Palate
3,808 words · 13 min read
Quick Definition
The roof of the mouth, consisting of the hard palate (bony front portion) and the soft palate (muscular back portion). The palate separates the oral cavity from the nasal cavity.
Palate: The Definitive Guide to the Roof of Your Mouth
The palate, commonly known as the roof of the mouth, is a critical anatomical structure that plays a multifaceted role in speech, swallowing, breathing, and overall oral health. Far more than just a simple partition, this complex structure separates your oral cavity from your nasal cavity, forming an essential boundary that influences everything from the sounds you make to the way you taste food.
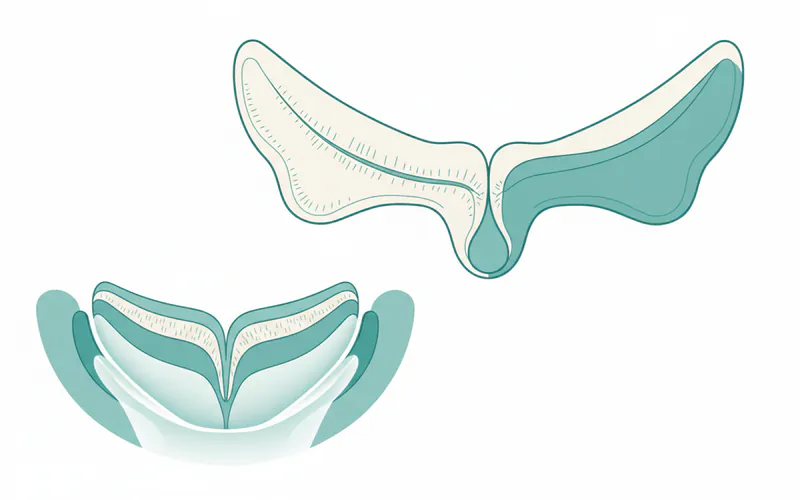
Understanding the palate is fundamental to appreciating its significance in dentistry. Issues with the palate can lead to a cascade of problems, impacting speech articulation, feeding efficiency, breathing patterns, and even the successful fitting of dental prosthetics like dentures. For example, conditions such as cleft palate are congenital anomalies that drastically alter a child's early development, necessitating extensive medical and dental intervention. Less severe but still impactful conditions like palatal tori can interfere with denture wear or oral hygiene.
In the United States, palatal health is a significant focus in dental and medical care. For instance, cleft lip and palate are among the most common birth defects, affecting approximately 1 in every 1,700 babies born in the U.S. (according to the CDC). While many palatal concerns are developmental, others can arise from trauma, infection, or even as benign anatomical variations. Regular dental check-ups are crucial for monitoring the health of your palate and addressing any concerns early, ensuring optimal oral function and quality of life.
Key Takeaways:
- Dual Structure: The palate is comprised of two main parts: the bony hard palate at the front and the muscular soft palate at the back, which includes the uvula.
- Vital Functions: It's essential for clear speech, efficient swallowing, proper breathing, and separating the oral and nasal cavities.
- Common Conditions: Issues can range from congenital defects like cleft palate to benign growths such as palatal tori, or even infections and cancerous lesions.
- Interconnectedness: The palate's health is closely linked to the maxilla (upper jaw bone), denture fit, and orthodontic treatments.
- Early Detection is Key: Persistent pain, swelling, lumps, discolored patches, or difficulty speaking/swallowing warrant immediate dental attention.
- Preventative Care: Good oral hygiene and regular dental check-ups are crucial for maintaining palatal health and detecting issues early.
Detailed Explanation
The palate is an intricate structure, vital for numerous physiological processes. Its dual nature, combining bone and muscle, allows it to serve both as a rigid separator and a flexible valve.
