Abscessed Tooth: Complete Guide
Key Takeaways
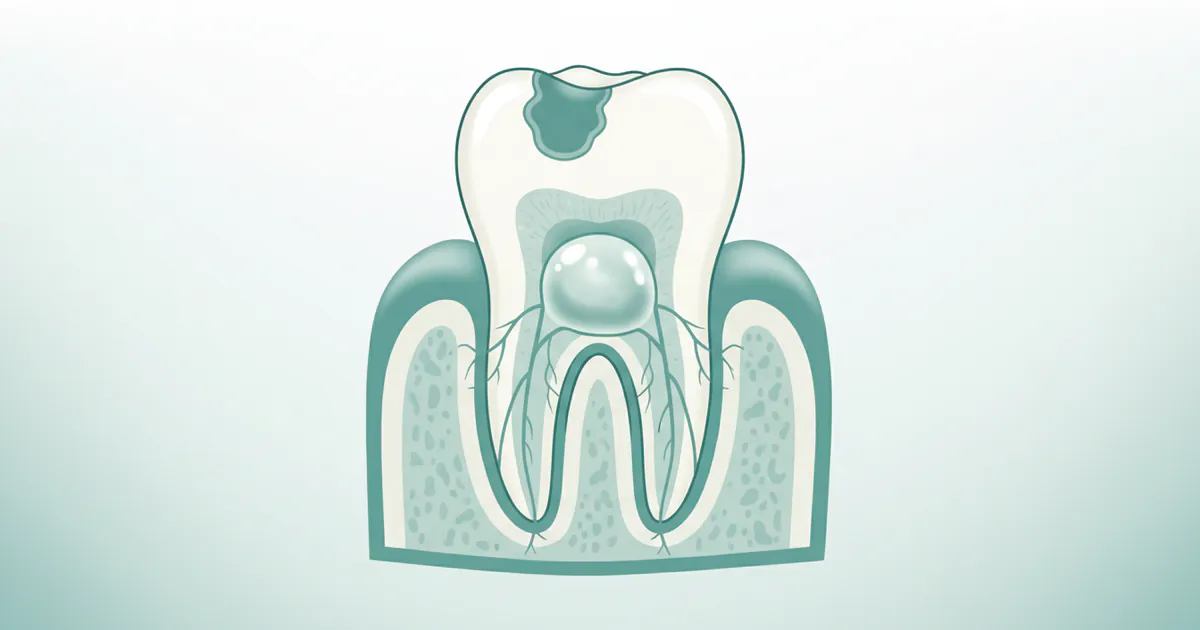
- An abscessed tooth is a painful bacterial infection that forms a pocket of pus in different parts of your tooth or gums. Left untreated, this common yet serious condition can lead to severe complications, including spread of infection to other parts of your body, potentially even becoming life-t
An abscessed tooth is a painful bacterial infection that forms a pocket of pus in different parts of your tooth or gums. Left untreated, this common yet serious condition can lead to severe complications, including spread of infection to other parts of your body, potentially even becoming life-threatening. Globally, dental abscesses are a significant public health concern, with millions experiencing the intense pain and potential dangers each year. In the United States, surveys suggest that up to 10-15% of adults have experienced a dental abscess at some point, highlighting its prevalence.
Understanding what an abscessed tooth is, why it occurs, and how it’s treated is crucial for preserving your oral health and overall well-being. This comprehensive guide from SmilePedia.net will equip you with all the essential information, from recognizing tooth infection symptoms to navigating treatment options, managing costs, and preventing future occurrences. We’ll delve into the various types of dental abscesses, the step-by-step treatment processes, and important considerations for recovery and aftercare. Your journey to understanding and overcoming an abscessed tooth starts here.
Key Takeaways:
- An abscessed tooth is a serious bacterial infection causing a pus pocket, typically due to untreated dental decay, trauma, or gum disease.
- Common tooth infection symptoms include severe, throbbing pain, sensitivity to hot/cold, facial swelling, fever, and a foul taste in the mouth.
- Immediate dental attention is critical; untreated abscesses can lead to life-threatening conditions like sepsis or Ludwig's Angina.
- Primary treatments involve root canal therapy (RCT) to save the tooth, or extraction if the tooth is beyond repair, often preceded by incision and drainage and antibiotics.
- Treatment costs in the US can range from $75 for a simple extraction to over $2,000 for complex root canal therapy, excluding crown costs. Insurance typically covers 50-80% of major procedures.
- Prevention hinges on excellent oral hygiene, regular dental check-ups (every 6 months), and a balanced diet.
What It Is / Overview
An abscessed tooth is essentially a localized collection of pus caused by a bacterial infection. This infection can develop in different areas around a tooth, leading to significant pain and potential health risks if not addressed promptly. The pus, a thick fluid composed of dead white blood cells, bacteria, and tissue debris, forms as your body's immune system tries to fight off the invading bacteria.
