Gum Disease
4,628 words · 15 min read
Quick Definition
An infection of the tissues that hold teeth in place, ranging from mild gingivitis to severe periodontitis that can destroy bone and lead to tooth loss.
Gum Disease: A Comprehensive Guide to Periodontal Health
Introduction
Gum disease, also known as periodontal disease, is a common but serious infection of the tissues that support your teeth. It begins with inflammation of the gums (gingivitis) and, if left untreated, can progress to a more severe form called periodontitis, which can destroy the bone supporting your teeth and ultimately lead to tooth loss. Far from being just a cosmetic concern, gum disease is a chronic inflammatory condition with significant implications for both your oral health and overall well-being.
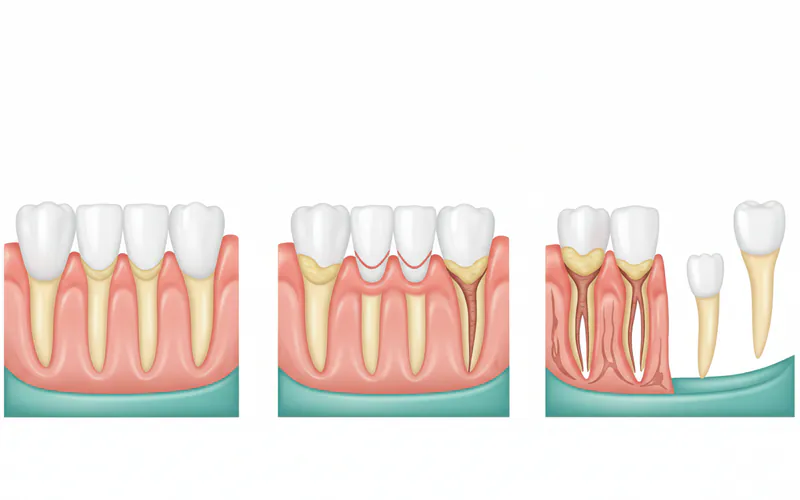
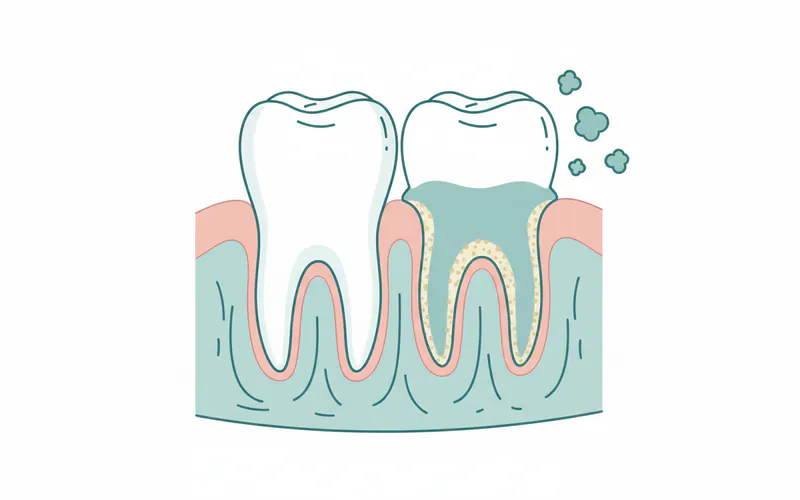
The Centers for Disease Control and Prevention (CDC) estimates that nearly half of adults aged 30 years or older (47.2%) in the United States show signs of gum disease, with the prevalence increasing to 64.7% for adults 65 years and older. This widespread issue highlights the critical importance of understanding gum disease, recognizing its signs, and taking proactive steps for prevention and treatment. This definitive guide will equip you with everything you need to know to protect your gums and maintain a healthy smile.
Key Takeaways:
- Gum disease is an infection and inflammation of the tissues supporting your teeth.
- It progresses from mild gingivitis to severe periodontitis, potentially causing bone loss and tooth loss.
