Abscess Gum: Complete Guide
Key Takeaways
- An alarming statistic reveals that over 15% of adults in the United States have experienced a dental abscess at some point in their lives, often presenting as an abscess gum. This painful and potentially dangerous condition is more than just a minor inconvenience; it's a serious bacterial in
An alarming statistic reveals that over 15% of adults in the United States have experienced a dental abscess at some point in their lives, often presenting as an abscess gum. This painful and potentially dangerous condition is more than just a minor inconvenience; it's a serious bacterial infection that can rapidly spread, leading to significant health complications if left untreated. Imagine a throbbing pain in your mouth, swelling that distorts your face, and a foul taste that won't go away – these are often the tell-tale signs of a developing gum abscess. Ignoring these signals isn't just uncomfortable; it can compromise your overall health, affecting everything from your ability to eat and speak to the health of your heart and other vital organs.
Understanding an abscess gum is crucial for every individual aiming to maintain optimal oral and systemic health. This comprehensive guide from SmilePedia.net will equip you with vital knowledge, from identifying the early warning signs and understanding the different types of abscesses, including the common periapical abscess, to exploring all available treatment options, recovery protocols, and crucial prevention strategies. We'll delve into the causes, typical costs in the US, what to expect during treatment, and when to seek immediate dental care, ensuring you have all the information you need to protect your smile and well-being.
Key Takeaways:
- An abscess gum is a localized bacterial infection forming a pocket of pus in the gum tissue or bone.
- There are several types, including periodontal (gum tissue), periapical (tooth root tip), and gingival (surface gum).
- Symptoms include severe, throbbing pain, swelling, sensitivity, fever, and a foul taste.
- Treatment involves drainage of pus, antibiotics, and addressing the root cause (e.g., root canal, deep cleaning, or extraction).
- Average treatment costs in the US range from $75 for emergency drainage to $1,500-$3,000+ for a root canal with crown or $150-$600 for an extraction, often covered partially by dental insurance.
- Untreated abscesses can lead to serious complications like cellulitis, sepsis, or tooth loss, requiring prompt medical attention.
- Prevention hinges on excellent oral hygiene, regular dental check-ups, and timely treatment of cavities or gum disease.
What It Is / Overview
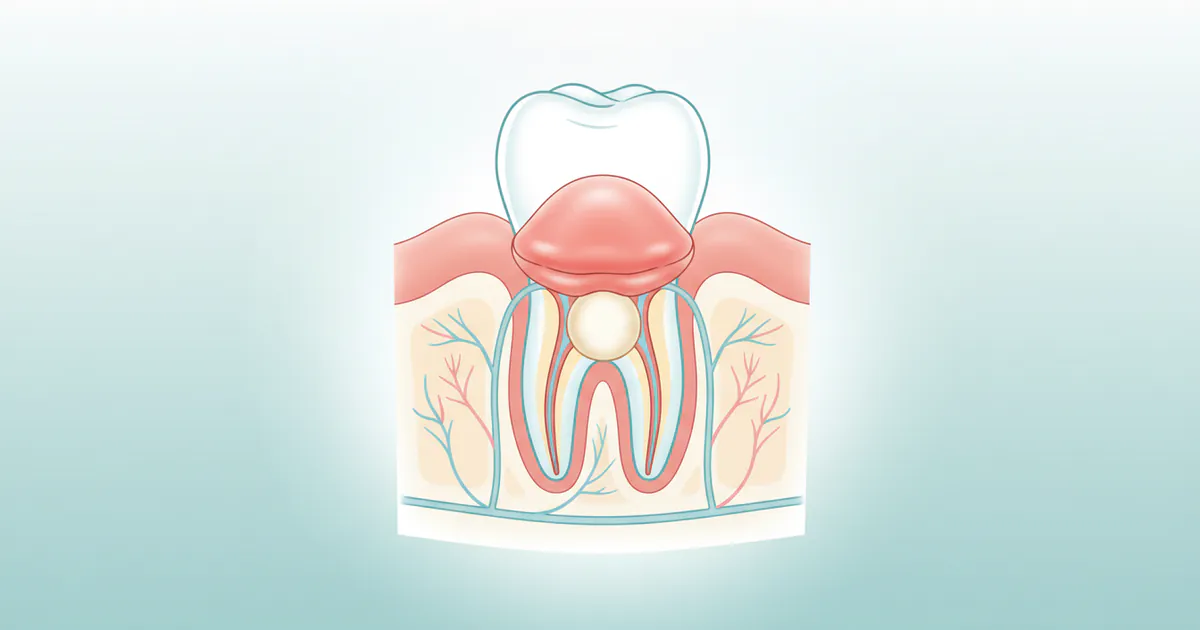
An abscess gum is a painful, localized collection of pus caused by a bacterial infection. This infection can originate in various parts of your oral cavity, but when we refer to an "abscess gum," it specifically points to an infection that manifests either within the gum tissue itself or at the apex (tip) of a tooth root, where it then affects the surrounding gum and bone. Essentially, your body's immune system sends white blood cells to fight the infection, and as these cells battle the bacteria, they form pus – a thick, yellowish fluid composed of dead cells, bacteria, and tissue debris. This pus then accumulates, creating a swollen, tender pocket.

The formation of an abscess gum signifies a significant breach in your oral defenses, often due to untreated dental issues. It's not merely a cosmetic concern but a medical emergency that requires prompt professional intervention. If left unaddressed, the infection can spread beyond the confines of your mouth, potentially leading to widespread systemic issues that can be life-threatening. The pain associated with an abscess is often described as severe, throbbing, and persistent, often radiating to the ear, jaw, or neck. Understanding the nature of this infection is the first step toward effective treatment and prevention.
``
Types / Variations of Abscess Gum
While often grouped under the general term "abscess gum," there are distinct types of dental abscesses, each with its own origin and characteristics. Understanding these differences is crucial for accurate diagnosis and effective treatment.
