Temporomandibular Joint (TMJ)
4,921 words · 16 min read
Quick Definition
The hinge joint connecting the lower jaw (mandible) to the skull, located just in front of each ear. TMJ disorders cause pain, clicking, and restricted jaw movement.
The temporomandibular joint (TMJ) is a complex and often overlooked component of our oral and overall health. Far more than just a simple hinge, it's a marvel of biomechanical engineering, crucial for everyday functions like speaking, chewing, and swallowing. When this delicate system goes awry, it can lead to a range of uncomfortable and sometimes debilitating conditions collectively known as Temporomandibular Disorders (TMDs). This comprehensive guide, part of SmilePedia.net, aims to be the definitive resource for understanding everything about your TMJ, from its anatomy to the latest treatment options.
For anyone searching "what is temporomandibular joint (tmj)" or "temporomandibular joint (tmj) dental," this article will unravel the complexities of this vital joint. We'll explore why its proper function is paramount to your dental health, how common these disorders are, and what steps you can take to maintain a healthy, pain-free jaw. Understanding your TMJ is the first step towards managing and preventing issues that can significantly impact your quality of life. An estimated 10 million Americans suffer from TMDs, with women, particularly those of childbearing age, being twice as likely to be affected as men. Most commonly, symptoms first appear between 20 and 40 years of age. Ignoring TMJ discomfort can lead to chronic pain and further dental complications, making early identification and intervention crucial.
Key Takeaways:
- The Temporomandibular Joint (TMJ) connects your lower jaw (mandible) to your skull, enabling vital functions like chewing and speaking.
- Problems with the TMJ are called Temporomandibular Disorders (TMDs), causing pain, clicking, and restricted jaw movement.
- TMDs affect an estimated 10 million Americans, with women being more commonly affected.
- Common causes include bruxism (teeth grinding/clenching), stress, trauma, and anatomical issues.
- Treatment often begins with conservative methods like self-care, nightguards, and physical therapy, with surgery as a last resort.
- Early diagnosis and intervention by a dental professional are key to successful management and preventing chronic pain.
Detailed Explanation
The temporomandibular joint (TMJ) is actually a pair of joints, one on each side of your head, located just in front of your ears. These intricate joints act like a sliding hinge, connecting your lower jaw, or mandible, to the temporal bone of your skull. This unique structure allows for a wide range of jaw movements, including opening and closing, side-to-side motion, and protraction (moving the jaw forward) and retraction (moving it backward).
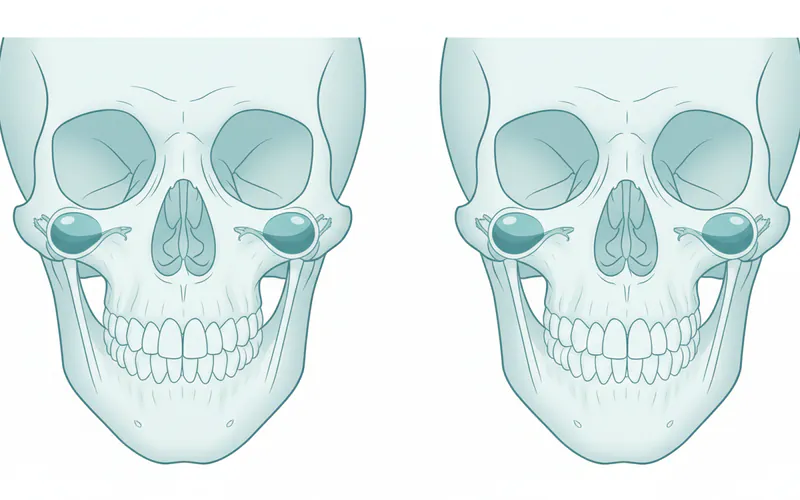
Each TMJ consists of several key components:
- Condyle: The rounded upper end of the mandible that fits into a socket in the skull.
- Articular Fossa: The socket in the temporal bone where the condyle rests.
- Articular Disc (Meniscus): A small, oval, cushion-like disc made of cartilage that sits between the condyle and the fossa. This disc acts as a shock absorber and allows the condyle to glide smoothly during jaw movements.
- Ligaments and Muscles: A complex network of ligaments provides stability, while several powerful muscles control the movement of the jaw, enabling chewing, speaking, and swallowing.
