What Are Calcium Deposits on Teeth
Key Takeaways
- Are you one of the millions of Americans who notices a stubborn, yellowish buildup on your teeth despite regular brushing? You're likely experiencing what many refer to as "calcium deposits on teeth." This common dental concern, medically known as dental calculus or tartar, affects a vast ma
What Are Calcium Deposits on Teeth
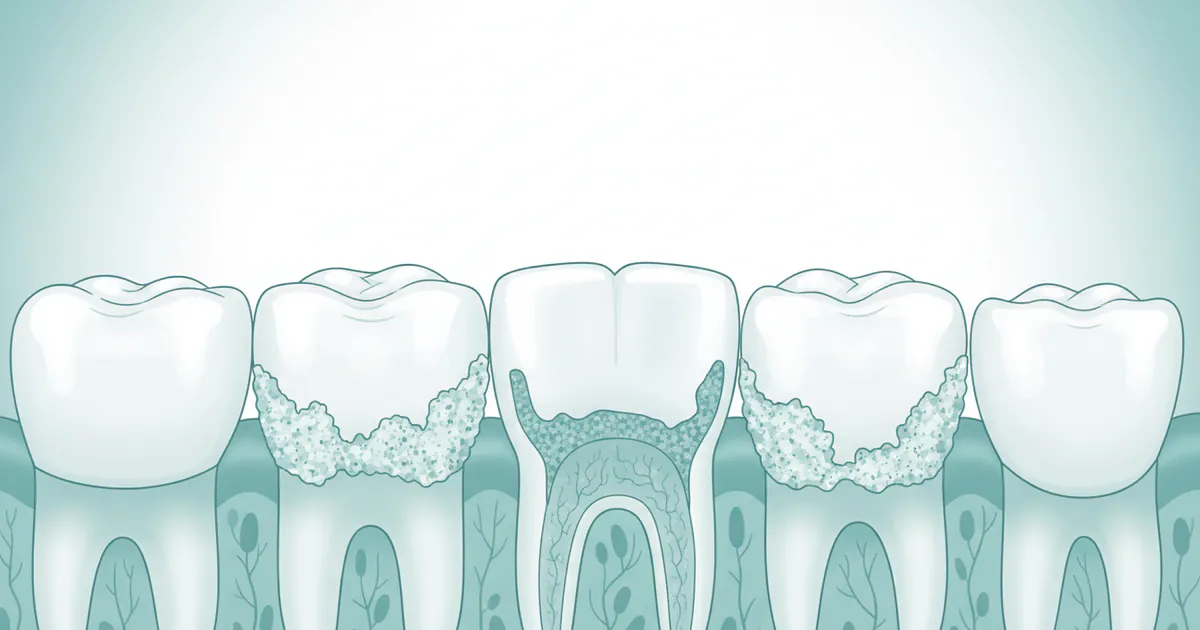
Are you one of the millions of Americans who notices a stubborn, yellowish buildup on your teeth despite regular brushing? You're likely experiencing what many refer to as "calcium deposits on teeth." This common dental concern, medically known as dental calculus or tartar, affects a vast majority of adults. In fact, research indicates that over 68% of adults develop calculus, and its presence is a significant risk factor for more serious oral health problems. But what exactly are these deposits, why do they form, and what can you do about them?
Understanding calcium deposits is crucial for maintaining optimal oral health and preventing issues like molar erosion, gum disease, and even tooth loss. These hardened mineral deposits form when plaque—a sticky film of bacteria, food particles, and saliva—is not removed effectively through daily brushing and flossing. Over time, the minerals in your saliva, primarily calcium and phosphate, cause this plaque to calcify and harden onto your tooth surfaces, making it impossible to remove with a toothbrush alone. This article from SmilePedia.net will serve as your definitive guide to understanding dental calculus, exploring its causes, symptoms, professional treatment options, and most importantly, how to prevent its formation to safeguard your smile. We'll delve into the nuances of this common issue, helping you distinguish it from other dental problems like teeth erosion and providing actionable steps to ensure your teeth remain healthy and strong.
Key Takeaways:
- Dental Calculus (Tartar): Often referred to as "calcium deposits on teeth," calculus is hardened plaque that cannot be removed by brushing or flossing alone. It's a significant risk factor for gum disease and cavities.
- Formation: Calculus forms when plaque—a sticky bacterial film—mineralizes due to calcium and phosphate in saliva. This process can start within 24-72 hours if plaque isn't removed.
- Types: Supragingival calculus forms above the gum line (visible, yellowish); subgingival calculus forms below the gum line (darker, harder to detect, more dangerous).
- Treatment: Professional dental scaling is the only effective treatment. This involves specialized instruments to scrape off the hardened deposits. Regular cleanings are essential.
- Cost: A routine dental cleaning (prophylaxis) in the US can range from $75 to $200. For significant calculus buildup requiring deep cleaning (scaling and root planing), costs can range from $250 to $800 per quadrant without insurance, potentially totaling $1,000 to $3,200 for a full mouth.
- Prevention: Excellent oral hygiene (brushing twice daily with fluoride toothpaste, flossing daily), a balanced diet, and regular dental check-ups (every 6 months) are critical for prevention.
- Distinction from Erosion: Calcium deposits (calculus) are additions to the tooth surface, while tooth erosion is the loss of tooth enamel dueused by acid. These are distinct problems needing different approaches.
