Mouth Cancer Mouth Ulcer: Complete Guide
Key Takeaways
- Mouth Cancer Mouth Ulcer: Complete Guide
Mouth Cancer Mouth Ulcer: Complete Guide
Few sensations are as universally uncomfortable as a persistent sore in the mouth. While most mouth ulcers are benign, painful, and fleeting, lasting only a week or two, the specter of a more serious condition like oral cancer can loom large, causing understandable anxiety. Did you know that oral cancer, including mouth cancer, claims one life every hour of every day in the United States? This sobering statistic underscores why understanding the crucial differences between a common mouth ulcer and a potentially cancerous lesion is not just helpful, but vital for your long-being. This comprehensive guide from SmilePedia.net will equip you with the knowledge to distinguish between these two conditions, recognize concerning symptoms like an oral cancer lump on gum or oral cancer white spots on gums, and understand the critical steps for diagnosis, treatment, and prevention. We will delve into what each condition is, their causes, the nuanced signs and symptoms, various treatment options, associated costs, recovery expectations, and essential preventive measures, ensuring you have the complete picture for your oral health.
Key Takeaways:
- Early Detection is Crucial: While most mouth ulcers are benign, any sore, lump, or discolored patch in your mouth that doesn't heal within 2-3 weeks warrants immediate professional evaluation.
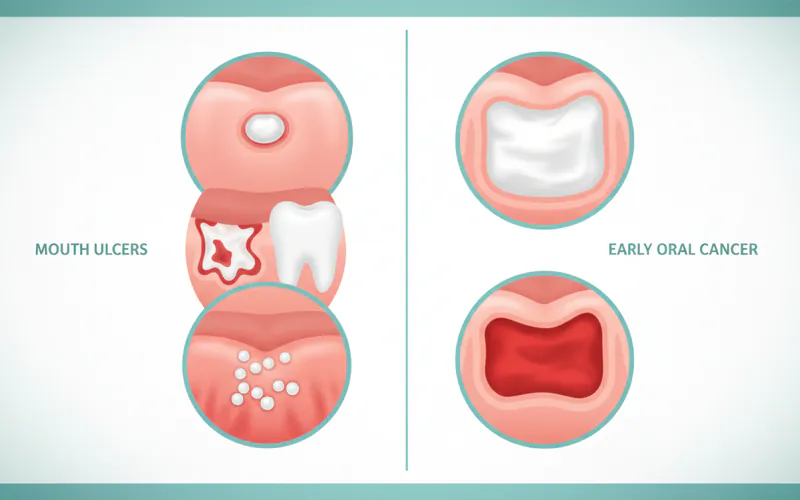
- Key Differentiators: Benign mouth ulcers are often painful, have a distinct round/oval shape with a red border and yellow/grey center, and typically heal within 7-14 days. Mouth cancer lesions are often painless in early stages, may appear as persistent red (erythroplakia) or white (leukoplakia) patches, non-healing sores, or firm lumps, and grow progressively.
- Diagnostic Process: A definitive diagnosis involves a thorough clinical examination by a dentist or oral surgeon, often followed by a biopsy. This procedure, typically costing $200-$800 in the US, is the only way to confirm cancer.
- Treatment for Oral Cancer: Treatment for mouth cancer can range from surgery (often $5,000-$50,000+ without insurance) to radiation and chemotherapy, depending on the stage. Early-stage detection significantly improves prognosis and may lead to less invasive treatments.
- Cost Considerations: While basic ulcer treatment is minimal, comprehensive oral cancer treatment can accrue costs ranging from tens of thousands to over $100,000, with significant variability based on stage, treatment modalities, and location. Insurance coverage is vital.
- Prevention is Paramount: Quitting tobacco and excessive alcohol, limiting sun exposure, and getting an HPV vaccination (if eligible) are key preventive measures for oral cancer. Regular dental check-ups, typically $75-$200 for a basic exam, include oral cancer screenings and are your first line of defense.
- Oral Self-Exams: Performing monthly self-checks of your mouth, looking for any changes, lumps, or discolored areas, can aid in early detection.
What It Is / Overview
When an abnormality appears in your mouth, it's natural to be concerned. Understanding the fundamental differences between a common mouth ulcer and mouth cancer is the first step toward informed action.

Mouth Ulcer (Aphthous Ulcer / Canker Sore)
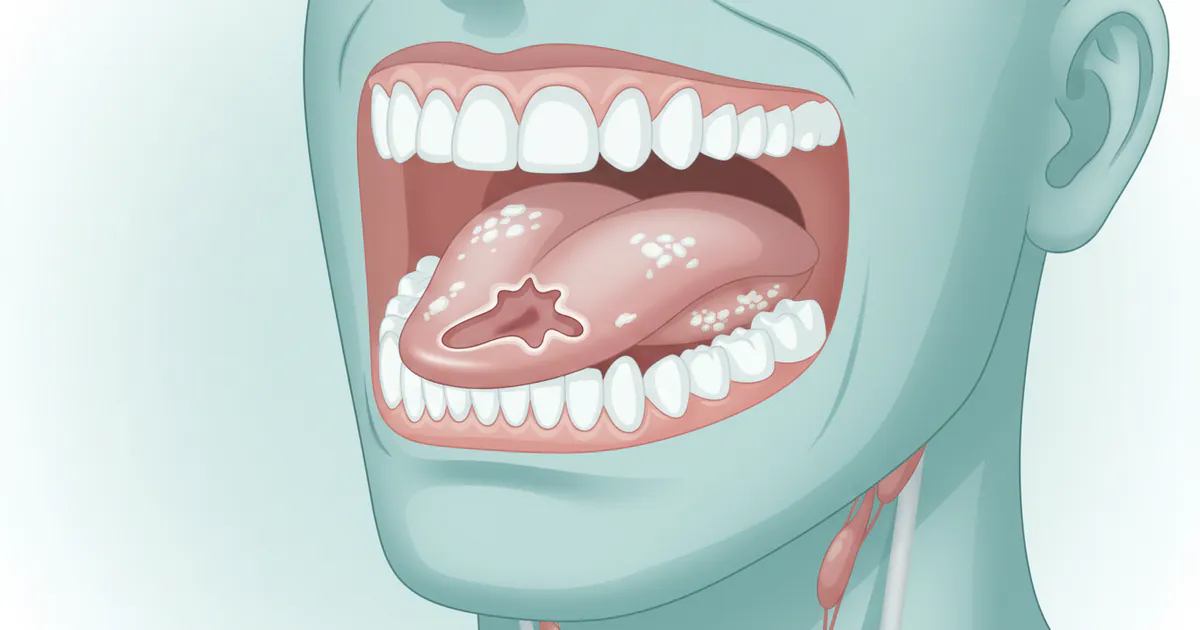
A mouth ulcer, often referred to as an aphthous ulcer or canker sore, is a common, non-contagious lesion that appears as an open sore inside the mouth. These are typically round or oval, with a distinct red border and a white, yellow, or grayish center. They can appear on the inside of the cheeks, lips, tongue, soft palate, or the base of the gums. While usually harmless, they can be quite painful, especially when eating or speaking.
