Maxilla
4,222 words · 14 min read
Quick Definition
The upper jawbone, which holds the upper teeth, forms the floor of the eye sockets, and contains the maxillary sinuses. Unlike the mandible, the maxilla is fixed to the skull.
What is the Maxilla? The Definitive Guide to Your Upper Jawbone
Welcome to SmilePedia.net, your trusted resource for comprehensive dental health information. Today, we delve into one of the most fundamental yet often overlooked structures of the human face: the maxilla. If you've ever searched "what is maxilla" or "maxilla dental," you're in the right place. This in-depth guide will demystify your upper jaw bone, explaining its critical role in everything from chewing and speaking to breathing and facial aesthetics.

The maxilla is the central bone of your midface, forming your upper jaw. Unlike its mobile counterpart, the mandible (lower jaw), the maxilla is firmly fixed to the rest of the skull. It's not just a tooth-bearing structure; this complex bone forms the floor of your eye sockets, parts of your nasal cavity, and houses the maxillary sinuses – air-filled cavities vital for reducing skull weight and resonance of your voice. Understanding the maxilla is paramount for grasping concepts related to orthodontics, dental implants, facial trauma, and even sleep apnea. Issues affecting the maxilla can dramatically impact oral function, comfort, and overall quality of life for millions of Americans. For instance, maxilla-related conditions like malocclusions affect an estimated 25-30% of the US population, necessitating orthodontic or surgical intervention.
Key Takeaways:
- The maxilla is your fixed upper jaw bone, essential for facial structure.
- It holds all your upper teeth and is crucial for proper bite (occlusion).
- The maxilla forms the roof of your mouth (palate), floor of your eye sockets, and part of your nasal cavity.
- It contains the maxillary sinuses, which can impact dental procedures like implant placement.
- Issues with the maxilla can lead to problems with chewing, speaking, breathing, and facial aesthetics.
- Its health is vital for successful dental implant integration and orthodontic stability.
Detailed Explanation of the Maxilla
The maxilla is a pair of fused bones that together form the entire upper jaw. It is a cornerstone of facial anatomy, articulating with nine other facial bones and contributing significantly to the structural integrity of the face. Its intricate design allows it to withstand significant forces during mastication while providing housing for teeth and airways.
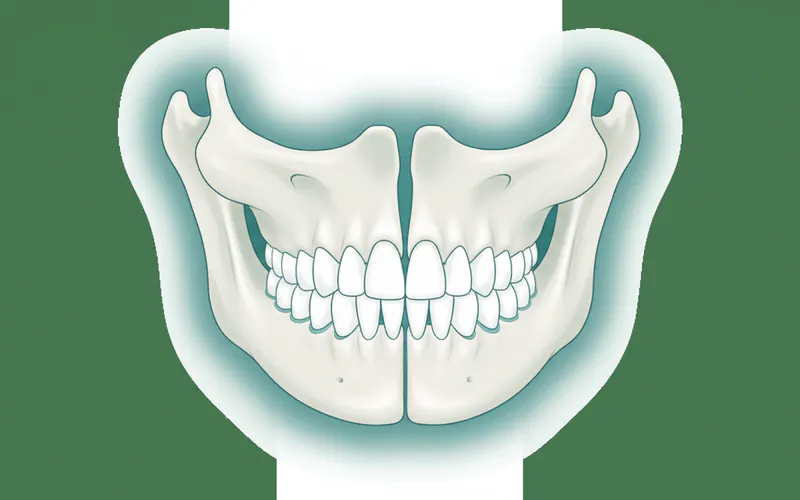
Anatomical Structure and Functions
- Alveolar Process: This is the thickest part of the maxilla that contains the sockets (alveoli) for the 16 upper teeth. The health and density of this bone are critical for supporting teeth and successful dental implant placement.
- Palatine Process: Extending horizontally, this process forms the anterior two-thirds of the hard palate (roof of the mouth). It separates the oral cavity from the nasal cavity, enabling us to chew and breathe simultaneously.
- Frontal Process: Extends upwards to meet the frontal bone, forming part of the side of the nose.
- Zygomatic Process: Projects laterally to join the zygomatic bone (cheekbone), contributing to facial prominence.
- Maxillary Sinuses: These large, air-filled cavities within the body of the maxilla lighten the skull, warm and moisten inhaled air, and contribute to voice resonance. Their proximity to the upper molar and premolar roots means dental infections can sometimes spread to the sinuses, and sinus anatomy can complicate dental implant procedures in the posterior upper jaw.
