Enamel
4,216 words · 14 min read
Quick Definition
The hard, translucent outer covering of the tooth crown. Enamel is the hardest substance in the human body, composed primarily of hydroxyapatite minerals.
Enamel: The Indomitable Shield of Your Smile
Introduction
Enamel is the incredibly hard, translucent outer covering of the tooth crown, the part of your tooth visible above the gum line. It is, unequivocally, the hardest substance in the human body, surpassing even bone in its mineral density. Composed primarily of a crystalline form of calcium phosphate known as hydroxyapatite, enamel provides the crucial protective layer for the softer, more sensitive inner structures of your teeth, namely the dentin and pulp.
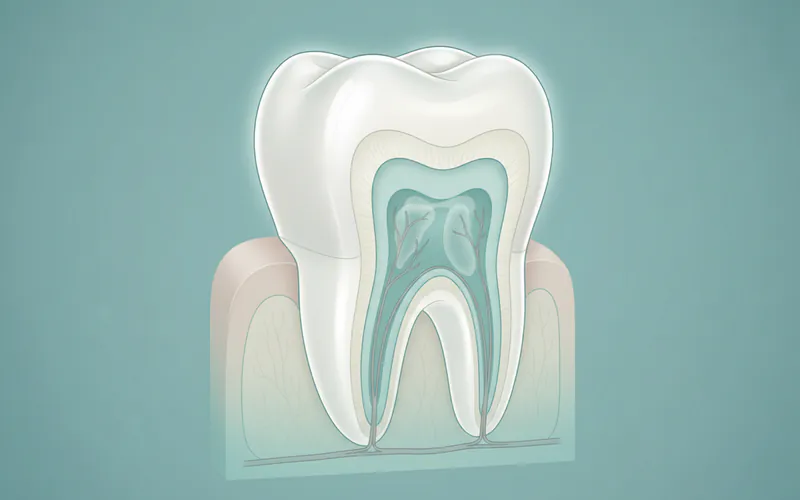
Why does enamel matter so much for dental health? Quite simply, it's your teeth's first and strongest line of defense. Every time you bite, chew, speak, or expose your teeth to temperature changes and various foods and drinks, it's your enamel that takes the brunt of the forces and chemical attacks. Healthy enamel protects against decay (caries), reduces tooth sensitivity, and maintains the structural integrity of your teeth. Without robust enamel, teeth would quickly succumb to wear, bacterial invasion, and damage, leading to pain, infection, and eventually tooth loss. While remarkably strong, enamel is not invincible and can be weakened and eroded by acids, physical wear, and certain conditions. Protecting your enamel is paramount for a lifetime of healthy smiles. According to the Centers for Disease Control and Prevention (CDC), dental caries, primarily affecting enamel, remains one of the most common chronic diseases in both children and adults in the United States, with approximately 92% of adults aged 20–64 having had dental caries in their permanent teeth.
Key Takeaways:
- Enamel is the hardest substance in the human body, primarily made of hydroxyapatite.
- It forms the outer protective layer of your tooth crown, shielding the sensitive dentin and pulp.
- Unlike bone, enamel cannot regenerate itself once lost or severely damaged.
- Acidic foods, drinks, and bacterial byproducts are the primary threats to enamel integrity.
- Fluoride is essential for strengthening enamel and making it more resistant to acid attacks.
- Good oral hygiene, a balanced diet, and regular dental check-ups are vital for preserving enamel.
Detailed Explanation
While enamel is often discussed as a single entity, its health can be impacted by a variety of conditions and factors. Understanding these aspects is crucial for prevention and effective management.
