Apicoectomy
4,074 words · 14 min read
Quick Definition
A surgical procedure in which the tip (apex) of a tooth's root is removed along with the surrounding infected tissue, and a small filling is placed to seal the root end. It is typically performed when a conventional root canal treatment has failed.
Apicoectomy: A Definitive Guide to Root End Surgery
Introduction
An apicoectomy is a specialized surgical procedure often described as a "second chance" for a tooth that has undergone a root canal but continues to harbor infection or inflammation. At its core, an apicoectomy involves the precise removal of the tip (apex) of a tooth's root along with any surrounding infected tissue. Following this, a small, biocompatible filling material is placed to seal the root end, preventing future bacterial leakage and promoting healing. This procedure falls under the specialty of Endodontics, which focuses on the diagnosis and treatment of diseases of the tooth pulp and surrounding tissues.
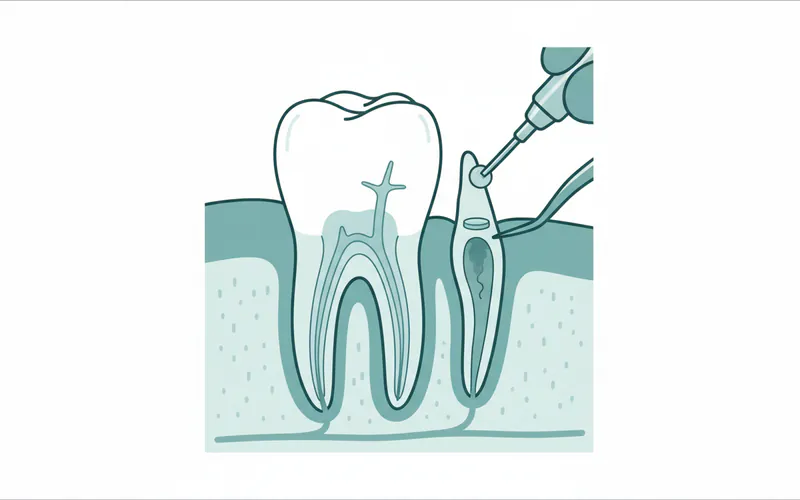
For many individuals, an apicoectomy serves as a critical, tooth-saving intervention when conventional, non-surgical root canal treatment: Everything You Need to Know") or retreatment has proven insufficient. It's typically recommended when infection persists or reappears at the root tip, leading to symptoms like pain, swelling, or the formation of an abscess – a pocket of pus. While root canal treatments boast a high success rate (often exceeding 95% for initial treatments), a small percentage, estimated between 5% to 10%, may fail to heal completely or develop new issues over time. When this occurs, an apicoectomy offers a targeted, effective solution to preserve the natural tooth and avoid extraction, thereby maintaining oral function and aesthetics.
Key Takeaways:
Key Takeaways:
- An apicoectomy is a surgical procedure to remove the infected tip of a tooth's root and seal it.
- It's performed by an endodontist: Everything You Need to Know") or oral surgeon, usually under local anesthesia").
- Often recommended when a prior root canal has failed or infection persists at the root tip.
- A micro-surgical approach enhances precision and success rates.
- It's a tooth-saving alternative to extraction, helping maintain natural bite and appearance.
- Recovery is generally quick, with most patients returning to normal activities within days.
Detailed Explanation
Types and Classifications
While the fundamental concept of an apicoectomy remains consistent – removing the root tip and sealing it – the procedure has significantly evolved, primarily due to advancements in technology and surgical techniques. Modern apicoectomies are overwhelmingly performed using a microsurgical approach.
- Traditional Apicoectomy: Historically, this involved a more open surgical field, using conventional instruments and visual acuity. While effective, it often led to larger incisions, more bone removal, and potentially longer recovery times.
- Microsurgical Apicoectomy (or Micro-apicoectomy): This is the gold standard today. It utilizes a high-powered operating microscope (up to 25x magnification) and specialized micro-instruments. The microscope allows the endodontist to visualize the tiny anatomical structures of the root end, identify accessory canals, and remove only the necessary amount of bone and infected tissue with extreme precision. This minimally invasive approach leads to:
- Increased Success Rates: Better visualization means more thorough removal of infected tissue and more accurate sealing.
