How to Remove Tooth Decay Yourself
Key Takeaways
- Imagine a tiny, invisible enemy slowly eroding the very foundation of your smile. This unseen adversary, tooth decay, affects a staggering number of Americans. According to the Centers for Disease Control and Prevention (CDC), 26% of adults aged 20 to 64 have untreated tooth decay, a statistic t
How to Remove Tooth Decay Yourself: Understanding Cavities and Why Professional Care is Essential
Imagine a tiny, invisible enemy slowly eroding the very foundation of your smile. This unseen adversary, tooth decay, affects a staggering number of Americans. According to the Centers for Disease Control and Prevention (CDC), 26% of adults aged 20 to 64 have untreated tooth decay, a statistic that underscores its widespread prevalence and the silent threat it poses. While the idea of tackling this problem yourself might seem appealing, perhaps out of concern for cost or discomfort, the reality is that you cannot safely or effectively remove tooth decay yourself. Attempting to do so risks severe pain, infection, and irreversible damage to your oral health.
This comprehensive guide from SmilePedia.net will delve deep into what tooth decay is, why it occurs, and why professional dental intervention is not just recommended but absolutely critical for its treatment. We'll explore the dangers of self-treatment, equip you with knowledge about effective professional solutions, discuss costs and prevention strategies, and address common questions about managing this pervasive dental issue. By the end, you'll understand why empowering yourself with knowledge and seeking timely professional care is the only true path to addressing tooth decay and protecting your smile.
Key Takeaways:
- Self-removal of tooth decay is impossible and dangerous. Tooth decay is structural damage requiring professional tools and expertise.
- Untreated decay can lead to severe pain, infection (including abscesses affecting the sinus cavity), and tooth loss.
- Professional treatments range from fluoride applications (for early demineralization) to fillings, crowns, root canals, or extractions for established cavities.
- Costs for professional treatment vary widely: A simple filling can range from $50 to $250 (amalgam) or $90 to $450 (composite), while a root canal plus crown can cost $1,500 to $4,000+. Insurance significantly impacts out-of-pocket expenses.
- Prevention is your most powerful tool. Excellent oral hygiene (brushing twice daily with fluoride toothpaste, flossing daily), a balanced diet, and regular dental check-ups (typically every 6 months) are crucial.
- Temporarily managing toothache with over-the-counter pain relievers or cold compresses can provide relief, but is not a substitute for professional dental care.
- Early detection through regular dental visits can save you pain, extensive treatment, and money in the long run.
Understanding Tooth Decay: Why Self-Removal Isn't an Option
Tooth decay, medically known as dental caries or a cavity, is a destructive process that damages the hard outer layers of your teeth. It's not a superficial problem that can be scraped off or scrubbed away. It's a progressive bacterial infection that creates actual holes in your tooth structure.
What is Tooth Decay?
Tooth decay begins when bacteria in your mouth, particularly Streptococcus mutans, feed on the sugars and starches from the foods and drinks you consume. These bacteria produce acids that erode the tooth's outermost layer, the enamel. This process is called demineralization. Initially, this might appear as a white spot, indicating a loss of minerals. With consistent acid attacks, this demineralization progresses, eventually breaking through the enamel and creating a tiny hole – a cavity.
Once the cavity breaches the enamel, it quickly penetrates the softer, more porous layer beneath, called the dentin. Dentin contains microscopic tubules that lead directly to the tooth's nerve center, the pulp. When decay reaches the dentin, the progression accelerates, and you're more likely to experience sensitivity and pain.
The Progression of Decay
Tooth decay follows a predictable path if left untreated:
- Enamel Decay (Early Stage): The acids create a soft spot or white lesion on the enamel. At this stage, it might be possible to reverse the process with professional fluoride treatments and improved oral hygiene, as the tooth can reabsorb minerals (remineralization).
- Dentin Decay (Moderate Stage): Once the decay penetrates the enamel, it quickly spreads through the softer dentin. This is when sensitivity to hot, cold, or sweet foods typically begins. A visible cavity, appearing as a pit or dark spot, often becomes apparent.
- Pulp Involvement (Advanced Stage): If decay reaches the pulp, the innermost part of the tooth containing nerves and blood vessels, it can cause severe pain, inflammation, and infection. This often leads to a dental abscess, a pocket of pus that forms at the root tip or in the surrounding bone. At this stage, a root canal or tooth extraction is usually necessary.