Key characteristics of a benign mouth ulcer:
- Painful: Often causes significant discomfort, especially when irritated.
- Distinct Shape: Typically round or oval with clear, well-defined edges.
- Appearance: Red inflamed border, with a yellow or gray center.
- Location: Can appear almost anywhere on the movable soft tissues inside the mouth.
- Healing Time: Most heal spontaneously within 7 to 14 days, rarely extending beyond three weeks.
Mouth Cancer (Oral Cancer)
Mouth cancer, also known as oral cancer, is a type of head and neck cancer that develops in the tissues of the mouth or throat. It can appear on the lips, tongue, cheeks, floor of the mouth, hard or soft palate, sinuses, or pharynx (throat). The vast majority (over 90%) of oral cancers are squamous cell carcinomas, meaning they originate from the flat, thin cells lining the mouth and throat. Unlike benign ulcers, cancerous lesions are often insidious, growing slowly and potentially spreading to other parts of the body if not treated early.
Key characteristics of mouth cancer:
- Painless in Early Stages: A critical differentiating factor; early cancerous lesions may not cause pain, leading to delayed detection.
- Irregular Shape/Appearance: Can be irregular, raised, sunken, or have a crusty appearance. Often appears as persistent red or white patches.
- Non-Healing: A defining feature is that it does not heal within the typical 2-3 week timeframe expected for benign ulcers. Instead, it often grows or changes.
- Firmness: May feel firm or hard to the touch, unlike the soft tissue surrounding a benign ulcer.
- Location: Can appear anywhere, including areas less common for benign ulcers, such as the back of the tongue, floor of the mouth, or as an oral cancer lump on gum.
It's important to remember that while a persistent mouth cancer mouth ulcer is a primary concern, oral cancer can also manifest as other changes like unexplained bleeding, numbness, or difficulty swallowing.
Types / Variations
Understanding the different types of mouth ulcers and oral cancers can help you recognize potential issues.
Types of Mouth Ulcers
- Aphthous Ulcers (Canker Sores): The most common type.
- Minor Aphthous Ulcers: Small (under 1 cm), round/oval, heal in 1-2 weeks without scarring.
- Major Aphthous Ulcers: Larger (over 1 cm), deeper, can take several weeks to months to heal and may leave scars. Less common.
- Herpetiform Aphthous Ulcers: Clusters of tiny ulcers (2-3 mm) that merge to form larger, irregular ulcers. Despite the name, they are not caused by the herpes virus.
- Traumatic Ulcers: Caused by physical injury to the mouth, such as accidentally biting your cheek or tongue, vigorous brushing, sharp edges of teeth or dental appliances (e.g., braces, ill-fitting dentures), or burns from hot food. They usually heal once the source of trauma is removed.
- Herpetic Ulcers (Cold Sores): Caused by the Herpes Simplex Virus (HSV-1). These typically appear on the outside of the lips (fever blisters) but can occur inside the mouth, usually on the firm, immovable tissues like the hard palate or attached gingiva. They appear as small, fluid-filled blisters that rupture and crust over. Highly contagious.
- Ulcers associated with Systemic Conditions: Less common, but ulcers can be a symptom of underlying systemic diseases like Crohn's disease, celiac disease, Behçet's disease, or certain autoimmune conditions.
Types of Mouth Cancer
The vast majority of oral cancers are squamous cell carcinomas. However, other less common types can also occur:
- Squamous Cell Carcinoma (SCC): Accounts for over 90% of all oral cancers. It originates in the flat, thin cells lining the mouth and throat. These can appear as non-healing sores, persistent red (erythroplakia) or white (leukoplakia) patches, or a firm oral cancer lump on gum or other areas.
- Verrucous Carcinoma: A rare, low-grade variant of SCC, often associated with tobacco and snuff use. It appears as a slow-growing, warty, white or pink lesion with a craggy surface. While it rarely metastasizes, it can be locally destructive.
- Minor Salivary Gland Cancers: These develop in the small salivary glands located throughout the mouth lining. Types include mucoepidermoid carcinoma and adenoid cystic carcinoma. They can appear as lumps or swellings in the palate or cheek.
- Lymphoma: While rare, lymphoma can manifest in the oral cavity, often appearing as a painless swelling or mass in the soft tissues or bone.
- Melanoma: Extremely rare in the mouth, but highly aggressive. It appears as dark, pigmented lesions.
Causes / Why It Happens
Understanding the causes helps in both prevention and identifying risk factors.
Causes of Mouth Ulcers
- Trauma: Accidental biting, aggressive brushing, sharp food, dental appliances.
- Stress and Anxiety: Emotional stress is a common trigger for aphthous ulcers.
- Nutritional Deficiencies: Lack of iron, folic acid, zinc, or B vitamins (especially B12).
- Food Sensitivities: Certain foods like chocolate, coffee, cheese, nuts, acidic fruits (lemons, oranges, pineapples), and spicy foods can trigger ulcers in some individuals.
- Hormonal Changes: Fluctuations during menstruation or pregnancy.
- Sodium Lauryl Sulfate (SLS): A foaming agent found in many toothpastes and mouthwashes; some individuals are sensitive to it.
- Systemic Diseases: As mentioned, conditions like Crohn's disease, celiac disease, weakened immune systems.
