Endodontics
3,769 words · 13 min read
Quick Definition
The branch of dentistry specializing in the diagnosis and treatment of diseases of the dental pulp and surrounding tissues, most commonly through root canal therapy.
Endodontics: Saving Your Smile from the Inside Out – A Definitive Guide
Welcome to SmilePedia.net, your trusted resource for comprehensive dental health information. This in-depth article will serve as the definitive guide to Endodontics, addressing everything you need to know if you've ever asked "what is endodontics?" or searched for "endodontics dental."
Introduction
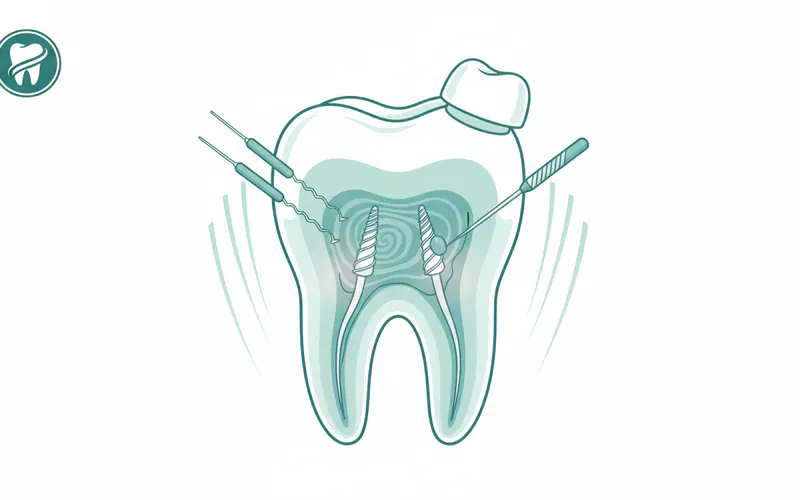
Endodontics is the specialized branch of dentistry focused on the diagnosis, prevention, and treatment of diseases and injuries of the dental pulp – the soft tissue inside your tooth. Often referred to as "root canal specialists," endodontists are experts at saving natural teeth that have become infected or damaged due, most commonly, to deep decay, cracks, or trauma. This vital field plays a crucial role in maintaining overall oral health by preserving teeth that might otherwise require extraction, helping you retain your natural smile, bite, and chewing function.
Millions of people in the United States experience issues with their dental pulp annually. In fact, over 15 million root canal treatments are performed each year, highlighting the widespread need for endodontic care. When the sensitive pulp tissue inside a tooth becomes inflamed or infected, it can lead to severe pain, abscess formation, and ultimately, tooth loss if left untreated. Endodontic procedures provide a pathway to resolve these issues, alleviate pain, and restore the tooth's health and functionality.
Key Takeaways:
- Endodontics is the dental specialty focused on the dental pulp and tooth root.
- Its primary goal is to save natural teeth from extraction due to infection or damage.
- Root canal therapy is the most common endodontic procedure.
- Endodontists are highly trained specialists, though general dentists also perform many endodontic treatments.
- Modern endodontic procedures are designed to be comfortable and effective, dispelling myths about pain.
- Proper endodontic care, followed by a permanent restoration, allows treated teeth to last a lifetime.
Detailed Explanation
What is Endodontics? Deeper Dive into the Core of Your Tooth
The term "Endodontics" originates from the Greek words "endo" (inside) and "odont" (tooth), literally meaning "inside the tooth." This specialty delves deep into the anatomy of your tooth, specifically the pulp chamber and root canals. The pulp is a living tissue composed of nerves, blood vessels, and connective tissue, nestled within the hard layers of dentin and enamel. It's responsible for the tooth's growth and development. Once a tooth is fully mature, it can survive without its pulp, nourished by the surrounding tissues.