``
Types and Classifications of Maxillary Conditions
While there aren't "types" of maxilla, there are classifications of conditions that affect it, particularly relevant to maxilla dental health:
- Skeletal Malocclusions: These refer to misalignments of the upper and lower jaw bones relative to each other, often involving the maxilla.
- Class I Malocclusion: Ideal relationship between the maxilla and mandible, but teeth may still be crowded or misaligned.
- Class II Malocclusion (Overbite/Retrognathism): The maxilla is too far forward, or the mandible is too far back. This is common, affecting an estimated 15-20% of the US population, often requiring orthodontic treatment.
- Class III Malocclusion (Underbite/Prognathism): The mandible is too far forward, or the maxilla is underdeveloped. This can be more complex to treat, affecting about 5-10% of Americans.
- Maxillary Hypoplasia/Hyperplasia:
- Hypoplasia: Underdevelopment of the maxilla, leading to a recessed midface, often seen in Class III malocclusions or conditions like cleft lip and palate.
- Hyperplasia: Overdevelopment of the maxilla, leading to a protrusive upper jaw or a "gummy smile" (excessive gingival display).
- Alveolar Ridge Defects: Insufficient bone volume in the alveolar process of the maxilla due to tooth loss, trauma, or periodontal disease. This is a primary concern for dental implant candidacy.
- Maxillary Sinus Pathology: Infections (sinusitis), cysts, or tumors affecting the maxillary sinuses, which can have dental implications.
- Cleft Lip and Palate: A congenital condition where parts of the lip and/or palate fail to fuse during fetal development. This directly involves the maxilla and requires extensive multi-disciplinary treatment from infancy. Affects about 1 in 700 births in the US.
Causes and Risk Factors for Maxillary Issues
Problems with the maxilla can arise from a variety of sources:
- Genetics: Many skeletal malocclusions (Class II, Class III) and developmental abnormalities like cleft lip and palate have a strong genetic component.
- Trauma: Direct impacts to the face can cause fractures of the maxilla (Le Fort fractures being common classifications), leading to significant structural damage, tooth loss, and functional impairment.
- Developmental Abnormalities:
- Cleft Lip and Palate: A failure of proper fusion during embryonic development.
- Syndromic Conditions: Certain genetic syndromes (e.g., Apert syndrome, Crouzon syndrome) are associated with characteristic maxillary underdevelopment.
- Bone Resorption: After tooth extraction, the alveolar bone in the maxilla naturally begins to resorb or shrink. If not addressed, this can lead to insufficient bone for dental implants and changes in facial contours. Periodontal disease also contributes to bone loss.
- Infections and Tumors: Severe dental infections can erode maxillary bone or spread to the maxillary sinuses. Rarely, benign or malignant tumors can develop within the maxilla, requiring surgical intervention.
- Poor Oral Habits: In childhood, prolonged thumb-sucking or pacifier use can influence maxilla and palate development, potentially leading to an open bite or narrow palate.
- Systemic Diseases: Conditions like osteoporosis can reduce bone density, potentially impacting maxilla health and implant success.
Signs and Symptoms to Watch For
Recognizing signs of a maxilla dental problem is crucial for early intervention. Be alert for:
- Pain: Chronic facial pain, upper toothaches, or pain localized to the sinus area.
- Swelling: Unexplained swelling in the midface, under the eyes, or around the upper jaw.
- Difficulty Chewing or Speaking: A misaligned bite can make it hard to properly incise and chew food, or articulate words clearly.
- Malocclusion: A noticeable overbite, underbite, crossbite, or open bite where upper and lower teeth don't meet correctly.
- Loose or Missing Teeth: Can indicate underlying bone loss in the alveolar process.
- Facial Asymmetry: One side of the face appearing different from the other.
- Chronic Sinus Issues: Recurrent sinus infections, congestion, or drainage that could be linked to dental problems or structural issues within the maxilla.
- Breathing Problems: Especially through the nose, which can sometimes be exacerbated by maxillary constriction.
- Clicking or Popping: While often associated with the TMJ (temporomandibular jaw joint), severe maxillary issues can indirectly influence jaw joint function.
- "Gummy Smile": Excessive display of gum tissue when smiling, often due to maxillary excess.
