Gum Abscess: Complete Guide
Key Takeaways
- A throbbing pain in your gums, accompanied by swelling and tenderness, can be an alarming experience. While often mistaken for a common toothache, these symptoms could signal a more serious underlying issue: a gum abscess. This localized infection, characterized by a pocket of pus forming in the
A throbbing pain in your gums, accompanied by swelling and tenderness, can be an alarming experience. While often mistaken for a common toothache, these symptoms could signal a more serious underlying issue: a gum abscess. This localized infection, characterized by a pocket of pus forming in the gum tissue, is not just a source of discomfort; it's a critical warning sign that demands immediate dental attention. Neglecting a gum abscess can lead to severe health complications, impacting not only your oral health but potentially your overall systemic well-being.
At SmilePedia.net, we understand the urgency and concern that comes with dental pain. This comprehensive guide will equip you with everything you need to know about gum abscesses, from understanding their causes and recognizing the signs, to exploring effective treatment options and critical prevention strategies. We'll delve into the different types of gum abscesses, what to expect during treatment, associated costs, recovery tips, and crucial advice for children and when to seek emergency care. Our goal is to empower you with the knowledge to protect your smile and ensure optimal dental health.
Key Takeaways:
- A gum abscess is a localized bacterial infection forming a pocket of pus in the gum tissue, often linked to gum disease or trauma.
- Common symptoms include throbbing pain, swelling, redness, tenderness, and sometimes pus discharge or fever.
- Prompt dental treatment is crucial; untreated abscesses can spread infection, leading to serious health complications like sepsis or bone loss.
- Treatment typically involves drainage of the pus, deep cleaning (scaling and root planing), and often antibiotics.
- Costs for treatment vary widely based on severity and procedures, ranging from $150 to over $2,500 without insurance, but most dental insurance plans cover a significant portion.
- Pro Tip: For temporary toothache relief, rinse with warm salt water and use over-the-counter pain relievers, but always see a dentist quickly.
- Prevention hinges on excellent oral hygiene, regular dental check-ups, and addressing gum disease early.
What It Is / Overview
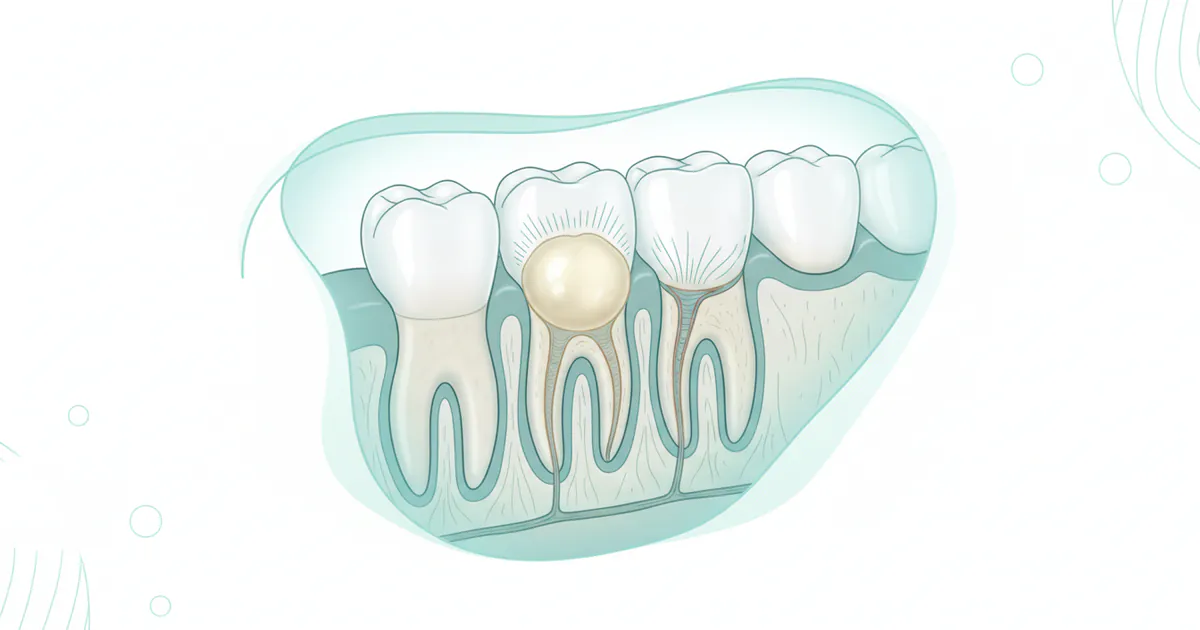
A gum abscess, medically known as a periodontal abscess, is an acute inflammatory lesion characterized by a localized accumulation of pus within the gum tissues surrounding a tooth. This pus-filled pocket develops as the body's immune system attempts to fight off a bacterial infection. Unlike a periapical abscess, which forms at the tip of the tooth root inside the bone, a gum abscess originates in the supporting structures of the tooth—the gums (gingiva), periodontal ligament, and alveolar bone.

The development of a gum abscess is a clear indication that bacteria have infiltrated the gum tissue, often through a periodontal pocket (a space that forms between the tooth and gum in individuals with gum disease) or due to trauma. The infection causes inflammation, leading to the formation of pus, which is a thick, yellowish fluid composed of dead white blood cells, bacteria, and tissue debris. As the pus accumulates, it exerts pressure on the surrounding tissues, resulting in the characteristic pain and swelling. If left untreated, this pressure can increase, and the infection can spread, potentially causing significant damage to the bone supporting the tooth, or even extending to other parts of the body. Understanding a gum abscess is the first step towards seeking timely and effective toothache relief.
Types / Variations
While the term "gum abscess" often refers broadly to any pus-filled lesion in the gums, dental professionals typically categorize them based on their location and primary cause. This distinction is vital for accurate diagnosis and targeted treatment. The three main types are:
Gingival Abscess
A gingival abscess is the least common and generally the least severe type. It is confined exclusively to the gum tissue, specifically the marginal gingiva (the gum edge) or the interdental papilla (the gum between teeth).
- Cause: Typically caused by trauma, such as aggressive brushing, or the impaction of a foreign body like a popcorn hull, a toothbrush bristle, or a seed, which gets lodged in the gum tissue and introduces bacteria. It usually occurs in otherwise healthy gum tissue.
