Mandible
4,542 words · 15 min read
Quick Definition
The lower jawbone, which is the largest and strongest bone of the face. The mandible holds the lower teeth and is the only movable bone in the skull.
The mandible, commonly known as the lower jawbone, stands as one of the most critical and distinct bones in the human skull. It is the largest and strongest bone of the face, performing a multitude of functions essential for daily life. Unlike any other bone in the skull, the mandible is uniquely movable, allowing for the complex actions of chewing, speaking, and facial expression. This exceptional mobility is facilitated by its articulation with the temporal bones of the skull, forming the Temporomandibular Joints (TMJ), which are among the most frequently used joints in the entire body.
For optimal dental health, understanding the mandible is paramount. Its primary role in anchoring the lower teeth directly impacts occlusion (how the upper and lower teeth meet), alignment, and the overall stability of your bite. Issues affecting the mandible, whether structural, functional, or traumatic, can profoundly impact an individual's ability to eat, speak, and even breathe comfortably, leading to widespread pain and significant quality-of-life concerns.
Mandibular disorders are more common than many people realize. For instance, Temporomandibular Joint (TMJ) disorders – often referred to broadly as "TMJ" – are estimated to affect over 35 million Americans annually, with women being disproportionately affected. Mandibular fractures, while less common, account for roughly 15% of all facial fractures, often resulting from trauma. Recognizing the signs of these conditions and understanding the treatment options is crucial for maintaining a healthy and functional smile. This comprehensive guide aims to be the definitive resource for anyone seeking to understand the mandible, its functions, common ailments, and what to expect from dental care related to this vital bone.
Key Takeaways:
- The mandible is the lower jawbone, the strongest and only movable bone of the skull, holding the lower teeth.
- It forms the Temporomandibular Joints (TMJ), crucial for chewing, speaking, and facial expression.
- Mandibular issues, including TMJ disorders and fractures, are common and can severely impact quality of life.
- Understanding the mandible's anatomy and common problems is key to maintaining overall oral health.
- Early diagnosis and intervention are vital for effective treatment and preventing long-term complications.
- Proper care and preventive measures can significantly reduce the risk of mandibular problems.
Detailed Explanation
The mandible is a U-shaped bone that forms the entire lower jaw. Its unique structure and mobility make it central to mastication (chewing), speech, and the overall aesthetic balance of the face. Understanding its intricate anatomy and diverse functions is the first step in appreciating its significance in dental health.
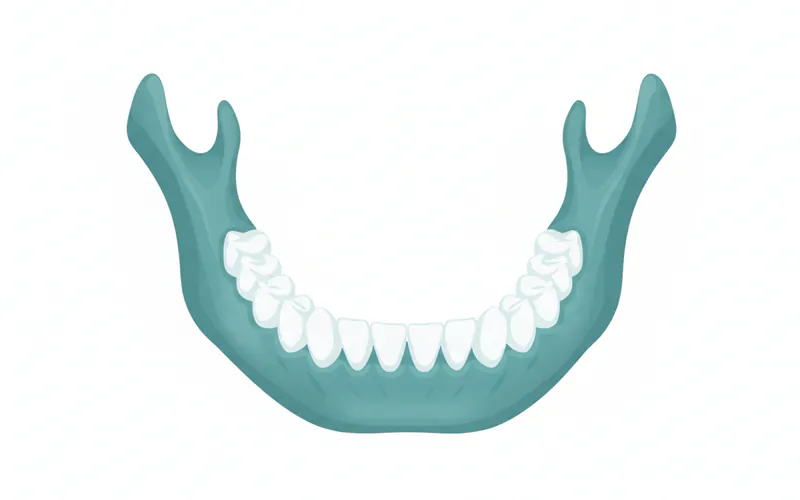
Anatomy and Function of the Mandible
The mandible is a marvel of biological engineering, designed for both strength and intricate movement. It consists of several key parts:
- Body: The horizontal, horseshoe-shaped part that forms the chin and anchors the lower teeth. It contains the alveolar process, which houses the tooth sockets (alveoli).
- Rami (plural for ramus): Two vertical plates that extend upwards from the posterior ends of the body. Each ramus has two processes at its superior end:
- Condylar Process: The posterior projection that articulates with the temporal bone of the skull to form the Temporomandibular Joint (TMJ). The rounded head of the condyle is critical for smooth jaw movement.