Periapical Abscess
The periapical abscess is perhaps the most common type of dental abscess and is often what people mean when they refer to a "tooth abscess" or an "abscess gum" originating from a tooth. This infection starts inside the tooth itself, specifically in the dental pulp (the innermost part of the tooth containing nerves, blood vessels, and connective tissue). When deep decay, a cracked tooth, or trauma allows bacteria to penetrate the enamel and dentin, they reach and infect the pulp. The infection then spreads down through the root canal to the apex (tip) of the tooth root, forming a pocket of pus in the surrounding bone. This pus creates pressure, causing intense pain, and can eventually break through the bone to form a visible swelling on the gum.
Key characteristics of a periapical abscess:
- Origin: Infected tooth pulp.
- Location: At the tip of the tooth root, inside the jawbone.
- Symptoms: Severe, throbbing pain, sensitivity to hot/cold, pain when biting, facial swelling, possible fever, and a "pimple" (fistula) on the gum where pus drains.
- Treatment Focus: Root canal therapy or tooth extraction.
Periodontal Abscess
A periodontal abscess, also frequently referred to as an abscess gum, is a localized collection of pus within the gum tissue itself, specifically in the periodontal pockets that form alongside the tooth root. Unlike a periapical abscess, this type typically does not originate from infection inside the tooth's pulp. Instead, it occurs in patients with pre-existing periodontal (gum) disease. When plaque and tartar accumulate, they lead to inflammation and the formation of deep pockets between the teeth and gums. If these pockets become blocked – for example, by trapped food debris or calculus – bacteria multiply rapidly within the enclosed space, leading to a quick-onset infection and pus formation.
Key characteristics of a periodontal abscess:
- Origin: Bacterial infection in deep periodontal pockets.
- Location: Alongside the tooth root, within the gum tissue and supporting bone.
- Symptoms: Localized, throbbing pain, shiny red or swollen gum, sensitivity to touch, pus discharge, bad taste, sometimes a mobile tooth. Pain often increases with pressure but may lessen after drainage.
- Treatment Focus: Drainage, deep cleaning (scaling and root planing), and potentially periodontal surgery.
Gingival Abscess
A gingival abscess is a less common and generally less severe form of abscess gum. It is an infection that affects only the gum tissue (gingiva) and does not involve the tooth's pulp or the deeper periodontal structures (like bone or periodontal ligament). This type of abscess often results from trauma or irritation, such as when a foreign object (like a popcorn kernel hull, toothbrush bristle, or a piece of food) becomes embedded in the gum tissue. It can also occur if bacteria enter a superficial cut or abrasion on the gums.
Key characteristics of a gingival abscess:
- Origin: Trauma or irritation, superficial bacterial infection.
- Location: Confined to the surface gum tissue, not involving the tooth or underlying bone.
- Symptoms: Localized swelling, redness, pain, tenderness, and possibly a visible pus-filled bump on the gum.
- Treatment Focus: Drainage and removal of any foreign object.
Pericoronal Abscess (Pericoronitis)
A pericoronal abscess is a specific type of periodontal abscess that develops around the crown of a partially erupted tooth, most commonly wisdom teeth (third molars). When a wisdom tooth is erupting but only partially breaks through the gum, a flap of gum tissue (operculum) can cover part of its chewing surface. This flap creates a perfect haven for food particles and bacteria to get trapped, making it difficult to clean effectively. This leads to inflammation of the gum tissue surrounding the crown, a condition known as pericoronitis, which can quickly progress to a full-blown infection and pus formation.
Key characteristics of a pericoronal abscess:
- Origin: Trapped food and bacteria under a gum flap around a partially erupted tooth.
- Location: Around the crown of a partially erupted tooth, usually wisdom teeth.
- Symptoms: Severe pain, swelling of the gum and cheek, difficulty opening the mouth (trismus), bad taste, pus discharge, swollen lymph nodes, and sometimes fever.
- Treatment Focus: Irrigation, drainage, antibiotics, and potentially extraction of the wisdom tooth or removal of the gum flap.
Causes / Why It Happens
An abscess gum is fundamentally caused by a bacterial infection. However, several underlying conditions and factors can create an environment ripe for these infections to take hold. Understanding these causes is critical for both prevention and targeted treatment.
1. Severe Tooth Decay (Cavities)
This is the primary cause of a periapical abscess. When a cavity is left untreated, bacteria can erode through the tooth's enamel and dentin layers, eventually reaching the pulp chamber. Once bacteria infect the pulp, the infection spreads down the root canal to the tip of the tooth root (apex), causing inflammation and pus accumulation in the surrounding bone.
2. Deep Cracks or Chips in Teeth
Any significant crack, chip, or fracture in a tooth, especially one that extends below the gum line or into the pulp, can create a pathway for bacteria to enter the tooth's sensitive inner structures. Even hairline fractures that are not visibly obvious can permit bacterial ingress, leading to pulp infection and a subsequent periapical abscess.
3. Gum Disease (Periodontitis)
Advanced gum disease, or periodontitis, is the leading cause of periodontal abscesses. Periodontitis is characterized by chronic inflammation and infection of the gums and the supporting bone around the teeth. As the disease progresses, deep pockets form between the teeth and gums. These pockets collect plaque, tartar, and bacteria. If these pockets become blocked or if the immune system is compromised, bacteria proliferate rapidly, leading to a localized infection and pus formation within the gum tissue.
4. Poor Oral Hygiene
Insufficient brushing and flossing allow plaque and tartar to accumulate on tooth surfaces and along the gum line. This buildup harbors billions of bacteria, which constantly produce acids that cause tooth decay and toxins that irritate and infect gum tissue. Over time, poor hygiene significantly increases the risk of both periapical (from cavities) and periodontal (from gum disease) abscesses. The American Dental Association (ADA) consistently stresses the importance of daily oral hygiene for preventing such conditions.
