Molar Root Canal: Complete Guide
Key Takeaways
- Few dental procedures evoke as much apprehension as a root canal. Yet, for millions of Americans each year, this vital treatment is the difference between saving a natural tooth and facing extraction. When the infection or inflammation targets one of your large back teeth, you're looking at a **mola
Molar Root Canal: Complete Guide
Few dental procedures evoke as much apprehension as a root canal. Yet, for millions of Americans each year, this vital treatment is the difference between saving a natural tooth and facing extraction. When the infection or inflammation targets one of your large back teeth, you're looking at a molar root canal, a procedure that demands precision and expertise. Molar root canals are particularly complex due to their intricate anatomy, often featuring multiple canals that house the tooth's sensitive pulp. Understanding this procedure is crucial for anyone experiencing severe tooth pain, as it can alleviate discomfort, restore dental health, and prevent the spread of infection. This comprehensive guide will walk you through every aspect of a molar root canal, from what it entails and why it's necessary, to the step-by-step treatment process, associated costs, recovery expectations, and crucial aftercare instructions.
Key Takeaways:
- A molar root canal is a specialized procedure to remove infected or inflamed pulp from the complex canal system of a molar tooth, saving it from extraction.
- The procedure typically costs between $900 and $2,000 for a molar without insurance, potentially reaching $2,500+ depending on complexity and location.
- Root canal recovery time is usually 1-3 days for initial discomfort, but complete healing and crown placement can take several weeks.
- Deep decay, trauma, and cracks are the leading causes of molar pulp infection.
- Severe, persistent pain, sensitivity to hot/cold, and swelling are common symptoms indicating the need for treatment.
- Success rates for molar root canals exceed 90-95% when performed correctly, preserving your natural tooth for many years.
- A permanent crown is almost always recommended after a molar root canal to protect the weakened tooth structure and prevent fracture.
What Is a Molar Root Canal?
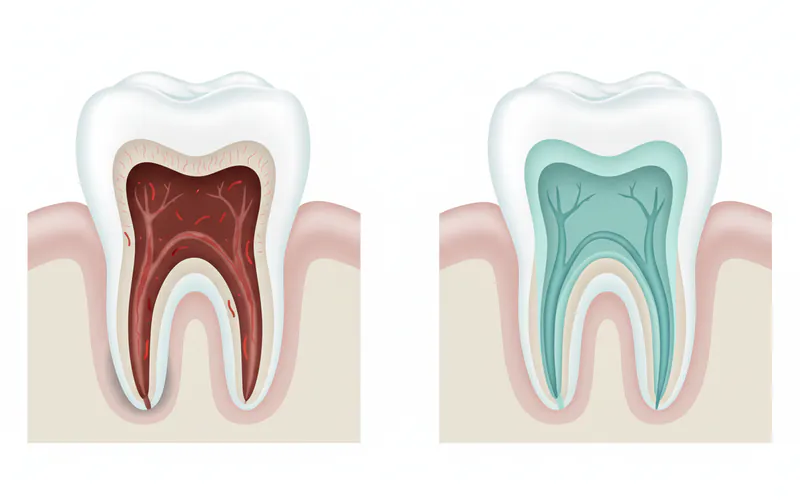
A molar root canal, formally known as endodontic therapy, is a dental procedure designed to save a tooth that has become severely infected or inflamed within its innermost layer, the dental pulp. The pulp contains nerves, blood vessels, and connective tissue, extending from the crown of the tooth down to the tips of the roots, located within the root canals. When this pulp becomes irreversibly damaged, it can cause excruciating pain and lead to serious dental abscesses if left untreated.
Molars, which are your large back teeth, are critical for chewing and grinding food. They are also known for having a more complex root system compared to front teeth (incisors) or canines. While incisors usually have one root and one canal, and premolars often have one or two, molars typically have two or three roots, each containing two or three canals, and sometimes even more (e.g., a "fourth" or "MB2" canal in upper molars). This intricate anatomy makes molar root canals more challenging and often requires the expertise of a specialist, an endodontist.
