Toothache Medicine: Complete Guide

Key Takeaways
- A throbbing ache, a sharp pang, or a dull, constant throb – a toothache can be one of the most debilitating and disruptive pains a person experiences. In fact, studies indicate that over 12% of adults in the US experience a toothache in any given year, making it a common reason for emergency den
A throbbing ache, a sharp pang, or a dull, constant throb – a toothache can be one of the most debilitating and disruptive pains a person experiences. In fact, studies indicate that over 12% of adults in the US experience a toothache in any given year, making it a common reason for emergency dental visits and lost productivity. When dental pain strikes, the immediate instinct is often to seek relief, and that's where toothache medicine comes into play. While medication can provide crucial temporary respite, understanding its types, uses, and limitations is paramount. It’s not just about silencing the pain; it’s about understanding the underlying cause and knowing when professional dental intervention is essential to prevent more serious complications.
This comprehensive guide from SmilePedia.net will equip you with a detailed understanding of toothache medicine, from over-the-counter remedies to prescription-strength antibiotics and pain relievers. We'll explore the various causes of toothaches, the different pharmacological approaches to managing them, and critical considerations for their safe and effective use. Furthermore, we’ll delve into essential aspects like cost, insurance, pediatric considerations, potential risks, and, most importantly, when to recognize that your toothache requires immediate professional dental attention. Our aim is to provide a definitive resource that empowers you to make informed decisions about managing dental pain and safeguarding your oral health.
Key Takeaways:
- Immediate Relief is Temporary: Over-the-counter (OTC) pain relievers like ibuprofen or acetaminophen offer temporary relief for toothaches but do not address the underlying cause.
- Dentist Visit is Crucial: Any persistent toothache (lasting more than 1-2 days) or one accompanied by swelling, fever, or difficulty opening your mouth requires immediate professional dental diagnosis and treatment.
- Antibiotics for Infection: Prescription antibiotics (e.g., amoxicillin, clindamycin) are only effective against bacterial infections like a periodontal abscess and should be used strictly as directed by a dentist or physician. They are not pain relievers.
- Average Medication Costs: OTC pain relievers range from $5 to $20, while prescription antibiotics can cost $15 to $50 (generic) or $50 to $200+ (brand name), and stronger prescription pain medications can be $30 to $150+.
- Insurance Coverage Varies: Dental insurance typically does not cover medication costs, but medical insurance often covers prescription drugs. Verify your plan's formulary.
- Severe Complications are Possible: Untreated dental infections can spread, leading to serious health issues, including systemic infections that can impact distant organs, emphasizing the need for timely dental care.
- Prevention is Key: Regular brushing, flossing, and dental check-ups are the best defense against toothaches and the need for medication.
What It Is / Overview
A toothache, medically known as odontalgia, is pain in or around a tooth, often originating from inflammation of the pulp (the innermost part of the tooth containing nerves and blood vessels). Toothache medicine refers to any pharmacological agent used to alleviate this pain, reduce inflammation, or combat the underlying infection. It encompasses a broad range of products, from readily available over-the-counter (OTC) pain relievers to potent prescription medications, including antibiotics and strong analgesics.
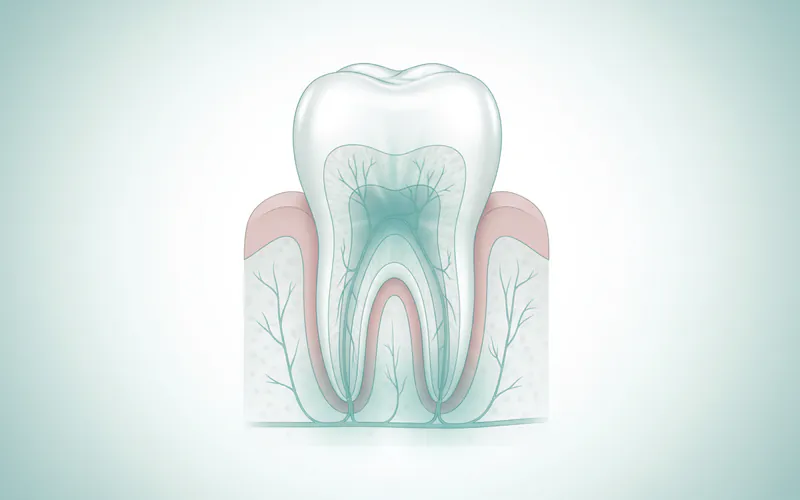
The primary goal of toothache medicine is to provide symptomatic relief, allowing an individual to function while the underlying cause is being diagnosed and treated by a dental professional. It’s critical to understand that medication, especially pain relievers, is rarely a cure for the root problem causing the toothache. For instance, an antibiotic can resolve a bacterial infection, but it won't fix a cavity or a cracked tooth that allowed the infection to start. Therefore, relying solely on medication without addressing the dental issue is a common pitfall that can lead to more severe complications.
