Signs of Oral Cancer: Complete Guide
Key Takeaways
- Oral cancer, often a silent but deadly disease, claims thousands of lives each year in the United States. In fact, an estimated 54,000 Americans are diagnosed with oral cancer annually, and approximately 11,000 succumb to it. These statistics highlight a critical truth: early detection dramatica
Oral cancer, often a silent but deadly disease, claims thousands of lives each year in the United States. In fact, an estimated 54,000 Americans are diagnosed with oral cancer annually, and approximately 11,000 succumb to it. These statistics highlight a critical truth: early detection dramatically improves survival rates. Understanding the signs of oral cancer is not just beneficial; it's potentially life-saving. Many people often mistake early symptoms for minor irritations, delaying crucial diagnosis. This comprehensive guide from SmilePedia.net aims to empower you with the knowledge to recognize the early indicators, understand the various forms of the disease, and navigate the journey from diagnosis to recovery and prevention. We will explore what oral cancer looks like, its common causes, detailed treatment options, associated costs, and vital steps for prevention, ensuring you have the most authoritative information at your fingertips.
Key Takeaways:
- Early Detection is Crucial: Oral cancer caught in its localized stage has an 85%+ five-year survival rate, compared to 39% if it has spread significantly.
- Common Signs: Be vigilant for persistent mouth sores (lasting over two weeks), red or white patches, unexplained lumps or swellings, difficulty chewing/swallowing, or persistent sore throats.
- Primary Risk Factors: Tobacco use (smoking and smokeless), heavy alcohol consumption, and Human Papillomavirus (HPV) infection are the leading causes.
- Diagnosis: A thorough visual and physical examination by a dentist or oral surgeon, followed by a biopsy, is the definitive diagnostic method.
- Treatment Options: Typically involves a combination of surgery, radiation therapy, and/or chemotherapy, tailored to the cancer's stage and type.
- Cost Implications: Treatment costs can range significantly, from $5,000 for early-stage surgery to over $150,000 for advanced, multi-modal care, often covered by medical (not dental) insurance.
- Prevention: The most effective prevention strategies include avoiding tobacco and limiting alcohol, HPV vaccination, using sun protection on lips, and regular dental check-ups with oral cancer screenings.
What Is Oral Cancer?
Oral cancer, often referred to as mouth cancer, is a type of head and neck cancer that can develop in any part of the oral cavity (mouth) or oropharynx (throat). This includes the lips, tongue, inner lining of the cheeks, the floor of the mouth, the roof of the mouth (hard and soft palate), the gums, the tonsils, and the back of the throat. The vast majority of oral cancers, accounting for about 90% of all cases, are squamous cell carcinomas. These cancers begin in the flat, thin squamous cells that line the moist surfaces inside your mouth and throat.

Oral cancer is characterized by the uncontrolled growth of abnormal cells that can invade and destroy surrounding tissues. If not detected and treated early, these cancer cells can spread from the mouth to other parts of the body, such as the lymph nodes in the neck, and then to more distant organs, a process known as metastasis. This spread significantly complicates treatment and reduces survival rates. The disease's impact can be profound, affecting speech, eating, swallowing, and facial appearance, making early awareness of the signs of oral cancer vitally important for positive outcomes.
Types of Oral Cancer
While squamous cell carcinoma is by far the most prevalent, several other types of cancer can occur in the oral cavity and oropharynx. Understanding these variations can help in accurate diagnosis and tailored treatment strategies.
Squamous Cell Carcinoma (SCC)
As mentioned, SCC is the most common type, originating in the squamous cells that line the mouth and throat. These cancers often develop from precancerous lesions, such as leukoplakia (white patches) or erythroplakia (red patches), which we will discuss in detail. SCC can manifest as persistent sores, ulcers, lumps, or areas of thickening that do not heal. It can affect any part of the oral cavity, but is particularly common on the tongue, lips, and floor of the mouth. The aggressive nature of SCC means early detection is paramount.
Verrucous Carcinoma
Verrucous carcinoma is a rare, low-grade variant of squamous cell carcinoma. It typically grows slowly and is less likely to spread to distant parts of the body compared to conventional SCC. This type of cancer often presents as a large, wart-like lesion with a cauliflower-like surface, usually on the gums or inner lining of the cheek. While less aggressive, it can still cause significant local destruction if left untreated.
Minor Salivary Gland Cancers
The oral cavity contains numerous small salivary glands (minor salivary glands) in the lining of the mouth and throat. Cancers can develop in these glands, though they are less common than SCC. Types include adenoid cystic carcinoma, mucoepidermoid carcinoma, and polymorphous adenocarcinoma. These cancers typically present as painless lumps or swellings in the palate, cheek, or lips. Their growth pattern can vary, with some being slow-growing and others more aggressive.
Lymphoma
While more commonly associated with the lymphatic system throughout the body, lymphoma can sometimes affect the oral cavity, particularly in the tonsils or the base of the tongue, areas rich in lymphatic tissue. Lymphoma typically presents as a rapidly growing mass or swelling and may be accompanied by other systemic symptoms like fever, night sweats, and weight loss.
Melanoma
Oral melanoma is an extremely rare but highly aggressive form of cancer that originates from pigment-producing cells called melanocytes. It can appear as a dark, discolored lesion (brown, black, blue, or even non-pigmented) on the gums, hard palate, or tongue. Due to its rarity and often delayed diagnosis, oral melanoma carries a poor prognosis compared to skin melanoma.
Causes and Risk Factors for Oral Cancer
Oral cancer doesn't usually develop overnight; it's often the result of a combination of risk factors accumulated over time. While some factors are beyond your control, many are linked to lifestyle choices, offering clear avenues for prevention.
Tobacco Use
Tobacco use, in any form, is the single largest risk factor for oral cancer. This includes smoking cigarettes, cigars, and pipes, as well as using smokeless tobacco products like chewing tobacco and snuff. The harmful chemicals in tobacco damage the DNA of cells in the mouth and throat, leading to uncontrolled growth. Smokers are six times more likely to develop oral cancer than non-smokers. For smokeless tobacco users, the risk is particularly high in the specific areas where the tobacco is held in the mouth (e.g., cheek or gum).
Alcohol Consumption
Heavy and prolonged alcohol consumption significantly increases the risk of oral cancer. Alcohol itself can act as an irritant, but it also facilitates the absorption of other carcinogens into the cells of the oral cavity. The risk is compounded dramatically when alcohol use is combined with tobacco use; these two factors have a synergistic effect, meaning they multiply each other's damaging impact. For example, a heavy drinker who also smokes heavily has a risk of developing oral cancer that is many times greater than the sum of the individual risks.
Human Papillomavirus (HPV)
In recent decades, Human Papillomavirus (HPV), particularly HPV-16, has emerged as a significant and growing risk factor for oropharyngeal cancers (cancers of the tonsils and base of the tongue). Unlike tobacco- and alcohol-related oral cancers, HPV-related oral cancers often affect younger individuals who do not have a history of heavy smoking or drinking. HPV is a sexually transmitted infection, and oral HPV infection is believed to occur through oral sex. The HPV vaccine, typically recommended for adolescents, can protect against the strains most commonly associated with these cancers.
