Complete Guide to Senior Dental Care: Everything You Need to Know

Key Takeaways
- As we age, our bodies undergo numerous changes, and our oral health is no exception. In fact, more than 70% of older adults (age 65 and older) in the United States have some form of periodontal (gum) disease, according to the Centers for Disease Control and Prevention (CDC). This statistic under
Complete Guide to Senior Dental Care: Everything You Need to Know
As we age, our bodies undergo numerous changes, and our oral health is no exception. In fact, more than 70% of older adults (age 65 and older) in the United States have some form of periodontal (gum) disease, according to the Centers for Disease Control and Prevention (CDC). This statistic underscores a critical truth: maintaining excellent dental hygiene isn't just for youth; it's a lifelong commitment that becomes even more vital in our golden years. Understanding the unique challenges and proactive steps necessary for senior dental care is paramount to preventing pain, preserving function, and safeguarding overall health.
This comprehensive guide from SmilePedia.net will equip you with all the essential knowledge to navigate senior oral health effectively. We’ll delve into common issues like receding gums and how to stop tooth root decay, explore advanced treatment options, discuss practical prevention strategies including how to eat fruit without damaging teeth, and provide crucial insights into managing costs and insurance. By the end of this article, you'll have a clear roadmap to ensure a healthy, comfortable smile for years to come.
Key Takeaways:
- Preventive Care is Paramount: Regular dental check-ups (at least twice a year) and diligent daily oral hygiene are the foundation of senior dental health, costing around $100-$300 per visit without insurance.
- Root Decay is a Major Concern: Receding gums, dry mouth, and lifelong wear contribute to increased risk. Prevention focuses on fluoride, meticulous hygiene, and addressing dry mouth. Treating root decay can range from $150 for a filling to $1,500+ for a root canal and crown.
- Dry Mouth (Xerostomia) is Widespread: Affecting up to 30% of older adults, often due to medications. Managing it is crucial for preventing decay and gum disease.
- Medicare's Limitations: Original Medicare generally does NOT cover routine dental care. Medicare Advantage plans often include some dental benefits, but coverage limits and deductibles vary significantly, typically offering $1,000-$2,000 in annual benefits.
- Dental Implants Offer Stability: While costly ($3,000-$6,000 per implant), they provide a durable, long-term solution for tooth loss, vastly improving quality of life compared to traditional dentures.
- Dietary Choices Matter: Modifying how you consume acidic or sugary foods (e.g., rinsing after fruit consumption, avoiding prolonged exposure) can significantly reduce enamel erosion and decay risk.
- Oral Health Impacts Systemic Health: Poor senior dental care is linked to increased risks of heart disease, diabetes complications, pneumonia, and even certain dementias.
What It Is / Overview: Understanding Senior Oral Health
Senior dental care isn't just about addressing problems; it's about understanding the unique physiological and lifestyle factors that impact oral health as we age. With advancements in modern dentistry and overall healthcare, more people are retaining their natural teeth longer than ever before. This is a tremendous benefit, but it also means those teeth have endured decades of use, chewing, and potential exposure to decay and disease.
Physiological Changes:
- Enamel Wear: Years of chewing, teeth grinding-teeth-grinding-everything-you-need-to-know "Complete Guide to Bruxism & Teeth Grinding: Everything You Need to Know") (bruxism), and acidic food/drink exposure can thin and weaken enamel, making teeth more susceptible to decay and sensitivity.
- Gum Recession: A common occurrence, gums naturally recede over time, exposing the tooth roots. Unlike enamel, tooth roots are covered by cementum, which is softer and more porous, making them highly vulnerable to decay.
- Reduced Saliva Flow (Dry Mouth): Often a side effect of medications (seniors typically take more prescriptions), certain medical conditions (e.g., Sjögren's syndrome, diabetes), or radiation therapy. Saliva is vital for washing away food particles, neutralizing acids, and remineralizing enamel. Its reduction dramatically increases the risk of decay and gum disease.
- Bone Density Loss: Can affect the jawbone, potentially impacting the stability of natural teeth and the success of dental implants.
- Decreased Dexterity: Conditions like arthritis or stroke can make effective brushing and flossing challenging.
Lifestyle and Health Factors:
- Medication Use: Polypharmacy (taking multiple medications) is prevalent in seniors, with many drugs causing dry mouth as a side effect.
- Systemic Diseases: Diabetes, heart disease, osteoporosis, and autoimmune disorders can all have significant oral manifestations or complicate dental treatments. The bidirectional relationship between oral health and systemic health is particularly pronounced in older adults.
