Tooth Whitening
4,562 words · 15 min read
Quick Definition
Cosmetic procedures that lighten tooth color by removing stains and discoloration, using peroxide-based bleaching agents or surface-level polishing techniques.
Tooth Whitening
Short Definition: Cosmetic procedures that lighten tooth color by removing stains and discoloration, using peroxide-based bleaching agents or surface-level polishing techniques.
Introduction
Tooth whitening, also commonly referred to as tooth bleaching, is a popular cosmetic dental procedure designed to lighten the shade of your teeth and improve the overall aesthetics of your smile. It involves breaking down stains on the enamel and dentin layers of the tooth, resulting in a brighter appearance. This quest for a radiant smile is incredibly common in the United States; surveys consistently show that over 80% of Americans desire whiter teeth, and tooth whitening remains one of the most frequently requested cosmetic dental treatments. Its importance extends beyond mere aesthetics, often boosting self-confidence and positively impacting social and professional interactions. While widely accessible through various methods, understanding the science, safety, and suitability of tooth whitening is crucial for achieving desired results while safeguarding your long-term oral health. This comprehensive guide will delve into everything you need to know about "tooth whitening dental" procedures and what truly constitutes "what is tooth whitening."
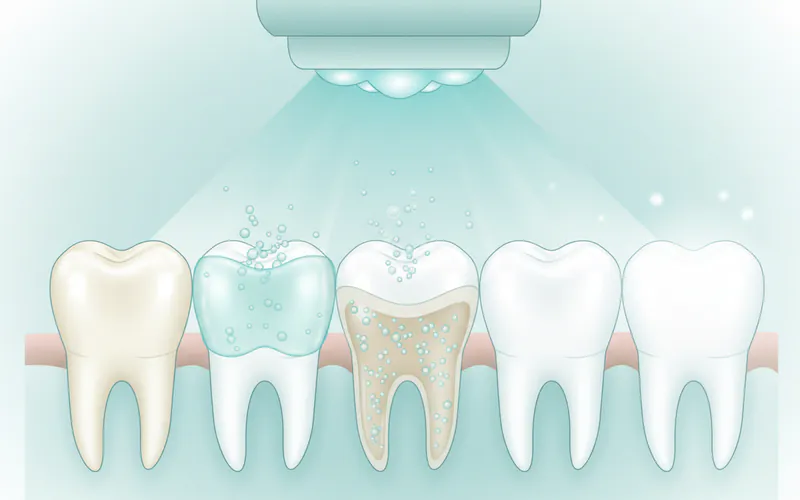
Key Takeaways:
- Tooth whitening lightens tooth color by breaking down stains, primarily using peroxide-based agents.
- It is a highly popular cosmetic procedure, with a significant majority of Americans seeking whiter teeth.
- Results vary based on the type of staining, product used, and individual tooth structure.
- Professional dental consultation is recommended before starting any whitening regimen to ensure safety and efficacy.
- Common side effects include temporary tooth sensitivity and gum irritation.
- Whitening is generally not permanent and requires maintenance to preserve results.
Detailed Explanation
Tooth whitening is a broad term encompassing various techniques aimed at achieving a brighter smile. The effectiveness and safety of these methods depend heavily on the underlying cause of discoloration, the health of your teeth and gums, and the active ingredients used.
Types and Classifications
Tooth discoloration typically falls into two main categories:
-
Extrinsic Stains: These are surface stains that accumulate on the enamel – the outermost layer of your teeth. They are primarily caused by exposure to certain foods, beverages, and lifestyle habits.
- Causes: Coffee, tea, red wine, dark sodas, berries, soy sauce, tobacco use (smoking, chewing).
- Treatment: Often responsive to surface polishing (e.g., during a dental cleaning) and over-the-counter whitening toothpastes or rinses, as well as professional bleaching.
