Calcium Deposit on Teeth: Complete Guide
Key Takeaways
- It's a common misconception that our teeth are static, unyielding structures. In reality, they are constantly interacting with our diet, oral hygiene, and unique biological makeup. One widespread issue that affects millions of Americans is the accumulation of calcium deposit on teeth, often visi
It's a common misconception that our teeth are static, unyielding structures. In reality, they are constantly interacting with our diet, oral hygiene, and unique biological makeup. One widespread issue that affects millions of Americans is the accumulation of calcium deposit on teeth, often visible as a hard, yellowish-brown substance. In fact, studies show that over 68% of adults aged 30 and older have some form of periodontal disease, often stemming from these very deposits. This seemingly innocuous buildup isn't just an aesthetic concern; it's a critical indicator of compromised oral health that can lead to serious problems like gum disease, tooth decay, and even tooth loss if left unaddressed. Understanding what these deposits are, why they form, and how to effectively manage them is paramount to maintaining a healthy smile and preventing more severe dental issues. This comprehensive guide will delve into every aspect of calcium deposits on teeth, from their formation and identification to the latest treatment options, prevention strategies, and essential considerations for all ages.
Key Takeaways:
- Calcium deposits on teeth are primarily dental calculus (tartar), hardened plaque formed by minerals in saliva. It's not excess calcium from supplements but a byproduct of poor oral hygiene and mineral-rich saliva.
- Regular dental cleanings are the only way to remove established calculus. Brushing and flossing effectively prevent its formation but cannot remove it once hardened.
- Professional scaling and root planing cost between $250 and $2,000 per quadrant without insurance, depending on severity and location, with full mouth deep cleaning potentially reaching $3,000-$4,500. Insurance typically covers a significant portion.
- Prevention is key and cost-effective. Diligent brushing twice daily, flossing daily, using fluoride toothpaste, and regular professional cleanings (every 6 months, typically $75-$200 per visit without insurance) are crucial.
- Untreated calculus leads to gum inflammation (gingivitis) and can progress to severe periodontal disease, potentially causing bone loss, loose teeth, and even systemic health issues like heart disease and diabetes complications.
- The process of removing calculus is generally well-tolerated. While scaling might cause some discomfort, local anesthetic can be used for deeper cleaning procedures. Recovery is usually quick, with minor sensitivity being common.
- Children are also susceptible to calculus buildup, necessitating good early oral hygiene habits and regular pediatric dental check-ups to prevent future problems.

What It Is / Overview
When dental professionals talk about "calcium deposit on teeth," they are primarily referring to dental calculus, more commonly known as tartar. This substance is a hardened form of dental plaque. To understand calculus, we first need to understand plaque.
Dental plaque is a colorless, sticky film of bacteria that constantly forms on your teeth. It consists of bacteria, food particles, and saliva components. If plaque is not removed through regular and effective brushing and flossing, the minerals present in your saliva—chiefly calcium and phosphate—begin to integrate into the plaque matrix. This process, known as mineralization, causes the soft plaque to harden into calculus.
Calculus can form both above the gumline (supragingival calculus) and below the gumline (subgingival calculus). Supragingival calculus is typically yellowish or brownish and visible, often accumulating near salivary gland openings, such as on the inner surfaces of your lower front teeth or the outer surfaces of your upper molars. Subgingival calculus, on the other hand, forms in the pockets between your teeth and gums. It is usually darker, ranging from dark brown to black, due to absorbing blood pigments from inflamed gum tissue.
It's important to clarify that this "calcium deposit" isn't a sign of too much calcium intake in your diet, nor is it related to calcium supplements. Instead, it's a consequence of the natural mineral content of your saliva interacting with neglected plaque. While calcium is vital for strong teeth and bones, its role in calculus formation is about its presence in saliva, not necessarily dietary excess.
Once plaque hardens into calculus, it creates a rough, porous surface that provides an ideal environment for more plaque to adhere and grow. This vicious cycle exacerbates bacterial accumulation, making it even more challenging to clean your teeth effectively. The presence of calculus is a significant risk factor for both gingivitis (gum inflammation) and periodontitis (a more severe form of gum disease that affects the bone supporting your teeth).
Types / Variations
Calcium deposits on teeth primarily manifest as two main types of calculus, distinguished by their location and characteristics:
Supragingival Calculus
Location: This type forms above the gum line (the visible part of your teeth). It's commonly found on the lingual (tongue-facing) surfaces of the lower front teeth and the buccal (cheek-facing) surfaces of the upper molars, areas close to the major salivary gland ducts. Appearance: Typically yellowish-white or creamy, but can darken to brown or black due to staining from food, beverages (like coffee, tea, red wine), or tobacco. It has a rough, uneven texture. Composition: Primarily composed of calcium phosphate, calcium carbonate, and magnesium phosphate, along with bacterial cells, food debris, and epithelial cells. Detection: Often visible to the naked eye as a rough, gritty buildup. A dental professional can easily identify it during an examination. Impact: While primarily an aesthetic concern, its rough surface provides a haven for plaque bacteria, leading to gingivitis (inflamed, bleeding gums) and contributing to bad breath.
Subgingival Calculus
Location: This type forms below the gum line, within the gingival sulcus (the shallow space between the tooth and the gum) and in periodontal pockets that deepen with gum disease. Appearance: Usually darker in color—brownish-black to greenish-black. This darker hue is due to the presence of blood products (hemoglobin) that seep from inflamed gum tissues into the calculus matrix. It's often denser and harder than supragingival calculus. Composition: Similar to supragingival calculus but tends to have a higher proportion of calcium phosphate and magnesium phosphate. It also contains bacterial cells, bacterial toxins, and inflammatory mediators. Detection: Not visible to the naked eye. A dental professional uses a periodontal probe and an explorer to detect it. Its presence indicates gum recession and potential periodontal pocketing. Impact: This is the more dangerous type of calculus. Its presence irritates the gum tissue, perpetuates inflammation, and provides a continuous reservoir for harmful bacteria and their toxins. This leads to chronic inflammation, deepening of periodontal pockets, progressive bone loss around the teeth, and eventually, tooth mobility and loss if left untreated. This is a key factor in the progression of periodontitis.