What Are Calcium Deposits on Teeth / Overview
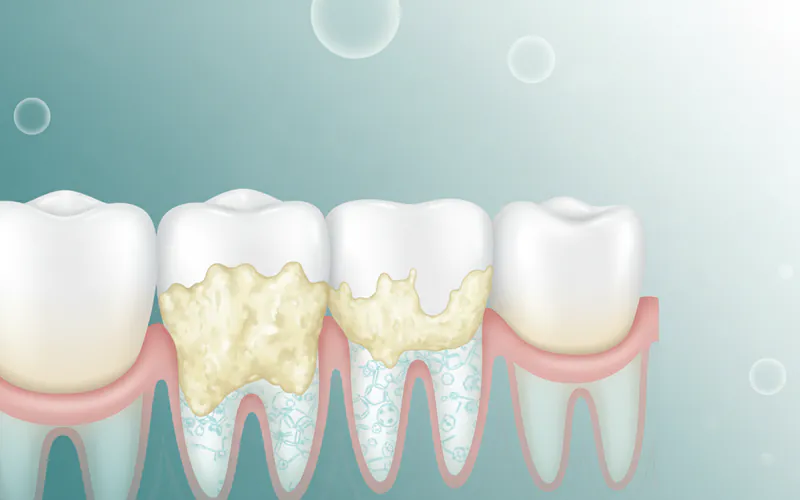
When we talk about "calcium deposits on teeth," we are primarily referring to dental calculus, commonly known as tartar. This is a hard, mineralized deposit that forms on the surfaces of your teeth and dental restorations (like fillings or crowns). It's essentially plaque that has undergone a chemical transformation, becoming rock-hard and firmly attached to the tooth structure.
Plaque itself is a colorless, sticky film of bacteria, food particles, and saliva that constantly forms on your teeth. If plaque is not meticulously removed through daily brushing and flossing, it begins to absorb minerals from your saliva, mainly calcium and phosphate. This process, known as mineralization, causes the soft plaque to harden into calculus. Once formed, calculus acts as a rough, porous surface that provides an ideal environment for more plaque to accumulate, creating a vicious cycle that exacerbates oral health problems.
It's crucial to distinguish calcium deposits (calculus) from other conditions that might sound similar but are entirely different. For instance, enamel erosion, sometimes referred to in queries about "molar erosion" or "what is teeth erosion," is the irreversible loss of tooth structure due to acidic attacks, not a buildup of material. While both calculus and erosion can compromise dental health, they are distinct problems with different origins and treatments. Calculus is an additive problem, where unwanted material accumulates, whereas erosion is a subtractive problem, where tooth material is lost. This article will focus on the former, clarifying its nature and implications.
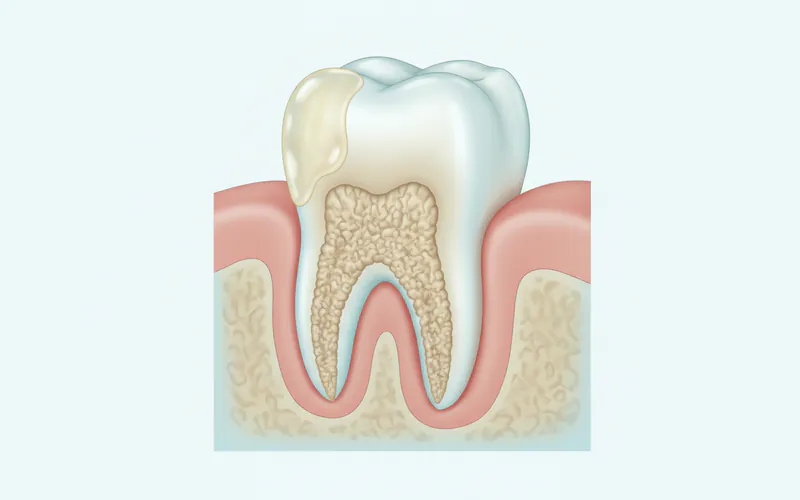
Types of Calcium Deposits (Calculus)
Dental calculus isn't a monolithic entity; it manifests in different forms and locations, each posing unique challenges and risks. Understanding these types is key to comprehending their impact on your oral health.
Supragingival Calculus
This is the type of calculus most people are familiar with, as it forms above the gum line.
- Appearance: It is typically yellowish or whitish-yellow, though it can become stained darker by tobacco, coffee, tea, or certain foods. It often has a rough, chalky texture.
- Location: Most commonly found on the lingual (tongue-facing) surfaces of the lower front teeth (incisors) and the buccal (cheek-facing) surfaces of the upper back teeth (molars). These areas are close to the salivary glands (sublingual and parotid glands, respectively), where saliva with its high mineral content bathes the teeth, accelerating mineralization.
- Detection: Supragingival calculus is often visible to the naked eye, either by you or your dentist during a routine examination.
- Risks: While primarily unsightly, supragingival calculus still provides a rough surface for further plaque accumulation, leading to cavities and contributing to gingivitis (gum inflammation).
Subgingival Calculus
This is the more insidious and dangerous form of calculus, as it forms below the gum line, within the gingival sulcus (the shallow groove between the tooth and the gum) and periodontal pockets.
- Appearance: Subgingival calculus is typically harder, denser, and darker in color—often brown or black. This darker pigmentation comes from blood pigments present in the inflamed gum tissues.
- Location: It adheres firmly to the tooth root surfaces within the periodontal pockets.
- Detection: It cannot be seen directly by the patient and often requires a dental professional to detect it using specialized instruments (periodontal probes and explorers) and dental X-rays.
- Risks: Subgingival calculus is a primary culprit in the progression of gum disease from gingivitis to periodontitis. It constantly irritates the gums, perpetuates inflammation, and provides a haven for harmful bacteria. These bacteria release toxins that destroy the supporting bone and connective tissues around the teeth, leading to deepening periodontal pockets, gum recession, tooth mobility, and eventually tooth loss if left untreated.
