Antibiotics for Tooth Infection: Complete Guide
Key Takeaways
- Have you ever experienced a throbbing, relentless toothache that made it impossible to eat, sleep, or even think straight? You're not alone. Dental infections, often called tooth abscesses, affect millions of Americans each year, with studies suggesting that **up to 12% of adults experience a dental
Antibiotics for Tooth Infection: Complete Guide
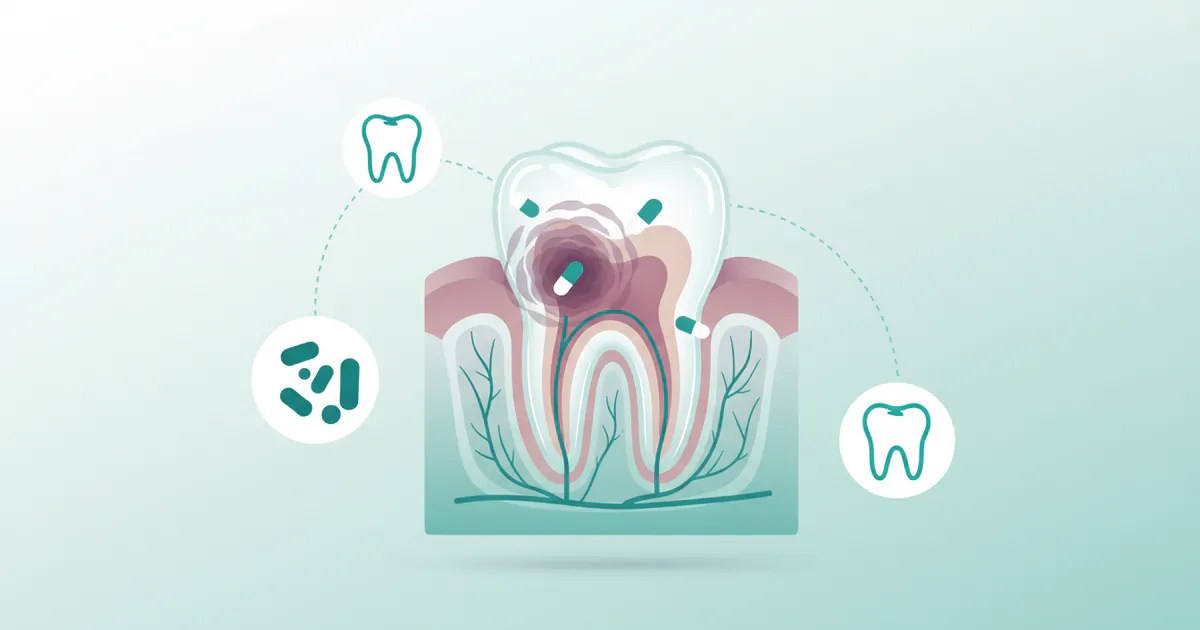
Have you ever experienced a throbbing, relentless toothache that made it impossible to eat, sleep, or even think straight? You're not alone. Dental infections, often called tooth abscesses, affect millions of Americans each year, with studies suggesting that up to 12% of adults experience a dental abscess at some point. When bacteria invade the innermost parts of your tooth or surrounding gums, the pain can be excruciating, and if left untreated, the infection can spread, leading to severe, even life-threatening complications. In many cases, antibiotics for tooth infection become a crucial first step in managing the acute symptoms and preventing further spread, buying time for a definitive dental procedure.
This comprehensive guide from SmilePedia.net will demystify tooth infections and the role of antibiotics in their treatment. We’ll delve into what causes these painful conditions—from deep decay to a broken tooth or cracked tooth—and explore the full spectrum of treatment options available. You'll learn when antibiotics are necessary, which types are commonly prescribed, what to expect during treatment, potential costs, and crucial prevention strategies to keep your smile healthy and pain-free. Understanding this vital information empowers you to make informed decisions about your dental health and seek timely, appropriate care.
Key Takeaways:
- Antibiotics are not a cure: They manage acute infection symptoms and prevent spread but do not eliminate the underlying cause of a tooth infection. Definitive dental treatment (e.g., root canal, extraction) is always required.
- Common Causes: Deep cavities, trauma resulting in a broken tooth or cracked tooth, and gum disease are primary entry points for bacteria.
- When Antibiotics Are Indicated: Typically prescribed when an infection shows signs of spreading (facial swelling, fever, swollen lymph nodes) or for immunocompromised patients. A localized abscess without systemic symptoms may not require antibiotics if definitive treatment can be performed immediately.
- Typical Course: Antibiotic treatment usually lasts 7-10 days, with symptom improvement often seen within 1-3 days. Always complete the full course.
- Cost Range: A dental exam and X-ray can range from $50 to $200. Generic antibiotics usually cost $10-$100 without insurance, while a root canal can be $700-$2,000+ and an extraction $150-$600+, depending on complexity and location.
- Serious Risks: Untreated tooth infections can lead to life-threatening conditions such as cellulitis, Ludwig's angina, sepsis, or even brain abscess.
- Prevention is Key: Maintain excellent oral hygiene, attend regular dental check-ups, and address dental issues like decay or minor cracks promptly.
