Pulp
5,691 words · 19 min read
Quick Definition
The soft tissue inside a tooth containing blood vessels, nerves, and connective tissue. The pulp nourishes the tooth during development and provides sensation throughout life.
Pulp
Short Definition: The soft tissue inside a tooth containing blood vessels, nerves, and connective tissue. The pulp nourishes the tooth during development and provides sensation throughout life.
Related Terms: Root Canal, Pulpitis, Dentin, Endodontics
The pulp, often referred to as the "heart" of your tooth, is a vital component nestled deep within its core. Far from being an inert structure, the pulp is a living, dynamic tissue essential for the health, development, and sensation of your teeth. Without a healthy pulp, a tooth cannot receive the necessary nourishment to stay vibrant, nor can it communicate issues like decay or injury through pain signals.
Understanding "what is pulp" and its critical role is fundamental to comprehending many common dental problems and their treatments. From the earliest stages of tooth formation to the ongoing health of an adult tooth, the pulp plays an indispensable part. When the pulp becomes inflamed or infected—a condition known as pulpitis—it can lead to severe pain and, if left untreated, could result in the loss of the tooth.
While everyone has pulp within their teeth, problems affecting the pulp are remarkably common. Deep cavities, dental trauma, and repeated procedures are frequent culprits. In the United States, millions of teeth are saved each year through procedures like Root Canal therapy, which directly addresses issues within the pulp. For instance, according to the American Association of Endodontists (AAE), over 15 million root canals are performed annually, underscoring the prevalence of pulp-related diseases. This article will be your definitive guide to understanding the pulp, its functions, common issues, and how modern dentistry works to preserve your natural teeth.
Key Takeaways:
- The dental pulp is the living tissue inside a tooth, containing nerves, blood vessels, and connective tissue.
- It is crucial for a tooth's development, providing nourishment, and transmitting sensations like hot, cold, and pain.
- Pulp is located within the pulp chamber in the crown and the root canals in the roots.
- Damage to the pulp, often from deep cavities or trauma, can lead to painful inflammation (pulpitis) or infection.
- Root Canal treatment is the primary procedure used to save a tooth when its pulp becomes irreversibly damaged or infected.
- Preserving pulp health through good oral hygiene and prompt dental care is essential to avoid severe dental issues.
What is Pulp? A Deep Dive into the Tooth's Living Core
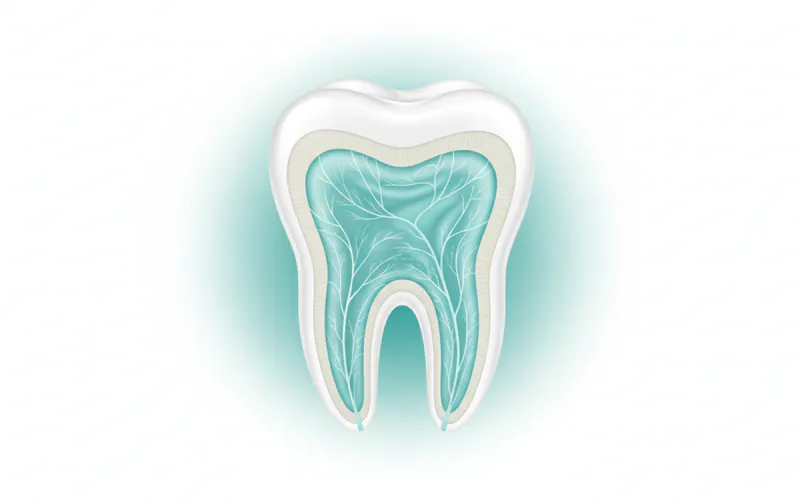
To truly understand the pulp, we must first appreciate its unique placement within the tooth's intricate architecture. Each tooth is composed of several distinct layers: the hard outer enamel, the underlying dentin, and then the innermost pulp.
Anatomy of the Pulp: The pulp occupies a space known as the pulp cavity, which extends from the crown of the tooth down into the roots.
- Pulp Chamber: This is the portion of the pulp cavity located within the crown of the tooth. It's typically larger and more expansive.
- Radicular Pulp (Root Canal): Extending from the pulp chamber into each root of the tooth are narrow, tube-like spaces called root canals. Each canal contains radicular pulp tissue. At the very tip of each root, these canals open into the surrounding bone through a tiny hole called the apical foramen. This opening allows blood vessels, nerves, and lymphatic vessels to enter and exit the pulp, connecting it to the body's overall circulatory and nervous systems.
Composition of the Pulp: Despite its small size, the pulp is a remarkably complex and highly specialized connective tissue. It consists of:
- Odontoblasts: These specialized cells line the periphery of the pulp, adjacent to the dentin. Their primary role is to form new dentin throughout life, a process known as dentinogenesis. They are also involved in transmitting sensory signals.