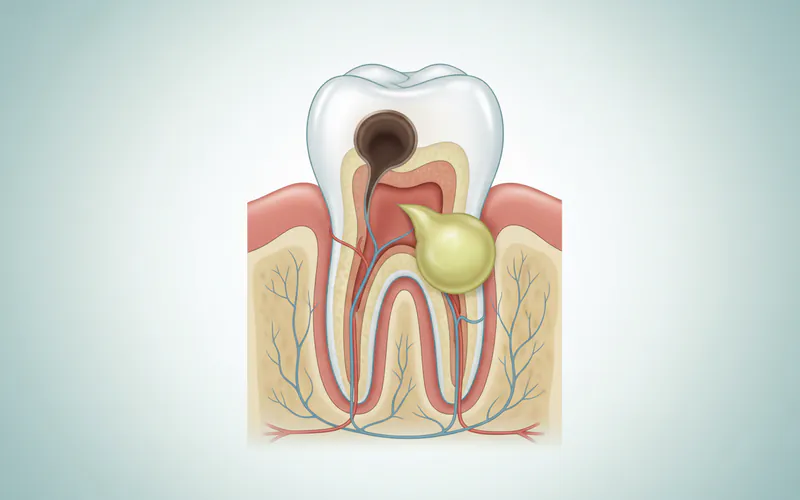
The root cause often stems from bacteria gaining entry to the sensitive inner structures of your tooth or the surrounding gum tissue. This can happen through various pathways, such as a deep cavity that penetrates the enamel and dentin to reach the dental pulp, a crack or chip in the tooth, or advanced gum disease. Once inside, the bacteria multiply rapidly, leading to inflammation and infection. As the infection progresses, the body attempts to contain it, resulting in the formation of an abscess.
It's vital to understand that a dental abscess is not just a localized annoyance; it's an active infection. If the infection remains untreated, it can spread beyond the tooth and surrounding bone, potentially entering the bloodstream or adjacent facial structures. The bone marrow, including the medullary cavity within the jawbone, is a potential pathway for infection dissemination, making prompt treatment essential to prevent severe systemic complications.
Types / Variations
Dental abscesses are primarily categorized by their location of origin. Understanding the different types helps in accurate diagnosis and targeted treatment.
Periapical Abscess (Root Abscess)
This is the most common type of dental abscess, forming at the tip of the tooth's root. It originates when bacteria invade the dental pulp – the innermost part of the tooth containing nerves, blood vessels, and connective tissue. This invasion typically occurs through:
- Deep, untreated dental decay: Cavities that extend through the enamel and dentin, eventually reaching the pulp.
- Dental trauma: A significant blow or injury to the tooth can damage the pulp, allowing bacteria to enter or causing pulp necrosis (death) which then becomes infected.
- Cracked or chipped teeth: These can create pathways for bacteria to penetrate the pulp.
- Failed root canal therapy: In some cases, a previously treated tooth may develop a new infection.
As the infection spreads from the pulp, it exits through the apical foramen (the opening at the root tip) and creates a pus pocket in the surrounding bone. This can be incredibly painful as the pressure builds.
Periodontal Abscess (Gum Abscess)
A periodontal abscess forms in the supporting structures around the tooth, specifically in the gum tissue and bone. Unlike a periapical abscess, the pulp of the tooth is usually healthy in this type of abscess. Periodontal abscesses are primarily caused by:
- Advanced periodontal disease (gum disease): Deep pockets form between the teeth and gums, where food debris and bacteria accumulate, leading to infection.
- Trauma to the gums: A foreign object, like a popcorn kernel or a toothbrush bristle, embedded in the gum tissue can trigger an infection.
- Impacted food: Food particles forced into the gum line can irritate and infect the tissue.
This type of abscess can cause significant swelling and redness of the gums, often accompanied by pain and pus discharge.
Gingival Abscess
A gingival abscess is the least common and typically the least severe type. It forms only in the gum tissue, usually on the surface, and does not involve the tooth or the periodontal ligament. It's often caused by:
- Trauma: A minor injury to the gum surface.
- Foreign body impaction: A small piece of food or a foreign object getting stuck in the gum.
Gingival abscesses are usually confined to the gum margin and tend to be less painful and resolve more easily than periapical or periodontal abscesses.
Causes / Why It Happens
Understanding the root causes of an abscessed tooth is key to prevention. The unifying factor across all types of dental abscesses is the invasion and proliferation of bacteria.
1. Untreated Dental Decay (Cavities)
This is the most frequent cause of periapical abscesses. When dental caries (cavities) are not treated, bacteria erode through the tooth's hard outer layers (enamel and dentin). Once they reach the soft, vital pulp chamber, they cause inflammation (pulpitis) and infection. The pulp tissue eventually dies (necrosis), and the infection spreads through the root canals to the bone at the tip of the root, forming an abscess.
2. Dental Trauma (Injury to the Tooth)
A blow to the tooth, a fall, or any significant impact can injure the dental pulp. Even if the tooth appears intact externally, the internal blood supply to the pulp can be severed, leading to pulp necrosis. Dead tissue is highly susceptible to bacterial infection, which can then lead to a periapical abscess weeks, months, or even years after the initial trauma. Cracks or chips in the tooth, especially those extending into the pulp, also serve as entry points for bacteria.
3. Advanced Gum Disease (Periodontitis)
Periodontal disease is a progressive infection of the gums and supporting bone around the teeth. In its advanced stages (periodontitis), deep pockets form between the teeth and gums. These pockets become reservoirs for bacteria, plaque, and calculus (hardened plaque) that are difficult to clean. This can lead to a localized infection within the gum tissue, forming a periodontal abscess.
4. Failed Root Canal Therapy
While root canal therapy is highly successful, sometimes an existing root canal can become reinfected. This can happen if:
- Incomplete cleaning: Some bacteria were left behind during the initial procedure.
