Root Canal
3,977 words · 13 min read
Quick Definition
A dental procedure that removes infected or damaged pulp from inside a tooth, cleans and shapes the canal system, and seals it with a filling material to save the tooth.
As an expert dental health writer for SmilePedia.net, it is my privilege to provide you with the definitive guide to understanding root canal treatment. This in-depth article will explain everything you need to know about this common and often misunderstood dental procedure.
Introduction
What is a root canal? At its core, a root canal is a highly effective dental procedure designed to save a tooth that has become severely infected or damaged. It involves carefully removing the inflamed or infected pulp (the soft tissue inside the tooth), meticulously cleaning and shaping the tooth's internal canal system, and then sealing it with a biocompatible filling material. Far from being the painful ordeal of common myth, modern root canal therapy is typically comfortable, thanks to advanced techniques and effective local anesthesia.
This procedure matters immensely for your overall dental health because it allows you to retain your natural tooth, preventing the complications associated with tooth extraction, such as shifting teeth, bone loss, and the need for expensive tooth replacements like implants or bridges. Preserving your natural tooth means maintaining your bite, chewing efficiency, and aesthetic appearance.
Root canal treatment is also incredibly common. According to the American Association of Endodontists (AAE), over 15 million root canals are performed in the United States each year, making it one of the most frequent dental procedures. That’s approximately 41,000 root canals performed every single day! This high prevalence underscores its importance and effectiveness in managing dental pain and preserving oral health for millions of Americans.
Key Takeaways:
- A root canal saves an infected or damaged tooth, preventing extraction.
- The procedure removes the diseased pulp, cleans the inner tooth, and seals it.
- Modern root canal therapy is generally comfortable, often no more painful than a filling.
- It is performed by general dentists or specialized dentists called endodontists.
- Saving your natural tooth helps maintain your bite, speech, and appearance.
- Root canal treatment has a high success rate, often allowing teeth to last a lifetime.
Detailed Explanation
Types and Classifications of Root Canal Treatment
While the term "root canal" typically refers to conventional root canal therapy (RCT) for mature permanent teeth, several variations and related procedures exist depending on the tooth's condition and the patient's age:
- Conventional Root Canal Therapy (RCT): This is the most common type, performed on fully developed permanent teeth with infected or irreversibly inflamed pulp. The goal is to clean out the infected tissue and seal the root canals.
- Endodontic Retreatment: If a tooth that has previously undergone root canal treatment becomes re-infected or fails to heal, endodontic retreatment may be necessary. This involves reopening the tooth, removing the previous filling material, re-cleaning the canals, and resealing them.
- Apicoectomy: This is a minor surgical procedure, also known as root-end resection. It is performed when inflammation or infection persists in the bony area around the end of your tooth after a conventional root canal or retreatment. The tip of the tooth’s root is removed, along with any infected tissue, and the end of the canal is sealed.
- Pulpotomy and Pulpectomy: These are root canal-related procedures primarily performed on primary (baby) teeth.
- A pulpotomy removes only the diseased portion of the pulp in the crown of the tooth, leaving the healthy pulp in the root canals intact. It's often called a "nerve treatment" for baby teeth.
- A pulpectomy involves removing all the pulp tissue from both the crown and the root canals of a baby tooth. The canals are then filled with a resorbable material that allows the tooth to eventually fall out naturally.
- Apexification and Apexogenesis: These procedures are performed on immature permanent teeth with incompletely formed roots due to trauma or deep decay.
- Apexogenesis aims to encourage the root to continue developing naturally by preserving the healthy pulp tissue.
- Apexification is used when the pulp is necrotic (dead) and the root has not fully formed. It stimulates the formation of a hard tissue barrier at the root end to seal the canal.
Causes and Risk Factors for Pulp Infection
The pulp, the innermost part of your tooth, contains nerves, blood vessels, and connective tissue. When this delicate tissue becomes infected or inflamed, a root canal is often the only way to save the tooth. Common causes and risk factors include:
- Deep Decay (Caries): Untreated dental caries (cavities) can progress deeply into the tooth, eventually reaching and contaminating the pulp chamber. This is the most common cause.
- Trauma: A direct blow to a tooth, a chip, or a crack can expose the pulp to bacteria, or disrupt its blood supply, leading to inflammation and death of the tissue.
- Repeated Dental Procedures: Multiple fillings or extensive dental work on the same tooth can sometimes cause trauma or irritation to the pulp, leading to inflammation over time.