-
Intrinsic Stains: These stains are deeper, embedded within the dentin (the layer beneath the enamel) or even the enamel itself. They can be more challenging to remove and often require more intensive bleaching or alternative cosmetic solutions like veneers.
- Causes:
- Aging: As we age, enamel thins, allowing the naturally yellowish dentin to show through more.
- Trauma: An injury to a tooth can cause internal bleeding and discoloration.
- Medications: Certain antibiotics (e.g., tetracycline taken during tooth development) can cause severe intrinsic staining.
- Excessive Fluoride (Fluorosis): High fluoride intake during tooth formation can lead to white or brown spots.
- Dental Restorations: Old amalgam (silver) fillings can leach metallic ions into the tooth structure, causing gray or blue discoloration.
- Genetics: Some individuals naturally have darker or yellower tooth shades.
- Causes:
Based on these classifications and the methods used, tooth whitening can be further categorized:
-
Bleaching: This is the most common and effective form of tooth whitening, using peroxide-based agents (hydrogen peroxide or carbamide peroxide) to penetrate the enamel and break down intrinsic and extrinsic stains.
- In-Office (Chairside) Whitening: Performed by a dentist, using high-concentration peroxide gels, often activated by a special light or laser. This provides the fastest and most dramatic results.
- At-Home Professional Whitening: Prescribed by a dentist, involving custom-fitted trays and professional-strength peroxide gel used daily for several weeks.
- Over-the-Counter (OTC) Whitening: Widely available products like strips, gels, toothpastes, and rinses with lower concentrations of peroxide.
-
Non-Bleaching Whitening: These methods primarily focus on removing extrinsic surface stains.
- Whitening Toothpastes and Rinses: Contain mild abrasives or chemical agents (like blue covarine) to polish surfaces or create an optical illusion of whiter teeth. They do not change the intrinsic color of the tooth.
- Dental Cleanings: Professional scaling and polishing remove plaque, tartar, and extrinsic stains, naturally brightening the teeth.
Causes and Risk Factors for Tooth Discoloration
Understanding the causes of tooth discoloration is crucial for effective whitening and prevention.
- Dietary Habits: Frequent consumption of highly pigmented foods and drinks like coffee, tea, red wine, dark berries, colas, and sauces (e.g., soy sauce, balsamic vinegar) is a primary contributor to extrinsic staining. The chromogens (color compounds) in these items adhere to the enamel surface.
- Tobacco Use: Both smoking and chewing tobacco are major culprits for severe extrinsic yellow and brown stains due to tar and nicotine.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque and tartar to accumulate, which can absorb stains and make teeth appear dull or discolored.
- Aging: As individuals age, the outer layer of enamel naturally thins, revealing more of the yellowish dentin beneath. Additionally, decades of exposure to staining agents contribute to cumulative discoloration.
- Trauma to the Tooth: A blow or injury to a tooth can damage the pulp (nerve and blood vessels), leading to internal bleeding and a grayish or brownish intrinsic discoloration over time.
- Certain Medications:
- Tetracycline and Doxycycline: If taken by pregnant women or children under 8 years old during tooth development, these antibiotics can cause permanent gray, blue, or brownish intrinsic staining.
- Antihistamines, Antipsychotics, and High Blood Pressure Medications: Some of these can contribute to tooth discoloration.
- Chlorhexidine: An antibacterial mouthwash sometimes prescribed by dentists, can cause temporary brown extrinsic staining.
- Excessive Fluoride Exposure (Fluorosis): Over-ingestion of fluoride during tooth formation (typically before age 8) can result in chalky white spots, streaks, or, in severe cases, brown pits and stains on the enamel.
- Genetic Factors: Tooth color is partly genetic. Some people naturally have brighter, whiter enamel, while others have a yellower or grayer natural shade.
- Dental Materials: Old silver amalgam fillings can corrode over time and leach metallic ions into the surrounding tooth structure, causing a grayish hue. Composite resin fillings can also stain over time.
