Nightguard
5,306 words · 18 min read
Quick Definition
A custom-made oral appliance worn during sleep to protect teeth from damage caused by bruxism (grinding and clenching). Also called an occlusal splint or bite guard.
A nightguard is a custom-made oral appliance worn primarily during sleep to protect teeth from the damaging effects of bruxism, a condition characterized by involuntary grinding or clenching of the teeth. Often referred to as an occlusal splint or bite guard, this device acts as a protective barrier, absorbing the forces generated by clenching and grinding and preventing direct tooth-to-tooth contact. Its importance for dental health cannot be overstated; unchecked bruxism can lead to significant tooth wear, fractures, gum recession, and even impact the Temporomandibular Joint (TMJ), which connects your jaw to your skull.
Bruxism is a remarkably common condition, affecting a significant portion of the population. Studies suggest that 10-15% of adults experience some form of bruxism, with rates potentially higher in children, where up to 1 in 3 may exhibit grinding behaviors, often outgrowing it. While occasional clenching or grinding might not be problematic, chronic bruxism can lead to a cascade of painful and costly dental issues, making the nightguard a crucial preventive and therapeutic tool. Understanding "what is nightguard" and "nightguard dental" is the first step toward safeguarding your smile and overall oral health.
Key Takeaways:
- A nightguard is a custom oral appliance protecting teeth from grinding (bruxism).
- It prevents tooth wear, fractures, and TMJ damage.
- Custom-fit nightguards are significantly more effective than over-the-counter options.
- Wearing a nightguard can alleviate headaches, jaw pain, and facial soreness.
- Bruxism affects 10-15% of adults and up to 1 in 3 children.
- Regular use and proper care are essential for a nightguard's effectiveness and longevity.
Detailed Explanation
Types and Classifications of Nightguards
Nightguards come in various materials and designs, primarily classified by their hardness and specific function. The choice of nightguard type is often dictated by the severity of bruxism, patient comfort, and the dentist's recommendation.
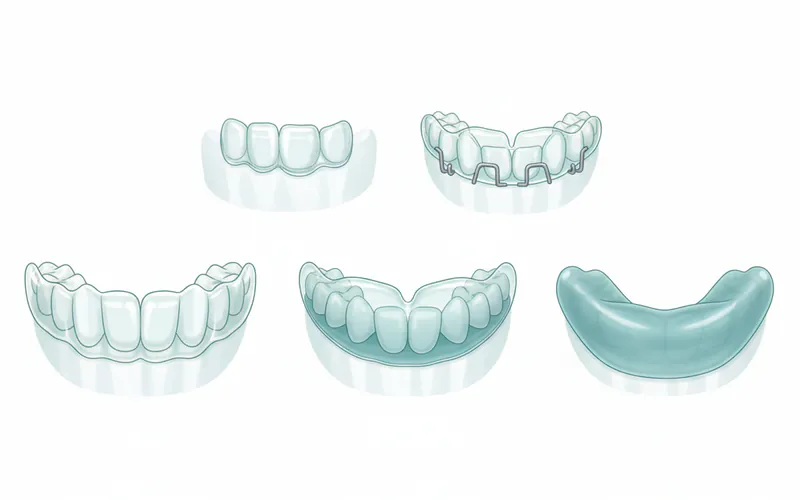
-
Soft Nightguards:
- Material: Made from a flexible, rubbery material, similar to a sports mouthguard.
- Pros: Most comfortable for initial wear, easy to adjust to, often less expensive than hard nightguards. Good for mild or occasional clenching and grinding, or for patients with sensitive teeth.
- Cons: Less durable, can wear through faster with severe grinding, and some patients may find they encourage more clenching due to their "chewy" texture. Not ideal for heavy grinders or those with TMJ disorders.
- Typical Lifespan: 6 months to 2 years.
-
Hard Nightguards (Acrylic Splints):
- Material: Constructed from rigid acrylic plastic.