- Characteristics: Presents as a localized, painful, rapidly developing swelling, often red and shiny.
- Severity: Generally doesn't involve the deeper periodontal structures or bone loss.
Periodontal Abscess
This is the most common type of gum abscess and is directly associated with pre-existing periodontal disease (gum disease).
- Cause: Occurs when bacteria from a deep periodontal pocket—a space formed between the tooth root and the gum due to chronic gum disease—get trapped. This can happen if the opening of the pocket becomes blocked, preventing drainage, or after certain dental procedures like scaling and root planing that can inadvertently push bacteria deeper into the pocket.
- Characteristics: Often characterized by a dull, throbbing pain, sensitivity to pressure, mobility of the affected tooth, and a visible swelling on the side of the gum that may eventually form a "pimple-like" lesion (fistula) through which pus drains. The tooth itself may feel elevated.
- Severity: More serious than a gingival abscess, as it indicates a progression of gum disease and can lead to significant bone loss around the affected tooth if not treated promptly.
Pericoronal Abscess (Pericoronitis)
While not strictly a "gum abscess" in the same vein as gingival or periodontal, a pericoronal abscess is a common gum infection that warrants inclusion due to its frequency and similar symptoms.
- Cause: Occurs when a wisdom tooth (or any other tooth) is partially erupted, leaving a flap of gum tissue (operculum) covering part of the crown. Food debris and bacteria can become trapped under this flap, leading to inflammation and infection. It's particularly common with lower wisdom teeth.
- Characteristics: Pain, swelling, redness, and tenderness in the gum tissue around the partially erupted tooth. There may be difficulty opening the mouth (trismus) and a foul taste if pus is draining. Systemic symptoms like fever and swollen lymph nodes are common.
- Severity: Can range from mild inflammation to a severe infection that spreads to the jaw and throat. Recurrence is common if the underlying cause (the partially erupted tooth) is not addressed.
Understanding these distinctions helps dental professionals tailor the most effective treatment, which might range from simple drainage for a gingival abscess to complex periodontal therapy or even tooth extraction for a severe periodontal or pericoronal abscess.
Causes / Why It Happens
The formation of a gum abscess is fundamentally a consequence of bacterial invasion and the body's immune response. Several factors can contribute to the development of these painful infections:
- Untreated Periodontal Disease (Gum Disease): This is the leading cause of periodontal abscesses. When gingivitis (inflammation of the gums) progresses, it turns into periodontitis, leading to the formation of deep pockets between the teeth and gums. These pockets become breeding grounds for bacteria. If the opening of a deep pocket becomes blocked—perhaps by food debris or by the gum tissue swelling—the bacteria can proliferate, and the pus cannot drain, leading to an abscess.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque (a sticky film of bacteria) and tartar (hardened plaque) to accumulate on tooth surfaces and beneath the gum line. This significantly increases the bacterial load in the mouth, exacerbating gum disease and the risk of infection.
- Trauma to the Gums: Physical injury to the gum tissue can create an entry point for bacteria. This can include aggressive brushing, cuts from sharp foods, dental instruments, or even chronic irritation from ill-fitting dental appliances like dentures or braces.
- Impacted Food Particles or Foreign Bodies: Small, sharp food particles (like popcorn kernels, seeds, or fish bones) or even fragments of a toothbrush bristle can become lodged in the gum tissue, particularly in individuals with gum recession or pockets. These foreign bodies not only introduce bacteria but also irritate the tissue, leading to inflammation and abscess formation (especially in gingival abscesses).
- Incomplete or Inadequate Dental Treatment:
- Scaling and Root Planing: If deep cleaning procedures don't thoroughly remove all calculus and bacteria from a periodontal pocket, or if they inadvertently push debris deeper, an abscess can form.
- Antibiotic Therapy: Sometimes, antibiotics prescribed for gum disease can temporarily suppress bacteria, but if the underlying cause (like a deep pocket) isn't physically cleaned, the infection can flare up again, potentially as an abscess.
- Restorative Dentistry: Overhanging fillings or crowns can trap food and bacteria, irritating the gums and creating an environment ripe for infection.
- Compromised Immune System: Individuals with weakened immune systems are more susceptible to infections, including gum abscesses. This includes people with:
- Diabetes: Poorly controlled diabetes can impair the immune response and blood flow, making individuals more prone to severe gum disease and abscesses.
- HIV/AIDS: Individuals with HIV/AIDS often have compromised immunity, increasing their risk.
- Medications: Certain medications, such as corticosteroids or immunosuppressants, can weaken the immune system.
- Stress: Chronic stress can also negatively impact immune function.
- Smoking: Smoking is a significant risk factor for gum disease, as it reduces blood flow to the gums, impairs immune function, and hinders healing, making smokers more susceptible to abscesses.
- Dental Caries (Cavities): While primarily causing periapical abscesses, deep cavities that extend below the gum line can sometimes lead to gum infections if bacteria spread to the surrounding periodontal tissues.
- Partially Erupted Teeth: As discussed with pericoronal abscesses, a flap of gum tissue over a partially erupted tooth (most commonly wisdom teeth) creates a perfect trap for food and bacteria, leading to inflammation and infection.
Understanding these root causes emphasizes the importance of both meticulous oral hygiene and regular professional dental care in preventing gum abscesses.
Signs and Symptoms
Recognizing the signs and symptoms of a gum abscess early is critical for prompt treatment and preventing further complications. While the intensity can vary, many symptoms are quite distinct:
- Persistent, Throbbing Pain: This is often the most prominent symptom. The pain is usually localized to the affected gum area but can radiate to the ear, jaw, or neck. It's often described as a dull ache that intensifies when chewing or applying pressure, making it a severe form of toothache relief challenge.
- Swelling of the Gums: The affected gum tissue will appear swollen, often red and shiny. The swelling may be localized to a specific spot, sometimes resembling a "pimple" on the gum (a fistula) where pus might be attempting to drain. In more severe cases, the swelling can extend to the face or neck.
- Tenderness to Touch: The swollen area will be very sensitive and painful when touched or probed.
- Pus Discharge: You might notice a foul taste in your mouth if the abscess is draining pus. This discharge can sometimes be visible as a yellowish fluid emanating from the gum near the tooth. This also contributes to bad breath (halitosis).
