Bleaching
3,353 words · 11 min read
Quick Definition
A cosmetic dental procedure that uses peroxide-based agents to lighten the color of teeth, removing stains and discoloration for a brighter smile.
Bleaching
Introduction
Bleaching, in the context of dental health, refers to a cosmetic dental procedure that uses peroxide-based agents to lighten the color of teeth. This process works by breaking down stains and discoloration, resulting in a brighter, more aesthetically pleasing smile. Often synonymous with "tooth whitening," dental bleaching has become one of the most popular and accessible ways to enhance one's smile, addressing concerns about yellowing, dullness, or dark spots.
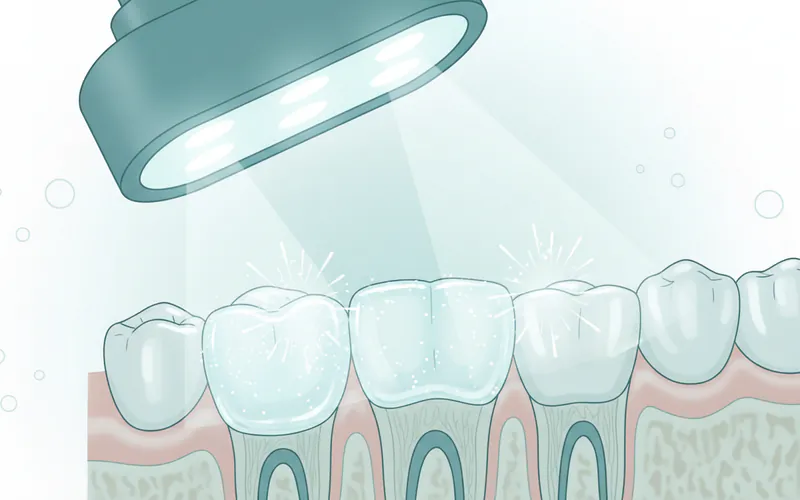
A bright, white smile is often associated with youth, health, and confidence, making bleaching a significant factor in overall dental aesthetics and personal well-being. According to the American Academy of Cosmetic Dentistry-complete-guide "Pediatric Dentist: Complete Guide") (AACD), teeth whitening is consistently ranked among the most requested cosmetic dental procedures. Millions of Americans seek solutions for tooth discoloration each year, reflecting a widespread desire for a radiant smile. Understanding the science, methods, and implications of bleaching is crucial for anyone considering this transformative treatment.
Key Takeaways:
- Bleaching uses peroxide-based agents to lighten tooth color by breaking down stains.
- Results vary based on the type and cause of discoloration, with yellow and brown stains typically responding best.
- Professional in-office treatments offer the fastest and most dramatic results, while take-home kits provide convenience and control.
- Temporary tooth sensitivity and gum irritation are common side effects but are usually mild and subside quickly.
- Bleaching does not alter the color of existing dental restorations like veneers, crowns, or composite fillings.
- Regular maintenance and good oral hygiene are essential to prolong the effects of bleaching.
Detailed Explanation
Types and Classifications
Dental bleaching can be broadly categorized into several types, each with its own methodology, active ingredients, and effectiveness. The primary active ingredients are hydrogen peroxide and carbamide peroxide, which break down into hydrogen peroxide.
-
Professional In-Office Bleaching (Chairside Whitening):
- Description: Performed by a dentist or dental hygienist in a clinical setting. It involves the application of a high-concentration hydrogen peroxide gel (typically 15-40%) to the teeth. Often, a special light, laser, or heat source is used to accelerate the chemical reaction and enhance the whitening effect, though the efficacy of light activation remains a debated topic among dental professionals.
- Pros: Fastest and most dramatic results, often achieved in a single 60-90 minute session. Treatment is supervised by a dental professional, ensuring safety and optimal application.
- Cons: Higher cost compared to other methods. Potential for increased temporary tooth sensitivity due to the higher concentration of peroxide.
