Bone Graft for Implant: Complete Guide
Key Takeaways
- Losing a tooth can impact more than just your smile; it initiates a complex biological process that can lead to significant bone loss in your jaw. In fact, studies show that within the first year of tooth extraction, the width of the alveolar ridge can decrease by up to 50%, with substantial ver
Bone Graft for Implant: Complete Guide
Losing a tooth can impact more than just your smile; it initiates a complex biological process that can lead to significant bone loss in your jaw. In fact, studies show that within the first year of tooth extraction, the width of the alveolar ridge can decrease by up to 50%, with substantial vertical bone loss following. This critical reduction in bone volume often prevents the successful placement of dental implants, a gold standard for tooth replacement. If you're considering a dental implant to restore your smile and chewing function, understanding the necessity of a bone graft for implant procedures is paramount. This comprehensive guide from SmilePedia.net will demystify bone grafting, explaining why it's crucial for implant success, the various types and processes involved, what to expect regarding cost and recovery, and how to ensure the best possible outcome for your oral health. We'll delve into everything from the initial assessment to long-term care, providing you with the knowledge needed to navigate your journey toward a strong, healthy smile.
Key Takeaways:
- Necessity: A bone graft for implant procedures is often crucial to provide sufficient bone volume and density for stable implant placement, especially after tooth loss, trauma, or periodontal disease.
- Types: Common graft materials include autograft (your own bone), allograft (donor human bone), xenograft (animal bone), and alloplast (synthetic materials).
- Procedures: Techniques vary, including socket preservation (after extraction), ridge augmentation (to rebuild width/height), and sinus lifts (for upper back jaw).
- Cost: Average costs in the US range from $200-$1,200 for a simple socket preservation to $1,500-$3,000+ for a complex sinus lift or large ridge augmentation, often not fully covered by dental insurance.
- Timeline: Healing typically takes 3-9 months before the dental implant can be placed, depending on the graft type and patient's healing capacity.
- Success Rate: With proper technique and patient adherence to aftercare, bone graft success rates are very high, often exceeding 95%, significantly improving implant longevity.
- Prevention: Prompt action after tooth loss, like immediate implant placement or socket preservation, can help prevent the need for more extensive bone grafting later.
What Is a Bone Graft for Implant? An Overview
A bone graft for a dental implant is a surgical procedure designed to restore lost bone in your jaw, creating a stable foundation for a dental implant. When a tooth is lost, whether due to extraction, trauma, or advanced periodontal disease, the bone that once supported it, known as the alveolar bone, begins to resorb or shrink away. This process of bone resorption can lead to insufficient bone volume or density in the jaw, making it impossible to place a dental implant securely.
Dental implants require a specific amount of healthy bone to achieve osseointegration, the process where the implant fuses directly with the jawbone. Without adequate bone, an implant might fail to integrate, become loose, or even fall out. A bone graft effectively adds new bone material to the deficient area, stimulating your body's natural healing mechanisms to grow new, healthy bone. This new bone then provides the robust support necessary for a successful, long-lasting dental implant, ensuring the stability and functionality of your new tooth. The goal is not just to fill a void, but to encourage your own body to regenerate the bone, making it a living part of your jaw.
Types of Bone Graft Materials and Techniques
Bone grafting for dental implants is not a one-size-fits-all procedure. The choice of material and technique depends on the extent of bone loss, the location in the mouth, and your individual health profile.
Bone Graft Materials
The source of the bone graft material is a critical distinction, each with its own advantages and considerations:
-
Autograft (Autogenous Bone Graft):
- Description: This is considered the "gold standard" because the bone is harvested from your own body. Common donor sites include the chin, ramus (back of the lower jaw), hip, or tibia.
- Pros: Highest success rate due to no risk of immune rejection; contains living bone cells (osteocytes) and growth factors that actively promote new bone formation (osteogenesis).
- Cons: Requires a second surgical site for harvesting, which means additional discomfort, longer recovery time, and increased surgical risk. Limited availability of donor bone.
- Use Case: Often preferred for larger defects or when rapid, robust bone regeneration is crucial.
-
Allograft (Allogeneic Bone Graft):
- Description: Bone harvested from a deceased human donor, processed and sterilized to remove all organic material and reduce the risk of disease transmission. Available as freeze-dried bone allograft (FDBA) or demineralized freeze-dried bone allograft (DFDBA).
- Pros: Readily available in various forms and quantities; avoids the need for a second surgical site; high success rates.
- Cons: Does not contain living cells (osteogenesis); acts more as a scaffold (osteoinduction and osteoconduction) for your body's cells to grow into. Small, theoretical risk of disease transmission (though rigorously screened and processed).