- Coronoid Process: The anterior projection, which serves as an attachment point for the temporalis muscle, a powerful muscle involved in closing the jaw.
- Angle of the Mandible: The point where the body and ramus meet, often a prominent landmark on the face.
- Mental Foramen: A small opening on the external surface of the body, typically below the premolars, through which nerves and blood vessels pass to supply the lower lip and chin.
- Mandibular Foramen: An opening on the medial surface of each ramus, allowing the inferior alveolar nerve (which supplies sensation to the lower teeth) and blood vessels to enter the bone.
The primary functions of the mandible include:
- Mastication (Chewing): Working in conjunction with the maxilla (the upper jawbone), the mandible's mobility allows for the grinding and tearing of food, the first step in digestion.
- Speech Articulation: The movement of the mandible is crucial for forming various sounds and words, allowing for clear communication.
- Support for Lower Teeth: The alveolar process securely holds the roots of the lower teeth, ensuring their stability during chewing and speaking.
- Facial Structure: The mandible contributes significantly to the shape and profile of the lower face.
- Protection: It provides a degree of protection for the soft tissues of the mouth and throat.
Common Conditions Affecting the Mandible
A variety of conditions can impact the mandible, ranging from traumatic injuries to chronic degenerative diseases.
1. Temporomandibular Joint (TMJ) Disorders
Often simply referred to as "TMJ," these disorders encompass a group of conditions causing pain and dysfunction in the jaw joint and the muscles that control jaw movement. They are among the most prevalent non-dental facial pain conditions, affecting an estimated 5% to 12% of the US population.
- Causes: Stress (leading to bruxism or teeth clenching/grinding), trauma to the jaw or head, arthritis (osteoarthritis, rheumatoid arthritis), disc displacement within the TMJ, congenital anomalies, and sometimes unknown factors.
- Types:
- Myofascial Pain: Pain in the muscles that control jaw function.
- Internal Derangement of the Joint: Displaced disc, dislocated jaw, or injury to the condyle.
- Degenerative Joint Disease: Arthritis in the jaw joint.
- Symptoms: Pain or tenderness in the jaw, ear, face, neck, or shoulders; clicking, popping, or grating sounds when opening or closing the mouth; difficulty chewing or discomfort while chewing; limited range of motion or jaw locking; changes in how the upper and lower teeth fit together (malocclusion).
2. Mandibular Fractures
A break in the mandible, usually caused by significant trauma. These are common facial fractures due to the mandible's exposed position.
- Causes: Motor vehicle accidents (most common, ~40-50%), assaults, sports injuries, falls, and industrial accidents.
- Types: Classified by location (symphysis, body, angle, ramus, condylar, coronoid process), type of fracture (simple, compound, comminuted), and displacement.
- Symptoms: Severe pain, swelling, bruising, difficulty opening or closing the mouth, inability to chew, numbness of the lower lip/chin, malocclusion, and bleeding.
3. Osteomyelitis of the Mandible
A serious infection of the mandibular bone, often resulting from odontogenic (dental) infections, trauma, or surgery.
- Causes: Untreated dental infections, complicated extractions, local trauma, systemic conditions like diabetes.
- Symptoms: Severe pain, swelling, fever, pus discharge, numbness, difficulty opening mouth, and potential bone necrosis.
4. Cysts and Tumors
Abnormal growths within the mandible can be benign (non-cancerous) or malignant (cancerous).
- Causes: Developmental abnormalities, genetic predispositions, chronic irritation, or unknown factors. Oral cancers can metastasize to the jawbone.
- Symptoms: Swelling, pain, numbness, tooth mobility, difficulty chewing, and facial asymmetry. Early detection is crucial for malignant lesions.
5. Ankylosis of the TMJ
A rare but severe condition where the condyle of the mandible fuses with the temporal bone, severely restricting or completely preventing jaw movement.
- Causes: Trauma (especially in children), infection, or systemic inflammatory diseases.
- Symptoms: Profound limitation in mouth opening (trismus), facial asymmetry, and difficulty with eating and speaking.
6. Mandibular Hypoplasia/Hyperplasia
Developmental conditions where the mandible is either underdeveloped (hypoplasia) or overdeveloped (hyperplasia), leading to significant facial and occlusal discrepancies.
