Sensitivity
4,779 words · 16 min read
Quick Definition
A sharp, temporary pain in one or more teeth triggered by hot, cold, sweet, acidic, or air stimuli. Also called dentin hypersensitivity, it occurs when dentin or tooth roots become exposed.
Sensitivity
Sensitivity refers to a sharp, temporary pain in one or more teeth triggered by specific stimuli such as hot, cold, sweet, acidic foods and drinks, or even air. Also widely known as dentin hypersensitivity, this common dental condition occurs when the underlying layer of your tooth, called dentin, or the tooth roots become exposed. When dentin, which contains thousands of microscopic tubules leading to the tooth's nerve, loses its protective covering, these tubules allow external stimuli to reach the nerve, causing a sudden jolt of pain.
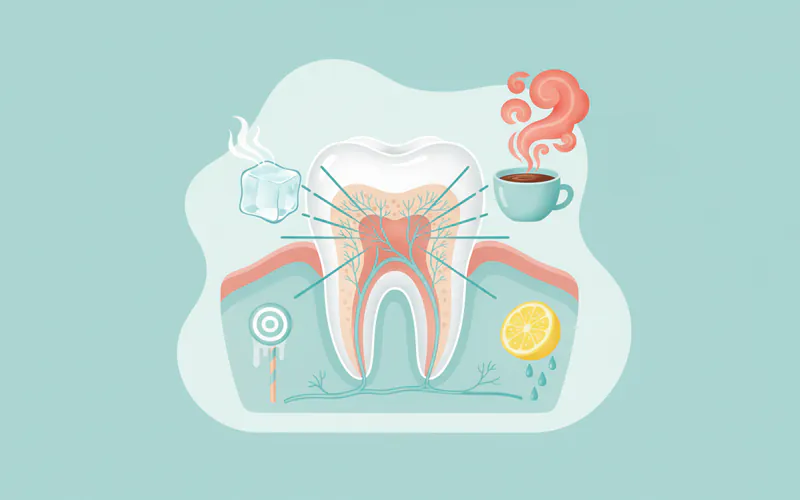
This condition is more than just an annoyance; it's a signal from your body that something is amiss with your oral health. While often manageable with simple interventions, persistent or severe sensitivity can indicate a more serious underlying problem that requires professional attention. Understanding what causes sensitivity, how to prevent it, and the available treatment options is crucial for maintaining optimal dental health and a comfortable daily life. It's an incredibly common issue, affecting a significant portion of the adult population in the US. Estimates suggest that between 30% and 40% of adults experience tooth sensitivity at some point, with prevalence often peaking in individuals between 20 and 50 years old. This makes "sensitivity dental" a prevalent concern, driving many to search "what is sensitivity" to find solutions and understanding.
Key Takeaways:
- Sensitivity (dentin hypersensitivity) is a sharp, temporary tooth pain from exposed dentin.
- It's triggered by hot, cold, sweet, acidic stimuli, or air.
- Affects 30-40% of US adults, most commonly between ages 20-50.
- Can be caused by gum recession, aggressive brushing, acidic diet, bruxism, or dental procedures.
- Manageable with home care, but persistent pain requires professional diagnosis and treatment.
- Early intervention is key to prevent worsening issues and restore comfort.
Types and Classifications
Tooth sensitivity primarily falls under the umbrella of dentin hypersensitivity, but it can manifest in various ways and be classified by its origin or duration:
- Dentin Hypersensitivity: This is the most common type, characterized by short, sharp pain resulting from exposed dentin. It's non-spontaneous, meaning it's only felt when a specific trigger is present, unlike the throbbing pain of an infection.
- Root Sensitivity: A specific form of dentin hypersensitivity where the tooth roots, which are naturally covered by gingiva (gum tissue), become exposed due to gum recession. Root surfaces lack the protective enamel layer, making them highly susceptible to sensitivity.
- Post-Treatment Sensitivity: Some individuals experience temporary sensitivity following dental procedures like fillings, crowns, root planing, scaling, or professional teeth whitening. This is usually due to temporary inflammation or irritation of the tooth nerve and typically resolves within a few days or weeks.
- Cracked Tooth Syndrome: Sensitivity, particularly when biting or releasing pressure, can be a symptom of a tiny crack in a tooth that isn't visible to the naked eye. The crack allows stimuli to reach the dentin and nerve.
