Deep Cleaning Teeth: Complete Guide
Key Takeaways
- Did you know that nearly half of all American adults over 30 suffer from some form of gum disease? Untreated, this common condition can lead to severe pain, tooth loss, and even contribute to systemic health issues like heart disease and diabetes. If you've been told you need a **deep cleaning t
Deep Cleaning Teeth: Complete Guide
Did you know that nearly half of all American adults over 30 suffer from some form of gum disease? Untreated, this common condition can lead to severe pain, tooth loss, and even contribute to systemic health issues like heart disease and diabetes. If you've been told you need a deep cleaning teeth procedure, also known as scaling and root planing, it's crucial to understand what this vital treatment entails and why it’s a cornerstone of managing gum disease. This comprehensive guide from SmilePedia.net will demystify deep cleaning, covering everything from its causes and process to costs, recovery, and essential prevention strategies, empowering you to take control of your oral health.

Key Takeaways:
- Deep cleaning (scaling and root planing) is a non-surgical procedure essential for treating moderate to severe gum disease (periodontitis).
- It removes plaque, calculus, and bacteria from above and below the gum line, smoothing root surfaces to prevent reattachment.
- The procedure typically involves local anesthesia and is often completed over 1-4 appointments, depending on the severity and number of affected quadrants.
- Costs in the US range from $200-$600 per quadrant, potentially totaling $800-$2,400 for a full mouth deep cleaning without insurance. Most dental insurance plans cover a significant portion.
- Recovery usually involves mild sensitivity and soreness for a few days, manageable with over-the-counter pain relievers and careful oral hygiene.
- Maintaining excellent daily oral hygiene and regular periodontal maintenance appointments (every 3-4 months) are crucial for long-term success and preventing recurrence.
What Deep Cleaning Teeth Is (Scaling and Root Planing)
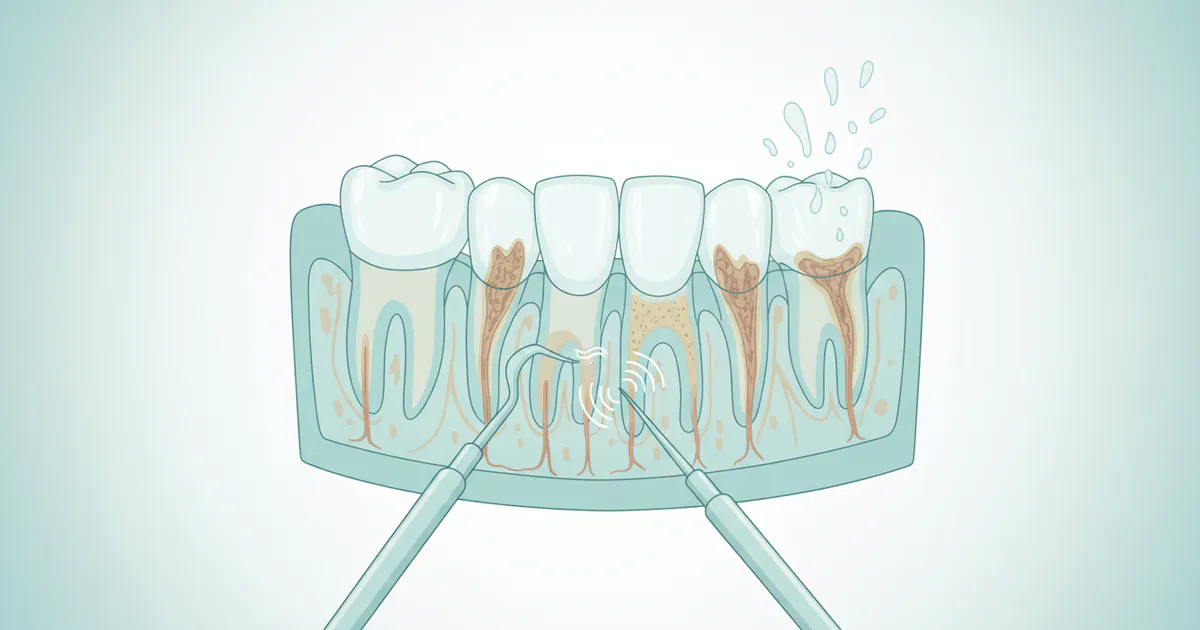
A deep cleaning teeth procedure, formally known as scaling and root planing (SRP), is a specialized, non-surgical treatment designed to thoroughly clean the surfaces of your teeth and roots. Unlike a routine dental cleaning, which primarily focuses on the visible parts of your teeth above the gum line, deep cleaning targets the areas below the gum line. This is where harmful bacteria, plaque, and hardened deposits called calculus (tartar) accumulate, forming pockets between your gums and teeth.
When these pockets deepen and harbor bacteria, they cause inflammation and infection, leading to periodontitis, a more advanced form of gum disease. Scaling and root planing aims to eliminate these irritants.
- Scaling: This step involves meticulously removing plaque and calculus from the tooth surfaces, both above and, crucially, below the gum line, extending into the periodontal pockets. Dental professionals use specialized instruments, including ultrasonic scalers and hand scalers, to meticulously scrape away these deposits.
- Root Planing: After scaling, the root surfaces are "planed" or smoothed. This process removes any remaining calculus, bacterial toxins, and diseased cementum from the root surfaces. Smoothing the roots helps to reduce inflammation, encourages the gum tissue to reattach more firmly to the cleaned tooth surface, and makes it more difficult for bacteria to adhere in the future.