- Causes: Congenital (e.g., Treacher Collins syndrome, hemifacial microsomia) or acquired during growth.
- Symptoms: Facial asymmetry, malocclusion, difficulty chewing, and speech problems.
Signs and Symptoms to Watch For
Recognizing potential issues with your mandible early can prevent more severe complications. Pay attention to any persistent or unusual symptoms in your jaw area:
- Pain: Persistent pain or tenderness in the jaw, face, ear, neck, or temple. This can range from a dull ache to sharp, shooting pain.
- Sounds: Clicking, popping, grinding, or grating sounds when opening or closing your mouth. While occasional sounds might be benign, persistent or painful sounds warrant attention.
- Restricted Movement: Difficulty opening your mouth widely, or feeling like your jaw is "locked" or "gets stuck."
- Malocclusion: A noticeable change in how your upper and lower teeth fit together, or feeling like your bite is "off."
- Swelling and Bruising: Localized swelling, tenderness, or bruising around the jaw, especially after an injury.
- Difficulty with Oral Functions: Trouble chewing, biting, swallowing, or speaking clearly.
- Numbness or Tingling: Sensations of numbness or tingling in the lower lip or chin (often indicative of nerve involvement).
- Headaches/Earaches: Frequent headaches, earaches, or ringing in the ears (tinnitus) that don't have another clear cause.
Diagnosis Process — What Your Dentist Does
Diagnosing a mandibular condition typically involves a thorough clinical examination combined with advanced imaging.
- Patient History: Your dentist will start by asking detailed questions about your symptoms, their duration, severity, contributing factors (e.g., trauma, stress), and any relevant medical history.
- Clinical Examination:
- Palpation: Your dentist will gently feel your jaw joints and the surrounding muscles to check for pain, tenderness, or muscle spasms.
- Range of Motion: They will assess how widely you can open and close your mouth, and if there's any deviation or limitation in movement.
- Auscultation: Listening for clicking, popping, or grating sounds in your TMJ using a stethoscope.
- Occlusal Analysis: Examining your bite for any signs of malocclusion, teeth grinding (bruxism), or abnormal wear patterns.
- Intraoral Examination: Checking for dental infections, gum disease, or other oral pathologies that could be affecting the mandible.
- Imaging Studies:
- Dental X-rays: Panoramic X-rays (orthopantomograms) provide a comprehensive view of the entire mandible, including the TMJs, teeth, and surrounding bone structures. Periapical X-rays focus on individual teeth and their roots.
- Computed Tomography (CT) Scan: Provides detailed cross-sectional images of the bone, excellent for diagnosing fractures, bone lesions, and assessing bone density.
- Magnetic Resonance Imaging (MRI): Best for visualizing soft tissues, such as the articular disc within the TMJ, ligaments, and muscles. Essential for diagnosing disc displacement and inflammation.
- Cone Beam Computed Tomography (CBCT): A specialized CT scan that produces 3D images with lower radiation doses than conventional CT, ideal for detailed assessment of the TMJ and dental structures.
Treatment Options with Pros, Cons, and Costs
Treatment for mandibular conditions varies widely depending on the underlying cause, severity, and individual patient needs. Options range from conservative, non-invasive therapies to complex surgical procedures.
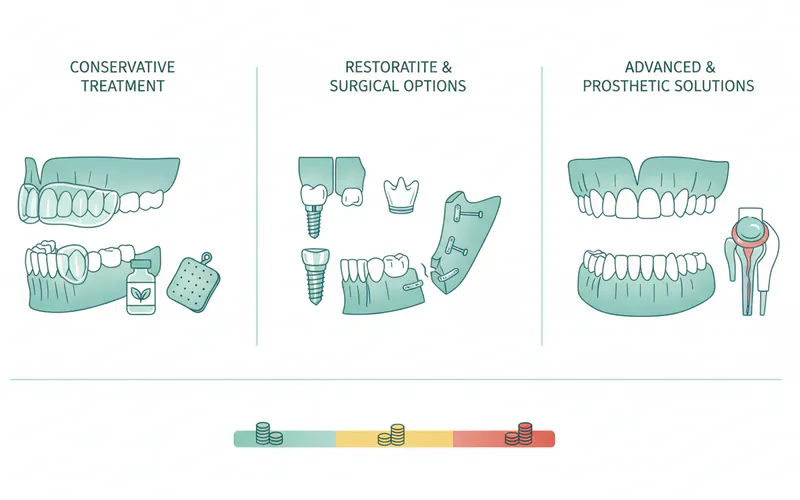
Non-Surgical Treatment Options
These are often the first line of defense, particularly for TMJ disorders and milder cases of inflammation or muscle pain.