- Fibroblasts: The most numerous cells in the pulp, responsible for producing the collagen fibers and ground substance that make up the pulp's extracellular matrix.
- Blood Vessels: An extensive network of arterioles, venules, and capillaries that supply nutrients to the odontoblasts and other pulp cells and remove waste products. This rich blood supply is critical for pulp vitality.
- Nerves: The pulp contains both sensory (afferent) and autonomic (sympathetic) nerve fibers. The sensory nerves are responsible for transmitting pain, temperature, and pressure sensations. They are primarily responsible for the acute pain experienced when the pulp is irritated or infected. The autonomic nerves regulate blood flow within the pulp.
- Lymphatic Vessels: These vessels are part of the immune system, helping to drain fluid and transport immune cells, playing a role in defense against infection.
- Extracellular Matrix: A gel-like substance composed of collagen fibers, ground substance, and various proteins, providing structural support to the pulp cells and facilitating nutrient exchange.
Functions of the Pulp: The pulp performs four crucial functions:
- Formative: During tooth development, the odontoblasts within the pulp are responsible for forming both primary and secondary dentin. Even in mature teeth, odontoblasts continue to produce secondary dentin throughout life in response to stimuli, slowly narrowing the pulp chamber and root canals.
- Nutritive: The extensive blood supply within the pulp nourishes the dentin, keeping it hydrated and vital. This internal supply is essential as enamel and dentin themselves do not have a direct blood supply.
- Sensory: The nerve fibers in the pulp transmit sensations of pain, temperature changes (hot/cold), and pressure to the brain. This sensory function acts as an alarm system, alerting us to potential problems like decay or trauma.
- Defensive/Protective: The pulp has an immune response capability, with various immune cells present to combat bacteria and inflammation. When irritated, odontoblasts can lay down tertiary dentin (also called reparative dentin) to protect the pulp from advancing decay or injury, acting as a barrier.
Pulp Health and Disease: Understanding the Spectrum
A healthy pulp is vital for a healthy tooth. However, due to its delicate nature and enclosed environment, the pulp is highly susceptible to damage and infection.
Causes and Risk Factors for Pulp Damage: The primary threats to pulp health stem from external factors that compromise the tooth's protective layers:
- Deep Dental Caries (Cavities): This is by far the most common cause of pulp damage. As bacteria erode enamel and dentin, they eventually reach the pulp chamber, leading to inflammation and infection. The deeper the cavity, the higher the risk.
- Dental Trauma: Accidents can lead to cracked, chipped, or fractured teeth, or even tooth displacement (luxation). Such injuries can expose the pulp, sever its blood supply, or cause internal bleeding and inflammation.
- Repeated Dental Procedures on the Same Tooth: While necessary, multiple fillings, crowns, or other restorative treatments on the same tooth over time can cumulatively stress the pulp, leading to chronic inflammation.
- Bruxism (Teeth Grinding/Clenching): Chronic grinding can put immense pressure on teeth, leading to small cracks and fractures that can penetrate the dentin and affect the pulp.
- Cracked Tooth Syndrome: Characterized by hairline fractures in the tooth that are often invisible to the naked eye but cause pain upon biting or temperature changes, eventually affecting the pulp.
- Advanced Periodontal Disease: In severe cases, periodontal (gum) disease can progress to affect the bone supporting the tooth. Infection can spread from the gums and bone through the apical foramen into the pulp, or through accessory canals in the roots.
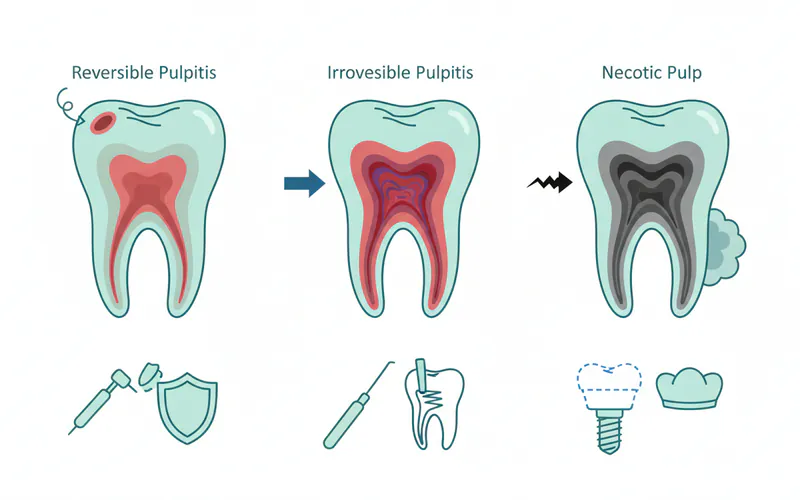
Types and Classifications of Pulp Conditions (Pulpitis): Pulpitis is the medical term for inflammation of the dental pulp. It's a spectrum of conditions, ranging from mild and reversible to severe and irreversible.