When the pulp becomes infected or inflamed, often due to deep cavities, trauma, or cracks, it can lead to excruciating pain and spread infection to the surrounding bone, forming an abscess. An endodontist is a dentist who has completed an additional 2-3 years of specialized training beyond dental school, focusing on complex diagnostic techniques and advanced treatment methods for these internal tooth issues. Their expertise is crucial for preserving your natural teeth and preventing more extensive dental problems.
Types of Endodontic Procedures
While root canal therapy is the most widely known procedure, endodontists perform a variety of treatments to save natural teeth:
- Root Canal Therapy (RCT): This is the most common endodontic procedure. It involves removing the infected or inflamed pulp from inside the tooth, thoroughly cleaning and disinfecting the root canals, and then filling and sealing them to prevent further infection. The tooth is then typically restored with a crown or filling to protect it.
- Endodontic Retreatment: Sometimes, a tooth that has previously undergone root canal therapy may fail to heal or develop new problems months or even years later. This can happen if the initial canals weren't thoroughly cleaned, new decay exposed the canals, or a crack developed. Retreatment involves reopening the tooth, removing the previous filling material, recleaning and reshaping the canals, and then resealing them.
- Apicoectomy (Root-End Resection): If an infection persists at the tip of the root after a conventional root canal, or if there are anatomical complexities preventing complete cleaning through the crown, an apicoectomy may be necessary. This surgical procedure involves making an incision in the gum tissue, removing the very tip of the tooth's root, cleaning out any infected tissue, and placing a small filling to seal the end of the root canal.
- Pulp Capping (Direct and Indirect): When decay or trauma gets very close to the pulp but hasn't fully exposed it (indirect) or has caused a very small, clean exposure (direct), a protective material can be placed over the dentin or directly over the pulp to encourage healing and prevent the need for a full root canal.
- Pulpotomy and Pulpectomy: These are often performed on primary (baby) teeth or immature permanent teeth. A pulpotomy involves removing only the infected portion of the pulp (usually the coronal part), leaving the healthy root pulp intact. A pulpectomy involves removing all the pulp tissue from both the crown and root, similar to a full root canal but often for specific pediatric cases or as an emergency measure.
- Traumatic Dental Injuries: Endodontists are adept at managing injuries like fractured, chipped, displaced (luxated), or knocked-out (avulsed) teeth, which often involve damage to the pulp. Procedures like apexogenesis (encouraging root development) and apexification (creating an apical barrier in immature roots) are vital for saving these teeth.
- Dental Abscess Drainage: In cases of acute infection, an endodontist may drain a dental abscess to relieve pressure and pain before performing definitive treatment.
Causes and Risk Factors for Pulp Damage
The dental pulp is remarkably resilient, but certain factors can compromise its health:
- Deep Decay: This is the most common cause. When a cavity progresses unchecked, bacteria eventually penetrate the enamel and dentin layers, reaching and infecting the sterile pulp chamber.
- Trauma: A direct blow to the mouth can fracture a tooth, crack it, or even dislodge it. These injuries can damage the pulp's blood supply and nerves, leading to inflammation or necrosis (tissue death).
- Cracked or Chipped Teeth: Even small cracks, often invisible to the naked eye, can allow bacteria to seep into the pulp or expose the pulp to chewing forces, leading to irritation and infection. This is sometimes referred to as "Cracked Tooth Syndrome."
- Repeated Dental Procedures: Teeth that have undergone multiple fillings, extensive restorative work, or large fillings close to the pulp can experience cumulative trauma, leading to pulp inflammation over time.
- Advanced Periodontal (Gum) Disease: While primarily affecting the gums and bone supporting the teeth, severe gum disease can sometimes spread infection to the tooth's pulp through accessory canals in the root.
- Bruxism (Teeth Grinding/Clenching): Chronic grinding or clenching can place excessive stress on teeth, leading to cracks and fractures that can impact pulp health.
Signs and Symptoms to Watch For
Recognizing the signs of pulp damage is crucial for timely intervention. While some teeth with pulp issues may be asymptomatic, common indicators include:
- Persistent Tooth Pain: This can range from mild to severe, often described as a throbbing or aching sensation. The pain may worsen when lying down or during chewing.