This procedure is a critical intervention to stop the progression of gum disease, reduce inflammation, and prevent further bone and tissue loss that can ultimately lead to tooth mobility and even tooth loss.
Types / Variations of Deep Cleaning
While the core principles of scaling and root planing remain consistent, there can be variations in the approach and adjunctive therapies used. Deep cleaning is typically performed in sections of the mouth, known as quadrants, over multiple appointments to ensure comfort and thoroughness.
Quadrant-Based Treatment
The mouth is usually divided into four quadrants: upper right, upper left, lower right, and lower left.
- Single Quadrant: In some cases, if gum disease is localized to a specific area, only one or two quadrants may require deep cleaning.
- Multiple Quadrants: Most commonly, patients with generalized periodontitis will need deep cleaning across all four quadrants. This is often done over two appointments, where two quadrants are treated per visit, allowing for adequate healing time between sides. Sometimes, it can be spread across three or four appointments for patient comfort or for very extensive cases.
Anesthesia and Pain Management
- Local Anesthesia: This is standard for deep cleaning. A numbing agent is injected into the gum tissue around the teeth being treated, ensuring the procedure is comfortable and pain-free.
- Sedation Dentistry: For patients with significant dental anxiety or those undergoing extensive treatment, options like nitrous oxide (laughing gas), oral conscious sedation (a prescribed pill), or IV sedation might be offered by a periodontist or general dentist with special training.
Adjunctive Therapies
To enhance the effectiveness of deep cleaning and combat persistent bacterial infection, dentists or periodontists may recommend additional treatments:
- Local Antibiotic Delivery: After scaling and root planing, tiny antimicrobial gels or antibiotic microspheres (e.g., Arestin, Atridox) can be placed directly into deep periodontal pockets. These slowly release medication over several days or weeks, helping to kill remaining bacteria and promote healing.
- Antimicrobial Rinses: Prescription-strength antimicrobial mouthrinses, such as chlorhexidine gluconate (CHX), are often prescribed for use at home after the procedure to reduce bacterial load and aid in gum healing.
- Laser-Assisted Periodontal Therapy (LAPT): Some dentists and periodontists use dental lasers in conjunction with traditional scaling and root planing. Lasers can help remove infected tissue, sterilize pockets, and reduce bacteria, potentially aiding in healing and reducing discomfort. The effectiveness and necessity of lasers as an addition to traditional SRP are still topics of ongoing research and debate within the dental community.
- Systemic Antibiotics: In very aggressive or widespread cases of periodontitis, a course of oral antibiotics may be prescribed to supplement local treatment, although this is less common for standard deep cleaning.
These variations and additions are always tailored to the individual's specific condition, the severity of their gum disease, and their overall health.
Causes / Why It Happens
The primary cause of the need for deep cleaning teeth is the progression of gum disease, which starts with inadequate oral hygiene. Here's a breakdown of the causative factors:
1. Plaque Accumulation
- Dental Plaque: A sticky, colorless film of bacteria constantly forms on your teeth. If not removed daily through brushing and flossing, these bacteria proliferate and irritate the gum tissue.
- Gingivitis: This is the earliest and mildest form of gum disease. It's characterized by inflamed, red, swollen gums that may bleed easily during brushing or flossing. Gingivitis is reversible with good oral hygiene and professional cleanings. However, if left untreated, it progresses.
2. Calculus (Tartar) Formation
- Hardened Plaque: When plaque remains on teeth, it eventually hardens into calculus (tartar). Calculus is extremely porous and provides an ideal surface for more plaque to accumulate and for bacteria to thrive.
- Irritation and Inflammation: Unlike plaque, calculus cannot be removed by brushing or flossing alone; it requires professional dental instruments. The presence of calculus below the gum line creates a constant source of irritation, leading to chronic inflammation.
3. Periodontal Pockets
- Gum Recession and Pockets: The chronic inflammation caused by plaque and calculus leads the gum tissue to pull away from the teeth, forming spaces called periodontal pockets. These pockets act as traps for food particles and bacteria, becoming increasingly difficult to clean with standard oral hygiene.
- Bone and Tissue Destruction: As bacteria multiply within these pockets, they release toxins that trigger an immune response, leading to the destruction of the bone and connective tissues that support the teeth. This is the hallmark of periodontitis, an irreversible condition if untreated.
Contributing Factors and Risk Factors
While poor oral hygiene is the direct cause, several factors can increase your susceptibility to developing gum disease and requiring deep cleaning:
- Smoking/Tobacco Use: One of the most significant risk factors. Smoking impairs the immune system's ability to fight off bacterial infections and can mask the symptoms of gum disease (e.g., less bleeding).
- Genetics: Some individuals are genetically predisposed to more severe forms of gum disease.
- Systemic Diseases: Conditions like diabetes (especially poorly controlled), autoimmune diseases, and heart disease can compromise the body's immune response, making individuals more vulnerable to gum infections.
- Hormonal Changes: Pregnancy, puberty, menopause, and menstruation can make gums more sensitive and prone to inflammation.
- Certain Medications: Drugs that cause dry mouth (xerostomia) reduce saliva flow, which is essential for washing away food particles and neutralizing acids. Other medications, like some anti-seizure drugs or calcium channel blockers, can cause gingival overgrowth, making cleaning difficult.
- Poor Nutrition: A diet lacking essential vitamins and nutrients can weaken the immune system and make gum tissue less resilient.
- Stress: Chronic stress can weaken the immune system, making it harder for the body to fight off infections, including gum disease.
- Misaligned Teeth or Poorly Fitting Restorations: These can create areas that are difficult to clean, leading to plaque accumulation.