- Nearly half of US adults over 30 have some form of gum disease.
- The primary cause is plaque buildup due to inadequate oral hygiene.
- Early detection and treatment are crucial to prevent irreversible damage.
- Good daily oral hygiene and regular dental check-ups are the best prevention.
Detailed Explanation
Types and Classifications of Gum Disease
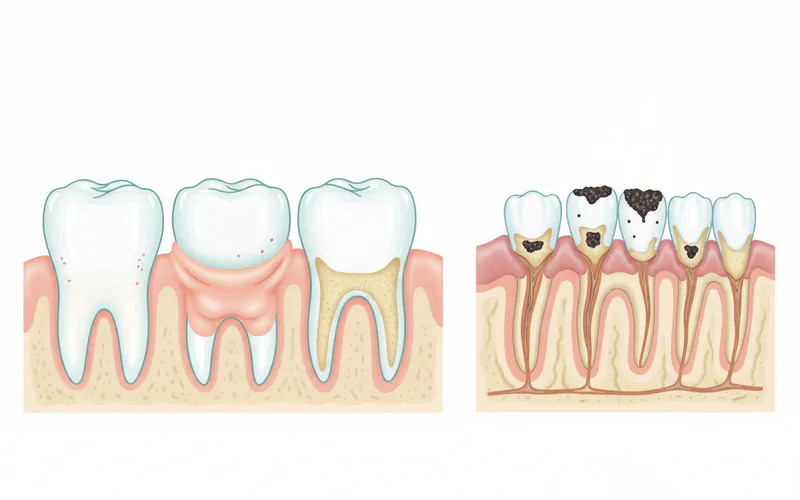
Gum disease is not a single condition but rather a spectrum of diseases, primarily categorized by severity and progression.
-
- What it is: The mildest form of gum disease, characterized by inflammation of the gums (gingiva) caused by plaque accumulation at the gumline.
- Characteristics: Gums become red, swollen, and bleed easily during brushing or flossing. There is typically no loss of bone or tissue supporting the teeth at this stage.
- Reversibility: Gingivitis is reversible with professional cleaning and diligent home oral care.
- Related Terms: Plaque (a sticky film of bacteria constantly forming on teeth).
-
- What it is: If gingivitis is left untreated, it can advance to periodontitis, a more destructive form of gum disease where the inflammation spreads from the gums to the deeper tissues and bone that support the teeth.
- Characteristics: The immune system's response to the chronic bacterial infection, combined with bacterial toxins, begins to break down the bone and connective tissue that hold teeth in place. This leads to the formation of "periodontal pockets" – spaces between the teeth and gums that become infected.
- Damage: This damage is often irreversible, though its progression can be halted or slowed with treatment.
- Types of Periodontitis:
- Chronic Periodontitis: The most common form, characterized by slow to moderate progression, typically affecting adults. It involves pocket formation and gradual attachment loss.
- Aggressive Periodontitis: A less common but rapidly progressing form, often seen in younger individuals (though it can affect anyone). It leads to severe destruction of periodontal tissue and bone in a short period.
- Necrotizing Periodontal Diseases: Characterized by the death of gum tissue, ligaments, and bone, often associated with systemic conditions like immunosuppression (e.g., HIV/AIDS) or severe malnutrition.
- Periodontitis as a Manifestation of Systemic Diseases: Gum disease can sometimes be a symptom or exacerbated by other medical conditions such as diabetes, heart disease, respiratory disease, or certain genetic disorders.
- Related Terms: Calculus (hardened plaque, also known as tartar), Periodontal Disease (an umbrella term for both gingivitis and periodontitis).
Causes and Risk Factors
The primary cause of gum disease is the accumulation of plaque, a sticky, colorless film of bacteria that constantly forms on your teeth. If plaque is not removed daily by brushing and flossing, it hardens into calculus (tartar), which can only be removed by a dental professional. The bacteria in plaque and calculus produce toxins that irritate the gums, leading to inflammation and infection.