What Is a Tooth Infection? An Overview
A tooth infection, medically known as a dental abscess, is a pocket of pus caused by bacterial infection. This pus is a collection of dead white blood cells, bacteria, and tissue debris that forms as your body fights the infection. The infection typically originates from bacteria entering the pulp (the innermost part of the tooth containing nerves, blood vessels, and connective tissue) or the surrounding gums and bone.
Once bacteria breach the protective enamel and dentin layers of your tooth, or the gum tissue around it, they proliferate, leading to inflammation and the body's immune response. This response creates pressure within the confined spaces of the tooth or jawbone, resulting in the characteristic severe pain associated with a dental abscess.
Types of Tooth Infections
There are primarily two types of dental abscesses, differentiated by their location and origin:
- Periapical Abscess: This is the most common type and forms at the tip of the tooth root. It occurs when bacteria infect the dental pulp, usually due to a deep cavity, a cracked tooth, or a broken tooth that exposes the pulp to bacteria. The infection then spreads down through the root canal to the bone at the apex (tip) of the root.
- Periodontal Abscess: This type of abscess forms in the gum tissue next to the root of a tooth. It's often a complication of severe gum disease (periodontitis), where bacteria accumulate in gum pockets and infect the supporting tissues and bone around the tooth. Food impaction or trauma can also cause it.
While both types are serious and require immediate dental attention, the treatment approach can differ based on the origin and extent of the infection.
Causes: Why Tooth Infections Happen
Dental infections don't appear out of nowhere; they are almost always the result of bacteria finding a way to invade the vulnerable tissues of your mouth. Understanding these causes is crucial for both prevention and prompt treatment.
1. Deep Tooth Decay (Cavities)
This is the most common culprit. When cavities are left untreated, they progressively erode the outer layers of the tooth (enamel and dentin). Eventually, the decay reaches the dental pulp, which is rich in nerves and blood vessels. Once bacteria infiltrate the pulp, an infection can quickly develop and spread, leading to a periapical abscess.
2. Trauma: A Broken Tooth or Cracked Tooth
Dental trauma, even seemingly minor, can provide a direct pathway for bacteria.
- Broken Tooth: A significant fracture, especially one that extends into the pulp chamber, immediately exposes the delicate inner tissues to oral bacteria. This can happen from biting on something hard, a fall, or a sports injury.
- Cracked Tooth: Even hairline cracks, which may not be immediately visible or painful, can allow bacteria to penetrate the enamel and dentin, slowly reaching the pulp over time. These cracks can be caused by teeth grinding (bruxism), large fillings weakening the tooth structure, or temperature changes. A cracked tooth syndrome can be notoriously difficult to diagnose, but it's a significant risk factor for infection.
3. Gum Disease (Periodontitis)
Advanced gum disease leads to the formation of deep pockets between the teeth and gums. These pockets become breeding grounds for bacteria, which can then infect the gum tissue, ligaments, and bone supporting the teeth, leading to a periodontal abscess. Without proper treatment, this can result in tooth mobility and eventual tooth loss.
4. Failed Dental Work
Sometimes, even previously treated teeth can develop infections. A leaky filling or crown can allow bacteria to seep underneath and reach the pulp. Similarly, an inadequately performed root canal (though rare) or re-infection of a previously treated root canal can also lead to an abscess.
5. Compromised Immune System
Individuals with weakened immune systems (due to conditions like diabetes, HIV/AIDS, cancer treatment, or long-term steroid use) are more susceptible to infections and may find it harder to fight them off. This makes prompt dental care even more critical for them.
Signs and Symptoms of a Tooth Infection
Recognizing the signs and symptoms of a tooth infection early is vital for preventing its spread and minimizing discomfort. While pain is the most common indicator, an abscess can manifest in several ways.
Common Symptoms:
- Severe, Persistent, Throbbing Toothache: This is often the hallmark symptom. The pain can be sharp, gnawing, or throbbing and may radiate to your ear, jaw, or neck. It often worsens when you lie down.
- Sensitivity to Hot and Cold: The affected tooth may become extremely sensitive to temperature changes, lingering even after the stimulus is removed.
- Sensitivity to Pressure or Chewing: Biting down or applying pressure to the infected tooth can cause intense pain.
- Swelling in the Face, Cheek, or Neck: The infection can spread to surrounding soft tissues, causing visible swelling. This swelling can sometimes make it difficult to open your mouth fully or swallow.
- Fever: A systemic sign indicating your body is fighting a significant infection.
- Swollen, Tender Lymph Nodes: Lymph nodes in your neck or under your jaw may become swollen and painful as they work to filter out the infection.
- Bad Taste in Your Mouth or Bad Breath: Pus draining from the abscess can cause an unpleasant taste or persistent bad breath, even with good oral hygiene.
- Pimple-like Bump on the Gums: A "fistula" or "gum boil" may appear on the gum near the infected tooth. This is where the pus is draining, often providing temporary relief from pain but indicating an active infection.
- Discolored Tooth: The infected tooth may appear darker than surrounding teeth due to internal changes.
Pro Tip: If you experience any of these symptoms, especially a severe toothache accompanied by swelling or fever, do not delay seeking dental attention. These are not symptoms that will resolve on their own.