- Dietary Changes: Some seniors may gravitate towards softer, often more processed or sugary foods if they have chewing difficulties, contributing to decay.
- Smoking and Alcohol Use: These habits significantly increase the risk of gum disease, oral cancer, and tooth loss.
- Cognitive Decline: Conditions like Alzheimer's or dementia can severely impair a person's ability to maintain personal oral hygiene, requiring caregiver involvement.
Understanding these intertwined factors is the first step toward proactive and effective senior dental care, aiming to preserve function, comfort, and overall well-being.
Common Dental Issues Affecting Seniors
As the body ages, so do the teeth and gums, making seniors particularly susceptible to a range of specific oral health concerns. Recognizing these issues early is key to effective intervention.
Root Decay
Root decay occurs on the exposed surfaces of the tooth roots, often due to gum recession. It is a significant concern for seniors because the cementum covering the root is softer than enamel and more vulnerable to acid attack.
- Causes: Primarily gum recession (exposing the root), dry mouth (lack of protective saliva), poor oral hygiene, and a diet high in sugars and acids.
- Signs: Darkened areas on the tooth near the gum line, sensitivity to hot, cold, or sweets, and sometimes pain when chewing.
- Pro Tip: If you notice new sensitivity or discolored spots near your gum line, schedule a dental check-up immediately. Early detection of root decay can often be treated with less invasive methods.
Gum Disease (Periodontal Disease)
Periodontal disease is an infection of the tissues that hold your teeth in place. It becomes more prevalent and often more severe with age.
- Causes: Primarily plaque buildup due to poor oral hygiene, exacerbated by dry mouth, systemic diseases (like diabetes), smoking, and hormonal changes.
- Signs: Red, swollen, or tender gums; bleeding gums (especially when brushing or flossing); persistent bad breath; receding gums; pus between teeth and gums; loose or separating teeth; changes in bite.
- Types:
- Gingivitis: The mildest form, reversible with good oral hygiene and professional cleaning.
- Periodontitis: More severe, involving bone loss around the teeth. Can be chronic or aggressive.
Dry Mouth (Xerostomia)
As mentioned, dry mouth is not a normal part of aging but is extremely common in seniors due to medications (antihistamines, decongestants, pain relievers, diuretics, blood pressure drugs, antidepressants, muscle relaxants), medical conditions (diabetes, Parkinson's, Alzheimer's, stroke, Sjogren's syndrome), and treatments like radiation therapy.
- Causes: Primarily medication side effects, systemic diseases, or medical treatments.
- Signs: A sticky, dry feeling in the mouth; frequent thirst; sores in the mouth; cracked lips; a dry, rough tongue; difficulty speaking, chewing, or swallowing; bad breath; increased tooth decay.
- Impact: Significantly increases the risk of tooth decay, gum disease, and oral infections like thrush.
Tooth Loss and Edentulism
While declining, tooth loss remains a major issue for seniors. Complete tooth loss (edentulism) impacts nutrition, speech, self-esteem, and overall quality of life.
- Causes: Untreated decay, severe gum disease, trauma, or previous extractions.
- Impact: Chewing difficulties, limited food choices (often leading to softer, less nutritious diets), digestive issues, speech impediments, changes in facial structure.
Denture-Related Issues
For those with dentures, issues can arise over time.
- Causes: Ill-fitting dentures (due to changes in jawbone density over time), improper cleaning, or prolonged wear.
- Signs: Sores or irritation in the mouth, difficulty chewing, clicking sounds during speech, oral thrush (denture stomatitis), or chronic bad breath.
- Types:
- Complete Dentures: Replace all teeth in an arch.
- Partial Dentures: Replace some missing teeth.
- Implant-Supported Dentures: Offer superior stability and retention.
Oral Cancer
The risk of oral cancer increases with age, particularly in those with a history of tobacco and alcohol use.
- Causes: Tobacco products (smoking, chewing), heavy alcohol consumption, human papillomavirus (HPV) infection, and prolonged sun exposure to the lips.
- Signs: Persistent sore, lump, or white/red patch in the mouth or on the lips; difficulty chewing or swallowing; numbness in the mouth; persistent sore throat; voice changes.
- Importance: Early detection is crucial for successful treatment outcomes. Regular dental check-ups include oral cancer screenings.
Oral Thrush (Candidiasis)
A fungal infection common in individuals with weakened immune systems, those taking antibiotics, or denture wearers.
- Causes: Candida albicans fungus overgrowth, often linked to dry mouth, diabetes, antibiotic use, or compromised immunity.