5. Failed Root Canal Treatment
While root canal therapy is highly effective, in rare cases, a previously treated tooth can become re-infected. This might happen if all infected tissue was not removed during the initial procedure, if there was contamination, if the filling material failed, or if a new cavity develops on the treated tooth. This re-infection can lead to the formation of another periapical abscess.
6. Trauma to the Tooth
An injury to a tooth, such as a severe blow or impact, can damage the blood vessels and nerves within the pulp, leading to its death (necrosis). A necrotic pulp is highly susceptible to bacterial infection, even without a visible crack or cavity, eventually resulting in a periapical abscess.
7. Compromised Immune System
Individuals with weakened immune systems are more vulnerable to infections, including dental abscesses. Conditions like diabetes, autoimmune diseases, cancer treatment (chemotherapy or radiation), HIV/AIDS, or prolonged steroid use can impair the body's ability to fight off bacterial invasions, making them more prone to developing an abscess gum and experiencing more severe complications.

8. Impacted Wisdom Teeth
As mentioned under pericoronal abscesses, a partially erupted wisdom tooth creates a vulnerable area where food and bacteria can get trapped under a gum flap. This environment is ideal for bacterial growth and infection, leading to a painful pericoronal abscess.
Signs and Symptoms
Recognizing the signs and symptoms of an abscess gum early is crucial for prompt treatment and preventing severe complications. While the specific presentation can vary slightly depending on the type of abscess, there are several common indicators to look out for.
Common Signs and Symptoms:
- Severe, Persistent, Throbbing Toothache: This is often the most prominent symptom. The pain can be sharp or dull, constant, and may radiate to your jawbone, neck, or ear. It often worsens when you lie down.
- Sensitivity to Hot and Cold Temperatures: Affected teeth or surrounding areas may react intensely to hot or cold foods and drinks.
- Pain When Chewing or Biting: Pressure on the affected tooth or gum can exacerbate the pain.
- Swelling in the Gum, Face, or Jaw: You may notice localized swelling around the affected tooth or a more generalized swelling of your cheek or jaw on the side of the abscess. The gum tissue itself might appear red, swollen, and tender to the touch.
- Pimple-Like Bump on the Gums (Fistula): As the infection progresses, pus may create a channel (called a fistula or sinus tract) through the bone and gum tissue, appearing as a small, pus-filled bump on your gum. If this ruptures, you might experience a sudden release of foul-tasting fluid.
- Foul Taste in Your Mouth / Bad Breath (Halitosis): The presence of pus and bacteria can lead to an unpleasant taste and persistent bad breath.
- Fever: A systemic sign that your body is fighting a significant infection.
- Swollen, Tender Lymph Nodes: Lymph nodes in your neck or under your jaw may become swollen and tender as they work to filter out the infection.
- Difficulty Opening Your Mouth (Trismus) or Swallowing: If the infection has spread to surrounding tissues, especially with a pericoronal abscess, it can cause muscle spasms that make it hard to open your jaw or swallow.
- Loose or Elevated Tooth: The pressure from the pus can sometimes cause the affected tooth to feel slightly loose or to sit higher than adjacent teeth.
Pro Tip: Do not ignore localized pain, even if it seems minor. Any persistent discomfort in your gums or teeth could be an early warning sign of an underlying issue that could develop into an abscess.
Treatment Options
Treating an abscess gum is critical to eliminate the infection, alleviate pain, and prevent its spread. The specific treatment approach depends on the type, location, and severity of the abscess. The primary goals are always to drain the pus, eliminate the source of infection, and save the tooth if possible.
1. Drainage of the Abscess (Incision and Drainage - I&D)
This is often the first and most immediate step to relieve pressure and pain. The dentist will make a small incision in the swollen gum tissue to allow the pus to drain. This procedure provides instant relief by reducing the pressure buildup.
- Pros: Immediate pain relief, helps contain infection, relatively quick procedure.
- Cons: Does not address the root cause of the infection; further treatment is always necessary.
- Timeline: 15-30 minutes for the procedure.
2. Antibiotics
Antibiotics are prescribed to help control the bacterial infection, especially if it has spread beyond the immediate abscess site, if you have a fever, or if your immune system is compromised. They are typically used in conjunction with drainage and other definitive treatments.
- Pros: Helps eliminate widespread bacteria, prevents further spread of infection.
- Cons: Not a standalone treatment for the abscess itself (won't remove pus or decayed tissue), can have side effects (nausea, diarrhea), potential for antibiotic resistance if overused.
- Timeline: 7-10 days course, takes 24-48 hours to start feeling effects.
3. Root Canal Therapy (Endodontic Treatment)
This is the preferred treatment for a periapical abscess when the tooth can be saved. The dentist or endodontist will drill a small hole into the crown of the infected tooth, remove the infected pulp and nerve tissue, clean and disinfect the internal root canals, and then fill and seal them. Finally, the tooth is usually restored with a dental crown to protect it from fracture.
- Pros: Saves the natural tooth, preserves chewing function and aesthetics.
- Cons: Multi-step procedure, can be costly, possibility of re-infection in rare cases.
- Timeline: 1-2 appointments, each 60-90 minutes. Crown placement adds another 1-2 appointments over several weeks.
4. Tooth Extraction
If a tooth is severely damaged, cannot be saved with a root canal (e.g., extensive decay below the gum line, severe fracture), or if the patient prefers it, extraction is an option. After the tooth is removed, the socket is thoroughly cleaned to ensure all infected tissue is gone.
- Pros: Eliminates the source of infection completely, often less expensive than a root canal with a crown.
- Cons: Loss of natural tooth, requires consideration of tooth replacement options (implant, bridge, partial denture) to prevent shifting of adjacent teeth and bone loss, which adds further cost and time.
- Timeline: 30-60 minutes for extraction. Healing takes several weeks.