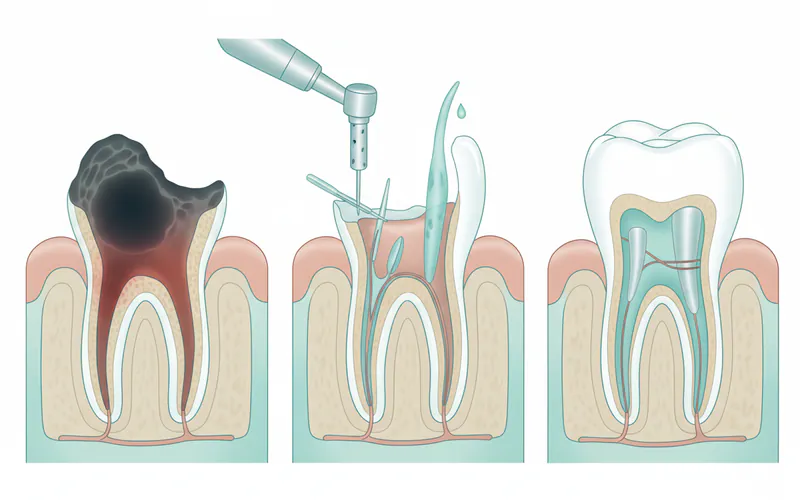
The goal of a molar root canal is to remove the diseased pulp, thoroughly clean and disinfect the entire canal system, and then seal it to prevent future infection. This process eliminates the source of pain and allows the tooth to remain in your mouth, functioning normally without its nerve, as the surrounding tissues will continue to nourish the tooth.
Anatomy of a Molar
Understanding molar anatomy helps explain the complexity:
- Crown: The visible part of the tooth above the gum line.
- Enamel: The hard, outer protective layer of the crown.
- Dentin: The layer beneath the enamel, making up the bulk of the tooth.
- Pulp Chamber: The hollow space within the crown containing the main part of the dental pulp.
- Root Canals: Narrow channels extending from the pulp chamber down through each root, housing the root portion of the pulp. Molars can have up to four or five canals, making thorough cleaning challenging.
- Apex: The very tip of each root, where nerves and blood vessels enter and exit the tooth.
Causes of Molar Pulp Infection or Inflammation
The dental pulp can become infected or inflamed due to several factors, primarily when bacteria find a way to penetrate the protective layers of enamel and dentin.
1. Deep Dental Decay (Cavities)
This is the most common cause. When a cavity is left untreated, bacteria erode through the enamel and dentin, eventually reaching the pulp chamber. Once bacteria invade the pulp, it becomes inflamed (pulpitis) and can lead to irreversible infection and necrosis (tissue death).
2. Tooth Trauma
A direct blow or injury to a molar can damage the pulp, even if there's no visible crack or chip. The trauma can sever blood vessels at the root tip, leading to pulp death over time. It can also cause internal resorption or calcification within the canals.
3. Cracks or Chips in the Tooth
Molars are subjected to significant biting forces, making them susceptible to cracks. A crack, whether visible or microscopic, can extend into the pulp chamber, allowing bacteria to enter and irritate the pulp. Vertical root fractures are particularly severe and often lead to extraction.
4. Repeated Dental Procedures
Multiple fillings, large fillings, or extensive restorative work on the same molar can sometimes weaken the tooth structure or irritate the pulp over time, eventually leading to inflammation or infection.
5. Advanced Gum Disease (Periodontal Disease)
In rare cases, severe periodontal disease can progress to the point where bacteria travel from the gum line down to the root tip, infecting the pulp through accessory canals in the root.
Signs and Symptoms You Need a Molar Root Canal
Recognizing the signs of pulp infection is crucial for seeking timely treatment and preventing further complications. While some people may experience no symptoms, most will have noticeable indicators.
Common Symptoms:
- Persistent or Spontaneous Pain: This is the hallmark symptom. The pain can range from mild to severe, often described as throbbing or aching. It may occur spontaneously without any trigger, especially at night, or linger for minutes/hours after a stimulus. This pain is often difficult to pinpoint to a specific tooth.
- Sensitivity to Hot and Cold: While mild sensitivity can indicate a simple cavity, severe and lingering sensitivity to hot or cold temperatures (the pain lasts for more than a few seconds after the stimulus is removed) is a strong sign of irreversible pulpitis.