- Reduced Post-operative Discomfort: Smaller incisions and less bone removal result in less swelling and pain.
- Faster Healing: The body heals more quickly when less tissue is disturbed.
- Better Prognosis: The tooth has a higher chance of long-term retention.
There aren't distinct "types" of apicoectomy in terms of different surgical goals, but rather different levels of technological assistance and precision employed. When discussing apicoectomies today, it is almost always assumed to be a microsurgical procedure.
Causes and Risk Factors for Needing an Apicoectomy
An apicoectomy is typically indicated when non-surgical endodontic treatments, such as a conventional root canal or root canal retreatment, have not been successful in eliminating infection or inflammation at the root tip. The primary reasons a tooth might require this procedure include:
- Persistent Apical Infection: This is the most common reason. Despite a thorough root canal, bacteria may remain in tiny, uninstrumented accessory canals, within the dentin tubules, or in the surrounding bone, leading to chronic inflammation or an abscess at the root end.
- Inaccessible Canal Anatomy: Some teeth have highly complex root canal systems with severe curves, calcifications, or extremely narrow canals that make it impossible for conventional instruments to thoroughly clean and seal the entire system from inside the tooth.
- Root Perforations or Blockages: During a root canal, instruments can sometimes create a perforation (an artificial hole) in the side of the root, or a canal may become blocked. If these issues cannot be corrected non-surgically, an apicoectomy can seal off the problematic area from the outside.
- Cysts or Granulomas: Persistent infections can lead to the formation of periapical cysts or granulomas around the root tip. These lesions often require surgical removal in conjunction with an apicoectomy for complete resolution.
- Fractured Root Tip: In rare cases, the very tip of a root might be fractured, leading to persistent irritation or infection. If this fracture cannot be addressed through retreatment, an apicoectomy can remove the fractured portion.
- Extruded Root Canal Filling Material: If root canal filling material (gutta-percha) extends beyond the root tip into the surrounding bone and causes irritation, an apicoectomy can remove the excess material and seal the root end properly.
- Diagnostic Uncertainty: Sometimes, even after a root canal, a tooth may exhibit symptoms, but the exact cause isn't clear from X-rays alone. An apicoectomy allows the endodontist to surgically examine the root end and surrounding bone directly, diagnose the problem, and treat it simultaneously.
Risk factors for needing an apicoectomy are essentially factors that increase the likelihood of a root canal failure, such as complex anatomy, inadequate initial treatment, or the development of new decay or trauma after the root canal.
Signs and Symptoms to Watch For
While some individuals might experience no symptoms, a failing root canal or persistent infection typically manifests with several noticeable signs:
- Persistent or Recurrent Pain: This can range from a dull ache to sharp, throbbing pain, particularly when chewing or applying pressure to the affected tooth. The pain might be localized or radiate to adjacent areas.
- Swelling: Swelling in the gums, cheek, or jaw near the affected tooth. This swelling may come and go or be constant.
- Tenderness: The tooth or surrounding gum tissue may be tender to touch or palpation.
- Gum "Pimple" or Fistula: A small, recurring bump on the gums (often called a "gum boil" or "pimple") that may periodically release pus or fluid. This is a sinus tract, indicating a chronic infection draining to the surface.
- Discoloration: In some cases, the tooth or surrounding gum tissue may appear discolored.
- Bad Taste or Odor: A persistent unpleasant taste or smell in the mouth, often due to the drainage of pus.
- Sensitivity to Hot or Cold: While less common after a root canal (as the nerve is removed), persistent sensitivity might indicate a crack or a new infection.
- Asymptomatic: Importantly, some chronic infections at the root tip may be entirely asymptomatic, discovered only during a routine dental X-ray.
If you experience any of these symptoms, especially after a prior root canal treatment, it’s crucial to see a dentist or endodontist promptly.