- Use Case: Widely used for many types of bone defects, especially where autograft harvesting is not practical or desired.
-
Xenograft:
- Description: Bone material derived from an animal source, typically bovine (cow) or porcine (pig). It is meticulously processed to ensure sterility and biocompatibility.
- Pros: Abundant supply; avoids a second surgical site; acts as an excellent scaffold (osteoconduction) for new bone growth.
- Cons: Slower rate of resorption and replacement by host bone compared to autografts or allografts; no living cells.
- Use Case: Very common for socket preservation and sinus lifts due to its structural stability and ability to maintain space.
-
Alloplast (Alloplastic Bone Graft):
- Description: Synthetic bone graft materials, often composed of calcium phosphate compounds (e.g., hydroxyapatite, tricalcium phosphate) or bioactive glass.
- Pros: Unlimited supply; no risk of disease transmission or immune rejection; acts as a highly biocompatible scaffold (osteoconduction).
- Cons: No living cells; variable rates of resorption and replacement by host bone; may be slower to integrate than other graft types.
- Use Case: Suitable for smaller defects, socket preservation, or as an extender mixed with other graft materials.
Bone Grafting Techniques
The method of bone grafting is chosen based on the specific anatomical deficiency:
-
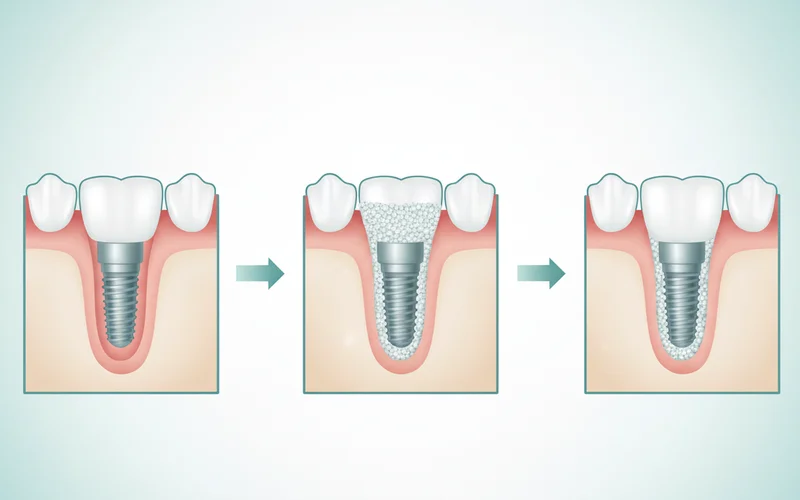
Socket Preservation (Alveolar Ridge Preservation):
- Purpose: To prevent bone loss immediately after a tooth extraction.
- Process: After the tooth is removed, the graft material is placed directly into the empty socket and often covered with a collagen membrane and sutured. This maintains the bone volume and width, making it easier for a one tooth implant to be placed later.
- Timeline: Implants can typically be placed after 3-6 months of healing.
- Pro Tip: This procedure is highly recommended when a tooth is extracted, especially if you plan for a future implant. It's much easier to preserve bone than to rebuild it once it's lost.
-
Ridge Augmentation (Horizontal and/or Vertical):
- Purpose: To increase the width and/or height of the jawbone when it has significantly shrunk.
- Process: An incision is made in the gum to expose the deficient bone. Graft material (often autograft or a mix) is placed on top of or alongside the existing bone. It is then covered with a protective membrane and the gum tissue is sutured back over it.
- Timeline: Healing typically takes 6-9 months before implant placement.
- Variations:
- Horizontal Augmentation: Widens a narrow ridge.
- Vertical Augmentation: Increases the height of a short ridge.
- Block Graft: A solid piece of autogenous bone is secured to the deficient area with small screws.
-
Sinus Lift (Sinus Augmentation):
- Purpose: To increase bone volume in the upper back jaw, which often has insufficient bone due to the proximity of the maxillary sinuses and natural bone resorption after upper molar loss.
- Process: The gum tissue is lifted, and a small "window" is created in the bone of the upper jaw. The membrane lining the sinus is gently lifted, and bone graft material is placed into the space created beneath it. The area is then closed with sutures.
- Timeline: Implants can often be placed 6-12 months after a sinus lift, depending on the amount of bone created. In some cases, a small amount of graft can be done concurrently with implant placement ("crestal" or "internal" sinus lift), reducing overall treatment time.
- Pro Tip: If you've lost upper back teeth many years ago, a sinus lift is a very common and successful procedure to enable implant placement.
Causes of Bone Loss Leading to the Need for Bone Graft for Implant
Understanding why bone loss occurs is crucial for prevention and timely intervention. Several factors can contribute to the degradation of jawbone density, leading to the need for a bone graft for implant procedures.