When Are Antibiotics for Tooth Infection Necessary?
It's a common misconception that every tooth infection requires antibiotics. While antibiotics are powerful tools, they are not always the first or only line of defense. The decision to prescribe antibiotics is based on the nature and severity of the infection, and it's always made by a dental professional.
When Antibiotics Are Typically Prescribed:
- Signs of Spreading Infection (Systemic Symptoms): This is the most crucial indicator. If the infection has spread beyond the immediate area of the tooth and is causing:
- Facial swelling: Swelling of the cheek, jaw, or neck (cellulitis).
- Fever: A body temperature of 100.4°F (38°C) or higher.
- Swollen lymph nodes: Tender, enlarged glands in the neck or under the jaw.
- Difficulty swallowing or breathing: This indicates a serious, rapidly spreading infection that can be life-threatening (e.g., Ludwig's angina).
- Immunocompromised Patients: Individuals with weakened immune systems (e.g., diabetics, cancer patients, organ transplant recipients) are more vulnerable to severe infections. Antibiotics may be prescribed more readily to prevent rapid progression.
- Prior to Definitive Treatment (Sometimes): In some cases, if the infection is acute and causing significant swelling, a dentist might prescribe antibiotics for a few days to reduce the inflammation and infection before performing a root canal or extraction. This makes the area more numb for local anesthetic and can reduce post-operative complications.
- Inability to Immediately Drain the Abscess: If the dentist cannot immediately perform an incision and drainage (I&D) or definitive treatment, antibiotics can help control the infection temporarily.
When Antibiotics May Not Be Necessary:
- Localized Abscess without Systemic Symptoms: If the infection is localized to the tooth and surrounding bone, and there are no signs of spreading or systemic illness, antibiotics may not be needed, especially if the abscess can be immediately drained or treated definitively (e.g., a simple root canal or extraction).
- Chronic Abscess with a Fistula: If an abscess has been draining through a "gum boil" (fistula) for some time, it may not require antibiotics, as the body is already effectively draining the pus. However, definitive dental treatment is still essential.
Important Note: Antibiotics kill bacteria but do not remove the source of the infection (the dead pulp tissue, the pus, or the bacterial biofilm within the tooth). Therefore, they are almost always a temporary measure to manage acute symptoms, buying time until definitive dental treatment can be performed.
Common Antibiotics Used for Tooth Infections
Several types of antibiotics are effective against the bacteria typically found in oral infections. Your dentist will choose the most appropriate one based on your medical history, any known allergies, and the specific characteristics of your infection.
Table 1: Common Antibiotics for Tooth Infections
| Antibiotic Type | Common Prescriptions | Typical Dosage & Duration (Adults) | Common Side Effects | Considerations |
|---|---|---|---|---|
| Penicillins | Amoxicillin, Penicillin V | 500mg, 3x/day for 7-10 days | Nausea, diarrhea, rash, allergic reactions | Broad-spectrum, generally well-tolerated. Penicillin V is narrower spectrum. |
| Nitroimidazoles | Metronidazole (often with Amoxicillin) | 500mg, 3x/day for 7-10 days | Nausea, metallic taste, dark urine, avoid alcohol | Effective against anaerobic bacteria; often combined with Amoxicillin. |
| Lincosamides | Clindamycin | 150-300mg, 4x/day for 7-10 days | Diarrhea (risk of C. difficile), nausea, rash | Alternative for penicillin-allergic patients; strong against anaerobes. |
| Macrolides | Azithromycin | Z-Pak (e.g., 500mg on day 1, then 250mg for 4 days) | Nausea, diarrhea, abdominal pain, heart rhythm changes | Alternative for penicillin-allergic patients; shorter course. |
| Cephalosporins (2nd Gen) | Cephalexin (Keflex), Cefaclor | 250-500mg, 4x/day for 7-10 days | Nausea, diarrhea, rash, allergic reactions | Broad-spectrum, sometimes used if penicillin allergy is mild. |
Pro Tip: Always take the full course of antibiotics as prescribed, even if your symptoms improve quickly. Stopping early can lead to antibiotic resistance and a recurrence of the infection.
``
Treatment Options for Tooth Infections (Beyond Antibiotics)
While antibiotics can alleviate symptoms and halt the spread of infection, they are never a cure for a tooth abscess. The source of the infection must be removed or treated. Here are the definitive treatment options:
1. Incision and Drainage (I&D)
- What it is: The dentist makes a small cut (incision) in the swollen gum tissue or skin to allow the pus to drain out of the abscess. A small rubber drain may be placed to keep the incision open and facilitate continued drainage.
- Pros: Provides immediate relief from pressure and pain, reduces swelling, and helps clear the infection. Can sometimes be performed as an emergency procedure.
- Cons: Does not address the underlying cause (e.g., deep decay or cracked tooth). Requires follow-up definitive treatment.
- Cost: Often part of an emergency visit, typically $75 - $250 in addition to the exam/X-ray.
2. Root Canal Therapy (RCT)
- What it is: This procedure removes the infected pulp from inside the tooth. The internal chambers are then cleaned, shaped, and filled with a biocompatible material, and the tooth is sealed, usually with a crown, to protect it from future infection and fracture.
