Best Calcium for Teeth: Complete Guide
Key Takeaways
- Calcium is renowned for its role in building strong bones, but its importance extends profoundly to maintaining robust dental health. In fact, your teeth, primarily composed of calcium phosphate, are the hardest substance in your body, and they rely heavily on a steady supply of this vital mineral.
Calcium is renowned for its role in building strong bones, but its importance extends profoundly to maintaining robust dental health. In fact, your teeth, primarily composed of calcium phosphate, are the hardest substance in your body, and they rely heavily on a steady supply of this vital mineral. Despite its critical role, many Americans don't consume enough calcium, leading to increased risks of dental issues like weakened enamel, cavities, and even gum disease. Understanding the best calcium for teeth is not just about avoiding deficiency; it's about actively supporting the continuous repair and strengthening processes that keep your smile healthy and resilient throughout life.
This comprehensive guide from SmilePedia.net will delve deep into the world of calcium and its impact on your dental health. We'll explore the different types of calcium, optimal dietary sources, the role of supplements, and crucial co-factors like Vitamin D and K2. You'll learn how calcium contributes to tooth repair, what signs indicate a deficiency, and practical strategies to ensure your teeth receive the calcium they need for lifelong strength and vitality. By the end of this article, you'll be equipped with the knowledge to make informed choices that can significantly improve your oral health and contribute to a healthier, brighter smile.
Key Takeaways:
- Daily Intake: Adults typically need 1,000-1,200 mg of calcium daily, with adequate Vitamin D (600-800 IU) for optimal absorption.
- Best Forms: Dietary calcium from dairy, fortified foods, and leafy greens is preferred. For supplements, Calcium Carbonate (best with food) and Calcium Citrate (good on an empty stomach) are common, costing around $10-$30 per month.
- Teeth Repair: Calcium, combined with phosphate, constantly remineralizes tooth enamel, reversing early decay and strengthening teeth. This is an ongoing process.
- Co-factors are Crucial: Vitamin D is essential for calcium absorption, while Vitamin K2 helps direct calcium to bones and teeth, preventing calcification in soft tissues. Magnesium and Phosphorus also play vital roles.
- Prevention is Key: A calcium-rich diet, excellent oral hygiene, and regular dental check-ups are the most effective ways to prevent deficiency-related dental issues.
- Cost of Deficiency: Untreated calcium deficiency can lead to increased cavities, sensitivity, and the need for fillings (costing $90-$450 per tooth), root canals (up to $2,000), or even extractions.
What It Is: The Indispensable Role of Calcium in Dental Health
Calcium (Ca) is the most abundant mineral in the human body, with 99% of it stored in bones and teeth. These structures serve as a vital reservoir for calcium, maintaining the body's overall calcium balance. For dental health, calcium is not just a building block; it's an active participant in a continuous process of strengthening and repair.

Your teeth are primarily composed of a mineral matrix called hydroxyapatite, which is a crystalline form of calcium phosphate. This robust compound gives enamel, the outermost layer of your teeth, its incredible hardness and resistance to daily wear and tear. Dentin, the layer beneath enamel, is also rich in calcium and phosphorus, providing the bulk of the tooth structure.
The oral environment is constantly in flux. Every time you eat or drink, especially acidic or sugary items, your tooth enamel undergoes a process called demineralization. During demineralization, acids produced by oral bacteria or present in food and drinks attack the enamel, dissolving calcium and phosphate ions from its surface. If this process goes unchecked, it can lead to microscopic pores in the enamel, eventually forming cavities.
However, your body has a natural defense mechanism: remineralization. Saliva, which is rich in calcium, phosphate, and fluoride ions, acts as a protective buffer. After an acid attack, these minerals in your saliva diffuse back into the demineralized enamel, repairing the microscopic damage and rebuilding the hydroxyapatite crystals. This constant give-and-take between demineralization and remineralization is critical for maintaining tooth integrity. A sufficient supply of calcium is absolutely essential for the remineralization process to effectively counteract demineralization, thereby preventing decay and keeping your enamel strong.
![A diagram showing the demineralization and remineralization process on tooth enamel, with arrows indicating calcium and phosphate ions moving in and out of the enamel surface. Saliva(/oral-conditions/dry-mouth-causes-complete-guide) droplets are shown bringing minerals to the tooth.]
Types and Variations: Sourcing Calcium for Optimal Dental Health
When it comes to ensuring your teeth receive adequate calcium, you have two primary avenues: dietary sources and supplements. Both play important roles, but their effectiveness can vary depending on individual needs and lifestyle.
Dietary Calcium Sources: The Foundation of Good Health
The most natural and often preferred way to get calcium is through your diet. Food sources not only provide calcium but also often come with other beneficial nutrients that aid in its absorption and utilization.
- Dairy Products: Milk, yogurt, and cheese are classic calcium powerhouses.
- Milk: A single 8-ounce glass of milk contains about 300 mg of calcium. Opt for low-fat or fat-free varieties.
- Yogurt: 1 cup of plain, low-fat yogurt can provide around 450 mg of calcium. Many yogurts are also fortified with Vitamin D, further boosting absorption.
- Cheese: Hard cheeses like Parmesan, Swiss, and cheddar are excellent sources. A 1.5-ounce serving of cheddar has about 300 mg.
- Fortified Foods and Beverages: For those who are lactose intolerant or prefer plant-based options, many foods are fortified with calcium.
- Fortified Plant Milks: Almond, soy, oat, and rice milks are often fortified to match the calcium content of dairy milk (around 300 mg per cup). Check labels carefully.
- Fortified Orange Juice: Some brands offer orange juice with added calcium and Vitamin D, providing around 350 mg per cup.
- Fortified Cereals: Many breakfast cereals are fortified with calcium, though the amount can vary widely.
- Leafy Green Vegetables: While generally not as high in calcium as dairy, they contribute significantly, especially when consumed regularly.
- Kale, Spinach, Collard Greens: These are good sources, though some (like spinach) also contain oxalates, which can slightly inhibit calcium absorption.
- Broccoli: Contains about 43 mg of calcium per cup, along with Vitamin C and K.
- Fish and Legumes:
- Sardines and Canned Salmon (with bones): These are surprisingly rich in calcium, offering around 325 mg and 232 mg per 3-ounce serving, respectively. The soft, edible bones are where the calcium is concentrated.
- Beans and Lentils: While not primary sources, black beans, pinto beans, and lentils contribute a moderate amount of calcium.
Calcium Supplements: When Diet Isn't Enough
For many people, meeting the daily recommended calcium intake (RDA: 1,000-1,200 mg for adults) through diet alone can be challenging. In these cases, supplements can be a valuable option, particularly for those with dietary restrictions, malabsorption issues, or increased needs.
Common Types of Calcium Supplements:
-
Calcium Carbonate:
- Elemental Calcium: Contains about 40% elemental calcium, meaning it provides a high amount of calcium per pill. This makes it a very efficient choice.