- Sensitivity to Hot and Cold: While mild, fleeting sensitivity is common, a key sign of pulp damage is prolonged or lingering sensitivity after exposure to hot or cold temperatures, even after the stimulus is removed.
- Swelling and Tenderness: Swelling in the gums, jaw, or face near the affected tooth, along with tenderness when touching the area, can indicate infection has spread.
- Pimple-Like Bump on the Gums (Fistula/Abscess): A small, often recurring, bump on the gums that may discharge pus is a classic sign of an abscess (a localized collection of pus) caused by a deep infection.
- Tooth Discoloration: An infected or dying pulp can cause the tooth to darken or take on a grayish hue.
- Pain When Chewing or Applying Pressure: Discomfort or sharp pain when biting down can indicate inflammation around the tooth's root.
- Fever: In severe cases of infection, especially with an abscess, a fever may develop.
Diagnosis Process — What Your Dentist Does
When you present with symptoms suggestive of pulp issues, your general dentist or endodontist will conduct a thorough examination:
- Patient History: The dentist will ask about your symptoms, including when they started, their intensity, and what triggers them.
- Visual Examination: The tooth and surrounding gums will be inspected for swelling, discoloration, cracks, or signs of decay.
- Palpation and Percussion Tests: The dentist will gently tap on the tooth (percussion test) and press on the gums (palpation) to check for tenderness or inflammation.
- Thermal Tests: A cotton swab with hot or cold material will be applied to the tooth to assess its reaction. A healthy pulp responds quickly and briefly; an inflamed pulp may show prolonged pain, while a necrotic pulp may not respond at all.
- Electric Pulp Test (EPT): A small electrical current is used to stimulate the nerve within the pulp to assess its vitality.
- Radiographs (X-rays): Digital X-rays are essential for visualizing the roots, surrounding bone, and detecting signs of infection such as bone loss around the root tip (a dark area indicating an abscess). ``
- Cone Beam Computed Tomography (CBCT): For complex cases, such as identifying subtle cracks, diagnosing unusual anatomy, or planning an apicoectomy, a 3D CBCT scan provides detailed cross-sectional images that conventional X-rays cannot.
Treatment Options with Pros, Cons, and Costs
When the pulp is irreversibly damaged or infected, the two primary treatment paths are endodontic therapy (saving the tooth) or extraction (removing the tooth).
1. Root Canal Therapy (RCT)
- Pros:
- Preserves your natural tooth: Maintains your original smile, bite, and chewing function.
- Highly successful: With proper care, a treated tooth can last a lifetime.
- Prevents adjacent teeth from shifting: Maintains proper alignment of your teeth.
- Cost-effective long-term: While the initial cost may seem higher than an extraction, it avoids the significant long-term costs and complications of tooth replacement.
- Cons:
- Requires multiple visits: Often 1-2 appointments, plus a separate visit for the final crown.
- Can be expensive without insurance: Initial outlay can be substantial.
- Potential for retreatment: Though rare, a treated tooth may require further intervention if it re-infects or fails to heal.
- Tooth requires a crown: A tooth that has undergone root canal therapy becomes more brittle and typically needs a crown for protection.
- Cost Ranges (US - without insurance):
- Front Tooth (Incisor/Canine): $700 - $1,500
- Bicuspid (Premolar): $800 - $1,800
- Molar: $1,000 - $2,500
- Note: These prices do not include the cost of a permanent crown, which can range from $800 - $2,000.
2. Apicoectomy
- Pros:
- Saves the tooth: An effective last resort for persistent infection after failed conventional root canal therapy.
- Targeted treatment: Addresses issues at the root tip directly, which might be otherwise inaccessible.
- Cons:
- Surgical procedure: More invasive than a conventional root canal, requiring gum incision and bone removal.
- Higher cost: Due to the surgical nature.
- Not 100% successful: While highly effective, there's always a small chance of failure.