Beyond plaque and calculus, several factors can increase your risk:
- Poor Oral Hygiene: Inadequate or infrequent brushing and flossing allow plaque to build up.
- Smoking/Vaping: This is one of the most significant risk factors. Smoking impairs the immune system, making it harder for gums to fight infection, and it restricts blood flow, masking the typical signs of gum disease like bleeding.
- Genetics: Some people are genetically predisposed to developing gum disease, even with good oral hygiene.
- Diabetes: People with diabetes are more susceptible to infections, including gum disease, and healing can be slower. Uncontrolled blood sugar levels worsen the condition.
- Hormonal Changes: Puberty, pregnancy, and menopause can make gums more sensitive and susceptible to gingivitis due to hormonal fluctuations.
- Certain Medications: Some drugs, such as antidepressants, antihistamines, and certain heart medications, can reduce saliva flow, leading to a dry mouth. Saliva helps neutralize acids and wash away food particles, so less saliva can increase plaque buildup.
- Stress: Stress can weaken the immune system, making it harder to fight off infections.
- Poor Nutrition: A diet lacking essential nutrients, especially Vitamin C, can compromise the immune system and gum health.
- Compromised Immune System: Conditions like HIV/AIDS or treatments like chemotherapy can weaken the body's ability to fight infection.
- Crooked or Crowded Teeth: Teeth that are difficult to clean properly can accumulate more plaque and calculus.
- Ill-fitting Dental Restorations: Crowns, bridges, or fillings that don't fit well can trap plaque and irritate gums.
- Bruxism (Teeth Grinding/Clenching): While not a direct cause, excessive force on teeth can accelerate the breakdown of periodontal tissues already compromised by disease.
Signs and Symptoms to Watch For
Recognizing the early signs of gum disease is crucial for effective treatment. Symptoms can vary depending on the stage of the disease.
Early Signs (Gingivitis):
- Red or swollen gums: Healthy gums are firm and pink.
- Bleeding gums: Gums that bleed easily during brushing, flossing, or even when eating. This is often the first and most obvious sign.
- Tender gums: Gums that are painful to the touch.
- Receding gums: Gums that pull away from the teeth, making teeth appear longer (though this can also be a sign of early periodontitis).
Advanced Signs (Periodontitis):
- Persistent bad breath (halitosis) or a bad taste in your mouth: Caused by the bacteria and infection.
- Pus between your teeth and gums: A clear sign of active infection.
- Deep pockets between teeth and gums: Spaces created as the gums pull away from the teeth and bone is lost.
- Loose or shifting teeth: As the bone and supporting structures are destroyed, teeth can become unstable.
- Changes in the way your teeth fit together when you bite: This can happen as teeth shift.
- Changes in the fit of partial dentures.
- Pain when chewing.
- Visible loss of gum tissue or exposed tooth roots.
If you notice any of these symptoms, especially bleeding gums, it's essential to schedule an appointment with your dentist promptly.
Diagnosis Process — What Your Dentist Does
Diagnosing gum disease is a straightforward process performed by your dentist or periodontist (a specialist in gum disease).
- Medical and Dental History Review: Your dentist will ask about your medical conditions, medications, and lifestyle habits (e.g., smoking), as these can impact your gum health.
- Visual Examination: The dentist will carefully examine your gums for signs of inflammation, redness, swelling, and bleeding.
- Periodontal Probing (Periodontal Charting): This is a key diagnostic tool. A small, gentle ruler-like probe is inserted into the "sulcus" (the space between your tooth and gum). Healthy gum pockets typically measure 1-3 millimeters (mm). Depths of 4mm or more indicate gum disease and periodontal pockets, meaning the gum has detached from the tooth due to bone loss. Your dentist will measure six sites around each tooth and record these measurements.