- Reversible Pulpitis: This refers to mild, temporary inflammation of the tooth pulp (the innermost part of the tooth containing nerves and blood vessels). It often presents as sensitivity to cold and is typically caused by minor decay, recent dental work, or trauma. It's "reversible" because the pulp can heal if the cause is addressed.
- Irreversible Pulpitis: More severe and persistent sensitivity, often spontaneous or prolonged after a stimulus, can indicate irreversible damage or infection of the pulp, typically requiring a root canal or extraction. While sensitivity is a symptom, the underlying issue is pulp inflammation, not just exposed dentin.
Causes and Risk Factors
Understanding the root causes of sensitivity is crucial for effective prevention and treatment. Multiple factors can contribute to exposed dentin or an irritated tooth nerve:
-
Receding Gums (Gingival Recession): This is one of the most significant causes. When the gingiva (gum tissue) pulls away from the tooth, it exposes the underlying root surface. Unlike the crown of the tooth, which is protected by tough enamel, the root surface is covered by a much softer material called cementum, which wears away easily, exposing the dentin. Receding gums can be caused by:
- Aggressive Toothbrushing: Brushing too hard or using a hard-bristled toothbrush can wear down enamel and gum tissue over time.
- Periodontal Disease (Gum Disease): Inflammation and infection of the gums and supporting bone can lead to gum recession and bone loss.
- Genetics: Some individuals are genetically predisposed to thinner gum tissue.
- Tobacco Use: Smoking and chewing tobacco are major risk factors for gum disease and recession.
- Orthodontic Treatment: In some cases, tooth movement can cause minor gum recession.
-
Enamel Erosion: The gradual wearing away of enamel, the outermost protective layer of the tooth, exposes the sensitive dentin underneath. Common causes include:
- Acidic Foods and Drinks: Frequent consumption of highly acidic beverages (soda, sports drinks, fruit juices) and foods (citrus fruits, pickles, vinegar) can dissolve enamel.
- Acid Reflux (GERD): Stomach acids can repeatedly reach the mouth, eroding enamel.
- Eating Disorders: Frequent vomiting exposes teeth to stomach acid, leading to rapid enamel erosion.
-
Bruxism (Teeth Grinding or Clenching): Chronic grinding or clenching of teeth, often during sleep, can wear down enamel, exposing dentin. It can also cause tiny cracks in teeth, which can lead to sensitivity. Bruxism puts immense pressure on teeth, leading to fractures and gum recession.
-
Tooth Decay (Cavities): A cavity is a hole in the enamel that exposes the dentin to bacteria and stimuli, causing localized sensitivity.
-
Cracked or Chipped Teeth: Trauma, bruxism, or biting on hard objects can create cracks in teeth. These cracks can extend into the dentin, allowing stimuli to reach the nerve.
-
Worn Fillings: Old or leaky fillings can allow bacteria and stimuli to penetrate the tooth.
-
Dental Procedures:
- Teeth Whitening: Bleaching agents can temporarily increase tooth permeability, leading to short-term sensitivity. This usually subsides within a few days.
- Recent Dental Work (Fillings, Crowns, Scaling, Root Planing): It's common to experience temporary sensitivity after these procedures as the tooth's nerve may be irritated, or gum tissue might be healing.
-
Over-the-Counter Whitening Products: Some whitening toothpastes and strips can be abrasive or contain ingredients that increase temporary sensitivity.
Signs and Symptoms to Watch For
The hallmark of tooth sensitivity is a specific type of pain that is distinct from a dull toothache or the constant throbbing of an infection. Look for these signs:
- Sharp, Sudden, and Temporary Pain: The pain typically appears immediately after contact with a trigger and quickly fades once the trigger is removed. It's often described as a "zing," "jolt," or "electric shock."
- Trigger-Specific Pain: The pain is reliably caused by certain stimuli:
- Cold: Ice water, cold air, ice cream, popsicles. This is one of the most common triggers.
- Hot: Hot coffee, tea, soup.
- Sweet: Candies, chocolates, sugary drinks.
- Acidic: Citrus fruits, vinegar-based dressings, sodas.
- Air: Inhaling cold air through the mouth, especially in winter.
- Brushing/Flossing: Sometimes even the mechanical action of cleaning can trigger pain in sensitive areas.