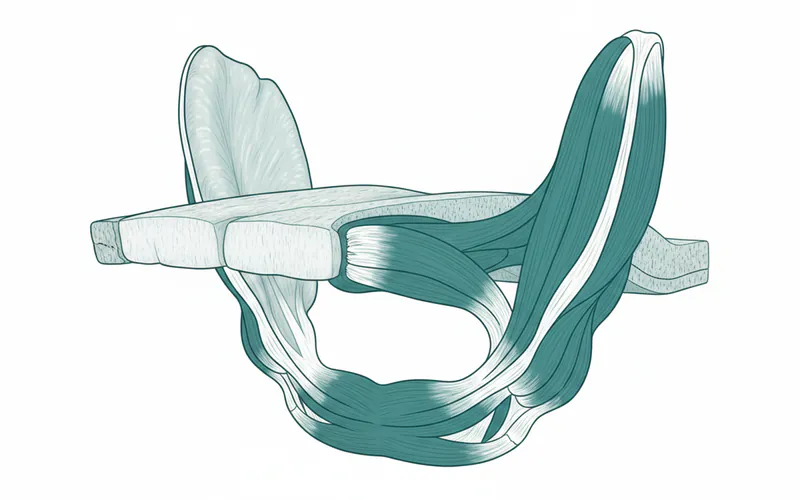
Types and Classifications
The palate is broadly divided into two distinct regions, each with unique anatomical features and functions:
-
The Hard Palate (Palatum Durum):
- Structure: This is the anterior (front) two-thirds of the palate, forming a rigid, bony vault. It is primarily composed of processes from the maxilla (the upper jaw bone) and the horizontal plates of the palatine bones. The median palatine raphe, a slightly raised line, runs down its center. The rugae, irregular ridges, are located on the anterior portion behind the upper incisors and aid in holding food during mastication.
- Function: The hard palate provides a firm surface against which the tongue presses food during chewing and swallowing. Its bony structure prevents food and liquids from entering the nasal cavity during these processes. It also plays a significant role in sound production, acting as a resonance chamber and providing a point of articulation for certain speech sounds.
- Related to Maxilla: The hard palate is a direct extension of the maxilla, forming its floor. Any structural issues with the maxilla can therefore impact the hard palate.
- ``
-
The Soft Palate (Velum Palati):
- Structure: This is the posterior (back) one-third of the palate, composed primarily of muscle and connective tissue, without any underlying bone. It extends posteriorly from the hard palate and terminates in a conical projection called the uvula. Five pairs of muscles work together to move the soft palate.
- Function: Unlike the rigid hard palate, the soft palate is highly mobile. During swallowing, it elevates to seal off the nasopharynx (the upper part of the throat behind the nose), preventing food and liquid from entering the nasal cavity. This action is known as velopharyngeal closure. It is also critical for speech, allowing for the production of non-nasal sounds by blocking airflow into the nasal cavity. When relaxed, it allows airflow through the nose, essential for nasal breathing.
- Uvula: The uvula, suspended from the soft palate, is thought to play a role in speech articulation, particularly in producing uvular consonants in some languages, and may also be involved in snoring and gag reflexes.
Anatomical Variations and Conditions:
- Palatal Tori (Torus Palatinus): These are benign, slow-growing, bony growths that can occur on the hard palate. They are typically asymptomatic but can become problematic if they grow large enough to interfere with denture placement, speech, or oral hygiene.
- Prevalence: Studies suggest palatal tori are present in 20-30% of the US population, with a higher incidence in females.
- ``
- Cleft Palate: A birth defect where the tissues of the palate do not fuse completely during fetal development, resulting in an opening between the mouth and nasal cavity. This can range from a small notch in the soft palate to a complete separation extending through the hard palate.
- High-Arched Palate: A palate that is unusually high and narrow. This can be genetic or associated with certain syndromes and may contribute to orthodontic issues or breathing difficulties.
- Palatal Abscess/Infection: Bacterial or fungal infections can occur on the palate, often presenting as painful sores, swelling, or pustules.
- Oral Cancer: While less common than on other oral sites, the palate (especially the soft palate) can be a site for oral squamous cell carcinoma or other malignancies.
Causes and Risk Factors (for Palatal Issues)
Understanding the origins of palatal problems is crucial for prevention and appropriate treatment.
- Cleft Palate:
- Genetics: Often runs in families, suggesting a genetic predisposition.