Pro Tip: While plaque is soft and can be removed with a toothbrush and floss, calculus is hard and firmly attached to the tooth surface. Once it has mineralized into calculus, only professional dental instruments can effectively remove it. No amount of brushing or flossing will scrape it off.
Causes / Why It Happens
The formation of calcium deposits, or dental calculus, is a multi-factorial process influenced by oral hygiene habits, individual biology, and dietary choices. Understanding these causes is crucial for effective prevention.
1. Inadequate Oral Hygiene
This is by far the most significant contributing factor. When plaque is not consistently and thoroughly removed from tooth surfaces and along the gumline through daily brushing and flossing, it remains on the teeth. Within 24-72 hours, this soft plaque begins to harden as minerals from saliva become incorporated into its structure.
- Infrequent Brushing: Not brushing at least twice a day allows plaque to accumulate rapidly.
- Ineffective Brushing: Brushing too quickly, too softly, or missing areas (e.g., the backs of teeth, gumline) leaves plaque undisturbed.
- Lack of Flossing: Brushing alone cleans only about 60% of tooth surfaces. Flossing is essential to remove plaque and food particles from between teeth and under the gumline, areas where calculus frequently forms.
2. Saliva Composition
The unique chemistry of an individual's saliva plays a critical role.
- High Mineral Content: Saliva that is naturally richer in calcium and phosphate ions can accelerate the mineralization of plaque into calculus. This is why some people seem to develop tartar more quickly than others, even with similar hygiene habits.
- Higher pH: Saliva with a higher pH (more alkaline) can also contribute to faster calculus formation, as it promotes the precipitation of calcium phosphate.
- Reduced Saliva Flow (Xerostomia): While seemingly counterintuitive, reduced saliva flow can lead to increased plaque accumulation because saliva naturally helps rinse away food debris and neutralize acids. However, the composition of the remaining saliva can still lead to mineralization.
3. Diet
What you eat and drink can influence plaque formation and, consequently, calculus buildup.
- Sugary and Starchy Foods: A diet high in refined carbohydrates (sugars and starches) feeds the bacteria in your mouth, causing them to produce more acid and multiply rapidly. This leads to increased plaque formation.
- Acidic Foods and Drinks: While not directly causing calculus, acidic foods and drinks (soda, fruit juices, citrus) can weaken enamel, making teeth more susceptible to bacterial adhesion in some instances, though their primary role is in erosion and decay.
- Soft, Sticky Foods: Foods that stick to teeth for long periods provide a prolonged food source for bacteria, contributing to plaque buildup.
4. Smoking and Tobacco Use
Tobacco products, whether smoked or chewed, significantly increase the risk of calculus formation and gum disease.
- Reduced Saliva Flow: Tobacco can reduce saliva production, hindering the natural cleansing process.
- Altered Oral Environment: It creates an oral environment that is more conducive to the growth of harmful bacteria and the adherence of plaque.
- Gum Inflammation: Tobacco use makes gums more susceptible to inflammation, which can further exacerbate the problem by providing an ideal environment for subgingival calculus.
5. Age
The risk of calculus formation tends to increase with age. Years of accumulation, changes in diet, and potentially less diligent oral hygiene over time can contribute to increased deposits.
6. Certain Medications and Health Conditions
Some medications can cause dry mouth, which reduces saliva's protective effects, leading to increased plaque and calculus. Systemic diseases like diabetes can also compromise oral health, making individuals more prone to gum issues and calculus buildup.
7. Tooth Alignment and Dental Restorations
- Crowded or Misaligned Teeth: Teeth that are crowded or overlapping create crevices and hard-to-reach areas where plaque can easily accumulate and be missed by brushing and flossing.
- Rough Fillings or Restorations: Imperfect or rough edges on fillings, crowns, or other dental restorations can create retention areas for plaque.
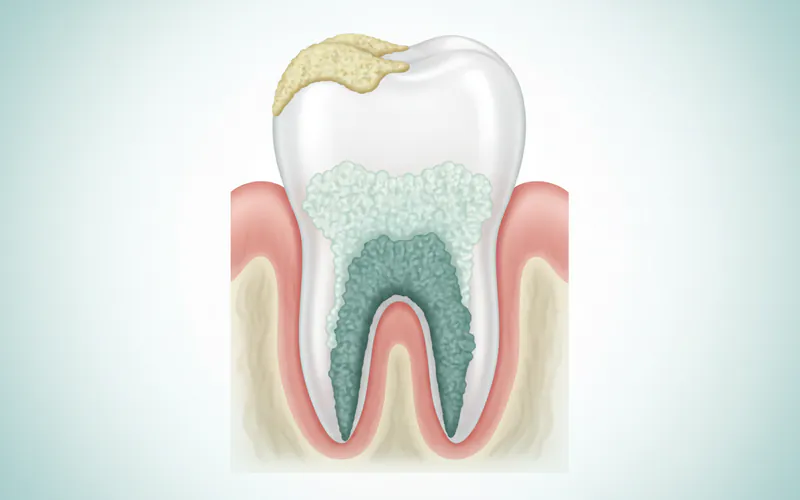
Signs and Symptoms
Identifying calcium deposits (calculus) on your teeth often involves both visual cues and tactile sensations. While a dental professional can definitively diagnose and measure these deposits, you might notice some signs yourself.
Visible Signs:
- Yellow or Brownish Stains: The most common visual indicator is a visible accumulation of yellowish or brownish material, particularly along the gumline or between teeth. This is typically supragingival calculus.
- Rough Texture: You might feel a rough or bumpy surface on your teeth, especially with your tongue, even after brushing. This texture provides a foothold for further plaque accumulation.