- Localized or Generalized: Sensitivity can affect just one tooth, a few teeth, or even multiple teeth across the mouth, depending on the underlying cause. Root sensitivity, for example, often affects several teeth with exposed roots.
- Pain Location: The pain is usually felt at the gumline where root exposure is common, or within the body of a tooth with enamel erosion or a cavity.
- Absence of Spontaneous Pain: Unlike a deep infection, sensitivity typically does not cause pain that arises without any external trigger.
It’s important to distinguish this from the persistent, throbbing pain that suggests a deeper infection or abscess, which requires immediate dental care.
Diagnosis Process — What Your Dentist Does
When you report tooth sensitivity, your dentist will conduct a thorough examination to determine the exact cause and rule out more serious conditions. The diagnostic process typically involves:
- Detailed Medical and Dental History: Your dentist will ask about your symptoms, including when the pain started, what triggers it, how long it lasts, your dietary habits (especially acidic food/drink intake), oral hygiene routine, and any recent dental work or trauma. They will also inquire about habits like bruxism.
- Visual Oral Examination: Your dentist will carefully inspect your teeth and gums for:
- Gum Recession: Looking for areas where the gingiva has pulled away from the tooth, exposing the root surface.
- Enamel Erosion: Identifying signs of wear on the tooth surfaces.
- Cavities: Checking for signs of tooth decay.
- Cracked or Chipped Teeth: Visually examining teeth for any visible fractures or damage.
- Worn Fillings or Restorations: Assessing the integrity of existing dental work.
- Signs of Bruxism: Looking for flattened or chipped tooth surfaces, or wear facets.
- Probing: A dental probe may be used to gently check for gum recession or areas of exposed root surface, and to measure gum pockets, which can indicate gum disease.
- Tactile Test: The dentist may gently tap or scratch the sensitive area with a dental instrument (explorer) to see if it elicits pain, helping to pinpoint exposed dentin.
- Thermal Tests:
- Cold Test: A common diagnostic tool involves applying a blast of cold air, a cotton swab dipped in cold water, or a specialized cold spray to the suspected tooth. The response (intensity and duration of pain) helps determine the extent of sensitivity and differentiate it from pulpitis.
- Hot Test: Less common for sensitivity diagnosis, but may be used to rule out pulp inflammation or nerve damage.
- Percussion Test: Tapping lightly on the tooth to check for pain, which can indicate inflammation of the ligament surrounding the tooth root or a cracked tooth.
- Bite Test: Asking you to bite down on a cotton roll or specialized biting stick can help identify a cracked tooth, as pain often occurs when releasing the bite.
- Dental X-rays: Radiographs are crucial for identifying issues that aren't visible during a visual exam, such as:
- Cavities between teeth or under existing fillings.
- Bone loss due to periodontal disease.
- Impacted teeth or other structural anomalies.
- Infections or abscesses at the tooth root.
``
Treatment Options with Pros, Cons, and Costs
Treatment for sensitivity depends entirely on the underlying cause. Your dentist will recommend the most appropriate solution based on their diagnosis.
1. At-Home Treatments
- Desensitizing Toothpaste:
- Mechanism: Contains compounds like potassium nitrate (which calms nerve endings) or stannous fluoride/strontium chloride (which block dentin tubules).
- Pros: Non-invasive, affordable, readily available, effective for mild to moderate sensitivity, can be used long-term for prevention.
- Cons: Takes 2-4 weeks of consistent use to show results, not effective for severe sensitivity or underlying structural issues.
- Cost: $5-$20 per tube.
- Soft-Bristled Toothbrush and Gentle Brushing Technique:
- Mechanism: Prevents further enamel abrasion and gum recession.
- Pros: Essential for preventing worsening sensitivity and maintaining gum health, no additional cost beyond regular toothbrush.
- Cons: Requires conscious effort to change brushing habits.
- Cost: $3-$15 for a soft toothbrush.
- Dietary Modifications:
- Mechanism: Reducing consumption of acidic foods and drinks minimizes enamel erosion.
- Pros: Non-invasive, beneficial for overall health.
- Cons: Requires dietary discipline.
- Cost: No direct cost, potentially cost-saving.
- Fluoride Mouthwash:
- Mechanism: Strengthens enamel and can help desensitize teeth over time.