Diagnosis Process — What Your Dentist Does
A thorough diagnosis of maxilla-related conditions involves a combination of clinical examination and advanced imaging:
- Clinical Examination: Your dentist or oral surgeon will perform a comprehensive visual and tactile examination of your face, mouth, and teeth. They will assess your bite, facial symmetry, and palpate the maxilla for any tenderness, swelling, or abnormalities. They will ask about your symptoms, medical history, and any trauma.
- Dental X-rays:
- Periapical X-rays: Provide detailed views of individual teeth and their surrounding alveolar bone.
- Bitewing X-rays: Show the crowns of upper and lower teeth, useful for assessing interproximal issues and bone levels.
- Panoramic X-ray (Panorex): Offers a broad view of the entire upper and lower jaw, including the maxilla, mandible, temporomandibular joints, and maxillary sinuses.
- Cephalometric X-ray: A lateral (side view) X-ray of the skull, used extensively in orthodontics and orthognathic surgery planning to assess the skeletal relationship between the maxilla and mandible.
- 3D Imaging (CBCT - Cone Beam Computed Tomography): This is a highly valuable tool, especially for complex cases. CBCT scans provide detailed 3D images of bone structure, nerve pathways, and soft tissues. They are indispensable for:
- Assessing bone volume and density for dental implant planning.
- Identifying precise locations of cysts, tumors, or infections.
- Planning orthognathic (jaw) surgery, allowing for virtual surgical simulation.
- Evaluating the relationship between tooth roots and the maxillary sinuses.
- Dental Impressions and Models: Casts of your teeth are made to study your occlusion (bite) in detail and plan orthodontic or surgical movements.
- Medical Consultations: In complex cases, collaboration with other specialists such as orthodontists, oral surgeons, ENTs (Ear, Nose, and Throat doctors), or plastic surgeons may be necessary.
Treatment Options with Pros, Cons, and Costs
Treatment for maxilla-related issues varies widely depending on the specific condition, its severity, and the patient's overall health. Here are common approaches:
| Treatment Option | Description | Pros | Cons | Estimated Cost (US, without insurance) |
|---|---|---|---|---|
| Orthodontics | Braces or clear aligners to move teeth and subtly influence jaw growth (in children) or compensate for minor skeletal discrepancies. | Non-invasive (no surgery), corrects bite, improves aesthetics. | Longer treatment duration (1-3 years), limited skeletal correction in adults. | $3,000 - $8,000 |
| Bone Grafting | Surgical procedure to add bone material (autogenous, allograft, xenograft, or alloplast) to areas of deficient maxillary bone. Often for implants. | Enables dental implant placement, restores lost bone volume, improves facial contour. | Surgical procedure, recovery time, risk of infection/graft failure, additional cost. | $400 - $3,000 per site |
| Sinus Lift (Sinus Augmentation) | A specific type of bone graft where the sinus membrane is gently lifted to create space for bone grafting, allowing for implant placement in the posterior maxilla. | Allows for implant placement in areas with insufficient bone due to large sinuses or bone loss. | Surgical procedure, longer healing time (4-9 months before implant placement), specific risks to sinus membrane. | $1,500 - $3,000 per sinus |
| Dental Implants | Surgical placement of titanium posts into the maxillary bone to replace missing teeth, acting as artificial tooth roots. | Permanent tooth replacement, preserves bone, high success rate (95-98%), natural feel and function. | Surgical procedure, requires adequate bone, higher initial cost, multi-stage process. | $3,000 - $6,000 per implant |
| Maxillary Osteotomy | Orthognathic surgery (jaw surgery) to reposition the entire maxilla (e.g., Le Fort I osteotomy) to correct severe malocclusions, facial asymmetry, or functional issues. | Corrects severe skeletal discrepancies, improves bite, aesthetics, breathing, and speech. | Major surgery, significant recovery time (6-12 weeks initial), risks of nerve damage, infection, numbness, costly. | $20,000 - $50,000+ (includes surgeon, anesthesia, hospital) |
| Palatal Expanders | Orthodontic appliance used primarily in children and adolescents to widen a narrow maxilla (and thus the palate). | Non-surgical (for children), creates space, corrects crossbite, improves breathing. | May require surgery in adults, temporary discomfort, visibility of appliance. | $1,500 - $4,000 |
| Trauma Repair | Surgical reduction and fixation of maxillary fractures using plates and screws. | Restores facial structure and function after injury, prevents long-term complications. | Emergency surgery, complex, risks of infection, nerve damage, scarring. | $10,000 - $60,000+ (depending on severity) |
| Cleft Palate Repair | A series of surgeries to close the opening in the palate and reconstruct the maxilla in infancy/childhood. | Enables normal feeding, speech development, and facial aesthetics. | Multiple surgeries over years, long-term dental and speech therapy required, high overall cost. | Highly Variable (often covered by specialized programs/insurance) |
Note: Costs are estimates and can vary significantly based on geographic location, complexity of the case, surgeon's fees, anesthesia, hospital charges, and whether it's an emergency or elective procedure.