5. Scaling and Root Planing (Deep Cleaning)
For a periodontal abscess, after initial drainage, deep cleaning of the periodontal pockets is crucial. This involves scaling (removing plaque and tartar from tooth surfaces above and below the gum line) and root planing (smoothing the root surfaces to remove bacterial toxins and prevent future buildup).
- Pros: Addresses the underlying gum disease, can resolve the infection and reduce pocket depth.
- Cons: Can be uncomfortable, multiple appointments may be needed, does not address periapical issues.
- Timeline: 1-4 appointments, each 45-90 minutes.
6. Pericoronitis Treatment
For a pericoronal abscess, initial treatment involves flushing the area under the gum flap with an antiseptic solution, drainage, and possibly antibiotics. If the condition recurs or is severe, the overlying gum flap (operculum) may be surgically removed (operculumectomy), or the tooth (often a wisdom tooth) may be extracted.
- Pros: Resolves the acute infection.
- Cons: If the tooth remains, recurrence is possible; extraction carries risks.
- Timeline: Initial cleaning 15-30 minutes. Extraction 30-60 minutes.
``
Step-by-Step Process: What to Expect During Treatment
Understanding the typical steps involved in treating an abscess gum can help alleviate anxiety and prepare you for your dental visit. While the exact process may vary slightly based on the type of abscess and the chosen treatment, here's a general overview.
Initial Consultation and Diagnosis:
- Patient History: Your dentist will start by asking about your symptoms, when they began, their severity, and any relevant medical history.
- Clinical Examination: The dentist will visually inspect your mouth, check for swelling, redness, and tenderness, and gently probe the affected area.
- X-rays: Dental X-rays (periapical and/or panoramic) are essential to determine the type and extent of the abscess, identify the source of the infection (e.g., deep cavity, bone loss, impacted tooth), and assess the surrounding structures.
- Vitality Testing: For suspected periapical abscesses, the dentist may perform pulp vitality tests (e.g., cold test, electric pulp test) to assess the health of the tooth's nerve.
Treatment Steps (Example: Periapical Abscess Treated with Root Canal):
- Anesthesia: Local anesthetic will be administered to thoroughly numb the affected tooth and surrounding gum tissue, ensuring you are comfortable throughout the procedure.
- Access Opening: For a periapical abscess, a small opening will be drilled through the crown of the tooth to access the pulp chamber and root canals.
- Pus Drainage: If there's significant pressure and pus accumulation, the dentist may facilitate drainage through the access opening or, if necessary, make a small incision in the gum (I&D) to release the pus directly. This immediately reduces pain.
- Cleaning and Shaping: Tiny instruments (files) are used to meticulously remove infected pulp tissue, bacteria, and debris from inside the root canals. The canals are then shaped to prepare them for filling.
- Disinfection: The canals are thoroughly irrigated with antiseptic solutions (e.g., sodium hypochlorite) to kill remaining bacteria and flush out debris.
- Filling and Sealing: Once the canals are clean and dry, they are filled with a biocompatible rubber-like material called gutta-percha and sealed with adhesive cement to prevent re-infection.
- Temporary Filling: A temporary filling is placed in the access opening until the tooth can be restored with a permanent crown or filling.
- Antibiotics (if prescribed): You may be given a prescription for antibiotics to take for 7-10 days, especially if the infection was widespread or if you have systemic symptoms like fever.
- Restoration (Crown/Filling): After the root canal, the treated tooth typically requires a permanent filling or, more commonly, a dental crown. This protects the now-brittle tooth from fracture and restores its function and appearance. This usually occurs in a separate appointment a few weeks later.

Treatment Steps (Example: Periodontal Abscess Treated with Drainage and Deep Cleaning):
- Anesthesia: Local anesthetic is applied to numb the gum area.
- Drainage: The dentist will make a small incision in the swollen gum to drain the pus. They might also gently probe the periodontal pocket to facilitate drainage.
- Irrigation: The pocket is irrigated with an antiseptic solution to flush out bacteria and debris.
- Scaling and Root Planing: Using specialized instruments, the dentist or hygienist will meticulously remove plaque and tartar from the tooth surfaces within the newly drained pocket and smooth the root surfaces to prevent future bacterial attachment.
- Antibiotics (if prescribed): Oral antibiotics may be prescribed to control the infection.
- Follow-up: You'll likely have a follow-up appointment to monitor healing and assess the overall periodontal health.
Cost and Insurance
The cost of treating an abscess gum in the United States can vary significantly based on the type of abscess, the complexity of the case, the chosen treatment, the region, and whether the procedure is performed by a general dentist or a specialist (e.g., endodontist, periodontist).
Typical US Cost Ranges (Without Insurance):
- Emergency Drainage (Incision & Drainage):
- $75 - $300 (Often billed as an emergency exam + minor procedure)
- Antibiotics:
- $10 - $60 (for a typical 7-10 day course, generic)
- Tooth Extraction:
- Simple Extraction: $150 - $450
- Surgical Extraction (e.g., impacted wisdom tooth): $300 - $800 per tooth
- Root Canal Therapy (Periapical Abscess):
- Front Tooth (Incisor/Canine): $700 - $1,200
- Premolar: $800 - $1,500
- Molar: $1,000 - $2,000+ (Molars have more roots and canals, increasing complexity and cost)
- Dental Crown (After Root Canal):
- $800 - $2,500+ (depending on material: porcelain-fused-to-metal, all-ceramic, zirconia, gold)
- Scaling and Root Planing (Periodontal Abscess):
- $200 - $500 per quadrant (usually 2-4 quadrants needed)
- Periodontal Surgery (if deep pockets persist):
- $500 - $3,000+ per quadrant, depending on type of surgery.
