Bruxism
4,753 words · 16 min read
Quick Definition
The involuntary grinding, clenching, or gnashing of teeth, often occurring during sleep. Bruxism can cause tooth wear, jaw pain, headaches, and damage to dental restorations.
Welcome to SmilePedia, your ultimate resource for understanding key dental health conditions. Today, we delve into Bruxism, a condition far more common and impactful than many realize. Often dismissed as a mere habit, bruxism is a serious dental and medical concern that can lead to significant oral health problems, chronic pain, and diminished quality of life.
At its core, bruxism is the involuntary grinding, clenching, or gnashing of teeth, often occurring during sleep (sleep bruxism) but can also happen subconsciously while awake (awake bruxism). This repetitive activity places immense, unnatural forces on the teeth, jaw muscles, and the intricate Temporomandibular Joint (TMJ) system, which connects your jaw to your skull. Unlike the controlled forces of chewing, bruxing can exert pressures many times greater, leading to a cascade of issues including severe tooth wear, fractures, jaw pain-jaw-disorders-everything-you-need-to-know "Complete Guide to TMJ & Jaw Disorders: Everything You Need to Know"), headaches, and damage to existing dental restorations like fillings, crowns, and veneers. Understanding bruxism is the first step toward managing its effects and preserving your oral health for years to come.
Bruxism affects a significant portion of the population across all age groups. Estimates suggest that 8-31% of the general population experiences bruxism, with prevalence rates fluctuating based on age and specific populations studied. Children are also frequently affected, with up to 15% of children exhibiting bruxism, although it often resolves spontaneously as they grow. Due to its often silent and subconscious nature, many individuals are unaware they have bruxism until a dental professional identifies the tell-tale signs or a partner points out the characteristic grinding sounds during sleep. Recognizing the symptoms early and seeking professional guidance is crucial to mitigate its destructive potential.
Key Takeaways:
- Bruxism is the involuntary grinding or clenching of teeth, occurring both awake and during sleep.
- It's a common condition, affecting 8-31% of adults and up to 15% of children.
- Consequences include tooth wear, fractures, jaw pain, headaches, and damage to dental work.
- Stress, anxiety, sleep disorders, and certain medications are major risk factors.
- Diagnosis often involves a dental exam and patient history; sleep studies may be used for severe cases.
- Treatment ranges from oral appliances (nightguards) to stress management, medications, and dental corrections.
Detailed Explanation
Bruxism is a complex condition, categorized by its timing, origin, and presentation. Understanding these distinctions is key to effective diagnosis and treatment.
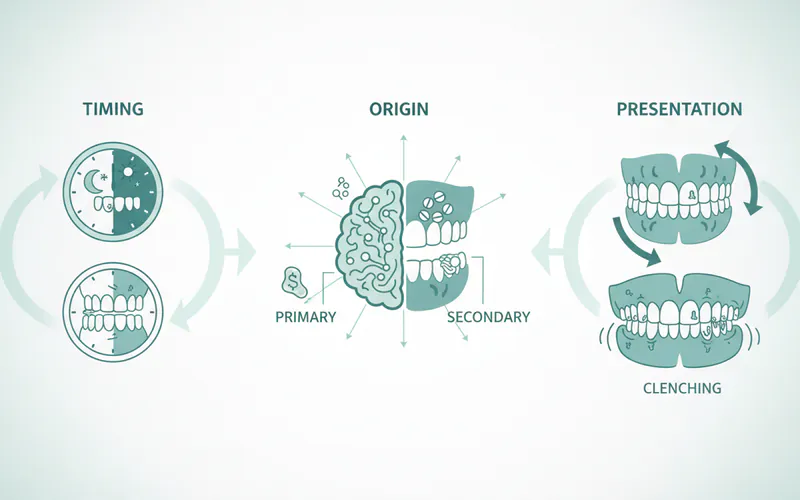
Types and Classifications of Bruxism
Bruxism is primarily classified into two main types:
- Sleep Bruxism (Nocturnal Bruxism): This is the more commonly recognized form, characterized by repetitive muscle activity during sleep, often involving clenching or grinding. It’s considered a sleep-related movement disorder, much like restless leg syndrome, and can often coincide with other sleep disorders, particularly sleep apnea. Individuals with sleep bruxism are often unaware of their condition until a sleep partner reports grinding sounds or a dentist identifies the physical signs.