- Pros: Saves the natural tooth, preserves chewing function, and prevents the need for extraction. Highly effective for periapical abscesses.
- Cons: Can be a multi-appointment procedure. The tooth will need a crown afterward, adding to the cost. Not suitable if the tooth is too damaged to be restored.
- Cost: $700 - $1,300 for an anterior (front) tooth, $1,000 - $2,000+ for a posterior (back) molar. A crown adds another $800 - $2,500.
3. Tooth Extraction
- What it is: If the tooth is severely damaged, cannot be saved with a root canal, or if the infection is too extensive, extraction (removal) of the tooth may be the only viable option.
- Pros: Completely removes the source of the infection. Can be a quick, definitive solution for unsalvageable teeth.
- Cons: Results in a missing tooth, which can affect chewing, speech, and the alignment of surrounding teeth. May require a prosthetic replacement (implant, bridge, partial denture), adding significant future costs.
- Cost: $150 - $450 for a simple extraction, $300 - $600+ for a surgical extraction (e.g., impacted molar, very fractured tooth).
Table 2: Comparison of Definitive Treatment Options
| Treatment Option | Primary Goal | Suitability for Type of Abscess | Pros | Cons | Typical Cost Range (US) |
|---|---|---|---|---|---|
| Incision & Drainage | Relieve pressure, remove pus | Periapical & Periodontal | Immediate pain relief, reduces swelling | Temporary, doesn't address root cause, requires follow-up | $75 - $250 (emergency fee) |
| Root Canal Therapy | Save the tooth, remove infection | Periapical (pulp infection) | Preserves natural tooth, maintains function | Multi-appointment, needs crown, higher initial cost | $700 - $2,000+ (plus crown) |
| Tooth Extraction | Complete removal of infected tooth | Both (if tooth unsalvageable) | Quick, definitive removal of infection source | Permanent tooth loss, may require prosthetic replacement, jawbone changes | $150 - $600+ (simple to surgical) |
Step-by-Step Process: From Diagnosis to Treatment
Understanding what to expect when you visit the dentist for a tooth infection can ease anxiety and ensure you follow the necessary steps for effective treatment.
-
Initial Examination and Diagnosis:
- Patient History: Your dentist will ask about your symptoms, when they started, their severity, and any relevant medical conditions or allergies.
- Visual Inspection: The dentist will examine your mouth, looking for swelling, redness, a visible fistula, or signs of a broken tooth or cracked tooth.
- Palpation: Gently pressing on your gums and jaw to locate the source of pain and swelling.
- Percussion Test: Tapping lightly on your teeth to identify the infected one, as infected teeth are often sensitive to percussion.
- Thermal Testing: Applying hot or cold stimuli to gauge pulp vitality and sensitivity response.
- X-rays: Crucial for identifying the extent of decay, the presence of an abscess at the root tip, bone loss, or deep cracks not visible to the naked eye. Digital X-rays are typically used.
- Pulp Vitality Test: An electric pulp tester may be used to determine if the tooth's nerve is alive or necrotic (dead).
-
Antibiotic Prescription (If Indicated):
- Based on the diagnosis, if systemic symptoms are present or the infection is spreading, your dentist will prescribe a suitable antibiotic (e.g., Amoxicillin, Clindamycin).
- You will receive instructions on dosage and duration. It’s critical to start the antibiotics immediately and complete the full course.
-
Infection Control (First Steps):
- If there's significant swelling and pus, the dentist may perform an incision and drainage (I&D) to release the pressure and drain the infection. This provides immediate symptomatic relief.
- Sometimes, if the tooth is severely decayed, the dentist might drill into the tooth to create an opening for drainage.
-
Definitive Dental Treatment:
- Once the acute infection is controlled (often within a few days of starting antibiotics and/or drainage), the definitive treatment will be performed. This could be:
- Root Canal Therapy: If the tooth is savable, the infected pulp is removed, and the tooth is sealed and eventually crowned.
- Tooth Extraction: If the tooth is beyond repair, it will be removed.
- Once the acute infection is controlled (often within a few days of starting antibiotics and/or drainage), the definitive treatment will be performed. This could be:
-
Follow-up Care:
- After definitive treatment, you'll receive post-operative instructions for pain management, diet, and oral hygiene.
- A follow-up appointment will typically be scheduled to monitor healing and, if applicable, to place a permanent crown after a root canal.
``
Cost and Insurance for Tooth Infection Treatment
Understanding the financial aspects of treating a tooth infection is crucial. Costs can vary significantly based on the complexity of the case, geographic location, type of dental office, and your insurance coverage.
Average US Cost Ranges (Without Insurance):
- Dental Exam & X-rays:
- Emergency Exam: $50 - $150
- Full Mouth X-rays: $100 - $250
- Periapical X-ray (specific tooth): $25 - $50
- Antibiotics:
- Generic Amoxicillin, Metronidazole, etc.: $10 - $100 (depending on pharmacy and dosage)
- Brand-name or specialized antibiotics: $100 - $300+
- Incision and Drainage (I&D): $75 - $250 (often billed as part of an emergency visit)
- Root Canal Therapy:
- Anterior (front) tooth: $700 - $1,300
- Premolar: $800 - $1,600
- Molar (back tooth, most complex): $1,000 - $2,000+
- Note: This does not include the cost of a dental crown, which is almost always necessary after a root canal.