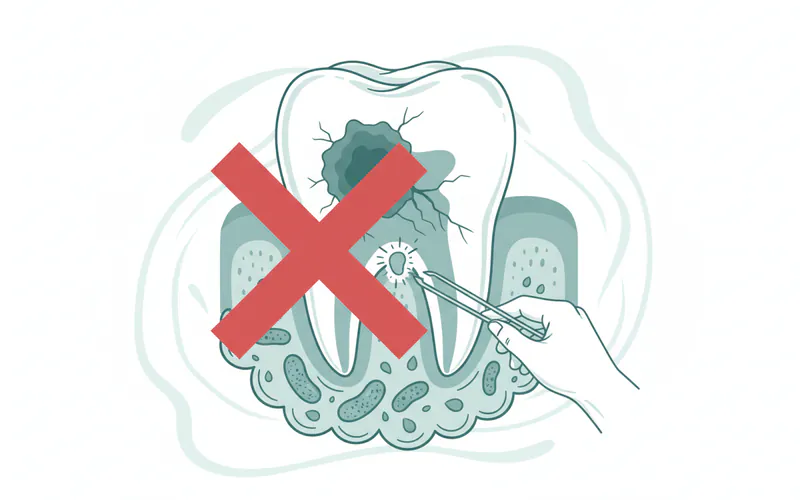
Why DIY Methods Fail and Are Dangerous
The concept of "removing tooth decay yourself" is fundamentally flawed because true decay is a structural defect in the tooth, not merely surface-level debris.
- Invisible Extent: Much of the decay often lies hidden from plain view, especially between teeth or under existing fillings. Dentists use specialized instruments, bright lights, dental mirrors, and X-rays to accurately diagnose the extent and location of decay. You simply cannot see or access these areas effectively.
- Inability to Sterilize: A dental office maintains a sterile environment to prevent infection. Any attempt to scrape, pick, or drill at a cavity at home would introduce countless bacteria into an already compromised tooth, leading to severe infection.
- Lack of Precision and Tools: Removing decay requires precise tools like dental drills that can selectively remove only the infected, softened tooth structure without damaging healthy tissue. Over-the-counter tools, if they even exist, are not designed for this delicate work and would likely cause more harm than good, chipping or cracking the tooth, or exposing the sensitive pulp.
- Irreversible Damage: Once a cavity forms, the lost tooth structure cannot regrow or repair itself naturally. It requires a dental material (like a filling or crown) to restore the tooth's integrity and function. Self-treatment would only exacerbate the problem, leading to larger cavities, nerve damage, and potentially tooth loss.
- Risk of Infection and Systemic Issues: Disturbing a cavity without proper sterilization and sealing can introduce bacteria into the tooth's pulp and bloodstream. This can lead to a painful abscess, facial swelling (cellulitis), and even life-threatening systemic infections like sepsis.
Pro Tip: If you notice a cavity or experience tooth pain, resist the urge to self-diagnose or self-treat. The best course of action is to schedule an appointment with your dentist as soon as possible.
The Real Causes of Tooth Decay
Understanding the root causes of tooth decay is the first step toward effective prevention. It's a multifactorial disease influenced by diet, oral hygiene, and individual susceptibility.
Bacterial Action
The primary culprits are specific types of bacteria in your mouth, particularly Streptococcus mutans and Lactobacillus. These bacteria form a sticky, colorless film on your teeth called plaque. When you consume sugary or starchy foods and drinks, these bacteria metabolize the carbohydrates, producing acids as a byproduct. These acids are what attack and demineralize your tooth enamel.
Dietary Factors
What you eat and drink plays a critical role:
- Sugary and Starchy Foods: Candies, cookies, sodas, fruit juices, refined carbohydrates (bread, pasta, chips) all provide fuel for cavity-causing bacteria.
- Frequency of Consumption: Grazing on snacks and sipping sugary drinks throughout the day exposes your teeth to acid attacks more frequently, giving your enamel less time to recover.
- Acidic Foods and Drinks: While not directly providing sugar for bacteria, acidic foods like citrus fruits and sodas can directly erode enamel, making it more vulnerable to bacterial acid attacks.
Poor Oral Hygiene
Insufficient or improper oral hygiene allows plaque to accumulate and harden into tartar (calculus). Plaque provides a protective environment for bacteria to thrive and produce acids against the tooth surface. Failing to brush twice a day with fluoride toothpaste and floss daily leaves these bacterial colonies undisturbed, perpetuating the acid attack cycle.
Other Contributing Factors
- Dry Mouth (Xerostomia): Saliva helps wash away food particles, neutralize acids, and provides minerals for remineralization. Conditions or medications that cause dry mouth (e.g., antihistamines, antidepressants) significantly increase decay risk.
- Genetics: Some individuals may have naturally weaker enamel or a particular oral microbiome that makes them more susceptible to cavities.
- Existing Dental Work: Old, leaky fillings can create gaps where bacteria can hide and cause secondary decay underneath the restoration.
- Acid Reflux (GERD): Stomach acids brought into the mouth can erode enamel, similar to direct acidic food exposure.