- Pros: Highly durable and long-lasting, providing excellent protection against heavy grinding and clenching. They offer stable jaw positioning, which is beneficial for managing TMJ disorders by guiding the jaw into a more relaxed position. Considered the gold standard for severe bruxism.
- Cons: Can be less comfortable initially due to their rigidity, requiring a longer adjustment period. More expensive than soft nightguards.
- Typical Lifespan: 3 to 10+ years.
-
Dual Laminate (Hybrid) Nightguards:
- Material: A combination of a soft inner layer for comfort and a hard outer layer for durability and protection.
- Pros: Offers the best of both worlds – comfort of a soft guard with the durability and protective qualities of a hard guard. They are well-suited for moderate to severe bruxism where patient comfort is a primary concern.
- Cons: Can be more expensive than soft guards, though often comparable to hard guards.
- Typical Lifespan: 2 to 5 years.
Key Consideration: Custom-Fit vs. Over-the-Counter (OTC) While OTC nightguards (boil-and-bite) are available, they are generally not recommended for long-term use or severe bruxism. Custom-fit nightguards, made by your dentist, offer superior fit, comfort, and protection. They are precisely molded to your unique dental anatomy, ensuring optimal occlusal balance and preventing potential issues like shifting teeth or exacerbating TMJ problems that can arise from ill-fitting OTC guards.
Causes and Risk Factors for Bruxism
Understanding the root causes of bruxism is crucial for effective management and prevention. While the exact etiology can be complex and multifactorial, several factors are commonly associated with the condition:
- Stress and Anxiety: This is arguably the most common culprit. Emotional stress, anxiety, frustration, or anger can manifest physically as clenching or grinding, particularly during sleep. Individuals under high pressure or those with anxious personalities are more prone.
- Sleep Disorders: Bruxism is often classified as a sleep-related movement disorder. It is frequently linked to other sleep conditions, most notably sleep apnea. The body may grind its teeth in an attempt to open the airway during apneic episodes. Other sleep disturbances, like restless leg syndrome, can also be associated.
- Lifestyle Factors:
- Caffeine and Alcohol: Excessive consumption of caffeine, particularly close to bedtime, and alcohol can disrupt sleep patterns and increase the likelihood of grinding.
- Smoking: Nicotine is a stimulant and can contribute to bruxism. Studies show smokers are almost twice as likely to have bruxism compared to non-smokers.
- Recreational Drugs: Amphetamines and ecstasy are well-known to cause teeth clenching and grinding.
- Medications: Certain medications, especially selective serotonin reuptake inhibitors (SSRIs) used to treat depression and anxiety, can have bruxism as a side effect.
- Malocclusion (Misaligned Bite): While historically thought to be a primary cause, current research suggests that an imperfect bite is less of a direct cause and more of a contributing or exacerbating factor. However, a bite that isn't properly aligned can sometimes lead to grinding as the jaw tries to find a comfortable resting position.
- Other Medical Conditions: Certain neurological conditions (e.g., Parkinson's disease, Huntington's disease) and gastroesophageal reflux disease (GERD) have been linked to bruxism.
- Genetics: There may be a hereditary component, as bruxism can run in families. If a parent has a history of grinding, their children may be at a higher risk.
Signs and Symptoms to Watch For
Recognizing the signs and symptoms of bruxism is often the first step toward seeking dental intervention. Many individuals are unaware they grind or clench their teeth, especially during sleep, until a partner observes it or a dentist identifies the damage.
- Tooth Damage:
- Worn-down, flattened, fractured, or chipped teeth: This is the most common and definitive sign. Enamel can be eroded, exposing the underlying dentin.
- Increased tooth sensitivity: Due to enamel wear, exposing dentin, or micro-fractures.
- Cracked or broken fillings, crowns, or veneers: The excessive force can damage dental restorations.
- Abfraction lesions: V-shaped notches near the gum line, often caused by stress from clenching and grinding.
- Jaw, Facial, and Head Pain:
- Sore or tired jaw muscles: Especially noticeable upon waking.
- Tight or stiff jaw muscles: Difficulty opening the mouth wide.
- Jaw pain or tenderness: Radiating to the ear or temple.
