Innovative Implant and Oral Surgery: Complete Guide
Key Takeaways
- For many Americans, the dream of a fully functional, healthy smile can be challenged by tooth loss, severe dental trauma, or complex oral health issues. Fortunately, the landscape of modern dentistry is continually evolving, offering advanced solutions that were once considered futuristic. Today, **
For many Americans, the dream of a fully functional, healthy smile can be challenged by tooth loss, severe dental trauma, or complex oral health issues. Fortunately, the landscape of modern dentistry is continually evolving, offering advanced solutions that were once considered futuristic. Today, innovative implant and oral surgery stands at the forefront of restorative and reconstructive dentistry, providing patients with opportunities to regain not just their smile, but also their confidence, chewing ability, and overall quality of life. From sophisticated dental implants that mimic natural teeth to intricate surgical procedures that rebuild bone and soft tissue, these advancements are revolutionizing how we address even the most complex dental challenges.
This comprehensive guide from SmilePedia.net will delve deep into the world of advanced dental implants and oral surgery, exploring the cutting-edge techniques, materials, and technologies that are transforming dental care. We'll cover everything from the fundamental principles to the latest innovations like the concept of a diamond tooth implant and the practical considerations of implant supported dentures cost. Whether you're researching solutions for missing teeth, considering complex oral reconstruction, or simply want to understand the possibilities of modern dentistry, this article will equip you with the knowledge to make informed decisions about your oral health journey.
Key Takeaways:
- Innovative implant and oral surgery offers advanced solutions for tooth loss, jawbone deficiencies, and complex oral health issues, leveraging digital planning and biomaterials.
- Dental implants, including traditional, mini, and zygomatic types, boast a 95-98% success rate and can last 20+ years with proper care.
- Implant supported dentures cost typically ranges from $12,000 to $25,000 per arch for a fixed solution, varying by location, materials, and number of implants.
- Advanced procedures like bone grafting, sinus lifts, and immediate load implants can significantly reduce treatment timelines and improve outcomes.
- The concept of a diamond tooth implant refers to innovative materials or aesthetic enhancements, potentially increasing costs by 10-20% above standard ceramic or zirconia.
- Comprehensive treatment plans often span 3-9 months, including healing periods, with immediate load options potentially completing in a single visit for suitable candidates.
- Insurance coverage for implants is limited, typically covering 0-15% of the cost, making financing plans and dental savings clubs important considerations.
What It Is / Overview: The Revolution in Restorative Dentistry
Innovative implant and oral surgery encompasses a broad spectrum of advanced dental procedures focused on restoring form, function, and aesthetics to the mouth and jaw. At its core, it involves the surgical placement of dental implants and other specialized procedures to address issues ranging from single tooth loss to complete oral rehabilitation. These aren't just standard extractions or fillings; they are precision-driven treatments often utilizing state-of-the-art technology like 3D imaging, computer-guided surgery, and advanced biomaterials.
The "innovative" aspect refers to the continuous evolution in techniques, materials, and digital workflows that enhance predictability, reduce recovery times, and improve long-term outcomes. This includes:
- Minimally Invasive Techniques: Utilizing smaller incisions, guided surgery, and advanced imaging to reduce trauma and speed healing.
- Biocompatible Materials: Employment of highly compatible materials like titanium, zirconia, and advanced ceramics that integrate seamlessly with the body.
- Digital Workflow: From initial diagnosis with cone-beam computed tomography (CBCT) to digital impression-taking and CAD/CAM (computer-aided design/computer-aided manufacturing) fabrication of prosthetics, digital dentistry enhances precision and efficiency.
- Advanced Bone Augmentation: Techniques like bone grafting (using synthetic, animal, or patient's own bone) and sinus lifts to create sufficient bone volume where it's lacking for implant placement.
- Immediate Load Implants: In suitable cases, placing the implant and attaching a temporary crown or bridge in a single appointment.
Oral surgery, a specialized field, extends beyond implants to include wisdom tooth extractions, corrective jaw surgery (orthognathic surgery), treatment of temporomandibular joint (TMJ) disorders, management of oral pathology (cysts, tumors), and complex trauma repair. When combined with innovative implant techniques, these procedures offer comprehensive solutions for even the most challenging cases.
Types / Variations of Innovative Implants and Oral Surgical Procedures
The field of innovative implant and oral surgery offers a diverse array of options tailored to individual needs and anatomical considerations.