- Grinding or Clenching Teeth (Bruxism): Can put excessive force on supporting tissues, potentially accelerating tissue destruction in the presence of gum disease.
Understanding these causes and risk factors is crucial for prevention and for appreciating the importance of deep cleaning once periodontitis has set in.
Signs and Symptoms That You Might Need a Deep Cleaning
It's essential to recognize the warning signs of gum disease, as early detection can prevent the need for more invasive treatments. If you notice any of these symptoms, it's time to schedule an appointment with your dentist.
Early Warning Signs (Gingivitis)
These symptoms indicate the initial stage of gum disease, which may still be reversible with improved oral hygiene and professional cleaning:
- Red, Swollen, or Tender Gums: Healthy gums are typically firm and pink. If yours appear puffy, inflamed, or a deep red/purplish color, it’s a sign of inflammation.
- Bleeding Gums: Gums that bleed during brushing, flossing, or even spontaneously are a primary indicator of gingivitis. Healthy gums should not bleed.
- Bad Breath (Halitosis): Persistent bad breath or a bad taste in your mouth, even after brushing, can be caused by the bacteria accumulating in plaque and pockets.
Advanced Warning Signs (Periodontitis, Indicating Need for Deep Cleaning)
If gingivitis is left untreated, it progresses to periodontitis, and these symptoms become more pronounced:
- Receding Gums: Your gums may pull away from your teeth, making your teeth appear longer. This exposes the root surfaces, which can lead to sensitivity.
- Deep Pockets Between Teeth and Gums: Your dentist will measure these with a periodontal probe. Pocket depths greater than 3mm typically indicate gum disease, and depths of 4mm or more often warrant deep cleaning.
- Pus Between Teeth and Gums: This is a clear sign of active infection.
- Loose or Shifting Teeth: As the bone and connective tissues supporting your teeth are destroyed, your teeth may become mobile or shift position.
- Changes in Bite: You might notice changes in how your teeth fit together when you bite down, or in the fit of partial dentures.
- Persistent Bad Taste: Similar to halitosis, but often more severe and constant.
- Increased Sensitivity: Exposed tooth roots due to gum recession can become sensitive to hot, cold, or sweet foods and drinks.

Pro Tip: Don't wait for pain. Gum disease is often a "silent" disease, meaning it can progress significantly without causing discomfort until it's in advanced stages. Regular dental check-ups are crucial for early detection, even if you don't notice symptoms.
Treatment Options for Gum Disease
When gum disease progresses beyond gingivitis, various treatment options are available, with deep cleaning being the most common non-surgical intervention for periodontitis.
1. Non-Surgical Treatments (Primary for moderate gum disease)
- Scaling and Root Planing (Deep Cleaning): As detailed, this is the first line of treatment for periodontitis. It aims to remove plaque and calculus from below the gum line and smooth root surfaces.
- Local Antibiotics: After SRP, antimicrobial gels or chips can be placed into deep pockets to continue fighting bacteria.
- Antimicrobial Mouthrinses: Prescription rinses help control bacteria in the mouth.
2. Surgical Treatments (For advanced periodontitis)
If deep cleaning and adjunctive therapies are insufficient to control the disease, or if bone loss is extensive, surgical interventions may be necessary. These are typically performed by a periodontist:
- Flap Surgery (Pocket Reduction Surgery): The gums are lifted back to allow for thorough cleaning of the root surfaces and removal of diseased tissue. The gums are then sutured back into place, often tighter around the teeth, to reduce pocket depth.
- Bone Grafts: If bone loss has occurred, fragments of your own bone, synthetic bone, or donated bone can be used to regenerate lost bone, providing a more stable foundation for your teeth.
- Soft Tissue Grafts: If gum recession is significant, soft tissue from another area of your mouth (like the palate) or a donor source can be used to cover exposed roots and prevent further recession.
- Guided Tissue Regeneration: A small piece of mesh-like fabric is placed between the bone and gum tissue to prevent the gum tissue from growing into the bone, allowing bone and connective tissue to regenerate more effectively.
3. Laser Periodontal Therapy
While often considered an adjunctive therapy, some practitioners use lasers for specific periodontal procedures. For instance, LANAP (Laser-Assisted New Attachment Procedure) is a specific protocol that uses a laser to remove diseased tissue and bacteria from periodontal pockets, potentially promoting reattachment of gum tissue and bone regeneration. It is a less invasive alternative to traditional flap surgery in some cases.
Comparison of Deep Cleaning vs. Surgical Treatment
| Feature | Deep Cleaning (Scaling & Root Planing) | Periodontal Surgery (e.g., Flap Surgery) |
|---|---|---|
| Purpose | Remove plaque/calculus, smooth roots, reduce inflammation, shrink pockets | Reduce deep pockets, regenerate lost bone/tissue, address severe recession |
| Target Pockets | Moderate (4-6mm generally) | Deep (>6mm typically), or areas unresponsive to SRP |
| Invasiveness | Non-surgical, minimal incision (only local anesthesia) | Surgical, involves incisions, lifting gum tissue, sutures |
| Anesthesia | Local anesthesia | Local anesthesia, sometimes with sedation |
| Recovery | Mild soreness/sensitivity, few days | More significant discomfort, swelling, potentially weeks of healing |
| Cost (per quadrant) | $200 - $600 | $500 - $3,000+ (depending on procedure) |
| Primary Benefit | Halts disease progression, preserves teeth, improves gum health | Restores structural integrity, saves teeth in advanced cases, enhances aesthetics |
The choice of treatment depends heavily on the severity of your gum disease, assessed through periodontal charting (pocket depths), X-rays to evaluate bone loss, and a comprehensive examination by your dentist or periodontist.