- Awake Bruxism (Diurnal Bruxism): This involves involuntary clenching or bracing of the teeth while a person is awake. Unlike sleep bruxism, grinding sounds are rare. Instead, it's characterized by sustained or intermittent jaw clenching, often in response to stress, concentration, or even while driving or exercising. Because it's a conscious (though involuntary) activity, individuals might be more aware of the habit, though still struggle to control it.
Further classifications include:
- Primary Bruxism: When bruxism occurs without an identifiable underlying medical or psychological condition.
- Secondary Bruxism: When bruxism is a symptom or side effect of another condition, such as certain medications, neurological disorders, or other sleep disorders.
Causes and Risk Factors
The exact cause of bruxism is often multifactorial, meaning several factors can contribute to its development.
- Stress and Anxiety: This is arguably the most common culprit. High-stress levels, anxiety, anger, frustration, or tension can manifest as physical clenching or grinding, particularly during sleep. Chronic emotional distress can prime the jaw muscles for constant tension.
- Sleep Disorders: Sleep bruxism is often linked to other sleep-related issues. Obstructive Sleep Apnea (OSA), a condition where breathing repeatedly stops and starts during sleep, has a strong correlation with bruxism. Other sleep disturbances, such as snoring or periodic limb movement disorder, can also be associated.
- Medications: Certain medications can have bruxism as a side effect. Antidepressants, particularly selective serotonin reuptake inhibitors (SSRIs) like fluoxetine (Prozac) and paroxetine (Paxil), are well-known for potentially inducing or exacerbating bruxism. Other drugs, including some antipsychotics and stimulants, can also be implicated.
- Lifestyle Factors: Regular consumption of caffeine, alcohol, and nicotine (smoking) can increase the risk of bruxism. These substances act as stimulants, affecting the central nervous system and potentially disrupting sleep patterns and muscle activity.
- Dental Factors (Malocclusion): While once considered a primary cause, the role of malocclusion (a misaligned bite or "bad bite") in bruxism is now debated. Some theories suggest that an uneven bite or specific tooth interferences might trigger grinding as the jaw attempts to find a comfortable position. However, many individuals with malocclusion do not brux and many bruxers have perfect occlusion. Most dental professionals now consider malocclusion a minor contributing factor, if at all, to the initiation of bruxism, though it can influence where the damage occurs.
- Genetics: There appears to be a hereditary component to bruxism. Individuals with a family history of bruxism are more likely to develop it themselves, suggesting a genetic predisposition.
- Age: While bruxism can affect anyone, it is particularly common in children and young adults, often decreasing in prevalence with age.
Signs and Symptoms to Watch For
The signs and symptoms of bruxism can vary widely in severity and presentation. Because sleep bruxism often goes unnoticed by the individual, it's important to be aware of the following indicators:
- Tooth Wear and Damage: This is one of the most definitive signs. Teeth may appear flattened, chipped, fractured, or excessively worn, especially the biting surfaces of molars and premolars. Enamel erosion can expose the underlying dentin, leading to tooth sensitivity. In severe cases, tooth mobility or even tooth loss can occur.
- Jaw Pain and Soreness: A common complaint, often worse in the morning for sleep bruxers. The muscles involved in chewing (masseter and temporalis muscles) can become fatigued, tender, and painful.
- Headaches: Tension-type headaches, particularly those originating in the temples or forehead, are frequently associated with bruxism due to sustained muscle tension.
- Facial Pain: General soreness or tightness in the face, especially around the cheeks and temples.
- Earaches: Though not a primary ear problem, the proximity of the jaw joint (TMJ) to the ear can lead to referred pain that mimics an earache.
- TMJ Disorders: Chronic clenching and grinding place immense stress on the Temporomandibular Joint (TMJ). This can lead to TMJ dysfunction (TMD), characterized by clicking, popping, or grinding sounds in the jaw joint, limited jaw opening, or the jaw getting "locked" in an open or closed position.
- Tooth Sensitivity: Exposed dentin from enamel wear can make teeth highly sensitive to hot, cold, sweet, or acidic foods and drinks.