- Pain When Chewing or Biting: Pressure sensitivity, especially when biting down, indicates inflammation around the root tip or within the tooth.
- Swelling: Swelling around the affected tooth, in the gum tissue, or even in the face or neck, signals an abscess (a pocket of pus) at the root tip due to advanced infection.
- Pimple-Like Bump on the Gums (Fistula): A small bump, often called a "gum boil," may appear on the gum near the infected tooth. This is a sign that the infection is draining, often temporarily relieving pain.
- Tooth Discoloration: The tooth may darken or appear grayish-black due to the death of the pulp tissue and internal bleeding.
- Tenderness to Touch: The tooth may feel tender when touched, indicating inflammation of the ligament surrounding the root.
Pro Tip: If you experience any of these symptoms, especially persistent pain or swelling, consult a dentist immediately. Delaying treatment can lead to more widespread infection, bone loss, and potentially the loss of the tooth.
Treatment Options
When the pulp of a molar is irreversibly damaged or infected, the primary treatment option is root canal therapy. However, it's important to understand the alternative, though it usually comes with longer-term consequences.
1. Root Canal Therapy (RCT) – The Recommended Treatment
Description: As detailed above, RCT involves removing the diseased pulp, thoroughly cleaning and shaping the root canals, and then sealing them to prevent reinfection. The tooth is then typically restored with a dental crown. Pros:
- Saves the natural tooth: Preserves your natural dentition, maintaining your bite and chewing function.
- Prevents spread of infection: Eliminates bacteria from the tooth, stopping an abscess and preventing systemic infection.
- Relieves pain: Effectively removes the source of excruciating pain.
- Cost-effective long-term: Often less expensive over time than extraction followed by a bridge or implant. Cons:
- Time-consuming: Requires one or more appointments.
- May require a crown: Adds to the overall cost and time.
- Potential for complications: Though rare, complications like missed canals or instrument separation can occur.
2. Tooth Extraction – The Alternative
Description: If a root canal is not possible, not desired, or if the tooth is too severely damaged to be saved, extraction is the only alternative. This involves surgically removing the entire tooth. Pros:
- Immediate relief from infection: Removes the source of infection entirely.
- Lower initial cost: Generally cheaper upfront than a root canal, especially without subsequent tooth replacement. Cons:
- Loss of natural tooth: Leads to a gap in your smile, which can affect aesthetics and function.
- Jawbone deterioration: The bone supporting the extracted tooth can resorb over time, leading to changes in facial structure and shifting of adjacent teeth.
- Shifting of adjacent teeth: Neighboring teeth can drift into the empty space, affecting your bite and potentially leading to new problems.
- Requires tooth replacement: To prevent issues like bone loss and shifting, the extracted tooth should ideally be replaced with a dental implant, bridge, or partial denture, which are often more costly and invasive than an initial root canal.
Comparison Table: Root Canal Therapy vs. Tooth Extraction
| Feature | Root Canal Therapy (RCT) | Tooth Extraction |
|---|---|---|
| Goal | Save natural tooth, remove infection, relieve pain | Remove infected tooth, relieve pain |
| Longevity | Can last a lifetime with proper care and restoration | Tooth is gone, requires replacement for long-term oral health |
| Cost (Initial) | Moderate to high (especially with crown) | Low to moderate (initially) |
| Cost (Long-Term) | Potentially lower than extraction + replacement | High if replaced with implant/bridge; can lead to other issues if not |
| Complexity | Moderate to high (especially for molars) | Moderate (surgical procedure) |
| Recovery | 1-3 days discomfort, permanent crown takes weeks | 3-7 days initial healing, bone graft/implant takes months |
| Effect on Adjacent Teeth | None, preserves natural bite and alignment | Can cause shifting, bite problems, and bone loss over time |
| Pain Relief | Excellent, targets source of infection | Excellent, but often replaced by discomfort from extraction site |
Step-by-Step Molar Root Canal Process
Understanding the steps involved can help alleviate anxiety about the procedure. A molar root canal typically takes one to two appointments, depending on the complexity of the infection and the number of canals.