Step-by-Step Process of Deep Cleaning (Scaling and Root Planing)
Understanding what to expect during your deep cleaning appointment can help alleviate anxiety. Here's a typical step-by-step breakdown:
1. Initial Examination and Diagnosis
Before the deep cleaning, your dentist or periodontist will perform a thorough examination.
- Periodontal Charting: They will use a small probe to measure the depth of the pockets between your teeth and gums. Pockets deeper than 3mm typically indicate gum disease, with 4mm+ often warranting deep cleaning.
- X-rays: Radiographs help assess the extent of bone loss around your teeth.
- Visual Inspection: Looking for signs of inflammation, bleeding, and calculus.
2. Numbing the Area
- Local Anesthesia: To ensure your comfort, the dental professional will administer a local anesthetic to numb the specific area (quadrant) being treated. This makes the procedure virtually painless. The numbing sensation typically lasts for a few hours after the procedure.
3. Scaling the Tooth Surfaces
- Ultrasonic Scaler: The hygienist or dentist will often start with an ultrasonic scaler. This instrument uses high-frequency vibrations and a fine spray of water to dislodge and rinse away large deposits of plaque and calculus from above and below the gum line. The water also helps to cool the instrument and flush out debris.
- Hand Scalers (Curettes): Following the ultrasonic scaler, specialized hand instruments called curettes are used. These curved, sharp tools allow for precise and thorough removal of smaller, more tenacious deposits from the tooth surfaces and deep within the periodontal pockets. This step requires great skill and meticulous attention to detail.
4. Root Planing
- Smoothing the Root Surfaces: Once the calculus is removed, the root surfaces are meticulously planed (smoothed). This is done with the same hand instruments, carefully scraping away any remaining bacterial toxins, rough spots, or diseased cementum from the root. A smooth root surface makes it harder for bacteria to reattach and encourages the gum tissue to heal and reattach more firmly.
5. Rinsing and Irrigation
- Throughout the procedure, water is used to rinse away debris. At the end, the pockets may be flushed with an antiseptic solution to further reduce bacteria.
6. Application of Local Antibiotics (If Prescribed)
- If deemed necessary, your dentist may place a tiny antibiotic gel or chip directly into the deepest pockets after the scaling and root planing is complete. This delivers medicine directly to the site of infection over an extended period.
7. Post-Procedure Instructions
- Before you leave, you will receive detailed instructions on how to care for your mouth during recovery, including advice on pain management, diet, and oral hygiene. You'll also be advised on follow-up appointments.
Most deep cleaning procedures are performed in one to four appointments, depending on the severity of your gum disease and the number of quadrants requiring treatment. For instance, two quadrants might be treated in one visit, and the remaining two in another, typically a week or two later. This approach minimizes discomfort and allows for thorough treatment.
Cost and Insurance for Deep Cleaning Teeth in the US
The cost of deep cleaning teeth (scaling and root planing) can vary significantly across the United States, influenced by factors such as location, the severity of the gum disease, the number of quadrants treated, the type of dental professional (general dentist vs. periodontist), and the need for adjunctive therapies.

Average US Cost Ranges Without Insurance
Deep cleaning is typically billed per quadrant of the mouth. A full mouth deep cleaning usually involves all four quadrants (upper right, upper left, lower right, lower left).
- Per Quadrant: Expect to pay anywhere from $200 to $600 per quadrant.
- Full Mouth (4 Quadrants): This can range from $800 to $2,400 or more for the entire procedure without insurance.
- Adjunctive Therapies:
- Local Antibiotic Placement (e.g., Arestin): $30-$100 per site (often per pocket).
- Antimicrobial Rinses (prescription): $20-$50 for a bottle.
- Nitrous Oxide/Sedation: Additional $50-$500+, depending on type and duration.
Factors Influencing Cost:
- Geographic Location: Costs are generally higher in major metropolitan areas and on the coasts compared to rural areas.
- Severity of Disease: Deeper pockets and more extensive calculus deposits require more time and effort, potentially increasing the cost.
- Dental Professional: Periodontists (gum specialists) may charge slightly more than general dentists due to their specialized training.
- Included Services: Some practices might bundle certain services, while others itemize every step, including X-rays and initial exams which are separate charges.
- Adjunctive Treatments: As mentioned, adding antibiotics or sedation will increase the overall cost.
Insurance Coverage Details
Most dental insurance plans do cover a significant portion of deep cleaning, as it is considered a necessary medical procedure to treat gum disease.
- Coverage Levels: Many plans cover 50% to 80% of the cost of scaling and root planing.
- Deductibles and Co-pays: You will likely be responsible for your annual deductible and a co-pay, which is the percentage of the cost not covered by insurance.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) before major procedures like deep cleaning are covered. Check your policy.
- Periodontal Maintenance: After deep cleaning, regular "periodontal maintenance" cleanings (typically every 3-4 months) are usually covered similarly to routine cleanings, but often at a higher frequency. Ensure your insurance covers these necessary follow-up appointments.
- CPT Codes: Dental insurance companies use specific codes for procedures. For deep cleaning, the codes are typically D4341 (Periodontal Scaling and Root Planing – Four or More Teeth Per Quadrant) and D4342 (Periodontal Scaling and Root Planing – One to Three Teeth Per Quadrant). Adjunctive therapies have separate codes.
Pro Tip: Always contact your dental insurance provider directly before your procedure to understand your specific coverage, deductibles, co-pays, and any annual maximums. Your dental office can often help you with this by submitting a pre-treatment estimate.