Sun Exposure
Prolonged and unprotected exposure to ultraviolet (UV) radiation from the sun is a primary cause of lip cancer, which is considered a type of oral cancer. This risk is similar to how sun exposure causes skin cancer elsewhere on the body. Individuals who spend a lot of time outdoors, such as farmers, construction workers, or avid sunbathers, are at higher risk if they don't protect their lips.
Poor Nutrition and Diet
A diet consistently low in fruits and vegetables and high in processed foods may contribute to an increased risk of various cancers, including oral cancer. Antioxidants and various vitamins found in fresh produce are believed to protect cells from damage that can lead to cancer.
Compromised Immune System
Individuals with weakened immune systems, such as organ transplant recipients on immunosuppressive drugs or people with HIV/AIDS, have a higher risk of developing certain cancers, including some oral cancers, as their bodies are less able to fight off abnormal cell growth or infections like HPV.
Genetic Predisposition
While not as strong a factor as tobacco or alcohol, a family history of oral cancer or certain genetic syndromes can slightly increase an individual's risk. However, most oral cancers are sporadic and not directly inherited.
Chronic Irritation (Less Proven)
Historically, chronic irritation from things like ill-fitting dentures or sharp teeth was thought to be a direct cause of oral cancer. While such irritations can certainly create chronic sores or inflammation, current research suggests they are rarely a direct cause of malignant transformation. However, they can potentially exacerbate existing precancerous conditions or mask the early signs of cancer.
Pro Tip: If you engage in any of the primary risk behaviors (tobacco use, heavy alcohol consumption, or have a history of HPV), discussing your risk profile with your dentist or doctor is essential. They can recommend more frequent screenings and advise on risk reduction strategies.
Key Signs and Symptoms of Oral Cancer: What to Look For
Recognizing the signs of oral cancer early is the most critical step toward successful treatment. Many early symptoms can be subtle and easily overlooked or mistaken for common mouth ailments. If any of these signs persist for more than two weeks, it's imperative to consult a dental professional or doctor.
Persistent Sores or Ulcers
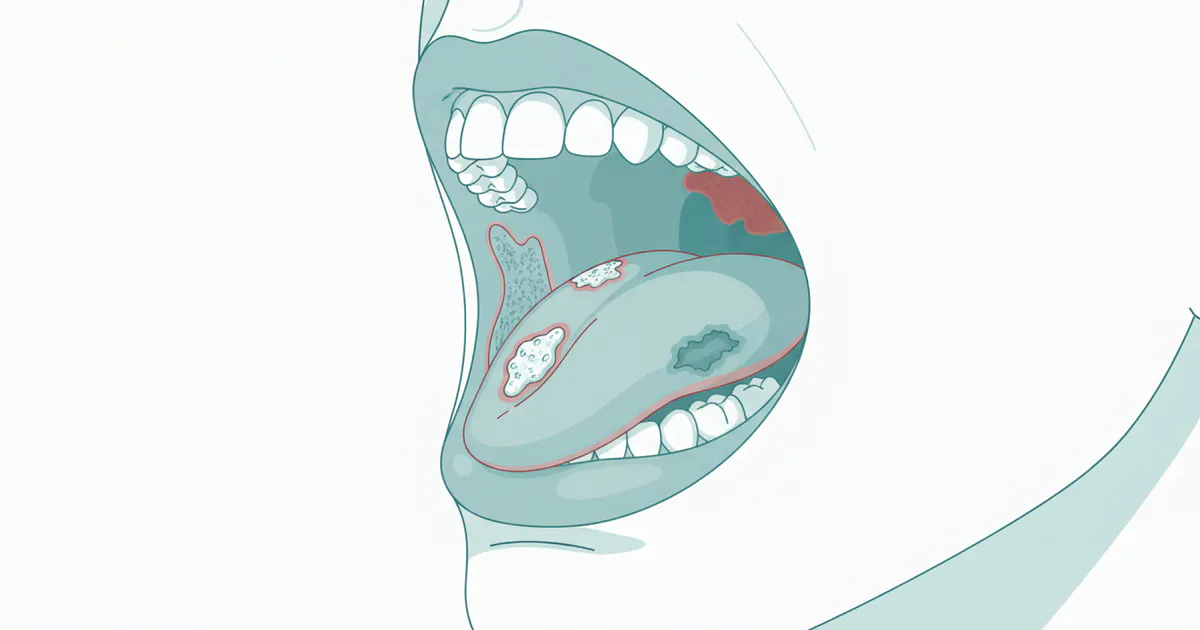
One of the most common and significant early indicators is a mouth sore, ulcer, or lesion that does not heal within two weeks. Unlike typical canker sores or injuries that usually resolve quickly, a cancerous lesion will persist, often remaining painless in its early stages. These sores can appear on the lips, tongue, gums, inside of the cheeks, or on the roof or floor of the mouth.
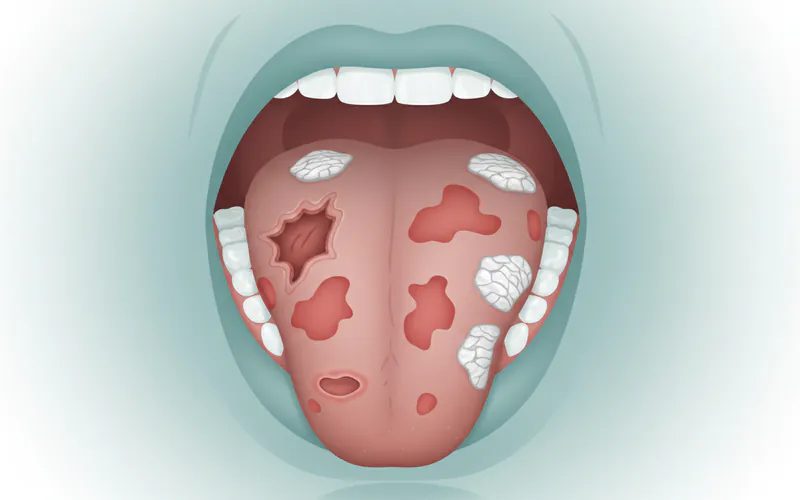
Red or White Patches (Leukoplakia and Erythroplakia)
These patches are often precancerous, meaning they have a higher risk of turning into cancer, especially erythroplakia.
- Leukoplakia: White or grayish patches that appear on the tongue, inside of the cheeks, or on the floor of the mouth. They cannot be scraped off. While many leukoplakias are benign, a significant percentage (5-17%) can develop into squamous cell carcinoma.
- Erythroplakia: Red, often velvety patches. These are less common than leukoplakia but have a much higher rate of malignant transformation (up to 90%). Any persistent red patch in the mouth should be viewed with extreme suspicion.
