Abscess
4,290 words · 14 min read
Quick Definition
A localized pocket of pus caused by a bacterial infection, occurring either at the tip of a tooth root (periapical abscess) or in the gums alongside a tooth root (periodontal abscess). An abscess requires prompt dental treatment and will not resolve on its own.
Abscess
An abscess-conditions-diseases-everything-you-need-to-know "Complete Guide to Dental Conditions & Diseases: Everything You Need to Know") is a localized pocket of pus that develops due to a bacterial infection. In dentistry, these often occur in one of two primary locations: at the tip of a tooth root (known as a periapical abscess) or within the gums and bone surrounding a tooth (called a periodontal abscess). Regardless of its location, an abscess is a serious condition that signals an active infection requiring prompt professional dental intervention. It will not resolve on its own and can lead to severe health complications if left untreated.
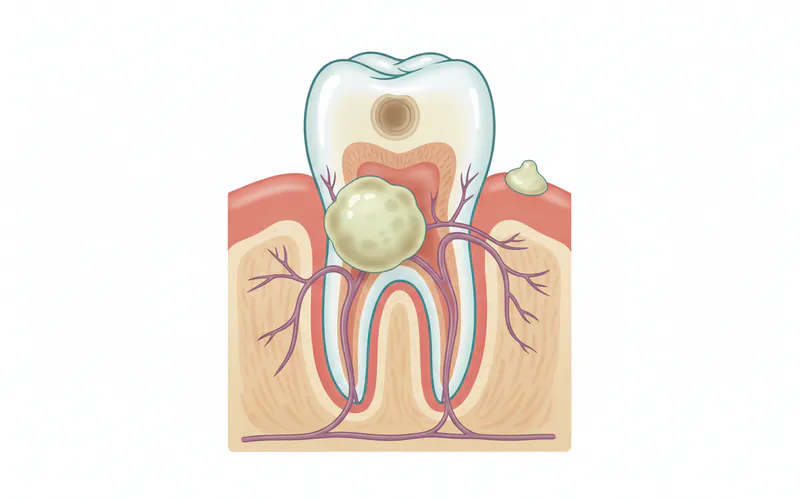
Abscesses are a common dental emergency, affecting millions of Americans annually. They can cause significant pain, disrupt daily life, and, in severe cases, spread the infection to other parts of the body, potentially leading to life-threatening conditions. Understanding the causes, symptoms, and necessary treatments for an abscess is crucial for maintaining optimal oral and overall health.
Key Takeaways:
- An abscess is a localized infection containing pus, often causing severe pain.
- It occurs either at the tooth root tip (periapical) or in the surrounding gum/bone (periodontal).
- Abscesses are caused by bacterial infections and will not heal without dental treatment.
- Symptoms include throbbing pain, swelling, fever, and sensitivity.
- Untreated abscesses can lead to serious, even life-threatening, systemic infections.
- Prompt diagnosis and treatment by a dentist are essential for resolution and prevention of complications.
Detailed Explanation
An abscess represents a body's defensive response to a bacterial invasion. When bacteria penetrate the protective layers of a tooth or gum tissue, the immune system dispatches white blood cells to fight the infection. The accumulation of these dead white blood cells, bacteria, and tissue debris forms pus, which then collects in a confined space, creating the abscess.
Types and Classifications
Understanding the different types of dental abscesses is critical for accurate diagnosis and effective treatment. They are primarily classified by their location:
- Periapical Abscess: This is the most common type, forming at the apex (tip) of a tooth's root. It originates when bacteria invade the dental pulp – the soft tissue inside your tooth containing nerves, blood vessels, and connective tissue. This usually happens due to an untreated deep cavity, a crack or chip in the tooth, or dental trauma that exposes the pulp. The infection spreads down through the root canal to the bone at the root tip, forming a pus-filled sac.
- Periodontal Abscess: This type forms in the gums, specifically in the periodontal pockets that can develop in individuals with periodontal disease (gum disease). Bacteria accumulate in these pockets, leading to inflammation and infection of the gum tissue and supporting bone around the tooth. It can also occur if food particles become lodged in a gum pocket or due to trauma to the gums. Unlike a periapical abscess, the tooth's pulp might be healthy in a periodontal abscess.