Total Cost Scenarios (without insurance):
- Mild Gingival Abscess: Drainage + antibiotics = $85 - $360
- Periodontal Abscess: Drainage + antibiotics + 4 quadrants scaling/root planing = $885 - $2,360
- Periapical Abscess (Root Canal + Crown on Molar): Root canal + crown + initial drainage/antibiotics = $1,985 - $4,860+
- Periapical Abscess (Extraction + Implant): Extraction + dental implant (post, abutment, crown) = $3,000 - $6,000+
Insurance Coverage:
Most dental insurance plans in the US offer some level of coverage for abscess gum treatments, but the extent of coverage varies widely:
- Preventive Care (e.g., exams, X-rays): Typically covered at 80-100%.
- Basic Restorative Care (e.g., fillings, simple extractions, emergency drainage): Often covered at 70-80%.
- Major Restorative Care (e.g., root canals, crowns, surgical extractions, periodontal surgery): Usually covered at 50-70%.
- Orthodontics and Cosmetic Procedures: Typically not covered or have separate, limited coverage.
Important Considerations:
- Deductibles: You will likely need to pay an annual deductible (e.g., $50-$100) before your insurance starts paying.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit (e.g., $1,000-$2,500). Once you reach this limit, you pay 100% out-of-pocket for any further treatments that year.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) before they cover major procedures like root canals or crowns.
- In-network vs. Out-of-network: Costs may be lower if you see an in-network dentist.
Pro Tip: Always contact your dental insurance provider directly or ask your dental office to perform a benefits check before beginning treatment to understand your specific coverage, deductibles, and annual maximums.
Recovery and Aftercare
Proper recovery and aftercare are crucial for successful healing after treatment for an abscess gum. Following your dentist's instructions diligently will minimize complications, manage discomfort, and promote a speedy recovery.
Immediately After Treatment:
- Pain Management: You will likely experience some soreness or discomfort once the local anesthetic wears off. Your dentist will recommend over-the-counter pain relievers like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol). For more severe pain, a prescription pain medication may be given. Take as directed.
- Swelling: Some residual swelling is normal. Applying a cold compress to the outside of your cheek for 15-20 minutes at a time, with 20-minute breaks, can help reduce swelling and discomfort for the first 24-48 hours.
- Bleeding (for extractions): Minor bleeding is normal after an extraction. Bite gently on a gauze pad for 30-45 minutes. Change the gauze if it becomes soaked. Avoid rinsing vigorously for the first 24 hours.
- Food and Drink: Stick to soft foods for the first few days (e.g., yogurt, mashed potatoes, soup, scrambled eggs). Avoid hot, spicy, acidic, crunchy, or sticky foods that could irritate the treated area or dislodge a clot (after extraction). Drink plenty of fluids, but avoid using a straw after an extraction, as the suction can dislodge the blood clot and lead to a painful dry socket.
- Activity: Avoid strenuous activity for at least 24-48 hours, as this can increase bleeding and swelling. Rest is important for healing.
Ongoing Aftercare:
- Oral Hygiene: Maintain good oral hygiene, but be gentle around the treated area.
- For Root Canal/Filling: Brush and floss normally, but avoid aggressive brushing on the treated tooth until your permanent crown is placed.
- For Extraction: Avoid brushing directly on the extraction site for the first 24 hours. After that, you can gently brush other areas and very carefully around the site. Your dentist may recommend a warm salt water rinse (1/2 teaspoon salt in 8 ounces warm water) 2-3 times a day starting 24 hours after extraction to keep the area clean and promote healing.
- For Deep Cleaning: Continue regular brushing and flossing. Your dentist might recommend an antiseptic mouthwash.
- Antibiotics: If antibiotics were prescribed, take the entire course as directed, even if you feel better. Stopping early can lead to a recurrence of the infection or antibiotic resistance.
- Avoid Irritants: Refrain from smoking or using tobacco products, as they significantly delay healing and increase the risk of complications. Avoid alcohol.
- Follow-Up Appointments: Attend all scheduled follow-up appointments with your dentist. These are crucial to ensure proper healing, check for any complications, and place permanent restorations (like crowns) if needed.
Pro Tip: If you experience severe pain that doesn't subside with medication, excessive bleeding, persistent fever, increasing swelling, or difficulty breathing/swallowing, contact your dentist immediately or seek emergency medical care. These could be signs of a spreading infection.
Prevention
Preventing an abscess gum is largely about maintaining excellent oral hygiene and addressing dental issues promptly. Consistent preventive care is your best defense against these painful infections.
1. Maintain Excellent Oral Hygiene
- Brush Twice Daily: Brush your teeth thoroughly for at least two minutes, twice a day, using a fluoride toothpaste. Ensure you reach all surfaces of your teeth and gently brush your gum line.
- Floss Daily: Flapse daily to remove food particles and plaque from between your teeth and under the gum line, areas your toothbrush can't reach. This is crucial for preventing gum disease and cavities.
- Use Mouthwash: An antiseptic or fluoride mouthwash can complement brushing and flossing by reducing bacteria and strengthening enamel. Discuss options with your dentist.
2. Regular Dental Check-ups and Cleanings
- Visit Your Dentist Regularly: Schedule professional dental check-ups and cleanings every six months, or as recommended by your dentist. These visits allow your dentist to:
- Identify and treat cavities early, before they become deep enough to cause an abscess.
- Detect and manage gum disease (gingivitis or periodontitis) before it progresses to a periodontal abscess.
- Remove plaque and tartar buildup that at-home brushing can't tackle.
- Monitor existing restorations (fillings, crowns) for potential issues.
3. Prompt Treatment of Dental Problems
- Don't Delay Cavity Treatment: If your dentist identifies a cavity, get it filled as soon as possible. Small cavities are easier and less expensive to treat and prevent the infection from reaching the tooth's pulp.
- Address Gum Disease: If you notice signs of gum disease (bleeding gums, redness, swelling), seek treatment promptly. Early intervention can prevent the formation of deep pockets and periodontal abscesses.
- Repair Chipped or Cracked Teeth: Any tooth with a significant chip or crack should be evaluated by a dentist. These can be entry points for bacteria.