- Erythroleukoplakia: A mixed red and white patch, which also carries a significant risk.
Lumps, Bumps, or Thickening
Any unexplained lump, swelling, or thickening of the tissue in the mouth, on the lips, or in the neck should be evaluated. These can be firm to the touch and may or may not be painful. These might indicate a growing tumor or, if in the neck, enlarged lymph nodes where cancer cells may have spread.
Persistent Sore Throat or Hoarseness
If you experience a sore throat that doesn't go away, a chronic feeling of something caught in your throat, or a change in your voice (hoarseness) that lasts for more than a couple of weeks, especially without an obvious cold or flu, it could be a sign of cancer in the oropharynx or vocal cords.
Difficulty Swallowing (Dysphagia) or Chewing
As a tumor grows, it can interfere with normal functions. Difficulty or pain when swallowing (dysphagia), a sensation that food is getting stuck, or problems with chewing can be indicative of oral or oropharyngeal cancer.
Numbness or Pain
While early oral cancers are often painless, as the disease progresses, it can cause persistent numbness, tingling, or pain in any area of the mouth, face, or neck. This can manifest as a burning sensation or a deep ache. Unexplained ear pain can also be a referred pain from oral cancer.
Unexplained Bleeding
Any unexplained bleeding from the mouth, not related to injury or routine dental procedures, should be investigated. This can occur from ulcerated lesions.
Loose Teeth or Dentures That No Longer Fit
If teeth become unexpectedly loose without a clear dental cause (like gum disease), or if dentures start to fit poorly or become uncomfortable due to changes in the underlying gum or bone structure, it could be a sign of cancer infiltrating the jawbone or soft tissues.
Unexplained Weight Loss
Significant, unintentional weight loss is a general symptom of many cancers, including advanced oral cancer. This can be due to the body's increased metabolic demands from the cancer, or difficulty eating and swallowing.
Swelling in the Jaw or Neck
Swelling in the jaw, often causing discomfort, can be a symptom of a tumor growing in the bone. Swelling or a persistent lump in the neck, especially if it feels firm and doesn't move, often indicates that cancer has spread to the lymph nodes.

Changes in Voice or Speech
Beyond hoarseness, a tumor affecting the tongue, palate, or throat can alter your voice quality or make speaking clearly difficult.
Pro Tip: Perform a monthly self-examination of your mouth. Stand in front of a mirror, use a good light source, and thoroughly inspect your lips, gums, tongue (top, sides, and underneath), the roof and floor of your mouth, and the inside of your cheeks. Feel your neck and jawline for any lumps or tenderness. Being familiar with your normal oral anatomy will help you detect any changes more quickly.
Diagnosis of Oral Cancer
If you or your dentist notice any suspicious signs of oral cancer, the next step is a thorough diagnostic process to confirm or rule out cancer and determine its extent.
Visual and Physical Examination
The diagnostic journey typically begins with a comprehensive oral examination by a dentist, oral surgeon, or ENT specialist. They will visually inspect your entire oral cavity, including the often-overlooked areas like the floor of the mouth and the back of the tongue. They will also physically palpate (feel) the tissues of your mouth, jaw, and neck for any lumps, swellings, or areas of tenderness. Many dental offices are equipped with advanced screening tools, such as special lights or dyes, that can help highlight abnormal tissues that might not be visible to the naked eye. The American Dental Association (ADA) recommends regular oral cancer screenings as part of routine dental check-ups.
Biopsy
A biopsy is the definitive method for diagnosing oral cancer. During this procedure, a small tissue sample is removed from the suspicious area and sent to a pathologist for microscopic examination.
- Incisional Biopsy: A small piece of tissue is cut from the abnormal area.
- Excisional Biopsy: The entire suspicious lesion is removed.
- Brush Biopsy: A less invasive method where cells are scraped from the lesion using a special brush. While useful for initial screening, if abnormal cells are found, a conventional biopsy is usually required for definitive diagnosis.
The pathologist determines if cancer cells are present, and if so, what type of cancer it is.
Imaging Tests
Once cancer is confirmed by biopsy, imaging tests are crucial for "staging" the cancer – determining its size, location, and whether it has spread to lymph nodes or other parts of the body.
- CT Scan (Computed Tomography): Provides detailed cross-sectional images of the head and neck, showing the extent of the tumor and potential spread to lymph nodes or bone.
- MRI (Magnetic Resonance Imaging): Uses magnetic fields to create detailed images of soft tissues, useful for assessing tumor depth and involvement of nerves or blood vessels.
- PET Scan (Positron Emission Tomography): Involves injecting a radioactive sugar tracer into the body. Cancer cells, which are metabolically active, absorb more of the sugar, making them glow brightly on the scan. This can detect cancer spread throughout the body.
- Chest X-ray: May be performed to check for lung metastasis.
Endoscopy
In some cases, a flexible tube with a camera (endoscope) may be inserted through the nose or mouth to visually inspect areas of the throat, larynx, or esophagus that are difficult to see during a standard oral exam. This helps to detect if the cancer has spread to adjacent areas.
Comparison Table 1: Diagnostic Methods for Oral Cancer
| Diagnostic Method | Description | Pros | Cons | Typical Cost Range (US$) |
|---|---|---|---|---|
| Visual/Physical Exam | Dentist/Specialist inspects and palpates oral cavity and neck | Non-invasive, quick, routine part of dental check-ups | Not definitive, can miss subtle lesions | Included in dental exam |
| Biopsy (Incisional) | Surgical removal of a tissue sample for microscopic analysis | Gold standard for definitive diagnosis | Minor surgical procedure, some discomfort, takes time for results | $300 - $1,000+ |
| CT Scan | X-ray images from different angles to create cross-sectional views | Excellent for bone involvement, quick | Radiation exposure, may require contrast dye | $300 - $3,000+ |
| MRI | Uses magnetic fields and radio waves for detailed soft tissue images | Excellent for soft tissue, no radiation | Longer procedure, noisy, not suitable for patients with certain implants | $500 - $4,000+ |
| PET Scan | Injectable radioactive tracer shows metabolic activity (cancer cells) | Detects spread throughout body, good for staging/recurrence | Radiation exposure, high cost, may show false positives | $1,500 - $7,000+ |
Treatment Options for Oral Cancer
The treatment plan for oral cancer is highly individualized, depending on the stage of the cancer (size, location, and spread), the type of cancer, the patient's overall health, and their preferences. A multidisciplinary team of specialists, including oral surgeons, oncologists, radiation oncologists, and reconstructive surgeons, typically collaborates to develop the best approach.
Surgery
Surgery is often the primary treatment for oral cancer, especially in its early stages. The goal is to remove the tumor completely, along with a margin of healthy tissue to ensure all cancer cells are gone.
- Resection: This involves surgically removing the tumor and a surrounding margin of healthy tissue. The extent of resection can vary from a small lesion on the lip to a partial glossectomy (removal of part of the tongue) or mandibulectomy (removal of part of the jawbone).