Dental Implants: Beyond the Basics
Dental implants are titanium or zirconia posts surgically placed into the jawbone to serve as stable anchors for artificial teeth. The innovation lies in the planning, materials, and application:
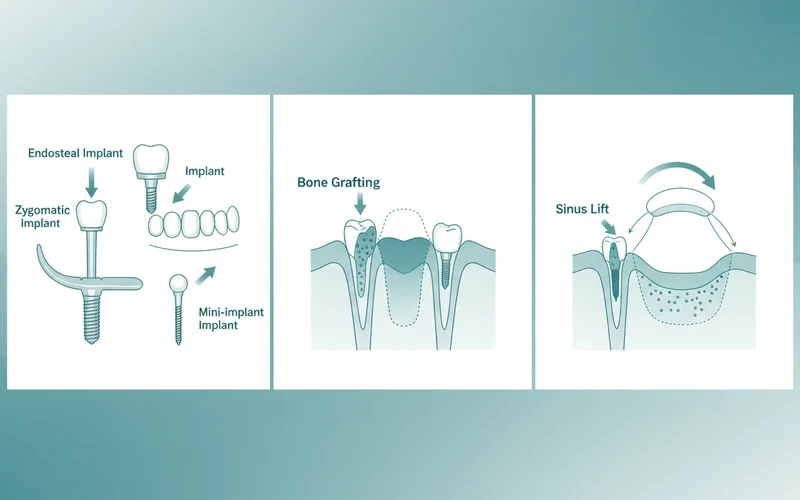
- Endosteal Implants: The most common type, these are surgically placed directly into the jawbone. Innovations include tapered designs for better primary stability, surface treatments that enhance osseointegration (bone fusion), and narrow-diameter implants for areas with limited bone width.
- Subperiosteal Implants: Once common but now rare, these fit on top of the jawbone but under the gum tissue. Modern advancements have largely superseded this type, but it might be considered in extreme cases of bone loss.
- Zygomatic Implants: A highly specialized solution for patients with severe upper jawbone loss, where traditional implants aren't feasible without extensive bone grafting. These longer implants anchor into the zygoma (cheekbone), often allowing for immediate provisional restorations.
- All-on-4® / All-on-6® Concepts: Revolutionary techniques where a full arch of teeth is supported by just four or six strategically placed implants, often with angled posterior implants to maximize bone contact and avoid anatomical structures. This frequently allows for immediate provisional restorations.
- Mini Dental Implants (MDIs): Smaller in diameter (less than 3mm) than traditional implants, MDIs are less invasive, often used for stabilizing dentures, especially in the lower jaw, or for temporary orthodontic anchorage. They are more affordable but have specific indications.
- Ceramic (Zirconia) Implants: A metal-free alternative for patients with metal sensitivities or those preferring a holistic approach. Zirconia offers excellent biocompatibility and aesthetics, though long-term data is still accumulating compared to titanium.
Advanced Oral Surgical Procedures
Innovative oral surgery often prepares the mouth for implants or addresses other complex issues:
- Bone Grafting: When there isn't enough jawbone to support an implant, bone grafting augments the bone volume.
- Autogenous Grafts: Bone harvested from the patient's own body (e.g., hip, tibia, or intraoral sites) is considered the gold standard due to superior integration.
- Allografts: Bone derived from a human donor (cadaver bone), processed to ensure safety.
- Xenografts: Bone derived from an animal source, typically bovine (cow) bone.
- Alloplasts: Synthetic bone graft materials, often made from calcium phosphate ceramics.
- Sinus Lift (Sinus Augmentation): A specific type of bone grafting procedure for the upper jaw when the maxillary sinuses are too close to the implant site. The sinus membrane is gently lifted, and bone graft material is placed to create sufficient height for implants.
- Ridge Augmentation: Used to restore the natural contour of the jawbone when it has receded due to tooth loss, trauma, or gum disease. This involves placing bone graft material to widen or heighten the ridge.
- Soft Tissue Grafting: Procedures to address gum recession around teeth or implants, improving aesthetics and preventing further bone loss. This can involve grafting tissue from other areas of the mouth.
- Piezosurgery: A minimally invasive surgical technique using ultrasonic micro-vibrations to cut bone without damaging soft tissues. This precision reduces patient discomfort and speeds healing, especially beneficial for delicate procedures like sinus lifts or bone harvesting.
- PRP/PRF (Platelet-Rich Plasma/Fibrin): Derived from the patient's own blood, these concentrated growth factors are used to enhance healing and regeneration after surgery, often mixed with bone grafts or applied directly to surgical sites.
Diamond Tooth Implant: A Glimpse into the Future
The term "diamond tooth implant" isn't currently a standard medical classification for a type of implant material. Instead, it typically refers to one of two concepts:
- Aesthetic Enhancement: Crowns or veneers that incorporate actual diamonds or diamond-like crystals for purely aesthetic, luxury purposes. These are custom-fabricated prosthetics that are attached to standard dental implants. The "diamond" refers to the aesthetic material on the crown, not the implant post itself.
- Advanced Material Science: Speculation or emerging research into ultra-hard, durable, and highly biocompatible materials that mimic the properties of diamond, or coatings that enhance the performance of existing implant materials. While not yet mainstream, research explores diamond-like carbon (DLC) coatings for improved wear resistance and biocompatibility in medical devices.
If considering aesthetic diamond enhancements, it's important to understand this is an added cosmetic feature to the crown, not inherent to the implant's function. For material advancements, ongoing research may eventually lead to implant components with "diamond-like" properties, but they are not yet widely available as a distinct "diamond tooth implant" category in clinical practice.