- New decay: A new cavity forms around the treated tooth, allowing bacteria to leak into the filling or crown.
- Cracked crown or filling: This can compromise the seal, allowing bacteria to enter.
- Undetected canal: An accessory canal or complex root anatomy was missed during the initial treatment.
5. Foreign Objects
Occasionally, foreign bodies such as popcorn kernels, toothbrush bristles, or even fish bones can get lodged in the gum tissue, particularly in individuals with gum pockets, leading to irritation and subsequent infection, forming a gingival or periodontal abscess.
6. Compromised Immune System
Individuals with weakened immune systems due due to conditions like diabetes, autoimmune disorders, HIV/AIDS, or those undergoing chemotherapy, are more susceptible to infections, including dental abscesses, and may experience more severe symptoms and slower healing.
Signs and Symptoms
Recognizing the tooth infection symptoms of an abscess is crucial for seeking timely treatment. The symptoms can vary in intensity but typically involve discomfort and visible changes.
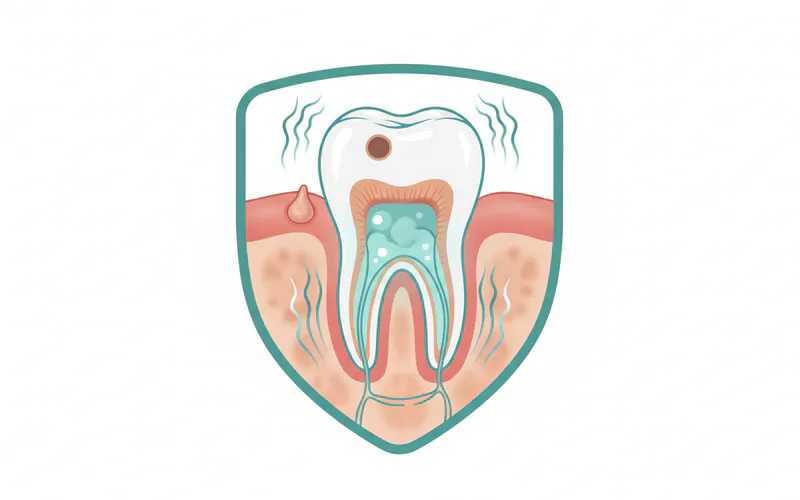
Primary Symptoms:
- Severe, persistent, throbbing toothache: This is often the most prominent symptom. The pain can radiate to your jawbone, neck, or ear and is frequently exacerbated by pressure or chewing. It can be so intense that it disrupts sleep.
- Sensitivity to hot and cold temperatures: Particularly prolonged sensitivity after exposure to hot or cold foods/drinks.
- Sensitivity to pressure: Pain when chewing or biting.
- Swelling in your face or cheek: This can range from mild puffiness to significant, noticeable swelling, often on one side of the face near the affected tooth.
- Tender, swollen lymph nodes: These may be felt under your jaw or in your neck, indicating your body is fighting the infection.
- Fever: A sign that the infection is spreading or the body is mounting a strong immune response.
- Bad breath and/or a foul taste in your mouth: This can be due to pus draining into your mouth.
- Pus discharge: Sometimes, a small, pimple-like bump (fistula or "gum boil") may appear on the gums near the infected tooth. If this ruptures, it can release pus, providing temporary relief from pain but not resolving the underlying infection.
Less Common or Later Symptoms:
- Difficulty opening your mouth (trismus): If the infection spreads to jaw muscles.
- Difficulty swallowing (dysphagia): If the infection spreads to throat tissues.
- General malaise: Feeling unwell, fatigued.
- Changes in skin color: Redness or discoloration of the skin over the affected area.
Pro Tip: If the pain suddenly subsides without any treatment, it may mean the abscess has ruptured. While this provides temporary relief, it does not mean the infection is gone. You still need immediate dental attention to drain the remaining infection and treat the source.
Treatment Options
Treating an abscessed tooth focuses on eliminating the infection, preserving the tooth if possible, and preventing complications. The specific treatment depends on the type, severity, and extent of the abscess.
1. Incision and Drainage (I&D)
- What it is: The dentist makes a small incision into the swollen area to allow the pus to drain. A rubber drain may be placed to keep the incision open and facilitate continued drainage.
- When it's used: Often the first step for acute, painful abscesses, especially those causing significant swelling, to relieve pressure and pain before definitive treatment. It does not treat the source of the infection.
- Pros: Provides immediate pain relief, reduces swelling, helps prevent further spread of infection.
- Cons: Does not cure the underlying problem; further treatment is always required.
- Cost: Typically ranges from $50 to $250, often covered by dental insurance.
2. Root Canal Therapy (Endodontic Treatment)
- What it is: This procedure aims to save the tooth by removing the infected pulp from within the tooth's root canals. The canals are then cleaned, shaped, disinfected, and filled with a rubber-like material (gutta-percha) to prevent reinfection. The tooth is usually capped with a crown afterwards to protect it.
- When it's used: The primary treatment for periapical abscesses when the tooth is restorable.
- Pros: Saves the natural tooth, preserves chewing function, avoids the need for a bridge or implant.
- Cons: Can be a multi-visit procedure; relatively higher cost than extraction; tooth may still require a crown, which is an additional cost.
- Cost: Varies significantly by tooth location and complexity.