- Medications: Certain drugs can cause oral ulcers as a side effect.
Causes of Mouth Cancer
Oral cancer development is often multifactorial, meaning several risk factors combine to increase the likelihood.
- Tobacco Use: By far the leading cause. This includes cigarettes, cigars, pipes, chewing tobacco, snuff, and even vaping. The carcinogens in tobacco products directly damage oral tissues.
- Alcohol Consumption: Heavy and prolonged alcohol use significantly increases risk. When combined with tobacco, the risk multiplies dramatically (synergistic effect).
- Human Papillomavirus (HPV) Infection: Specifically HPV-16, is a growing cause of oropharyngeal cancers (cancers of the back of the throat, base of the tongue, and tonsils). Oral sex is a primary mode of transmission.
- Sun Exposure: Prolonged and unprotected exposure to UV radiation is a primary cause of lip cancer.
- Age: The risk increases with age, with most oral cancers diagnosed in people over 40.
- Diet and Nutrition: A diet poor in fruits and vegetables, and rich in processed foods, may increase risk.
- Genetics/Family History: A family history of head and neck cancer may slightly increase your risk, though genetics play a lesser role than lifestyle factors.
- Weakened Immune System: Individuals with compromised immune systems are at a higher risk.
- Poor Oral Hygiene and Chronic Irritation: While not a direct cause, chronic irritation from rough dentures or sharp teeth combined with other risk factors might contribute. Persistent irritation, however, usually doesn't cause cancer on its own.
- Previous Cancer Diagnosis: Individuals who have had one type of cancer, especially head and neck cancer, are at higher risk for developing a second primary cancer.
Pro Tip: If you use tobacco or drink alcohol regularly, understand that these habits dramatically increase your risk of developing mouth cancer. Quitting these habits is the single most impactful step you can take to reduce your risk.
Signs and Symptoms
This section is crucial for differentiating between a benign ulcer and a potentially cancerous lesion. Pay close attention to persistence and appearance.
Signs and Symptoms of a Benign Mouth Ulcer
- Pain: Typically the most prominent symptom, ranging from mild to severe, especially when eating or speaking.
- Appearance: A small, well-defined lesion, usually round or oval, with a distinct red border and a white, yellow, or gray center.
- Location: Can appear on any movable soft tissue inside the mouth (cheeks, lips, tongue, soft palate, floor of the mouth).
- Onset: Often appears suddenly.
- Healing: Heals completely within 7-14 days, rarely exceeding three weeks, without scarring (except for major aphthous ulcers).
- No Associated Swelling: Generally, no significant external swelling or lymph node involvement.
Signs and Symptoms of Mouth Cancer
Oral cancer can be insidious, often presenting with subtle or painless symptoms in its early stages. Persistence is the key red flag.
- Non-healing Sore or Ulcer: This is the most common and critical sign. A sore, lesion, or ulcer in the mouth that does not heal within 2-3 weeks is highly suspicious and requires immediate evaluation. Unlike benign ulcers, it may not be painful.
- Red or White Patches (Erythroplakia and Leukoplakia):
- Leukoplakia: Oral cancer white spots on gums or other areas. These are thick, white, or grayish patches that cannot be scraped off. While many are benign, some (especially speckled leukoplakia) are precancerous or cancerous.
- Erythroplakia: Red patches that are often flat or slightly raised. These are less common than leukoplakia but have a much higher risk (up to 90%) of being precancerous or cancerous. Any persistent red patch is a significant red flag.
- Lump, Thickening, or Swelling: A persistent oral cancer lump on gum, cheek, tongue, or anywhere in the mouth or neck area that doesn't resolve. It may feel firm or hard.
- Persistent Sore Throat or Hoarseness: A chronic sore throat, a feeling of something caught in your throat, or a change in voice quality (hoarseness) that lasts for more than a few weeks.
- Difficulty Swallowing (Dysphagia) or Chewing: Pain or difficulty when swallowing food or liquids, or difficulty chewing.
- Difficulty Moving the Jaw or Tongue: Stiffness or pain when trying to open the mouth wide, move the tongue, or speak.
- Unexplained Numbness or Pain/Tenderness: Numbness, tingling, or persistent localized pain in the face, mouth, or neck without an obvious cause.
- Unexplained Bleeding: Any persistent, unexplained bleeding from the mouth.
- Changes in Fit of Dentures: If dentures suddenly feel uncomfortable or ill-fitting.
- Weight Loss: Unexplained and significant weight loss.
- Persistent Earache: A persistent earache in one ear that is not associated with an infection and that can signal cancer in the back of the throat.
Pro Tip: Perform a monthly self-oral cancer screening. In a well-lit room, use a mirror to systematically check your lips (inside and out), gums, cheeks, tongue (top, sides, and underneath), roof of your mouth, and the floor of your mouth. Feel for any lumps or tender areas.
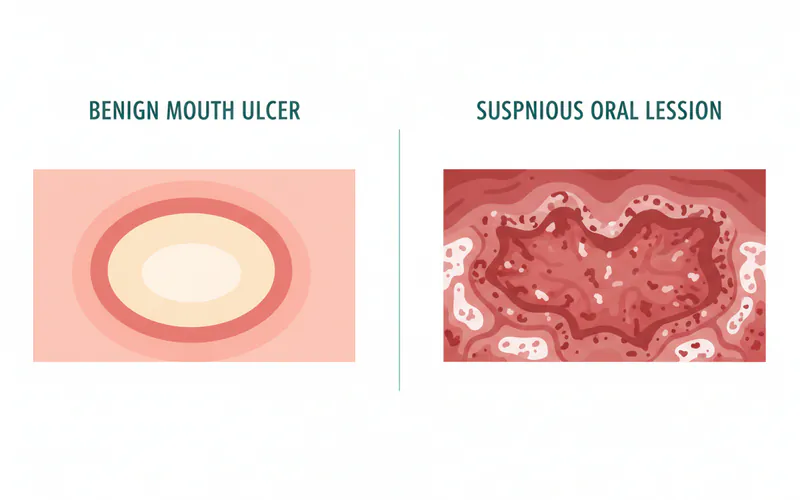
| Feature | Benign Mouth Ulcer (Canker Sore) | Suspicious Oral Lesion (Potential Mouth Cancer) |
|---|---|---|
| Pain Level | Often painful, especially upon irritation | Often painless in early stages |
| Appearance | Round/oval, red border, yellow/gray center | Irregular shape, red (erythroplakia) or white (leukoplakia) patches, raised or sunken, may bleed easily, firm texture |
| Healing Time | Heals within 7-14 days (max 3 weeks) | Does not heal within 2-3 weeks; grows or changes over time |
| Texture | Soft tissue surrounding the lesion | Firm, hard, or indurated to the touch |
| Associated Lumps | Generally none | May present as a persistent lump or thickening (e.g., oral cancer lump on gum) |
| Other Symptoms | No general systemic symptoms | Difficulty swallowing/chewing, persistent sore throat, numbness, unexplained bleeding, weight loss, difficulty moving jaw/tongue |
| Contagious? | No | No |
Treatment Options
Treatment approaches differ dramatically for benign mouth ulcers versus oral cancer.
