Leukoplakia Tongue: Complete Guide
Key Takeaways
- Imagine finding an unexplained white patch on your tongue that won't go away. While it might seem minor, such a finding could be a sign of leukoplakia tongue, a condition affecting approximately 1-3% of the adult population in the United States. Though often harmless initially, leukoplakia i
Leukoplakia Tongue: Complete Guide
Imagine finding an unexplained white patch on your tongue that won't go away. While it might seem minor, such a finding could be a sign of leukoplakia tongue, a condition affecting approximately 1-3% of the adult population in the United States. Though often harmless initially, leukoplakia is considered a potentially malignant disorder, meaning it has the capacity to transform into oral cancer. Early detection and proper management are paramount, as the survival rate for oral cancer significantly improves when caught in its earliest stages. Missing the signs or delaying evaluation can have severe consequences for your long-term health.

This comprehensive guide from SmilePedia.net aims to empower you with in-depth knowledge about leukoplakia of the tongue. We will explore what this condition is, its various forms, the underlying causes, crucial signs to look for, and the range of diagnostic and treatment options available. Understanding the costs, recovery processes, and vital prevention strategies will equip you to take proactive steps toward safeguarding your oral health.
Key Takeaways:
- Definition: Leukoplakia tongue is a persistent, non-scrapable white patch on the tongue that is considered a potentially malignant disorder, with a 5-17% chance of transforming into oral cancer.
- Primary Cause: Tobacco use (smoking and smokeless) and excessive alcohol consumption are the leading risk factors, significantly increasing the likelihood of developing leukoplakia.
- Diagnosis is Key: A definitive diagnosis requires a biopsy, which involves taking a small tissue sample for microscopic examination. This is crucial to rule out other conditions and assess malignant potential.
- Treatment Varies: Options range from watchful waiting for low-risk lesions to surgical excision (scalpel, laser, cryotherapy) for higher-risk or dysplastic lesions. Early removal improves outcomes.
- Cost & Insurance: Initial consultation and biopsy may range from $150-$700. Surgical removal can cost $500-$3,000+, depending on the method and lesion size. Most dental PPO and some medical insurance plans (for medically necessary procedures like biopsies) cover a portion of these costs.
- Prevention & Follow-up: Quitting tobacco and alcohol is the most effective prevention. Regular dental check-ups every 3-6 months are critical after diagnosis, even after treatment, to monitor for recurrence.
- Prognosis: While leukoplakia itself is not cancer, its malignant transformation risk necessitates vigilance. Early detection and treatment of high-risk lesions significantly reduce the chance of developing full-blown oral cancer.
What It Is / Overview
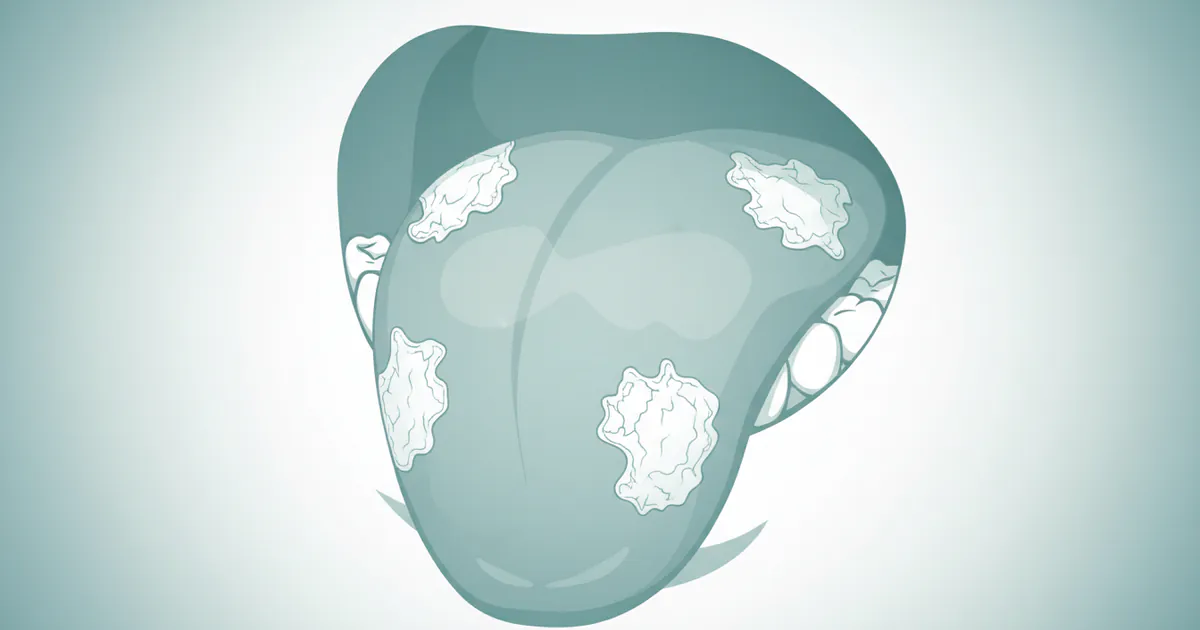
Leukoplakia is formally defined by the World Health Organization (WHO) as "a white plaque of questionable risk, after the exclusion of other known diseases or disorders that carry no increased risk for cancer." When this white patch manifests on the tongue, it's specifically referred to as leukoplakia tongue. This condition is characterized by a thickened, white, or grayish-white lesion that cannot be rubbed or scraped off and cannot be classified clinically or pathologically as any other identifiable disease.
The tongue is a common site for leukoplakia, alongside the buccal mucosa (inner cheek), floor of the mouth, and gingiva (gums). Its significance lies in its precancerous potential. While many leukoplakic lesions remain benign, a notable percentage—ranging from 5% to as high as 17% in some studies—can undergo malignant transformation into squamous cell carcinoma, the most common type of oral cancer. This makes it a crucial subject for vigilance and early intervention within the field of oral cancer & pathology.
Prevalence: Leukoplakia affects approximately 1-3% of the general adult population, with a higher incidence in older males and individuals with significant risk factors like tobacco and alcohol use. The risk increases with age, typically affecting individuals over 40.
Why It Matters: The insidious nature of leukoplakia tongue is that it is often asymptomatic, meaning it causes no pain or discomfort. This lack of symptoms can lead to delayed detection, allowing the lesion more time to potentially develop into cancer. Understanding what leukoplakia is and recognizing its appearance is the first crucial step in preventing a more serious outcome. It serves as a stark reminder that persistent, unexplained changes in your mouth warrant immediate professional evaluation.
Types / Variations
Leukoplakia is not a monolithic condition; it presents in several forms, each carrying a different level of risk for malignant transformation. Understanding these variations is critical for accurate diagnosis and prognosis.