- Headaches: Often tension-type headaches, starting in the temples.
- Facial pain: Generalized soreness in the face.
- TMJ Symptoms:
- Clicking, popping, or grating sounds in the jaw joint when opening or closing the mouth.
- Limited jaw movement or inability to open the mouth fully.
- Jaw locking: The jaw getting "stuck" in an open or closed position.
- Earache: Often misdiagnosed as an ear infection, as TMJ pain can refer to the ear.
- Other Symptoms:
- Disrupted sleep for a bed partner: They may hear the grinding sounds.
- Indentations on the tongue: From pressing against teeth during clenching.
- Bite marks on the inside of the cheek.
- Gum recession: Exposing tooth roots due to excessive force.
Diagnosis Process — What Your Dentist Does
Diagnosing bruxism and determining the need for a nightguard is typically a straightforward process conducted by your dentist.
- Patient History and Symptom Review: The dentist will begin by asking about your symptoms, such as jaw pain, headaches, tooth sensitivity, or if a partner has noticed you grinding. They'll inquire about your stress levels, sleep habits, lifestyle factors (caffeine, alcohol, smoking), and medications.
- Comprehensive Dental Examination:
- Visual Inspection: The dentist will carefully examine your teeth for signs of wear, chips, fractures, or cracks. They'll look for flattened occlusal surfaces (the biting surfaces of your teeth) or sharp edges created by grinding.
- Soft Tissue Examination: They will check for any indentations on your tongue or bite marks on your cheeks.
- Gum Health Assessment: To check for signs of gum recession or inflammation that might be exacerbated by grinding.
- Palpation of Jaw Muscles: The dentist will gently feel your jaw muscles (masseter and temporalis muscles) while you clench and relax to check for tenderness, soreness, or hypertrophy (enlargement) which indicates overuse.
- TMJ Examination: They will listen and feel for clicks, pops, or crepitus (grating sounds) in your TMJ when you open and close your mouth. They will also assess your range of motion and check for any tenderness in the joint itself.
- Bite Analysis (Occlusal Assessment): The dentist will evaluate your bite to see how your upper and lower teeth meet. While malocclusion isn't always the primary cause, an unbalanced bite can contribute to grinding patterns.
- X-rays: Dental X-rays may be taken to assess the bone structure around your teeth and TMJ, rule out other dental issues, and check for any signs of bone damage due to excessive force.
- Differential Diagnosis: The dentist will rule out other conditions that might present with similar symptoms, such as sinus infections, ear infections, or other sources of facial pain.
- Observation/Monitoring: In some cases, if the symptoms are mild or unclear, the dentist might recommend a period of observation or suggest keeping a symptom diary to track when pain occurs.
If bruxism is confirmed, a custom-fitted nightguard is often the primary recommended intervention.
Treatment Options for Bruxism with Pros, Cons, and Costs
While a nightguard is the cornerstone of bruxism management, a holistic approach often involves several strategies.

1. Custom-Fitted Nightguard (Occlusal Splint)
- Description: The most common and effective treatment. A clear, custom-made acrylic or laminate device worn over the upper or lower teeth to prevent direct tooth-on-tooth contact and distribute biting forces evenly.
- Pros:
- Highly effective in protecting teeth from wear and fractures.
- Reduces jaw muscle strain and TMJ stress.
- Alleviates symptoms like headaches, jaw pain, and tooth sensitivity.
- Non-invasive and generally well-tolerated.
- Cons:
- Initial cost can be significant.
- Requires a period of adjustment to get used to wearing it.
- Needs regular cleaning and maintenance.
- Doesn't address the underlying causes of bruxism, only manages the symptoms.
- Cost Range in the US: $300 - $800 (without insurance) depending on material, complexity, and geographic location.
2. Behavioral Therapies and Stress Management
- Description: Techniques aimed at reducing stress and becoming more aware of clenching habits. This includes relaxation exercises, meditation, yoga, biofeedback, and counseling.
- Pros:
- Addresses the root cause (stress/anxiety).