Types / Variations of Toothache Medicine
Toothache medicine can be broadly categorized into several types, each with a distinct mechanism of action and intended use. Understanding these distinctions is crucial for selecting the appropriate medication and managing expectations.
1. Over-the-Counter (OTC) Pain Relievers
These are the most common initial choice for toothache relief due to their accessibility and generally good safety profile when used as directed.
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs):
- Mechanism: NSAIDs like ibuprofen (Advil, Motrin) and naproxen (Aleve) work by inhibiting cyclooxygenase (COX) enzymes, which are involved in the synthesis of prostaglandins – chemicals that promote inflammation, pain, and fever.
- Benefits: Excellent for reducing both pain and inflammation, making them highly effective for toothaches, especially those caused by pulp inflammation. They are often recommended by dentists as a first-line treatment.
- Dosage & Considerations: Typically taken every 4-6 hours for ibuprofen or every 8-12 hours for naproxen. Adhere strictly to package instructions to avoid gastrointestinal side effects (e.g., stomach upset, ulcers) and potential kidney issues, particularly with prolonged use or in individuals with pre-existing conditions.
- Acetaminophen (Tylenol):
- Mechanism: Acetaminophen's exact mechanism isn't fully understood, but it's believed to act primarily in the central nervous system to reduce pain and fever. It has minimal anti-inflammatory effects.
- Benefits: A good alternative for individuals who cannot take NSAIDs due to stomach problems, kidney issues, or certain medical conditions.
- Dosage & Considerations: Typically taken every 4-6 hours. The maximum daily dose for adults is generally 3,000-4,000 mg. Overdosing can lead to severe liver damage, so it's crucial to be mindful of other medications you might be taking that also contain acetaminophen.
- Aspirin:
- Mechanism: Aspirin is also an NSAID, but it has anti-platelet effects, meaning it can thin the blood.
- Benefits: Effective for pain relief and inflammation.
- Dosage & Considerations: Due to its blood-thinning properties, aspirin may not be suitable for everyone, especially those on blood thinners or with bleeding disorders. It should not be given to children or teenagers due to the risk of Reye's syndrome, a rare but serious condition.
2. Topical Anesthetics
These medicines provide localized numbing directly to the affected area.
- Benzocaine (Orajel, Anbesol):
- Mechanism: Benzocaine is a local anesthetic that works by temporarily blocking nerve signals in the area where it's applied, leading to numbness.
- Benefits: Can provide very fast, targeted relief for localized pain.
- Dosage & Considerations: Available as gels, liquids, and sprays. Apply a small amount directly to the painful tooth and surrounding gum. Relief is temporary, usually lasting for 15-20 minutes. Pro Tip: Avoid using large quantities or frequently, especially in infants under 2 years old, due to a rare but serious risk of methemoglobinemia, a blood disorder. The American Dental Association (ADA) generally advises against its use in infants for teething.
- Lidocaine:
- Mechanism: Similar to benzocaine, lidocaine is a local anesthetic that numbs the area.
- Benefits: Often found in oral rinses or patches, it can provide more prolonged local numbness.
- Dosage & Considerations: Follow product instructions. Lidocaine rinses can be useful for widespread oral soreness, such as from gum inflammation.
3. Prescription Medications
These are prescribed by a dentist or physician when OTC options are insufficient or when an infection is present.
- Prescription-Strength NSAIDs:
- Mechanism: Stronger doses of NSAIDs like ibuprofen (e.g., 600 mg, 800 mg) or other types like celecoxib (Celebrex) are available by prescription.
- Benefits: Provide more potent pain and inflammation reduction than OTC versions.
- Dosage & Considerations: Used for more severe pain or when OTC doses aren't effective. Requires a prescription and careful monitoring for side effects.
- Opioid Pain Relievers:
- Mechanism: Opioids (e.g., hydrocodone with acetaminophen, oxycodone) work by binding to opioid receptors in the brain and spinal cord, altering the perception of pain.