- Fluoride Deficiency: Fluoride is a natural mineral that strengthens enamel and makes it more resistant to acid attacks. Lack of fluoride exposure (e.g., non-fluoridated water, non-fluoride toothpaste) increases susceptibility.
Recognizing the Signs and Symptoms of Tooth Decay
Catching tooth decay early is crucial for simpler, less invasive, and less expensive treatment. Knowing what to look for can help you seek timely professional care.
Early vs. Advanced Decay
- Early Decay: Often presents with no noticeable symptoms. A dentist might spot it as a white, chalky spot on the enamel during a routine check-up. This stage is ideal for intervention, as remineralization treatments might be effective.
- Advanced Decay: As decay progresses into the dentin and pulp, symptoms become more pronounced and painful.
Common Indicators
- Tooth Sensitivity: A common early sign is a sharp, fleeting pain when consuming hot, cold, or sweet foods and drinks. This indicates that the decay has likely reached the dentin.
- Toothache: Persistent pain, especially a throbbing or sharp pain that occurs without an obvious trigger, indicates more significant decay, possibly involving the pulp. Pain that worsens when biting down can also be a sign.
- Visible Pits or Holes: You might notice a small hole (cavity) or pit in your tooth, especially in the chewing surfaces of your back teeth.
- Dark Spots or Staining: Brown, black, or even white stains on the tooth surface can indicate decay. These might be tricky to differentiate from simple tooth discoloration without a dental exam.
- Bad Breath (Halitosis): As bacteria thrive in cavities, they produce foul-smelling gases, leading to persistent bad breath.
- Pus Around the Tooth or Gums: This is a serious sign of infection (abscess) and requires immediate dental attention.
- Swelling: Swelling in the gums or face near the affected tooth also points to a severe infection.
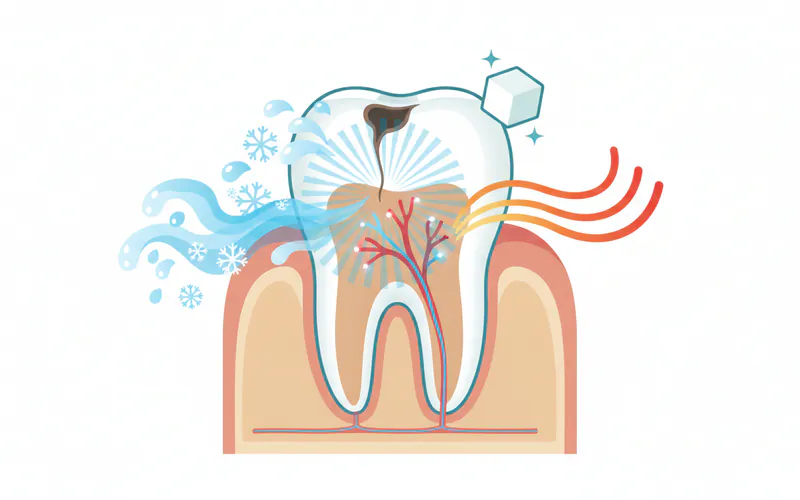
When Decay Affects the Sinus Cavity
This is a specific, often painful, complication that can arise from untreated decay in the upper back teeth (molars and premolars). The roots of these teeth are very close to, or sometimes even extend into, the maxillary sinus cavity.
If decay in an upper back tooth progresses to the point of a severe infection (dental abscess), the infection can spread upwards into the sinus. This is known as odontogenic sinusitis. Symptoms can mimic a common sinus infection:
- Sinus pressure and pain: Especially under the eyes or across the cheeks.
- Nasal congestion or discharge.
- Headache.
- Tooth pain: The original dental pain might be masked by the broader sinus pain.
- Fever and general malaise.
Differentiating between a dental infection and a viral sinus infection can be challenging for the patient, but a dentist can often pinpoint the dental origin with X-rays and vitality testing of the teeth. If an infection is confirmed to be dental, treating the tooth (e.g., root canal or extraction) is essential to resolve the sinus issue.
The ONLY Effective Treatment: Professional Dental Care
Let's be clear: the only way to effectively and safely remove tooth decay is through professional dental intervention. A dentist has the knowledge, training, tools, and sterile environment necessary to stop the decay process and restore your tooth.
Dental Examination and Diagnosis
Your dental journey begins with a thorough examination:
- Visual Inspection: The dentist will visually check your teeth for signs of decay, using a small mirror and explorer tool to probe for soft spots.
- Dental X-rays: These are indispensable. Bitewing X-rays show decay between teeth, while periapical X-rays can reveal infections at the root tips and their proximity to the sinus cavity or other structures.
- Other Diagnostic Tools: Sometimes, a dentist might use a cavity detector dye or a special light to identify decay that's not immediately visible.