- Synovial Fluid: A lubricating fluid within the joint capsule that reduces friction.
When any of these components become inflamed, damaged, or misaligned, it can lead to Temporomandibular Disorders (TMDs). These disorders are often mistakenly referred to simply as "TMJ," but TMJ is the name of the joint itself, while TMD refers to the conditions affecting it.
Types and Classifications of Temporomandibular Disorders (TMDs)
TMDs are a collection of conditions, not a single disease, making their diagnosis and treatment multifaceted. They are generally categorized into three main groups:
- Myofascial Pain: This is the most common type of TMD, characterized by pain or discomfort in the muscles that control jaw function, as well as the muscles of the head and neck. The pain is often described as a dull, aching sensation, sometimes accompanied by muscle tenderness or trigger points. This type of pain often results from overuse, stress, or habitual clenching/grinding (bruxism).
- Internal Derangement of the Joint: This category involves a problem within the joint itself, most often related to the articular disc.
- Disc Displacement with Reduction: The disc is out of its normal position when the jaw is closed but snaps back into place when the mouth opens, often causing a "click" or "pop" sound.
- Disc Displacement without Reduction: The disc remains out of place even when the mouth opens, leading to restricted jaw movement (sometimes called "locked jaw") and pain.
- Dislocation: The mandible moves entirely out of the joint socket, requiring manual repositioning.
- Degenerative Joint Disease (Arthritis): Like other joints in the body, the TMJ can be affected by various forms of arthritis.
- Osteoarthritis: Caused by the breakdown of cartilage and bone in the joint, often due to aging or excessive wear and tear.
- Rheumatoid Arthritis: An autoimmune disease that can affect the TMJ, causing inflammation, pain, and damage.
Some individuals may experience a combination of these types, further complicating their symptoms and treatment needs.
Causes and Risk Factors
The exact cause of TMD is often difficult to pinpoint and can be multifactorial. However, several common factors and risk factors have been identified:
- Trauma to the Jaw, Head, or Neck: A direct blow to the jaw, a whiplash injury, or even a dental procedure that requires the mouth to be open for extended periods can trigger TMD.
- Bruxism (Teeth Grinding or Clenching): This involuntary habit, often occurring during sleep but also subconsciously during waking hours, places immense stress on the TMJ and surrounding muscles. It is a leading cause of myofascial pain and can contribute to disc displacement. A nightguard is often prescribed to manage this.
- Stress and Anxiety: Psychological stress is a significant contributor, as it often leads to increased muscle tension and habits like bruxism. The body's "fight or flight" response can cause clenching of the jaw muscles.
- Malocclusion (Misaligned Bite): While historically believed to be a primary cause, current research suggests that bite issues play a less direct role than previously thought. However, a significant malocclusion can sometimes contribute to uneven stress on the joints.
- Arthritis: Degenerative conditions like osteoarthritis or inflammatory conditions like rheumatoid arthritis can directly affect the TMJ cartilage and bone.
- Connective Tissue Diseases: Conditions that affect the body's connective tissues, such as Ehlers-Danlos syndrome, can lead to hypermobility of the joint and disc displacement.
- Gender and Hormones: Women are more prone to TMDs, with hormonal fluctuations (especially estrogen) thought to play a role. The prevalence is highest in women of childbearing age.
- Poor Posture: Forward head posture, common with extended computer use, can strain the neck and jaw muscles, indirectly affecting the TMJ.
- Diet: A consistently hard or chewy diet can exacerbate symptoms in susceptible individuals.
Signs and Symptoms to Watch For
The symptoms of TMDs can vary widely in severity and presentation. They can be intermittent or chronic and may affect one or both sides of the face. It's important to recognize these signs early:
- Pain or Tenderness:
- Aching pain in and around the ear, which may spread to the face, jaw, or neck.
- Tenderness in the jaw muscles, especially when touched or chewing.
- Jaw Dysfunction:
- Clicking, popping, or grinding sounds (crepitus) when opening or closing the mouth. These sounds are common and not always indicative of a problem, but if accompanied by pain or limited movement, they are a concern.
- Difficulty or pain when chewing, speaking, or yawning.
- A feeling that the jaw "locks" or "gets stuck" in either an open or closed position.
- Limited opening of the mouth.
- Headaches:
- Often described as tension-type headaches, located in the temples, forehead, or behind the eyes.