Causes of Calcium Deposits / Why It Happens
The formation of calcium deposits on teeth is a multi-factorial process rooted primarily in oral hygiene habits and exacerbated by various other factors.
1. Inadequate Oral Hygiene
This is the number one cause. When plaque is not thoroughly removed from tooth surfaces and along the gum line through consistent and effective brushing and flossing, it begins to mineralize. This process can start within 24 to 72 hours if plaque is left undisturbed.
- Improper Brushing: Not brushing twice daily, not brushing for two minutes, or using incorrect techniques leaves behind substantial plaque.
- Infrequent Flossing: Flossing is crucial for removing plaque and food particles from between teeth and below the gum line, areas a toothbrush cannot reach effectively.
2. Saliva Composition
Your saliva plays a dual role in oral health—it helps wash away food particles and neutralizes acids, but it also contains the minerals (calcium and phosphate) essential for calculus formation.
- High Mineral Content: Individuals with saliva that is naturally richer in calcium and phosphate ions may be more prone to faster calculus formation.
- Salivary Flow: Reduced salivary flow (xerostomia or dry mouth) can also contribute indirectly, as there's less natural rinsing action to clear away plaque.
3. Diet and Nutrition
While often associated with tooth decay, dietary choices also influence calculus formation.
- Sugary and Starchy Foods: These foods provide a feast for oral bacteria, leading to increased plaque production.
- Acidic Foods/Drinks: While directly causing teeth erosion, acidic environments can sometimes alter the oral pH in ways that might influence plaque adhesion or the speed of mineralization. However, the primary link is indirect, through general poor oral health.
4. Tobacco Use
Smoking and other forms of tobacco use significantly increase the risk and rate of calculus formation, especially subgingival calculus. Tobacco users tend to have more tenacious plaque that mineralizes more readily.
5. Genetics and Individual Susceptibility
Some individuals are simply genetically predisposed to forming calculus more rapidly or having a greater quantity of it. This can be due to variations in salivary composition, immune response, or the types of bacteria dominant in their oral microbiome.
6. Systemic Health Conditions
Certain systemic conditions, particularly those affecting the immune system or bone metabolism, can influence calculus formation or complicate its management. For example, individuals with diabetes may be more susceptible to gum inflammation, which can be worsened by calculus.
7. Orthodontic Appliances
Braces, retainers, and other orthodontic devices create more surfaces and crevices where plaque can accumulate, making oral hygiene more challenging and increasing the risk of calculus.
8. Age
As people age, the risk of calculus formation tends to increase, partly due to years of accumulated plaque and partly due to changes in salivary flow and gum recession.
Signs and Symptoms of Calcium Deposits
Recognizing the signs of calculus formation early can help you seek timely professional intervention.
- Visible Deposits: The most obvious sign is a hard, rough, yellowish, or brownish buildup on your teeth, especially near the gum line, often seen on the back of your lower front teeth or the outside of your upper molars.
- Rough Texture: You might notice a rough or bumpy surface on your teeth when you run your tongue over them. Unlike smooth enamel, calculus has a gritty feel.
- Bad Breath (Halitosis): Calculus is porous and provides an ideal surface for bacteria to thrive. These bacteria release volatile sulfur compounds, leading to persistent bad breath.
- Gum Inflammation (Gingivitis): Calculus irritates the gums, causing them to become red, swollen, tender, and prone to bleeding easily, especially during brushing or flossing. This is the hallmark of gingivitis.
- Receding Gums: In more advanced cases, prolonged irritation from calculus can lead to the gums pulling away from the teeth, exposing the tooth roots.
- Increased Tooth Sensitivity: Exposed tooth roots due to gum recession can lead to sensitivity to hot, cold, or sweet stimuli.
- Difficulty Brushing/Flossing: As calculus accumulates, it can make it harder for your toothbrush bristles or floss to effectively clean the tooth surfaces, perpetuating the problem.
- Metallic Taste in Mouth: Some individuals report a persistent metallic taste, often associated with gum inflammation and bacterial activity around calculus.
Pro Tip: If you notice any of these signs, particularly bleeding gums or visible hard deposits, schedule an appointment with your dentist promptly. Early intervention can prevent the progression to more serious gum disease.
Treatment Options for Calcium Deposits
Once calculus has formed, it's impossible to remove it effectively with regular brushing and flossing. It requires professional dental intervention. The primary treatment methods revolve around various forms of professional dental cleaning.
1. Prophylaxis (Routine Dental Cleaning)
- What it is: For individuals with minimal calculus buildup and healthy gums, a standard professional cleaning is performed. It focuses on removing plaque and calculus above the gum line (supragingival) and in the shallow gum pockets.
- Process: A dental hygienist uses hand scalers, ultrasonic instruments, or both, to meticulously scrape away deposits. This is followed by polishing the teeth to remove surface stains and smooth the enamel.
- Pros: Non-invasive, relatively quick, prevents progression of gum disease, leaves teeth feeling clean and smooth.
- Cons: Not sufficient for significant subgingival calculus or advanced gum disease.
- Best for: Patients with good oral health and regular maintenance.
2. Scaling and Root Planing (Deep Cleaning)
- What it is: This procedure is necessary when calculus has extended below the gum line (subgingival calculus) and has caused gingivitis or early to moderate periodontitis. It's often referred to as "deep cleaning."
- Process:
- Scaling: Involves meticulously removing plaque and calculus from above and below the gum line, down to the bottom of the periodontal pockets. This is typically done quadrant by quadrant (one-fourth of the mouth at a time) over multiple appointments, often with local anesthesia to ensure comfort.