-
Reversible Pulpitis:
- Definition: A mild inflammation of the pulp where the tissue is capable of healing if the irritant is removed.
- Causes: Early or shallow cavities, minor trauma, recent dental procedures, exposed dentin, or a cracked tooth that hasn't fully compromised the pulp.
- Symptoms: Sharp, transient pain to cold stimuli (e.g., cold drinks, cold air) that quickly subsides once the stimulus is removed. There's usually no spontaneous pain or pain to heat.
- Prognosis: Excellent if treated promptly.
- Treatment: Addressing the underlying cause, such as placing a filling for a cavity, repairing a minor crack, or desensitizing agents for exposed dentin.
-
Irreversible Pulpitis:
- Definition: Severe inflammation of the pulp where the tissue has been damaged beyond its ability to heal, even if the irritant is removed. It will eventually progress to pulp necrosis if untreated.
- Causes: Deep cavities that have reached or are very close to the pulp, severe trauma, or recurrent decay under a filling.
- Symptoms:
- Symptomatic Irreversible Pulpitis: Characterized by spontaneous pain (pain that occurs without external stimulus), lingering pain to cold (pain that persists for more than 15-30 seconds after the stimulus is removed), pain to heat, or pain that radiates to other areas. The pain can be moderate to severe, often described as throbbing or sharp, and may worsen at night or when lying down.
- Asymptomatic Irreversible Pulpitis: The pulp is irreversibly inflamed but the patient experiences few or no symptoms. This can occur with chronic inflammation and is often discovered during routine X-rays or when the tooth eventually becomes necrotic.
- Prognosis: The pulp will not heal and requires Root Canal treatment or extraction.
- Treatment: Endodontics (root canal therapy) to remove the infected pulp or tooth extraction.
-
Pulp Necrosis (Pulp Death):
- Definition: The complete death of the dental pulp tissue. It is a consequence of untreated irreversible pulpitis, where the inflammation cuts off the blood supply to the pulp.
- Causes: Untreated irreversible pulpitis, severe trauma that severs the blood supply.
- Symptoms: Often, there are no symptoms initially, as the nerve tissue has died. However, the dead tissue can become infected by bacteria, leading to an abscess. Symptoms might then include swelling, pain on biting, a draining fistula (gum boil), or generalized malaise/fever. The tooth may also appear discolored (darker).
- Implications: The dead pulp tissue is a breeding ground for bacteria, which can spread beyond the tooth's root tip into the surrounding bone, causing an infection (apical periodontitis or periapical abscess).
- Treatment: Root Canal treatment (to clean out the necrotic tissue and disinfect the canals) or tooth extraction.
-
Calcific Metamorphosis (Pulp Calcification/Dentinogenesis Imperfecta):
- Definition: A condition where the pulp chamber and root canals become partially or completely filled with calcified tissue (dentin-like material). This is often a response to trauma or slow-advancing decay, where the odontoblasts lay down excessive secondary or tertiary dentin.
- Implications: While often asymptomatic, it can make future Root Canal treatment very challenging due to the narrowed or obliterated canals. The tooth may appear discolored (yellowish-brown).
Signs and Symptoms to Watch For
Recognizing the early signs of pulp problems can save your tooth and prevent significant pain. Be vigilant for any of these indicators:
- Pain:
- Sharp, sudden pain: Often triggered by hot, cold, or sweet foods/drinks. If it's brief, it might be reversible pulpitis or exposed dentin.
- Lingering pain: If pain to cold or hot persists for more than 15-30 seconds after the stimulus is removed, it strongly suggests irreversible pulpitis.
- Spontaneous pain: Pain that arises without any obvious trigger, often throbbing, indicates irreversible pulpitis or an acute infection. It might wake you up at night.
- Pain on biting or chewing: Can indicate inflammation around the root tip (periapical inflammation) or a cracked tooth.
- Sensitivity:
- Heightened sensitivity to hot and cold: Especially if it lingers.
- Sensitivity to sweets: Often indicates a cavity.
- Swelling:
- Swelling around the affected tooth: In the gum, face, or neck, indicating an infection (abscess) has spread from the pulp.
- A "pimple" on the gum: A fistula or sinus tract, which is an outlet for pus draining from an infection.