- Environmental Factors: Maternal exposure to certain substances during pregnancy, such as smoking, excessive alcohol consumption, and certain medications (e.g., anti-seizure drugs), can increase risk. Nutritional deficiencies (e.g., folic acid) may also play a role.
- Palatal Tori:
- Genetics: Strong genetic component; if a parent has tori, their children are more likely to develop them.
- Chewing Stress: Some theories suggest that increased chewing forces or chronic clenching/grinding of teeth (bruxism) may contribute to their development over time.
- Infections and Inflammation:
- Poor Oral Hygiene: Allows bacteria or fungi to proliferate.
- Trauma: Burns from hot food/drinks, sharp foods, or ill-fitting dentures can create entry points for infection.
- Systemic Conditions: Immunocompromised states (e.g., diabetes, HIV) can increase susceptibility.
- Trauma:
- Accidents: Falls, sports injuries, or car accidents can cause fractures or lacerations to the palate.
- Thermal Burns: Consuming excessively hot food or liquids is a common cause of palatal burns.
- Oral Cancer:
- Tobacco Use: Smoking, chewing tobacco, and snuff are major risk factors.
- Alcohol Consumption: Heavy and prolonged alcohol use increases risk, especially when combined with tobacco.
- Human Papillomavirus (HPV): Certain high-risk strains of HPV are increasingly linked to oropharyngeal cancers, including those on the soft palate.
- Excessive Sun Exposure: Can contribute to lip and potentially hard palate cancers.
- Age: Risk generally increases with age.
Signs and Symptoms to Watch For
Recognizing potential problems early is key to successful intervention. Consult a dentist if you experience any of the following:
- Persistent Pain or Soreness: Especially if it doesn't resolve within a week or two.
- Lumps, Bumps, or Growths: While many are benign (like tori), new or changing growths should always be evaluated.
- White or Red Patches: Persistent discolored areas on the palate, especially if they are rough, can be precancerous or cancerous.
- Difficulty Swallowing (Dysphagia) or Speaking: Can indicate issues with the soft palate's function or a mass obstructing normal movement.
- Sores that Don't Heal: Any ulcer or sore on the palate that persists for more than 2-3 weeks needs professional attention.
- Changes in Voice Quality: Nasal-sounding speech (hypernasality) can suggest issues with soft palate closure.
- Unexplained Bleeding: Especially if not associated with trauma.
- Numbness or Tingling: A less common but serious symptom that could indicate nerve involvement.
- Loose Teeth or Dentures that No Longer Fit: Changes in palate shape or structure can impact dental stability.
Diagnosis Process — What Your Dentist Does
A thorough diagnostic process helps pinpoint the exact nature of any palatal issue.
- Comprehensive Oral Examination: Your dentist will visually inspect your entire oral cavity, including a careful examination of your hard and soft palate. They will use a mirror and light to look for any abnormalities, changes in color, swelling, or lesions.
- Palpation: The dentist will gently feel your palate with gloved fingers to check for lumps, tenderness, texture changes, or bony growths (like palatal tori).
- Medical and Dental History Review: Discussion of your symptoms, their duration, any risk factors (e.g., smoking, alcohol), and relevant medical conditions.
- Imaging:
- Dental X-rays: Periapical or panoramic X-rays may be used to assess underlying bone structure, especially for issues related to the hard palate or maxilla.
- CT Scans or MRI: For more complex cases, such as suspected tumors, infections extending into deeper tissues, or assessing the extent of cleft palate, advanced imaging provides detailed cross-sectional views.
- Biopsy: If a suspicious lesion (e.g., a persistent white or red patch, an ulcer, or a rapidly growing lump) is found, a small tissue sample will be taken and sent to a lab for microscopic examination. This is the definitive way to diagnose precancerous changes or oral cancer.
- Referral to Specialist: Depending on the diagnosis, your dentist may refer you to an oral and maxillofacial surgeon, periodontist, orthodontist, or an ENT (Ear, Nose, and Throat) specialist.