Causes / Why Innovative Implant and Oral Surgery is Needed
The need for innovative implant and oral surgery stems from various complex oral health issues, often resulting in tooth loss or significant structural damage:
- Tooth Loss: The most common reason. This can be due to:
- Severe Decay: Untreated cavities that destroy too much tooth structure to save.
- Periodontal Disease (Gum Disease): Advanced stages can lead to the destruction of supporting bone and ligaments, causing teeth to loosen and fall out. This is a leading cause of tooth loss in adults.
- Trauma: Accidents, sports injuries, or falls that knock out teeth or cause irreparable damage.
- Failed Root Canal Treatment or Fractured Teeth: When previous treatments fail or teeth crack beyond repair.
- Congenital Absence: Some individuals are born without certain teeth (hypodontia).
- Insufficient Jawbone Volume: A common challenge for implant placement.
- Long-term Tooth Loss: When a tooth is lost, the jawbone in that area no longer receives stimulation from chewing, leading to bone resorption (shrinkage). This can make implant placement impossible without bone grafting.
- Gum Disease: Can also destroy bone surrounding teeth.
- Trauma or Infection: Can result in significant bone loss.
- Complex Anatomical Challenges:
- Sinus Proximity: In the upper jaw, the maxillary sinuses can expand after tooth loss, leaving insufficient bone height for implants.
- Nerve Proximity: In the lower jaw, the inferior alveolar nerve must be avoided during implant placement.
- Impacted Teeth: Most commonly wisdom teeth, which can cause pain, infection, damage to adjacent teeth, or orthodontic issues if they don't erupt properly.
- Jaw Misalignment (Malocclusion): Severe cases may require orthognathic surgery to correct functional and aesthetic issues.
- Oral Pathology: Cysts, tumors, or lesions in the mouth and jaw that require surgical removal and sometimes reconstruction.
Signs and Symptoms Indicating a Need for Oral Surgical Intervention
While regular dental check-ups are crucial for early detection, certain signs and symptoms may indicate a need to consult with an oral surgeon or a dentist experienced in implantology:
- Missing Teeth: Obvious gaps in your smile, difficulty chewing, or changes in speech.
- Loose or Shifting Teeth: A clear sign of advanced gum disease or severe bone loss.
- Persistent Toothache or Sensitivity: Especially if accompanied by swelling, fever, or difficulty opening your mouth, which could indicate a severe infection requiring extraction or other surgical intervention.
- Pain or Tenderness in the Jaw: Can indicate TMJ issues, impacted teeth, or nerve problems.
- Difficulty Chewing or Biting: If chewing is painful or impossible, it suggests underlying dental issues.
- Chronic Facial Pain or Headaches: Can sometimes be linked to TMJ disorders or impacted teeth.
- Swelling in the Jaw or Face: A critical sign of infection that requires immediate attention.
- Clicking or Popping Sounds in the Jaw Joint: Suggestive of TMJ dysfunction.
- Lesions or Lumps in the Mouth: Any persistent sores, red or white patches, or growths should be examined by a dentist immediately as they could indicate oral cancer.
- Dentures that are Loose or Uncomfortable: If your existing dentures constantly slip, cause sores, or make chewing difficult, implant-supported dentures might be a suitable solution.
Treatment Options: A Spectrum of Advanced Solutions
The choice of treatment depends heavily on the specific condition, patient health, and desired outcomes. An oral surgeon or periodontist will conduct a thorough evaluation, often involving CBCT scans and digital planning, to determine the most appropriate approach.
For Missing Teeth
- Single Dental Implants: The gold standard for replacing a single missing tooth, providing a standalone restoration without affecting adjacent teeth.
- Pros: Highly durable, feels and functions like a natural tooth, preserves jawbone, excellent aesthetics.
- Cons: Higher initial cost than bridges, requires surgery, longer treatment time (healing).
- Implant-Supported Bridges: Used to replace several missing teeth in a row. Instead of supporting a bridge on natural teeth, it's anchored by two or more implants.
- Pros: More stable than traditional bridges, preserves bone, avoids stressing natural teeth.
- Cons: Requires multiple implants and surgery, higher cost than traditional bridges.
- Implant-Supported Dentures (Fixed or Removable): A revolutionary option for people with multiple missing teeth or those wearing traditional dentures.
- Removable (Overdentures): Snapped onto a few implants (typically 2-4 in the lower jaw, 4-6 in the upper) for vastly improved stability compared to conventional dentures. Patients can remove them for cleaning.
- Pros: Improved stability and chewing efficiency, reduced bulk compared to traditional dentures, more affordable than fixed options.
- Cons: Still removable, may have some movement.
- Fixed (Hybrid Dentures / All-on-X): Permanently attached to a greater number of implants (e.g., All-on-4, All-on-6), only removable by a dentist. These feel and function much more like natural teeth.
- Pros: Superior stability and chewing power, non-removable, preserves bone, excellent aesthetics.
- Cons: Higher cost, requires more implants and extensive surgery.
- Removable (Overdentures): Snapped onto a few implants (typically 2-4 in the lower jaw, 4-6 in the upper) for vastly improved stability compared to conventional dentures. Patients can remove them for cleaning.