- Neck Dissection: If there is evidence or suspicion that cancer cells have spread to the lymph nodes in the neck, a neck dissection may be performed. This procedure removes some or all of the lymph nodes from one or both sides of the neck.
- Reconstruction: After extensive surgical removal, reconstructive surgery may be necessary to rebuild parts of the mouth, jaw, or face. This can involve using tissue flaps from other parts of the body (e.g., forearm, leg, or back) to restore appearance and function (e.g., ability to speak, chew, swallow).
- Pros: Offers immediate removal of the visible tumor, potentially curative for early-stage cancers.
- Cons: Can lead to disfigurement, functional impairments (speech, swallowing, chewing), and requires a significant recovery period.
Radiation Therapy
Radiation therapy uses high-energy beams (like X-rays or protons) to kill cancer cells or inhibit their growth. It can be used:
- Alone: For small tumors or for patients who are not candidates for surgery.
- After Surgery (Adjuvant Therapy): To kill any remaining cancer cells and reduce the risk of recurrence, especially if margins were close or lymph nodes were involved.
- Before Surgery (Neoadjuvant Therapy): To shrink a large tumor, making it easier to remove surgically.
- With Chemotherapy (Chemoradiation): For more advanced cancers, chemotherapy can make cancer cells more sensitive to radiation.
- External Beam Radiation Therapy (EBRT): The most common type, where radiation is delivered from a machine outside the body.
- Brachytherapy: Radioactive seeds or ribbons are placed directly into or near the tumor.
- Pros: Non-invasive (external), can preserve oral function and appearance in some cases, effective for localized control.
- Cons: Significant side effects including mucositis (mouth sores), dry mouth (xerostomia), taste changes, jaw stiffness, and in severe cases, osteoradionecrosis (bone death due to radiation).
Chemotherapy
Chemotherapy involves using powerful drugs, often given intravenously, to kill cancer cells throughout the body.
- Adjuvant/Neoadjuvant: Often used in combination with radiation therapy (chemoradiation) for advanced stages, or to reduce tumor size before surgery.
- Palliative: To control symptoms and improve quality of life in advanced, metastatic cancer.
- Pros: Can treat cancer cells that have spread beyond the primary tumor site.
- Cons: Significant systemic side effects due to its impact on healthy rapidly dividing cells, including nausea, vomiting, fatigue, hair loss, mouth sores, and weakened immune system.
Targeted Therapy
Targeted therapies are a newer class of drugs that specifically target molecules involved in cancer cell growth and survival, while minimizing harm to healthy cells. For some oral cancers, drugs like cetuximab (Erbitux), which targets the epidermal growth factor receptor (EGFR), may be used.
- Pros: Can be more precise than traditional chemotherapy, potentially leading to fewer severe side effects for some patients.
- Cons: Only effective for cancers with specific molecular targets, can still have side effects.
Immunotherapy
Immunotherapy is an innovative approach that boosts the body's own immune system to recognize and destroy cancer cells. Drugs called checkpoint inhibitors (e.g., pembrolizumab, nivolumab) are approved for certain advanced or recurrent head and neck cancers, including oral cancer, particularly if standard treatments have failed.
- Pros: Can lead to durable responses in some patients, effective for hard-to-treat cancers.
- Cons: Can cause immune-related side effects, high cost, not effective for all patients.
Pro Tip: Your treatment team will discuss the pros and cons of each option with you in detail, helping you make informed decisions. Don't hesitate to ask questions about potential side effects, recovery timelines, and long-term impacts on your quality of life.
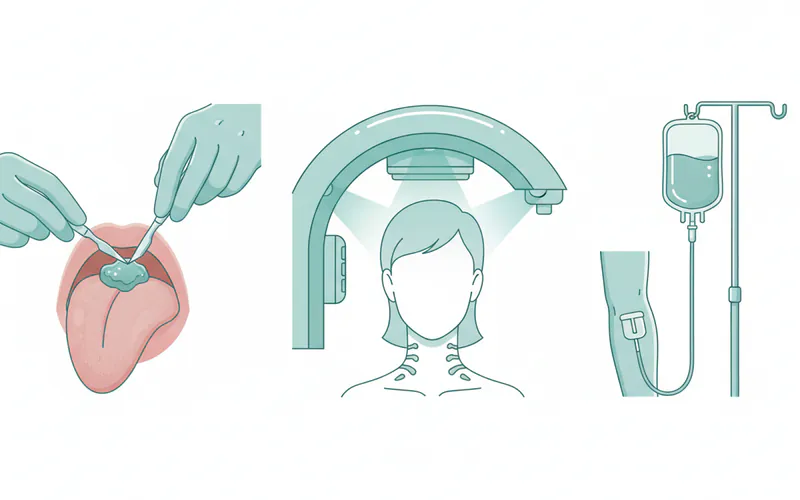
The Treatment Journey: Step-by-Step Process
Undergoing oral cancer treatment is a complex journey, often involving multiple stages and specialists. Knowing what to expect can help you prepare mentally and practically.
1. Diagnosis and Staging (Weeks 1-4):
- Initial Consultation: You'll meet with a dentist, oral surgeon, or ENT who identifies the suspicious lesion.
- Biopsy: A tissue sample is taken and analyzed by a pathologist. This is the definitive diagnostic step.
- Imaging: If cancer is confirmed, you'll undergo CT, MRI, and/or PET scans to determine the cancer's stage (size, location, and spread to lymph nodes or other organs).
2. Treatment Planning (Weeks 4-6):
- Multidisciplinary Team Meeting: Your case will be reviewed by a team including surgeons, medical oncologists, radiation oncologists, pathologists, and potentially reconstructive surgeons, speech therapists, and nutritionists.
- Personalized Plan: Based on the cancer's stage, type, and your overall health, a comprehensive treatment plan will be developed, outlining the sequence and types of therapies.
3. Primary Treatment (Varies, Weeks to Months):
- Surgery: If surgery is the primary treatment, it will be scheduled. This may involve removal of the tumor, lymph nodes (neck dissection), and possibly initial reconstructive procedures. Surgical recovery typically takes several weeks to months.
- Radiation Therapy: If radiation is chosen, or if it follows surgery, you'll have a planning session (simulation) to precisely map the treatment area. Treatment typically occurs 5 days a week for 5-7 weeks.
- Chemotherapy: Chemotherapy can be given alone, before, during, or after radiation or surgery. Cycles typically last a few weeks with rest periods in between.
4. Adjuvant Therapy (Post-Primary Treatment):
- After initial treatment (especially surgery), additional therapy (e.g., radiation, chemotherapy, or both) may be recommended to eradicate any remaining cancer cells and reduce the risk of recurrence. This phase also typically lasts several weeks to months.
5. Rehabilitation and Support (Ongoing):
- Speech and Swallowing Therapy: Crucial for regaining function after treatment, especially if the tongue, palate, or throat were affected. This can start during treatment and continue for months or even years.
- Nutritional Support: A dietitian will help manage changes in eating, taste, and swallowing. A feeding tube (e.g., PEG tube) might be temporarily or permanently necessary.