- X-rays (Radiographs): Dental X-rays are taken to assess the condition of the bone supporting your teeth and to identify any bone loss that might not be visible during a clinical exam. They can also show calculus buildup below the gumline.
- Assessment of Tooth Mobility: Your dentist will check if any teeth are loose or shifting.
- Bleeding on Probing: The dentist will note if your gums bleed when probed, which is an indicator of inflammation.
Based on these findings, your dentist will classify the severity of your gum disease (gingivitis, mild, moderate, or severe periodontitis) and develop a personalized treatment plan.
Treatment Options with Pros, Cons, and Costs
Treatment for gum disease aims to stop its progression, reduce inflammation, eliminate infection, and, in some cases, regenerate lost tissue. Treatment options vary depending on the severity of the disease.
Non-Surgical Treatments
These are typically used for gingivitis and mild to moderate periodontitis.
-
Professional Dental Cleaning (Prophylaxis):
- What it is: A routine cleaning to remove plaque and calculus from above the gumline and slightly below it.
- Pros: Prevents gingivitis from progressing, removes irritants, relatively inexpensive, quick.
- Cons: Not sufficient for established periodontitis with deep pockets.
- Cost Range (US): $75 - $200 (often covered by insurance for twice-yearly visits).
-
Scaling and Root Planing (SRP) – "Deep Cleaning":
- What it is: A non-surgical procedure for periodontitis. Scaling involves meticulously removing plaque and calculus from both above and below the gumline, all the way down to the bottom of the periodontal pocket. Root planing smooths the root surfaces to remove bacterial toxins and prevent future plaque buildup, allowing gums to reattach to clean root surfaces. It often requires local anesthetic and multiple appointments.
- Pros: Highly effective for mild to moderate periodontitis, can reverse early bone loss, less invasive than surgery, relatively good patient comfort with anesthetic.
- Cons: May require several appointments, can cause temporary tooth sensitivity and gum soreness, not always sufficient for very deep pockets or advanced bone loss.
- Cost Range (US): $200 - $500 per quadrant (a quadrant is one-quarter of your mouth). A full mouth SRP could cost $800 - $2,000. Insurance often covers a significant portion.
-
Antibiotics (Topical or Oral):
- What it is: Can be used in conjunction with SRP to control bacterial infection.
- Topical: Applied directly to periodontal pockets (e.g., antibiotic gels, chips, or mouth rinses).
- Oral: Systemic antibiotics taken in pill form for widespread or aggressive infections.
- Pros: Helps eliminate stubborn bacteria, reduces infection, can enhance healing.
- Cons: Topical treatments are limited to specific sites, oral antibiotics can have side effects (e.g., digestive upset, yeast infections) and contribute to antibiotic resistance.
- Cost Range (US): $20 - $200 (depending on type and duration).
- What it is: Can be used in conjunction with SRP to control bacterial infection.
Surgical Treatments
These are typically recommended for moderate to severe periodontitis when non-surgical treatments are insufficient.
-
Flap Surgery (Pocket Reduction Surgery):
- What it is: The periodontist makes small incisions in the gum tissue to lift back a section of the gums (a "flap"). This allows for thorough cleaning of the root surfaces and removal of diseased tissue and calculus from deep pockets. Irregular bone surfaces damaged by the disease can be smoothed to reduce areas where bacteria can accumulate. The gums are then sutured back into place, fitting more snugly around the teeth.
- Pros: Very effective at reducing pocket depth, allows for thorough cleaning of infected areas, can halt disease progression, prevents further bone loss.
- Cons: More invasive, requires a longer recovery time, can cause temporary discomfort, swelling, and tooth sensitivity. Gums may appear more "receded" afterward, exposing more tooth root.
- Cost Range (US): $500 - $3,000+ per quadrant, depending on complexity.
-
Bone Grafting:
- What it is: Used when gum disease has destroyed bone around the tooth root. Fragments of your own bone, synthetic bone, or donated bone are placed in the area of bone loss to encourage the regeneration of new bone and tissue.