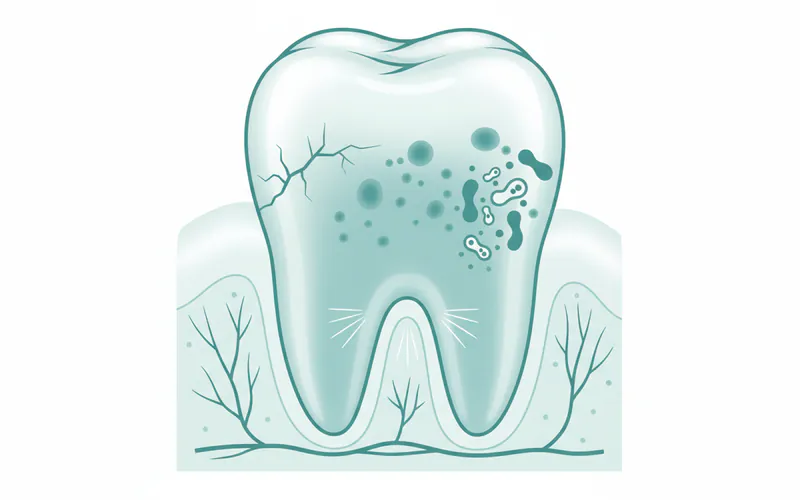
Conditions Affecting Enamel (Types and Classifications)
Instead of "types" of enamel, which is a singular tissue, it's more accurate to discuss the conditions and defects that affect enamel's structure and integrity. These can be broadly categorized as developmental defects or acquired damage.
- Enamel Hypoplasia: This is a developmental defect where the enamel doesn't form properly during tooth development, resulting in thinner, weaker, or missing patches of enamel. It can appear as pits, grooves, or discolored spots on the tooth surface.
- Causes: Genetic factors, nutritional deficiencies (e.g., Vitamin D, calcium), high fevers, certain medications taken by the mother during pregnancy or by the child in early life, pre-term birth, trauma to primary teeth affecting permanent tooth buds.
- Impact: Teeth with hypoplasia are highly susceptible to caries and sensitivity due to the compromised protective layer.
- Enamel Erosion: This is the loss of tooth enamel due to acid attack, not involving bacterial action initially. Acids can come from external sources (extrinsic) or internal sources (intrinsic).
- Extrinsic Erosion: Caused by highly acidic foods and drinks (sodas, fruit juices, citrus fruits, sports drinks, vinegars), or acidic medications.
- Intrinsic Erosion: Caused by gastric acids from conditions like gastroesophageal reflux disease (GERD), bulimia, or chronic vomiting.
- Impact: Leads to thinning of enamel, yellowing of teeth (as dentin becomes more visible), increased sensitivity, and eventual tooth loss if severe.
- Enamel Attrition: This is the wear of tooth enamel caused by tooth-to-tooth contact, such as from chewing, grinding (bruxism), or clenching.
- Causes: Malocclusion (improper bite), missing teeth (leading to increased load on remaining teeth), habits like bruxism.
- Impact: Leads to flattened chewing surfaces, shortened teeth, cracks, and increased sensitivity.
- Enamel Abrasion: This is the wear of enamel due to friction from foreign objects or substances, not tooth-to-tooth contact.
- Causes: Aggressive tooth brushing (especially with hard-bristled brushes or abrasive toothpastes), using teeth as tools (e.g., opening bottles, chewing on pens), chewing tobacco, abrasive dental habits.
- Impact: Notched or grooved areas near the gum line, especially on the sides of teeth, leading to sensitivity and potential gum recession.
- Enamel Abfraction: These are wedge-shaped lesions at the gum line caused by stresses from biting forces that flex the tooth structure. The enamel chips away where the tooth flexes most.
- Causes: Occlusal (biting) forces, particularly in individuals with bruxism or an uneven bite.
- Impact: Can cause sensitivity, potential gum recession, and create areas prone to caries.
- Dental Caries (Cavities): While not a "type" of enamel, caries are the direct result of bacterial acids dissolving enamel. This is the most common form of enamel damage.
Causes and Risk Factors for Enamel Damage
Several factors can contribute to the weakening and loss of enamel:
- Dietary Habits:
- High consumption of acidic foods and drinks: Sodas, fruit juices, sports drinks, citrus fruits, vinegars, sour candies. These directly dissolve enamel.
- Frequent snacking on sugary foods: Provides a constant food source for acid-producing bacteria in plaque.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque to accumulate, leading to bacterial acid production and caries.
- Medical Conditions:
- Gastroesophageal Reflux Disease (GERD): Chronic acid reflux brings stomach acid into the mouth, eroding enamel.