- Signs: Creamy white lesions on the tongue, inner cheeks, roof of the mouth, gums, or tonsils; slight bleeding if lesions are scraped; pain; difficulty swallowing.
Advanced Treatment Options for Senior Dental Health
Modern dentistry offers a wide array of treatment options tailored to the specific needs of seniors, from conservative interventions to advanced restorative procedures.
Fillings
For cavities, including those on exposed root surfaces.
- Process: Removal of decayed material, cleaning, and filling with composite resin (tooth-colored) or amalgam (silver). Root surface fillings often use specific materials designed for cementum.
- Pros: Restores tooth structure, prevents further decay, relatively inexpensive.
- Cons: Not permanent, may need replacement.
- Cost: $150-$400 per filling, depending on material and size.
Root Canals
When decay or trauma reaches the tooth's pulp (nerve) causing infection.
- Process: Removal of infected pulp, cleaning and shaping the root canal, filling with a sterile material, and usually capping with a crown to protect the weakened tooth.
- Pros: Saves a natural tooth from extraction, preserves chewing function.
- Cons: Can be costly, multiple appointments, temporary sensitivity.
- Cost: $700-$1,500 for a front tooth, $1,000-$2,000 for a molar (excluding crown cost).
Gum Disease Treatments
Treatment depends on the severity.
- Scaling and Root Planing (Deep Cleaning): Removal of plaque and tartar from above and below the gum line, and smoothing rough spots on the roots to remove bacteria.
- Pros: Non-surgical, highly effective for moderate gum disease.
- Cons: May require local anesthesia, minor discomfort afterward.
- Cost: $200-$500 per quadrant.
- Periodontal Surgery: For advanced cases to reduce pocket depth, regenerate bone, or cover exposed roots.
- Pros: Can halt disease progression, save teeth.
- Cons: Invasive, longer recovery, more expensive.
- Cost: $500-$3,000 per quadrant, depending on procedure.
Restorative Dentistry
Restoring missing or damaged teeth.
- Crowns: Caps placed over damaged teeth to restore shape, size, strength, and appearance.
- Pros: Protects weakened teeth, improves aesthetics.
- Cons: Requires tooth reduction, costly.
- Cost: $800-$2,500 per crown (porcelain-fused-to-metal, all-ceramic).
- Bridges: Fixed prosthetics to replace one or more missing teeth by cementing crowns to adjacent natural teeth (abutments).
- Pros: Non-removable, restores chewing and speech.
- Cons: Requires modifying healthy adjacent teeth, can be challenging to clean.
- Cost: $2,000-$5,000 for a 3-unit bridge.
- Dental Implants: Titanium posts surgically placed into the jawbone to serve as artificial tooth roots.
- Pros: Most natural-feeling and durable replacement option, preserves bone, non-removable, does not affect adjacent teeth.
- Cons: High initial cost, surgical procedure, longer treatment timeline (several months), not suitable for everyone (requires adequate bone density).
- Cost: $3,000-$6,000 per implant (crown extra).
- Dentures (Full & Partial): Removable appliances to replace missing teeth and surrounding tissues.
- Pros: Cost-effective, non-invasive (traditional), improves aesthetics and function.
- Cons: Can be less stable than implants, may require adjustments, needs diligent cleaning.
- Types: Conventional, immediate, overdentures (supported by implants).
- Cost: $1,000-$3,000 for a conventional full upper or lower denture; $4,000-$8,000+ for implant-supported dentures.
Addressing Dry Mouth
- Strategies: Use over-the-counter saliva substitutes (gels, sprays, rinses), chew sugar-free gum or suck on sugar-free candies, use a humidifier at night, increase water intake, avoid caffeine and alcohol. Your dentist may also recommend prescription medications (e.g., pilocarpine, cevimeline) to stimulate saliva flow.
- Importance: Crucial for preventing widespread decay and improving comfort.
Oral Cancer Screenings
- Process: A routine part of every dental exam, involving visual and tactile examination of the entire mouth, throat, and neck for any suspicious lesions or lumps.
- Importance: Early detection significantly increases survival rates.
Step-by-Step Process: What to Expect During Common Senior Dental Procedures
Understanding what happens during a dental procedure can alleviate anxiety. Here's a brief overview of what to expect for two common treatments for seniors.