- Gingival Abscess: This is a less common and generally less severe type, forming only in the gum tissue, not involving the tooth or periodontal ligament. It typically results from a foreign object (like a popcorn hull or toothbrush bristle) becoming embedded in the gum line, causing a localized infection.
Abscesses can also be classified by their duration:
- Acute Abscess: Characterized by rapid onset, severe pain, and noticeable swelling. It signifies a very active and often painful infection.
- Chronic Abscess: This type may have a slower onset, less intense pain, or even be painless. It often involves a "fistula" or "sinus tract" – a small pimple-like bump on the gum that periodically drains pus, relieving pressure and pain. While less painful, a chronic abscess still represents an active infection that is slowly damaging the surrounding bone.
Causes and Risk Factors
The root cause of any dental abscess is bacterial infection, but various factors can contribute to its development:
For Periapical Abscesses:
- Untreated Tooth Decay (Cavities): The most common cause. When a cavity progresses deeply enough, bacteria penetrate the enamel and dentin to reach the tooth's pulp, leading to inflammation (pulpitis) and subsequent infection.
- Trauma to the Tooth: A chipped, cracked, or fractured tooth can expose the pulp to bacteria. Even a significant blow to a tooth without visible damage can damage the pulp, leading to necrosis (tissue death) and infection.
- Previous Dental Procedures: While rare, a failed or incomplete root canal treatment: Everything You Need to Know") can sometimes lead to a recurrent infection at the root tip.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque and bacteria to accumulate, increasing the risk of decay that can lead to abscess formation.
For Periodontal Abscesses:
- Periodontal Disease (Gum Disease): This is the leading cause. Untreated gingivitis can progress to periodontitis, where bacteria-filled pockets form between the teeth and gums. These pockets can deepen, trapping bacteria and food, leading to an abscess.
- Impacted Food: Food particles (especially seeds, kernels, or fibrous foods) lodged in a deep gum pocket can act as a breeding ground for bacteria and cause an infection.
- Gum Trauma: Injury to the gums, such as aggressive flossing or a foreign object embedding in the tissue, can create an entry point for bacteria.
- Orthodontic Treatment: In rare cases, braces or other orthodontic appliances can sometimes create areas where food traps or trauma occurs, leading to a periodontal abscess.
General Risk Factors for Any Abscess:
- Poor Oral Hygiene: Insufficient brushing and flossing allow bacteria to thrive.
- High Sugar Diet: Frequent consumption of sugary foods and drinks fuels bacteria that cause tooth decay.
- Weakened Immune System: Conditions like diabetes, autoimmune diseases, HIV/AIDS, or medications (e.g., steroids, chemotherapy) can impair the body's ability to fight off infections, making individuals more susceptible.
- Smoking: Tobacco use significantly increases the risk of periodontal disease and impairs healing, making abscesses more likely.
- Dry Mouth (Xerostomia): A lack of saliva reduces the mouth's natural cleansing mechanisms, increasing the risk of decay and gum disease.
Signs and Symptoms to Watch For
Recognizing the signs and symptoms of a dental abscess early is crucial for prompt treatment and preventing complications. While pain is the most common symptom, its nature can vary:
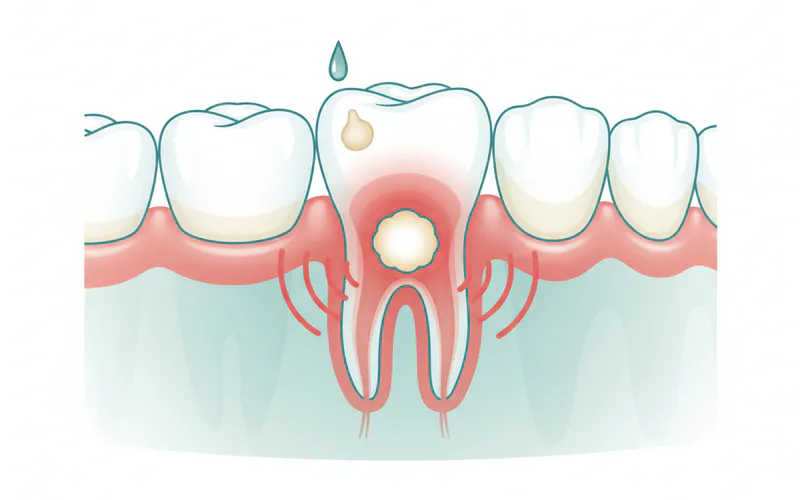
- Persistent, Throbbing Toothache: This is often the hallmark symptom, ranging from mild to severe. The pain may radiate to your ear, jaw, or neck. It often worsens when lying down or with pressure on the affected tooth.