Diagnosis Process — What Your Dentist Does
Diagnosing the need for an apicoectomy involves a thorough examination and advanced imaging:
-
Clinical Examination:
- Patient History: The dentist will ask about your symptoms (when they started, their intensity, what makes them better or worse) and your medical and dental history, particularly any previous root canals.
- Visual Inspection: Looking for swelling, discoloration, or a fistula (gum "pimple").
- Palpation: Gently pressing on the gums and bone around the tooth to check for tenderness or swelling.
- Percussion: Tapping lightly on the tooth to assess sensitivity.
- Mobility Test: Checking if the tooth is loose.
-
Radiographic Evaluation (X-rays):
- Periapical X-rays: These traditional 2D X-rays provide a good view of the root tip and surrounding bone, allowing the dentist to identify areas of bone loss or radiolucency (dark areas indicating infection/inflammation).
- Panoramic X-rays: Offer a broader view of the entire jaw but are less detailed for specific root apices.
-
Cone Beam Computed Tomography (CBCT): This is perhaps the most critical diagnostic tool for apicoectomies.
- 3D Imaging: Unlike 2D X-rays, CBCT provides a detailed 3D view of the tooth, root canals, surrounding bone, and adjacent anatomical structures (like sinuses or nerves).
- Enhanced Precision: It allows the endodontist to pinpoint the exact location and extent of infection, identify complex root anatomy, detect root fractures that might be invisible on 2D X-rays, and meticulously plan the surgical approach. This significantly improves predictability and success.
Based on these findings, especially the CBCT, the endodontist can determine if an apicoectomy is the most appropriate course of action, differentiate it from other issues, and plan the surgery with maximum precision.
Treatment Options with Pros, Cons, and Costs
When dealing with persistent infection after a root canal, several treatment paths can be considered. The choice depends on the specific cause of failure, the tooth's condition, and patient preferences.
| Treatment Option | Description | Pros | Cons | Estimated Cost Range (US, without insurance) |
|---|---|---|---|---|
| Apicoectomy | Surgical removal of the root tip and infected tissue, sealing the root end. | Tooth-saving procedure, high success rate (especially microsurgical), targeted approach for apical issues. | Invasive surgery, recovery period, higher initial cost than retreatment, slight risk of nerve/sinus involvement. | $900 - $2,500+ per tooth |
| Root Canal Retreatment | Re-opening the tooth, removing old filling material, re-cleaning, reshaping, and re-sealing the canals. | Non-surgical (initially), can address issues within the canal system (e.g., missed canals, inadequate seal). | May not resolve issues outside the canal (e.g., cysts), can be complex/time-consuming, might not be possible if a post/crown is present. | $700 - $1,500+ per tooth |
| Tooth Extraction | Complete removal of the affected tooth. | Eliminates the source of infection definitively, often quickest immediate solution. | Permanent tooth loss, requires subsequent replacement (implant, bridge, denture) to maintain function and bone health, can be more costly long-term. | $150 - $600 (simple), $250 - $800+ (surgical) |
| Observation | Monitoring the tooth with regular check-ups and X-rays if it is asymptomatic or symptoms are very mild. | No immediate cost or intervention. | Infection can worsen, potentially leading to more extensive damage, acute pain, or spread of infection, less predictable. | Varies (cost of exams/X-rays) |
Cost Ranges in the US (with/without insurance):
The cost of an apicoectomy in the US can vary significantly based on several factors, including:
-
Location: Urban areas generally have higher costs than rural ones.
-
Complexity: Molar teeth are typically more challenging and thus more expensive than incisors or canines.
-
Endodontist's Fees: Experience and reputation can influence cost.
-
Anesthesia: Type of anesthesia used (local, sedation).
-
Diagnostic Imaging: The use of CBCT adds to the cost.
-
Without Insurance: A typical apicoectomy can range from $900 to $2,500 per tooth. Complex cases, particularly those involving molars, might even exceed $3,000. This fee usually includes the surgical procedure itself but may not cover initial consultations, CBCT scans, or post-operative follow-ups.