- Physical Therapy: To address jaw stiffness (trismus) or neck mobility issues.
- Psychological Support: Counseling, support groups, and patient navigators can help you cope with the emotional and psychological challenges of cancer treatment.
6. Follow-up and Surveillance (Lifelong):
- Regular follow-up appointments (initially every 1-3 months, then gradually less frequent) are essential to monitor for any signs of recurrence, manage long-term side effects, and screen for new primary cancers. This involves visual examinations, palpation, and sometimes imaging.
Pro Tip: Appoint a family member or friend to accompany you to appointments. They can take notes, ask questions you might forget, and provide emotional support. Don't hesitate to seek a second opinion on your diagnosis and treatment plan; it's a common practice and can provide peace of mind.
Cost and Insurance for Oral Cancer Treatment
The financial burden of oral cancer treatment in the US can be substantial, ranging from relatively modest for very early-stage cases to extremely high for advanced, complex multi-modal treatments and long-term rehabilitation.
Oral cancer treatment costs can range significantly, from $5,000 for early-stage surgical removal of a small lesion to over $150,000 for advanced, multi-modal treatment involving extensive surgery, radiation, chemotherapy, and reconstructive procedures. These figures do not include lost income, travel, or ongoing rehabilitation costs.
Insurance Coverage
- Medical Insurance is Key: It is crucial to understand that oral cancer treatment is typically covered by your medical insurance, not your dental insurance. Dental insurance usually covers routine preventative care, fillings, crowns, and extractions, but not major medical procedures like cancer treatment.
- In-Network vs. Out-of-Network: Choosing in-network providers and facilities will significantly reduce your out-of-pocket costs, as insurance companies have negotiated lower rates with these providers. Out-of-network care will often result in higher co-pays, deductibles, and a larger percentage of the bill being your responsibility.
- Deductibles, Co-pays, and Coinsurance: You will likely be responsible for meeting your annual deductible before your insurance begins to pay a larger share. Co-pays are fixed amounts paid per service (e.g., doctor's visit, prescription), while coinsurance is a percentage of the total cost you're responsible for after meeting your deductible.
- Out-of-Pocket Maximums: Most insurance plans have an annual out-of-pocket maximum. Once you reach this limit, your insurance plan typically covers 100% of covered medical expenses for the rest of the plan year.
- Reconstructive Surgery: Insurance typically covers reconstructive surgery deemed medically necessary to restore function, but cosmetic aspects may not be fully covered.
Uninsured Costs
For individuals without adequate medical insurance, the costs of oral cancer treatment can be catastrophic. A biopsy alone can range from $300-$1,000+, and complex surgeries can run tens of thousands of dollars. Radiation and chemotherapy regimens can easily add another $30,000-$100,000+.
Regional Variations
Treatment costs can vary significantly depending on the region of the US, the specific hospital or clinic (e.g., academic medical center vs. community hospital), and the expertise of the treating physicians. Major metropolitan areas or specialized cancer centers may have higher charges.
Comparison Table 2: Estimated Oral Cancer Treatment Costs (US Dollars)
| Treatment Component | Without Insurance (Estimate) | With Insurance (Out-of-Pocket Estimate) | Notes |
|---|---|---|---|
| Initial Consultation/Exam | $150 - $500 | $20 - $100 (Co-pay) | Specialist visit |
| Biopsy & Pathology | $300 - $1,500 | $50 - $300 (Co-pay/Deductible) | Includes procedure and lab analysis |
| Imaging (CT/MRI/PET) | $500 - $7,000 (per scan) | $100 - $1,500 (Deductible/Coinsurance) | PET scans are typically the most expensive |
| Early Stage Surgery | $5,000 - $30,000 | $1,000 - $7,000 (Deductible/Coinsurance) | Removal of small tumor, minimal reconstruction |
| Advanced Stage Surgery | $30,000 - $100,000+ | $5,000 - $20,000+ (Deductible/Coinsurance) | Extensive resection, neck dissection, complex reconstruction |
| Radiation Therapy | $20,000 - $70,000 (full course) | $2,000 - $15,000 (Deductible/Coinsurance) | Per course (5-7 weeks), external beam vs. brachytherapy |
| Chemotherapy | $10,000 - $100,000+ (per course) | $1,000 - $20,000+ (Deductible/Coinsurance) | Varies greatly by drug, duration, and type |
| Targeted Therapy/Immunotherapy | $10,000 - $20,000+ (per month) | $1,000 - $5,000+ (per month, if covered) | Newer, often high-cost drugs; coverage varies |
| Rehabilitation (Speech/PT) | $100 - $300 (per session) | $20 - $70 (Co-pay) | Multiple sessions over months/years can add up |
| Total Comprehensive Care | $50,000 - $200,000+ | $5,000 - $25,000+ | This is a broad estimate; actual costs can be lower or significantly higher based on individual case. |
Payment Plans and Financing Options:
- Hospital Financial Aid: Many hospitals have patient assistance programs or financial counselors who can help you apply for aid or set up payment plans.
- Government Programs: Medicaid or state-specific programs may provide assistance for eligible low-income individuals.
- Non-Profit Organizations: Organizations like the Oral Cancer Foundation or CancerCare offer financial assistance, grants, and other support for patients.
- Clinical Trials: Participating in a clinical trial may cover some or all treatment costs, in addition to providing access to cutting-edge therapies.
Cost-Saving Tips:
- Always verify your insurance coverage and obtain pre-authorizations for major procedures.
- Ask about generic alternatives for medications.
- Utilize patient advocacy services offered by your healthcare provider or non-profits.
- Keep detailed records of all medical bills and insurance claims.
Recovery and Aftercare
Recovery from oral cancer treatment can be a long and challenging process, often extending for months or even years beyond the active treatment phase. Comprehensive aftercare is essential to manage side effects, regain function, and maintain quality of life.
Pain Management
Pain is a common issue during and after treatment, especially following surgery or radiation. Your medical team will work with you to manage pain effectively using a combination of medications, nerve blocks, or other therapies. It's important to communicate your pain levels openly.
Nutritional Support
Treatment for oral cancer can severely impact your ability to eat, chew, and swallow.
- Dietary Modifications: You may need to adhere to a soft or liquid diet for an extended period.
- Nutritional Counseling: A registered dietitian will provide guidance on maintaining adequate nutrition and weight.
- Feeding Tubes (PEG Tubes): Many patients, particularly those undergoing radiation to the throat or extensive surgery, may require a temporary or permanent feeding tube (percutaneous endoscopic gastrostomy) to ensure they receive sufficient nutrients and hydration directly into the stomach.
Oral Hygiene
Maintaining meticulous oral hygiene is critical. Radiation and chemotherapy can cause dry mouth (xerostomia), making you more susceptible to tooth decay and gum disease.
- Specialized Products: Use fluoride rinses, gels, and artificial saliva substitutes to combat dry mouth and protect teeth.