Types of Professional Treatments
The type of treatment depends on the severity and extent of the decay:
- Fluoride Treatments/Remineralization (Early Decay): If decay is very superficial (only affecting the enamel as a white spot, without a cavity forming), professional high-concentration fluoride applications can sometimes help the enamel remineralize and reverse the early stages of decay. This reinforces the tooth structure.
- Dental Fillings (Most Common): For small to moderate cavities in the enamel or dentin, a dental filling is the standard treatment.
- Process: The dentist will numb the area, use a drill (or sometimes a laser or air abrasion) to remove the decayed portion of the tooth, and then clean and prepare the space. The cavity is then filled with a restorative material.
- Materials and Pros/Cons:
- Amalgam (Silver) Fillings: Durable, less expensive. Contains mercury (though considered safe by ADA). Visible in the mouth. Lasts 10-15 years or more.
- Composite (Tooth-Colored) Fillings: Esthetically pleasing, can bond directly to tooth structure. More expensive than amalgam. May not be as durable for very large fillings in high-stress areas. Lasts 5-10 years.
- Porcelain/Ceramic Fillings (Inlays/Onlays): Custom-made in a lab, very natural-looking, durable. More expensive, requires two visits. Lasts 10-20 years.
- Gold Fillings (Inlays/Onlays): Highly durable, biocompatible. Most expensive, requires two visits, visible. Lasts 15-30 years.
- Crowns (Extensive Decay, Weakened Tooth): When a cavity is too large for a filling, or if the tooth is significantly weakened, a dental crown (a cap) is often recommended.
- Process: The tooth is reshaped, impressions are taken, and a custom crown (porcelain, ceramic, metal, or a combination) is fabricated. A temporary crown is placed, and the permanent one is cemented on a subsequent visit.
- Root Canal Therapy (Pulp Involvement): If decay has reached the pulp and caused inflammation or infection (abscess), a root canal is performed to save the tooth.
- Process: The infected pulp is removed, the root canals are cleaned and disinfected, and then filled with a rubber-like material. The tooth is then sealed, often requiring a crown to protect it from fracture.
- Tooth Extraction (Severe, Untreatable Decay): In cases of extremely severe decay, extensive infection that cannot be resolved with a root canal, or significant structural damage, the tooth may need to be extracted.
- Process: The tooth is carefully removed. Options for replacing the missing tooth (dental implant, bridge, or partial denture) should be discussed to prevent shifting of adjacent teeth and maintain chewing function.
What to Expect During a Professional Tooth Decay Removal
Knowing what happens during a filling or other decay removal procedure can help alleviate anxiety.
Anesthesia and Numbing
The first step is typically to numb the area around the affected tooth. Your dentist will apply a topical anesthetic gel to the gum, followed by a local anesthetic injection (usually lidocaine or similar). This ensures you won't feel pain during the procedure, though you might feel pressure or vibration.
Decay Removal
Once the area is numb, the dentist will use a small, high-speed handpiece (the "dental drill") or sometimes a laser or air abrasion tool to carefully remove the decayed and softened tooth structure. The goal is to remove all infected material while preserving as much healthy tooth structure as possible. A suction device will be used to keep the area dry and clear of debris.
Restoration
After the decay is completely removed, the remaining healthy tooth structure is prepared for the chosen restorative material:
- For Fillings: The cavity is cleaned, sometimes a liner or base is applied to protect the pulp, and then the filling material (e.g., composite resin) is placed in layers, shaped, and hardened with a special light. Finally, the filling is polished for a smooth surface.
- For Crowns: If a crown is needed, the tooth will be shaped to accommodate the crown, an impression will be taken, and a temporary crown will be placed while the permanent one is being fabricated in a lab. You'll return for a second appointment to have the permanent crown cemented.
- For Root Canal Therapy: This is a more involved procedure where the infected pulp is removed, the canals are cleaned and shaped, and then filled and sealed. A temporary filling is placed, and often a crown is needed afterwards to protect the weakened tooth.
The entire process for a simple filling usually takes between 30 minutes to an hour. More complex procedures like root canals or crowns will take longer and typically require multiple appointments.
Cost of Professional Tooth Decay Treatment in the US
The cost of dental treatment for tooth decay can vary significantly based on several factors. Understanding these can help you anticipate expenses.
Factors Influencing Cost
- Severity of Decay: A small cavity treated with a filling will be much less expensive than extensive decay requiring a root canal and crown.
- Location of the Tooth: Front teeth (incisors, canines) are often easier to access and may be slightly less expensive to treat than molars, especially wisdom teeth.
- Type of Material Used: Composite (tooth-colored) fillings are typically more expensive than amalgam (silver) fillings. Gold and porcelain restorations are the most costly.
- Dentist's Fees: Fees vary by practice location (urban vs. rural), experience of the dentist, and overhead costs.