- Bad Breath (Halitosis): Calculus provides an ideal breeding ground for bacteria, many of which produce foul-smelling gases. Persistent bad breath that doesn't improve with brushing and mouthwash can be a sign of significant calculus buildup.
- Receding Gums: As calculus irritates the gum tissue, it can lead to inflammation and eventually gum recession, where the gum tissue pulls away from the tooth roots, making the teeth appear longer.
- Bleeding Gums: Healthy gums should not bleed when you brush or floss. If your gums frequently bleed, it's a strong indicator of gingivitis, often triggered or exacerbated by calculus.
- Inflamed, Swollen Gums: Gums that appear red, swollen, or tender to the touch are characteristic signs of inflammation caused by bacterial irritation from plaque and calculus.
Less Obvious Signs (often detected by a dentist):
- Periodontal Pockets: During a dental exam, a dentist or hygienist uses a periodontal probe to measure the depth of the gum pockets around your teeth. Deeper pockets (over 3mm) can indicate subgingival calculus and bone loss.
- Increased Tooth Sensitivity: While not a direct sign of calculus, the gum recession caused by calculus can expose sensitive tooth roots.
Pro Tip: Don't wait until you see visible signs of calculus. Regular dental check-ups are essential because subgingival calculus, the more harmful type, is not visible to the naked eye and requires professional detection.
Treatment Options
Once plaque has hardened into calculus, it cannot be removed with a toothbrush or dental floss. Professional intervention is required. The primary treatment for calcium deposits on teeth is a professional dental cleaning, which may range from a routine prophylaxis to a deep cleaning, depending on the severity of the buildup and the presence of gum disease.
1. Routine Dental Cleaning (Prophylaxis)
- What it is: A standard cleaning performed for individuals with healthy gums or mild gingivitis. It primarily targets supragingival calculus and plaque.
- Process: A dental hygienist or dentist uses specialized instruments to manually scrape away calculus (scaling) and then polish the teeth to remove stains and smooth the tooth surfaces.
- Pros:
- Effective for preventing gum disease and maintaining oral health.
- Relatively quick and painless.
- Generally covered by dental insurance plans.
- Cons:
- Not sufficient for removing subgingival calculus or treating active periodontal disease.
- Cost: Typically $75 - $200 per visit without insurance.
2. Scaling and Root Planing (Deep Cleaning)
- What it is: A non-surgical procedure performed when there is subgingival calculus, gum inflammation, and early to moderate periodontal disease (characterized by periodontal pockets greater than 3mm). It's often done under local anesthesia.
- Process:
- Scaling: Involves meticulous removal of calculus, plaque, and toxins from above and below the gumline, extending into the periodontal pockets. This can be done with manual instruments (curettes and scalers) and/or ultrasonic devices.
- Root Planing: After scaling, the root surfaces are smoothed to remove any remaining calculus, bacterial toxins, and rough spots. This helps reduce inflammation, allows the gum tissue to reattach more firmly to the tooth, and makes it harder for plaque to accumulate.
- Pros:
- Highly effective in treating gingivitis and early to moderate periodontitis.
- Reduces inflammation, pocket depth, and bacterial load.
- Can prevent the progression of gum disease and tooth loss.
- Cons:
- May require local anesthesia, leading to temporary numbness.
- Can cause temporary tooth sensitivity and gum tenderness.
- Often requires multiple appointments (e.g., one quadrant per visit).
- More expensive than a routine cleaning.
- Cost: Typically $250 - $2,000 per quadrant without insurance, meaning a full mouth deep cleaning could range from $1,000 to $4,500.
3. Laser Dentistry (Adjunct Therapy)
- What it is: Lasers can be used as an adjunct to traditional scaling and root planing, especially for treating periodontal disease.
- Process: Specific dental lasers can target and vaporize bacteria and diseased tissue within periodontal pockets, often with less bleeding and discomfort than conventional methods. They are used to enhance the effectiveness of mechanical debridement.
- Pros:
- Potentially less invasive with minimal bleeding.
- Promotes faster healing in some cases.
- Can kill bacteria effectively.
- Cons:
- Often an additional cost to scaling and root planing.
- Not all dental practices have laser technology.
- Long-term efficacy is still an area of ongoing research compared to traditional methods for calculus removal.
- Cost: Additional $100-$300 per quadrant when used with scaling and root planing.
4. Antimicrobial Rinses and Local Antibiotics
- What it is: Used in conjunction with scaling and root planing, especially for moderate to severe periodontal disease.
- Process:
- Antimicrobial Rinses: Chlorhexidine gluconate rinses can be prescribed for short-term use to reduce bacterial levels after deep cleaning.
- Local Antibiotics: Small antibiotic gels, chips, or microspheres can be placed directly into deep periodontal pockets after scaling and root planing to provide sustained release of medication and further reduce bacterial load.
- Pros:
- Enhances the effects of mechanical cleaning.
- Targets specific bacteria causing gum disease.
- Cons:
- Not a standalone treatment for calculus.
- Chlorhexidine can cause temporary staining and taste alteration.
- Antibiotics may have side effects.
- Cost: Rinses $15-$30, local antibiotics $50-$150 per site.
5. Periodontal Surgery (for advanced cases)
- What it is: If non-surgical treatments are insufficient to manage advanced periodontal disease, surgical options may be recommended.
- Process: Procedures like flap surgery (gingival flap surgery) allow the dentist to lift the gum tissue back, thoroughly remove calculus from root surfaces, and reshape bone where necessary. Other procedures include bone grafting or guided tissue regeneration.
- Pros:
- Can treat severe periodontitis and save teeth that would otherwise be lost.
- Can reduce pocket depths significantly.
- Cons:
- Invasive, with a longer recovery period.
- More expensive.
- Potential for post-operative discomfort, swelling, and sensitivity.
- Cost: Ranges from $500 to $10,000+ depending on the complexity and number of areas treated.