- Tooth Discoloration: A tooth turning darker (yellowish, grayish, or brownish) can be a sign of internal bleeding within the pulp or pulp necrosis.
- Fever: In more severe cases of infection, especially if an abscess is present, a fever may develop.
- Bad taste in the mouth/Bad breath: Can be associated with pus drainage from an infection.
Diagnosis Process — What Your Dentist Does
When you present with symptoms suggestive of pulp problems, your dentist will conduct a thorough examination to accurately diagnose the condition. This typically involves:
- Patient History and Symptom Description: Your dentist will ask detailed questions about your pain (onset, duration, intensity, triggers, character) and any other symptoms.
- Clinical Examination:
- Visual Inspection: Looking for cavities, cracks, fractures, swelling, or changes in tooth color.
- Percussion Test: Tapping gently on the suspected tooth and adjacent teeth to check for tenderness, which indicates inflammation around the root tip.
- Palpation Test: Gently pressing on the gum tissue near the root tip to check for tenderness or swelling.
- Mobility Test: Checking if the tooth is loose, which can indicate severe infection or trauma.
- Bite Test: Asking you to bite down on a specific instrument (e.g., a "Tooth Slooth") to pinpoint pain from a cracked tooth.
- Pulp Vitality Tests: These tests assess the responsiveness and health of the pulp nerves.
- Cold Test: Applying a cold stimulus (e.g., cotton pellet sprayed with Endo-Ice) to the tooth surface. A quick, transient response suggests normal or reversible pulpitis. A lingering, intense response suggests irreversible pulpitis. No response suggests pulp necrosis.
- Heat Test: Applying a warm stimulus (e.g., heated gutta-percha or a hot water bath). A quick, transient response is normal. Lingering pain or intense pain to heat strongly suggests irreversible pulpitis or necrosis with an acute exacerbation.
- Electric Pulp Test (EPT): Delivers a mild electric current to the tooth. A response indicates nerve vitality; no response suggests necrosis. It doesn't assess the health of the pulp, only its innervation.
- Radiographs (X-rays):
- Periapical X-rays: Provide a detailed view of the entire tooth, including the root and surrounding bone, helping to detect bone loss (radiolucency) at the root tip, which is indicative of an infection.
- Bitewing X-rays: Primarily used to detect cavities between teeth, but can also show deep cavities nearing the pulp.
- Cone-Beam Computed Tomography (CBCT): In complex cases, a 3D image might be used to detect subtle fractures, complex canal anatomy, or the extent of infection more accurately.
By combining these diagnostic tools, your dentist or endodontist (a dental specialist in pulp and root canal treatments) can accurately determine the condition of your pulp and recommend the most appropriate treatment.
Treatment Options with Pros, Cons, and Costs
The treatment for pulp problems depends entirely on the diagnosis—whether the pulpitis is reversible, irreversible, or necrotic.
Treatment for Reversible Pulpitis:
-
Conservative Treatments (Fillings, Desensitizing Agents):
- Procedure: If a cavity is causing reversible pulpitis, removing the decay and placing a dental filling is usually sufficient. For exposed dentin, applying desensitizing agents or bonding agents can help.
- Pros: Simple, cost-effective, preserves the tooth's natural structure.
- Cons: Only effective if the pulp damage is truly reversible.
- Cost Range (US):
- Dental Filling: $100 - $400 (for one surface composite filling, without insurance).
- Desensitizing Treatment: $50 - $150 per tooth.
-
Pulp Capping (Direct/Indirect):
- Procedure:
- Indirect Pulp Cap: When a deep cavity is very close to the pulp but not exposed. A small layer of decay closest to the pulp is intentionally left, and a medicated liner (e.g., calcium hydroxide or mineral trioxide aggregate - MTA) is placed, followed by a permanent filling. The goal is to allow the pulp to heal and form reparative dentin.
- Direct Pulp Cap: If the pulp is accidentally exposed during cavity removal or due to a small trauma, a medicated material (MTA is preferred) is placed directly over the exposed pulp tissue, followed by a permanent restoration. The success depends on the pulp being vital and uninfected.
- Pros: Aims to preserve the vitality of the pulp, avoids Root Canal treatment.
- Cons: Not always successful, especially with direct pulp caps or when there's pre-existing inflammation. May eventually require root canal if it fails.
- Cost Range (US): $150 - $400 (in addition to the cost of the filling).
- Procedure:
Treatment for Irreversible Pulpitis or Pulp Necrosis:
When the pulp is irreversibly damaged or necrotic, it cannot heal and must be removed to prevent further infection and save the tooth.