- Absorption: Best absorbed when taken with food, as stomach acid helps in its dissolution.
- Availability: Widely available, often the least expensive.
- Potential Side Effects: Can cause constipation or bloating in some individuals.
- Example: Tums, Viactiv, Caltrate.
- Cost: Approximately $10-$20 per month for generic brands.
-
Calcium Citrate:
- Elemental Calcium: Contains about 21% elemental calcium, so you may need to take more pills to get the same amount of calcium as carbonate.
- Absorption: Can be absorbed equally well with or without food, making it a good option for those with less stomach acid (e.g., older adults, people taking acid blockers).
- Availability: Widely available, usually slightly more expensive than carbonate.
- Potential Side Effects: Generally well-tolerated, less likely to cause constipation than carbonate.
- Example: Citracal.
- Cost: Approximately $15-$30 per month for generic brands.
-
Calcium Lactate and Calcium Gluconate:
- Elemental Calcium: Contain much lower percentages of elemental calcium (13% for lactate, 9% for gluconate). This means you would need to take many more tablets to meet your daily needs, making them less practical for supplementation.
- Absorption: Generally well-absorbed.
- Availability: Less common as primary calcium supplements.
- Use: Often used in food fortification or as intravenous calcium for medical conditions.
Synergistic Nutrients for Calcium Absorption and Utilization:
Calcium doesn't work alone. Several other vitamins and minerals are critical for its proper absorption and deposition into bones and teeth.
- Vitamin D: Absolutely essential. Vitamin D helps your body absorb calcium from the digestive tract into the bloodstream. Without sufficient Vitamin D, even a high calcium intake can be ineffective. Sun exposure, fatty fish, and fortified foods are good sources. The ADA recommends adequate vitamin D intake for oral and overall health.
- Vitamin K2: This often-overlooked vitamin plays a crucial role in directing calcium to the right places – bones and teeth – and preventing its deposition in soft tissues like arteries. It activates proteins like osteocalcin, which binds calcium to the bone matrix, and matrix Gla protein, which inhibits arterial calcification. Sources include fermented foods (natto), certain cheeses, and egg yolks.
- Magnesium: Involved in over 300 enzymatic reactions in the body, including those that activate Vitamin D and help regulate calcium levels. It also plays a role in the formation of healthy tooth enamel. Sources include leafy greens, nuts, seeds, and whole grains.
- Phosphorus: The second most abundant mineral in the body, phosphorus partners with calcium to form hydroxyapatite, the primary mineral component of teeth and bones. Most protein-rich foods (meat, dairy, nuts) are good sources.
Pro Tip: When choosing a calcium supplement, look for one that also includes Vitamin D to maximize absorption. If you're concerned about arterial health, consider a supplement that also provides Vitamin K2, or ensure you get enough from your diet. Always consult your dentist or physician before starting any new supplement regimen.
Causes: Why Calcium Deficiency Affects Your Teeth
A sufficient supply of calcium is fundamental for strong teeth and a healthy mouth. When calcium intake or absorption is inadequate, or when factors accelerate calcium loss, your dental health can be significantly compromised.
1. Dietary Insufficiency
The most straightforward cause of calcium deficiency is simply not consuming enough calcium-rich foods. Modern diets, often high in processed foods and low in nutrient-dense options, can easily fall short of the recommended daily intake.
- Lack of Dairy: For individuals who are lactose intolerant, have dairy allergies, or follow vegan diets, ensuring adequate calcium can be challenging without careful planning and fortification.
- Limited Variety: A diet lacking a diverse range of fruits, vegetables, and fortified products can lead to calcium gaps.
2. Impaired Calcium Absorption
Even if you consume enough calcium, your body might not be absorbing it effectively.
- Vitamin D Deficiency: This is a major culprit. Without adequate Vitamin D, your body can only absorb 10-15% of dietary calcium. Vitamin D facilitates the absorption of calcium in the intestines.
- Certain Medical Conditions:
- Malabsorption Syndromes: Conditions like Celiac disease, Crohn's disease, and ulcerative colitis can damage the intestinal lining, impairing nutrient absorption, including calcium.
- Kidney Disease: The kidneys play a crucial role in activating Vitamin D and regulating calcium levels. Impaired kidney function can lead to calcium imbalances.
- Parathyroid Gland Disorders: The parathyroid glands regulate calcium and phosphate levels. Hypoparathyroidism (underactive glands) leads to low calcium, while hyperparathyroidism (overactive glands) can disrupt calcium balance.
- Medications: Some medications can interfere with calcium absorption or increase calcium excretion.
- Proton Pump Inhibitors (PPIs): Used for acid reflux, PPIs can reduce stomach acid, which is necessary for the absorption of calcium carbonate.
- Corticosteroids: Long-term use can decrease calcium absorption and increase bone loss.
- Certain Diuretics: Some diuretics can increase calcium excretion.
3. Increased Calcium Loss
Factors that accelerate calcium loss from the body can also contribute to deficiency.
- High Sodium Intake: Excessive sodium can lead to increased calcium excretion through urine.
- Excessive Caffeine and Alcohol: High consumption of caffeine and alcohol has been linked to reduced calcium absorption and increased loss, though the effect is usually modest in healthy individuals.
- Acidic Foods and Drinks: While not directly causing systemic calcium deficiency, frequent consumption of highly acidic beverages (soda, fruit juices, energy drinks) and foods directly attacks tooth enamel. This acid erosion leaches minerals (including calcium) from the tooth surface, initiating demineralization. This process outpaces remineralization if calcium supply is insufficient, leading to weakening and decay.
- Poor Oral Hygiene: Accumulation of plaque and tartar creates an acidic environment in the mouth, fueling bacterial growth and acid production. This significantly accelerates demineralization, making teeth more vulnerable even with adequate systemic calcium.
4. Hormonal Changes
- Menopause: Estrogen plays a role in calcium regulation. After menopause, women experience a significant drop in estrogen, which can lead to accelerated bone loss and increased risk of calcium deficiency.
- Pregnancy and Lactation: The body's demand for calcium increases significantly during these periods to support fetal development and milk production, requiring higher dietary intake.
Understanding these underlying causes is the first step toward addressing calcium deficiency and safeguarding your dental health.
Signs and Symptoms of Calcium Deficiency in Teeth
Recognizing the signs and symptoms of inadequate calcium intake or absorption is crucial for early intervention and preventing more severe dental problems. These signs can manifest both orally and systemically.
Oral Signs and Symptoms:
These are directly related to the impact of calcium deficiency on tooth structure and oral health.
- Increased Tooth Sensitivity: As enamel weakens and demineralizes, the underlying dentin, which contains tiny tubules leading to the tooth's nerve, becomes exposed. This can lead to sensitivity to hot, cold, sweet, or acidic foods and drinks.