- Front Tooth (Incisor/Canine): $700 - $1,100
- Premolar: $800 - $1,400
- Molar: $1,000 - $2,000+
- These costs do not include the crown, which can add another $800 - $1,800.
3. Tooth Extraction
- What it is: The complete removal of the infected tooth.
- When it's used: When the tooth is too severely damaged by decay, trauma, or infection to be saved with a root canal, or if root canal therapy is not a viable option due to cost or patient preference.
- Pros: Immediately removes the source of infection; often less expensive than root canal therapy initially.
- Cons: Loss of a natural tooth, which can lead to shifting of adjacent teeth, chewing difficulties, and bone loss over time. May require further procedures like bridges or dental implants to replace the missing tooth, adding to long-term costs.
- Cost:
- Simple Extraction: $75 - $300 (for teeth that are visible and easily removed)
- Surgical Extraction: $200 - $600+ (for impacted teeth or those requiring bone removal/sectioning)
4. Antibiotics
- What it is: Medications that kill or inhibit the growth of bacteria.
- When it's used: Antibiotics are typically prescribed if the infection has spread beyond the immediate abscess site (e.g., causing facial swelling, fever, or swollen lymph nodes) or if the patient is immunocompromised. They are also often used as an adjunct to drainage or definitive treatment to help control the infection.
- Pros: Helps control systemic spread of infection, reduces swelling.
- Cons: Do not eliminate the source of the infection (the pus pocket itself); should never be used as the sole treatment for an abscess. Overuse can lead to antibiotic resistance.
- Cost: Generic antibiotics are often covered by medical insurance and can range from $10 to $50 for a typical course.
Pro Tip: Always complete the full course of antibiotics, even if your symptoms improve quickly, to ensure the infection is fully controlled and to minimize the risk of antibiotic resistance.
Step-by-Step Process: What to Expect During Treatment
The journey through treating an abscessed tooth often involves several stages, particularly for root canal therapy. Here’s a general overview:
Initial Visit and Diagnosis:
- Patient History and Examination: The dentist will ask about your symptoms, medical history, and conduct a thorough oral examination.
- X-rays: One or more X-rays will be taken to visualize the tooth's roots, the surrounding bone, and the presence of any abscess or bone loss.
- Diagnosis: Based on the examination and X-rays, the dentist will diagnose the type and extent of the abscess and recommend the appropriate treatment plan. This may involve referral to an endodontist (root canal specialist) or an oral surgeon for complex cases.
Treatment for Acute Abscess with Swelling:
- Local Anesthesia: The area around the affected tooth is numbed with local anesthetic to ensure you are comfortable.
- Incision and Drainage (if needed): If there is significant swelling and a collection of pus, the dentist may perform an incision to drain the abscess. This provides immediate relief and allows the infection to clear. A small rubber drain might be placed.
- Antibiotic Prescription: If the infection has spread or there's significant swelling, a course of antibiotics will likely be prescribed to help control the bacterial infection.
Definitive Treatment (Root Canal Therapy):
- Isolation: A rubber dam is placed around the tooth to keep it dry and free from saliva during the procedure.
- Access Opening: A small opening is made through the crown of the tooth to access the pulp chamber and root canals.
- Pulp Removal: The infected or necrotic (dead) pulp tissue is carefully removed from the pulp chamber and the root canals using specialized instruments called files.
- Cleaning and Shaping: The root canals are thoroughly cleaned, disinfected, and shaped to prepare them for filling. This step is crucial to remove all bacteria and debris.
- Filling the Canals: The cleaned and shaped canals are filled with a biocompatible material, usually gutta-percha, often sealed with an adhesive cement. This prevents bacteria from re-entering.
- Temporary Filling: A temporary filling is placed in the access opening to protect the tooth until the permanent restoration (usually a crown) is placed.
- Permanent Restoration (Crown): In a subsequent appointment (typically 1-2 weeks later), the temporary filling is removed, and a custom-made crown is placed over the treated tooth. This strengthens the tooth and restores its appearance and function.
- ``
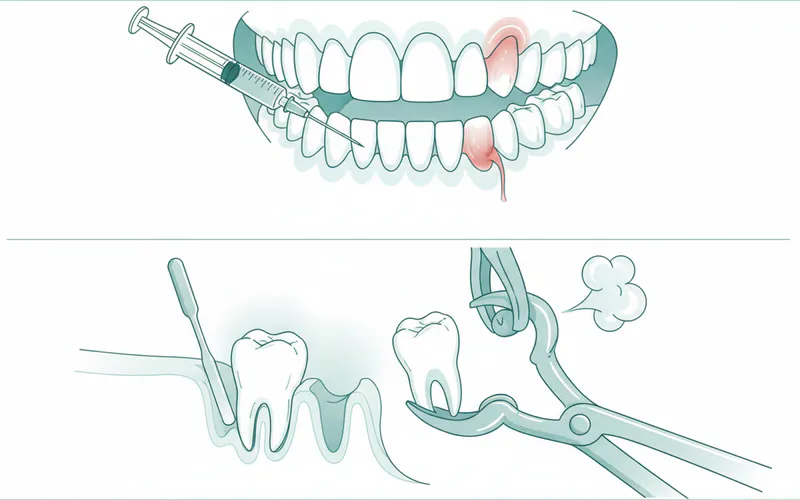
Definitive Treatment (Tooth Extraction):
- Local Anesthesia: The area around the tooth is numbed.