Cost Breakdown Table (Examples)
| Service | Average Cost (Without Insurance) | Average Cost (With Insurance, 50-80% coverage) |
|---|---|---|
| Scaling & Root Planing (per quadrant) | $200 - $600 | $100 - $300 (your out-of-pocket) |
| Full Mouth Deep Cleaning (4 quadrants) | $800 - $2,400 | $400 - $1,200 (your out-of-pocket) |
| Local Antibiotic (per site) | $30 - $100 | $15 - $50 (your out-of-pocket) |
| Initial Exam & X-rays | $100 - $300 | $20 - $100 (your out-of-pocket) |
| Periodontal Maintenance (per visit) | $100 - $200 | $20 - $80 (your out-of-pocket) |
Recovery and Aftercare After Deep Cleaning
Proper recovery and diligent aftercare are crucial for the success of your deep cleaning procedure and the long-term health of your gums.
Immediate Post-Procedure Experience (First 24-48 Hours)
- Numbness: The local anesthetic will wear off gradually, usually within 1-3 hours.
- Soreness and Tenderness: It's common to experience some gum soreness, tenderness, and mild swelling. This is a normal part of the healing process.
- Sensitivity: Your teeth, especially where roots may have been exposed, might be more sensitive to hot, cold, or even air for a few days to a few weeks.
- Minor Bleeding: You might notice slight bleeding when you brush or rinse for a day or two. This is usually minimal.
Pain Management
- Over-the-Counter Pain Relievers: For most patients, over-the-counter pain medications like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are sufficient to manage discomfort. Follow dosage instructions.
- Prescription Pain Relievers: In rare cases, for severe discomfort, your dentist might prescribe a stronger pain medication.
Diet and Eating
- Soft Foods: Stick to soft foods for the first 24-48 hours. Examples include yogurt, smoothies, mashed potatoes, soups, scrambled eggs, and cooked pasta.
- Avoid Irritating Foods: Stay away from very hot, cold, spicy, acidic, crunchy, or chewy foods that could irritate your tender gums or dislodge blood clots.
- Chew on Opposite Side: If only one side of your mouth was treated, try to chew on the untreated side.
Oral Hygiene Instructions
- Gentle Brushing: Continue to brush your teeth gently but thoroughly with a soft-bristled toothbrush. You might need to be extra careful around the treated areas for a few days.
- Flossing: Resume flossing daily, being gentle near the gum line of treated teeth.
- Saltwater Rinses: Rinsing with warm salt water (1/2 teaspoon of salt in 8 ounces of warm water) 2-3 times a day for the first few days can help soothe gums, reduce swelling, and promote healing.
- Antimicrobial Rinses: If your dentist prescribed an antimicrobial mouthwash (like chlorhexidine), use it as directed. This is usually started 24 hours after the procedure.
- Avoid Alcohol-Based Rinses: These can be irritating to healing tissues.
What to Avoid
- Smoking/Tobacco: Avoid all tobacco products, as they significantly impede healing and increase the risk of re-infection and complications. This is one of the most critical steps for successful recovery.
- Alcohol: Avoid alcohol for at least 24-48 hours, as it can interfere with healing and medications.
Follow-Up Appointments
- Periodontal Maintenance: Deep cleaning is not a one-time fix. To maintain the results and prevent recurrence of gum disease, you will need to schedule regular periodontal maintenance appointments. These are more frequent than routine cleanings, typically every 3-4 months, as directed by your dentist or periodontist. These specialized cleanings focus on keeping your pockets clear of bacteria and monitoring your gum health.
- Re-evaluation: Your dentist may schedule a re-evaluation appointment a few weeks after your deep cleaning to assess how your gums have healed and to measure pocket depths again.
By adhering to these aftercare instructions, you significantly increase the chances of successful healing and long-term gum health.
Prevention of Gum Disease and the Need for Deep Cleaning
The best deep cleaning is the one you never need. Preventing gum disease involves a combination of consistent oral hygiene, a healthy lifestyle, and regular professional dental care.
1. Excellent Daily Oral Hygiene
This is the cornerstone of prevention, targeting plaque, the primary cause of gum disease.
- Brush Twice a Day: Brush your teeth for at least two minutes, twice a day, using a soft-bristled toothbrush and fluoride toothpaste. Angle the brush at 45 degrees to the gum line, gently sweeping away plaque.
- Floss Daily: Flossing removes plaque and food particles from between your teeth and under the gum line, areas your toothbrush can't reach. It's crucial for preventing interdental gum disease.
- Use Mouthwash (Optional but Recommended): An antimicrobial mouthwash can help reduce bacteria. Look for ADA-accepted rinses.
- Tongue Cleaning: Gently clean your tongue to remove bacteria that contribute to bad breath and can spread to your gums.

2. Regular Dental Check-ups and Cleanings
- Professional Cleanings: Schedule routine dental cleanings (prophylaxis) at least twice a year, or more frequently if recommended by your dentist. These cleanings remove hardened calculus (tartar) that brushing and flossing cannot, preventing it from accumulating below the gum line.
- Dental Exams: Regular exams allow your dentist to identify early signs of gum disease, measure pocket depths, and recommend interventions before the condition becomes severe.
3. Lifestyle Modifications (Gum Disease Self-Care)
- Quit Smoking/Tobacco: This is arguably the most impactful change you can make. Smoking severely impairs gum health and healing. Quitting significantly reduces your risk of severe periodontitis.