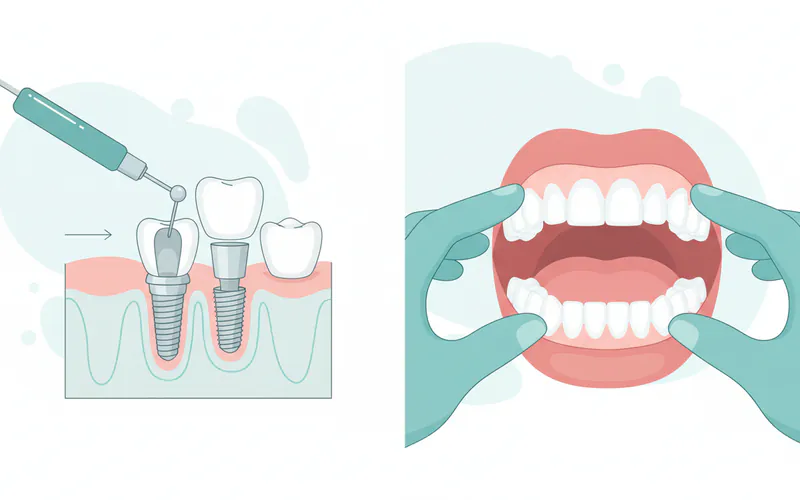
1. Dental Implant Placement (Single Tooth)
- Initial Consultation & Planning: Your dentist will conduct a thorough examination, including X-rays and 3D scans, to assess your jawbone density and determine if you are a candidate for implants. This phase is crucial for precise placement.
- Tooth Extraction (if needed): If the damaged tooth is still present, it will be extracted. The site may need time to heal, or immediate implant placement might be possible.
- Bone Grafting (if needed): If your jawbone isn't dense enough, a bone graft may be performed to build up the bone. This adds several months to the overall treatment timeline.
- Implant Placement Surgery: Under local anesthesia (and sometimes sedation), the dentist or oral surgeon makes a small incision in your gum to expose the bone. A pilot hole is drilled, and the titanium implant screw is carefully placed into the jawbone. The gum is then sutured closed.
- Osseointegration (Healing): This is the critical period (3-6 months) where the implant fuses with your jawbone. You'll likely wear a temporary crown or partial denture during this time.
- Abutment Placement: Once osseointegration is complete, a small connector piece (abutment) is attached to the implant, extending above the gum line.
- Crown Placement: Impressions are taken, and a custom-made crown (matching your natural teeth) is fabricated. This crown is then cemented or screwed onto the abutment, completing the restoration.
- Follow-up Care: Regular check-ups are essential to ensure the implant remains healthy.
2. Scaling and Root Planing (Deep Cleaning)
- Assessment: Your dental hygienist or dentist will assess your gum health, measure periodontal pockets, and identify areas of plaque and tartar buildup.
- Anesthesia (Optional): For comfort, local anesthetic may be administered to numb the specific areas being treated, especially if pockets are deep or gums are sensitive.
- Scaling: Using specialized instruments (ultrasonic scalers and hand scalers), the hygienist meticulously removes plaque and tartar from above and below the gum line, down into the periodontal pockets.
- Root Planing: The root surfaces are then smoothed to remove any remaining bacterial toxins and rough spots. This helps the gums reattach to the teeth more effectively and makes it harder for plaque to accumulate.
- Antimicrobial Rinse/Medication (Optional): In some cases, an antimicrobial rinse or antibiotic medication may be placed in the pockets to help control infection.
- Post-Procedure Care: You may experience some sensitivity or soreness for a few days. The dental team will provide instructions on home care and schedule follow-up appointments to monitor healing. Often, deep cleaning is done in multiple appointments, treating one or two quadrants of the mouth at a time.
Preventing Dental Issues in Seniors: Your Proactive Guide
Prevention is the cornerstone of effective senior dental care. By adopting diligent habits and making informed choices, you can significantly reduce your risk of common oral health problems.
Daily Oral Hygiene
Consistent and thorough daily care is non-negotiable.
- Brushing: Brush at least twice a day for two minutes each time, using a soft-bristled toothbrush or an electric toothbrush. Electric toothbrushes are often recommended for seniors, especially those with arthritis or dexterity issues, as they do most of the work for you and can be more effective at plaque removal. Use a fluoride toothpaste. The ADA recommends brushing all surfaces of your teeth, including the gum line.
- Flossing / Interdental Cleaners: Floss daily to remove plaque and food particles from between teeth and under the gum line where a toothbrush can't reach. If traditional floss is difficult, consider using floss picks, interdental brushes, or a water flosser.
- Mouthwash: Use an antimicrobial, alcohol-free mouthwash, especially if recommended by your dentist for gum health or dry mouth. Alcohol can further dry out the mouth.