- Eating Disorders (Bulimia): Frequent vomiting exposes teeth to highly acidic stomach contents.
- Dry Mouth (Xerostomia): Saliva helps neutralize acids and remineralize enamel. Reduced saliva flow (due to medications, medical conditions, or radiation therapy) increases erosion risk.
- Certain Medications: Antihistamines, decongestants, painkillers, and diuretics can cause dry mouth. Some acidic medications (e.g., chewable aspirin, some Vitamin C supplements) can directly erode enamel.
- Parafunctional Habits:
- Bruxism (Teeth Grinding/Clenching): Puts immense pressure on teeth, leading to attrition and abfraction.
- Using teeth as tools: Opening packages, biting nails, chewing on pens.
- Genetic Predisposition: Some individuals may have naturally thinner or softer enamel due to genetic factors, making them more susceptible to damage.
- Environmental Factors: Excessive exposure to certain industrial acids (e.g., in some workplaces) can also contribute to erosion.
Signs and Symptoms to Watch For
Recognizing the early signs of enamel damage can significantly impact treatment success and prevent further deterioration.
- Increased Sensitivity: This is often one of the earliest and most common symptoms. You might feel a sharp, fleeting pain when consuming hot, cold, sweet, or acidic foods and drinks. This happens as the enamel thins, exposing the underlying dentin, which contains microscopic tubules leading to the nerve.
- Discoloration/Yellowing: As enamel erodes, the yellowish dentin beneath becomes more visible, making the teeth appear less white or more yellow.
- Transparency: The biting edges of the front teeth might appear more translucent or glassy, a sign of severe enamel thinning.
- Rough Spots/Irregularities: The tooth surface might feel rough or develop small pits or grooves, indicating localized enamel loss (e.g., from hypoplasia or early erosion).
- Cracks or Chips: Weakened enamel is more prone to fracture, leading to visible cracks or small chips, especially on the biting surfaces or edges.
- "Cupping" on Chewing Surfaces: This refers to small indentations or depressions that form on the chewing surfaces of teeth, often with a darker dentin exposed in the center, characteristic of severe erosion.
- Tooth Shortening: In cases of severe attrition or bruxism, teeth may appear visibly shorter or flattened.
Diagnosis Process — What Your Dentist Does
Diagnosing enamel issues is typically straightforward and involves a combination of visual inspection, patient history, and sometimes imaging.
- Comprehensive Dental Examination:
- Visual Inspection: Your dentist will carefully examine your teeth for signs of wear, erosion, discoloration, cracks, and cavities. They'll look for specific patterns of wear that might indicate bruxism, erosion, or abrasion.
- Dental Explorer: A small, sharp instrument is used to gently probe the tooth surface to detect soft spots, rough areas, or sticky areas that indicate caries or demineralization.
- Transillumination: A bright light shone through the tooth can reveal cracks or areas of demineralization that might not be visible otherwise.
- Patient History: Your dentist will ask detailed questions about your:
- Dietary habits: Frequent consumption of acidic or sugary foods/drinks.
- Oral hygiene routine: Brushing technique, type of toothbrush, flossing habits.
- Medical history: Conditions like GERD, eating disorders, medications that cause dry mouth.
- Lifestyle factors: Bruxism, use of teeth as tools, habits like chewing tobacco.
- Symptoms: When sensitivity occurs, its duration, and what triggers it.
- Radiographs (X-rays): While X-rays don't directly show enamel erosion, they are crucial for detecting caries that have penetrated the enamel into the dentin, as well as assessing the overall health of the tooth structure and surrounding bone.
- Photographs: In some cases, especially for monitoring progression, your dentist might take intraoral photographs to document the initial state of enamel damage.
