How Much Is an Implant Tooth
Key Takeaways
- Losing a tooth can be more than just an aesthetic concern; it can profoundly impact your ability to chew, speak, and even affect the health of your remaining teeth and jawbone. For many Americans, dental implants have emerged as the gold standard for tooth replacement, offering a durable, natural-lo
How Much Is an Implant Tooth: A Comprehensive Guide to Costs, Care, and Considerations
Losing a tooth can be more than just an aesthetic concern; it can profoundly impact your ability to chew, speak, and even affect the health of your remaining teeth and jawbone. For many Americans, dental implants have emerged as the gold standard for tooth replacement, offering a durable, natural-looking, and functional solution. However, one of the most common questions our readers at SmilePedia.net ask is: how much is an implant tooth?
The truth is, the cost of a dental implant isn't a single, fixed number. It's an investment influenced by a myriad of factors, from the complexity of your specific case and the number of implants required to geographic location and the materials used. Understanding these variables is crucial for making an informed decision about your oral health. This comprehensive guide will meticulously break down the typical costs associated with dental implants in the US, explore payment options, detail the treatment process, and arm you with the knowledge you need to navigate this important dental procedure confidently. We’ll delve into what an implant entails, different types available, the step-by-step journey, and crucial aftercare to ensure your investment lasts a lifetime.
Key Takeaways:
- A single dental implant in the US typically costs between $3,000 and $6,000, encompassing the implant post, abutment, and crown.
- Additional procedures like bone grafting or extractions can add $200 to $3,000+ per tooth to the total cost.
- The entire implant process, from initial surgery to final crown placement, usually spans 3 to 9 months, depending on healing and preparatory procedures.
- Dental insurance often provides limited or no coverage for implants; explore medical insurance, HSAs, FSAs, and financing options.
- Implants are a long-term investment, often lasting 20-30 years or more with proper care, making them highly cost-effective compared to other alternatives over time.
- Geographic location and the specific dental professional's expertise significantly influence pricing.
What is a Dental Implant? An Overview
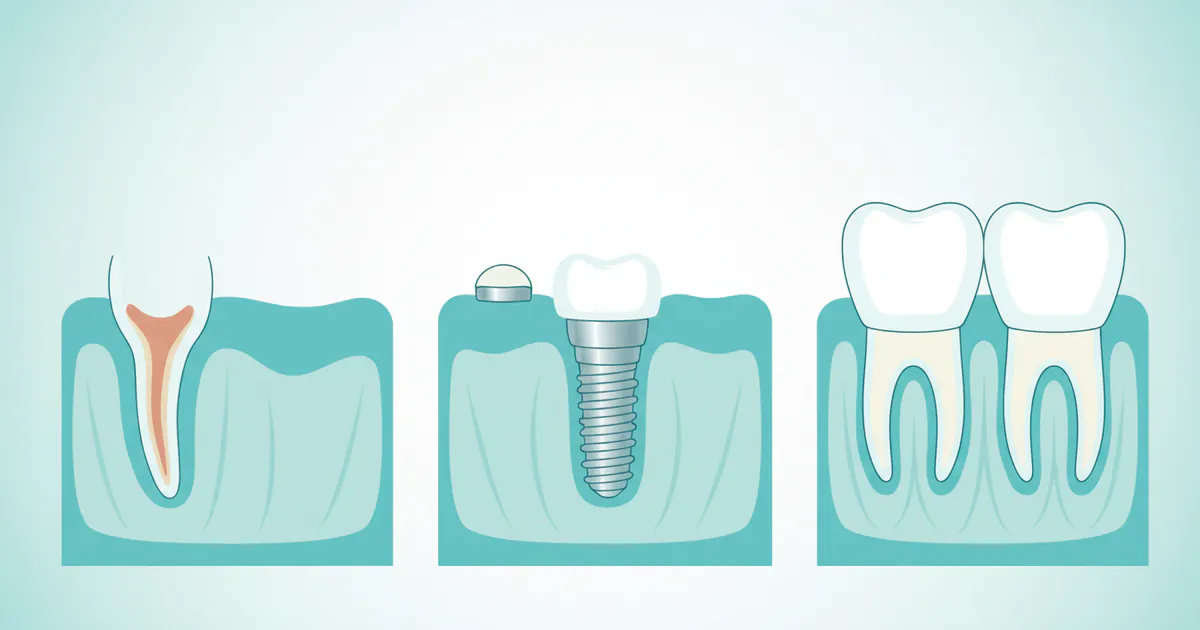
A dental implant is a sophisticated medical device designed to replace the root of a missing tooth. Unlike dentures or bridges, which sit on top of the gums or rely on adjacent teeth for support, an implant is surgically placed into the jawbone, providing a stable and permanent foundation for a replacement tooth. This integration with the bone is called osseointegration and is the key to an implant's strength and longevity.