- Benefits: Reserved for severe, acute pain that is not adequately managed by NSAIDs or acetaminophen.
- Dosage & Considerations: Due to significant risks of dependence, addiction, and serious side effects (nausea, constipation, drowsiness, respiratory depression), these are prescribed for short durations and with extreme caution. The ADA promotes responsible prescribing and limits opioid use.
- Antibiotics:
- Mechanism: Antibiotics combat bacterial infections by either killing bacteria (bactericidal) or inhibiting their growth (bacteriostatic). They are NOT pain relievers.
- Benefits: Essential for treating bacterial dental infections like an abscess (e.g., periodontal abscess, periapical abscess) that involves swelling, pus, or fever. Common antibiotics for dental infections include amoxicillin, clindamycin, metronidazole, and penicillin.
- Dosage & Considerations: Must be prescribed by a dental professional or physician after diagnosis of an active bacterial infection. It is crucial to complete the entire course of antibiotics as prescribed, even if symptoms improve, to prevent antibiotic resistance and ensure complete eradication of the infection. Inappropriate use of antibiotics contributes to global antibiotic resistance, a major public health concern.
Causes / Why It Happens
Understanding the cause of a toothache is crucial because the medicine can only provide symptomatic relief; the underlying issue requires specific dental treatment.
- Dental Caries (Cavities): The most common cause. When decay penetrates the enamel and dentin, it can reach the pulp, causing inflammation and pain.
- Dental Abscess: A localized collection of pus, usually caused by a bacterial infection.
- Periapical Abscess: Occurs at the tip of the tooth root, often due to untreated decay or trauma leading to pulp necrosis (death).
- Periodontal Abscess: This involves infection in the gum tissue surrounding the tooth, often due to severe gum disease (periodontitis) or food impaction in a gum pocket. A periodontal abscess can cause intense, throbbing pain, swelling, and sometimes a foul taste. It can lead to significant bone loss around the tooth if left untreated.
- Cracked or Fractured Tooth: Chips, cracks, or fractures can expose the sensitive inner layers of the tooth to temperature changes and bacteria, leading to pain.
- Gum Disease (Periodontitis/Gingivitis): Inflammation and infection of the gums can cause sensitivity, bleeding, and eventually toothache as the supporting structures of the teeth are compromised.
- Sensitive Teeth: Exposed dentin (due to receding gums, aggressive brushing, or enamel erosion) can cause sharp, temporary pain in response to hot, cold, sweet, or acidic foods.
- Bruxism (Teeth Grinding): Chronic grinding or clenching of teeth can put excessive pressure on teeth and jaw joints, leading to diffuse tooth pain, muscle soreness, and headaches.
- Impacted Wisdom Teeth: Wisdom teeth that don't have enough room to erupt properly can cause pain, inflammation, and infection (pericoronitis) of the surrounding gum tissue.
- Referred Pain: Pain originating from other areas can be perceived as a toothache. This includes:
- Sinusitis: Inflammation of the sinus cavities (often due to colds or allergies) can cause pressure and pain in the upper back teeth, which share nerve pathways.
- Temporomandibular Joint (TMJ) Disorders: Problems with the jaw joint can refer pain to the teeth, face, and head.
- Ear infections or Headaches: Less common, but possible.
Signs and Symptoms
Recognizing the specific characteristics of your toothache can help your dentist diagnose the problem.
- Sharp, Shooting Pain: Often triggered by hot, cold, or sweet stimuli, indicative of a cavity reaching the dentin or pulp, or a cracked tooth.
- Dull, Constant Ache: Can suggest persistent inflammation of the pulp or nerve, or general jaw pain from clenching.
- Throbbing Pain, Swelling, Redness: Strongly suggests a bacterial infection and abscess formation, particularly in the case of a periodontal abscess. This pain may worsen when lying down.
- Pain on Biting or Chewing: Can point to a cracked tooth, a cavity, a loose filling, or a dental abscess.
- Tenderness to Touch: A tooth that is exquisitely sensitive to even light touch or pressure often has an acute inflammatory or infectious process.
- Facial Swelling: Swelling around the jaw, cheek, or neck is a serious sign of spreading infection and warrants immediate dental attention.
- Fever or Chills: These systemic symptoms indicate a spreading infection that requires prompt medical intervention.