- Dental Crown:
- Porcelain-fused-to-metal (PFM): $800 - $1,500
- All-porcelain/ceramic: $1,000 - $2,500
- Gold: $900 - $2,000+
- Tooth Extraction:
- Simple extraction: $150 - $450
- Surgical extraction (e.g., impacted or fractured tooth): $300 - $600+
Insurance Coverage:
Most dental insurance plans in the US cover a portion of the costs associated with treating tooth infections.
- Diagnostic (Exams, X-rays): Typically covered at 80-100%.
- Basic Procedures (Fillings, Extractions, I&D): Usually covered at 50-80%.
- Major Procedures (Root Canals, Crowns): Often covered at 30-50%.
- Antibiotics: Usually covered by medical insurance (prescription drug plan) rather than dental insurance. Your co-pay could be as low as $5-$10 for generics.
- Deductibles and Annual Maximums: Be aware of your plan's deductible (the amount you pay before insurance starts covering) and annual maximum (the total amount your insurance will pay in a year, typically $1,000 - $2,000). Once you hit your maximum, you'll pay out-of-pocket for the rest of the year.
- Waiting Periods: Some plans have waiting periods for major procedures (e.g., 6-12 months) before they will cover root canals or crowns.
Pro Tip: Always contact your dental insurance provider beforehand to understand your specific coverage, deductibles, co-pays, and annual maximums. Ask your dental office for a pre-treatment estimate to avoid financial surprises.
Recovery and Aftercare
Proper aftercare is crucial for successful healing and to prevent complications after treating a tooth infection, whether you received antibiotics, a root canal, or an extraction.
After Antibiotic Treatment:
- Complete the Course: Finish all prescribed antibiotics, even if symptoms improve. Stopping early can lead to recurrence and antibiotic resistance.
- Monitor Symptoms: Continue to watch for any signs of worsening infection (increased pain, swelling, fever). If they return, contact your dentist immediately.
- Follow Up: Ensure you attend your follow-up appointment for definitive dental treatment.
After Incision and Drainage (I&D):
- Pain Management: Over-the-counter pain relievers (ibuprofen, acetaminophen) are usually sufficient. Your dentist may prescribe stronger pain medication if needed.
- Saltwater Rinses: Gently rinse your mouth with warm salt water several times a day to promote healing and keep the area clean.
- Soft Diet: Stick to soft foods for a few days to avoid irritating the area.
- Monitor for Bleeding/Swelling: Minor bleeding is normal. Contact your dentist if bleeding is heavy or swelling increases.
After Root Canal Therapy:
- Pain Management: Mild to moderate pain and sensitivity are common for a few days. Over-the-counter pain relievers usually suffice.
- Avoid Chewing on the Tooth: Until a permanent crown is placed, the tooth is vulnerable to fracture. Avoid biting or chewing on the treated tooth.
- Maintain Oral Hygiene: Continue brushing and flossing normally, but be gentle around the treated tooth.
- Get Your Crown: The final and crucial step is placing a permanent crown, usually 1-3 weeks after the root canal. This protects the weakened tooth from fracturing.
After Tooth Extraction:
- Bleeding Control: Bite firmly on the gauze pad provided for 30-45 minutes. Change gauze as needed.
- Pain Management: Use prescribed pain medication or over-the-counter options as directed.
- Swelling Reduction: Apply an ice pack to the outside of your cheek for 20 minutes on, 20 minutes off, for the first 24 hours.
- Avoid "Dry Socket": For at least 24-48 hours, avoid spitting, rinsing vigorously, using straws, smoking, or consuming alcohol, as these can dislodge the blood clot and lead to a painful "dry socket."
- Soft Diet: Eat soft foods and chew on the opposite side of your mouth for a few days.
- Oral Hygiene: Gently brush other teeth but avoid the extraction site for the first 24 hours. After 24 hours, gentle saltwater rinses can help.
- Rest: Get plenty of rest to aid healing.
ADA Guidelines: The American Dental Association (ADA) emphasizes the importance of following your dentist's post-operative instructions meticulously to ensure proper healing and prevent complications. They also advocate for judicious use of antibiotics to combat antibiotic resistance, stressing that they are an adjunct to, not a replacement for, definitive dental treatment.
Prevention of Tooth Infections
The best way to deal with a tooth infection is to prevent it from happening in the first place. Many dental infections stem from preventable issues like untreated decay or trauma to a broken tooth or cracked tooth.
-
Maintain Excellent Oral Hygiene:
- Brush Twice Daily: Brush your teeth for two minutes, twice a day, using fluoride toothpaste.
- Floss Daily: Floss at least once a day to remove food particles and plaque from between teeth and under the gum line, where brushes can't reach.
- Use Mouthwash: An antimicrobial mouthwash can help reduce bacteria in your mouth.
-
Regular Dental Check-ups and Cleanings:
- Visit your dentist for professional cleanings and check-ups every six months (or as recommended by your dentist).
- Regular exams allow your dentist to identify and treat cavities early, before they become deep enough to infect the pulp. They can also spot early signs of gum disease or a cracked tooth that might lead to infection.