Step 1: Diagnosis and Treatment Planning
Your dentist or endodontist will perform a thorough examination, including X-rays, to assess the extent of the infection and the anatomy of your molar's root canals. A vitality test (checking sensitivity to hot/cold) and percussion test (tapping the tooth) may also be performed. This step is crucial for accurate diagnosis and determining if a molar root canal is the appropriate treatment.
Step 2: Anesthesia
Before beginning, the dentist will administer a local anesthetic to numb the tooth and surrounding gum tissue. Modern anesthetics are highly effective, ensuring you won't feel pain during the procedure. You may feel pressure, but no sharp pain.
Step 3: Isolation
A rubber dam, a thin sheet of latex or non-latex material, is placed around the affected tooth. This isolates the tooth from saliva and bacteria in the mouth, keeping the area clean and dry throughout the procedure. It also prevents you from swallowing small instruments or debris.
Step 4: Access Cavity Preparation
The dentist will create a small opening (access cavity) through the crown of the tooth, usually on the chewing surface, to reach the pulp chamber and root canals. For molars, this access point is carefully designed to allow direct access to all canals, which can be challenging due to their posterior location and varied anatomy.
Step 5: Cleaning and Shaping the Canals (Instrumentation)
Using very small, flexible instruments called files (manual or rotary), the dentist carefully removes the infected or inflamed pulp tissue from the pulp chamber and each root canal. The canals are then meticulously cleaned and shaped to create a smooth, tapered space that can be effectively filled. This step is critical for molars, as their multiple and often curved canals require meticulous attention to ensure all infected tissue is removed. Irrigation solutions, such as sodium hypochlorite, are used repeatedly throughout this phase to disinfect the canals and flush out debris.
Step 6: Disinfection
Throughout the cleaning and shaping process, antibacterial and antiseptic solutions are used to thoroughly disinfect the root canals. In some cases, if the infection is severe, medication may be placed inside the canals and a temporary filling applied, requiring a second appointment for sealing.
Step 7: Filling and Sealing the Canals (Obturation)
Once the canals are clean, disinfected, and dry, they are filled with a biocompatible, rubber-like material called gutta-percha. This material is inserted into each canal along with an adhesive sealer to completely fill the space and prevent bacteria from re-entering. This process ensures a tight, hermetic seal.
Step 8: Temporary Restoration
After the canals are sealed, a temporary filling is placed in the access cavity to protect the tooth until a permanent restoration can be applied.
Step 9: Permanent Restoration (Crown)
This is a crucial final step, especially for molars. Because a root-canaled tooth is no longer vital and often has had significant tooth structure removed during the procedure or due to decay, it becomes more brittle and susceptible to fracture. A dental crown (a cap that covers the entire tooth) is almost always recommended to protect the tooth, restore its strength, and ensure its long-term success. This permanent restoration typically happens a few weeks after the root canal by your general dentist.
Pro Tip: Do not delay getting your permanent crown. A root-canaled molar without a crown is at a significantly higher risk of fracturing, potentially leading to the loss of the tooth you just worked to save. The American Dental Association (ADA) emphasizes the importance of a proper final restoration for root canal longevity.
Cost and Insurance for a Molar Root Canal
The cost of a molar root canal can vary significantly based on several factors, including the specific tooth being treated, the complexity of the case, the geographical location of the dental practice, and whether a general dentist or a specialist (endodontist) performs the procedure. Molars are generally more expensive than anterior teeth or premolars due to their multiple, complex canals.
Average US Cost Ranges (Without Insurance):
- Molar Root Canal: $900 to $2,000
- In some complex cases or high-cost-of-living areas, this can extend to $2,500 or more.
- Important Note: This cost typically covers only the root canal procedure itself. The cost of the permanent restoration (dental crown) is separate and typically ranges from $800 to $2,500.
Factors Influencing Cost:
- Tooth Location: Molars (back teeth) have more roots and canals, making them harder to treat, thus more expensive.
- Complexity: Re-treatment of a failed root canal, teeth with severely curved or calcified canals, or those requiring special techniques will cost more.
- General Dentist vs. Endodontist: An endodontist (root canal specialist) typically charges more due to their specialized training, equipment (like operating microscopes), and expertise. However, their higher success rates can make it a worthwhile investment, especially for molars.