- Bad Taste or Odor: A persistent foul taste or odor, especially if accompanied by a small pimple-like bump on the gum, may indicate pus drainage from an abscess.
- Difficulty Opening Mouth (Trismus): A sign that the infection or inflammation is affecting the muscles of mastication.
Treatment Options (Beyond Medicine)
While medicine provides relief, comprehensive dental treatment is necessary to resolve the underlying cause of a toothache.
- For Cavities:
- Dental Fillings: For small to moderate cavities, the decayed portion is removed, and the tooth is restored with a filling material (composite, amalgam).
- Crowns: For larger cavities or fractured teeth where a filling isn't sufficient, a crown (cap) is placed over the tooth.
- For Pulp Infection/Abscess:
- Root Canal Treatment (Endodontic Therapy): If the pulp is irreversibly inflamed or infected, the diseased pulp tissue is removed, the canals are cleaned and disinfected, and then filled and sealed. A crown usually follows to protect the tooth.
- Tooth Extraction: If the tooth is too damaged to be saved or if root canal therapy is not feasible, extraction may be necessary. For a severe periodontal abscess, deep cleaning, drainage, and sometimes surgical intervention may be required in conjunction with antibiotics.
- For Gum Disease/Periodontal Abscess:
- Deep Cleaning (Scaling and Root Planing): Removal of plaque and tartar from above and below the gumline.
- Antibiotics: Often prescribed alongside deep cleaning for significant infections.
- Gum Surgery: In advanced cases, surgical procedures may be needed to reduce pocket depths and regenerate lost bone.
- For Cracked/Fractured Teeth:
- Bonding or Filling: For minor cracks.
- Crown: For larger cracks that threaten the integrity of the tooth.
- Root Canal/Extraction: If the crack extends into the pulp or below the gum line.
- For Impacted Wisdom Teeth:
- Extraction: Surgical removal of the wisdom tooth is often the definitive treatment to prevent recurrent infection and pain.
Step-by-Step Process: Managing a Toothache with Medicine and Seeking Care
When a toothache strikes, knowing the proper steps can guide you towards relief and appropriate dental care.
-
Assess the Pain and Your Symptoms:
- Is the pain mild, moderate, or severe?
- Is it constant, throbbing, or sharp?
- Are there any associated symptoms like swelling, fever, difficulty eating, or opening your mouth?
-
Initial Self-Care and OTC Medicine:
- Rinse Your Mouth: Gently rinse your mouth with warm salt water (1/2 teaspoon of salt in 8 ounces of warm water) to clean the area and reduce inflammation.
- Floss: Gently floss around the affected tooth to remove any trapped food particles that might be exacerbating the pain.
- OTC Pain Relievers:
- Take an NSAID like ibuprofen (200-400 mg every 4-6 hours, maximum 1200 mg/day for OTC) or naproxen (220-440 mg every 8-12 hours, maximum 660 mg/day for OTC).
- If NSAIDs are contraindicated, consider acetaminophen (325-500 mg every 4-6 hours, maximum 3000-4000 mg/day).
- Follow dosage instructions carefully.
- Topical Anesthetic: Apply a small amount of benzocaine gel (e.g., Orajel) directly to the painful tooth and gum for temporary numbing.
-
Contact Your Dentist:
- If the pain is severe, persistent (more than 1-2 days), or accompanied by swelling, fever, or difficulty swallowing/breathing, call your dentist immediately. Explain your symptoms clearly.
- Even if OTC medicine provides relief, schedule an appointment to have the underlying cause diagnosed and treated.
- Pro Tip: Be prepared to describe the nature, location, and intensity of your pain, as well as any triggers or relieving factors.
-
Dental Examination and Diagnosis:
- Your dentist will perform a thorough examination, which may include X-rays to identify the source of the problem (e.g., cavity, abscess, crack).
- They may also perform tests like pulp vitality testing (checking nerve response) and percussion tests (tapping the tooth) to pinpoint the affected tooth.
-
Prescription Medication (If Indicated):
- If a bacterial infection (like a periodontal abscess) is diagnosed, your dentist will prescribe antibiotics.
- Important: Start the antibiotics as prescribed and complete the entire course, even if your pain subsides. Stopping early can lead to recurrence and antibiotic resistance.
- For very severe pain, your dentist might prescribe stronger pain medication for a short period.
- Pro Tip: Discuss all your current medications and medical conditions with your dentist to avoid potential drug interactions or adverse effects.