- Migraine-like headaches.
- Ear-Related Symptoms:
- Earache (often mistaken for an ear infection).
- Ringing in the ears (tinnitus).
- A feeling of fullness or pressure in the ears.
- Decreased hearing.
- Other Symptoms:
- Dizziness or vertigo.
- Facial swelling on the affected side.
- Toothache (without a specific dental cause).
- Sensitivity of teeth.
- Changes in the way the upper and lower teeth fit together (occlusion).
Diagnosis Process — What Your Dentist Does
Diagnosing TMD requires a comprehensive approach, as symptoms can mimic other conditions. Your dentist is often the first healthcare professional to evaluate TMJ concerns. The diagnostic process typically involves:
- Detailed Medical History: Your dentist will ask about your symptoms (when they started, their severity, what makes them better or worse), medical history, habits (like bruxism), stress levels, and any previous trauma.
- Physical Examination:
- Palpation: Your dentist will carefully feel your jaw joints and muscles (masseter, temporalis) for pain, tenderness, and trigger points.
- Range of Motion: They will assess how widely you can open your mouth, and if there's any deviation or restriction in movement.
- Joint Sounds: Listening for clicks, pops, or grinding sounds while you open and close your mouth.
- Bite Assessment (Occlusion): Evaluating how your upper and lower teeth come together.
- Imaging Studies (if necessary):
- Dental X-rays: Standard panoramic X-rays can show the overall structure of the jaw and teeth, but often don't provide detailed TMJ images.
- CT Scans (Computed Tomography): Provide detailed images of the bones of the joint, useful for detecting arthritis, fractures, or structural abnormalities.
- MRI Scans (Magnetic Resonance Imaging): The gold standard for visualizing the soft tissues of the joint, especially the articular disc, ligaments, and fluid. This is crucial for diagnosing disc displacement.
- Arthrography: A less common procedure where a dye is injected into the joint to highlight the disc and joint space on X-rays or CT scans.
It's important to note that diagnosis is primarily clinical, based on your symptoms and the physical exam. Imaging is often used to confirm or rule out specific structural problems rather than as a primary diagnostic tool for all TMDs.
Treatment Options with Pros, Cons, and Costs
Treatment for TMDs aims to reduce pain, restore normal jaw function, and prevent further damage. The approach is typically conservative and multidisciplinary, starting with the least invasive options.
A. Conservative / Non-Invasive Treatments
Most people with TMD find relief with these approaches.
- Self-Care and Lifestyle Modifications:
- Pros: Cost-effective, can be done at home, often provides significant relief.
- Cons: Requires discipline, may not be sufficient for severe cases.
- Cost: Minimal (over-the-counter pain relievers, heat/cold packs).
- Details: Eating soft foods, avoiding extreme jaw movements (wide yawning, gum chewing), applying moist heat or ice packs, gentle jaw stretches, stress reduction techniques, and practicing good posture.
- Medications:
- Pros: Reduces pain and inflammation.
- Cons: Temporary relief, potential side effects, does not address underlying causes.
- Cost: $10 - $100 per prescription/month (OTC much less).
- Details: Over-the-counter pain relievers (NSAIDs like ibuprofen), muscle relaxants (e.g., cyclobenzaprine), tricyclic antidepressants (at low doses for pain and sleep), anti-anxiety medications.
- Oral Appliances (Nightguards/Splints):
- Pros: Protects teeth from bruxism, reduces stress on TMJ, custom-fit for comfort.
- Cons: Can be expensive if custom, requires consistent use, not a cure for all TMDs.
- Cost: $300 - $800 for a custom-made nightguard or splint from a dentist; OTC guards are cheaper but less effective and can sometimes worsen issues.
- Details: A custom-made acrylic appliance that fits over your upper or lower teeth. It prevents tooth grinding and clenching, helping to relax jaw muscles and reposition the mandible or disc. There are different types: stabilization splints (most common) and repositioning splints (less common, for specific disc problems).
- Physical Therapy:
- Pros: Strengthens muscles, improves range of motion, reduces pain, teaches self-management.
- Cons: Requires commitment to exercises, multiple sessions needed.
- Cost: $50 - $200 per session (often 6-12 sessions needed).
- Details: Exercises to stretch and strengthen jaw muscles, massage, ultrasound, electrical stimulation (TENS), and postural correction.