- Cost Ranges (US - without insurance): $900 - $2,500
3. Tooth Extraction (Alternative, not endodontic treatment)
- Pros:
- Immediate pain relief: The source of infection is entirely removed.
- Definitive removal: Eliminates the problem tooth.
- Cons:
- Loss of natural tooth: Leads to functional and aesthetic compromises.
- Requires replacement: An empty space needs to be filled to prevent shifting of adjacent teeth, bone loss, and bite problems. Replacements include dental implants, bridges, or partial dentures, which add significant further costs.
- Potential for bone loss: The jawbone can resorb in the area of the missing tooth.
- Cost Ranges (US - without insurance):
- Simple Extraction: $150 - $400
- Surgical Extraction: $300 - $800
- Note: Costs for replacement can be substantial:
- Dental Implant: $2,000 - $6,000+ per tooth (including abutment and crown)
- Dental Bridge: $2,000 - $5,000+ (for a 3-unit bridge)
Comparison Table: Endodontic Treatment vs. Extraction
| Feature | Root Canal Therapy (RCT) | Tooth Extraction (with Replacement) |
|---|---|---|
| Primary Goal | Preserve the natural tooth and its function | Remove the diseased tooth to eliminate infection and pain |
| Procedure | Remove infected pulp, clean, shape, and seal root canals. | Physically remove the entire tooth from the jawbone. |
| Long-term Outcome | Tooth remains, maintains bone structure, functions naturally. | Loss of natural tooth, requires a prosthetic replacement (implant/bridge) |
| Average Cost (US) | $700 - $2,500 (RCT) + $800 - $2,000 (Crown) | $150 - $800 (Extraction) + $2,000 - $6,000+ (Replacement) |
| Impact on Jawbone | Helps preserve existing jawbone | Can lead to jawbone loss (resorption) over time |
| Adjacent Teeth | No impact | Risk of adjacent teeth shifting into the empty space |
| Chewing Function | Restored with the natural tooth | Restored with a prosthetic, which may feel different |
| Recovery | Mild soreness for a few days | Healing of socket, possible swelling and discomfort for a week |
Step-by-Step: What to Expect During Root Canal Therapy
Most root canal procedures can be completed in one to two appointments, depending on the complexity of the case. Here's a typical breakdown:
- Anesthesia: The first step is to numb the affected tooth and surrounding area completely using a local anesthetic. You should feel no pain during the procedure.
- Dental Dam Placement: A small sheet of latex or non-latex material, called a dental dam, is placed around the tooth. This isolates the tooth, keeping it clean and dry from saliva and preventing anything from falling into your mouth.
- Access Opening: The dentist or endodontist creates a small opening in the crown of the tooth to gain access to the pulp chamber and root canals.
- Pulp Removal and Cleaning: Tiny instruments, called endodontic files, are used to carefully remove the infected or damaged pulp tissue from the pulp chamber and each root canal. The canals are meticulously cleaned and shaped.
- Disinfection: Throughout the cleaning process, the canals are irrigated with antiseptic solutions (like sodium hypochlorite) to kill bacteria and flush out debris.
- Filling the Canals: Once the canals are thoroughly cleaned, shaped, and disinfected, they are filled and sealed with a biocompatible, rubber-like material called gutta-percha. This material prevents bacteria from re-entering.
- Temporary Restoration: A temporary filling is placed in the access opening to seal the tooth until a permanent restoration can be placed.
- Permanent Restoration: On a subsequent visit (or sometimes on the same day), your general dentist will place a permanent crown or a robust filling. A crown is typically recommended, especially for molars and premolars, to protect the treated tooth from fracture, as it can become more brittle after root canal therapy. ``
Recovery Timeline and Aftercare
Recovery from root canal therapy is generally straightforward:
- Immediately After: You'll experience residual numbness from the anesthetic for a few hours.
- First Few Days: It's normal to experience some mild discomfort, tenderness, or sensitivity, especially when chewing, as the surrounding tissues heal. This can usually be managed with over-the-counter pain relievers (e.g., ibuprofen, acetaminophen). Avoid chewing hard foods on the treated tooth until your permanent restoration is in place.