- Tooth Extraction: This is the most common cause. Once a tooth is removed, the bone that once supported it no longer receives the stimulation from chewing forces. Without this functional load, the bone naturally begins to resorb and shrink. The rate and extent of bone loss vary among individuals but can be significant within the first few months.
- Periodontal Disease (Gum Disease): Advanced periodontitis is an infection that destroys the soft tissues and bone supporting the teeth. If left untreated, the inflammatory process erodes the alveolar bone, leading to tooth mobility and eventually tooth loss, leaving behind a compromised bone structure.
- Trauma or Injury: Fractures to the jawbone, avulsed (knocked out) teeth, or severe blows to the face can cause immediate bone loss or damage that impairs future bone regeneration, necessitating grafting for implant placement.
- Long-Term Edentulism (Missing Teeth): If teeth have been missing for an extended period (years), the bone in that area will have significantly atrophied. The longer a tooth is absent, the more bone loss typically occurs, making implant placement progressively more challenging without a graft.
- Dentures or Bridges: While replacing missing teeth, traditional dentures and bridges do not stimulate the underlying jawbone. Over time, the pressure from dentures can even accelerate bone resorption.
- Infections: Chronic dental infections, such as those caused by abscesses or cysts, can destroy surrounding bone tissue.
- Systemic Conditions: Certain medical conditions like osteoporosis, Paget's disease, or metabolic disorders can affect bone density and healing capabilities, increasing the risk of bone loss.
- Developmental Defects: In rare cases, some individuals may have congenital conditions resulting in insufficient jawbone volume.
Signs and Symptoms of Insufficient Bone
Unlike many dental problems, insufficient jawbone for an implant often doesn't present with clear "signs and symptoms" that you can feel or see yourself until a professional examination. The bone loss happens silently and progressively. However, a dentist will typically identify this issue during a comprehensive implant assessment.
Here's what a dental professional will look for:
- Clinical Examination: The dentist may observe a noticeable indentation or concavity in the gum line where a tooth has been missing, indicating a loss of underlying bone volume.
- Radiographic Imaging: This is the primary diagnostic tool.
- Dental X-rays (Periapical, Panoramic): Provide a two-dimensional view of bone height and general density.
- Cone Beam Computed Tomography (CBCT) Scans: This is the gold standard for implant planning. A CBCT provides a detailed 3D image of your jawbone, allowing the dentist to accurately measure bone width, height, and density, identify vital structures (like nerves and sinuses), and determine precisely where a bone graft is needed.
- Palpation: The dentist may gently feel the jawbone through the gums to assess its contour and thickness.
If you have been missing teeth for a while, had a complicated extraction, or experienced advanced gum disease, it's highly probable that some degree of bone loss has occurred. This is why a thorough examination, including advanced imaging, is always performed before considering any dental implant procedure.
Treatment Options for Bone Deficiency (Bone Grafting Techniques)
While the focus here is bone grafting, it's essential to understand that the "treatment options" for bone deficiency are the specific types of bone grafts and techniques discussed earlier. There are generally no other viable long-term solutions for creating the biological environment necessary for conventional implant osseointegration if significant bone is missing.
When considering treatment for bone deficiency, your dentist will evaluate:
- Extent and Location of Bone Loss: A small, localized defect might be treated with socket preservation, while a widespread loss of height and width may require extensive ridge augmentation or a sinus lift.
- Quality of Remaining Bone: The density and health of your existing bone play a role in predicting graft success.
- Overall Health: Systemic conditions, medications, and habits like smoking can affect healing and graft success.
- Patient Preferences: Some patients may prefer to avoid autografts due to the second surgical site, opting for allograft or xenograft materials if appropriate.
In very rare and extreme cases where bone grafting is not feasible or desired, alternatives like zygomatic implants (which anchor into the cheekbone) or removable prosthetics might be considered. However, for most patients seeking fixed dental implants, bone grafting remains the most common and predictable solution for addressing bone deficiencies.