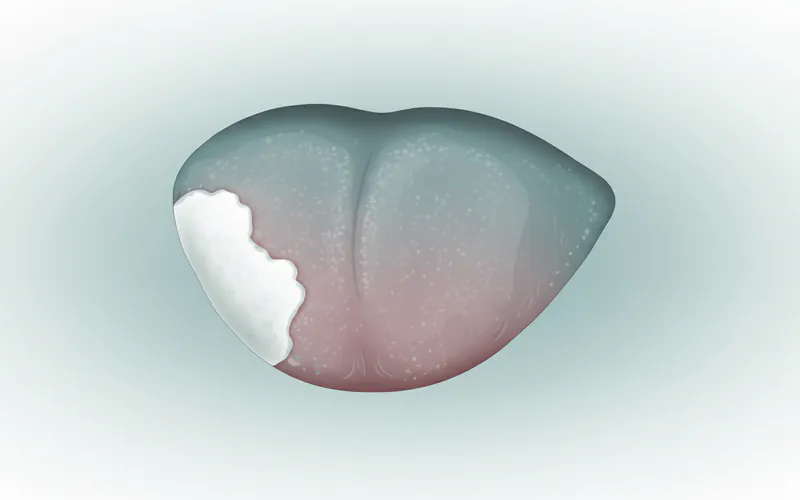
1. Homogeneous Leukoplakia (or Uniform Leukoplakia)
This is the most common and generally considered the least risky form.
- Appearance: Typically a thin, uniform, flat white patch with a smooth or finely wrinkled surface. Its color is consistently white or grayish-white throughout.
- Feel: Soft and pliable to the touch.
- Location: Can occur anywhere in the mouth, including the tongue.
- Malignant Potential: Lower risk compared to non-homogeneous types, usually below 5%.
2. Non-Homogeneous Leukoplakia
This category encompasses lesions that are not uniform in appearance and are associated with a significantly higher risk of malignant transformation. They are often described as having an irregular surface or mixed red and white areas.
- Erythroleukoplakia (or Speckled Leukoplakia):
- Appearance: This is a mixed red and white lesion, often appearing as red areas interspersed with white patches. The redness indicates inflammation and thinning of the epithelium, which can be more prone to dysplasia (abnormal cell growth).
- Malignant Potential: Considered one of the highest-risk forms of leukoplakia, with a malignant transformation rate often cited between 20% and 50%. This is why some refer to it as "erythroplakia with white patches" since pure erythroplakia (red lesions) have an even higher malignant potential.
- Nodular Leukoplakia:
- Appearance: Characterized by small, rounded, elevated white nodules or lumps on a background of leukoplakia.
- Malignant Potential: High risk, often similar to or higher than erythroleukoplakia.
- Verrucous Leukoplakia:
- Appearance: Has a warty, corrugated, or exophytic (outward-growing) surface. It can be quite thick and rough.
- Malignant Potential: High risk, as these lesions often harbor significant dysplasia or even early carcinoma.
3. Proliferative Verrucous Leukoplakia (PVL)
PVL is a distinct and aggressive subtype of non-homogeneous leukoplakia.
- Appearance: It's characterized by multiple, often widespread, persistent, and slowly progressing verrucous (wart-like) white lesions. It tends to spread to different areas of the oral mucosa over time.
- Recurrence: Has a strong tendency to recur even after surgical removal.
- Malignant Potential: Extremely high malignant transformation rate, often reaching 70-100% over time, frequently transforming into verrucous carcinoma or conventional squamous cell carcinoma. It is generally resistant to various treatments and has a poor prognosis.
Pro Tip: While these descriptions help differentiate types, only a skilled oral pathologist can definitively categorize a lesion after a biopsy. Never attempt self-diagnosis.
| Type of Leukoplakia | Appearance Description | Malignant Transformation Risk (Approximate) | Key Characteristic |
|---|---|---|---|
| Homogeneous Leukoplakia | Uniformly white, flat, smooth or finely wrinkled patch | 3-5% | Most common, lowest risk, soft and pliable |
| Erythroleukoplakia | Mixed red and white patches, irregular areas of redness | 20-50% | Highest risk among non-homogeneous, "speckled" appearance |
| Nodular Leukoplakia | White patch with small, rounded, elevated white nodules/lumps | 20-40% | Lumpy surface, often with high dysplasia |
| Verrucous Leukoplakia | Warty, corrugated, or exophytic (outward-growing) thick surface | 15-30% (can be higher with progression) | Rough, irregular texture, prone to early carcinoma |
| Proliferative Verrucous Leukoplakia (PVL) | Multiple, widespread, persistent, and recurrent verrucous lesions | 70-100% | Aggressive, recurrent, often multifocal |
Causes / Why It Happens
The exact cause of leukoplakia is not always clear, but several factors are strongly implicated, particularly for leukoplakia on the tongue. These are often chronic irritants or systemic issues that contribute to abnormal cell growth.
1. Tobacco Use (Primary Cause)
Tobacco is by far the leading etiological factor for leukoplakia. Its carcinogenic chemicals directly irritate oral tissues, leading to cellular changes.
- Smoking: Cigarettes, cigars, and pipe smoking expose the oral mucosa to numerous toxins, leading to a high incidence of leukoplakia. The heat and chemical irritants are major contributors.
- Smokeless Tobacco: Chewing tobacco, snuff, and dip are particularly potent causes. The habit of holding smokeless tobacco in a specific area (often the buccal vestibule) can lead to lesions (known as "smoker's keratosis" or "snuff dipper's lesion") that are a form of leukoplakia. While the tongue isn't the primary site for direct contact with smokeless tobacco, the systemic absorption and general oral environment can still contribute to lesions on the tongue.
2. Alcohol Consumption
Heavy and chronic alcohol intake is another significant risk factor. Alcohol, especially when combined with tobacco, acts synergistically to increase the risk of leukoplakia and its malignant transformation. The combination of both habits multiplies the risk far beyond the sum of their individual risks.
3. Chronic Irritation
While less common for the tongue specifically, chronic physical irritation can contribute to leukoplakia in other oral sites.
- Sharp Teeth or Restorations: A chronically rough tooth surface or a poorly fitting dental restoration rubbing against the tongue can, in rare cases, lead to localized irritation and subsequent leukoplakia. However, these usually cause frictional keratosis, which resolves when the irritant is removed, unlike true leukoplakia. It’s crucial for a dentist to differentiate this.
4. Human Papillomavirus (HPV) Infection
Certain high-risk strains of HPV, particularly HPV-16 and HPV-18, are increasingly recognized as contributors to oral cancer, and by extension, some cases of leukoplakia. While HPV-related lesions are more commonly found in the oropharynx (back of the throat), their role in oral cavity lesions, including on the tongue, is an area of ongoing research.
5. Weakened Immune System
Individuals with compromised immune systems, such as those with HIV/AIDS or organ transplant recipients, may have an increased susceptibility to oral lesions, including a specific type of leukoplakia called "hairy leukoplakia."