- Frequent Cavities (Dental Caries): When remineralization cannot keep pace with demineralization due to insufficient calcium, the enamel becomes more porous and susceptible to acid attacks from oral bacteria, leading to the formation of new cavities or the worsening of existing ones. This is a primary indicator that the body struggles with calcium for teeth repair.
- Weakened, Brittle, or Chipping Teeth: Enamel may appear translucent or develop small cracks. Teeth may chip more easily, even with minor trauma, as their structural integrity is compromised.
- Enamel Erosion: While often caused by acidic foods/drinks or acid reflux, insufficient calcium exacerbates the problem by making it harder for the enamel to rebuild itself after these erosive events. You might notice a dull, worn appearance on your tooth surfaces.
- Gum Issues (Indirectly): While calcium deficiency primarily affects teeth and bones, severe, long-term deficiency can contribute to issues like gum recession and even bone loss in the jaw, which supports the teeth. This makes teeth more vulnerable to periodontal disease.
- Delayed Tooth Eruption (in Children): In children, severe calcium deficiency can lead to delays in the eruption of primary (baby) and permanent teeth.
- Poorly Formed Enamel: In developing teeth, a lack of calcium can result in hypomineralization, where the enamel forms incompletely or is weaker than it should be, making teeth prone to decay from the moment they erupt.
Systemic Signs and Symptoms (Indicating Overall Calcium Deficiency):
These symptoms are not dental-specific but signal a broader calcium deficiency that will undoubtedly impact oral health.
- Muscle Cramps and Spasms: Often in the back, thighs, and calves. Low calcium can impair muscle function.
- Numbness and Tingling: Particularly in the fingers, toes, and around the mouth (paresthesia).
- Fatigue and Lethargy: A general feeling of tiredness and lack of energy.
- Brittle Nails: Nails may become weak, prone to breaking, or develop ridges.
- Dry Skin and Hair: Skin may become dry and flaky, and hair may appear coarse or brittle.
- Osteoporosis (Long-term): If the body consistently draws calcium from its reserves (bones and teeth) to maintain blood calcium levels, it can lead to reduced bone density and eventually osteoporosis, significantly increasing fracture risk.
- Irregular Heartbeat: Severe calcium deficiency can affect heart rhythm, though this is less common and usually indicates an urgent medical situation.
If you experience any combination of these symptoms, especially the oral ones, it's crucial to consult with your dentist or physician to assess your calcium status and determine the best course of action. Early detection and intervention are key to preserving both your dental and overall health.
Treatment Options: Addressing Calcium Deficiency and Its Dental Effects
Addressing calcium deficiency and its impact on your teeth requires a multi-faceted approach, combining dietary changes, supplementation, and targeted dental treatments. The goal is not just to replace lost calcium but to prevent future issues and repair existing damage.
1. Dietary Modification and Nutritional Counseling
This is the cornerstone of long-term calcium management.
- Description: Working with a registered dietitian or your dentist/physician to evaluate your current diet and create a meal plan rich in calcium, Vitamin D, and other synergistic nutrients.
- Pros: Natural, holistic approach; provides other essential nutrients; sustainable in the long run.
- Cons: Requires commitment and dietary changes; may not be sufficient for severe deficiencies or malabsorption issues.
- Cost: Nutritional counseling can range from $75 to $200 per session without insurance, often partially covered by health insurance for specific conditions.
2. Calcium and Vitamin D Supplementation
When dietary intake is insufficient, supplements become necessary.
- Description: Taking oral calcium supplements (e.g., calcium carbonate or citrate) combined with Vitamin D. Dosage will depend on your existing intake and needs, usually 500-1000 mg of elemental calcium per day, in divided doses, with 600-800 IU of Vitamin D.
- Pros: Effective for increasing calcium levels quickly; convenient; targeted intervention.
- Cons: Potential for side effects (constipation, bloating); risk of over-supplementation if not monitored; requires consistent adherence.
- Cost: Calcium supplements typically cost $10-$30 per month for good quality brands.
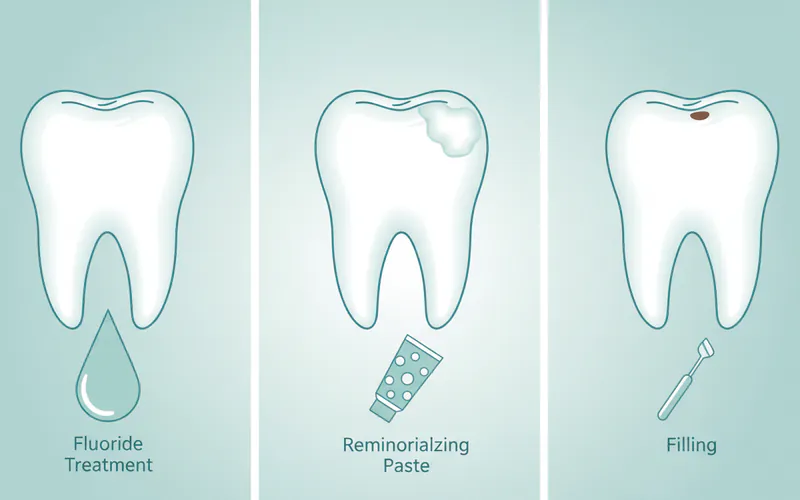
3. Professional Fluoride Treatments
Fluoride works synergistically with calcium to strengthen teeth.
- Description: In-office fluoride varnishes, gels, or foams applied by a dental professional. Fluoride is integrated into the enamel, forming fluorapatite, which is more resistant to acid attacks than regular hydroxyapatite, enhancing the remineralization process.
- Pros: Highly effective at strengthening enamel and preventing cavities; quick and painless.
- Cons: Not a direct source of calcium; requires regular reapplication (typically every 3-6 months).
- Cost: $25-$75 per application, often covered by dental insurance, especially for children.
4. Remineralizing Dental Products
These products aim to deliver calcium, phosphate, and sometimes fluoride directly to the tooth surface.
- Description: Toothpastes and mouthwashes containing ingredients like calcium phosphate (e.g., amorphous calcium phosphate (ACP), casein phosphopeptide-amorphous calcium phosphate (CPP-ACP/Recaldent), NovaMin) or nanohydroxyapatite. These components can help replenish mineral content in enamel.
- Pros: Non-invasive; can be used daily as part of routine oral hygiene; can reduce sensitivity.
- Cons: May take time to show noticeable results; best used as an adjunct to other treatments.
- Cost: $8-$25 for specialized toothpastes/mouthwashes.
5. Dental Restorations for Existing Damage
For damage that has already occurred due to calcium deficiency and subsequent decay, restorative treatments are necessary.
- Description:
- Fillings: For cavities, amalgam or composite resin fillings restore the tooth's structure and prevent further decay.
- Dental Bonding: For minor chips, cracks, or enamel erosion, a tooth-colored resin can be applied and sculpted.