- Can improve overall well-being.
- No side effects from medication or devices.
- Cons:
- Requires patient commitment and discipline.
- Results can be slow or inconsistent.
- May require professional guidance (e.g., therapist), incurring costs.
- Cost Range in the US: Varies widely, from free (self-practice) to $50 - $200+ per session for therapy.
3. Medications
- Description: Typically used for short-term relief in severe cases.
- Muscle Relaxants: Prescribed for a few days to relax jaw muscles and reduce pain.
- Botox Injections: Injected into the jaw muscles (masseter) to temporarily paralyze them, significantly reducing the force of clenching. This is an off-label use for bruxism but is increasingly common.
- Pros:
- Rapid relief from pain and muscle tension (muscle relaxants).
- Highly effective in reducing grinding force (Botox).
- Cons:
- Temporary relief; doesn't cure the underlying condition.
- Side effects possible (drowsiness, dry mouth from muscle relaxants; temporary weakness in jaw muscles, altered smile from Botox).
- Costly for ongoing treatment (Botox).
- Not a first-line treatment.
- Cost Range in the US:
- Muscle Relaxants: $10 - $50 (generic) per prescription.
- Botox: $500 - $1000+ per treatment (lasts 3-6 months).
4. Occlusal Adjustments (Bite Adjustments)
- Description: In some cases, if a specific tooth or restoration is interfering with the bite, the dentist may make minor adjustments to the chewing surfaces to create a more balanced occlusion. This is done cautiously and rarely as a standalone treatment.
- Pros:
- Can correct specific bite interferences.
- May improve overall bite comfort.
- Cons:
- Irreversible removal of tooth structure.
- Not always effective for bruxism, especially if the cause is not primarily occlusal.
- Should only be performed by dentists experienced in occlusal principles.
- Cost Range in the US: $50 - $200 per session, depending on complexity.
Comparison Table: Custom-Fit Nightguard vs. Over-the-Counter Nightguard
| Feature | Custom-Fit Nightguard | Over-the-Counter (OTC) Nightguard |
|---|---|---|
| Fit | Precisely molded to your unique dental anatomy | "Boil-and-bite" or one-size-fits-all |
| Comfort | Excellent; designed for long-term wear | Can be bulky, uncomfortable, or ill-fitting |
| Protection | Superior; even distribution of forces, high durability | Limited; may not fully protect or distribute forces |
| Effectiveness | Highly effective for moderate to severe bruxism | Less effective; suitable for very mild, temporary use |
| Material | Medical-grade acrylic, hard/soft laminate | Softer, less durable plastics |
| Lifespan | 2-10+ years (depending on type and care) | Few weeks to 6 months |
| Cost | $300 - $800+ | $15 - $50 |
| Dental Oversight | Required; made by a dentist or dental lab | None; purchased directly by consumer |
| TMJ Health | Can help stabilize and protect the TMJ | Can potentially worsen TMJ issues if ill-fitting |
Step-by-Step: What to Expect During Nightguard Treatment
Getting a custom-fitted nightguard is a straightforward process, typically involving two to three dental visits.
-
Initial Consultation and Examination (Visit 1):
- Your dentist will perform a thorough examination, as described in the "Diagnosis Process" section, to confirm bruxism and assess your dental health.
- They will discuss your symptoms, lifestyle, and medical history.
- Once a nightguard is deemed appropriate, the dentist will discuss the different types (soft, hard, hybrid) and recommend the best option for your specific needs.
- Dental Impressions/Scans: The dentist or a dental assistant will take precise impressions of your upper and lower teeth. This is done either using a soft, putty-like material in a tray that sets in your mouth, or with a digital intraoral scanner that creates a 3D model of your teeth. These impressions are crucial for creating a nightguard that fits perfectly.
- Bite Registration: The dentist will also take a "bite registration" to capture how your upper and lower jaws meet when your muscles are relaxed. This helps the lab ensure the nightguard positions your jaw correctly.
``
-
Fabrication (Off-site):
- The impressions or digital scans, along with the bite registration and your dentist's specific instructions, are sent to a specialized dental laboratory.