Pro Tip: The best "treatment" is always prevention. Consistent and effective oral hygiene, combined with regular professional cleanings, can significantly reduce your need for more intensive and costly treatments like deep cleaning or surgery. The American Dental Association (ADA) recommends routine dental check-ups and cleanings at least once a year, and often every six months for most individuals.
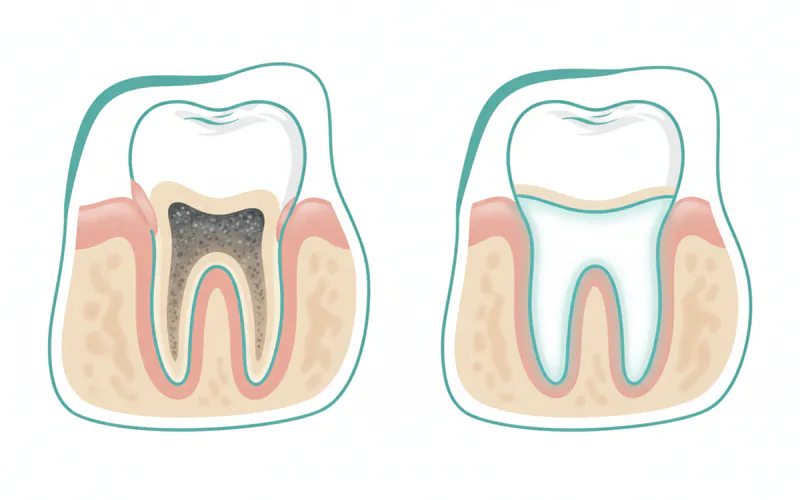
Step-by-Step Process: What to Expect During Treatment
The process of removing calcium deposits (calculus) varies depending on the severity of the buildup and whether you're receiving a routine cleaning or a deep cleaning (scaling and root planing).
For a Routine Dental Cleaning (Prophylaxis):
- Dental Examination: The hygienist or dentist will first perform a visual examination of your teeth and gums, sometimes using a small mirror. They will look for any signs of decay, gum inflammation (gingivitis), or significant calculus buildup.
- Plaque and Calculus Detection: They may use a dental explorer to feel for rough spots (calculus) on your tooth surfaces.
- Scaling (Calculus Removal): Using specialized instruments, either manual scalers and curettes or an ultrasonic scaler, the hygienist will carefully scrape away calculus from the tooth surfaces, especially along the gumline.
- Ultrasonic Scaler: This device uses high-frequency vibrations to break down and dislodge calculus. It also sprays a fine mist of water to wash away debris and cool the tip. It's often preferred for larger deposits.
- Hand Instruments: Manual scalers are used to meticulously remove smaller deposits and ensure thoroughness, particularly in tight spaces.
- Polishing: After scaling, a rotating rubber cup with a gritty prophylactic paste is used to polish the tooth surfaces. This removes surface stains and leaves the teeth feeling smooth, making it harder for plaque to adhere.
- Flossing: The hygienist will thoroughly floss between your teeth to remove any remaining paste and check that all areas are clean.
- Fluoride Treatment (Optional but Recommended): A fluoride gel, foam, or varnish may be applied to your teeth. Fluoride helps strengthen tooth enamel and makes it more resistant to decay.
- Final Rinse: You'll rinse your mouth to wash away any debris.

The entire routine cleaning process usually takes about 30-60 minutes. It's generally not painful, though you might experience minor pressure or vibrations.
For Scaling and Root Planing (Deep Cleaning):
This procedure is more involved and often requires local anesthesia. It's typically performed in quadrants of the mouth (e.g., upper left, lower left) over 2-4 appointments, each lasting 60-90 minutes.
- Local Anesthesia: Before starting, the dentist or hygienist will administer a local anesthetic to numb the gum tissue and teeth in the specific area being treated. This ensures you remain comfortable throughout the procedure.
- Periodontal Examination and Charting: Before or during the procedure, detailed measurements of your periodontal pockets will be taken and recorded.
- Deep Scaling: Using both ultrasonic and hand instruments, the hygienist will meticulously remove calculus, plaque, and bacterial toxins from the tooth surfaces, extending deep into the periodontal pockets, well below the gumline. This is a more thorough and time-consuming process than routine scaling.
- Root Planing: Once the calculus is removed, the root surfaces of the teeth are carefully smoothed. This process removes microscopic amounts of the root surface, eliminating bacterial toxins and rough spots. The goal is to create a clean, smooth surface that discourages bacterial re-colonization and allows the gum tissue to reattach firmly.
- Irrigation (Optional): Some dentists may irrigate the pockets with an antimicrobial solution (like chlorhexidine) after scaling and root planing to further reduce bacteria.
- Local Antibiotic Placement (If necessary): In some cases, a slow-release antimicrobial agent may be placed into particularly deep or persistent pockets.
- Post-Procedure Instructions: Once the procedure is complete for that quadrant, you will receive detailed instructions on post-treatment care.
You might be asked to return for a follow-up appointment (often called a "re-evaluation" or "perio maintenance") 4-6 weeks later to check the healing of your gums and determine if further treatment is needed. After deep cleaning, patients typically transition to more frequent professional cleanings, often every 3-4 months, known as periodontal maintenance, to prevent recurrence.
Cost and Insurance
Understanding the financial aspect of treating calcium deposits on teeth is crucial, as costs can vary significantly based on the type of treatment, geographic location, and insurance coverage. All costs mentioned below are general US ranges and can fluctuate.