- Root Planing: After scaling, the root surfaces are smoothed to remove any remaining calculus, bacterial toxins, and rough spots. This smoothing helps prevent plaque from re-adhering and allows the gum tissue to reattach more firmly to the clean root surface.
- Pros: Effectively removes subgingival calculus, reduces gum inflammation, helps shrink periodontal pockets, and can halt the progression of gum disease.
- Cons: More invasive than prophylaxis, requires local anesthesia, can cause temporary discomfort and sensitivity, takes more time (multiple appointments).
- Best for: Patients diagnosed with gingivitis or periodontitis, characterized by significant calculus below the gum line, bleeding gums, and periodontal pockets.
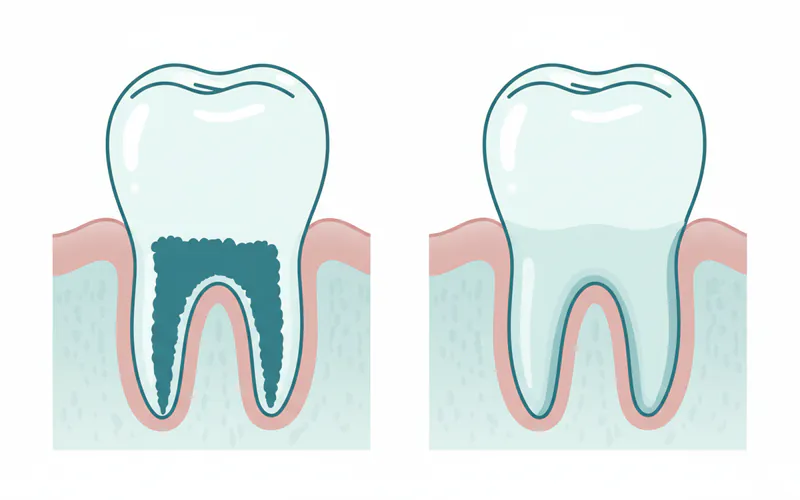
3. Adjunctive Therapies
In some cases, especially with advanced periodontitis, your dentist may recommend adjunctive therapies alongside scaling and root planing.
- Local Antibiotics: Small antibiotic gels, chips, or fibers may be placed directly into deep periodontal pockets to target specific bacteria.
- Antimicrobial Rinses: Prescription mouthwashes containing chlorhexidine can be used for a limited time to reduce bacterial load.
- Laser Therapy: Lasers can be used to remove inflamed tissue, sterilize pockets, and potentially aid in calculus removal, often as an adjunct to traditional scaling. However, the ADA's position emphasizes that lasers are not a standalone replacement for mechanical debridement.
Pro Tip: Discuss your symptoms and oral health history thoroughly with your dentist. They will conduct a comprehensive examination, including X-rays and periodontal probing, to determine the most appropriate treatment plan for your specific needs.
Step-by-Step Process of Professional Calculus Removal
Knowing what to expect during a professional dental cleaning can ease any anxiety. Here's a general overview of the process, particularly for scaling and root planing:
1. Initial Assessment and Preparation
- Examination: Your dentist or hygienist will perform a thorough examination, visually inspecting your mouth, checking for signs of inflammation, measuring pocket depths around your teeth (periodontal probing), and reviewing X-rays to assess bone levels and calculus presence.
- Anesthesia (if needed): For deep cleanings (scaling and root planing), local anesthesia will be administered to numb the specific area(s) being treated, ensuring your comfort during the procedure. This typically involves a quick injection that numbs the gums, teeth, and surrounding tissues.
2. Calculus Removal (Scaling)
- Ultrasonic Scaler: The hygienist will often start with an ultrasonic scaler. This device uses high-frequency vibrations and a continuous stream of water to break down calculus and wash away debris. The tip of the scaler vibrates against the calculus, shattering it without harming the tooth surface. The water also helps to cool the tip and flush out bacteria from the pockets.
- Hand Scalers and Curettes: After or in conjunction with the ultrasonic scaler, specialized hand instruments called scalers and curettes are used. These precisely shaped tools allow the hygienist to meticulously scrape away any remaining calculus deposits, both above and below the gum line, ensuring all surfaces are thoroughly cleaned. This step requires great skill and precision to reach into deep pockets and navigate around the tooth's anatomy.
3. Root Planing (for Deep Cleanings)
- Smoothing Root Surfaces: If you are undergoing scaling and root planing, after the calculus is removed, the hygienist will use specialized curettes to meticulously smooth the root surfaces. This process removes any embedded bacterial toxins and rough spots on the root, which helps prevent future plaque accumulation and allows the gum tissue to reattach more readily.
4. Polishing and Rinsing
- Polishing: Once all calculus and significant stains are removed, a rotating rubber cup with a gritty prophylactic paste is used to polish the tooth surfaces. This makes the enamel smooth, reducing areas where plaque can easily adhere.
- Rinsing: You'll be asked to rinse your mouth thoroughly to wash away any remaining debris.
5. Fluoride Treatment (Optional)
- Enamel Strengthening: Often, a fluoride treatment (gel, foam, or varnish) is applied after cleaning to help strengthen tooth enamel, reduce sensitivity, and protect against cavities.
6. Post-Procedure Instructions
- Aftercare: Your hygienist will provide specific instructions regarding post-treatment care, including what to expect (e.g., mild sensitivity), pain management, and proper oral hygiene techniques to maintain your clean teeth and gums.
Pro Tip: Don't hesitate to communicate any discomfort during the procedure. Your dental team is there to ensure you are as comfortable as possible.
Cost and Insurance for Calculus Removal in the US
The cost of treating calcium deposits on teeth (calculus) in the United States can vary significantly based on the type of cleaning needed, your geographical location, the dental practice, and whether you have dental insurance.