- Receding Gums and Abfractions: The extreme forces can cause gum tissue to recede and lead to abfractions, which are V-shaped or wedge-shaped notches at the gum line of teeth.
- Indentations on the Tongue or Cheek: The pressure from clenching can cause the tongue to press against the teeth, leaving scalloped edges, or cause indentations on the inside of the cheeks.
- Damaged Dental Restorations: Fillings can chip, crowns can fracture, and veneers can crack or pop off due to the relentless forces of bruxism.
- Sleep Disruption: While the bruxer may not always be aware, a sleep partner might report loud grinding noises or disturbed sleep. The bruxer themselves might wake up with jaw soreness or a headache.
Diagnosis Process — What Your Dentist Does
Diagnosing bruxism typically involves a comprehensive approach by your dental professional. Since many individuals are unaware they brux, especially during sleep, the diagnosis often begins with a thorough dental examination and a detailed discussion of your symptoms and lifestyle.
- Patient History: Your dentist will ask a series of questions about:
- Any jaw pain, headaches, or facial soreness you experience.
- Tooth sensitivity.
- Difficulty chewing or opening your mouth wide.
- Any sounds a sleep partner might have noticed (grinding, clenching).
- Your stress levels, sleep quality, caffeine/alcohol consumption, and medications.
- Medical history, including any sleep disorders like sleep apnea.
- Clinical Dental Examination: Your dentist will carefully examine your mouth for the physical signs of bruxism:
- Tooth Wear: Inspecting the biting surfaces of your teeth for excessive wear, flattening, fractures, or chips.
- Gum Recession and Abfractions: Checking for signs of gum recession or wedge-shaped defects at the gumline.
- Muscle Palpation: Gently feeling your jaw muscles (masseter and temporalis) for tenderness, soreness, or hypertrophy (enlargement).
- TMJ Examination: Listening for clicking, popping, or grinding noises in your Temporomandibular Joint (TMJ) when you open and close your mouth, and assessing the range of jaw motion.
- Oral Soft Tissues: Looking for indentations on your tongue or buccal mucosa (inside of your cheeks).
- Existing Restorations: Checking for cracks or damage to fillings, crowns, or other dental work.
- Bite Assessment: Your dentist may assess your bite (occlusion) to identify any potential interferences, although as mentioned, this is generally considered a minor factor in bruxism itself.
- Imaging (Occasionally): X-rays might be taken to evaluate the bone structure around the teeth and TMJ, and to rule out other conditions.
- Referral for Sleep Study (Polysomnography): If sleep bruxism is severe, or if other sleep disorders like sleep apnea are suspected, your dentist may refer you to a sleep specialist for a polysomnography. This overnight study monitors brain activity, heart rate, breathing, oxygen levels, and jaw muscle activity (EMG) to accurately diagnose sleep bruxism and co-existing sleep disorders. While not typically the first step, it provides the most definitive diagnosis for sleep bruxism.
Treatment Options with Pros, Cons, and Costs
Treatment for bruxism is aimed at protecting teeth from damage, reducing pain, and addressing underlying causes. The best approach often involves a combination of strategies.
1. Oral Appliances (Nightguards / Occlusal Splints)
These are the most common and often first-line treatment, particularly for sleep bruxism. A custom-made nightguard is a removable acrylic appliance that fits over your upper or lower teeth, creating a physical barrier between them.
- Pros:
- Protects Teeth: Prevents direct tooth-on-tooth contact, significantly reducing wear, fractures, and damage to dental work.
- Reduces Muscle Activity: Can help relax jaw muscles and distribute forces more evenly, reducing pain and soreness.
- Custom Fit: Made by your dentist, ensuring comfort and effectiveness.
- Cons:
- Cost: Custom nightguards can be a significant upfront expense.
- Adjustment Period: Some people find them bulky or uncomfortable initially.
- Maintenance: Requires regular cleaning and occasional replacement.
- Does Not Cure: Treats symptoms and protects teeth but doesn't eliminate the underlying cause of bruxism.
- Cost Range (US):
- Custom-Made by Dentist: $300 - $800, depending on material (soft, hard, hybrid) and complexity. Some high-end appliances can exceed $1,000.
- Boil-and-Bite (OTC): $20 - $50. While cheaper, these are generally less effective, less comfortable, can shift teeth, and offer inferior protection compared to custom appliances. Not recommended for long-term use.