Treatment for Mouth Ulcers
Most benign mouth ulcers resolve on their own. Treatment focuses on pain relief and accelerating healing.
- Home Remedies:
- Saltwater Rinses: Rinse with warm salt water several times a day to soothe and clean the area.
- Baking Soda Paste: A mixture of baking soda and water applied directly to the ulcer can help neutralize acids and reduce pain.
- Honey: Has antiseptic and anti-inflammatory properties.
- Avoiding Irritants: Steer clear of spicy, acidic, or abrasive foods and hot beverages.
- Over-the-Counter (OTC) Products:
- Topical Anesthetics: Gels or sprays containing benzocaine (e.g., Orajel, Anbesol) to numb the area.
- Protective Pastes/Gels: Products that form a protective barrier over the ulcer (e.g., Kanka, Orabase) to shield it from irritation.
- Antiseptic Mouthwashes: Alcohol-free mouthwashes can help keep the area clean and prevent secondary infection.
- Prescription Medications (for severe or persistent ulcers):
- Topical Steroids: Prescription gels or pastes (e.g., triamcinolone acetonide) can reduce inflammation and speed healing.
- Antimicrobial Rinses: Chlorhexidine mouth rinse may be prescribed to reduce bacteria.
- Systemic Medications: In very severe cases of recurrent aphthous stomatitis, systemic corticosteroids or immunomodulators may be considered by a specialist.
Pros of Ulcer Treatment:
- Pain relief.
- Faster healing.
- Prevention of secondary infection. Cons of Ulcer Treatment:
- Most are temporary symptom relief, not a cure for recurrence.
- Some OTC products can cause temporary numbness or altered taste.
Treatment for Mouth Cancer
Treatment for oral cancer is complex and depends heavily on the stage of cancer, its location, the patient's overall health, and whether the cancer has spread. A multidisciplinary team (oral surgeon, oncologist, radiation oncologist, dietitian, speech therapist) typically coordinates care.
-
Surgery: The primary treatment for most oral cancers, especially in early stages.
- Tumor Excision: The cancerous tissue and a margin of healthy tissue around it are surgically removed.
- Neck Dissection: If cancer has spread to lymph nodes in the neck, or if there's a high risk of spread, these lymph nodes are removed.
- Reconstructive Surgery: After significant tissue removal, reconstructive surgery (using tissue from other parts of the body) may be necessary to restore appearance and function (speech, swallowing).
- Pros: Often curative for early-stage cancers; allows for pathological examination of the removed tissue.
- Cons: Can be extensive, leading to changes in facial appearance, speech, and swallowing; risk of infection, bleeding, nerve damage.
-
Radiation Therapy: Uses high-energy rays to kill cancer cells.
- External Beam Radiation: A machine outside the body delivers radiation.
- Brachytherapy: Radioactive seeds or wires are placed directly into or near the tumor.
- Pros: Can be used alone for early-stage cancers, or in combination with surgery (adjuvant therapy) or chemotherapy. Can preserve organs and function in some cases.
- Cons: Significant side effects including dry mouth (xerostomia), difficulty swallowing, mouth sores (mucositis), changes in taste, fatigue, and potential long-term damage to bone (osteoradionecrosis).
-
Chemotherapy: Uses drugs to kill cancer cells, often administered intravenously.
- Pros: Can shrink large tumors before surgery or radiation, kill remaining cancer cells after surgery, or treat widespread cancer.
- Cons: Significant systemic side effects (nausea, vomiting, hair loss, fatigue, weakened immune system, mouth sores).
-
Targeted Therapy: Drugs that target specific molecules involved in cancer growth and spread.
- Pros: Can be more precise than chemotherapy, often with fewer side effects.
- Cons: Only works for cancers with specific molecular targets; resistance can develop.
-
Immunotherapy: Helps the body's immune system fight cancer.
- Pros: Can be effective for advanced or recurrent cancers; may offer long-term control for some patients.
- Cons: Can have unique immune-related side effects; not effective for all patients.
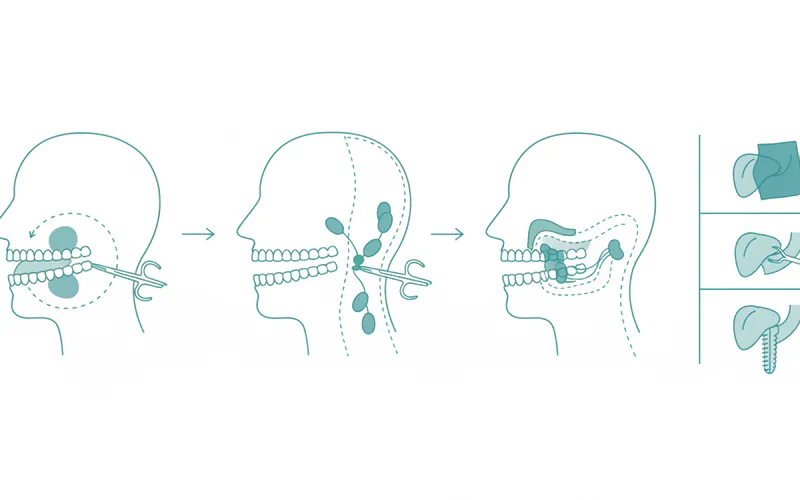
Step-by-Step Process (Diagnosis and Treatment)
Here’s what to expect if you present with a suspicious oral lesion.