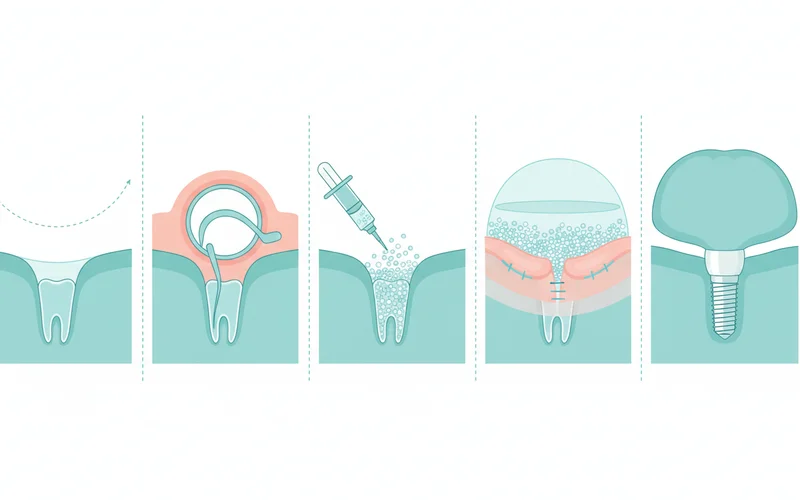
Step-by-Step Process for a Bone Graft for Implant
Understanding the journey helps to alleviate anxiety and sets realistic expectations. The process typically involves several stages:
-
Initial Consultation and Planning:
- Comprehensive Exam: Your dentist or oral surgeon will perform a thorough oral examination, take detailed medical and dental histories, and discuss your treatment goals.
- Diagnostic Imaging: This is crucial. CBCT scans (Cone Beam Computed Tomography) will be taken to create 3D images of your jawbone, precisely measuring bone volume, density, and identifying the location of vital structures like nerves and sinuses. This allows for precise planning of the graft type and implant placement.
- Treatment Plan Discussion: The dentist will explain the recommended bone grafting technique, the type of graft material, the anticipated timeline, costs, and potential risks and benefits.
-
The Bone Graft Surgery:
- Anesthesia: The procedure is typically performed under local anesthesia, often supplemented with oral or IV sedation to ensure your comfort. For extensive grafts, general anesthesia may be used.
- Preparation: The surgical site is numbed and sterilized.
- Incision: The dentist makes a small incision in your gum tissue to expose the underlying jawbone where the graft is needed.
- Graft Placement:
- For Socket Preservation: Graft material is gently packed into the empty tooth socket.
- For Ridge Augmentation: Graft material is carefully placed to rebuild the lost width or height of the bone. In some cases, a solid block of bone (autograft) may be secured with tiny screws.
- For Sinus Lift: A small window is created in the upper jawbone, the sinus membrane is gently lifted, and graft material is placed into the space.
- Membrane Placement (Optional but Common): A protective barrier membrane (often collagen-based) is frequently placed over the graft material. This membrane helps to stabilize the graft, prevent soft tissue from growing into the grafted area prematurely, and promote guided bone regeneration.
- Closure: The gum tissue is carefully sutured back into place, covering the graft site.
-
Healing and Osseointegration:
- This is the longest phase, typically lasting 3 to 9 months, sometimes longer for extensive grafts.
- During this time, the graft material acts as a scaffold, and your body's natural healing processes work to replace the graft with your own healthy bone. Blood vessels grow into the graft, and bone-forming cells (osteoblasts) begin to lay down new bone tissue.
- Regular follow-up appointments may be scheduled to monitor healing.
-
Dental Implant Placement:
- Once sufficient new bone has formed and matured, a second surgical procedure is performed to place the dental implant.
- Another small incision is made to expose the newly regenerated bone.
- A pilot hole is drilled, and the titanium implant post is carefully screwed into the bone.
- In some cases, a healing cap is placed immediately, allowing the gum tissue to heal around it. In others, the implant is covered by gum tissue and allowed to heal for another 3-6 months before being exposed for the final restoration.
- For a one tooth implant, this second stage is often straightforward once the bone graft has healed.
-
Prosthetic Restoration:
- After the implant has fully integrated with the bone (another 3-6 months), an impression is taken.
- A custom-made crown, bridge, or denture is fabricated to fit precisely onto the implant(s). This is where discussions about materials like a ceramic or even a gold tooth implant crown might occur, depending on aesthetic and functional preferences.
- The final restoration is then attached to the implant, completing the process and restoring your smile and chewing function.
Cost and Insurance for Bone Graft for Implant in the US
The cost of a bone graft for implant varies significantly based on the type of graft, the material used, the complexity of the procedure, the geographical location within the US, and the expertise of the dental professional (general dentist vs. oral surgeon vs. periodontist).
Average US Cost Ranges:
- Socket Preservation (Single Tooth): $200 - $600 (often less if performed immediately after extraction by the same dentist).
- Small Localized Graft (Minor Ridge Augmentation): $300 - $1,000.
- Moderate Ridge Augmentation: $700 - $2,000.
- Extensive Ridge Augmentation (Vertical or Large Horizontal): $1,500 - $3,500+.
- Sinus Lift Procedure:
- Crestal (Internal) Sinus Lift (Minor): $1,000 - $2,000 (often done concurrently with implant placement).
- Lateral (External) Sinus Lift (Major): $1,500 - $3,000+ per sinus.