4. Healthy Diet and Lifestyle
- Limit Sugary and Acidic Foods/Drinks: Reduce your intake of sugary snacks, sodas, and acidic foods, which contribute to tooth decay.
- Stay Hydrated: Drink plenty of water throughout the day. Water helps wash away food particles and bacteria.
- Avoid Tobacco Products: Smoking and chewing tobacco severely compromise oral health, increase the risk of gum disease, and impair healing.
- Manage Underlying Health Conditions: If you have conditions like diabetes, ensure they are well-controlled, as they can impact your oral health and immune response.
5. Protect Your Teeth
- Wear a Mouthguard: If you play contact sports, wear a custom-fitted mouthguard to protect your teeth from trauma and fractures.
- Address Bruxism (Teeth Grinding): If you grind or clench your teeth, especially at night, talk to your dentist about a nightguard, as excessive force can lead to cracks and damage.

By diligently following these preventive measures, you can significantly reduce your risk of developing an abscess gum and maintain a healthy, pain-free smile.
Risks and Complications
While an abscess gum initially presents as a localized infection, ignoring it or delaying treatment carries significant risks and can lead to severe, potentially life-threatening complications.
1. Spread of Infection
This is the most serious risk. The bacteria from an abscess can spread rapidly to other parts of the body:
- Osteomyelitis: The infection can spread to the jawbone itself, causing inflammation and destruction of the bone tissue.
- Cellulitis: This is a serious bacterial skin infection that can develop if the abscess spreads to the surrounding soft tissues of the face, neck, or even under the tongue (Ludwig's angina). Cellulitis causes widespread redness, swelling, warmth, and tenderness and can lead to airway obstruction if it affects the neck.
- Sepsis: If bacteria from the abscess enter the bloodstream, it can lead to sepsis, a life-threatening systemic response to infection. Sepsis can cause organ damage, septic shock, and can be fatal.
- Cavernous Sinus Thrombosis: Although rare, an infection in the upper jaw can spread to the cavernous sinus (a large vein behind the eyes), leading to a blood clot, which can cause vision problems, headaches, facial paralysis, and can be life-threatening.
- Brain Abscess: In extremely rare and severe cases, the infection can travel to the brain, forming a brain abscess, which is a medical emergency requiring immediate neurosurgical intervention.
2. Tooth Loss
If the infection is severe and extensive, or if the tooth is too damaged by decay or fracture, it may not be savable, even with a root canal. In such cases, the tooth will need to be extracted, leading to tooth loss.
3. Damage to Adjacent Teeth and Bone
The pus and inflammation from a prolonged abscess can erode the surrounding jawbone and damage the roots of adjacent healthy teeth.
4. Facial Deformity
Severe swelling of the face and jaw due to the abscess or spreading cellulitis can cause significant facial disfigurement.
5. Chronic Pain
Even if the acute infection subsides temporarily (e.g., if the pus drains spontaneously), the underlying cause remains. This can lead to chronic, low-grade pain and recurring abscesses.
Pro Tip: Do not attempt to pop or drain an abscess yourself. This can push the infection deeper into the tissues, introduce new bacteria, and significantly worsen the condition. Always seek professional dental care.
Comparison Table: Abscess Types, Causes, and Primary Treatments
| Abscess Type | Primary Cause | Location of Infection | Key Symptoms | Primary Treatment Approaches |
|---|---|---|---|---|
| Periapical | Deep tooth decay, trauma, cracked tooth | At the tooth's root tip, in the jawbone | Severe, throbbing toothache, sensitivity to hot/cold, facial swelling, "pimple" on gum | Root canal therapy or tooth extraction, drainage, antibiotics |
| Periodontal | Advanced gum disease (periodontitis), blocked gum pocket | Alongside tooth root, in gum tissue and supporting bone | Localized gum swelling, throbbing pain, pus, loose tooth, bad taste | Drainage, deep cleaning (scaling & root planing), antibiotics, periodontal surgery |
| Gingival | Trauma, foreign object embedded in gum | Confined to superficial gum tissue (gingiva) | Localized swelling, redness, pain on gum, visible pus bump | Drainage, foreign object removal, good oral hygiene |
| Pericoronal | Trapped food/bacteria under gum flap of partially erupted tooth (wisdom tooth) | Around crown of partially erupted tooth, in gum tissue | Severe pain, gum/cheek swelling, difficulty opening mouth, bad taste, fever | Irrigation, drainage, antibiotics, operculumectomy or tooth extraction |
Comparison Table: Common Treatment Costs and Recovery Timelines (US Average, without complications)
| Treatment Option | Average Cost Range (USD) | Typical Recovery Time | Key Pros | Key Cons |
|---|---|---|---|---|
| Emergency Drainage | $75 - $300 | Immediate relief, 1-2 days discomfort | Immediate pain relief, quick | Doesn't resolve underlying cause, temporary |
| Antibiotics (7-10 days) | $10 - $60 | 24-48 hours for effect, 7-10 days course | Fights widespread infection | Not a standalone treatment, side effects, resistance risk |
| Simple Tooth Extraction | $150 - $450 | 3-7 days for initial healing | Quick resolution of infection source | Tooth loss, potential need for replacement |
| Surgical Tooth Extraction | $300 - $800 | 7-14 days for initial healing | Necessary for impacted/complex teeth | More invasive, longer recovery, potential for dry socket |
| Root Canal Therapy (Molar) | $1,000 - $2,000+ | 2-7 days discomfort after procedure | Saves natural tooth, preserves function | High cost, multiple visits, requires a crown |
| Dental Crown (after RCT) | $800 - $2,500+ | 1-2 weeks for cement to set, long-term | Protects treated tooth, restores aesthetics | Additional significant cost, multiple visits |
| Scaling & Root Planing (4 Qds) | $800 - $2,000 | 1-3 weeks for gum healing | Addresses gum disease, prevents recurrence | Can be uncomfortable, multiple visits, not for periapical abscess |
Children / Pediatric Considerations
Children are also susceptible to developing an abscess gum, and the condition can be particularly concerning due to the rapid progression of infection in developing oral structures and the potential impact on permanent teeth.