Average US Costs (without insurance):
| Procedure Type | Description | Average Cost Range (Per Visit/Quadrant) |
|---|---|---|
| Routine Dental Cleaning | (Prophylaxis) For healthy gums/mild gingivitis, supragingival calculus. | $75 - $200 (per visit) |
| Scaling and Root Planing (SRP) | (Deep Cleaning) For subgingival calculus, moderate periodontitis. | $250 - $500 (per quadrant) |
| Full Mouth Deep Cleaning (SRP) | Total cost for all four quadrants. | $1,000 - $2,000+ (full mouth) |
| Local Anesthesia (per quadrant) | Often included for SRP, but can be separate. | $25 - $75 |
| Local Antibiotic Application | For specific deep pockets (e.g., Arestin). | $50 - $150 (per site) |
| Periodontal Maintenance | Cleanings after SRP, typically every 3-4 months. | $100 - $300 (per visit) |
| Laser Debridement (Adjunct) | Used with SRP for enhanced bacterial reduction. | $100 - $300 (per quadrant, additional) |
| Periodontal Surgery | For advanced gum disease, bone grafts, flap surgery. | $500 - $10,000+ (highly variable) |
Regional Cost Variations: Costs can be higher in major metropolitan areas (e.g., New York City, Los Angeles, Boston) and lower in rural or less populated areas. For example, a routine cleaning might be $100 in rural Kansas but $180 in Manhattan.
Insurance Coverage Details:
Most dental insurance plans (PPO, HMO, DHMO) offer coverage for treatments related to calculus removal, but the extent of coverage varies significantly.
- Routine Cleanings (Prophylaxis): Typically, dental insurance plans cover 80-100% of the cost for two routine cleanings per year (every six months). Some plans might cover up to four if medically necessary (e.g., for specific health conditions like diabetes).
- Scaling and Root Planing (Deep Cleaning): This is considered a "major" or "basic" procedure by most insurance companies. Coverage usually ranges from 50-80% of the cost after your deductible is met. Many plans have waiting periods (e.g., 6-12 months) before they cover major procedures. Some plans also limit SRP to once every 2-3 years for the same area.
- Periodontal Maintenance: After deep cleaning, subsequent maintenance cleanings are crucial. Insurance typically covers these at a similar rate to routine cleanings (e.g., 80%) but may limit the frequency (e.g., four per year) or require specific coding from the dentist to differentiate them from standard cleanings.
- Local Anesthesia: Often covered as part of the procedure or reimbursed at a high percentage (e.g., 80-100%).
- Local Antibiotics: Coverage for these can be hit-or-miss. Some plans cover them; others may classify them as an elective or non-covered service.
- Laser Therapy and Periodontal Surgery: These procedures often fall under "major" services and may have lower coverage (e.g., 50%) or specific limitations. Pre-authorization from your insurance company is highly recommended for any surgical procedure.
Payment Plans and Financing Options:
For out-of-pocket costs, many dental offices offer:
- In-house Payment Plans: Monthly installments directly with the practice.
- Third-Party Financing: Companies like CareCredit or LendingClub offer healthcare credit cards with deferred interest options for qualified patients.
- Dental Discount Plans: Not insurance, but provides a discount on services for an annual fee. Can save 10-60% on procedures.
Pro Tip: Always contact your dental insurance provider directly before treatment to understand your specific coverage, deductibles, annual maximums, and any waiting periods. Provide the dental office with your insurance information so they can submit a pre-treatment estimate (pre-authorization) for more extensive procedures like SRP or surgery.
Recovery and Aftercare
After professional calculus removal, especially scaling and root planing, proper recovery and diligent aftercare are essential to ensure healing and prevent recurrence.
Immediate Post-Treatment (First 24-72 hours):
- Sensitivity: It's very common to experience increased tooth sensitivity to hot, cold, or even sweet foods/drinks for a few days to a few weeks. This is because the root surfaces, previously covered by calculus, are now exposed.
- Management: Use toothpaste specifically designed for sensitive teeth (e.g., Sensodyne, Colgate Sensitive). Avoid extremely hot or cold foods.
- Gum Soreness and Bleeding: Your gums may be tender, swollen, or bleed slightly when brushing for a few days. This is normal as they heal from the inflammation and manipulation.
- Management: Rinse gently with warm salt water (1/2 teaspoon salt in 8 ounces of warm water) 2-3 times a day to soothe gums and aid healing. Avoid aggressive brushing or flossing initially.
- Anesthetic Effects: If local anesthesia was used, your mouth will remain numb for a few hours. Be careful not to bite your tongue or cheek.
- Management: Avoid chewing until the numbness wears off to prevent accidental injury.
- Pain Relief: Over-the-counter pain relievers like ibuprofen (Advil) or acetaminophen (Tylenol) can manage discomfort. Follow dosage instructions.
Long-Term Aftercare:
- Maintain Excellent Oral Hygiene: This is the most critical step.
- Brush: Brush your teeth thoroughly twice a day for at least two minutes with a soft-bristled toothbrush and fluoride toothpaste. Consider an electric toothbrush for superior plaque removal.
- Floss: Floss daily to clean between teeth and below the gumline. If traditional floss is difficult, consider water flossers or interdental brushes.
- Mouthwash: Use an antimicrobial mouthwash (like chlorhexidine if prescribed, but only short-term due to potential staining) or a therapeutic fluoride mouthwash as recommended by your dentist.
- Regular Dental Check-ups and Cleanings:
- For those who have undergone scaling and root planing, routine check-ups and cleanings typically shift to "periodontal maintenance" cleanings, often recommended every 3-4 months. This more frequent schedule is crucial to prevent the re-accumulation of calculus and monitor gum health, as individuals susceptible to calculus formation remain at higher risk.
- Healthy Diet: Limit sugary and starchy foods and drinks, which contribute to plaque formation. Opt for a balanced diet rich in fruits, vegetables, and whole grains.
- Avoid Tobacco: If you smoke or use other tobacco products, quitting is highly recommended. Tobacco significantly exacerbates gum disease and calculus buildup.
- Monitor for Recurrence: Pay attention to any signs of returning gum inflammation, bleeding, or sensitivity. Report any concerns to your dentist promptly.
Pro Tip: Your commitment to at-home oral care after treatment is just as important as the professional cleaning itself. Without it, calculus will quickly return, and gum disease can progress. Think of professional cleanings as hitting the "reset" button, and your daily routine as maintaining that reset.