- Pros: Can help regenerate lost bone, stabilize loose teeth, and prepare the area for future dental implants.
- Cons: Invasive, requires significant healing time, success varies, more expensive.
- Cost Range (US): $400 - $1,200 per site, excluding associated surgery.
-
Soft Tissue Grafts (Gum Grafts):
- What it is: Used to reinforce thin gums or fill in areas where gums have receded, exposing tooth roots. Tissue is typically taken from the roof of your mouth or used from a donor source and then attached to the affected area.
- Pros: Covers exposed roots, reduces tooth sensitivity, protects roots from decay, improves gum aesthetics.
- Cons: Can be uncomfortable at the donor site (if using your own tissue), requires careful aftercare, more expensive.
- Cost Range (US): $300 - $1,000 per site, excluding associated surgery.
-
Guided Tissue Regeneration (GTR):
- What it is: A surgical procedure that uses a small piece of mesh-like fabric (a membrane) inserted between the bone and gum tissue. This membrane prevents the gum tissue from growing into the area where bone should be, allowing slower-growing bone cells to regenerate.
- Pros: Encourages the regeneration of lost bone and periodontal ligament, which are essential for supporting teeth.
- Cons: Invasive, requires specialized skill, longer healing period, can be expensive.
- Cost Range (US): $500 - $2,000 per site, excluding associated surgery.
Comparison of Common Treatment Options
| Feature | Professional Cleaning (Prophylaxis) | Scaling & Root Planing (SRP) | Flap Surgery |
|---|---|---|---|
| Purpose | Preventative, mild gingivitis | Treat mild-moderate periodontitis | Treat moderate-severe periodontitis |
| Severity | Mild | Mild to Moderate | Moderate to Severe |
| Invasiveness | Minimal | Moderate (non-surgical) | High (surgical) |
| Anesthesia | Often none | Local anesthetic | Local anesthetic, sometimes sedation |
| Duration | 30-60 minutes | 1-2 hours per quadrant (multiple appointments) | 1-3 hours per area |
| Recovery | Immediate | Mild soreness for 1-2 days | 1-2 weeks significant soreness, swelling |
| Primary Benefit | Prevents disease | Halts disease progression, reduces pockets | Eliminates deep infection, allows bone contouring |
| Potential Risks | Minor sensitivity | Temporary sensitivity, soreness | Sensitivity, recession, discomfort, swelling, infection |
| Cost (US) | $75 - $200 | $800 - $2,000 (full mouth) | $2,000 - $12,000+ (full mouth) |
| Insurance | Often fully covered | Usually partially covered (up to 80%) | Usually partially covered (up to 50%) |
Step-by-Step: What to Expect During Treatment
Let's detail what a typical Scaling and Root Planing (SRP) procedure would entail, as it's the most common initial treatment for periodontitis.
-
Preparation:
- Numbing: The dental hygienist or dentist will administer local anesthetic to numb the area being treated. This ensures you are comfortable throughout the procedure.
- Quadrant-by-Quadrant: SRP is often performed on one or two quadrants (sections) of the mouth per visit to allow for thoroughness and reduce patient fatigue.
-
Scaling:
- Tools: Specialized instruments, including ultrasonic scalers (which use vibrations to break up calculus and rinse away debris) and hand scalers, are used.
- Process: The hygienist or dentist will meticulously remove plaque and calculus from the tooth surfaces, both above and, crucially, below the gumline, extending into the periodontal pockets. You might hear scraping sounds or feel some pressure, even with numbing.
-
Root Planing:
- Process: After scaling, the root surfaces of the teeth are carefully smoothed. This step is vital because rough root surfaces can harbor bacteria and make it easier for plaque to reattach. Smoothing the roots removes any remaining bacterial toxins and helps the gums reattach more firmly to the clean, smooth tooth surface.