- Autogenous Block Graft: This can be more expensive due to the need for a second surgical site, potentially adding $500 - $1,500 to the cost of the graft itself, not including hospital facility fees if harvested from the hip/tibia.
Additional Costs to Consider:
- Consultation & Imaging: CBCT scans can range from $150 - $450.
- Anesthesia/Sedation: Oral sedation $100 - $300, IV sedation $400 - $1,000+.
- Membranes: Resorbable membranes can add $100 - $400, non-resorbable slightly more.
- Post-operative medications: Antibiotics, pain relievers.
Insurance Coverage Details:
Dental insurance often categorizes bone grafting as a "major procedure" or "adjunctive procedure" to an implant. Coverage varies widely:
- Medical vs. Dental Insurance: Sometimes, if the bone loss is due to trauma or a medical condition (not just routine tooth extraction), your medical insurance might cover a portion of the bone graft, especially if performed by an oral surgeon. It's crucial to have your dental office submit a pre-determination to both dental and medical insurance.
- Dental Insurance:
- Many dental insurance plans cover 0% to 50% of bone grafting procedures.
- Socket preservation immediately following an extraction might have better coverage than extensive ridge augmentation performed years later.
- Some plans explicitly state that bone grafting for implant placement is not covered, as implants themselves are often considered cosmetic or elective.
- Coverage limits (annual maximums) are a significant factor. A complex graft could easily exceed a typical annual maximum of $1,000 - $2,000.
- ADA Codes: Your dental office will use specific ADA (American Dental Association) codes for billing. Examples include:
- D7953: Bone replacement graft for ridge preservation - per site.
- D7951: Sinus augmentation with bone or bone substitute - per sinus.
- D7950: Osseous, osteoperiosteal, or cartilage graft of the mandible or maxilla - autogenous or non-autogenous.
Pro Tip: Always request a pre-treatment estimate from your dental provider, which they can submit to your insurance companies. This will give you a clear understanding of what your out-of-pocket costs will be before committing to the procedure. Discuss payment plans or financing options with your provider.
Cost Comparison Table: Common Bone Graft Procedures (US Averages)
| Procedure Type | Average Cost Range (USD) | Typical Coverage by Dental Insurance | Healing Time Before Implant |
|---|---|---|---|
| Socket Preservation | $200 - $600 | 20-50% | 3-6 months |
| Small Ridge Augmentation | $300 - $1,000 | 0-30% | 4-7 months |
| Moderate Ridge Augmentation | $700 - $2,000 | 0-20% | 6-9 months |
| Lateral Sinus Lift | $1,500 - $3,000+ | 0-10% | 6-12 months |
| Crestal Sinus Lift | $1,000 - $2,000 | 0-10% | 4-8 months |
| Autogenous Block Graft | $1,500 - $3,500+ | 0-10% (often considered part of implant surgery not separately) | 6-9 months |
Recovery and Aftercare for a Bone Graft for Implant
Proper recovery and diligent aftercare are essential for the success of your bone graft. Following your dentist's instructions precisely will minimize complications and promote optimal healing and bone regeneration.
Immediate Post-Operative Period (First 24-72 hours):
- Bleeding: Some light bleeding or oozing from the surgical site is normal for the first 24-48 hours. Bite firmly on the gauze pads provided, replacing them every 30-45 minutes until bleeding subsides. Avoid spitting, rinsing vigorously, or using straws, as this can dislodge the blood clot and cause a dry socket.
- Swelling: Swelling is common and may peak on the second or third day. Apply ice packs to the outside of your face (15 minutes on, 15 minutes off) for the first 24-48 hours to help reduce swelling.
- Pain Management: You will likely experience some discomfort. Take prescribed pain medication as directed. Over-the-counter pain relievers like ibuprofen or acetaminophen can also be used as needed.
- Diet: Stick to soft, cool foods for the first few days (e.g., yogurt, smoothies, mashed potatoes, scrambled eggs). Avoid hot, spicy, crunchy, or chewy foods that could irritate the surgical site or dislodge the graft.
- Oral Hygiene:
- Do NOT rinse your mouth for the first 24 hours.
- After 24 hours, you may gently rinse with warm salt water (1/2 teaspoon salt in 8 ounces of warm water) 2-3 times a day, especially after meals. Do not swish vigorously; just let the water gently wash over the area.
- Avoid brushing directly on the surgical site for the first week. Brush other areas normally. Your dentist may prescribe an antimicrobial mouth rinse (e.g., chlorhexidine) for specific use.
- Activity: Rest and avoid strenuous physical activity for at least 48-72 hours. Elevated heart rate and blood pressure can increase bleeding and swelling.