- Medical Conditions: Certain rare medical conditions and treatments (e.g., chemotherapy, radiation to the head and neck) can affect tooth development and color.
Signs and Symptoms to Watch For
The primary "symptom" of discoloration is simply a change in the aesthetic appearance of your teeth. However, it's important to differentiate between superficial stains and underlying issues.
- Visible Discoloration: Your teeth appear yellower, browner, grayer, or have noticeable spots compared to their original shade or your desired shade.
- Uneven Coloration: Some teeth are darker than others, which could indicate a devitalized (dead) tooth due to trauma or infection.
- Sensitivity (post-whitening): While not a sign of discoloration, it's a common temporary symptom after tooth whitening, indicating the whitening agent has affected the pulp.
- Gum Irritation (post-whitening): Redness or soreness of the gums can occur if the whitening gel comes into contact with soft tissues.
If you notice sudden, significant discoloration, especially in a single tooth, accompanied by pain or swelling, it's crucial to consult your dentist immediately, as this could indicate a serious underlying problem.
Diagnosis Process — What Your Dentist Does
Before recommending any tooth whitening procedure, a thorough dental examination is essential. This diagnostic process ensures that whitening is appropriate, safe, and will yield satisfactory results.
- Comprehensive Oral Exam: Your dentist will first assess the overall health of your teeth and gums. This includes checking for cavities, gum disease, exposed roots, cracked teeth, or existing dental restorations (fillings, crowns, veneers). Whitening agents can irritate these issues or cause uneven results.
- Shade Assessment: Using a dental shade guide, your dentist will determine your current tooth shade. This provides a baseline and helps set realistic expectations for the outcome.
- Identification of Discoloration Type: Your dentist will identify whether your stains are extrinsic (surface) or intrinsic (internal). This is crucial because intrinsic stains from tetracycline or fluorosis are much harder to treat with conventional whitening and might require alternative solutions like bonding or veneers.
- Review of Medical History: They will ask about any medications you are taking, allergies, and existing medical conditions, as these can influence the safety and effectiveness of whitening.
- Discussion of Expectations and Realistic Outcomes: Your dentist will discuss how many shades lighter you can realistically expect your teeth to get, as well as the potential side effects and maintenance required. For example, teeth do not whiten beyond their natural maximum lightness, and restorations like fillings and crowns will not whiten and may need replacement to match newly whitened teeth.
- Pre-Whitening Treatment (if necessary): Before whitening, a professional dental cleaning is often recommended to remove plaque, tartar, and extrinsic surface stains, allowing the whitening agent to work more effectively and evenly. Any cavities or gum disease should also be treated beforehand.
Treatment Options with Pros, Cons, and Costs
The choice of tooth whitening treatment depends on your budget, desired speed of results, and the type of discoloration.
| Treatment Option | Description | Pros | Cons | Estimated Cost (US) |
|---|---|---|---|---|
| In-Office (Chairside) Whitening | Performed by a dentist in one or more appointments (typically 1-2 hours per session). Uses high-concentration hydrogen peroxide gels (15-40%) often activated by a special light (LED, laser, UV) to accelerate the bleaching process. Gums are protected with a barrier. | - Fastest, most dramatic results: Can lighten teeth by several shades in a single visit. - Professional supervision: Safest option as a dentist monitors for sensitivity and gum irritation. - Effective for stubborn stains: Higher concentration gels provide superior results. - Long-lasting: Results typically last 1-3 years with proper maintenance. |
- Most expensive upfront. - Can cause temporary but significant tooth sensitivity. - Gum irritation if gel contacts soft tissue. - Not always effective for severe intrinsic stains (e.g., tetracycline). - Requires dental visits. |
$400 - $1,000+ per session (insurance rarely covers cosmetic procedures). |