- Skilled technicians will then fabricate your custom nightguard using the chosen material (acrylic, laminate, etc.). This process can take anywhere from 1 to 3 weeks.
-
Fitting and Adjustment (Visit 2):
- Once your nightguard returns from the lab, you'll have an appointment for fitting.
- The dentist will carefully place the nightguard in your mouth, usually on your upper teeth (though lower nightguards are also common).
- They will check its fit, ensuring it's snug but comfortable, without any sharp edges or pressure points.
- Bite Check: You'll be asked to bite down, and the dentist will use articulating paper to identify any high spots or areas where your bite is uneven. They will then make precise adjustments by gently grinding and polishing the nightguard until your bite feels balanced and comfortable.
- Instructions: You'll receive detailed instructions on how to wear, clean, and care for your new nightguard. The dentist will explain what to expect during the initial adjustment period.
-
Follow-up (Optional, Visit 3):
- Sometimes, a follow-up appointment a few days to a week later may be scheduled to ensure continued comfort and make any minor final adjustments after you've worn the nightguard for a short period. This allows the dentist to address any new pressure points or discomfort that arise during initial use.
The goal is a nightguard that feels natural and provides optimal protection without causing discomfort or altering your bite negatively.
Recovery Timeline and Aftercare
Using a nightguard effectively involves an initial adjustment period and diligent long-term care to ensure its longevity and efficacy.
Recovery Timeline:
- First Few Nights: It's common to experience some initial discomfort or a feeling of bulkiness in your mouth. Your mouth may produce more saliva than usual. You might also notice your bite feels "different" when you take the nightguard out in the morning. This is normal as your jaw muscles adjust to the new resting position.
- First Week: Most people adapt within a few nights to a week. Consistent wear is key during this period. Your jaw muscles will begin to relax, and symptoms like morning headaches and jaw soreness should start to diminish.
- Ongoing Use: With regular use, the nightguard becomes a routine part of your sleep. You should experience significant relief from bruxism symptoms and observe a reduction in tooth wear.
Aftercare for Your Nightguard:
Proper cleaning and storage are critical for maintaining hygiene, preventing bacterial growth, and extending the life of your nightguard.
- Clean Immediately After Each Use:
- As soon as you remove your nightguard in the morning, rinse it thoroughly under cool (not hot) running water.
- Gently brush it with a soft-bristled toothbrush and a non-abrasive, non-whitening toothpaste, or a mild hand soap/dish soap. Avoid abrasive cleaners as they can scratch the surface, creating nooks for bacteria.
- Specific nightguard cleaning solutions or denture cleansers (dissolvable tablets) can be used periodically (e.g., once a week) for a deeper clean and to remove any plaque or stains. Always follow the product instructions.
- Rinse Before Each Use: Before putting your nightguard back in at night, rinse it with cool water to remove any dust or debris.
- Store Properly:
- After cleaning, ensure your nightguard is thoroughly dry to prevent bacterial or fungal growth.
- Store it in the protective case provided by your dentist. This protects it from damage, keeps it clean, and prevents it from getting lost or exposed to pets.
- Do not leave it exposed to high temperatures (e.g., in a hot car, near a window, or in boiling water), as this can warp the material and ruin its fit.
- Regular Dental Check-ups: Bring your nightguard to every dental appointment. Your dentist will inspect it for wear and tear, cleanliness, and fit, making any necessary adjustments to ensure it remains effective.
- Watch for Wear: Even the most durable nightguards will eventually show signs of wear (e.g., holes, cracks, thinning). If you notice significant damage, it's time to talk to your dentist about a replacement.
- Avoid Harmful Chemicals: Do not use harsh chemicals like bleach, mouthwash containing alcohol, or abrasive household cleaners on your nightguard, as these can damage the material.
By following these guidelines, your nightguard will provide years of effective protection for your teeth and relief from bruxism symptoms.