- Hairy Leukoplakia: This form is distinct from conventional leukoplakia. It's caused by the Epstein-Barr virus (EBV) and almost exclusively seen in immunocompromised individuals. It typically appears as white, corrugated, or "hairy" lesions on the lateral borders of the tongue. Unlike conventional leukoplakia, hairy leukoplakia is generally considered benign and does not have a high malignant potential, though it signals a compromised immune status. This article primarily focuses on conventional leukoplakia, but it's important to differentiate.
6. Other Contributing Factors
- UV Light Exposure: While primarily linked to lip cancer, extensive sun exposure over many years can contribute to actinic keratosis on the lips, a precancerous lesion, and theoretically could affect the tongue if exposed, though this is rare.
- Nutritional Deficiencies: Some studies suggest deficiencies in vitamins A and B complex may play a role, but evidence is not as strong as for tobacco and alcohol.
- Genetic Predisposition: A family history of oral cancer or certain genetic mutations may increase an individual's susceptibility.
Pro Tip: If you notice a white patch on your tongue, think about potential irritants in your lifestyle. Quitting tobacco and reducing alcohol intake are the most impactful steps to prevent and potentially reverse early leukoplakia.
Signs and Symptoms
The most significant characteristic of leukoplakia tongue is its visual presentation. Unfortunately, symptoms are often minimal, which can delay diagnosis.
What to Look For: The Visual Signs
- White or Grayish-White Patch: The hallmark of leukoplakia is a persistent white or grayish-white patch on the tongue. It can vary in size from a small spot to a large area.
- Non-Scrapable: Unlike conditions like thrush (oral candidiasis), which can be wiped away, leukoplakia cannot be removed by rubbing or scraping. This is a crucial diagnostic differentiator.
- Location on the Tongue: Leukoplakia can appear on various parts of the tongue:
- Lateral Borders (Sides): A very common site, especially for hairy leukoplakia, but also conventional leukoplakia.
- Dorsal Surface (Top): Can appear on the top surface.
- Ventral Surface (Underside): Less common, but possible.
- Texture Variations:
- Smooth and Flat: Homogeneous leukoplakia often presents as a thin, smooth, flat patch.
- Rough, Thickened, or Fissured: Some lesions can feel rough, leathery, or have cracks/fissures on the surface.
- Nodular or Warty: More concerning forms (non-homogeneous) can present with elevated lumps or a verrucous (wart-like) appearance.
- Mixed Red and White: Erythroleukoplakia combines white patches with areas of redness. The red areas are particularly suspicious for dysplasia.
- Borders: The edges of the lesion can be well-defined or blend into the surrounding normal tissue.
What It May Feel Like (or Not Feel Like)
- Usually Asymptomatic: The vast majority of leukoplakia lesions on the tongue cause no pain, discomfort, or altered sensation. This is why regular self-examinations and professional dental check-ups are so vital.
- Mild Discomfort (Rare): In some cases, a very large or thickened lesion might cause mild irritation when speaking, eating, or swallowing, especially if it's rubbing against teeth.
- Burning or Sensitivity (Rare): If the lesion is inflamed or has transformed into an early cancer, there might be localized burning, tenderness, or increased sensitivity to hot/cold foods, but this is less common in the precancerous stage.
When to Be Concerned: Any white patch on your tongue that persists for more than two weeks and cannot be scraped off warrants immediate professional evaluation. Pay particular attention if the patch:
- Changes in color (develops red areas)
- Becomes lumpy, firm, or raised
- Causes pain, burning, or numbness
- Bleeds easily
- Is accompanied by difficulty moving the tongue, speaking, or swallowing.
These could be signs of advanced dysplasia or malignant transformation.
Diagnosis
A thorough and accurate diagnosis is the cornerstone of managing leukoplakia tongue effectively. It involves a combination of clinical examination and, most importantly, a tissue biopsy.
1. Clinical Examination
- Visual Inspection: Your dentist or oral surgeon will carefully examine your entire oral cavity, paying close attention to the size, shape, color, texture, and location of the white patch on your tongue. They will assess if it's scrapable or non-scrapable.
- Palpation: The clinician will gently feel the lesion and the surrounding tissues to check for any firmness, induration (hardening), or changes in texture that might suggest deeper involvement or malignancy.
- Medical and Dental History: A detailed history will be taken, including questions about tobacco and alcohol use, past medical conditions, medications, and any other symptoms you might be experiencing.
- Risk Factor Assessment: The clinician will identify and discuss any risk factors present, such as smoking, chewing tobacco, or heavy alcohol consumption.
2. Adjunctive Screening Techniques (Optional, but helpful)
These tools are not diagnostic on their own but can help identify areas that require closer inspection or biopsy.
- Toluidine Blue Staining: A dye that preferentially stains dysplastic or malignant cells due to their higher nuclear activity. It can highlight suspicious areas. However, false positives can occur (e.g., from inflammation).
- Chemexfoliation / Vizilite Plus / Velscope Vx: These are light-based systems that use specific light wavelengths to visualize changes in oral tissues. Abnormal tissues may fluoresce differently or absorb light differently. Again, these are screening aids, not definitive diagnostic tools.
3. Biopsy (The Gold Standard)
A biopsy is the only way to definitively diagnose leukoplakia, determine the presence and degree of dysplasia (abnormal cell growth), and rule out oral cancer. There are several types:
- Incisional Biopsy: The most common approach. A small sample of tissue is surgically removed from the most suspicious area of the lesion. This is usually done under local anesthesia in the dental office or oral surgery clinic.
- Excisional Biopsy: If the lesion is small and easily accessible, the entire lesion may be removed during the biopsy procedure. If pathology confirms no malignancy, this can be both diagnostic and curative.
- Brush Biopsy (OralCDx): A less invasive method where a special brush is used to collect cells from the entire thickness of the lesion. While it's easy to perform and causes minimal discomfort, it's generally considered less reliable than an incisional biopsy for definitive diagnosis, especially for high-risk lesions, as it might miss deeper dysplastic cells. It's often used as an initial screening tool or for follow-up.
4. Histopathological Examination
Once the tissue sample is obtained, it is sent to an oral pathologist. The pathologist examines the tissue under a microscope to assess the cellular architecture and identify any signs of dysplasia or carcinoma. The degree of dysplasia is critical:
- Hyperkeratosis without Dysplasia: Thickening of the keratin layer, but cells appear normal. Low risk.
- Mild Dysplasia: Slight cellular abnormalities.
- Moderate Dysplasia: More significant cellular abnormalities, but not yet cancer.
- Severe Dysplasia (Carcinoma in situ): Significant cellular abnormalities affecting the full thickness of the epithelium, but the cells have not yet invaded the underlying connective tissue. This is considered the earliest form of cancer.
- Invasive Squamous Cell Carcinoma: Cancer cells have broken through the basement membrane and invaded the deeper tissues.
Pro Tip: Never delay a recommended biopsy. It is the single most important step in differentiating benign lesions from precancerous changes or early-stage oral cancer.