For Jawbone Deficiencies
- Bone Grafting: Essential for preparing the jaw for implants.
- Pros: Creates necessary bone volume, improves implant success rates.
- Cons: Adds to treatment time (healing typically 3-9 months), additional surgical procedure, potential for discomfort.
- Sinus Lift: Specifically for upper back jaw deficiencies.
- Pros: Allows implant placement where it otherwise wouldn't be possible, good success rates.
- Cons: Technically complex, longer healing time, risk of sinus membrane perforation.
For Other Oral Surgical Needs
- Wisdom Tooth Extraction: Common procedure to remove impacted or problematic wisdom teeth.
- Pros: Relieves pain, prevents infection, prevents damage to adjacent teeth.
- Cons: Swelling, discomfort, potential for dry socket or nerve damage (rare).
- Corrective Jaw Surgery (Orthognathic Surgery): Addresses severe malocclusions, facial imbalances, or sleep apnea.
- Pros: Significant functional and aesthetic improvements, resolves severe bite issues.
- Cons: Major surgery, long recovery, typically involves orthodontics before and after.
- Biopsy and Excision of Oral Lesions: Removal and analysis of suspicious tissues.
- Pros: Diagnostic and curative for oral pathology, early detection of oral cancer.
- Cons: Surgical discomfort, potential for scarring depending on location and size.
Comparison Table: Implant-Supported Prostheses
| Feature | Single Dental Implant | Implant-Supported Bridge | Implant-Supported Denture (Removable) | Implant-Supported Denture (Fixed - e.g., All-on-4) |
|---|---|---|---|---|
| Replaces | 1 missing tooth | 2-4 missing teeth in a row | Full arch of missing teeth (top or bottom) | Full arch of missing teeth (top or bottom) |
| Number of Implants | 1 | 2-3 | 2-6 (typically 2-4 for lower, 4-6 for upper) | 4-6 |
| Removable by Patient | No | No | Yes (snaps in and out) | No (only by dentist) |
| Stability/Feel | Most like a natural tooth | Very stable, excellent function | Significantly more stable than traditional dentures | Most stable, feels very close to natural teeth |
| Bone Preservation | Excellent, stimulates bone at site | Very good, stimulates bone at implant sites | Good, stimulates bone at implant sites | Excellent, stimulates bone at implant sites |
| Estimated Cost | $3,000 - $6,000 (per tooth) | $6,000 - $15,000+ (per bridge) | $6,000 - $18,000 (per arch, including implants & denture) | $12,000 - $25,000+ (per arch, including implants & bridge) |
| Typical Timeline | 3-9 months | 4-10 months | 3-9 months | 3-12 months (often with immediate provisional) |
Step-by-Step Process: What to Expect During Treatment
While each patient's journey is unique, a general roadmap for innovative implant and oral surgery often follows these stages:
-
Initial Consultation & Diagnosis (1-2 visits):
- Comprehensive Examination: The oral surgeon or periodontist will review your medical history, perform an oral examination, and discuss your goals.
- Advanced Imaging: A crucial step involves taking CBCT (cone-beam computed tomography) scans. This 3D imaging provides incredibly detailed views of your jawbone, nerve pathways, and sinus cavities, allowing for precise treatment planning and identification of potential issues. Digital intraoral scans may also be taken.
- Treatment Plan Development: Based on the diagnosis, a customized treatment plan is created. This plan will outline the specific procedures, number and type of implants, need for bone grafting, estimated timeline, and detailed cost breakdown. Pro Tip: Don't hesitate to ask questions about every aspect of your proposed treatment.
-
Preparatory Procedures (If needed, 1-2 visits, plus healing time):
- Tooth Extractions: Any remaining unsalvageable teeth in the area will be gently extracted.
- Bone Grafting/Sinus Lift: If there isn't enough bone, these procedures will be performed. This often requires a significant healing period (typically 3-9 months) before implants can be placed, allowing the bone to fully integrate and mature.
-
Implant Placement (1 surgical visit):
- Anesthesia: Local anesthesia is always used, and often combined with sedation (oral, IV, or nitrous oxide) to ensure comfort and anxiety relief.
- Surgical Incision: A small incision is made in the gum tissue to expose the jawbone.
- Osteotomy (Bone Preparation): Using precise drills, a small channel (osteotomy) is carefully created in the bone at the exact location determined by the digital plan. Computer-guided surgery often uses a custom surgical guide to ensure unparalleled accuracy.
- Implant Insertion: The titanium or zirconia implant post is gently screwed into the prepared site.
- Suture: The gum tissue is closed over the implant (submerged technique) or a healing abutment is placed, allowing the top of the implant to be exposed (non-submerged technique).
- Post-Operative Instructions: Detailed instructions for pain management, diet, and oral hygiene are provided.
-
Osseointegration (Healing Period, 3-6 months):
- This is the critical phase where the implant physically fuses with your jawbone. It's a natural biological process that creates a strong, stable anchor. During this time, you may wear a temporary denture or bridge. Pro Tip: Adhere strictly to your dentist's post-operative instructions to ensure optimal healing and successful osseointegration.