- Cracked or Chipped Teeth: Fractures in the tooth structure can create pathways for bacteria to enter the pulp chamber, even if the decay isn't deep.
- Large Fillings: Over time, large or leaky fillings can allow bacteria to penetrate beneath them and reach the pulp.
- Advanced Gum Disease: In rare, severe cases, infection from advanced periodontal (gum) disease can spread through accessory canals in the tooth roots and affect the pulp.
- Untreated Pulpitis: Pulpitis is inflammation of the pulp. If irreversible, meaning the pulp cannot heal on its own, it will eventually lead to necrosis (tissue death) and infection, necessitating a root canal.
Signs and Symptoms to Watch For
While some people experience no symptoms, others can have severe pain. It's crucial to recognize these warning signs that indicate your tooth's pulp might be infected or inflamed:
- Persistent Tooth Pain: This is the most common symptom. The pain can range from mild to severe, spontaneous, or triggered by chewing. It might be constant or intermittent, and often worsens when lying down.
- Sensitivity to Hot and Cold: Lingering sensitivity to hot or cold temperatures, especially if the sensation persists for several seconds or minutes after the stimulus is removed, is a strong indicator of pulp damage.
- Swelling and Tenderness in the Gums: Inflammation or infection can spread to the surrounding tissues, causing the gums near the affected tooth to become swollen, red, and tender to the touch.
- Pimple-like Bump on the Gums (Dental Abscess): A small, pus-filled bump (a fistula or abscess) might appear on the gums near the problematic tooth. This indicates that the infection has spread and is draining.
- Pain When Chewing or Touching: If applying pressure to the tooth, such as when chewing, causes sharp pain, it could mean the ligaments around the tooth are inflamed due.
- Darkening or Discoloration of the Tooth: An infected tooth may appear darker or grayish due to internal bleeding and tissue death within the pulp chamber.
Diagnosis Process — What Your Dentist Does
Diagnosing the need for a root canal involves a thorough examination by your general dentist or an endodontist (a dental specialist who treats diseases of the pulp and root of the tooth). The diagnostic process typically includes:
- Clinical Examination: Your dentist will visually inspect your tooth and the surrounding gums for signs of swelling, redness, or discoloration. They will also gently tap on your tooth (percussion test) and press on your gums (palpation test) to check for tenderness.
- Dental X-rays: Digital X-rays are crucial. They allow the dentist to see the extent of decay, any bone loss around the root tip, and the presence of an abscess. X-rays also reveal the number, shape, and length of the root canals, which is vital for treatment planning. ``
- Pulp Vitality Tests:
- Cold Test: A small amount of cold stimulus (like an ice stick or cotton pellet sprayed with a refrigerant) is applied to the tooth. A healthy tooth will react briefly and then stop. Lingering pain or no sensation at all can indicate pulp damage.
- Heat Test: Similar to the cold test, heat can also be used. Lingering pain indicates irreversible pulpitis.
- Electric Pulp Tester: This device sends a mild electric current to the tooth. A response indicates viable nerve tissue, while no response suggests pulp necrosis.
- Selective Anesthesia: In some complex cases, a local anesthetic may be used to determine which specific tooth is causing pain, especially when referred pain from other areas is present.
Treatment Options: Root Canal vs. Extraction
When the pulp is irreversibly damaged or infected, you essentially have two main treatment paths: saving the tooth with a root canal or extracting it.
Root Canal Therapy (RCT)
- Pros:
- Preserves Natural Tooth: The primary benefit is keeping your own tooth, which maintains your natural bite, chewing ability, and aesthetic appearance.
- Prevents Bone Loss: Keeping the tooth root stimulated helps prevent bone loss in the jaw.
- Cost-Effective in the Long Run: While the initial cost can be significant, it’s often less expensive over time than extracting a tooth and replacing it with an implant or bridge.
- Minimally Invasive Compared to Extraction & Replacement: It avoids the surgical aspect of an implant and the preparation of adjacent teeth required for a bridge.
- Cons:
- Requires Subsequent Restoration: The tooth will need a permanent filling and, in most cases, a dental crown to protect it from fracture after the procedure. This adds to the overall cost and appointment time.
- Potential for Re-treatment: Though highly successful, there's a small chance of needing retreatment if the initial procedure fails.
- Multiple Appointments: While many are completed in one visit, some complex cases may require two appointments.
Tooth Extraction
- Pros:
- Immediate Relief of Infection: Removing the tooth immediately eliminates the source of infection.
- Lower Initial Cost: The cost of extraction is typically lower than a root canal.