-
Prompt Treatment of Dental Issues:
- Don't ignore tooth pain or sensitivity. What might seem like a minor issue could be a developing cavity or crack.
- If you notice a broken tooth or suspect a cracked tooth, see your dentist immediately. Even a small chip can be an entry point for bacteria.
- Address gum disease early. If diagnosed with gingivitis or periodontitis, follow your dentist's treatment plan diligently.
-
Protect Your Teeth:
- Mouthguards: If you play contact sports, wear a custom-fitted mouthguard to protect your teeth from trauma that could lead to a broken tooth.
- Nightguards: If you grind or clench your teeth (bruxism), a nightguard can protect your teeth from excessive wear and potential cracks.
- Avoid Hard Foods: Be cautious with extremely hard foods like ice, hard candies, or unpopped popcorn kernels, which can cause chips or cracks.
-
Healthy Diet:
- Limit sugary foods and drinks, which feed the bacteria that cause tooth decay.
- Eat a balanced diet rich in fruits, vegetables, and whole grains to support overall health, including oral health.
Risks and Complications of Untreated Tooth Infections
Ignoring a tooth infection or failing to receive definitive treatment can lead to severe, potentially life-threatening complications. The infection does not simply "go away"; it will likely spread.
-
Spread of Infection to Other Areas:
- Cellulitis: The infection can spread into the soft tissues of the face and neck, causing widespread swelling and redness. This is a serious condition requiring immediate medical attention.
- Ludwig's Angina: A rapidly spreading, severe infection of the floor of the mouth and neck. It can obstruct the airway, making breathing difficult, and is a medical emergency that can be fatal.
- Osteomyelitis: Infection of the jawbone itself, which can be chronic and difficult to treat.
- Cavernous Sinus Thrombosis: A rare but extremely dangerous complication where the infection spreads to a blood clot in the cavernous sinus (a large vein at the base of the brain). This can lead to vision loss, stroke, or even death.
- Brain Abscess: In very rare cases, bacteria from an oral infection can travel to the brain, forming a life-threatening abscess.
-
Sepsis (Blood Poisoning):
- If the infection enters the bloodstream, it can spread throughout the body, triggering a widespread inflammatory response known as sepsis. Sepsis is a medical emergency that can lead to organ damage, shock, and death. Symptoms include fever, chills, rapid heart rate, confusion, and difficulty breathing.
-
Tooth Loss:
- Left untreated, the infection can destroy the bone supporting the tooth, leading to its loosening and eventual loss.
-
Antibiotic Resistance:
- Misuse or overuse of antibiotics, or not completing the full course, contributes to the development of antibiotic-resistant bacteria, making future infections harder to treat.
Pro Tip: Never underestimate a tooth infection. If you have symptoms, especially swelling, fever, or difficulty swallowing/breathing, seek immediate medical attention.
Children / Pediatric Considerations
Tooth infections in children are a serious concern and require prompt attention. While children's teeth (primary or "baby" teeth) are temporary, an infection can have significant implications for their developing permanent teeth and overall health.
Why Children Are Susceptible:
- Diet: Children often consume more sugary foods and drinks, increasing their risk of cavities.
- Oral Hygiene: Developing good brushing and flossing habits can be challenging for young children, leading to inadequate plaque removal.
- Trauma: Children are more prone to falls and accidents, which can result in a broken tooth or cracked tooth, providing entry points for bacteria.
- Rapid Progression: Infections can sometimes progress more quickly in children due to their smaller pulp chambers and more porous bone.
Special Considerations for Children:
- Impact on Permanent Teeth: An infection in a primary tooth can spread to the developing permanent tooth underneath, potentially causing developmental defects (e.g., discoloration, enamel hypoplasia) or even hindering its eruption.
- Antibiotic Choices: Pediatric dentists will select antibiotics appropriate for a child's age, weight, and any allergies. Dosage is carefully calculated.
- Treatment Approach:
- Pulp Therapy (Pulpotomy/Pulpectomy): For primary teeth, similar to a root canal, the infected pulp may be partially or completely removed, and the tooth is filled and often crowned (usually with a stainless steel crown) to maintain its space until the permanent tooth is ready to erupt.
- Extraction: If the primary tooth is too damaged or the infection too severe, extraction may be necessary. A space maintainer might be used to prevent adjacent teeth from shifting and blocking the permanent tooth's eruption path.
- Early Intervention is Key: Parents should be vigilant for any signs of tooth pain, swelling, or unusual discoloration in their child's mouth. Early intervention can prevent serious complications and ensure the healthy development of permanent teeth.
Pro Tip for Parents: Teach good oral hygiene habits early, limit sugary snacks, and schedule regular pediatric dental check-ups. If your child complains of tooth pain or you notice swelling, see a pediatric dentist immediately.
Cost Breakdown (Detailed)
To provide a clearer picture, here's a detailed breakdown of potential costs for treating a tooth infection in the US, considering various scenarios.