- Tooth Removal: The tooth is gently loosened and removed using forceps and elevators. For surgical extractions, a small incision in the gum or removal of bone may be necessary.
- Socket Care: The socket is cleaned, and gauze is placed to control bleeding. Instructions for aftercare, including managing pain and promoting healing, are provided.
- Discussion of Replacement Options: The dentist will discuss options for replacing the missing tooth, such as a dental implant, bridge, or partial denture, to prevent future complications like shifting teeth or bone loss.
Cost and Insurance
The cost of treating an abscessed tooth in the US can vary widely based on the type of treatment, the tooth's location and complexity, the dentist's or specialist's fees, and geographic location.
Average US Cost Ranges:
| Procedure | Front Tooth (Incisor/Canine) | Premolar | Molar (Back Tooth) | Notes |
|---|---|---|---|---|
| Incision & Drainage | $50 - $250 | $50 - $250 | $50 - $250 | Often a preliminary step, included in larger treatment fees by some dentists. |
| Simple Extraction | $75 - $250 | $100 - $300 | $150 - $350 | For visible, easily removed teeth. |
| Surgical Extraction | $200 - $400 | $250 - $500 | $300 - $600+ | For impacted, fractured, or difficult-to-remove teeth. |
| Root Canal Therapy | $700 - $1,100 | $800 - $1,400 | $1,000 - $2,000+ | Periapical abscesses; does not include crown cost. |
| Crown (Post-Root Canal) | $800 - $1,500 | $900 - $1,600 | $1,000 - $1,800 | Essential for protecting a root-canal-treated tooth. |
| Antibiotics | $10 - $50 | $10 - $50 | $10 - $50 | Often covered by medical insurance plans. |
Regional Cost Variations:
- Metropolitan Areas (e.g., NYC, LA, Chicago): Generally higher costs, potentially 10-30% above national averages.
- Rural Areas/Smaller Towns: Typically lower costs, potentially 10-20% below national averages.
Insurance Coverage Details:
Most dental insurance plans in the US categorize procedures into preventive, basic, and major:
- Preventive (e.g., exams, X-rays, cleanings): Often covered at 80-100%. Initial diagnostic costs fall here.
- Basic (e.g., fillings, simple extractions): Typically covered at 70-80%. Simple extractions may fall into this category.
- Major (e.g., root canals, crowns, surgical extractions): Usually covered at 50%. This is where root canal therapy and crowns typically fall.
Important Considerations:
- Deductibles: You'll likely need to pay a certain amount out-of-pocket before your insurance coverage kicks in (e.g., $50-$150 annually).
- Annual Maximums: Most dental plans have an annual limit on what they will pay (e.g., $1,000 - $2,500 per year). If your treatment costs exceed this, you'll pay the remainder.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) before covering major procedures. This means if you buy a new plan, you might not be covered for a root canal for a year.
- PPO vs. HMO:
- PPO (Preferred Provider Organization): Offers more flexibility in choosing dentists, but out-of-network costs are higher.
- HMO (Health Maintenance Organization): Requires you to choose a dentist from a specific network, often with lower out-of-pocket costs but less choice.
- Medical Insurance for Dental: While rare, some severe dental infections (like those leading to hospitalizations for sepsis or deep space infections) might have portions of their treatment covered by medical insurance, especially if performed in a hospital setting.
Cost-Saving Tips:
- Early Intervention: Addressing decay early with a filling costs significantly less than waiting until a root canal or extraction is necessary.
- Preventive Care: Regular check-ups and cleanings prevent most serious issues.
- Dental Schools: University dental schools often offer discounted services performed by supervised students.
- Payment Plans/Financing: Many dental offices offer in-house payment plans or work with third-party financing like CareCredit.
- Community Clinics: Federally Qualified Health Centers (FQHCs) and other community dental clinics often provide services on a sliding scale based on income.
Recovery and Aftercare
Proper recovery and aftercare are crucial for successful healing and preventing complications following treatment for an abscessed tooth.
Post-Root Canal Therapy:
- Pain Management: Mild to moderate pain and sensitivity are common for a few days. Over-the-counter pain relievers like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are usually sufficient. Your dentist may prescribe stronger medication if needed.
- Diet: Stick to soft foods for the first few days. Avoid chewing on the treated tooth until the permanent crown is placed to prevent fracture.
- Oral Hygiene: Continue regular brushing and flossing, but be gentle around the treated area.
- Temporary Filling Care: Be careful with the temporary filling; it's not as strong as a permanent one. If it comes out, contact your dentist immediately.
- Crown Placement: Return for your follow-up appointment to have the permanent crown placed. This is a critical step to protect the tooth from fracture and reinfection.
- Avoid Smoking: Smoking can significantly impair healing and increase the risk of complications.
Post-Tooth Extraction:
- Bleeding Control: Bite down firmly on the gauze pad for 30-60 minutes after the extraction. Replace it if it becomes saturated. Slight oozing is normal for up to 24 hours.
- Pain Management: Over-the-counter pain relievers are usually sufficient, but your dentist may prescribe stronger medication.
- Swelling Reduction: Apply an ice pack to the outside of your cheek for 15-20 minutes on, 15-20 minutes off, during the first 24 hours to minimize swelling.
- Diet: Consume soft, cool foods and liquids for the first 24-48 hours. Avoid hot liquids, alcohol, and using straws (the sucking motion can dislodge the blood clot, leading to a painful dry socket).