Routine Dental Cleaning (Prophylaxis - D1110)
- Without Insurance: A standard dental cleaning usually ranges from $75 to $200. In major metropolitan areas, it might lean towards the higher end or slightly exceed it.
- With Insurance: Most dental insurance plans cover 100% of the cost for two routine cleanings per year, often without a deductible or co-pay, as they are considered preventive care.
Scaling and Root Planing (Deep Cleaning - D4341, D4342)
This procedure is typically billed per quadrant of the mouth (upper right, upper left, lower right, lower left).
- Without Insurance:
- Per Quadrant: Expect to pay between $250 and $800 per quadrant.
- Full Mouth: For a full mouth deep cleaning (all four quadrants), the total cost can range from $1,000 to $3,200 or more.
- With Insurance:
- Scaling and root planing is generally covered by insurance, but usually at a lower percentage than routine cleanings, often 50% to 80% after you meet your deductible.
- You will likely have a co-pay and will be responsible for a portion of the total cost.
- Many plans have an annual maximum benefit, which can be reached quickly with deep cleaning procedures.
Adjunctive Therapies
- Local Antibiotics: If used, these can add $30 to $100 per tooth or site.
- Antimicrobial Rinses: Prescription rinses might cost $20 to $50 for a bottle.
- Laser Therapy: If used, this can add $50 to $200 per tooth or quadrant, depending on the extent and specific laser used.
Factors Influencing Cost:
- Geographic Location: Costs are generally higher in urban areas and regions with a higher cost of living.
- Dentist's Experience/Specialty: Periodontists (gum specialists) might charge slightly more than general dentists for deep cleanings.
- Severity of Condition: More extensive calculus and deeper pockets might require longer, more complex procedures, affecting the overall cost.
- Additional Procedures: If other issues like fillings or extractions are needed, these will add to the total cost.
Cost-Saving Tips:
- Preventive Care: The best way to save money is to prevent calculus buildup in the first place through excellent daily oral hygiene and regular routine cleanings.
- Dental Insurance: Maximize your insurance benefits. Understand your plan's coverage for both preventive and periodontal treatments.
- Payment Plans: Many dental offices offer in-house payment plans or work with third-party financing options (e.g., CareCredit) to break down large costs into manageable monthly payments.
- Dental Schools: Dental schools often provide services at a reduced cost, as procedures are performed by students under the supervision of experienced faculty.
- Community Clinics: Some community dental clinics offer services on a sliding scale based on income.
Recovery and Aftercare
After professional calculus removal, especially scaling and root planing, proper aftercare is essential for healing and preventing recurrence.
Immediate Post-Treatment (24-48 hours)
- Sensitivity: You might experience temporary tooth sensitivity to hot, cold, or sweet foods/drinks, especially if deep cleaning was performed. This is normal as gums heal and exposed root surfaces become accustomed to the new environment. Over-the-counter pain relievers (e.g., ibuprofen, acetaminophen) can help manage discomfort.
- Gum Soreness/Bleeding: Your gums may be sore, swollen, or bleed slightly after the procedure. This should subside within a day or two.
- Diet: Stick to soft foods for the first 24-48 hours. Avoid very hot, cold, spicy, or crunchy foods that could irritate your tender gums.
- Rinsing: Your dentist might recommend a warm salt water rinse (1/2 teaspoon salt in 8 ounces warm water) several times a day to aid healing and reduce swelling. Avoid harsh mouthwashes with alcohol for a few days.
- Brushing/Flossing: Continue gentle brushing immediately, but be very careful around sensitive areas. Flossing might be uncomfortable for a day or two, but it's important to resume as soon as possible to prevent new plaque buildup.
Long-Term Aftercare (Ongoing)
- Excellent Oral Hygiene: This is paramount.
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Consider an electric toothbrush for superior plaque removal. Brush for at least two minutes, covering all tooth surfaces and along the gum line.
- Floss Daily: Floss thoroughly once a day to remove plaque and food particles from between teeth and under the gum line. This prevents plaque from mineralizing into new calculus.
- Mouthwash: An antimicrobial mouthwash can be a helpful adjunct, but it's not a substitute for brushing and flossing.
- Regular Dental Check-ups: Adhere to your dentist's recommended schedule for follow-up appointments and routine cleanings. For individuals prone to calculus or with a history of gum disease, recall appointments might be recommended every 3-4 months instead of the standard 6 months.
- Healthy Diet: Limit sugary and starchy foods and drinks. These contribute to plaque formation. Consume a balanced diet rich in fruits, vegetables, and whole grains.
- Avoid Tobacco: If you smoke or use other tobacco products, quitting is one of the most impactful steps you can take for your oral and overall health.
- Address Underlying Issues: If dry mouth or other systemic conditions contribute to your calculus formation, discuss management strategies with your dentist and physician.
Prevention of Calcium Deposits
Preventing calculus buildup is significantly easier and less costly than treating it. A proactive approach to oral hygiene and lifestyle choices is key.
1. Meticulous Oral Hygiene Routine
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes each time, covering all tooth surfaces (front, back, chewing surfaces) and paying special attention to the gum line. Consider using an electric toothbrush, as many studies show they are more effective at removing plaque.
- Floss Daily: This is non-negotiable for preventing calculus between teeth and below the gum line. Proper flossing technique is crucial: curve the floss against each tooth in a "C" shape and gently slide it under the gum line.
- Antimicrobial Mouthwash: An over-the-counter antiseptic mouthwash can help reduce plaque bacteria, but it should be used as an addition to, not a replacement for, brushing and flossing.