-
Abutment Placement (1 visit, optional if healing abutment was used):
- Once osseointegration is complete, a small connector piece called an abutment is attached to the implant. This piece extends through the gum line and serves as the base for your new crown, bridge, or denture. If a healing abutment was already in place, this step may be minimal or unnecessary.
-
Prosthetic Restoration (2-3 visits):
- Impressions: Digital or traditional impressions are taken of your mouth and the abutment.
- Custom Fabrication: A dental lab meticulously crafts your custom crown, bridge, or denture, matching the shape, size, and color of your natural teeth. For diamond tooth implants (aesthetic enhancements), this is where those elements would be incorporated into the crown.
- Final Placement: Once fabricated, your new restoration is cemented or screwed onto the abutment, completing your smile. Adjustments are made to ensure a perfect fit and comfortable bite.
Cost and Insurance: Understanding the Investment in Your Smile
The cost of innovative implant and oral surgery varies significantly based on several factors, including the type and number of implants, the complexity of the surgical procedures (e.g., bone grafting, sinus lifts), the materials used for the prosthetic (crown, bridge, denture), the geographic location of the practice, and the experience of the dental professional.
Average US Cost Ranges (Out-of-Pocket, without insurance)
These are general ranges, and a detailed quote from your provider is essential.
- Single Dental Implant (Implant, Abutment, Crown): $3,000 - $6,000
- Lower Cost Areas: $2,500
- Higher Cost Areas (e.g., major metropolitan areas): $7,000+
- Bone Grafting (per site): $300 - $2,500 (depending on material and volume needed)
- Sinus Lift (per side): $1,500 - $3,500
- Implant Supported Denture (Removable, per arch, 2-4 implants): $6,000 - $18,000
- Implant Supported Denture (Fixed, e.g., All-on-4, per arch): $12,000 - $25,000
- Full Mouth Restoration (Upper & Lower All-on-4/6): $25,000 - $60,000+
- Wisdom Tooth Extraction (per tooth):
- Simple: $75 - $200
- Impacted (Surgical): $200 - $600
- With Sedation: Add $300 - $1,000+
- Diamond Tooth Implant (Aesthetic Crown Overlay): This is an added cosmetic expense on top of the standard implant and crown cost, potentially increasing the total by $500 - $2,000+ per tooth, depending on the size and quality of the diamonds/materials.
Geographic Cost Variation
Costs tend to be higher in urban areas and on the coasts (e.g., New York, California) compared to rural areas or the Midwest. For example, a single implant might cost $4,500-$6,500 in NYC, while the same procedure might be $3,500-$5,000 in Kansas City.
Insurance Coverage
Unfortunately, dental insurance coverage for implants and advanced oral surgery is often limited.
- Many traditional dental insurance plans classify implants as a "major procedure" and may cover only a small percentage (e.g., 0-15%) of the cost, or exclude them entirely.
- Some plans may cover the extraction and bone grafting procedures, but not the implant itself or the prosthetic crown.
- Medically Necessary Clause: If the oral surgery is deemed medically necessary (e.g., removal of a tumor, severe trauma reconstruction), a portion might be covered by your medical insurance, not dental. This requires thorough documentation from your surgeon.
- Max Annual Benefit: Most dental plans have an annual maximum benefit, typically $1,000 - $2,500, which is often quickly exhausted by complex procedures.
Payment Plans and Financing Options
Because of the significant investment, many practices offer:
- In-house Payment Plans: Monthly installments directly with the dental office.
- Third-Party Financing: Companies like CareCredit or LendingClub provide healthcare-specific credit lines with various interest rates and repayment terms, often with promotional periods of 0% APR.
- Dental Savings Plans: These are not insurance but membership programs where you pay an annual fee for discounted rates on dental procedures. Discounts can range from 10-60%.
Pro Tip: Always get a detailed written estimate outlining all costs before beginning treatment. Ask about payment options and verify your insurance coverage directly with your provider and your dental office's billing specialist.
Recovery and Aftercare: Ensuring Long-Term Success
Proper recovery and diligent aftercare are paramount for the long-term success of innovative implant and oral surgery.
Immediate Post-Operative Care (First 24-72 hours):
- Bleeding Control: Bite firmly on gauze packs for 30-60 minutes, replacing as needed. A small amount of oozing is normal.
- Swelling Reduction: Apply ice packs to the outside of your face for 20 minutes on, 20 minutes off, for the first 24-48 hours.
- Pain Management: Take prescribed pain medication as directed. Over-the-counter anti-inflammatories (like ibuprofen) can also be very effective.
- Diet: Stick to soft, cool foods and liquids for the first few days (e.g., yogurt, smoothies, mashed potatoes, soup). Avoid hot foods, spicy foods, alcohol, and carbonated beverages.
- Oral Hygiene: Do NOT rinse vigorously or spit for the first 24 hours to avoid dislodging the blood clot. After 24 hours, gentle salt water rinses (1/2 tsp salt in 8 oz warm water) 2-3 times a day can help keep the area clean. Avoid brushing the surgical site directly for the first few days.