- Oral Hygiene: Do not rinse vigorously or brush directly on the extraction site for 24 hours. After 24 hours, you can gently rinse with warm salt water (1/2 teaspoon salt in 8 ounces warm water) several times a day.
- Rest: Avoid strenuous activity for 24-48 hours.
- Avoid Smoking: Extremely important to avoid smoking as it significantly increases the risk of dry socket and impairs healing.
- Follow-up: Attend any scheduled follow-up appointments to ensure proper healing.
General Aftercare for Any Abscess Treatment:
- Antibiotics: If prescribed, complete the entire course of antibiotics, even if symptoms improve.
- Monitor Symptoms: Watch for signs of worsening infection, such as increased swelling, severe pain, fever, or difficulty swallowing/breathing. Contact your dentist immediately if these occur.
- Hydration: Drink plenty of water.
- ADA Guidelines: The American Dental Association (ADA) emphasizes consistent oral hygiene and regular dental visits as critical for long-term success after any dental procedure.
Prevention
Preventing an abscessed tooth is largely about maintaining excellent oral hygiene and proactive dental care.
1. Maintain Excellent Oral Hygiene:
- Brush Twice Daily: Brush your teeth for at least two minutes, twice a day, using a fluoride toothpaste. The ADA recommends soft-bristled brushes.
- Floss Daily: Floss at least once a day to remove food particles and plaque from between your teeth and under the gum line, areas your toothbrush can't reach.
- Use Mouthwash: An antiseptic mouthwash can help reduce bacteria in your mouth, but it's not a substitute for brushing and flossing.
2. Regular Dental Check-ups and Cleanings:
- Every Six Months: Visit your dentist for routine check-ups and professional cleanings at least twice a year. These appointments allow your dentist to identify and treat decay or gum disease early, before they progress to an abscess.
- X-rays: Regular X-rays help detect hidden decay or early signs of infection that aren't visible during a visual exam.
3. Healthy Diet:
- Limit Sugary Foods and Drinks: Sugar feeds the bacteria that cause tooth decay. Reduce your intake of soda, candy, pastries, and other sugary snacks.
- Eat Nutrient-Rich Foods: A balanced diet rich in fruits, vegetables, and whole grains supports overall oral health.
4. Protect Your Teeth:
- Wear a Mouthguard: If you play contact sports, wear a custom-fitted mouthguard to protect your teeth from trauma that could lead to pulp damage and subsequent abscess.
- Avoid Biting Hard Objects: Don't chew on ice, hard candies, or use your teeth to open packages, as this can cause cracks or chips.

5. Address Dental Problems Promptly:
- Don't Ignore Pain: Any persistent toothache or sensitivity is a sign that something is wrong. Don't delay seeing a dentist. Early intervention for cavities, gum inflammation, or cracked teeth can prevent an abscess from forming.
- Complete Treatment: If you start treatment for a dental issue (e.g., a filling), ensure you complete all recommended appointments.
Risks and Complications
While an abscessed tooth primarily affects your oral cavity, if left untreated, the infection can spread, leading to severe and potentially life-threatening complications.
Localized Complications:
- Tooth Loss: If the infection is too severe, or if a root canal fails, the tooth may need to be extracted.
- Spread of Infection to Adjacent Teeth/Bone: The infection can spread to neighboring teeth, causing them to abscess, or to the surrounding jawbone, leading to osteomyelitis (bone infection).
- Jaw Cyst Formation: A persistent periapical abscess can develop into a dental cyst (radicular cyst), which is a fluid-filled sac at the root tip. These cysts grow slowly and can destroy significant amounts of jawbone.
- Sinus Involvement: An abscess in an upper back tooth can perforate into the maxillary sinus, leading to sinusitis (sinus infection).
Systemic Complications (Spread Beyond the Oral Cavity):
- Cellulitis: This is a rapidly spreading bacterial infection of the skin and underlying tissues, causing widespread facial swelling, redness, and warmth. This can quickly become dangerous if it obstructs airways.
- Osteomyelitis: The infection can spread to the jawbone (maxilla or mandible), causing inflammation and destruction of bone tissue, including the medullary cavity. This requires aggressive antibiotic therapy and possibly surgical debridement.
- Ludwig's Angina: A severe and potentially fatal form of cellulitis that affects the floor of the mouth and neck. It can cause rapid and significant swelling that obstructs the airway, leading to difficulty breathing and swallowing. This is a medical emergency requiring immediate hospitalization and often surgical intervention.
- Cavernous Sinus Thrombosis: A rare but extremely serious complication where the infection spreads to the cavernous sinus, a large vein located at the base of the brain. This can lead to blood clot formation, vision loss, paralysis of eye muscles, brain abscess, stroke, and even death.
- Sepsis: The most critical complication, where bacteria from the dental abscess enter the bloodstream and spread throughout the body, triggering a widespread inflammatory response. Sepsis can lead to organ damage, septic shock, and death if not treated urgently in a hospital setting. Symptoms include high fever, chills, rapid heart rate, confusion, and difficulty breathing.