Step 1: Initial Examination and Evaluation (Dental Office)
- Oral Cancer Screening: Your dentist will perform a visual and tactile examination of your entire mouth, throat, and neck during routine check-ups. They'll look for any red or white patches, lumps, or non-healing sores.
- Discussion of Symptoms: You'll be asked about your symptoms, duration, pain level, and risk factors (tobacco, alcohol, HPV history).
- Referral: If a suspicious lesion is found, your dentist will likely refer you to an oral surgeon or an ear, nose, and throat (ENT) specialist for further evaluation.
Step 2: Diagnostic Procedures (Specialist's Office)
- Advanced Imaging (Optional, but common): Your specialist may order imaging tests like CT scans, MRI, or PET scans to assess the extent of the lesion and check for spread to lymph nodes or other parts of the body.
- Biopsy: This is the definitive diagnostic step.
- Incisional Biopsy: A small piece of the suspicious tissue is surgically removed under local anesthesia.
- Excisional Biopsy: If the lesion is small, the entire lesion might be removed.
- Brush Biopsy: Less invasive, using a special brush to collect cells, but less definitive than an incisional biopsy and often requires follow-up with incisional biopsy if positive.
- Pathology Report: The tissue sample is sent to a pathologist who examines it under a microscope to determine if cancer cells are present and, if so, the type and grade of cancer. This report is critical for treatment planning.
Step 3: Staging (If Cancer is Confirmed)
- TNM Classification: Cancer is staged using the TNM system (Tumor, Node, Metastasis), which describes the size of the primary tumor (T), whether it has spread to nearby lymph nodes (N), and whether it has metastasized to distant sites (M).
- Team Consultation: An oncology team reviews all findings to determine the most appropriate treatment plan.
Step 4: Treatment Implementation
- Surgery: If surgery is the chosen primary treatment, it will be scheduled. This could range from a simple excision to extensive removal of tissue, bone, or lymph nodes, potentially followed by reconstructive surgery.
- Adjuvant Therapies: Depending on the pathology report and staging, radiation therapy, chemotherapy, or a combination may follow surgery to destroy any remaining cancer cells and reduce the risk of recurrence.
- Primary Radiation/Chemotherapy: For some advanced cancers or if surgery is not feasible, radiation and/or chemotherapy might be the primary treatment.
Step 5: Follow-up and Surveillance
- Regular Check-ups: Frequent follow-up appointments with your oncology team are crucial to monitor recovery, manage side effects, and check for recurrence.
- Imaging: Periodic imaging tests may be performed.
- Rehabilitation: May include speech therapy, swallowing therapy, and nutritional counseling to help recover function.
Cost and Insurance
The financial burden of oral health issues, particularly oral cancer, can be significant. Costs vary widely across the US due to geographic location, facility fees, and the complexity of the case.
Cost of Mouth Ulcer Treatment (Self-Pay/Out-of-Pocket)
- Home Remedies: Minimal to none (cost of salt, baking soda, honey).
- Over-the-Counter Products: $5 - $20 for topical anesthetics, protective pastes, or antiseptic rinses.
- Dental Visit for Diagnosis/Prescription:
- Consultation/Exam: $75 - $200
- Prescription Medication (e.g., topical steroid): $10 - $50 (with a coupon or insurance)
- Total for a typical ulcer: $5 - $200
Cost of Oral Cancer Diagnosis and Treatment (Self-Pay/Out-of-Pocket Estimates)
These are broad ranges, as the specifics are highly individualized.
- Initial Specialist Consultation (Oral Surgeon/ENT): $200 - $600
- Biopsy (Incisional):
- Procedure fee: $200 - $800
- Pathology analysis: $150 - $400
- Total for biopsy: $350 - $1,200
- Imaging (without insurance):
- CT Scan: $500 - $3,000
- MRI: $700 - $4,000
- PET Scan: $1,500 - $7,000
- Surgery (highly variable):
- Early-stage tumor excision: $5,000 - $20,000
- Extensive surgery with neck dissection and reconstruction: $25,000 - $100,000+
- Includes surgeon's fees, anesthesia, hospital fees.
- Radiation Therapy:
- Full course (25-35 sessions): $20,000 - $70,000+
- Chemotherapy:
- Each cycle: $1,000 - $10,000+, with multiple cycles often needed.
- Targeted Therapy/Immunotherapy:
- Can be tens of thousands of dollars per month for certain drugs.
- Rehabilitation (Speech/Swallowing Therapy): $50 - $200 per session, multiple sessions over weeks/months.
- Follow-up Appointments: $100 - $500 per visit, plus imaging costs.
Total Cost for Oral Cancer Treatment: Without insurance, the total cost for a full course of oral cancer treatment can range from $30,000 for early-stage localized cancer to well over $150,000 for advanced cases requiring multiple modalities and extensive reconstruction.
Insurance Coverage
- Medical Insurance: Oral cancer diagnosis and treatment are generally covered by standard medical health insurance plans. Coverage will depend on your specific plan's deductibles, co-payments, and out-of-pocket maximums. It's crucial to understand your plan's benefits for oncology services, hospital stays, and specialist visits.
- Dental Insurance: Dental insurance typically covers diagnostic procedures like biopsies and some oral surgeries, especially if performed by an oral surgeon. However, major cancer treatments like radiation, chemotherapy, and extensive reconstructive surgery that involves multiple body parts usually fall under medical insurance. Some dental plans may cover immediate post-treatment dental rehabilitation, like prosthetics.
- Navigating Costs:
- Pre-authorization: Always get pre-authorization from your insurance company for major procedures and treatments.
- Financial Counselors: Most hospitals and cancer centers have financial counselors who can help you understand your insurance coverage, estimate costs, and explore financial assistance programs.
- Payment Plans: Discuss payment plans with your providers for out-of-pocket expenses.
- Patient Assistance Programs: Pharmaceutical companies and non-profit organizations offer programs to help cover the cost of medications or treatment.