- Pros: Easy to incorporate into routine, good for overall oral health.
- Cons: Less potent than professional fluoride treatments.
- Cost: $5-$15 per bottle.
2. In-Office Treatments
- Professional Fluoride Varnish/Gel:
- Mechanism: Applied by the dentist, this highly concentrated fluoride strengthens enamel and blocks dentin tubules.
- Pros: Quick application, immediate relief for some, stronger than OTC fluoride.
- Cons: Temporary relief (may need reapplication every 3-6 months), minor temporary tooth discoloration.
- Cost: $25-$75 per application (often covered by insurance).
- Dental Bonding or Sealants:
- Mechanism: A tooth-colored resin material is applied to cover exposed root surfaces or areas of enamel erosion, effectively sealing the dentin tubules.
- Pros: Effective for localized sensitivity, durable for several years, cosmetic improvement.
- Cons: Can chip or wear over time, may require replacement.
- Cost: $100-$400 per tooth.
- Gum Graft Surgery:
- Mechanism: For significant gum recession, healthy gum tissue is taken from another part of your mouth (or a donor source) and surgically placed over exposed roots.
- Pros: Permanently covers exposed roots, resolves sensitivity caused by recession, improves aesthetics.
- Cons: Surgical procedure, longer recovery time, higher cost, potential for discomfort post-op.
- Cost: $600-$1200+ per tooth, depending on the type of graft and complexity.
- In-Office Desensitizing Agents:
- Mechanism: Dentists can apply specialized agents like oxalate, glutaraldehyde, or specific bonding agents that immediately block dentin tubules.
- Pros: Immediate relief, targeted application.
- Cons: May require repeat applications, less permanent than bonding.
- Cost: Varies, often included as part of a general cleaning or minor restorative procedure, or $50-$150 if a standalone service.
- Crown or Inlay/Onlay:
- Mechanism: If sensitivity is due to a large cavity, crack, or severe enamel loss, a crown (full tooth cap) or inlay/onlay (partial crown) can restore the tooth's structure and protect the underlying dentin and nerve.
- Pros: Provides comprehensive protection, restores function and aesthetics, durable.
- Cons: More invasive and costly, requires multiple appointments.
- Cost: $800-$2,500+ per tooth for a crown; $600-$1,500+ for an inlay/onlay.
- Root Canal Treatment:
- Mechanism: If severe sensitivity is caused by irreversible pulp inflammation or infection, a root canal removes the infected pulp (nerve tissue) from inside the tooth, effectively eliminating the pain source.
- Pros: Highly effective for severe, persistent nerve pain, saves the natural tooth.
- Cons: More invasive procedure, higher cost, requires subsequent crown placement to protect the treated tooth.
- Cost: $700-$2,000+ for an anterior tooth; $1,000-$2,500+ for a molar (before crown).
- Nightguard (for Bruxism):
- Mechanism: A custom-fitted acrylic appliance worn during sleep protects teeth from grinding and clenching forces, preventing enamel wear and potential cracks.
- Pros: Prevents further tooth damage, reduces muscle strain.
- Cons: Requires consistent use, initial adjustment period.
- Cost: $300-$800 for a custom nightguard from a dentist (OTC versions $20-$100 but less effective).
``
Step-by-step: What to Expect During Treatment
Let's look at common in-office treatments:
- Fluoride Varnish Application:
- Preparation: Your teeth are cleaned and dried.
- Application: The dentist or hygienist uses a small brush to paint a thin layer of fluoride varnish onto the sensitive areas, often at the gumline.
- Drying: The varnish dries quickly, often with a slightly tacky or yellowish appearance initially.
- Aftercare: You'll be advised to avoid eating, drinking, or brushing for a short period (30 minutes to a few hours) to allow the fluoride to absorb. You might be asked to avoid hot drinks or alcohol for the rest of the day.
- Dental Bonding for Exposed Roots:
- Preparation: The tooth surface is gently cleaned, and a mild etching solution is applied for a few seconds to create a microscopic texture for better bond adhesion.
- Bonding Agent: A liquid bonding agent is applied, acting as a primer.
- Composite Resin: A tooth-colored composite resin (a plastic material) is meticulously applied to the exposed root surface, covering the dentin.