- Cost: Generally ranges from $400 to $1,000 per session in the US.
-
Professional Take-Home Bleaching Kits:
- Description: Prescribed by a dentist, these kits typically include custom-fitted trays made from impressions of your teeth and a professional-grade carbamide peroxide gel (usually 10-22%) or hydrogen peroxide gel (around 6-10%). Patients apply the gel to the trays and wear them for a specified period daily (e.g., 30 minutes to a few hours) or overnight, usually for 1-2 weeks.
- Pros: Highly effective and provides consistent results. More affordable than in-office treatment. Custom trays ensure even gel distribution and minimize gum contact, reducing irritation. Patients have control over the whitening process.
- Cons: Requires patient compliance and takes longer to achieve desired results compared to in-office treatment.
- Cost: Typically ranges from $200 to $600.
-
Over-the-Counter (OTC) Bleaching Products:
- Description: Widely available in pharmacies and supermarkets, these products include whitening strips, gels, pens, and toothpaste. They contain lower concentrations of hydrogen peroxide or carbamide peroxide (e.g., 3-10% hydrogen peroxide for strips).
- Pros: Most affordable and convenient option.
- Cons: Less effective than professional treatments, results are often subtle and may be uneven. Generic trays or strips may not fit well, leading to gum irritation or inconsistent whitening. Misuse can lead to enamel damage or prolonged sensitivity.
- Cost: Ranges from $20 to $100.
-
Internal Bleaching (Non-Vital Bleaching):
- Description: This specialized procedure is used for a single tooth that has darkened from the inside out, typically after a root canal treatment or trauma that has caused the tooth's pulp to die. Instead of applying bleach to the external surface, the dentist places a peroxide agent inside the tooth's pulp chamber, sealing it in place for several days or weeks.
- Pros: Effectively targets intrinsic discoloration in non-vital teeth that external bleaching cannot reach.
- Cons: Only applicable to teeth that have had root canal treatment. Requires multiple appointments. Potential for root resorption if not done carefully.
- Cost: Typically ranges from $200 to $500 per tooth, in addition to the root canal cost.
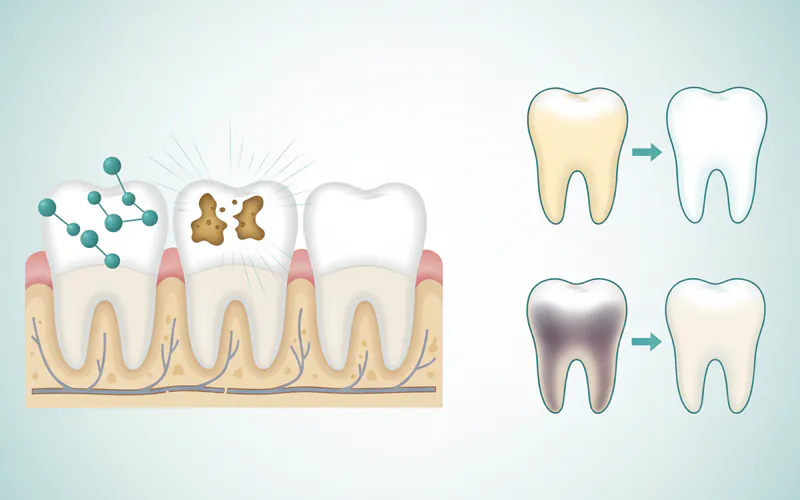
Causes and Risk Factors for Tooth Discoloration
Understanding why teeth become discolored is key to choosing the right bleaching approach and setting realistic expectations. Tooth discoloration can be broadly classified into extrinsic and intrinsic stains.
-
Extrinsic Stains: Occur on the outer surface of the tooth, primarily on the enamel, due to exposure to chromogenic (color-producing) agents.
- Diet: Frequent consumption of darkly pigmented foods and beverages such as coffee, tea, red wine, colas, berries (blueberries, blackberries), and certain spices (turmeric, curry).