Treatment Options with Pros, Cons, and Costs
Treatment for palatal issues varies widely depending on the underlying condition.
| Treatment Option | Condition Treated | Pros | Cons | Estimated Cost Range (US) (without insurance) |
|---|---|---|---|---|
| Excision of Palatal Torus | Palatal Tori | Improves comfort for denture wear; prevents trauma to overlying mucosa | Invasive surgical procedure; risk of infection, bleeding, or recurrence; temporary dietary restrictions | $1,000 - $3,000 |
| Cleft Palate Repair (Palatoplasty) | Cleft Palate | Restores normal feeding, speech, and dental development; improves facial aesthetics | Requires multiple surgeries (often over years); lengthy recovery; potential for speech therapy and orthodontic treatment | $5,000 - $20,000+ per surgery (can be covered by medical insurance) |
| Palatal Expander | Narrow Palate, Crossbite (related to Orthodontics) | Widens upper jaw; corrects bite issues; creates space for crowded teeth | Initial discomfort; visible appliance; requires consistent adjustments; lengthy treatment time (months-years) | $1,500 - $4,000 (often part of larger orthodontic treatment) |
| Antibiotics/Antifungals | Palatal Infections | Non-invasive; resolves infection quickly; relatively low cost | May require multiple doses; potential for side effects (e.g., GI upset); recurrence if underlying cause not addressed | $20 - $200 (medication cost) |
| Surgical Excision of Lesion | Benign/Precancerous Lesions | Removes problematic tissue; definitive diagnosis | Invasive; may require stitches; recovery time | $500 - $3,000+ |
| Oral Cancer Treatment | Oral Cancer | Life-saving; removes cancerous cells | Highly invasive (surgery, radiation, chemo); significant side effects; long recovery; high cost | $10,000 - $100,000+ (can be covered by medical insurance) |
| Denture Adjustment/Reline | Ill-fitting Dentures (due to palatal changes) | Improves comfort, fit, and function of dentures | Temporary fix if underlying palatal issue progresses; may need new dentures eventually | $100 - $400 |
Note: Costs are estimates and can vary significantly based on location, complexity, and practitioner fees. Insurance coverage varies widely.
Step-by-Step: What to Expect During Treatment (Example: Palatal Tori Removal)
If you require surgical removal of palatal tori, here’s a typical outline of what to expect:
- Consultation and Planning: Your oral surgeon will discuss the procedure, potential risks, and benefits. X-rays may be taken to assess the extent of the tori and proximity to other structures. You'll receive pre-operative instructions.
- Anesthesia: On the day of the procedure, local anesthesia will be administered to numb the surgical area completely. For anxious patients or more complex cases, sedation (oral or intravenous) may also be offered.
- Incision: The surgeon will make a small incision along the ridge of the torus to expose the underlying bone.
- Bone Removal: Specialized instruments (e.g., a surgical bur or bone chisel) are used to carefully reduce or remove the bony growth. The surgeon will work meticulously to reshape the palate, ensuring a smooth contour.
- Suturing: Once the desired contour is achieved, the gum tissue is repositioned over the area, and sutures (stitches) are placed to close the incision. These may be dissolvable or require removal at a follow-up appointment.
- Post-Operative Instructions: You'll receive detailed instructions on pain management, diet, oral hygiene, and signs of complications to watch for.
Recovery Timeline and Aftercare (Example: Palatal Tori Removal)
- Immediately After: You will feel numbness for several hours. Mild pain and swelling are common.
- First Few Days: Pain can be managed with over-the-counter pain relievers or prescribed medication. Swelling usually peaks on day 2-3. A soft diet is recommended to avoid irritating the surgical site. Avoid very hot, spicy, or crunchy foods.
- First Week: Continue with a soft diet. Gentle oral hygiene is crucial, typically involving saline rinses or a prescribed antimicrobial mouthwash. Avoid brushing directly on the surgical site.
- 2-4 Weeks: Most swelling and discomfort should resolve. If non-dissolvable sutures were used, they will be removed around 7-10 days post-op. The tissue continues to heal and strengthen. You can gradually return to a more normal diet.
- Full Recovery: Complete healing of the soft tissue takes approximately 4-6 weeks. The underlying bone takes longer to remodel, but this typically doesn't impact daily function.