Treatment Options with Pros, Cons, and Costs
Treatment for enamel issues depends heavily on the extent and type of damage. The goal is to prevent further loss, reduce sensitivity, and restore tooth structure and aesthetics.
| Treatment Option | Description | Pros | Cons | US Cost Range (Self-Pay) |
|---|---|---|---|---|
| Fluoride Treatments | Professional application of high-concentration fluoride varnish, gel, or foam. | Strengthens enamel, remineralizes early lesions, reduces sensitivity, prevents caries. Non-invasive. | Not a restorative treatment for significant loss. Requires regular applications. | $25 - $75 per application |
| Desensitizing Toothpastes | Over-the-counter toothpastes containing ingredients like potassium nitrate or stannous fluoride to block pain signals or occlude dentinal tubules. | Easy to use, affordable, effective for mild sensitivity. | Requires consistent use. Not a cure for underlying enamel loss. Effects are temporary if discontinued. | $5 - $20 (OTC) |
| Dental Bonding | Application of tooth-colored composite resin directly to the tooth, sculpted to match, and hardened with a light. | Minimally invasive, preserves more tooth structure, relatively quick and affordable. Good for minor chips, cracks, and surface irregularities. | Less durable than veneers or crowns (can chip/stain). May need replacement every 5-10 years. Not ideal for extensive damage. Pigmentation can occur over time. | $150 - $600 per tooth (depending on size and complexity) |
| Dental Fillings | Primarily used to treat caries (cavities) that have penetrated enamel. Composite (tooth-colored) or amalgam (silver) materials are used. | Restores tooth function and structure after decay removal. Prevents further decay. Durable. | Requires removal of tooth structure. Amalgam is visible; composite may stain over time. Can cause temporary sensitivity. Not for generalized erosion. | Composite: $100 - $350 per tooth (depending on size/location) Amalgam: $50 - $200 per tooth (less common for enamel repair) |
| Dental Veneers | Custom-made, thin shells (porcelain or composite) bonded to the front surface of teeth to improve aesthetics and protect compromised enamel. | Highly aesthetic, durable (porcelain), good for moderate to severe erosion/discoloration on front teeth. | Irreversible (requires removal of some enamel). More expensive. Can chip or debond. Not ideal for biting surfaces. | Porcelain: $900 - $2,500+ per tooth Composite: $250 - $1,500 per tooth |
| Dental Crowns | A cap that covers the entire tooth, restoring its shape, size, strength, and appearance. Made from porcelain, ceramic, metal, or a combination. | Highly durable, provides comprehensive protection, restores severely damaged or weakened teeth. | Requires significant removal of tooth structure. Most expensive option. Can be sensitive initially. | $800 - $3,000+ per tooth (material dependent) |
| Nightguard/Splint | Custom-fitted oral appliance worn at night to protect teeth from grinding/clenching forces (bruxism). | Prevents further attrition and abfraction, reduces jaw pain, protects restorations. | Requires consistent wear. Can be uncomfortable initially. Does not treat existing damage, only prevents future. | $300 - $800 (custom-made) |
| Dietary/Lifestyle Modif. | Counseling on reducing acidic foods, improving oral hygiene, managing GERD, quitting smoking/tobacco, treating eating disorders. | Non-invasive, fundamental for long-term enamel health, no direct cost beyond counseling. | Requires significant patient commitment and behavior change. | No direct cost (covered by regular dental visits) |
Step-by-Step: What to Expect During Treatment
Let's detail the process for some common restorative treatments for enamel damage:
-
Dental Bonding:
- Preparation: The tooth surface is gently etched with a mild phosphoric acid gel to create a slightly rough surface for strong adhesion. No anesthesia is usually needed unless the damage is near the nerve.
- Application: A conditioning liquid is applied, followed by the composite resin, which the dentist carefully sculpts to match the natural tooth shape and color.
- Curing: A special curing light is used to harden the resin in seconds.
- Finishing: The bonded material is trimmed, shaped, and polished for a natural appearance and comfortable bite.
- Duration: Typically 30-60 minutes per tooth.
-
Porcelain Veneers:
- Consultation & Planning: Discuss goals, take impressions, photos, and possibly create a wax-up model of the proposed changes.
- Preparation: A small amount of enamel (usually less than a millimeter) is removed from the front surface of the tooth to make space for the veneer. Impressions are taken, and temporary veneers may be placed.
- Fabrication: Impressions are sent to a dental lab where custom veneers are crafted (takes 1-2 weeks).