- Tobacco Use: Smoking and chewing tobacco cause significant brown and black stains that are difficult to remove.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque and tartar to accumulate, creating a rough surface where stains can more easily adhere.
- Certain Medications: Chlorhexidine mouth rinses, iron supplements.
-
Intrinsic Stains: Occur within the tooth structure, either in the enamel or dentin. These are generally more challenging to remove with external bleaching alone.
- Aging: As we age, the outer enamel layer thins, revealing more of the naturally yellowish dentin underneath. The dentin itself also darkens over time.
- Genetics: Some individuals are naturally predisposed to having darker or more yellow teeth.
- Trauma: An injury to a tooth can cause internal bleeding and breakdown of blood cells, leading to a dark, often gray or brown, discoloration. This is common in non-vital teeth requiring internal bleaching.
- Medications (especially during tooth development):
- Tetracycline and Doxycycline: If taken by pregnant mothers or children during tooth development (up to age 8), these antibiotics can cause permanent gray, brown, or blue-gray banding within the tooth structure.
- Minocycline: Can cause similar intrinsic staining in adults.
- Excessive Fluoride (Fluorosis): Overexposure to fluoride during tooth formation can lead to white spots, streaks, or, in severe cases, brown pitting and mottling of the enamel.
- Dental Restorations: Old amalgam (silver) fillings can cast a gray shadow through the tooth structure. Old composite fillings or veneers may also stain or degrade over time, but these are not bleached; rather, they would need replacement.
- Dental Diseases: Conditions like dentinogenesis imperfecta or amelogenesis imperfecta, which affect tooth development, can lead to abnormal tooth color.
Signs and Symptoms to Watch For
The primary "sign" of needing bleaching is visible tooth discoloration. This can manifest as:
- General yellowing or dullness of teeth.
- Brown, gray, or black spots or streaks.
- Uneven tooth color across different teeth.
- Darkening of a single tooth, often following trauma or root canal treatment.
- White spots (especially from fluorosis) that become more noticeable against a darker background.
It's important to note that changes in tooth color are usually gradual and painless. If you notice sudden, severe discoloration accompanied by pain, swelling, or sensitivity, it could indicate a more serious underlying dental issue that requires immediate attention from a dentist.
Diagnosis Process — What Your Dentist Does
Before recommending any bleaching treatment, your dentist will conduct a thorough examination to determine the cause and type of discoloration and assess if you are a suitable candidate.
- Comprehensive Oral Examination: This includes checking for cavities, gum disease, worn-out fillings, cracks, or exposed roots. Bleaching agents can cause severe sensitivity or damage if applied to compromised teeth.
- Medical and Dental History Review: Your dentist will inquire about any medications you take, previous dental trauma, history of root canals, and dietary habits to identify potential causes of staining.
- Shade Assessment: Using a shade guide, your dentist will record your current tooth shade. This provides a baseline to compare against after treatment and helps set realistic expectations for the outcome.
- Identification of Stain Type: The dentist will differentiate between extrinsic and intrinsic stains. They will also determine if the discoloration affects all teeth evenly or if it's localized to specific teeth or areas.
- Assessment of Existing Restorations: Crucially, bleaching agents do not change the color of existing crowns, veneers, composite fillings, or other dental restorations. If you have these in visible areas, your dentist will explain that they might appear darker or mismatched after your natural teeth are whitened, and replacement may be necessary to achieve a uniform look.
- Discussion of Expectations and Contraindications: Your dentist will discuss realistic outcomes, potential side effects (like sensitivity), and any reasons why bleaching might not be appropriate for you (e.g., pregnancy, severe gum disease, allergies to peroxide).