- ``
Comparison of Abscess Types and Characteristics:
| Feature | Periapical Abscess | Periodontal Abscess | Gingival Abscess |
|---|---|---|---|
| Location | At the tip of the tooth root, inside the bone. | In the gum tissue and supporting bone beside the tooth root. | In the gum tissue only, usually at the gum margin. |
| Primary Cause | Untreated decay, trauma, cracked tooth, failed root canal. | Advanced gum disease, foreign body impaction. | Trauma to gums, superficial foreign body. |
| Tooth Pulp Status | Infected/necrotic (dead). | Usually vital (healthy). | Usually vital (healthy). |
| Pain Character | Severe, throbbing, constant; sensitive to hot/cold/pressure. | Localized, throbbing, sensitive to pressure; gum tenderness. | Localized gum pain, sometimes mild swelling. |
| Associated Swelling | Facial swelling, swelling around root. | Swelling of the gum tissue, sometimes facial. | Localized swelling on gum. |
| Primary Treatment | Root canal therapy or extraction. | Drainage, scaling/root planing, antibiotics if spread. | Drainage, removal of foreign body, good oral hygiene. |
| Urgency | High (can lead to serious systemic issues). | High (can lead to tooth loss if untreated). | Moderate (usually resolves with simple care). |
Children / Pediatric Considerations
Dental abscesses in children are just as serious as in adults and require immediate attention. While primary teeth (baby teeth) are eventually replaced, their health is critical for proper development of permanent teeth, chewing, speech, and maintaining space in the arch.
Common Causes in Children:
- Early Childhood Caries (ECC) / Nursing Bottle Decay: Extensive decay, often affecting multiple front teeth, caused by prolonged exposure to sugary liquids (e.g., milk, juice in bottles, especially at night).
- Dental Trauma: Children are prone to falls and accidents, which can lead to fractured or knocked-out teeth, or internal damage to the pulp that may abscess later.
- Poor Oral Hygiene: Inconsistent brushing and flossing can lead to cavities and gum inflammation.
Signs and Symptoms in Children:
Children may not always articulate their pain clearly. Parents should look for:
- Irritability and restlessness.
- Difficulty eating, especially hard or cold foods.
- Refusal to eat.
- Facial swelling, often noticeable around the jaw or eye.
- Fever.
- Red, swollen gums or a "pimple" on the gums near a tooth.
- Persistent bad breath.
- Swollen lymph nodes in the neck.
Treatment Options for Children:
- Pulpotomy or Pulpectomy: Similar to a root canal for adults, but often for primary teeth. A pulpotomy involves removing only the infected pulp from the crown portion of the tooth, while a pulpectomy removes pulp from the entire root canal. The tooth is then typically covered with a stainless steel crown.
- Extraction: If the tooth is too severely damaged or the infection is too extensive, extraction may be necessary. For primary teeth, space maintainers might be placed after extraction to ensure proper eruption of the permanent tooth.
- Incision and Drainage / Antibiotics: Used in similar situations as adults to control acute infection.
Importance of Primary Teeth:
- Space Maintenance: Primary teeth hold space for permanent teeth. Premature loss can lead to crowding or misalignment of permanent teeth.
- Chewing and Nutrition: Healthy primary teeth are essential for proper chewing and digestion.
- Speech Development: They play a role in clear speech.
- Self-Esteem: A healthy smile contributes to a child's confidence.
Pro Tip for Parents: Never ignore a child's toothache or facial swelling. Even if it's a baby tooth, an abscess can cause significant pain, affect the developing permanent tooth underneath, and spread infection throughout the body.
Cost Breakdown (Summary)
While detailed costs were provided in the main section, here's a summary of average US costs for an abscessed tooth treatment, with and without insurance, along with payment options.
| Procedure (Typical Range) | Average Cost (Without Insurance) | Average Cost (With Insurance, 50-80% Coverage) |
|---|---|---|
| Initial Exam & X-rays | $100 - $300 | $0 - $60 (often 80-100% covered) |
| Incision & Drainage (I&D) | $50 - $250 | $25 - $125 (if separate procedure) |
| Antibiotics (Prescription) | $10 - $50 | $0 - $20 (often covered by medical insurance) |
| Root Canal (Molar) | $1,000 - $2,000+ | $500 - $1,000+ |
| Crown (Post-Root Canal) | $1,000 - $1,800 | $500 - $900 |
| Simple Extraction | $75 - $350 | $15 - $105 (70-80% coverage) |
| Surgical Extraction | $300 - $600+ | $150 - $300+ |
| Total for Root Canal + Crown | $2,000 - $3,800+ | $1,000 - $1,900+ |
| Total for Extraction | $75 - $600+ | $15 - $300+ |
Note: These are estimates. Your actual costs may vary based on your specific case, dentist, location, and insurance plan details (deductibles, annual maximums, waiting periods).
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental practices offer flexible payment schedules, allowing you to pay for treatment in installments.
- CareCredit / LendingClub: These are popular third-party healthcare financing options that offer credit cards specifically for medical and dental expenses. They often have deferred interest plans for a certain period if you pay the balance in full.
- Health Savings Accounts (HSAs) / Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these tax-advantaged accounts to pay for dental treatment.
- Dental Schools: As mentioned, dental schools can offer quality care at reduced prices.
- Community Health Centers: These clinics often provide care on a sliding scale based on income.
Frequently Asked Questions
What happens if an abscessed tooth is left untreated?
If an abscessed tooth is left untreated, the infection will not resolve on its own and will likely spread. It can lead to severe complications such as extensive bone loss, tooth loss, the formation of a cyst, or dangerous systemic infections like cellulitis, Ludwig's Angina, or potentially life-threatening sepsis.
Is an abscessed tooth an emergency?