- Sensitivity to Hot and Cold: The affected tooth may become extremely sensitive to temperature changes.
- Sensitivity to Pressure or Chewing: Biting down or touching the tooth can trigger intense pain.
- Swelling: Noticeable swelling in the gum, face, or jaw around the infected tooth. This can sometimes extend to the neck.
- Redness and Tenderness in Gums: The gum tissue around the tooth may appear inflamed, red, and be painful to touch.
- Fever: A sign that the infection is spreading and the body is fighting it.
- Swollen Lymph Nodes: Lymph nodes under your jaw or in your neck may become tender and enlarged as they filter infection.
- Foul Taste in Mouth/Bad Breath: A persistent bitter taste or foul odor may indicate pus drainage, especially if a sinus tract has formed.
- Difficulty Opening Mouth, Chewing, or Swallowing: If swelling is severe, it can restrict jaw movement.
- Pimple-like Bump on the Gums (Fistula/Sinus Tract): This bump may intermittently release pus and blood, which can temporarily relieve pressure and pain.
It's important to note that sometimes a chronic abscess might be asymptomatic or cause only mild, intermittent discomfort, making it harder to detect without a dental exam.
Diagnosis Process — What Your Dentist Does
Diagnosing a dental abscess typically involves a combination of examination and imaging:
- Medical and Dental History: Your dentist will ask about your symptoms, when they started, their severity, and any relevant medical conditions or medications.
- Visual Examination: The dentist will carefully examine your mouth, looking for signs of swelling, redness, a visible cavity, a fractured tooth, or a draining fistula on the gums.
- Palpation: Gentle pressure applied to the affected tooth and surrounding gum tissue can help identify the source of pain and swelling.
- Percussion Test: Tapping on the affected tooth with a dental instrument to check for tenderness, which is a common indicator of inflammation around the root.
- Pulp Vitality Tests: For periapical abscesses, your dentist might use a cold test (applying a cold stimulus to the tooth) or an electric pulp tester to assess the vitality of the tooth's nerve. A non-responsive or dead pulp is often indicative of a periapical infection.
- Periodontal Probing: For suspected periodontal abscesses, the dentist will measure the depth of gum pockets around the teeth to assess the extent of periodontal disease.
- Dental X-rays: These are indispensable for diagnosing an abscess.
- Periapical X-rays: Provide a detailed view of one or two teeth, showing the tip of the root and surrounding bone, often revealing a dark spot (radiolucency) where bone has been destroyed by the infection.
- Panoramic X-rays: Offer a broader view of the entire mouth, which can be useful if the infection is widespread or to rule out other issues.
- 3D Cone Beam CT Scans: In complex cases, a 3D scan can provide an even more detailed image of the bone and root structure, helping to precisely locate the infection and plan treatment.
Treatment Options with Pros, Cons, and Costs
The primary goals of abscess treatment are to eliminate the infection, preserve the tooth if possible, and prevent further complications. Treatment options vary depending on the type and severity of the abscess.
1. Drainage of the Abscess
- Description: The initial step for most acute abscesses involves draining the pus to relieve pressure and pain. This is typically done by making a small incision in the swollen gum tissue (incision and drainage, or I&D) or by accessing the pulp chamber of the tooth if it's a periapical abscess.