Treatment Options with Pros, Cons, and Costs
| Treatment Option | Pros | Cons | Average Cost (USD) |
|---|---|---|---|
| Professional In-Office Bleaching | Fastest, most dramatic results (1-2 shades per session, up to 8 shades overall), professionally supervised, safest. | Highest cost, potential for temporary increased sensitivity. | $400 - $1,000 |
| Professional Take-Home Kits | Highly effective, customizable, good control, more affordable than in-office. | Requires patient compliance, slower results (1-2 weeks), potential for temporary sensitivity. | $200 - $600 |
| Over-the-Counter (OTC) Products | Most affordable, convenient, easily accessible. | Less effective, inconsistent results, potential for gum irritation if misused, lower peroxide concentration. | $20 - $100 |
| Internal Bleaching | Specifically targets intrinsic discoloration in non-vital teeth. | Only for root-canal-treated teeth, potential for root resorption (rare). | $200 - $500 per tooth |
Step-by-Step: What to Expect During Treatment
For Professional In-Office Bleaching:
- Preparation: Your dental hygienist will typically clean your teeth to remove plaque and tartar. A protective barrier (liquid dam or resin) is then carefully applied to your gums and lips to prevent the bleaching gel from irritating soft tissues.
- Gel Application: A high-concentration hydrogen peroxide gel is applied directly to the front surfaces of your teeth.
- Activation (Optional): If a light, laser, or heat source is used, it will be positioned over your teeth to activate the gel. You'll relax for about 15-20 minutes during this phase.
- Rinse and Reapply: The gel is suctioned off, and the process is typically repeated 2-3 times in the same appointment, depending on the desired shade and your sensitivity levels.
- Final Rinse and Fluoride: After the final application, the gel is thoroughly rinsed off, and the gum barrier is removed. A fluoride treatment may be applied to help reduce post-treatment sensitivity. ``
For Professional Take-Home Kits:
- Impressions: Your dentist will take impressions of your teeth to create custom-fitted bleaching trays.
- Tray Delivery and Instructions: At a subsequent appointment, you will receive your custom trays and the bleaching gel. Your dentist will provide detailed instructions on how to load the trays with the correct amount of gel, how long to wear them (e.g., 30 minutes daily or overnight), and how to care for your trays and teeth during the treatment period (typically 1-2 weeks).
- At-Home Application: You will follow your dentist's instructions, wearing the trays for the prescribed duration.
- Follow-up: Your dentist may schedule a follow-up appointment to assess your results and address any concerns.
Recovery Timeline and Aftercare
Immediately after bleaching, especially professional in-office treatments, it's common to experience:
- Sensitivity: Your teeth may be sensitive to hot and cold temperatures. This usually subsides within 24-48 hours. Your dentist may recommend using desensitizing toothpaste or a fluoride rinse to help manage this.
- "White Diet": For the first 24-48 hours after treatment, your teeth are more susceptible to re-staining due to the open pores in the enamel. Dentists often advise a "white diet," avoiding highly pigmented foods and drinks like coffee, tea, red wine, dark sodas, berries, chocolate, and tobacco. Stick to foods like chicken, rice, pasta, white fish, milk, and clear liquids.
Long-Term Aftercare:
- Maintain Good Oral Hygiene: Brush twice daily and floss once daily to prevent new stain accumulation.
- Limit Staining Foods/Drinks: While you don't have to eliminate them entirely, moderation is key. Consider using a straw for colored beverages to minimize contact with your teeth.
- Regular Dental Cleanings: Professional cleanings every six months help remove extrinsic stains and maintain your results.
- Touch-up Treatments: Bleaching results are not permanent. The effects typically last from six months to two years, depending on your habits. Your dentist may provide touch-up kits for periodic use to refresh your smile.
Prevention Strategies
Preventing tooth discoloration starts with lifestyle choices and excellent oral hygiene.
- Oral Hygiene: Brush your teeth at least twice a day with fluoride toothpaste and floss daily. This removes plaque and food debris that can contribute to stains.
- Dietary Choices: Limit consumption of highly pigmented foods and beverages. Rinse your mouth with water after consuming staining items to wash away residue.