- Cons:
- Loss of Natural Tooth: This is the biggest drawback, as it leads to significant long-term consequences.
- Requires Tooth Replacement: The gap left by an extracted tooth must be filled to prevent shifting of adjacent teeth, bite problems, and bone loss. Replacement options (implants, bridges, partial dentures) are often more costly and invasive than root canal treatment over time.
- Impact on Oral Health: Can lead to chewing difficulties, changes in speech, and altered facial aesthetics.
Comparison Table: Root Canal vs. Extraction
| Feature | Root Canal Therapy (RCT) | Tooth Extraction |
|---|---|---|
| Goal | Save the natural tooth | Remove the diseased tooth |
| Tooth Preservation | Yes, preserves natural tooth | No, tooth is lost |
| Long-term Cost | Often less costly when considering replacement options | Lower initial cost, but significantly higher long-term if replaced |
| Bone Health | Maintains jawbone density | Leads to jawbone loss over time if not replaced by implant |
| Adjacent Teeth | No impact on adjacent teeth | Adjacent teeth may shift, affecting bite and alignment |
| Appearance | Preserves natural appearance with a crown | Gap in smile, unless replaced |
| Treatment Complexity | Requires precision and specialized instruments | Relatively straightforward, but may involve surgery for impacted teeth |
| Recovery | Minor soreness, followed by placement of permanent restoration | Swelling, bleeding, risk of dry socket; healing of extraction site |
| Follow-up | Requires permanent restoration (crown or filling) | Requires consideration of replacement options (implant, bridge, denture) |
| Success Rate | Over 95% | High, but leads to other dental issues if not replaced |
Step-by-Step: What to Expect During Root Canal Treatment
Root canal treatment is typically performed in one or two appointments and is a meticulous process designed to thoroughly clean and seal the tooth. Here’s a general overview:
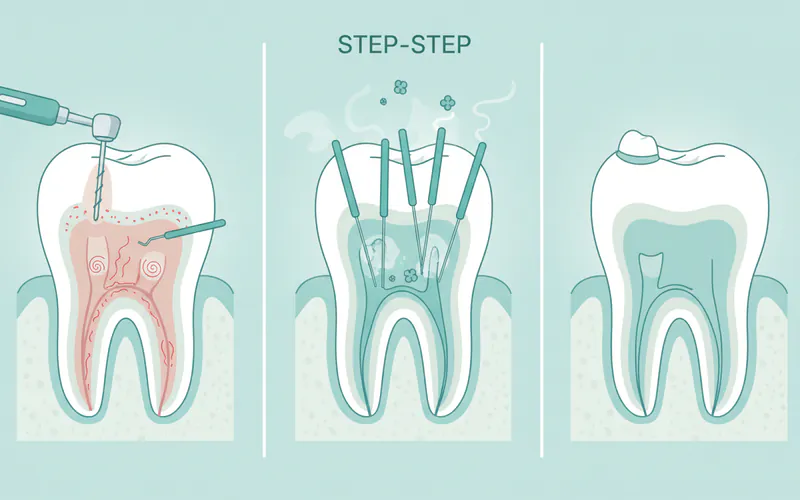
- Anesthesia: The first step is to numb the affected tooth and surrounding area with a local anesthetic. This ensures you feel no pain during the procedure.
- Dental Dam Placement: A small sheet of latex or non-latex material called a dental dam is placed over the tooth, isolating it from the rest of the mouth. This keeps the tooth clean and dry, preventing bacteria from saliva from entering the tooth and protecting you from ingesting materials used during the procedure.
- Access Opening: A small opening is carefully made through the crown of the tooth to access the pulp chamber and the root canals.
- Pulp Removal: Using specialized, very fine instruments called endodontic files, the infected or inflamed pulp tissue is carefully removed from the pulp chamber and the root canals.
- Cleaning and Shaping: The root canals are thoroughly cleaned, disinfected, and shaped to prepare them for filling. This involves using various sizes of files and irrigating the canals with antimicrobial solutions to remove bacteria and debris. ``
- Filling the Canals (Obturation): Once the canals are meticulously cleaned, shaped, and disinfected, they are filled with a biocompatible, rubber-like material called gutta-percha. A dental adhesive (sealer) is used with the gutta-percha to ensure a complete seal, preventing re-infection.
- Temporary Filling: A temporary filling is placed in the access opening to seal the tooth until the permanent restoration (usually a crown) can be placed.