- Bonding: The temporaries are removed. The tooth surface is cleaned and etched. The veneer is meticulously placed, checked for fit and color, and then permanently bonded with a strong dental cement, cured with a light.
- Duration: Two appointments, each 1-2 hours, over a couple of weeks.
-
Dental Crowns:
- Preparation: The tooth is reshaped, removing enamel and some dentin to create a stable base for the crown. Anesthesia is typically used.
- Impressions: Digital or traditional impressions are taken. A temporary crown is placed to protect the prepared tooth.
- Fabrication: The impressions are sent to a lab to create the custom crown (1-2 weeks).
- Placement: The temporary crown is removed. The permanent crown is checked for fit, bite, and color match, then cemented into place.
- Duration: Two appointments, each 1-2 hours, over a couple of weeks. Some clinics offer same-day crowns using CAD/CAM technology.
Recovery Timeline and Aftercare
Recovery and aftercare depend on the treatment performed:
- Fluoride Treatments & Desensitizing Pastes: No recovery needed. Continue with good oral hygiene. For fluoride, avoid eating/drinking for 30 minutes after application.
- Dental Bonding:
- Recovery: Minimal. May experience mild sensitivity to hot/cold for a few days.
- Aftercare: Avoid hard, sticky, or staining foods for the first 24-48 hours. Practice excellent oral hygiene. Avoid using bonded teeth for biting hard objects.
- Dental Fillings:
- Recovery: Numbness from anesthesia usually wears off in a few hours. Mild sensitivity for a few days to weeks is common.
- Aftercare: Avoid chewing on the filling until the numbness wears off. Maintain good oral hygiene.
- Veneers & Crowns:
- Recovery: May experience temporary sensitivity to hot/cold after preparation and placement, lasting a few days to a few weeks. The bite might feel slightly different initially.
- Aftercare: Treat veneers and crowns like natural teeth. Practice diligent oral hygiene (brushing, flossing). Avoid biting hard objects directly with veneers. If bruxism is present, continue to wear a nightguard. Regular dental check-ups are crucial to monitor their longevity.
Prevention Strategies
Prevention is truly the best medicine when it comes to enamel, as it cannot regenerate.
- Maintain Excellent Oral Hygiene:
- Brush twice daily with a fluoride toothpaste for two minutes using a soft-bristled brush.
- Floss daily to remove plaque and food particles from between teeth.
- Consider an antimicrobial mouthwash if recommended by your dentist.
- Manage Dietary Habits:
- Limit acidic foods and drinks: Reduce consumption of sodas, fruit juices, sports drinks, and highly acidic fruits.
- Rinse with water: After consuming acidic foods/drinks, rinse your mouth with plain water to help neutralize acids. Wait at least 30 minutes before brushing to avoid abrading acid-softened enamel.
- Use a straw: When drinking acidic beverages, use a straw to minimize contact with teeth.
- Choose water: Make water your primary beverage choice.
- Utilize Fluoride:
- Ensure your drinking water is fluoridated (if available).
- Use fluoride toothpaste.
- Ask your dentist about professional fluoride treatments or prescription-strength fluoride rinses/pastes if you're at high risk for enamel erosion or caries.
- Address Underlying Medical Conditions:
- Seek treatment for GERD from a medical professional.
- If you have an eating disorder, seek professional help.
- Discuss dry mouth with your dentist or doctor; they may recommend saliva substitutes or medications.
- Protect Against Bruxism: If you grind or clench your teeth, especially at night, talk to your dentist about a custom-fitted nightguard. This protects enamel from destructive forces.
- Avoid Destructive Habits: Do not use your teeth as tools. Avoid chewing on ice, pens, or other hard objects.
- Regular Dental Check-ups: Visit your dentist every six months for professional cleanings and examinations. Early detection of enamel issues allows for less invasive and more effective treatment.
Cost Ranges in the US (with/without insurance)
Dental costs in the US vary significantly based on location, the dentist's fees, and the complexity of the case. The table above provides self-pay ranges.
- With Dental Insurance: Most dental insurance plans cover a percentage of preventative and restorative care.
- Preventative (Fluoride, cleanings): Often covered at 80-100%.