- Geographic Location: Dental costs are generally higher in major metropolitan areas or regions with a higher cost of living.
- Ancillary Costs: This might include diagnostic X-rays, emergency exams, post-and-core buildup (if significant tooth structure is lost), and the final crown.
How Much Is a Root Canal Without Insurance?
For individuals without dental insurance, the full cost of a molar root canal and its subsequent crown will be your responsibility. This is why understanding the ranges is critical.
- Total estimated cost (root canal + crown) without insurance can be between $1,700 and $4,500, or even higher.
- Many dental offices offer discounts for cash payments or payment plans for uninsured patients. Always ask about these options.
Dental Insurance Coverage:
Most dental insurance plans offer some coverage for root canal therapy, as it is considered a major restorative procedure.
- PPO Plans: Typically cover 50% to 80% of the root canal cost after your deductible is met, often subject to an annual maximum benefit (e.g., $1,000-$2,000 per year). You usually have the freedom to choose any dentist.
- HMO/DMO Plans: These plans often require you to see an in-network dentist and may have a co-pay or fixed fee for the procedure, which can be significantly lower than PPO plans.
- Medicaid: Coverage for root canals under Medicaid varies significantly by state. Some states offer comprehensive adult dental benefits, while others provide very limited or no coverage for complex procedures like molar root canals. You must check with your state's Medicaid program directly.
- Waiting Periods: Be aware that many dental insurance plans have waiting periods (e.g., 6-12 months) before covering major procedures like root canals.
Pro Tip: Before undergoing any procedure, always get a detailed written estimate from your dentist, outlining the costs for the root canal and the necessary crown. Submit this pre-treatment estimate to your insurance company to understand your exact out-of-pocket expenses.
Cost Breakdown Table: Molar Root Canal (US Averages, 2024)
| Item | Average Cost Range (Without Insurance) | Average Insurance Coverage (PPO, 50-80%) | Estimated Patient Out-of-Pocket (PPO) |
|---|---|---|---|
| Molar Root Canal | $900 - $2,000 | $450 - $1,600 | $300 - $1,000 (after deductible) |
| Post and Core (if needed) | $200 - $500 | $100 - $400 | $100 - $250 |
| Dental Crown (Permanent) | $800 - $2,500 | $400 - $2,000 | $400 - $1,250 |
| Total Estimated Cost | $1,900 - $5,000+ | (Varies greatly by plan & max) | $800 - $2,500+ (after deductible & max) |
| Note: Costs are approximate and can vary widely. Always confirm with your provider and insurance. |
Recovery and Aftercare for a Molar Root Canal
Root canal recovery time is generally straightforward, but it's essential to follow your dentist's instructions carefully to ensure proper healing and prevent complications.
Immediately After the Procedure (First 24-48 hours):
- Numbness: Your mouth will likely remain numb for several hours after the procedure due to the local anesthetic. Avoid chewing on the treated side until the numbness completely wears off to prevent accidental biting of your cheek or tongue.
- Mild Discomfort/Soreness: It's normal to experience some mild discomfort, tenderness, or dull ache around the treated tooth and gum area once the anesthesia wears off. This is due to the inflammation from the infection and the manipulation during the procedure.
- Pain Management: Over-the-counter pain relievers like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are usually sufficient to manage post-operative pain. Your dentist may prescribe stronger pain medication if necessary. Take as directed.
- Diet: Stick to soft foods for the first day or two. Avoid very hot, cold, crunchy, or chewy foods that could irritate the area or dislodge the temporary filling. Chew on the opposite side of your mouth.
- Avoid Smoking and Alcohol: These can impair healing and should be avoided.
Short-Term Recovery (First Few Days to Weeks):
- Swelling: Minimal swelling is possible but should subside quickly. Apply a cold compress to your cheek if needed.
- Oral Hygiene: Continue your regular brushing and flossing routine, but be gentle around the treated tooth.
- Temporary Filling Care: Be mindful of the temporary filling. While durable, it's not as strong as your permanent restoration. Avoid chewing directly on it excessively. If it falls out or feels loose, contact your dentist immediately.