- Pro Tip: If you have limited dexterity, consider modifying your toothbrush handle (e.g., adding a tennis ball or bicycle grip) or using an electric toothbrush with a larger handle.
Dietary Habits and How to Eat Fruit Without Damaging Teeth
Your diet plays a crucial role in preventing decay and maintaining gum health.
- Limit Sugary and Acidic Foods/Drinks: Sugars feed bacteria that produce acids, leading to decay. Acids directly erode enamel. This includes candies, sodas, fruit juices, and many processed snacks.
- Embrace Water: Drink plenty of water throughout the day, especially if you experience dry mouth. Water helps rinse away food particles and acids.
- Dairy for Strength: Calcium and phosphate in dairy products like milk, cheese, and yogurt can help remineralize enamel and strengthen bones.
- Crunchy Fruits and Vegetables: Foods like apples, carrots, and celery act as natural tooth scrubbers, increasing saliva flow.
- Eating Fruit Without Damaging Teeth: Fruits, while healthy, can be acidic and contain natural sugars. To minimize damage:
- Eat with Meals: Eating fruit as part of a meal (rather than snacking throughout the day) exposes your teeth to acid for a shorter, concentrated period, allowing saliva more time to neutralize it afterward.
- Rinse with Water: After eating acidic fruits, rinse your mouth thoroughly with plain water to wash away residual acids and sugars.
- Wait to Brush: Avoid brushing immediately after eating acidic foods, as this can scrub the softened enamel. Wait at least 30 minutes to an hour.
- Choose Less Acidic Fruits: Opt for berries, melons, and bananas more often than citrus fruits (oranges, grapefruits) or grapes if you have concerns about acidity.
- Pair with Neutralizers: Eat acidic fruits with cheese or milk, which can help neutralize acids.
Regular Dental Check-ups
- Frequency: Visit your dentist at least twice a year for professional cleanings and examinations. More frequent visits may be recommended if you have gum disease, dry mouth, or other ongoing issues.
- What to Expect: These appointments include a thorough cleaning, an examination for cavities, gum disease assessment, and an oral cancer screening. Your dentist can also review your medications and discuss any oral health concerns related to them.
Managing Dry Mouth
Proactive management of dry mouth is critical for preventing widespread decay.
- Stay Hydrated: Sip water frequently throughout the day.
- Sugar-Free Stimulants: Chew sugar-free gum or suck on sugar-free lozenges to stimulate saliva flow.
- Saliva Substitutes: Use over-the-counter artificial saliva sprays, gels, or rinses.
- Humidifier: Use a humidifier in your bedroom at night.
- Medication Review: Discuss dry mouth with your physician. They may be able to adjust your medications or prescribe saliva-stimulating drugs.
Denture Care
If you wear dentures, proper care is essential.
- Clean Daily: Remove and brush dentures daily with a non-abrasive denture cleanser and a soft brush.
- Soak Overnight: Soak dentures overnight in a cleaning solution or plain water to keep them moist and prevent warping.
- Clean Your Mouth: Brush your gums, tongue, and roof of your mouth daily with a soft toothbrush before reinserting dentures.
- Regular Check-ups: Visit your dentist if dentures become ill-fitting, cause sores, or break. The ADA recommends regular denture checks.
Quitting Smoking and Limiting Alcohol
These habits are major risk factors for gum disease, tooth loss, and oral cancer. Quitting smoking is one of the single most impactful steps you can take for your oral and overall health.
Costs of Senior Dental Care and Insurance Considerations
Understanding the financial aspect of senior dental care in the US is crucial, as costs can vary significantly, and insurance coverage is often complex.
Average US Costs for Common Procedures
Prices fluctuate based on location (urban vs. rural), dentist's expertise, and materials used. The ranges below are approximate.
| Procedure | Average Low Cost (US$) | Average Mid Cost (US$) | Average High Cost (US$) |
|---|---|---|---|
| Routine Check-up & Cleaning | $75 | $150 | $300 |
| Composite Filling (1 surface) | $150 | $250 | $400 |
| Root Canal (Molar) | $1,000 | $1,500 | $2,000+ |
| Porcelain Crown | $800 | $1,300 | $2,500 |
| Dental Implant (per implant) | $3,000 | $4,500 | $6,000+ |
| Full Upper or Lower Denture | $1,000 | $2,000 | $3,000 |
| Scaling & Root Planing (per quadrant) | $200 | $350 | $500 |
| Tooth Extraction (simple) | $75 | $200 | $400 |
Insurance Coverage for Seniors
This is often the most confusing aspect of senior dental care.