- Basic Restorative (Fillings, Bonding): Typically covered at 50-80% after a deductible.
- Major Restorative (Crowns, Veneers - if medically necessary): Often covered at 25-50% after a deductible. Veneers for purely cosmetic reasons are rarely covered.
- Without Insurance: You will pay the full out-of-pocket cost. Many dentists offer payment plans, or you might consider dental discount plans or health savings accounts (HSAs)/flexible spending accounts (FSAs).
For Parents / Pediatric Considerations
Children's enamel is particularly vulnerable for several reasons, making pediatric enamel health a critical concern.
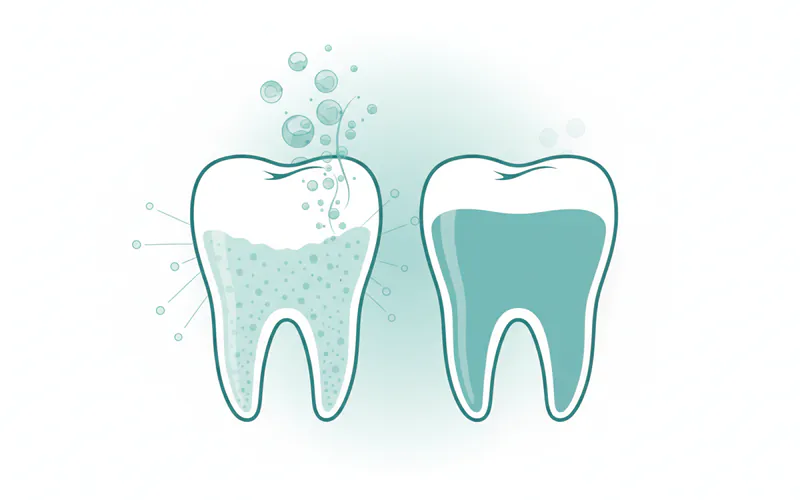
- Developing Enamel: Both primary (baby) and permanent teeth are still developing their enamel structure through childhood and adolescence. Issues like enamel hypoplasia can occur during this crucial developmental period, making teeth more prone to caries.
- Dietary Habits: Children often consume more sugary and acidic snacks and drinks (juices, sodas), which pose a significant risk for erosion and caries.
- Oral Hygiene Compliance: Young children may not have the dexterity or discipline to brush effectively, requiring parental supervision and assistance until they are about 7-8 years old.
- Risk of Caries: According to the CDC, approximately 45% of children aged 2-19 years have had dental caries, emphasizing the importance of early intervention and prevention.
- Thumb Sucking/Pacifier Use: Prolonged habits can affect tooth alignment and contribute to wear patterns.
Parental Strategies:
- Start Early: Begin cleaning a baby's gums even before teeth erupt. Brush with a soft infant toothbrush and a tiny smear of fluoride toothpaste (rice grain size) once teeth appear. For children 3-6 years old, use a pea-sized amount of fluoride toothpaste.
- Supervise Brushing: Ensure children brush thoroughly for two minutes, twice a day.
- Dietary Control: Limit sugary and acidic snacks and drinks. Offer water between meals.
- Regular Dental Visits: Begin routine dental check-ups by age one or when the first tooth erupts.
- Fluoride and Sealants: Ask the dentist about professional fluoride treatments and dental sealants (thin plastic coatings applied to the chewing surfaces of molars) to protect against caries.
- Address Bruxism: If a child grinds their teeth, especially at night, discuss it with the dentist.
Frequently Asked Questions
Q1: Can enamel grow back or regenerate?
A: No, unfortunately, once enamel is lost due to erosion, attrition, or caries, the human body cannot regenerate it. Unlike bone, enamel contains no living cells, so it lacks the capacity for self-repair. However, early stages of enamel demineralization can be reversed through a process called remineralization, primarily aided by fluoride and minerals from saliva, which can strengthen the remaining enamel and stop the progression of a cavity.
Q2: What's the main difference between enamel erosion and a cavity (caries)?