Treatment Options
The treatment approach for leukoplakia tongue depends heavily on the histopathological findings from the biopsy, specifically the presence and degree of dysplasia, as well as the lesion's size, location, and the patient's overall health and risk factors.
1. Watchful Waiting and Risk Factor Elimination (For Low-Risk Lesions)
- Description: For homogeneous leukoplakia with no or very mild dysplasia, and particularly if clear risk factors like tobacco use are present, the initial approach may be to eliminate the irritant and observe the lesion.
- Process: The patient is strongly advised to quit smoking and/or reduce alcohol intake. Regular follow-up appointments (e.g., every 3-6 months) are scheduled to monitor the lesion for any changes in size, color, or texture.
- Pros: Non-invasive, avoids surgical risks.
- Cons: Risk of malignant transformation, even if low, remains. Requires strict patient compliance and vigilant monitoring. If the lesion does not resolve or changes, intervention becomes necessary.
- Cost: Primarily consultation fees (e.g., $75-$250 per visit).
2. Surgical Excision
This is the most common and often preferred treatment for dysplastic leukoplakia or lesions that do not resolve after risk factor elimination.

-
a. Scalpel Excision:
- Description: The lesion is surgically cut out using a traditional scalpel. The surrounding tissue is also removed (a small margin) to ensure complete removal.
- Process: Performed under local anesthesia, sometimes with sedation. The area is numbed, the lesion is excised, and the wound is closed with sutures.
- Pros: Allows for complete histopathological examination of the entire lesion, high success rate for complete removal.
- Cons: Can result in scarring, potential for post-operative pain and swelling, risk of nerve damage if lesion is deep or near critical structures.
- Cost: $500 - $1,500 for a simple excision of a small lesion, potentially higher for larger or more complex cases requiring general anesthesia.
-
b. Laser Ablation/Excision (CO2 Laser):
- Description: A CO2 laser is used to vaporize or precisely cut away the leukoplakic tissue.
- Process: Similar to scalpel excision, performed under local anesthesia. The laser beam precisely removes the abnormal tissue.
- Pros: Minimizes bleeding during the procedure due to cauterization, often less post-operative swelling and pain, faster healing in some cases, high precision.
- Cons: May make histopathological evaluation slightly more challenging if the tissue is vaporized rather than excised cleanly, specialized equipment and training required, can be more expensive.
- Cost: $800 - $2,500 depending on the size of the lesion and clinic.
-
c. Cryotherapy:
- Description: The lesion is frozen using liquid nitrogen, causing the cells to die and slough off.
- Process: Applied directly to the lesion, typically requires multiple freeze-thaw cycles. Usually done under local anesthesia.
- Pros: Minimally invasive, relatively quick, less scarring than scalpel.
- Cons: Lack of tissue sample for histopathological confirmation (unless a biopsy was done prior), potential for discomfort, blistering, and swelling, multiple sessions might be needed. Not ideal for highly suspicious lesions without prior biopsy.
- Cost: $300 - $800 per session.
3. Photodynamic Therapy (PDT)
- Description: Involves the application of a photosensitizing agent to the lesion, followed by exposure to a specific wavelength of light. The light activates the agent, which then produces reactive oxygen species that destroy abnormal cells.
- Process: The photosensitizing agent (e.g., aminolevulinic acid) is applied topically or injected. After a waiting period, the lesion is exposed to laser light.
- Pros: Minimally invasive, highly selective for abnormal cells, good cosmetic outcomes, can treat large or multifocal lesions.
- Cons: Skin sensitivity to light (photosensitivity) for several days post-treatment, may require multiple sessions, can be costly. Not widely available for oral lesions.
- Cost: $1,000 - $4,000 per session, often requiring multiple sessions.
4. Systemic Retinoids (e.g., Vitamin A derivatives)
- Description: Oral medications derived from Vitamin A, such as isotretinoin or etretinate, which are known to influence cell growth and differentiation.
- Process: Prescribed as a course of treatment, often for widespread or recurrent leukoplakia, or as an adjunctive therapy post-surgery.
- Pros: Non-surgical approach, can treat multiple lesions.
- Cons: Significant side effects (dry skin/lips, liver toxicity, birth defects if pregnant), high recurrence rates once discontinued, requires close monitoring, generally considered for widespread or difficult cases.
- Cost: Varies by drug and insurance, but can be $50 - $200+ per month for medication, plus monitoring costs.
Pro Tip: For lesions with moderate to severe dysplasia, complete surgical excision is generally recommended by the American Dental Association (ADA) and oral pathology guidelines due to the high risk of malignant transformation.
Step-by-Step Process: What to Expect During Treatment
The journey from initial detection of a white patch on your tongue to definitive treatment typically follows a structured process. Here’s what you can expect:
Step 1: Initial Consultation and Oral Examination
- What happens: You notice a white patch on your tongue and schedule an appointment with your dentist or an oral medicine specialist. They will conduct a thorough visual and tactile examination of your entire mouth, focusing on the lesion. They'll ask about your medical history, lifestyle habits (especially tobacco and alcohol), and when you first noticed the patch.
- Purpose: To clinically evaluate the lesion, rule out other conditions (like thrush or frictional keratosis), and determine the next steps.
Step 2: Diagnostic Biopsy
- What happens: If the lesion is suspicious for leukoplakia, a biopsy will be recommended. This is usually an incisional biopsy, where a small tissue sample from the most suspicious part of the lesion is taken.
- Preparation: You'll receive local anesthesia to numb the area around the patch. You might feel a slight pinch during the injection, but no pain during the biopsy.
- Procedure: A small piece of tissue (typically 2-4 mm) is carefully removed. Any bleeding is controlled, and the site may be closed with a few dissolvable sutures. The entire process usually takes 15-30 minutes.
- Post-Biopsy: You'll receive instructions for care, including pain management (over-the-counter pain relievers), soft diet, and avoiding irritants.
- Purpose: To obtain tissue for microscopic examination by an oral pathologist to confirm the diagnosis, determine the type of leukoplakia, and assess the presence and degree of dysplasia.
Step 3: Pathology Report and Treatment Planning
- What happens: The biopsy sample is sent to an oral pathology lab. It typically takes 7-14 business days to receive the final report. Your dentist or specialist will review the report with you, explaining the findings (e.g., hyperkeratosis without dysplasia, mild dysplasia, severe dysplasia, or carcinoma).
- Purpose: Based on the pathology report, a personalized treatment plan will be formulated.
- No or Mild Dysplasia: Often watchful waiting, combined with aggressive risk factor elimination (e.g., quitting tobacco).
- Moderate to Severe Dysplasia or PVL: Surgical excision is typically recommended.