2. Regular Dental Check-ups and Cleanings
- Every Six Months: Schedule and attend professional dental cleanings and examinations every six months, or more frequently if recommended by your dentist (e.g., every 3-4 months for those with a history of gum disease). These appointments allow dental professionals to remove any nascent plaque and calculus before it becomes problematic.
3. Healthy Diet
- Limit Sugary and Starchy Foods/Drinks: Reduce your intake of candies, cookies, sodas, and refined carbohydrates. These fuel plaque-forming bacteria.
- Increase Fibrous Foods: Crunchy fruits and vegetables like apples and carrots can act as natural tooth scrubbers, stimulating saliva and helping to clean teeth between meals.
- Water Intake: Drink plenty of water, especially after meals, to help rinse away food particles and neutralize acids.
4. Avoid Tobacco Products
- Quitting smoking or other tobacco use is one of the most effective ways to reduce calculus formation and improve overall gum health.
5. Toothpaste Choices
- Tartar-Control Toothpaste: Look for toothpastes that contain ingredients like pyrophosphates or zinc citrate. These compounds help inhibit the mineralization of plaque into calculus. While they can help prevent new calculus, they cannot remove existing deposits.
- Fluoride Toothpaste: Fluoride strengthens enamel and helps prevent cavities, which is a related but distinct benefit from tartar control.
6. Dental Sealants (Especially for Molars)
- While primarily for preventing cavities, sealants can make molar surfaces smoother and easier to clean, indirectly reducing areas where plaque and calculus can accumulate. This is especially relevant when discussing "molar erosion," as healthy sealed molars are easier to maintain.
Pro Tip: Consistency is key. A diligent daily routine, combined with professional care, is your best defense against calcium deposits and the associated dental problems.
Risks and Complications of Untreated Calcium Deposits
Ignoring calcium deposits on your teeth can lead to a cascade of serious oral health problems, extending beyond mere aesthetics.
1. Gum Disease (Gingivitis to Periodontitis)
- Gingivitis: Calculus, particularly when it forms along and under the gum line, constantly irritates the soft gum tissue. This leads to gingivitis, characterized by red, swollen, tender, and easily bleeding gums. Gingivitis is reversible with professional cleaning and improved oral hygiene.
- Periodontitis: If gingivitis is left untreated, the inflammation progresses. The bacterial toxins from plaque and calculus destroy the fibers that attach the gums to the teeth, creating periodontal pockets. These pockets become deeper and harbor more bacteria and calculus. The infection then spreads to the underlying bone, leading to bone loss around the teeth. This advanced stage is called periodontitis, which is irreversible and can ultimately lead to tooth loss.
2. Tooth Decay (Cavities)
- Calculus provides a rough, porous surface where plaque can easily accumulate and thrive. The bacteria in plaque produce acids that erode tooth enamel, leading to cavities. Since calculus often forms near the gum line, it can contribute to root surface decay if gums have receded.
3. Bad Breath (Halitosis)
- The vast number of bacteria trapped within the porous structure of calculus, especially subgingival calculus, release foul-smelling gases (volatile sulfur compounds), leading to chronic and persistent bad breath that cannot be masked by mouthwash.
4. Tooth Loss
- The most severe complication of untreated periodontitis (caused by calculus) is tooth loss. As the supporting bone and ligaments are progressively destroyed, teeth become loose and eventually fall out or need to be extracted.
5. Aesthetic Concerns
- Calculus is unsightly, appearing yellow, brown, or black, especially when stained by food, drinks, or tobacco. It can significantly detract from the appearance of your smile and affect self-confidence.
6. Systemic Health Connections
- Research increasingly points to a link between chronic inflammation from gum disease (driven by calculus) and various systemic health issues, including:
- Cardiovascular Disease: Periodontal inflammation may contribute to arterial plaque buildup.
- Diabetes: Periodontitis can make blood sugar control more difficult, and uncontrolled diabetes can worsen gum disease.
- Respiratory Infections: Bacteria from the mouth can be aspirated into the lungs, potentially contributing to pneumonia or bronchitis.
- Adverse Pregnancy Outcomes: Gum disease has been linked to preterm birth and low birth weight.
Comparison Table: Calculus vs. Enamel Erosion
| Feature | Calcium Deposits (Calculus/Tartar) | Enamel Erosion (Molar Erosion/Teeth Erosion) |
|---|---|---|
| Nature of Problem | Hardened buildup on tooth surfaces | Irreversible loss of tooth structure (enamel) |
| Primary Cause | Mineralized dental plaque due to inadequate hygiene | Acidic attacks on tooth enamel |
| Appearance | Yellow, brown, or black rough deposits | Smooth, shiny, "scooped out" appearance, sometimes dull |
| Texture | Rough, gritty, chalky | Smooth, potentially glassy or concave |
| Location | Near gum line, between teeth, salivary gland openings | Chewing surfaces, smooth surfaces, especially near gums |
| Detection | Visible, felt with tongue, detected by dentist's explorer | Visual inspection, often detected by increased sensitivity |
| Key Symptoms | Gum inflammation, bad breath, rough feeling | Tooth sensitivity, discoloration, changes in tooth shape |
| Treatment | Professional scaling and root planing | Fluoride treatments, bonding, crowns, dietary changes |
| Prevention | Brushing, flossing, regular cleanings, tartar-control toothpaste | Reduce acidic foods/drinks, rinse with water, fluoride |
| Risk of Tooth Loss | High (via periodontitis) | High (via progressive wear and sensitivity) |
Children / Pediatric Considerations
While often associated with adults, calcium deposits (calculus) can and do occur in children. The reasons are similar to adults, but with some specific considerations for pediatric dental health.