- Sensitivity to Hot and Cold: The affected tooth or surrounding gums may become sensitive to temperature changes, similar to what you'd experience with a cavity.
- Pain When Chewing or Biting: Pressure on the affected tooth or gum during eating can exacerbate the pain, making it difficult to chew comfortably.
- Loose Tooth: The infection and inflammation around the tooth can compromise its supporting structures, making the tooth feel loose or mobile. This is a particularly concerning sign as it indicates significant damage to the periodontal ligament and bone.
- Elevated Tooth: Sometimes, the pressure from the pus can push the tooth slightly out of its socket, making it feel "higher" than the adjacent teeth when you bite down.
- Bad Breath (Halitosis): The presence of bacteria and pus contributes to persistent bad breath that cannot be resolved by brushing alone.
- Systemic Symptoms (in severe cases): If the infection is widespread or severe, it can lead to:
- Fever: An elevated body temperature is a sign the infection is impacting your entire system.
- Swollen Lymph Nodes: Lymph nodes in the neck and under the jaw may become tender and enlarged as they work to fight the infection.
- Malaise/Fatigue: A general feeling of being unwell or tired.
- Difficulty Swallowing or Opening Mouth: Especially common with pericoronal abscesses or if the infection has spread significantly.
If you experience any combination of these symptoms, especially severe pain and swelling, it is crucial to seek immediate dental attention. Ignoring these signs can lead to more serious health complications.
``
Treatment Options
Treating a gum abscess is a multi-step process focused on eliminating the infection, relieving pain, and addressing the underlying cause to prevent recurrence. The specific approach will depend on the type and severity of the abscess, as well as the patient's overall health.
1. Initial Emergency Treatment (Pain and Infection Management)
- Incision and Drainage (I&D): This is often the first and most critical step. The dentist will numb the area and make a small incision in the swollen gum to allow the pus to drain. This immediately relieves pressure and pain. The area may then be gently rinsed with a saline solution or antiseptic.
- Pros: Rapid pain relief, reduces swelling, removes the source of infection.
- Cons: Temporary discomfort during the procedure, may require follow-up.
- Antibiotics: If the infection has spread beyond the immediate area, if there are systemic symptoms (fever, swollen lymph nodes), or if the patient has a compromised immune system, antibiotics will be prescribed. Common choices include amoxicillin, clindamycin, or metronidazole.
- Pros: Kills bacteria, prevents spread of infection.
- Cons: Potential side effects (nausea, diarrhea), can contribute to antibiotic resistance if overused, does not remove the physical source of infection (pus) and so drainage is still usually necessary.
- Pain Management: Over-the-counter pain relievers like ibuprofen or acetaminophen are typically recommended for toothache relief. In cases of severe pain, a dentist may prescribe stronger pain medication for a short period.
- Pros: Alleviates discomfort.
- Cons: Does not treat the underlying infection.
2. Definitive Treatment (Addressing the Underlying Cause)
Once the acute infection is under control, the dentist will address the root cause of the abscess to prevent recurrence.
- Scaling and Root Planing (Deep Cleaning): For periodontal abscesses, this is often the next step. It involves meticulously cleaning the tooth root surfaces below the gum line to remove plaque, tartar, and bacterial toxins from the periodontal pockets. This helps the gums reattach to the tooth and reduces pocket depth.
- Pros: Treats the underlying gum disease, prevents future abscesses, improves overall gum health.
- Cons: Can be uncomfortable, may require multiple appointments and local anesthesia.
- Root Canal Treatment (Endodontic Therapy): While primarily for periapical abscesses, if the tooth's pulp (nerve) has become irreversibly infected due to deep decay or trauma, or if a periodontal abscess is associated with a failing root canal, root canal treatment may be necessary. This involves removing the infected pulp, cleaning and shaping the canals, and sealing them.
- Pros: Saves the natural tooth, eliminates infection from within the tooth.
- Cons: Can be costly, requires follow-up crown, may not be suitable if tooth structure is severely compromised.
- Tooth Extraction: If the tooth is severely damaged, has significant bone loss, or if other treatments are not viable, extraction may be the only option. This is often the case with severely compromised teeth due to advanced periodontal disease or in some pericoronal abscesses where the wisdom tooth is problematic.
- Pros: Permanently removes the source of infection, quick resolution for severe cases.
- Cons: Loss of a natural tooth, requires replacement options (implant, bridge) which can be costly and time-consuming.
- Periodontal Surgery: For persistent or complex periodontal pockets that don't respond to scaling and root planing, surgical procedures like flap surgery may be required. This involves lifting the gum tissue to allow for better access to clean the root surfaces and reshape damaged bone.
- Pros: More thorough cleaning, can reduce pocket depths, potentially regenerate lost bone.
- Cons: Invasive, longer recovery time, higher cost.
- Operculectomy or Wisdom Tooth Extraction: For pericoronal abscesses, treatment might involve removing the problematic gum flap (operculectomy) or, more commonly, extracting the partially erupted wisdom tooth to prevent future infections.
- Pros: Eliminates the cause of pericoronitis, permanent solution.
- Cons: Surgical procedure with associated risks (pain, swelling, dry socket).
Pro Tip: Never attempt to drain a gum abscess at home. This can push the infection deeper, introduce more bacteria, and lead to serious complications. Always seek professional dental care.
Step-by-Step Process: What to Expect During Treatment
Understanding the typical steps involved in treating a gum abscess can help alleviate anxiety and prepare you for your dental visit.
1. Diagnosis and Initial Assessment
- Patient History: Your dentist will start by asking about your symptoms, when they began, your medical history, and any relevant dental history.
- Clinical Examination: The dentist will visually inspect the affected area, check for swelling, redness, and tenderness. They will also gently probe the gum pockets around your teeth to measure their depth and assess for pus discharge.
- X-rays: Dental X-rays (usually periapical or panoramic) are essential to assess the bone level around the tooth, identify any bone loss, rule out a periapical abscess, and check for foreign bodies or impacted teeth.
- Vitality Test: In some cases, a vitality test (testing the nerve response of the tooth) may be performed to determine if the tooth itself is also infected.