Detailed Cost Breakdown for Tooth Infection Treatment (US Dollars)
| Service/Procedure | Low Range (no insurance) | Mid Range (no insurance) | High Range (no insurance) | With Insurance (typical patient portion) | Payment Plans/Tips |
|---|---|---|---|---|---|
| Emergency Dental Exam | $50 | $100 | $150 | $0 - $50 (if diagnostic covered) | Ask for a cash discount. |
| Periapical X-ray | $25 | $35 | $50 | $0 - $15 | Often included in emergency visit fee. |
| Prescription Antibiotics | $10 | $50 | $100+ | $5 - $25 (medical insurance co-pay) | Ask for generics. Use discount cards (GoodRx). |
| Incision & Drainage (I&D) | $75 | $150 | $250 | $20 - $75 | Essential for acute swelling relief. |
| Root Canal (Anterior Tooth) | $700 | $1,000 | $1,300 | $300 - $650 | Consider dental schools for lower costs. |
| Root Canal (Premolar) | $800 | $1,200 | $1,600 | $400 - $800 | Many offices offer payment plans. |
| Root Canal (Molar) | $1,000 | $1,500 | $2,000+ | $500 - $1,200 | Maximize annual dental benefits. |
| Dental Crown (after RCT) | $800 | $1,500 | $2,500 | $400 - $1,200 | Essential for tooth longevity; compare materials. |
| Simple Tooth Extraction | $150 | $250 | $450 | $50 - $150 | Community clinics offer reduced rates. |
| Surgical Tooth Extraction | $300 | $450 | $600+ | $100 - $300 | |
| Post-Op Pain Medication | $10 | $30 | $50+ | $5 - $20 (medical insurance co-pay) | Generics are much cheaper. |
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental offices offer interest-free payment plans, allowing you to pay for treatment over several months.
- Third-Party Financing (e.g., CareCredit): These services offer special healthcare financing options, often with low or no interest for a set period.
- Dental Discount Plans: These are not insurance but offer reduced fees for dental services from participating providers for an annual membership fee.
- Dental Schools: University dental schools often provide high-quality care at a lower cost, as treatment is performed by students under the supervision of experienced faculty.
- Community Dental Clinics: Many communities have clinics that offer reduced-cost dental care, sometimes on a sliding scale based on income.
Cost-Saving Tips:
- Preventive Care: The most significant cost-saving tip is prevention. Regular check-ups and good hygiene prevent expensive treatments.
- Get Estimates: Always ask your dentist for a detailed treatment plan and cost estimate before starting any major procedure.
- Compare Prices: If you have time and the infection is not an emergency, call different dental offices for price comparisons.
- Negotiate Cash Discounts: Some offices offer discounts for patients who pay in full with cash.
- Utilize HSAs/FSAs: If you have a Health Savings Account (HSA) or Flexible Spending Account (FSA), these funds can be used for dental expenses tax-free.
Frequently Asked Questions
Can a tooth infection go away on its own?
No, a tooth infection will not go away on its own. While antibiotics can temporarily manage symptoms and prevent spread, they do not remove the source of the infection. Without definitive dental treatment like a root canal or extraction, the infection will persist and can lead to severe complications, eventually destroying the tooth and potentially spreading to other parts of your body.
How long does it take for antibiotics to work for a tooth infection?
You may start to feel some relief from pain and swelling within 1 to 3 days of starting antibiotics. However, it's crucial to complete the entire course of medication, typically 7 to 10 days, to ensure all bacteria are eliminated and to prevent recurrence and antibiotic resistance. Always follow your dentist's specific instructions.
What happens if I don't take antibiotics for a tooth infection?
If antibiotics are prescribed for a spreading infection and you don't take them, the infection can worsen rapidly. This could lead to increased pain, more significant facial swelling, fever, and potentially life-threatening conditions like cellulitis, Ludwig's angina, or sepsis. Even without systemic symptoms, the infection will continue to damage your tooth and jawbone.
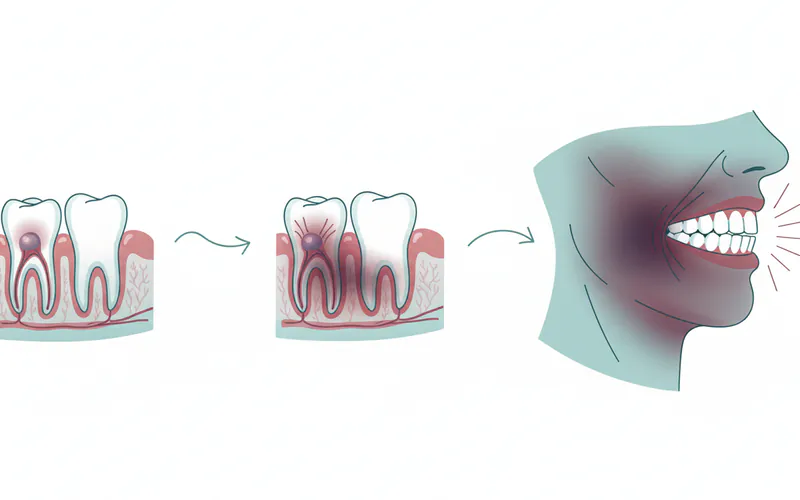
What are the side effects of antibiotics for a tooth infection?