Ongoing Care (Weeks to Months):
- Medications: Continue taking any prescribed antibiotics as directed to prevent infection, even if you feel fine.
- Smoking and Alcohol: ABSOLUTELY AVOID SMOKING AND ALCOHOL during the entire healing period. Smoking significantly impairs blood flow, hinders bone regeneration, and dramatically increases the risk of graft failure and complications. Alcohol can interfere with medications and dehydrate you.
- Diet: Gradually reintroduce normal foods as comfort allows, but continue to avoid chewing directly on the grafted area until instructed otherwise.
- Sutures: Some sutures are dissolvable and will disappear on their own. Non-dissolvable sutures will need to be removed by your dentist, usually 7-14 days after surgery.
- Membrane Considerations: If a non-resorbable membrane was used, it would need to be removed in a separate minor procedure, usually a few weeks after the graft. If a resorbable membrane was used, it will dissolve on its own.
- Avoid Pressure: Do not place any pressure on the grafted area, such as from ill-fitting dentures. Your dentist may modify or reline your existing denture or provide a temporary partial denture (flipper) that avoids the surgical site.
- Follow-Up Appointments: Attend all scheduled follow-up appointments with your dentist or oral surgeon. These are critical for monitoring healing progress and ensuring the graft is integrating properly.
- Patience: Bone grafting takes time. The full maturation of new bone can take several months. Rushing the implant placement can jeopardize the entire process. Adhere strictly to the recommended healing period before proceeding with implant surgery.
Prevention of Bone Loss
Preventing bone loss is always preferable to treating it. Proactive measures can significantly reduce the likelihood of needing a bone graft for implant placement.
- Prompt Replacement of Missing Teeth: The most effective way to prevent bone loss after an extraction is to replace the tooth promptly.
- Immediate Implant Placement: In some cases, a dental implant can be placed at the same time the tooth is extracted. This preserves the bone and often reduces overall treatment time.
- Socket Preservation: If immediate implant placement isn't possible, a socket preservation procedure (as described earlier) is highly recommended. By placing graft material into the empty socket, it helps to maintain the bone's width and height, making future implant placement much easier and more predictable.
- Effective Management of Periodontal Disease: Regular dental check-ups, professional cleanings, and diligent home oral hygiene (brushing twice daily, flossing daily) are crucial for preventing and managing gum disease. If diagnosed, follow your dentist's treatment plan rigorously to stop the progression of bone-destroying infection.
- Good Oral Hygiene: Consistent brushing and flossing help prevent cavities and gum disease, which are major contributors to tooth loss and subsequent bone atrophy.
- Protective Gear for Trauma: If you participate in contact sports, wear a custom-fitted mouthguard to protect your teeth and jaws from injury.
- Address Bruxism (Teeth Grinding): Chronic teeth grinding can put excessive stress on teeth and bone, potentially contributing to bone loss. Your dentist may recommend a nightguard to protect your teeth.
- Balanced Diet and Healthy Lifestyle: A diet rich in calcium and vitamin D supports overall bone health. Avoid smoking, as it severely compromises bone density and healing capabilities throughout the body, including the jaw.
- Regular Dental Check-ups: Visiting your dentist every six months allows for early detection and intervention for any issues that could lead to bone loss.
Risks and Complications of Bone Graft for Implant
While bone grafting is a highly successful and safe procedure, as with any surgery, there are potential risks and complications. It's important to be aware of these to make an informed decision and to know when to contact your dental professional.
- Infection: This is the most common complication. Signs include persistent pain, swelling, pus, fever, and redness around the surgical site. Infection can compromise graft integration and lead to graft failure.
- Graft Failure/Non-Integration: The graft material may not successfully integrate with your existing bone or stimulate new bone growth. This can occur due to infection, insufficient blood supply, smoking, certain systemic conditions, or premature pressure on the graft. If the graft fails, it may need to be removed, and another attempt might be necessary after a healing period.
- Bleeding: While some oozing is normal, excessive or prolonged bleeding can occur.
- Swelling and Bruising: Expected post-operatively, but severe or persistent swelling should be monitored.
- Pain and Discomfort: Manageable with medication, but severe or worsening pain requires attention.
- Nerve Damage (Paresthesia/Dysesthesia): Rare, but possible, especially in the lower jaw where the inferior alveolar nerve runs. This can result in temporary or, very rarely, permanent numbness, tingling, or altered sensation in the lip, chin, or tongue.
- Sinus Perforation (during Sinus Lift): A rare complication where the sinus membrane is torn during a sinus lift. Small perforations can often be repaired during surgery. Larger tears may require delaying the graft or implant.
- Graft Exposure: The covering membrane or graft material can become exposed through the gum tissue, increasing the risk of infection and graft failure. This may require further surgical intervention to re-cover the site or remove exposed material.