- Dental Crowns: For extensively damaged or weakened teeth, a cap (crown) can cover and protect the entire tooth.
- Inlays/Onlays: For larger cavities that don't require a full crown, these custom-made restorations fit within the tooth's cusps.
- Pros: Restores tooth function and aesthetics; prevents further deterioration.
- Cons: Invasive procedures; can be costly; does not address the underlying calcium deficiency.
- Cost:
- Fillings: $90-$450 per tooth (composite), $50-$250 per tooth (amalgam).
- Bonding: $300-$600 per tooth.
- Crowns: $800-$2,500 per tooth.
Pro Tip: Always discuss your symptoms and concerns with your dentist. They can diagnose the extent of any deficiency-related damage and recommend the most appropriate combination of treatments, from dietary adjustments to restorative procedures. The American Dental Association (ADA) emphasizes the importance of a balanced diet for oral health and regular dental check-ups for early detection and intervention of dental issues.
Step-by-Step Process: Optimizing Calcium for Your Dental Health
Taking a proactive approach to ensure adequate calcium for your teeth involves several key steps, often in consultation with healthcare professionals. This isn't a one-time fix but an ongoing commitment to your oral and overall health.
Step 1: Dental Consultation and Comprehensive Assessment
- What to Expect: Your journey begins with a visit to your dentist. They will perform a thorough oral examination, which may include X-rays, to assess the current state of your teeth and jawbone. They will look for signs of demineralization, existing cavities, enamel erosion, and gum health.
- Discussion: Be prepared to discuss your dietary habits, any existing medical conditions, medications you're taking, and any symptoms you've experienced (e.g., sensitivity, frequent cavities). This information helps your dentist understand potential causes of calcium-related issues.
- Initial Recommendations: Based on the assessment, your dentist might recommend initial treatments like fluoride applications or prescribe remineralizing toothpastes to address immediate concerns.
Step 2: Dietary Evaluation and Nutritional Guidance
- Reviewing Your Diet: Your dentist or a referred registered dietitian will help you evaluate your current calcium and Vitamin D intake from food sources. This often involves keeping a food diary for a few days.
- Personalized Plan: You'll receive guidance on incorporating more calcium-rich foods into your daily diet. This could include dairy products, fortified plant milks and juices, dark leafy greens, and certain fish. You'll also learn about foods rich in Vitamin D (fatty fish, fortified cereals) and K2 (fermented foods, certain cheeses) to optimize calcium utilization.
- Target: Aim for the recommended daily allowance (RDA) of calcium (1,000-1,200 mg for adults) and Vitamin D (600-800 IU).
Step 3: Supplement Recommendation and Selection (If Needed)
- Doctor's Order: If dietary intake alone isn't sufficient or if you have specific malabsorption issues, your physician or dentist may recommend calcium and Vitamin D supplements.
- Choosing the Right Type: They will advise on the best form of calcium (e.g., calcium carbonate with food, calcium citrate for sensitive stomachs) and the appropriate dosage.
- Timing: Supplements are often recommended to be taken in divided doses (e.g., 500 mg twice a day) rather than a single large dose, as the body can only absorb a limited amount of calcium at one time. They'll also instruct you on whether to take it with or without food.
Step 4: Enhanced Oral Hygiene and Remineralizing Products
- Brushing and Flossing: Consistent and effective oral hygiene is paramount. Brush twice daily with a fluoride toothpaste and floss once daily to remove plaque and food debris that contribute to acid production.
- Therapeutic Toothpastes/Mouthwashes: Your dentist may recommend specific toothpastes or mouthwashes containing remineralizing agents (like nanohydroxyapatite or CPP-ACP) to further aid in strengthening enamel and reducing sensitivity.
- Limit Acidic/Sugary Intake: Reduce consumption of highly acidic beverages and sugary snacks, which contribute to demineralization. If consumed, rinse your mouth with water afterward.
Step 5: Regular Monitoring and Follow-up
- Dental Check-ups: Maintain regular dental check-ups and professional cleanings (typically every six months) to monitor your oral health, assess the effectiveness of interventions, and catch any new issues early.
- Blood Tests: For systemic calcium deficiency, your physician may order follow-up blood tests to monitor your calcium and Vitamin D levels and adjust supplement dosages as needed.
- Ongoing Commitment: Remember that maintaining optimal calcium levels for your teeth is a continuous process that requires lifelong attention to diet, hygiene, and professional care.

By following these steps, you can create a comprehensive plan to ensure your teeth receive the calcium they need, supporting their strength, repairing early damage, and preserving your healthy smile.
Cost and Insurance: Understanding the Financial Aspect of Calcium for Teeth
When addressing calcium deficiency and its dental consequences, it's important to understand the associated costs and how insurance may play a role. These costs can range from daily supplements to more extensive dental procedures.
Costs of Calcium-Related Care (US Averages):
-
Calcium and Vitamin D Supplements:
- Average Cost: $10-$30 per month for a good quality brand. This can vary based on brand, form (carbonate vs. citrate), and whether it includes Vitamin D or other co-factors.
- Without Insurance: Typically an out-of-pocket expense, as most health insurance plans do not cover over-the-counter supplements.
- With Insurance: Some FSA/HSA accounts can be used for certain supplements if prescribed by a doctor.
-
Nutritional Counseling:
- Average Cost: $75-$200 per session. Follow-up sessions are usually less expensive.
- Without Insurance: Full out-of-pocket.
- With Insurance: Some health insurance plans may cover nutritional counseling, especially if linked to a specific medical condition (e.g., Celiac disease, chronic kidney disease). Coverage varies widely, often requiring a doctor's referral.
-
Professional Fluoride Treatments:
- Average Cost: $25-$75 per application.
- Without Insurance: Out-of-pocket.
- With Insurance: Most dental insurance plans cover fluoride treatments, especially for children, often at 80-100% as a preventive service. Adults may have limited or no coverage depending on the plan.
-
Remineralizing Toothpastes/Mouthwashes (Prescription Strength):
- Average Cost: $15-$40 per tube/bottle.
- Without Insurance: Out-of-pocket.
- With Insurance: Rarely covered by dental insurance, though some FSA/HSA accounts may allow for reimbursement if prescribed.
-
Dental Restorations (Due to Calcium Deficiency-Related Decay):
- Dental Fillings:
- Amalgam (silver): $50-$250 per tooth.
- Composite (tooth-colored): $90-$450 per tooth.
- Dental Bonding (for chips/erosion): $300-$600 per tooth.
- Dental Crowns (for severe damage): $800-$2,500 per tooth. (Varies by material – porcelain, ceramic, metal, gold).
- Without Insurance: Full out-of-pocket.
- With Insurance: Dental insurance typically covers a portion of restorative procedures:
- Basic Services (Fillings): Often covered at 50-80% after deductible.