Prevention Strategies for Bruxism
While not all cases of bruxism are preventable, especially those linked to genetics or certain medical conditions, many strategies can help reduce the incidence and severity, particularly when stress and lifestyle factors are involved.
- Stress Reduction: Since stress and anxiety are major contributors to bruxism, managing them effectively is paramount.
- Relaxation Techniques: Practice deep breathing exercises, meditation, yoga, or progressive muscle relaxation.
- Mindfulness: Be present and aware of tension in your body, especially in your jaw.
- Time Management: Reduce overloaded schedules and carve out time for leisure and relaxation.
- Professional Help: Consider counseling or therapy if stress and anxiety are overwhelming.
- Improve Sleep Hygiene: Good sleep habits can significantly reduce sleep-related bruxism.
- Consistent Sleep Schedule: Go to bed and wake up at the same time each day, even on weekends.
- Comfortable Sleep Environment: Ensure your bedroom is dark, quiet, and cool.
- Avoid Stimulants Before Bed: Limit caffeine and alcohol, especially in the hours leading up to sleep.
- Screen Time: Reduce exposure to screens (phones, tablets, computers) at least an hour before bedtime.
- Address Sleep Disorders: If you suspect a sleep disorder like sleep apnea, seek diagnosis and treatment from a medical professional.
- Dietary and Lifestyle Modifications:
- Limit Stimulants: Cut down on caffeine and alcohol, particularly in the evenings.
- Quit Smoking: Nicotine is a stimulant and can contribute to bruxism.
- Avoid Hard, Chewy Foods: While managing symptoms, temporarily avoiding excessively chewy foods (e.g., chewing gum, tough meats, nuts) can give your jaw muscles a break.
- Jaw Awareness and Habit Reversal:
- "Lips Together, Teeth Apart": Practice keeping your lips closed but your teeth slightly apart, with your tongue resting gently on the roof of your mouth. This is the natural resting position for your jaw.
- Self-Monitoring: Throughout the day, especially during stressful periods, become aware if you are clenching your jaw. If you catch yourself, consciously relax your jaw muscles. You can use sticky notes or phone reminders to prompt this awareness.
- Regular Dental Check-ups: Your dentist can spot early signs of wear or TMJ issues, even before you notice symptoms. Early intervention can prevent more significant damage.
Cost Ranges in the US (with/without Insurance)
The cost of a nightguard in the US can vary significantly based on several factors, including the type of material, the complexity of your case, the dentist's fees, and your geographic location.
- Custom-Fitted Nightguard (Dentist-Prescribed):
- Without Insurance: Expect to pay anywhere from $300 to $800. Some highly specialized or complex cases involving TMJ treatment might even reach $1,000 or more. This cost typically includes the impressions, laboratory fabrication, fitting, and initial adjustments.
- With Insurance: Dental insurance plans often provide partial coverage for nightguards, as they are considered a medical necessity for protecting teeth and jaw health. Coverage typically ranges from 20% to 80%, depending on your specific plan and deductible. You might pay an out-of-pocket amount of $100 to $400 after insurance, but it's essential to check with your provider for exact details. Many plans categorize nightguards as a "major restorative" service or under specific TMJ clauses.
- Over-the-Counter (OTC) Nightguards:
- These are much cheaper, typically ranging from $15 to $50. They are boil-and-bite devices or one-size-fits-all. While they offer temporary, minimal protection, they are not custom-fitted and can potentially cause more harm than good in the long run if used incorrectly or for severe bruxism. Insurance does not cover OTC options.
Factors Influencing Cost:
- Type of Material: Hard acrylic nightguards are generally more expensive than soft or hybrid ones due to material cost and fabrication complexity.
- Geographic Location: Costs can be higher in metropolitan areas or regions with a higher cost of living.
- Dentist's Fees: Experienced or specialist dentists (e.g., those specializing in TMJ disorders) might have higher fees.
- Additional Procedures: If extensive dental work is required before the nightguard (e.g., treating cavities, severe wear), those costs will be separate.
It's always recommended to discuss the full cost breakdown with your dentist's office and inquire about your insurance benefits before proceeding with treatment.