2. Stress Management & Behavioral Therapies
Addressing the psychological components of bruxism is crucial, especially for awake bruxism.
- Pros:
- Addresses Root Cause: Can reduce or eliminate the underlying stress and anxiety contributing to bruxism.
- Holistic Benefits: Improves overall well-being, sleep quality, and mental health.
- Non-Invasive: No physical intervention needed.
- Cons:
- Requires Commitment: Success depends on consistent effort and self-discipline.
- Delayed Results: May take time to see significant improvements.
- Cost of Therapy: Professional therapy can be expensive.
- Cost Range (US):
- Counseling/Therapy: $75 - $200+ per session, often requiring multiple sessions.
- Meditation Apps/Courses: Free - $100+ annually.
- Yoga/Exercise Classes: $10 - $30 per class or $50 - $150 per month.
3. Medications
Used short-term to manage pain or muscle spasms, or for specific underlying conditions.
- Pros:
- Quick Symptom Relief: Can temporarily alleviate pain and muscle tension.
- Targets Specific Issues: Muscle relaxants for spasms, certain antidepressants for anxiety.
- Cons:
- Temporary Solution: Does not address the root cause.
- Side Effects: Drowsiness, dizziness, dependence (for some muscle relaxants).
- Not for Long-Term Use: Most are prescribed for short durations.
- Cost Range (US): Varies widely based on medication and insurance coverage. Typically $10 - $100+ per prescription.
4. Botox Injections
Botulinum toxin (Botox) can be injected into the masseter and temporalis muscles to temporarily weaken them, reducing the force of clenching and grinding. This is an off-label use for bruxism, typically reserved for severe cases unresponsive to other treatments.
- Pros:
- Significant Force Reduction: Can dramatically decrease the intensity of clenching.
- Pain Relief: Often provides substantial relief from jaw pain and headaches.
- Temporarily Shrinks Muscles: Can reduce the appearance of a bulky jawline.
- Cons:
- Temporary: Effects last 3-6 months, requiring repeat injections.
- Cost: Very expensive and often not covered by dental or medical insurance for bruxism.
- Potential Side Effects: Temporary facial asymmetry, difficulty chewing certain foods, flu-like symptoms.
- Cost Range (US): $500 - $1,500+ per treatment, depending on the number of units used and the provider.
5. Dental Corrections
For cases where bruxism has already caused significant damage, restorative dentistry may be necessary.
- Pros:
- Restores Function and Aesthetics: Repairs damaged teeth, improving bite and appearance.
- Long-Term Solutions: Crowns, veneers, or orthodontic treatment can provide lasting results.
- Cons:
- Invasive: Involves drilling, shaping teeth, or orthodontics.
- Expensive: Often the most costly treatment option.
- Does Not Address Bruxisum: Repairs damage but doesn't prevent future grinding or clenching. A nightguard is still crucial post-treatment.
- Cost Range (US): Highly variable.
- Fillings: $100 - $400 per tooth.
- Crowns: $800 - $2,500+ per tooth.
- Orthodontics (Braces/Aligners): $3,000 - $8,000+.
Step-by-Step: What to Expect During Treatment
Let's detail the typical process for getting a custom nightguard, as it's the most common intervention.
- Initial Consultation and Diagnosis: Your dentist will examine your mouth, discuss your symptoms, and confirm the diagnosis of bruxism. They will explain why a nightguard is recommended and answer any initial questions.
- Impressions/Digital Scans: To create a custom-fit appliance, your dentist will take either traditional physical impressions of your teeth using a putty-like material or perform a digital scan with an intraoral scanner. This ensures the nightguard precisely matches your unique dental anatomy.
- Lab Fabrication: The impressions or digital files are sent to a dental laboratory, where skilled technicians craft your custom nightguard from durable acrylic materials. This process typically takes 1-2 weeks.
- Fitting Appointment: Once the nightguard is ready, you'll return for a fitting appointment. Your dentist will ensure it fits comfortably and securely, without putting undue pressure on any teeth or soft tissues. They may make minor adjustments by carefully trimming or smoothing edges. They will also check your bite with the nightguard in place.