A: Enamel erosion is the direct chemical dissolution of enamel by acids, typically from dietary sources or stomach acid (e.g., GERD). It affects broad areas of the tooth surface. A cavity (caries) is caused by specific bacteria in plaque metabolizing sugars and producing acids, which then demineralize and create a hole in the enamel. While both involve acid, erosion is a generalized chemical attack, and caries is a localized bacterial infection.
Q3: Does tooth whitening damage enamel?
A: When done professionally and under the guidance of a dentist, tooth whitening is generally safe and does not cause permanent damage to enamel. Over-the-counter products can be safe when used as directed, but overuse or misuse can lead to temporary sensitivity and potential irritation of gums. Whitening agents typically open the pores of the enamel to remove stains but do not dissolve the enamel itself. Always consult your dentist before starting any whitening treatment.
Q4: How long does a dental filling or bonding last for enamel repair?
A: The longevity depends on the material, location, size, and your oral hygiene habits.
- Dental Bonding: Typically lasts 5 to 10 years before needing repair or replacement.
- Composite Fillings: Usually last 5 to 7 years, but can last longer with good care.
- Amalgam Fillings: Can last 10 to 15 years or more.
- Veneers and Crowns: Generally the most durable, lasting 10 to 15 years or even longer with proper care. Regular dental check-ups help monitor the condition of restorations.
Q5: Is enamel sensitivity always a sign of serious damage?
A: Not always. Mild sensitivity can be a temporary symptom of exposed dentin due to receding gums, aggressive brushing, or even temporary issues like new whitening treatments. However, persistent or worsening sensitivity to hot, cold, or sweets should always be evaluated by a dentist, as it can be an early indicator of enamel erosion, caries, a crack, or other underlying dental problems that require attention.
Q6: How much does enamel restoration typically cost, and is it covered by insurance?
A: Costs vary significantly. For minor enamel issues or early caries:
- Fluoride Treatments: $25-$75 (often covered by insurance).
- Dental Bonding: $150-$600 per tooth.
- Composite Fillings: $100-$350 per tooth. Many basic restorative treatments like fillings and bonding are typically covered by dental insurance at 50-80% after a deductible. For more extensive damage requiring veneers ($900-$2,500+ per tooth) or crowns ($800-$3,000+ per tooth), insurance coverage may be 25-50% for medically necessary procedures, but often less or none for purely cosmetic cases. It's crucial to check with your specific insurance provider for details.
Q7: What alternatives exist if I don't want a filling or crown?
A: Alternatives depend on the severity of the damage. For very early enamel demineralization (pre-cavity lesions), your dentist might recommend remineralization strategies like high-strength fluoride applications, specialized pastes, and strict dietary changes. For minor chips or cosmetic improvements, dental bonding is a less invasive alternative to veneers or crowns. However, for established caries or significant structural loss, restorative treatments like fillings, onlays, or crowns are usually necessary to prevent further decay, pain, and eventual tooth loss. Delaying necessary treatment can lead to more extensive and costly procedures in the future.
When to See a Dentist
Given enamel's vital role and inability to regenerate, knowing when to seek professional dental care is crucial.
Emergency Signs (See a dentist immediately):
- Sudden, severe tooth pain that persists or is unbearable, especially if accompanied by swelling or fever.
- A broken or chipped tooth where a large piece of enamel (or other tooth structure) has fractured off, exposing dentin or causing sharp edges.
- Acute sensitivity that suddenly becomes extreme and doesn't subside.
Routine Care (Schedule an appointment as soon as possible):
- Persistent tooth sensitivity: If you experience ongoing discomfort to hot, cold, sweet, or acidic foods/drinks.
- Visible changes to your teeth: Noticing yellowing, transparency at the edges, rough spots, pits, grooves, or "cupping" on chewing surfaces.
- New cracks or small chips that develop on your teeth.
- Pain when chewing or biting down.
- Bleeding or tender gums alongside any of the above, as it could indicate gum recession exposing tooth roots, which lack enamel.
- If you suspect you grind your teeth (bruxism) or have been diagnosed with conditions like GERD that can impact dental health.
- Regular check-ups: Even without symptoms, everyone should visit their dentist every six months for a professional cleaning and examination. Early detection is key to preventing minor enamel issues from becoming major problems.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.