2. Anesthesia
- Before any invasive procedure, the dentist will administer a local anesthetic to numb the affected area. This ensures you remain comfortable and pain-free during the treatment. You may feel a slight pinch initially, followed by numbness in the gum, tooth, and surrounding tissues.

3. Drainage of the Abscess
- Incision: Using a sterile scalpel or laser, the dentist will make a small incision into the swollen gum tissue at the most prominent point of the abscess. This allows the accumulated pus to escape.
- Irrigation: After drainage, the dentist may gently irrigate the area with an antiseptic solution (like chlorhexidine or saline) to flush out remaining bacteria and debris from the abscess cavity.
- Placement of a Drain (Optional): In some cases, especially for larger abscesses, a small rubber drain may be temporarily placed in the incision site for 24-48 hours. This helps ensure continuous drainage and prevents the abscess from reforming immediately.
4. Cleaning the Area (Addressing the Cause)
- Scaling and Root Planing: If the abscess is periodontal, the dentist or hygienist will perform a deep cleaning. This involves using specialized instruments (scalers and curettes) to meticulously remove plaque, tartar, and bacterial toxins from the tooth root surfaces deep within the periodontal pockets. Ultrasonic devices may also be used to dislodge debris and irrigate the pockets.
- Foreign Body Removal: If a foreign body caused a gingival abscess, it will be carefully removed.
5. Antibiotic Prescription (If Necessary)
- If the infection is widespread, severe, or if you have systemic symptoms or a compromised immune system, your dentist will prescribe a course of oral antibiotics (e.g., amoxicillin, clindamycin). It's crucial to take the full course of antibiotics as prescribed, even if your symptoms improve quickly.
6. Post-Treatment Instructions and Follow-up
- Aftercare Guidance: You will receive detailed instructions on how to care for the treated area, including pain management, oral hygiene practices (gentle brushing, salt water rinses), and dietary recommendations.
- Follow-up Appointment: A follow-up visit, usually within a week to a few weeks, will be scheduled to monitor healing, remove any drain, and reassess the underlying periodontal condition. Further treatment, such as more extensive periodontal therapy, root canal, or extraction, will be planned if needed.
The entire process, from diagnosis to initial drainage, typically takes between 30 minutes to an hour, depending on the complexity. You should experience significant toothache relief shortly after drainage.
``
Cost and Insurance
The cost of treating a gum abscess in the US can vary significantly based on the severity of the infection, the specific procedures required, the location of the dental practice, and whether you have dental insurance. It's important to understand these factors when budgeting for treatment.
Typical Cost Ranges (Without Insurance)
Here's an estimated breakdown of common procedures related to gum abscess treatment:
- Emergency Exam & Diagnosis (including X-rays): $50 - $250
- Incision and Drainage (I&D) of Abscess: $150 - $400
- Prescription Antibiotics: $10 - $60 (cost of medication itself)
- Scaling and Root Planing (per quadrant): $200 - $600 (a full mouth might involve 4 quadrants, totaling $800 - $2,400)
- Tooth Extraction (simple): $150 - $450
- Tooth Extraction (surgical, e.g., impacted wisdom tooth): $300 - $800+
- Root Canal Treatment (anterior tooth): $700 - $1,200
- Root Canal Treatment (molar tooth): $1,000 - $2,500+
- Periodontal Surgery (e.g., flap surgery): $1,000 - $3,000+ (per quadrant)
Total Estimated Cost for a Gum Abscess (without insurance): A basic treatment involving an exam, drainage, and antibiotics could be $210 - $710. If scaling and root planing are needed for a single quadrant, the cost could rise to $410 - $1,310. For more complex cases requiring extraction or root canal therapy, the total cost could range from $500 to over $2,500.
Impact of Dental Insurance
Most dental insurance plans in the US categorize gum abscess treatment as a "basic" or "major" procedure.
- Diagnostic & Preventative: Exams and X-rays are typically covered at a high percentage (e.g., 80-100%).
- Basic Procedures: Incision and drainage, scaling and root planing, and sometimes simple extractions are usually covered at 70-80% after you meet your deductible.
- Major Procedures: Root canal therapy, surgical extractions, and periodontal surgery are generally covered at 50% after your deductible.
- Deductibles: Most plans have an annual deductible (e.g., $50-$100) that you must pay out-of-pocket before your insurance coverage kicks in.
- Annual Maximums: Dental insurance plans also have an annual maximum benefit (e.g., $1,000-$2,000), which is the most your insurance company will pay in a calendar year. For extensive treatments, you might exceed this maximum.
Example Scenario (with insurance): Let's assume a plan with 80% coverage for basic procedures, 50% for major, and a $50 deductible with a $1,500 annual maximum.
- Emergency Exam & X-rays: $150 (covered at 100% after deductible, so you pay $50 deductible, then insurance pays $100. Out-of-pocket: $50)
- Incision and Drainage: $250 (covered at 80%. Insurance pays $200, you pay $50. Out-of-pocket: $50)
- Antibiotics: $30 (you pay full amount as it's often not covered by dental insurance, but by medical insurance with a separate deductible/copay)
- Scaling and Root Planing (one quadrant): $400 (covered at 80%. Insurance pays $320, you pay $80. Out-of-pocket: $80)
Total Out-of-Pocket for this scenario: $50 (deductible) + $50 (I&D) + $30 (antibiotics) + $80 (SRP) = $210. The insurance paid $100 + $200 + $320 = $620, leaving plenty of room under the $1,500 annual maximum.
Regional Cost Variations
Dental costs can vary significantly by region. Major metropolitan areas (e.g., New York, Los Angeles) generally have higher dental fees than rural areas or states with a lower cost of living. For instance, an I&D that costs $200 in the Midwest might be $350 in a coastal city.
Payment Plans and Financing Options
If you don't have insurance or face high out-of-pocket costs, several options can help:
- Dental Payment Plans: Many dental offices offer in-house payment plans, allowing you to pay in installments.
- Third-Party Financing: Services like CareCredit or LendingClub offer specialized healthcare credit cards with low or no-interest payment plans for qualified patients.
- Community Dental Clinics: These often offer services at reduced rates based on income.
- Dental Schools: University dental schools typically provide high-quality care at a lower cost, as procedures are performed by students under the supervision of experienced faculty.