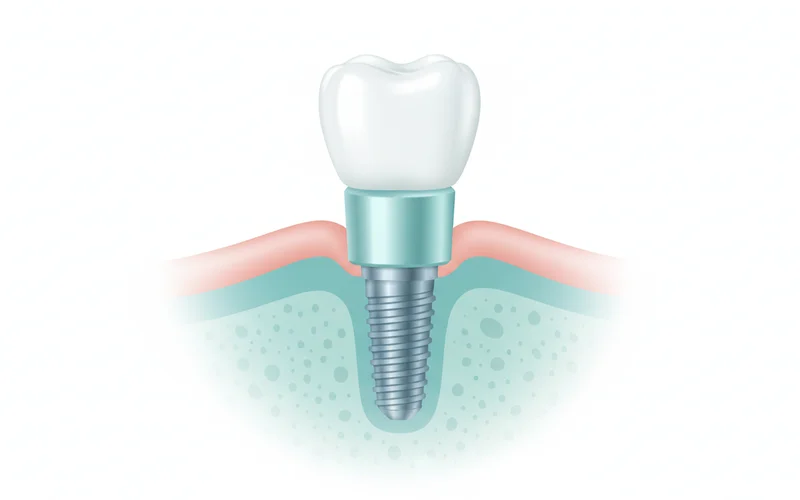
A complete dental implant typically consists of three main components:
- The Implant Post (Fixture): This is a small, screw-shaped cylinder, usually made of biocompatible titanium, that is surgically placed into the jawbone. It acts as the artificial tooth root.
- The Abutment: Once the implant post has fused with the jawbone (osseointegrated), an abutment is attached. This small connector extends above the gum line and serves as the anchor for the final restoration.
- The Dental Crown (Prosthesis): This is the visible, custom-made tooth restoration that is secured to the abutment. Crowns are typically made from durable materials like porcelain, zirconia, or ceramic, designed to match the color and shape of your natural teeth.
Together, these components create a replacement tooth that looks, feels, and functions remarkably like a natural tooth. Dental implants are a preferred solution because they restore chewing ability, improve speech, prevent bone loss in the jaw, and maintain the alignment of surrounding teeth.
Why Consider a Dental Implant? The Benefits of a Permanent Solution
Choosing a dental implant goes beyond simply filling a gap in your smile. It's an investment in your overall oral health and quality of life. The benefits are numerous and far-reaching:
- Improved Aesthetics: Implants are custom-made to match your natural teeth, providing a seamless and natural-looking restoration that enhances your smile and facial appearance.
- Enhanced Functionality: Unlike removable dentures, implants function like natural teeth, allowing you to chew, bite, and speak with confidence and comfort. There's no slipping, clicking, or discomfort.
- Preservation of Bone Health: When a tooth is lost, the jawbone in that area can begin to resorb or shrink due to lack of stimulation. Implants, by integrating with the bone, provide the necessary stimulation to preserve bone density and prevent further bone loss, which can maintain facial structure.
- Protection of Adjacent Teeth: Traditional dental bridges require altering (grinding down) healthy adjacent teeth to serve as anchors. Implants stand alone, leaving your natural teeth untouched and preserving their long-term health.
- Durability and Longevity: With proper care and oral hygiene, dental implants are incredibly durable and can last for decades, often a lifetime. This makes them a highly cost-effective solution over the long term compared to alternatives that may need frequent replacement.
- Comfort and Convenience: Implants are a permanent part of your mouth, eliminating the inconvenience and potential discomfort of removable dentures. You brush and floss them just like natural teeth.
- Improved Oral Health: By preventing the shifting of adjacent teeth into the gap, implants help maintain proper occlusion (bite) and make it easier to clean your teeth, reducing the risk of gum disease and cavities.
The risks of not replacing a missing tooth include shifting of surrounding teeth, overeruption of the opposing tooth, difficulty chewing, speech impediments, and significant bone loss, which can lead to a "sunken" facial appearance over time. Considering these factors, the initial investment in a dental implant often proves to be a wise decision for long-term health and well-being.
Understanding Dental Implant Types and Variations
While the basic structure of a dental implant (post, abutment, crown) remains consistent, there are several types and approaches to suit different patient needs, bone structures, and budgets. Understanding these variations can help you discuss the best option with your dentist.
Standard Implant Types
- Endosteal Implants: These are the most common type of dental implant. They are typically titanium, screw-shaped posts surgically placed directly into the jawbone. Once the surrounding bone has healed around the implant (osseointegration), an abutment and crown are attached. Endosteal implants are suitable for most patients with sufficient bone density.
- Subperiosteal Implants: These implants are rarely used today. Instead of being placed in the bone, they rest on the jawbone, just under the gum tissue. A metal frame is custom-made to fit over the bone, with posts protruding through the gums to hold the prosthesis. These were primarily used for patients who could not wear conventional dentures and had minimal bone height.
- Zygomatic Implants: These are much longer implants used for severe bone loss in the upper jaw, where standard endosteal implants aren't feasible. They anchor into the cheekbone (zygoma) instead of the maxilla (upper jawbone). Zygomatic implants are complex procedures performed by highly specialized oral surgeons.
Specialized Implant Approaches and Solutions
- Mini Dental Implants (MDIs): These are smaller in diameter than conventional implants (typically less than 3mm). MDIs are primarily used to stabilize lower dentures, providing a more secure fit and improved chewing ability. They can also be used for temporary tooth replacement or in areas with very limited bone width where traditional implants might not fit. They are generally less expensive and involve a less invasive procedure.