Prevention
Preventing calcium deposits (calculus) on teeth is far more effective and less costly than treating them. The cornerstone of prevention lies in consistent, effective oral hygiene and regular professional dental care.
1. Master Your Brushing Technique
- Frequency: Brush at least twice a day, every day, for a full two minutes each time.
- Technique: Use a soft-bristled toothbrush (manual or electric) at a 45-degree angle to the gumline. Gently brush with small, circular, or back-and-forth strokes, ensuring you clean all surfaces of every tooth (outer, inner, and chewing surfaces). Pay special attention to the gumline, as plaque tends to accumulate there.
- Toothpaste: Use a fluoride toothpaste. Fluoride helps strengthen enamel, making it more resistant to acid attacks from bacteria and promoting remineralization of early demineralized spots. The ADA endorses fluoride as safe and effective for cavity prevention.
2. Floss Daily
- Consistency is Key: Flossing once a day is non-negotiable. Brushing alone misses about 40% of your tooth surfaces—the areas between your teeth and just below the gumline. These are prime locations for plaque to hide and harden into calculus.
- Proper Technique: Use about 18 inches of floss, winding most of it around your middle fingers. Guide about an inch of floss between your teeth, forming a "C" shape against one tooth, and gently slide it under the gumline. Move the floss up and down, cleaning the side of the tooth, then repeat on the adjacent tooth before moving to the next gap.
3. Use an Antimicrobial Mouthwash (Optional but Beneficial)
- An antimicrobial mouthwash can help reduce bacteria in your mouth that contribute to plaque formation. However, it's an adjunct, not a substitute, for brushing and flossing. Look for mouthwashes with ingredients like cetylpyridinium chloride (CPC) or essential oils, and always check for the ADA Seal of Acceptance.
4. Maintain a Healthy Diet
- Limit Sugary and Starchy Foods: These foods fuel the bacteria in your mouth, leading to increased plaque production. Reduce consumption of soda, candies, cookies, and highly processed carbohydrates.
- Choose Tooth-Friendly Foods: Opt for crunchy fruits and vegetables (like apples, carrots, celery) that can help naturally scrub your teeth and stimulate saliva flow. Dairy products (cheese, milk, yogurt) contain calcium and phosphate, which can help remineralize enamel, and cheese has been shown to neutralize acids.
- Hydrate with Water: Drink plenty of water throughout the day, especially after meals, to help rinse away food particles and neutralize acids.
5. Regular Professional Dental Cleanings
- Schedule: Visit your dentist or dental hygienist for professional cleanings and check-ups at least twice a year (every six months). For individuals prone to calculus buildup or with a history of gum disease, more frequent visits (e.g., every 3-4 months) may be recommended.
- Why it's essential: Even with the best home care, small amounts of plaque can be missed and harden into calculus. Dental professionals have specialized tools and training to remove these hardened deposits before they cause significant problems.
6. Avoid Tobacco Products
- Smoking and chewing tobacco significantly increase the risk of plaque and calculus buildup, gum disease, and other oral health issues. Quitting tobacco is one of the best things you can do for your oral and overall health.
7. Address Tooth Misalignment
- If you have severely crowded or misaligned teeth that make effective cleaning difficult, discuss orthodontic options with your dentist. Straightening teeth can significantly improve your ability to remove plaque and prevent calculus formation.
Pro Tip: Look for the ADA Seal of Acceptance on toothbrushes, toothpastes, and mouthwashes. This seal indicates that the product has met the ADA's criteria for safety and effectiveness.
Risks and Complications
Failing to address calcium deposits (calculus) on teeth carries a significant risk of developing various oral health complications, some of which can have systemic health implications.
1. Gingivitis
- What it is: The earliest and mildest form of gum disease, characterized by inflammation of the gums.
- How calculus contributes: Calculus provides a rough surface where bacteria thrive. These bacteria irritate the gum tissue, leading to inflammation, redness, swelling, and bleeding during brushing or flossing.
- Reversibility: Gingivitis is reversible with professional cleaning and diligent home oral hygiene. If left untreated, it can progress to periodontitis.
2. Periodontitis
- What it is: A more severe and destructive form of gum disease where the inflammation extends beyond the gums to affect the underlying bone and connective tissues supporting the teeth.
- How calculus contributes: Subgingival calculus (below the gumline) is a major culprit. The chronic inflammation it causes leads to the breakdown of the tissues and bone that hold teeth in place. Periodontal pockets deepen, accumulating more plaque and calculus, creating a vicious cycle.
- Consequences: Bone loss, gum recession, loose teeth, bad breath, pus formation, and eventually, tooth loss. Periodontitis is a leading cause of tooth loss in adults.
3. Tooth Decay (Cavities)
- How calculus contributes: Calculus creates a rough, porous surface that makes it easier for plaque to adhere. The bacteria within this plaque produce acids that erode tooth enamel, leading to cavities. While plaque directly causes decay, calculus makes plaque control much harder.
4. Halitosis (Persistent Bad Breath)
- How calculus contributes: The rough surfaces of calculus provide abundant spaces for odor-producing bacteria to colonize and flourish. These bacteria release volatile sulfur compounds that cause chronic bad breath that cannot be resolved by simple brushing or mouthwash.
5. Aesthetic Concerns
- How calculus contributes: Supragingival calculus is often yellow or brown and can accumulate significantly, becoming highly visible and unsightly. It also readily absorbs stains from food, beverages, and tobacco, further darkening the teeth.
6. Systemic Health Connections
- Cardiovascular Disease: The inflammation and bacteria associated with severe gum disease (periodontitis) have been linked to an increased risk of heart disease, stroke, and other cardiovascular problems. Bacteria from infected gums can enter the bloodstream and contribute to arterial plaque formation.
- Diabetes: There's a bidirectional relationship between diabetes and periodontal disease. Uncontrolled diabetes makes individuals more susceptible to severe gum disease, and severe gum disease can make it harder for diabetics to control their blood sugar levels.