- Prevalence: Calculus is less common in very young children but can become more prevalent during adolescence, especially as permanent teeth erupt. Studies indicate that prevalence in children can range from 5% to 30% depending on age and population studied.
- Causes in Children:
- Inadequate Brushing and Flossing: Children may not have the manual dexterity or discipline to brush and floss effectively, leading to plaque accumulation. Parents need to supervise and assist with oral hygiene until children are around 7-8 years old.
- Diet: A diet high in sugary snacks, juices, and soft drinks contributes to plaque formation, even if these foods are associated more with cavities, they indirectly lead to calculus risk.
- Mouth Breathing: Children who breathe primarily through their mouth (due to allergies, adenoid issues, etc.) can experience dry mouth, which may alter saliva composition and increase calculus risk in specific areas.
- Orthodontic Appliances: Braces create numerous traps for food and plaque, making oral hygiene challenging for children and significantly increasing their risk for calculus and white spots (early enamel demineralization).
- Signs in Children: Similar to adults, parents might notice yellowish or brownish buildup near the gum line, especially on lower front teeth or upper back molars. Gums might appear red or bleed during brushing.
- Treatment: Professional dental cleanings are the primary treatment. Pediatric dentists and hygienists are trained to work with children, using gentle techniques and often child-friendly tools. If significant calculus and gingivitis are present, deep cleaning might be necessary, though less common than in adults.
- Prevention in Children:
- Parental Involvement: Parents are key. Help children brush and floss until they can do it proficiently.
- Education: Teach children about the importance of oral hygiene from a young age.
- Regular Dental Visits: Schedule routine check-ups and cleanings with a pediatric dentist every six months. These visits allow for early detection and professional removal of plaque and calculus.
- Dietary Guidance: Encourage healthy eating habits and limit sugary snacks and drinks.
- Fluoride: Ensure children are using fluoride toothpaste and receiving adequate fluoride exposure (e.g., fluoridated water, fluoride treatments at the dentist) to strengthen enamel and prevent cavities.
- Sealants: Dental sealants on permanent molars can prevent plaque and food from getting trapped in the deep grooves, indirectly reducing calculus risk.
Cost Breakdown for Calculus Treatment (US)
To provide a clearer picture, here's a detailed breakdown of potential costs for professional calculus removal in the US, along with considerations for insurance and payment.
| Procedure Type | ADA Code | Average US Cost (Without Insurance) | Average US Cost (With Insurance - Patient Portion) |
|---|---|---|---|
| Routine Cleaning (Prophylaxis) | D1110 | $75 - $200 | $0 - $50 (Often 100% covered) |
| Scaling & Root Planing (Per Quadrant) | D4341 | $250 - $800 | $50 - $400 (Typically 50-80% covered) |
| Full Mouth Deep Cleaning | D4341 x 4 | $1,000 - $3,200 | $200 - $1,600 |
| Periodontal Maintenance (Post-SRP) | D4910 | $100 - $300 | $20 - $150 (Often 80-100% covered) |
| Local Antibiotic Placement (Per Site) | D4381 | $30 - $100 | $10 - $50 |
| Prescription Antimicrobial Rinse | N/A | $20 - $50 | $0 - $20 (If covered by medical/dental) |
Key Cost Considerations:
-
Insurance Coverage:
- Preventive Care (D1110): Most dental insurance plans prioritize preventive care, covering routine cleanings at 100% (often two per year). This is because preventing problems is cheaper than treating them.
- Basic/Major Restorative (D4341, D4910): Scaling and root planing and subsequent periodontal maintenance are often considered basic or major procedures. Coverage for these usually ranges from 50% to 80% after your deductible has been met.
- Deductibles: This is the amount you must pay out-of-pocket before your insurance begins to cover costs. Common deductibles range from $50 to $150 per year.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit, typically ranging from $1,000 to $2,500. Once you reach this limit, you are responsible for 100% of further costs until the next plan year. Deep cleanings can quickly exhaust an annual maximum.
-
Payment Plans and Financing Options:
- In-Office Plans: Many dental practices offer their own payment plans, allowing you to pay in installments.
- Third-Party Financing: Services like CareCredit or Alphaeon Credit offer specialized healthcare credit cards with deferred interest options if paid within a certain timeframe.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these tax-advantaged accounts to pay for dental treatments.
-
Cost-Saving Tips Revisited:
- Prevention: The single most effective cost-saving measure is diligent oral hygiene to prevent calculus and the need for expensive deep cleanings.
- In-Network Providers: Choose a dentist who is in-network with your insurance plan to receive the highest level of coverage.
- Compare Costs: Don't hesitate to call a few dental offices in your area to inquire about their fees for specific procedures.
- Dental Discount Plans: These are not insurance but offer a reduced fee for services with participating dentists, often for an annual membership fee.
Frequently Asked Questions
Is "calcium deposits on teeth" the same as plaque?
No, they are related but distinct. Plaque is a soft, sticky film of bacteria that constantly forms on your teeth. If plaque is not removed, minerals from your saliva cause it to harden into calcium deposits, which is medically known as calculus or tartar. Calculus is plaque that has calcified.