- Immediate Load Implants ("Teeth in a Day"): In specific cases where bone quality is excellent and primary stability is high, a temporary crown can be placed on the implant immediately after surgical placement. This allows patients to leave with a temporary tooth, though it still requires careful chewing restrictions until full osseointegration occurs. Not all patients are candidates for this.
- All-on-4® or All-on-6® Dental Implants: These are full-arch rehabilitation solutions designed to replace an entire set of upper or lower teeth using only four or six strategically placed implants. The implants are angled to maximize contact with available bone, often eliminating the need for bone grafting. A full arch of prosthetic teeth is then attached to these implants. This option offers a complete, fixed solution for patients missing all or most of their teeth.
- Implant-Supported Bridge: If you are missing several adjacent teeth, an implant-supported bridge can be used. Instead of needing an implant for every missing tooth, two or more implants are placed, and then a bridge spanning the gap is anchored to them. This provides a stable, fixed solution without affecting healthy teeth.
Each type has specific indications, advantages, and cost implications. Your dental professional will assess your oral health, bone density, and aesthetic goals to recommend the most appropriate implant solution for you.
The Dental Implant Process: A Step-by-Step Guide
The journey to a new smile with dental implants is a carefully planned and executed process, often spanning several months. While individual timelines can vary, here’s a general overview of what you can expect:
Step 1: Initial Consultation and Comprehensive Planning
This crucial first step involves a thorough examination by your dentist or oral surgeon. They will:
- Review your medical and dental history.
- Take X-rays, 3D cone-beam computed tomography (CBCT) scans, and digital impressions to assess your bone structure, nerve pathways, and sinus cavities.
- Discuss your goals and evaluate your suitability for implants, considering factors like bone density, overall health, and oral hygiene.
- Develop a personalized treatment plan, including the type of implant, the number of implants, and any necessary preparatory procedures.
- Pro Tip: Don't hesitate to ask about the full cost breakdown and financing options during this initial consultation.
Step 2: Preparatory Procedures (If Needed)
Some patients may require additional procedures before implant placement to ensure a successful outcome:
- Tooth Extraction: If the damaged tooth is still present, it will need to be carefully extracted.
- Bone Grafting: If you have insufficient jawbone density (common after tooth loss), bone grafting may be necessary. This involves adding bone material (from your own body, a donor, or synthetic sources) to the jawbone to create a strong foundation for the implant. This process can take 3-6 months to heal and integrate before implant placement can proceed.
- Sinus Lift (Sinus Augmentation): If an implant is needed in the upper jaw and the sinus floor is too close to the jaw, a sinus lift procedure may be performed. This involves lifting the sinus membrane and adding bone material to increase bone height. This also requires a healing period of several months.
Step 3: Dental Implant Placement Surgery
Once your jawbone is ready, the implant post (the titanium screw) is surgically placed into the bone. This outpatient procedure typically involves:
- Local anesthesia (and sometimes sedation) to ensure your comfort.
- A small incision in the gum to expose the bone.
- A precise hole drilled into the jawbone.
- The implant post being carefully screwed into place.
- Sutures to close the gum tissue over the implant, or a healing cap may be placed. The surgical procedure itself usually takes 1-2 hours for a single implant.
Step 4: Osseointegration (Healing Period)
This is the most critical phase, where the titanium implant post fuses with your jawbone. This natural biological process, called osseointegration, creates a robust and stable anchor for your new tooth. This healing period typically lasts 3 to 6 months, during which you may wear a temporary removable prosthesis if desired.
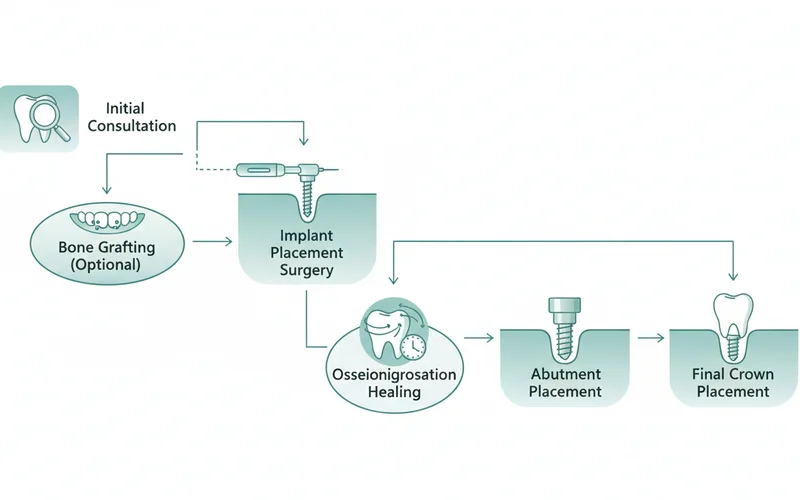
Step 5: Abutment Placement (If Not Already Integrated)
After successful osseointegration, a second minor surgical procedure may be required. This involves:
- Making a small incision in the gum to expose the top of the implant.
- Attaching the abutment (the connector piece) to the implant post.
- Closing the gum tissue around the abutment. This typically requires a short healing period of 1-2 weeks for the gums to heal around the abutment. In some cases, the implant and abutment are placed as one piece, or the abutment is placed during the initial surgery.