- Aftercare: Follow all post-operative instructions diligently. Avoid smoking and alcohol, as they can impair healing. Attend all follow-up appointments.
Prevention Strategies
While some palatal issues are genetic or developmental, many can be prevented or mitigated.
- Good Oral Hygiene: Brush twice daily and floss once daily to prevent infections and maintain overall oral health.
- Avoid Tobacco and Excessive Alcohol: These are major risk factors for oral cancers, including those affecting the palate.
- Protective Gear for Sports: Wearing a mouthguard during contact sports can prevent traumatic injuries to the palate and other oral structures.
- Regular Dental Check-ups: Routine visits (typically every 6 months) allow your dentist to examine your palate for any early signs of issues, including benign growths, infections, or potentially cancerous lesions. Early detection is key to successful treatment.
- Healthy Diet: A balanced diet supports overall health, including the immune system, which helps prevent infections.
- Limit Hot Foods/Drinks: Be cautious with very hot foods and beverages to avoid thermal burns to the palate.
- Manage Bruxism: If you clench or grind your teeth, discuss solutions with your dentist, as this can contribute to palatal tori development.
- Maternal Health During Pregnancy: For expecting parents, maintaining good health, avoiding smoking/alcohol, and discussing all medications with a healthcare provider can reduce the risk of congenital conditions like cleft palate.
Cost Ranges in the US (with/without insurance)
The cost of palatal treatments in the US varies significantly based on the complexity of the procedure, the practitioner's fees, geographic location, and whether it's covered by dental or medical insurance.
- Routine Check-up (includes palatal exam): $50 - $200 (often covered by dental insurance with a copay).
- X-rays: $25 - $200 per set.
- Biopsy (incisional): $200 - $800 (cost of procedure, lab fees additional).
- Palatal Tori Removal: As mentioned above, $1,000 - $3,000. Dental insurance may cover a portion if deemed medically necessary (e.g., interfering with denture placement).
- Cleft Palate Repair: As mentioned above, $5,000 - $20,000+ per surgery. These complex surgeries are typically considered medical procedures and are often covered by medical insurance, though deductibles and out-of-pocket maximums apply.
- Palatal Expander (Orthodontics): $1,500 - $4,000 for the appliance and initial fitting. This is usually part of a larger orthodontic treatment plan, which can range from $3,000 - $8,000 for comprehensive care. Dental insurance with orthodontic benefits may cover 25-50%.
- Treatment for Infections (medication): $20 - $200. Generally not covered by dental insurance; often covered by medical insurance for prescription drugs.
With Insurance: For procedures deemed medically necessary (like cleft palate repair or oral cancer treatment), medical insurance typically provides significant coverage, though you will be responsible for deductibles, copayments, and coinsurance (e.g., 10-50% of the cost after deductible). For dental procedures, dental insurance may cover 50-80% of the cost of basic services (like fillings, extractions) and sometimes 50% for major services (like oral surgery or dentures), up to an annual maximum (e.g., $1,000 - $2,000). Orthodontics often has separate lifetime maximums.
It's crucial to contact your specific insurance provider to understand your benefits and coverage before undergoing any significant procedure. Many offices can help you verify benefits and provide a detailed estimate of your out-of-pocket costs.
For Parents / Pediatric Considerations
The palate is particularly important in pediatric dental health due to its role in development and growth.
- Cleft Palate: This is a primary concern for parents. If detected prenatally or at birth, a team of specialists (pediatrician, oral surgeon, plastic surgeon, orthodontist, speech therapist) will be involved. Early intervention with feeding specialized bottles and subsequent surgeries (often starting around 6-12 months of age) are crucial for speech, feeding, and dental development. Orthodontics often plays a vital role in managing the alignment of the dental arches, which are often affected in children with cleft palate, typically involving braces or other appliances.
- Palatal Expanders: These orthodontic appliances are very common in children with a narrow upper jaw (maxilla). An expander slowly widens the hard palate, creating more space for crowded teeth, correcting crossbites, and sometimes improving nasal breathing. This is a key part of interceptive orthodontics.