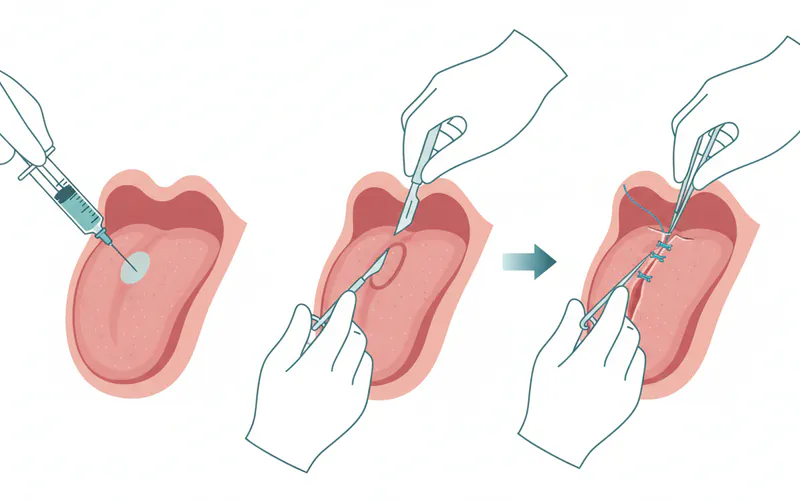
Step 4: Definitive Treatment (If Required)
- Surgical Excision (Scalpel, Laser, or Cryotherapy):
- Preparation: Similar to the biopsy, the area will be numbed with local anesthesia. For larger lesions or anxious patients, sedation or general anesthesia might be used.
- Procedure: The chosen method (scalpel, laser, or cryotherapy) will be used to remove or destroy the entire lesion, often with a small margin of healthy tissue. For scalpel or laser excision, the wound is typically closed with sutures.
- Duration: The procedure can range from 30 minutes to over an hour, depending on the size and complexity of the lesion.
- Photodynamic Therapy (PDT):
- Preparation: A photosensitizing agent is applied or injected, followed by a waiting period (hours to days).
- Procedure: The lesion is exposed to a specific wavelength of light to activate the agent.
- Purpose: To completely remove or destroy the precancerous cells to prevent malignant transformation or to treat early-stage oral cancer.
Step 5: Recovery and Aftercare
- What happens: You will receive detailed post-operative instructions specific to your treatment. This will include advice on pain management (prescribed or OTC pain relievers), diet (soft foods initially), oral hygiene (gentle rinsing, careful brushing), and avoiding strenuous activity or irritating foods/drinks.
- Purpose: To promote healing, minimize discomfort, and prevent complications.
Step 6: Follow-up and Long-Term Monitoring
- What happens: Regular follow-up appointments are crucial, typically every 3-6 months for the first few years, then annually. These appointments involve a thorough oral examination to check the healing site and screen for any recurrence or new lesions.
- Purpose: Leukoplakia has a tendency to recur, and patients who have had leukoplakia are at a higher lifetime risk for developing new lesions or oral cancer. Consistent monitoring is vital for early detection of any new changes.
Pro Tip: Active participation in your treatment plan, including diligently following post-operative instructions and attending all follow-up appointments, significantly impacts your long-term prognosis.
Cost and Insurance
Understanding the financial aspects of diagnosing and treating leukoplakia tongue is important for patients in the US. Costs can vary widely based on the complexity of the case, the chosen treatment method, geographic location, and whether you have dental or medical insurance.
Average US Cost Ranges (Without Insurance)
- Initial Consultation / Oral Exam: $75 - $250
- Factors: Specialist (oral surgeon, oral medicine) vs. general dentist, comprehensiveness of exam.
- Diagnostic Biopsy (Incisional/Excisional): $300 - $700
- Includes: Local anesthesia, biopsy procedure, lab fees for pathology.
- Note: A brush biopsy is generally less expensive, around $150 - $350, but may not be definitive.
- Surgical Excision (Scalpel): $500 - $1,500 for a small, simple lesion.
- Factors: Size/complexity of lesion, need for sutures, type of anesthesia (local vs. sedation vs. general), geographic region.
- Larger/complex lesions with general anesthesia can range from $2,000 - $4,000+.
- Laser Ablation/Excision: $800 - $2,500
- Factors: Similar to scalpel, often slightly higher due to specialized equipment.
- Cryotherapy: $300 - $800 per session
- Note: May require multiple sessions.
- Photodynamic Therapy (PDT): $1,000 - $4,000 per session
- Note: Often multiple sessions are needed, and it's less commonly available for oral lesions.
- Follow-up Appointments: $75 - $250 per visit
- Usually involves: Oral examination and counseling.
Insurance Coverage Details
Leukoplakia is generally considered a medical condition due to its precancerous nature, rather than a purely dental issue. This means that medical insurance (not just dental insurance) is often the primary payer for diagnosis and treatment.
-
Medical Insurance (PPO, HMO, EPO, etc.):
- Diagnosis (Biopsy): Most medical insurance plans cover medically necessary biopsies. You will likely be responsible for your deductible, co-insurance (e.g., 10-30% of the cost after deductible), and co-pays.
- Treatment (Surgery, PDT): Treatment for leukoplakia, especially dysplastic lesions, is generally covered by medical insurance as a medically necessary procedure to prevent or treat cancer. Again, deductibles, co-insurance, and co-pays apply.
- In-Network vs. Out-of-Network: Costs will be significantly lower if you choose providers (oral surgeons, hospitals, pathology labs) who are in your insurance network.
- Pre-authorization: For more expensive procedures like surgery, your provider's office may need to obtain pre-authorization from your medical insurance company.
-
Dental Insurance (PPO, HMO, DHMO):
- Some dental PPO plans may offer limited coverage for oral surgery procedures, especially if they are deemed "medically necessary" and involve the hard and soft tissues of the mouth. However, dental insurance typically has lower annual maximums (e.g., $1,000-$2,000) compared to medical insurance.
- Dental HMO/DHMO plans usually require you to see a specific network dentist and may have very limited or no coverage for specialist oral surgery outside their network.
- Coordination of Benefits: If you have both medical and dental insurance, they may coordinate benefits. Medical insurance is usually primary for medically necessary surgical procedures in the oral cavity.
Pro Tip: Always call both your medical and dental insurance providers before any procedure to understand your specific benefits, deductibles, co-pays, and out-of-pocket maximums. Request CPT codes from your dental office and provide them to your insurance company for accurate estimates.
Recovery and Aftercare
Proper recovery and diligent aftercare are essential for healing, minimizing complications, and preventing recurrence after treatment for leukoplakia tongue.
Immediately After Procedure (First 24-72 Hours)
- Pain Management: Expect some discomfort, especially after surgical excision. Your dentist or surgeon may prescribe pain medication or recommend over-the-counter options like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol).
- Bleeding: Minor oozing or spotting is normal. Avoid rinsing vigorously or spitting, as this can dislodge the blood clot. Apply gentle pressure with a clean gauze if needed.
- Swelling: Some swelling of the tongue is common. Applying a cold compress to the outside of your jaw/neck area intermittently for the first 24 hours can help reduce swelling. Keep your head elevated.