- Shaping and Curing: The dentist carefully shapes the resin to blend seamlessly with your tooth, then uses a special blue light to harden (cure) the material.
- Polishing: The bonded area is polished for a smooth, natural finish.
- Gum Graft Surgery:
- Anesthesia: Local anesthesia is administered to numb the treatment area. You might also receive sedation.
- Tissue Collection (if applicable): If using your own tissue, a small piece of gum tissue is carefully removed from the roof of your mouth or another donor site.
- Recipient Site Preparation: The exposed root surface is cleaned, and a small flap is created in the existing gum tissue to receive the graft.
- Graft Placement: The donor tissue is precisely placed over the exposed root and secured with tiny sutures.
- Dressing: A protective dressing may be placed over the surgical site.
- Recovery: Detailed post-operative instructions will be provided, including pain management, dietary restrictions, and oral hygiene guidelines.
Recovery Timeline and Aftercare
Recovery timelines vary significantly based on the treatment:
- Desensitizing Toothpaste/Fluoride Mouthwash: No recovery time. Continue daily use.
- Professional Fluoride Varnish: No downtime. Avoid brushing/eating for a short period as advised.
- Dental Bonding/Sealants: No downtime. Avoid hard or sticky foods for the first 24-48 hours to ensure the bond sets completely. Maintain good oral hygiene.
- Gum Graft Surgery:
- Initial Discomfort: Expect some soreness, swelling, and minor bleeding for the first few days. Pain medication will be prescribed.
- Diet: Soft diet for 1-2 weeks.
- Oral Hygiene: Special instructions for cleaning the surgical site will be given (e.g., specific mouth rinses, avoiding brushing the area).
- Full Healing: Takes several weeks to months for complete tissue integration.
- Crown/Inlay/Onlay: Some temporary sensitivity after placement is normal. Avoid very hard or sticky foods initially.
- Root Canal Treatment: Tooth may be sensitive for a few days. The tooth usually requires a crown within a few weeks to months for full protection and restoration.
General Aftercare for Sensitivity:
- Maintain Excellent Oral Hygiene: Gentle but thorough brushing with a soft-bristled brush, flossing daily.
- Use Desensitizing Products: Continue using desensitizing toothpaste as a preventive measure if recommended.
- Avoid Triggers: Limit highly acidic foods and drinks, and be mindful of extreme hot/cold stimuli.
- Regular Dental Check-ups: Essential for monitoring the treated area and catching any new issues early.
Prevention Strategies
Preventing tooth sensitivity often involves adopting better oral hygiene habits and making conscious lifestyle choices:
- Brush Gently: Use a soft-bristled toothbrush and a gentle, circular motion. Avoid aggressive scrubbing, especially along the gumline. Electric toothbrushes with pressure sensors can be helpful.
- Use Fluoride Toothpaste: Opt for a desensitizing or fluoride toothpaste to strengthen enamel and block dentin tubules.
- Limit Acidic Foods and Drinks: Reduce consumption of sodas, sports drinks, fruit juices, citrus fruits, and other acidic items that erode enamel. If consumed, rinse your mouth with water immediately afterward.
- Wait to Brush After Acidic Intake: After consuming acidic foods or drinks, wait at least 30 minutes before brushing. Acid softens enamel, and brushing immediately can cause further erosion.
- Address Bruxism: If you grind or clench your teeth, especially at night, talk to your dentist about a custom-fitted nightguard to protect your teeth from excessive wear.
- Treat Gum Disease: Regular dental cleanings and proper at-home care are crucial for preventing and managing gum disease, which can lead to gum recession and exposed roots.
- Regular Dental Check-ups and Cleanings: Professional cleanings remove plaque and tartar buildup, and your dentist can spot early signs of gum recession, enamel erosion, or decay before sensitivity becomes severe.
- Avoid Over-the-Counter Whitening Products: If you have a history of sensitivity, consult your dentist before using whitening toothpastes or strips, as they can exacerbate the problem. Professional whitening supervised by a dentist is often a safer option.