| At-Home Professional Whitening | Dentist provides custom-fitted trays (made from impressions of your teeth) and professional-strength carbamide peroxide gel (10-35%) or hydrogen peroxide gel (3-15%). Used daily for 30 minutes to a few hours or overnight, typically for 1-2 weeks. | - Effective results: Significant whitening over time. - Convenient: Used at home on your own schedule. - Custom trays: Ensure even gel distribution and minimize gum exposure, leading to less irritation than OTC products. - More affordable than in-office. - Trays can be reused for touch-ups. |
- Slower results than in-office whitening. - Requires discipline and consistent use. - Can cause temporary tooth sensitivity and gum irritation if trays are overfilled or worn too long. - Still requires an initial dental visit for impressions. |
$200 - $600 (insurance rarely covers). |
| Over-the-Counter (OTC) Products | Widely available at drugstores. Includes whitening strips, brush-on gels, whitening toothpastes, rinses, and trays (boil-and-bite). Contain lower concentrations of peroxide (3-10% hydrogen peroxide or 10-22% carbamide peroxide). | - Most affordable option. - Easily accessible: No dental visit required. - Can provide noticeable results for mild extrinsic stains. |
- Less effective than professional options, especially for intrinsic stains. - Ill-fitting trays or strips can lead to uneven whitening and significant gum irritation. - Higher risk of misuse and potential damage if not used correctly. - Results are often less dramatic and may not last as long. - Whitening toothpastes/rinses primarily remove surface stains, providing minimal actual bleaching. |
$20 - $100 (depends on product type and brand). |
| Non-Peroxide Whitening | Products that use ingredients like blue covarine (optical brighteners in some toothpastes) or surface abrasives (in many whitening toothpastes) to physically remove surface stains or create an optical illusion of whiter teeth. | - Can help remove extrinsic stains caused by food/drink. - Some provide an immediate, temporary optical brightening effect. - Generally safe for daily use. |
- Do not truly whiten teeth by changing intrinsic tooth color. - Only effective for extrinsic stains. - Abrasive toothpastes can cause enamel wear over long-term use if used too aggressively. |
$5 - $20 for toothpaste/rinse. |
| Veneers | Thin, custom-made shells of tooth-colored materials (porcelain or composite resin) that are bonded to the front surface of teeth. Used for severe intrinsic staining, chips, gaps, or misshapen teeth that cannot be whitened effectively. | - Excellent for severe intrinsic stains that don't respond to bleaching. - Provides a complete smile makeover. - Durable and long-lasting (10-15+ years for porcelain). - Resistant to future staining. - Can correct multiple cosmetic issues beyond just color. |
- Irreversible (some natural enamel must be removed). - Significantly more expensive than whitening. - Requires multiple dental visits. - Cannot be whitened in the future; if surrounding natural teeth stain, veneers may no longer match. - Potential for chipping or debonding. |
$900 - $2,500+ per tooth (porcelain); $250 - $1,500+ per tooth (composite). |
Step-by-Step: What to Expect During Treatment
1. Professional In-Office Whitening:
- Initial Consultation: As described in the diagnosis section, your dentist will examine your teeth, discuss your goals, and ensure you're a good candidate.
- Preparation: Your teeth will be professionally cleaned. Your lips and gums will be covered with a protective barrier (often a liquid dam or resin) to prevent the high-concentration bleaching gel from irritating soft tissues. A retractor is used to keep your mouth open.
- Gel Application: The high-concentration hydrogen peroxide gel is carefully applied to the front surfaces of your teeth.
- Activation (Optional): Many in-office systems use a special light (LED, laser, or UV lamp) to accelerate the chemical reaction of the gel. While studies show the light itself doesn't whiten teeth, it can speed up the process.
- Waiting Period: The gel remains on your teeth for 15-20 minutes per application, often with 2-4 applications in a single session.
- Rinse and Repeat: After each application, the old gel is suctioned off, the teeth are rinsed, and a new layer of gel is applied.
- Post-Treatment: After the final application, all protective barriers are removed. Your dentist will rinse your mouth and assess the initial results. A fluoride treatment may be applied to help reduce sensitivity.