- Weeks to Months: The soft tissues and bone around the treated tooth will continue to heal. Any previous swelling or abscess should resolve.
- Long-Term: With proper care, a tooth treated with root canal therapy and restored with a permanent crown can function normally for a lifetime. Maintain excellent oral hygiene, including regular brushing and flossing, and attend your routine dental check-ups.
Prevention Strategies
Preventing pulp damage is always the best approach:
- Maintain Excellent Oral Hygiene: Brush your teeth twice daily with fluoride toothpaste and floss daily to remove plaque and food debris, which cause cavities.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and examinations. Early detection of small cavities can prevent them from reaching the pulp.
- Protect Your Teeth from Trauma: Wear a mouthguard during sports activities or if you clench or grind your teeth (bruxism).
- Avoid Chewing on Hard Objects: Don't chew ice, popcorn kernels, or hard candies, as these can crack teeth.
- Address Dental Problems Promptly: Don't ignore tooth pain or sensitivity. Seek dental care immediately if you suspect a cavity or experience a dental injury.
Cost Ranges in the US (with/without insurance)
As discussed in the "Treatment Options" section, the cost of endodontic treatment in the US can vary significantly based on the tooth's location (front tooth vs. molar), the complexity of the case, the experience of the practitioner (general dentist vs. specialist endodontist), and your geographic location.
- Without Dental Insurance:
- Root Canal Therapy: $700 - $2,500 (plus $800 - $2,000 for a crown).
- Apicoectomy: $900 - $2,500.
- Endodontic Retreatment: Often slightly more expensive than initial root canal, $1,000 - $3,000.
- With Dental Insurance:
- Most dental insurance plans typically cover a significant portion of endodontic procedures, usually 50% to 80%, after your deductible has been met.
- You will be responsible for your deductible, co-pays, and any remaining percentage not covered by your plan.
- It's crucial to contact your insurance provider directly to understand your specific benefits, annual maximums, and whether your chosen dentist or endodontist is in-network. Specialists may sometimes be out-of-network, leading to higher out-of-pocket costs.
For Parents / Pediatric Considerations
Endodontic issues aren't exclusive to adults; children can also require specialized care, especially concerning primary (baby) teeth and newly erupted permanent teeth.
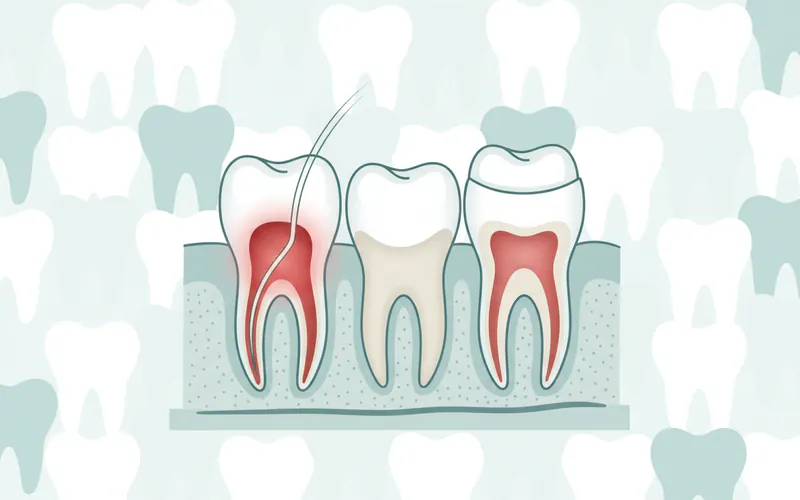
- Primary Teeth: While they are eventually replaced, baby teeth are crucial for proper chewing, speech development, and maintaining space for permanent teeth. If a baby tooth becomes infected, a pulpotomy ("nerve treatment") or pulpectomy may be performed to save it, preventing premature loss that could lead to alignment issues for permanent teeth.