Pro Tip: Early detection of oral cancer not only dramatically improves survival rates but can also lead to less extensive and therefore less costly treatment. Regular dental check-ups, which include oral cancer screenings, are an affordable investment in your long-term health.
| Aspect | Benign Mouth Ulcer (Self-Pay) | Early-Stage Oral Cancer (Self-Pay) | Advanced Oral Cancer (Self-Pay) |
|---|---|---|---|
| Initial Visit | $75 - $200 (dentist) | $200 - $600 (specialist) | $200 - $600 (specialist) |
| Diagnostic Tests | N/A (clinical diagnosis) | $350 - $1,200 (biopsy) | $2,000 - $10,000+ (biopsy, multiple scans) |
| Primary Treatment | $5 - $50 (OTC/Rx) | $5,000 - $20,000 (surgery) | $25,000 - $100,000+ (extensive surgery, radiation, chemo) |
| Additional Therapies | N/A | $20,000 - $70,000 (radiation, if needed) | $20,000 - $100,000+ (radiation, multiple chemo cycles, targeted/immuno) |
| Rehabilitation/Aftercare | N/A | $500 - $5,000 | $5,000 - $20,000+ |
| Estimated Total Range | $5 - $250 | $25,000 - $90,000 | $75,000 - $250,000+ |
| Insurance Coverage | Often out-of-pocket or minor dental | Primarily medical insurance | Primarily medical insurance |
Recovery and Aftercare
Recovery and aftercare differ vastly depending on the condition and treatment received.
Recovery and Aftercare for Mouth Ulcers
- Healing Time: Most minor aphthous ulcers heal within 7-14 days. Major ulcers may take longer. Traumatic ulcers heal once the irritant is removed.
- Pain Management: Continue with warm saltwater rinses, OTC pain relievers (e.g., ibuprofen, acetaminophen), and topical anesthetics as needed.
- Diet: Stick to soft, bland, cool foods. Avoid anything spicy, acidic, hot, or abrasive that could irritate the ulcer.
- Oral Hygiene: Continue gentle brushing and flossing to prevent secondary infection, being careful around the ulcer.
- Prevention of Recurrence: Identify and avoid triggers if possible (stress, certain foods, SLS toothpastes). Ensure adequate nutrition.

Recovery and Aftercare for Mouth Cancer
Recovery from oral cancer treatment can be a long and challenging process, often involving physical, emotional, and psychological support.
- Post-Surgical Care:
- Pain Management: Prescription pain medication will be provided.
- Wound Care: Instructions for caring for surgical sites in the mouth or neck.
- Dietary Modifications: A soft or liquid diet may be necessary initially, often with a feeding tube if swallowing is severely compromised.
- Speech and Swallowing Therapy: Critical for regaining function, often starting soon after surgery.
- Managing Radiation/Chemotherapy Side Effects:
- Oral Mucositis (Mouth Sores): Painful sores are common. Rinsing with prescribed mouthwashes, pain control, and adhering to a bland, soft diet are essential.
- Dry Mouth (Xerostomia): A long-term side effect of radiation. Use saliva substitutes, drink plenty of water, chew sugar-free gum, and avoid caffeine/alcohol. Good oral hygiene is paramount to prevent rampant dental decay due to lack of saliva.
- Taste Changes: Foods may taste different or bland. Experiment with different seasonings and temperatures.
- Fatigue: Rest is crucial.
- Nutritional Support: A registered dietitian will help ensure adequate caloric and nutrient intake, often through supplements or specialized formulas.
- Physical and Emotional Rehabilitation:
- Physical Therapy: To regain range of motion in the neck and shoulders after surgery or radiation.
- Psychological Support: Cancer diagnosis and treatment can take a significant emotional toll. Counseling, support groups, and connecting with others who have undergone similar experiences can be invaluable.
- Dental Rehabilitation: Prosthetics, dentures, or implants may be needed to replace lost teeth or structures after extensive surgery. Regular dental care is vital to manage dry mouth and prevent further dental issues.
- Long-Term Follow-up:
- Surveillance: Regular check-ups with your oncology team are critical for several years to monitor for recurrence and manage late-stage side effects. The American Dental Association (ADA) recommends regular follow-ups for oral cancer survivors.
- Smoking/Alcohol Cessation: If you haven't already, complete cessation of tobacco and alcohol is imperative to prevent recurrence or a second primary cancer.
Prevention
Prevention strategies for mouth ulcers and mouth cancer differ but share a common theme: good oral health and healthy lifestyle choices.
Prevention of Mouth Ulcers
- Identify and Avoid Triggers: Pay attention to what might trigger your ulcers (e.g., certain foods, stress, SLS in toothpaste).
- Good Oral Hygiene: Gentle but thorough brushing with a soft-bristled toothbrush and daily flossing helps maintain a healthy oral environment and prevents infections.
- Manage Stress: Techniques like meditation, yoga, or adequate sleep can reduce stress-related ulcers.
- Balanced Diet: Ensure adequate intake of vitamins and minerals, especially B vitamins, iron, and folic acid.
- Address Dental Issues: Smooth sharp tooth edges or adjust ill-fitting dentures.
- Stay Hydrated: Drink plenty of water.
Prevention of Mouth Cancer
Many cases of oral cancer are preventable through lifestyle modifications and vaccinations.
- Avoid Tobacco in All Forms: This is the single most effective preventive measure. The risk of developing oral cancer drops significantly after quitting.
- Limit Alcohol Consumption: Moderate or avoid alcohol, especially if you also use tobacco.
- HPV Vaccination: The HPV vaccine (Gardasil 9) is recommended by the CDC for adolescents and young adults (typically up to age 26, and in some cases up to 45 after discussion with a doctor) to prevent HPV-related cancers, including oropharyngeal cancers.
- Sun Protection for Lips: Use lip balms with SPF, wear wide-brimmed hats when outdoors, and seek shade to protect your lips from UV radiation.
- Balanced Diet Rich in Fruits and Vegetables: A diet rich in antioxidants found in fresh produce may help protect against various cancers.
- Regular Dental Check-ups: Visit your dentist at least twice a year. Dentists and dental hygienists are trained to perform oral cancer screenings during routine exams. Early detection is often the key to successful treatment.
- ADA Recommendation: The American Dental Association emphasizes the importance of routine oral exams, including visual and tactile inspections for oral cancer.