- Instructions: You'll receive aftercare instructions, including avoiding staining foods/drinks for the first 24-48 hours (the "white diet").
2. Professional At-Home Whitening:
- Initial Consultation: Similar to in-office, your dentist will examine your oral health and discuss expectations.
- Impressions: Impressions of your upper and lower teeth are taken to create custom-fitted plastic trays in a dental lab. This usually takes a few days.
- Tray Delivery & Instructions: You return to the dental office to pick up your custom trays and the professional-strength whitening gel. Your dentist will demonstrate how to apply a small amount of gel into the trays and how to properly seat them on your teeth.
- Home Use: You will typically wear the trays for a specified duration each day (e.g., 30 minutes to a few hours, or overnight) for 1-2 weeks, depending on the gel concentration and desired results.
- Monitoring: Your dentist may schedule a follow-up appointment to check your progress and address any sensitivity.
- Maintenance: Keep your custom trays for future touch-ups.
3. Over-the-Counter Products:
- Read Instructions Carefully: Adhere strictly to the manufacturer's guidelines for application time and frequency.
- Preparation: Brush and floss your teeth thoroughly before application.
- Application:
- Strips: Apply the gel-coated strips directly to the front teeth, pressing firmly for good contact.
- Brush-on Gels: Apply a thin layer directly to the tooth surfaces with a brush.
- Boil-and-Bite Trays: Mold the tray to your teeth by softening it in hot water and biting down, then add gel and wear as directed.
- Duration: Leave on for the recommended time (e.g., 30 minutes for strips, 5 minutes for rinses).
- Rinse: Rinse your mouth after use.
- Consistency: OTC products require consistent, daily use over several weeks to see noticeable results.
Recovery Timeline and Aftercare
Regardless of the method, proper aftercare is crucial for maximizing results and minimizing side effects.
-
Immediate Post-Whitening (First 24-48 hours):
- Sensitivity: This is the most common side effect. Teeth may feel sensitive to hot, cold, or air. It's usually temporary and subsides within a day or two. Using a desensitizing toothpaste (containing potassium nitrate or strontium chloride) can help. Your dentist might also prescribe a fluoride varnish or gel.
- "White Diet": Avoid all staining foods and beverages (coffee, tea, red wine, dark sodas, berries, ketchup, mustard, tobacco) for at least 24-48 hours as your teeth are highly porous and susceptible to re-staining immediately after whitening.
- Gum Irritation: If whitening gel contacted your gums, they might appear white or irritated initially, but this typically resolves within a few hours.
-
Long-Term Maintenance:
- Oral Hygiene: Maintain excellent oral hygiene: brush twice daily, floss daily.
- Regular Dental Cleanings: Schedule professional cleanings every 6 months to remove new extrinsic stains.
- Touch-Ups: Whitening is not permanent. Results typically last 6 months to 3 years depending on the method and your habits. You may need touch-up treatments, especially if you consume staining foods/drinks regularly. For professional at-home kits, you can reuse your custom trays with new gel.
- Avoid Re-Staining: Reduce consumption of highly staining foods and drinks, or rinse your mouth with water immediately after consuming them. If you smoke, quitting will significantly prolong your whitening results.
- Straw Use: Using a straw for staining beverages can help minimize contact with your front teeth.
Prevention Strategies
Preventing tooth discoloration involves maintaining good oral hygiene and making conscious lifestyle choices.
- Practice Excellent Oral Hygiene: Brush your teeth for two minutes, twice a day, and floss daily to remove plaque, food debris, and surface stains. Consider using an electric toothbrush for more effective cleaning.
- Regular Dental Cleanings: Visit your dentist for professional cleanings and check-ups every 6 months. Dental hygienists are adept at removing extrinsic stains that accumulate over time.
- Mind Your Diet: Limit consumption of known staining agents like coffee, tea, red wine, dark sodas, dark berries, and highly pigmented sauces. If you do consume them, rinse your mouth with water afterward or brush your teeth (wait 30 minutes after acidic foods/drinks to prevent enamel erosion).