- Stress Management and Biofeedback:
- Pros: Addresses a major contributing factor, empowers patients.
- Cons: Requires sustained effort, may need professional guidance.
- Cost: Varies for therapy sessions, biofeedback equipment.
- Details: Techniques like meditation, yoga, deep breathing, and counseling to manage stress, which often manifests as jaw tension and bruxism. Biofeedback helps patients learn to control muscle tension.
B. Minimally Invasive Procedures
If conservative treatments aren't effective, these options may be considered.
- Botulinum Toxin (Botox) Injections:
- Pros: Effectively relaxes hyperactive jaw muscles, reduces pain, lasts several months.
- Cons: Temporary, requires repeat injections, cost can add up, not FDA-approved for TMD (off-label use), potential side effects.
- Cost: $400 - $1000 per treatment, typically needed every 3-4 months.
- Details: Injections into the masseter and temporalis muscles to temporarily paralyze or weaken them, reducing clenching and pain.
- Corticosteroid Injections:
- Pros: Reduces inflammation and pain directly in the joint.
- Cons: Temporary relief, can have side effects with repeated use, risk of infection.
- Cost: $100 - $300 per injection.
- Details: Anti-inflammatory medication injected directly into the TMJ space.
C. Surgical Interventions
Surgery is generally a last resort, reserved for severe cases where other treatments have failed, or for significant structural problems.
- Arthrocentesis:
- Pros: Minimally invasive, can quickly relieve pain and improve jaw movement.
- Cons: Not suitable for all types of TMD, temporary relief in some cases.
- Cost: $500 - $1500.
- Details: Involves inserting small needles into the joint to flush out inflammatory byproducts and adhesions, sometimes followed by lubricant injection. Done under local anesthesia.
- Arthroscopy:
- Pros: Minimally invasive, allows direct visualization and minor repairs inside the joint.
- Cons: More invasive than arthrocentesis, still a surgical procedure with risks.
- Cost: $2,000 - $5,000.
- Details: A small incision is made, and a tiny camera (arthroscope) is inserted to visualize the joint. Instruments can then be used to remove inflamed tissue, smooth rough surfaces, or reposition the disc.
- Open-Joint Surgery (Arthroplasty):
- Pros: Can address severe structural damage not fixable with less invasive methods.
- Cons: Highly invasive, longer recovery, significant risks (nerve damage, infection, scarring), last resort.
- Cost: $5,000 - $25,000+ (depending on complexity, e.g., joint replacement).
- Details: Used for severe disc problems, bony fusion (ankylosis), tumors, or severe degenerative changes. Procedures include discectomy (removal of disc), condylotomy (reshaping the mandible condyle), or total joint replacement (for severely damaged joints).
Comparison Table of Common Treatment Options
| Treatment Option | Description | Pros | Cons | Estimated Cost Range (USD) |
|---|---|---|---|---|
| Self-Care / Lifestyle | Soft diet, heat/cold, stress reduction | Very low cost, no side effects | Requires discipline, may not be enough alone | < $50 |
| OTC/Rx Medications | Pain relievers, muscle relaxants, antidepressants | Quick pain relief, accessible | Temporary, side effects, doesn't address root cause | $10 - $100/month |
| Oral Appliance (Nightguard) | Custom-made splint for teeth grinding/clenching | Protects teeth, reduces muscle strain, custom fit | Can be expensive, requires consistent use | $300 - $800 |
| Physical Therapy | Exercises, massage, posture correction | Improves function, strengthens muscles, long-term | Requires commitment, multiple sessions | $50 - $200/session |
| Botox Injections | Relaxes jaw muscles, reduces clenching/pain | Effective for muscle pain, lasts months | Temporary, not FDA-approved for TMD, repeat injections costly | $400 - $1000/treatment |
| Arthrocentesis | Joint lavage to remove inflammatory substances | Minimally invasive, quick relief for some disc issues | Temporary for some, not for all TMD types | $500 - $1500 |
| Arthroscopy | Small camera for viewing and minor repairs | Minimally invasive surgery, direct visualization | More invasive than injections, surgical risks | $2,000 - $5,000 |
| Open-Joint Surgery | Major repair or replacement for severe damage | Resolves severe structural issues | Highly invasive, long recovery, significant risks | $5,000 - $25,000+ |
Step-by-Step: What to Expect During Treatment
The journey through TMD treatment is often progressive, starting with the simplest interventions.