- Major Services (Crowns, Inlays/Onlays): Typically covered at 20-50% after deductible, sometimes with a waiting period.
- Annual Maximums: Most dental plans have an annual maximum benefit, often ranging from $1,000 to $2,000. Once this limit is reached, you pay 100% of costs.
- Dental Fillings:
Insurance Coverage Details:
- Preventive Care: Most dental insurance plans prioritize preventive care, covering routine check-ups, cleanings, and sometimes fluoride treatments at 80-100% with no deductible. This is a significant cost-saver, as preventing decay is always cheaper than treating it.
- Basic vs. Major Restorative: Coverage percentages typically decrease for more extensive procedures. For example, fillings might be 80% covered, while a crown might be 50% covered.
- Waiting Periods: Some plans, especially new ones, may have waiting periods (e.g., 6-12 months) before major restorative procedures are covered.
- Deductibles: You'll typically need to pay an annual deductible (e.g., $50-$100) before your insurance begins to pay its share.
- HMO vs. PPO:
- HMO (Dental Health Maintenance Organization): Lower premiums, but you must choose a dentist within the network. Referrals often needed for specialists.
- PPO (Preferred Provider Organization): Higher premiums, but more flexibility to choose any dentist (though in-network dentists result in lower out-of-pocket costs).
Pro Tip: Always call your dental insurance provider to verify coverage details for specific procedures before your appointment. Many dental offices also offer in-house payment plans or work with third-party financing options like CareCredit to help manage costs for extensive treatments. Investing in preventive care and maintaining adequate calcium levels can significantly reduce the need for costly restorative dental work down the line.
Recovery and Aftercare: Maintaining Your Remineralized Smile
Once you've taken steps to address calcium deficiency and its dental effects, the "recovery" process is less about healing from a single event and more about establishing a lifelong regimen of maintenance and prevention. This continuous commitment is crucial for ensuring your teeth remain strong, resilient, and resistant to future damage.
1. Consistent Dietary Adherence: The Lifelong Plan
- Prioritize Calcium-Rich Foods: Continue to incorporate a wide variety of calcium-rich foods into your daily diet. Don't view dietary changes as temporary; they are the foundation of sustained oral and overall health.
- Don't Forget Co-factors: Ensure adequate intake of Vitamin D (through diet, sun exposure, or supplements as advised), Vitamin K2, and Magnesium, as these are critical for calcium absorption and utilization.
- Hydration: Drink plenty of water throughout the day. Water helps produce saliva, which is vital for natural remineralization and rinsing away food particles and acids.
2. Regular Supplementation (If Recommended)
- Adhere to Dosage: If your physician or dentist has recommended calcium and/or Vitamin D supplements, take them consistently as prescribed. Do not stop without professional guidance, even if you feel your diet has improved.
- Monitor for Side Effects: Be aware of any potential side effects like constipation (especially with calcium carbonate) and discuss them with your doctor. They may suggest adjusting the type or dose of calcium.
3. Meticulous Oral Hygiene
- Brush Twice Daily: Continue to brush your teeth thoroughly for two minutes, twice a day, using a fluoride toothpaste. If prescribed, use a remineralizing toothpaste.
- Floss Daily: Flossing removes plaque and food debris from between teeth and along the gumline, preventing acid production in these hard-to-reach areas.
- Therapeutic Rinses: If recommended, use antiseptic or fluoride mouthwashes to further support oral health and remineralization.
- Tongue Cleaning: Clean your tongue daily to reduce oral bacteria.
4. Limit Acidic and Sugary Exposures
- Reduce Frequency: Minimize snacking, especially on sugary or acidic foods and drinks. Each exposure initiates an acid attack on your enamel.
- Strategic Consumption: If you consume acidic beverages (sodas, fruit juices), do so quickly, preferably with a meal, and use a straw to minimize contact with teeth. Rinse your mouth with water immediately afterward, but wait at least 30 minutes before brushing to avoid abrading softened enamel.
5. Regular Dental Check-ups and Professional Cleanings
- Preventive Visits: Schedule and attend your routine dental check-ups and cleanings every six months (or as recommended by your dentist). These visits are crucial for monitoring your oral health, detecting any new signs of demineralization or decay early, and receiving professional fluoride applications.
- Open Communication: Discuss any ongoing sensitivity, new symptoms, or dietary changes with your dentist during these visits.
By integrating these practices into your daily life, you actively support the remineralization process, strengthen your enamel, and dramatically reduce your risk of future dental issues stemming from calcium deficiency. This proactive approach ensures your teeth benefit from the best calcium for teeth consistently.
Prevention: Proactive Steps to Safeguard Your Teeth with Calcium
Preventing calcium deficiency and its associated dental problems is far more effective and less costly than treating them. A comprehensive prevention strategy involves a combination of dietary choices, excellent oral hygiene, and consistent professional dental care.
1. Balanced, Calcium-Rich Diet
- Meet Daily Requirements: Aim for the recommended daily allowance (RDA) of calcium (1,000-1,200 mg for most adults) through a diverse diet. Incorporate dairy products (milk, yogurt, cheese), fortified plant-based alternatives, leafy green vegetables (kale, broccoli), and certain fish (sardines, salmon with bones).
- Prioritize Vitamin D: Ensure adequate Vitamin D intake (600-800 IU daily) from sunlight exposure, fatty fish, fortified foods, or supplements, as it's critical for calcium absorption.
- Include Co-factors: Don't forget other vital nutrients like Vitamin K2 and Magnesium, which work synergistically with calcium.
- Limit Calcium Inhibitors: Reduce excessive consumption of sodium, caffeine, and alcohol, which can interfere with calcium absorption or increase its excretion.
2. Excellent Oral Hygiene Practices
- Brush with Fluoride Toothpaste: Brush your teeth twice a day for two minutes with a fluoride toothpaste. Fluoride directly helps remineralize enamel and makes it more resistant to acid attacks.
- Floss Daily: Floss once a day to remove plaque and food particles from between teeth and under the gumline, areas where bacteria thrive and produce acids that demineralize enamel.
- Use Remineralizing Products: Consider using an over-the-counter fluoride mouthwash or a specialized remineralizing toothpaste (e.g., containing nanohydroxyapatite or CPP-ACP) if you're at higher risk for demineralization or sensitivity.
3. Limit Sugary and Acidic Foods/Beverages
- Reduce Frequency: Minimize consumption of sugary snacks, sodas, fruit juices, and energy drinks. The sugars fuel acid-producing bacteria, and the acids directly erode enamel.
- Strategic Consumption: If you do consume these items, do so with meals to buffer the acid, and rinse your mouth with water afterward. Avoid sipping acidic beverages over extended periods.
4. Regular Dental Check-ups and Professional Cleanings
- Routine Visits: Visit your dentist every six months for a comprehensive oral examination and professional cleaning. These visits allow your dentist to:
- Identify early signs of demineralization before they become cavities.