Common side effects include nausea, diarrhea, stomach upset, and skin rash. Some antibiotics can cause a metallic taste in the mouth or increase sensitivity to sunlight. More serious, but rare, side effects can include severe allergic reactions (hives, difficulty breathing), or a severe form of diarrhea called C. difficile infection, especially with antibiotics like clindamycin.
How much do antibiotics for a tooth infection cost?
The cost of antibiotics varies. Generic antibiotics like Amoxicillin or Metronidazole typically range from $10 to $100 without insurance, often less with a prescription drug discount card. With medical insurance, your co-pay might be as low as $5-$25. Brand-name or specialized antibiotics can be more expensive.
Can I get antibiotics for a tooth infection without seeing a dentist?
In most cases, no. A dentist or physician needs to diagnose the infection to determine if antibiotics are appropriate and which type to prescribe. Self-medicating with old antibiotics or trying to get a prescription without an examination is risky and can lead to incorrect treatment, masking of symptoms, or serious complications.
What if antibiotics don't work for my tooth infection?
If your symptoms don't improve or worsen after a few days on antibiotics, contact your dentist immediately. This could mean the wrong antibiotic was prescribed, the infection is resistant, or it's a more severe infection requiring immediate drainage or a different approach. Do not stop taking the medication without consulting your dentist.
Is a tooth extraction always necessary for a tooth infection?
No, extraction is not always necessary. Many tooth infections, especially periapical abscesses, can be successfully treated with root canal therapy, which saves the natural tooth. Extraction is usually recommended if the tooth is too damaged to be restored, if a root canal has failed, or if the infection is too severe to treat conservatively.
How long does a tooth infection last with antibiotics?
Antibiotics typically clear the acute bacterial infection within 7-10 days, but the infection source (e.g., dead pulp) remains. Without definitive treatment, the infection will likely return. The goal of antibiotics is to control the infection long enough for a root canal or extraction to be performed.
Can a cracked tooth cause an infection?
Yes, absolutely. A cracked tooth, especially if the crack extends into the pulp chamber or deep into the dentin, creates an open pathway for oral bacteria to enter the tooth's sensitive inner tissues. Over time, these bacteria can lead to inflammation, infection, and abscess formation.
When to See a Dentist
Recognizing when to seek dental care is critical for your health. Delaying treatment for a tooth infection can have severe consequences.
Immediate Emergency Care (See a dentist or ER right away) if you experience:
- Severe, Unbearable Pain: If the pain is constant, throbbing, and not relieved by over-the-counter pain medication.
- Significant Facial Swelling: Swelling in your cheek, jaw, or neck that is rapidly increasing.
- Difficulty Breathing or Swallowing: This is a red flag indicating the infection is spreading to vital areas and can be life-threatening (e.g., Ludwig's angina).
- Fever and Chills: Especially if accompanied by widespread body aches, indicating a systemic infection.
- Rapidly Spreading Redness: On your face or neck, possibly with tenderness to touch.
- Eye Swelling or Vision Changes: These are rare but extremely serious signs of infection spreading towards the brain.
Urgent Care (See a dentist within 24-48 hours) if you experience:
- Persistent Toothache: Any toothache that lasts more than a day or two, even if mild.
- Sensitivity to Hot, Cold, or Pressure: If it lingers after the stimulus is removed.
- A Pimple-like Bump (Fistula) on Your Gums: This indicates chronic drainage but still signifies an active infection needing treatment.
- Swollen or Tender Gums Around a Tooth: Even without severe pain, this could be a periodontal abscess.
- Bad Taste in Your Mouth or Persistent Bad Breath: Especially if accompanied by other symptoms.
- A Recently Broken Tooth or Cracked Tooth: Even if not painful initially, it needs immediate assessment to prevent infection.
Routine Care (Schedule an appointment soon) for:
- Any tooth sensitivity that is mild and comes and goes.
- Minor chips or cracks that are not causing pain or discomfort.
- Routine check-ups and cleanings.
Your oral health is intrinsically linked to your overall health. Never ignore the signs of a tooth infection. Prompt diagnosis and treatment are essential for resolving the infection, preserving your tooth, and preventing serious, potentially life-threatening complications. If you suspect you have a tooth infection, contact your dentist at SmilePedia.net today.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Is an Abscess
Imagine a throbbing pain deep within your jaw, a persistent ache that keeps you awake at night and makes even the softest foods unbearable. This isn't just a bad toothache; it could be a sign of something much more serious: a dental abscess. Affecting millions of Americans annually, an abscess is an
February 22, 2026
Cracked Tooth Syndrome: Complete Guide
Cracked Tooth Syndrome: Complete Guide Category: Dental Conditions & Diseases
February 22, 2026
Dentinogenesis Imperfecta: Complete Guide
Imagine a world where your teeth, fundamental to chewing, speaking, and even smiling confidently, are inherently fragile, discolored, and prone to rapid wear from the moment they emerge. For individuals affected by dentinogenesis imperfecta (DI), this is a reality. While relatively rare, affecti
February 22, 2026
Stage 1 Early Cavity: Complete Guide
Did you know that dental cavities are one of the most common chronic diseases globally, affecting both children and adults? In the United States, over 90% of adults have had a cavity, and a significant portion of these begin as a stage 1 early cavity. Often invisible and painless in its nasc
February 22, 2026