Step 6: Fabrication and Placement of the Permanent Crown
Once your gums have healed around the abutment, impressions of your mouth are taken. These impressions are sent to a dental lab where your custom-made crown, bridge, or full arch of teeth will be fabricated to precisely match your natural teeth in color, shape, and size.
- You may have several appointments for fitting and adjustments.
- The final crown is then securely cemented or screwed onto the abutment.
The entire process, from consultation to final crown placement, generally takes 3 to 9 months, sometimes longer if extensive bone grafting or other preliminary procedures are needed. While it may seem lengthy, each step is vital for ensuring the long-term success and stability of your dental implant.
How Much is an Implant Tooth? A Comprehensive Cost Breakdown
Understanding the cost of a dental implant requires breaking down the various components and factors that contribute to the final price. While we aim for specific numbers, it's crucial to remember that these are averages and can fluctuate significantly. Generally, how much are tooth implants? For a single tooth, expect to pay between $3,000 and $6,000+ in the United States.
Factors Influencing Implant Cost
Several variables play a role in determining how much does an implant cost:
- Number of Implants: A single implant is less expensive than multiple implants or full-arch solutions.
- Location of the Implant: Implants in the anterior (front) aesthetic zone might require more precise placement and finer materials, potentially increasing costs. The complexity of the bone structure also varies between the upper and lower jaws.
- Additional Procedures (Site Preparation):
- Tooth Extraction: If the tooth needs removal, it can cost $75 - $300 for a simple extraction, or $200 - $600+ for a surgical extraction (e.g., impacted molar).
- Bone Grafting: This is a significant cost factor, ranging from $200 to $2,000+ per site, depending on the material used and the extent of the graft. A full sinus lift can be $1,500 - $3,000+.
- Soft Tissue Grafting: If gum recession is present, a gum graft may be needed, costing $300 - $1,500.
- Type of Implant:
- Standard endosteal implants are the most common.
- Mini implants are generally less expensive per unit but are used for specific purposes like denture stabilization, not single-tooth replacement.
- Zygomatic implants are highly specialized and significantly more expensive.
- Material of the Crown:
- Porcelain Fused to Metal (PFM): Often more affordable, $800 - $1,500.
- All-Ceramic (Zirconia or Emax): More aesthetic and biocompatible, $1,000 - $2,500+.
- Geographic Location: Costs are typically higher in major metropolitan areas and on the coasts compared to rural areas or the Midwest.
- Dentist's Experience and Specialization:
- General dentists performing implants may charge less than board-certified oral surgeons, periodontists, or prosthodontists. However, specialists often have advanced training and equipment.
- Technology Used: The use of advanced technology like 3D imaging (CBCT scans), guided surgery templates, and intraoral scanners can contribute to the overall cost but often leads to more predictable and safer outcomes.
Average US Costs for a Single Dental Implant
To get a clearer picture of how much an implant tooth typically costs, let's break down the components for a single tooth replacement:
- Implant Post (Titanium Screw): $1,500 - $3,000
- This covers the surgical placement and the implant device itself.
- Abutment (Connector Piece): $500 - $1,000
- This is the piece that connects the implant post to the crown.
- Dental Crown (Prosthesis): $1,000 - $2,500
- This is the visible, custom-made tooth that fits over the abutment.
Total Estimated Cost for a Single Dental Implant (Post, Abutment, Crown, and basic surgery): $3,000 - $6,000+
This range does not include potential preparatory procedures like bone grafts or extractions, which would be added on top.
Costs for Multiple Implants and Full-Arch Solutions
If you need to replace several teeth or an entire arch, the costs escalate, but often become more cost-effective per tooth compared to individual implants due to economies of scale for laboratory work and surgery.
- Implant-Supported Bridge (e.g., replacing 3-4 teeth with 2 implants): $6,000 - $15,000+
- Full Arch Dental Implants (All-on-4® or All-on-6®):
- Per Arch (upper or lower): $20,000 - $40,000+
- Full Mouth (both arches): $40,000 - $80,000+ These comprehensive solutions typically include all surgical fees, implants, abutments, and a full set of prosthetic teeth for the arch.
Regional Cost Variations
Costs can vary significantly across different states and even within different cities. Here's a generalized table showing potential differences:
| US Region | Single Implant (Post, Abutment, Crown) | Full Arch (All-on-4/6) |
|---|---|---|
| Northeast | $3,500 - $6,500 | $25,000 - $45,000 |
| West Coast | $3,800 - $7,000 | $28,000 - $48,000 |
| South | $3,000 - $5,500 | $22,000 - $40,000 |
| Midwest | $2,800 - $5,000 | $20,000 - $38,000 |
Note: These are average ranges and can vary based on specific practices and patient needs.
Navigating Insurance and Payment Options
The financial investment in dental implants is significant, but many options exist to make them more accessible. Understanding insurance coverage and financing alternatives is key.
Does Dental Insurance Cover Implants?
This is a frequently asked question, and the answer is often complex.
- Limited or No Coverage: Historically, most dental insurance plans have categorized implants as a "cosmetic" procedure or "major dental work" with very limited or no coverage. Many plans cap annual benefits at $1,000 - $2,000, which barely covers a fraction of the total implant cost.