- Resorption of Graft Material: While some resorption is normal as your body replaces the graft with its own bone, excessive resorption can lead to insufficient bone for the implant.
- Donor Site Complications (for Autografts): Pain, swelling, infection, or nerve damage at the site where your own bone was harvested.
When to Contact Your Dentist Immediately:
- Severe or worsening pain that is not controlled by medication.
- Persistent or heavy bleeding beyond the first 48 hours.
- Signs of infection: fever, pus, severe swelling, spreading redness.
- Numbness or tingling that persists beyond the expected local anesthetic effects.
- Sudden increase in swelling after the initial 2-3 days.
- Graft material or membrane becoming visible or feeling loose.
Children / Pediatric Considerations
Dental implants, and consequently bone grafts for implant placement, are generally not recommended for children or adolescents whose jawbones are still growing and developing. Placing an implant in a growing jaw can lead to complications such as the implant submerging into the bone, causing adjacent teeth to tilt, or disrupting the natural growth pattern of the jaw.
The general guideline is to wait until jaw growth is complete, which typically occurs around 18-20 years of age for females and 20-25 years of age for males, though this can vary.
If a child loses a permanent tooth due to trauma or other reasons, the focus shifts to temporary solutions to maintain space and aesthetics until adulthood. Options may include:
- Space maintainers: To prevent adjacent teeth from drifting into the gap.
- Removable partial dentures (flippers): To restore aesthetics and some chewing function.
- Orthodontic treatment: To manage space and alignment.
In rare cases of severe trauma or developmental defects in children, a bone graft might be considered for reconstructive purposes independent of implant placement, but this would be a highly specialized decision made by an oral surgeon in conjunction with a multidisciplinary team. For the purpose of dental implants, however, it is standard practice to delay any bone grafting or implant placement until skeletal maturity is reached.
Frequently Asked Questions
How long does a bone graft take to heal before implant placement?
Healing time for a bone graft typically ranges from 3 to 9 months. Simpler grafts like socket preservation usually heal faster (3-6 months), while more extensive procedures like large ridge augmentations or sinus lifts can take 6-9 months or even up to a year to fully mature before the dental implant can be safely placed. Your body needs sufficient time to integrate the graft material and regenerate strong, natural bone.
Is a bone graft painful?
During the procedure, you will be comfortably numb due to local anesthesia, often supplemented with sedation. Post-operatively, you will experience some discomfort, swelling, and bruising, which can be managed with prescribed pain medication and over-the-counter anti-inflammatories. Most patients report manageable pain, but individual tolerance varies.
What are the alternatives to a bone graft for implant?
If a bone graft isn't suitable or desired, alternatives are limited. Smaller or shorter implants might be used if only minor bone deficiency exists. In the upper jaw, zygomatic implants anchor into the cheekbone, bypassing the need for a sinus lift. However, these are specialized procedures. The most common alternative is a traditional removable partial denture or a fixed dental bridge that relies on adjacent teeth for support, though these do not prevent ongoing bone loss.
Can a dental implant be placed without a bone graft if there's bone loss?
Generally, no. A minimum amount of healthy, dense bone is absolutely essential for the successful osseointegration and long-term stability of a dental implant. Attempting to place an implant into insufficient bone dramatically increases the risk of implant failure, poor stability, and complications. A bone graft provides the necessary foundation.
How successful are bone grafts for implants?
When performed by experienced professionals and with proper patient adherence to aftercare, bone grafts for dental implants have a very high success rate, often exceeding 95%. This success significantly contributes to the high success rates of dental implants themselves, which are consistently above 90-95%.
Will my insurance cover a gold tooth implant crown?
While dental insurance often covers a portion of standard crowns, coverage for premium materials like a gold tooth implant crown can vary significantly. Some plans may cover the cost up to that of a basic porcelain or metal crown, requiring you to pay the difference for gold. Others may not cover gold at all due to its higher cost. Always check with your insurance provider and discuss material options with your dentist.
Can I get a one tooth implant immediately after extraction?
Yes, in some cases, a one tooth implant can be placed immediately after extraction. This is called immediate implant placement. It is ideal when there is no infection, sufficient healthy bone, and excellent primary stability can be achieved. However, if there's significant bone damage or infection, a bone graft (like socket preservation) may be done first, with implant placement delayed by a few months.
What is the typical recovery timeline?
Initial recovery from the bone graft surgery itself takes about 1-2 weeks for swelling and discomfort to subside. The critical bone regeneration phase, where the graft integrates and new bone forms, takes 3 to 9 months. After this, the implant is placed, and another 3-6 months are needed for implant osseointegration. The entire process from graft to final crown can take 6-18 months.