For Parents / Pediatric Considerations
Bruxism in children, often referred to as "sleep grinding" or "nocturnal bruxism," is a common occurrence, affecting an estimated 15% to 33% of children. While the sounds of a child grinding their teeth at night can be alarming for parents, it's typically a self-limiting condition that most children outgrow by adolescence.
Common Causes in Children:
- Stress and Anxiety: Similar to adults, emotional stress from school, family changes, or even minor anxieties can trigger grinding.
- Growth and Development: Grinding can be related to the development of the jaw and teeth, especially during periods of tooth eruption (baby teeth coming in, permanent teeth replacing baby teeth).
- Allergies: Some theories suggest a link between allergies and upper airway congestion, leading to grinding.
- Other Medical Conditions: Less commonly, conditions like cerebral palsy, certain medications, or attention deficit hyperactivity disorder (ADHD) can be associated.
- Sleep Disorders: Like adults, sleep apnea or other disturbed sleep patterns can sometimes be linked.
When is a Nightguard Necessary for Children?
For most children, bruxism resolves on its own without intervention. A nightguard is usually only considered if:
- Significant Tooth Damage: There is visible wear, chipping, or sensitivity that is impacting the child's oral health.
- Pain or Discomfort: The child complains of jaw pain, headaches, or facial soreness upon waking.
- Impact on Permanent Teeth: If the grinding is severe enough to damage newly erupted permanent teeth.
- TMJ Issues: Rarely, children can develop TMJ symptoms that warrant intervention.
Considerations for Pediatric Nightguards:
- Growth Changes: A child's mouth is constantly changing as they grow and lose baby teeth. A nightguard for a child will need to be replaced more frequently than an adult's, possibly every 6-12 months, to accommodate these changes.
- Custom-Fit is Crucial: Just like for adults, a custom-fitted appliance is essential to ensure it doesn't impede jaw growth or tooth eruption.
- Compliance: Children may be less compliant with wearing an appliance consistently. Parents need to emphasize the importance and help establish a routine.
- Soft Material Preference: Often, softer, more flexible nightguards are chosen for children for comfort and ease of adjustment.
If you suspect your child is grinding their teeth, observe for signs and symptoms, and consult with a pediatric dentist. They can assess the severity, rule out other causes, and determine if a nightguard or other interventions are appropriate.
Frequently Asked Questions
How much does a nightguard cost?
The cost of a custom-fitted nightguard from a dentist in the US typically ranges from $300 to $800 without insurance. Prices can vary based on the type of material (hard acrylic, soft, hybrid), geographic location, and the dentist's fees. With dental insurance, patients can expect to pay an out-of-pocket amount closer to $100 to $400, as many plans cover a portion of the cost. Over-the-counter nightguards are much cheaper ($15-$50) but are not custom-fitted and generally not recommended for long-term use due to potential dental issues.
Is wearing a nightguard painful?
Most people find wearing a custom-fitted nightguard to be comfortable after a short adjustment period. Initially, you might experience a feeling of bulkiness, increased saliva production, or a slight soreness in your jaw muscles as they adapt to the new resting position. Any pain or significant discomfort should be reported to your dentist, as the nightguard may require minor adjustments to ensure a perfect fit and balanced bite. An ill-fitting over-the-counter nightguard, however, can cause pain or exacerbate TMJ issues.
How long does a nightguard last?
The lifespan of a nightguard depends on its material, the severity of your bruxism, and how well you care for it.
- Soft nightguards: Typically last 6 months to 2 years.
- Hybrid (dual laminate) nightguards: Generally last 2 to 5 years.
- Hard acrylic nightguards: Are the most durable, lasting anywhere from 3 to 10+ years. Regular dental check-ups, proper cleaning, and storage can help maximize its longevity. Your dentist will monitor its wear and advise you when a replacement is needed.
Are there alternatives to a nightguard?
While a nightguard is the most common and effective treatment for protecting teeth from bruxism, other strategies can help manage the condition:
- Stress Management: Relaxation techniques, meditation, yoga, counseling.