- Rest: Elevate your head with pillows when lying down. Avoid strenuous activity for at least 48-72 hours.
- Smoking/Vaping: Absolutely avoid smoking or vaping, as it severely impairs healing and dramatically increases the risk of complications like dry socket and implant failure.
During the Healing Period (Weeks to Months):
- Follow Diet Restrictions: Depending on the procedure (e.g., bone graft, immediate load implant), you may have specific dietary restrictions for several weeks or months to protect the surgical site.
- Medication Adherence: Continue antibiotics if prescribed, completing the full course.
- Oral Hygiene: Maintain excellent oral hygiene, brushing and flossing other areas normally. Gently clean around the surgical site as instructed by your surgeon.
- Regular Check-ups: Attend all scheduled follow-up appointments with your oral surgeon to monitor healing.
- Protect Temporary Restorations: If you have a temporary crown, bridge, or denture, treat it gently. Avoid sticky or hard foods that could dislodge it.
Long-Term Aftercare (For Implants):
- Excellent Oral Hygiene: Brush twice daily and floss daily. Consider using an interdental brush or water flosser specifically designed for implant care.
- Regular Dental Check-ups & Cleanings: Visit your general dentist and hygienist at least twice a year. They will monitor your implant's health and provide specialized cleaning.
- Avoid Damaging Habits: Refrain from biting on hard objects (ice, hard candy), grinding your teeth (consider a nightguard), or using your teeth as tools.
- Address Issues Promptly: If you notice any pain, swelling, loosening of the crown/abutment, or changes around the implant, contact your dentist immediately.
Pro Tip: The ADA recommends regular dental check-ups and thorough daily oral hygiene for maintaining the longevity of dental implants, just as you would for natural teeth.
Prevention: Minimizing the Need for Future Oral Surgery
While some needs for oral surgery are unavoidable (e.g., congenital conditions, accidents), many can be prevented or mitigated through proactive measures:
- Excellent Oral Hygiene: The foundation of all dental health. Brush twice daily with fluoride toothpaste and floss daily to remove plaque and food debris, preventing decay and gum disease.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleaning and examination. Early detection of issues like cavities, gum disease, or wisdom tooth problems can prevent them from escalating to require surgery.
- Balanced Diet: Limit sugary and acidic foods and drinks, which contribute to tooth decay. Consume a diet rich in fruits, vegetables, and calcium for strong teeth and bones.
- Protect Your Teeth:
- Mouthguards: Wear a custom-fitted mouthguard during sports to prevent dental trauma.
- Nightguards: If you grind or clench your teeth (bruxism), a nightguard can protect your teeth from excessive wear and potential fractures.
- Quit Smoking/Vaping: Tobacco use is a major risk factor for gum disease, oral cancer, and implant failure. Quitting significantly improves your oral and overall health.
- Address Dental Problems Promptly: Don't ignore persistent toothaches, bleeding gums, or sensitivity. Early intervention for issues like small cavities or early gum disease can prevent them from progressing to tooth loss or the need for extensive surgery.
- Manage Systemic Diseases: Conditions like diabetes can impact oral health. Work with your physician to manage any chronic health conditions.
Risks and Complications: What Can Go Wrong
While innovative implant and oral surgery has high success rates, no surgical procedure is entirely without risk. It's crucial to be aware of potential complications:
- General Surgical Risks:
- Infection: Though antibiotics are often prescribed, infection can occur at the surgical site.
- Bleeding: Some bleeding is normal, but excessive or prolonged bleeding can be a complication.
- Swelling and Bruising: Common post-surgery, but severe or persistent swelling should be reported.
- Pain: Managed with medication, but persistent or worsening pain is a concern.
- Allergic Reaction: To anesthesia, medications, or implant materials (rare).
- Implant-Specific Complications:
- Implant Failure: The implant may not properly integrate with the bone (osseointegration failure) or may fail later due to infection, excessive force, or poor hygiene. Rates are generally low (2-5%).
- Nerve Damage: Rare but possible, particularly in the lower jaw, leading to numbness, tingling, or pain in the lip, chin, or tongue. This can be temporary or, in very rare cases, permanent. Precise planning with CBCT scans minimizes this risk.
- Sinus Perforation: During upper jaw implant placement or sinus lift, the sinus membrane can be torn. Usually repairable, but may require delaying implant placement.
- Peri-implantitis: An inflammatory condition affecting the tissues surrounding a dental implant, similar to gum disease around natural teeth, potentially leading to bone loss and implant failure. Often linked to poor hygiene or smoking.
- Implant Overload: Placing too much force on the implant too soon (e.g., immediate loading without adequate bone density) can lead to failure.
- Bone Grafting/Sinus Lift Complications:
- Graft Failure: The bone graft material may not integrate properly.
- Sinus Infection (Sinusitis): A risk following sinus lift procedures.
- Wisdom Tooth Extraction Complications:
- Dry Socket (Alveolar Osteitis): When the blood clot at the extraction site dislodges prematurely, exposing the bone. This causes intense pain and delays healing.
- Damage to Adjacent Teeth or Fillings: Though rare.
- Nerve Damage: Similar to implant placement, though usually temporary.