- Manage Systemic Health Conditions: If you have diabetes, heart disease, or other chronic conditions, work with your doctor to manage them effectively. Well-controlled diabetes, for example, is linked to better gum health.
- Balanced Diet: Eat a healthy diet rich in fruits, vegetables, and whole grains. Limit sugary foods and drinks that promote bacterial growth. Vitamin C, in particular, is important for gum health.
- Stay Hydrated: Drink plenty of water throughout the day. Water helps wash away food particles and maintains saliva flow, which protects against bacteria.
- Stress Management: Chronic stress can weaken the immune system, making you more susceptible to infections, including gum disease.
4. Address Contributing Factors
- Treat Dry Mouth: If you suffer from dry mouth, discuss solutions with your dentist or doctor. They might recommend specific rinses, medications, or saliva substitutes.
- Correct Misaligned Teeth: Orthodontic treatment can straighten teeth, making them easier to clean and reducing areas where plaque can accumulate.
- Replace Old Restorations: Worn out or ill-fitting fillings and crowns can create traps for bacteria; replace them as needed.
By integrating these preventive measures into your daily routine, you can significantly reduce your risk of developing gum disease and potentially avoid the need for deep cleaning altogether. Remember, consistent effort in gum disease self-care is key to maintaining a healthy smile.
Risks and Complications of Deep Cleaning
While deep cleaning is a common and generally safe procedure, it's important to be aware of potential risks and complications, although severe issues are rare.
- Post-Procedure Sensitivity: This is the most common side effect. You may experience increased sensitivity to hot, cold, or sweet stimuli, especially if root surfaces were exposed by gum recession. This typically subsides within a few days to a few weeks but can occasionally persist longer. Desensitizing toothpaste or fluoride varnishes can help.
- Gum Soreness and Tenderness: It's normal for your gums to feel sore, tender, and slightly swollen for a few days after the procedure, similar to a deep bruise. Over-the-counter pain relievers usually manage this effectively.
- Mild Bleeding: Some minor bleeding during brushing or flossing can occur for a day or two after deep cleaning. Persistent or heavy bleeding should be reported to your dentist.
- Gum Recession (Apparent): After inflammation subsides and swelling reduces, your gums may appear to have receded more, making your teeth look longer. This isn't actual recession but rather the shrinkage of swollen, inflamed gum tissue back to a healthier level. While it can be a cosmetic concern for some, it indicates healing and reduced pocket depths.
- Pain: While the procedure itself is numbed, some post-operative pain is expected. Severe or escalating pain could indicate a complication.
- Infection: Although rare due to the cleaning process itself, there's a small risk of infection, especially in individuals with compromised immune systems. Your dentist might prescribe antibiotics if there's a high risk.
- Damage to Dental Work: If not performed carefully, existing fillings, crowns, or veneers could potentially be chipped or damaged during scaling, especially with aggressive use of ultrasonic instruments. This is why it's crucial to have deep cleaning performed by an experienced professional.
- Temporary Jaw Stiffness or Discomfort: Keeping your mouth open for an extended period during the procedure can lead to temporary jaw stiffness or discomfort.
- Adverse Reaction to Anesthesia: While uncommon, some individuals may experience adverse reactions to local anesthetics, such as dizziness, lightheadedness, or allergic reactions. Inform your dentist of any known allergies or medical conditions beforehand.
Pro Tip: If you experience severe pain, excessive bleeding, swelling that worsens after a few days, or signs of infection (e.g., pus, fever), contact your dental office immediately.
Children / Pediatric Considerations for Deep Cleaning
Deep cleaning (scaling and root planing) is rarely necessary for children. Periodontitis, the advanced form of gum disease that necessitates deep cleaning, is far less common in pediatric populations compared to adults.
However, certain circumstances might lead to a child needing more than a routine cleaning:
- Aggressive Periodontitis (Rare): Some children and adolescents can develop aggressive forms of periodontitis, which can be linked to genetic factors or specific bacterial infections. This type of gum disease progresses rapidly and can cause significant bone loss. In such cases, deep cleaning, possibly combined with antibiotics, might be indicated.
- Specific Syndromes or Systemic Conditions: Children with certain systemic diseases (e.g., Down syndrome, Papillon-Lefèvre syndrome, Type 1 diabetes) or immune deficiencies may be at a higher risk for early-onset gum disease. Their dental care may need to be more intensive.
- Severe Gingivitis/Poor Oral Hygiene: While deep cleaning isn't usually the first step for gingivitis, chronic, severe gingivitis due to extremely poor oral hygiene might, in rare cases, require more extensive cleaning than a standard prophylaxis, even if true pocketing isn't present.
When deep cleaning is performed on a child, it is done with the same meticulous care as with adults, often utilizing local anesthesia to ensure comfort. Pediatric dentists or periodontists specializing in children's oral health will assess the child's specific needs, temperament, and health history to determine the most appropriate course of action. They may also focus heavily on parental education regarding improved oral hygiene techniques for the child.
For most children, the focus remains on preventative care:
- Consistent Brushing and Flossing: Teaching children proper brushing and flossing techniques from an early age.
- Healthy Diet: Limiting sugary snacks and drinks.
- Regular Pediatric Dental Check-ups: These are crucial for early detection of any oral health issues, including signs of gum inflammation.
If a child shows signs of gum disease, early intervention is key to prevent its progression.
Cost Breakdown for Deep Cleaning Teeth
A detailed understanding of the cost components of deep cleaning is vital for financial planning. As mentioned, costs are typically calculated per quadrant, and several factors influence the final price.
Average US Costs (Without Insurance)
- Low Range: $200-$350 per quadrant (e.g., in rural areas, general dentist).