Pro Tip: Always discuss costs and payment options with your dental office before starting treatment. They can provide a detailed estimate and help you understand your insurance benefits.
Recovery and Aftercare
Proper recovery and aftercare are crucial for successful healing after a gum abscess treatment and for preventing recurrence. Your dentist will provide specific instructions, but here are general guidelines:
1. Pain Management
- Over-the-Counter (OTC) Pain Relievers: For most people, ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are effective for managing post-procedure discomfort. Ibuprofen also helps reduce inflammation.
- Prescription Pain Medication: If your pain is severe, your dentist may prescribe a stronger pain reliever for a few days. Take it exactly as directed.
- Cold Compress: Applying a cold compress to the outside of your cheek near the treated area can help reduce swelling and discomfort, especially in the first 24 hours. Use for 15-20 minutes at a time, with 20-minute breaks.
2. Oral Hygiene
- Gentle Brushing: Continue to brush your teeth twice a day, but be very gentle around the treated area. Use a soft-bristled toothbrush.
- Salt Water Rinses: Rinse your mouth with warm salt water (1/2 teaspoon of salt in 8 ounces of warm water) 2-3 times a day, especially after meals. This helps to soothe the tissues, reduce inflammation, and promote healing by keeping the area clean. This is an excellent natural toothache remedy.
- Antiseptic Mouthwash: Your dentist may prescribe an antiseptic mouthwash (e.g., chlorhexidine) for a short period to further reduce bacterial load and aid healing. Use as directed.
- Flossing: Avoid flossing directly around the treated area for a few days, or as advised by your dentist. Resume flossing gently once the area feels less tender.

3. Dietary Adjustments
- Soft Foods: Stick to soft, easy-to-chew foods for the first few days after treatment. Examples include yogurt, soup, mashed potatoes, scrambled eggs, smoothies, and cooked pasta.
- Avoid Irritating Foods: Stay away from hot, spicy, acidic, crunchy, or sticky foods that could irritate the healing gums or dislodge any temporary packing.
- Hydration: Drink plenty of water to stay hydrated.
- Avoid Straws: If you had a tooth extraction as part of the treatment, avoid using straws as the sucking motion can dislodge the blood clot (leading to a dry socket).
4. Lifestyle Adjustments
- Avoid Smoking and Alcohol: Smoking severely impairs healing and increases the risk of complications. Alcohol can also irritate tissues and interact with medications. Avoid both during your recovery period.
- Rest: Get adequate rest to allow your body to heal.
- Elevate Your Head: When sleeping, elevate your head slightly with an extra pillow to help reduce swelling.
5. What to Watch For
Contact your dentist immediately if you experience any of the following:
- Increasing Pain or Swelling: If the pain or swelling worsens instead of improving after a few days.
- Fever: A persistent or recurring fever.
- Difficulty Swallowing or Breathing: These are signs of a spreading infection and require urgent medical attention.
- Pus Discharge: Continued or new pus drainage from the treated area.
- Uncontrolled Bleeding: Although some slight oozing is normal, heavy or persistent bleeding is not.
- Adverse Reaction to Medication: Rash, severe nausea, or other allergic reactions.
6. Follow-Up Appointments
- Attend all scheduled follow-up appointments. These visits are essential for your dentist to monitor the healing process, assess the success of the treatment, and address any ongoing issues. They will also reinforce good oral hygiene practices to prevent future problems.
Adhering strictly to these aftercare instructions is vital not only for comfortable recovery but also for ensuring the long-term success of your gum abscess treatment and maintaining optimal oral health.
Prevention
Preventing a gum abscess largely involves maintaining excellent oral hygiene and addressing gum disease early. Proactive measures are your best defense against this painful infection.
1. Excellent Oral Hygiene
- Brush Twice Daily: Brush your teeth for two minutes, twice a day, using a soft-bristled toothbrush and fluoride toothpaste. Pay attention to all surfaces of your teeth and gently brush along the gum line.
- Floss Daily: Flossing once a day is crucial to remove plaque and food particles from between your teeth and under the gum line, where your toothbrush can't reach. This is vital for preventing gum disease and subsequent abscesses.
- Use an Antiseptic Mouthwash: Incorporate an antimicrobial mouthwash into your routine, especially if you're prone to gingivitis, as recommended by your dentist.
2. Regular Dental Check-ups and Professional Cleanings
- Every Six Months: Schedule regular dental check-ups and professional cleanings (scaling) at least twice a year, or more frequently if recommended by your dentist due to existing gum disease. These appointments allow dentists to:
- Remove hardened plaque (tartar) that cannot be removed by brushing alone.
- Detect and treat early signs of gum disease (gingivitis or periodontitis).
- Identify potential problems like deep pockets, overhanging fillings, or partially erupted teeth that could predispose you to an abscess.
3. Manage Gum Disease Promptly
- If you've been diagnosed with gingivitis or periodontitis, adhere strictly to your dentist's treatment plan. This might include more frequent professional cleanings (scaling and root planing), local antibiotic applications, or even surgical interventions to reduce pocket depths. Effective management of gum disease is the primary way to prevent periodontal abscesses.
4. Healthy Lifestyle Choices
- Balanced Diet: Eat a diet rich in fruits, vegetables, and whole grains, and limit sugary snacks and drinks. A healthy diet supports overall immune function and gum health.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and bacteria.
- Avoid Smoking and Tobacco Products: Smoking is a major risk factor for gum disease and significantly hinders healing. Quitting greatly reduces your risk of gum abscesses and other oral health issues.
- Manage Systemic Health Conditions: If you have conditions like diabetes, ensure they are well-controlled. Poorly managed diabetes, for example, can increase your susceptibility to infections, including gum abscesses.
5. Protect Your Gums
- Avoid Trauma: Be mindful of what you eat; avoid chewing on extremely hard objects like ice or unpopped popcorn kernels that could injure your gums or teeth.
- Address Dental Issues Promptly: Don't delay treatment for cavities, broken teeth, or ill-fitting dental work (fillings, crowns). These can all create niches for bacteria and lead to gum irritation or infection.
- Guard Against Foreign Bodies: Be careful when eating foods with small, sharp components (e.g., seeds, bone fragments) that could get lodged in your gums.
By consistently following these preventive measures, you significantly reduce your risk of developing a painful and potentially dangerous gum abscess.