- Respiratory Diseases: Inhaling bacteria from infected gums can potentially contribute to respiratory infections, especially in individuals with compromised immune systems.
- Pregnancy Complications: Periodontal disease has been linked to adverse pregnancy outcomes, including preterm birth and low birth weight.

7. Tooth Loss
- Ultimately, if periodontitis is left untreated, the progressive destruction of bone and connective tissue will lead to teeth becoming loose and eventually requiring extraction or falling out on their own.
Pro Tip: The progression from gingivitis to severe periodontitis and its associated systemic risks is often slow and painless until significant damage has occurred. This is why regular dental check-ups are vital, even if you don't feel any pain or obvious symptoms.
Comparison Tables
To help visualize the differences between key aspects of calcium deposits and their treatments, here are two comparison tables.
Table 1: Plaque vs. Calculus (Tartar)
| Feature | Dental Plaque | Dental Calculus (Tartar) |
|---|---|---|
| Appearance | Colorless or pale yellow, sticky film | Yellowish, brownish, or dark brown/black, hard |
| Composition | Bacteria, food debris, saliva components, proteins | Mineralized plaque (calcium, phosphate), dead bacteria |
| Texture | Soft, sticky, fuzzy | Hard, rough, brittle |
| Removability | Can be removed by daily brushing and flossing | Requires professional scaling with dental instruments |
| Impact | Direct cause of tooth decay and gingivitis | Creates a rough surface for more plaque, irritates gums, leads to periodontitis |
| Time to Form | Continuously forms, visible within hours | Forms within 24-72 hours if plaque isn't removed |
Table 2: Treatment Options Comparison
| Treatment Option | Target Deposits | Severity of Gum Disease | Anesthesia Needed | Typical US Cost Range (per Quadrant/Visit, without insurance) | Recovery Time | Main Advantage | Main Disadvantage |
|---|---|---|---|---|---|---|---|
| Routine Cleaning (Prophylaxis) | Supragingival Plaque & Calculus | Healthy gums/Mild gingivitis | Rarely | $75 - $200 (per visit) | Immediate | Preventive, quick, affordable | Not for subgingival calculus or advanced disease |
| Scaling & Root Planing (Deep Cleaning) | Supragingival & Subgingival Calculus | Early to Moderate Periodontitis | Often | $250 - $500 (per quadrant) | Few days to weeks | Effective for active gum disease, prevents progression | More invasive, potential sensitivity, multiple visits |
| Periodontal Maintenance | Light Plaque & Calculus | Post-SRP, controlled periodontitis | Rarely | $100 - $300 (per visit) | Immediate | Maintains health after deep cleaning, prevents recurrence | Requires regular, frequent visits |
| Laser Debridement (Adjunct) | Bacteria, diseased tissue | Moderate Periodontitis | Yes | $100 - $300 (additional to SRP) | Few days | Less invasive, bacterial reduction | Added cost, not standalone, limited availability |
| Periodontal Surgery | Extensive Subgingival Calculus, bone defects | Advanced Periodontitis | Yes | $500 - $10,000+ (highly variable) | Weeks to months | Can save teeth, rebuilds bone, reduces pockets | Most invasive, expensive, longer recovery |
Children / Pediatric Considerations
While often associated with adults, children can also develop calcium deposits (calculus) on their teeth. Pediatric dentists emphasize prevention and early intervention to ensure lifelong oral health.
Why Children Get Calculus:
- Poor Oral Hygiene: Just like adults, the primary cause in children is inadequate brushing and flossing. Children may not have the dexterity or discipline to clean their teeth thoroughly.
- Diet: Frequent consumption of sugary snacks and drinks increases plaque formation.
- Saliva Composition: Some children naturally have saliva with a higher mineral content, predisposing them to faster calculus formation.
- Location: Calculus in children is most commonly found on the inside surfaces of the lower front teeth and the outside surfaces of the upper molars, similar to adults, because these areas are near salivary gland ducts.
Signs in Children:
- Yellowish or brownish buildup near the gumline.
- Red, swollen, or bleeding gums.
- Bad breath.
Specific Guidance for Parents:
- Start Early: Begin cleaning your baby's gums with a soft cloth even before teeth erupt. As soon as the first tooth appears (around 6 months), start brushing twice a day with a soft-bristled toothbrush and a tiny smear of fluoride toothpaste (rice-grain size) until age 3.
- Supervise Brushing: From ages 3-6, use a pea-sized amount of fluoride toothpaste and supervise your child's brushing to ensure thoroughness. Many children need assistance or full supervision with brushing until they are about 7 or 8 years old, or until they can tie their own shoelaces, which is an indicator of sufficient dexterity.
- Flossing: Start flossing your child's teeth once a day as soon as two teeth touch.
- Regular Pediatric Dental Visits: The American Academy of Pediatric Dentistry (AAPD) recommends the first dental visit by age 1 or when the first tooth erupts. Regular check-ups every six months are crucial for monitoring oral development, providing preventive care, and removing any calculus that might form.
- Dietary Guidance: Limit sugary drinks and snacks. Encourage water consumption and a balanced diet.
- Education: Teach children about the importance of good oral hygiene in an age-appropriate manner. Make brushing and flossing a fun, consistent routine.
Pro Tip: If your child develops visible calculus, do not attempt to scrape it off at home. Only a dental professional can safely and effectively remove it without damaging the tooth enamel or gums. Early removal helps prevent gingivitis and other more serious problems.
Frequently Asked Questions
1. What exactly is calcium deposit on teeth?
Calcium deposit on teeth refers to dental calculus, commonly known as tartar. It's hardened plaque that forms when minerals from your saliva, primarily calcium and phosphate, crystallize within the sticky bacterial film (plaque) that constantly forms on your teeth. It is not caused by excessive calcium intake from your diet or supplements.
2. Can I remove calcium deposits myself at home?
No. Once plaque hardens into calculus, it is firmly attached to the tooth surface and cannot be removed by brushing, flossing, or over-the-counter products. Attempting to scrape it off yourself with household tools can damage your tooth enamel and gums, leading to more serious problems. Professional dental instruments are required for safe and effective removal.