- Increasing Coverage: As implants become more common and recognized for their health benefits, some newer, higher-tier dental insurance plans are beginning to offer partial coverage (e.g., 20-50%) for specific components, such as the crown or even the implant placement itself.
- Medical vs. Dental Insurance: In certain circumstances, if tooth loss is due to an accident, trauma, or a medical condition (e.g., cancer treatment), your medical insurance might cover a portion of the surgical costs. It's essential to have your dentist or oral surgeon provide a detailed treatment plan and medical necessity letter for submission to your medical insurer.
- ADA Codes: Your dental provider will use specific American Dental Association (ADA) codes when submitting claims. For example, D6010 for surgical placement of implant body, D6057 for implant abutment, and D6058 for implant crown. Check with your insurer about their coverage for these codes.
- Waiting Periods: Be aware that many dental plans have waiting periods (often 6-12 months) for major procedures like implants, meaning you can't get coverage immediately after signing up.
Pro Tip: Always contact your dental and medical insurance providers directly to confirm your specific benefits for dental implants. Request a pre-treatment estimate from your dentist to know exactly what your out-of-pocket costs will be.
Financing and Payment Plans
Even if insurance coverage is limited, several options can help manage the cost:
- Dental Credit Cards (e.g., CareCredit, LendingClub): These specialized healthcare credit cards offer promotional financing options, often with 0% interest for a certain period (e.g., 6, 12, or 18 months), if the balance is paid in full. If not, interest rates can be high.
- In-House Payment Plans: Many dental practices offer their own flexible payment plans, allowing you to pay for your treatment in installments over several months.
- Personal Loans: Banks and credit unions offer personal loans that can cover dental expenses. These typically have fixed interest rates and repayment schedules.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these tax-advantaged accounts to pay for dental implants and associated costs with pre-tax dollars. This can lead to significant savings.
- Medical Tourism (Caution Advised): Some individuals explore traveling to other countries (e.g., Mexico, Costa Rica) for lower implant costs. While prices can be significantly cheaper, it's crucial to thoroughly research the qualifications of the dentists, the quality of materials, and the hygiene standards to avoid potential complications or subpar results. Consider follow-up care challenges.
Cost-Saving Strategies
- Comparison Shopping: Get quotes from several reputable dentists or specialists in your area. Prices can vary significantly for the same procedure.
- Dental Schools: Dental schools often offer treatments at a reduced cost because procedures are performed by students under the supervision of experienced faculty. This can be a more affordable option, though it may take longer.
- Ask About Package Deals: If you need multiple implants or a full arch, some practices offer package pricing that might be more economical than paying for each component separately.
- Negotiate: In some cases, practices may be willing to adjust their fees or offer discounts, especially for uninsured patients paying in cash. It never hurts to ask politely.
Recovery and Aftercare: Ensuring Implant Longevity
The success and longevity of your dental implant largely depend on proper recovery and diligent aftercare. A well-cared-for implant can last for decades, often a lifetime.
Immediate Post-Surgery Care (First Few Days to Weeks)
- Pain Management: Your dentist will likely prescribe pain medication or recommend over-the-counter options like ibuprofen. Swelling and minor discomfort are normal. Apply ice packs to the outside of your face intermittently for the first 24-48 hours.
- Bleeding: Some light bleeding or oozing is normal for the first day. Bite gently on gauze pads if recommended.
- Diet: Stick to soft foods (e.g., soup, yogurt, mashed potatoes, scrambled eggs) for the first few days or weeks. Avoid hard, crunchy, sticky, or hot foods that could irritate the surgical site.
- Oral Hygiene: Be gentle! Avoid brushing directly on the surgical site for the first day. Your dentist may recommend a prescription antimicrobial mouthwash (e.g., chlorhexidine) to keep the area clean. Continue to brush and floss your other teeth normally.
- Activity: Avoid strenuous physical activity for at least 48-72 hours post-surgery to prevent increased bleeding or swelling.
- Smoking/Alcohol: Absolutely avoid smoking and alcohol during the healing period. Smoking significantly impairs healing and increases the risk of implant failure.
- Follow-Up Appointments: Attend all scheduled follow-up appointments so your dentist can monitor healing and remove sutures if necessary.
Osseointegration Period Care (Several Months)
During the several months of osseointegration, continue to:
- Maintain excellent oral hygiene to prevent infection.
- Avoid chewing hard foods on the implant site, especially if a temporary restoration is in place, to allow undisturbed fusion with the bone.
- Refrain from smoking.
Long-Term Maintenance for Implant Longevity
Once your final crown is placed, your implant functions like a natural tooth, but it still requires dedicated care:
- Regular Brushing: Brush your implant and natural teeth at least twice a day with a soft-bristled toothbrush and fluoride toothpaste.
- Flossing/Interdental Cleaning: Floss around your implant daily. Special implant-specific floss, interdental brushes, or water flossers (like Waterpik) can be highly effective in cleaning around the base of the implant and abutment.
- Pro Tip: Unlike natural teeth, implants are not surrounded by a periodontal ligament, making them more susceptible to peri-implantitis (gum disease around an implant) if not cleaned meticulously. Your hygienist can show you specialized techniques.