Step-by-Step: What to Expect During Treatment (Example: Maxillary Osteotomy)
Let's consider a common surgical treatment for severe maxillary issues: a Le Fort I Maxillary Osteotomy, often performed to correct Class II or Class III malocclusions or a "gummy smile."
- Pre-surgical Planning (Several Months):
- Orthodontics: You'll likely wear braces for 6-18 months before surgery to align your teeth within your current jaw structures.
- Imaging & Models: Extensive X-rays (including CBCT), cephalometric analyses, and dental impressions are taken.
- Virtual Surgical Planning: The surgical team uses 3D software to plan the precise movements of your maxilla, often creating custom surgical guides.
- Consultations: Meetings with your orthodontist, oral surgeon, and possibly other specialists to discuss the plan, risks, and recovery.
- The Day of Surgery:
- Anesthesia: You will receive general anesthesia in a hospital setting.
- Incisions: The surgeon makes incisions inside your mouth (no external scars) along the gum line above your upper teeth.
- Bone Cuts: Using specialized instruments, the surgeon carefully cuts the bone of the maxilla to allow it to be separated from the rest of the skull.
- Repositioning: The entire maxilla is then moved into its planned new position (forward, backward, upward, or rotated).
- Fixation: Small titanium plates and screws are used to secure the maxilla in its new position. These are biocompatible and usually remain permanently.
- Closure: The incisions are closed with dissolvable sutures.
- Duration: Maxillary osteotomy typically takes 2-4 hours.
- Immediate Post-operative Care (Hospital Stay 1-3 days):
- Monitoring: You'll be closely monitored as you recover from anesthesia.
- Pain Management: Medications will be administered to manage pain and swelling.
- Diet: You'll start with a liquid diet, progressing to soft foods.
- Jaw Immobilization: Your jaw may be gently wired shut or elastic bands used to guide your bite for the first few weeks.
Recovery Timeline and Aftercare
Recovery from maxillary surgery, or even significant bone grafting, is a process that requires patience and diligent adherence to post-operative instructions.
- Initial Swelling & Discomfort (First 1-2 Weeks): Significant swelling and bruising are common. Pain will be managed with prescribed medications. A liquid to soft diet is mandatory. Oral hygiene is critical, often involving gentle rinses. Most patients return to light, non-strenuous activities within 1-2 weeks.
- Healing & Gradual Improvement (Weeks 3-6): Swelling gradually subsides. You can typically transition to a pureed or very soft diet. Physical activity remains restricted. Your surgeon will monitor your healing during follow-up appointments. If the jaw was immobilized, elastic bands will likely replace wires around Week 3-4.
- Bone Consolidation (Months 2-6): The bones continue to heal and fuse in their new positions. You'll gradually introduce firmer foods as tolerated. Orthodontic treatment often resumes after 6-8 weeks to fine-tune the bite.
- Full Recovery (6-12 Months): Full bone consolidation takes up to a year. You should be able to resume all normal activities and diet. Numbness, if present, usually resolves over this period, though some subtle changes in sensation can be long-term.
Aftercare is crucial:
- Oral Hygiene: Meticulous but gentle cleaning, often with prescribed mouthwashes.
- Dietary Restrictions: Strictly follow dietary guidelines to protect the healing bones.
- Avoid Smoking/Alcohol: These can severely impair healing.
- Limit Strenuous Activity: No heavy lifting or contact sports until cleared by your surgeon.
- Regular Follow-ups: Attend all scheduled appointments with your surgeon and orthodontist.
Prevention Strategies
While some maxillary conditions are genetic or due to unavoidable trauma, several strategies can help prevent or mitigate issues:
- Protective Gear: Wear mouthguards during sports to prevent facial and jaw trauma.