-
With Insurance: Most dental insurance plans offer some coverage for endodontic surgery. The percentage covered can range from 50% to 80%, depending on your specific plan and deductible. You will be responsible for the remaining co-pay. It's crucial to contact your insurance provider directly to understand your specific benefits and estimated out-of-pocket costs before proceeding with the procedure.
Step-by-Step: What to Expect During Treatment
An apicoectomy is typically performed by an endodontist (a dental specialist in root canals and related surgeries) or sometimes an oral surgeon. The procedure usually takes 30 to 90 minutes, depending on the tooth's location and complexity.
- Anesthesia: The area around the tooth will be numbed with a local anesthetic (like Novocain or lidocaine). If you're anxious, your endodontist might offer sedation options (e.g., nitrous oxide, oral conscious sedation) to help you relax.
- Incision: A small incision is made in the gum tissue near the affected tooth. This creates a flap, which is gently lifted to expose the underlying bone and root tip.
- Bone Removal (Osteotomy): A small amount of bone covering the root tip is carefully removed using specialized instruments. This step is precise, often guided by the prior CBCT scan, to access the infected area.
- Infected Tissue Removal: The infected or inflamed tissue, granuloma, or abscess around the root tip is thoroughly cleaned and removed. ``
- Root Tip Resection: The very tip of the root (typically 1-3 millimeters) is precisely removed. This step ensures that any tiny, uninstrumented accessory canals at the very end of the root, which might harbor bacteria, are excised.
- Retro-preparation: A small cavity is prepared in the cut surface of the root end. This preparation is meticulously cleaned.
- Retro-filling (Root End Filling): A biocompatible material, such as Mineral Trioxide Aggregate (MTA) or Super EBA cement, is carefully placed into the prepared cavity to seal the root canal system from the outside. This prevents bacteria from re-entering the tooth through the root tip. ``
- Tissue Repositioning and Suturing: The gum flap is gently repositioned back over the bone, and sutures (stitches) are placed to hold it in place. The sutures are often self-dissolving but may need to be removed by the endodontist after about a week.
- Post-Operative Instructions: You'll receive detailed instructions for aftercare, including pain management, diet, and oral hygiene.
Recovery Timeline and Aftercare
Recovery from an apicoectomy is generally straightforward, with most patients resuming normal activities within a few days.
Immediate Aftercare (First 24-72 hours):
- Pain Management: You will likely experience some discomfort as the local anesthetic wears off. Your endodontist may prescribe pain medication (e.g., ibuprofen, acetaminophen, or a stronger prescription opioid if needed) or recommend over-the-counter options. Take as directed.
- Swelling: Some swelling of the lip, gum, or cheek is normal. Apply a cold compress or ice pack to the outside of your face (15 minutes on, 15 minutes off) for the first 12-24 hours to minimize swelling. Swelling usually peaks around 24-48 hours and then gradually subsides.
- Bleeding: Slight oozing or discoloration of saliva is normal. Avoid vigorous rinsing, spitting, or disturbing the surgical site.
- Diet: Stick to soft foods and liquids for the first few days. Avoid hot, spicy, or crunchy foods that could irritate the surgical site. Chew on the opposite side of your mouth.
- Oral Hygiene: Gently brush other areas of your mouth. For the surgical site, avoid brushing directly. Your endodontist might recommend a prescription antimicrobial mouth rinse (e.g., chlorhexidine) to keep the area clean.
- Activity: Avoid strenuous physical activity for at least 24-48 hours to prevent increased bleeding or swelling. Rest is important for healing.
- Smoking/Alcohol: Avoid smoking and alcohol, as they can impair healing and increase the risk of complications.
- Antibiotics: If prescribed, take the full course of antibiotics exactly as directed, even if you feel better.
Longer-Term Recovery (First Week and Beyond):
- Suture Removal: If non-dissolving sutures were used, you'll have an appointment to have them removed around 5-7 days after the procedure.
- Bruising: Bruising on the face or neck can occur, particularly in individuals prone to bruising. It will resolve on its own, typically within a week or two.