- Routine Dental Check-ups: Continue to visit your dentist for professional cleanings and check-ups every six months, or as recommended. Your hygienist will use specialized tools designed for implants to avoid scratching the titanium.
- Avoid Biting Hard Objects: Just like natural teeth, implants can be damaged by biting on ice, pens, or hard candies.
- Address Bruxism (Teeth Grinding): If you grind or clench your teeth, your dentist may recommend a nightguard to protect your implant and natural teeth from excessive force.
By adhering to these recovery and aftercare guidelines, you significantly increase the chances of your dental implant being a long-lasting, successful investment in your oral health.
Risks and Potential Complications
While dental implant procedures have a high success rate (generally over 95%), like any surgical procedure, there are potential risks and complications to be aware of:
- Infection at the Implant Site: This is the most common complication. Symptoms include pain, swelling, pus, and fever. Good oral hygiene and antibiotics can help manage or prevent this.
- Nerve Damage: Although rare, nerve damage can occur, especially in the lower jaw. This can lead to numbness, tingling, or pain in the natural teeth, gums, lips, or chin. Often temporary, it can occasionally be permanent. Careful planning with 3D imaging helps mitigate this risk.
- Sinus Problems: For implants placed in the upper jaw, especially near the back, the implant can protrude into one of your sinus cavities. This can lead to sinus inflammation or infection. A sinus lift procedure can prevent this.
- Implant Failure (Lack of Osseointegration): The implant may not properly fuse with the jawbone. This can be due to poor bone quality, infection, excessive pressure on the implant during healing, or certain medical conditions (e.g., uncontrolled diabetes). If an implant fails, it usually needs to be removed, the site allowed to heal, and potentially another implant placed after a period.
- Peri-Implantitis: This is an inflammatory condition affecting the soft tissues and bone surrounding a dental implant, similar to gum disease (periodontitis) in natural teeth. It's often caused by poor oral hygiene and can lead to bone loss around the implant and eventual implant failure if untreated.
- Implant Loosening or Fracture: While rare with modern implants, excessive force, grinding, or trauma can cause the implant, abutment, or crown to loosen or fracture.
- Allergic Reaction: Although titanium is highly biocompatible, rare allergic reactions can occur.
- Healing Complications: Delayed healing, excessive bleeding, or prolonged swelling are possible, though typically manageable.
Your dentist or oral surgeon will thoroughly review these risks with you during your consultation and take all necessary precautions to minimize their occurrence. Following all pre- and post-operative instructions is crucial for a successful outcome.
Alternatives to Dental Implants
While dental implants are often the preferred solution for tooth replacement, they may not be suitable or desired by everyone. Several alternatives exist, each with its own set of pros, cons, and cost implications.
Comparison Table: Implants vs. Bridges vs. Dentures
| Feature | Dental Implants | Traditional Dental Bridge | Partial/Complete Dentures |
|---|---|---|---|
| Cost (Single Tooth/Area) | $3,000 - $6,000+ per tooth | $2,000 - $5,000+ (for 3-unit bridge) | $600 - $2,500+ (partial); $1,500 - $8,000+ (complete) |
| Durability/Lifespan | 20-30+ years, often a lifetime | 5-15 years | 5-10 years (often need relining/replacement) |
| Bone Health | Preserves jawbone density | Does not prevent bone loss under the missing tooth area | Accelerates bone loss due to pressure on gums |
| Impact on Adjacent Teeth | No impact, stands alone | Requires grinding down healthy adjacent teeth | Rests on gums or clasps onto adjacent teeth (can wear them) |
| Functionality/Comfort | Most natural feel, strong chewing ability | Good chewing, can feel somewhat natural | Less stable, reduced chewing power, can slip/cause sores |
| Aesthetics | Excellent, indistinguishable from natural teeth | Good, custom-made to match adjacent teeth | Can look natural, but bulkier, sometimes visible clasps |
| Maintenance | Brush & floss like natural teeth, regular dental visits | Requires special flossing tools under the bridge | Daily removal for cleaning, adhesives often needed |
| Reversibility | Not reversible | Not reversible (teeth are altered) | Removable |
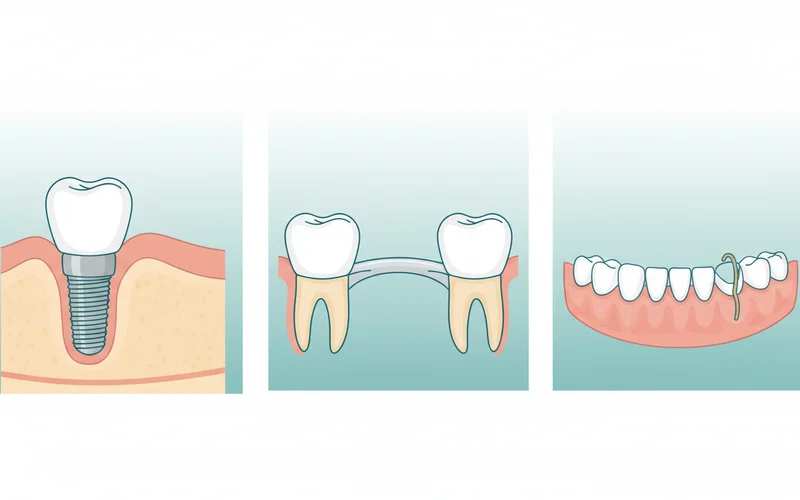
Detailed Look at Alternatives:
-
Traditional Dental Bridge:
- What it is: A fixed prosthesis that replaces one or more missing teeth by being anchored to crowns placed on the natural teeth on either side of the gap.