3. How much does it cost to remove calcium deposits from teeth?
The cost varies based on the severity and type of cleaning. A routine cleaning (prophylaxis) typically costs $75-$200 without insurance. If deep cleaning (scaling and root planing) is needed for significant deposits and gum disease, it can range from $250-$500 per quadrant, totaling $1,000-$2,000+ for a full mouth. Insurance usually covers routine cleanings at 80-100% and deep cleanings at 50-80%.
4. Is the removal process painful?
Routine cleanings are generally not painful, though you might experience some pressure or mild sensitivity. For deep cleanings (scaling and root planing), local anesthesia is often used to numb the gums and teeth, making the procedure comfortable. You may experience some soreness, sensitivity, or mild bleeding for a few days afterward, which can be managed with over-the-counter pain relievers.
5. How long does it take to remove calcium deposits?
A routine cleaning usually takes 30-60 minutes. If deep cleaning (scaling and root planing) is necessary, it's often done in sections (quadrants) of the mouth over 2-4 appointments, with each appointment lasting 60-90 minutes.
6. What happens if I don't get the calcium deposits removed?
Untreated calcium deposits (calculus) lead to persistent gum inflammation (gingivitis), which can progress to periodontitis. This more severe gum disease can cause bone loss, gum recession, bad breath, loose teeth, and eventually tooth loss. It's also linked to systemic health issues like heart disease and diabetes.
7. How often should I get my teeth professionally cleaned to prevent deposits?
For most individuals with good oral health, the American Dental Association (ADA) recommends professional dental cleanings and check-ups every six months. If you are prone to calculus buildup or have a history of gum disease, your dentist may recommend more frequent "periodontal maintenance" cleanings, typically every 3-4 months.
8. Can certain foods or drinks cause calcium deposits?
Sugary and starchy foods and drinks contribute to plaque formation by feeding oral bacteria. While these don't directly cause calculus, they indirectly lead to its formation if plaque isn't thoroughly removed. Calculus is primarily formed by minerals in saliva interacting with existing plaque.
9. Are there any natural remedies to remove calculus?
No, there are no scientifically proven natural remedies or home hacks that can safely and effectively remove hardened dental calculus. Remedies like oil pulling, baking soda, or apple cider vinegar might help reduce plaque or surface stains, but they cannot remove established calculus. Rely only on professional dental care for calculus removal.
10. Does fluoride help prevent calcium deposits?
Fluoride primarily helps strengthen tooth enamel and prevent cavities by making teeth more resistant to acid attacks. While it doesn't directly prevent calculus from forming on existing plaque, it contributes to overall oral health, which indirectly reduces the conditions favorable for severe calculus accumulation.
When to See a Dentist
Recognizing when to seek professional dental care for calcium deposits is crucial for preventing severe oral health complications.
Red Flags - See a Dentist Immediately or Very Soon:
- Severe Gum Pain or Swelling: If your gums are intensely painful, significantly swollen, or have pus present, this indicates an active infection or advanced gum disease.
- Persistent Bleeding: Gums that bleed heavily or continuously when brushing, flossing, or even spontaneously, are a sign of serious inflammation or infection.
- Loose Teeth: Any noticeable loosening of teeth is a critical sign of significant bone loss due to advanced periodontal disease. This requires immediate attention to potentially save the teeth.
- Persistent Bad Breath that Worsens: While bad breath can be a sign of many things, a foul odor that doesn't improve with diligent hygiene and worsens over time, especially if accompanied by other gum symptoms, suggests significant bacterial buildup from calculus.
- Visible Abscess or Sores: Any painful bump or sore on your gums that resembles a pimple or an ulcer, particularly if it's accompanied by swelling, indicates an infection.
Routine Care Guidance - Schedule an Appointment:
- Visible Buildup: If you can see yellowish or brownish hard deposits on your teeth, especially along the gumline or between your lower front teeth.
- Rough or Gritty Feeling: If your teeth feel rough or gritty, even after brushing, it's likely due to calculus.
- Red, Tender, or Slightly Swollen Gums: These are early signs of gingivitis, often caused or exacerbated by plaque and calculus.
- Minor Gum Bleeding: If your gums bleed occasionally when brushing or flossing, it's a sign that calculus and plaque are irritating them.
- It's Been Over Six Months: If it's been more than six months since your last professional dental cleaning, it's time to schedule one, regardless of whether you notice symptoms. Regular check-ups are key to prevention and early detection.
- Increased Tooth Sensitivity: While not always due to calculus, gum recession caused by calculus can expose sensitive root surfaces.
Pro Tip: Don't ignore symptoms. Dental problems rarely resolve on their own and often worsen over time. Early intervention is always less invasive, less costly, and more effective than addressing advanced issues. Consistent communication with your dental team is essential for maintaining optimal oral health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Are Calcium Deposits on Teeth
Are you one of the millions of Americans who notices a stubborn, yellowish buildup on your teeth despite regular brushing? You're likely experiencing what many refer to as "calcium deposits on teeth." This common dental concern, medically known as dental calculus or tartar, affects a vast ma
February 23, 2026
Calcium Good for Teeth: Complete Guide
More than 99% of your body's calcium resides in your bones and teeth, making it an undeniable cornerstone of skeletal and oral health. But did you know that an estimated 42% of American adults don't get enough calcium from their diet? This staggering statistic underscores a critical question
February 23, 2026
What Do Bulimia Teeth Look Like
"Bulimia teeth" refers to the specific and often severe damage that the self-induced vomiting characteristic of bulimia nervosa inflicts on a person's oral health. It's a critical issue, affecting approximately 1.5% of women and 0.5% of men in the US at some point in their lives, with many more
February 23, 2026

Erosion in Teeth: Complete Guide
Erosion in Teeth: Complete Guide
February 23, 2026