- Initial Consultation and Diagnosis: Your first step is with your dentist. They will perform a thorough examination, take your history, and potentially recommend initial imaging.
- Conservative Management (Phase 1): If a TMD is diagnosed, your dentist will likely recommend a combination of self-care, over-the-counter pain relief, and possibly a custom-made nightguard or splint. They might also refer you to a physical therapist for jaw exercises. This phase usually lasts for several weeks to a few months.
- Medication Management: If pain persists, prescription medications like muscle relaxants or stronger NSAIDs might be prescribed for a limited period.
- Specialist Referral (if needed): If conservative measures are insufficient, your dentist may refer you to a TMJ specialist (an oral and maxillofacial surgeon, or a prosthodontist specializing in TMD) or a pain management specialist.
- Minimally Invasive Procedures: Under specialist guidance, options like Botox or corticosteroid injections, or arthrocentesis, may be considered if muscle or joint pain is severe and localized. These are typically done in an outpatient setting.
- Surgical Evaluation (Last Resort): For chronic, debilitating pain and confirmed structural damage that hasn't responded to other treatments, surgical options will be discussed. This involves detailed consultations, risks vs. benefits analysis, and comprehensive pre-operative planning.
Throughout your treatment, regular follow-up appointments with your dentist or specialist are crucial to monitor progress and adjust the treatment plan as needed.
Recovery Timeline and Aftercare
Recovery from TMD treatment is highly variable, depending on the severity of the condition and the type of intervention.
- Conservative Treatments (Self-care, Nightguard, PT): You may start feeling relief within days to weeks. Full symptom resolution can take several months of consistent effort. Aftercare involves continued use of your nightguard, regular exercises, and ongoing stress management.
- Injections (Botox, Corticosteroids): Relief usually begins within a few days to a week. The effects typically last 3-6 months, requiring repeat treatments. Aftercare is minimal, usually just avoiding strenuous jaw activities for a day or two.
- Arthrocentesis: Recovery is relatively quick, often with significant improvement in pain and movement within 1-2 weeks. You'll likely be advised to maintain a soft diet and perform gentle jaw exercises.
- Arthroscopy: Expect some swelling and discomfort for 1-2 weeks. A soft diet and limited jaw movement are recommended initially. Full recovery and return to normal activities might take 4-6 weeks. Physical therapy is often part of the aftercare.
- Open-Joint Surgery: This is the most extensive, with the longest recovery period. Initial recovery involves significant swelling, pain, and restricted jaw movement for several weeks. A liquid or soft diet will be necessary for an extended period. Full recovery can take several months to a year, often requiring extensive physical therapy and follow-up care.
Regardless of the treatment, patient commitment to aftercare instructions is paramount for successful long-term outcomes. This includes adherence to home exercises, continuous use of oral appliances like a nightguard, and ongoing stress reduction.
Prevention Strategies
While not all TMDs are preventable, many cases can be mitigated or avoided by adopting healthy habits and being mindful of jaw stress.
- Manage Stress: Since stress often leads to bruxism and muscle tension, incorporating stress-reduction techniques (meditation, yoga, exercise, hobbies) into your daily routine is vital.
- Avoid Jaw Overuse:
- Limit hard, chewy, or sticky foods.
- Avoid gum chewing.
- Refrain from biting nails, pen caps, or ice.
- Be mindful of clenching your teeth during the day; consciously relax your jaw.
- Address Bruxism: If you grind or clench your teeth, especially at night, talk to your dentist about a custom-made nightguard. This will protect your teeth and reduce strain on your TMJ.
- Maintain Good Posture: Keep your head aligned over your spine, especially when working at a computer or reading, to reduce neck and jaw muscle strain.
- Practice Jaw Relaxation: Keep your lips together but your teeth apart, with your tongue resting gently on the roof of your mouth behind your upper front teeth. This is the ideal resting position for your jaw.
- Regular Dental Check-ups: Your dentist can spot early signs of wear from bruxism or other jaw issues before they escalate into significant TMDs.
Cost Ranges in the US (with/without Insurance)
The cost of TMD treatment varies dramatically based on the type of treatment, geographic location, and the healthcare provider.
- Initial Consultation & Diagnosis:
- Without Insurance: $100 - $300 (for exam and basic X-rays).