- Diet: Stick to soft, bland foods that are easy to chew and swallow. Avoid spicy, acidic, hot, or crunchy foods that could irritate the wound. Examples: yogurt, applesauce, mashed potatoes, soft scrambled eggs, lukewarm soups. Stay well-hydrated.
- Oral Hygiene: Gently rinse your mouth with a warm salt water solution (1/2 teaspoon salt in 8 ounces warm water) several times a day, especially after meals. Avoid direct brushing of the surgical site for the first few days, but continue to gently brush other areas of your mouth.
- Activity: Rest and avoid strenuous physical activity for 24-48 hours.
Long-Term Aftercare and Monitoring (Weeks to Years)
- Suture Removal (if non-dissolvable): If non-dissolvable sutures were used, they will typically be removed by your dentist or surgeon 7-10 days post-procedure. Dissolvable sutures will fall out on their own.
- Oral Hygiene: Maintain excellent oral hygiene. Gentle but thorough brushing and flossing are crucial to prevent infection and promote overall oral health.
- Avoid Irritants: This is paramount.
- Quit Tobacco: If you smoke or use smokeless tobacco, this is the most critical step. Continuing tobacco use significantly increases the risk of recurrence and new lesions.
- Limit Alcohol: Reduce or eliminate alcohol consumption, as it also contributes to the risk.
- Avoid Chronic Irritation: Ensure any sharp tooth edges or ill-fitting dentures are addressed by your dentist to prevent new irritation.
- Self-Examination: Regularly examine your tongue and entire oral cavity in a well-lit mirror. Look for any new white or red patches, lumps, or changes in texture. Familiarize yourself with how your mouth normally looks.
- Regular Dental Check-ups: This is perhaps the most important long-term aftercare step. Patients with a history of leukoplakia require more frequent and thorough oral cancer screenings. Typically, this means check-ups every 3-6 months for the first few years, then annually for life. Your dentist will monitor the treated area and screen for new lesions.
- Nutritional Support: A balanced diet rich in fruits, vegetables, and antioxidants can support overall oral health.
- Sun Protection: If you spend significant time in the sun, use lip balm with SPF to protect your lips, as sun exposure can contribute to some oral lesions.
Pro Tip: Be proactive. If you notice any new or changing spots on your tongue or elsewhere in your mouth, do not wait for your next scheduled appointment. Contact your dentist or oral surgeon immediately. Early detection of recurrence is vital.
Prevention
Preventing leukoplakia tongue, and more importantly, preventing its progression to oral cancer, revolves primarily around lifestyle modifications and diligent oral health practices.
1. Eliminate Tobacco Use (Most Critical Step)
- Quit Smoking: Cigarettes, cigars, and pipes are major culprits. Seek support through cessation programs, nicotine replacement therapy, or prescription medications.
- Stop Smokeless Tobacco: Chewing tobacco, snuff, and dip are directly linked to leukoplakia and oral cancer. Quitting these products is non-negotiable for prevention.
2. Limit Alcohol Consumption
- Reduce or ideally eliminate heavy alcohol intake. Alcohol acts synergistically with tobacco, multiplying the risk of oral cancer. The CDC recommends limiting alcohol to 2 drinks or less per day for men and 1 drink or less per day for women on days when alcohol is consumed.
3. Regular Dental Check-ups and Oral Cancer Screenings
- Routine Visits: Schedule regular dental examinations at least twice a year (every 6 months), or more frequently if you have risk factors.
- Comprehensive Screenings: During these visits, your dentist performs a thorough visual and tactile oral cancer screening, examining your tongue, cheeks, lips, gums, and throat for any suspicious lesions. Early detection is key.
4. Practice Excellent Oral Hygiene
- Brush your teeth twice a day and floss daily. While poor hygiene isn't a direct cause of leukoplakia, maintaining a healthy oral environment is crucial for overall tissue health and can help your dentist better spot anomalies.
5. Healthy Diet
- Consume a diet rich in fruits, vegetables, and whole grains. Antioxidants found in these foods may help protect cells from damage. Limit processed foods and excessive sugar.
6. HPV Vaccination
- The Human Papillomavirus (HPV) vaccine (Gardasil 9) is primarily known for preventing cervical cancer, but it also protects against high-risk HPV strains that can cause oral cancers. Discuss with your medical doctor if the HPV vaccine is appropriate for you or your children, especially given the rising incidence of HPV-related oral cancers.
7. Avoid Chronic Irritation
- Ensure any sharp or broken teeth are repaired, and ill-fitting dentures or dental appliances are adjusted or replaced. While not a primary cause of leukoplakia, eliminating chronic physical trauma is a good preventative measure for overall oral health.

8. Self-Examination
- Perform regular self-examinations of your mouth in a well-lit mirror. Pull out your tongue, look at the top, bottom, and sides. Feel your tongue with your finger. Look at your inner cheeks, gums, and roof of your mouth. Get to know what your mouth normally looks like and feels like, so you can quickly spot any changes.
Pro Tip: Prevention is always better than cure. Adopting these habits can significantly reduce your risk of developing leukoplakia tongue and subsequent oral cancer.
Risks and Complications
While leukoplakia itself is not cancer, it carries significant risks and potential complications, primarily centered around its propensity for malignant transformation and issues related to its treatment.
1. Malignant Transformation (The Primary Risk)
- Progression to Oral Cancer: The most severe risk of leukoplakia tongue is its potential to develop into squamous cell carcinoma, the most common type of oral cancer. This transformation can occur over months or years. The risk is higher for non-homogeneous types (erythroleukoplakia, nodular, verrucous) and especially high for Proliferative Verrucous Leukoplakia (PVL).
- Invasion: If cancer develops, it can invade deeper tissues of the tongue, potentially leading to pain, difficulty swallowing or speaking, and disfigurement.
- Metastasis: Untreated or advanced oral cancer can spread (metastasize) to nearby lymph nodes in the neck and then to distant organs, significantly worsening the prognosis and becoming life-threatening.
2. Recurrence
- Even after successful removal or treatment of a leukoplakic lesion, there is a risk of the lesion recurring in the same spot or developing new lesions elsewhere in the mouth (field cancerization). This risk is particularly high for individuals who continue to engage in high-risk behaviors (tobacco, alcohol) or for aggressive forms like PVL.
- Recurrence necessitates ongoing vigilance and regular follow-up appointments.
3. Treatment-Related Complications
While treatments are generally safe, they carry potential risks:
- Pain and Discomfort: Post-operative pain is common, especially after surgical excision. It usually subsides within a few days to a week.
- Swelling and Bruising: Temporary swelling and bruising around the treated area are normal.
- Infection: Any surgical site carries a risk of infection. Following post-operative care instructions, including oral hygiene, is crucial to minimize this risk.
- Bleeding: While usually minor and easily controlled, excessive bleeding can occur, especially if blood thinners are being taken.