- Perform Monthly Oral Self-Exams: Take a few minutes each month to systematically check your mouth for any changes.
- Know Your Family History: While not a primary risk factor, being aware of a family history of head and neck cancers can prompt more diligent screening.
Risks and Complications
Both mouth ulcers and mouth cancer can lead to complications, though cancer carries far more severe risks.
Risks and Complications of Mouth Ulcers
- Secondary Infection: An open sore can become infected by bacteria or fungi, especially if oral hygiene is poor.
- Pain and Discomfort: Can interfere with eating, speaking, and overall quality of life.
- Nutritional Deficiencies: Severe or numerous ulcers can make eating painful, potentially leading to inadequate nutrient intake.
- Recurrence: For those prone to aphthous ulcers, they often recur.
- Scarring: Large or deep ulcers (major aphthous ulcers) can leave scars.
Risks and Complications of Mouth Cancer
The risks and complications associated with oral cancer are extensive and can be life-altering.
- Metastasis (Spread): The most serious complication. Cancer cells can spread from the mouth to nearby lymph nodes in the neck, and then to distant parts of the body (lungs, liver, bones), making treatment more difficult and prognosis poorer.
- Recurrence: Even after successful treatment, oral cancer can recur in the original site or develop as a new primary cancer elsewhere in the mouth or throat.
- Functional Impairment:
- Speech Difficulties (Dysarthria): Removal of parts of the tongue, jaw, or soft palate can affect articulation.
- Swallowing Difficulties (Dysphagia): Can lead to malnutrition, weight loss, and aspiration (food or liquid entering the airway).
- Chewing Problems: Due to loss of teeth, jaw bone, or muscle function.
- Disfigurement: Extensive surgery, especially with removal of jawbone or soft tissues, can significantly alter facial appearance, leading to body image issues.
- Quality of Life Impact: Chronic pain, dry mouth, altered taste, speech/swallowing difficulties, and emotional distress can severely impact a patient's quality of life.
- Treatment-Related Complications:
- Osteoradionecrosis: Damage to the jawbone from radiation, leading to bone death and potential infection, which is difficult to treat.
- Trismus: Restricted jaw opening due to scarring or muscle damage from radiation or surgery.
- Nerve Damage: Can result in numbness, weakness, or altered sensation in the face, tongue, or jaw.
- Thyroid Dysfunction: Radiation to the neck can affect the thyroid gland.
- Dental Issues: Increased risk of tooth decay, gum disease, and tooth loss due to dry mouth from radiation or salivary gland damage.
Children / Pediatric Considerations
While mouth ulcers are common in children, mouth cancer is extremely rare in this age group.
- Mouth Ulcers in Children: Children frequently develop mouth ulcers due to minor trauma (biting cheek, toothbrush injury), viral infections (e.g., hand, foot, and mouth disease, herpetic gingivostomatitis), or canker sores similar to adults. Stress or nutritional deficiencies can also play a role.
- When to Worry: If an ulcer in a child is unusually large, extremely painful, persistent for more than 2 weeks, accompanied by high fever or severe fatigue, or if the child is unable to eat or drink due to pain, a dental or medical evaluation is warranted.
- Oral Cancer in Children: Oral cancer in children is exceptionally rare. When it does occur, it may present differently than in adults (e.g., rhabdomyosarcoma, lymphoma). Any persistent lump, swelling, or non-healing sore in a child's mouth should be evaluated by a pediatrician or pediatric dentist, even if the risk of cancer is very low. Genetic syndromes can predispose some children to certain cancers.
- HPV Vaccination: It's important to remember that HPV vaccination is recommended for pre-teens (around ages 11-12) to protect them from HPV-related cancers, including those of the oropharynx, later in life.
Cost Breakdown (for US Market)
Let's summarize the costs more clearly. These are average ranges and can fluctuate based on region (e.g., urban vs. rural), facility type (hospital vs. outpatient clinic), and specific provider fees.
Average US Costs:
- Dentist Consultation/Exam: $75 - $200
- Specialist (Oral Surgeon/ENT) Consultation: $200 - $600
- Incisional Biopsy (including pathology): $350 - $1,200
- CT Scan (without insurance): $500 - $3,000
- MRI (without insurance): $700 - $4,000
- PET Scan (without insurance): $1,500 - $7,000
- Oral Cancer Surgery (localized, early stage): $5,000 - $20,000
- Oral Cancer Surgery (extensive with reconstruction): $25,000 - $100,000+
- Course of Radiation Therapy: $20,000 - $70,000+
- Chemotherapy (per cycle): $1,000 - $10,000+
- Speech/Swallowing Therapy (per session): $50 - $200
With vs. Without Insurance:
- With Insurance (Medical): For oral cancer, medical insurance will cover a significant portion after deductibles and co-payments are met. Out-of-pocket maximums typically range from $3,000 to $10,000 per year for individual plans, limiting your total exposure. However, you'll still be responsible for these amounts.
- Without Insurance: As detailed above, the costs are substantial, ranging from tens of thousands to hundreds of thousands of dollars for comprehensive oral cancer treatment.
Payment Plans and Financing Options:
- Hospital Financial Assistance: Many hospitals offer financial assistance programs or charity care for uninsured or underinsured patients.
- Payment Plans: Discuss payment plans directly with your healthcare providers. Many offer interest-free monthly installments.
- Medical Credit Cards: Options like CareCredit offer financing for healthcare expenses, often with deferred interest periods.
- Patient Advocacy Groups: Organizations like the Oral Cancer Foundation or the American Cancer Society can provide resources for financial assistance.
Cost-Saving Tips:
- Preventive Care: Regular dental check-ups are cost-effective prevention.
- Early Detection: The earlier oral cancer is detected, the less extensive and costly the treatment is likely to be.
- Understand Your Insurance: Know your plan's deductibles, co-pays, and out-of-pocket maximums before treatment.
- Generic Medications: Ask your doctor if generic versions of prescribed drugs are available.
- Shop Around: For non-emergency procedures or diagnostic tests, compare prices from different facilities if possible (e.g., imaging centers vs. hospital-based imaging).
Frequently Asked Questions
What is the primary difference between a mouth ulcer and mouth cancer?