- Good Oral Hygiene: Regular brushing, flossing, and dental check-ups prevent gum disease and tooth loss, which can lead to bone resorption in the maxilla.
- Early Orthodontic Intervention: For children, early assessment can identify and address developing malocclusions or narrow palates before they become more severe, often with less invasive treatments like palatal expanders.
- Address Habits in Children: Discourage prolonged thumb-sucking or pacifier use, which can affect maxillary growth and palate shape.
- Prompt Treatment of Missing Teeth: If a tooth is extracted from the maxilla, discuss options like dental implants or bridges with your dentist promptly to prevent significant bone loss.
- Avoid Smoking: Smoking is a major risk factor for periodontal disease and can compromise bone health, affecting implant success.
Cost Ranges in the US (with/without insurance)
The financial aspect of maxilla dental treatments can be substantial. Here’s a general overview:
- Orthodontics (Braces/Aligners):
- Without Insurance: $3,000 - $8,000.
- With Insurance: Dental insurance often covers a portion of orthodontic treatment, typically 25-50%, with lifetime maximums ranging from $1,000 - $3,000.
- Bone Grafting/Sinus Lift:
- Without Insurance: $400 - $3,000 per site for a bone graft; $1,500 - $3,000 per sinus lift.
- With Insurance: Dental insurance may offer limited coverage for grafting if it's considered part of a restorative procedure (e.g., prior to an implant). Medical insurance might cover it if medically necessary (e.g., after trauma or tumor removal).
- Dental Implants:
- Without Insurance: $3,000 - $6,000 per implant (not including crown). A full arch of implants can easily exceed $25,000 - $50,000.
- With Insurance: Dental insurance typically covers the crown and sometimes a small portion of the implant surgery. Some premium dental plans or medical insurance might cover more if a tooth loss was due to a medical condition or trauma.
- Maxillary Osteotomy (Orthognathic Surgery):
- Without Insurance: This is a major surgery, ranging from $20,000 - $50,000+. This includes surgeon's fees, anesthesia, and hospital costs.
- With Insurance: Medical insurance often provides significant coverage for orthognathic surgery if it's deemed medically necessary to correct functional problems (e.g., severe malocclusion impacting chewing/speech, sleep apnea). Coverage can range from 50-80% after deductibles. It's crucial to get pre-authorization.
- Cleft Lip and Palate Repair:
- Without Insurance: The total cost over a child's lifetime, including multiple surgeries, orthodontics, speech therapy, etc., can easily reach hundreds of thousands of dollars.
- With Insurance: Often covered by medical insurance due to its medical necessity. State programs and charities also provide significant financial assistance.
It's always recommended to discuss costs and insurance coverage thoroughly with your dental and medical providers, as well as your insurance company, before proceeding with any treatment.
For Parents / Pediatric Considerations
The development of the maxilla is a critical aspect of a child's overall facial and oral health. Parents play a vital role in monitoring and addressing potential issues early.
- Growth and Development: The maxilla grows significantly during childhood and adolescence. This period is opportune for interceptive orthodontics.
- Early Detection of Malocclusions: Keep an eye out for signs of crossbites (upper teeth bite inside lower teeth), open bites (front teeth don't meet), or significant overbites/underbites. These can sometimes be corrected with simpler appliances in childhood rather than surgery later.
- Impact of Oral Habits: Prolonged thumb-sucking, pacifier use beyond age 3-4, and tongue thrusting can exert pressure on the developing maxilla and palate, potentially leading to a narrow upper jaw, open bite, or anterior crossbite. Early intervention can redirect growth.
- Cleft Lip and Palate: If your child is born with a cleft lip or palate, a multidisciplinary team (oral surgeon, orthodontist, speech therapist, ENT) will be involved from birth to guide a series of treatments aimed at functional and aesthetic reconstruction of the maxilla and surrounding structures.
- Trauma Prevention: Encourage the use of mouthguards for children participating in sports to protect the developing maxilla and teeth from injury.
- Regular Dental Check-ups: Starting around age one, regular visits to a pediatric dentist can help identify and address any developmental concerns with the maxilla and teeth promptly. Early intervention can often lead to less extensive and less costly treatments.
``
Frequently Asked Questions
How painful is maxillary surgery or major maxilla dental treatment?
The level of pain varies. For procedures like bone grafts or sinus lifts, post-operative pain is typically managed with prescribed pain medication and subsides within a few days to a week. For major surgeries like maxillary osteotomy, the initial pain can be more significant, but it's well-controlled with strong pain medication. Most patients report more discomfort from swelling and the restricted diet than from severe pain after the first few days.
