000 - $2,000+ (without insurance)
- Many insurance plans cover 50% of root canal costs, after your deductible.
- Tooth Extraction:
- Simple Extraction: $75 - $300 (without insurance)
- Surgical Extraction (impacted or complex): $200 - $600+ (without insurance)
- Extractions are often covered at 50-80% by insurance, depending on the complexity and your plan.
It's crucial to always get a detailed cost estimate from your dentist before any procedure and to understand your dental insurance benefits. Many dental plans categorize fillings as "basic care," while crowns and root canals are "major care," with different levels of coverage.
For Parents / Pediatric Considerations
Cavities in children, known as Early Childhood Caries (ECC) or baby bottle tooth decay, are a significant concern. They can lead to pain, infection, difficulty eating, and speech problems, and even impact a child's growth and development.
- First Dental Visit: The American Academy of Pediatric Dentistry recommends a child's first dental visit by their first birthday or within 6 months of the eruption of their first tooth. This allows the dentist to assess risk, provide guidance, and establish good habits early.
- Preventing ECC: Avoid putting your baby to bed with a bottle containing anything other than water. Limit sugary drinks and frequent snacking. Wipe your baby's gums with a clean cloth after feedings, and begin brushing with a tiny smear of fluoride toothpaste (rice-grain size) as soon as the first tooth appears.
- Fluoride Varnish: Pediatric dentists frequently apply fluoride varnish to children's teeth to strengthen enamel and prevent cavities, especially for those at high risk.
- Dental Sealants: These protective coatings are highly recommended for children as soon as their permanent molars erupt (around ages 6 and 12). Sealants are a simple, pain-free way to prevent pit and fissure cavities, which are common in young children. The CDC estimates that sealants prevent 80% of cavities in the back teeth, where 9 out of 10 cavities occur.
- Lead by Example: Parents play a crucial role in modeling good oral hygiene habits and making healthy dietary choices.
Frequently Asked Questions
How much does a cavity filling cost?
The cost of a cavity filling varies widely, typically ranging from $100 to $450 per tooth without insurance. This depends on the size of the cavity, its location, and the material used. Amalgam (silver) fillings are generally less expensive ($100-$350) than composite (tooth-colored) fillings ($150-$450). Ceramic fillings can be even more expensive, sometimes overlapping with crown costs. Dental insurance usually covers a percentage of filling costs, often 50-80%, after you meet your deductible.
Is getting a cavity filled painful?
Modern dental techniques make getting a cavity filled a relatively comfortable procedure. Your dentist will use a local anesthetic to thoroughly numb the area around the tooth, so you should not feel any pain during the actual decay removal or filling placement. You might feel some pressure or vibration from the drill, but no sharp pain. After the numbness wears off, some temporary sensitivity or mild soreness is common, which can usually be managed with over-the-counter pain relievers.
How long does a filling last?
The lifespan of a dental filling depends on the material used, the size of the filling, your oral hygiene habits, and your biting forces.
- Amalgam fillings are very durable and can last 10-15 years or even longer.
- Composite fillings typically last 5-10 years.
- Glass ionomer fillings are generally less durable and may last 3-5 years.
- Ceramic fillings are quite strong and can last 10-15 years. Regular check-ups allow your dentist to monitor the condition of your fillings and recommend replacement if they show signs of wear, cracks, or leakage.
Are there alternatives to dental fillings for cavities?
For very small, initial areas of demineralization (not yet a true hole), your dentist might recommend fluoride varnish or highly concentrated fluoride gels to encourage remineralization and potentially reverse the early decay. Dental sealants can prevent cavities from forming in pits and fissures but aren't a treatment for existing cavities. Once a true hole (cavity) has formed in the enamel, it is irreversible and requires a filling or other restorative treatment to prevent further progression. There are no at-home remedies or alternative treatments that can effectively eliminate an existing cavity.
Does insurance cover cavity treatment?
Most dental insurance plans do cover cavity treatment, but the extent of coverage varies significantly.
- Fillings are usually categorized as "basic restorative care" and are often covered at 50-80% after your deductible.
- Crowns and Root Canal Treatment are typically considered "major restorative care" and may be covered at a lower percentage, often 50%, with higher deductibles and annual maximums. It's essential to review your specific insurance policy or contact your provider to understand your benefits, coverage percentages, deductibles, and annual maximums.
Can a cavity heal itself?
Unfortunately, a true cavity – a physical hole in the tooth enamel – cannot heal itself. While very early stages of demineralization (often appearing as white spots on the enamel) can potentially be reversed or arrested with fluoride treatment and improved oral hygiene (remineralization), once the enamel surface has broken down and a hole has formed, it requires professional intervention by a dentist to remove the decay and fill the tooth. Leaving a cavity untreated will only allow it to grow larger, leading to pain, infection, and potentially more extensive and costly treatments like a root canal or even tooth extraction.
When to See a Dentist
Regular dental check-ups, typically every six months, are your best defense against cavities. These routine visits allow your dentist to detect and treat cavities early, often before they cause any noticeable symptoms.
However, you should schedule an appointment with your dentist immediately if you experience any of the following:
- Persistent Toothache: Any tooth pain that lasts for more than a day or two, especially if it's severe or throbbing.
- Sharp Pain When Biting Down: This could indicate a significant cavity, a cracked tooth, or a problem with an existing filling.
- Increased Sensitivity: If your teeth become unusually sensitive to hot, cold, or sweet substances, and this sensitivity doesn't subside quickly.
- Visible Holes or Pits: If you notice any new holes, dark spots, or significant discolorations on your teeth.
- Swelling or Pus Around a Tooth: These are signs of a severe infection (dental abscess) that requires urgent attention to prevent it from spreading.
- Chipped or Broken Fillings: This can expose the tooth to new decay or cause sensitivity.
Don't wait for pain to be your guide; by then, a cavity may have progressed significantly, requiring more complex and expensive treatment. Early detection and intervention are key to preserving your oral health.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.