- Scarring: Surgical excision can leave a scar on the tongue, which might be noticeable depending on the size and location of the lesion.
- Altered Sensation or Numbness: If nerves are involved or inadvertently damaged during surgical removal, there's a risk of temporary or, rarely, permanent numbness or altered sensation in a part of the tongue. This is more of a concern for deeper or larger excisions.
- Speech and Swallowing Difficulties: For larger lesions requiring extensive removal, there might be temporary difficulty with speech (dysarthria) or swallowing (dysphagia) until the tongue heals and adapts.
- Side Effects of Systemic Therapies: If retinoids are used, side effects like dry skin, dry lips, liver toxicity, and birth defects (if pregnant) are significant concerns, requiring close medical monitoring.
4. Psychological Impact
- The diagnosis of a potentially malignant disorder can cause significant anxiety and stress. Living with the risk of cancer and undergoing frequent follow-ups can have a psychological toll.
Pro Tip: The best way to mitigate these risks is through early detection, accurate diagnosis, appropriate treatment, and rigorous adherence to follow-up schedules and preventative measures.
Children / Pediatric Considerations
Leukoplakia tongue is exceedingly rare in children. When it does occur, the causes and management differ significantly from those in adults.
- Rarity: Conventional leukoplakia, strongly associated with tobacco and alcohol, is virtually nonexistent in children, as these risk factors are typically absent.
- Hairy Leukoplakia: In immunocompromised children (e.g., those with HIV/AIDS, undergoing chemotherapy, or post-organ transplant), hairy leukoplakia (caused by Epstein-Barr virus) can be seen. This appears as corrugated white patches, usually on the lateral borders of the tongue. Hairy leukoplakia is generally benign and not considered precancerous.
- Other Causes of White Patches in Children: More common causes for white patches on a child's tongue include:
- Oral Thrush (Candidiasis): Easily scraped off, revealing red, bleeding tissue underneath. Common in infants and children with weakened immune systems or those on antibiotics.
- Frictional Keratosis: Caused by chronic irritation, such as a sharp tooth, thumb sucking, or biting. These lesions typically resolve once the irritant is removed.
- Lichen Planus: An inflammatory condition that can appear as white lacy patterns or patches. Less common in children but possible.
- Geographic Tongue: Not a leukoplakia, but an inflammatory condition where areas of the tongue appear smooth and red, bordered by raised white lines, constantly changing patterns. Harmless.
- Diagnosis in Children: Any persistent white lesion on a child's tongue that cannot be identified as a common benign condition should be evaluated by a pediatric dentist or oral medicine specialist. A biopsy might still be necessary to rule out rare but serious conditions.
- Treatment in Children: If conventional leukoplakia were diagnosed (extremely rare), treatment would focus on identifying and eliminating the cause. Surgical excision would be considered if dysplasia is present, with extreme care to minimize impact on the developing oral structures. For hairy leukoplakia, treating the underlying immune condition is key; the lesions themselves may regress or be treated symptomatically.
Pro Tip for Parents: While leukoplakia is rare in children, any persistent, unexplained white patch on your child's tongue that does not resolve within a week or two should be evaluated by a pediatric dentist.
Cost Breakdown
A detailed breakdown of costs for leukoplakia tongue diagnosis and treatment in the US, considering various scenarios.
US Average Costs (Out-of-Pocket, Without Insurance)
- Initial Evaluation:
- General Dentist Consultation: $75 - $150
- Oral Medicine Specialist/Oral Surgeon Consultation: $150 - $250
- Diagnostic Procedures:
- Incisional Biopsy (including lab fees): $300 - $700
- Brush Biopsy (less definitive, may or may not include lab fee): $150 - $350
- Treatment Procedures:
- Watchful Waiting (per visit): $75 - $250 (for follow-up exams)
- Scalpel Excision (Local Anesthesia):
- Small lesion: $500 - $1,500
- Medium/Complex lesion (may require sedation): $1,500 - $3,000
- Large/Highly complex lesion (may require hospital setting/general anesthesia): $3,000 - $6,000+
- Laser Ablation/Excision (Local Anesthesia):
- Small lesion: $800 - $1,800
- Medium/Complex lesion: $1,800 - $3,000
- Cryotherapy (per session): $300 - $800 (often multiple sessions required)
- Photodynamic Therapy (per session): $1,000 - $4,000 (multiple sessions typical)
- Systemic Retinoids (Medication Cost per month): $50 - $200+ (plus monitoring lab tests)
- Post-Treatment Follow-up Exams (each): $75 - $250
With Insurance (Medical vs. Dental)
- Medical Insurance (Primary for Diagnosis/Treatment):
- Deductible: You'll pay 100% of costs until your annual deductible (e.g., $500 - $5,000) is met.
- Co-insurance: After deductible, you pay a percentage (e.g., 10-30%) of the allowed charges, and insurance pays the rest.
- Co-pay: A fixed amount paid per visit (e.g., $20 - $50) for consultations.
- Out-of-Pocket Maximum: A cap on how much you pay in a year. Once reached, insurance covers 100% of in-network costs.
- Example: A $1,500 surgical excision might cost you $700 if you have a $500 deductible and 20% co-insurance.
- Dental Insurance (Secondary or Limited Coverage):
- May cover a small portion of oral surgery procedures, but often subject to lower annual maximums ($1,000 - $2,000 typically).
- Good for routine check-ups and cleanings, which are vital for ongoing monitoring.
Payment Plans and Financing Options
- In-Office Payment Plans: Many dental and oral surgery offices offer interest-free payment plans for a few months for balances not covered by insurance.
- Third-Party Financing (e.g., CareCredit): These credit cards are specifically designed for healthcare expenses, often offering interest-free promotional periods (e.g., 6, 12, 18 months) if the balance is paid in full by the end of the period.
- Healthcare Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use pre-tax dollars to cover medical and dental expenses, effectively reducing your out-of-pocket costs.
Cost-Saving Tips
- Verify Insurance Coverage: Always contact both your medical and dental insurance providers before any procedure. Ask for CPT codes from the office to get precise benefit information.
- Choose In-Network Providers: Staying within your insurance network can drastically reduce costs.
- Discuss All Options: Talk to your oral surgeon about the most cost-effective yet appropriate treatment for your specific situation.
- Community Health Centers/Dental Schools: These institutions often provide high-quality care at a reduced cost, especially for diagnostic procedures and follow-up. They are excellent resources if you are uninsured or underinsured.
- Negotiate: For significant out-of-pocket costs, you may be able to negotiate a discount with the provider's office for upfront cash payment.
Frequently Asked Questions
1. Is leukoplakia tongue always cancerous?
No, leukoplakia tongue is not always cancerous. It is considered a "potentially malignant disorder," meaning it has the potential to transform into oral cancer, specifically squamous cell carcinoma. The risk of transformation varies significantly depending on the type of leukoplakia and the presence of dysplasia (abnormal cells) on biopsy, ranging from 3% to 50% or even higher for aggressive forms like Proliferative Verrucous Leukoplakia.