-
Rinsing:
- Throughout the procedure, your mouth will be rinsed to remove debris and bacteria. An antimicrobial rinse might be used.
-
Completion and Post-Op Instructions:
- Once a quadrant is complete, you'll receive detailed instructions on aftercare, including pain management, diet, and how to maintain oral hygiene in the treated area.
- You'll schedule your next appointment for additional quadrants or a follow-up visit.
For surgical procedures, the process is similar in terms of preparation (anesthetic) but will involve incisions, lifting of gum tissue, direct cleaning, and then suturing the gums back in place. The recovery will be more involved.
Recovery Timeline and Aftercare
Recovery varies significantly depending on the treatment type.
For Scaling and Root Planing:
- Immediate Aftermath (0-24 hours): Gums may feel sore, tender, and slightly swollen. Some minor bleeding might occur. Teeth may be temporarily sensitive to hot or cold.
- First Few Days: Mild discomfort can be managed with over-the-counter pain relievers (e.g., ibuprofen). Avoid very hot, cold, spicy, or crunchy foods. Continue gentle oral hygiene as instructed by your dentist.
- 1-2 Weeks: Sensitivity usually subsides. Gums should appear less red and swollen and stop bleeding. You might notice a slight gum recession as the inflammation resolves and gums tighten.
- Aftercare:
- Maintain Excellent Oral Hygiene: This is paramount. Brush twice daily with a soft-bristled toothbrush, floss daily, and use an antimicrobial mouthwash if recommended.
- Avoid Smoking: Smoking significantly hinders healing and increases the risk of recurrence.
- Follow-up Appointments: Regular recall appointments (often every 3-4 months, called "periodontal maintenance") are crucial to monitor gum health, remove new plaque/calculus, and prevent disease relapse.
For Surgical Treatments (Flap Surgery, Grafts):
- Immediate Aftermath (0-48 hours): Expect more significant discomfort, swelling, and possibly bruising. Bleeding is more common. Pain medication (prescription or OTC) will likely be needed. A soft diet is usually recommended.
- First Week: Stitches typically remain for 7-10 days and may need to be removed by your dentist. Avoid vigorous brushing or flossing near the surgical site. Use prescribed rinses. Avoid strenuous activity.
- 2-4 Weeks: Swelling and bruising should subside. Gums will continue to heal and remodel. Tooth sensitivity can be more pronounced and may last for several weeks or months.
- Aftercare:
- Strict Adherence to Post-Op Instructions: This is non-negotiable for successful healing.
- Soft Diet: For several weeks to protect the surgical site.
- Avoid Smoking: Absolutely critical for proper healing and preventing complications.
- Excellent Oral Hygiene: Gentle but thorough cleaning of non-surgical areas, and very careful cleaning around surgical sites as instructed.
- Regular Follow-up: Multiple post-operative visits are required to monitor healing, remove sutures, and assess long-term outcomes.
- Long-Term Periodontal Maintenance: Essential to prevent recurrence and maintain results.
Prevention Strategies
Prevention is always better than cure, especially with gum disease. The vast majority of gingivitis cases are preventable.
- Brush Your Teeth Twice a Day: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes each time, covering all surfaces of your teeth and gently along the gumline.
- Floss Daily: Flossing removes plaque and food particles from between your teeth and under the gumline where a toothbrush can't reach. This is arguably the most crucial step for preventing gum disease.
- Use Mouthwash: An antiseptic mouthwash can help reduce bacteria and control plaque, but it should not replace brushing and flossing.
- Regular Dental Check-ups and Professional Cleanings: Visit your dentist at least once every six months (or more often if you have risk factors or a history of gum disease). Professional cleanings remove calculus (hardened plaque) that you cannot remove at home.
- Don't Smoke or Vape: Quitting smoking is one of the most impactful things you can do for your gum health.
- Manage Systemic Health Conditions: If you have diabetes, heart disease, or other conditions, work with your doctor to manage them effectively.