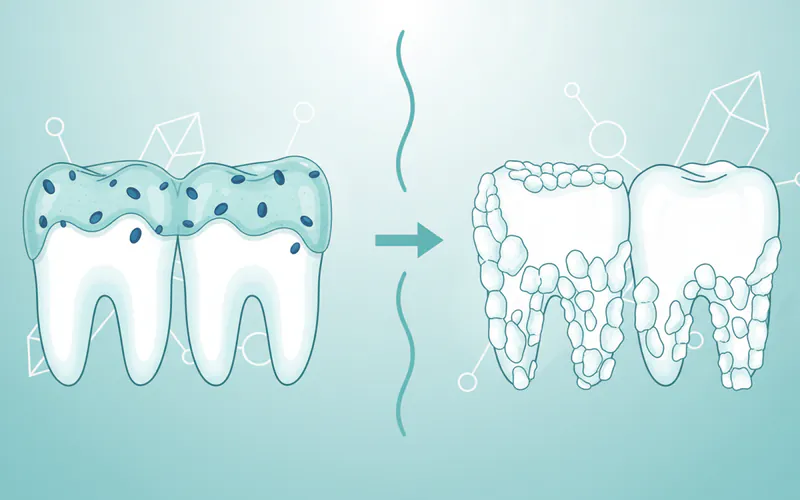
Can I remove calcium deposits myself at home?
No, once plaque has hardened into calculus, it is impossible to remove with a toothbrush, floss, or any over-the-counter tools. Attempting to scrape it off yourself can damage your tooth enamel and gums, leading to more serious issues. Professional scaling by a dentist or hygienist is the only safe and effective method.
How often should I get my teeth professionally cleaned to prevent calculus?
For most individuals, a professional dental cleaning every six months is recommended to remove plaque and calculus and maintain gum health. However, if you are prone to rapid calculus buildup or have a history of gum disease, your dentist might recommend more frequent cleanings, such as every three or four months.
Do tartar-control toothpastes really work?
Tartar-control toothpastes, which contain ingredients like pyrophosphates or zinc citrate, can help slow down the mineralization of new plaque into calculus. They are effective at preventing new calculus formation but cannot remove existing, hardened calculus deposits. They are a good preventive measure but not a treatment for existing buildup.
What's the difference between calculus and cavities?
Calculus is a mineralized buildup on the tooth surface. Cavities, or tooth decay, are structural damage to the tooth (holes) caused by acids produced by bacteria breaking down enamel. While calculus can harbor bacteria that cause cavities, they are different issues.
Does dental insurance cover deep cleaning (scaling and root planing)?
Yes, most dental insurance plans do cover scaling and root planing, but usually at a lower percentage than routine cleanings, often 50% to 80% after you meet your annual deductible. You will typically be responsible for a co-pay and a portion of the remaining cost, and the procedure can quickly exhaust your annual maximum benefit.
Is the deep cleaning procedure painful?
During scaling and root planing, your dentist or hygienist will typically use local anesthesia to numb the treated area, making the procedure comfortable. You might feel some pressure or vibrations. After the anesthesia wears off, it's normal to experience some temporary soreness, tenderness, and sensitivity for a few days, which can usually be managed with over-the-counter pain relievers.
Can calcium deposits cause bad breath?
Yes, absolutely. Calculus has a rough, porous surface that traps bacteria and food particles. These bacteria release volatile sulfur compounds, which are the primary cause of persistent and unpleasant bad breath (halitosis). Professional removal of calculus often significantly improves bad breath.
When to See a Dentist
Recognizing the signs and knowing when to seek professional dental care is critical for preventing calcium deposits from causing irreversible damage.
Schedule a routine check-up and cleaning if:
- You notice any yellowish or brownish deposits on your teeth, especially near the gum line or on the inner surfaces of your lower front teeth.
- Your gums appear slightly red or swollen, or bleed minimally when you brush or floss.
- You feel a rough texture on your teeth with your tongue.
- It's been six months or more since your last professional dental cleaning.
See a dentist promptly (within a few days to a week) if:
- Your gums are noticeably red, swollen, tender, or bleed consistently and heavily during brushing or flossing. These are signs of worsening gingivitis or early periodontitis.
- You experience persistent bad breath that doesn't improve with brushing and flossing.
- You notice your gums pulling away from your teeth (receding gums), making your teeth appear longer.
- Your teeth feel sensitive to hot, cold, or sweet stimuli, which could indicate exposed root surfaces due to gum recession or early enamel erosion.
- You have a persistent metallic taste in your mouth.
Seek immediate dental attention (emergency appointment) if:
- You notice any of your teeth becoming loose or shifting position. This is a severe sign of advanced periodontitis and significant bone loss, requiring urgent intervention to potentially save the tooth.
- You experience severe, throbbing pain in your gums or teeth accompanied by swelling, fever, or pus, as this could indicate a dental abscess or severe infection requiring immediate treatment.
Regular visits to your dentist for preventive care are the best way to detect and address calcium deposits and other oral health concerns before they escalate. Don't wait until discomfort forces you to seek care; proactive maintenance ensures a healthy, confident smile for years to come.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Calcium Good for Teeth: Complete Guide
More than 99% of your body's calcium resides in your bones and teeth, making it an undeniable cornerstone of skeletal and oral health. But did you know that an estimated 42% of American adults don't get enough calcium from their diet? This staggering statistic underscores a critical question
February 23, 2026
What Do Bulimia Teeth Look Like
"Bulimia teeth" refers to the specific and often severe damage that the self-induced vomiting characteristic of bulimia nervosa inflicts on a person's oral health. It's a critical issue, affecting approximately 1.5% of women and 0.5% of men in the US at some point in their lives, with many more
February 23, 2026

Erosion in Teeth: Complete Guide
Erosion in Teeth: Complete Guide
February 23, 2026
Do Teeth Have Calcium
When you flash a confident smile, what are you truly showing? Many people might assume their teeth are solid, unchanging structures made primarily of bone, or even pure calcium. But do teeth have calcium? The answer is a resounding yes, though not in the simplistic way some might imagine. Calciu
February 23, 2026