- Original Medicare (Part A & B): Generally does NOT cover routine dental care, such as cleanings, fillings, dentures, or extractions. It might cover dental services if they are part of a covered medical procedure (e.g., a dental exam before a kidney transplant).
- Medicare Advantage Plans (Part C): These are private insurance plans approved by Medicare that offer an alternative to Original Medicare. Many Medicare Advantage plans include dental benefits, often covering routine care (cleanings, X-rays), and sometimes offering partial coverage for more extensive procedures like fillings, crowns, and dentures.
- Coverage Varies Widely: It's essential to research specific plans, as coverage limits (e.g., $1,000-$2,000 annual maximum), deductibles, co-pays, and provider networks can differ significantly.
- HMO vs. PPO: HMO plans usually require you to stay within a specific network, while PPO plans offer more flexibility but may have higher out-of-pocket costs for out-of-network providers.
- Private Dental Insurance for Seniors: Various private companies offer stand-alone dental insurance plans. These often have waiting periods for major procedures (e.g., 6-12 months for crowns), annual maximums ($1,000-$2,500), and varying coverage percentages (e.g., 100% for preventive, 80% for basic, 50% for major).
- Dental Discount Plans: Not insurance, but a membership program where you pay an annual fee and receive discounted rates (typically 10%-60%) on dental services from participating dentists. There are no deductibles, annual maximums, or waiting periods.
- Veterans Affairs (VA) Dental Benefits: For eligible veterans, the VA provides comprehensive dental care. Eligibility is usually tied to service-connected disabilities, POW status, or being enrolled in a VA vocational rehabilitation program.
Comparison of Senior Dental Coverage Options
| Feature | Original Medicare | Medicare Advantage | Private Dental Insurance | Dental Discount Plan |
|---|---|---|---|---|
| Routine Coverage | No | Often included | Yes | Discounted rates |
| Major Procedures | No | Limited coverage | Partial coverage | Discounted rates |
| Annual Max. | N/A | Typically $1K-$2K | Often $1K-$2.5K | N/A |
| Deductible | N/A | Common | Common | N/A |
| Waiting Periods | N/A | Less common | Common (major work) | No |
| Provider Network | Any Medicare provider | Specific networks | PPO/HMO | Participating dentists |
| Monthly Cost | N/A (Part B premium) | Varies, often $0 extra | $30-$70+ | $15-$30 |
Recovery and Aftercare: Ensuring Lasting Oral Health
Proper recovery and diligent aftercare are essential for the longevity of any dental treatment and for maintaining overall oral health.
General Post-Procedure Advice
- Pain Management: Follow your dentist's instructions for over-the-counter pain relievers (ibuprofen, acetaminophen) or prescription medication.
- Soft Diet: Stick to soft foods for the first few days (e.g., soups, yogurt, mashed potatoes) to avoid irritating the treated area. Gradually reintroduce harder foods as tolerated.
- Oral Hygiene: Continue to brush and floss gently, avoiding the surgical site if applicable. Your dentist may recommend a special mouth rinse.
- Avoid Smoking/Alcohol: These can impede healing and increase the risk of complications.
- Follow-up Appointments: Attend all scheduled follow-up visits to ensure proper healing and address any concerns.
Specific Aftercare
- After Extractions: Apply gentle pressure with gauze, avoid strenuous activity, don't use straws, and avoid spitting forcefully for 24-48 hours to prevent dry socket.
- After Root Canal: Avoid chewing on the treated tooth until it's permanently crowned to prevent fracture. Expect some sensitivity for a few days.
- After Dental Implants: Meticulous oral hygiene around the implant is critical, as is avoiding hard or sticky foods during the initial healing phase. Implants require the same care as natural teeth (brushing, flossing, regular check-ups).
- Denture Care: Continue daily cleaning and overnight soaking. Report any soreness or ill-fitting issues to your dentist promptly. Regular relines may be needed every few years, and dentures typically last 5-10 years before needing replacement.
Risks and Complications in Senior Dental Care
While dental treatments are generally safe and effective, certain risks and complications can arise, especially in older adults due to age-related factors or systemic health conditions.
- Infection: Any invasive procedure carries a risk of infection. Seniors with compromised immune systems or those taking immunosuppressants may be more susceptible.
- Delayed Healing: Age can sometimes slow down the body's natural healing processes, particularly after extractions or surgeries like implant placement.