- Eat a Balanced Diet: A diet rich in vitamins and minerals (especially Vitamin C) supports a healthy immune system and overall gum health. Limit sugary foods and drinks that promote bacterial growth.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and bacteria.
Cost Ranges in the US (with/without insurance)
The cost of gum disease treatment varies widely based on the severity of the disease, the type of treatment, the dental professional's fees, and your geographic location. Insurance coverage also plays a significant role.
- Routine Professional Cleaning (Prophylaxis):
- Without insurance: $75 - $200
- With insurance: Often 100% covered for two visits per year.
- Scaling and Root Planing (SRP):
- Without insurance: $200 - $500 per quadrant. A full mouth (4 quadrants) could be $800 - $2,000.
- With insurance: Typically covered 50% - 80% after deductible.
- Antibiotics (Topical/Oral):
- Without insurance: $20 - $200
- With insurance: Usually covered like other prescriptions.
- Periodontal Maintenance Cleanings (after SRP):
- Without insurance: $100 - $300 per visit (often required 3-4 times a year).
- With insurance: May be covered 50% - 80%, sometimes grouped with routine cleanings.
- Flap Surgery (Pocket Reduction):
- Without insurance: $500 - $3,000+ per quadrant. Full mouth could be $2,000 - $12,000+.
- With insurance: Usually covered 20% - 50%, with annual maximums.
- Bone Grafts:
- Without insurance: $400 - $1,200 per site (excluding surgical fees).
- With insurance: Highly variable, often 20% - 50% coverage.
- Soft Tissue Grafts (Gum Grafts):
- Without insurance: $300 - $1,000 per site (excluding surgical fees).
- With insurance: Highly variable, often 20% - 50% coverage.
- Guided Tissue Regeneration:
- Without insurance: $500 - $2,000 per site (excluding surgical fees).
- With insurance: Variable, often 20% - 50% coverage.
It's crucial to discuss costs and insurance coverage with your dental office before starting any treatment. Many offices offer payment plans or financing options.
For Parents / Pediatric Considerations
While gum disease is predominantly an adult condition, it can affect children and adolescents, though less commonly.
- Gingivitis in Children: Mild gingivitis is quite common in children, often due to inconsistent brushing and flossing. Swollen, red, and bleeding gums are the typical signs. This is usually reversible with improved oral hygiene.
- "Puberty Gingivitis": Hormonal changes during puberty can exacerbate gingivitis in teenagers, making their gums more sensitive to plaque.
- Aggressive Periodontitis: In rare cases, children and adolescents can develop aggressive forms of periodontitis, which can lead to significant bone loss and tooth mobility. This often has a strong genetic component or is associated with certain systemic conditions.
- Importance of Early Habits: Teaching children proper brushing and flossing techniques from an early age is vital for preventing gum disease throughout life. Regular dental check-ups are also crucial to monitor gum health and catch any issues early.
- Image Placeholder: ``
Frequently Asked Questions
Q1: Is gum disease painful?
A: In its early stages (gingivitis), gum disease is often painless, which is why many people don't realize they have it. As it progresses to periodontitis, you might experience pain when chewing, extreme sensitivity to hot or cold, or a dull ache in your gums. Bleeding gums, however, are a common sign of inflammation and should not be ignored.
Q2: How long does gum disease treatment take?
A: The duration of treatment varies greatly. Gingivitis can often be resolved with one or two professional cleanings and improved home care within a few weeks. Scaling and Root Planing typically involves 2-4 appointments over several weeks. Surgical treatments require separate appointments for the procedure and subsequent follow-up visits, with healing taking weeks to months. Regardless of the initial treatment, ongoing periodontal maintenance cleanings (often every 3-4 months) are essential for long-term management.
Q3: Will my dental insurance cover gum disease treatment?