- Pros: Immediate pain relief, reduction of swelling, quick removal of infectious material.
- Cons: Not a definitive treatment; only addresses the symptom (pus accumulation), not the source of the infection.
- Cost (US): Varies from $100 to $300, often included as part of a larger treatment plan.
- Antibiotics: Often prescribed alongside drainage to help control the spread of infection, especially if there's significant swelling, fever, or compromised immune system. Antibiotics alone are not a cure for an abscess, as they cannot penetrate the pus-filled cavity effectively.
2. Root Canal Treatment (for Periapical Abscesses)
- Description: If the tooth is restorable, a root canal is the definitive treatment for a periapical abscess. It involves removing the infected pulp tissue from inside the tooth, thoroughly cleaning and shaping the root canals, and then filling and sealing them to prevent reinfection. The tooth is then typically restored with a crown.
- Pros: Saves the natural tooth, preserves chewing function, avoids the need for extraction and subsequent tooth replacement. High success rate (over 95%).
- Cons: Can be a multi-appointment procedure, requires a skilled endodontist for complex cases, relatively higher initial cost compared to extraction.
- Cost (US):
- Front Tooth: $700 - $1,500
- Premolar: $800 - $1,800
- Molar: $1,000 - $2,200
- These costs are for the root canal procedure: Everything You Need to Know") itself, not including the final crown (an additional $800 - $2,000).
3. Periodontal Treatment (for Periodontal Abscesses)
- Description: For a periodontal abscess, treatment focuses on deep cleaning and elimination of the infection within the gum pocket. This often involves scaling and root planing, a procedure that removes plaque and tartar from above and below the gum line and smooths the root surfaces. In some cases, minor surgical procedures like gingival flap surgery may be necessary to access and clean deeper pockets or remove damaged tissue.
- Pros: Can resolve the infection and save the tooth, improves gum health, prevents further bone loss.
- Cons: May require multiple appointments, can be uncomfortable, may involve gum recession.
- Cost (US):
- Scaling and Root Planing (per quadrant): $150 - $400 (a full mouth typically involves 4 quadrants).
- Periodontal Surgery: $500 - $3,000+ per quadrant, depending on complexity.
4. Tooth Extraction
- Description: If the tooth is severely damaged, non-restorable, or if other treatments are not feasible or successful, extraction (removal of the tooth) may be necessary. This eliminates the source of the infection.
- Pros: Immediate and definitive removal of the infection source, often less expensive upfront than a root canal followed by a crown.
- Cons: Creates a gap in the smile, can lead to shifting of adjacent teeth, bone loss in the jaw, and impact chewing ability. Requires subsequent tooth replacement (implant, bridge, or denture) which adds significant cost and time.
- Cost (US):
- Simple Extraction: $75 - $300
- Surgical Extraction: $150 - $650
- Impacted Wisdom Tooth Extraction: $250 - $800+
- These costs do not include the cost of tooth replacement, which can range from $2,000 - $6,000+ for a dental implant.
Comparison Table: Root Canal vs. Extraction for a Periapical Abscess
| Feature | Root Canal Treatment | Tooth Extraction |
|---|---|---|
| Goal | Save the natural tooth, eliminate infection | Remove the infected tooth, eliminate infection |
| Tooth Status | Preserved | Removed, creating a gap |
| Treatment Time | 1-2 appointments for root canal, plus crown placement | 1 appointment for extraction |
| Initial Cost | Higher (root canal + crown) | Lower (extraction only) |
| Long-term Cost | Typically lower if tooth is successfully saved | Significantly higher if tooth replacement is desired |
| Functionality | Maintains natural biting and chewing | Requires replacement for optimal function |
| Bone Health | Preserves jawbone | Leads to localized bone loss over time |
| Complexity | Moderate to high | Simple to moderate (can be complex for impacted teeth) |
Step-by-Step: What to Expect During Treatment
While treatments vary, here's a general idea of what to expect:
1. Initial Visit & Drainage:
- Your dentist will confirm the diagnosis, often with an X-ray.
- Local anesthetic will be administered to numb the area.