Yes, an abscessed tooth, especially one causing significant pain, facial swelling, fever, or difficulty swallowing/breathing, is considered a dental emergency. It requires immediate attention from a dentist or, in severe cases, an emergency room, to prevent the spread of infection and serious complications.
Can antibiotics alone cure an abscessed tooth?
No, antibiotics alone cannot cure an abscessed tooth. While they can help control the spread of bacterial infection and reduce swelling, they do not remove the source of the infection (the pus pocket and necrotic tissue). Definitive treatment like root canal therapy or extraction is always required to eliminate the problem.
How much pain can I expect from an abscessed tooth?
An abscessed tooth typically causes severe, throbbing, and persistent pain. This pain can radiate to your jaw, ear, or neck and is often exacerbated by hot, cold, or pressure. The intensity can be debilitating and interfere with daily activities and sleep.
What is the typical recovery time after treating an abscessed tooth?
Recovery time varies. For a root canal, initial pain subsides in a few days, but the tooth needs a crown in 1-2 weeks. After an extraction, soft tissue healing takes about 7-10 days, with bone healing taking several months. Following aftercare instructions is crucial for a smooth recovery.
Are there any home remedies for an abscessed tooth?
While some home remedies like warm salt water rinses or cold compresses can offer temporary symptomatic relief, they cannot cure an abscessed tooth. They do not address the underlying bacterial infection and should never delay seeking professional dental care, which is essential.
How long can an abscessed tooth last without treatment?
An abscessed tooth can persist indefinitely without treatment, slowly worsening over weeks, months, or even years. The pain may fluctuate or temporarily subside if the pus drains, but the infection remains active and continues to cause damage and pose a risk of spreading.
What are the alternatives to root canal therapy for an abscessed tooth?
The primary alternative to root canal therapy for an abscessed tooth is tooth extraction. While extraction removes the infected tooth entirely, it also leads to tooth loss, which can necessitate further restorative procedures like dental implants or bridges to maintain oral function and aesthetics.
Can an abscessed tooth affect my overall health?
Absolutely. The bacteria from an abscessed tooth can enter your bloodstream and spread throughout your body. This can exacerbate existing conditions like diabetes or heart disease, and in severe cases, lead to life-threatening systemic infections such as sepsis, Ludwig's Angina, or cavernous sinus thrombosis.
Will my dental insurance cover the cost of treating an abscessed tooth?
Most dental insurance plans cover a portion of the cost of treating an abscessed tooth, typically classifying root canal therapy, crowns, and surgical extractions as "major procedures" and covering around 50%. Simple extractions may fall under "basic procedures" with 70-80% coverage. However, deductibles, annual maximums, and waiting periods apply.
When to See a Dentist
Recognizing the urgency of an abscessed tooth is paramount for your health. Do not delay seeking professional dental care if you experience any of the following:
Immediate Dental Attention (Emergency):
- Severe, persistent, throbbing toothache: Especially if it doesn't respond to over-the-counter pain relievers.
- Facial swelling: Swelling of your cheek, jaw, or around your eye that is increasing rapidly. This is a critical sign of infection spread.
- Fever and chills: These indicate a systemic infection.
- Difficulty breathing or swallowing: This is a life-threatening symptom indicating the infection is severely obstructing your airway or throat. Go to an emergency room immediately.
- Redness and warmth on the skin: Over the area of swelling, suggesting cellulitis.
- Rapidly worsening symptoms: Any sudden and significant escalation of pain, swelling, or general malaise.
Prompt Dental Appointment (Within 24-48 hours):
- Pimple-like bump on your gums (fistula): Even if it's painless, this indicates an underlying chronic infection that needs treatment.
- Persistent sensitivity to hot or cold: Especially if it lingers after the stimulus is removed.
- Pain when chewing or biting: Suggesting pressure on an infected tooth.
- A foul taste in your mouth: Potentially from draining pus.
Red Flags vs. Routine Care: Any pain, swelling, or unusual discharge in your mouth is a red flag and warrants a dental visit. Do not dismiss these symptoms as minor. Routine care focuses on prevention and early intervention (like fillings for small cavities). An abscess requires immediate, often emergency, intervention.
Pro Tip: If you cannot reach your regular dentist for an emergency, seek care at an urgent dental clinic or an emergency room. Do not attempt to self-treat a dental abscess.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Is an Abscess
Imagine a throbbing pain deep within your jaw, a persistent ache that keeps you awake at night and makes even the softest foods unbearable. This isn't just a bad toothache; it could be a sign of something much more serious: a dental abscess. Affecting millions of Americans annually, an abscess is an
February 22, 2026
Cracked Tooth Syndrome: Complete Guide
Cracked Tooth Syndrome: Complete Guide Category: Dental Conditions & Diseases
February 22, 2026
Dentinogenesis Imperfecta: Complete Guide
Imagine a world where your teeth, fundamental to chewing, speaking, and even smiling confidently, are inherently fragile, discolored, and prone to rapid wear from the moment they emerge. For individuals affected by dentinogenesis imperfecta (DI), this is a reality. While relatively rare, affecti
February 22, 2026
Stage 1 Early Cavity: Complete Guide
Did you know that dental cavities are one of the most common chronic diseases globally, affecting both children and adults? In the United States, over 90% of adults have had a cavity, and a significant portion of these begin as a stage 1 early cavity. Often invisible and painless in its nasc
February 22, 2026