- Pros: Can be a quicker process than implants, fixed (not removable), good aesthetics.
- Cons: Requires permanent alteration (grinding down) of healthy adjacent teeth. Does not stimulate the jawbone, leading to bone loss in the missing tooth area over time. Requires special cleaning under the bridge.
- Cost: Generally less than implants for a single tooth replacement, but considering the cost of potential future replacements and impact on adjacent teeth, long-term costs can accumulate.
-
Removable Partial Denture:
- What it is: A removable appliance that replaces one or more missing teeth, typically made of an acrylic base and metal clasps that attach to existing teeth.
- Pros: Most affordable initial cost. Non-invasive (no surgery).
- Cons: Removable, can feel bulky and less stable than fixed options. May affect speech and chewing ability. Can put strain on adjacent teeth and accelerate bone loss. Needs daily removal and cleaning.
- Cost: Significantly lower than implants or bridges initially, but may need relining or replacement every 5-10 years, adding to long-term costs.
-
Complete Dentures:
- What it is: A full set of removable teeth for patients who have lost all teeth in an arch.
- Pros: Replaces all teeth, relatively affordable initially.
- Cons: Prone to slipping, can cause sores, significantly reduced chewing efficiency (only 10-20% of natural teeth). Accelerates jawbone resorption, leading to a "sunken" facial appearance over time and needing frequent relining or replacement.
- Cost: Varies widely based on materials and customization, but typically $1,500 - $8,000+ per arch. Implant-supported dentures are a much better option for stability and bone preservation.
When evaluating these options, it's essential to consider not just the upfront cost but also the long-term implications for your oral health, comfort, function, and aesthetics. While the initial investment for dental implants is higher, their longevity and benefits often make them the most cost-effective and beneficial solution in the long run.
Prevention: Protecting Your Oral Health
While dental implants are an excellent solution for tooth loss, the best approach is always prevention. Maintaining good oral health can help you keep your natural teeth for a lifetime and avoid the need for costly restorative procedures.
Here are key preventive measures:
- Practice Excellent Oral Hygiene:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste for at least two minutes, morning and night.
- Floss Daily: Clean between your teeth and under the gumline at least once a day to remove plaque and food particles that your toothbrush can't reach. The American Dental Association (ADA) recommends flossing to prevent gum disease and cavities.
- Use Mouthwash: An antimicrobial or fluoride mouthwash can provide an extra layer of protection, but it's not a substitute for brushing and flossing.
- Regular Dental Check-ups and Professional Cleanings:
- Visit your dentist at least twice a year (every six months) for comprehensive examinations and professional cleanings. These appointments allow your dentist to identify and address issues like cavities, gum disease, or other problems early before they become severe and require extensive treatment.
- Maintain a Balanced Diet:
- Limit sugary foods and drinks, as sugar feeds the bacteria that cause tooth decay.
- Eat plenty of fruits, vegetables, and whole grains, which provide essential vitamins and minerals for healthy teeth and gums.
- Ensure adequate calcium and Vitamin D intake for strong bones, including your jawbone.
- Avoid Tobacco Products:
- Smoking and chewing tobacco are major risk factors for gum disease, oral cancer, and tooth loss. They also significantly impair healing and success rates of dental implants.
- Limit Alcohol Consumption:
- Excessive alcohol intake can contribute to dry mouth, increasing the risk of cavities and gum disease.
- Protect Your Teeth from Trauma:
- Wear a mouthguard during sports or any activity with a risk of facial impact.
- If you grind or clench your teeth (bruxism), talk to your dentist about a custom nightguard to protect your teeth from excessive wear and potential fractures.
- Address Dental Issues Promptly:
- Don't ignore tooth sensitivity, persistent bad breath, bleeding gums, or any oral pain. Early intervention can prevent minor issues from becoming major problems requiring tooth extraction.
By committing to these preventive strategies, you significantly reduce your risk of tooth loss and the subsequent need for dental implants, preserving your natural smile and saving on future dental expenses.
Children and Adolescents: When Implants Aren't an Option (Yet)
Dental implants are an excellent long-term solution for missing teeth in adults, but they are generally not recommended for children and adolescents. The primary reason for this is that the jawbones of young individuals are still developing and growing.
- Growth Plate Considerations: The jawbone, like other bones in the body, contains growth plates that continue to expand and change shape until early adulthood. Placing a dental implant in a growing jaw can interfere with natural bone development, leading to the implant becoming misaligned or "submerged" as the surrounding bone continues to grow. This can cause significant aesthetic and functional problems later on.
- Age Guidelines: Most dental professionals recommend waiting until the jawbone has fully matured, which typically occurs around 18-20 years of age for females and 20-25 years for males. A dental evaluation, including X-rays, can help determine if bone growth is complete.