- Crown Placement: The most critical part of molar root canal aftercare is the placement of the permanent crown. This typically occurs within 2-4 weeks after the root canal. Do not delay this step, as the tooth is vulnerable to fracture without it.
Long-Term Care:
- Permanent Crown: Once the permanent crown is placed, your tooth should feel and function like a normal tooth.
- Oral Hygiene: Maintain excellent oral hygiene with regular brushing (twice daily) and flossing (daily).
- Regular Dental Check-ups: Continue with your routine dental exams and cleanings (usually every six months). Your dentist will monitor the treated tooth and the surrounding tissues to ensure long-term success.
- Avoid Hard Foods: While a crowned tooth is strong, avoid excessively hard or sticky foods that could potentially damage the crown or the underlying tooth structure.
- Nightguards: If you clench or grind your teeth (bruxism), a nightguard can protect your root-canaled and crowned tooth from excessive forces.
Pro Tip: Most people can return to their normal activities, including work or school, the day after a root canal. If you experience severe pain, swelling, or an allergic reaction, contact your dentist immediately.
Prevention of Molar Root Canal
Preventing the need for a molar root canal largely revolves around maintaining excellent oral hygiene and addressing dental problems promptly.
1. Excellent Oral Hygiene
- Brush Twice Daily: Use fluoride toothpaste and brush for at least two minutes, focusing on all surfaces of your molars.
- Floss Daily: Flossing removes plaque and food particles from between teeth and along the gum line, where toothbrushes can't reach. This is especially important for molars, which have large contact points.
- Antiseptic Mouthwash: Using an ADA-accepted antiseptic mouthwash can help reduce bacteria in the mouth.
2. Regular Dental Check-ups and Cleanings
- Bi-annual Visits: Visit your dentist every six months for professional cleanings and examinations. Regular check-ups allow your dentist to detect and treat cavities early, before they become deep enough to infect the pulp. X-rays can reveal problems not visible to the naked eye.
3. Prompt Treatment of Cavities
- Don't ignore small cavities. Fillings can repair decay and prevent it from progressing to the pulp. Addressing a cavity early is significantly less invasive and expensive than a root canal.
4. Protect Your Teeth from Trauma
- Mouthguards for Sports: If you play contact sports, wear a custom-fitted mouthguard to protect your molars from impact injuries.
- Nightguards for Bruxism: If you grind or clench your teeth (bruxism), your dentist can provide a custom nightguard to protect your teeth from excessive wear, cracks, and fractures.
5. Limit Sugary and Acidic Foods/Drinks
- Frequent consumption of sugary snacks and acidic beverages can erode enamel and contribute to cavity formation. Opt for a balanced diet rich in fruits, vegetables, and whole grains.
Risks and Complications of a Molar Root Canal
While root canal therapy has a high success rate (over 90-95% for initial treatment), like any medical procedure, there are potential risks and complications, although they are generally rare.
1. Persistent Infection or Re-infection
- Missed Canals: Molars, especially upper molars, can have extra or very small, calcified canals (like the MB2 canal) that are difficult to locate and clean. If a canal is missed, infection can persist.
- Incomplete Cleaning: In rare cases, bacteria may remain in the canals if the cleaning and shaping were not thorough enough.
- Recurrent Decay: New decay under the crown or filling can allow bacteria to re-enter the tooth.
- Leakage: A leaky permanent filling or crown can allow bacteria to penetrate the sealed canals.
- Cracked Tooth/Root: A new crack or fracture in the tooth after the procedure can allow bacteria to enter.
2. Instrument Separation
During the cleaning and shaping phase, a small, delicate file can sometimes break off inside the root canal. While endodontists are skilled at removing these fragments, sometimes they cannot be retrieved. If the canal is already mostly clean, the fragment can be sealed within the canal, and the tooth may still be successfully saved. If the fragment blocks further cleaning in an infected area, it might require surgical removal or impact the prognosis.
3. Perforation
Accidental creation of a hole in the side of the tooth or root during access or canal preparation. Small perforations can often be repaired, but larger ones may compromise the tooth's long-term prognosis.