- Instructions for Use and Care: You'll receive detailed instructions on how to insert and remove the nightguard, how often to wear it (usually every night for sleep bruxism), and how to clean and maintain it. Proper cleaning is essential to prevent bacterial buildup and odors.
- Follow-Up: A follow-up appointment is usually scheduled a few weeks after you start wearing the nightguard to assess comfort, effectiveness, and to make any further adjustments if needed. This also allows your dentist to monitor your progress and check for any continued signs of bruxism.
For other treatments like stress management, the process involves consultations with a therapist or counselor, setting goals, and practicing techniques over time. For Botox, it's a quick series of injections performed in the dental or medical office.
Recovery Timeline and Aftercare
Recovery from bruxism symptoms isn't a single event but an ongoing process of management and prevention.
- Initial Relief (Days to Weeks): With a custom nightguard, many patients experience a noticeable reduction in jaw pain, headaches, and tooth sensitivity within a few days to a few weeks. Muscles begin to relax, and teeth are protected immediately.
- Long-Term Management: Bruxism is often chronic, so treatment is focused on long-term management rather than a "cure."
- Nightguard Aftercare:
- Clean Daily: Brush your nightguard with a toothbrush and mild soap or non-abrasive denture cleaner after each use. Rinse thoroughly.
- Store Properly: Keep it in its protective case when not in use to prevent damage and contamination.
- Avoid Heat: Never expose your nightguard to hot water or direct sunlight, as this can warp the material.
- Regular Dental Check-ups: Bring your nightguard to every dental appointment so your dentist can inspect it for wear and proper fit. Nightguards typically last 3-5 years but may need replacement sooner if wear is severe.
- Stress Management: Continued practice of relaxation techniques, mindfulness, and healthy coping mechanisms is essential for sustained relief.
- Medication Use: Follow your doctor's instructions meticulously for any prescribed medications.
- Botox Aftercare: Avoid rubbing or massaging the injection sites for 24 hours. You may experience mild redness or bruising. Avoid strenuous exercise for 24-48 hours.
Prevention Strategies
While not all bruxism can be prevented, especially primary bruxism, several strategies can significantly reduce the risk and severity of symptoms:
- Stress Reduction: Implement stress-reducing techniques into your daily routine. This could include meditation, deep breathing exercises, yoga, regular physical activity, spending time in nature, or engaging in hobbies.
- Good Sleep Hygiene: Establish a consistent sleep schedule. Ensure your bedroom is dark, quiet, and cool. Avoid screens (phones, tablets, TV) for at least an hour before bed. Create a relaxing pre-sleep routine.
- Limit Stimulants: Reduce or eliminate consumption of caffeine (especially in the afternoon and evening), alcohol, and nicotine. These substances can disrupt sleep and increase muscle activity.
- Mindfulness for Awake Bruxism: Become aware of when you are clenching your jaw during the day. Practice consciously relaxing your jaw muscles by letting your lips touch and your teeth remain apart. You can use sticky notes as reminders in common clenching spots (e.g., computer screen, car dashboard).
- Regular Dental Check-ups: Regular visits allow your dentist to monitor your oral health, spot early signs of bruxism, and intervene before significant damage occurs.
- Identify and Address Underlying Conditions: If you suspect you have sleep apnea or other sleep disorders, talk to your dentist or physician about getting tested and treated.
Cost Ranges in the US (with/without insurance)
The cost of bruxism treatment varies widely based on the chosen therapy, the provider, and geographical location.
- Dental Consultation & Exam: $50 - $200 (often covered by insurance).
- Custom Nightguard:
- Without Insurance: $300 - $800+.
- With Insurance: Many dental insurance plans offer partial coverage for nightguards (often considered a "major procedure"), covering 50-80% after your deductible. Your out-of-pocket could range from $100 - $400. Check your specific plan for details.
- Boil-and-Bite Nightguard (OTC): $20 - $50 (not covered by insurance).
- Therapy/Counseling:
- Without Insurance: $75 - $200+ per session.
- With Insurance: Mental health coverage varies greatly. Co-pays can range from $20 - $75 per session if covered.
- Botox Injections for Bruxism:
- Without Insurance: $500 - $1,500+ per treatment cycle. This is almost never covered by dental or medical insurance for bruxism, as it's considered an off-label cosmetic or experimental treatment by many insurers.