- If a bacterial infection (like a periodontal abscess) is diagnosed, your dentist will prescribe antibiotics.
-
Definitive Dental Treatment:
- Once the acute symptoms are managed and the diagnosis is confirmed, your dentist will proceed with the appropriate treatment (filling, root canal, extraction, deep cleaning, etc.) to resolve the underlying cause of the toothache.
- IMAGE: A flowchart illustrating the decision-making process for toothache: "Toothache? -> Mild/Temporary? -> OTC Meds/Home Remedies. -> Persistent/Severe/Swelling/Fever? -> Contact Dentist. -> Dentist Exam/X-ray -> Diagnosis -> Prescribed Meds/Dental Procedure."
Cost and Insurance
The costs associated with toothache medicine and the necessary dental treatments can vary widely.
Medication Costs:
- Over-the-Counter (OTC) Pain Relievers:
- Ibuprofen, acetaminophen, naproxen: $5 - $20 for a standard bottle, depending on brand and quantity.
- Topical anesthetics (benzocaine): $8 - $15 per tube/bottle.
- Prescription Medications:
- Generic Antibiotics (e.g., Amoxicillin, Metronidazole): $15 - $50 for a typical course (7-14 days) without insurance.
- Brand-Name Antibiotics (if generic not available or suitable): $50 - $200+.
- Prescription-Strength NSAIDs (e.g., higher dose ibuprofen): $20 - $70.
- Opioid Pain Relievers (e.g., Hydrocodone-acetaminophen): $30 - $150+ for a limited supply, highly dependent on the drug and quantity.
Dental Procedure Costs:
These costs are for the actual treatment of the underlying cause, not just the medication. Prices vary significantly by region (e.g., metropolitan vs. rural areas) and the complexity of the case.
| Procedure Type | Average US Cost Range (without insurance) |
|---|---|
| Emergency Exam & X-ray | $75 - $250 |
| Simple Filling (Amalgam) | $50 - $150 |
| Composite (Tooth-Colored) Filling | $100 - $300 |
| Simple Tooth Extraction | $150 - $450 |
| Surgical Extraction (Impacted) | $300 - $800+ |
| Root Canal Treatment (front tooth) | $700 - $1,200 |
| Root Canal Treatment (molar) | $1,000 - $2,000+ |
| Dental Crown | $800 - $2,500+ |
| Scaling & Root Planing (per quadrant) | $200 - $500 |
| Incision and Drainage of Abscess | $100 - $300 |
Insurance Coverage:
- Dental Insurance: Typically covers a portion of diagnostic (exams, X-rays) and restorative procedures (fillings, root canals, extractions). Coverage levels vary (e.g., 80-100% for preventive, 50-80% for basic restorative, 20-50% for major restorative). Most dental plans do not cover prescription medications, though they may cover some in-office procedures like antibiotics placed directly into gum pockets.
- Medical Insurance: Prescription medications (antibiotics, pain relievers) are usually covered under your medical insurance's prescription drug plan. Your co-pay or deductible will apply. It's essential to check your specific plan's formulary (list of covered drugs) and tier system.
- No Insurance: Many dental offices offer discounts for cash payments or in-house payment plans. Dental schools often provide lower-cost treatment options. Federally Qualified Health Centers (FQHCs) may offer services on a sliding scale fee based on income.
Recovery and Aftercare
Once the toothache has been addressed, whether through medication, a dental procedure, or both, proper aftercare is crucial for healing and preventing recurrence.
- For Medication Use (Antibiotics):
- Complete the Full Course: Finish all prescribed antibiotics, even if symptoms improve, to ensure the infection is fully eradicated and prevent antibiotic resistance.
- Manage Side Effects: Be aware of potential side effects (e.g., nausea, diarrhea) and discuss them with your dentist or pharmacist. Some antibiotics may interact with alcohol or other medications.
- After Dental Procedures:
- Pain Management: Take prescribed or OTC pain relievers as directed.
- Swelling: Apply a cold compress to the outside of your cheek for 15-20 minutes on, 15-20 minutes off, for the first 24-48 hours to reduce swelling.
- Diet: Stick to soft foods initially and avoid chewing on the treated side until the area heals or a permanent restoration (like a crown) is placed.
- Oral Hygiene: Gently brush and floss around the treated area, avoiding vigorous rinsing for the first 24 hours to protect blood clots or surgical sites.