| Treatment Option | Pros | Cons | Typical Cost Range (US) (without insurance) |
|---|---|---|---|
| Medications | Pain relief, muscle relaxation, inflammation reduction | Side effects, temporary relief, doesn't address underlying cause | $10-$200 per prescription |
| (NSAIDs, muscle relaxants, corticosteroids) | |||
| Oral Appliances | (Nightguards, splints) Protect teeth from bruxism, stabilize TMJ, reduce muscle strain | Can be uncomfortable, require consistent use, may need adjustments | $300-$800 (for custom nightguard/splint) |
| Physical Therapy/Exercises | Improves range of motion, strengthens muscles, reduces pain | Requires patient compliance, slow progress | $50-$200 per session (often 6-12 sessions needed) |
| Lifestyle Modifications | Reduces stress, avoids aggravating factors, generally low cost | Requires significant patient commitment, may not be sufficient | Minimal (dietary changes, stress management techniques) |
| Botox Injections | Relaxes hyperactive jaw muscles, effective for pain/bruxism | Temporary (lasts 3-6 months), requires repeat injections, costly | $300-$1,000 per session (depending on units needed) |
| Arthrocentesis | Minimally invasive, flushes joint, reduces inflammation | May require multiple sessions, not always effective for disc issues | $500-$2,000 per joint |
Surgical Treatment Options
Reserved for cases that don't respond to conservative treatments, severe injuries (like fractures), or significant structural abnormalities.
| Treatment Option | Pros | Cons | Typical Cost Range (US) (without insurance) |
|---|---|---|---|
| TMJ Arthroscopy | Minimally invasive, diagnoses and treats certain joint problems | Limited scope, may not address severe damage, risks of surgery | $5,000-$15,000 per joint |
| Open-Joint Surgery | Directly repairs or reconstructs joint structures (e.g., disc repositioning, joint replacement) | Highly invasive, longer recovery, higher risks of complications | $15,000-$50,000+ per joint (depending on complexity and replacement) |
| Mandibular Fracture Repair | Restores function and aesthetics, stabilizes bone | Invasive, risk of infection, nerve damage, need for hardware removal | $2,000-$25,000 (varies greatly by complexity and hardware) |
| Cyst/Tumor Removal | Eliminates growth, prevents spread (for malignant cases) | Varies by size and location, potential for bone grafting | $1,000-$10,000+ (complex cases can be much higher) |
| Orthognathic Surgery | Corrects severe jaw discrepancies, improves bite and facial balance | Major surgery, long recovery, extensive planning, high cost | $20,000-$50,000+ |
Note on Costs: These are approximate ranges and can vary significantly based on the surgeon's fees, anesthesia costs, facility fees, geographic location, and whether the procedure is performed in an outpatient clinic or hospital. Insurance coverage is highly variable; always check with your provider.
Step-by-Step: What to Expect During Treatment
Let's look at what to expect for a few common scenarios:
For TMJ Splint Therapy:
- Initial Consultation & Diagnosis: Your dentist will perform an exam and potentially order X-rays or MRI.
- Impression Taking: Molds of your teeth are taken to create a custom-fitted splint (often called a nightguard or orthotic).
- Splint Fabrication & Delivery: The lab creates the splint, and you'll return for fitting and adjustments.
- Instructions & Usage: Your dentist will instruct you on how and when to wear the splint (e.g., primarily at night, or full-time), and how to care for it.
- Follow-up Appointments: Regular visits are needed to monitor progress, adjust the splint as your bite changes, and ensure comfort. This phase can last several months.
For Mandibular Fracture Repair (Open Reduction Internal Fixation - ORIF):
- Emergency Assessment: Initial stabilization, pain management, and detailed imaging (CT scan) to assess the fracture.
- Anesthesia: The procedure is typically performed under general anesthesia in a hospital setting.