- Use a Straw: When drinking coffee, tea, soda, or red wine, using a straw can reduce contact with your front teeth.
- Quit Tobacco: Eliminating smoking and chewing tobacco is one of the most effective ways to prevent severe extrinsic staining and improve overall oral health.
- Regular Dental Check-ups and Cleanings: Professional cleanings remove extrinsic stains and tartar buildup that you can't remove at home. This also allows your dentist to monitor for early signs of discoloration or other dental issues. ``
Cost Ranges in the US
The cost of dental bleaching in the US varies significantly based on the type of treatment, geographic location, and the dentist's fees.
- Professional In-Office Bleaching: Typically ranges from $400 to $1,000 per session. Some patients may need multiple sessions for optimal results.
- Professional Take-Home Kits: Generally cost between $200 and $600, which includes the custom trays and bleaching gel. Refill gels are less expensive, usually $40-$80.
- Over-the-Counter Products: Highly variable, from $20 to $100 for strips, gels, or pens. Whitening toothpaste is typically priced similar to regular toothpaste, around $5-$15.
- Internal Bleaching: Ranges from $200 to $500 per tooth. This does not include the cost of the initial root canal treatment if it hasn't already been performed.
Insurance Coverage: Dental bleaching is almost universally considered a cosmetic procedure by dental insurance providers. Therefore, it is rarely covered by insurance. Patients typically pay for the full cost out-of-pocket. It's always advisable to check with your specific insurance provider for clarification.
For Parents / Pediatric Considerations
Dental bleaching is generally not recommended for children or adolescents. There are several reasons for this:
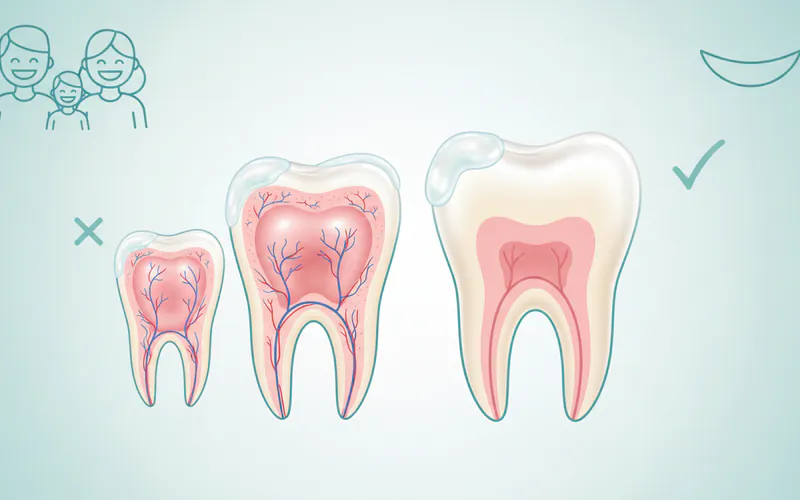
- Developing Pulp: Young teeth have larger pulp chambers and nerve tissues that are closer to the surface. Bleaching agents can cause significant, prolonged sensitivity or even damage to the developing pulp.
- Enamel Development: The enamel of permanent teeth in children is still maturing and may be more porous, making it more susceptible to sensitivity or uneven results.
- Temporary Teeth: There's no benefit to bleaching primary (baby) teeth, as they will eventually be replaced by permanent teeth.
- Underlying Causes: Discoloration in children's teeth often points to other issues, such as trauma, severe decay, or intrinsic staining from medications or fluorosis. A pediatric dentist should always evaluate any discoloration in a child's teeth to diagnose the underlying cause and recommend appropriate treatment, which may not be bleaching.
- Unrealistic Expectations: Children and teens may have unrealistic expectations for whitening results, and their compliance with at-home treatments might be low.