- Medication Interactions: Certain medications (e.g., blood thinners, bisphosphonates for osteoporosis) can complicate dental procedures, such as increasing bleeding risk or affecting bone healing (e.g., osteonecrosis of the jaw). Always provide a complete medical history and list of medications to your dentist.
- Nerve Damage: Though rare, nerve damage can occur during procedures like extractions or implant placement, leading to temporary or permanent numbness or altered sensation.
- Failure of Restoration/Prosthesis: Fillings, crowns, or dentures can fail over time due to wear, recurrent decay, or changes in oral structures. Implants can fail to integrate with the bone.
- Systemic Complications: Untreated dental infections can spread, potentially leading to serious systemic health issues like endocarditis (heart infection), pneumonia (especially aspiration pneumonia in frail seniors), or worsening control of diabetes.
Your dentist will discuss potential risks specific to your health status and proposed treatments, ensuring you make informed decisions.
Cost Breakdown
Understanding the overall cost landscape for senior dental care and how to manage it effectively is a major concern for many.
Average US Costs (Low, Mid, High)
As seen in the table above, costs vary. A routine check-up and cleaning without insurance might cost $100-$300. A simple filling can be $150-$400. Major procedures like a dental implant can run $3,000-$6,000 per tooth (plus crown). A full set of conventional dentures (upper and lower) could cost anywhere from $2,000-$6,000.
With vs. Without Insurance
- With Insurance (Medicare Advantage or private): For covered services, you'll typically pay a co-pay or a percentage of the cost after meeting your deductible. For example, a cleaning might be fully covered or require a $20-$50 co-pay. A crown might be covered at 50%, meaning you pay $600-$1,250 of a $1,200-$2,500 procedure, up to your annual maximum. Once you hit the annual maximum (e.g., $1,500), you are responsible for 100% of further costs until the next plan year.
- Without Insurance: You pay the full, unsubsidized cost for all services. This can make extensive treatments prohibitive.
Payment Plans and Financing Options
- In-Office Payment Plans: Many dental offices offer their own payment plans, allowing you to pay for treatment in installments over several months, often without interest if paid on time.
- CareCredit and Similar Healthcare Credit Cards: These specialized credit cards offer promotional financing options, often with 0% interest for a set period (e.g., 6, 12, 18 months), if the balance is paid in full by the due date. Standard interest rates can be high after the promotional period.
- Personal Loans: Banks or credit unions may offer personal loans for larger dental expenses.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have access to these accounts (usually through employment or a spouse's employment), they allow you to set aside pre-tax money for qualified medical and dental expenses.
- Community Dental Clinics / Dental Schools: These institutions often provide high-quality care at significantly reduced costs, as treatment is performed by students under the close supervision of experienced faculty. Wait times might be longer.
- State and Local Programs: Some states or local health departments offer dental assistance programs for low-income seniors.
Cost-Saving Tips
- Prioritize Prevention: Regular cleanings and exams are the most cost-effective way to prevent expensive treatments down the line.
- Compare Plans: If considering Medicare Advantage or private insurance, meticulously compare plans for benefits, costs, and provider networks.
- Dental Discount Plans: Consider these as an alternative to insurance, especially if you anticipate moderate treatment and prefer no waiting periods.
- Ask for Cash Discounts: Many dentists offer a discount (e.g., 5-10%) for patients who pay in full at the time of service, especially if they don't have insurance.
- Get Multiple Opinions: For major procedures, getting a second or third opinion can help you compare treatment plans and costs.
Frequently Asked Questions
Is Medicare dental coverage enough for most seniors?
No, Original Medicare (Parts A & B) generally does not cover routine dental care such as cleanings, fillings, or dentures. While some Medicare Advantage (Part C) plans offer dental benefits, these often have annual maximums (typically $1,000-$2,000) and may not cover extensive or complex procedures fully, meaning most seniors will have out-of-pocket expenses.
How often should a senior see the dentist?
Most seniors should see the dentist at least twice a year for professional cleanings and examinations. However, if you have ongoing gum disease, chronic dry mouth, or other significant oral health concerns, your dentist may recommend more frequent visits, such as every three or four months.
What are the signs of gum disease in older adults?
Signs of gum disease in older adults include red, swollen, or tender gums; gums that bleed easily when brushing or flossing; persistent bad breath; receding gums that make teeth appear longer; pus between teeth and gums; changes in the way your teeth fit together; and loose or separating teeth.
Can I still get dental implants if I have bone loss?