4. Post-operative Flare-up
While discomfort is normal, some patients experience a significant increase in pain and swelling a few days after the procedure. This "flare-up" is usually manageable with medication but requires follow-up with the dentist.
5. Allergic Reaction
Though rare, an allergic reaction to the anesthetic, rubber dam, or materials used to clean or fill the canals can occur.
6. Tooth Fracture
As mentioned, a root-canaled tooth becomes more brittle. Without a proper, timely permanent crown, the tooth is at a significantly higher risk of fracturing, especially a molar which bears heavy chewing forces. A severe fracture might necessitate extraction.
7. Discoloration
While less common with modern techniques, some root-canaled teeth, especially those treated for trauma, can darken over time. This can often be managed with internal bleaching or a crown.
Pro Tip: Choosing an experienced endodontist for your molar root canal can significantly reduce the risk of complications, especially for complex cases. Their specialized training and advanced equipment allow for more precise and thorough treatment.
Children / Pediatric Considerations for Molar Root Canals
While primary (baby) teeth molars can get infections, they are typically treated with procedures like pulpotomies (partial pulp removal) or pulpectomies (complete pulp removal in the crown and canals, similar to a root canal but for primary teeth), followed by a stainless steel crown. The goal is to save the baby tooth until it naturally falls out, preserving space for the permanent tooth.
For permanent molars in children and adolescents, root canal therapy is performed similarly to adults. However, there are unique considerations:
- Immature Apex: If a young permanent molar has not fully developed its root (an "open apex"), special procedures like apexification or revascularization (regenerative endodontic procedures) may be performed. These aim to encourage continued root development and strengthen the tooth, rather than merely filling the canal. These advanced techniques are typically performed by an endodontist.
- Trauma: Children are prone to dental trauma, which can damage the pulp of developing permanent molars, necessitating root canal treatment or one of the regenerative procedures.
- Early Decay: Despite preventive efforts, some children develop deep cavities in their permanent molars early on, potentially leading to pulp infection.
- Cooperation: Younger children might find it more challenging to sit through a lengthy procedure. Pediatric dentists and endodontists are skilled at managing children's anxiety and pain.
Pro Tip for Parents: If your child complains of persistent tooth pain, sensitivity, or has swelling around a molar, seek dental care immediately. Early intervention can often save a permanent molar, which is crucial for their developing bite and overall oral health.
Frequently Asked Questions
What is the difference between a root canal and an extraction?
A root canal is a procedure to save an infected tooth by removing the diseased pulp and sealing the inner tooth structure. An extraction is the complete removal of the tooth from the mouth. While an extraction is simpler initially, it leads to a missing tooth that often needs replacement with an implant or bridge for long-term oral health, which can be more costly and complex than a root canal.
How painful is a molar root canal?
With modern anesthetics, a molar root canal is typically no more painful than getting a routine filling. The goal of the procedure is to relieve the severe pain caused by the infection. You may feel some pressure during the procedure and mild soreness for a few days afterward, which is usually manageable with over-the-counter pain medication.
How long does a molar root canal take?
A molar root canal usually takes 90 minutes to 3 hours for a single appointment. If the infection is severe or the case is particularly complex, it may require two appointments, spread over a few days or weeks, to ensure thorough disinfection and allow the infection to subside before final sealing.
Can a molar root canal fail?
Yes, though the success rate is very high (over 90-95%). Failure can occur if a canal is missed during cleaning, the seal breaks down allowing bacteria to re-enter, or if the tooth fractures. In such cases, re-treatment (another root canal), apicoectomy (surgical removal of the root tip), or extraction might be necessary.
Will I need a crown after a molar root canal?
Yes, for molars, a permanent crown is almost always recommended and is crucial for the long-term success of the root canal. A root-canaled molar, without its blood supply and nerve, becomes more brittle and is significantly more prone to fracture without the protective coverage of a dental crown.
How much is a molar root canal without insurance?
Without insurance, a molar root canal can cost anywhere from $900 to $2,000, with some complex cases potentially exceeding $2,500. This estimate does not include the separate cost of the permanent dental crown, which can add another $800 to $2,500.
Are there alternatives to a molar root canal?