- Incision: The surgeon makes an incision (either intraorally or externally on the face/neck, depending on the fracture location) to access the bone.
- Reduction & Fixation: The fractured bone segments are realigned ("reduced") and then secured with small titanium plates and screws ("internal fixation").
- Closure: The incisions are closed with sutures.
- Post-Operative Care: You'll likely stay in the hospital for a day or two, receiving pain medication and instructions for a soft or liquid diet. Jaw wiring may be used in some cases to stabilize the jaw.
Recovery Timeline and Aftercare
Recovery timelines vary drastically depending on the condition and treatment complexity.
- Non-Surgical (e.g., splints, physical therapy, medication):
- Timeline: Improvements can be noticed within weeks to a few months. Full resolution may take 6-12 months, or ongoing management may be required for chronic conditions.
- Aftercare: Consistent use of appliances, adherence to exercises, dietary modifications (soft foods), stress management, and regular follow-up with your dentist/therapist.
- Surgical (e.g., fracture repair, TMJ surgery):
- Timeline: Initial healing takes 4-8 weeks. Full recovery, including regaining normal function, can take 3-6 months or longer.
- Aftercare:
- Pain Management: Prescription pain relievers initially, then over-the-counter options.
- Diet: A soft or liquid diet is crucial for several weeks to allow the bone and tissues to heal. Hard, chewy, or crunchy foods must be avoided.
- Oral Hygiene: Gentle cleaning, often with antiseptic rinses, is vital to prevent infection.
- Activity Restrictions: Avoid strenuous activity, contact sports, and any trauma to the jaw area for several months.
- Physical Therapy: Often begins shortly after surgery to restore range of motion and strength.
- Follow-up: Regular appointments with your surgeon to monitor healing and remove any non-dissolving sutures.
Prevention Strategies
While not all mandibular problems are preventable, several strategies can significantly reduce your risk:
- Protect Your Jaw from Trauma: Wear a custom-fitted mouthguard during sports or activities with a risk of facial injury. Use seatbelts in vehicles.
- Manage Stress: Stress and anxiety can lead to bruxism (teeth grinding/clenching), a major contributor to TMJ disorders. Practice relaxation techniques, meditation, or seek professional help for stress management.
- Avoid Excessive Jaw Habits: Refrain from clenching your teeth, chewing gum excessively, biting nails, or using your teeth to open packages.
- Maintain Good Posture: Poor posture can strain the neck and jaw muscles, contributing to TMJ pain.
- Regular Dental Check-ups: Routine visits allow your dentist to identify early signs of bruxism, malocclusion, or other issues that could affect your mandible. They can also address dental infections promptly before they spread to the bone.
- Eat a Balanced Diet: A diet rich in calcium and Vitamin D supports strong bones.
- Proper Ergonomics: If you work at a computer, ensure your screen is at eye level and your workstation promotes good posture.
Cost Ranges in the US (with/without insurance)
The cost of treating mandibular conditions in the US varies widely due to factors like the complexity of the condition, geographic location, provider's fees, and facility charges. Insurance coverage is a critical factor.
- Dental Insurance: Typically covers a portion of diagnostic X-rays, basic oral appliances (like nightguards for bruxism), and sometimes parts of fracture repair if it's considered a dental emergency. It rarely covers major medical procedures like extensive TMJ surgery or orthognathic surgery.
- Medical Insurance: Usually covers medically necessary procedures related to the mandible, such as fracture repair, TMJ surgery (especially for severe conditions like ankylosis or significant disc displacement), and tumor removal. Diagnostic imaging (CT, MRI) is usually covered.
- Without Insurance (Estimated Ranges):
- Consultation & Basic X-rays: $100 - $500
- Custom Nightguard/Splint: $300 - $800
- Botox for TMJ/Bruxism: $300 - $1,000 per session (often not covered by insurance)
- Physical Therapy: $50 - $200 per session
- TMJ Arthroscopy: $5,000 - $15,000 per joint
- Open TMJ Surgery: $15,000 - $50,000+ per joint (can be much higher for total joint replacement)
- Mandibular Fracture Repair (ORIF): $2,000 - $25,000+ (depending on severity, hospital stay, and hardware)
- Orthognathic Surgery: $20,000 - $50,000+ (often involves orthodontics too)
It's imperative to get a detailed breakdown of costs from your provider and verify your insurance coverage (both dental and medical) before proceeding with any treatment. Many offices offer payment plans or financing options.