-
Root Canal Treatment (Endodontics):
- Procedure: This is the standard procedure to save a tooth with irreversible pulpitis or necrosis. The infected or inflamed pulp tissue is removed from the pulp chamber and root canals. The canals are then thoroughly cleaned, shaped, and disinfected. Finally, they are filled with a biocompatible material (usually gutta-percha) and sealed. A permanent crown is typically placed afterward to protect the tooth. (Detailed step-by-step below).
- Pros: Saves the natural tooth, prevents the need for extraction and subsequent prosthetic replacement (implant, bridge), preserves chewing function and aesthetics. High success rate (over 95% for initial treatment).
- Cons: Can be more costly than extraction in the short term, requires multiple appointments (often 1-2, sometimes more), the tooth becomes brittle and requires a crown.
- Cost Range (US, without insurance):
- Anterior (front) tooth: $700 - $1,200
- Premolar tooth: $800 - $1,500
- Molar tooth: $1,000 - $2,000
- Note: These costs do NOT include the necessary crown, which can add another $800 - $2,500.
-
Tooth Extraction:
- Procedure: The entire tooth, including the root, is surgically removed from its socket.
- Pros: Immediate relief from pain, often a quicker and less expensive initial solution than a root canal for severe infection.
- Cons: Loss of a natural tooth, leading to potential chewing difficulties, shifting of adjacent teeth, bone loss in the jaw, and aesthetic concerns. Requires subsequent replacement (dental implant, bridge, or partial denture) to maintain oral health, which adds significant long-term costs and complexity.
- Cost Range (US, without insurance):
- Simple extraction: $75 - $300
- Surgical extraction (more complex, impacted): $150 - $650
- Note: This does not include the cost of tooth replacement, which can range from $1,500 - $6,000+ for an implant and crown, or $2,000 - $5,000 for a bridge.
Comparison Table: Root Canal vs. Extraction
| Feature | Root Canal Treatment (Endodontics) | Tooth Extraction |
|---|---|---|
| Primary Goal | Save the natural tooth | Remove the diseased tooth |
| Procedure | Remove infected pulp, clean and fill canals, crown tooth | Remove entire tooth from socket |
| Treatment Time | Usually 1-2 appointments (plus crown appointment) | Single appointment for extraction |
| Initial Cost | Higher (RC + Crown) | Lower (extraction only) |
| Long-Term Cost | Lower (preserves natural tooth) | Potentially much higher (requires replacement) |
| Natural Tooth | Preserved | Lost |
| Chewing | Preserved | May be impaired without replacement |
| Bone Loss | Minimized | Occurs at extraction site over time |
| Adjacent Teeth | Protected from shifting | May shift into the gap |
| Success Rate | >95% with proper restoration | 100% removal of tooth; success depends on replacement |
Step-by-Step: What to Expect During Root Canal Treatment
Root canal treatment, often performed by a general dentist or an endodontist, is a precise procedure designed to save your natural tooth. Here's what you can generally expect:
- Diagnosis and Anesthesia: After a thorough diagnosis, local anesthesia is administered to numb the tooth and surrounding area, ensuring you are comfortable and pain-free throughout the procedure.
- Dental Dam Placement: A small sheet of latex or non-latex material called a dental dam is placed around the tooth. This isolates the tooth, keeps it clean and dry, and prevents bacteria from saliva from entering the treatment area. It also protects you from ingesting materials used during the procedure.
- Access Opening: A small opening is made through the crown of the tooth, usually on the chewing surface of back teeth or the lingual (tongue side) surface of front teeth. This provides access to the pulp chamber and root canals.
- Pulp Removal (Pulpectomy): Using very fine, specialized instruments (files and reamers), the infected or inflamed pulp tissue is carefully removed from the pulp chamber and each root canal.
- Cleaning and Shaping: The root canals are meticulously cleaned and shaped with increasingly larger endodontic files. This process removes any remaining tissue, bacteria, and debris, and creates a clean, tapered space for the filling material. The canals are continuously irrigated with an antimicrobial solution (like sodium hypochlorite) to disinfect them.
- Disinfection: After shaping, the canals are thoroughly disinfected to eliminate bacteria. In some cases, medication may be placed in the canals and a temporary filling applied, requiring a second appointment to complete the filling process.
- Filling the Canals (Obturation): Once the canals are clean, dry, and free of infection, they are filled with a biocompatible, rubber-like material called gutta-percha. This material is used in conjunction with a sealer to fill and seal the entire canal system, preventing future bacterial re-entry.
- Temporary Filling: A temporary filling is placed in the access opening of the tooth to protect it until a permanent restoration can be placed.
- Permanent Restoration (Crown): This is a critical final step. After a root canal, the tooth can become more brittle and prone to fracture. A dental crown (or sometimes a large filling or onlay) is typically placed over the treated tooth to provide strength, protection, and restore its appearance and function. This usually happens at a separate appointment.