Why Children are at Risk:
- High Incidence of Cavities: Children, especially those with diets high in sugar, are prone to tooth decay. Untreated cavities in baby teeth (primary teeth) can quickly lead to a periapical abscess.
- Trauma: Children are more active and prone to falls or injuries, which can lead to dental trauma and subsequent abscess formation.
- Developing Teeth: An infection in a primary tooth can potentially affect the developing permanent tooth underneath it, causing developmental defects or impacting eruption.
- Poor Oral Hygiene: Some children may not have fully developed brushing and flossing habits, increasing their risk.
Signs and Symptoms in Children:
The signs of an abscess gum in children are similar to adults but might be harder to pinpoint:
- Irritability or Fussiness: Children may not be able to articulate pain clearly.
- Difficulty Eating: Refusal to eat, especially hard or chewy foods.
- Swelling: Noticeable facial swelling, particularly around the jaw or cheek.
- Fever: Often present with a spreading infection.
- Persistent Bad Breath: A sign of underlying infection.
- Visible Pus or "Pimple" on Gums: Parents may notice a small bump.
- Tenderness to Touch: The child may resist touch on the affected area.
Treatment for Children:
- Drainage and Antibiotics: Similar to adults, immediate drainage and antibiotics are often the first steps to control the infection.
- Pulpectomy (Baby Root Canal): For primary teeth with a periapical abscess, a pulpectomy may be performed. This involves removing the infected pulp from the crown and root canals of the baby tooth, disinfecting them, and then filling them with a resorbable material. The tooth is then usually covered with a stainless steel crown. This treatment aims to save the baby tooth until the permanent tooth is ready to erupt, preserving space.
- Extraction: If the baby tooth is severely damaged, if the infection is too widespread, or if the permanent tooth is close to eruption, extraction may be the best option.
- Space Maintainer: If a primary tooth is extracted prematurely, a space maintainer may be placed to prevent adjacent teeth from drifting and ensure adequate space for the permanent tooth to erupt correctly.
Pediatric Prevention:
- Early Dental Visits: Schedule your child's first dental visit by their first birthday or when their first tooth erupts.
- Good Oral Hygiene Habits: Start brushing your child's teeth as soon as they erupt. Supervise and assist with brushing and flossing until they are proficient (usually around 7-8 years old).
- Limit Sugary Foods and Drinks: Encourage a balanced diet and restrict frequent snacking on sugary items.
- Fluoride: Ensure your child receives adequate fluoride through fluoridated water, fluoride toothpaste, or professional fluoride treatments.
- Dental Sealants: Discuss dental sealants with your pediatric dentist to protect molars from decay.

Parents should seek immediate dental care if they suspect their child has an abscess gum to prevent pain, further infection, and potential damage to developing permanent teeth.
Frequently Asked Questions
1. What happens if an abscess gum goes untreated?
If an abscess gum is left untreated, the infection can spread beyond your mouth, potentially leading to serious complications such as cellulitis (a severe skin infection), osteomyelitis (jawbone infection), Ludwig's angina (a life-threatening infection under the tongue), or even sepsis (a full-body inflammatory response that can be fatal). It can also result in permanent tooth loss and damage to surrounding healthy teeth and bone.
2. Can an abscess gum heal on its own?
No, an abscess gum will not heal on its own. While the pain might temporarily subside if the pus drains spontaneously, the underlying bacterial infection remains. Without proper dental treatment to eliminate the source of the infection, the abscess will almost certainly recur and continue to pose a risk to your oral and overall health.
3. How long does it take for a gum abscess to go away after treatment?
After initial drainage, pain relief is usually immediate, and swelling starts to subside within 24-48 hours. If antibiotics are prescribed, they typically take 24-48 hours to begin working effectively. Complete healing of the gum tissue or tooth may take several weeks or months, depending on the definitive treatment (e.g., root canal, extraction, or deep cleaning), but the infection should be controlled quickly.
4. Is an abscess gum always painful?
While a gum abscess is typically associated with severe, throbbing pain, not all abscesses cause immediate or intense pain. Some may cause only mild discomfort, or the pain might subside if the abscess drains, leading to a false sense of security. However, even if the pain is minimal, the infection is still present and requires professional attention.
5. Can I use home remedies for an abscess gum?
Home remedies like warm salt water rinses can offer temporary relief by drawing out some fluid and soothing inflammation, but they cannot cure an abscess gum. They do not eliminate the bacterial infection or address the underlying cause. Relying solely on home remedies delays essential professional treatment and increases the risk of serious complications.
6. What's the difference between a periapical abscess and a periodontal abscess?
A periapical abscess originates from an infection inside the tooth's pulp (nerve) due to severe decay or trauma, forming at the tip of the tooth root. A periodontal abscess, on the other hand, starts in the gum tissue itself due to untreated gum disease or a blocked gum pocket, affecting the tissues surrounding the tooth but not the tooth's internal nerve.
7. How much does it cost to treat an abscess gum with insurance?
The cost with insurance varies significantly based on your specific plan's coverage, deductible, and annual maximums. Most dental insurance plans cover 70-80% of basic procedures like drainage or extractions and 50-70% of major procedures like root canals or crowns, after you've met your deductible. It's crucial to check with your provider for an accurate estimate.
8. What are the alternatives to a root canal for a periapical abscess?
For a periapical abscess, the primary alternative to a root canal is tooth extraction. While extraction permanently removes the infected tooth, it means losing a natural tooth and often requires considering replacement options like a dental implant or bridge, which involve additional time and cost.
9. Can an abscess affect other parts of my body?
Yes, absolutely. An untreated abscess gum can have systemic effects. Bacteria can enter the bloodstream and spread to other organs, potentially leading to severe conditions like heart infections (endocarditis), brain abscesses, or general body infection (sepsis), especially in individuals with compromised immune systems.