- With Insurance: Often covered by dental or medical insurance, co-pay applies.
- Oral Appliance (Nightguard/Splint):
- Without Insurance: $300 - $800 (custom-made). Over-the-counter options are $20 - $50 but generally not recommended for long-term use.
- With Insurance: May be partially covered by dental insurance (e.g., 50-80% coverage), leaving $100 - $400 out-of-pocket. Some medical plans might cover it if deemed medically necessary.
- Physical Therapy:
- Without Insurance: $50 - $200 per session. A full course of treatment can be $500 - $2,000+.
- With Insurance: Often covered by medical insurance, with co-pays ranging from $20 - $50 per session.
- Medications:
- Without Insurance: $10 - $100 per prescription (monthly).
- With Insurance: Co-pays for prescriptions are usually $5 - $30.
- Botox Injections:
- Without Insurance: $400 - $1,000 per treatment, required every 3-4 months. Annual cost can be $1,200 - $4,000.
- With Insurance: Generally not covered, as it's considered off-label for TMD and often cosmetic. Some plans may cover if proven medically necessary after extensive appeals.
- Arthrocentesis:
- Without Insurance: $500 - $1,500.
- With Insurance: Often covered by medical insurance, with deductibles and co-insurance applying.
- Arthroscopy:
- Without Insurance: $2,000 - $5,000.
- With Insurance: Typically covered by medical insurance, subject to deductibles and co-insurance (e.g., 80% coverage after deductible, leaving $400 - $1,000+ out-of-pocket).
- Open-Joint Surgery:
- Without Insurance: $5,000 - $25,000+ (can be much higher for total joint replacement).
- With Insurance: Covered by medical insurance, but significantly high deductibles and co-insurance may apply, leaving $1,000 - $5,000+ out-of-pocket.
It's crucial to check with both your dental and medical insurance providers to understand your specific coverage for TMD diagnosis and treatment, as policies vary greatly. Many treatments for TMJ disorders, even those provided by a dentist, may fall under medical insurance rather than dental.
For Parents / Pediatric Considerations
While TMDs are more common in adults, children and adolescents can also experience TMJ issues. The prevalence in children is estimated to be around 5-10%, though it may be underdiagnosed.

- Causes in Children:
- Trauma: Falls, sports injuries, or direct blows to the jaw are common.
- Orthodontic Treatment: While often helpful, improper forces or prolonged opening during procedures can sometimes contribute.
- Bruxism: Night grinding is common in children and can strain the TMJ.
- Juvenile Idiopathic Arthritis: Can affect the TMJ, leading to growth disturbances of the mandible.
- Congenital Malformations: Rare, but can lead to structural problems.
- Signs to Watch For: Parents should look for similar symptoms as adults, such as jaw pain, clicking or popping sounds when eating, difficulty opening the mouth wide, headaches, or unusual chewing patterns. Children might also complain of earaches without infection.
- Diagnosis and Treatment: Diagnosis involves a thorough clinical exam. Imaging like MRI might be used if structural issues are suspected. Treatment is almost always conservative, focusing on:
- Soft Diet: Reducing stress on the jaw.
- Pain Management: Over-the-counter pain relievers.
- Physical Therapy: Gentle exercises.
- Oral Appliances: Custom nightguards for bruxism.
- Behavioral Therapy: To address habits like nail-biting or clenching.
- Surgical intervention is extremely rare and considered only in severe, debilitating cases with significant structural abnormalities affecting growth.
Early detection in children is vital to prevent potential long-term issues with jaw development and function.
Frequently Asked Questions
What is the primary function of the temporomandibular joint (TMJ)?
The primary function of the temporomandibular joint (TMJ) is to act as a hinge and a sliding joint, connecting your lower jaw (mandible) to your skull. This unique design allows for all the essential movements of the jaw, including opening and closing your mouth, moving your jaw from side to side, and moving it forward and backward. These actions are crucial for everyday activities such as chewing, speaking, yawning, and swallowing. Without a healthy functioning TMJ, these basic functions would be severely impaired.
Is TMJ pain usually permanent, or can it go away?
For most people, TMJ pain, formally known as a Temporomandibular Disorder (TMD), is not permanent and can resolve with conservative treatments or even self-care. Many cases of acute TMJ pain are temporary and can be managed effectively with rest, a soft diet, over-the-counter pain relievers, and stress reduction. However, if left untreated, or in cases involving significant structural damage or chronic bruxism, TMD can become persistent and lead to chronic pain. Early intervention significantly increases the likelihood of full recovery.