- Healing: The soft tissues usually heal within a couple of weeks. Bone healing takes longer, often several months.
- Follow-up Appointments: Your endodontist will schedule follow-up appointments (typically at 6 months and 1 year) to check the healing progress with X-rays. Full bone healing around the root tip can take up to a year or more. ``
Potential Complications (Rare): While apicoectomies are highly successful, potential complications include:
- Continued infection (rare, requiring further treatment).
- Nerve damage (very rare, especially with careful planning, but possible if a nerve is very close to the surgical site).
- Sinus perforation (if the tooth is in the upper jaw and close to the maxillary sinus).
- Fracture of the root or tooth (rare).
Following your endodontist's instructions precisely is the best way to ensure a smooth recovery and successful outcome.
Prevention Strategies
While an apicoectomy is a treatment for a failed root canal, preventing the initial need for a root canal, and ensuring its success, are the primary preventive strategies.
-
Excellent Oral Hygiene:
- Brush twice daily: Use fluoride toothpaste and brush for at least two minutes each time.
- Floss daily: Remove plaque and food particles from between teeth and under the gumline.
- Use mouthwash: An antiseptic mouthwash can help reduce bacteria. Good oral hygiene significantly reduces the risk of dental decay, gum disease, and subsequent pulp infections that necessitate root canal treatment.
-
Regular Dental Check-ups and Cleanings:
- Visit your dentist at least twice a year for professional cleanings and examinations.
- Early detection of cavities, cracks, or gum disease allows for timely intervention before infections reach the pulp.
-
Prompt Treatment of Dental Problems:
- Don't ignore toothaches, sensitivity, or fractured teeth. Seek dental attention immediately.
- Treating cavities while they are small prevents them from deepening and reaching the pulp.
-
Protect Your Teeth:
- Wear a mouthguard during sports to prevent dental trauma that could damage teeth and lead to pulp exposure or infection.
- If you grind or clench your teeth (bruxism), wear a nightguard to protect against cracks and fractures.
-
Quality Root Canal Treatment:
- If you need a root canal, seek treatment from an experienced general dentist or an endodontist. Specialists have advanced training, equipment (like operating microscopes), and expertise to perform root canals with the highest success rates, minimizing the chances of failure and the subsequent need for an apicoectomy.
- Ensure proper post-root canal restoration (crown) is placed in a timely manner to protect the treated tooth from re-infection or fracture.
For Parents / Pediatric Considerations
Apicoectomies are generally performed on permanent teeth. While root canal treatments can be performed on primary (baby) teeth, the need for an apicoectomy on a baby tooth is extremely rare, as extraction is typically the preferred course if infection persists.
However, an apicoectomy can be considered for a permanent tooth in an adolescent or younger adult if a prior root canal has failed. This is particularly true for anterior (front) teeth, which are crucial for aesthetics and speech. When considering an apicoectomy in a younger patient, the endodontist will carefully evaluate:
- Root Development: If the root is still developing (an "open apex"), other procedures like apexification or regenerative endodontic procedures might be preferred to encourage further root growth. An apicoectomy is generally reserved for fully formed permanent roots.
- Patient Cooperation: The procedure requires the child or adolescent to remain still for an extended period, so their ability to cooperate is important. Sedation might be a more common consideration in younger patients.
- Overall Oral Health: The dentist will assess the child's overall oral hygiene and commitment to post-operative care.
In essence, the principles of apicoectomy remain the same regardless of age, provided the tooth is a permanent one with a fully developed root. The decision is made on a case-by-case basis, always prioritizing the long-term health and preservation of the tooth.
Frequently Asked Questions
How much does an apicoectomy cost?
The cost of an apicoectomy in the US typically ranges from $900 to $2,500 per tooth without insurance, with molars often being more expensive due to their complexity. This cost can vary by geographic location, the specific tooth, and the endodontist's fees. With dental insurance, you can expect coverage of 50% to 80% after deductibles, though it's essential to verify your specific plan benefits.

Is an apicoectomy painful?