Comparison Table: Non-Surgical vs. Surgical TMJ Treatment
| Feature | Non-Surgical TMJ Treatment (e.g., splints, PT, meds) | Surgical TMJ Treatment (e.g., arthroscopy, open-joint) |
|---|---|---|
| Indications | Mild to moderate pain, muscle disorders, early disc displacement, conservative approach failure | Severe pain and dysfunction, locked jaw, significant structural damage, failed conservative treatment |
| Invasiveness | Minimal to non-invasive | Moderately to highly invasive |
| Risks | Minimal (discomfort, temporary bite changes) | Infection, nerve damage, anesthesia risks, scarring, longer recovery |
| Recovery Time | Weeks to months for improvement, ongoing management for chronic cases | Weeks for initial healing, months for full functional recovery |
| Cost | Lower (hundreds to low thousands) | Higher (thousands to tens of thousands, or more for joint replacement) |
| Effectiveness | Often highly effective for muscle-related pain and early disc issues | Can be very effective for structural problems, but last resort due to risks |
| Duration of Effect | Varies; can be long-term with adherence, or temporary if underlying issues persist | Can be long-lasting, but no guarantee of permanent relief; may require revisions |

For Parents / Pediatric Considerations
The mandible undergoes significant development throughout childhood and adolescence, making specific considerations vital for parents.
- Growth and Development: The mandible grows considerably from birth through puberty. Issues like early tooth loss, thumb sucking, or pacifier use can affect jaw growth and tooth alignment, leading to malocclusion or even early TMJ issues.
- Pediatric Mandibular Fractures: Children's bones are more flexible, but fractures can still occur, often from falls or playground accidents. Condylar fractures are relatively common in children and, if not managed properly, can affect jaw growth, leading to facial asymmetry or ankylosis.
- Congenital Anomalies: Some children are born with developmental issues of the mandible, such as micrognathia (abnormally small lower jaw) or hemifacial microsomia (underdevelopment of one side of the face, including the jaw). These often require early orthodontic and surgical intervention.
- Early TMJ Issues: While less common than in adults, children can develop TMJ disorders, often related to trauma, bruxism (especially sleep bruxism), or inflammatory conditions. Symptoms might include difficulty chewing, facial pain, or clicking sounds.
- Orthodontic Intervention: Early orthodontic assessment (around age 7) can identify jaw growth problems or malocclusion that may benefit from early intervention, such as expanders or functional appliances, to guide proper mandibular development.
Parents should seek dental consultation if their child experiences persistent jaw pain, difficulty chewing, noticeable facial asymmetry, or any clicking/popping sounds from the jaw.
Frequently Asked Questions
Is mandible pain always TMJ?
No, mandible pain is not always TMJ disorder. While TMJ disorders are a very common cause of jaw pain, other conditions can also lead to discomfort in the mandible. These include dental issues (cavities, gum disease, abscesses, impacted wisdom teeth), mandibular fractures, infections like osteomyelitis, nerve pain (trigeminal neuralgia), salivary gland issues, and even referred pain from other areas like the ears, sinuses, or neck muscles. A thorough dental examination is necessary to accurately diagnose the cause of your pain.
Can a broken mandible heal on its own?
While minor, non-displaced fractures of any bone might technically heal without intervention, a broken mandible typically requires professional medical and dental treatment for proper healing and to restore function. Without intervention, a fractured mandible can heal improperly, leading to severe malocclusion, chronic pain, infection, difficulty eating and speaking, and even facial deformity. Treatment usually involves stabilization (e.g., wiring the jaws shut, or using plates and screws) to ensure the bone segments unite correctly.
How long does TMJ treatment last?
The duration of TMJ treatment varies significantly depending on the specific diagnosis, severity of the condition, and chosen treatment approach. Conservative treatments like oral appliances or physical therapy might require several weeks to months to show significant improvement, with ongoing management for chronic issues. Surgical treatments involve initial healing of 4-8 weeks, but full recovery and functional restoration can take 3-6 months or even a year. Many individuals with chronic TMJ disorders may require ongoing management and lifestyle modifications to prevent recurrence of symptoms.