How painful are TMJ treatments?
The pain level associated with TMJ treatments varies widely depending on the chosen method. Conservative treatments like wearing a nightguard, physical therapy, or medication are generally low in pain, primarily focusing on pain relief and muscle relaxation. Injections (Botox, corticosteroids) involve a brief needle stick but are typically well-tolerated. More invasive procedures like arthrocentesis, arthroscopy, or open-joint surgery will involve post-operative pain managed with medication, similar to any surgical recovery. Your dental professional will discuss pain management strategies for any recommended treatment.
Can TMJ disorders be cured?
While the term "cure" implies complete elimination of a disease, many Temporomandibular Disorders (TMDs) can be effectively managed to the point where symptoms are resolved, and the individual can live pain-free with normal jaw function. This might involve long-term management strategies, such as consistent nightguard use for bruxism, ongoing stress management, or occasional physical therapy. For specific structural issues, surgery can offer a definitive solution. The goal is to restore function and eliminate pain, which is achievable for a vast majority of patients.
Are there alternatives to surgery for TMJ?
Yes, absolutely. Surgery for TMJ is considered a last resort, recommended only when all conservative and minimally invasive treatments have failed to provide relief for severe, persistent symptoms or significant structural problems. The vast majority of individuals with Temporomandibular Disorders (TMDs) find significant relief through non-surgical approaches. These alternatives include self-care, pain relievers, physical therapy, oral appliances (nightguards), stress management, and even injections like Botox or corticosteroids. Always explore conservative options thoroughly with your dentist before considering surgery.
Does dental insurance cover TMJ treatment?
Coverage for TMJ treatment is often a complex issue, as it can fall under both dental and medical insurance, or sometimes neither. Many diagnostic procedures and conservative treatments (like exams, X-rays, and even custom nightguards) may be partially covered by dental insurance. However, more extensive treatments, physical therapy, medications, and surgical procedures are typically covered by medical insurance, subject to your plan's deductibles, co-pays, and co-insurance. It is essential to contact both your dental and medical insurance providers directly to understand your specific benefits and coverage for Temporomandibular Disorders (TMDs).
How long does it take for a TMJ nightguard to work?
A custom-made TMJ nightguard (or splint) can often provide relief relatively quickly, with some patients noticing a difference in jaw discomfort and muscle soreness within a few days to a week of consistent use. However, for significant and long-term improvement, it typically takes several weeks to a few months. The nightguard works by repositioning the mandible, relaxing the jaw muscles, and preventing the damaging effects of bruxism, so consistent nightly use is crucial to allow the muscles and joint to heal and adapt over time.
Can orthodontics help with TMJ problems?
The relationship between orthodontics and TMJ problems is complex and debated. While some severe bite problems (malocclusion) can contribute to jaw pain, orthodontic treatment alone is generally not recommended as a primary treatment for Temporomandibular Disorders (TMDs). However, in specific cases where a significant bite discrepancy is identified as a contributing factor, orthodontics might be part of a broader treatment plan. It's crucial that any orthodontic intervention for TMD is carefully planned and executed by a dentist or orthodontist experienced in TMD, usually after conservative TMD treatments have been exhausted.
When to See a Dentist
It's important to know when jaw discomfort warrants a visit to your dentist or a specialist.
- Routine Care: If you experience any persistent pain or tenderness in your jaw, face, or around your ear, or if you notice clicking, popping, or grinding sounds accompanied by discomfort or restricted movement, schedule an appointment with your general dentist. They can properly diagnose and often manage the initial stages of Temporomandibular Disorders (TMDs). Even if symptoms are mild, early intervention can prevent escalation.
- Emergency Signs: Seek immediate dental or medical attention if:
- Your jaw locks completely open or closed, making it impossible to move.
- You experience sudden, severe, and debilitating pain in your jaw or face, especially after an injury.
- You notice significant swelling around your TMJ or face that develops rapidly.
- You cannot close your mouth after yawning or opening wide (jaw dislocation).
Don't wait for the pain to become unbearable. Prompt evaluation by a dental professional is key to effective management and preventing chronic issues with your temporomandibular joint (TMJ).
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.