Cost Ranges in the US (with/without insurance)
The cost of treating sensitivity varies widely based on the cause, complexity, and type of treatment. Insurance coverage also plays a significant role. Here are general estimated ranges in the US:
| Treatment Type | Average Cost (without insurance) | Average Cost (with insurance coverage) | Notes |
|---|---|---|---|
| Desensitizing Toothpaste | $5 - $20 | N/A (OTC product) | Daily use product. |
| Soft-Bristled Toothbrush | $3 - $15 | N/A (OTC product) | Essential preventive tool. |
| Professional Fluoride Varnish | $25 - $75 per application | $0 - $30 per application | Often covered under preventive care. |
| Dental Bonding (for exposed roots) | $100 - $400 per tooth | $50 - $200 per tooth | Coverage varies (restorative vs. cosmetic). |
| In-Office Desensitizing Agents | $50 - $150 per application | $0 - $75 per application | May be bundled with other services. |
| Custom Nightguard (for Bruxism) | $300 - $800 | $100 - $400 | Coverage varies (preventive vs. major restorative). |
| Gum Graft Surgery | $600 - $1,200+ per tooth | $300 - $800+ per tooth | Often considered a major procedure, coverage varies. |
| Dental Crown | $800 - $2,500+ per tooth | $400 - $1,200+ per tooth | Usually covered as a major restorative procedure. |
| Root Canal Treatment | $700 - $2,500+ per tooth | $350 - $1,200+ per tooth | Varies by tooth (front vs. molar). Followed by a crown. |
Note: These are general ranges, and actual costs can vary based on your location, the dentist's fees, and your specific insurance plan. It's always best to get a detailed cost estimate from your dentist before proceeding with any major treatment.
Comparison Table: Common Sensitivity Treatments
| Feature | Desensitizing Toothpaste | Professional Fluoride Varnish | Dental Bonding (Exposed Roots) | Gum Graft Surgery | Root Canal Treatment |
|---|---|---|---|---|---|
| Mechanism | Blocks tubules, calms nerves | Strengthens enamel, blocks tubules | Covers exposed dentin | Covers exposed roots with tissue | Removes infected nerve |
| Severity | Mild to moderate | Mild to moderate | Moderate to severe (localized) | Severe (due to recession) | Severe (irreversible pulpitis) |
| Invasiveness | None (OTC) | Non-invasive | Minimally invasive | Surgical procedure | Moderately invasive |
| Pain Relief | Gradual (weeks) | Quick, temporary | Quick, durable | Gradual, permanent for recession | Immediate & permanent for nerve pain |
| Duration of Effect | Ongoing with use | 3-6 months | Several years | Permanent (if successful) | Permanent (saves tooth) |
| Cost Range (US) | $5-$20 | $25-$75 | $100-$400 | $600-$1,200+ | $700-$2,500+ |
| Pros | Affordable, easy, preventive | Quick, effective, covered | Durable, cosmetic, targeted | Permanent solution for recession | Saves tooth, eliminates severe pain |
| Cons | Not for severe cases, takes time | Temporary, minor temporary stain | Can chip/wear, not for widespread pain | Surgical, costly, recovery time | Costly, requires crown, invasive |
For Parents / Pediatric Considerations
Children can also experience tooth sensitivity, though the causes and approaches might differ from adults.
- Common Causes in Children:
- New Permanent Teeth: Newly erupted permanent teeth, especially molars, sometimes have very thin enamel initially, leading to temporary sensitivity.
- Cavities: Decay is a leading cause of sensitivity in children, as it exposes the dentin.
- Enamel Hypoplasia: A developmental defect where enamel doesn't form properly, leaving thin or weak spots.
- Dental Trauma: Chipped or cracked teeth from falls or sports injuries can cause sensitivity.
- Aggressive Brushing: While less common, improper brushing can contribute.
- Acidic Diet: High consumption of sugary and acidic drinks/candies is a major contributor to enamel erosion and cavities.
- Signs to Watch For: Children may not articulate "sensitivity" well. Look for grimacing or pulling away when eating cold foods, refusing certain drinks, or complaining of pain while brushing.
- Pediatric Diagnosis: A pediatric dentist will use similar diagnostic tools as with adults, but with a child-friendly approach. X-rays are often crucial for detecting hidden cavities.
- Treatment for Children:
- Fluoride Varnish: A common and effective treatment for strengthening enamel and reducing sensitivity.
- Dental Sealants: Applied to the chewing surfaces of molars to prevent cavities, which in turn prevents sensitivity.
- Fillings: For cavities, fillings restore the tooth's structure.