- For immediate relief, the dentist may make a small incision in the gum to drain the pus. A rubber drain might be placed for 1-2 days to allow continuous drainage.
- For a periapical abscess, the dentist might drill into the tooth's crown to allow pus to drain through the tooth's pulp chamber.
- Antibiotics may be prescribed.
2. Definitive Treatment (e.g., Root Canal):
- Numbing: The area around the tooth is thoroughly numbed.
- Isolation: A dental dam (a thin sheet of rubber) is placed around the tooth to keep it dry and free from saliva.
- Access Hole: A small opening is made in the crown of the tooth to access the pulp chamber and root canals.
- Cleaning & Shaping: Tiny instruments are used to remove the infected pulp and nerve tissue, and the root canals are cleaned, disinfected, and shaped.
- Filling: The cleaned canals are filled with a biocompatible material, usually gutta-percha, and sealed.
- Temporary Filling: A temporary filling is placed in the crown opening.
- Crown Placement (subsequent visit): After the root canal is complete and the tooth has healed, a permanent crown is usually placed to protect the tooth from fracture and restore its full function and appearance.
3. Definitive Treatment (e.g., Extraction):
- Numbing: The tooth and surrounding tissues are numbed with local anesthetic.
- Loosening the Tooth: The dentist uses specialized instruments to gently loosen the tooth from its socket.
- Removal: The tooth is carefully extracted.
- Socket Care: The empty socket is cleaned, and gauze is placed to control bleeding. Instructions for aftercare are provided to promote healing and prevent dry socket.
Recovery Timeline and Aftercare
Recovery varies based on the treatment received:
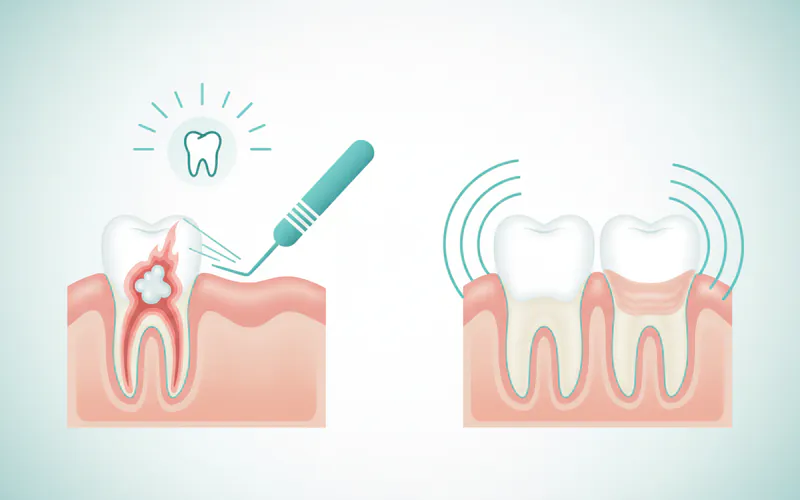
-
Drainage/Extraction:
- Immediate: Pain relief is usually noticeable within hours. Swelling may take a few days to subside.
- First 24-48 hours: Expect some discomfort, bleeding, and swelling. Manage pain with prescribed or over-the-counter pain relievers.
- Aftercare: Avoid spitting, rinsing vigorously, or using straws for the first 24 hours. Eat soft foods, avoid hard/chewy foods. Maintain good oral hygiene, but be gentle around the extraction site. Follow all post-operative instructions carefully to prevent complications like dry socket. Complete any prescribed antibiotics.
- Full recovery: Typically within 1-2 weeks for the extraction site to heal significantly.
-
Root Canal Treatment:
- Immediate: You may experience some mild soreness or sensitivity for a few days as the inflammation subsides. Pain medications can help manage this.
- First Few Days: Avoid chewing on the treated tooth until the permanent crown is placed.
- Aftercare: Continue regular brushing and flossing. Attend the follow-up appointment for the permanent crown.
- Full recovery: The infection is typically resolved immediately, but the tooth needs permanent restoration. The tooth itself integrates back into its socket over several weeks to months.