- Geographic Region: Dental costs are generally higher in major metropolitan areas and specific regions of the US.
Average Cost Ranges (Without Insurance, US Dollars)
Here's a general idea of what you might expect to pay for common decay treatments:
| Treatment Type | Average Low Cost | Average High Cost |
|---|---|---|
| Simple Filling (Amalgam) | $50 | $250 |
| Simple Filling (Composite) | $90 | $450 |
| Inlay/Onlay (Porcelain/Gold) | $600 | $1,500 |
| Dental Crown (Porcelain Fused to Metal) | $800 | $1,800 |
| Dental Crown (All Ceramic/Porcelain) | $1,000 | $2,500 |
| Root Canal (Front Tooth) | $700 | $1,200 |
| Root Canal (Molar) | $1,000 | $2,000 |
| Tooth Extraction (Simple) | $75 | $300 |
| Tooth Extraction (Surgical/Impacted) | $200 | $600+ |
Note: These are average ranges and can fluctuate. Always get a detailed estimate from your dentist.
Dental Insurance Coverage
Most dental insurance plans in the US categorize treatments into different tiers:

- Preventive Care (e.g., cleanings, exams, X-rays): Often covered at 80-100%.
- Basic Procedures (e.g., fillings, simple extractions): Typically covered at 70-80% after you meet your deductible.
- Major Procedures (e.g., crowns, root canals, dentures): Usually covered at 50% after your deductible. Orthodontics may be a separate benefit.
Deductible: The amount you must pay out-of-pocket before your insurance starts to cover costs (e.g., $50-$100 per year). Co-pay: A fixed amount you pay for a service. Annual Maximum: The maximum amount your insurance will pay in a year (e.g., $1,000-$2,000). Once reached, you pay 100% of costs.
Table: Impact of Insurance on Decay Treatment Costs (Example Scenario)
| Procedure (Avg. Cost) | Without Insurance | With Insurance (80% coverage after $50 deductible, $150 procedure) | Out-of-Pocket with Insurance |
|---|---|---|---|
| Composite Filling ($250) | $250 | ($250 - $50 deductible) * 20% = $40 | $90 |
| Root Canal (Molar, $1500) | $1,500 | ($1,500 - $50 deductible) * 50% = $725 | $775 |
| Porcelain Crown ($1800) | $1,800 | ($1,800 - $50 deductible) * 50% = $875 | $925 |
This table is a simplified example. Your actual costs will depend on your specific plan's details, your deductible status, and how much of your annual maximum remains.
Cost-Saving Tips
- Prevention, Prevention, Prevention: The cheapest treatment for decay is preventing it entirely. Regular brushing, flossing, and dental check-ups are your best investment.
- Early Treatment: Small cavities are cheaper to treat than large ones requiring extensive procedures. Don't delay!
- Dental Schools: Many university dental schools offer high-quality care at reduced rates, as procedures are performed by students under the close supervision of experienced faculty.
- Payment Plans/Financing: Discuss payment options with your dentist. Many offer in-house payment plans or work with third-party financing companies like CareCredit.
- Dental Discount Plans: These are not insurance but offer a discount on services for an annual fee.
Recovery and Aftercare After Professional Treatment
After having tooth decay professionally removed and the tooth restored, proper aftercare is essential for a smooth recovery and the longevity of your new filling or crown.
Post-Filling Care
- Numbness: The local anesthetic will wear off in a few hours. Avoid chewing on the treated side until the numbness is completely gone to prevent accidentally biting your cheek or tongue.
- Sensitivity: It's common to experience some sensitivity to hot, cold, or pressure for a few days or even weeks after a filling. This is usually temporary and should subside. If it persists or worsens, contact your dentist.
- Chewing: You can generally eat normally once the numbness wears off, though your dentist might recommend avoiding hard or sticky foods for the first 24 hours with certain composite fillings.
- Oral Hygiene: Continue your regular brushing and flossing routine.
Post-Crown Care
- Temporary Crown: You'll wear a temporary crown for about 1-3 weeks. Be gentle with it: avoid sticky or very hard foods, chew on the opposite side, and slide floss out from between your teeth rather than pulling up, which can dislodge the temporary.
- Permanent Crown: Once the permanent crown is cemented, it should feel like your natural tooth. Some minor sensitivity to hot or cold is normal for a short period.
- Bite Adjustment: If your bite feels "off" or high, contact your dentist immediately, as this can lead to discomfort and damage.
- Oral Hygiene: Maintain excellent oral hygiene, brushing and flossing around your crown as you would your natural teeth. Crowns can still get decay at their margins if not properly cleaned.
Post-Root Canal Care
- Pain/Soreness: It's normal to experience some pain and soreness for a few days after a root canal, especially when chewing. Over-the-counter pain relievers (ibuprofen, acetaminophen) are usually sufficient.