- Quit Tobacco: Smoking and chewing tobacco are major contributors to severe tooth discoloration and numerous oral health problems. Quitting is the single most effective way to prevent tobacco-related stains.
- Use a Straw: When drinking staining beverages, using a straw can help bypass direct contact with the front surfaces of your teeth.
- Stay Hydrated: Drinking water throughout the day helps wash away food particles and acids, reducing the potential for staining and decay.
- Consider Whitening Toothpastes (with caution): While they don't truly bleach, some whitening toothpastes contain mild abrasives or chemical stain removers that can help remove new surface stains. Use them as directed, as overuse of highly abrasive toothpastes can potentially wear down enamel.
Cost Ranges in the US (with/without insurance)
The cost of tooth whitening in the US varies significantly based on the method chosen and geographical location.
- In-Office Professional Whitening: Expect to pay between $400 and $1,000+ per session. Many individuals opt for one session and then maintain with at-home products. Some severe cases might require two sessions.
- Professional At-Home Whitening Kits (Custom Trays): These typically range from $200 to $600. This includes the dental visit, impressions, custom trays, and several tubes of professional-strength gel. Replacement gel syringes are usually much cheaper, around $20-$50 each.
- Over-the-Counter Products:
- Whitening Strips: $20 - $50 per box.
- Whitening Toothpastes/Rinses: $5 - $20.
- Boil-and-Bite Trays with Gel: $30 - $80.
Insurance Coverage: It is important to understand that dental insurance typically does NOT cover cosmetic procedures, including tooth whitening. Since the primary purpose of whitening is aesthetic improvement rather than treating a medical condition, it's considered an elective procedure. You will almost certainly be responsible for the full out-of-pocket cost. Some dentists offer payment plans or financing options.
For Parents / Pediatric Considerations
Tooth whitening is generally not recommended for children and adolescents. There are several important reasons for this:
- Developing Teeth: Children's teeth (both primary/baby teeth and newly erupted permanent teeth) have larger pulp chambers and thinner enamel compared to adult teeth. This makes them more susceptible to sensitivity and potential damage from whitening agents.
- Unnecessary: Most discoloration in children is extrinsic (surface stains) from diet or poor hygiene, which can typically be resolved with improved brushing and regular professional dental cleanings.
- Unknown Long-Term Effects: The long-term effects of bleaching agents on developing teeth are not fully understood.
- Uneven Results: If a child still has a mix of primary and permanent teeth, whitening would result in uneven tooth color as only the permanent teeth would be whitened, and the baby teeth would retain their original shade. Fillings or crowns on baby teeth also won't whiten.
- Compliance: Younger children may not be able to follow instructions for at-home whitening trays, increasing the risk of misuse and gum irritation.
When it might be considered (rarely): In very rare cases, severe intrinsic staining in an adolescent (e.g., from tetracycline or fluorosis) might lead a dentist to discuss highly supervised, low-concentration whitening as an option, but only after careful consideration and usually not before the permanent teeth are fully developed and roots are closed (typically around 14-16 years old). More often, bonding or veneers might be considered for such cases in adulthood. Parents concerned about their child's tooth color should always consult a pediatric dentist.
Frequently Asked Questions
How much does tooth whitening cost?
The cost varies widely based on the method. Over-the-counter products range from $20-$100. Professional at-home kits prescribed by a dentist typically cost $200-$600. In-office professional whitening is the most expensive, usually between $400-$1,000+ per session. Dental insurance typically does not cover cosmetic tooth whitening procedures.
How painful is tooth whitening?
Tooth whitening is generally not painful, but temporary tooth sensitivity is a common side effect, especially with professional-strength treatments. This sensitivity can range from mild to moderate and is usually characterized by sharp, fleeting pains in response to hot, cold, or air. It typically subsides within 24-48 hours after treatment. Your dentist can provide desensitizing toothpaste or gels to help manage this discomfort. Gum irritation can also occur if the whitening gel contacts the soft tissues, but this is also usually temporary.