Recovery Timeline and Aftercare
Following a root canal treatment, proper aftercare is essential for successful healing and long-term tooth survival.
Immediate Post-Treatment (First Few Days):
- Numbness: The area will remain numb for several hours after the local anesthesia. Avoid chewing on the treated side until the numbness wears off to prevent accidental biting of your cheek or tongue.
- Mild Discomfort: It's normal to experience some mild discomfort, tenderness, or sensitivity for a few days, especially when chewing. This is due to inflammation from the procedure and should subside. Over-the-counter pain relievers (like ibuprofen or acetaminophen) are usually sufficient.
- Avoid Chewing: Try to avoid chewing on the treated tooth until the permanent crown or restoration is placed. The tooth is more vulnerable to fracture with only a temporary filling.
- Oral Hygiene: Continue your regular brushing and flossing routines, being gentle around the treated tooth.
Weeks to Months Post-Treatment:
- Permanent Restoration: The most crucial step for long-term success is the placement of a permanent crown or suitable restoration. This typically occurs within a few weeks to a month or two after the root canal. Delaying this step significantly increases the risk of fracture or re-infection.
- Healing: The bone around the root tip, if previously infected, will gradually heal over several months to a year.
- Follow-up: Your dentist or endodontist will likely schedule a follow-up appointment (often with an X-ray) a few months after treatment to ensure the infection has cleared and the bone is healing properly.
Long-Term Care and Prognosis: With proper care and a good final restoration, a tooth treated with a root canal can last a lifetime.
- Maintain Good Oral Hygiene: Brush twice daily, floss daily, and use mouthwash as recommended.
- Regular Dental Check-ups: Continue seeing your dentist for routine check-ups and cleanings (every six months) to monitor the health of all your teeth, including the root-canal-treated one.
- Protect Your Teeth: If you grind or clench your teeth (bruxism), wear a nightguard. Avoid chewing on hard objects like ice, pens, or popcorn kernels to prevent fractures.
Prevention Strategies
Preventing pulp damage is always preferable to treating it. A proactive approach to oral health is your best defense:
- Maintain Excellent Oral Hygiene:
- Brush: Brush your teeth at least twice a day for two minutes each time, using a fluoride toothpaste.
- Floss: Floss daily to remove plaque and food particles from between teeth and under the gumline, areas your toothbrush can't reach.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and examinations. Early detection of cavities or other issues can prevent them from progressing to the pulp.
- Prompt Treatment of Cavities: Do not delay treatment for even small cavities. The sooner a cavity is filled, the less chance it has to reach the pulp.
- Protect Your Teeth from Trauma:
- Wear a Mouthguard: If you play contact sports or engage in activities where dental injury is possible, always wear a custom-fitted athletic mouthguard.
- Address Bruxism: If you grind or clench your teeth, especially at night, talk to your dentist about a custom nightguard to protect your teeth from excessive force and potential cracks.
- Avoid Hard Foods and Habits: Refrain from chewing on ice, popcorn kernels, hard candies, or using your teeth as tools (e.g., opening bottles, tearing packages). These habits can lead to chips, cracks, and fractures that damage the pulp.
- Limit Sugary and Acidic Foods/Drinks: These contribute to tooth decay. If consumed, rinse your mouth with water afterward.
Cost Ranges in the US (with/without insurance)
Dental costs can vary significantly based on location, the dentist's fees, the complexity of the case, and the type of insurance. The following are general ranges for the US market, without insurance coverage, with estimates for the potential reduction with insurance.
-
Dental Filling (for reversible pulpitis/small cavity):
- Without Insurance: $100 - $400 (composite, one surface)
- With Insurance: Often 80-100% covered after deductible, reducing out-of-pocket to $0 - $100.
-
Pulp Capping (direct or indirect):
- Without Insurance: $150 - $400 (in addition to filling cost)
- With Insurance: May be covered under restorative procedures, reducing cost to $50 - $200.
-
Root Canal Treatment (Endodontics):
- Without Insurance:
- Anterior (front) tooth: $700 - $1,200
- Premolar tooth: $800 - $1,500
- Molar tooth: $1,000 - $2,000
- With Insurance: Most dental insurance plans cover a portion of root canal treatments, typically 50-80% of the cost after your deductible is met. This could reduce your out-of-pocket expense to $350 - $1,000 per tooth (not including the crown).
- Without Insurance:
-
Dental Crown (post-root canal):
- Without Insurance: $800 - $2,500 (depending on material: porcelain-fused-to-metal, all-ceramic, zirconia)
- With Insurance: Crowns are often covered at 50%, reducing out-of-pocket to $400 - $1,250.