- Antibiotics: If an infection was present, your dentist might prescribe antibiotics. Take them as directed.
- Crown Placement: A tooth that has had a root canal is more brittle and prone to fracture. It's crucial to follow up with your dentist to get a permanent crown placed soon after the root canal to protect the tooth.
- Avoid Chewing: Avoid chewing on the treated tooth until the permanent restoration (usually a crown) is placed to prevent fracture.
Managing Sensitivity
For temporary sensitivity after any procedure, consider using a toothpaste designed for sensitive teeth (containing ingredients like potassium nitrate or strontium chloride) and avoid very hot or cold foods. If sensitivity persists or is severe, consult your dentist.
Prevention: Your Best Defense Against Tooth Decay
Since you can't remove tooth decay yourself, your best strategy is to prevent it from happening in the first place or catch it at its earliest, most treatable stage.
Excellent Oral Hygiene
- Brush Twice Daily (2 Minutes Each Time): Use an ADA-accepted fluoride toothpaste and a soft-bristled toothbrush. Brush all surfaces of your teeth, including the chewing surfaces, the outer surfaces, and the inner surfaces. Don't forget to brush your tongue!
- ADA Guidelines: The American Dental Association recommends brushing for two minutes, twice a day, and flossing daily.
- Floss Daily: Flossing removes plaque and food particles from between your teeth and under the gumline where a toothbrush can't reach. This is critical for preventing interproximal (between teeth) cavities.
- Mouthwash (Optional): An antimicrobial or fluoride mouthwash can provide an added layer of protection but should not replace brushing and flossing.
Pro Tip: Choose an ADA-accepted fluoride toothpaste for optimal protection against decay. Look for the ADA Seal of Acceptance on the packaging.
Dietary Modifications
- Limit Sugary and Acidic Foods/Drinks: Reduce your intake of soda, fruit juices, sports drinks, candy, pastries, and refined carbohydrates.
- Eat Tooth-Friendly Snacks: Opt for fresh fruits, vegetables, cheese, nuts, and plain yogurt.
- Drink Water: Water helps rinse away food particles and acids. Fluoridated tap water is especially beneficial.
- Chew Sugar-Free Gum: Chewing gum stimulates saliva flow, which helps neutralize acids and wash away food. Look for gum sweetened with xylitol, which has been shown to reduce cavity-causing bacteria.
Fluoride's Role
Fluoride is a miracle mineral for dental health:
- Strengthens Enamel: It helps remineralize weakened enamel spots and makes the tooth structure more resistant to acid attacks.
- Community Water Fluoridation: Many US communities have fluoridated public water supplies, a safe and effective public health measure.
- Fluoride Toothpaste/Rinses: Essential components of daily oral hygiene.
- Professional Fluoride Applications: Your dentist can apply concentrated fluoride varnish or gel during check-ups, especially for children or adults at high risk of decay.
Regular Dental Check-ups and Cleanings
- Frequency: Visit your dentist typically every six months for a comprehensive exam and professional cleaning. This schedule allows for:
- Early Detection: Your dentist can spot decay at its earliest stages, often before symptoms appear, allowing for simpler, less invasive treatment.
- Plaque and Tartar Removal: Professional cleanings remove hardened plaque (tartar) that cannot be removed by brushing and flossing alone.
- Personalized Advice: Your dentist can assess your individual risk factors and provide tailored advice for prevention.
Dental Sealants
- What they are: Thin, protective coatings painted onto the chewing surfaces of the back teeth (molars and premolars). These surfaces often have deep grooves and pits where food particles and bacteria can get trapped.
- How they work: Sealants fill in these grooves, creating a smooth surface that's easier to clean and protecting the enamel from decay.
- Who benefits: Highly recommended for children and teenagers, but adults at high risk of decay can also benefit.
Risks and Complications of Untreated Tooth Decay (or Failed DIY Attempts)
Ignoring tooth decay or attempting to treat it yourself can lead to severe and potentially life-threatening consequences.
Severe Pain and Infection
- Dental Abscess: As decay progresses into the pulp, bacteria can cause an infection that leads to a painful pocket of pus (abscess) at the root tip. This can cause severe, throbbing pain, facial swelling, fever, and swollen lymph nodes.
- Cellulitis: A dental abscess can spread into the surrounding soft tissues of the face, neck, or jaw, causing a serious bacterial infection called cellulitis. This requires immediate medical attention and intravenous antibiotics.
Tooth Loss
If decay is too extensive, or if an infection is too severe to treat with a root canal, the tooth may need to be extracted. Missing teeth can lead to difficulty chewing, changes in speech, and shifting of adjacent teeth, impacting your overall oral health and appearance.