- Biofeedback: Learning to control jaw muscle activity.
- Medications: Short-term muscle relaxants or Botox injections (off-label use) for severe pain and muscle spasm.
- Lifestyle Changes: Avoiding caffeine, alcohol, and smoking, especially before bed.
- Occlusal Adjustments: Minor reshaping of teeth in rare cases of severe bite interference.
- Addressing Underlying Sleep Disorders: Treating conditions like sleep apnea. It's important to consult with your dentist to determine the best treatment plan for your specific situation.
Does insurance cover nightguards?
Many dental insurance plans do offer coverage for custom-fitted nightguards, as they are considered a medical necessity to prevent further dental damage from bruxism. The extent of coverage varies widely by plan, but you can expect it to cover anywhere from 20% to 80% of the cost after your deductible. It's crucial to contact your insurance provider directly, provide the dental code (often D9940 for occlusal guard), and verify your specific benefits to understand your out-of-pocket expenses. Over-the-counter nightguards are not covered by insurance.
Can I use an over-the-counter nightguard?
While readily available and inexpensive, over-the-counter (OTC) nightguards (like boil-and-bite options) are generally not recommended for long-term use or for individuals with moderate to severe bruxism or TMJ issues. They offer a generic fit that may be uncomfortable, ineffective, and can potentially worsen jaw problems or even shift your teeth if not properly fitted. Custom-fitted nightguards from your dentist provide superior protection, comfort, and precise occlusal balance, making them the preferred choice for lasting dental health.
How do I clean my nightguard?
To keep your nightguard hygienic and extend its life, clean it thoroughly every day. After removal, rinse it under cool running water. Gently brush it with a soft-bristled toothbrush and a non-abrasive, non-whitening toothpaste, or mild hand soap/dish soap. Rinse well. You can also use specialized nightguard cleaning tablets or denture cleansers periodically for a deeper clean. Always dry your nightguard completely before storing it in its protective case to prevent bacterial growth. Avoid hot water, harsh chemicals, or abrasive cleaners.
How long until I see results from wearing a nightguard?
Many individuals experience a noticeable reduction in symptoms such as jaw pain, headaches, and facial muscle soreness within a few days to a week of consistently wearing a custom-fitted nightguard. For significant tooth protection, the benefits accumulate over time, preventing further wear and damage. Full adaptation to the nightguard and maximum symptom relief may take a few weeks as your jaw muscles learn to relax. Consistency is key for optimal results.
When to See a Dentist
It's important to be proactive about your dental health and seek professional advice if you suspect bruxism or are experiencing related symptoms.
Routine Care / When to Schedule an Appointment:
- Suspected Bruxism: If you or a bed partner notice grinding or clenching sounds during sleep.
- New or Worsening Symptoms: You start experiencing unexplained headaches (especially upon waking), jaw pain, facial soreness, or tooth sensitivity.
- Signs of Tooth Damage: You notice your teeth appear worn, flattened, chipped, or fractured.
- Difficulty Opening/Closing Jaw: Your jaw feels stiff, tired, or you have limited range of motion.
- TMJ Symptoms: You hear clicking, popping, or grating sounds in your jaw joint.
- Regular Dental Check-ups: Your dentist can often spot early signs of bruxism even before you experience severe symptoms, during your routine exams.
Emergency Signs / When to See a Dentist Immediately:
- Severe, Acute Jaw Pain: Sudden, intense pain in your jaw or TMJ area that doesn't subside.
- Jaw Locking: Your jaw locks in an open or closed position, making it impossible to move.
- Facial Swelling: Unexplained swelling around your jaw or face, especially if accompanied by fever.
- Broken Tooth or Filling: If a significant portion of a tooth breaks off, or a filling falls out due to grinding, creating sharp edges or extreme sensitivity.
Early diagnosis and treatment of bruxism are vital to prevent irreversible damage to your teeth, gums, and TMJ, saving you from more extensive and costly dental procedures down the line. Don't hesitate to consult your dentist if you have any concerns about your dental health.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.