How long does recovery take for maxilla-related treatments?
Minor procedures like single bone grafts might have a recovery of 1-2 weeks before returning to normal activity, though bone maturation for implant placement takes 3-6 months. A sinus lift requires 4-9 months of healing before implants can be placed. Major maxillary surgery (osteotomy) involves 6-12 weeks for initial healing and several more months for full bone consolidation and nerve regeneration. Orthodontic treatment can take 1-3 years.
Can I get dental implants if my maxilla bone is weak or insufficient?
Yes, in many cases! This is a common challenge, especially in the posterior maxilla due to the presence of the maxillary sinuses and bone loss after tooth extraction. Procedures like bone grafting (to add bone height or width) and sinus lifts (to add bone in the sinus area) are specifically designed to regenerate sufficient bone to support dental implants. Your oral surgeon or periodontist will assess your bone quality and recommend the appropriate pre-implant procedure.
What's the difference between the maxilla and the mandible?
The maxilla is your upper jaw bone, which is a fixed part of your skull. It holds your upper teeth and is integral to your midface, contributing to your nasal cavity and eye sockets. The mandible is your lower jaw bone, which is the only movable bone of the skull. It articulates with the skull at the temporomandibular joints (TMJ), allowing you to chew, speak, and open and close your mouth. Both are crucial for dental function and facial structure, but their mobility is their key distinction.
Does insurance cover treatments for the maxilla?
Coverage varies significantly. Dental insurance typically covers routine dental care, some restorative work, and portions of orthodontics. Medical insurance may cover treatments if they are deemed medically necessary (e.g., correcting severe malocclusion affecting speech/chewing, trauma repair, tumor removal, or surgery for sleep apnea). Procedures like bone grafting for implant placement can fall into a gray area – sometimes partially covered by dental or medical if restorative, sometimes not. It's critical to verify coverage with both your dental and medical insurance providers and obtain pre-authorization for major procedures.
What are the alternatives to maxillary surgery for correcting bite problems?
For minor bite problems, orthodontics (braces or clear aligners) can often correct the issue by moving teeth. In growing children, functional appliances or palatal expanders can influence jaw growth. However, for severe skeletal discrepancies where the maxilla itself is significantly mispositioned or underdeveloped/overdeveloped relative to the mandible, surgical correction via maxillary osteotomy is often the only way to achieve a stable, functional, and aesthetically pleasing result. Non-surgical options in such cases might only camouflage the problem rather than truly correct it.
How do I know if I have a maxillary problem?
Many maxillary problems present with noticeable symptoms such as pain, swelling, difficulty chewing, speaking, or breathing, and visible changes in your bite or facial appearance. Persistent sinus issues or loose upper teeth can also be signs. If you experience any of these, or if you notice a significant change in your bite or facial structure, it's essential to see a dentist. They can perform a clinical examination and use imaging like X-rays or CBCT scans to diagnose the issue.
When to See a Dentist
Given the maxilla's critical role, knowing when to seek professional help is vital.
See a dentist for routine care or concerning symptoms:
- Persistent Pain: Any ongoing pain in your upper jaw, teeth, or face that doesn't resolve.
- Changes in Bite: If you notice your upper and lower teeth no longer fit together correctly.
- Difficulty Chewing or Speaking: If you struggle with these basic functions.
- Chronic Sinus Issues: Especially if accompanied by tooth sensitivity or drainage.
- Loose Upper Teeth: This could indicate underlying bone loss or periodontal disease.
- Planning Dental Implants: If you have missing upper teeth and are considering implants.
- Developmental Concerns in Children: If you observe unusual facial growth or oral habits in your child.
Seek immediate dental or medical attention (emergency signs):
- Facial Trauma: Any injury to your face that causes severe pain, swelling, bleeding, or a noticeable change in your jaw alignment. This could indicate a maxillary fracture.
- Acute, Severe Swelling: Rapidly progressing swelling, especially if it affects your breathing or vision.
- Uncontrolled Bleeding: From your mouth or nose after an injury.
- Sudden Numbness: In your face or upper jaw following trauma.
The maxilla is more than just a bone; it's a foundational element of your oral and facial health. Understanding its importance and knowing when to seek expert care can help ensure a lifetime of healthy smiles.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.