Spread of Infection
A dental infection isn't confined to your mouth:
- Sinuses: As mentioned, upper tooth infections can spread to the maxillary sinus, causing odontogenic sinusitis.
- Bloodstream (Sepsis): In rare but severe cases, bacteria from a dental abscess can enter the bloodstream and spread throughout the body, leading to a life-threatening condition called sepsis, a systemic inflammatory response.
- Brain Abscess/Cavernous Sinus Thrombosis: Extremely rare but serious complications where infection spreads to the brain or a critical blood clot forms near the brain.
Damage to Adjacent Teeth
Untreated decay can create an environment conducive to decay in neighboring teeth, especially if food and bacteria are constantly trapped.
Emergency Dental Situations
Many dental emergencies, such as severe toothache, facial swelling, or a knocked-out tooth, are a direct result of neglected tooth decay. These require immediate and often expensive treatment.
Children and Pediatric Considerations for Tooth Decay
Tooth decay is a significant concern for children, even at a very young age. Early childhood caries (ECC) is a serious form of decay that affects infants and toddlers.
Early Childhood Caries (ECC)
- Causes: ECC is often associated with prolonged exposure to sugary liquids. This can happen when a baby falls asleep with a bottle containing milk, formula, juice, or sweetened liquids, or uses a pacifier dipped in sugar or honey. The sugars pool around the teeth, providing fuel for bacteria during sleep when saliva flow is reduced.
- Appearance: Typically affects the upper front teeth first, appearing as white spots, then turning brown or black, leading to severe decay and often requiring extensive restorative work.
Importance of First Dental Visit
The American Academy of Pediatric Dentistry (AAPD) and the ADA recommend that a child's first dental visit should occur by their first birthday or within six months of the eruption of their first tooth. This allows the dentist to:
- Assess oral health and development.
- Provide guidance on proper brushing, flossing, and diet.
- Discuss fluoride needs.
- Educate parents on preventive strategies for ECC.
Preventive Measures for Kids
- Wipe Gums: Even before teeth erupt, gently wipe your baby's gums with a clean, damp cloth after feedings.
- Brush with Fluoride Toothpaste: As soon as the first tooth appears, brush twice daily with a tiny smear (rice-grain size) of fluoride toothpaste for children under 3. For children 3-6 years old, use a pea-sized amount.
- Limit Sugary Drinks: Avoid giving babies bottles of sugary liquids at bedtime. Offer water after meals. Transition children from bottles to sippy cups by age 1.
- Dental Sealants: Sealants are highly effective in preventing decay on the chewing surfaces of children's molars once they erupt. They are typically applied around ages 6 and 12 for the first and second permanent molars, respectively.
- Professional Fluoride Varnish: Pediatric dentists frequently apply fluoride varnish to children's teeth to strengthen enamel and prevent cavities.
Early and consistent dental care for children is vital for establishing good habits and protecting their developing smiles.
Frequently Asked Questions
Can I really remove tooth decay myself?
No, you cannot safely or effectively remove tooth decay yourself. Tooth decay is structural damage caused by bacterial acid, forming a hole (cavity) in the tooth. Removing it requires specialized dental tools to precisely excavate infected tissue and restore the tooth with a filling material, all within a sterile environment. Attempting DIY removal will only cause further damage, pain, infection, and potentially tooth loss.
What are some home remedies for toothache while I wait for a dental appointment?
While home remedies cannot cure tooth decay, they can temporarily alleviate pain. Rinse your mouth with warm salt water to reduce inflammation. Apply a cold compress to your cheek outside the painful area. Over-the-counter pain relievers like ibuprofen or acetaminophen can also help. You can also try clove oil (applied carefully with a cotton swab, avoiding swallowing). Crucially, these are temporary measures; always see a dentist for diagnosis and treatment.
How quickly does tooth decay progress?
The progression of tooth decay varies greatly depending on factors like diet, oral hygiene, and individual saliva chemistry. It can take months or even years for a cavity to form and progress from early enamel demineralization to a deep cavity affecting the dentin or pulp. However, once a cavity forms, it tends to accelerate in the softer dentin. For children, decay can progress much faster.
Is it possible for a cavity to heal on its own?
A true cavity, meaning a hole has formed in the tooth, cannot heal itself. Once the tooth structure is physically lost, it requires professional restoration (a filling or crown) to be repaired. However, very early stages of demineralization, often appearing as white spots on the enamel, can sometimes be reversed with improved oral hygiene and professional fluoride treatments, allowing the tooth to remineralize.
What is the most expensive type of tooth decay treatment?
Generally, treatment for advanced tooth decay, especially when it results in tooth loss, is the most expensive. This would include root canal therapy followed by a crown (potentially $1,500-$4,000+), or tooth extraction followed by a dental implant and crown (often $3,000-$6,000+ per tooth). Prevention and early intervention are always the most cost-effective strategies.