A: Most dental insurance plans cover a portion of gum disease treatment, but the extent of coverage varies. Routine cleanings are often 100% covered. Scaling and Root Planing is usually covered 50-80% after a deductible. Surgical procedures tend to have lower coverage, sometimes only 20-50%, and are often subject to annual maximums. It's crucial to check with your insurance provider and dental office for a pre-treatment estimate.
Q4: Are there alternatives to traditional gum disease treatments?
A: For established periodontitis, traditional treatments like Scaling and Root Planing or surgery are the gold standard because they physically remove bacteria and infected tissue. Some dentists might use laser therapy as an adjunct or alternative to traditional scaling, or use antimicrobial agents. However, these are often used in conjunction with conventional methods, not as standalone replacements for severe cases. The most effective "alternative" is consistent, excellent daily oral hygiene to prevent the disease from starting or progressing.
Q5: Can gum disease lead to other health problems?
A: Yes, there's growing evidence linking severe gum disease to various systemic health issues. The chronic inflammation and bacteria in the mouth can enter the bloodstream and contribute to conditions such as:
- Heart disease and stroke: Bacteria from gum disease may contribute to arterial plaque formation.
- Diabetes: Gum disease can make blood sugar control more difficult, and diabetes can worsen gum disease. It's a two-way street.
- Respiratory diseases: Inhaling bacteria from infected gums can lead to respiratory problems like pneumonia.
- Adverse pregnancy outcomes: Gum disease has been linked to preterm birth and low birth weight.
- Rheumatoid arthritis: Some studies suggest a link between the two inflammatory conditions.
Q6: Can gum disease be cured permanently?
A: Gingivitis is reversible and can be fully "cured." However, once periodontitis develops, the damage to the bone and supporting tissues is often irreversible. While treatment can effectively halt the progression of the disease, eliminate infection, and reduce pocket depths, the lost bone typically doesn't fully regenerate without specific regenerative procedures (like bone grafts). Therefore, periodontitis is often managed as a chronic condition, requiring ongoing maintenance and vigilant home care to prevent recurrence.
Q7: What if I don't treat my gum disease?
A: Untreated gum disease will almost certainly progress. As the infection and inflammation worsen, more bone and tissue supporting your teeth will be destroyed. This will lead to:
- Increasingly loose teeth.
- Pain and difficulty chewing.
- Persistent bad breath.
- Gum recession and root exposure.
- Ultimately, tooth loss. Furthermore, the systemic health risks mentioned above will also increase.
Q8: What's the difference between plaque and calculus?
A: Plaque is a soft, sticky, colorless biofilm of bacteria that constantly forms on your teeth. It can be removed daily with proper brushing and flossing. If plaque is not removed, it absorbs minerals from saliva and hardens into calculus (also known as tartar). Calculus is a rough, porous deposit that firmly attaches to tooth surfaces, often appearing yellow or brown. Unlike plaque, calculus cannot be removed by brushing or flossing and requires professional dental cleaning.
- Image Placeholder: ``
When to See a Dentist
It's crucial to be proactive about your gum health.
Routine Care:
- Schedule annual dental check-ups and bi-annual professional cleanings. These visits are vital for early detection and prevention, even if you don't notice any symptoms.
When to See a Dentist Promptly (Non-Emergency but Urgent):
- Bleeding gums: If your gums bleed regularly when you brush or floss, or spontaneously.
- Red, swollen, or tender gums.
- Persistent bad breath or a bad taste in your mouth.
- Receding gums (teeth appearing longer).
- Any noticeable loose teeth or changes in your bite.
Emergency Signs (See a Dentist Immediately):
- Severe, throbbing pain in your gums or teeth.
- Pus oozing from around your teeth.
- Rapidly worsening swelling in your gums or face.
- A tooth suddenly becomes very loose or falls out.
Ignoring gum disease can lead to irreversible damage and serious health complications. Early detection and consistent treatment are the keys to preserving your smile and your overall health.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.