During the procedure, you will be completely numbed with local anesthesia, so you should feel no pain, only pressure. After the procedure, it's normal to experience some discomfort, swelling, and bruising for a few days. This can usually be managed effectively with over-the-counter pain relievers or prescription medication provided by your endodontist. Most patients report that the post-operative pain is manageable and subsides quickly.
How long does an apicoectomy take?
An apicoectomy usually takes between 30 to 90 minutes to complete. The exact duration depends on the specific tooth being treated (e.g., front teeth are generally quicker than molars), the complexity of the root anatomy, and the extent of the infection.
What are the alternatives to an apicoectomy?
The primary alternatives to an apicoectomy for a failed root canal include:
- Root Canal Retreatment: Re-opening the tooth, cleaning, and re-sealing the canals.
- Tooth Extraction: Removing the tooth entirely, which would then require replacement with a dental implant, bridge, or partial denture.
- Observation: In some asymptomatic cases, the dentist might recommend monitoring the tooth, though this carries the risk of the infection worsening over time. The best alternative depends on the specific cause of the root canal failure and the tooth's condition.
Does dental insurance cover apicoectomies?
Most dental insurance plans do offer coverage for apicoectomies, as it's considered a major restorative procedure. Coverage typically ranges from 50% to 80% of the procedure cost, after you've met your deductible. However, plan benefits vary greatly, so it's always advisable to contact your insurance provider directly before the procedure to understand your specific coverage and estimated out-of-pocket expenses.
What is the success rate of an apicoectomy?
The success rate of modern, microsurgical apicoectomies is quite high, generally ranging from 85% to 95%. Factors influencing success include the skill of the endodontist, the type of tooth, the extent of the infection, and the patient's overall health and adherence to post-operative care instructions.
Can I eat normally after an apicoectomy?
Immediately after the procedure, you should stick to soft foods and liquids for a few days. Avoid hot, spicy, or crunchy foods that could irritate the surgical site. As healing progresses, you can gradually reintroduce more solid foods, but it's best to avoid chewing on the treated side for about a week. Your endodontist will provide specific dietary instructions.
Is an apicoectomy a last resort?
An apicoectomy is often considered a "last resort" in the sense that it's typically performed after non-surgical root canal treatment or retreatment has failed. It's a highly specialized surgical procedure reserved for specific situations where conventional methods cannot resolve the infection at the root tip. However, it's a critical and effective tooth-saving option that helps patients avoid extraction and preserve their natural dentition.
When to See a Dentist
Knowing when to seek professional dental care is crucial, especially when dealing with potential complications after a root canal or persistent dental issues.
Emergency Signs (See a dentist immediately):
- Severe, throbbing pain that doesn't subside with over-the-counter pain relievers.
- Rapidly spreading swelling in your face, jaw, or neck, potentially making it difficult to swallow or breathe.
- Fever accompanied by dental pain or swelling.
- Acute facial trauma that has damaged a tooth previously treated with a root canal.
These symptoms can indicate a severe infection that requires urgent attention to prevent it from spreading further and causing more serious health complications.
Urgent, but not always Emergency (See a dentist within 24-48 hours):
- Persistent dull ache or tenderness in a tooth that previously had a root canal.
- Swelling in the gums around a treated tooth, even if mild.
- A gum "pimple" or fistula that appears and disappears, even if it's not painful.
- Sensitivity to chewing or pressure on a previously treated tooth.
- Any concerns about post-operative healing after an apicoectomy (e.g., unexpected bleeding, persistent pain).
Routine Care / Follow-up:
- Regular dental check-ups (every 6 months): Essential for maintaining overall oral health and catching potential issues early.
- Scheduled follow-up appointments with your endodontist after an apicoectomy (typically at 6 months and 1 year) to monitor healing and assess the long-term success of the procedure with X-rays.
Never hesitate to contact your dental professional if you have any concerns about your dental health. Early diagnosis and intervention are key to preserving your teeth and ensuring your overall well-being.
apicoectomyroot end surgeryfailed root canalroot tip removalendodontic surgery
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.