What foods should I avoid with mandible pain?
If you're experiencing mandible pain, especially due to TMJ disorders or recovering from surgery/injury, it's best to avoid foods that put excessive strain on your jaw. This includes:
- Hard foods: Nuts, raw carrots, apples (unless cut into small pieces), hard candies, crusty bread.
- Chewy foods: Gum, tough meats, bagels, caramel.
- Sticky foods: Taffy, sticky candies.
- Foods that require wide opening: Large sandwiches, burgers. Opt for a soft diet consisting of mashed potatoes, yogurt, smoothies, cooked vegetables, soft fish, eggs, and pasta.
Is surgery for the mandible always necessary?
No, surgery for the mandible is not always necessary. For many conditions, especially TMJ disorders, conservative and non-surgical treatments are the first line of approach and are often highly effective. Surgery is typically reserved for severe cases where conservative treatments have failed, or for specific conditions like significant mandibular fractures, advanced joint degeneration, or the removal of large cysts or tumors. Your dentist or oral surgeon will recommend surgery only when it is deemed the most appropriate and beneficial course of action.
How much does mandible surgery cost with insurance?
The cost of mandible surgery with insurance can vary greatly, ranging from a few hundred dollars to several thousands of dollars, depending on your specific insurance plan (deductibles, co-pays, out-of-pocket maximums), the type of surgery (e.g., minor arthroscopy vs. major open-joint reconstruction), and the facility where it's performed. For example, a TMJ arthroscopy might cost you a few thousand dollars out-of-pocket with a good medical insurance plan, while a complex mandibular fracture repair or orthognathic surgery could still leave you with $5,000-$15,000+ in expenses even with insurance. It is crucial to contact your insurance provider directly for a detailed breakdown of coverage and your estimated out-of-pocket costs.
What's the difference between the mandible and the jaw?
The terms "mandible" and "jaw" are often used interchangeably, but there's a subtle distinction. The mandible specifically refers to the lower jawbone. The broader term "jaw" can refer to both the upper and lower structures that hold the teeth. Therefore, when people talk about the "jaw," they might be referring to the mandible, the maxilla (upper jawbone), or the entire apparatus that includes both bones and the associated muscles and joints. In dental and medical contexts, "mandible" is used to specifically denote the lower jawbone.
When to See a Dentist
It's important to know when to seek professional dental or medical attention for issues related to your mandible.
Routine Care/Non-Emergency Situations (Schedule an appointment soon):
- Persistent Pain: Any ongoing pain or tenderness in your jaw, face, ear, or neck that doesn't resolve with basic home care (like over-the-counter pain relievers or a soft diet).
- Clicking or Popping Sounds: If you experience frequent clicking, popping, or grinding sounds in your jaw joints, especially if accompanied by pain or limited movement.
- Difficulty Chewing or Speaking: If you notice a change in your ability to chew food comfortably or speak clearly.
- Limited Jaw Movement: If your jaw feels stiff, "gets stuck," or you cannot open your mouth as widely as usual.
- Changes in Bite: If your teeth no longer fit together properly (malocclusion).
- Swelling or Tenderness: If you observe unexplained swelling or tenderness around your jaw.
- Signs of Bruxism: If you wake up with jaw pain, headaches, or notice excessive wear on your teeth, which might indicate teeth grinding or clenching.
Emergency Situations (Seek immediate dental or medical attention):
- Severe Trauma: If you've sustained a significant injury to your face or jaw (e.g., from an accident or assault), especially if accompanied by intense pain, bleeding, or difficulty moving your jaw.
- Inability to Close Your Mouth: If your jaw feels dislocated or "locked open" and you cannot close your mouth.
- Suspected Fracture: If you suspect your mandible is broken (e.g., due to severe pain, visible deformity, significant swelling, numbness of the lip, or difficulty biting down).
- Profuse Bleeding: Any uncontrollable bleeding from the mouth or jaw area.
- Signs of Infection: Rapidly spreading swelling, severe pain, fever, and pus discharge from the jaw area.
Your dentist is your primary resource for diagnosing and managing most conditions affecting the mandible. They can also refer you to a specialist, such as an oral and maxillofacial surgeon or an orthodontist, if advanced care is required. Early intervention often leads to better outcomes and prevents the progression of more serious problems.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.