- Dental Restorations (to repair damage):
- Fillings: $100 - $400 (often 80-100% covered).
- Crowns: $800 - $2,500+ (often 50% covered).
- Orthodontics: $3,000 - $8,000+ (some plans offer partial coverage, especially for children).
- Sleep Study (Polysomnography):
- Without Insurance: $1,000 - $3,000+.
- With Medical Insurance: Often covered by medical insurance if deemed medically necessary, with standard co-pays and deductibles applying (e.g., $200 - $1,000 out-of-pocket).
Comparison Table: Key Bruxism Treatment Options
| Feature | Custom Nightguard (Occlusal Splint) | Stress Management (Therapy, Mindfulness) | Botox Injections (for Masseter) | Dental Restorations (e.g., Crowns) |
|---|---|---|---|---|
| Primary Goal | Protect teeth, reduce pain | Address underlying cause, reduce tension | Reduce clenching force, pain | Repair existing damage |
| Method | Custom-fit oral appliance | Behavioral changes, psychological tools | Injections into jaw muscles | Dental procedures (drilling, etc.) |
| Effectiveness | High for protection & symptom relief | Variable, depends on commitment | High for severe clenching/pain | High for restoring tooth structure |
| Duration of Effect | Ongoing while worn (appliance lasts 3-5 yrs) | Long-term with consistent practice | 3-6 months (requires re-treatment) | Many years (if bruxism managed) |
| Cost (US) | $300 - $800+ | $75 - $200+ per session | $500 - $1,500+ per cycle | $100 - $2,500+ per tooth |
| Insurance Coverage | Often partial dental | Variable medical/mental health | Rarely covered | Often partial dental |
| Invasive? | Non-invasive | Non-invasive | Minimally invasive | Invasive |
| Side Effects | Initial discomfort, speech changes | None | Temporary asymmetry, chewing diff. | Tooth sensitivity, re-treatments |
For Parents / Pediatric Considerations
Bruxism in children is remarkably common, affecting anywhere from 6% to 50% of children, with some studies suggesting rates as high as 15% in preschoolers and school-aged children. It often peaks during periods of tooth development, such as when primary teeth erupt or when permanent teeth begin to come in.

- Why Children Brux: Similar to adults, stress and anxiety (e.g., starting school, family changes, new siblings) can play a role. However, other factors unique to children include:
- Growth and Development: Jaw development and tooth eruption can cause temporary bite imbalances, leading to grinding.
- Allergies and Adenoids: Nasal obstruction and difficulty breathing through the nose (often due to enlarged adenoids or chronic allergies) can contribute to mouth breathing and bruxism.
- Sleep Disorders: Sleep apnea, though less common in children, can also be a factor.
- Medications: Certain medications, like those for ADHD, can sometimes induce bruxism.
- Signs in Children: Parents might notice grinding sounds during sleep, tooth wear (though less pronounced than in adults due to primary teeth), jaw soreness, or headaches. Children may not always be able to articulate their discomfort.
- When to Worry / See a Dentist: Most childhood bruxism is benign and often resolves spontaneously without intervention, particularly as permanent teeth fully emerge. However, you should consult a pediatric dentist if:
- Your child complains of jaw pain, headaches, or facial soreness.
- There is visible significant wear or chipping of teeth.
- Bruxism is disrupting your child's sleep or their sleep partner's sleep.
- Your child has trouble eating or experiences increased tooth sensitivity.
- Your dentist might recommend a custom-fitted nightguard for children with severe symptoms, although often conservative approaches like stress reduction and addressing any underlying breathing issues are tried first.
Frequently Asked Questions
Q1: Is bruxism curable, or is it a lifelong condition?
A: Bruxism is often a chronic condition that is managed rather than permanently "cured." While specific triggers (like temporary stress) can resolve, the underlying predisposition to clench or grind may remain. Treatment focuses on symptom relief, preventing dental damage, and managing contributing factors. Many people successfully manage their bruxism to the point where it no longer causes significant problems.
Q2: How much does a custom nightguard typically cost in the US, and does insurance cover it?
A: A custom-made nightguard from a dentist typically costs between $300 and $800, with some high-end appliances exceeding $1,000. Many dental insurance plans offer partial coverage, usually treating it as a "major procedure" and covering 50-80% after your deductible. This means your out-of-pocket expense could range from $100 to $400. It's crucial to check with your specific insurance provider for exact coverage details.