- Apply professional fluoride treatments to strengthen enamel.
- Address any underlying issues that might contribute to calcium deficiency in the mouth.
- Discuss Concerns: Talk to your dentist about any tooth sensitivity, changes in your diet, or medications you are taking that could impact your calcium levels or dental health.
5. Address Underlying Medical Conditions
- Manage Chronic Diseases: Work with your physician to effectively manage medical conditions like Celiac disease, Crohn's disease, or kidney disease, which can impair calcium absorption or increase its loss.
- Review Medications: Discuss with your doctor if any long-term medications you are taking might be affecting your calcium levels or dental health.
By proactively incorporating these preventive measures into your lifestyle, you create an optimal environment for your teeth to constantly remineralize and stay strong, significantly reducing the risk of dental decay and other issues related to calcium deficiency. This is the ultimate strategy for leveraging the best calcium for teeth for lifelong oral health.
Risks and Complications: Understanding Potential Downsides
While calcium is essential for healthy teeth and bones, both too little and, paradoxically, too much can lead to health problems. It's crucial to understand these risks to maintain a healthy balance.
Risks of Inadequate Calcium (Deficiency):
As extensively discussed, insufficient calcium carries significant risks for oral and systemic health:
- Increased Risk of Dental Caries (Cavities): Without enough calcium, remineralization cannot keep up with demineralization, leading to weaker enamel and increased susceptibility to decay.
- Tooth Sensitivity: Thinning or weakened enamel exposes underlying dentin, causing sensitivity.
- Enamel Erosion and Weakness: Teeth become more prone to chipping, cracking, and generalized wear.
- Periodontal Disease Risk: While not a direct cause, chronic calcium deficiency can weaken alveolar bone (the bone supporting teeth), potentially exacerbating gum disease and leading to tooth loss.
- Osteoporosis: The most significant systemic complication, characterized by brittle bones prone to fractures, as the body draws calcium from its skeletal reserves to maintain vital blood calcium levels.
- Hypocalcemia: Critically low blood calcium levels can lead to muscle spasms, numbness, tingling, and in severe cases, seizures or heart rhythm abnormalities.
Risks of Excessive Calcium (Hypercalcemia):
While difficult to achieve through diet alone, taking very high doses of calcium supplements, especially without adequate Vitamin D, can lead to hypercalcemia (too much calcium in the blood) and other complications.
- Hypercalcemia Symptoms:
- Mild: Nausea, vomiting, constipation, increased thirst, frequent urination, fatigue.
- Severe: Kidney problems (including kidney stones), bone pain, confusion, heart rhythm disturbances, coma.
- Kidney Stones: Excess calcium can be filtered by the kidneys and, if not properly excreted, can crystallize to form kidney stones. This risk is primarily associated with high-dose calcium supplementation (over 2,000 mg/day) and can be exacerbated by dehydration.
- Cardiovascular Issues: Some studies suggest a potential link between high calcium supplement intake (without corresponding Vitamin D and K2) and an increased risk of heart disease, as excess calcium might deposit in arteries. However, this is a complex and debated area of research, with dietary calcium generally considered safe. Vitamin K2 is particularly important for directing calcium to bones and teeth while preventing soft tissue calcification.
- Drug Interactions: High doses of calcium can interfere with the absorption of certain medications, including:
- Thyroid Hormones: Take calcium at least 4 hours apart from thyroid medication.
- Antibiotics (Tetracyclines, Fluoroquinolones): Calcium can bind to these antibiotics, reducing their effectiveness. Take calcium several hours before or after.
- Bisphosphonates: Medications for osteoporosis.
- Iron Supplements: Calcium can inhibit iron absorption.
- Constipation: A common side effect of calcium carbonate supplements.
Pro Tip: Always adhere to the recommended daily allowance (RDA) for calcium and consult your doctor or dentist before taking high-dose supplements. They can assess your individual needs, especially if you have underlying health conditions or are taking other medications. "More is not always better" when it comes to nutrient intake.
Comparison Tables: Calcium Sources and Supplements
To help you make informed decisions about how to best incorporate calcium into your routine, here are two comparison tables outlining key aspects of dietary sources and different supplement types.
Table 1: Dietary Calcium Sources vs. Supplements
| Feature | Dietary Calcium Sources | Calcium Supplements |
|---|---|---|
| Primary Benefit | Comprehensive nutrient profile (Vitamins D, K, Magnesium, etc.), natural absorption. | Targeted, convenient way to meet needs when diet falls short. |
| Absorption | Generally good, often aided by natural co-factors in food. Bioavailability varies (e.g., oxalates in spinach). | Varies by type (carbonate needs food, citrate does not), often includes Vitamin D. |
| Cost | Varies widely based on food choices. Generally part of regular grocery budget. | $10-$30 per month for most common types, typically an out-of-pocket expense. |
| Side Effects | Rarely any, unless allergic (e.g., dairy intolerance). | Constipation (carbonate), bloating, potential for hypercalcemia with excessive intake. |
| Best For | Most individuals, as a primary source of calcium. Essential for overall nutrition. | Individuals with insufficient dietary intake, malabsorption, or increased needs (e.g., post-menopause). |
| Dental Impact | Sustained, steady supply for remineralization and strong enamel. | Can help bridge gaps to support remineralization and reduce decay risk. |
Table 2: Common Calcium Supplement Types
| Supplement Type | Elemental Calcium Content | Absorption Profile | Pros | Cons | Typical Monthly Cost |
|---|---|---|---|---|---|
| Calcium Carbonate | ~40% | Best absorbed with food (requires stomach acid). | High elemental calcium (fewer pills), inexpensive, widely available. | Can cause constipation/bloating, must be taken with meals. | $10-$20 |
| Calcium Citrate | ~21% | Absorbed well with or without food. | Less likely to cause digestive upset, good for those with low stomach acid. | Lower elemental calcium (more pills needed), slightly more expensive. | $15-$30 |
| Calcium Lactate | ~13% | Generally well-absorbed. | Good for sensitive stomachs. | Very low elemental calcium (impractical for daily needs). | Higher (less common) |
| Calcium Gluconate | ~9% | Generally well-absorbed. | Often used intravenously in medical settings. | Very low elemental calcium (impractical for daily needs). | Higher (less common) |
Pro Tip: When comparing supplements, always check the "elemental calcium" amount, not just the total weight of the calcium compound. The elemental calcium is what your body actually uses.
Children / Pediatric Considerations: Calcium for Growing Smiles
Calcium is critically important for children, not just for strong bones, but for the proper development and mineralization of both primary (baby) and permanent teeth. The stages of tooth formation are highly reliant on a consistent and adequate supply of calcium and its co-factors.
Why Calcium is Crucial for Children's Teeth:
- Tooth Development: During infancy and early childhood, teeth are actively forming beneath the gums. Calcium and phosphorus are the primary minerals that build the enamel and dentin structure. Insufficient calcium during these formative years can lead to hypomineralization, resulting in weaker, less dense enamel that is highly susceptible to decay from the moment teeth erupt.