It depends on the severity and location of the bone loss. While adequate bone density is crucial for implant success, advancements in dentistry offer solutions like bone grafting or sinus lifts that can rebuild lost bone, making implants a viable option for many seniors who initially might not have qualified. Your dentist or oral surgeon will assess your specific case.
How can I manage dry mouth effectively?
Managing dry mouth involves sipping water frequently, chewing sugar-free gum or sucking on sugar-free candies, using over-the-counter saliva substitutes (sprays, gels), running a humidifier at night, and avoiding caffeine and alcohol. Most importantly, discuss your medications with your doctor, as many prescription drugs cause dry mouth, and adjustments might be possible.
What's the best way to clean dentures?
Dentures should be cleaned daily by brushing them with a soft-bristled brush and a non-abrasive denture cleanser, not regular toothpaste which can be too abrasive. They should be soaked overnight in plain water or a denture cleaning solution to keep them moist and prevent bacterial growth. Remember to also brush your gums, tongue, and roof of your mouth daily.
Is root decay preventable, and what can I do about it?
Yes, root decay is largely preventable. Key strategies include meticulous oral hygiene (brushing with fluoride toothpaste, flossing), managing dry mouth, using fluoride rinses or prescription-strength fluoride toothpaste as recommended by your dentist, and adopting a diet low in sugars and acids. Regular dental check-ups are also crucial for early detection and treatment.
Are electric toothbrushes better for seniors, especially with dexterity issues?
Many dental professionals recommend electric toothbrushes for seniors, particularly those with arthritis, Parkinson's disease, or other conditions affecting dexterity. Electric toothbrushes do most of the work for you, have timers for proper brushing duration, and often come with larger, easier-to-grip handles, making them more effective at plaque removal.
How long do dentures typically last, and when should I replace them?
Conventional dentures typically last between 5 to 10 years. They may need replacement sooner if they become ill-fitting, cause chronic sores, break, or if your jawbone and gum ridges change significantly. Regular dental check-ups are important for assessing the fit and condition of your dentures.
Is it painful to get a root canal?
Modern root canal treatments are performed under local anesthesia, so the procedure itself is typically no more painful than getting a filling. Most patients report feeling pressure rather than pain. You might experience some sensitivity or mild discomfort for a few days after the procedure, which can usually be managed with over-the-counter pain relievers.
When to See a Dentist
Knowing when to seek dental care is critical for seniors, as some issues require immediate attention while others can be addressed during routine visits.
Emergency Situations (See a Dentist Immediately):
- Severe Toothache: Intense, throbbing pain that doesn't subside with over-the-counter pain medication.
- Swelling: Any sudden or significant swelling in your gums, face, or jaw, which could indicate a serious infection or abscess.
- Trauma: A broken, knocked-out, or severely cracked tooth resulting from an accident or fall.
- Uncontrolled Bleeding: Persistent bleeding from your gums or mouth after a procedure or injury that doesn't stop with pressure.
- Abscess: A painful, pus-filled lump on the gums, often accompanied by fever.
- Sudden Loosening of Multiple Teeth: This could indicate severe gum disease or trauma.
Red Flags for Scheduled Appointments (See a Dentist Soon):
- Persistent Dry Mouth: If over-the-counter remedies aren't helping, it's crucial to discuss this with your dentist and physician to prevent widespread decay.
- Chronic Bad Breath or Unpleasant Taste: Could indicate gum disease, infection, or poor hygiene.
- Loose or Shifting Teeth: A sign of advanced gum disease or bone loss.
- Changes in Denture Fit: If your dentures suddenly feel loose, click, or cause sores, they likely need adjustment or relining.
- Difficulty Chewing or Swallowing: Can indicate a range of issues from ill-fitting dentures to more serious oral conditions.
- Any Sore, Lump, or White/Red Patch in Your Mouth: Especially if it doesn't heal within two weeks. This requires an immediate evaluation for oral cancer screening.
- Increased Sensitivity: New or worsening sensitivity to hot, cold, or sweets, which could signal decay or exposed roots.
- Bleeding Gums: While common, persistent bleeding gums are often a sign of gingivitis or periodontitis and should not be ignored.
Routine Care Guidance:
- Regular Check-ups: Even without specific symptoms, regular dental check-ups every six months are essential for preventive care, professional cleaning, and early detection of potential problems.
- Medication Review: Inform your dentist about any new medications or changes to existing prescriptions, as they can impact your oral health.
Prioritizing your dental health is an investment in your overall well-being. By understanding the unique needs of senior dental care and proactively seeking professional guidance, you can maintain a healthy, functional, and confident smile throughout your golden years.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.