Can I get an infection from tooth decay?
Yes, absolutely. Untreated tooth decay eventually reaches the pulp, the innermost part of the tooth containing nerves and blood vessels. Once bacteria infect the pulp, it can lead to a painful dental abscess, a pocket of pus at the root tip. This infection can spread to surrounding bone, gums, face, or even into the bloodstream, becoming a serious medical emergency.
How often should I get dental check-ups to prevent decay?
For most healthy individuals, the American Dental Association recommends a dental check-up and professional cleaning every six months. Your dentist may recommend more frequent visits if you have specific risk factors for decay, gum disease, or other ongoing dental issues. Regular check-ups are vital for early detection and prevention.
Does chewing gum help prevent cavities?
Chewing sugar-free gum can help prevent cavities, primarily by stimulating saliva flow. Saliva helps neutralize acids, wash away food particles, and delivers minerals to the tooth surface for remineralization. Gum sweetened with xylitol is particularly beneficial, as xylitol can inhibit the growth of cavity-causing bacteria. However, it's not a substitute for brushing and flossing.
What is the difference between plaque and decay?
Plaque is a sticky, colorless film of bacteria that constantly forms on your teeth. These bacteria, when they consume sugars, produce acids. Tooth decay (a cavity) is the result of these acids eroding the tooth enamel and dentin, leading to actual holes or structural damage in the tooth. Plaque causes decay, but they are not the same thing.
Can certain foods really help remineralize teeth?
While no food can "heal" a cavity, some foods can support the natural remineralization process of enamel. Dairy products (milk, cheese, yogurt) are rich in calcium and phosphates, which are key minerals for enamel. Chewing fibrous foods like fruits and vegetables stimulates saliva flow, aiding in acid neutralization and rinsing away food debris. However, these benefits are part of an overall healthy diet and oral hygiene routine.
When to See a Dentist
Given that self-removal of tooth decay is neither possible nor safe, knowing when to seek professional dental help is paramount. Do not delay seeing a dentist if you experience any of these signs.
Clear Warning Signs That Need Immediate Attention
Contact your dentist or seek emergency dental care immediately if you experience:
- Severe, persistent toothache: Especially if it's throbbing, keeps you awake at night, or doesn't respond to over-the-counter pain relievers.
- Swelling: Any swelling in your face, jaw, or gums. This is a strong indicator of a serious infection (abscess) that can spread rapidly.
- Pus or Foul Taste: The presence of pus around a tooth or a persistent foul taste in your mouth often signifies a dental abscess.
- Fever: A fever accompanied by tooth pain or swelling indicates a spreading infection that requires urgent medical and dental care.
- Difficulty Swallowing or Breathing: These are critical symptoms indicating a severe, rapidly spreading infection that could be life-threatening. Seek emergency medical attention (e.g., go to an emergency room) immediately.
Red Flags vs. Routine Care Guidance
- Red Flags (Needs Prompt Appointment):
- Sensitivity to hot, cold, or sweets that persists for more than a few days.
- Visible holes, pits, or dark spots on your teeth.
- Pain when biting down or chewing.
- Food getting consistently stuck in a particular spot.
- Chipped or broken fillings.
- Persistent bad breath despite good oral hygiene.
- Pain or pressure in your upper teeth that might be related to your sinus cavity.
- Routine Care Guidance: Even without symptoms, adhere to your recommended schedule of regular dental check-ups and cleanings (typically every 6 months). These routine visits are crucial for detecting early decay, identifying potential problems before they become severe, and maintaining optimal oral health. Prevention and early intervention are always the best course of action.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Is an Abscess
Imagine a throbbing pain deep within your jaw, a persistent ache that keeps you awake at night and makes even the softest foods unbearable. This isn't just a bad toothache; it could be a sign of something much more serious: a dental abscess. Affecting millions of Americans annually, an abscess is an
February 22, 2026
Cracked Tooth Syndrome: Complete Guide
Cracked Tooth Syndrome: Complete Guide Category: Dental Conditions & Diseases
February 22, 2026
Dentinogenesis Imperfecta: Complete Guide
Imagine a world where your teeth, fundamental to chewing, speaking, and even smiling confidently, are inherently fragile, discolored, and prone to rapid wear from the moment they emerge. For individuals affected by dentinogenesis imperfecta (DI), this is a reality. While relatively rare, affecti
February 22, 2026
Stage 1 Early Cavity: Complete Guide
Did you know that dental cavities are one of the most common chronic diseases globally, affecting both children and adults? In the United States, over 90% of adults have had a cavity, and a significant portion of these begin as a stage 1 early cavity. Often invisible and painless in its nasc
February 22, 2026