- Regular Dental Care: Frequent dental check-ups and cleanings with a dentist familiar with oncology patients are vital to manage potential complications like osteoradionecrosis (bone death due to radiation) and secondary infections.
Speech and Swallowing Therapy
These therapies are cornerstone to recovery, especially after treatments that affect the tongue, jaw, or throat.
- Speech-Language Pathologists (SLPs): SLPs will work with you through exercises to improve your speech clarity, voice quality, and ability to swallow safely and effectively. This can prevent aspiration (food or liquid entering the airway).
- Physical Therapy: To address jaw stiffness (trismus), which can be a significant side effect of radiation or surgery, and improve neck mobility.
Psychological and Emotional Support
Coping with cancer and its aftermath takes a tremendous toll emotionally.
- Counseling: Individual or group counseling can help you process the trauma, anxiety, depression, and body image concerns.
- Support Groups: Connecting with others who have gone through similar experiences can provide invaluable emotional support and practical advice.
- Patient Navigators: These professionals can help you navigate the complex healthcare system and connect you with resources.
Reconstructive Surgery Aftercare
If you underwent reconstructive surgery, specific aftercare instructions will be provided, including wound care, monitoring for infection, and rehabilitation exercises to optimize the function and appearance of the reconstructed area.
Follow-up Schedule
Lifelong follow-up is essential. Initially, appointments will be frequent (e.g., every 1-3 months) to check for recurrence or new primary cancers. Over time, these become less frequent but remain critical for continued surveillance and management of long-term side effects.
Prevention of Oral Cancer
While we've emphasized the signs of oral cancer for early detection, prevention is always the best strategy. Many oral cancers are preventable by modifying lifestyle choices and adhering to regular health screenings.

Avoid Tobacco and Limit Alcohol
This is by far the most impactful step you can take.
- Quit Smoking/Chewing: If you use any form of tobacco, quitting immediately and completely drastically reduces your risk over time.
- Moderate Alcohol Intake: For men, this means no more than two drinks per day; for women, no more than one. Ideally, avoid alcohol if you are also a tobacco user.
HPV Vaccination
The HPV vaccine, typically recommended for adolescents and young adults (ages 9-26, though sometimes up to 45), protects against the strains of HPV most commonly associated with oropharyngeal cancers (HPV-16). Discuss this with your doctor.
Protect Lips from Sun
Just like your skin, your lips need sun protection.
- Use SPF Lip Balm: Apply lip balm with an SPF of 15 or higher regularly when outdoors.
- Wear Hats: Broad-brimmed hats can provide additional shade for your face and lips.
Healthy Diet
A balanced diet rich in fruits, vegetables, and whole grains provides essential vitamins, minerals, and antioxidants that can help protect cells from cancerous changes. Limit processed foods and red meats.
Regular Dental Check-ups with Oral Cancer Screenings
This is where your dentist plays a crucial role in early detection.
- Every 6-12 Months: Schedule routine dental examinations at least once a year, or ideally every six months, as recommended by the ADA.
- Comprehensive Screening: During these visits, your dentist will perform a visual and tactile oral cancer screening, looking for any suspicious lesions, lumps, or changes in your mouth and neck. Early-stage signs of oral cancer are often asymptomatic, making professional screening indispensable.
Self-Examinations
In addition to professional screenings, regularly performing a self-examination of your mouth (as described in the "What to Look For" section) allows you to become familiar with your normal oral anatomy and quickly spot any new or persistent changes. Aim for a quick check once a month.
Risks and Complications of Oral Cancer and Its Treatment
Beyond the initial diagnosis and treatment, oral cancer patients face a range of potential risks and complications, both from the disease itself and from the intensive treatments.
Recurrence
One of the most significant risks is the recurrence of cancer, either in the original site (local recurrence), in nearby lymph nodes, or in other areas of the body. Regular follow-up appointments are crucial to detect recurrence early.
Metastasis
If not treated effectively, oral cancer cells can spread (metastasize) to distant parts of the body, most commonly the lungs, liver, and bones. This makes the cancer much more difficult to treat and significantly reduces prognosis.
Functional Impairment
Treatment, especially extensive surgery or radiation to the head and neck, can lead to permanent or long-term functional impairments:
- Speech Difficulties (Dysarthria): Problems articulating words clearly due to changes in the tongue, palate, or jaw.
- Swallowing Difficulties (Dysphagia): Trouble chewing, moving food, or safely swallowing, which can lead to aspiration pneumonia and malnutrition.
- Chewing Problems: Due to jaw resection, nerve damage, or radiation-induced dry mouth.
- Jaw Stiffness (Trismus): Difficulty opening the mouth widely, making eating and oral hygiene challenging.
Disfigurement
Extensive surgery, particularly for advanced oral cancers, can result in significant changes to facial appearance and oral structures, which can be emotionally devastating and impact self-esteem. Reconstructive surgery aims to minimize this, but complete restoration is not always possible.
Treatment Side Effects
- Radiation Therapy:
- Xerostomia (Dry Mouth): Permanent reduction in saliva production, leading to discomfort, difficulty speaking/swallowing, and increased risk of dental decay.
- Mucositis: Painful inflammation and ulceration of the oral lining.
- Taste Changes: Altered or lost sense of taste.
- Osteoradionecrosis: Death of bone tissue (usually jawbone) due to reduced blood supply from radiation, a severe and difficult-to-treat complication.
- Trismus: Jaw stiffness.
- Chemotherapy:
- Nausea, vomiting, fatigue, hair loss, weakened immune system (increasing risk of infection).
- Peripheral neuropathy (nerve damage causing numbness/tingling).
- Surgery: Pain, swelling, infection, nerve damage, scarring.
Secondary Cancers
Survivors of oral cancer, especially those with ongoing risk factors (e.g., continued smoking or drinking), have an increased risk of developing a second primary cancer elsewhere in the head and neck region, or in other organs like the lungs or esophagus. This further emphasizes the importance of continued surveillance and risk factor modification.
Children and Pediatric Considerations
Oral cancer, particularly squamous cell carcinoma, is extremely rare in children. When abnormal growths or lesions are found in a child's mouth, they are far more likely to be benign conditions such as cysts, viral infections (e.g., warts), or reactive lesions from trauma.
However, certain rare types of head and neck cancers, such as rhabdomyosarcoma (a soft tissue sarcoma), lymphoma, or specific salivary gland tumors, can occur in children and sometimes manifest in the oral or oropharyngeal region. While the signs of oral cancer as described for adults are generally not applicable to routine pediatric screening, any persistent, unexplained lump, swelling, or non-healing sore in a child's mouth or neck should prompt immediate evaluation by a pediatrician or a pediatric dentist. Early and accurate diagnosis, even for rare pediatric conditions, is crucial for effective treatment.