- Eruption Timing: Severe calcium deficiency can sometimes lead to delays in tooth eruption.
- Jawbone Development: Calcium is essential for the growth and development of the jawbones, which support the teeth and dictate facial structure.
- Prevention of Early Childhood Caries (ECC): While ECC is primarily caused by prolonged exposure to sugary liquids, strong, well-mineralized enamel (built with sufficient calcium) offers better resistance to acid attacks.

Recommended Daily Allowances (RDAs) for Children:
The calcium needs of children vary significantly by age:
- 0-6 months: 200 mg (from breast milk or formula)
- 7-12 months: 260 mg
- 1-3 years: 700 mg
- 4-8 years: 1,000 mg
- 9-18 years: 1,300 mg (peak bone and tooth development during adolescence)
Sources of Calcium for Children:
- Breast Milk and Formula: For infants, these are the primary and ideal sources of calcium.
- Dairy Products: Milk, yogurt, and cheese are excellent options for toddlers and older children.
- Fortified Foods: Calcium-fortified cereals, juices, and plant-based milks can help meet needs.
- Leafy Greens: Incorporate greens like broccoli and kale into meals, perhaps hidden in smoothies or sauces if kids are resistant.
Pediatric Dental Care and Calcium:
- Early Dental Visits: The American Academy of Pediatric Dentistry (AAPD) recommends a child's first dental visit by age one or when the first tooth erupts. This helps dentists monitor tooth development and provide guidance on diet and oral hygiene.
- Fluoride Varnish: Pediatric dentists frequently apply fluoride varnish, which helps strengthen developing enamel and enhance remineralization, acting as a crucial defense against decay.
- Parental Guidance: Parents play a vital role in ensuring their children receive adequate calcium through a balanced diet. They also need to model good oral hygiene habits and limit sugary snacks and drinks, which undermine the benefits of calcium.
Pro Tip for Parents: If your child has dietary restrictions (e.g., dairy allergy, vegan diet), consult with your pediatrician or a registered dietitian to ensure they are getting enough calcium and Vitamin D, potentially through fortified foods or supplements. Never give calcium supplements to children without professional medical advice.
Cost Breakdown: A Deeper Dive into Dental Expenses Related to Calcium Deficiency
Understanding the full financial picture associated with maintaining optimal calcium levels and treating any resulting dental issues is critical for planning and budgeting. This breakdown provides more detailed average costs in the U.S.
I. Preventive & Maintenance Costs
These are proactive steps to prevent calcium deficiency or its consequences, often significantly cheaper than treating problems.
-
Calcium & Vitamin D Supplements:
- Low End: Generic Calcium Carbonate + Vitamin D3: $10-$15/month
- Mid-Range: Reputable brand Calcium Citrate + Vitamin D3: $15-$25/month
- High End: Specialized formulations (e.g., with K2, magnesium): $25-$40/month
- Without Insurance: 100% out-of-pocket, as most health insurance does not cover OTC supplements.
- With Insurance: Can sometimes be reimbursed via FSA/HSA accounts if medically prescribed.
-
Nutritional Counseling:
- Per Session: $75-$200
- Package (e.g., 3-5 sessions): $300-$800
- Without Insurance: Full out-of-pocket.
- With Insurance: Some health insurance plans may cover, particularly if linked to a diagnosed medical condition, often with a co-pay (e.g., $20-$50).
-
Professional Fluoride Treatments:
- Per Application: $25-$75
- Without Insurance: Out-of-pocket.
- With Insurance: Often covered at 80-100% by dental insurance, especially for children.
-
Prescription-Strength Remineralizing Toothpastes/Mouthwashes:
- Per Tube/Bottle: $15-$40
- Without Insurance: Out-of-pocket.
- With Insurance: Rarely covered by dental insurance.
II. Restorative Treatment Costs (When Deficiency Leads to Decay)
These costs are incurred when prevention fails and dental work is needed to repair damage.
-
Dental Fillings:
- Amalgam (Silver):
- 1-surface: $50-$150
- 2-surface: $100-$200
- 3+ surface: $150-$250
- Composite (Tooth-Colored):
- 1-surface: $90-$200
- 2-surface: $150-$300
- 3+ surface: $250-$450
- Without Insurance: Full out-of-pocket.
- With Insurance: Basic services typically covered at 50-80% after deductible.
- Amalgam (Silver):
-
Dental Bonding:
- Per Tooth: $300-$600
- Without Insurance: Full out-of-pocket.
- With Insurance: May be considered cosmetic (not covered) or restorative (partially covered, e.g., 20-50%).
-
Dental Crowns:
- Porcelain Fused to Metal (PFM): $800-$1,500
- All-Ceramic/Porcelain: $1,000-$2,000
- Gold/Metal: $1,200-$2,500
- Without Insurance: Full out-of-pocket.
- With Insurance: Major services typically covered at 20-50% after deductible, often with waiting periods and annual maximums.
-
Root Canal Treatment (if decay reaches the pulp):
- Front Tooth: $700-$1,200
- Premolar: $800-$1,500
- Molar: $1,000-$2,000
- (Crown often needed afterwards): Additional $800-$2,500
- Without Insurance: Full out-of-pocket.
- With Insurance: Basic/Major services, typically 50-80% covered for the root canal, with separate coverage for the crown.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental practices offer internal payment plans, allowing patients to spread the cost of treatment over several months, often interest-free.
- Third-Party Financing (e.g., CareCredit, LendingClub): These companies offer specialized healthcare credit cards or loans with various interest rates and payment terms, some offering 0% APR for a promotional period.
- Dental Savings Plans: Not insurance, but a membership program where you pay an annual fee and receive discounts (typically 10-60%) on dental procedures from participating dentists.
- Flexible Spending Accounts (FSAs) & Health Savings Accounts (HSAs): These tax-advantaged accounts allow you to save money for qualified medical and dental expenses.
Cost-Saving Tips:
- Prioritize Prevention: The single most effective way to save money is to prevent dental problems in the first place through good diet, hygiene, and regular check-ups.
- Maximize Insurance Benefits: Understand your plan's coverage, annual maximums, and deductibles. Schedule treatments strategically.
- Ask for Fee Estimates: Always request a detailed cost estimate from your dentist before any major procedure.
- Compare Prices: For extensive work, it's acceptable to get second opinions and compare pricing from different reputable dentists.
- Utilize Dental Schools: Dental school clinics often offer services at a reduced cost, performed by supervised students.
Investing in your calcium intake and preventive dental care can save you thousands of dollars in restorative treatments over your lifetime.
Frequently Asked Questions
How much calcium do I need daily for healthy teeth?