The primary alternative to a molar root canal is tooth extraction. While extraction provides immediate relief from the infected tooth, it creates a gap that can lead to shifting teeth, bone loss, and issues with chewing. The extracted tooth should ideally be replaced with a dental implant or bridge to maintain oral health.
What is the root canal recovery time?
Initial root canal recovery time from discomfort typically lasts 1-3 days, managed with over-the-counter pain relievers. The tooth will need a few weeks to heal before the permanent crown is placed. Complete healing of the bone around the root can take several months, but you can usually resume normal activities quickly.
Can a general dentist perform a molar root canal, or do I need a specialist?
General dentists are trained to perform root canals, and many successfully treat molars. However, due to the complex anatomy of molar root canals (multiple, often curved or calcified canals), your general dentist may refer you to an endodontist, who is a root canal specialist. Endodontists have advanced training and specialized equipment (like operating microscopes) that can improve success rates for complex cases.
Will my tooth be dead after a root canal?
No, not in the traditional sense. The pulp, which contains the nerves and blood vessels inside the tooth, is removed. This means the tooth itself is no longer "vital" or "alive" in terms of feeling hot/cold or pain. However, the tooth structure remains, and it is still nourished by the surrounding tissues and periodontal ligament, allowing it to function normally in your mouth.
When to See a Dentist
Recognizing the signs that warrant immediate dental attention is critical for preventing the escalation of dental problems.
See a Dentist Immediately If You Experience:
- Severe, persistent toothache: Especially if it wakes you up at night, throbs constantly, or doesn't respond to over-the-counter pain relievers. This is a classic sign of irreversible pulpitis.
- Extreme sensitivity to hot or cold: If the pain lingers for more than 30 seconds after the stimulus is removed, it indicates serious pulp damage.
- Swelling in your gums, cheek, or jaw: This points to a spreading infection (abscess) that requires urgent treatment to prevent systemic complications.
- A "pimple" or boil on your gums: This is a fistula, a sign of infection draining, and needs to be addressed promptly.
- Pain when chewing or biting: Especially if it's localized to one molar and severe.
- Darkening or discoloration of a tooth: This can signify a dying nerve and warrants investigation.
- Trauma to a tooth: If a molar has been chipped, cracked, or knocked (even if not visibly damaged), seek dental attention to assess potential pulp damage.
Red Flags That Need Prompt Attention (Within 24-48 Hours):
- Any of the above symptoms, even if mild at first, that start to worsen or become more frequent.
- A lost or damaged temporary filling after a previous dental procedure.
- Increasing tenderness to touch around a molar.
Routine Care Guidance:
- Regular dental check-ups and cleanings (every six months) are essential to catch problems like cavities early, before they progress to the point of needing a root canal.
- Don't ignore mild sensitivity or minor toothaches, as they can be early warning signs of developing issues that are easier and less expensive to treat in their initial stages.
Trust your instincts. If something feels wrong with your molar, it's always best to err on the side of caution and schedule an appointment with your dentist or an endodontist. Early diagnosis and treatment are key to preserving your natural teeth and maintaining optimal oral health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Stop Throbbing Pain After Root Canal
Undergoing a root canal procedure is often a necessary step to save a tooth severely damaged by decay or infection, preventing further complications and excruciating pain. While the procedure itself is performed under local anesthesia to ensure comfort, it's common for patients to experience some le
February 22, 2026
Root Canal After Care: Complete Guide
A root canal procedure can be a tooth-saving treatment, offering relief from pain and preventing further infection. However, the success and longevity of this crucial dental intervention heavily rely on diligent root canal after care. Neglecting post-treatment instructions can lead to complicati
February 22, 2026

Can You Drive After a Root Canal
Undergoing a root canal procedure can understandably bring up a host of questions and concerns, from understanding the process itself to managing recovery. One of the most common and practical inquiries people have is: can you drive after a root canal? The answer isn't always a simple yes or no,
February 22, 2026
Is a Root Canal Painful
When facing the prospect of a root canal, one of the most common and immediate questions that comes to mind is: is a root canal painful? It's a valid concern, stemming from outdated perceptions and anecdotal stories. However, modern root canal therapy is a highly effective and generally comforta
February 22, 2026