Prevention Strategies
Preventing dental abscesses largely comes down to excellent oral hygiene and regular dental care:
- Practice Excellent Oral Hygiene: Brush your teeth at least twice a day with fluoride toothpaste for two minutes each time. Floss daily to remove food particles and plaque from between teeth and under the gum line.
- Regular Dental Check-ups and Cleanings: Visit your dentist at least every six months for professional cleanings and examinations. Early detection of cavities or gum disease can prevent them from progressing to an abscess.
- Limit Sugary Foods and Drinks: Reduce your intake of items that contribute to tooth decay.
- Use Fluoride: Fluoridated water, toothpaste, and mouth rinses strengthen tooth enamel, making it more resistant to decay.
- Protect Your Teeth: Wear a mouthguard during contact sports to prevent dental trauma that could expose the pulp. If you grind or clench your teeth (bruxism), a nightguard can protect them from cracks.
- Address Periodontal Disease Early: If you notice signs of gum disease (bleeding gums, redness, bad breath), seek treatment promptly to prevent the formation of periodontal pockets that can harbor bacteria.
- Don't Ignore Dental Pain: Any persistent toothache or sensitivity is a sign that something is wrong. Seek dental attention immediately.
Cost Ranges in the US (with/without insurance)
The cost of treating an abscess can vary significantly based on the type of abscess, the chosen treatment, the complexity of the case, geographic location, and the dentist's fees.
-
Initial Exam & X-rays: $50 - $250
-
Abscess Drainage (I&D): $100 - $300 (often part of a larger treatment)
-
Antibiotics: $10 - $60 (prescription cost)
-
Root Canal Treatment (Periapical Abscess):
- Without Insurance: $700 - $2,200 (depending on tooth type)
- With Insurance: Many dental insurance plans cover a portion of root canals (e.g., 50-80%) after deductibles. Your out-of-pocket cost could range from $200 - $1,000+ for the procedure.
- Crown (needed post-root canal): $800 - $2,000 (without insurance); $300 - $1,000+ (with insurance).
-
Periodontal Treatment (Periodontal Abscess):
- Scaling and Root Planing (per quadrant): $150 - $400 (without insurance); $50 - $200 (with insurance).
- Periodontal Surgery: $500 - $3,000+ (without insurance); $200 - $1,500+ (with insurance).
-
Tooth Extraction:
- Simple Extraction: $75 - $300 (without insurance); $0 - $150 (with insurance, often fully covered).
- Surgical Extraction: $150 - $650 (without insurance); $50 - $350 (with insurance).
- Cost of Tooth Replacement (if extracted):
- Dental Implant: $2,000 - $6,000+ (without insurance)
- Dental Bridge: $2,000 - $5,000+ (without insurance)
- Partial Denture: $300 - $2,000+ (without insurance)
- Insurance coverage for tooth replacement varies widely.
It's always recommended to consult with your dental office and insurance provider to get an accurate estimate of costs based on your specific plan and treatment needs.
For Parents / Pediatric Considerations
Children are also susceptible to dental abscesses, primarily due to untreated cavities in their primary (baby) teeth. While baby teeth are temporary, an abscess in a primary tooth is just as serious as one in an adult tooth and requires immediate attention.
- Causes in Children: Deep cavities are the most common cause. Dental trauma (e.g., falls, sports injuries) can also lead to pulp exposure and infection.
- Symptoms in Children: May be similar to adults but can sometimes be harder to identify. Look for:
- Persistent fussiness or crying (especially when eating).
- Refusal to eat or drink.
- Sensitivity to hot/cold or chewing.
- Facial swelling (often more noticeable than in adults).
- Fever.
- A "pimple" on the gums near a tooth.
- Darkened or discolored tooth.
- Importance of Treatment: An untreated abscess in a baby tooth can have serious consequences:
- Spread of Infection: The infection can spread to other parts of the face and neck, potentially leading to serious conditions like cellulitis or even affecting the airway.
- Damage to Permanent Tooth: The infection can damage the developing permanent tooth underneath, leading to enamel defects or eruption problems.