For most adults, the recommended daily allowance (RDA) of calcium is 1,000 mg. For women over 50 and men over 70, it increases to 1,200 mg. Children and adolescents (9-18 years) need 1,300 mg. It's also crucial to get 600-800 IU of Vitamin D daily, as it's essential for calcium absorption.
Are calcium supplements better than food sources for teeth?
No, food sources are generally preferred. Dietary calcium comes with other beneficial nutrients that aid absorption and overall health, such as Vitamin K2 and magnesium. Supplements are best used to bridge the gap when dietary intake is insufficient or for individuals with specific medical conditions that impair absorption, and should always be discussed with a healthcare professional.
Can calcium reverse tooth decay?
Calcium, combined with phosphate and fluoride, can reverse early tooth decay in the form of demineralization (white spot lesions) through the natural process of remineralization. However, it cannot reverse established cavities (holes in the tooth). Once a cavity has formed, it typically requires a dental filling or other restorative treatment.
What's the best form of calcium supplement for dental health?
The "best" form depends on individual needs. Calcium carbonate offers the highest elemental calcium and is most effective when taken with food. Calcium citrate is well-absorbed with or without food and may be better for those with sensitive stomachs or low stomach acid. Always look for supplements that include Vitamin D for optimal absorption.
Does calcium help with sensitive teeth?
Yes, calcium plays a role in reducing tooth sensitivity. By supporting the remineralization process, calcium helps to strengthen and rebuild weakened enamel, which can reduce the exposure of dentin tubules and thereby decrease sensitivity to hot, cold, or sweet stimuli. Remineralizing toothpastes often contain calcium compounds to aid this process directly.
How long does it take to see results from increased calcium intake for teeth?
You won't see immediate changes, as remineralization is a slow, ongoing process. Systemic benefits (like improved bone density) take months or even years. For dental health, consistent dietary intake and good oral hygiene habits over several weeks to months can help strengthen enamel and reduce the progression of early demineralization. Regular dental check-ups are key to monitoring progress.
Are there risks to taking too much calcium?
Yes, excessive calcium intake, primarily from high-dose supplements, can lead to hypercalcemia (too much calcium in the blood), which may cause symptoms like nausea, constipation, kidney stones, and potentially more serious cardiovascular issues. It's important to adhere to the recommended daily allowance and consult a doctor before taking supplements, especially if consuming more than 2,000-2,500 mg per day.
What other nutrients are important for calcium absorption and dental health?
Vitamin D is crucial for calcium absorption from the gut. Vitamin K2 helps direct calcium to bones and teeth and away from soft tissues like arteries. Magnesium aids in Vitamin D activation and plays a role in enamel formation. Phosphorus is the other primary mineral alongside calcium that forms hydroxyapatite, the main component of teeth.
Does taking calcium supplements cause constipation?
Calcium carbonate, a common form of calcium supplement, is known to sometimes cause constipation, bloating, or gas. Calcium citrate is generally less likely to cause these digestive side effects. If you experience constipation, discuss it with your doctor or dentist; they may recommend switching to a different form or adjusting your intake.
Can pregnant women take calcium supplements for their teeth?
Yes, pregnant and breastfeeding women have increased calcium needs (typically 1,000 mg per day) to support both their own health and fetal development/milk production. Calcium is vital for the baby's developing teeth and bones. However, any supplementation during pregnancy should always be discussed and approved by an OB/GYN or healthcare provider to ensure appropriate dosage and safety.
When to See a Dentist: Don't Wait for a Crisis
While this guide emphasizes the importance of calcium for preventive dental health, it's crucial to know when to seek professional dental care. Certain signs and symptoms indicate that routine calcium intake and good hygiene alone are not enough and that a dentist's intervention is needed.
Immediate Attention (Emergency or Urgent Care within Days):
- Sudden, Severe Tooth Pain: Especially if it's constant, throbbing, or wakes you up at night, this can indicate deep decay reaching the tooth's pulp, an infection, or a fracture.
- Swelling in Your Gums or Face: This is a strong indicator of a serious infection (abscess) that requires immediate treatment to prevent it from spreading.
- Loose or Shifting Teeth (in adults): While calcium deficiency can weaken bone over time, acutely loose teeth can be a sign of advanced gum disease, trauma, or significant bone loss requiring urgent evaluation.
- Chipped or Broken Tooth (especially if painful or exposing dentin): This can lead to increased sensitivity and potential infection if not treated promptly.
Scheduled Appointment (Within Weeks to a Month):
- Persistent Tooth Sensitivity: If you experience ongoing sensitivity to hot, cold, or sweet foods/drinks that doesn't improve with over-the-counter sensitive toothpastes, it could be a sign of enamel erosion, receding gums, or early decay due to demineralization.
- Noticeable White Spots or Dull Areas on Enamel: These are early signs of demineralization that your dentist can assess and treat with fluoride or remineralizing agents before they become cavities.
- New Cavities or Enlarging Fillings: If you suspect a new cavity (dark spot, sticky area, or small hole) or notice that an existing filling appears to be failing, schedule an appointment for evaluation and treatment.
- Bleeding Gums During Brushing/Flossing: While not directly a calcium issue, it indicates gum inflammation (gingivitis or periodontitis), which can indirectly impact tooth support.
- Concerns About Your Diet or Supplementation: If you are struggling to meet your calcium needs, suspect a deficiency, or have questions about which calcium vitamins for teeth might be right for you, consult your dentist for personalized advice.
Routine Care (Every Six Months):
- Regular Check-ups and Cleanings: Even if you have no specific concerns, these routine visits are vital for preventive care. Your dentist can detect problems early, provide professional cleanings, and apply fluoride treatments to strengthen your teeth, making them more resilient to demineralization.
Red Flags: Never ignore persistent pain, swelling, or changes in your teeth or gums. While calcium is crucial, it's not a substitute for professional dental care. Early intervention is always the best approach to maintain your oral health and prevent more serious and costly problems down the line.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Are Calcium Deposits on Teeth
Are you one of the millions of Americans who notices a stubborn, yellowish buildup on your teeth despite regular brushing? You're likely experiencing what many refer to as "calcium deposits on teeth." This common dental concern, medically known as dental calculus or tartar, affects a vast ma
February 23, 2026
Calcium Good for Teeth: Complete Guide
More than 99% of your body's calcium resides in your bones and teeth, making it an undeniable cornerstone of skeletal and oral health. But did you know that an estimated 42% of American adults don't get enough calcium from their diet? This staggering statistic underscores a critical question
February 23, 2026
What Do Bulimia Teeth Look Like
"Bulimia teeth" refers to the specific and often severe damage that the self-induced vomiting characteristic of bulimia nervosa inflicts on a person's oral health. It's a critical issue, affecting approximately 1.5% of women and 0.5% of men in the US at some point in their lives, with many more
February 23, 2026

Erosion in Teeth: Complete Guide
Erosion in Teeth: Complete Guide
February 23, 2026