Cost Breakdown
As detailed previously, oral cancer treatment represents a significant financial undertaking in the United States. To reiterate:
-
Average US Costs:
- Low (Early Stage, Localized Surgery): $5,000 - $30,000
- Mid (Surgery + Radiation OR Chemoradiation): $40,000 - $100,000
- High (Advanced Stage, Multi-modal, Extensive Reconstruction): $100,000 - $200,000+
- These ranges cover the primary treatments but often exclude long-term rehabilitation, follow-up care, and indirect costs like lost wages.
-
With vs. Without Insurance:
- Without Insurance: You are responsible for 100% of these costs, which can quickly lead to medical bankruptcy. A single biopsy could be several hundred dollars, while a full course of treatment could be hundreds of thousands.
- With Insurance: While medical insurance significantly mitigates the financial burden, you will still likely incur out-of-pocket expenses for deductibles (e.g., $1,500 - $10,000+ annually), co-pays (e.g., $20 - $70 per visit/prescription), and coinsurance (e.g., 10-30% of covered services after deductible). Most plans have an out-of-pocket maximum, typically ranging from $5,000 to $15,000 for individuals, which caps your annual financial liability.
-
Payment Plans and Financing Options: Hospitals and cancer centers often have financial assistance programs, counselors, and charity care options for those who qualify. Non-profit organizations specializing in cancer support can also offer grants or help with navigating financial aid. Patients may also explore medical credit cards or personal loans, though these come with interest rates.
-
Cost-Saving Tips: Proactively communicate with your insurance provider and healthcare team about costs. Inquire about generic medications, look into patient assistance programs offered by pharmaceutical companies, and always ask for itemized bills to scrutinize for errors.
Frequently Asked Questions
What are the earliest signs of oral cancer?
The earliest signs often include a persistent mouth sore, ulcer, or lesion that does not heal within two weeks, or the appearance of a red (erythroplakia) or white (leukoplakia) patch in the mouth. These early signs may be painless, making regular self-examination and professional screenings crucial.
What does oral cancer look like in its early stages?
In its early stages, oral cancer can appear as a small, flat white or reddish patch, or a tiny, ulcer-like lesion with raised edges. It might look similar to a canker sore or a common irritation, but critically, it will not resolve on its own within two weeks.
Is oral cancer painful?
Oral cancer is often painless in its earliest stages, which is a major reason for delayed diagnosis. As the cancer grows and invades surrounding tissues, it can cause pain, tenderness, numbness, or a burning sensation. Pain usually signifies a more advanced stage.
How long does it take for oral cancer to develop?
Oral cancer often develops slowly over several years, frequently beginning as precancerous lesions like leukoplakia or erythroplakia. However, some aggressive forms can progress more rapidly, evolving from normal tissue to advanced cancer within a shorter timeframe.
Can oral cancer be cured?
Yes, oral cancer can be cured, especially with early detection and prompt treatment. The five-year survival rate for localized oral cancer is over 85%, emphasizing the profound impact of recognizing the signs of oral cancer early.
What is the survival rate for oral cancer?
The overall five-year survival rate for oral cancer in the US is approximately 68%. This rate improves significantly to over 85% if the cancer is localized (confined to the primary site) at diagnosis, but drops to around 39% if it has spread to distant parts of the body.
Are there any home tests for oral cancer?
There are no definitive home tests for oral cancer. However, performing regular monthly self-examinations of your mouth (looking and feeling for any changes) is a vital tool for noticing suspicious signs early. Any persistent changes should always be evaluated by a dental professional.