- Premature Tooth Loss: An abscess often necessitates the extraction of the baby tooth, which can lead to space loss and crowding issues for the permanent teeth later on.
- Treatment Options: Similar to adults, but often focused on maintaining space for permanent teeth. This may include:
- Pulp Therapy (Pulpotomy or Pulpectomy): "Baby root canal" procedures to save the tooth.
- Extraction: If the tooth is severely infected or unrestorable. A space maintainer may be recommended after extraction to prevent other teeth from shifting.
- Prevention: Excellent oral hygiene from infancy, regular pediatric dental visits, and limiting sugary snacks are paramount for preventing cavities and abscesses in children.
Frequently Asked Questions
How much does it cost to treat a dental abscess in the US?
The cost varies widely based on the specific treatment needed. An initial drainage might be $100-$300. A root canal can range from $700-$2,200 (plus $800-$2,000 for a crown), while an extraction typically costs $75-$650. These are without insurance; coverage can significantly reduce your out-of-pocket expenses.
How painful is an abscess, and will treatment hurt?
An abscess itself can cause severe, throbbing pain due to pressure from the pus. During treatment, your dentist will use local anesthetics to thoroughly numb the area, making the procedure as comfortable as possible. You might feel some pressure or vibration, but typically no sharp pain. Afterward, some soreness is common as the area heals, which can be managed with pain relievers.
How long does it take for an abscess to heal after treatment?
The infection typically begins to resolve immediately after drainage and definitive treatment. Pain relief is often felt within hours. Swelling usually subsides within a few days. The tooth or gum tissue will continue to heal over 1-2 weeks, and bone healing around a root canal-treated tooth can take several months. It's crucial to complete any prescribed antibiotics and follow all aftercare instructions.
Can a dental abscess go away on its own?
No, a dental abscess will not go away on its own. While the pain might temporarily subside if the abscess drains on its own, the underlying bacterial infection remains and will continue to cause damage and can flare up again. Leaving an abscess untreated is dangerous and can lead to severe health complications.
Are there any home remedies for a dental abscess?
Home remedies can provide temporary pain relief but will not cure an abscess. Rinsing with warm salt water can help soothe the area and draw some pus out, but it is not a substitute for professional dental treatment. Over-the-counter pain relievers can help manage discomfort. Do not apply aspirin directly to the gum tissue, as it can cause a chemical burn. Always seek dental care for an abscess.
Will my dental insurance cover the cost of abscess treatment?
Most dental insurance plans provide some coverage for abscess treatment, especially for procedures considered medically necessary. Diagnostic procedures (X-rays, exams) are often covered at a high percentage (e.g., 80-100%). Restorative treatments like root canals, extractions, or periodontal treatments are usually covered at a lower percentage (e.g., 50-80%) after your deductible. It's essential to contact your insurance provider directly to understand your specific benefits and estimated out-of-pocket costs.
Can an abscess spread to other parts of my body?
Yes, an untreated dental abscess can spread. The bacteria can enter the bloodstream and cause systemic infections. It can spread to the jaw, neck, face (leading to cellulitis), or even more distant organs. In rare but serious cases, it can lead to life-threatening conditions like Ludwig's angina (a severe infection of the floor of the mouth that can block the airway) or sepsis (a full-body inflammatory response to infection).
When to See a Dentist
Any suspected dental abscess is a dental emergency and warrants immediate attention. Do not wait for symptoms to worsen.
See a dentist IMMEDIATELY if you experience:
- Severe, throbbing toothache that interferes with daily activities.
- Visible swelling in your face, jaw, or neck.
- Fever or chills.
- Difficulty breathing or swallowing. (These are signs of a rapidly spreading, potentially life-threatening infection – go to an emergency room if your dentist is unavailable.)
- A persistent foul taste in your mouth accompanied by a draining pimple on your gums.
- Increased sensitivity to hot, cold, or pressure.
If you have any suspicion of an abscess, contact your dentist right away. Early diagnosis and treatment are critical to prevent complications and preserve your overall health.
dental abscesstooth abscess treatmentabscess symptomsperiapical abscesstooth infection
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.