- Follow-Up: Attend all scheduled follow-up appointments with your dentist to ensure proper healing and address any concerns.
- Pro Tip: If you experience increasing pain, swelling that doesn't subside, fever, or difficulty swallowing after a dental procedure, contact your dentist immediately.
Prevention
Preventing toothaches is always better than treating them. Most toothaches are preventable with good oral hygiene and regular dental care.
- Brush Twice Daily: Use a fluoride toothpaste and brush for at least two minutes, morning and night.
- Floss Daily: Remove plaque and food particles from between teeth and under the gumline where a toothbrush can't reach. This is critical for preventing gum disease and periodontal abscesses.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and examinations. This allows for early detection and treatment of cavities and gum disease before they cause pain. The ADA recommends these regular visits.
- Limit Sugary and Acidic Foods/Drinks: Reduce consumption of items that promote tooth decay and enamel erosion.
- Use Fluoride: Consider fluoride rinses or treatments if recommended by your dentist, especially if you have a high risk of cavities.
- Wear a Mouthguard: If you grind your teeth (bruxism) or play contact sports, a custom-fitted mouthguard can protect your teeth from damage and excessive wear.
- Avoid Smoking and Tobacco Products: Tobacco significantly increases the risk of gum disease, tooth decay, and oral cancer.
Risks and Complications
While toothache medicine is generally safe when used as directed, there are potential risks and complications. More importantly, the risks of an untreated toothache can be severe.
Risks of Medication:
- Gastrointestinal Issues: NSAIDs can cause stomach upset, heartburn, ulcers, and bleeding. Long-term use can lead to kidney problems.
- Liver Damage: Overdosing on acetaminophen can cause severe, irreversible liver damage. Be careful not to exceed the maximum daily dose and check other medications for hidden acetaminophen.
- Allergic Reactions: Any medication can cause an allergic reaction, ranging from mild rash to severe anaphylaxis (difficulty breathing, swelling of the face/throat), which is a medical emergency.
- Antibiotic Resistance: Misuse or overuse of antibiotics contributes to the development of antibiotic-resistant bacteria, making future infections harder to treat. This is why antibiotics should only be used when a bacterial infection is confirmed.
- Opioid Risks: Addiction, dependence, overdose, and severe side effects like respiratory depression, nausea, and constipation.
- Methemoglobinemia: A rare but serious blood disorder associated with excessive use of topical benzocaine, especially in very young children.
Risks of Untreated Toothache/Infection:
- Spread of Infection: A dental infection, particularly an abscess, can spread to surrounding tissues, including the jawbone, neck, face, and even into serious anatomical spaces.
- Cellulitis: A rapidly spreading bacterial infection of the skin and soft tissues.
- Ludwig's Angina: A severe, potentially life-threatening infection of the floor of the mouth that can compromise the airway.
- Cavernous Sinus Thrombosis: A rare but deadly blood clot in the brain's venous sinuses, often stemming from dental infections.
- Sepsis: A life-threatening condition caused by the body's overwhelming response to an infection, which can lead to organ damage or failure. In extremely rare and severe cases of unchecked systemic infection, bacterial dissemination through the bloodstream (bacteremia) could theoretically lead to abscess formation in distant organs, including those in the abdominal cavity, although this is an exceptionally uncommon complication directly from a dental source alone and often linked to immunocompromised states. More commonly, NSAIDs used for toothache can cause gastrointestinal ulcers or bleeding, impacting the abdominal cavity directly.
- Tooth Loss: Untreated cavities or gum disease can lead to extensive tooth destruction, requiring extraction.
- Bone Loss: Chronic periodontal abscesses and periodontitis can destroy the bone supporting the teeth, leading to tooth mobility and eventual loss.
- Systemic Health Impacts: Chronic oral inflammation and infection have been linked to an increased risk of systemic conditions such as cardiovascular disease, diabetes complications, and adverse pregnancy outcomes.
Children / Pediatric Considerations
Managing toothache in children requires special care and attention.
- Never Give Aspirin: As mentioned, aspirin is contraindicated in children and teenagers due to the risk of Reye's syndrome.
- Age-Appropriate Dosing: Always use children's formulations of acetaminophen or ibuprofen and follow the dosing instructions precisely based on the child's weight or age. If unsure, consult a pediatrician or pharmacist.
- Topical Anesthetics: Use benzocaine products sparingly and with extreme caution, if at all, for children under 2. Consult a dentist or pediatrician for teething pain.