2. Can leukoplakia on the tongue go away on its own?
Sometimes, especially if the cause is identified and eliminated. For instance, if a white patch is mainly due to tobacco use, quitting smoking or chewing tobacco may lead to its regression or complete disappearance. However, if there is dysplasia, or if the lesion persists despite removing risk factors, it is unlikely to resolve on its own and often requires intervention.
3. How painful is a biopsy on the tongue?
A biopsy on the tongue is typically not painful during the procedure itself, as a local anesthetic is administered to thoroughly numb the area. You might feel a slight pressure or tugging sensation. After the anesthetic wears off, you can expect some mild to moderate discomfort, soreness, and swelling for a few days, which can usually be managed with over-the-counter pain relievers or prescribed medication.
4. What is the difference between leukoplakia and oral thrush?
The key difference is scrapability. Oral thrush (candidiasis) is a white, creamy fungal infection that can usually be rubbed or scraped off, revealing a red, sometimes bleeding, surface underneath. Leukoplakia, on the other hand, is a persistent white patch that cannot be scraped off and remains fixed to the tissue.
5. What are the chances of leukoplakia recurring after treatment?
The chance of recurrence varies but can be significant, especially if risk factors (like continued tobacco or alcohol use) persist. Even after successful removal, new lesions can appear in the same area or elsewhere in the mouth due to a phenomenon called "field cancerization." This is why strict follow-up and monitoring are crucial.
6. Can HPV cause leukoplakia on the tongue?
Yes, certain high-risk strains of the Human Papillomavirus (HPV), particularly HPV-16, are increasingly recognized as contributing factors to oral lesions, including some cases of leukoplakia. While HPV is more commonly associated with oral cancers in the tonsils and base of the tongue, its role in oral cavity leukoplakia is an area of ongoing research and concern.
7. How long does it take for leukoplakia to turn into cancer?
There is no fixed timeline. The malignant transformation of leukoplakia into cancer can occur over several months to many years, or it may never happen. Factors like the degree of dysplasia, type of leukoplakia (non-homogeneous types have a faster progression risk), and continued exposure to risk factors influence the speed of transformation. Regular monitoring is key.
8. What are some alternatives to surgery for leukoplakia?
Alternatives to surgery include watchful waiting (for very low-risk lesions), laser ablation (using a laser to remove the tissue), cryotherapy (freezing the lesion), and photodynamic therapy (using light-activated drugs). Systemic retinoids (Vitamin A derivatives) may also be used, but generally carry significant side effects and recurrence rates. The best alternative depends on the lesion's characteristics and pathology findings.
9. How often should I have follow-up appointments after being diagnosed with leukoplakia?
The frequency of follow-up appointments is determined by your dentist or oral specialist based on your individual risk factors and the nature of your lesion. Typically, patients are advised to have oral examinations every 3-6 months for the first few years, and then annually for life. This vigilant monitoring is crucial for detecting any recurrence or new lesions early.
10. Does a white tongue always mean leukoplakia?
No, a white tongue does not always mean leukoplakia. Many conditions can cause a white appearance on the tongue, including oral thrush (which can be scraped off), geographic tongue (migratory patterns of white and red), hairy tongue (elongated papillae), and frictional keratosis (due to irritation). Only a persistent, non-scrapable white patch should raise suspicion for leukoplakia.
When to See a Dentist
Given the potentially serious nature of leukoplakia tongue, knowing when to seek professional dental attention is critical for your oral health and overall well-being.
Immediate Attention (Schedule an appointment within days):
- Any persistent white patch on your tongue that does not go away within two weeks: This is the primary warning sign for leukoplakia. If you notice a white area that cannot be rubbed off or scraped away, it warrants evaluation.
- Any white patch that changes in appearance: If a previously observed white patch starts to become red, lumpy, thickened, or develops ulcers within it.
- Accompanying symptoms: If the white patch on your tongue is associated with:
- Unexplained pain or soreness that doesn't go away.
- Numbness or tingling in the tongue or mouth.
- Difficulty chewing, swallowing, or moving your tongue.
- Bleeding from the lesion.
- A persistent sore throat or hoarseness.
- A lump or swelling in your neck.
Routine Care Guidance:
- Regular Dental Check-ups: Even if you don't notice any specific symptoms, consistent oral cancer screenings are a vital part of your routine dental visits. The ADA recommends annual oral cancer screenings, especially if you have risk factors such as tobacco or alcohol use.
- If You Have Risk Factors: If you smoke, use smokeless tobacco, or consume alcohol regularly, you should be particularly vigilant about self-examinations and never miss your routine dental appointments, as you are at a higher risk for leukoplakia and oral cancer.
Emergency vs. Scheduled Appointment:
- While most leukoplakia findings are not acute emergencies, any rapidly changing lesion, sudden severe pain, or difficulty breathing/swallowing should prompt an emergency medical evaluation.
- For persistent white patches without acute symptoms, a scheduled appointment with your general dentist is the first step. They can assess the lesion and refer you to an oral medicine specialist or oral surgeon if a biopsy or further specialized evaluation is needed.
Red Flags to Never Ignore:
- A non-healing sore or ulcer in the mouth lasting more than 2 weeks.
- Any unexplained lump or thickening in the mouth or neck.
- Difficulty swallowing or persistent hoarseness.
- Numbness in the face, mouth, or neck.
- Unexplained weight loss.
Early detection of leukoplakia and its potential transformation into oral cancer is your best defense. Don't hesitate to reach out to your dental professional with any concerns about your oral health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Floor of Mouth Cancer: Complete Guide
Each year, over 54,000 Americans are diagnosed with oral cavity or oropharyngeal cancer, making it a significant public health concern. While often overlooked, floor of mouth cancer is a particularly aggressive and common form of oral cancer, accounting for a substantial percentage of all oral c
February 23, 2026
Oral Cancer Stages Pictures: Complete Guide
Oral cancer, a serious and potentially life-threatening disease, affects thousands of Americans each year. According to the American Cancer Society, approximately 54,000 new cases of oral cavity or oropharyngeal cancer are diagnosed annually in the United States. While these numbers can be daunt
February 23, 2026
Can You Die From Mouth Cancer
Oral cancer is a formidable disease, often striking with insidious subtlety before revealing its devastating potential. It's a question that weighs heavily on the minds of those who receive a diagnosis or even those simply concerned about unusual oral symptoms: can you die from mouth cancer? The
February 23, 2026
Mouth Cancer Photos: Complete Guide
Oral cancer is a formidable disease that affects tens of thousands of Americans each year, often with devastating consequences if not detected early. According to the Oral Cancer Foundation, approximately 54,000 Americans are diagnosed with oral or oropharyngeal cancer annually, and nearly 11,23
February 23, 2026