-
Tooth Extraction:
- Without Insurance:
- Simple extraction: $75 - $300
- Surgical extraction: $150 - $650
- With Insurance: Simple extractions are often covered at 80-100%, surgical at 50-80%. Out-of-pocket could be $0 - $200.
- Without Insurance:
-
Dental Implant (replacement for extracted tooth):
- Without Insurance: $3,000 - $6,000+ (per tooth, including implant post, abutment, and crown)
- With Insurance: Coverage varies widely. Some plans may cover a small portion (e.g., 10-20%) or none at all, potentially reducing the cost by $300 - $1,200.
It's crucial to contact your specific dental insurance provider to understand your individual coverage, deductibles, annual maximums, and waiting periods for major procedures. Many dentists also offer payment plans or financing options to help manage costs.
For Parents / Pediatric Considerations
Pulp health is equally important in children, both for their primary (baby) teeth and their developing permanent teeth. The pulp in primary teeth is relatively larger than in permanent teeth, making it more susceptible to decay reaching it quickly.
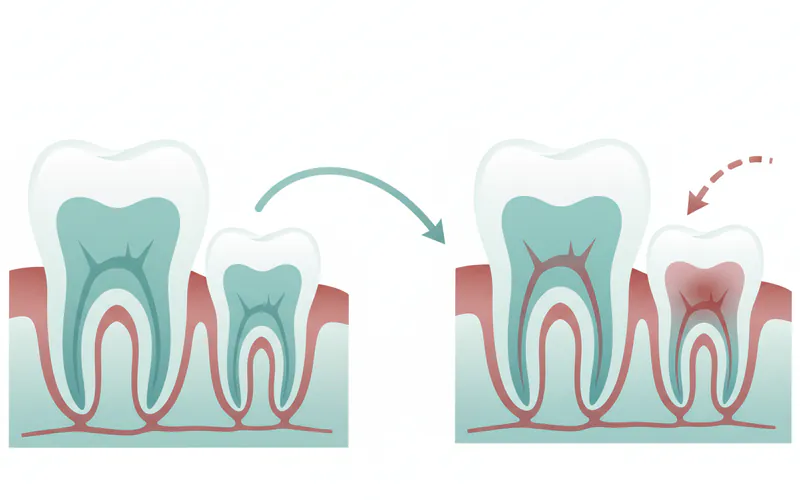
- Primary Teeth Pulp: When decay affects the pulp of a baby tooth, treatment is essential. Not treating it can lead to pain, infection, premature tooth loss, and potential damage to the underlying developing permanent tooth.
- Pulpotomy: If the infection is limited to the pulp in the crown of a baby tooth, a pulpotomy may be performed. Only the infected coronal pulp is removed, and a medicated material is placed over the remaining healthy radicular pulp to preserve its vitality. The tooth is then sealed, often with a stainless steel crown.
- Pulpectomy: If the infection has spread to the pulp in the root canals of a baby tooth, a pulpectomy is done. This involves removing all the infected pulp tissue from the crown and root canals, which are then filled with a resorbable material (that will disappear as the permanent tooth erupts), and the tooth is restored, usually with a crown.
- Immature Permanent Teeth: In young children, permanent teeth may erupt before their roots are fully formed and closed at the apex (root tip).
- Apexogenesis: If the pulp of an immature permanent tooth is vital but inflamed, a pulpotomy-like procedure can be performed to encourage continued root development and apex closure.
- Apexification: If the pulp of an immature permanent tooth is necrotic (dead) and the root tip is open, a procedure called apexification is done. This involves removing the necrotic pulp and placing a material to stimulate the formation of a calcified barrier at the root end, allowing for a permanent root canal filling later.
- Prevention: Good oral hygiene and regular dental visits from an early age are paramount to prevent pulp issues in children. Early detection and filling of cavities are critical.
Frequently Asked Questions
How much does a root canal cost without insurance?
Without insurance, the cost of a root canal typically ranges from $700 to $2,000, depending on the tooth's location (front teeth are generally less expensive than molars). This cost does not include the essential dental crown, which can add another $800 to $2,500.
Is root canal treatment painful?
Modern root canal treatment is performed under local anesthesia, making the procedure itself typically no more painful than getting a filling. Most patients report feeling only pressure. Post-procedure, some mild discomfort or soreness is normal for a few days, which can be managed with over-the-counter pain relievers. The goal of a root canal is to relieve the severe pain caused by infected or inflamed pulp.
How long does a root canal procedure take?