- Permanent Restoration: This is a crucial final step. After a few weeks of healing, you will return to your dentist to have a permanent crown or a permanent filling placed. A crown is usually recommended, especially for back teeth (molars and premolars), to protect the now brittle tooth from fracture and restore its full function.
Recovery Timeline and Aftercare
Most patients find recovery from a root canal to be relatively straightforward.
- Immediate Aftercare:
- Avoid chewing on the treated tooth until your permanent crown or restoration is placed, as the tooth is vulnerable to fracture.
- It's normal to experience some mild discomfort, tenderness, or sensitivity for a few days after the procedure, especially as the local anesthetic wears off.
- Over-the-counter pain relievers (like ibuprofen or acetaminophen) are usually sufficient to manage any pain. Your dentist may prescribe stronger medication if necessary.
- Recovery Timeline:
- The initial soreness typically subsides within a few days to a week.
- Once the permanent crown is placed, the tooth should feel and function like any other tooth.
- Complete healing of the tissues around the root can take several months, which your dentist will monitor with follow-up X-rays.
- Long-Term Care:
- Maintain excellent oral hygiene: brush twice daily, floss daily, and use an antimicrobial mouthwash.
- Continue regular dental check-ups and professional cleanings.
- Avoid hard, sticky foods that could damage your crown or cause a temporary filling to dislodge.
- If you grind or clench your teeth (bruxism), your dentist might recommend a nightguard to protect your newly restored tooth.
Prevention Strategies
Preventing the need for a root canal primarily involves maintaining excellent oral hygiene and addressing dental problems promptly:
- Practice Good Oral Hygiene: Brush your teeth twice a day with fluoride toothpaste and floss daily to remove plaque and food particles, preventing cavities and gum disease.
- Regular Dental Check-ups and Cleanings: Visit your dentist at least twice a year for professional cleanings and examinations. Early detection and treatment of cavities can prevent them from reaching the pulp.
- Treat Cavities Promptly: Don't delay treatment for even small cavities. The sooner they are filled, the less chance they have to progress and infect the pulp.
- Wear a Mouthguard: If you play contact sports, wear a custom-fitted mouthguard to protect your teeth from trauma that could lead to pulp damage. If you clench or grind your teeth at night, a nightguard can prevent excessive wear and potential cracks.
- Avoid Chewing Hard Objects: Don't chew on ice, popcorn kernels, or non-food items like pen caps, which can crack or chip teeth.
- Limit Sugary and Acidic Foods/Drinks: These contribute to tooth decay.
Cost Ranges in the US (with/without insurance)
The cost of a root canal in the United States can vary significantly based on several factors:
- Location of the Tooth:
- Front Teeth (Incisors/Canines): These typically have one root canal and are the least expensive. Cost without insurance: $700 - $1,200.
- Premolars (Bicuspids): These usually have one or two root canals. Cost without insurance: $800 - $1,500.
- Molars: These teeth have multiple (often three or more) root canals and are the most complex to treat, thus the most expensive. Cost without insurance: $1,000 - $2,000+.
- Complexity of the Case: Severely curved canals, calcified canals, or re-treatment cases can increase the cost.
- General Dentist vs. Endodontist: Endodontists (specialists) often charge more than general dentists due to their advanced training, specialized equipment, and expertise.
- Geographic Location: Costs can vary depending on the state, city, and even neighborhood.
Cost with Dental Insurance: Most dental insurance plans typically cover a portion of root canal treatment, often 50% to 80% after your deductible is met. Your out-of-pocket cost with insurance could range from $200 - $800+, depending on your plan's coverage, your deductible, and the total fee.
Important Note: The costs listed above do not include the price of the permanent restoration (e.g., a dental crown), which is almost always necessary after a root canal. A crown can add an additional $800 - $2,500+ to the overall cost, depending on the material and the complexity. It is essential to factor in this additional cost when planning your treatment.
``
For Parents / Pediatric Considerations
Children's teeth, both primary (baby) and young permanent teeth, can also require procedures similar to root canals. Early intervention is crucial:
- Pulpotomy and Pulpectomy for Baby Teeth: If a baby tooth develops a deep cavity or is injured, the pulp can become infected. Instead of immediate extraction, which can lead to space loss and problems for the developing permanent tooth, a pulpotomy or pulpectomy (as described earlier) may be performed. These procedures aim to save the baby tooth until it's naturally ready to fall out, preserving the space for the permanent tooth.