Risks and Complications
While a gum abscess often presents as a localized problem, ignoring it or delaying treatment carries significant risks and can lead to severe, potentially life-threatening complications.
- Spread of Infection: This is the most serious risk. The bacteria from the abscess can spread from the gum to other parts of the body:
- Bone Loss: The infection can destroy the alveolar bone supporting the tooth, leading to tooth mobility and eventually tooth loss.
- Cellulitis: A widespread bacterial infection of the soft tissues (skin and underlying tissues) of the face, neck, or jaw. This can cause severe swelling, redness, and pain.
- Ludwig's Angina: A rapidly spreading, severe infection of the tissues in the floor of the mouth and neck. This is a medical emergency, as the swelling can block the airway, making breathing difficult or impossible.
- Cavernous Sinus Thrombosis: A very rare but life-threatening complication where a blood clot forms in the cavernous sinus (a large vein at the base of the brain), caused by the spread of infection from the face or mouth.
- Sepsis: If the infection enters the bloodstream, it can lead to sepsis, a severe, life-threatening response to infection that can cause organ damage and failure. Symptoms include high fever, chills, rapid heartbeat, rapid breathing, and confusion.
- Tooth Loss: Persistent infection and bone destruction around the tooth will eventually weaken its support, leading to its extraction or natural loss.
- Recurrence: If the underlying cause (e.g., deep periodontal pockets, impacted wisdom tooth) is not adequately addressed after initial drainage, the gum abscess is highly likely to recur.
- Chronic Pain: Left untreated, an abscess can lead to chronic, persistent pain and discomfort, significantly impacting quality of life.
- Sinusitis: An upper jaw abscess can sometimes spread to the maxillary sinuses, causing a sinus infection.
- Dental Fistula: The infection might create a chronic drainage channel (fistula or sinus tract) through the gum to release pus. While this can temporarily relieve pressure and pain, it means the infection is still present and actively draining.
These potential complications underscore why a gum abscess should never be ignored. Early diagnosis and prompt, appropriate treatment by a dental professional are paramount to preventing these severe outcomes and ensuring your overall health and well-being.
Comparison Tables
To help visualize the differences between abscess types and treatment costs, here are two comparison tables:

Table 1: Comparison of Gum Abscess Types
| Feature | Gingival Abscess | Periodontal Abscess | Pericoronal Abscess (Pericoronitis) |
|---|---|---|---|
| Primary Cause | Foreign body impaction, trauma | Pre-existing periodontal disease (gum disease) | Partially erupted tooth (often wisdom tooth) |
| Location | Confined to marginal gum tissue | Deep in periodontal pocket, involves supporting bone | Gum flap (operculum) over partially erupted tooth |
| Severity | Generally mild, localized | Moderate to severe, can cause bone loss | Can be severe, spread to jaw/throat, difficult chewing |
| Pain Level | Acute, localized, usually sharp | Dull, throbbing, constant, often radiating | Throbbing, severe, difficulty opening mouth |
| Tooth Mobility | Rarely affects tooth mobility | Common, tooth may feel loose or elevated | Tooth itself usually not mobile, but surrounding tissue is painful |
| Typical Onset | Rapid onset | Can be gradual or acute flare-up | Often acute, recurrent episodes |
| Treatment | Drainage, foreign body removal, antibiotics (if needed) | Drainage, scaling & root planing, antibiotics, potentially surgery/extraction | Drainage, antibiotics, operculectomy, wisdom tooth extraction |
Table 2: Estimated Cost Comparison for Gum Abscess Treatment (US, without Insurance)
| Procedure | Low Estimate | Mid Estimate | High Estimate | Key Factors Influencing Cost |
|---|---|---|---|---|
| Emergency Exam & X-rays | $50 | $150 | $250 | Clinic location, type of X-rays (periapical vs. panoramic) |
| Incision and Drainage (I&D) | $150 | $250 | $400 | Complexity, amount of pus, geographic location |
| Antibiotics (prescription cost) | $10 | $30 | $60 | Type of antibiotic, brand vs. generic, pharmacy pricing |
| Scaling & Root Planing (per quadrant) | $200 | $400 | $600 | Severity of gum disease, number of teeth per quadrant, geographic location, periodontist vs. general dentist |
| Simple Tooth Extraction | $150 | $300 | $450 | Location of tooth, complexity of extraction (e.g., roots fractured), anesthesia used |
| Surgical Tooth Extraction | $300 | $550 | $800+ | Impaction level of tooth, need for bone removal, sedation options, oral surgeon vs. general dentist |
| Root Canal (Anterior Tooth) | $700 | $950 | $1,200 | Geographic location, complexity of canals, general dentist vs. endodontist |
| Root Canal (Molar Tooth) | $1,000 | $1,750 | $2,500+ | Geographic location, number of canals, complexity, general dentist vs. endodontist |
| Periodontal Flap Surgery (per quadrant) | $1,000 | $2,000 | $3,000+ | Severity of bone loss, number of teeth, need for bone grafting, periodontist fees |
(Note: These are estimated ranges and can vary widely. It is essential to get a specific treatment plan and cost estimate from your dental provider.)
Children / Pediatric Considerations
Gum abscesses can affect children, though they are often less common than in adults. When they do occur, they warrant immediate attention due to the developing nature of a child's dentition and potential for rapid spread of infection. Parents should be particularly vigilant for signs of pain and swelling in their child's mouth.
Why Gum Abscesses Occur in Children
- Dental Trauma: Children are more prone to falls and accidents, which can injure the gums or teeth, creating entry points for bacteria.
- Deep Cavities: Untreated, extensive tooth decay can lead to a periapical abscess (at the tooth root), which can then drain into the gum tissue, mimicking a gum abscess, or in some cases, directly infect the surrounding gums.
- Erupting Teeth (Teething): While most teething discomfort is normal, sometimes a partially erupted tooth (especially primary molars or permanent molars) can develop a pericoronal-like infection if food or bacteria get trapped under the gum flap.
- Poor Oral Hygiene: Inadequate brushing and flossing, often seen in children, can lead to plaque buildup and gingivitis, increasing the risk of gum inflammation and infection.
- Foreign Bodies: Children might accidentally get food particles (e.g., popcorn kernels) or small toy parts lodged in their gums.