- Education: Teaching proper, gentle brushing techniques and encouraging a balanced diet low in acidic and sugary items is paramount.
- Mouthguards: For children involved in sports to prevent dental trauma that could lead to chips or cracks. Parents should consult a pediatric dentist promptly if their child complains of tooth sensitivity, as early intervention can prevent more serious problems.
Frequently Asked Questions
What is the typical cost for sensitivity treatment in the US?
The cost varies significantly based on the cause and treatment. Over-the-counter desensitizing toothpastes range from $5-$20. In-office fluoride treatments are typically $25-$75. More involved treatments like dental bonding can be $100-$400 per tooth, while gum graft surgery can range from $600-$1,200+ per tooth. Root canals, for severe nerve issues, range from $700-$2,500+.
How much pain should I expect during sensitivity treatment?
Most common treatments for sensitivity are minimally uncomfortable or painless. Fluoride varnish application is quick and involves no pain. Dental bonding requires numbing if the area is very sensitive, but the procedure itself is typically comfortable. Surgical procedures like gum grafts or root canals involve local anesthesia to ensure you are numb during the procedure; you might experience some soreness or discomfort during recovery, managed with pain medication.
How long does it take for sensitivity to go away after treatment?
For at-home desensitizing toothpastes, it usually takes 2-4 weeks of consistent use to notice significant improvement. Professional fluoride applications can offer immediate relief for some, but it may take a few days. Dental bonding or sealants provide relief as soon as they are placed. For surgical treatments like gum grafts, the sensitivity directly related to exposed roots should resolve once healing is complete, which can take several weeks to months. If sensitivity is due to a cavity or infection, it resolves once the underlying issue is treated.
Are there any natural or alternative treatments for tooth sensitivity?
While not scientifically proven as definitive treatments, some people explore natural remedies like oil pulling (swishing oil around the mouth), using saltwater rinses, or applying clove oil. However, these are generally not recommended as primary treatments for dentin hypersensitivity, which often has a clear physiological cause. For lasting relief and to address the root cause, professional dental care is crucial. Always consult your dentist before relying on alternative treatments.
Does dental insurance cover sensitivity treatments?
Coverage varies by plan and the type of treatment. Preventive treatments like professional fluoride applications are often fully or partially covered. Restorative procedures like dental bonding for exposed roots, crowns, or root canals are typically covered, but usually at a percentage (e.g., 50-80%) after a deductible. Gum graft surgery, often considered a major procedure, may have higher out-of-pocket costs even with insurance. It's essential to check with your insurance provider and get a pre-treatment estimate from your dentist.
Can sensitivity be a sign of something more serious?
Yes, absolutely. While often benign, sensitivity can be an early indicator of serious issues like a progressing cavity, a cracked tooth, severe gum disease leading to significant root exposure, or even an infection in the tooth's pulp (nerve). Persistent, severe, or spontaneous sensitivity that doesn't resolve with at-home care warrants immediate dental attention to rule out these more serious underlying conditions.
When to See a Dentist
While occasional, mild sensitivity that responds to desensitizing toothpaste might not always require an immediate visit, there are clear situations when professional dental evaluation is crucial:
- Persistent or Worsening Pain: If your sensitivity doesn't improve after 1-2 weeks of using desensitizing toothpaste, or if it gets worse, it's time to see your dentist.
- Spontaneous Pain: If you experience tooth pain that arises without any obvious trigger (hot, cold, sweet, etc.), it could indicate a more serious issue like pulp inflammation or infection.
- Prolonged Pain: If the pain lingers for more than a few seconds after the trigger is removed, this is a red flag for potential nerve damage or infection.
- Localized Pain: If the sensitivity is focused on a single tooth and is severe, it could indicate a deep cavity, crack, or abscess.
- Pain with Biting: If you experience pain specifically when biting down or releasing pressure, it could be a sign of a cracked tooth.
- Visible Issues: If you notice new cracks, chips, swelling around a tooth, or significant gum recession.
- Concerns about OTC Whitening: If you experience severe sensitivity after using at-home whitening products.
Don't wait if the pain is severe, constant, or accompanied by swelling, fever, or a foul taste in your mouth. These could be signs of an emergency dental situation requiring immediate care. Even if it's "just" sensitivity, getting a professional diagnosis ensures you address the root cause and prevent minor issues from becoming major problems.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.