How do I know if my bone graft is failing?
Signs of a failing bone graft include persistent or worsening pain, significant swelling that doesn't subside, pus or discharge from the surgical site, fever, numbness, or if the graft material becomes exposed and loose. If you experience any of these symptoms, contact your dental professional immediately.
Is a bone graft always necessary for dental implants?
No, a bone graft is not always necessary. If you have sufficient natural bone volume and density in your jaw, you may proceed directly to implant placement. However, it's very common to need some form of bone augmentation, especially if teeth have been missing for a while, after a complicated extraction, or due to gum disease. Your dental professional will determine your specific needs with advanced imaging.
When to See a Dentist
It is crucial to see a dentist promptly if you are considering dental implants or have concerns about bone loss.
Immediate Attention (Red Flags):
- After a Bone Graft Procedure:
- Uncontrolled bleeding: If biting on gauze for an hour doesn't stop heavy bleeding.
- Signs of infection: Fever, severe or increasing pain, significant swelling that re-emerges days after surgery, pus or foul taste.
- Numbness or tingling that persists hours after the local anesthetic should have worn off.
- Sudden onset of severe pain or swelling days after the initial recovery period.
- Graft material becomes visible or dislodged.
- After Tooth Loss or Injury:
- If you experience trauma that results in a knocked-out tooth or a jaw injury.
- If you've had a tooth extracted and notice unusual pain, swelling, or signs of infection in the socket.
Scheduled Appointments (Routine Care and Planning):
- If you have one or more missing teeth: Even if you've been missing teeth for years, a consultation is essential to assess your current bone structure and discuss options like a bone graft for implant.
- If you are considering dental implants: A comprehensive evaluation, including CBCT scans, is required to determine if you have adequate bone for implant placement.
- If you have ongoing gum disease: Early treatment of periodontal disease can prevent further bone loss.
- Before a tooth extraction: Discussing socket preservation with your dentist before an extraction is a proactive step to prevent future bone loss and potentially simplify future implant placement.
Don't wait until complications arise. Regular dental check-ups and prompt attention to any dental concerns are the best ways to maintain your oral health and ensure successful outcomes for any necessary treatments, including bone grafting for dental implants.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
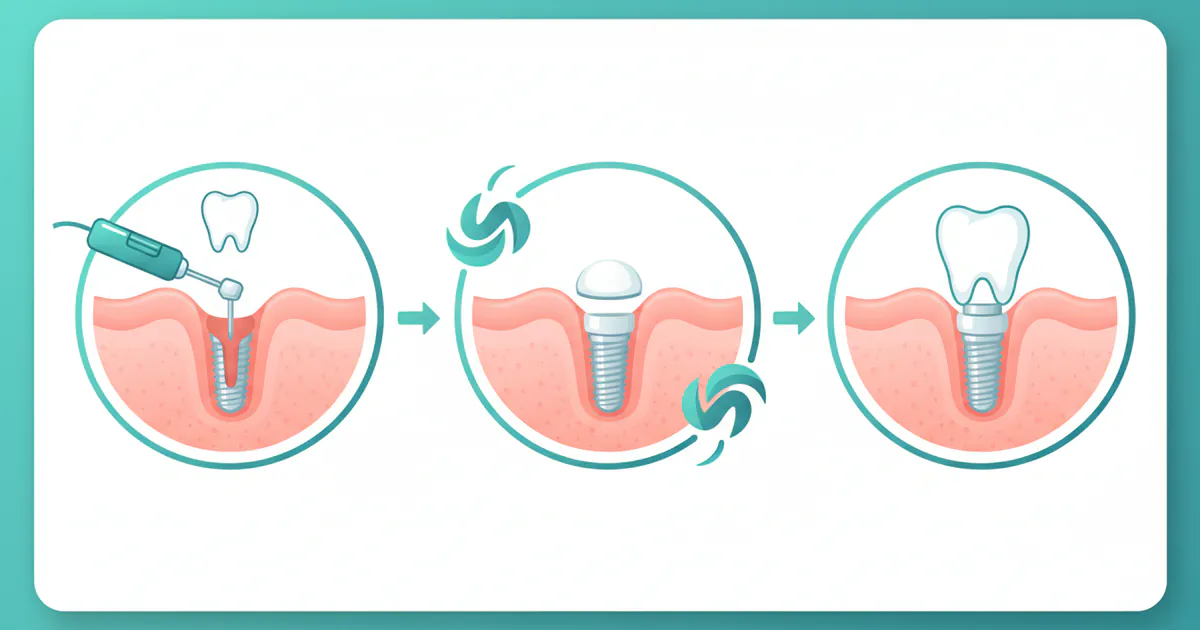
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026