Specific Symptoms to Watch For in Kids
Children may not always articulate their pain clearly. Parents should look for:
- Irritability or Fussiness: Unexplained changes in mood.
- Difficulty Eating: Refusal to eat, especially hard or chewy foods, or favoring one side of the mouth.
- Swelling: Visible swelling in the gums, cheek, or around a specific tooth.
- Redness or Shininess of Gums: Inflammation in the affected area.
- Fever: A general sign of infection.
- Bad Breath: Persistent bad breath not resolved by brushing.
- Sensitivity: Child reacting to hot or cold foods.
- Pimple-like Bump: A small bump on the gum, sometimes with pus drainage.
Treatment Approaches for Children
Treatment for a gum abscess in a child focuses on resolving the infection and preserving the developing dentition.
- Early Diagnosis: A pediatric dentist will use visual examination and potentially X-rays (digital X-rays minimize radiation exposure) to diagnose the abscess.
- Drainage: Similar to adults, incision and drainage may be performed under local anesthesia to relieve pressure and remove pus.
- Antibiotics: Antibiotics are often prescribed, especially if there are systemic signs like fever or if the infection is spreading.
- Addressing the Cause:
- For cavities: The affected tooth will need to be restored or, if severely infected, extracted (especially primary teeth).
- For foreign bodies: Removal of the object.
- For erupting teeth: Sometimes, a minor procedure to help the tooth erupt, or simply careful monitoring and hygiene.
- Emphasis on Prevention: Education for both parents and children on proper brushing, flossing, and the importance of a healthy diet is paramount to prevent future issues. Regular dental check-ups are vital.
Pro Tip for Parents: If your child complains of tooth or gum pain, or if you notice any swelling or redness, do not delay seeing a pediatric dentist. Early intervention is key to preventing the spread of infection and protecting your child's developing teeth and overall health.
Cost Breakdown
While we covered costs in the main content, let's provide a specific cost breakdown for a typical gum abscess scenario, along with payment and cost-saving options.
Average US Costs for a Typical Gum Abscess Scenario
Let's consider a scenario where a patient presents with a moderate periodontal abscess requiring drainage, antibiotics, and initial deep cleaning (scaling and root planing for one quadrant).
-
Low Cost Scenario (e.g., rural area, basic clinic):
- Emergency Exam & X-rays: $75
- Incision and Drainage: $175
- Antibiotics: $20
- Scaling & Root Planing (1 quadrant): $250
- Total without Insurance: $520
- Total with Insurance (e.g., 80% coverage after $50 deductible): $50 (deductible) + $35 (I&D 20%) + $20 (antibiotics) + $50 (SRP 20%) = $155 out-of-pocket
-
Mid Cost Scenario (e.g., suburban area, standard practice):
- Emergency Exam & X-rays: $150
- Incision and Drainage: $250
- Antibiotics: $35
- Scaling & Root Planing (1 quadrant): $400
- Total without Insurance: $835
- Total with Insurance (e.g., 80% coverage after $50 deductible): $50 (deductible) + $50 (I&D 20%) + $35 (antibiotics) + $80 (SRP 20%) = $215 out-of-pocket
-
High Cost Scenario (e.g., major city, specialist clinic):
- Emergency Exam & X-rays: $225
- Incision and Drainage: $350
- Antibiotics: $50
- Scaling & Root Planing (1 quadrant): $550
- Total without Insurance: $1,175
- Total with Insurance (e.g., 80% coverage after $50 deductible): $50 (deductible) + $70 (I&D 20%) + $50 (antibiotics) + $110 (SRP 20%) = $280 out-of-pocket
(These scenarios are illustrative. Actual costs and insurance coverage can vary greatly. Remember, this doesn't include any subsequent major procedures like root canals or extractions if needed.)
Payment Plans and Financing Options
Even with insurance, dental costs can accumulate, especially if you exceed your annual maximum or require major procedures.
- In-Office Payment Plans: Many dental practices offer flexible payment options directly. This usually involves an initial down payment and then monthly installments. Inquire with the office manager about their policies.
- Dental Financing Companies (e.g., CareCredit, LendingClub): These are specialized credit cards designed for healthcare expenses. They often offer short-term (6-24 months) interest-free financing options for qualified applicants if the balance is paid in full within the promotional period. Be aware of deferred interest if you don't pay it off in time.
- Personal Loans: Banks or credit unions may offer personal loans for larger dental expenses. These typically have fixed interest rates and repayment schedules.
- Flexible Spending Accounts (FSA) / Health Savings Accounts (HSA): If you have an FSA or HSA through your employer, you can use these tax-advantaged accounts to pay for qualified dental expenses. You contribute pre-tax dollars, which reduces your taxable income.
- Dental Discount Plans: These are not insurance but membership plans where you pay an annual fee to get reduced prices (e.g., 10-60% off) on dental procedures from participating dentists. These can be a good option if you don't have traditional insurance.
Cost-Saving Tips
- Compare Prices: If it's not an emergency, call different dental offices to inquire about their fees for specific procedures.
- Utilize Dental Schools: Dental schools often provide services at a reduced cost, performed by students under the close supervision of experienced dentists. The quality of care is usually excellent.
- Community Dental Clinics: Many communities have clinics that offer affordable dental care, often on a sliding scale based on income.
- Preventative Care: The best cost-saving tip is prevention. Regular check-ups and cleanings, good oral hygiene, and addressing issues early can prevent costly emergencies like abscesses.
- Negotiate: Don't be afraid to discuss your financial situation with your dentist's office. They may be willing to work with you on a payment plan or suggest alternative solutions.
Pro Tip: Always get a detailed written estimate for your treatment plan before proceeding. This will outline all anticipated costs and help you plan financially.
Frequently Asked Questions
How long does a gum abscess last if untreated?
An untreated gum abscess will not go away on its own. While the pain might temporarily subside if the pus finds a way to drain, the underlying infection will persist and can lead to chronic issues. The infection will continue to spread, potentially causing severe bone loss, damage to surrounding teeth, and systemic complications over weeks, months, or even years.

Can a gum abscess heal on its own?
No, a gum abscess cannot heal on its own. It requires professional dental intervention to drain the pus and eliminate the bacterial infection. Attempting to manage it at home can lead to serious complications and a worsening of the infection.