For parents concerned about their child's tooth color, the focus should be on excellent oral hygiene, limiting sugary and staining foods, and regular dental check-ups. If discoloration is persistent or concerning, consult a pediatric dentist to explore the cause and safe, age-appropriate solutions. In cases of severe intrinsic staining, alternative cosmetic solutions like composite bonding or veneers might be considered for older adolescents, but usually after tooth development is complete.
Frequently Asked Questions
How much does dental bleaching cost?
The cost of dental bleaching varies widely depending on the method. Professional in-office bleaching typically ranges from $400 to $1,000. Dentist-prescribed take-home kits are usually $200 to $600. Over-the-counter products are the most affordable, ranging from $20 to $100. Internal bleaching for a single non-vital tooth costs approximately $200 to $500.
Is dental bleaching painful?
Most people do not find dental bleaching painful, but temporary tooth sensitivity is a common side effect, especially to hot and cold temperatures. This sensitivity typically subsides within 24-48 hours after treatment. Your dentist can provide desensitizing agents or recommend specific toothpaste to help manage discomfort. Gum irritation can also occur if the bleaching gel comes into contact with soft tissues, but professional treatments use protective barriers to minimize this.
How long do bleaching results last?
The longevity of bleaching results varies from person to person, typically lasting anywhere from six months to two years. Factors influencing this include your diet (consumption of staining foods/drinks), tobacco use, and oral hygiene habits. Regular touch-up treatments, often with take-home kits, can help maintain your bright smile.
What are the alternatives to bleaching?
If bleaching is not suitable or doesn't achieve the desired results, several cosmetic alternatives can improve tooth color and aesthetics:
- Dental Veneers: Thin, custom-made shells (porcelain or composite) that cover the front surface of teeth. They offer a significant aesthetic improvement, can correct severe discoloration, shape issues, and minor misalignments, but require some removal of enamel.
- Composite Bonding: Tooth-colored resin is applied to the tooth and hardened with a special light. This is a less invasive and more affordable option for minor discoloration, chips, or gaps.
- Dental Crowns: Full coverage restorations used for severely damaged or discolored teeth, often when structural integrity is also compromised.
- Professional Cleaning: Sometimes, extrinsic stains can be effectively removed by a professional dental cleaning, revealing the natural, lighter tooth shade underneath.
Does dental insurance cover bleaching?
No, dental bleaching is almost universally considered a cosmetic procedure by dental insurance companies. Therefore, it is typically not covered by insurance, and the patient is responsible for the full cost out-of-pocket. It's always best to confirm with your specific insurance provider.
How long does a bleaching session take?
A single professional in-office bleaching session usually takes about 60-90 minutes. This includes preparation, multiple applications of the bleaching gel, and any light activation cycles. For take-home kits, the daily application time varies, often between 30 minutes to a few hours, or even overnight, for a period of 1-2 weeks.
Can bleaching damage my teeth or enamel?
When performed correctly under professional guidance, dental bleaching is considered safe and does not cause permanent damage to tooth enamel. The temporary sensitivity is due to the peroxide reaching the dentin tubules. Misuse of over-the-counter products, such as using them too frequently or for too long, can potentially lead to increased sensitivity, gum irritation, and in rare cases, uneven results or even some enamel erosion. Always follow product instructions or your dentist's guidance.
When to See a Dentist
It is always recommended to see a dentist before starting any form of tooth bleaching. Your dentist can assess the cause of your discoloration, determine if you are a suitable candidate, and recommend the most effective and safest treatment option.
You should definitely see a dentist if you experience:
- Sudden or severe tooth discoloration.
- Persistent or worsening tooth sensitivity after attempting any whitening product.
- Gum irritation, bleeding, or pain during or after bleaching.
- Uneven whitening results or white spots that become more noticeable.
- If you have existing dental restorations (fillings, veneers, crowns) that might not bleach evenly with your natural teeth.
- If you have any underlying dental conditions like cavities, gum disease, or exposed roots.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.