- Mid Range: $350-$500 per quadrant (e.g., suburban areas, standard general dentist fee).
- High Range: $500-$600+ per quadrant (e.g., major metropolitan areas, periodontist, complex cases).
Therefore, a full mouth deep cleaning (4 quadrants) can range from $800 (low end) to $2,400+ (high end) without insurance coverage.
With vs. Without Insurance
- Without Insurance: You are responsible for 100% of the cost. Many dental offices offer a discount for cash payments or payment plans.
- With Insurance: Most dental insurance plans classify deep cleaning as a "basic" or "major" procedure.
- Deductible: You'll typically need to meet your annual deductible first (e.g., $50-$150).
- Co-insurance: After your deductible, insurance usually covers 50-80% of the allowable fee. So, you'd pay the remaining 20-50% (your co-insurance).
- Annual Maximum: Be aware of your plan's annual maximum coverage (e.g., $1,000-$2,000). If your deep cleaning plus other procedures exceed this, you'll pay out-of-pocket for the remainder.
- Example: If a deep cleaning costs $1,600 (4 quadrants at $400 each), and your plan covers 80% after a $100 deductible:
- You pay the $100 deductible.
- Remaining balance: $1,500.
- Insurance pays 80% of $1,500 = $1,200.
- You pay the remaining 20% of $1,500 = $300.
- Total out-of-pocket: $100 (deductible) + $300 (co-insurance) = $400.
Payment Plans and Financing Options
Many dental offices understand the financial burden of deep cleaning and offer various payment solutions:
- In-Office Payment Plans: Some practices allow you to pay in installments over several months, often without interest.
- Third-Party Financing (e.g., CareCredit): These are healthcare credit cards that offer special financing options, including interest-free periods if paid in full within a certain timeframe (e.g., 6, 12, or 18 months).
- Dental Discount Plans: These are not insurance but membership plans where you pay an annual fee and get reduced rates on dental services from participating providers. Discounts can range from 10% to 60%.
Cost-Saving Tips
- Shop Around: Get estimates from a few different dental offices in your area. Prices can vary.
- Ask About Cash Discounts: Many offices offer a percentage discount (e.g., 5-10%) for patients paying in full with cash.
- Utilize Your Insurance: Understand your benefits and maximize your coverage, especially if you have a deductible or annual maximum that resets at the end of the year.
- Preventive Care: The most effective cost-saving tip is to prevent the need for deep cleaning altogether through diligent oral hygiene and regular check-ups. Catching gingivitis early is much less expensive than treating periodontitis.
- Dental Schools: University dental schools often provide services at a reduced cost, as procedures are performed by students under the supervision of experienced faculty.
Remember to always request a detailed treatment plan and cost estimate before proceeding with deep cleaning, so you have a clear understanding of the financial commitment.
Frequently Asked Questions
Is deep cleaning teeth painful?
The procedure itself is typically not painful because local anesthesia is administered to numb the gums and teeth. You may feel some pressure or vibrations, but sharp pain should be minimal. After the anesthesia wears off, it's common to experience some soreness, tenderness, and sensitivity for a few days, which can usually be managed with over-the-counter pain relievers.
How long does a deep cleaning take?
A deep cleaning usually takes longer than a routine cleaning. It's often divided into multiple appointments, with each appointment lasting 45 minutes to 90 minutes per quadrant or two. For a full mouth deep cleaning, it could take a total of 2 to 4 hours spread across several visits.

How often do I need a deep cleaning?
A deep cleaning is generally a one-time intensive treatment for active periodontitis. After the initial deep cleaning, you will typically need to schedule more frequent follow-up appointments called "periodontal maintenance cleanings," usually every 3 to 4 months, to prevent the disease from recurring.
What are the alternatives to deep cleaning?
For moderate periodontitis, deep cleaning (scaling and root planing) is the gold standard non-surgical treatment. If gum disease is very mild (gingivitis), regular cleanings and improved oral hygiene are sufficient. For advanced periodontitis, surgical options like flap surgery, bone grafts, or gum grafts may be necessary if deep cleaning is not enough.
Can gum disease return after deep cleaning?
Yes, gum disease can absolutely return if proper aftercare and maintenance are not followed. Deep cleaning removes existing bacteria and calculus, but diligent daily oral hygiene (brushing, flossing) and regular periodontal maintenance appointments (every 3-4 months) are crucial to prevent plaque and calculus from reaccumulating and causing recurrence.
What happens if I don't get a deep cleaning?
If you have periodontitis and don't get a deep cleaning, the disease will likely progress. The bacterial infection will continue to destroy the bone and soft tissues supporting your teeth, leading to deepening periodontal pockets, increased gum recession, tooth mobility, persistent bad breath, pain, and eventually, tooth loss. Untreated gum disease can also impact your overall systemic health.
How soon after deep cleaning can I eat normally?
It's generally recommended to stick to soft foods for the first 24-48 hours after your deep cleaning, especially avoiding very hot, cold, spicy, acidic, crunchy, or chewy foods. You can gradually reintroduce your normal diet as your gums feel more comfortable, typically within a few days.
Is deep cleaning covered by insurance?
Most dental insurance plans do cover a significant portion of deep cleaning, as it's considered a necessary procedure for treating gum disease. Coverage typically ranges from 50% to 80% after your deductible is met. It's essential to check your specific policy for details on coverage levels, deductibles, co-pays, and any waiting periods.
Can deep cleaning help bad breath?