Your oral surgeon will discuss all relevant risks specific to your chosen procedure and take every precaution to minimize complications. Following all pre- and post-operative instructions is vital for a successful outcome.
Children / Pediatric Considerations
While dental implants are generally not recommended for children or adolescents because their jawbones are still developing, oral surgery does play a significant role in pediatric dental care.
Common oral surgical procedures for children include:
- Extractions: Removing severely decayed or damaged primary (baby) teeth, or permanent teeth that are impacted or crowding the mouth.
- Frenectomy: A simple procedure to release a tight frenum (the tissue connecting the lip to the gum or the tongue to the floor of the mouth), which can cause speech impediments (tongue-tie) or gum recession.
- Exposure of Impacted Canines: Sometimes, an unerupted permanent canine tooth may be impacted. An oral surgeon can expose the tooth, allowing an orthodontist to guide it into proper position with braces.
- Removal of Cysts or Lesions: Similar to adults, children can develop cysts or benign lesions in the mouth or jaw that require surgical removal.
- Trauma Management: Oral surgeons are often involved in treating facial and dental injuries in children resulting from accidents.
For growing children, the emphasis is on preserving existing teeth, guiding proper jaw development, and addressing issues that could impact permanent dentition. Implants are typically only considered after facial growth is complete, usually in the late teens or early twenties, to ensure the implant remains stable relative to the surrounding dentition. Any surgical intervention in children requires careful consideration of their growth plates and emotional well-being.
Cost Breakdown: Detailed Insights
To provide a clearer picture of the financial commitment, let's break down costs further, focusing on the components that contribute to the total:
Components of Implant Cost
- Surgical Fee (Implant Placement): This covers the oral surgeon's expertise, the actual implant post, and the surgical procedure itself.
- Average: $1,500 - $3,000 per implant.
- Abutment: The connector piece between the implant and the crown/prosthetic.
- Average: $500 - $1,000 per abutment.
- Restoration (Crown, Bridge, Denture): This is the visible part that looks like a tooth.
- Crown (Single Tooth): $1,000 - $2,500 (material variations like porcelain fused to metal, all-ceramic, zirconia affect cost).
- Bridge (Implant-supported): $2,500 - $5,000+ per unit, depending on number of teeth.
- Denture (Fixed, per arch): $8,000 - $15,000+ (includes custom design, materials, and lab fees).
- Anesthesia/Sedation:
- Local: Usually included.
- Oral Sedation: $100 - $300.
- IV Sedation: $500 - $1,500 per appointment (hourly rate).
- Pre-surgical Procedures (if needed):
- Extractions: $75 - $600 per tooth.
- Bone Grafting: $300 - $2,500 per site.
- Sinus Lift: $1,500 - $3,500 per side.
- Diagnostics:
- CBCT Scan: $250 - $600.
- Models/Impressions: $100 - $300.
Cost-Saving Tips:
- Consult Multiple Providers: Get detailed quotes from several qualified oral surgeons or periodontists. While quality is paramount, prices can vary.
- Explore Dental Schools: University dental schools often offer procedures at a reduced cost, as they are teaching institutions. The work is supervised by experienced faculty.
- Dental Savings Plans: As mentioned, these can provide significant discounts for an annual fee.
- Payment Plans: Utilize interest-free financing options through your provider or third-party lenders.
- Health Savings Accounts (HSAs) / Flexible Spending Accounts (FSAs): Use pre-tax dollars for dental expenses.
- Consider Alternatives (Carefully): While implants are often the best long-term solution, discuss less costly alternatives like traditional bridges or partial dentures with your dentist, understanding their limitations.
- Travel for Treatment: In some cases, patients may travel to areas with lower living costs for more affordable treatment, but consider follow-up care and the need for multiple visits.
Table: Average US Cost Ranges for Key Procedures
| Procedure | Low Estimate (USD) | Mid Estimate (USD) | High Estimate (USD) |
|---|---|---|---|
| Single Dental Implant (full restoration) | $3,000 | $4,500 | $6,000 |
| Bone Graft (small site) | $300 | $800 | $1,500 |
| Sinus Lift (per side) | $1,500 | $2,500 | $3,500 |
| Implant Supported Denture (Removable, 2 implants) | $6,000 | $9,000 | $12,000 |
| Implant Supported Denture (Fixed, All-on-4) | $12,000 | $18,000 | $25,000 |
| Surgical Wisdom Tooth Extraction (per tooth) | $200 | $400 | $600 |
Frequently Asked Questions
What is the success rate for innovative dental implant procedures?
Modern dental implants boast an impressive success rate, typically ranging from 95% to 98%, especially when performed by experienced specialists like oral surgeons or periodontists. This high success rate is attributed to advancements in implant design, materials, surgical techniques, and precise digital planning using CBCT imaging.
Is dental implant surgery painful?
Dental implant surgery is performed under local anesthesia, often supplemented with various forms of sedation (oral, IV, or nitrous oxide), ensuring you feel little to no pain during the procedure. Post-operative discomfort is manageable with prescribed pain medication and over-the-counter anti-inflammatories, usually subsiding within a few days.