- Traumatic Injuries: Children are highly susceptible to dental trauma (falls, sports injuries), which can damage the pulp of both primary and permanent teeth. Endodontists specialize in treating these injuries, sometimes performing procedures like apexogenesis (encouraging continued root development in immature permanent teeth with vital pulp) or apexification (stimulating root-end closure in immature teeth where the pulp has died).
- Early Detection: Regular dental check-ups are vital for children to catch and treat cavities before they reach the pulp, preventing the need for more complex endodontic procedures.
Frequently Asked Questions
Q1: Is endodontic treatment painful?
A: No, modern endodontic treatment, particularly root canal therapy, is performed with highly effective local anesthesia, making the procedure itself typically painless. The pain you might experience is usually from the infection before treatment. Post-treatment discomfort is usually mild and manageable with over-the-counter pain relievers.
Q2: How long does a root canal take?
A: A typical root canal procedure takes between 90 minutes to 2 hours per appointment. Most cases require one or two appointments, followed by a separate appointment with your general dentist for the final crown.
Q3: How much does a root canal cost in the US?
A: Without insurance, a root canal can cost $700 to $1,500 for a front tooth, $800 to $1,800 for a bicuspid, and $1,000 to $2,500 for a molar. This does not include the cost of the permanent crown ($800 to $2,000), which is usually necessary. Costs vary by region and practitioner.
Q4: Can a root canal be done by my regular dentist, or do I need to see an endodontist?
A: Many general dentists are skilled at performing routine root canals, especially on front teeth and premolars. However, an endodontist (a specialist) is often recommended for more complex cases, such as molars, re-treatments, teeth with unusual anatomy, or surgical procedures like an apicoectomy. Your general dentist will advise you if a referral to an endodontist is appropriate.
Q5: What are the alternatives to a root canal?
A: The only alternative to root canal therapy for an infected or severely damaged tooth is tooth extraction. While extraction provides immediate relief, it results in the loss of your natural tooth, which then requires replacement with a dental implant, bridge, or partial denture. This often entails higher long-term costs, additional procedures, and potential complications like bone loss and shifting teeth.
Q6: Does dental insurance cover endodontic treatment?
A: Most dental insurance plans do cover endodontic treatment. Typically, they cover 50% to 80% of the cost after your deductible, up to your annual maximum. However, coverage specifics vary greatly between plans, so it's essential to contact your insurance provider to understand your individual benefits, co-pays, and whether your dentist or endodontist is in-network.
Q7: How long does a tooth last after a root canal?
A: With proper care, including a timely permanent restoration (usually a crown) and good oral hygiene, a tooth that has undergone root canal therapy can last a lifetime. Regular dental check-ups are important to monitor its health.
Q8: What is an abscess, and how does it relate to endodontics?
A: An abscess is a localized collection of pus caused by a bacterial infection. A dental abscess often forms at the tip of a tooth's root when an infection from the dental pulp spreads to the surrounding bone. Endodontic treatment, such as root canal therapy, is critical for treating an abscess by removing the source of the infection from within the tooth.
When to See a Dentist
Don't wait for excruciating pain to seek dental care. Early intervention can often save a tooth and prevent more serious complications.
- Emergency Signs (See a dentist immediately):
- Severe, persistent, throbbing tooth pain that disrupts sleep or daily activities.
- Significant swelling in your gums, cheek, or jaw.
- A visible abscess (pimple-like bump) on your gums.
- Fever accompanied by dental pain or swelling.
- A knocked-out or severely fractured tooth.
- Routine Care / Lingering Concerns (Schedule an appointment soon):
- Lingering sensitivity to hot or cold foods/drinks.
- Tooth discoloration.
- Tenderness when chewing or touching a specific tooth.
- Any unexplained discomfort or unusual sensations in a tooth.
By understanding Endodontics and being proactive about your dental health, you empower yourself to make informed decisions that can preserve your natural teeth and maintain a healthy, beautiful smile for years to come.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.