Yes, deep cleaning can significantly help reduce or eliminate bad breath (halitosis) caused by gum disease. By removing the bacteria, plaque, and calculus that accumulate in periodontal pockets and release foul-smelling gases, deep cleaning addresses a primary source of chronic bad breath.
Will deep cleaning make my teeth sensitive?
Temporary tooth sensitivity is a common side effect after deep cleaning. This occurs because the procedure exposes parts of the tooth root that were previously covered by inflamed gum tissue or calculus. This sensitivity usually subsides within a few days to a few weeks. Using desensitizing toothpaste can help manage this discomfort.
When to See a Dentist
Recognizing the signs and knowing when to seek professional dental care is paramount to preventing the progression of gum disease and avoiding more severe interventions.
Immediate Attention (Red Flags)
You should schedule an immediate appointment with your dentist if you experience any of the following:
- Sudden, severe, or persistent tooth pain that doesn't subside.
- Excessive bleeding from your gums that doesn't stop, especially outside of brushing/flossing.
- Visible pus coming from your gums or around a tooth.
- A loose or shifting tooth that you notice wasn't loose before.
- Persistent swelling in your gums, face, or jaw that is painful or growing.
- Difficulty chewing or a sudden change in your bite.
These symptoms could indicate an active infection, an abscess, or rapidly progressing gum disease that requires urgent care.
Scheduled Appointment (Warning Signs of Gum Disease)
If you notice any of these signs, you should schedule a non-emergency appointment with your dentist soon:
- Red, swollen, or tender gums.
- Gums that bleed easily when you brush or floss.
- Persistent bad breath or a bad taste in your mouth.
- Gums that appear to be pulling away from your teeth (receding gums).
- Increased sensitivity to hot or cold temperatures.
- Any concerns about your gum health or changes you've observed.
These are classic indicators of gingivitis or early to moderate periodontitis, which can often be effectively managed with professional intervention like a deep cleaning.
Routine Care Guidance
Even if you don't experience any symptoms, regular dental check-ups and professional cleanings are essential.
- Adults: The ADA recommends routine dental exams and cleanings at least once or twice a year.
- Individuals with Gum Disease History: If you have a history of gum disease or have undergone deep cleaning, your dentist will likely recommend periodontal maintenance cleanings every 3-4 months.
These routine visits allow your dentist to monitor your oral health, detect problems early, remove plaque and calculus before they cause damage, and provide personalized advice for your at-home oral hygiene. Don't wait for pain or obvious problems; proactive care is the best defense against gum disease.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
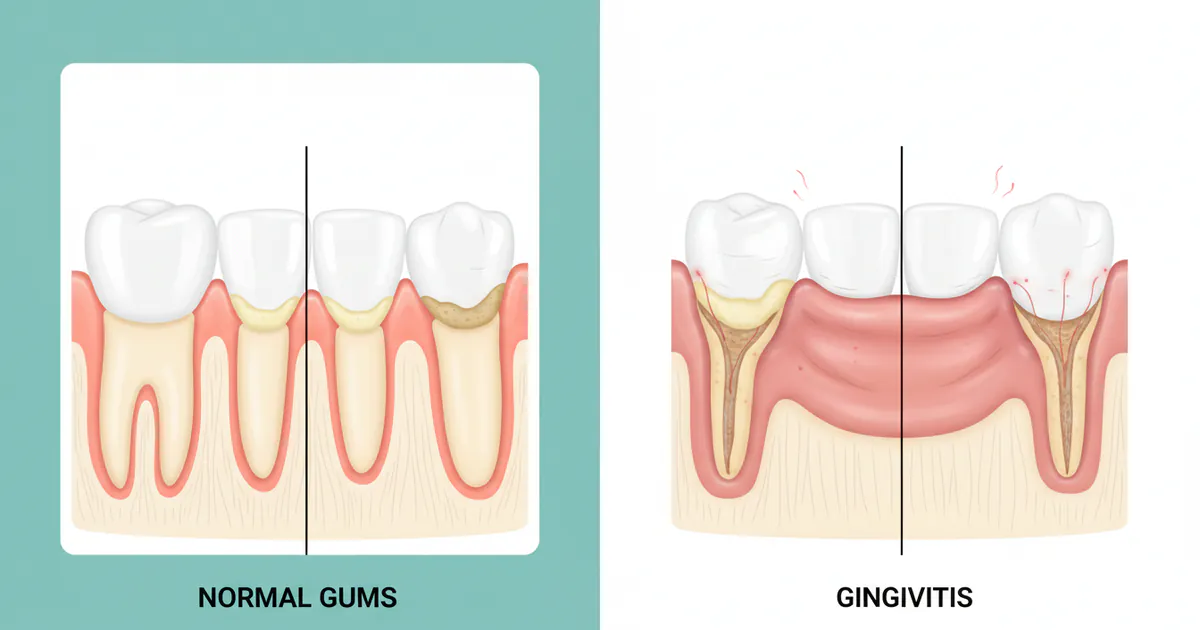
Normal Gums vs Gingivitis: Complete Comparison Guide
Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is cruc
February 22, 2026
Can You Get Rid of Gingivitis
More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good ne
February 22, 2026
What Causes Receding Gums
Receding gums, a condition where the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or the tooth's root, affects a significant portion of the adult population in the United States. In fact, estimates suggest that **up to 88% of people over the age of 65 have on
February 22, 2026
Signs of Gingivitis: Complete Guide
Did you know that nearly half of American adults aged 30 and older suffer from some form of gum disease? While that statistic might sound alarming, the good news is that the earliest and most common stage, gingivitis, is entirely reversible. Recognizing the signs of gingivitis early is your
February 22, 2026