The primary difference lies in their persistence and nature. A benign mouth ulcer is typically painful, has a distinct appearance (red border, yellow/grey center), and heals completely within 2-3 weeks. Mouth cancer, on the other hand, is often painless in its early stages, may appear as a persistent red or white patch or lump, and crucially, does not heal within the normal timeframe, instead growing or changing over time.
How quickly does mouth cancer spread?
The rate at which mouth cancer spreads varies significantly depending on the type of cancer, its aggressiveness, and the individual's biology. Some can grow and spread relatively quickly within months, while others are slower. Early detection before it spreads to lymph nodes or distant sites is critical for successful treatment and prognosis.
Are oral cancer white spots on gums always cancerous?
No, oral cancer white spots on gums (leukoplakia) are not always cancerous, but they are considered potentially precancerous. A significant percentage of leukoplakia lesions can transform into squamous cell carcinoma. Any persistent white patch that cannot be scraped off warrants a biopsy to determine its exact nature and rule out malignancy.
Can an oral cancer lump on gum be mistaken for a benign growth?
Yes, an oral cancer lump on gum can initially be mistaken for a benign growth like a fibroma, pyogenic granuloma, or even an abscess. However, benign growths typically have a clear cause (like trauma or irritation) and may resolve or remain stable. A cancerous lump will persist, grow, or change, and usually lacks an obvious benign cause, necessitating a biopsy for definitive diagnosis.
Is mouth cancer painful?
Early-stage mouth cancer is often painless, which is one reason it can be overlooked. Pain usually develops as the cancer grows larger, invades nerves, or ulcerates. Therefore, the absence of pain should never be a reason to delay evaluation of a suspicious, non-healing lesion.
What are the survival rates for mouth cancer?
Oral cancer survival rates vary significantly based on the stage at diagnosis. For localized oral cancer (Stage I or II), the 5-year survival rate can be around 84%. If it has spread to regional lymph nodes (Stage III or IV), the rate drops to about 67%. If it has metastasized to distant sites, the 5-year survival rate is around 40%. Early detection is paramount.
What is the cost of an oral cancer screening at a regular dental check-up?
Oral cancer screenings are typically included as part of your routine comprehensive dental examination, which usually costs between $75 and $200 without insurance. Many dental insurance plans cover preventive exams at 100% or with a small co-pay.
How long does it take to recover from oral cancer surgery?
Recovery time varies greatly based on the extent of the surgery. For minor resections, recovery might be a few weeks. For extensive surgery involving reconstruction, recovery can take several months, often requiring prolonged hospitalization, followed by rehabilitation therapies (speech, swallowing, physical therapy) for many more months or even years.
Can mouth ulcers be a sign of a serious underlying condition other than cancer?
Yes, recurrent or unusually severe mouth ulcers can sometimes be a symptom of various underlying systemic conditions. These include autoimmune diseases (like lupus or Behçet's disease), inflammatory bowel diseases (Crohn's disease, ulcerative colitis), celiac disease, certain blood disorders, or immune deficiencies. If you experience persistent or recurrent ulcers, discuss this with your dentist or doctor.
What alternatives are there to traditional oral cancer treatments if I'm not a candidate for surgery?
If surgery isn't an option due to the cancer's location, stage, or the patient's overall health, alternative primary treatments include radiation therapy, chemotherapy, targeted therapy, or immunotherapy. These can be used alone or in combination to control or eradicate the cancer. Your oncology team will determine the best course of action based on your specific case.
When to See a Dentist
Given the potentially serious nature of oral cancer, knowing when to seek professional advice is critical.
You should make an appointment with your dentist or an oral surgeon IMMEDIATELY if you experience any of the following red flags:
- Any mouth sore, ulcer, lump, or patch (red or white) that does not heal or resolve within 2-3 weeks. This is the single most important warning sign.
- A new or persistent lump or thickening in your mouth, on your tongue, cheek, or neck, especially if it feels firm.
- Persistent red or white patches (erythroplakia or leukoplakia) in your mouth that cannot be scraped off.
- Unexplained bleeding from the mouth.
- Persistent numbness or tenderness in any area of your face, mouth, or neck.
- Difficulty or pain when chewing, swallowing, or moving your tongue or jaw.
- A persistent sore throat or hoarseness that lasts for more than a few weeks without an obvious cause.
- Any significant changes in the fit of your dentures.
For routine care and prevention:
- Schedule regular dental check-ups, typically every six months, for comprehensive oral exams and professional cleanings. These appointments include oral cancer screenings and are your first line of defense.
- Discuss any recurring mouth ulcers or concerns you have about your oral health during these routine visits.
Emergency vs. Scheduled Appointment Guidance: While a persistent, non-healing lesion constitutes an urgent concern that warrants a prompt evaluation, it is generally not a dental emergency that requires an immediate trip to the ER. Contact your dentist or an oral surgeon's office as soon as possible to schedule an urgent appointment. Clearly explain your symptoms when you call so the office can prioritize your visit.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Floor of Mouth Cancer: Complete Guide
Each year, over 54,000 Americans are diagnosed with oral cavity or oropharyngeal cancer, making it a significant public health concern. While often overlooked, floor of mouth cancer is a particularly aggressive and common form of oral cancer, accounting for a substantial percentage of all oral c
February 23, 2026
Oral Cancer Stages Pictures: Complete Guide
Oral cancer, a serious and potentially life-threatening disease, affects thousands of Americans each year. According to the American Cancer Society, approximately 54,000 new cases of oral cavity or oropharyngeal cancer are diagnosed annually in the United States. While these numbers can be daunt
February 23, 2026
Can You Die From Mouth Cancer
Oral cancer is a formidable disease, often striking with insidious subtlety before revealing its devastating potential. It's a question that weighs heavily on the minds of those who receive a diagnosis or even those simply concerned about unusual oral symptoms: can you die from mouth cancer? The
February 23, 2026
Mouth Cancer Photos: Complete Guide
Oral cancer is a formidable disease that affects tens of thousands of Americans each year, often with devastating consequences if not detected early. According to the Oral Cancer Foundation, approximately 54,000 Americans are diagnosed with oral or oropharyngeal cancer annually, and nearly 11,23
February 23, 2026