A standard root canal procedure usually takes 1 to 2 hours to complete, often in a single appointment. However, complex cases, re-treatments, or teeth with multiple canals (like molars) might require a second appointment. This time estimate does not include the separate appointment needed for placing the permanent crown.
Are there alternatives to a root canal?
For irreversible pulpitis or pulp necrosis, the main alternative to a root canal is tooth extraction. While extraction provides immediate relief from pain, it results in the loss of the natural tooth, which then requires replacement with a dental implant, bridge, or partial denture to maintain oral health and function, incurring significant additional costs and procedures.
Does dental insurance cover root canals?
Most dental insurance plans do cover a portion of root canal treatments. Typically, plans may cover 50-80% of the cost after your deductible is met, up to your annual maximum. However, coverage varies widely, so it's essential to check with your specific insurance provider for details on your plan.
Can pulp heal itself?
Only in cases of reversible pulpitis can the pulp potentially heal itself once the irritant (like a shallow cavity) is removed. If the inflammation is severe and the pulp is irreversibly damaged or necrotic, it cannot heal on its own and requires professional dental intervention (root canal or extraction) to prevent further infection.
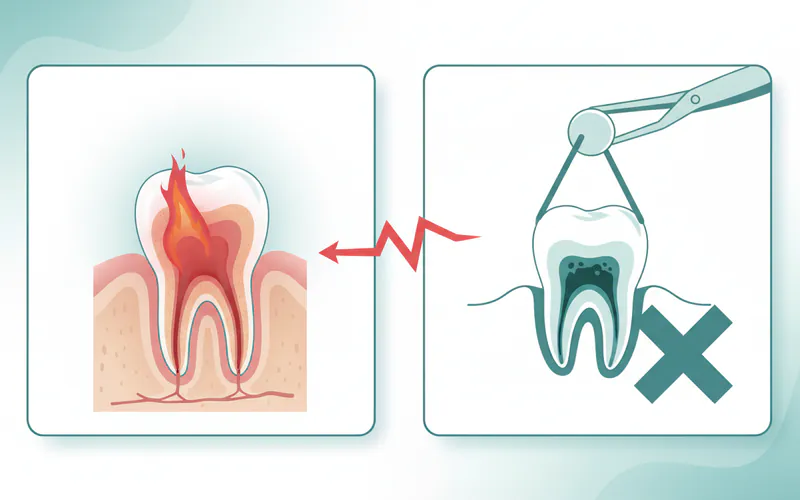
What happens if I don't treat a damaged pulp?
If a damaged or infected pulp is left untreated, the infection will spread beyond the tooth's root tip into the surrounding bone and soft tissues. This can lead to a painful dental abscess, which may cause swelling in your face or jaw, fever, and persistent throbbing pain. In severe cases, the infection can spread to other parts of your body, leading to serious systemic health issues, and eventually, the tooth will be lost.
How can I tell if my pulp is infected?
Signs of an infected pulp often include severe, lingering pain (especially to hot or cold), spontaneous pain that wakes you up at night, pain when chewing, swelling in your gums or face, a "pimple" on your gum, or tooth discoloration. However, sometimes there are no symptoms (asymptomatic infection). If you experience any of these symptoms, it's crucial to see a dentist immediately for diagnosis.
When to See a Dentist
Recognizing when to seek dental care for pulp-related issues is crucial for preserving your oral health and preventing emergencies.
Emergency Signs (See a Dentist Immediately):
- Severe, persistent, or throbbing pain: Especially if it disrupts sleep or doesn't respond to over-the-counter pain medication.
- Visible swelling: In your gums, face, or neck. This indicates a spreading infection that requires urgent attention.
- A "pimple-like" bump on your gum: A fistula or abscess that is draining pus.
- Fever: Accompanied by dental pain or swelling, indicating a serious infection.
- Difficulty swallowing or breathing: This is a rare but life-threatening sign that a dental infection has spread significantly and requires immediate emergency medical care, not just dental.
Routine Care / Non-Emergency Signs (Schedule an Appointment Soon):
- Lingering sensitivity: If a tooth remains sensitive to hot or cold for more than a few seconds after the stimulus is removed.
- Pain on biting or chewing: A persistent ache or sharp pain when pressure is applied to a specific tooth.
- Tooth discoloration: A tooth that has gradually darkened without obvious trauma.
- Dull ache or pressure: A persistent, low-grade discomfort in a tooth or area of your mouth.
- Any concerns about a deep cavity or cracked tooth: Even if currently asymptomatic, these can quickly lead to pulp problems.
Don't wait for pain to become unbearable. Early detection and intervention are key to successfully treating pulp issues and saving your natural tooth. Regular dental check-ups are your best defense against pulp-related problems progressing to the point of severe pain or tooth loss.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.