- Early Intervention: Children's dental problems can progress rapidly. Any persistent toothache in a child warrants an immediate dental visit.
- Baby Teeth Matter: While baby teeth eventually fall out, they are crucial for speech, eating, and guiding the eruption of permanent teeth. Untreated infections in baby teeth can affect the developing permanent teeth beneath them.
- Prevention is Paramount: Instill good brushing and flossing habits early. Limit sugary snacks and drinks. Regular pediatric dental check-ups are essential from the appearance of the first tooth.
- Pro Tip: If a child's toothache is accompanied by swelling, fever, or signs of systemic illness, seek emergency medical or dental care immediately.
Cost Breakdown
Understanding the various components of cost related to toothache management can help with financial planning.
- Initial Consultation/Emergency Exam:
- Low: $75 - $150 (basic exam, no X-rays or single X-ray)
- Mid: $150 - $250 (exam, limited X-rays, often includes a prescription)
- High: $250 - $400+ (after-hours emergency, extensive diagnostics)
- Medication Costs (covered earlier):
- OTC: $5 - $20
- Prescription (generic): $15 - $50
- Procedure Costs (as per table above): These vary most widely.
- With Insurance vs. Without Insurance:
- With Insurance: You'll pay your deductible (if applicable), co-pays for office visits, and a percentage of the procedure costs (co-insurance) as determined by your plan's coverage levels (e.g., 20% for basic, 50% for major). For medications, your medical insurance drug co-pay will apply. Your annual maximum benefit for dental insurance typically ranges from $1,000 to $2,000.
- Without Insurance: You are responsible for 100% of all costs. This is where payment plans, dental schools, or community clinics can be vital.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental practices offer interest-free payment plans for a few months, especially for larger treatments.
- Third-Party Financing (e.g., CareCredit): These credit cards specifically for healthcare can offer deferred interest or low-interest financing for longer periods, often for costs ranging from $200 to $25,000.
- Dental Schools: Often provide high-quality treatment at significantly reduced costs (e.g., 30-50% less) because patients are treated by supervised students.
- Community Dental Clinics/FQHCs: May offer services on a sliding scale based on income, providing affordable care for uninsured or underinsured individuals.
- Dental Discount Plans: Not insurance, but these plans offer a discount on services from participating dentists for an annual fee, typically saving 10-60% on procedures.
Cost-Saving Tips:
- Preventive Care: The single best way to save money is to prevent dental problems with regular brushing, flossing, and check-ups. Catching a small cavity early with a $100 filling is far cheaper than a $1,500 root canal and crown later.
- Compare Prices: Don't hesitate to call different dental offices and inquire about costs for specific procedures.
- Ask for Cash Discounts: Many practices offer a discount (e.g., 5-10%) for patients paying in full at the time of service.
- Negotiate: For extensive treatment plans, discuss payment options and potential adjustments with your dentist's office.
Frequently Asked Questions
What is the strongest toothache medicine?
The "strongest" toothache medicine depends on whether you're referring to pain relief or infection control. For pain, prescription opioids (like hydrocodone) are typically the most potent but come with significant risks. However, often a combination of a prescription-strength NSAID (like ibuprofen) and acetaminophen provides very effective pain relief with fewer side effects. For infection, a targeted antibiotic prescribed by a dentist is the strongest medicine, as pain relievers do not kill bacteria.
How long does it take for toothache medicine to work?
Over-the-counter NSAIDs (like ibuprofen) or acetaminophen usually begin to work within 30-60 minutes. Topical anesthetics (like benzocaine) can provide near-instantaneous, but short-lived, numbing. Prescription antibiotics typically take 24-48 hours to start reducing infection-related pain, as they need time to fight the bacteria, and their full effect may not be felt for several days.
Can I get antibiotics for a toothache without seeing a dentist?
In most cases, no. Dentists and physicians are ethically and legally bound to prescribe antibiotics only when a bacterial infection has been diagnosed. Self-diagnosing and using leftover antibiotics is dangerous, contributes to antibiotic resistance, and can mask a serious underlying dental issue that needs professional treatment.
Does toothache medicine cure the toothache?
No, most toothache medicine provides only temporary symptomatic relief. Pain relievers reduce pain and inflammation, and antibiotics fight infection, but they do not fix the underlying structural problem causing the toothache, such as a cavity, crack, or abscess. A dentist must address the root cause to provide a permanent solution.