- Apexification and Apexogenesis for Young Permanent Teeth: When a permanent tooth erupts, its roots are not fully developed. If such a tooth suffers trauma or decay, it might require apexogenesis (to encourage continued root development) or apexification (to create a seal at the root tip). These treatments are vital to allow the tooth to mature and become stronger, avoiding premature loss.
- Trauma is Common: Children are prone to dental injuries during play or sports. Any dental trauma should be evaluated by a dentist immediately, as even a seemingly minor injury could affect the pulp and lead to future complications.
- Early Diagnosis is Key: Just like adults, children can experience pain, sensitivity, or swelling from infected teeth. Regular dental check-ups are essential for detecting problems early.
Frequently Asked Questions
Is a root canal painful?
Contrary to popular belief, modern root canal treatment is typically not painful. Thanks to effective local anesthesia, the procedure itself is often no more uncomfortable than getting a routine filling. The severe pain often associated with root canals is actually caused by the infection or inflammation before the procedure, not the treatment itself. The root canal treatment is designed to relieve that pain.
How long does a root canal take?
The duration of a root canal procedure usually ranges from 1 to 2 hours for a single tooth. Simpler cases, like front teeth with one canal, might take less time, while molars with multiple, complex canals could take longer. Many root canals can be completed in a single appointment, but some complex cases or re-treatments may require two visits.
What are the alternatives to a root canal?
The primary alternative to a root canal is tooth extraction. If the tooth is removed, you would then need to consider options for replacing the missing tooth, such as a dental implant, a fixed bridge, or a removable partial denture. While extraction provides immediate relief from infection, preserving your natural tooth with a root canal is almost always the preferred option for long-term oral health and function.
Will my insurance cover a root canal?
Most dental insurance plans do cover a portion of root canal treatment, typically 50% to 80% of the cost after your deductible has been met. However, coverage can vary widely depending on your specific plan. It's always best to contact your insurance provider directly or have your dental office submit a pre-treatment estimate to understand your exact out-of-pocket expenses.
What happens if I don't get a root canal when needed?
Ignoring the need for a root canal can lead to serious consequences. The infection within the tooth will not heal on its own and will likely spread. This can result in:
- Worsening and persistent pain.
- Formation of a dental abscess, which is a pus-filled pocket that can damage the jawbone.
- Facial or neck swelling.
- Spread of infection to other parts of your body, potentially leading to systemic health issues, fever, and severe illness.
- Eventual loss of the tooth, as the infection weakens its supporting structures.
Do I need a crown after a root canal?
In most cases, yes, a dental crown is highly recommended after a root canal, especially for molars and premolars. A root-canaled tooth becomes more brittle and susceptible to fracture because the pulp (which provides nourishment) has been removed, and some tooth structure is lost during the procedure. A crown encases the entire tooth, providing essential strength and protection against chewing forces, restoring its function and preventing future breakage. Front teeth might sometimes only require a permanent filling, but a crown is often still a good idea for added protection and aesthetics.
Who performs root canal procedures?
Both general dentists and endodontists perform root canal procedures. A general dentist can perform many routine root canals. However, for more complex cases, such as those involving severely curved canals, re-treatment, or diagnostic challenges, your general dentist may refer you to an endodontist. An endodontist is a dental specialist who has completed additional years of training specifically focused on diagnosing and treating diseases of the dental pulp and the root structures of teeth.
How successful are root canals?
Root canal treatment is highly successful, with success rates often exceeding 95% when performed correctly. With proper care and a good permanent restoration, a tooth treated with a root canal can last a lifetime, functioning just like your other natural teeth.
When to See a Dentist
It's crucial to seek dental attention if you experience any signs or symptoms of a potential pulp infection or damage.
Emergency Signs (See a Dentist Immediately):
- Severe, persistent tooth pain that doesn't subside with over-the-counter pain relievers.
- Swelling in your face or jaw, indicating a spreading infection.
- A pimple-like bump on your gums (abscess), suggesting infection drainage.
- Fever in conjunction with tooth pain or swelling.
- Difficulty swallowing or breathing, which could signify a serious, rapidly spreading infection.
Routine Care (Schedule an Appointment Soon):
- Any prolonged sensitivity to hot or cold.
- Noticeable darkening or discoloration of a tooth.
- Pain when chewing or biting down.
- Tenderness or mild swelling in your gums around a specific tooth.
Do not wait for pain to become unbearable. Early diagnosis and treatment can prevent the infection from worsening, potentially saving your tooth and preventing more extensive health problems. Regular dental check-ups are your best defense against such issues, allowing your dentist to identify problems before they become critical.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.