Q3: How painful is bruxism treatment, particularly getting a nightguard or Botox?
A:
- Nightguard: Getting a nightguard is generally not painful. Impressions or digital scans are non-invasive. There might be a short adjustment period (a few days to a week) where the nightguard feels bulky or causes slight tooth soreness, but this typically resolves as you get used to it.
- Botox Injections: Botox involves injections, so you might feel a brief sting or pinch, similar to any injection. The area can be numbed with a topical cream beforehand. Mild soreness or bruising at the injection site can occur for a day or two afterward, but it's generally well-tolerated.
Q4: Are there effective alternatives to a nightguard for bruxism?
A: Yes, depending on the cause and severity of your bruxism, alternatives or complementary treatments include:
- Stress Management: Counseling, meditation, yoga, biofeedback.
- Medications: Muscle relaxants (short-term), certain antidepressants (if bruxism is a side effect of others), or Botox for severe cases.
- Addressing Sleep Disorders: Treatment for conditions like sleep apnea.
- Physical Therapy: For TMJ pain and jaw muscle rehabilitation. However, for direct tooth protection, a custom nightguard remains the gold standard.
Q5: Can over-the-counter (OTC) nightguards be as effective as custom ones?
A: Generally, no. OTC "boil-and-bite" nightguards, costing around $20-$50, offer minimal protection compared to custom appliances. They are often ill-fitting, bulky, uncomfortable, and can even exacerbate jaw problems or shift teeth if not fitted correctly. While they might provide very temporary relief, they are not a recommended long-term solution for serious bruxism and often don't provide the even bite surface needed for true muscle relaxation.
Q6: What's the difference between grinding and clenching?
A:
- Grinding: Involves rubbing the upper teeth against the lower teeth, often with a lateral (side-to-side) motion. This typically produces the characteristic loud sounds associated with sleep bruxism and leads to significant tooth wear and flattening.
- Clenching: Involves forcefully holding the upper and lower teeth tightly together, without much movement. Clenching is often silent and common in both awake and sleep bruxism. It places immense pressure on the jaw muscles and TMJ, leading to muscle soreness, headaches, and sometimes tooth fractures, but less often the flattened wear patterns seen with grinding.
Q7: Can bruxism be linked to Temporomandibular Joint (TMJ) issues?
A: Absolutely. Chronic bruxism is a major contributing factor to the development and exacerbation of Temporomandibular Joint Disorder (TMD). The sustained and excessive forces from grinding and clenching put immense strain on the TMJ (the hinge connecting your jaw to your skull), the ligaments, and the muscles surrounding it. This can lead to pain, clicking, popping, limited jaw movement, and inflammation within the joint. Many individuals with bruxism also experience TMD symptoms.
When to See a Dentist
It's crucial to seek professional dental advice if you suspect you or a loved one has bruxism. While some level of clenching or grinding might be occasional, certain signs warrant prompt attention:
- Persistent Jaw Pain or Stiffness: If you frequently wake up with a sore jaw, experience pain when chewing, or have difficulty opening your mouth wide.
- Frequent Headaches or Earaches: Especially if they are worse in the morning and cannot be attributed to other causes.
- Visible Tooth Damage: If you notice flattened, chipped, fractured, or excessively worn teeth, or increased tooth sensitivity.
- Damaged Dental Restorations: If fillings, crowns, or veneers are repeatedly cracking or breaking.
- Loud Grinding Noises at Night: If a sleep partner reports that you make loud grinding or clenching noises during sleep.
- Suspected Sleep Apnea: If you have symptoms like loud snoring, daytime fatigue, or observed pauses in breathing during sleep, combined with bruxism symptoms.
- Concerns about a Child's Bruxism: If your child exhibits significant tooth wear, complains of pain, or if their bruxism is affecting their quality of life.
Even if you don't experience severe pain, early detection by your dentist can prevent irreversible damage to your teeth and jaw. Regular dental check-ups are key to identifying the subtle signs of bruxism before it progresses to more serious complications. Your dentist can accurately diagnose the condition, discuss the various treatment options, and help you develop a personalized management plan to protect your oral health and alleviate your symptoms.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.