What are the side effects of toothache medicine?
Common side effects of NSAIDs include stomach upset, heartburn, and in rare cases, ulcers or bleeding. Acetaminophen can cause liver damage if overdosed. Opioids carry risks of nausea, constipation, drowsiness, and addiction. Antibiotics can cause gastrointestinal upset, diarrhea, and allergic reactions. Always read the package inserts and discuss potential side effects with your dentist or pharmacist.
Are home remedies effective for toothache?
Home remedies like warm salt water rinses, clove oil, or cold compresses can provide temporary comfort by reducing inflammation or numbing the area. However, they are not substitutes for professional dental care, especially for persistent or severe toothaches. They should be seen as adjuncts to aid comfort until you can see a dentist.
How much does it cost to get medicine for a toothache?
The cost varies. Over-the-counter pain relievers typically range from $5 to $20. Prescription antibiotics can cost $15 to $50 for generic versions with insurance, and up to $200+ for brand names or without insurance. Stronger prescription pain medications can be $30 to $150+. These costs do not include the dental exam or the definitive treatment for the underlying issue.
Can a toothache spread to other parts of my body?
Yes, an untreated dental infection, particularly an abscess, can spread. It can lead to severe complications like cellulitis in the face or neck, Ludwig's angina (a life-threatening infection of the mouth floor), or even systemic infections like sepsis. While rare, unchecked infections can even lead to abscesses in distant organs, emphasizing the importance of prompt dental intervention.
When to See a Dentist
While over-the-counter toothache medicine can provide temporary relief, it's crucial to know when to seek professional dental attention. Delaying treatment can lead to more severe pain, complicated procedures, and even life-threatening systemic infections.
See a dentist immediately or seek emergency care if you experience any of the following warning signs:
- Severe, persistent toothache: Pain that lasts for more than 1-2 days and doesn't respond well to OTC pain relievers.
- Swelling: Any visible swelling in your face, jaw, gums, or neck. This is a strong indicator of infection, such as a periodontal abscess, that needs urgent attention.
- Fever or Chills: These are systemic signs that the infection may be spreading beyond the tooth and into your body.
- Difficulty Breathing or Swallowing: This is a medical emergency, as a severe oral infection can spread to the airway, potentially blocking it. Call 911 or go to the nearest emergency room.
- Pus Drainage: A foul taste in your mouth, or a small pimple-like bump on your gum (a "fistula") that drains pus, indicates an active infection.
- Pain on Opening Mouth (Trismus): If you find it difficult or painful to open your mouth wide.
- Trauma: A toothache following an injury, accident, or trauma to your mouth or face.
- Tooth that Feels "Long" or Loose: Can indicate inflammation around the root or bone loss due to infection.
For non-emergency situations, you should still schedule an appointment with your dentist if:
- You experience sensitivity to hot, cold, or sweet foods/drinks that is persistent.
- You notice any new cavities or black/brown spots on your teeth.
- A filling or crown becomes loose or falls out.
- You have persistent bad breath or bleeding gums.
Pro Tip: Do not wait for the pain to become unbearable. Early intervention for dental problems is almost always simpler, less expensive, and more effective than waiting until the issue has become severe. Your dentist can accurately diagnose the cause of your toothache and provide the definitive treatment needed, beyond just symptomatic relief from medicine.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Is an Abscess
Imagine a throbbing pain deep within your jaw, a persistent ache that keeps you awake at night and makes even the softest foods unbearable. This isn't just a bad toothache; it could be a sign of something much more serious: a dental abscess. Affecting millions of Americans annually, an abscess is an
February 22, 2026
Cracked Tooth Syndrome: Complete Guide
Cracked Tooth Syndrome: Complete Guide Category: Dental Conditions & Diseases
February 22, 2026
Dentinogenesis Imperfecta: Complete Guide
Imagine a world where your teeth, fundamental to chewing, speaking, and even smiling confidently, are inherently fragile, discolored, and prone to rapid wear from the moment they emerge. For individuals affected by dentinogenesis imperfecta (DI), this is a reality. While relatively rare, affecti
February 22, 2026
Stage 1 Early Cavity: Complete Guide
Did you know that dental cavities are one of the most common chronic diseases globally, affecting both children and adults? In the United States, over 90% of adults have had a cavity, and a significant portion of these begin as a stage 1 early cavity. Often invisible and painless in its nasc
February 22, 2026