Does HPV cause oral cancer?
Yes, certain strains of Human Papillomavirus, particularly HPV-16, are a leading cause of oropharyngeal cancers (cancers of the tonsils and base of the tongue), and to a lesser extent, other oral cancers. This is becoming an increasingly prevalent risk factor, especially among younger, non-smoking individuals.
How often should I get screened for oral cancer?
The American Dental Association (ADA) recommends that oral cancer screenings be a routine part of your regular dental check-ups, typically performed every six months to a year. If you have significant risk factors, your dentist may suggest more frequent screenings.
What is the typical cost of a biopsy for oral cancer?
The typical cost of an oral cancer biopsy in the US can range from $300 to $1,500 or more, depending on the complexity of the procedure (e.g., incisional vs. excisional, location), the facility, and the pathologist's fees. This cost is usually covered by medical insurance after deductibles and co-pays.
When to See a Dentist
Given the aggressive nature of oral cancer and the importance of early detection, knowing when to seek professional medical attention is critical.
You should see a dentist immediately if you experience any of the following:
- Any mouth sore, ulcer, lump, or discolored patch (red or white) that does not heal or resolve within two weeks. This is the most crucial "two-week rule."
- Unexplained numbness, pain, or tenderness in your mouth, face, or neck that persists.
- Persistent difficulty swallowing, chewing, or moving your tongue or jaw.
- A persistent sore throat or hoarseness that lasts more than two weeks, without a clear cause like a cold.
- Any unexplained bleeding from your mouth.
- A sudden change in how your teeth fit together or how your dentures fit.
- A persistent lump or swelling in your neck.
These are not "routine care" issues; they are potential red flags that require urgent evaluation. Do not wait for pain to develop, as early oral cancers are often painless. If your regular dentist identifies a suspicious area, they will likely refer you to an oral surgeon, ENT specialist, or oral pathologist for further evaluation and biopsy. Your proactive approach in noticing the signs of oral cancer and seeking timely professional advice can significantly improve your prognosis and potentially save your life.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Floor of Mouth Cancer: Complete Guide
Each year, over 54,000 Americans are diagnosed with oral cavity or oropharyngeal cancer, making it a significant public health concern. While often overlooked, floor of mouth cancer is a particularly aggressive and common form of oral cancer, accounting for a substantial percentage of all oral c
February 23, 2026
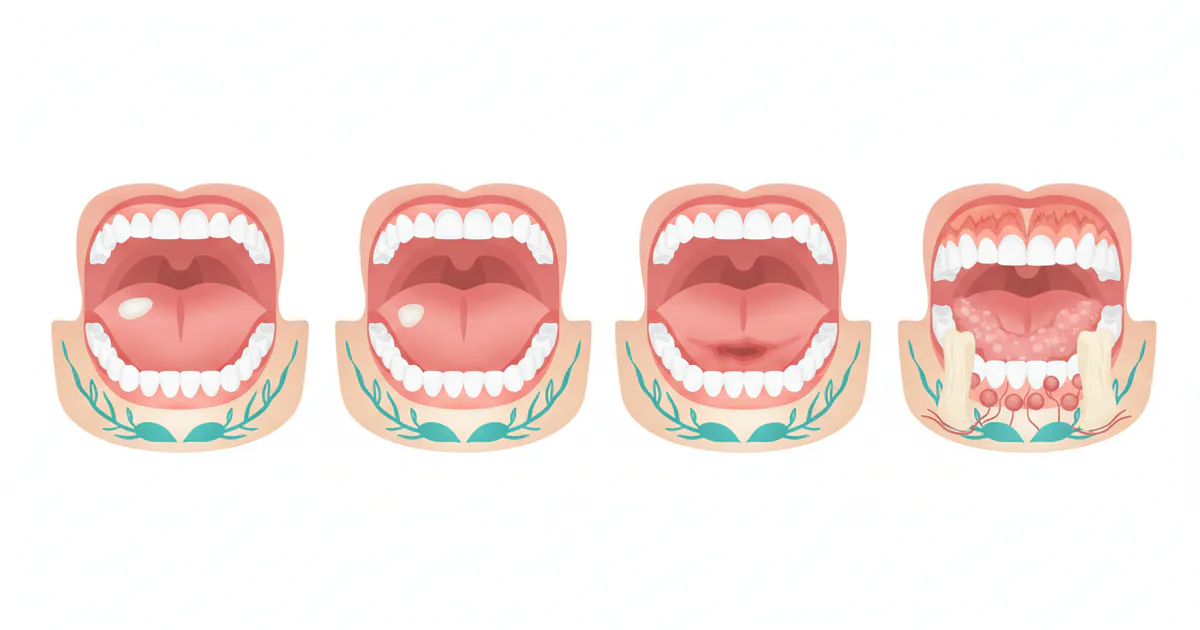
Oral Cancer Stages Pictures: Complete Guide
Oral cancer, a serious and potentially life-threatening disease, affects thousands of Americans each year. According to the American Cancer Society, approximately 54,000 new cases of oral cavity or oropharyngeal cancer are diagnosed annually in the United States. While these numbers can be daunt
February 23, 2026
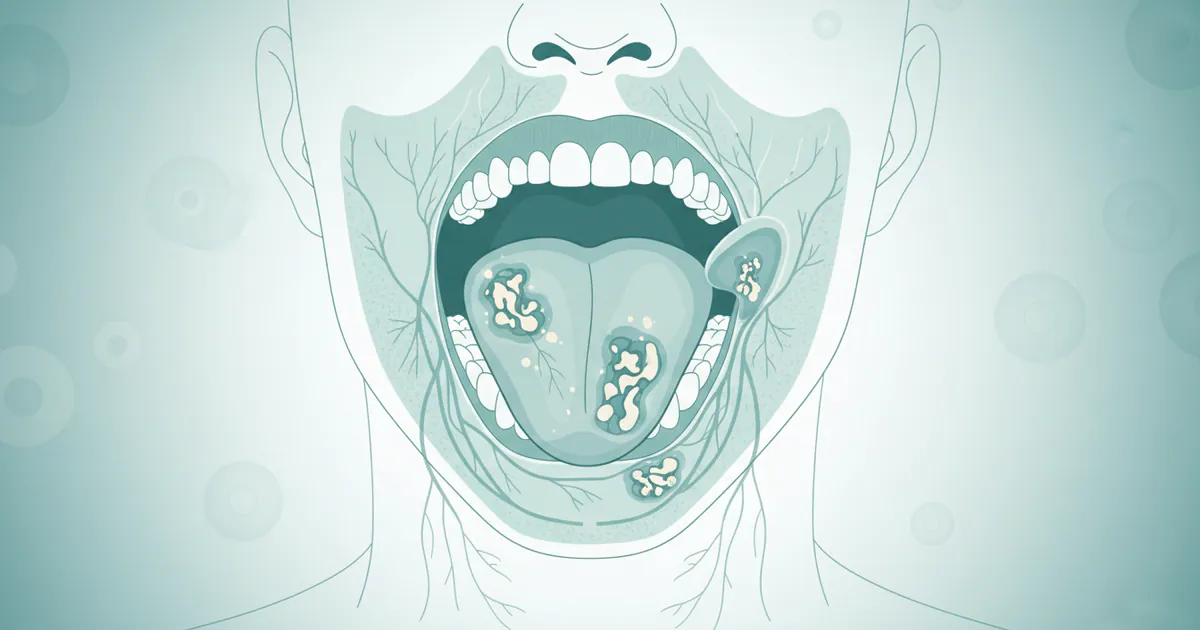
Can You Die From Mouth Cancer
Oral cancer is a formidable disease, often striking with insidious subtlety before revealing its devastating potential. It's a question that weighs heavily on the minds of those who receive a diagnosis or even those simply concerned about unusual oral symptoms: can you die from mouth cancer? The
February 23, 2026
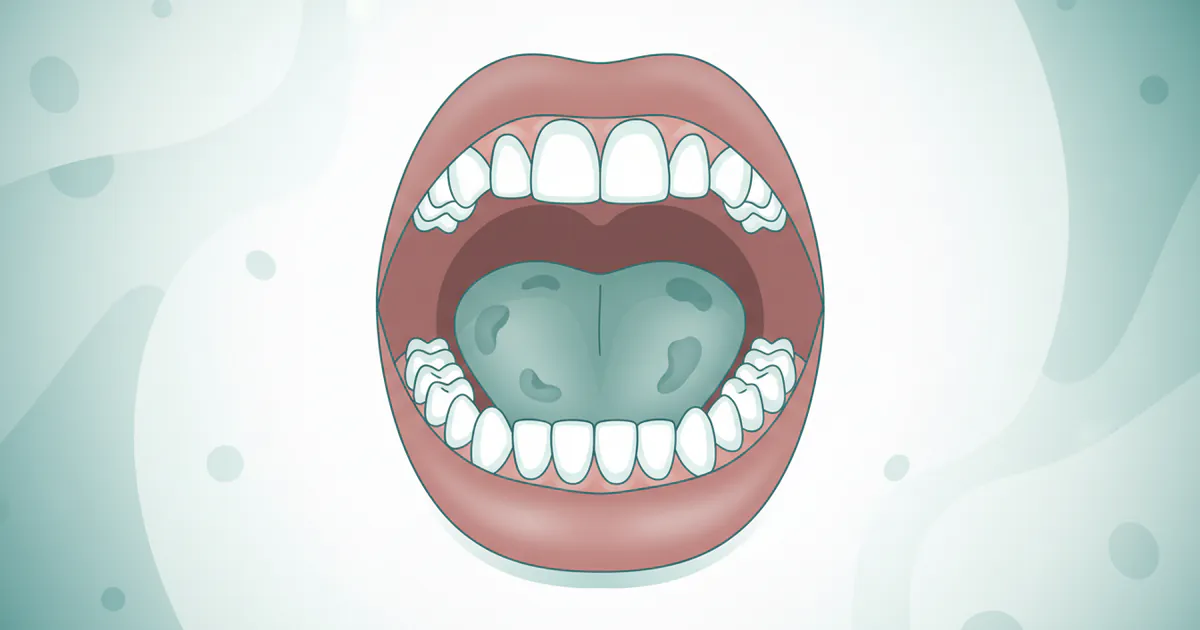
Mouth Cancer Photos: Complete Guide
Oral cancer is a formidable disease that affects tens of thousands of Americans each year, often with devastating consequences if not detected early. According to the Oral Cancer Foundation, approximately 54,000 Americans are diagnosed with oral or oropharyngeal cancer annually, and nearly 11,23
February 23, 2026