How long do tooth whitening results last?
The duration of tooth whitening results varies significantly. In-office professional whitening can last 1-3 years, while professional at-home kits may last 6 months to 2 years. Over-the-counter products often provide shorter-lived results, typically a few months. Factors like your diet (consumption of staining foods/drinks), tobacco use, and oral hygiene habits heavily influence how long your teeth stay white. Regular touch-ups and good oral hygiene are essential for maintaining a bright smile.
What are the alternatives to tooth whitening for discolored teeth?
If tooth whitening isn't suitable or effective for your specific type of discoloration, or if you have other cosmetic concerns, several alternatives exist. These include:
- Dental Bonding: A tooth-colored resin material is applied to the tooth and bonded with a special light, ideal for minor chips, gaps, or small areas of discoloration.
- Dental Veneers: Thin, custom-made shells (often porcelain or composite) are bonded to the front surface of teeth to cover severe discoloration, chips, or reshape teeth for a complete smile makeover.
- Crowns: If a tooth is severely damaged, discolored, or weakened, a full dental crown might be necessary, covering the entire visible portion of the tooth.
- Internal Bleaching: For a single tooth that has discolored internally due to trauma or root canal treatment, a special whitening agent can be placed inside the tooth.
Will tooth whitening damage my enamel?
When performed correctly under professional guidance, tooth whitening using peroxide-based agents does not permanently damage your tooth enamel. The active ingredients penetrate the enamel to break down stain molecules, but they do not alter or remove the structure of the enamel itself. Overuse or misuse of highly acidic or abrasive whitening products, particularly over-the-counter options, can potentially lead to enamel erosion or increased sensitivity, which is why professional consultation is always recommended.
Does dental insurance cover tooth whitening?
No, dental insurance typically does not cover tooth whitening. As it is considered an elective cosmetic procedure rather than a medically necessary treatment, the cost is almost always entirely out-of-pocket for the patient. You should confirm this with your specific insurance provider, but it is a general rule across most plans in the US.
Can tooth whitening whiten dental restorations like fillings or crowns?
No, tooth whitening agents only work on natural tooth structure. Existing dental restorations such as composite fillings, porcelain crowns, veneers, or bonding will not change color during the whitening process. This is an important consideration, as whitened natural teeth may then appear mismatched with existing restorations. If you plan to whiten your teeth and have visible restorations, you may need to consider replacing them after whitening to achieve a uniform color.
Is teeth whitening safe?
Yes, when used as directed and preferably under the supervision of a dental professional, teeth whitening is considered safe. The most common side effects are temporary tooth sensitivity and gum irritation, which typically resolve shortly after treatment. Your dentist can help determine if you are a good candidate for whitening, recommend the safest and most effective method for your specific situation, and monitor for any adverse reactions.
When to See a Dentist
While many over-the-counter whitening options are available, consulting a dentist is always recommended before starting any whitening regimen.
See your dentist for routine care related to whitening if:
- You are considering tooth whitening for the first time.
- You want to understand the best and safest options for your specific needs.
- You have existing dental work (fillings, crowns, veneers) that you are concerned about.
- You experience persistent tooth sensitivity or gum irritation during or after whitening.
- Your teeth have severe or unusual discoloration that you suspect might be intrinsic.
- You are unsure if you are a good candidate for whitening due to oral health concerns (e.g., gum disease, exposed roots, cavities).
Seek immediate dental attention (not emergency, but promptly) if:
- You experience severe, sharp, or prolonged tooth pain that does not subside after whitening.
- You notice significant gum swelling, bleeding, or pain after using whitening products.
- You experience an allergic reaction to a whitening product.
- A single tooth suddenly changes color dramatically, especially if accompanied by pain, as this could indicate a devitalized tooth or infection.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.