10. How can I prevent an abscess gum from recurring?
Prevention focuses on excellent oral hygiene: brush twice daily with fluoride toothpaste, floss daily, and use an antimicrobial mouthwash. Regular dental check-ups and professional cleanings (every six months) are vital to catch and treat issues like cavities or gum disease early. Promptly address any dental pain or problems, and avoid tobacco products.
When to See a Dentist
Recognizing when to seek professional dental care for an abscess gum is paramount to preventing severe pain and life-threatening complications.
Seek IMMEDIATE Emergency Dental Care (within hours) if you experience:
- Sudden, Severe, and Unrelenting Throbbing Pain: Especially if it's accompanied by swelling that is rapidly increasing.
- Significant Facial or Jaw Swelling: If the swelling is spreading to your eye, throat, or neck, or if it makes it difficult to breathe or swallow, this is a medical emergency.
- Fever or Chills: These are signs that the infection is spreading systemically.
- Difficulty Opening Your Mouth (Trismus): This can indicate that the infection is affecting jaw muscles.
- Feeling Generally Unwell: Nausea, vomiting, lightheadedness, or extreme fatigue coupled with dental pain.
These symptoms suggest a spreading infection that requires urgent intervention to prevent serious health risks. Do not wait for a regular appointment; contact your dentist's emergency line or go to an urgent care center or emergency room if your dentist is unavailable.
Schedule a Prompt Dental Appointment (within 1-2 days) if you notice:
- Persistent Toothache or Gum Pain: Even if it's mild or comes and goes.
- Localized Gum Swelling or Redness: A "pimple" or boil-like bump on your gums.
- Sensitivity to Hot, Cold, or Chewing: That doesn't resolve within a day or two.
- A Foul Taste in Your Mouth or Bad Breath: That persists despite good oral hygiene.
- A Loose Tooth: That feels different than usual.
While these signs may not indicate an immediate life-threatening emergency, they certainly point to an active infection or a problem that could quickly escalate into an abscess gum. Addressing these issues early can prevent more extensive treatment and discomfort.
Pro Tip: Never hesitate to contact your dentist if you have concerns about oral pain or swelling. Early detection and treatment are always the safest and most effective approaches to managing any dental condition, especially an abscess gum.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
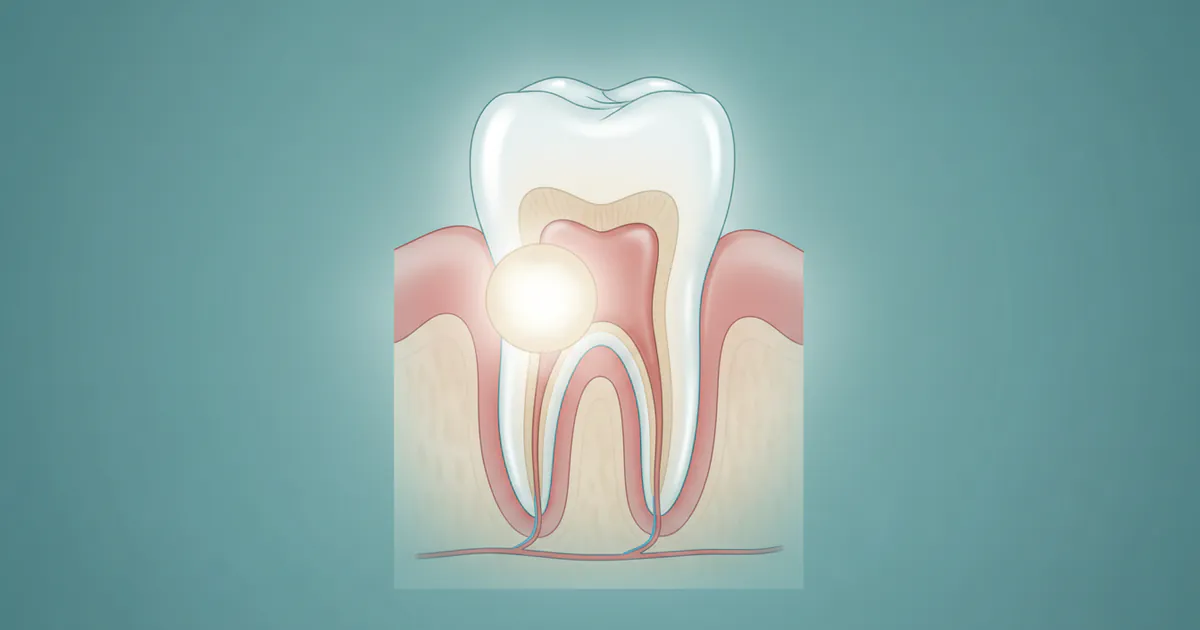
What Is an Abscess
Imagine a throbbing pain deep within your jaw, a persistent ache that keeps you awake at night and makes even the softest foods unbearable. This isn't just a bad toothache; it could be a sign of something much more serious: a dental abscess. Affecting millions of Americans annually, an abscess is an
February 22, 2026
Cracked Tooth Syndrome: Complete Guide
Cracked Tooth Syndrome: Complete Guide Category: Dental Conditions & Diseases
February 22, 2026
Dentinogenesis Imperfecta: Complete Guide
Imagine a world where your teeth, fundamental to chewing, speaking, and even smiling confidently, are inherently fragile, discolored, and prone to rapid wear from the moment they emerge. For individuals affected by dentinogenesis imperfecta (DI), this is a reality. While relatively rare, affecti
February 22, 2026
Stage 1 Early Cavity: Complete Guide
Did you know that dental cavities are one of the most common chronic diseases globally, affecting both children and adults? In the United States, over 90% of adults have had a cavity, and a significant portion of these begin as a stage 1 early cavity. Often invisible and painless in its nasc
February 22, 2026