- ``
- Thumb Sucking and Pacifier Use: Prolonged or intense thumb sucking or pacifier use beyond age 4-5 can significantly alter the development of the palate, leading to a high-arched palate and potential bite problems like anterior open bite or posterior crossbite. Early cessation is encouraged, sometimes with the help of habit-breaking appliances.
- Oral Hygiene: Teaching children good oral hygiene habits from a young age is essential to prevent infections and maintain overall palatal health.
Frequently Asked Questions
How much does palatal tori removal cost in the US?
Without insurance, palatal tori removal typically costs between $1,000 and $3,000. The price can vary based on the size and number of tori, the complexity of the surgery, and your geographic location. Dental insurance may cover a portion if the removal is deemed medically necessary, for example, if the tori interfere with denture placement or cause chronic trauma.

Is palate surgery painful?
During the procedure, you will receive local anesthesia, so you should not feel any pain. After the anesthesia wears off, you can expect some discomfort, swelling, and soreness. This is usually managed effectively with over-the-counter pain relievers or prescribed medication. Recovery pain typically subsides within a few days to a week.
How long does it take to recover from palate surgery?
Recovery time varies depending on the type and complexity of the surgery. For minor procedures like palatal tori removal, initial discomfort and swelling usually resolve within 1-2 weeks, with complete soft tissue healing taking 4-6 weeks. More extensive surgeries, like cleft palate repair or oral cancer removal, involve longer and more intensive recovery periods, potentially spanning several months with follow-up treatments.
Can palate problems affect speech?
Absolutely. The soft palate plays a crucial role in speech by controlling the airflow into the nasal cavity. Issues like a short or immobile soft palate (often seen in cleft palate patients) can lead to hypernasal speech (sounding like air is escaping through the nose). Obstructions or pain on the hard palate can also interfere with tongue movement, affecting articulation. Orthodontic issues related to palate shape can also impact speech.
Does insurance cover palate treatments?
Coverage depends on the specific condition and your insurance plan. Dental insurance typically covers a portion of procedures like palatal tori removal or orthodontic appliances (like palatal expanders), often up to an annual maximum. Medical insurance generally covers procedures considered medically necessary, such as cleft palate repair, oral cancer treatment, or complex infections. It's vital to verify coverage with both your dental and medical insurance providers.
What causes a bump on the roof of my mouth?
The most common cause of a hard, bony bump on the roof of your mouth is a palatal torus (torus palatinus), which is a benign bony growth. Other possibilities include cysts, abscesses, salivary gland issues, or, less commonly, cancerous lesions. Any new or changing bump should be evaluated by a dentist for proper diagnosis.
Are there non-surgical alternatives for palate issues?
For conditions like palatal tori, surgical removal is the only definitive treatment; however, if they are not causing symptoms, they can often be left alone. For infections, antibiotics or antifungals are non-surgical treatments. For narrow palates, orthodontics uses palatal expanders, which are appliances rather than surgery. For specific speech issues, speech therapy can be a non-surgical approach. However, for congenital defects like cleft palate or malignant growths, surgery is usually essential.
When to See a Dentist
Your palate is a window into your overall oral health. While routine check-ups (every 6 months) are essential for preventative care, certain signs warrant immediate attention:
- Persistent Pain or Tenderness: Especially if it doesn't resolve within a week.
- New or Changing Lumps/Bumps: Any new growth, or an existing one that changes size, shape, or color, should be promptly evaluated.
- White, Red, or Dark Patches: Persistent discolored areas, particularly if rough or ulcerated, need urgent assessment for oral cancer screening.
- Difficulty Swallowing, Chewing, or Speaking: If these functions become impaired or painful, it could indicate a serious underlying problem.
- Unexplained Bleeding: Any bleeding from the palate that isn't due to obvious trauma.
- Sores that Don't Heal: Any ulcer or lesion on your palate that persists for more than 2-3 weeks.
- Rapid Swelling: Sudden or unexplained swelling of the palate could indicate an infection or other acute issue.
Don't wait if you notice any concerning changes in your palate. Early diagnosis and treatment are critical for achieving the best possible outcomes and maintaining your oral health.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.