How long does the entire dental implant process take?
The timeline for a dental implant can vary significantly. For a single implant, the process typically takes 3 to 9 months, including initial consultation, potential preparatory procedures (like bone grafting with its own healing time), implant placement, osseointegration (3-6 months), and final crown placement. Immediate load implants can shorten this to a single day for suitable candidates.
What are implant-supported dentures and how do they differ from traditional dentures?
Implant-supported dentures are prosthetic teeth that are anchored by dental implants rather than relying solely on the gums for support, like traditional dentures. They offer superior stability, chewing efficiency, and comfort, and they help preserve jawbone structure. They can be either removable (snapped onto implants) or fixed (permanently attached).
Are there alternatives to dental implants for missing teeth?
Yes, alternatives include traditional dental bridges, which use adjacent natural teeth as anchors for a prosthetic tooth, and removable partial or full dentures. While these options are generally less expensive upfront, they do not offer the same level of stability, bone preservation, or long-term durability as dental implants.
Can I get a "diamond tooth implant"?
The term "diamond tooth implant" usually refers to an aesthetic enhancement where a dental crown (which sits on an implant) is customized to incorporate diamonds or diamond-like materials for cosmetic purposes. It does not refer to the implant post itself being made of diamond. Such aesthetic additions are highly customized and add to the overall cost.
How do I care for my dental implants after surgery?
Initial aftercare involves managing swelling and pain with ice and medication, adhering to a soft diet, and avoiding strenuous activity. Long-term care is similar to natural teeth: brush twice daily, floss meticulously around the implants, and attend regular dental check-ups and professional cleanings, as recommended by the ADA.
What happens if I don't have enough bone for dental implants?
If you have insufficient jawbone volume, your oral surgeon may recommend a bone grafting procedure or a sinus lift (for the upper jaw) to augment the bone. These procedures create a solid foundation for the implant, making it possible to proceed with treatment after a healing period, typically 3-9 months.
Will my dental insurance cover the cost of innovative implant and oral surgery?
Dental insurance coverage for implants and advanced oral surgery is often limited. Many plans categorize implants as a "major procedure" with minimal coverage (0-15%) or exclude them entirely. However, some aspects like extractions or medically necessary procedures might be covered by either dental or medical insurance. Always verify coverage with your provider.
How long do dental implants last?
With proper oral hygiene, regular dental check-ups, and good overall health, dental implants have an excellent long-term prognosis. The implant post itself can often last a lifetime, while the crown, bridge, or denture attached to it may need replacement every 10-15 years due to wear and tear.
When to See a Dentist
Knowing when to seek professional dental attention is crucial for maintaining oral health and preventing minor issues from becoming major problems.
When to Seek Immediate/Emergency Dental Care (Red Flags):
- Severe, Unrelenting Pain: Especially if accompanied by swelling, fever, or difficulty swallowing. This could indicate a serious infection (abscess) requiring immediate intervention.
- Facial Swelling: Swelling around the jaw, cheek, or eye that is rapidly spreading could signify a dangerous infection.
- Trauma to the Mouth or Jaw: If you've had an accident that resulted in knocked-out teeth, fractured teeth, a lacerated gum, or a suspected broken jaw, seek emergency dental or medical care immediately.
- Uncontrolled Bleeding: Bleeding that doesn't stop after applying pressure, especially following an extraction or oral surgery.
- Difficulty Breathing or Swallowing: If an oral infection or injury is impacting your airway, go to an emergency room.
- Loose or Dislodged Implant/Prosthetic: While not always an emergency, if an implant feels loose or a crown/bridge detaches, contact your dentist promptly to prevent further damage or complications.
When to Schedule a Routine or Urgent Appointment:
- Persistent Toothache or Sensitivity: If a tooth aches when you bite down, is sensitive to hot or cold, or throbs regularly, it's a sign of decay, crack, or infection that needs evaluation.
- Bleeding, Red, or Swollen Gums: These are classic signs of gingivitis or periodontitis, which can lead to bone loss and tooth loss if left untreated.
- Loose Teeth: Beyond routine baby tooth loss, adult teeth should be firmly anchored. Loose teeth indicate advanced gum disease or bone loss.
- Chronic Bad Breath (Halitosis): Can be a symptom of gum disease, decay, or other oral health issues.
- Clicking or Popping Jaw: Suggestive of TMJ dysfunction.
- Sores, Lumps, or Lesions in the Mouth: Any unusual changes in your mouth that don't heal within two weeks should be examined to rule out oral cancer or other serious conditions.
- Broken or Chipped Teeth/Fillings: Even if not painful, these can worsen over time and expose the inner tooth to decay.
- Difficulty Chewing or Biting: May indicate bite problems, missing teeth, or underlying dental issues.
- Changes in Denture Fit: If your dentures feel loose or uncomfortable, it could mean bone loss and a need for relining or implant support.
Regular dental check-ups (every 6 months) are your best defense. Your dentist can identify subtle issues before they become painful or require extensive surgical intervention, aligning with ADA guidelines for preventive care.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026