Temporary Solutions for Children and Adolescents
If a child or teenager loses a permanent tooth due to trauma, decay, or a congenital condition, several temporary solutions can be considered until they are old enough for an implant:
- Space Maintainers: For very young children who lose a baby tooth prematurely, a space maintainer can prevent adjacent teeth from shifting into the gap, preserving space for the permanent tooth to erupt.
- Removable Partial Dentures (Flippers): These are temporary, lightweight, removable appliances that have a false tooth attached. They are primarily used for aesthetic purposes and to hold space. They are not designed for heavy chewing.
- Bonded Bridges (Maryland Bridges): For older adolescents, a bonded bridge can be a temporary solution. It involves a false tooth with metal or composite "wings" that are bonded to the back of adjacent natural teeth. This is less invasive than a traditional bridge as it doesn't require grinding down healthy teeth.
- Orthodontic Treatment: In some cases, orthodontics can be used to close the gap created by a missing tooth or to prepare the space for a future implant.
These temporary measures help maintain aesthetics, preserve chewing function, and most importantly, hold the space until the child's jaw is fully developed and ready for a permanent dental implant. Regular consultation with a pediatric dentist or orthodontist is essential to manage these cases appropriately.
Frequently Asked Questions
How painful is a dental implant procedure?
Most patients report that the dental implant procedure itself is less painful than expected. It's typically performed under local anesthesia, so you won't feel pain during the surgery. Post-surgery, you might experience discomfort, swelling, and bruising, which can be managed with prescribed pain medication and over-the-counter anti-inflammatories. Most people return to normal activities within a few days.
How long does a dental implant last?
With proper oral hygiene and regular dental check-ups, a dental implant can last for 20-30 years or even a lifetime. The implant post itself is incredibly durable. The crown attached to the implant may need to be replaced after 10-15 years due to wear and tear, similar to a natural tooth crown.
Is a dental implant worth the cost?
For many, the long-term benefits of a dental implant – including superior aesthetics, natural function, preservation of jawbone, and no impact on adjacent teeth – make it a highly worthwhile investment despite the upfront cost. When compared to the recurring costs and potential compromises of bridges or dentures over decades, implants often prove to be more cost-effective in the long run and provide a significantly higher quality of life.
Can anyone get a dental implant?
Not everyone is an ideal candidate for dental implants. Good candidates typically have sufficient healthy jawbone to support the implant, healthy gum tissue, and good overall health. Conditions like uncontrolled diabetes, severe gum disease, heavy smoking, or certain medical treatments (e.g., radiation to the head/neck) can affect implant success. A thorough dental and medical evaluation by your dentist is essential.
What is the success rate of dental implants?
Dental implants boast an impressive success rate, generally ranging from 95% to 98%, depending on the location of the implant and individual patient factors. Success rates are slightly lower for implants placed in the posterior (back) of the upper jaw due to bone density variations. Following pre- and post-operative instructions is crucial for maximizing success.
How long does the entire implant process take?
The full dental implant process, from initial consultation to the final placement of the crown, typically takes 3 to 9 months. This timeline includes any necessary preparatory procedures (like bone grafting, which can add several months) and the critical 3-6 month period for osseointegration (when the implant fuses with the jawbone).
Are dental implants covered by Medicare?
Generally, no, Medicare does not cover dental implants. Original Medicare (Part A and Part B) does not cover routine dental care, including most dental procedures like fillings, extractions, and dentures. Some Medicare Advantage (Part C) plans may offer limited dental benefits, but comprehensive implant coverage is rare. It's best to check with your specific plan provider.
What are the risks of getting a dental implant?
While highly successful, risks include infection at the implant site, nerve damage (leading to numbness or pain), sinus problems (for upper jaw implants), and peri-implantitis (inflammation around the implant). In rare cases, the implant may fail to integrate with the bone. Your dental professional will discuss these risks and how they are minimized during your consultation.
When to See a Dentist
Prompt action regarding your oral health can save you discomfort, complications, and significant expense in the long run.
See a dentist for evaluation as soon as possible if:
- You have a missing tooth or teeth: Even if it's in the back of your mouth, a missing tooth can lead to shifting of adjacent teeth, bone loss, and changes in your bite. Early intervention can simplify treatment.
- You're considering tooth replacement options: If you have an existing bridge or denture that is uncomfortable, failing, or you're simply curious about permanent solutions, schedule a consultation to discuss all options, including dental implants.
- You experience any of the following around an existing implant:
- Persistent pain or tenderness: While some initial discomfort after surgery is normal, ongoing or worsening pain is a red flag.
- Swelling or redness around the implant site: These can indicate infection or inflammation (peri-implantitis).
- Pus or discharge: Any fluid drainage from around the implant is a sign of infection.
- The implant feels loose: A healthy implant should be firmly integrated with your bone. Any movement or wobbling requires immediate attention.
- Difficulty chewing or biting with the implant: This could indicate an issue with the crown, abutment, or the implant itself.
For routine care and preventive guidance:
- Schedule regular dental check-ups and cleanings every six months, or as recommended by your dentist. This is crucial for maintaining overall oral health and ensuring the longevity of any dental work, including implants.
Don't wait until a small problem becomes a major emergency. Your dental health impacts your overall well-being, and a proactive approach is always the best strategy.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026