What does a gum abscess look like?
A gum abscess typically appears as a red, swollen, and tender bump on the gum tissue near a tooth. It might resemble a "pimple" or boil, and in some cases, you may see pus draining from it, giving it a yellowish or whitish center. The surrounding gum tissue will often appear inflamed and shiny.
Is a gum abscess an emergency?
Yes, a gum abscess is considered a dental emergency. While some may be less immediately painful than others, the risk of the infection spreading rapidly is significant. You should seek dental attention as soon as possible, ideally within 24-48 hours, especially if you have severe pain, swelling, fever, or difficulty swallowing.
What pain relief can I use for a gum abscess before seeing a dentist?
For temporary pain relief, you can rinse your mouth with warm salt water (1/2 teaspoon of salt in 8 ounces of warm water) several times a day to soothe the area and reduce inflammation. Over-the-counter pain relievers like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) can also help manage the discomfort. However, these are temporary measures and do not treat the underlying infection.
How much does it cost to drain a gum abscess?
The cost to drain a gum abscess (incision and drainage) typically ranges from $150 to $400 without insurance in the US. This cost can vary based on your location and the specific dental office. This initial procedure often doesn't include the cost of follow-up treatments like antibiotics or deep cleaning to address the root cause.
What if I ignore a gum abscess?
Ignoring a gum abscess is extremely dangerous. The infection will continue to spread, potentially leading to severe bone loss around the affected tooth, tooth loss, or serious systemic complications such as cellulitis (widespread soft tissue infection), Ludwig's angina (life-threatening infection of the mouth floor), or even sepsis (blood poisoning), which can be fatal.
What is the difference between a gum abscess and a tooth abscess?
A gum abscess (periodontal abscess) originates in the gum tissue and surrounding supporting structures of the tooth (periodontal ligament, bone). A tooth abscess (periapical abscess) originates inside the tooth, at the tip of the root, due to an infected nerve (pulp). While both involve pus and cause pain, their origins and primary treatments differ.
Can a gum abscess cause bad breath?
Yes, a gum abscess can cause significant bad breath (halitosis). The accumulation of bacteria and pus, particularly if the abscess is draining, produces volatile sulfur compounds that contribute to a foul odor in the mouth. This bad breath typically won't resolve until the infection is treated.
How can I prevent a gum abscess from recurring?
Preventing recurrence involves addressing the underlying cause. This includes maintaining excellent daily oral hygiene (brushing and flossing), attending regular dental check-ups and professional cleanings, thoroughly treating any existing gum disease (e.g., scaling and root planing), and managing systemic health conditions like diabetes effectively.
When to See a Dentist
Recognizing when to seek dental care for a gum abscess is crucial for preventing severe complications. Here's guidance on when to see a dentist:
Immediate Dental Attention (Emergency - See a Dentist Today or Go to an ER)
You should seek immediate dental attention if you experience any of the following, as these indicate a potentially rapidly spreading and dangerous infection:
- Severe, Throbbing, or Unbearable Pain: Pain that is constant, disrupts sleep, and is not alleviated by over-the-counter pain medication.
- Rapidly Spreading Swelling: Swelling that is increasing quickly, extending beyond the immediate gum area to your cheek, jaw, eye, or neck.
- Difficulty Breathing or Swallowing: This is a critical sign that the infection is spreading into your airway and can be life-threatening. Go to the nearest emergency room immediately.
- High Fever and Chills: Systemic symptoms like fever, chills, and general malaise indicate a significant infection that requires prompt medical and dental intervention.
- Facial Asymmetry: Noticeable lopsidedness of your face due to swelling.
- Unusual Fatigue or Confusion: These can be signs of a more widespread infection, including sepsis.
Urgent Dental Care (See a Dentist Within 24-48 Hours)
If you have these symptoms, you need to see a dentist very soon, even if they don't feel immediately life-threatening:
- Persistent Gum Swelling and Redness: Even if the pain is manageable, visible swelling and inflammation of the gums that doesn't resolve within a day or two.
- Localized Tenderness and Pain: Pain when chewing, touching the gum, or around a specific tooth.
- Pimple-like Bump on Gums: A visible lesion on the gum that may be draining pus.
- Foul Taste or Bad Breath: A persistent bad taste in your mouth or noticeable bad breath originating from a specific gum area.
- Loose Tooth: Any new or increased mobility of a tooth associated with gum pain or swelling.
Routine Dental Care (Schedule an Appointment Soon)
If you notice any of the following, it's wise to schedule a non-emergency appointment to get checked out, as these could be early signs of gum disease or issues that could lead to an abscess:
- Bleeding Gums: Gums that bleed when you brush or floss.
- Red or Swollen Gums: Gums that appear persistently red or puffy.
- Receding Gums: Gums that appear to be pulling away from your teeth.
- Chronic Bad Breath: Persistent bad breath that doesn't improve with brushing.
Pro Tip: When in doubt, always call your dentist. Describe your symptoms clearly. They can advise you on the urgency of your situation and ensure you receive the appropriate care promptly. Do not wait for symptoms to worsen, as early intervention significantly improves outcomes and prevents serious complications.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Is an Abscess
Imagine a throbbing pain deep within your jaw, a persistent ache that keeps you awake at night and makes even the softest foods unbearable. This isn't just a bad toothache; it could be a sign of something much more serious: a dental abscess. Affecting millions of Americans annually, an abscess is an
February 22, 2026
Cracked Tooth Syndrome: Complete Guide
Cracked Tooth Syndrome: Complete Guide Category: Dental Conditions & Diseases
February 22, 2026
Dentinogenesis Imperfecta: Complete Guide
Imagine a world where your teeth, fundamental to chewing, speaking, and even smiling confidently, are inherently fragile, discolored, and prone to rapid wear from the moment they emerge. For individuals affected by dentinogenesis imperfecta (DI), this is a reality. While relatively rare, affecti
February 22, 2026
Stage 1 Early Cavity: Complete Guide
Did you know that dental cavities are one of the most common chronic diseases globally, affecting both children and adults? In the United States, over 90% of adults have had a cavity, and a significant portion of these begin as a stage 1 early cavity. Often invisible and painless in its nasc
February 22, 2026